Poster Presentation
Environmental Cleaning
Using Ultraviolet C (UVC) in Operating Rooms: A Hygiene Improvement
- Roberta Bosco, Gabriele Messina, Davide Amodeo, Gabriele Cevenini, Simona Gambelli
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s63
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Disinfection procedures are an essential aspect of preventing cross contamination, especially in situations where the risk of infection is higher, such as in operating rooms (ORs). Disinfection procedures in ORs at the end of each surgery session are not the same as final cleaning procedures. We assessed the difference in microbial contamination between different levels of disinfection, before T(0) and after T(1) the use of an ultraviolet C device (UVC-D). Methods: A cross-sectional study was conducted between December 2019 and August 2020 in a private clinic. Three sanitation levels (SL1–SL3) were compared for the reduction in colony-forming units (CFU) between T(0) and T(1): (1) no disinfection after surgery (SL1);, (2) after in-between cleaning (SL2), and (3) after terminal cleaning (SL3). UVC-D was used for 6 minutes, 3 minutes per bed side. Overall, 260 Petri dishes were used in 3 ORs, incubated at 36°C, and CFU were counted after 48 hours. Descriptive statistics, Wilcoxon test, and MANOVA for repeated measures were performed to verify the 95% statistical difference between T(0) and T(1), both on the whole sample and combined with the different SLs. Results: The unstratified analysis showed statistically significant differences (Wilcoxon test, p < 0.05) between T(0) and T(1), with means and standard deviations of 11.42 ± SD 41.19 CFU/PD and 5.91 ± SD 30.89, respectively. The Manova test for repeated measures, applied to 54 pairs of measurements, showed no significant difference between SLs in T(0)-T(1) CFU reduction. Overall, the mean percent reduction in CFU was 93.48% (CI95% = 86.97-99.99%). Conclusions: The results showed significant improvements in disinfection under any condition tested with UVC-D. Using the device immediately after surgery (SL1), before standard cleaning procedures, reduced CFUs by 97.3%. In some situations, UVC light was sufficient to reduce CFU to zero, even without chemical and mechanical cleaning. However, we do not recommend this approach; UVC light disinfection should be applied only after sanitization procedures because it does not remove dirt.
Funding: UltraViolet Device, Inc
Disclosures: None
Hand Hygiene
Building on the Foundation of a Sustainable Hand Hygiene Program During the COVID-19 Pandemic
- Lisa Stancill, Emily Sickbert-Bennett Vavalle, Lauren DiBiase
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s63-s64
-
- Article
-
- You have access Access
- Open access
- Export citation
-
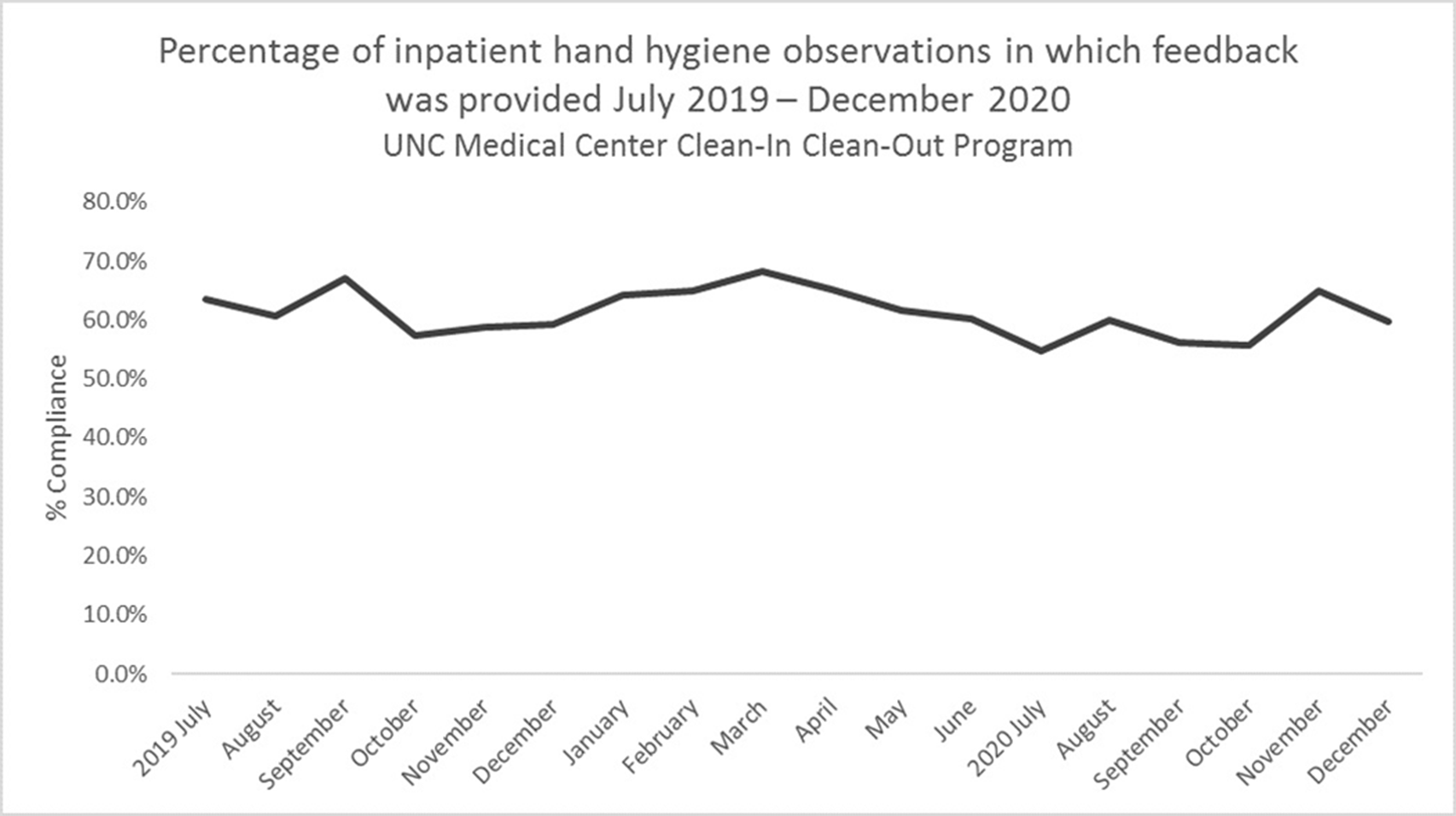
Background: Hand hygiene is essential to preventing the spread of disease in hospitals. Renewed emphasis has been placed on hand hygiene during the COVID-19 pandemic. We investigated whether UNC Medical Center’s well-established Clean-In Clean-Out (CICO) program for hand hygiene observations was sustainable throughout a public health and healthcare crisis and whether the COVID-19 pandemic had an effect on hand hygiene compliance. Methods: UNC Medical Center utilizes a crowd-sourced hand-hygiene audit application, CICO, to track hand-hygiene observations, compliance, and feedback. This application encourages participation from all staff and promotes providing real-time feedback in the form of a compliment or reminder when performing hand hygiene observations. During this evaluation, hand hygiene data were queried from the CICO application on the number of observations performed, hand hygiene compliance percentage, and feedback compliance percentage from July 2019 to December 2020. Hand hygiene data were compared to patient volumes in different care settings and the number of hospitalized patients being treated for COVID-19. Results: Initial increases in hand hygiene observations, compliance, and feedback were detected in the months leading up to UNC Medical Center receiving its first SARS-CoV-2–positive patient. Observations were highest when patient volumes were low due to closed clinics and restrictions on elective surgeries (Figure 1). When patient volumes returned to pre–COVID-19 levels coupled with treating more COVID-19 patients, the number of observations and compliance rate metrics declined. Feedback compliance percentage remained relatively stable through the entire period (Figure 2). Conclusions: Despite the additional strain on healthcare staff during COVID-19, the CICO model was a sustainable method to track hand hygiene observations and compliance. Notably, however, engagement was highest when patient census was lower, demonstrating that operating at a high capacity is not beneficial for patient safety. Due to the success and sustainment of the CICO program, UNC Medical Center used this model to create a Mask-On Mask-Up campaign to engage staff to submit observations, track compliance, and encourage feedback to promote the appropriate use of masks during COVID-19.
Funding: No
Disclosures: None
Figure 1.
