5 results
From contact coverage to effective coverage of community care for patients with severe mental disorders: a real-world investigation from Italy. Methodology and results from the QUADIM project
- M. Monzio Compagnoni, G. Corrao, A. Barbato, B. D’Avanzo, T. Di Fiandra, F. Carle, L. Ferrara, V. D. Tozzi, A. Gaddini, A. Saponaro, S. Scondotto, D. Chisholm, A. Lora
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S66-S67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The evaluation of healthcare pathways must be considered of fundamental importance. The quality of care provided to patients with severe mental disorders (SMD) does not correspond to the standards set by the recommendations. Therefore, measures such as the real coverage rate of psychiatric patients’ needs (contact coverage), by comparing epidemiological prevalence rates and the number of patients receiving adequate care, could be a valuable resource for implementing the transition to community mental health. However, simple assessment and reporting of rates of contact with mental healthcare potentially overestimate the full expected health benefits of services. Therefore, in addition to monitor the coverage rate achieved by the services, the evaluation of the effectiveness of the care provided (effective coverage) [De Silva et al. Int J Epidemiol 2014;43(2):341–53] is also of relevant importance.
ObjectivesTo measure the gap between contact and effective coverage of mental healthcare, i.e., the effectiveness of interventions provided by services for the treatment of SMD in preventing an exacerbation of psychiatric symptoms.
MethodsData were retrieved from Healthcare Utilization databases of four Italian Regions (Lombardy, Emilia-Romagna, Lazio, Sicily). 45,761 newly taken-in-care cases of depression, schizophrenia, bipolar, and personality disorder were included. A variant of the self-controlled case series method was used to estimate the incidence rate ratio (IRR) for the relationship between exposure (use of different types of mental healthcare such as pharmacotherapy, generic contacts with the outpatient service, psychosocial interventions, and psychotherapies) and relapse episodes (mental illness emergency hospital admissions).
Results11,500 relapses occurred. Relapse risk was reduced (Figure) during periods covered by (i) psychotherapy for patients with depression (IRR 0.67; 95% CI, 0.49 to 0.91) and bipolar disorder (0.64; 0.29 to 0.99); (ii) psychosocial interventions for those with depression (0.74; 0.56 to 0.98), schizophrenia (0.83; 0.68 to 0.99) and bipolar disorder (0.55; 0.36 to 0.84), (iii) pharmacotherapy for those with schizophrenia (0.58; 0.49 to 0.69), and bipolar disorder (0.59; 0.44 to 0.78). Coverage with generic mental healthcare, in the absence of psychosocial/psychotherapeutic interventions, did not affect the risk of relapse.
Image:
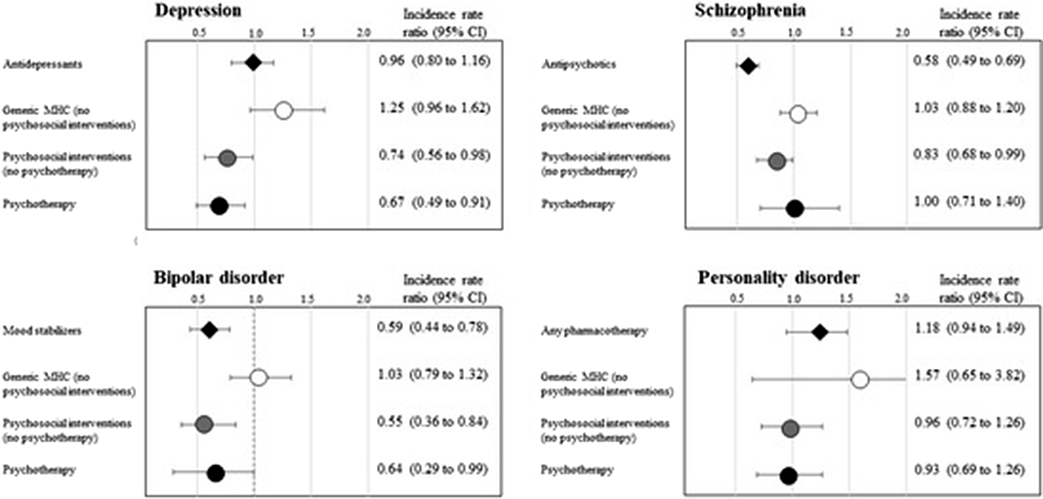 Conclusions
ConclusionsPsychosocial interventions, psychotherapies and specific pharmacotherapies can be considered particularly effective in treating patients with bipolar, depressive, and schizophrenic disorders. This study ascertained the gap between utilization of mental healthcare and effective coverage, showing that real-world data can represent a useful resource to monitor mental healthcare paths and to assess the effectiveness of a mental health system.
