15 results
106 Transforming Health Equity with an Innovative Social Determinants of Health Platform: Application of HOUSES Index to Colorectal Cancer Screening
- Part of
- Chung-il Wi, Madison J. Roy, Euijung Ryu, Philip H. Wheeler, Gokhan Anil, Kathy A. Madden, Folakemi T. Odedina, James R. Cerhan, Young J. Juhn
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue s1 / April 2024
- Published online by Cambridge University Press:
- 03 April 2024, p. 30
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: To tackle population-level health disparities, quality dashboards can leverage individual socioeconomic status (SES) measures, which are not always readily accessible. This study aimed to assess the feasibility of a population health management strategy for colorectal cancer (CRC) screening rates using the HOUSES index and heatmap analysis. METHODS/STUDY POPULATION: We applied the 2019 Minnesota Community Measurement data for optimal CRC screening to eligible Mayo Clinic Midwest panel patients. SES was defined by HOUSES index, a validated SES measure based on publicly available property data for the U.S. population. We first assessed the association of suboptimal CRC screening rate with HOUSES index adjusting for age, sex, race/ethnicity, comorbidity, and Zip-code level deprivation by using a mixed effects logistic regression model. We then assessed changes in ranking for performance of individual clinics (i.e., % of patients with optimal CRC screening rate) before and after adjusting for HOUSES index. Geographical hotspots of high proportions of low SES AND high proportions of suboptimal CRC screening were superimposed to identify target population for outreach. RESULTS/ANTICIPATED RESULTS: A total of 58,382 adults from 41 clinics were eligible for CRC screening assessment in 2019 (53% Female). Patients with lower SES defined by HOUSES quartile 1-3 have significantly lower CRC screening compared to those with highest SES (HOUSES quartile 4) (adj. OR [95% CI]: 0.52 [0.50-0.56] for Q1, 0.66 [0.62-0.70] for Q2, and 0.81 [0.76-0.85]) for Q3). Ranking of 26 out of 41 (63%) clinics went down after adjusting for HOUSES index suggesting disproportionately higher proportion of underserved patients with suboptimal CRC screening. We were able to successfully identify hotspots of suboptimal CRC (area with greater than 130% of expected value) and overlay with higher proportion of underserved population (HOUSES Q1), which can be used for data-driven targeted interventions such as mobile health clinics. DISCUSSION/SIGNIFICANCE: HOUSES index and associated heatmap analysis can contribute to advancing health equity. This approach can aid health care organizations in meeting the newly established standards by The Joint Commission, which have elevated health equity to a national safety priority.
Randomised controlled trial of the short-term effects of osmotic-release oral system methylphenidate on symptoms and behavioural outcomes in young male prisoners with attention deficit hyperactivity disorder: CIAO-II study
- Philip J. Asherson, Lena Johansson, Rachel Holland, Megan Bedding, Andrew Forrester, Laura Giannulli, Ylva Ginsberg, Sheila Howitt, Imogen Kretzschmar, Stephen M. Lawrie, Craig Marsh, Caroline Kelly, Megan Mansfield, Clare McCafferty, Khuram Khan, Ulrich Müller-Sedgwick, John Strang, Grace Williamson, Lauren Wilson, Susan Young, Sabine Landau, Lindsay D. G. Thomson
-
- Journal:
- The British Journal of Psychiatry / Volume 222 / Issue 1 / January 2023
- Published online by Cambridge University Press:
- 03 June 2022, pp. 7-17
- Print publication:
- January 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Research has shown that 20–30% of prisoners meet the diagnostic criteria for attention-deficit hyperactivity disorder (ADHD). Methylphenidate reduces ADHD symptoms, but effects in prisoners are uncertain because of comorbid mental health and substance use disorders.
AimsTo estimate the efficacy of an osmotic-release oral system methylphenidate (OROS-methylphenidate) in reducing ADHD symptoms in young adult prisoners with ADHD.
MethodWe conducted an 8-week parallel-arm, double-blind, randomised placebo-controlled trial of OROS-methylphenidate versus placebo in male prisoners (aged 16–25 years) meeting the DSM-5 criteria for ADHD. Primary outcome was ADHD symptoms at 8 weeks, using the investigator-rated Connors Adult ADHD Rating Scale (CAARS-O). Thirteen secondary outcomes were measured, including emotional dysregulation, mind wandering, violent attitudes, mental health symptoms, and prison officer and educational staff ratings of behaviour and aggression.
