2 results
Eating cognitions, emotions and behaviour under treatment with second generation antipsychotics: A systematic review and meta-analysis
- H. Mutwalli, J. L. Keeler, S. Bektas, N. Dhopatkar, J. Treasure, H. Himmerich
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S71-S72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Weight gain and metabolic disturbances are frequent in people treated with second generation antipsychotics (SGA).
ObjectivesWe aimed to investigate the effect of SGAs on eating behaviors, cognitions and emotions, as a possible contributor to weight gain and metabolic disturbances.
MethodsA systematic review and meta-analysis was conducted following the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines. Original articles measuring outcomes relating to eating cognitions, behaviours and emotions, during treatment with SGAs were included in this review. A total of 92 papers with 11,274 participants were included from three scientific databases (PubMed, Web of Science and PsycInfo). Results were synthesized descriptively except for the continuous data where meta-analyses were performed and for the binary data where odds ratios were calculated.
ResultsHunger was increased in participants treated with SGAs with an odds ratio for appetite increase of 1.51 (95% CI [1.04, 1.97]; z=6.40; p<0.001)(see Figure 1.). Compared to controls, our results showed that craving for fat and carbohydrates are the highest among other craving subscales. There was a small increase in dietary disinhibition (SMD=0.40) and restrained eating (SMD=0.43) in participants treated with SGAs compared to controls and substantial heterogeneity across studies reporting these eating traits (See figure 2 and 3). There were few studies examining other eating-related outcomes such as food addiction, satiety, fullness, caloric intake and dietary quality and habits.
Image:
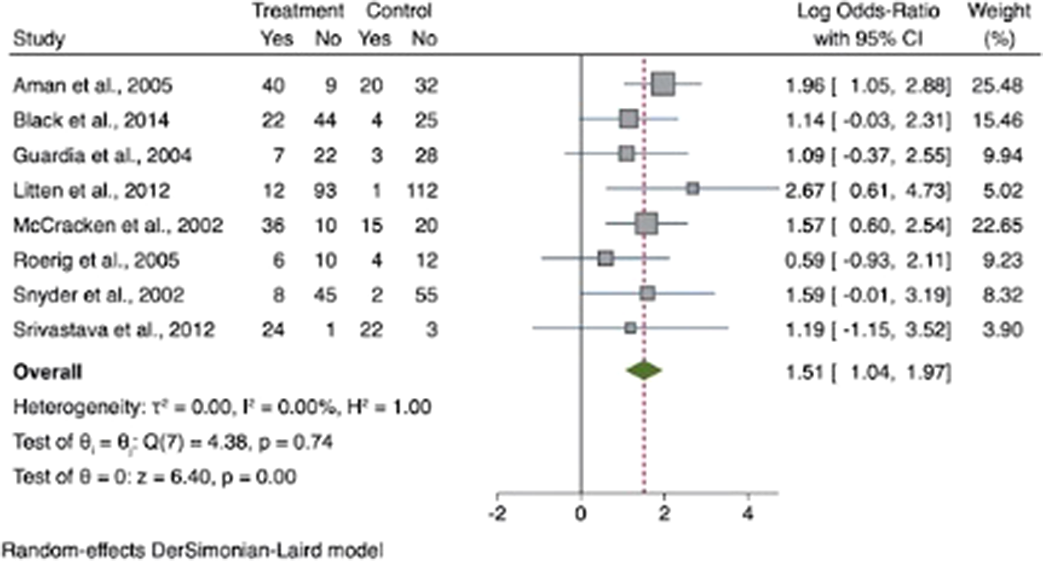
Image 2:
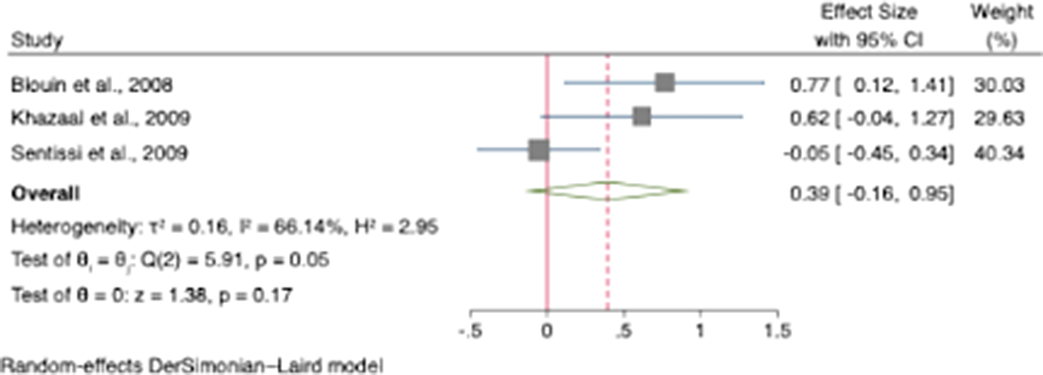
Image 3:
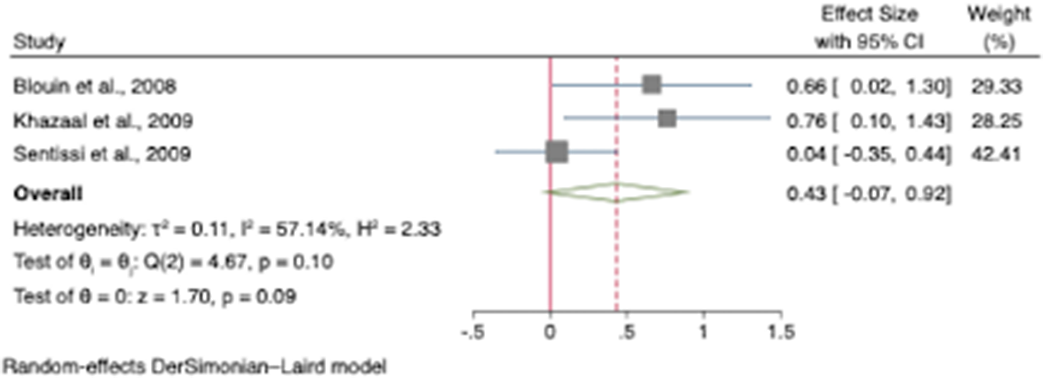 Conclusions
ConclusionsUnderstanding the mechanisms associated with appetite and eating-related psychopathology changes in patients treated with antipsychotics is needed to reliably inform the development of effective preventative strategies.
