Community treatment orders (CTOs) exist in many countries. They were introduced into legislation for England & Wales in 2007 and into Scotland's legislation in 2005. The use of CTOs and the research into their effectiveness has caused much debate. The aim of this article is to give an accessible overview of: the spread and use of CTO legislation; the evidence base for CTO effectiveness; the arguments in the debates about CTOs and their evidence; and the way forward for CTO practice.
The spread and use of CTO legislation
Community compulsion and deinstitutionalization
In most industrialised Western countries, there has been a massive change towards closing hospital beds and delivering mental healthcare in the community. This presents new challenges, particularly for patients who do not want to accept treatment but whose lives are adversely affected by their mental illness. Some end up in the ‘revolving door’ of frequent readmissions. The response in many jurisdictions has been to introduce legislation for compulsory community treatment in the form of CTOs. These make adherence to treatment a legal requirement, and allow swift admission to hospital when necessary.
CTOs are designed to ensure that patients who need treatment but are well enough for that treatment to be delivered outside hospital get the care they need even if they are not willing to accept it voluntarily. This is anticipated to reduce relapse rates and hospital admissions and to help patients gain insight into their situation, so that over time they choose to engage in treatment voluntarily.
Differences in CTO legislation
CTOs were first conceived as a less restrictive alternative to involuntary hospital admission. They allowed patients detainable under mental health legislation to be treated outside hospital and had the same stringent criteria as involuntary admissions. From the perspective of clinicians, patients and their families, as well as human rights lawyers, ‘least restrictive’ CTOs were considered preferable to hospital detention. Gradually, so-called ‘preventive’ CTOs were developed that could be imposed to prevent hospital admission or harm, rather than being an alternative for patients already admitted. These have been criticised for lowering the threshold for the use of mental health legislation and for being preoccupied with public fear and control of risk, thereby extending the net of social control. Thus, there was a shift from CTOs perceived as liberty enhancing to CTOs as legal, controlling treatment regimes (Reference Churchill, Owen and SinghChurchill 2007).
This difference is visible in current regimes. In some countries, such as England & Wales and Sweden, a patient can only be placed on a CTO following a hospital admission. In most other jurisdictions, including Scotland, a patient can be placed on a CTO directly from the community, although in practice this is relatively uncommon. CTO regimes also differ in their duration, how they are linked to treatment, the threshold for compulsion and whether patients must have a history of admissions (Reference DawsonDawson 2005).
The spread of CTO legislation in different parts of the world
Legal regimes for community compulsion now exist in around 75 different jurisdictions. From the 1980s onwards, most North American states and provinces introduced court-ordered CTOs (called variously ‘outpatient commitment’, ‘mandatory out patient care’ and, more recently, ‘assisted outpatient treatment’ in the US literature). The Australian territories and New Zealand followed suit from the early 1990s, introducing clinician-initiated CTOs (Reference DawsonDawson 2005). Since then, CTOs have been introduced in many European, and some Asian, countries (Box 1).
BOX 1 Jurisdictions where CTOs are used
-
Australia (all 7 states/territories)
-
Belgium
-
Canada (9 of 13 provinces/territories)
-
England & Wales
-
Fiji
-
Gibraltar
-
Hong Kong
-
Israel
-
Luxembourg
-
New Zealand
-
Norway
-
Portugal
-
Samoa
-
Scotland
-
Spain (despite no explicit legislation they are used some places)
-
Sweden
-
Switzerland (all 26 cantons)
-
Taiwan
-
Tonga
-
USA (46 states/districts)
In the UK, CTOs were introduced first in Scotland in 2005, via the Mental Health (Care and Treatment) (Scotland) Act 2003, and then in England & Wales in 2007, via amendments to the Mental Health Act 1983 (Box 2). CTOs are not available in Northern Ireland, but draft legislation is being considered.
BOX 2 CTOs in England & Wales
CTOs in England & Wales are governed by section 17a of the Mental Health Act 1983 (as amended in 2007). To impose a CTO, all of the following criteria must be fulfilled:
-
• the person has a mental disorder of a nature or degree that makes it appropriate for them to receive medical treatment
-
• it is necessary for the person's health or safety or for the protection of others that they should receive treatment
-
• treatment can continue in the community without the person being detained in hospital
-
• it is necessary that it be possible to recall the person swiftly to hospital if needed
-
• appropriate medical treatment is available.