ResultsIn the OROS-methylphenidate arm, mean CAARS-O score at 8 weeks was estimated to be reduced by 0.57 points relative to the placebo arm (95% CI −2.41 to 3.56), and non-significant. The responder rate, defined as a 20% reduction in CAARS-O score, was 48.3% for the OROS-methylphenidate arm and 47.9% for the placebo arm. No statistically significant trial arm differences were detected for any of the secondary outcomes. Mean final titrated dose was 53.8 mg in the OROS-methylphenidate arm.
ConclusionsADHD symptoms did not respond to OROS-methylphenidate in young adult prisoners. The findings do not support routine treatment with OROS-methylphenidate in this population. Further research is needed to evaluate effects of higher average dosing and adherence to treatment, multi-modal treatments and preventative interventions in the community.
Role of geographic risk factors and social determinants of health in COVID-19 epidemiology: Longitudinal geospatial analysis in a midwest rural region
- Philip H. Wheeler, Christi A. Patten, Chung-Il Wi, Joshua T. Bublitz, Euijung Ryu, Elizabeth H. Ristagno, Young J. Juhn
-
- Journal:
- Journal of Clinical and Translational Science / Volume 6 / Issue 1 / 2022
- Published online by Cambridge University Press:
- 27 December 2021, e51
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Studies examining the role of geographic factors in coronavirus disease-2019 (COVID-19) epidemiology among rural populations are lacking.
Methods:Our study is a population-based longitudinal study based on rural residents in four southeast Minnesota counties from March through October 2020. We used a kernel density estimation approach to identify hotspots for COVID-19 cases. Temporal trends of cases and testing were examined by generating a series of hotspot maps during the study period. Household/individual-level socioeconomic status (SES) was measured using the HOUSES index and examined for association between identified hotspots and SES.
Results:During the study period, 24,243 of 90,975 residents (26.6%) were tested for COVID-19 at least once; 1498 (6.2%) of these tested positive. Compared to other rural residents, hotspot residents were overall younger (median age: 40.5 vs 43.2), more likely to be minorities (10.7% vs 9.7%), and of higher SES (lowest HOUSES [SES] quadrant: 14.6% vs 18.7%). Hotspots accounted for 30.1% of cases (14.5% of population) for rural cities and 60.8% of cases (27.1% of population) for townships. Lower SES and minority households were primarily affected early in the pandemic and higher SES and non-minority households affected later.
Conclusion:In rural areas of these four counties in Minnesota, geographic factors (hotspots) play a significant role in the overall burden of COVID-19 with associated racial/ethnic and SES disparities, of which pattern differed by the timing of the pandemic (earlier in pandemic vs later). The study results could more precisely guide community outreach efforts (e.g., public health education, testing/tracing, and vaccine roll out) to those residing in hotspots.
Mobile home residence as a risk factor for adverse events among children in a mixed rural–urban community: A case for geospatial analysis
- Archna A. Patel, Philip H. Wheeler, Chung-Il Wi, Chris Derauf, Euijung Ryu, David Zahrieh, Kara A. Bjur, Young J. Juhn
-
- Journal:
- Journal of Clinical and Translational Science / Volume 4 / Issue 5 / October 2020
- Published online by Cambridge University Press:
- 06 April 2020, pp. 443-450
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Given the significant health effects, we assessed geospatial patterns of adverse events (AEs), defined as physical or sexual abuse and accidents or poisonings at home, among children in a mixed rural–urban community.
