3 results
COVID-19 related Delusional Beliefs: A Case Report
- S. Akyildirim Cor, B. D. Akcay
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S809-S810
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A delusion is a fixed false belief based on an inaccurate interpretation of an external reality despite evidence to the contrary. The diagnosis of a delusional disorder is made when a person has one or more non-bizarre (situations that are not real but also not impossible) delusional thoughts for one month or more that cannot be explained by any other condition. In patients with delusional disorder, delusions(s) do not impact the functionality and the patient’s behavior is not overtly bizarre. Although delusional core themes tend to be the same throughout different epochs (i.e., persecution, grandiosity, guilt, religion, hypochondria, love, or jealous), clinicians commonly notice how delusions tend to rapidly incorporate popular hot topical issues. Hence, delusions are dynamic and often represent a combination of psychopathology and external events.
ObjectivesThe COVID-19 outbreak has affected millions of people globally and it also has a huge psychological impact. The objective of this case report is to outline the possible effect of the COVID-19 pandemic to delusional disorder in patients with healthy person.
MethodsThe 40-year-old gentleman, a drum major (field commander), married, living with his wife and daughter (4,5 years old). He’s current complaints started when he did not want to have the Covid vaccine in April 2021 and therefore was exposed to mobbing at work. It is understood that the patient had irrevocable ideas about vaccine and PCR testing (radioactive lights were coming out from the PCR rod in a video he watched). For this reason, it is understood during the clinical interview that the patient was exposed to social restrictions at work and in his social life (he could not travel by public transport, plane, bus, and enter social facilities because he did not have a vaccination card or did not have a PCR test).He was admitted to our ward for the purpose of arranging his diagnosis and treatment.
ResultsOn our ward, the patient showed poor insight with persistence of delusions. The impression was delusinal disorder. He was treated with olanzapine up to 5 mg/day and sertraline up to 100 mg/day, with a progressive resolution of symptoms.
ConclusionsThere are other case reports on COVID-19 delusional themes in patients with schizophrenia and patients with no history of mental illness, which means that this phenomenon is not exclusive to affective disorders. In this case, different from the literature, the patient has never had covid. An area of clinical concern is the potential of the pandemic’s psychological context to trigger psychotic disorders and influence their symptomatology. A review of contemporary epidemics and pandemics psychosis research found no evidence of changes in the form and content of psychotic symptoms. Further research should examine those biopsychosocial COVID-related factors that predispose to, precipitate, and perpetuate psychosis.
Disclosure of InterestNone Declared
Psychological Inflexibility in Depression with Psychotic Features: A Case Report
- S. Akyildirim Cor, S. Yetkin
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1027
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a mood disorder that can last for weeks or even months, in which there is a depressed mood accompanied by anxiety, in addition to negative changes in cognitive functions, psychomotor movement and vegetative functions. Depression with psychotic features is a psychiatric syndrome that progresses with delusions as well as severe symptoms such as psychomotor retardation or agitation, depressive ruminations, deterioration in cognitive functions, and confusion. Compared to the subtypes without psychotic features, the symptoms are more severe, the age of onset is earlier, and the duration of the disease is longer. Feelings of guilt, worthlessness and suicidal thoughts and attempts at suicide are more common. The risk of exacerbation is greater. Diagnosis of bipolar disorder and schizophrenia is more common in first-degree relatives of these patients.
ObjectivesAn 18-year-old female patient with somatic delusions and psychotic persistence that started after a sexual trauma and persisted for 1 month was consulted after organic exclusions were made. It is understood from the anamnesis that the patient had a manic episode about 6 months ago and that his mother was followed up with a diagnosis of bipolar disorder. The patient’s current clinical picture was evaluated as depression with psychotic features, and after hospitalization, the treatment was adjusted as fluoxetine 20 mg/g, olanzapine 5 mg/g, and lithium 900 mg/g. Self as context, cognitive defusion and acceptance interventions were applied to the patient.
MethodsWhen the Cognitive Fusion Questionnaire(CFQ), Self-as-Context Scale(SACS), Acceptance and Action Questionnaire(AAQ-II) completed by the patient during hospitalization and in remission periods were compared, it was observed that there was a significant regression in the patient’s psychological inflexibility during the period of remission. Written informed consent was obtained from the patient whose clinical picture was presented in order to contribute to the scientific literature.
ResultsDepression with psychotic features is another clinical picture in which psychological inflexibility increases, and it has been observed that interviews to increase psychological flexibility during the treatment process contribute positively to the treatment process. For this reason, the contribution to the healing process can be better clarified in further studies on interventions to increase psychological flexibility applied in addition to pharmacological treatments.
