186 results
A causal roadmap for generating high-quality real-world evidence
- Lauren E. Dang, Susan Gruber, Hana Lee, Issa J. Dahabreh, Elizabeth A. Stuart, Brian D. Williamson, Richard Wyss, Iván Díaz, Debashis Ghosh, Emre Kıcıman, Demissie Alemayehu, Katherine L. Hoffman, Carla Y. Vossen, Raymond A. Huml, Henrik Ravn, Kajsa Kvist, Richard Pratley, Mei-Chiung Shih, Gene Pennello, David Martin, Salina P. Waddy, Charles E. Barr, Mouna Akacha, John B. Buse, Mark van der Laan, Maya Petersen
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 22 September 2023, e212
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Increasing emphasis on the use of real-world evidence (RWE) to support clinical policy and regulatory decision-making has led to a proliferation of guidance, advice, and frameworks from regulatory agencies, academia, professional societies, and industry. A broad spectrum of studies use real-world data (RWD) to produce RWE, ranging from randomized trials with outcomes assessed using RWD to fully observational studies. Yet, many proposals for generating RWE lack sufficient detail, and many analyses of RWD suffer from implausible assumptions, other methodological flaws, or inappropriate interpretations. The Causal Roadmap is an explicit, itemized, iterative process that guides investigators to prespecify study design and analysis plans; it addresses a wide range of guidance within a single framework. By supporting the transparent evaluation of causal assumptions and facilitating objective comparisons of design and analysis choices based on prespecified criteria, the Roadmap can help investigators to evaluate the quality of evidence that a given study is likely to produce, specify a study to generate high-quality RWE, and communicate effectively with regulatory agencies and other stakeholders. This paper aims to disseminate and extend the Causal Roadmap framework for use by clinical and translational researchers; three companion papers demonstrate applications of the Causal Roadmap for specific use cases.
Night-time/daytime Protein S100B serum levels in paranoid schizophrenic patients
- E. Diaz-Mesa, A. Morera-Fumero, L. Torres-Tejera, A. Crisostomo-Siverio, P. Abreu-Gonzalez, R. Zuñiga-Costa, S. Yelmo-Cruz, R. Cejas-Mendez, C. Rodriguez-Jimenez, L. Fernandez-Lopez, M. Henry-Benitez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S445-S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
S100B is a calcium-binding astrocyte-specific cytokine, that is considered a biomarker of neurodegeneration; which may be involved in the imbalance of the inflammatory response observed in several brain disorders, including major depression and schizophrenia. Two meta-analyses have reported higher serum levels of S100B in patients with schizophrenia respect to healthy controls.
Different studies have described circadian and seasonal variations of biological variables, such as melatonin or cortisol. It has been reported that there is not circadian rhythm of S100B blood levels in healthy subjects. However, it is not known whether there are circadian oscillations in S100B blood concentrations in patients with schizophrenia.
ObjectivesThe aim of this study is to describe S100B serum levels in patients with schizophrenia and to analyse whether they follow a circadian rhythm.
MethodsOur sample consists in 47 patients in acute phase and stabilized status. Blood samples were collected at 12:00 and 00:00 hours by venipuncture. Serum levels of Protein S100B were measured three times: at admission, discharge and three months after discharge. Protein S100B was measured by means of ELISA (Enzyme-linked immunosorbent assay) techniques.
Results12:00 24:00 P ADMISSION 132,95±199,27 85,85±121,44 0,004 DISCHARGE 73,65±71,744 75,80±123,628 0,070 CONTROL 43,49±34,60 40,14±23,08 0,47 P global P Admission Vs. Discharge P Admission Vs. Control P Discharge Vs. Control 0,97 There is a significance difference between 12:00 and 24:00 at admission for the Protein S100B.However, these difference did not occur at discharge and at three months after discharge.It can be interpreted as there is a circadian rhythm of Protein S100B when the patient has got a psychotic outbreak and disappears at discharge and when is psychopathologically stable.
ConclusionsWith respect to our results we can hypothesize that schizophrenic patients in acute relapse present circadian S100B rhythm that is not present when the patients are clinically stable.Furthermore, the decrease of serum protein S100B levels at discharge is indicative of a reduction of the cerebral inflammation, thus it can be a biomarker of cerebral inflammation and this reduction can be the effect of the treatment. Finally, its circadianity could be a guide of this process and clinical improvement.
Disclosure of InterestNone Declared
Thyroid Stimulating Hormone circadian variations in paranoid schizophrenic psychosis between acute and stable phases. A comparative study.
- A. Marcos-Rodrigo, A. L. Morera-Fumero, P. Abreu-Gonzalez, E. Diaz-Mesa, L. Fernandez-Lopez, J. J. Tascon-Cervera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S186
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Day-night changes in several molecules are studied as biomarkers of circadian rhytms (Morera-Fumero, A. L. et al. Progress in Neuro-Psychopharmacology and Biological Psychiatry 2017; 75 207-212). Circadian rhythmicity of the pituitary-thyroid axis has been proven in healthy individuals, with a Thyroid Stimulating Hormone (TSH) peak in serum around midnight and peaks during day hours (Bellastella, G. et al. Life 2021; 11(5), 426). A recent meta-analysis has reported differences in serum TSH levels between first-episode psychosis and multiple-episode schizophrenia (Misiak, B. et al. Progress in Neuro-Psychopharmacology and Biological Psychiatry 2021; 111, 110402). However, studies assessing quantitative circadian variations on TSH serum in schizophrenic patients are scant.
ObjectivesComparing serum TSH levels at two different times of the day (12:00 and 24:00 hours) and the differences between the acute (hospital admission) and recovered phase (hospital discharge) of the disease.
MethodsFourteen male patients (age 26,8±9,3 years) with the diagnosis of paranoid schizophrenia psychosis according to the DSM-IV partake in the study. Patients were admitted to the University Hospital of the Canary Islands psychiatric room because of acute relapse. Blood samples were taken in the first 24 h of admission and at 24 h. before discharge. All patients gave written consent to participate in the research study. Serum TSH was determined by ELISA methods. Paired sample t-tests were performed between TSH serum levels at admission and discharge at 12:00 and 24:00 hours. Statistical analyses were performed using IBM® SPSS® Statistics 25 software for MAC (IBM Corporation 1989, 2017).