The order is made by the responsible clinician (usually a psychiatrist) and an approved mental health professional (usually a social worker). The order lasts for 6 months. It can then be renewed for a further 6 months, and thereafter for 12-month periods. The order can be ended by the responsible clinician at any time and by reviews by managers of the treating hospital or a mental health review tribunal.
All CTOs include two mandatory conditions. These are that patients must make themselves available:
-
• to be assessed by a second psychiatrist in order to complete the mandatory peer review of their treatment without consent, when required
-
• for assessment concerning renewal of the CTO.
The responsible clinician and approved mental health professional may also specify discretionary conditions that are needed to ensure that the patient receives medical treatment, or to prevent risks of harm to the patient or others, based on their knowledge of the individual patient. These may subsequently be varied by the responsible clinician.
Patients on CTOs may be recalled to hospital for up to 72 h if they:
-
• breach a mandatory condition; or
-
• require further treatment in hospital and there would be a risk of harm to self or others if they were not recalled.
Recall can be used for assessment or to provide treatment without consent for up to 72 h. After that, one of three courses can be taken: (a) the patient returns to the community under the CTO; (b) the CTO is revoked and the patient remains in hospital for involuntary treatment under section 3 of the Mental Health Act; or (c) the patient is discharged from involuntary care.
Debates about CTOs
The introduction of CTOs proved extremely controversial in some jurisdictions, not least where it was preceded by public pressure after high-profile killings by psychiatric patients. In the US state of New York, for example, CTO legislation became known as Kendra's law, named after a young woman killed by a man with diagnosed psychosis known not to be taking his medication. Despite being welcomed in some quarters there, CTOs were met with strong opposition from patient advocates, and mixed views were expressed by clinicians (Reference GellerGeller 2006). In England & Wales, the power of CTOs had been sought by professional bodies for 20 years (Royal College of Psychiatrists 1993), but when the law was eventually passed it was resisted by a coalition of 32 professional and patient organisations (Mental Health Alliance 2005).
Human rights issues are often central to the debate. In some places, including both New York State and England & Wales, the focus is often on negative rights, such as the right not to have one's liberty restricted. In other contexts, such as Norway and Sweden, positive rights, such as entitlement to care, are more prominent (Reference Sjöström, Zetterberg and MarkströmSjöström 2011). Some of the arguments in the debate are summarised in Box 3.
BOX 3 Arguments in debates leading up to the introduction of CTOs

| For | Against |
|---|---|
| • CTOs can reduce risk to patients and others and address the public's fear of risk posed by patients • The poor outcomes experienced by ‘revolving-door’ patients must be addressed • To defend individuals’ right to remain in unhealthy/unsafe situations runs counter to professionals’ obligations to help • Appropriate treatment should be available in the community as well as in hospital • CTOs may pave the way for patients to use a range of services • There are some reports of good outcomes of CTOs |
• Public fear is an insufficient justification for restricting individuals who have not broken the law • A more coercive system is not therapeutic and might alienate patients • Individuals have the right to make lawful decisions about their own lives (provided that they have capacity to do so) • A principle of reciprocity would require that restrictions of civil liberties are matched by providing adequate, high-quality services • Compulsion might become a cheap alternative to investing in decent services • The efficacy of CTOs lacks an evidence base |
The literature on CTO effectiveness (reviewed later in this article) has been interpreted by people on opposite sides of the debate as supporting their position (Reference Sjöström, Zetterberg and MarkströmSjöström 2011). Several ethical analyses have concluded that CTOs are justifiable (Reference Munetz, Galon and FreseMunetz 2003; Reference Snow and AustinSnow 2009). These analyses have, however, often been based on an assumption that CTOs benefit patients.
CTO use: variation between jurisdictions, services and psychiatrists
The rate of CTO usage varies enormously between jurisdictions. In the USA, use at any one time in different states varies between 1 and 50 per 100 000 population. They are less frequently used in Canada (Reference Lawton-SmithLawton-Smith 2005). Corresponding figures in Australian jurisdictions range from around 32 to 100 per 100 000 (Reference Light, Kerridge and RyanLight 2012). In the UK, recent figures suggest that 10 in 100 000 people in England and Wales (Health and Social Care Information Centre 2015) and 17 in 100 000 in Scotland are on a CTO at any one time (Mental Welfare Commission for Scotland 2015).