Disclosure of InterestNone Declared
Monitoring of Essential Levels of mental healthcare during the Covid-19 epidemic outbreak. Evidence from an Italian Real-World study
- G. Caggiu, M. Monzio Compagnoni, G. Corrao, M. Franchi, A. Lora
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S402-S403
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental healthcare proved to have experienced a clear-cut reduction during the Covid-19 outbreak, and its responsiveness to patients’ health needs showed relevant declines. Moreover, the impact of the pandemic on usual outpatient healthcare has never been systematically measured with a person-level approach in analytical studies.
ObjectivesTo assess how the access to, and the delivery of, recommended healthcare for patients with severe mental illness has changed during the Covid-19 pandemic.
MethodsData were retrieved from the HCU of Lombardy Region (Italy), and a population-based study estimated the association between the level of epidemic restrictions (free, severe, light and moderate) and the recommended healthcare provided (outcome) to patients with schizophrenic and depressive disorders. For each disorder, prevalent and incident patients in the year 2019 were identified. These patients were then observed from 1st January 2020 to December 31, 2020. A Self-Controlled Case Series (SCCS) design was applied, and estimates were obtained with a conditional Poisson regression model. Adjustments for seasonality of medical services delivering were performed (SCC-RS design, with recruitment of a specific reference cohort in 2018, evaluated in 2019). The estimates were stratified according to gender, age and comorbidity profile of the patients included.
ResultsPatients with prevalent schizophrenic disorder were 29,516 (Prevalence Rate=35.5x10’000 inhabitants, Image 1), 292 with incident disorder; patients with prevalent depressive disorder were 37,764 (PR=45.4, Image 2), 4,349 with incident disorder. The largest reductions were observed in the rate of psychosocial interventions delivery during the