ResultsThere were statistical differences between the 12:00 h and the 24:00 h of the TSH serum levels at admission (12:00: 145,856±156,961vs. 00:00: 192,006± 122,757, p = 0.04); TSH discharge, (12:00: 134,483±72,882vs 00:00: 244,214±148,697, p = 0.002). There were no statistical differences between the 12:00 TSH levels at admission and discharge (145,856±156,961 vs. 134,483± 72,882, p = 0.66). The 24:00 h comparison of TSH levels neither elicited significant results (admission: 192,006±122,757 vs. discharge: 244,214± 148,697, p = 0.15).
ConclusionsSchizophrenic patients undergo TSH serum changes in a circadian pattern during the acute and stable phases of the disease; nevertheless, they experience smaller deviations during the acute phase. Higher levels of TSH were observed around midnight, as it happens in healthy individuals, with higher peaks during the stable phase compared to the acute one.
Disclosure of InterestNone Declared
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
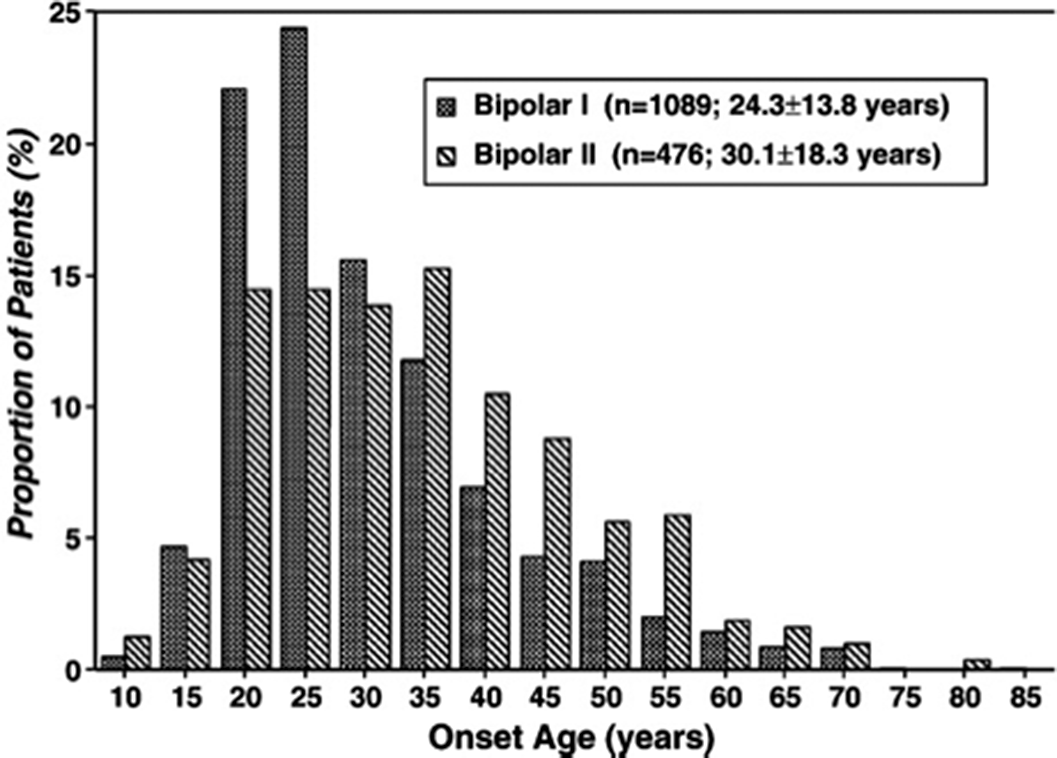
Image 2:
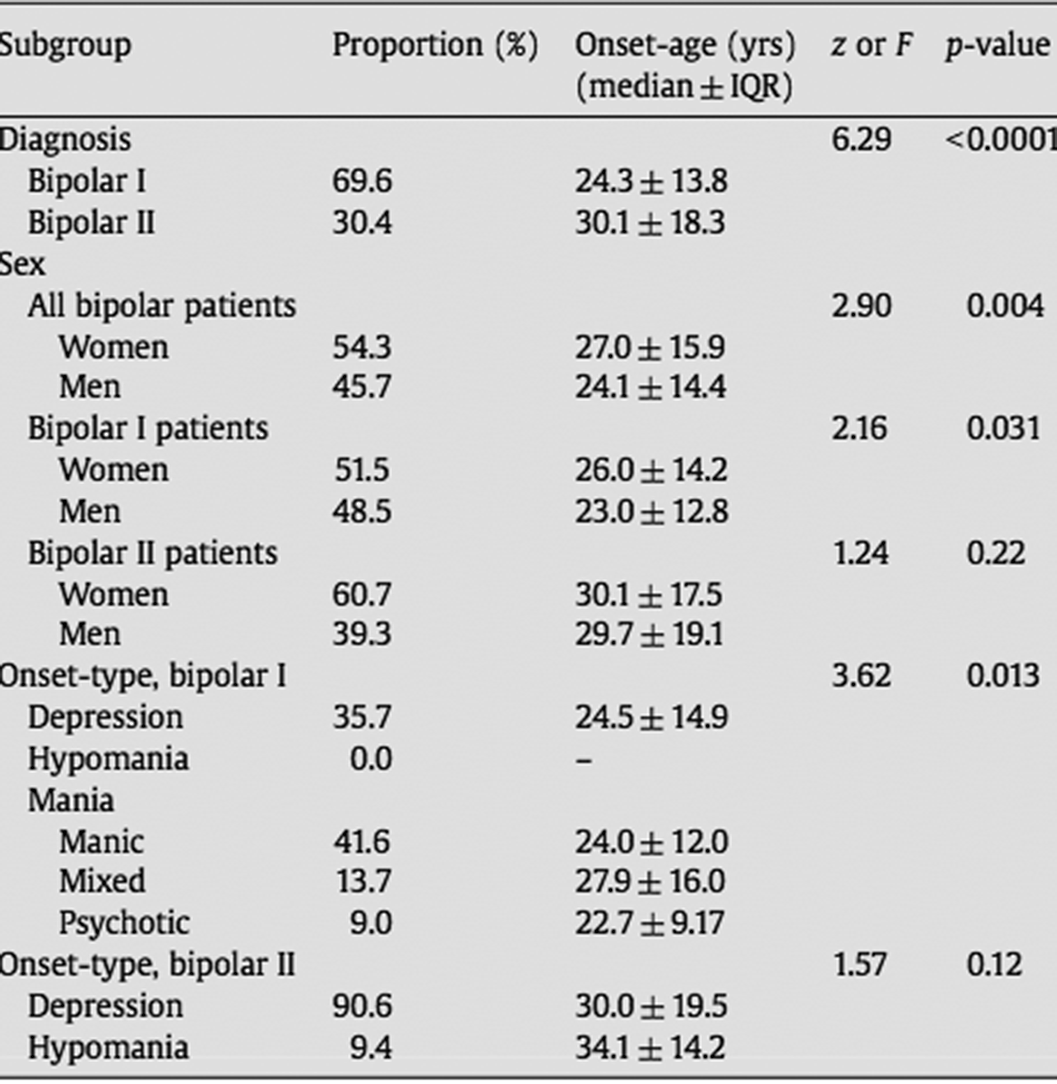 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Memory deficits in children and adolescents with psychotic disorders: A systematic review and meta-analysis
- E. Rodríguez Toscano, P. Díaz-Carracedo, P. de la Higuera-González, G. Padilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S332
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive symptoms in psychosis represent a major unmet clinical need (Acuna-Vargas et al. Cog in Psych 2019; 21(3), 223–224). Deficit in memory has been largely described in first episode early onset psychosis (Mayoral et al. Eur Psych 2008; 23(5), 375-383) and has been associated to a worse functionality (Øie et al. Neuropsychology 2011; 25(1), 25–35). However, results from existing studies are quite mixed on memory deficits of early psychosis patients, particularly in terms of memory contents and storage resources.
ObjectivesThe aims of this study were 1) to examine the nature and extent of cognitive impairment in early-onset psychosis and 2) to analyze which type of memory (verbal and visual) is more affected in the disorder.
MethodsThe present systematic review and meta-analysis was conducted according to the PRISMA criteria (Moher et al. Systematic Reviews 2015; 4(1), 1 - 9). A systematic search of CINAHL, PsycInfo, PubMed, Redalyc, SCOPUS and Web of Science (published from 2000 to 2020) identified case-control studies of early onset psychotic disorder (under 18 years old). Those studies focused on both verbal and visual memory performance.