There are also differences in how frequently CTOs are used within jurisdictions (Reference Lawton-SmithLawton-Smith 2005). In England, the percentage of patients on a CTO among all those subjected to the Mental Health Act in 2015 was 27.4%, but this varied between NHS trusts from 8.3% to 52.8%. In the independent sector, the average was 2.1%, but varied between 1.2% and 80% (raw data available in Health and Social Care Information Centre 2015).
Usage also varies between psychiatrists. In a recent survey, individual UK psychiatrists reported that they had used between 0 and 100 CTOs (Reference DeRidder, Molodynski and ManningDeRidder 2015). Although there are differences in services and case-loads, it seems reasonable to assume that this varied usage reflects differing views among clinicians and that variation in clinical practice remains beyond the control of legislators (Reference Sjöström, Zetterberg and MarkströmSjöström 2011).
Patients on CTOs: a consistent pattern across countries
Despite the apparently random variation in CTO prevalence, the characteristics of patients subject to CTOs are reassuringly consistent across countries. Around two-thirds are male, and the same proportion is diagnosed with schizophrenia. The mean age is around 40, and patients typically have several prior hospital admissions and a history of non-adherence to out-patient care. Many have problems with substance misuse and have criminal records. Most are single, live in rented accommodation alone or, less often, with their family, and almost none are in regular employment (Reference DawsonDawson 2005; Reference Churchill, Owen and SinghChurchill 2007). This is also the group of patients on CTOs in the UK (Reference Evans, Makala and HumphreysEvans 2010; Care Quality Commission 2011; Reference Dye, Dannaram and LoynesDye 2012; Reference Lepping and MalikLepping 2013; Reference McKieMcKie 2014; Reference Rawala and GuptaRawala 2014; Reference Smith, Branton and CardnoSmith 2014). Less than 5% of CTO patients in England and Wales are discharged onto a CTO from court-ordered hospital admission (Health and Social Care Information Centre 2015).
Prevalence and incidence of CTOs in England and Wales
After its introduction, clinicians in England and Wales were quick to use the new regime, and more than 30 000 CTOs have been issued to date. As shown in Table 1, there was a steady, though small, increase in both prevalence and incidence of CTO use between 2010 and 2015. This increase was not matched by reductions in hospital detention, the prevalence of which continues to increase. It seems that the overall level of coercion has gone up following the introduction of CTOs. A pattern of increased prevalence of CTOs and of overall coercion has also been reported in other jurisdictions (Reference Lawton-SmithLawton-Smith 2005; Reference Light, Kerridge and RyanLight 2012; Reference O'Donoghue, Brophy and OwensO'Donoghue 2016).
TABLE 1 Prevalence and incidence of the use of the Mental Health Act 1983 (MHA) and community treatment orders (CTOs) in England and Wales, 2010–2015
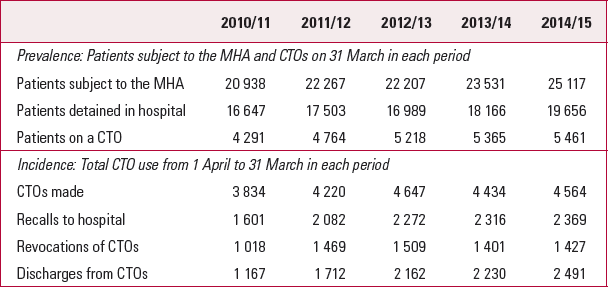
On the basis of the figures in Table 1, we can estimate that between 40% and 50% of CTOs are recalled (i.e. the patient is returned briefly to hospital to consider imposing treatment). Of these, 60–70% are revoked (i.e. the order stops and compulsory hospital treatment is imposed). The most frequently stipulated conditions written into virtually all CTOs are to take medication as prescribed and to remain in contact with the mental health team (Care Quality Commission 2011; Reference Lepping and MalikLepping 2013; Reference Smith, Branton and CardnoSmith 2014; Reference Rugkåsa, Yeeles and KoshiarisRugkåsa 2017). Around a third of CTOs require the patient to live at a specified address (Reference Rugkåsa, Yeeles and KoshiarisRugkåsa 2017). A range of other conditions, such as abstinence from drugs or alcohol, or restrictions on places that the patient is permitted to visit (e.g. schools), are also reported.