Methods:We conducted a population-based cohort study of children (<18 years) living in Olmsted County, Minnesota, to assess geographic patterns of AEs between April 2004 and March 2009 using International Classification of Diseases, Ninth Revision codes. We identified hotspots by calculating the relative difference between observed and expected case densities accounting for population characteristics (
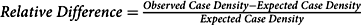 $$Relative\;Difference = {\rm{ }}{{Observed\;Case\;Density - Expected\;Case\;Density} \over {Expected\;Case\;Density}}$$; hotspot ≥ 0.33) using kernel density methods. A Bayesian geospatial logistic regression model was used to test for association of subject characteristics (including residential features) with AEs, adjusting for age, sex, and socioeconomic status (SES).Results:
$$Relative\;Difference = {\rm{ }}{{Observed\;Case\;Density - Expected\;Case\;Density} \over {Expected\;Case\;Density}}$$; hotspot ≥ 0.33) using kernel density methods. A Bayesian geospatial logistic regression model was used to test for association of subject characteristics (including residential features) with AEs, adjusting for age, sex, and socioeconomic status (SES).Results:Of the 30,227 eligible children (<18 years), 974 (3.2%) experienced at least one AE. Of the nine total hotspots identified, five were mobile home communities (MHCs). Among non-Hispanic White children (85% of total children), those living in MHCs had higher AE prevalence compared to those outside MHCs, independent of SES (mean posterior odds ratio: 1.80; 95% credible interval: 1.22–2.54). MHC residency in minority children was not associated with higher prevalence of AEs. Of addresses requiring manual correction, 85.5% belonged to mobile homes.
Conclusions:MHC residence is a significant unrecognized risk factor for AEs among non-Hispanic, White children in a mixed rural–urban community. Given plausible outreach difficulty due to address discrepancies, MHC residents might be a geographically underserved population for clinical care and research.
Intervention to Reduce Broad-Spectrum Antibiotics and Treatment Durations Prescribed at the Time of Hospital Discharge: A Novel Stewardship Approach
- Norihiro Yogo, Katherine Shihadeh, Heather Young, Susan L. Calcaterra, Bryan C. Knepper, William J. Burman, Philip S. Mehler, Timothy C. Jenkins
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 5 / May 2017
- Published online by Cambridge University Press:
- 06 March 2017, pp. 534-541
- Print publication:
- May 2017
-
- Article
- Export citation
-
OBJECTIVE
For most common infections requiring hospitalization, antibiotic treatment is completed after hospital discharge. Postdischarge therapy is often unnecessarily broad spectrum and prolonged. We developed an intervention to improve antibiotic selection and shorten treatment durations.
DESIGNSingle center, quasi-experimental retrospective cohort study
METHODSPatients prescribed oral antibiotics at hospital discharge before (July 2012–June 2013) and after (October 2014–February 2015) an intervention consisting of (1) institutional guidance for oral step-down antibiotic selection and duration of therapy and (2) pharmacy audit of discharge prescriptions with real-time prescribing recommendations to providers. The primary outcomes measured were total prescribed duration of therapy and use of antibiotics with broad gram-negative activity (ie, fluoroquinolones or amoxicillin-clavulanate).
RESULTSOverall, 300 cases from the preintervention period and 200 cases from the intervention period were included. Compared with the preintervention period, the use of antibiotics with broad gram-negative activity decreased during the intervention (51% vs 40%; P=.02), particularly fluoroquinolones (38% vs 25%; P=.002). The total duration of therapy decreased from a median of 10 days (interquartile range [IQR], 7–13 days) to 9 days (IQR, 6–13 days) but did not reach statistical significance (P=.13). However, the duration prescribed at discharge declined from 6 days (IQR, 4–10 days) to 5 days (IQR, 3–7 days) (P=.003). During the intervention, there was a nonsignificant increase in the overall appropriateness of discharge prescriptions from 52% to 66% (P=.15).
CONCLUSIONSA multifaceted intervention to optimize antibiotic prescribing at hospital discharge was associated with less frequent use of antibiotics with broad gram-negative activity and shorter postdischarge treatment durations.
