14 results
PP129 Health Technology Assessment Adaptation: Pharyngolaryngeal Biopsies (OLB) For People with Suspected Head and Neck Cancer in the Outpatient Setting
- Charlotte Bowles, Rebecca Boyce, Gareth Hopkin, Matthew Prettyjohns, Sophie Hughes, Elise Hasler, Katie McDermott, Susan Myles
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 39 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 14 December 2023, p. S86
-
- Article
-
- You have access Access
- Export citation
-
Introduction
In the UK over 12,400 yearly cases of head and neck cancers are reported (2021). Pharyngolaryngeal biopsies (OLB) may improve the speed of diagnosis and treatment of head and neck cancers under local anesthetic. The Scottish Health Technologies Group (SHTG) published advice on this technology in 2018. Since this, additional evidence has been published to warrant a health technology assessment (HTA) for Wales. The aim of this review was to provide update on the clinical and cost-effectiveness of OLB when compared to undergoing biopsy in an operating theatre (OTB) under general anesthetic to inform decision making in Wales.
MethodsA rapid review was undertaken of relevant databases since 2018 of the clinical evidence, health economics and patient perspectives relevant to Wales. Health Technology Wales (HTW) developed a de-novo cost-utility analysis comparing OLB to OTB over a lifetime horizon. Inputs were sourced from the SHTG budget impact analysis, updated with values more relevant to a Welsh setting.
ResultsFrom consultation to biopsy procedure, the mean number of days was 1.3 for OLB compared to 17.4 days under OTB (p < 0.05). The mean time from consultation to start of treatment was 27 days for OLB compared to 41.5 days for OTB (p < 0.05). The economic analysis found a resulting ICER of GBP21,011 (EUR23,824.23) in a population with 2,183 at risk patients. As OLB was associated with lower costs (GBP816 per person) (EUR925.26) and fewer quality adjusted life years than OTB (-0.04), this ICER corresponds to OLB being considered a cost-effective diagnostic strategy.
ConclusionsHTW guidance was able to recommend use of OLB within the diagnostic pathway for head and neck cancers within Wales. For people with a positive test, OLB is sufficient to confirm a diagnosis but should not be used to rule out a diagnosis due to the potential in reducing the time to diagnosis and treatment in a cost-saving way.
Attribution of nosocomial seeding to long-term care facility COVID-19 outbreaks
- Joe Flannagan, Dimple Y Chudasama, Russell Hope, Simon M Collin, Alex Bhattacharya, Rachel Merrick, Nurin Abdul Aziz, Susan Hopkins, Gavin Dabrera, Theresa Lamagni
-
- Journal:
- Epidemiology & Infection / Volume 151 / 2023
- Published online by Cambridge University Press:
- 25 October 2023, e191
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Residents of long-term care facilities (LTCFs) were disproportionately affected by the COVID-19 pandemic. We assessed the extent to which hospital-associated infections contributed to COVID-19 LTCF outbreaks in England. We matched addresses of cases between March 2020 and June 2021 to reference databases to identify LTCF residents. Linkage to health service records identified hospital-associated infections, with the number of days spent in hospital before positive specimen date used to classify these as definite or probable. Of 149,129 cases in LTCF residents during the study period, 3,748 (2.5%) were definite or probable hospital-associated and discharged to an LTCF. Overall, 431 (0.3%) were identified as index cases of potentially nosocomial-seeded outbreaks (2.7% (431/15,797) of all identified LTCF outbreaks). These outbreaks involved 4,521 resident cases and 1,335 deaths, representing 3.0% and 3.6% of all cases and deaths in LTCF residents, respectively. The proportion of outbreaks that were potentially nosocomial-seeded peaked in late June 2020, early December 2020, mid-January 2021, and mid-April 2021. Nosocomial seeding contributed to COVID-19 LTCF outbreaks but is unlikely to have accounted for a substantial proportion. The continued identification of such outbreaks after the implementation of preventative policies highlights the challenges of preventing their occurrence.