period of exposure to severe restrictions (IRR: 0.35; 95% CI: 0.34 - 0.36 for patients with schizophrenic disorder and 0.49; 0.45 - 0.53 for patients with depression, Image 3), compared to the pre-pandemic period. For patients with incident disorder, the largest reduction concerned the delivery of psychoeducational interventions during the period of exposure to moderate restrictions (0.19; 0.06 - 0.64 for patients with schizophrenic disorder and 0.27; 0.13 - 0.55 for patients with depressive disorder), compared to the pre-pandemic period.
Image:
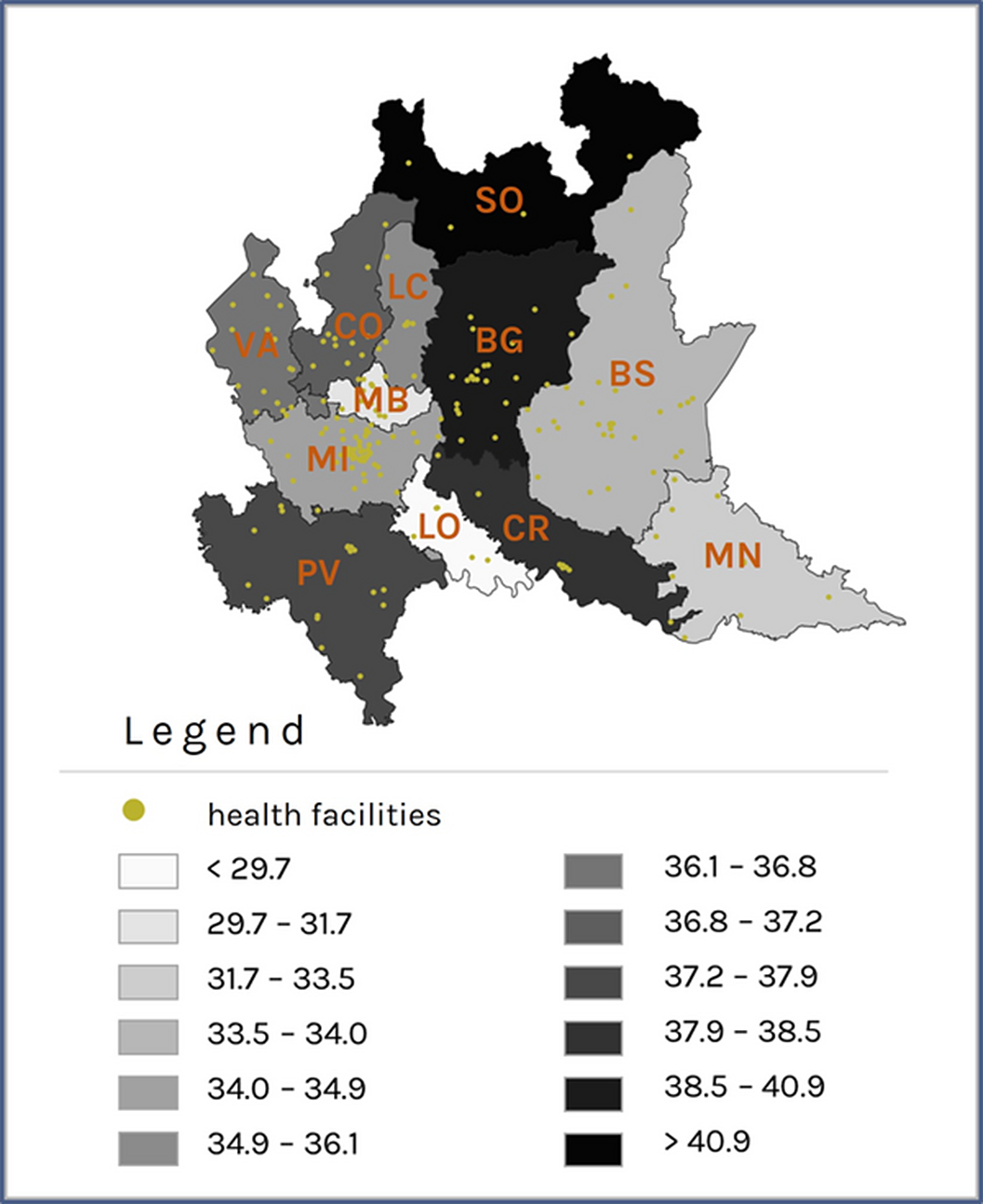
Image 2:
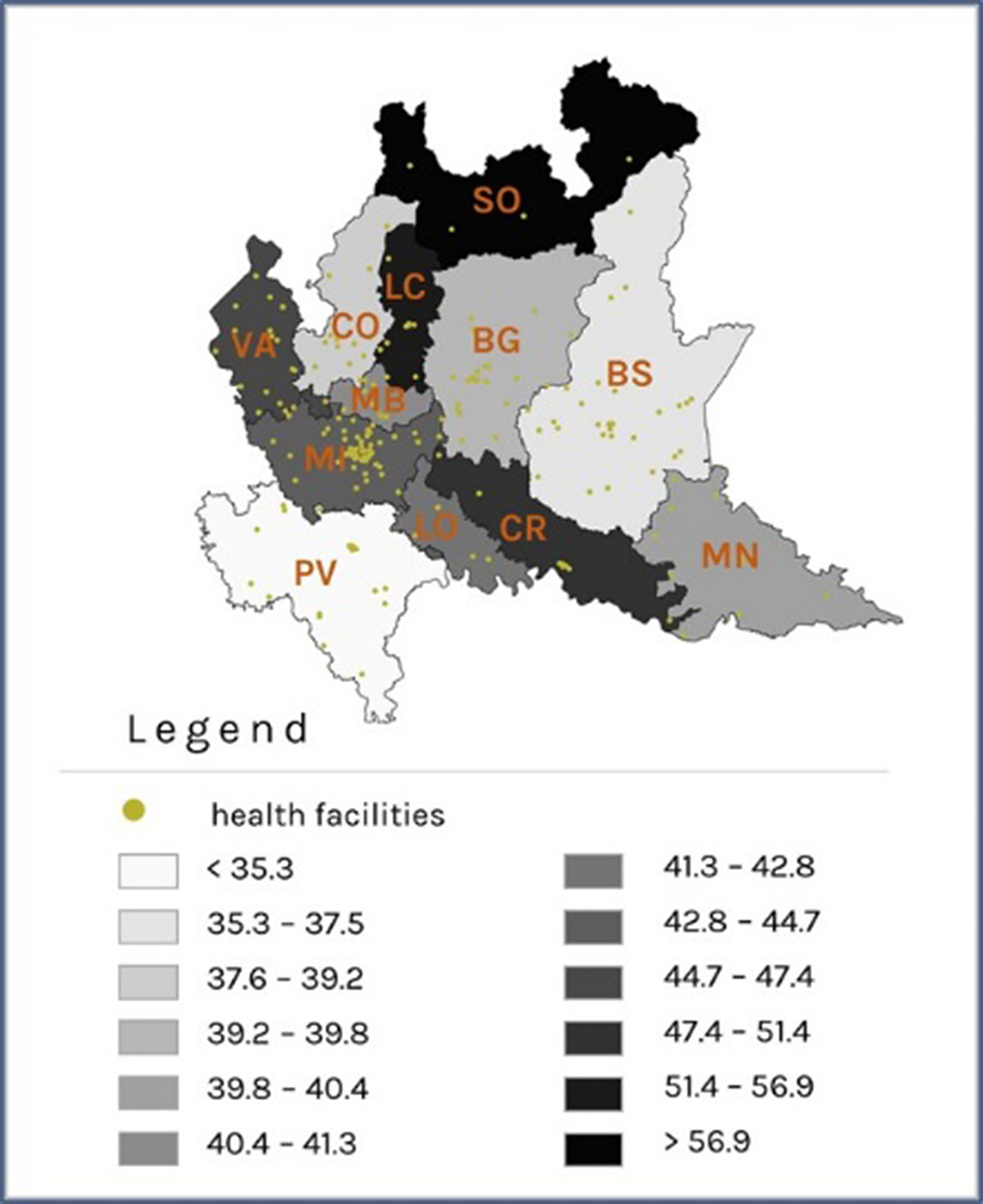
Image 3:
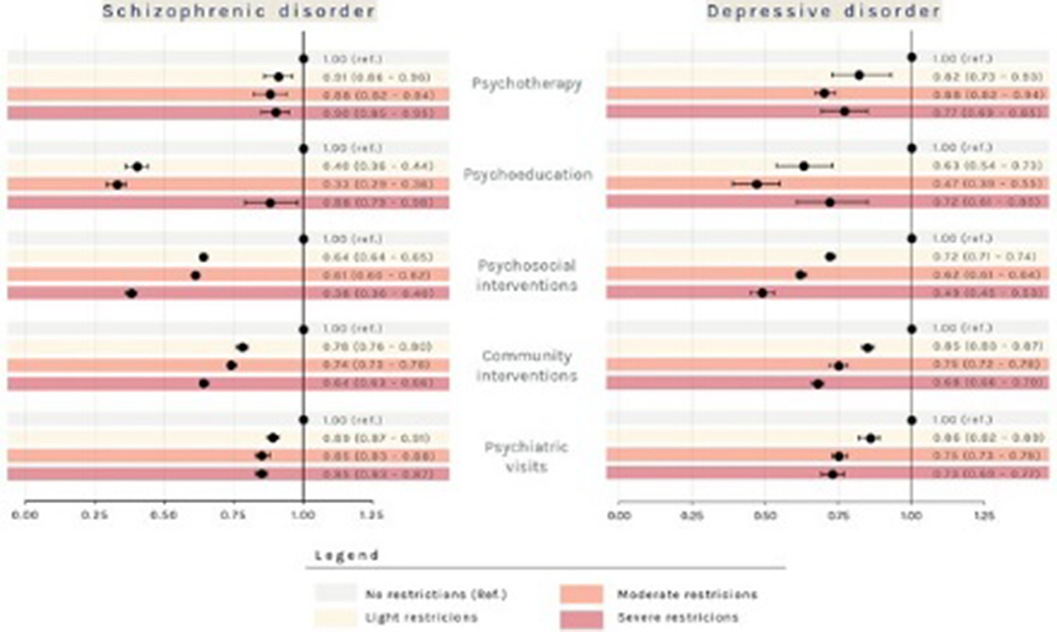 Conclusions
ConclusionsReal-world data can be used to assess how the individual access to psychiatric recommended healthcare changed during the Covid-19 epidemic. Also, compared to the pre-pandemic period, there was a general reduction in the delivery of recommended interventions to patients with mental disorders during the pandemic period.