Infect Control Hosp Epidemiol 2017;38:534–541
TEM Characterization of ion radiation damage in Ca(1-X)La2X/3TiO3 Perovskites
- Mohsen Danaie, Stella Pedrazzini, Neil P. Young, Paul A. J. Bagot, Karl R. Whittle, Philip D. Edmondson
-
- Journal:
- Microscopy and Microanalysis / Volume 21 / Issue S3 / August 2015
- Published online by Cambridge University Press:
- 23 September 2015, pp. 1335-1336
- Print publication:
- August 2015
-
- Article
-
- You have access Access
- Export citation
Contributors
-
- By Lenard A. Adler, Pinky Agarwal, Rehan Ahmed, Jagga Rao Alluri, Fawaz Al-Mufti, Samuel Alperin, Michael Amoashiy, Michael Andary, David J. Anschel, Padmaja Aradhya, Vandana Aspen, Esther Baldinger, Jee Bang, George D. Baquis, John J. Barry, Jason J. S. Barton, Julius Bazan, Amanda R. Bedford, Marlene Behrmann, Lourdes Bello-Espinosa, Ajay Berdia, Alan R. Berger, Mark Beyer, Don C. Bienfang, Kevin M. Biglan, Thomas M. Boes, Paul W. Brazis, Jonathan L. Brisman, Jeffrey A. Brown, Scott E. Brown, Ryan R. Byrne, Rina Caprarella, Casey A. Chamberlain, Wan-Tsu W. Chang, Grace M. Charles, Jasvinder Chawla, David Clark, Todd J. Cohen, Joe Colombo, Howard Crystal, Vladimir Dadashev, Sarita B. Dave, Jean Robert Desrouleaux, Richard L. Doty, Robert Duarte, Jeffrey S. Durmer, Christyn M. Edmundson, Eric R. Eggenberger, Steven Ender, Noam Epstein, Alberto J. Espay, Alan B. Ettinger, Niloofar (Nelly) Faghani, Amtul Farheen, Edward Firouztale, Rod Foroozan, Anne L. Foundas, David Elliot Friedman, Deborah I. Friedman, Steven J. Frucht, Oded Gerber, Tal Gilboa, Martin Gizzi, Teneille G. Gofton, Louis J. Goodrich, Malcolm H. Gottesman, Varda Gross-Tsur, Deepak Grover, David A. Gudis, John J. Halperin, Maxim D. Hammer, Andrew R. Harrison, L. Anne Hayman, Galen V. Henderson, Steven Herskovitz, Caitlin Hoffman, Laryssa A. Huryn, Andres M. Kanner, Gary P. Kaplan, Bashar Katirji, Kenneth R. Kaufman, Annie Killoran, Nina Kirz, Gad E. Klein, Danielle G. Koby, Christopher P. Kogut, W. Curt LaFrance, Patrick J.M. Lavin, Susan W. Law, James L. Levenson, Richard B. Lipton, Glenn Lopate, Daniel J. Luciano, Reema Maindiratta, Robert M. Mallery, Georgios Manousakis, Alan Mazurek, Luis J. Mejico, Dragana Micic, Ali Mokhtarzadeh, Walter J. Molofsky, Heather E. Moss, Mark L. Moster, Manpreet Multani, Siddhartha Nadkarni, George C. Newman, Rolla Nuoman, Paul A. Nyquist, Gaia Donata Oggioni, Odi Oguh, Denis Ostrovskiy, Kristina Y. Pao, Juwen Park, Anastas F. Pass, Victoria S. Pelak, Jeffrey Peterson, John Pile-Spellman, Misha L. Pless, Gregory M. Pontone, Aparna M. Prabhu, Michael T. Pulley, Philip Ragone, Prajwal Rajappa, Venkat Ramani, Sindhu Ramchandren, Ritesh A. Ramdhani, Ramses Ribot, Heidi D. Riney, Diana Rojas-Soto, Michael Ronthal, Daniel M. Rosenbaum, David B. Rosenfield, Durga Roy, Michael J. Ruckenstein, Max C. Rudansky, Eva Sahay, Friedhelm Sandbrink, Jade S. Schiffman, Angela Scicutella, Maroun T. Semaan, Robert C. Sergott, Aashit K. Shah, David M. Shaw, Amit M. Shelat, Claire A. Sheldon, Anant M. Shenoy, Yelizaveta Sher, Jessica A. Shields, Tanya Simuni, Rajpaul Singh, Eric E. Smouha, David Solomon, Mehri Songhorian, Steven A. Sparr, Egilius L. H. Spierings, Eve G. Spratt, Beth Stein, S.H. Subramony, Rosa Ana Tang, Cara Tannenbaum, Hakan Tekeli, Amanda J. Thompson, Michael J. Thorpy, Matthew J. Thurtell, Pedro J. Torrico, Ira M. Turner, Scott Uretsky, Ruth H. Walker, Deborah M. Weisbrot, Michael A. Williams, Jacques Winter, Randall J. Wright, Jay Elliot Yasen, Shicong Ye, G. Bryan Young, Huiying Yu, Ryan J. Zehnder