PP72 SARS-CoV-2: A Rapid Review On The Effectiveness Of Face Coverings To Reduce Transmission
- Thomas Winfield, Gareth Hopkin, Lauren Elston, Claire Davis, Jenni Washington, David Jarrom, Katie McDermott, Susan Myles
-
- Journal:
- International Journal of Technology Assessment in Health Care / Volume 38 / Issue S1 / December 2022
- Published online by Cambridge University Press:
- 23 December 2022, pp. S63-S64
-
- Article
-
- You have access Access
- Export citation
-
Introduction
At various stages of the COVID-19 pandemic, face coverings have been recommended and encouraged as one of the interventions to reduce transmission of the SARS-CoV-2 virus. However, in the earlier stages of the pandemic, decisions on face coverings relied primarily on evidence based on other viral respiratory infections. More direct evidence on the use of face coverings with COVID-19 developed in tandem with the pandemic.
Health Technology Wales undertook an ultra-rapid review to inform national guidelines, the work assessed the evidence on the effectiveness of face coverings to reduce SARS-CoV-2 transmission. We also reviewed evidence on the efficacy of different types of face coverings.
MethodsWe conducted a systematic literature search for evidence to address (i) the effectiveness of face coverings to reduce the spread of COVID-19 in the community, and (ii) the efficacy of different types of face coverings designed for use in community settings. We identified a rapid review in 2021 by Public Health England that closely aligned with our review questions. This provided the main source for identifying relevant studies, supplemented by a search for publications following their search date.
ResultsWe identified two evidence reviews (including the Public Health England review) that examined the effectiveness of face coverings on reducing transmission of SARS-CoV-2; reporting on 31 and 39 studies, respectively. Two further primary studies were published after the two evidence review searches were included. Overall, the evidence suggested that face coverings may provide benefits in preventing SARS-CoV-2 transmission, although the higher-quality studies suggested that these benefits may be modest. Medical masks appeared to have higher efficacy than fabric masks, although the evidence was mixed.
ConclusionsAt the time of this review, evidence on the effectiveness of face coverings remains limited and conclusions rely on low-quality sources of evidence with high risk of bias, although higher-quality evidence points to some benefit. Face coverings may play a role in preventing transmission of SARS-CoV-2, particularly as part of a bundle of other preventative measures.
Public health impact of mass sporting and cultural events in a rising COVID-19 prevalence in England
- Part of
- Jenifer A. E. Smith, Susan Hopkins, Charlie Turner, Kyle Dack, Anna Trelfa, Jerlyn Peh, Paul S. Monks
-
- Journal:
- Epidemiology & Infection / Volume 150 / 2022
- Published online by Cambridge University Press:
- 31 January 2022, e42
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
A subset of events within the UK Government Events Research Programme (ERP), developed to examine the risk of transmission of COVID-19 from attendance at events, was examined to explore the public health impact of holding mass sporting events. We used contact tracing data routinely collected through telephone interviews and online questionnaires, to describe the potential public health impact of the large sporting and cultural events on potential transmission and incidence of COVID-19. Data from the EURO 2020 matches hosted at Wembley identified very high numbers of individuals who tested positive for COVID-19 and were traced through NHS Test & Trace. This included both individuals who were potentially infectious (3036) and those who acquired their infection during the time of the Final (6376). This is in contrast with the All England Lawn Tennis Championships at Wimbledon, where there were similar number of spectators and venue capacity but there were lower total numbers of potentially infectious cases (299) and potentially acquired cases (582). While the infections associated with the EURO 2020 event may be attributed to a set of socio-cultural circumstances which are unlikely to be replicated for the forthcoming sporting season, other aspects may be important to consider including mitigations for spectators to consider such as face coverings when travelling to and from events, minimising crowding in poorly ventilated indoor spaces such as bars and pubs where people may congregate to watch events, and reducing the risk of aerosol exposure through requesting that individuals avoid shouting and chanting in large groups in enclosed spaces.