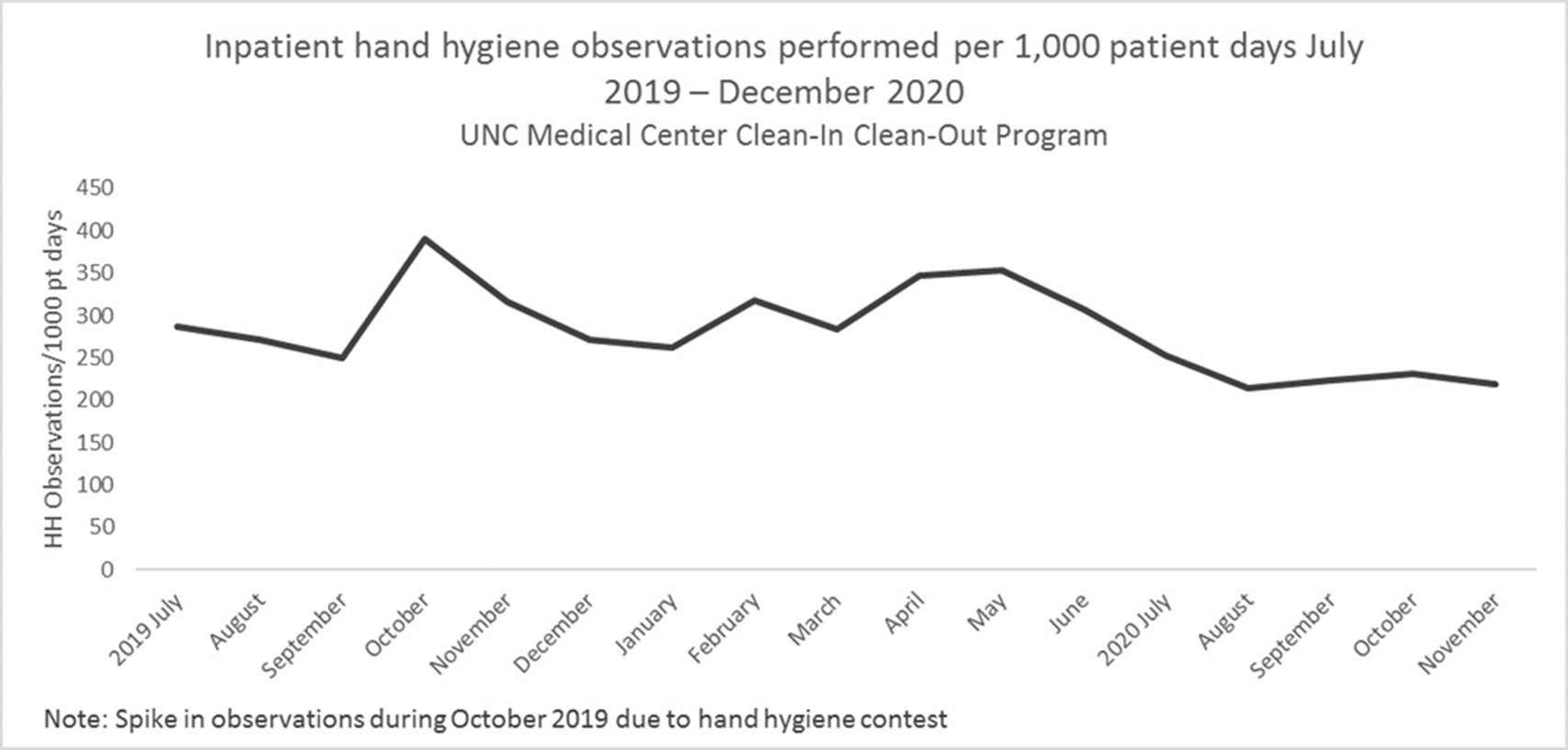
Figure 2.
Appropriate Number of Observations to Determine Hand Hygiene Compliance Among Healthcare Workers
- Se Yoon Park, Eunjung Lee, Suyeon Park, Tae Hyong Kim, Sungho Won
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s64
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: We sought to determine the minimum number of observations needed to determine hand hygiene (HH) compliance among healthcare workers. Methods: The study was conducted at a referral hospital. We retrospectively analyzed the result of HH monitoring from January to December 2018. HH compliance was calculated by dividing the number of observed HH actions by the total number of opportunities. Appropriate HH compliance rates were calculated based on the 6-step technique, modified from the World Health Organization (WHO) recommendation. The minimum number of required observations (n) was calculated by the following equation using overall mean value (r), absolute precision (d), and confidence interval (1-α) [The equation: n3 Zα/22×ρ×1-ρ/d2]. We considered ds of 5%, 10%, 20%, and 30%, with CIs of 99%, 95%, and 90%, respectively. Among the various cases, we focused on 10% for d and 95% for CI. Results: During the study period, 8,791 opportunities among 1,168 healthcare workers were monitored. The mean HH compliance and appropriate HH compliance rates were 80.3% and 59.7%, respectively (Table 1). The minimum number of observations required to determine HH compliance rates ranged from 2 (d, 30%; CI, 90%) to 624 (d, 5%; CI, 99%), and the minimum number of observations for optimal HH compliance ranged from 5 (d, 30%, CI, 90%) to 642 (d, 5%; CI, 99%) (Figure 1). At 10% absolute precision with 95% confidence, the minimum number of observations to determine HH and optimal HH compliance were 61 and 92, respectively. Conclusions: The minimum number of observations to determine HH compliance varies widely according to setting, but at least 5 were needed to determine optimal HH compliance.
Funding: No
Disclosures: None
Figure 1.
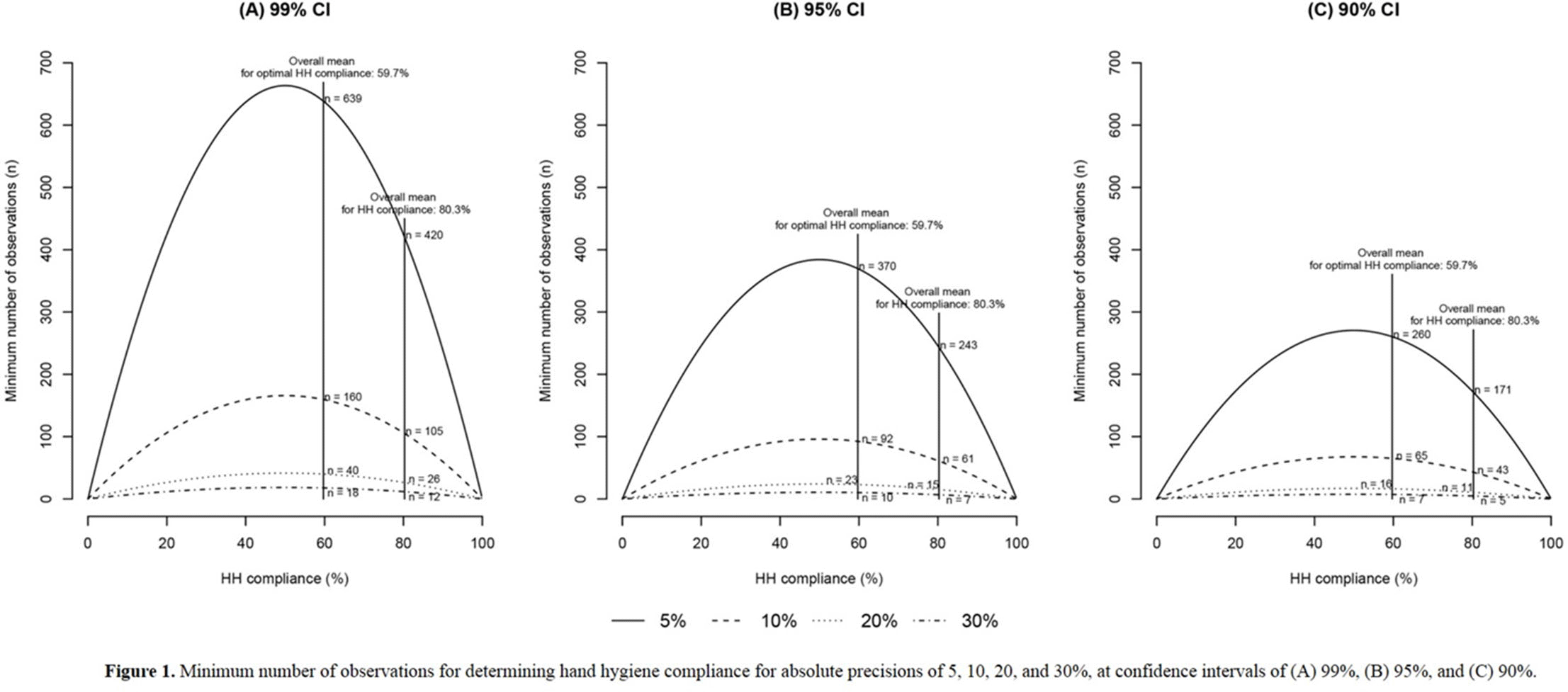
Table 1. 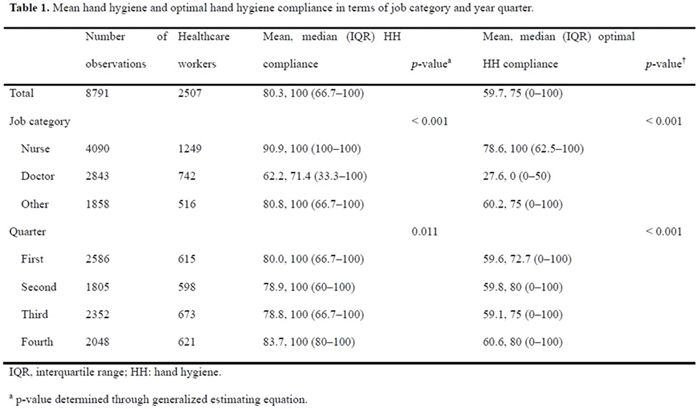
Implementation Science
Results of a Stepped-Wedge Cluster-Randomized Implementation Science Trial to Improve Chlorhexidine Gluconate Bathing Compliance
- Staci Reynolds, Edward Keating
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s65
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Daily chlorhexidine gluconate (CHG) bathing in intensive care units (ICUs) is widely supported in the literature to decrease risk of central-line-associated infections (CLABSIs). However, adoption of this practice is inconsistent. The primary objective of this implementation science study was to assess the effect of a bathing intervention on compliance with the AHRQ CHG bathing protocol. Secondary objectives were to examine (1) moderating effects of unit characteristics, (2) the intervention effect on nursing staff’s knowledge and perceptions of CHG bathing, and (3) the intervention effect on CLABSI rates. Methods: A stepped-wedge cluster-randomized design was used to implement and evaluate the effectiveness of a CHG bathing intervention. At 2 large hospitals, 14 units were clustered into 4 sequences. Units included 9 adult ICUs, 3 pediatric ICUs, 1 pediatric bone marrow transplant unit, and 1 adult hematology-oncology unit. Sequences were enrolled into the active intervention phase over the course of 4 months. The intervention included 2 evidence-based implementation strategies: (1) educational outreach visits and (2) audit and feedback on CHG bathing compliance. Compliance with the CHG bathing processes and daily CHG bathing documentation were assessed. At 12 months after the last enrolled date, booster sessions were completed, and outcomes were assessed for sustainability. Results: In models of CHG bathing process compliance, the implementation strategy was significant (b = 6.97; P = .009), indicating that compliance was 6.97% higher after the intervention than before. There was a statistically significant improvement in nursing knowledge of CHG bathing (χ2 = 9.32, p = .002) and perception of the priority of CHG bathing (t = 2.56; P = .01). Daily CHG bathing documentation compliance and CLABSI rates did not significantly improve immediately following the intervention; however, a clinically significant decrease (27.4%) in CLABSI rate was observed. At 12 months after the intervention, improvements in CHG bathing documentation and process outcomes were sustained. There was no change in bathing process compliance after 12 months (b = −0.19; P = .87; intercept=96.96, p < .001), and compliance remained high at 96.96%. There was no change in documentation compliance after 12 months (b=3.89, p=.37, intercept=78.72, p < .001), and compliance remained high at 78.72%. After 12 months, CLABSI rates were statistically significantly reduced (b = −0.16; P = .009; intercept =1.97, p < .001). Conclusions: Using educational outreach visits and audit-and-feedback strategies can improve the adoption of evidence-based CHG bathing practices. CHG bathing—a simple, nurse-driven practice—can make a significant improvement in patient outcomes.