Disclosure of InterestNone Declared
The quality of mental health care delivered to patients with schizophrenic disorder in the Italian mental health system. The QUADIM project A multi-regional Italian investigation based on healthcare utilization databases
- M. Monzio Compagnoni, G. Corrao, L. Allevi, A. Barbato, B. D’Avanzo, F. Carle, A. Saponaro, A. Gaddini, S. Scondotto, L. Ferrara, V. D. Tozzi, T. Di Fiandra, A. Lora
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S486
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The 1978 Italian reform of psychiatric services initiated the closure of psychiatric hospitals encouraging the development of community mental health. However, there is wide variability across regions in the amount of resources devoted to community-based psychiatric care, and the range of services provided still is cause of concern.
ObjectivesTo evaluate the quality of mental health care delivered to patients with schizophrenia and related disorders taken-in-care by mental health services in four Italian regions (Lombardy, Emilia-Romagna, Lazio, Sicily).
MethodsThirty-one clinical indicators concerning accessibility, appropriateness, continuity, and safety were defined and estimated using healthcare utilization (HCU) databases, containing data on mental health treatments, hospital admissions, outpatient interventions, lab tests and drug prescriptions.
ResultsA total of 70,586 prevalent patients with schizophrenia treated in 2015 were identified, of whom 1,752 were newly taken-in-care. For most patients community care was accessible and moderately intensive. However, care pathways were not implemented based on a structured assessment and only half of the patients received psychosocial treatments. One patient out of ten had access to psychological interventions and psychoeducation. Activities specifically addressed to families involved a third of prevalent patients and less than half of new patients. One patient out of six was admitted to a community residential facility, and one out of ten to a general hospital psychiatric ward (GHPW); higher values were identified in new cases. In general hospitals, one-fifth of the admissions were followed by readmission within 30 days of discharge. For two- thirds of patients continuity of community care was met, and six times out of ten a discharge from a GHPW was followed by an outpatient contact within two weeks. For cases newly taken-in-care the continuity of community care was uncommon, while the readiness of outpatient contacts after discharge was slightly more frequent. Most of the patients received antipsychotic medication, but their adherence to long-term treatment was low. Antipsychotic polytherapy was frequent and the control of metabolic side effects was poor. The variability between regions was high and consistent.
ConclusionsThe Italian mental health system could be improved by increasing the accessibility to psychosocial interventions, improving the quality of care for newly taken-in-care patients, focusing on somatic health and mortality, and reducing regional variability. Clinical indicators demonstrate the strengths and weaknesses of the mental health system in these regions, and, as HCU databases, they could be useful tools in the routine assessment of mental healthcare quality at regional and national levels.
Disclosure of InterestNone Declared
Organizational features of mental health facilities and adequacy of treatment. Multilevel analysis from the italian region lombardy
- C. Conflitti, M. Monzio Compagnoni, A. Lora, G. Corrao
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S170-S171
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental healthcare represents a significant issue for the Healthcare System [1]: one of the major causes is the high heterogeneity in the provision of care, due to the differences among the Departments of Mental Health (DMHs).
ObjectivesTo identify the predictors of an adequate treatment for patients with severe mental disorders (SMDs), both at an individual and structural level, the latter considering the major features of the Psychiatric Operative Units (POUs), in the Italian region Lombardy.
MethodsHealthcare Utilization Databases, collecting data on the services provided to beneficiaries of the National Health Service (NHS), have been used to retrieve data.
Patients that during 2015 were resident in Lombardy; suffered from depressive, bipolar or schizophrenic disorder; were in contact with the DMHs, have been identified.
Adequateness of treatment has been evaluated according to the Minimally Adequate Treatment (MAT) [2,3]: a combination of psychiatric visits and specific pharmacological treatment, or psychotherapeutic sessions. Having received a MAT has been assessed during a one-year period.