Disclosure of InterestH. Mutwalli Grant / Research support from: The Saudi Arabian Government Educational Sponsorship for PhD, J. Keeler Grant / Research support from: The Medical Research Council, S. Bektas Grant / Research support from: The Turkish Ministry of National Education for PhD training, N. Dhopatkar Employee of: South London and Maudsley NHS Foundation Trust (SLaM), J. Treasure Grant / Research support from: The National Institute for Health Research (NIHR) Biomedical Research Centre (BRC) at the South London and Maudsley NHS Foundation Trust (SLaM), Employee of: King’s College London, H. Himmerich Grant / Research support from: The National Institute for Health Research (NIHR) Biomedical Research Centre (BRC) at the South London and Maudsley NHS Foundation Trust (SLaM), Employee of: King’s College London.
A review of mechanistic and clinical evidence for the use of probiotics and prebiotics in anorexia nervosa
- N. Dhopatkar, J. L. Keeler, H. Mutwalli, K. Whelan, H. Himmerich, J. Treasure
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S852
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Evidence is growing for the bio-immuno-metabolic model of pathogenesis in anorexia nervosa (AN), an eating disorder with a chronic and relapsing nature. The role of the gut microbiome in this process is also receiving intense research interest. The gut microbiome and the use of probiotics and prebiotics have been extensively studied in gastrointestinal (GI) disorders such as inflammatory bowel disease (IBD) and functional GI disorders (FGIDs). Exploring links between AN and these GI disorders may open new avenues of treatment such as the use of probiotics and prebiotics in AN.
ObjectivesThis review explores: i) GI presentation in AN and its relationship with the gut microbiome ii) factors influencing the gut microbiome presentation in AN including dietary patterns iii) whether the gut microbiome may be involved in the pathogenesis and maintenance of AN iv) gut microbiome presentation in GI disorders and commonalities with AN v) evidence for the potential use of probiotics and prebiotics as adjunct treatment in AN.
MethodsGI symptomatology and gut microbiome presentation in AN were examined through literature searches. Gut microbiome changes related to common dietary patterns in AN were explored. Microbiome changes that may influence development or maintenance of AN were considered. Microbiome alterations seen in relevant GI disorders were explored and commonalities considered between these and alterations in the microbiome in AN. Literature searches were performed for the use of probiotics and prebiotics in AN and relevant GI disorders.
ResultsGI symptoms occur commonly in AN with evidence suggesting some symptoms continuing beyond weight restoration. Significant disruption of the gut microbiome has been associated with AN with some changes related to typical dietary patterns seen during AN development. Additionally, similarities exist between microbiome alterations in AN and those seen in IBD and FGIDs indicating factors apart from the diet, such as a pro-inflammatory milieu, in play. These changes may not only influence GI presentation in AN but may also have a role in maintenance of the disorder. Some evidence suggests that the pre-morbid gut microbiome may influence risk for AN development. Preliminary evidence of the use of probiotics in AN indicates a positive influence on immune modulation although no evidence exists as yet of their influence on AN symptomatology. There has been extensive research into the use of probiotics and prebiotics in IBD and FGIDs with some evidence for reduction in disease parameters and symptomatology with the use of multi-strain probiotics.
ConclusionsSome theoretical, mechanistic and clinical evidence exists for the use of probiotics in ameliorating GI symptoms in AN. However, further research is needed into the context of the gut microbiome changes in AN, the specifics of efficacy and the effects that probiotics and prebiotics may have in AN.
Disclosure of InterestNone Declared