Funding: No
Disclosures: None
Antibiotic Stewardship Implementation at Hospitals Without On-Site Infectious Disease Specialists: A Mixed-Methods Study
- Daniel Livorsi, Eli Perencevich, Kenda Stewart Steffensmeier, Matthew Goetz, Heather Reisinger
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s65
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Hospitals are required to have antibiotic stewardship programs (ASPs), but there are few models for implementing ASPs without the support of an infectious disease (ID) specialist, defined as an ID physician and/or ID pharmacist. In this study, we sought to understand ASP implementation at hospitals within the Veterans’ Health Administration (VHA) that lack on-site ID support. Methods: Using a mandatory 2016 VHA survey, we identified acute-care hospitals that lacked an on-site ID specialist. For each hospital, antibiotic use (2018–2019) was quantified as days of therapy (DOT) per 1,000 days present, based on NHSN methodology for tracking all antibacterial agents. From July 2019 through April 2020, we conducted semistructured interviews with personnel involved in or affected by ASP activities at 7 qualifying hospitals. All interview transcripts were analyzed using thematic content analysis. Results: Of the 7 acute-care hospitals, 6 (86%) had a long-term care unit; 3 (43%) had an intensive care unit; and 2 (29%) had full-time employment equivalents dedicated to stewardship. Sites averaged 1,075 (SD, ±654) and 148 (SD, ±96) admissions per year in acute-care and long-term care, respectively. At the site-level, mean antibiotic use was 486 DOT (SD, ±98) per 1,000 days-present in acute-care and 207 DOT (SD, ±74) per 1,000 days present in long-term care. We interviewed 42 personnel across the 7 sites. Although sites reported using similar interventions to promote antibiotic stewardship, the shape of these interventions varied. The following 4 common themes were identified: (1) The primary responsibility for ASPs fell on the pharmacist champions, who were typically assigned multiple other non-ASP responsibilities. (2) The pharmacist champions were more successful at gaining buy-in for stewardship initiatives when they had established rapport with clinicians, but at some sites, the use of contract physicians and frequent staff turnover were potential barriers. (3) Some sites felt that having access to an off-site ID specialist was important for overcoming institutional barriers to stewardship and improving the acceptance of their stewardship interventions. (4) In general, stewardship champions struggled to mobilize institutional resources, which made it difficult to advance their programmatic goals. Conclusions: In this study of 7 hospitals without local ID support, we found that ASPs are largely a pharmacy-driven process. Remote ID support, if available, was seen as helpful for implementing stewardship interventions. These findings may inform the future implementation of ASPs in settings lacking local ID expertise.
Funding: No
Disclosures: None
Other
Gamifying the Infection Control Curriculum: The Impact on Nursing Students’ Knowledge, Exam Performance, and Course Perception
- Tomislav Mestrovic, Jasminka Talapko, Tina Cikac, Marijana Neuberg
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s65-s66
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Unlike passive didactic teaching, the introduction of innovative active-learning approaches to university nursing curricula aims to address the educational content in an interactive learning environment, improving in turn the learning process and problem-solving skills indispensable for future infection control professionals. One such strategy is the use of educational games, which can motivate students and enhance the degree of their engagement. We appraised the effectiveness of introducing an interactive game based on a popular television quiz show “Who Wants to be a Millionaire?” for educational attainment, exam performance, and course perception in nursing students. Methods: A whole generation of second-year undergraduate nursing students (126 female and 27 male participants; age range, 19–41 years) from a public university in Croatia (University Centre Varazdin, University North) were divided into 2 groups by cluster randomization; one group had received additional hours of game play after core training curriculum in a “Hygiene and Epidemiology” course, while the other had not. Game play was accomplished by employing ‘edutaining’ interactive multimedia approach, and covered primarily hand hygiene, cough etiquette, the use of personal protective equipment, sterilization and disinfection, and safe injection practices. Quantitative results of multiple-choice exams were used to evaluate any differences in the knowledge level of respective groups. A satisfaction opinion survey was used to gauge attitudes of students attending the course. Statistical significance was defined as P < .05 (2-tailed). Results: The mean baseline examination score was 28.30±5.79 points for the game group and 24.65±5.94 points for the control group, demonstrating improved knowledge retention when the interactive game was introduced into the curriculum. The statistically significant improvement in knowledge was observed in the domains of personal protective equipment and safe injection practices. There was no statistically significant difference in the overall scores between male and female students. Students who were subjected to game play expressed more agreement on a Likert scale regarding course enjoyment and innovativeness, albeit they did not differ from control group when assessing the educational merit of the course. Conclusions: Introducing interactive games to university courses that cover infection control may boost student enjoyment and enhance long-term retention of information, as confirmed by this study. Nonetheless, extra care should be taken when specific games that have not been assessed objectively are implemented. Further research in this field will elucidate how this increased knowledge retention in infection control principles translates to quotidian practice, for the benefit of students and (ultimately) patients.
Funding: No
Disclosures: None
Infection Control in Low- and Middle-Income Countries
Assessment of COVID-19 Infection Prevention and Control Capabilities in 39 Haitian Hospitals
- Afeke Kambui, Mentor Lucien, Catherine Emilien, Francois Staco, Ymeline Pateau St Vil, Pierre Philippe Wilson Registe, Mackenley Brice, Dassaëve Brice, Nathan Zephirin, Sandra Benjamin, Martha Murdock
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s66
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infection prevention and control (IPC) is key (1) to keeping health workers and patients safe from contracting infections during care, (2) to enabling continuity of essential health services, and (3) to pandemic preparedness and response. Frontline health workers are at 3-fold increased risk for COVID-19 (Lancet 2020) and account for 6% of COVID-19 hospitalizations (CDC 2020). With the support of the US Agency for International Development Bureau of Humanitarian Assistance (USAID/BHA) and collaboration of the Haitian Ministry of Health (MSPP), MSH’s Rapid Support to COVID-19 Response in Haiti project (RSCR Haiti) developed an instrument to assess select public hospitals and identify IPC gaps that informed COVID-19 response and system strengthening measures for increasing patient and provider safety. Methods: The IPC tool contains 13 IPC domains and 80 questions, for a total of 600 points. It was developed based on the World Health Organization IPC Assessment Framework for Health Facilities (2018) and US Centers for Disease Control Facility Readiness Assessment for COVID-19 (2020). In total, 39 health facilities chosen by the MSPP across all 10 departments of Haiti were evaluated in October 2020. Data were analyzed in Microsoft Excel by category, site, and IPC capabilities then classified as inadequate, basic, intermediate or advanced. Results: IPC capabilities scored as inadequate in 18% and basic in 67% of hospitals (Graph 1). No institution was advanced. Among health facilities, IPC programs existed in only 18%; IPC guidelines or procedures were present in 38%; staff were trained regularly in 12%; and healthcare-associated infection surveillance was performed in 19%. Systems for COVID-19 triage existed in 56%; 39% had IPC commodity management systems; 45% provided COVID-19 training; 26% practiced monitoring of staff and patients for COVID-19; 36% had protocols for an influx of COVID-19 cases; and 72% practiced risk communication (Table 1). Conclusions: No health facility was sufficiently equipped to implement adequate COVID-19 IPC measures, and all needed strengthening, even in the highest-scoring IPC areas. Through RSCR Haiti, MSH and MSPP were able to identify and address priorities in hospitals: establishing hospital IPC programs; training staff; monitoring health workers and patients; and implementing guidance, triage, and commodity-management systems. This study demonstrates that it is possible to do a quick yet thorough assessment to rapidly identify IPC needs and opportunities, using the results to rapidly build response capacity. Haiti’s experience of integrating locally contextualized global IPC tools to inform systemic COVID-19 response measures can benefit other experts globally.