Image:
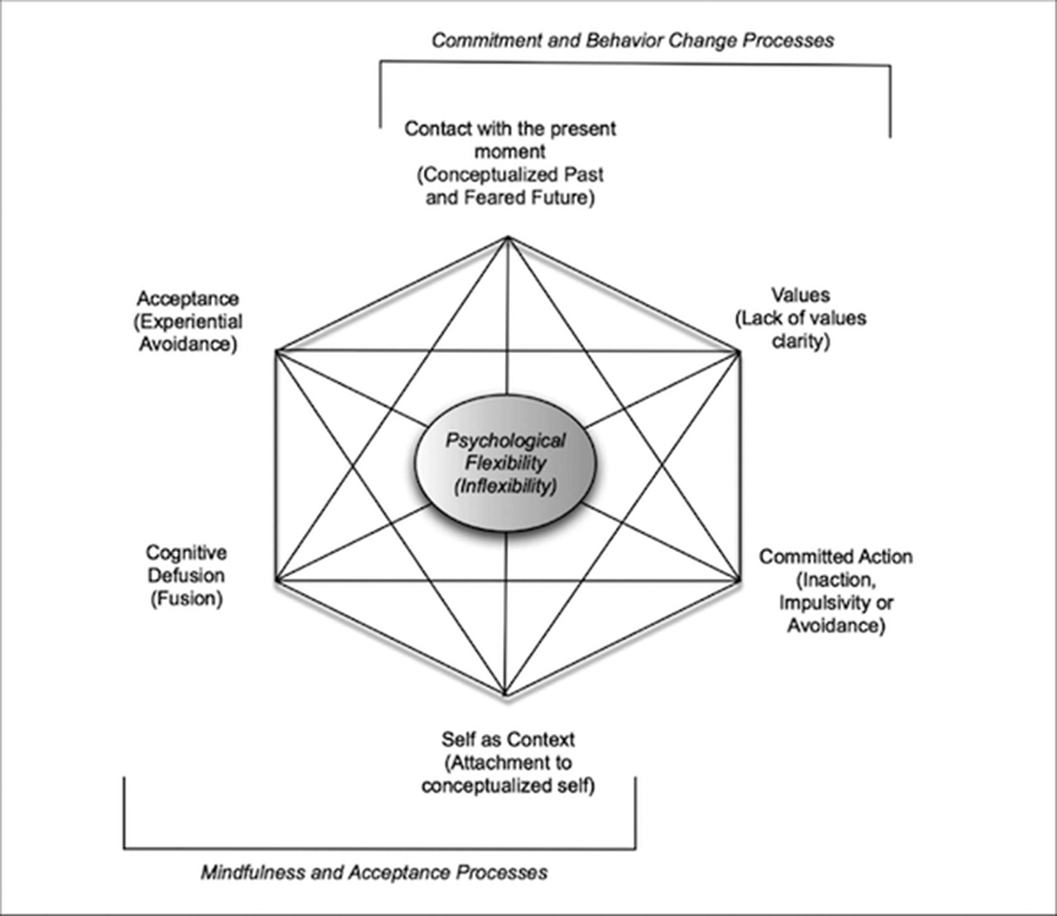 Conclusions
ConclusionsPsychological inflexibility is an effort to control a person’s emotion, thought, behavior or experience in a dysfunctional way in the face of an undesired experience. It has been seen in studies conducted in recent years that; There is a significant positive correlation between high psychological inflexibility and somatization, depression, anxiety and other psychological disorders.
Disclosure of InterestNone Declared
A Case of Adult Attention Deficit Hyperactivity Disorder with Non-Organic Psychosis Comorbidity
- S. Akyıldırım Çor, M. Duman, Ö. Uzun
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S468-S469
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Although ADHD is the most frequently diagnosed psychiatric disorder in childhood, the majority of adults with ADHD are not diagnosed and 90% of the cases remain untreated. One of the main reasons that may lead to the missed diagnosis of ADHD in adults may be the high rate of comorbid psychiatric conditions masking the main symptoms.
ObjectivesIn this study, it was aimed to present a case who was followed up with the diagnosis of ADHD since childhood and developed psychosis after a recent traumatic life event.
MethodsA 19-year-old male patient was consulted because of his complaints of persecution delusions, and disorganized speech that started 2 years ago. IIt was learned that the first psychiatry application of the patient was 10 years ago with complaints of impulsivity, aggression, increased psychomotor movements, and methylphenidate treatment was started during this period. The patient, whose current clinical picture was evaluated as psychosis, was discharged after the symptoms subsided with paliperidone depot 100mg/month treatment after hospitalization. It is understood that his psychotic complaints completely regressed in the follow-ups.
ResultsIt is stated that approximately 80% of adult ADHD cases have at least one accompanying psychiatric disorder. However, there are limited studies in the literature on the relationship between psychotic disorders and ADHD.
ConclusionsRecent studies indicate that beyond the fact that ADHD is a feature of the schizophrenia prodrome, ADHD diagnosis may be associated with an increased risk of psychosis in the future. Therefore, this association can be better clarified in further studies on comorbidities.
DisclosureNo significant relationships.