Antimicrobial Stewardship-Driven Monoclonal Antibody Treatment Program for COVID-19 Patients in the Bronx, New York
- Yi Guo, Victor Chen, Lauren Allen, Kelsie Cowman, Una Hopkins, Carol Sheridan, Edwin A Torres, Patricia Davis, Susan Sakalian, Frank Sosnowski, Priya Nori, Liise-anne Pirofski, Adam Haviland, James Rossi, Hongkai (Jack) Bao
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 1 / Issue S1 / July 2021
- Published online by Cambridge University Press:
- 29 July 2021, p. s57
-
- Article
-
- You have access Access
- Open access
- Export citation
-
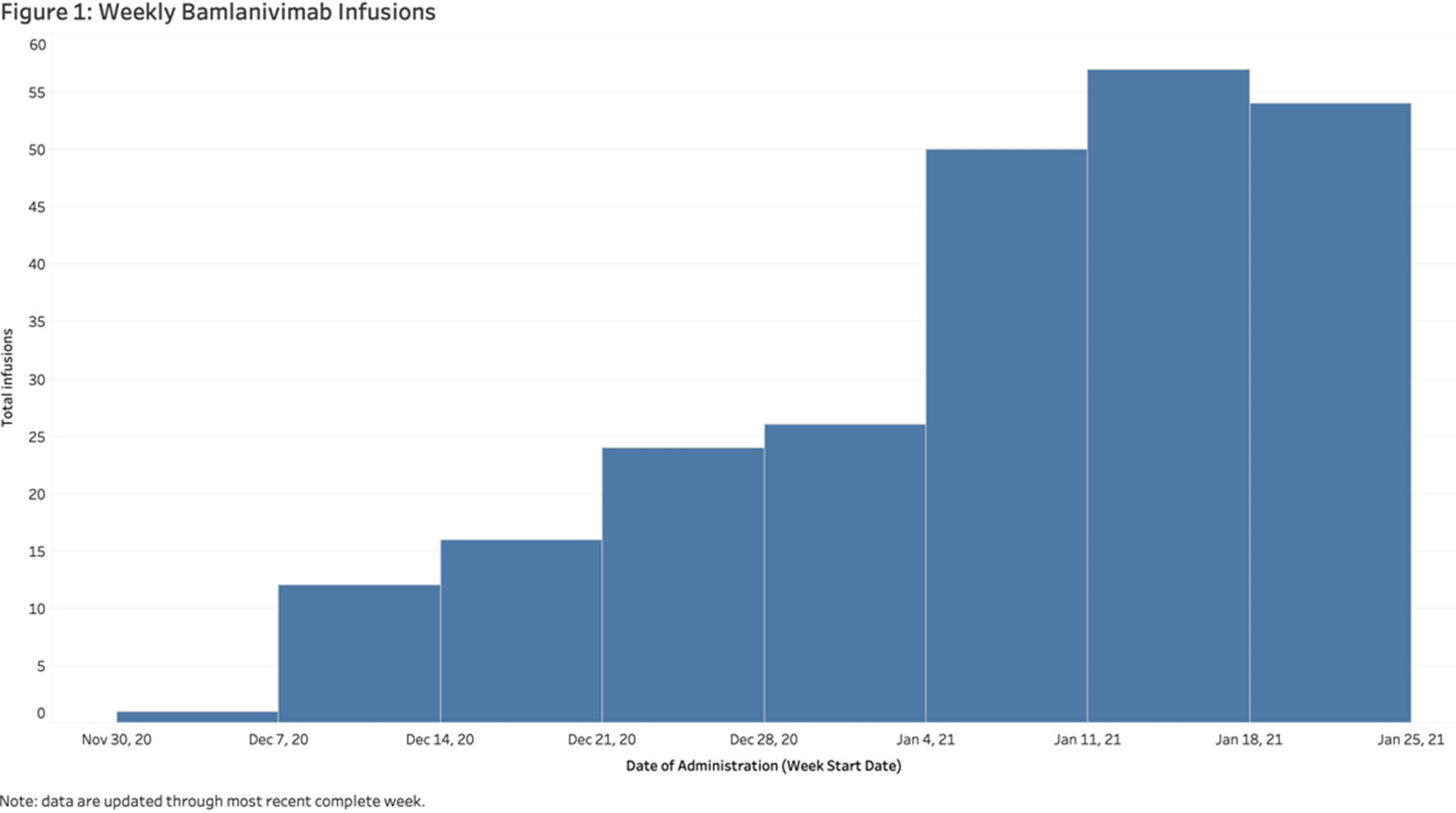
Background: In November 2020, bamlanivimab received emergency use authorization (EUA) to treat patients with early, mild-to-moderate COVID-19 who are at high risk of progression. Montefiore Medical Center serves an economically underserved community of >1.4 million residents in the Bronx, New York. Montefiore’s antimicrobial stewardship team (AST) developed a multidisciplinary treatment pathway for patients meeting EUA criteria: (1) outpatients and hospital associates and (2) acute-care patients (EDs or inpatient). Methods: The Montefiore AST established a centralized process for screening high-risk COVID-19 patients 7 days a week. Referrals were sent by e-mail from occupational health, primary care practices, specialty practices, emergency departments, and urgent care centers. Patients were screened in real time and were treated in the ED or a newly established infusion center within 24 hours. After infusion, all patients received phone calls from nurses and had an infectious diseases televisit. Demographics, clinical symptoms, subsequent ED visit or hospital admission, and timing from infusion to ED or hospitalization were obtained from the electronic health record. Results: In total, 281 high-risk patients (median age, 62 years; 57% female) received bamlanivimab at the infusion center or in the acute-care setting between December 2, 2020, and January 27, 2021 (Table 1). The number of treated patients increased weekly (Figure 1). Also, 62% were Hispanic or black, and 96% met EUA criteria. Furthermore, 51 (18%) were referred from occupational health, 205 (73%) were referred from the community, and 25 (9%) were inpatients (https://www.fda.gov/media/143605/download). All patients were successfully infused without adverse reactions. In addition, 23 patients (8.2%) were hospitalized and 6 (2.1%) visited EDs within 30 days of treatment. The average number of days between symptom onset and infusion was 4.9. The median age of admitted versus nonadmitted patients was 68 years versus 61.5 years (P = .07). Conclusions: An AST-coordinated bamlanivimab treatment program successfully treated multiple high-risk COVID-19 patients and potentially reduced hospitalizations. However, the effort, personnel, and resources required are significant. Dedicated hospital investment is necessary for maximal success.