- Edited by Alan B. Ettinger, Albert Einstein College of Medicine, New York, Deborah M. Weisbrot, State University of New York, Stony Brook
-
- Book:
- Neurologic Differential Diagnosis
- Published online:
- 05 June 2014
- Print publication:
- 17 April 2014, pp xi-xx
-
- Chapter
- Export citation
Irradiation Induced Effects at Interfaces in a Nanocrystalline Ceria Thin Film on a Si Substrate
- Philip D Edmondson, Neil P Young, Chad M Parish, Fereydoon Namavar, William J Weber, Yanwen Zhang
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1514 / 2013
- Published online by Cambridge University Press:
- 18 March 2013, pp. 87-92
- Print publication:
- 2013
-
- Article
- Export citation
-
Thin films of nanocrystalline ceria on a Si substrate have been irradiated with 3 MeV Au+ ions to fluences of up to 1x1016 ions cm-2, at temperatures ranging between 160 to 400 K. During the irradiation, a band of contrast is observed to form at the thin film/substrate interface. Analysis by scanning transmission electron microscopy in conjunction with energy dispersive and electron energy loss spectroscopy techniques revealed that this band of contrast was a cerium silicate amorphous phase, with an approximate Ce:Si:O ratio of 1:1:3.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Deficits in facial, body movement and vocal emotional processing in autism spectrum disorders
- R. C. M. Philip, H. C. Whalley, A. C. Stanfield, R. Sprengelmeyer, I. M. Santos, A. W. Young, A. P. Atkinson, A. J. Calder, E. C. Johnstone, S. M. Lawrie, J. Hall
-
- Journal:
- Psychological Medicine / Volume 40 / Issue 11 / November 2010
- Published online by Cambridge University Press:
- 27 January 2010, pp. 1919-1929
-
- Article
- Export citation
-
Background
Previous behavioural and neuroimaging studies of emotion processing in autistic spectrum disorder (ASD) have focused on the use of facial stimuli. To date, however, no studies have examined emotion processing in autism across a broad range of social signals.
MethodThis study addressed this issue by investigating emotion processing in a group of 23 adults with ASD and 23 age- and gender-matched controls. Recognition of basic emotions (‘happiness’, ‘sadness’, ‘anger’, disgust' and ‘fear’) was assessed from facial, body movement and vocal stimuli. The ability to make social judgements (such as approachability) from facial stimuli was also investigated.
ResultsSignificant deficits in emotion recognition were found in the ASD group relative to the control group across all stimulus domains (faces, body movements and voices). These deficits were seen across a range of emotions. The ASD group were also impaired in making social judgements compared to the control group and this correlated with impairments in basic emotion recognition.
ConclusionsThis study demonstrates that there are significant and broad-ranging deficits in emotion processing in ASD present across a range of stimulus domains and in the auditory and visual modality; they cannot therefore be accounted for simply in terms of impairments in face processing or in the visual modality alone. These results identify a core deficit affecting the processing of a wide range of emotional information in ASD, which contributes to the impairments in social function seen in people with this condition.