Funding: United States Agency for International Development Bureau of Humanitarian Assistance (USAID/BHA)
Disclosures: None
Figure 1.
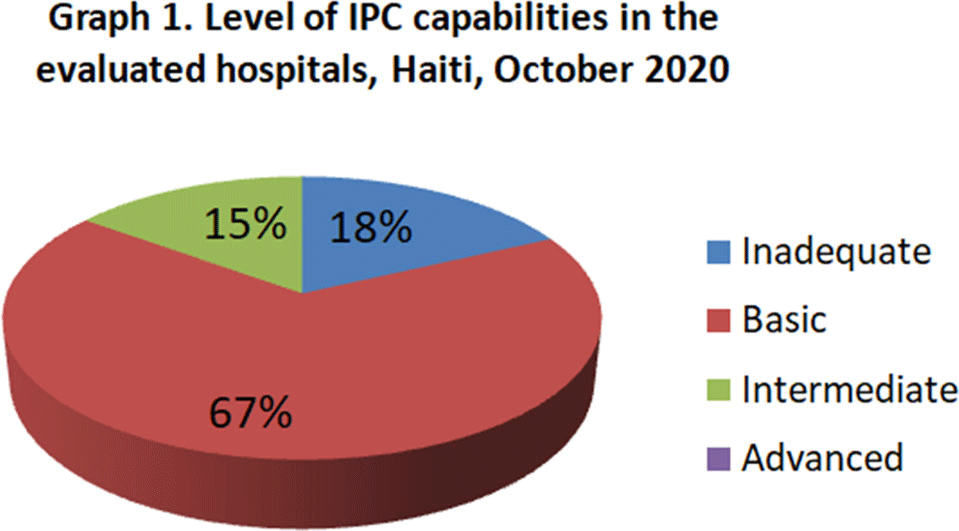
Table 1. 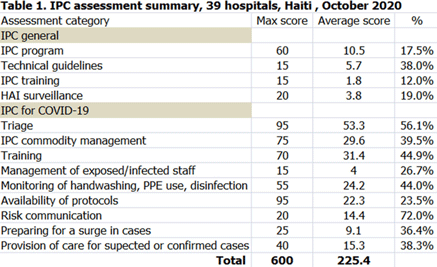
An Observational Study on CRE Colonization and Subsequent Risk of Infection in Adult ICU Patients
- Kirtika Sharma, Vibhor Tak, Vijaya Lakshmi Nag
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s66-s67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Carbapenem-resistant Enterobactericeae (CRE) has emerged as a global health threat with increasing incidence. It is a particular problem in India because control over antibiotics prescription is really poor; these agents can be easily bought over the counter and the antibiotic prescription threshold is low among Indian doctors. Also, even when administered, antibiotics are given in inappropriate dosages and durations. CRE infections are a healthcare challenge due to their difficulty to treat and high morbidity and mortality. Colonization requires infection prevention measures, and it should be prioritized. Methods: We sought to determine the prevalence rate of CRE colonization in the gastrointestinal tract in newly admitted ICU patients along with follow-up of any subsequent infection following colonization. A prospective observational study was carried out among ICU patients from January 2019 to August 2020 by collecting perirectal swabs from patients who gave consent. Clinical variables were identified, and the relationship between CRE colonization and subsequent systemic CRE infection was assessed. Processing was carried out by culturing on MacConkey agar plate with ertapenem disk and further identified using conventional microbiological techniques. The ertapenem MIC was determined using an Epsillometer (E) test. The modified carbapenem inactivation (mCIM) test and the EDTA carbapenem inactivation method (eCIM) were used to confirm carbapenem resistance using Clinical Laboratory Standards Institute 2020 guidelines (Figure 1). Results: Among 192 ICU patients, 37 (19.27%) were colonized with CRE (Table 1). Also, 13 (35.13%) CRE isolates showed metallo-β-lactamase resistance. Furthermore, 18 CRE isolates (48.64%) showed serine carbapenemase activity; 6 CRE isolates showed no carbapenemase activity. Klebsiella pneumoniae (n = 25 of 37, 67.56%) was the most common CRE isolated followed by Escherichia coli (n = 11 of 37, 29.72%) and 1 isolate of Enterobacter spp (n = 1 of 37, 0.02%). Of 37 patients, 33 (89.18%) developed CRE infection during their hospital stay. Pneumonia was the most common infection developed (36.36%), followed by surgical site infection (21.21%) and urinary tract infection (12.12%). Only 1 patient developed a bloodstream infection. However, 9 patients (27.27%) developed multiple-site infections. Of 37 CRE-colonized patients, 10 (27.02%) died during their hospital stay. Conclusions: Our study highlights the increased risk of CRE infection and mortality in patients with CRE colonization in ICU patients. Hence, CRE perirectal screening for detection of asymptomatic carriers should be conducted, and strict infection control measures, such as isolation and cohorting with barrier nursing of such patients, should be done to prevent further spread of CREs in hospital settings.
Funding: No
Disclosures: None
Figure 1.
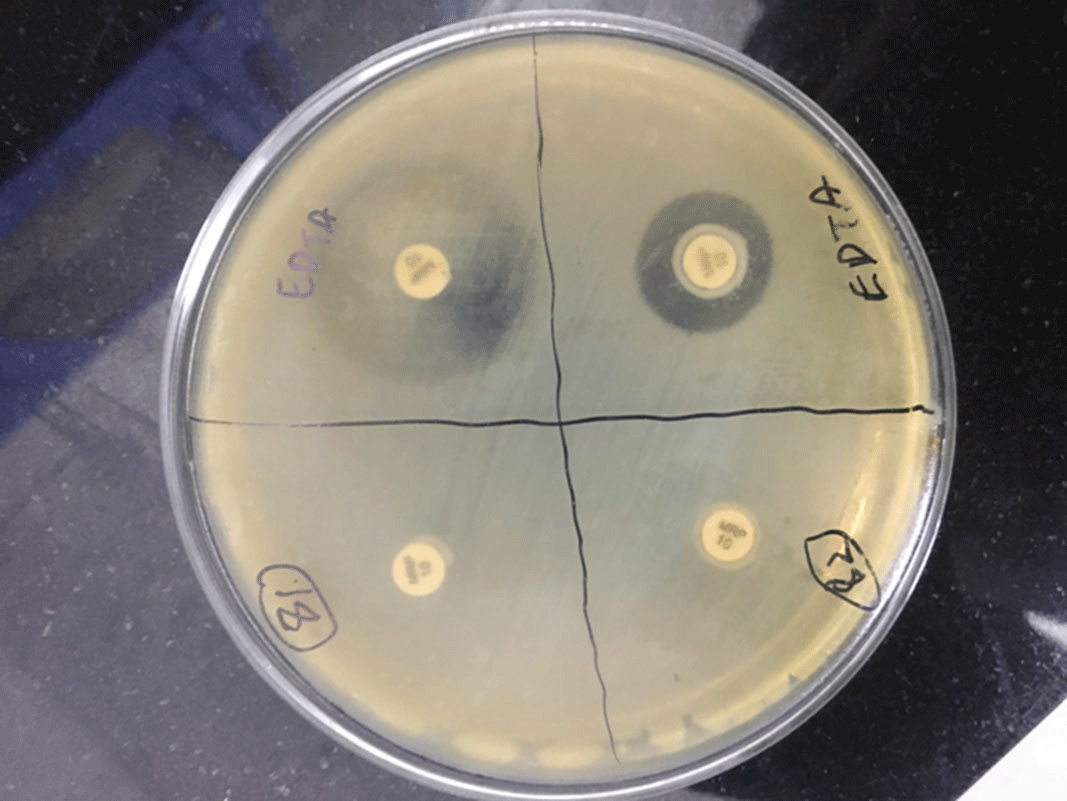
Table 1. 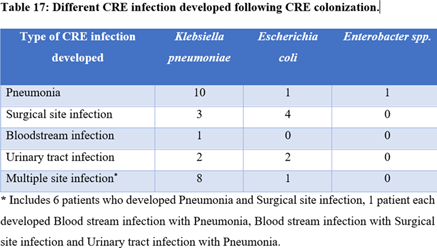
Table 2. 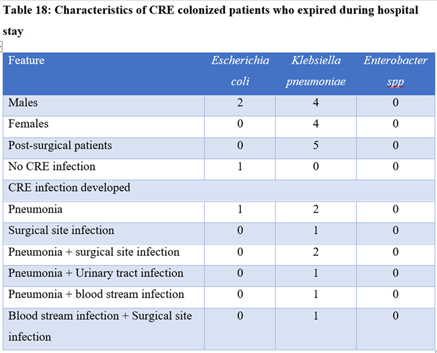
Infection Prevention
Medical Tape Contamination Study: Effect of Packaging on the Reduction of Cross Contamination
- Kheng Vang, Graham Smith, Sara J Pastoor
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s67-s68
-
- Article
-
- You have access Access
- Open access
- Export citation
-
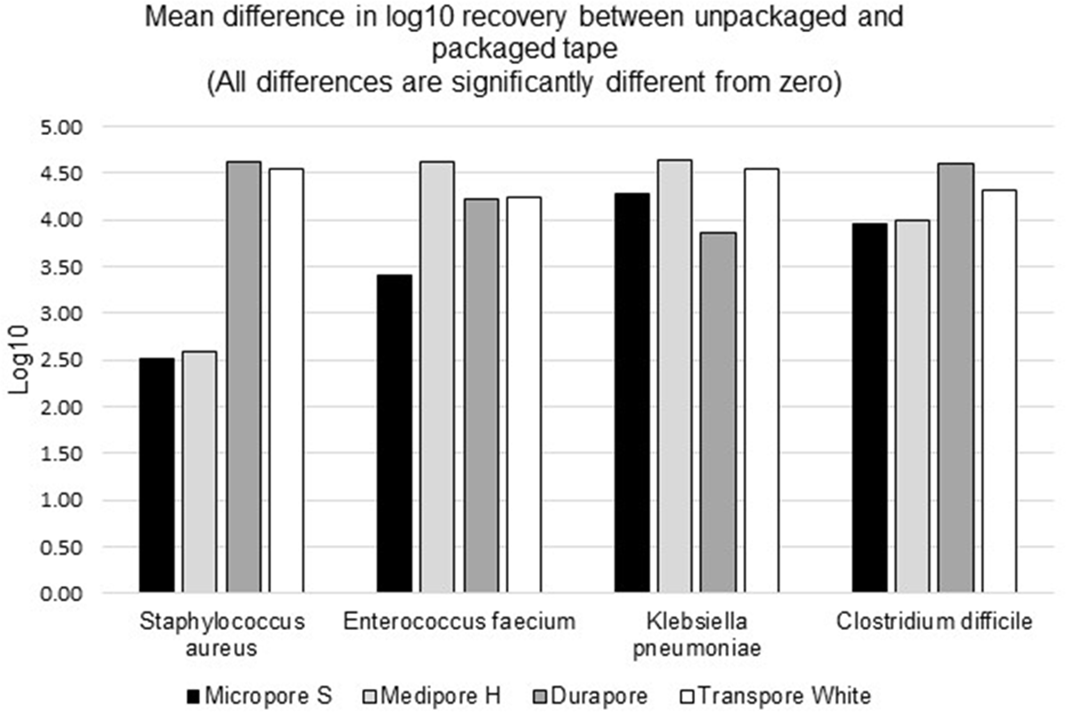
Background: Medical tape is used routinely for a variety of tasks across healthcare settings. The literature contains numerous publications in which common practices around medical tapes have been suspected to lead to infection transmission. Healthcare providers can turn to individually packaged single-patient-use medical tape rolls to help reduce cross-contamination risk by limiting exposure to environmental contaminants, minimizing contact with hospital surfaces and equipment, and minimizing exposure to healthcare workers’ hands and other patients. Methods: We evaluated the effect of individually packaged tape on cross contamination using a controlled laboratory assay. Ceramic tiles were inoculated with microorganisms evenly spread across the surface and allowed to air dry. Using gloves, packaged and unpackaged tapes were rolled over their entire outside circumference onto the contaminated tiles to simulate cross contamination. Using new gloves, the packaged tapes were then removed from their package with minimum contact. All cross-contaminated tape rolls were placed in phosphate-buffered water and mixed in a vortexer for bacterial recovery procedures. Serial dilutions were plated on appropriate media for bacterial enumeration. The