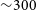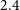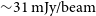100 results
Abbreviations
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp xii-xiv
-
- Chapter
- Export citation
Index
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 247-250
-
- Chapter
- Export citation
Part II - Genres
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 59-108
-
- Chapter
- Export citation
Part I - Contexts
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 9-58
-
- Chapter
- Export citation
Contents
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp v-vi
-
- Chapter
- Export citation
Further Reading
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 237-246
-
- Chapter
- Export citation
Copyright page
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp iv-iv
-
- Chapter
- Export citation
Part III - Reading Gulliver’s Travels
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 109-176
-
- Chapter
- Export citation
Figures
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp vii-viii
-
- Chapter
- Export citation
Notes on Contributors
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp ix-xi
-
- Chapter
- Export citation
Introduction
-
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 1-8
-
- Chapter
- Export citation
Part IV - Afterlives
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp 177-236
-
- Chapter
- Export citation
Chronology
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp xvi-xx
-
- Chapter
- Export citation
Note on the Text
-
- Book:
- The Cambridge Companion to <i>Gulliver's Travels</i>
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023, pp xv-xv
-
- Chapter
- Export citation

The Cambridge Companion to Gulliver's Travels
-
- Published online:
- 05 October 2023
- Print publication:
- 19 October 2023
Use of Cognitive Aids to Augment Point of Care Hemorrhage Control Skills in Laypersons
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 17 / 2023
- Published online by Cambridge University Press:
- 12 July 2023, e428
-
- Article
- Export citation
A calibration and imaging strategy at 300 MHz with the Murchison Widefield Array (MWA)
- Part of
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 38 / 2021
- Published online by Cambridge University Press:
- 10 December 2021, e063
-
- Article
-
- You have access
- HTML
- Export citation
Copyright page
-
- Book:
- The Cambridge Companion to Music in Digital Culture
- Published online:
- 30 August 2019
- Print publication:
- 19 September 2019, pp vi-vi
-
- Chapter
- Export citation
Acknowledgements
-
- Book:
- The Cambridge Companion to Music in Digital Culture
- Published online:
- 30 August 2019
- Print publication:
- 19 September 2019, pp xiv-xiv
-
- Chapter
- Export citation
Introduction
-
-
- Book:
- The Cambridge Companion to Music in Digital Culture
- Published online:
- 30 August 2019
- Print publication:
- 19 September 2019, pp 1-4
-
- Chapter
- Export citation