Contributors
-
- By Sonia Ancoli-Israel, Ragnar Asplund, Michel Billiard, Theresa M. Buckley, Rohit Budhiraja, Robert N. Butler, Daniel J. Buysse, Scott S. Campbell, Daniel P. Cardinali, Julie Carrier, Cynthia L. Comella, Jana R. Cooke, Pietro Cortelli, Agnès Demazieres, Glenna A. Dowling, Luigi Ferini-Strambi, Philip R. Gehrman, Nalaka Sudheera Gooneratne, David S. Hallegua, Patrick J. Hanly, David G. Harper, Orla P. Hornung, Magdolna Hornyak, Michal Karasek, Milton Kramer, Andrew D. Krystal, Malcolm H. Lader, Rachel Leproult, Kenneth L. Lichstein, Andrea H.S. Loewen, Rémy Luthringer, Laurin J. Mack, Evelyn Mai, Atul Malhotra, Jennifer L. Martin, Judy Mastick, Monique A.J. Mets, Andrew A. Monjan, Timothy H. Monk, Daniel Monti, Jaime M. Monti, Patricia J. Murphy, C. Ineke Neutel, Eric A. Nofzinger, Seithikurippu R. Pandi-Perumal, Scott B. Patton, Donald B. Penzien, Max H. Pittler, Giora Pillar, Marc J. Poulin, Louis J. Ptácek, Stuart F. Quan, Jeanetta C. Rains, Megan E. Ruiter, Bruce D. Rybarczyk, Colin M. Shapiro, Vijay Kumar Sharma, D. Warren Spence, Kai Spiegelhalder, Luc Staner, Stephanie A. Studenski, Nikola N. Trajanovic, Eve Van Cauter, Gregory S. Vander Wal, Joris C. Verster, Aleksandar Videnovic, Matthew P. Walker, Daniel J. Wallace, David K. Welsh, David P. White, Barbara Wider, Theresa B. Young, Stefano Zanigni
- Edited by S. R. Pandi-Perumal, Jaime M. Monti, Universidad de la República, Uruguay, Andrew A. Monjan, National Institute on Aging, Bethesda, Maryland
-
- Book:
- Principles and Practice of Geriatric Sleep Medicine
- Published online:
- 04 August 2010
- Print publication:
- 26 November 2009, pp ix-xii
-
- Chapter
- Export citation
Contributors
-
- By Phillip L. Ackerman, Neil Anderson, Jens B. Asendorpf, R. Michael Bagby, Michael Harris Bond, Gregory J. Boyle, Andrea L. Briggs, Giles St J. Burch, Turhan Canli, David Canter, Gianvittorio Caprara, Charles S. Carver, Douglas F. Cellar, Gordon Claridge, Susan Cloninger, Elisabeth D. Conradt, Philip J. Corr, Sharon Dawe, Ian J. Deary, Boele De Raad, Edward L. Deci, Colin G. DeYoung, M. Brent Donnellan, Juris G. Draguns, Marko Elovainio, Aurelio José Figueredo, David C. Funder, Paul Gladden, Rapson Gomez, Samuel D. Gosling, Jeremy R. Gray, Robert D. Hare, B. Austin Harley, Edward Helmes, Robert Hogan, Lauri A. Jensen-Campbell, Daniel Nelson Jones, Mika Kivimäki, Jennifer M. Knack, James T. Lamiell, Natalie J. Loxton, Geoff MacDonald, Gerald Matthews, Robert R. McCrae, Mario Mikulincer, Stephanie N. Mullins-Sweatt, Marcus R. Munafò, Vickie Nam, Craig S. Newmann, Rainer Reisenzein, Madeline Rex-Lear, Richard W. Robins, Michael D. Robinson, Mary K. Rothbart, Richard M. Ryan, Gerard Saucier, Michael F. Scheier, Constantine Sedikides, Phillip R. Shaver, Brad E. Sheese, Yuichi Shoda, Ronald E. Smith, Alice F. Stuhlmacher, Rhonda Swickert, Avril Thorne, David D. Vachon, Geneva Vásquez, Michele Vecchione, Seth A. Wagerman, Fiona Warren, Hannelore Weber, Thomas A. Widiger, Pedro Sofio Abril Wolf, Donna Youngs, Moshe Zeidner
- Edited by Philip J. Corr, University of East Anglia, Gerald Matthews, University of Cincinnati
-
- Book:
- The Cambridge Handbook of Personality Psychology
- Published online:
- 05 June 2012
- Print publication:
- 16 July 2009, pp xv-xvii
-
- Chapter
- Export citation
Longitudinal decrements in iron status during military training in female soldiers
- James P. McClung, J. Philip Karl, Sonya J. Cable, Kelly W. Williams, Andrew J. Young, Harris R. Lieberman
-
- Journal:
- British Journal of Nutrition / Volume 102 / Issue 4 / 28 August 2009
- Published online by Cambridge University Press:
- 28 January 2009, pp. 605-609
- Print publication:
- 28 August 2009
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Fe is an essential micronutrient required for optimal cognitive and physical performance. Cross-sectional studies indicate that training degrades Fe status in female military personnel; however, longitudinal studies to measure the direct impact of military training on Fe status and performance have not been conducted. As such, the objective of the present study was to determine the longitudinal effects of military training on Fe status in female soldiers. Fe status was assessed in ninety-four female soldiers immediately before and following a 9-week basic combat training (BCT) course. Fe status indicators included Hb, erythrocyte distribution width (RDW), serum ferritin, transferrin saturation and soluble transferrin receptor (sTfR). A 2-mile (3·2 km) run test was performed at the end of BCT to assess aerobic performance. Fe status was affected by BCT, as all Fe status indicators, excluding Hb, were diminished (P ≤ 0·01) at the end of BCT. Fe status indicators at the end of BCT (Hb and RDW) were associated (P ≤ 0·05) with running performance, as was the change in sTfR over the training period (r 0·320; P ≤ 0·05). In conclusion, Fe status in female soldiers is degraded during BCT, and degraded Fe status is associated with diminished aerobic performance. Female athletes and military personnel should strive to maintain Fe status to optimise physical performance.