Funding: No
Disclosures: None
Table 1. 
Figure 1.
A Ten-Year Review of Carbapenemase Producing Enterobacterales (CPE) in London, United Kingdom
- Bharatkumar Patel, Katie Hopkins, Daniele Meunier, Peter Staves, Susan Hopkins, Neil Woodford
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, pp. s6-s7
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: To determine the pattern of CPE observed in a single region in the United Kingdom. Methods: From 2009 to 2018, clinical laboratories in England were requested to send suspected CPE from all sites to the national reference laboratory for confirmation and investigation of carbapenem resistance mechanism(s). Isolates of Enterobacterales from London laboratories and confirmed to have 1 or more carbapenemase genes were included in the analysis. Result: Between 2009 and 2018, 5,133 isolates were confirmed to produce a carbapenemase; at least 1 CPE was identified in every London Laboratory and hospital. Confirmations increased from 28 isolates in 2009 to 1857 in 2018 and with a sharp rise after the introduction of the ‘PHE toolkit’ in 2013 (Fig. 1). Most CPE (2655, 51.7%) were from rectal screens (the 3 most frequently identified carbapenemase families were OXA-48–like in 1,263 isolates, NDM in 971 and IMP in 128), 631 (12.3%) were from urine samples, 180 (3.5%) from blood cultures, 103 (2.0%) from sputum specimens and the remainder (1564, 30.5%) were swabs, fluids and tissues from various body sites. Moreover, 51 CPE (1%) were identified from environmental swabs. Isolates were predominantly Klebsiella spp (2,525, 49%; 2,088 were K. pneumoniae), followed by Escherichia coli (1,434, 27.9%), Enterobacter spp (746, 14.5%; 605 were E. cloacae complex), and Citrobacter spp (349, 6.8%); 10 other species contributed smaller numbers. Within the carbapenemase families, OXA-48-like enzymes predominated overall (2303, 44.9%), followed by NDM (1822, 35.5%), IMP (313, 6.1%), VIM (207, 4.0%), NDM+OXA-48-like (205, 4.0%), and KPC (196, 3.8%). The first detection of a CPE with 2 distinct enzymes occurred in 2012 (OXA-48-like and NDM) and since then 235 co-detections have been identified; 233 related to OXA-48-like with another gene. Conclusion: The first CPE isolate in London was identified in 2003, a Klebsiella spp with a VIM enzyme. The number of isolates submitted to the national reference laboratory has continued to increase year on year. VIM and NDM carbapenemases predominated in the early years, because of their association with several outbreaks; these have now been overwhelmed by OXA-48-like detections and outbreaks. The increasing numbers of CPE with a combination of a metallo- and a non-metallo carbapenemase increases the therapeutic challenges to treat infected patients. Bacteremia caused by CPE remains rare, suggesting that infection prevention and control efforts are having some impact. However, as colonization prevalence increases, the number of clinical infections will rise in the future unless control measures to limit transmission and spread are improved.