average log10 colony-forming unit (CFU) recovery was measured for comparison. We used 4 types of tapes in this study (3M Micropore S Surgical Tape, 3M Medipore H Soft Cloth Surgical Tape, 3M Durapore Surgical Tape, and 3M Transpore White Surgical Tape). We used 4 different microorganisms as inoculates: Staphylococcus aureus (methicillin-resistant), Enterococcus faecium (vancomycin-resistant), Klebsiella pneumoniae (carbapenem-resistant), and Clostridium difficile (spore). Each test (tape and bacteria combination) was done in 3 or 6 replicates; each bacterial enumeration was the average of duplicate plates. The detection limit for this method is 8 CFU per sample, which is equivalent to 0.9 log10. Results: The results for all tapes tested showed a statistically significant lower mean log10 recovery of each of the microorganisms tested for packaged versus unpackaged tape (Figure 1). The mean differences of log10 recoveries from a packaged and unpackaged tape ranged from 2.51 log10 (for S. aureus on Micropore S) to 4.64 log10 (for K. pneumoniae on Medipore H). This is equivalent to 99%–99.99% cross-contamination protection from the 4 organisms tested. Conclusions: Individual packaging of medical tape rolls protects them from external contaminants. Even if the packaging becomes contaminated, the tape retrieved from the package will be significantly less contaminated than it would have been from exposure to the same contaminants without packaging.
Funding: 3M Company
Disclosures: None
Figure 1.
Long-Term Care
Nursing-Home Patient Functional and Microbiota Status Drive Environmental Contamination with Vancomycin-Resistant Enterococci
- Joyce Wang, Betsy Foxman, A. Krishna Rao, Lona Mody, Evan Snitkin
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s68
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Patient colonization and shedding of vancomycin-resistant enterococci (VRE) is a major source of environmental contamination leading to VRE transmission in nursing homes. We hypothesize that we can inform mitigation strategies by identifying patient clinical and microbiota features associated with environmental contamination with VRE. Methods: During a 6-month period of active surveillance in 6 Michigan nursing homes, 245 patients (with 806 follow-up visits) were enrolled. Patient clinical data and swabs for VRE were collected from multiple body sites and high-touch environmental surfaces. In total, 316 perirectal swabs were collected from 137 patients for gut microbiota analysis and community status type (CST) assignment based on taxonomic composition. The associations between VRE colonization pattern, gut microbial CST, and patient factors were examined using multivariable generalized estimating equations, adjusting for patient-and facility-level clustering. We used VRE colonization patterns to group study visits: “uncolonized” (patient−/environment−); “environment-only” (patient−/environment+); “patient-only” (patient+/environment−); “both” (patient+/environment+). Results: Across all study visits, VRE colonization on patient hand and groin/perirectal area was positively correlated with VRE contamination of high-touch environmental surfaces, suggesting direct transfer of VRE between patient and environment via patient hands (Figure 1A). We next set out to identify patient factors associated with patient colonization and environmental contamination. At baseline, while patients in the “both” group had anticipated risk factors such as longer prior hospitalization and more frequent broad-spectrum antibiotic use, they were unexpectedly younger than “uncolonized” patients and had similar functional status. This last feature contrasted with the “patient-only” group, characterized by higher urinary catheter use and higher functional dependence, suggestive of lower functional dependence facilitating patient contamination of their environment. No clinical features distinguished “uncolonized” and “environment-only” patients (Table 1). Lastly, in multivariable analyses, we determined the contribution of patient functional status and gut microbiota features to environmental contamination. Low-diversity CST, characterized by reduced anaerobic taxa, was weakly associated with “patient-only” and significantly associated with “both.” Notably, high functional dependence was significantly associated with “environment-only” and “patient-only” but not “both,” indicating high-functioning patients with disrupted gut microbiota as drivers of environmental contamination (Figure 1B). Conclusions: Our findings suggest that antimicrobial exposure disrupts patient gut microbiota, a significant mediator of colonization dynamics between patients and their environment, and that high-functioning patients may be more likely to spread VRE between their body sites and high-touch environmental surfaces (Figure 2). These findings highlight both antibiotic stewardship and patient hand hygiene as important targets for interrupting transmission mediated by environmental contamination.
Funding: No
Disclosures: None
Figure 1.