ResultsTwenty articles were included in the review. A deficit in memory in child and adolescent psychotic disorders was obtained displaying a large effect size in memory tasks (g = -0.83). Also, a medium effect size was found in visual memory tasks (g = - 0.61) and a large effect size was found in verbal memory tasks (g = -1.00).
ConclusionsIt was observed a strong memory deficit on early psychotic disorders already present at the onset of the illness. This deficit was stronger when verbal memory tasks were used compared to the effect found with visual memory tasks. Based on previous literature (García-Nieto et al. Jou Cli Child & Ado Psych 2011; 40(2), 266-280; Lepage et al. Eur Psych 2008; 23(5):368- 74; Hui et al. Psych Med 2016; 46(11):2435-44), these results contribute to describe and characterize the cognitive symptoms in the first-episode psychosis in a youth population.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
Positive relationships and academic stressors in the post-pandemic context of covid-19 in adolescents from a school in Córdoba, Colombia.
- E. P. Ruiz Gonzalez, M. F. Martinez Burgos, V. Contrera Montiel, M. N. Muñoz Argel, J. J. Diaz Muñoz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S214
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Berscheid (1999), taken from Lacunza & Contini (2016), indicated that social relations were the foundation of the human condition. From positive psychology, Park et al. (2013) point out good relationships as a factor that contributes to a good psychological life, since they provide emotional and instrumental support in times of stress and challenge, indicating, in turn, normal evolutionary development and the avoidance of psychopathological problems.
ObjectivesTo establish the relationship between positive relationships and the presence of stressors in adolescents.
MethodsA cross-sectional, descriptive-correlational study was carried out in 109 (N= 109) adolescents. The SISCO Inventory was used to study academic stress as well as the Ryff Psychological Well-Being Scale.
ResultsA negative magnitude correlation was found between positive relationships and stressors. ( Table 1).
As a secondary result, 60.6% of the evaluated adolescents presented life purpos as the factor with the highest score in the psychological well-being variable. This points to authors such as Erikson (1988, p. 96), who define adolescence as a space characterized by feelings of creativity, productivity, new ideas, and a period of cognitive and social maturation, which leads to a definitive commitment to life itself. (Graph 1).