Funding: None
Disclosures: None
113 Dasotraline for the Treatment of Moderate to Severe Binge Eating Disorder in Adults: Results From a Randomized, Double-Blind, Placebo-Controlled Study
- Bradford Navia, James I. Hudson, Susan L McElroy, Anna I. Guerdjikova, Ling Deng, Kaushik Sarma, Seth Hopkins, Kenneth Koblan, Antony Loebel, Robert Goldman
-
- Journal:
- CNS Spectrums / Volume 23 / Issue 1 / February 2018
- Published online by Cambridge University Press:
- 15 June 2018, pp. 72-73
-
- Article
-
- You have access Access
- Export citation
-
Objectives
Binge eating disorder (BED) is the most common eating disorder in the US, with a lifetime prevalence of 2.8%. Disturbances in reward circuitry have been implicated in its pathogenesis. Dasotraline is a novel and potent dopamine and norepinephrine reuptake inhibitor with slow absorption and a long half-life resulting in stable plasma concentrations over 24 hours with once-daily dosing. This study evaluated the efficacy and safety of flexibly-dosed dasotraline (4, 6, and 8 mg/day) vs placebo in adults with moderate to severe BED over a 12-week period (NCT02564588).
MethodsKey inclusion criteria included moderate to severe BED based on a history of ≥2 binge eating days/week for ≥6 months prior to screening, and ≥3 binge eating days for each of2 weeks prior to randomization, as documented in participant’s binge eating diary. Patients were randomized 1:1 to flexibly-dosed dasotraline (4, 6, 8 mg/day) or placebo. Theprimary endpoint was change from baseline (CFB) in the number of binge eating days per week at Week 12. Key secondary endpoints were: CFB in Clinical Global Impression–Severity (CGI-S) Scale at Week 12; CFB in Yale-Brown Obsessive Compulsive Scale Modified for Binge Eating (YBOCS-BE) at Week 12; and the percentage ofsubjects with a 4-week cessation from binge eating prior to Week 12 or end of treatment (EOT). Except for 4-week cessation, the other three variables were analyzed using amixed model for repeated measures (MMRM).
Results317 subjects (84% female) received ≥1 dose of study medication (mean age was 38.2 years; mean number of binge eating days per week, 4.25; mean CGI-S score, 4.5; mean BMI, 34.7). The MMRM analysis of CFB at Week 12 in the number of binge days/week yielded a significant mean difference of –0.99 (95% CI: –0.65 to –1.33; p<0.001) infavour of dasotraline (–3.74 in the dasotraline group vs –2.75 in the placebo group). All three key secondary endpoints were met at Week 12 or EOT: 46.5% of subjects in thedasotraline group achieved at least 4 consecutive weeks’ cessation from binge eating vs 20.6% in the placebo group (p<0.001); CFB in CGI-S and YBOCS-BE scores were also statistically significant in favour of dasotraline (p<0.001). The treatment-emergent adverse events (TEAEs) that occurred more frequently with dasotraline vs placebo at >2% incidence included: insomnia (44.6% vs 8.1%), dry mouth (27.4% vs 5.0%), decreased appetite (19.7% vs 6.9%), anxiety (17.8% vs 2.5%), nausea (12.7% vs 6.9%) and decreased body weight (12.1% vs 0%). Discontinuation due to AEs occurred in 11.5% of patients taking dasotraline vs 2.5% taking placebo.
ConclusionsIn adults with moderate to severe BED, there were highly significant and clinically meaningful reductions with dasotraline vs placebo in the frequency of binge eating, global severity of illness, and obsessive-compulsive symptoms related to binge eating. These results suggest dasotraline may offer a novel, well-tolerated and efficacious treatmentfor BED.
Funding AcknowledgementsStudy sponsored by Sunovion Pharmaceuticals Inc.
Understanding the Impact of Interventions to Prevent Antimicrobial Resistant Infections in the Long-Term Care Facility: A Review and Practical Guide to Mathematical Modeling
- Alicia Rosello, Carolyne Horner, Susan Hopkins, Andrew C. Hayward, Sarah R. Deeny
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 38 / Issue 2 / February 2017
- Published online by Cambridge University Press:
- 19 December 2016, pp. 216-225
- Print publication:
- February 2017
-
- Article
- Export citation
-
OBJECTIVES
(1) To systematically search for all dynamic mathematical models of infectious disease transmission in long-term care facilities (LTCFs); (2) to critically evaluate models of interventions against antimicrobial resistance (AMR) in this setting; and (3) to develop a checklist for hospital epidemiologists and policy makers by which to distinguish good quality models of AMR in LTCFs.