Predictive factors have been classified into two hierarchical levels: individual (first) level and structural (second) level. At the first level, clinical and socio-demographics characteristics have been evaluated for each patient. At the second level, the organizational structure of each POU has been examined: the number of patients taken in care, number of community-care facilities, and hours worked by each class of healthcare providers (psychiatrists, nurses, psychologists, psychosocial staff).
A log-binomial model has been used to evaluate the association between the first-level factors and having received a MAT; a multilevel log-binomial model for the second-level factors considered the hierarchical structure of data.
Results72115 patients have been identified: 33974 (47.1%), 28407 (39.4%) and 9734 (13.5%) suffering from depressive, schizophrenic or bipolar disorder respectively; 45.4% of them (32773 patients) received a MAT.
Compared with patients affected by depression, those with bipolar or schizophrenic disorder show a higher probability of receiving a MAT (+23%, +11% respectively).
Patients living alone have a lower probability of receiving a MAT, unlike patients with a higher level of education or employment, underlining the social burden related to SMDs.
Organizational features have proven significant: centres with a higher activity volume and with more community-care facilities seem more likely to guarantee MAT. Moreover, the higher the hours worked by psychiatrists, nurses and psychologists, the higher the probability of providing MAT.
ConclusionsPatients with SMDs are still untreated in an appropriate way. Results highlight the importance of the community-care facilities, as well as of the composition of the multidisciplinary teams working there.
Disclosure of InterestNone Declared
Coping with COVID: risk and resilience factors for mental health in a German representative panel study
- Antje Riepenhausen, Ilya M. Veer, Carolin Wackerhagen, Zala C. Reppmann, Göran Köber, José Luis Ayuso-Mateos, Sophie A. Bögemann, Giovanni Corrao, Mireia Felez-Nobrega, Josep Maria Haro Abad, Erno Hermans, Judith van Leeuwen, Klaus Lieb, Vincent Lorant, Murielle Mary-Krause, Roberto Mediavilla, Maria Melchior, Ellenor Mittendorfer-Rutz, Matteo Monzio Compagnoni, Kuan-Yu Pan, Lara Puhlmann, Karin Roelofs, Marit Sijbrandij, Pierre Smith, Oliver Tüscher, Anke Witteveen, Matthias Zerban, Raffael Kalisch, Hannes Kröger, Henrik Walter
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 9 / July 2023
- Published online by Cambridge University Press:
- 01 March 2022, pp. 3897-3907
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
The coronavirus disease 2019 (COVID-19) pandemic might affect mental health. Data from population-representative panel surveys with multiple waves including pre-COVID data investigating risk and protective factors are still rare.
MethodsIn a stratified random sample of the German household population (n = 6684), we conducted survey-weighted multiple linear regressions to determine the association of various psychological risk and protective factors assessed between 2015 and 2020 with changes in psychological distress [(PD; measured via Patient Health Questionnaire for Depression and Anxiety (PHQ-4)] from pre-pandemic (average of 2016 and 2019) to peri-pandemic (both 2020 and 2021) time points. Control analyses on PD change between two pre-pandemic time points (2016 and 2019) were conducted. Regularized regressions were computed to inform on which factors were statistically most influential in the multicollinear setting.
ResultsPHQ-4 scores in 2020 (M = 2.45) and 2021 (M = 2.21) were elevated compared to 2019 (M = 1.79). Several risk factors (catastrophizing, neuroticism, and asking for instrumental support) and protective factors (perceived stress recovery, positive reappraisal, and optimism) were identified for the peri-pandemic outcomes. Control analyses revealed that in pre-pandemic times, neuroticism and optimism were predominantly related to PD changes. Regularized regression mostly confirmed the results and highlighted perceived stress recovery as most consistent influential protective factor across peri-pandemic outcomes.
ConclusionsWe identified several psychological risk and protective factors related to PD outcomes during the COVID-19 pandemic. A comparison of pre-pandemic data stresses the relevance of longitudinal assessments to potentially reconcile contradictory findings. Implications and suggestions for targeted prevention and intervention programs during highly stressful times such as pandemics are discussed.