Image:
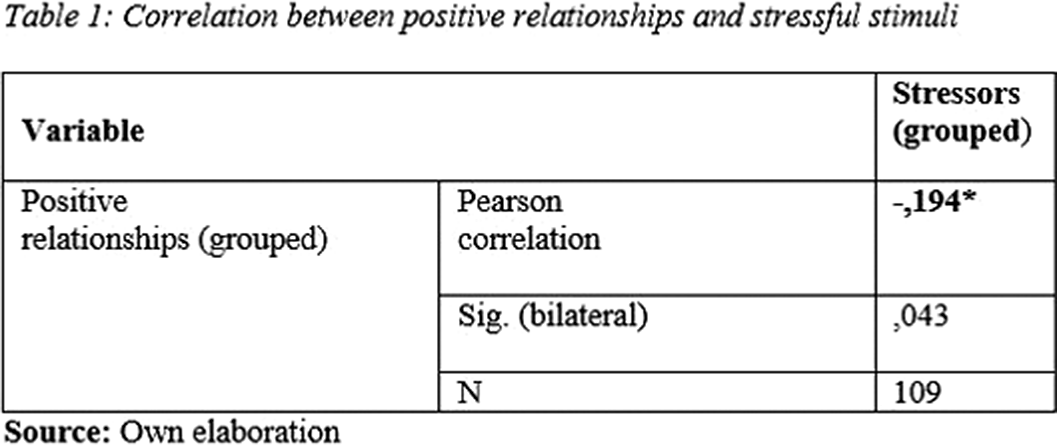
Image 2:
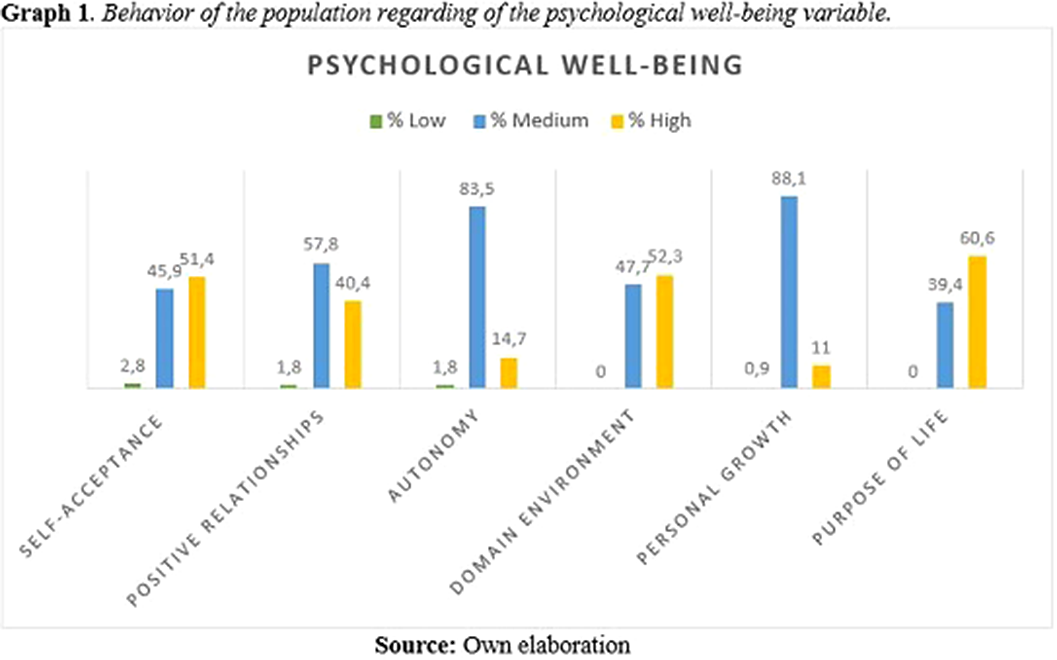 Conclusions
ConclusionsPositive relationships in adolescents decrease the presence of stimuli considered stressors.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
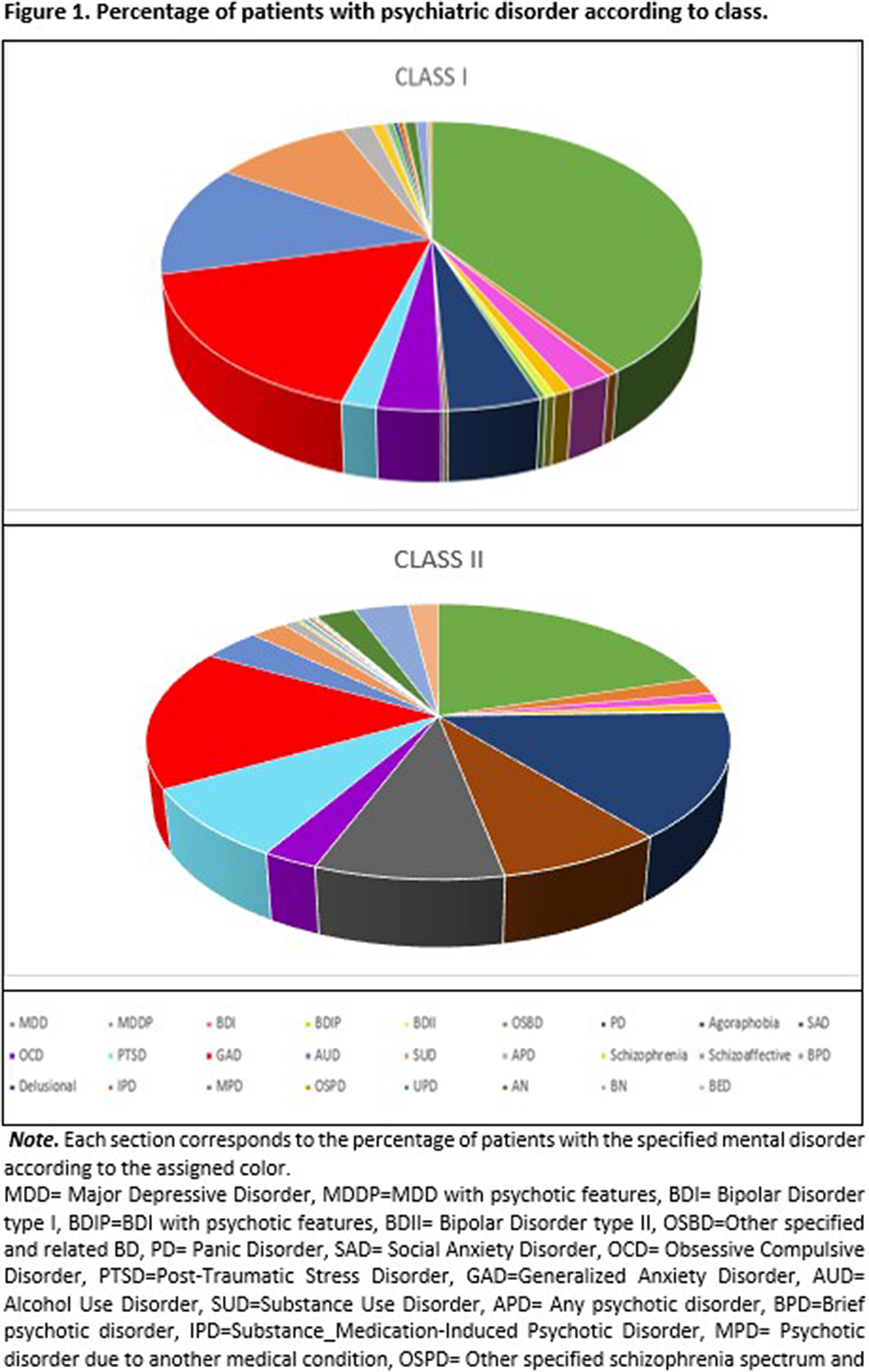 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Chronic disease (CD) during transition from child to adult.Psychopathological consequences and coping strategies
- S. Rubio Corgo, M. Arrieta Pey, A. M. Matas Ochoa, M. I. Duran Cristobal, E. Perez Vicente, A. Delgado Campos, C. Diaz Gordillo, A. C. Castro Ibañez, A. Alvarez Astorga, P. Alcindor Huelva
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S745
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
CD is characterized by at least three features: its duration is prolonged, it does not resolve spontaneously and it is rarely completely cured. Approximately 10-15% of young people have CD. Adolescents with CD often have emotional and behavioral problems.