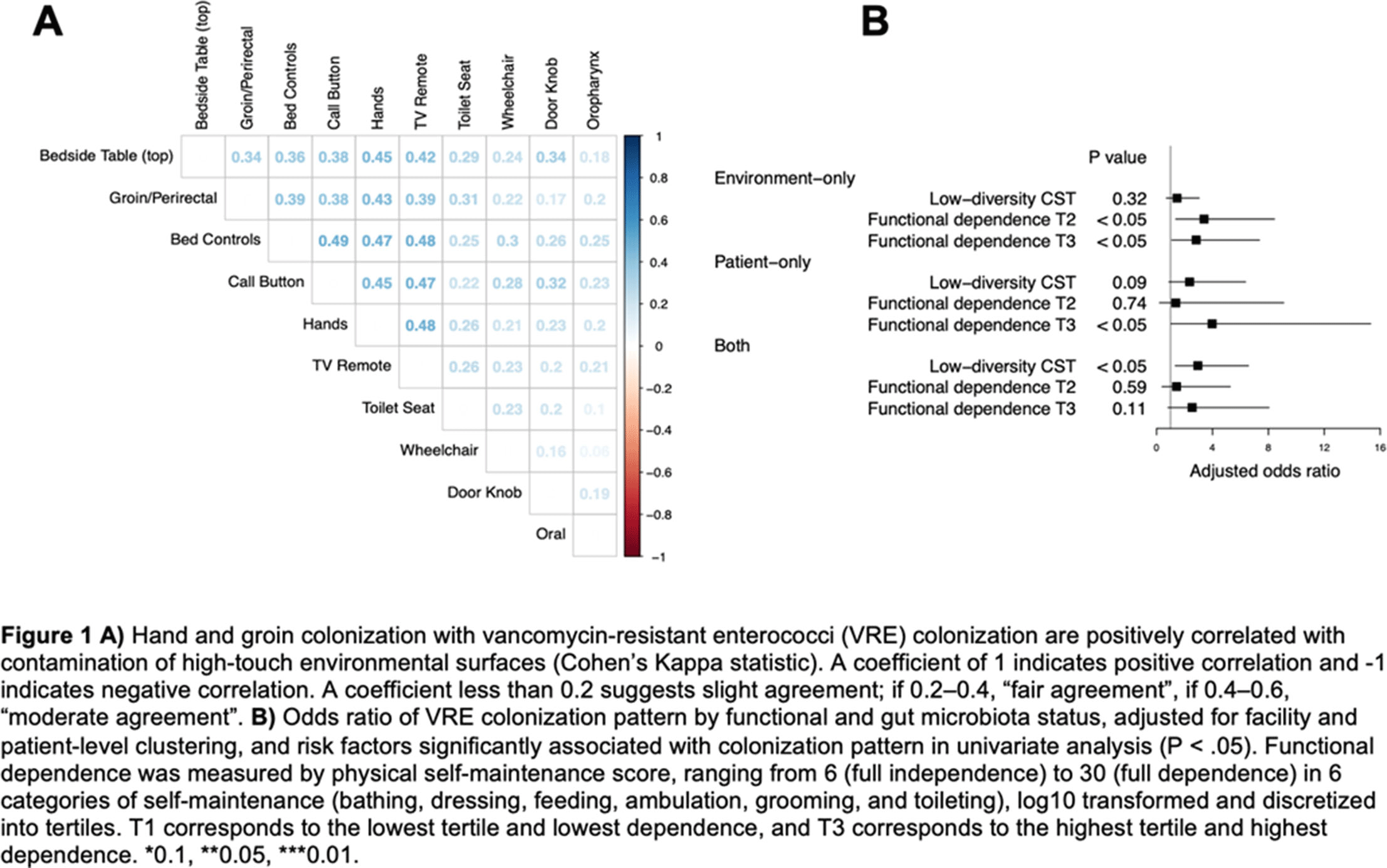
Table 1. 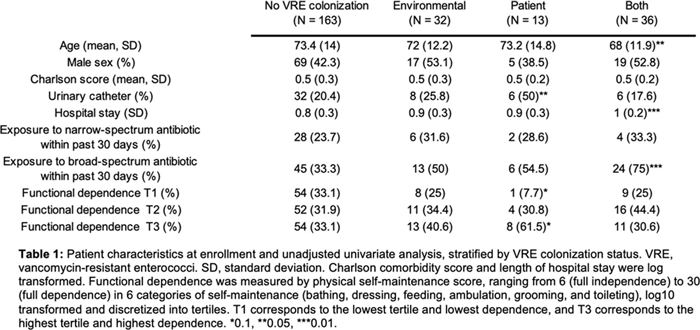
Figure 2.
Racial Differences in Infection Management and Palliative Care at End-of-Life in Nursing Homes Nationwide
- Leah Estrada, Andrew Dick, Patricia Stone, Jordan Harrison
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s69
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infections are common at end-of-life in older nursing-home residents. This often leads to the overuse of antibiotics and burdensome treatments. Improving infection management through palliative care at the end of life has been proposed as a key strategy to reducing inappropriate antibiotic use. Black nursing-home residents tend to reside in poorly performing nursing homes. We examined palliative care services in nursing homes with varying proportions of black residents. Methods: Cross-sectional, nationally representative nursing-home survey data (2017–2018) was combined with the Minimum Data Set 3.0 (nursing-home resident characteristics), the Certification and Survey Provider Enhanced Reporting data (nursing-home facility characteristics), and the Multidimensional Deprivation Index (county-level poverty estimates). The survey included 24 validated items on nursing-home palliative care services, as well as the nursing home’s infection control program and integration of infection management and palliative care (summative score, 0–100). We used nursing-home facility-level multivariate regression to estimate the relationship between proportion of black residents and palliative care scores, before and after controlling for county-level poverty estimates, facility characteristics, and resident characteristics. We categorized proportion of black residents using methods reported in the literature (25%). Results: The mean weighted palliative-care score in our sample of 869 nursing homes (weighted n = 15,020) was 47.7 (SE, 0.70). In unadjusted analyses, nursing homes with higher proportions of black residents provided significantly fewer palliative care services than nursing homes with no black residents, with the greatest differences (P = .027) observed between nursing homes with >25% black residents (mean palliative care score, 43.82; SE, 2.31) versus nursing homes with no black residents (mean palliative care score, 49.47; SE, 1.08). These disparities persisted after adjustment for urbanicity and county-level poverty rates (p < 0.01) but were attenuated after further adjustment for resident and facility level characteristics (p=0.138). Conclusions: Our findings demonstrate that wide variations in nursing-home palliative-care services exist with increased proportions of black residents, even after accounting for community characteristics. Further research is needed to identify and understand the specific community characteristics that play a role in the provision of palliative care services. Palliative care is a method to reduce inappropriate antimicrobial use at the end of life and should be expanded with a focus on nursing homes with higher proportions of black residents.
Funding: No
Disclosures: None
Table 1. 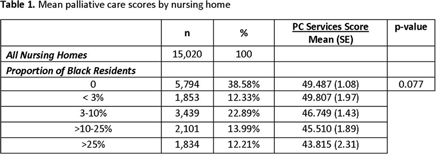
MDR GNR
Evaluation of Ceftolozane/Tazobactam, Ceftazidime/Avibactam and Meropenem/Vaborbactam Against Multidrug-Resistant (MDR) Pseudomonas
- Haider Shamsulddin, Jeffrey Lin, Julie Ribes, Thein Myint
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s69-s70
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Data on the patient outcomes for newer β-lactam–β-lactamase inhibitor (BLBI) drugs compared to carbapenem-containing combination antibiotics for multidrug-resistant (MDR)–Pseudomonas aeruginosa infections are limited. Methods: This retrospective, case–control observational study was based on chart review of the patients managed at the University of Kentucky. Results: In total, 143 patients with MDRO Pseudomonas aeruginosa infections were identified and divided into 2 groups: 1 group received newer BLBI combinations with or without aminoglycosides or polymyxins, for at least 72 hours, and the control group received carbapenem containing combination antibiotics or other antibiotics. Baseline characteristics and patient outcomes are shown in Table 1. Discussion: The newer BLBI combinations group consisted of 60.8% MDR Pseudomonas bacteremia, whereas the control group had 68.4% of MDR Pseudomonas respiratory cultures. Overall, the use of newer BLBI combinations such as ceftazidime/avibactam, ceftolozane/tazobactam, and meropenem/vaborbactam was associated with lower rates of acute kidney injury (AKI), shorter LOS, and lower mortality rates compared to the control group, and these differences were statistically significant. Because the 2 populations of patient differed significantly based on the site of infection (sepsis vs pneumonia), the data were reanalyzed to evaluate the impact of therapy on the occurrence of AKI, LOS, and mortality based on the site of infection. Only those patients with sepsis who received the newer combination drugs had significantly better rates of AKI, lower LOS, and had lower rates of mortality. The 2 treatment arms were not statistically different when comparing patients with pneumonia. Additionally, the use of these new combination therapies did not make a difference regarding readmission rates or duration of bacteremia for the patients included in the study.
Funding: No
Disclosures: None
Table 1. 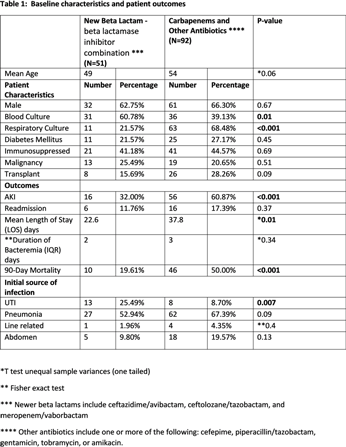
Table 2. 
Time Above All Else: Pharmacodynamic Analysis of Β-Lactams in Critically Ill Patients
- Katherine Landmesser, David Burgess, Justin Clark
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s70
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Despite the development of new β-lactam agents, gram-negative resistance continues to be an increasing concern in the healthcare setting. The understanding and optimizing antimicrobial pharmacokinetics and pharmacodynamics are essential to enhance activity of appropriate therapy, improve clinical outcomes, and reduce the development of resistance. Methods: A pharmacodynamic analysis was performed for 4 β-lactams (aztreonam, cefepime, piperacillin/tazobactam, and meropenem) and 14 dosage regimens as either intermittent bolus (IB) or prolonged infusion (PI) against 7 gram-negative pathogens: Klebsiella pneumoniae, K. oxytoca, Escherichia coli, Enterobacter cloacae, E. aerogenes, Acinetobacter baumannii, and Pseudomonas aeruginosa. Unit-specific minimum inhibitory concentration (MIC) distribution data were generated using antibiogram data over a decade for 4 intensive care units within our institution: medical ICU, cardiovascular ICU, surgical ICU, and neurosurgical ICU. Published pharmacokinetic parameter estimates in critically ill patients, combined with this MIC distribution data, were utilized to perform Monte Carlo simulations for each antimicrobial regimen. The percentage of time for which the unbound concentration of antibiotic remained above the MIC (ƒT>MIC) was utilized as the pharmacodynamic target for each agent: 40% ƒT>MIC for meropenem, 50% ƒT>MIC for piperacillin/tazobactam, 60% ƒT>MIC for aztreonam, and 70% ƒT>MIC for cefepime. Regimens were modeled using Oracle Crystal Ball software to determine the likelihood of achieving >90% probability of target attainment (PTA). Because resistance rates were significantly higher for P. aeruginosa and A. baumannii, cumulative PTAs for K. pneumoniae, K. oxytoca, E. coli, E. cloacae, and E. aerogenes were analyzed separately to determine the relative PTA for Enterobacterales in each ICU. Results: No intermittent infusion regimens of piperacillin/tazobactam, aztreonam, or cefepime achieved >90% PTA for any organism. Piperacillin/tazobactam 4.5 g infused over 4 hours (PI q6h) and aztreonam 2 g PI q6h failed to achieve adequate PTA for Enterobacterales with only 84% and 85% PTA, respectively. For Enterobacterales, the only regimens to achieve >90% PTA included cefepime 2 g infused over 3 hours (PI q8h) and meropenem 1g IB q8h with 95% and 99% PTA, respectively. Meropenem 2 g PI q8h was the only regimen capable of achieving >90% PTA for both A. baumannii and P. aeruginosa with 97% and 92% PTA, respectively. Conclusions: Although utilization of high doses and prolonged infusions dramatically improve the pharmacodynamics of β-lactam therapy, the only regimen capable of achieving adequate PTA for all organisms analyzed was meropenem 2g PI q8h. To reduce carbapenem use, combination therapy may be considered for critically ill patients receiving aztreonam, cefepime, or piperacillin/tazobactam for empiric treatment of gram-negative infections.