The evidence base for CTOs
The established scientific hierarchy of evidence-based medicine from the highest to the lowest level is as follows:
-
1 systematic reviews and meta-analyses (that pool data from high-quality studies)
-
randomised controlled trials (RCTs)
-
controlled outcome studies
-
uncontrolled outcome studies
-
observational studies
-
opinion.
It is generally accepted that only studies at the top levels can establish causality.
Personal experience and views of CTOs
Personal experiences of CTOs have been explored in a handful of jurisdictions, including the UK (Reference Ridley, Hunter and RosengardRidley 2010; Reference Canvin, Rugkåsa and SinclairCanvin 2014; Reference Stroud, Banks and DoughtyStroud 2015), all with similar findings. Patients, clinicians and family members agree that CTOs are preferable to treatment in hospital (Reference Swartz, Swanson and WagnerSwartz 2003). Clinicians generally prefer working in a system with CTOs (although there are exceptions) and find them helpful. Patients are mixed in their appraisals of how well CTOs work, identifying a potential for safeguards, but also many problematic effects (particularly surrounding medication) of coercion ‘moving into your home’ (Reference Riley, Hoyer and LoremRiley 2014). Family caregivers are generally in favour of CTOs and find increased control useful, but are very concerned that they do not ensure support beyond medication (Reference Rugkåsa, Molodynski, Rugkåsa and BurnsRugkåsa 2016a). In some jurisdictions, access to services is conditional on the patient being on a CTO. In England, however, the legislation was explicit that CTOs could not be used for rationing services. Psychiatrists confirm that this is the case in practice (Reference Canvin, Rugkåsa and SinclairCanvin 2014).
Outcome studies
Around 60 outcome studies of CTOs have been published. Most have used admission to hospital as the primary outcome measure. This is because the purpose of a CTO (and of maintenance medication in psychosis) is primarily to reduce relapse, and admission is a good measure of whether this is achieved.
Authors of CTO studies and reviews have identified a range of problems that make this body of literature difficult to address as a whole, including:
-
• a vast number of different outcome measures are used
-
• outcomes are not measured consistently
-
• follow-up periods vary
-
• some studies have very small samples
-
• some focus on subgroups (e.g. patients on a CTO <6 months), others on whole CTO populations
-
• many studies analyse CTOs linked with other interventions (e.g. assertive community treatment), making it impossible to isolate independent effects
-
• studies take different views on what is part of the CTO process and what is its outcome (e.g. intensity of service use; brief readmissions)
-
• context-specific factors may limit generalisation.
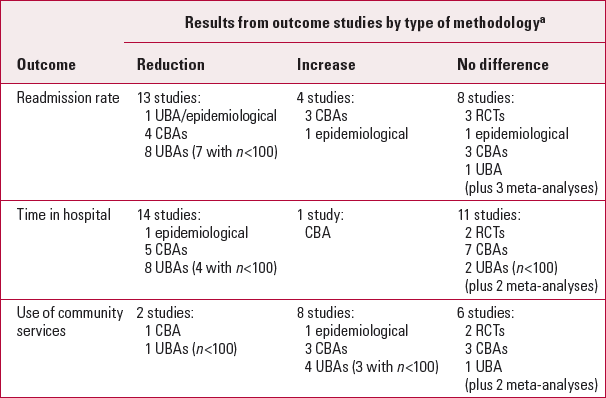
The most frequently measured outcomes are readmission to hospital, time in hospital and the use of community services. Table 2 summarises the results of the 37 studies reporting on these outcomes (for full details, see Reference RugkåsaRugkåsa 2016b). It shows a mixed picture, with the majority of studies reporting either improved outcomes on CTOs or that the orders did not make a difference, and in a smaller number that outcomes worsened. It is essential, however, to look in detail at the methods and quality of these studies.
TABLE 2 Community treatment order outcome studies reporting readmission, time in hospital and/or use of community services
Non-randomised outcome studies
The majority of experimental studies are non-randomised uncontrolled before-and-after (UBA) studies – where a patient's hospital admission outcomes are simply compared before and after being placed on a CTO – or controlled before-and-after (CBA) studies. CBA studies are a somewhat stronger test in which the differences in admission of CTO patients before and after are compared with those of a sample usually matched for diagnosis, duration of illness and psychiatric history.