ObjectivesTo assess risk factors, derived psychiatric pathologies and coping strategies for a CD diagnosis in adolescence.
MethodsAn extensive literature review was carried out on the subject in question, extracting information mainly from scientific articles, manuals and books.
ResultsThe main risk factors are those related with the CD in question, physical sequelae, the need for long-term hospital admissions or the use of drugs whose side effects include affective or behavioral symptoms; those related to the personality traits of the affected child or adolescent. In addition, as far as the family is concerned, the presence of a low level of education, lack of support or communication, as well as the presence of psychiatric disorders or serious medical conditions in parents. Among the most frequent psychiatric disorders associated with CD are affective and anxiety disorders, adaptive disorders, somatoform disorders, eating disorders and behavioral disorders. Whatever the CD is, it generates high levels of stress and uncertainty in the patient and family, which must be dealt together from a flexible perspective, allowing child or adolescent to adapt to the changes, reorganize and facing them with adaptive patterns of behavior. For this, it will be essential to have adequate social and family support with relational style based on communication, trust and acceptance.
ConclusionsIn general, both adolescents with CD and their families have an adequate capacity to adapt to the repercussions and effects derived from the disease. Nevertheless, in case of possible emotional difficulties that may appear, a comprehensive and individualized approach to these adolescents and their families is necessary to provide them resources and coping strategies in different areas and contexts in which the disease debuts.The comprehensive therapeutic approach will consist of interventions at the individual and family level. Among the main objectives of these interventions are to achieve acceptance and adaptation to CD provinding adequate psychosocial support to enable them to cope with CD in the best possible way and to detect and address the emotional implications, even coexisting psychopathology.
Disclosure of InterestNone Declared
Psychopathological symptoms as clinical phenotypes in suicide attempters: relation in terms of suicidal ideation, suicidal related behaviors and medical damage of the attempt
- D. Saiz-Gonzalez, P. Diaz-Carracedo, A. Pemau, W. Ayad-Ahmed, F.-R. Veronica, M. Navas Tejedor, A. de la Torre-Luque, M. Diaz-Marsa
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S560-S561
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide behaviour is a complex and multifactor concept that includes different risk factors. According with literature a dimensional concept of illness could help to understand this complexity and clarify clinical aspects of suicide risk.
ObjectivesThe aim of this study is to identify different profiles of symptoms in a sample of suicide attempters and the relationship between this profiles and suicide behaviour in terms of outcome: presence and intensity of suicidal ideation, presence and number of attempts and severity of the medical damage in the current attempt.
Methods634 patients were recruited at the psychiatry emergency of eight public general hospitals in Spain between November 2020 until February 2022 in the SURVIVE protocol. The patients were assessed in 15 days using a battery of clinical tools that includes Brief Symptom Inventory, a sociodemographic interview, Mini Clinical Interview and C-SSRS, ACSS and BIS-11 scales. Latent profile analysis was applied to obtain profile symptoms. Logistic and multivariant regression was used to obtain data about outcome.
ResultsThree clinical profiles of psychiatric symptoms were described in suicide attempters (p < 0.01): high symptoms (HS) (45.02%), moderate symptoms (MS) (42.5 %) and low symptoms (LS) (12.48%). Significant differences were found between classes in four symptom domains (Figure 1): anxiety, obsessive-compulsive, sensitivity, and somatization (p < 0.01). Participants of the HS class showed higher values in relation with the BSI summary indexes, and more diagnoses, higher levels of suicidal ideation and suicidal related behaviour as well as higher acquired capability for suicide. Participants of the LS class were more likely to be women, older and unemployed and was related, according the analysis, with severe medical damage when compared with other groups (P< 0.01).