Funding: No
Disclosures: None
Difference in Susceptibility Between Carbapenemase- and Non–Carbapenemase-Producing Carbapenem-Resistant Enterobacteriaceae
- Justin Clark, David Burgess
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s70
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Carbapenem-resistant Enterobacteriaceae (CRE) remain among the most urgent infectious threats according to the CDC Threats Reports. Although focus has often been placed on carbapenemase-producing phenotypes, there is increasing interest in distinguishing the optimal treatment and outcomes of carbapenemase-producing (CP) and non–carbapenemase-producing (NCP) CRE. We compare antimicrobial susceptibility patterns between CP-CRE and NCP-CRE isolated from patients at our academic medical center. Methods: All CRE isolates of Enterobacter cloacae, Escherichia coli, Klebsiella aerogenes, K. oxytoca, and K. pneumoniae in adult inpatients from 2010 to 2019 were included in this study. Susceptibility testing was performed using the BD Phoenix Automated System (BD Diagnostics, Sparks, MD). CLSI susceptibility break points were utilized in the susceptibility analyses of all antimicrobials tested. To determine carbapenemase production, isolates resistant only to ertapenem were considered NCP-CRE, and those resistant to both ertapenem and meropenem were considered CP-CRE. Statistical comparisons of susceptibility profiles were performed using either the χ2 test or the Fisher exact test. All data preprocessing and statistical analyses were performed using Python software. Results: Over the decade, we identified 291 CRE isolates (216 isolates resistant only to ertapenem and 75 resistant to ertapenem and meropenem). The ertapenem-resistant–only phenotype comprises ~66% of the total CRE population and is largely composed of E. cloacae (67%). As expected, most β-lactam susceptibilities were negligibly low between the 2 groups; however, other clinically relevant antimicrobials (aminoglycosides, fluoroquinolones, and sulfamethoxazole/trimethoprim) exhibited starkly different susceptibility profiles (P value Conclusions: These findings suggest that the most predominant CRE phenotype at our institution is not carbapenemase production. Evaluation of outcomes between CP- and NCP-CRE should be pursued further. The large differences in the MIC distributions may lead to differing outcomes for the affected patients.
Funding: No
Disclosures: None
Stewardship Nightmare: Ceftolozane/Tazobactam–Resistant Pseudomonas aeruginosa Infections Accelerated by the COVID-19 Pandemic
- Adam Haviland, Gregory Weston, Priya Nori, Wendy Szymczak, Yi Guo, Rebecca M. Marrero Rolon
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s70-s71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The Centers for Disease Control and Prevention reported 32,600 cases, 2,700 deaths, and healthcare costs of 767 million dollars attributed to multidrug-resistant Pseudomonas aeruginosa. A recent study of 128 patients with nosocomial pneumonia due to P. aeruginosa showed the noninferiority of ceftolozane-tazobactam compared to meropenem. However, the resistance of ceftolozane-tazobactam due to AmpC mutations has been described. Compared with 2019, we observed an increase from 2 to 13 cases of ceftolozane-tazobactam–resistant P. aeruginosa (CRPA) during the COVID-19 pandemic at our institution in the Bronx, New York. Methods: A report of patients with CRPA between March and August 2020 was obtained. Data collected included demographics, hospitalization/IV antibiotic use in prior 90 days, SARS-CoV-2 PCR result, ICU admission, length of stay, antibiotic days of therapy, mortality, etc. Results: In total, 13 patients with CRPA infection were reviewed (Table 1). Among them, 2 patients were on the same inpatient medical-surgical unit but separated by 5 months. Also, 11 patients were from different medical-surgical units or ICUs. In addition, 5 patients (38%) were SARS-CoV-2 PCR positive. None of these COVID-19 patients were cohorted on the same unit, making horizontal spread of CRPA or COVID-19 unlikely. Finally, 8 of these patients died while hospitalized (4 were COVID-19 patients). Conclusions: We found a high incidence of mortality in patients with CRPA infection. Many patients had prolonged hospital stay and required ICU admission. Few patients were from long-term care facilities. Given the associated morbidity and mortality, increased surveillance and intensified antimicrobial stewardship efforts are needed to mitigate the impact of CRPA during the COVID-19 pandemic.
Funding: No
Disclosures: None
Table 1. 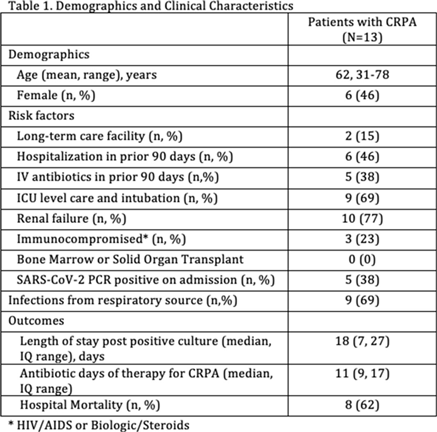
Treatment of Extensively Drug-Resistant (XDR) Acinetobacter in US Veterans’ Affairs (VA) Medical Centers
- Margaret Fitzpatrick, Katie Suda, Linda Poggensee, Amanda Vivo, Geneva Wilson, Makoto Jones, Martin Evans, Nasia Safdar, Charlesnika Evans
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s71
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Infections caused by Acinetobacter spp are often healthcare acquired and associated with high mortality. Extensively drug-resistant (XDR) Acinetobacter are nonsusceptible to at least 1 agent in all but 2 or fewer antibiotic classes. Few of the new antibiotics targeting multidrug-resistant gram-negative bacteria are effective against XDR Acinetobacter. Recent national guidelines for treatment of resistant gram-negative infections do not include Acinetobacter, leaving a knowledge gap in best practices. Methods: This retrospective cohort study included microbiology, clinical, and pharmacy data from all patients hospitalized between 2012 and 2018 at any Veterans’ Affairs medical center who had cultures that grew XDR Acinetobacter spp. Bivariate unadjusted analyses compared clinical outcomes by monotherapy versus combination therapy. Using mixed-effects ordinal logistic regression, propensity score–adjusted models accounting for severity of illness and other variables associated with treatment were fit to compare outcomes. Results: Of 11,546 patients with 15,364 cultures that grew Acinetobacter spp, 408 patients (3.5%) had 666 cultures (4.3%) with XDR Acinetobacter. Moreover, 276 of these patients (67.6%) had gram-negative targeted antibiotic treatment within −2 to +5 days from the culture. Furthermore, 118 patients (42.8%) received monotherapy, most commonly piperacillin-tazobactam (n = 54, 45.7%) or an anti-Pseudomonas cephalosporin (n = 21, 17.8%). Also, 158 (57.2%) patients received combination therapy, most commonly a carbapenem (n = 93, 58.9%) and/or polymyxin (n = 68, 43.0%). Moreover, 41 patients (25.9%) received both a carbapenem and polymyxin. In both unadjusted and adjusted analyses, there were no significant differences in the odds of 30-day mortality (aOR, 1.43; 95% CI, 0.86–2.38) or 1-year mortality (aOR, 1.04; 95% CI, 0.68–1.60) between combination therapy and monotherapy groups. Among 264 patients (96%) whose cultures occurred during an inpatient or long-term care admission, unadjusted analyses showed increased odds of in-hospital mortality (OR, 1.89; 95% CI, 1.08–3.29) and longer postculture length of stay in the combination therapy group: median, 23 days (IQR, 11–57) versus 14 days (IQR, 7–32) (P = .02). However, with propensity score adjustment, these associations were no longer significant. Furthermore, there was no significant difference in odds of 90-day readmission between groups in either unadjusted or adjusted analyses (aOR, 1.20; 95% CI, 0.74–1.95). Conclusions: In this large national cohort of patients with XDR Acinetobacter cultures, more patients received combination therapy than monotherapy, and carbapenems and polymyxins were the most-used classes. However, there were no significant differences in outcomes between patients receiving combination therapy and monotherapy, suggesting lack of clinical benefit to the common practice of treating XDR Acinetobacter infections with multiple antibiotics. Further research is needed to determine optimal treatment strategies for this pathogen.