Contributors
-
- By Nicholas B. Allen, Joan Rosenbaum Asarnow, Jeanne Brooks-Gunn, Ronald E. Dahl, Joanne Davila, Laura M. DeRose, Lea R. Dougherty, Nancy Eisenberg, Erika E. Forbes, Wyndol Furman, Paul Gilbert, Julia A. Graber, Danielle M. Hessler, Erin C. Hunter, Chris Irons, Lynn Fainsilber Katz, Amanda Kesek, Daniel N. Klein, Annette M. La Greca, Rebecca S. Laptook, Reed W. Larson, Primrose Letcher, Peter M. Lewinsohn, Marc D. Lewis, Christine McDunn, James W. McKowen, Christopher S. Monk, Amanda Sheffield Morris, Thomas M. Olino, Tomáš Paus, Daniel S. Pine, Ann V. Sanson, John R. Seeley, Lisa B. Sheeber, Rebecca Siegel, Jennifer S. Silk, Diana Smart, Martha C. Tompson, Julie Vaughan, Brennan J. Young, Philip David Zelazo
- Edited by Nicholas B. Allen, University of Melbourne, Lisa B. Sheeber
-
- Book:
- Adolescent Emotional Development and the Emergence of Depressive Disorders
- Published online:
- 14 September 2009
- Print publication:
- 20 November 2008, pp ix-xiv
-
- Chapter
- Export citation
POPULATION-BASED AND OPPORTUNISTIC SCREENING AND ERADICATION OF HELICOBACTER PYLORI: An Analysis Using Trial Baseline Data
- James M. Mason, Paul Moayyedi, Philip J. Young, Sara Duffett, Will Crocombe, Michael F. Drummond, Anthony T. R. Axon, For the Leeds H. pylori Study Group
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 15 / Issue 4 / October 1999
- Published online by Cambridge University Press:
- 01 October 1999, pp. 649-660
-
- Article
- Export citation
-
Objectives: To examine whether screening and eradication of Helicobacter pylori by population-based invitation or opportunistic screening by general practitioners reduces costs to the National Health Service (NHS) of treating dyspepsia.
Methods: A limited dependent, variable, two-step regression analysis was used to explore the baseline annual health care costs of dyspepsia for men and women aged 40–49 enrolled in the Leeds H. pylori screening and eradication trial.
Results: Epidemiological and clinical questionnaires, general practitioner notes, and 13C urea breath test results were available for 4,754 individuals. After adjusting for covariates, H. pylori was associated with a 6.7% increased probability of incurring gastrointestinal-related NHS costs (p < .0001) in the population aged 40-49. Additionally, H pylori increased average costs in those who seek medical care (p = .001). In consequence, H. pylori is associated with an average increased cost to the NHS of £0.30 per year (95% CI: £0.17 to £0.45) per adult aged 40–49. In those consulting for dyspepsia, the increased cost to the NHS was £1.04 per year (95% CI: £0.42 to £1.75) per patient. The cost of population screening and treatment would not be recovered in reduced dyspepsia costs in the lifetime of those screened. Assuming laboratory-based serology screening is used opportunistically in patients presenting with dyspepsia, it is estimated that costs would be recouped in 18 years.
Conclusions: This observational data set suggests that the costs of screening and treatment in all individuals aged 40–49 or in those presenting in primary care with dyspeptic symptoms are unlikely to be attractive on the basis of cost savings alone.