Image:
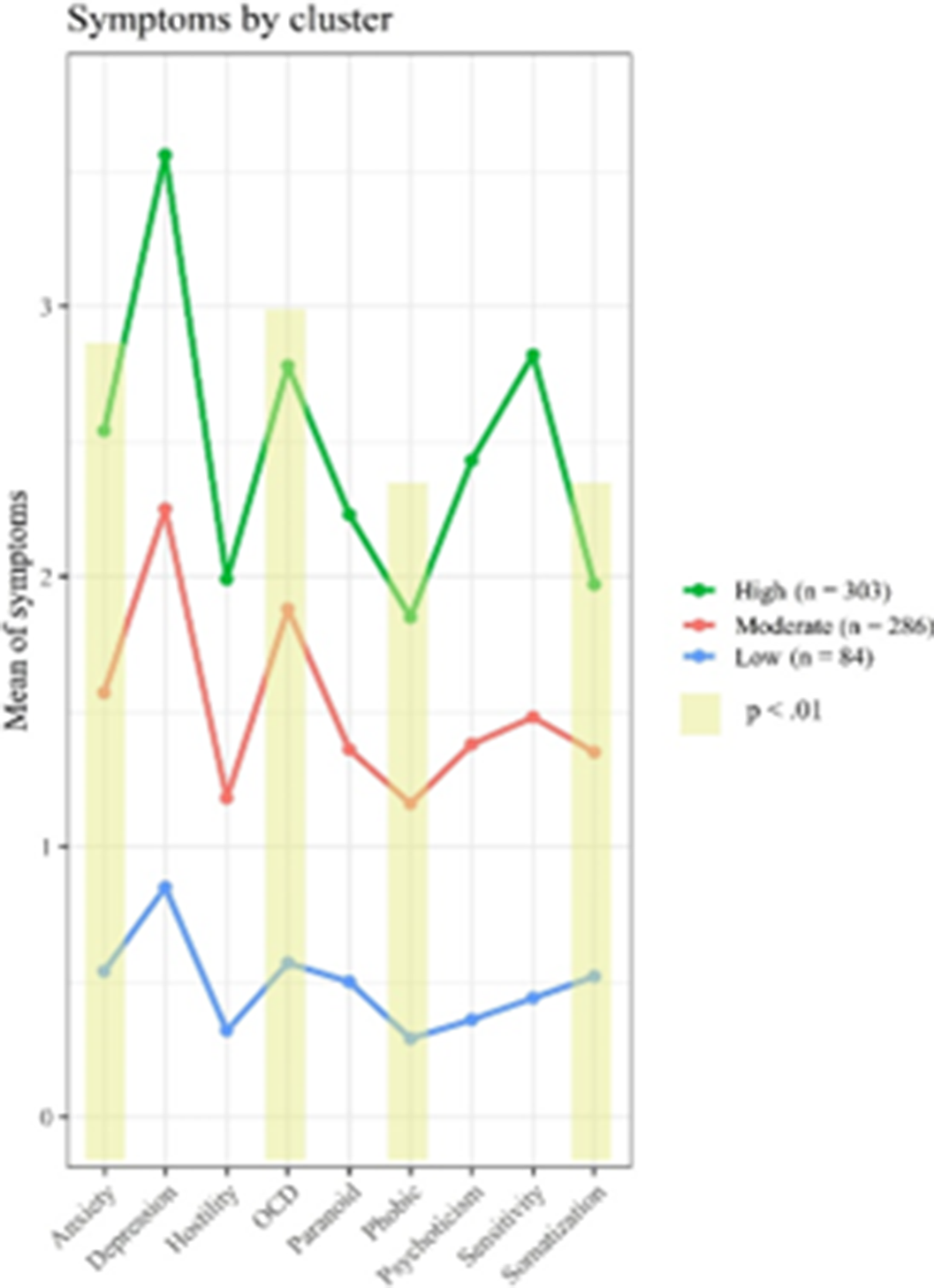 Conclusions
ConclusionsAccording with the predictive model the study suggests different symptom-frequency clusters related with suicide attempt outcomes. Suicide ideation presence and intensity is related with HS class and acquired capability of suicide. Suicide ideation intensity is also related with number of diagnosis and number of previous attempts. Suicide behaviours presence is associated with being student and number with HS profile. Both presence and number were related with number of diagnosis as well as number of previous attempts (the higher all these clinical factors, the more intense of ideation in the last month). Finally, the severity of medical damage was related with LS profile and unemployed/retired work status. The dimensional symptom profile could be useful to predict suicide attempt outcome. Further study is needed to clarify this relation.
Disclosure of InterestNone Declared
Study of mentalizing ability in borderline personality disorder: relationship with impulsivity
- A. Galvez-Merlin, P. de la Higuera-Gonzalez, J. M. Lopez-Villatoro, A. de la Torre-Luque, M. Diaz-Marsa, J. L. Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S114
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Borderline personality disorder (BPD) is a severe mental disorder characterized by affective, behavioral and relational instability, along with interpersonal hypersensitivity and unstable affective relationships (APA 2013). Poor interpersonal functioning could be associated with critical deficits in the ability to mentalize in these patients, together with high levels of impulsivity. Although most studies have described hypermentalization deficits among BPD patients (Bora Psychol Med 2021;51 2541-2551), existing literature is still scarce on this aspect, as well as its relationship with the impulsive behavior.
Objectives1) to assess specific mentalizing deficits in BPD compared to healthy controls in a complex ecological mentalization task; 2) evaluate the relationship between mentalization and impulsivity in BPD.
Methods63 patients diagnosed with borderline personality disorder and 31 control subjects were studied using the Movie for the Assessment of Social Cognition -MASC- (Dziobeck et al. J Autism Dev Disord 2006; 36 623-636) and the Barratt Impulsivity Scale -BIS-11- (Patton et al. J Clin Psychol 1995; 51 768-774), as well as other sociodemographic and clinical factors. The clinical research study was approved by the Clinical Research Ethics Committee of the Hospital Clínico San Carlos (Madrid, Spain).
ResultsThe results showed significant differences in the scores related to correct mentalization, hypomentalization, and non-mentalizing responses between patients and controls, with BPD patients showing worse performance. A significant negative relationship was also observed between impulsivity scores and correct mentalizing responses in BPD patients.
ConclusionsThe results showed a deficit in the ability to mentalize in BPD patients, compared to control subjects, characterized by a hypomentalization and an absence of mentalization. Likewise, this deficit in mentalization ability was related to greater impulsive behavior in patients. These results would be consistent with the hyperarousal hypothesis in BPD, which would reduce inhibitory control, causing mentalization deficits (Euler et al. J Pers Disord. 2021; 35 177-193). Future studies will try to associate specific impulsive behaviors associated with the characteristics of hypomentalization and absence of mentalization observed in our results.
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Psychosomatics and mentalization
- A. M. Delgado Campos, P. Alcindor Huelva, A. Alvarez Astorga, S. Rubio Corgo, E. Pérez Vicente, M. Arrieta Pey, C. Diaz Gordillo, P. Del Sol Calderón, A. C. Martín Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1024
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We have investigated the relationship between the Psychosomatic Classification method (Marty) and the Rorschach Test, with respect to the diagnosis of psychosomatic disorders, within the framework of the degree of mentalization measured by both.
ObjectivesA) To verify statistical coincidence with respect to the degree of mentalization (risk of generating psychosomatic disorders in a subject) between the Rorschach Test and the diagnostic technique Psychosomatic Classification, by P. Marty. B) To test the hypothesis: Patients diagnosed with infertility, whose degree of mentalization is good, will have a greater probability of achieving a successful pregnancy throught Assisted Reproduction Techniques.