The UBA studies are clustered in the ‘reduction’ cells in Table 2. Many of them have very small samples, usually because recruitment was limited to one service. The lack of matched controls means that it is impossible to rule out that the results are due to patients improving naturally over time (regression to the mean) or to changes in services, and not to the CTO. The results of CBA studies (which had controls, although inadequately matched in some cases) are more varied. However, most are in the ‘no difference’ cells.
As CTOs were introduced in the UK only relatively recently, there are few outcome studies so far. Some local studies and service audits report improved admission outcomes (Reference Dye, Dannaram and LoynesDye 2012; Reference Lepping and MalikLepping 2013; Reference Rawala and GuptaRawala 2014). These are all UBAs with small samples (n = 21–37). A larger UBA in Scotland (n = 1558) showed a reduction in length of stay, but not in readmission rates (Reference Taylor, Macpherson, Macleod and LyonsTaylor 2015).
Some epidemiological studies that observe, but do not match, CTO and non-CTO populations have also been conducted. Their results are spread across the cells in Table 2.
Overall therefore, non-randomised studies give a mixed picture, and their methods and quality mean that they give no convincing answer to the question of CTO effectiveness.
Randomised controlled trials (RCTs)
RCTs are considered the gold standard for evidence of effectiveness of clinical treatment or interventions because randomising treatment is the most powerful method of reducing the biases that might influence other types of study. Three RCTs of CTOs have been conducted; two in the USA and one in England. All their results fall in the ‘no difference’ category in Table 2. All three have important features, so we outline them next.
The New York State RCT
The RCT in the state of New York randomised 142 patients to either treatment under a CTO or voluntary status; both groups also received case management. At 11-month follow-up, no difference was found in the primary outcome of readmission (Reference Steadman, Gounis and DennisSteadman 2001), nor in the outcomes of length of stay, contact with services, adherence, functioning, symptoms, quality of life, arrests, homelessness and perceived coercion (Reference Churchill, Owen and SinghChurchill 2007). The trial experienced severe methodological problems, however. A smaller than expected sample and high attrition mean that its statistical power might have been insufficient (Reference Swartz and SwansonSwartz 2004; Reference Kisely and CampbellKisely 2006). The New York findings are usually treated with caution.
The North Carolina RCT
This trial randomised 264 patients to CTO or voluntary status. Here also, both groups received case management. Attrition was low (18%) and equally distributed in the two groups. The primary outcome of readmission to hospital showed no difference between the groups over 12 months (Reference Swartz, Swanson and WagnerSwartz 1999). No difference was found in treatment adherence, quality of life, service intensity, arrests, homelessness, quality of life and perceived coercion (Reference Churchill, Owen and SinghChurchill 2007). A significant reduction was detected in victimisation (being a victim of crime) in those in the CTO group.
Fourteen exploratory subgroup or regression analyses were conducted on the North Carolina RCT data. These explored moderators or predictors of associations between CTOs and various outcomes and they are often quoted as evidence for effectiveness of longer-term CTOs. However, many of these analyses included a non-randomised sample of 67 violent patients and/or analysed groups of patients on the basis of how long they were on a CTO (less than or more than 6 months) and not their randomised condition. Many of these analyses are wrongly cited as if they were randomised. Instead, they should be considered exploratory and they are not included in Table 2. As there were no significant differences in outcomes in the original trial, they cannot be used to infer causality, although they may be useful in hypothesis development (Reference Churchill, Owen and SinghChurchill 2007). Several studies have since adopted 6 months as a comparison period, but it is important to be aware that there is no solid scientific support for this. A careful examination of the reported figures (Reference Swartz, Swanson and WagnerSwartz 1999) would suggest that a selection effect (patients thought to do well because of their CTO are kept on the order, whereas others are not) might explain the difference, because the divergence in readmission rates between those on CTOs for more than 6 months and controls actually started at randomisation, not at 6 months.
The OCTET RCT and its longer-term follow-up
The largest RCT to date of the effectiveness of CTOs, the OCTET study, was conducted in England immediately after their introduction. In all, 336 patients were randomised to leave hospital on a CTO or to voluntary status via Mental Health Act section 17 leave of absence (with a median duration of 8 days); both groups received case management both before and during the trial. Attrition was negligible, at 1%. No effect was found on readmission outcomes or service use (Reference Burns, Rugkåsa and MolodynskiBurns 2013). There was also no difference in social functioning, symptoms, insight, adherence, substance misuse, employment, therapeutic relationships, satisfaction with services and perceived coercion (Reference Rugkåsa, Vazquez Montes and BennettRugkåsa 2015). No difference in readmissions was found in subgroups based on gender, ethnicity, diagnosis, living situation, education, symptoms or functioning (Reference Rugkåsa, Vazquez Montes and BennettRugkåsa 2015).