METHODSThe CINAHL, EMBASE, Global Health, MEDLINE, and Scopus databases were systematically searched for studies of dynamic mathematical models set in LTCFs. Models of interventions targeting methicillin-resistant Staphylococcus aureus in LTCFs were critically assessed. Using this analysis, we developed a checklist for good quality mathematical models of AMR in LTCFs.
RESULTS AND DISCUSSIONOverall, 18 papers described mathematical models that characterized the spread of infectious diseases in LTCFs, but no models of AMR in gram-negative bacteria in this setting were described. Future models of AMR in LTCFs require a more robust methodology (ie, formal model fitting to data and validation), greater transparency regarding model assumptions, setting-specific data, realistic and current setting-specific parameters, and inclusion of movement dynamics between LTCFs and hospitals.
CONCLUSIONSMathematical models of AMR in gram-negative bacteria in the LTCF setting, where these bacteria are increasingly becoming prevalent, are needed to help guide infection prevention and control. Improvements are required to develop outputs of sufficient quality to help guide interventions and policy in the future. We suggest a checklist of criteria to be used as a practical guide to determine whether a model is robust enough to test policy.
Infect Control Hosp Epidemiol 2017;38:216–225
Chapter 20 - Microbiology
- from 9 - Microbiology
- Edited by Alison Fiander, Cardiff University, Baskaran Thilaganathan
-
- Book:
- MRCOG Part One
- Published online:
- 27 January 2017
- Print publication:
- 13 October 2016, pp 317-342
-
- Chapter
- Export citation
Gene × Environment effects of serotonin transporter, dopamine receptor D4, and monoamine oxidase A genes with contextual and parenting risk factors on symptoms of oppositional defiant disorder, anxiety, and depression in a community sample of 4-year-old children
- John V. Lavigne, Laura B. K. Herzing, Edwin H. Cook, Susan A. Lebailly, Karen R. Gouze, Joyce Hopkins, Fred B. Bryant
-
- Journal:
- Development and Psychopathology / Volume 25 / Issue 2 / May 2013
- Published online by Cambridge University Press:
- 30 April 2013, pp. 555-575
-
- Article
- Export citation
-
Genetic factors can play a key role in the multiple level of analyses approach to understanding the development of child psychopathology. The present study examined gene–environment correlations and Gene × Environment interactions for polymorphisms of three target genes, the serotonin transporter gene, the D4 dopamine receptor gene, and the monoamine oxidase A gene in relation to symptoms of anxiety, depression, and oppositional behavior. Saliva samples were collected from 175 non-Hispanic White, 4-year-old children. Psychosocial risk factors included socioeconomic status, life stress, caretaker depression, parental support, hostility, and scaffolding skills. In comparison with the short forms (s/s, s/l) of the serotonin transporter linked polymorphic repeat, the long form (l/l) was associated with greater increases in symptoms of oppositional defiant disorder in interaction with family stress and with greater increases in symptoms of child depression and anxiety in interaction with caretaker depression, family conflict, and socioeconomic status. In boys, low-activity monoamine oxidase A gene was associated with increases in child anxiety and depression in interaction with caretaker depression, hostility, family conflict, and family stress. The results highlight the important of gene–environment interplay in the development of symptoms of child psychopathology in young children.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
8 - Vertebrate life at high altitude
- Edited by Göran E. Nilsson, Universitetet i Oslo
-
- Book:
- Respiratory Physiology of Vertebrates
- Published online:
- 05 June 2012
- Print publication:
- 28 January 2010, pp 265-299
-
- Chapter
- Export citation
-
Summary
Introduction
The physiological stresses and limited resources at high altitude pose limits on vertebrate life in this environment. Primary stresses include low oxygen pressure, temperatures, and humidity, and increased radiation. High-altitude ecosystems are characterized by less diversity, rugged topography, and marginal availability of certain nutrients. However, given the amazing physiological abilities to cope with low oxygen described in this book, it is not surprising that there are numerous examples of life at high altitude. Representatives from every class of vertebrates are found living at altitudes of 4000 m above sea level, where the PO2 is less than 100 Torr, including fish (trout) in Andean lakes and rivers (Bouverot et al., 1985). (A pressure of 1 Torr = 1/760 atmosphere = 1 mmHg). The primary focus of this chapter on species that are native to high altitudes is to emphasize adaptations to life with limited oxygen instead of reviewing physiological acclimatization to high altitude. Adaptations to hypoxia in fishes are covered in Chapter 5, so here we focus on air-breathing vertebrates.