Funding: No
Disclosures: None
Molecular Epidemiology
Extended-Spectrum Β-Lactamases in E. coli Isolates From Hospitalized Patients: A Single-Center Snapshot From Croatia
- Tomislav Mestrovic, Branka Bedenic, Maja Tomic-Paradzik, Domagoj Drenjancevic
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s71-s72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: A significant increasing trend in the prevalence of Escherichia coli strains that produce extended-spectrum β-lactamases (ESBLs) has been observed in recent years, both in the community setting and in the healthcare arena. We aimed to provide a snapshot of the current situation with E. coli β-lactamase–producing strains in a single general hospital by appraising their β-lactamase content and plasmid types, which will inform further clinical and research efforts. Methods: Our study population consisted of all hospitalized patients in different clinical units of the General Hospital in Slavonski Brod during a 1-year period: internal medicine, infectious disease, surgery, urology and ICU. Phenotypic tests for the detection of ESBLs and plasmid-mediated AmpC β-lactamases were initially pursued, followed by the molecular detection (polymerase chain reaction, PCR) of resistance genes using primers for blaTEM, blaCTX-M, and blaSHV. PCR-based replicon typing (PBRT) was conducted to type resistance plasmids carrying ESBL genes. Results: During the study period, 30 E. coli isolates with reduced susceptibility to third-generation cephalosporins (ie, ceftazidime, cefotaxime, and ceftriaxone) were detected in hospitalized patients. These isolates stemmed from blood culture (66.7%), wound swabs (13.3%), urine (13.3%), and drainage content (6.7%). Alongside complete resistance to β-lactam antimicrobial agents, they were also characterized by high resistance to gentamicin (93.3%) and ciprofloxacin (96.7%), whereas 23.3% of isolates were also resistant to ertapenem. Most isolates harbored both blaCTX-M and blaTEM genes concurrently (46.7%), while solitary blaTEM and blaCTX-M genes were found in 33.3% and 20% of these isolates, respectively. The presence of SHV β-lactamases was not found in any of the isolates. PBRT revealed a wide array of diverse plasmid groups, with most of the isolates harboring different combinations; however, 80% of isolates were characterized by plasmid incompatibility group B/O (IncB/O). Conclusions: We detected increased frequency of both TEM and CTX-M type β-lactamases in E. coli isolates from a single-hospital setting, with significant consequences for further treatment approaches. The high prevalence of broad- and extended-spectrum β-lactamase producers tends to prompt an increased carbapenem use (potentially resulting in increased resistance to carbapenems); thus, this type of analytical work should become a standard approach (where possible) in hospital centers in our country and worldwide.
Funding: No
Disclosures: None
MRSA/VRE
Hospital Onset Vancomycin-Resistant Enterococci Infections in a Northern California Tertiary-Care Center From 2019 to 2020
- Stephanie Rasmussen, Sarah Waldman
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Understanding the epidemiology and risk factors for nosocomial infections with vancomycin-resistant enterococci (VRE) is necessary for the prevention and control of VRE infections in the hospital setting. We sought to determine the incidence of nosocomial infections of VRE and to ascertain predictors associated with nosocomial infection. Methods: In this retrospective cohort study, data were collected from patients with VRE infection from January 2019 to December 2020 at a tertiary-care center in northern California. VRE infections were designated as hospital onset (HO) if the specimen was collected >3 days after hospital admission or community onset (CO) if the specimen was collected ≤3 days after admission. Associations between HO infections with time, unit, and specimen were identified. Results: Over the 2-year period, 214 unique VRE infections were identified in hospitalized patients; 115 infections were CO and 99 were HO. HO-VRE were associated most frequently with stay in medical/telemetry units (68%), followed by oncology–transplant units (15%) and ICUs (12%). There were ~4.7 and ~3.6 HO-VRE infections per month in 2019 and 2020, respectively. No differences were identified between HO-VRE infections in 2 medical units regarding glycopeptide and cephalosporin use in those units. The sources of VRE infections were urinary 45%, bloodstream 15%, stool 10%, and other 30%. Of the 45 infections in urine, 51% were identified from catheters (Foley and straight) and 27% were identified from clean-catch urine. Interestingly, 71% of patients with VRE identified from urine did not report urinary tract infection (UTI) symptoms at the time of collection. Urine was most often collected for urinalysis and culture from patients with nonspecific symptoms such as fever, leukocytosis, hypotension, tachycardia, or altered mental status. All urine collected from patients who reported UTI symptoms grew >100,000 CFU/mL in culture, while only 75% of cultures from patients without symptoms grew >100,000 CFU/mL. The most common antibiogram was resistance to ampicillin, cefazolin, levofloxacin, minocycline, penicillin, tetracycline, and/or vancomycin (42% of cases) and susceptibility to both daptomycin and linezolid (60% of cases). Conclusions: HO-VRE infections were frequently identified with urinary sources and were often associated with catheter use. However, the frequent lack of concurrent UTI symptoms suggests VRE colonization rather than infection in many cases. Understanding the epidemiology and risk factors for HO-VRE infections is essential for developing infection prevention protocols to reduce the incidence of those infections.
Funding: No
Disclosures: None
Occupational Health
Experience with Bloodborne Pathogen Exposures Among Operation Room Nurses in Korea: A Qualitative Study
- JaHyun Kang, Hyunsook Lee
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s72
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Operation room (OR) nurses are at a high risk for bloodborne pathogen (BBP) exposures because they are constantly in contact with blood and body fluid (BBF) through surgical sites, and they frequently use sharp surgical instruments and sutures during surgeries. We explored occupational experiences with BBP exposures among OR nurses in South Korea. Methods: With an institutional review board’s approval, this qualitative research was performed with 12 OR nurses who had worked for >3 months and had experienced BBP exposures. Based on the main research question “How is the experience of BBP exposure among OR nurses?” the semistructured questions for in-depth interview were prepared. Narrative data were collected through 1-hour individual interviews from June to September 2020 and were analyzed using a thematical analysis method. Results: The average age of the participants was 34.4 years with an average 9.75 years of clinical experience. The main theme extracted was “The nurses are alerted to their safety after experiencing the aftereffects and emotional trauma from BBP exposures,” with 4 subthemes and 14 concepts. The first subtheme, “OR nurses risking exposure to BBF,” included (1) hurried doctors and hasty nurses; (2) sharp surgical instruments everywhere; (3) deprioritized self-protection due to ongoing surgery; (4) inattentive to BBF risk; and (5) uncomfortable, foggy goggles and receded safety devices. The second subtheme, “BBP exposures occurred in a flash,” included (1) sharp injury occurred in a split second; (2) temporarily treat sharp wounds while hiding frightened feelings; and (3) OR nurses concentrated on surgery by suppressing anxiety and sharp wounds. The third subtheme, “Burdened time that could be overwhelmed alone,” included (1) BBP exposures moments that I wish to reverse; (2) anger over dangerous environments and the turmoil of anxiety; (3) exhausted body and facial discoloration due to taking postexposure prophylaxis; and (4) exposure to BBP that I want to hide from family and friends. The fourth subtheme, “Voice for everyone’s safety,” included (1) establishing a safety culture, which requires everyone’s efforts, and (2) necessity of practical resources for decreasing BBP exposures. Conclusions: The participating OR nurses felt that they were working with a high risk to BBF exposures and called for institutional interventions to reduce the risks, including surgeons’ attentive collaboration. Korean hospitals should make greater efforts to establish safety culture in ORs and to provide repeated, tailored education to prevent BBF exposures. They should also supply high-quality protective equipment and safety-engineered devices for OR nurses.
Funding: No
Disclosures: None
Outbreaks
Zero Healthcare-Associated COVID-19
- Moi Lin Ling, Molly How, Kwee Yuen Tan, Elaine Wee, Phoon Poh Choo, Lai Chee Lee
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: The ongoing COVID-19 pandemic tests the healthcare system in many ways. The scarcity of resources poses challenges to infection prevention (IP) practices. We describe our experience in managing such scarcity in our care of COVID-19 patients in the hospital as well as community settings. Methods: The hospital pandemic plan traditionally included only plans for healthcare delivery management within the hospital. However, on March 25, 2020, a decision was made by the Ministry of Health to set up swab isolation (SIFs) and community care facilities (CCFs) to meet the growing demand for isolation beds for migrant workers infected by COVID-19. The CCFs were located in convention halls and resort centers and the SIFs were located in facilities previously functioning as hotels. Mobile medical teams were activated to run clinics at the dormitories housing 200,000 migrant workers. The IP team of an acute- and tertiary-care hospital in Singapore was activated to oversee IP measures at facilities managed by medical teams from the hospital, with the goal of zero healthcare-associated COVID-19 cases among staff. Two IP leaders were set up to oversee the IP program at 8 dormitories, 4 SIFs, and 2 CCFs. In total, 12 IP staff and 15 infection prevention liaison officers (IPLOs) were deployed from 2 acute-care hospitals and 3 specialty centers to conduct training in hand hygiene and the use of personal protective equipment, and to conduct daily audits of compliance to practice guidelines. Education on personal hygiene was also given to patients in these facilities in at least 7 languages. In the SIFs and dormitories, IPLOs were recruited to perform daily audits and feedback to the IP team on issues related to IP at the sites. Results: Since our first COVID-19 patient on January 23, 2020, there has been no report of healthcare-associated COVID-19 within the hospital nor among the medical, administrative, and support service staff working in the external operation facilities. Daily audits showed an average of 99.4% compliance to IP guidelines. Conclusions: IPLOs or IP champions play a significant role in ensuring compliance to IP guidelines. This compliance allows the IP professional to focus on the evaluation of the IP program, managing IP consultations, and planning and implementation of the IP program in nontraditional healthcare settings. The key success factors of the program included the ability to contextualize the planning and implementation of IP programs in various settings, strong leadership support, cohesive teamwork, and effective communication at various levels.
Funding: No
Disclosures: None



