MethodsTwo evaluation tools were used: a) Psychosomatic Classification based on the criteria established by this diagnostic method; b) The Rorschach test (based on the evaluation of 29 indicators, selected according to their greater relevance in the generation of somatic symptoms).
A sample of 120 patients (women) diagnosed infertility at the Assisted Reproduction Unit (U.R.A.) at Hospital Universitario 12 de Octubre in Madrid was recruited. The method of ‘statistical correlation of coincidence’ between the results of the two diagnostic instruments used was used. Once both tests had been assessed by the “inter-judge” method and the quantitative values of the selected items had been weighted, the KAPPA statistical method was applied to establish the “correlation of coincidence” between the results of the two assessment instruments.
ResultsConsidering that the KAPPA method takes values between “0" and ”1" and that between 0.6 and 0.8 the agreement or coincidence is considered good, and above 0.8 very good, the result applied to the hypothesis is 0’76 (’good’).
ConclusionsA) Using the Rorschach Test and P. Marty’s Psychosomatic Classification in a complementary manner, these two instruments together provide high reliability, with respect to the degree of mentalization (a subject’s risk of suffering psychosomatic disorders). B) The degree of mentalization has a significant impact on the success or failure in the application of Assisted Reproduction Techniques in infertile women.
Disclosure of InterestNone Declared
Daytime/nighttime levels of serum IL-33 in schizophrenia at hospital admission and before discharge
- J. J. Tascon-Cervera, A. Morera-Fumero, P. Abreu-Gonzalez, E. Diaz-Mesa, M. R. Cejas-Mendez, S. Yelmo-Cruz, L. Fernandez-Lopez, A. Marcos-Rodrigo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1062-S1063
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It has been reported an inflammatory state in schizophrenia, with altered levels of some cytokines (Zhou et al. Cytokine 2021; 141:155441). Recent publications have shown the importance of IL- 33, a member of the IL-1 cytokine family which acts as an alarmin (Han et al. Neurosci Bull 2011; 27, 351-357). The role of this cytokine as a biomarker has been investigated in schizophrenia (Koricanac et al. Front Psychiatry 2022; 13, 925757). However, results are controversial. Some studies have not found significant associations between IL-33 and chronic schizophrenia (Campos-Carli et al. Compr Psychiatry 2017; 74 96-101), while other papers have reported increased levels (Kozlowska et. al. J Psychiatr Res. 2021; 138 380-387). In all these studies, levels of IL-33 were measured in a single daily measure, so that it has not been studied if IL-33 has changes during hospitalization.
ObjectivesTo study the serum level of IL-33 at 12:00 and 00:00 hours in schizophrenia patients at admission and before hospital discharge.
MethodsFifteen inpatients with diagnosis of paranoid schizophrenia according to ICD-10 criteria were studied. Patients were hospitalized at the University Hospital of the Canary Islands psychiatric ward because of an acute relapse. A total of four blood samples were taken from each patient: at 12:00 and 00:00 hours the day after admission and at 12:00 and 00:00 hours the day before discharge. Serum IL-33 levels were measured by ELISA techniques. Daytime and nighttime IL-33 serum levels at admission and discharge were compared using a non-parametric Wilcoxon signed-rank test.
ResultsIn table 1 the results of the comparison of IL-33 at admission and discharge are presented. There is a significant reduction of IL-33 levels at 00:00 h. at discharge in comparison with the IL-33 levels at 00:00 h. at admission (p=0.028). No other statistically significant differences were observed.
Serum IL-33 Admission Mean±sd Discharge Mean±sd Z P value 12:00 h. 191.0±348.7 247.0±378.2 -0.166 0.868 00:00 h. 218.8±370.3 153.6±275.7 -2.203 0.028 ConclusionsThe decrease of serum IL-33 at 00:00 at discharge compared to the 00:00 IL-33 serum level at admission points to the utility of this biomarker as a surrogate of brain inflammation.
Disclosure of InterestNone Declared
Female infertility, Alexithymia and Stress
- A. M. Delgado Campos, P. Alcindor Huelva, A. Alvarez Astorga, S. Rubio Corgo, E. Pérez Vicente, M. Arrieta Pey, C. Diaz Gordillo, P. del Sol Calderón, A. C. Martín Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S648
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In this research the Paris School (I.P.S.O.), by P. Marty, is chosen as the theoretical and clinical basis of Psychosomatics. We work with the degree of mentalization (good, bad and uncertain) -obtained through Marty’s Psychosomatic Classification-, as a previous diagnosis and prognosis of 120 infertile women undergoing treatment at the Assisted Reproduction Unit (ARU) at Hospital Universitario 12 de Octubre in Madrid.
Objectivesa) To analyse the statistical coincidence between female infertility, stress and alexithymia syndrome. b) To verify the differences between psychosomatic disorders and other somatoform symptoms and syndromes (conversive and hypochondriac). c) To test the following hypothesis: subjects whose degree of mentalization is deficient, present high degree of alexithymia and stress.
Methods120 infertile women undergoing treatment with Assisted Reproduction Techniques were examined by means of psychodiagnostic tests.
Diagnostic tools: P. Mary’s Psychosomatic Classification (P.C.) (semi-structured interview), as a means of diagnosing the degree of mentalization; T.A.S. (Toronto Alexithymia Scale); Battery of stress measurement questionnaires (H.A.D., PANAS. IRE, MCMQ).
The correlation of coincidence between the results of C.P. and the different Alexithymia and Stress questionnaires with the independent variable (success or failure of pregnancy in the selected subjects) has been studied, applying Spearman’s Correlation Coefficient.
ResultsWith respect to what was obtained in the Psychosomatic Classification:
- T.A.S. questionnaire yields a coefficient of [-0.48]. Therefore, there is a negative correlation between the degree of mentalization and the presence of alexithymia; in other words, as the degree of mentalization increases, the degree of alexithymia decreases and vice versa;
- There is positive correlation [0.39] between the results of Mentalization (Psychosomatic Classification) and the degree of stress; therefore, the existence of stress does not prevent better mentalization.