The high-altitude environment
Paul Bert first demonstrated that the primary physiological challenge at high altitude is reduced oxygen partial pressure (PO2) as a result of reduced barometric pressure (Bouverot et al.,1985). Various algorithms have been devised to estimate the fall in barometric pressure with altitude, such as the International Civil Aviation Organization (1964) or National Oceanic and Atmospheric Administration (1976) standard atmospheres.
Healthcare-Associated Staphylococcus aureus Bacteremia and the Risk for Methicillin Resistance: Is the Centers for Disease Control and Prevention Definition for Community-Acquired Bacteremia Still Appropriate?
- Olivier Lesens, Yves Hansmann, Eimar Brannigan, Susan Hopkins, Pierre Meyer, Brian O'Connel, Gilles Prévost, Colm Bergin, Daniel Christmann
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 26 / Issue 2 / February 2005
- Published online by Cambridge University Press:
- 21 June 2016, pp. 204-209
- Print publication:
- February 2005
-
- Article
- Export citation
-
Objective:
To evaluate a new classification for bloodstream infections that differentiates hospital acquired, healthcare associated, and community acquired in patients with blood cultures positive for Staphylococcus aureus.
Design:Prospective, observational study.
Setting:Three tertiary-care, university-affiliated hospitals in Dublin, Ireland, and Strasbourg, France.
Patients:Two hundred thirty consecutive patients older than 18 years with blood cultures positive for S. aureus.
Methods:S. aureus bacteremia (SAB) was defined as hospital acquired if the first positive blood culture was performed more than 48 hours after admission. Other SABs were classified as healthcare associated or community acquired according to the definition proposed by Friedman et al. When available, strains of methicillin-resistant Staphylococcus aureus (MRSA) were analyzed by pulsed-field gel electrophoresis (PFGE).
Results:Eighty-two patients were considered as having community-acquired bacteremia according to the Centers for Disease Control and Prevention (CDC) classification. Of these 82 patients, 56% (46) had healthcare-associated SAB. MRSA prevalence was similar in patients with hospital-acquired and healthcare-associated SAB (41% vs 33%; P > .05), but significantly lower in the group with community-acquired SAB (11%; P < .03). PFGE of MRSA strains showed that most community-acquired and healthcare-associated MRSA strains were similar to hospital-acquired MRSA strains. On multivariate analysis, Friedman's classification was more effective than the CDC classification for predicting MRSA.
Conclusion:These results support the call for a new classification for community-acquired bacteremia that would account for healthcare received outside the hospital by patients with SAB.
Simplified Surveillance for Nosocomial Bloodstream Infections
- Deborah S. Yokoe, Jane Anderson, Robert Chambers, Maureen Connor, Robert Finberg, Cyrus Hopkins, Deborah Lichtenberg, Susan Marino, Dorothy McLaughlin, Edward O'Rourke, Matthew Samore, Kenneth Sands, Judith Strymish, Elise Tamplin, Nancy Vallonde, Richard Platt
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 19 / Issue 9 / September 1998
- Published online by Cambridge University Press:
- 02 January 2015, pp. 657-660
- Print publication:
- September 1998
-
- Article
- Export citation
-
Objective:
To compare a surveillance definition of nosocomial bloodstream infections requiring only microbiology data to the Centers for Disease Control and Prevention's (CDC) current definition.
Setting:Six teaching hospitals.
Methods:We classified a representative sample of 73 positive blood cultures from six hospitals growing common skin contaminant isolates using a definition for bacteremia requiring only microbiology data and the CDC definition for primary bloodstream infection (National Nosocomial Infections Surveillance [NNIS] System review method). The classifications assigned during routine prospective surveillance also were noted, and the time required to classify isolates by the two methods was compared.
Results:Among 65 blood cultures growing common skin contaminant isolates obtained from adults, the agreement rate between the microbiology data method and the NNIS review method was 91%. Agreement was significantly poorer for the eight blood cultures growing common skin contaminant isolates obtained from pediatric patients. The microbiology data method requires approximately 20 minutes less time per isolate than does routine surveillance.
Conclusions:A definition based on microbiology data alone yields the same result as the CDC's definition in the large majority of instances. It is more resource-efficient than the CDC's current definition