ConclusionsThe present research concludes: a) that people at risk for psychosomatic disorders have high scores on “alexithymia”; b) that patients at high risk for psychosomatic disorders do not necessarily suffer from “stress” situations; c) that there are many indicators in behavior and psychological functioning that differentiate psychosomatic disorders from conversive and hypochondriac disorders - both in their etiology and their development; d) there is a statistical correlation between female infertility and alexithymia; e) there is no statistical correlation between female infertility and stress.
Disclosure of InterestNone Declared
Tobacco use in first-episode psychosis, a multinational EU-GEI study
- T. Sánchez-Gutiérrez, E. Rodríguez-Toscano, L. Roldán, L. Ferraro, M. Parellada, A. Calvo, G. López, M. Rapado-Castro, D. La Barbera, C. La Cascia, G. Tripoli, M. Di Forti, R. M. Murray, D. Quattrone, C. Morgan, J. van Os, P. García-Portilla, S. Al-Halabí, J. Bobes, L. de Haan, M. Bernardo, J. L. Santos, J. Sanjuán, M. Arrojo, A. Ferchiou, A. Szoke, B. P. Rutten, S. Stilo, G. D'Andrea, I. Tarricone, EU-GEI WP2 Group, C. M. Díaz-Caneja, C. Arango
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 7265-7276
-
- Article
- Export citation
-
Background
Tobacco is a highly prevalent substance of abuse in patients with psychosis. Previous studies have reported an association between tobacco use and schizophrenia. The aim of this study was to analyze the relationship between tobacco use and first-episode psychosis (FEP), age at onset of psychosis, and specific diagnosis of psychosis.
MethodsThe sample consisted of 1105 FEP patients and 1355 controls from the European Network of National Schizophrenia Networks Studying Gene–Environment Interactions (EU-GEI) study. We assessed substance use with the Tobacco and Alcohol Questionnaire and performed a series of regression analyses using case-control status, age of onset of psychosis, and diagnosis as outcomes and tobacco use and frequency of tobacco use as predictors. Analyses were adjusted for sociodemographic characteristics, alcohol, and cannabis use.
ResultsAfter controlling for cannabis use, FEP patients were 2.6 times more likely to use tobacco [p ⩽ 0.001; adjusted odds ratio (AOR) 2.6; 95% confidence interval (CI) [2.1–3.2]] and 1.7 times more likely to smoke 20 or more cigarettes a day (p = 0.003; AOR 1.7; 95% CI [1.2–2.4]) than controls. Tobacco use was associated with an earlier age at psychosis onset (β = −2.3; p ⩽ 0.001; 95% CI [−3.7 to −0.9]) and was 1.3 times more frequent in FEP patients with a diagnosis of schizophrenia than in other diagnoses of psychosis (AOR 1.3; 95% CI [1.0–1.8]); however, these results were no longer significant after controlling for cannabis use.
ConclusionsTobacco and heavy-tobacco use are associated with increased odds of FEP. These findings further support the relevance of tobacco prevention in young populations.
The price of gaining: maximization in decision-making, regret and life satisfaction
- Emilio Moyano-Díaz, Agustín Martínez-Molina, Fernando P. Ponce
-
- Journal:
- Judgment and Decision Making / Volume 9 / Issue 5 / September 2014
- Published online by Cambridge University Press:
- 01 January 2023, pp. 500-509
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Maximizers attempt to find the best solution in decision-making, while satisficers feel comfortable with a good enough solution. Recent results pointed out some critical aspects of this decision-making approach and some concerns about its measurement and dimensional structure. In addition to the analysis of these aspects, we tested the possible mediational role of regret in this psychological process. The Maximization Inventory (MI; satisficing, decision difficulty, and alternative search), regret, and Satisfaction with Life Scale (SWLS) were translated and adapted to Spanish in order to answer these issues with a Chilean sample. Validity and reliability analysis of the MI reports that only two dimensions of the MI have enough dimensional support (decision difficulty, alternative search). The tested structural model shows good fit of partial mediation effect of regret between decision difficulty and SWLS. At the same time, alternative search has a positive relation with SWLS. These results suggest that Regret becomes crucial for prescribing behavior to decision makers.
Sex differences in regional gray matter density in pre-adolescent binge eating disorder: a voxel-based morphometry study
- Stuart B. Murray, Joel P. Diaz-Fong, Christina J. Duval, Ane A. Balkchyan, Jason M. Nagata, Darrin J. Lee, Kyle T. Ganson, Arthur W. Toga, Steven J. Siegel, Kay Jann
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 13 / October 2023
- Published online by Cambridge University Press:
- 28 October 2022, pp. 6077-6089
-
- Article
- Export citation
-
Background
Binge eating disorder (BED) is a pernicious psychiatric disorder which is linked with broad medical and psychiatric morbidity, and obesity. While BED may be characterized by altered cortical morphometry, no evidence to date examined possible sex-differences in regional gray matter characteristics among those with BED. This is especially important to consider in children, where BED symptoms often emerge coincident with rapid gray matter maturation.
MethodsPre-adolescent, 9–10-year old boys (N = 38) and girls (N = 33) with BED were extracted from the 3.0 baseline (Year 0) release of the Adolescent Brain Cognitive Development Study. We investigated sex differences in gray matter density (GMD) via voxel-based morphometry. Control sex differences were also assessed in age and body mass index and developmentally matched control children (boys N = 36; girls N = 38). Among children with BED, we additionally assessed the association between dorsolateral prefrontal (dlPFC) GMD and parent-reported behavioral approach and inhibition tendencies.
ResultsGirls with BED uniquely demonstrate diffuse clusters of greater GMD (p < 0.05, Threshold Free Cluster Enhancement corrected) in the (i) left dlPFC (p = 0.003), (ii) bilateral dmPFC (p = 0.004), (iii) bilateral primary motor and somatosensory cortex (p = 0.0003) and (iv) bilateral precuneus (p = 0.007). Brain-behavioral associations suggest a unique negative correlation between GMD in the left dlPFC and behavioral approach tendencies among girls with BED.
ConclusionsEarly-onset BED may be characterized by regional sex differences in terms of its underlying gray matter morphometry.