The OCTET Follow-Up Study (a naturalistic follow-up of the trial sample) found that, over 36 months, the median duration of CTOs was 346 days, but found no long-term effects on hospital outcomes or on disengagement from services (Reference Burns, Yeeles and KoshiarisBurns 2015). Perhaps the most remarkable finding was that only 19 patients (6%) had disengaged by the end of 3 years, regardless of being on a CTO or not, and that nearly three contacts per month was sustained with the sample throughout.
Systematic reviews
There have been several systematic reviews of the CTO literature. The largest included 72 studies prior to 2006, of which 28 were outcome studies. The conclusion was that, except for a reduced likelihood of being a victim of violence in the North Carolina study, there was no effect on hospital, clinical or social outcomes (Reference Churchill, Owen and SinghChurchill 2007). The quality of the majority of studies was considered poor. A second review, of studies published between 2006 and 2013, came to the same conclusion of no effect (Reference Maughan, Molodynski and RugkåsaMaughan 2014), as did a third review (using the same search terms but not reported as a systematic review), which included studies up to 2015 (Reference RugkåsaRugkåsa 2016b).
Meta-analyses
A Cochrane review of raw outcome data for 416 patients in the two US RCTs (Reference KiselyKisely 2014a) found no effect, except a reduced likelihood of victimisation. The same authors conducted a meta-analysis of these two RCTs and five non-randomised studies of high enough quality to be included (n = 1108), and came to the same result (Reference Kisely, Campbell and ScottKisely 2007). Finally, a meta-analysis of all three RCTs (n = 749) also concluded that CTOs do not have any benefit on readmissions, duration of readmission, symptoms or social functioning (Reference Kisely and HallKisely 2014b). Summing up the evidence, Reference KiselyKisely (2015) states that ‘the better the control of confounding and other bias through randomisation, matching or multivariate analyses, the less likely it is that CTOs reduce readmission or bed-days’.
Why is the evidence still debated?
All existing evidence at the level where causality may be inferred indicates no patient benefit from CTOs. Patients on CTOs experience significant periods of community coercion, but do not have better outcome than patients not on CTOs. Nevertheless, there are still debates about how to interpret the evidence. These debates possibly reflect different attitudes to the role of evidence-based practice in community psychiatry. Some of the issues being debated are the following.
Have RCTs included the right patients?
Critics of the RCT evidence claim that these studies have not included the ‘right’ group of patients, that is, those who would most benefit from a CTO (Reference GellerGeller 2013; Reference MustafaMustafa 2015a). However, the profile of the patients in the trials matches closely those on CTOs across countries (Reference Burns, Rugkåsa and MolodynskiBurns 2013; Reference Rugkåsa, Vazquez Montes and BennettRugkåsa 2015). According to Reference Heun, Dave and RowlandsHeun and colleagues (2016), and we would agree, given the current evidence base the onus should now be on proponents of CTOs to identify, with some scientific rigor, which subgroup would benefit.
Are we measuring the right outcomes?
It is argued that CTOs might have benefits for patients that do not show up in research focused on rates of hospital admission. For example, length of time in hospital is suggested as a better reflection of a patient's condition than admission rates. However, there is a worry that, where clinicians are under pressure to reduce the use of beds, shorter time in hospital could reflect bed shortage and/or great faith in the CTO regime rather than clinical improvement in the patient.
Hospital admission is commonly used in the general psychiatric literature as an indicator of relapse (Reference BurnsBurns 2007). Admissions have the advantage that they are likely to be consistent within individual services and, crucially, can be determined accurately from medical records. Even so, measurement of a wider range of clinical and social outcomes, including outcomes defined by patients themselves, has also been advocated. Done well, and separating features of the CTO process from its outcome, this could add to the evidence base. However, it is difficult to conceive of improvements for patients that would not also show up in reduced admission rates.
Should CTO evidence be measured against the hierarchy of evidence?
Several commentators have stated that, given some methodological limitations to the three RCTs, their evidence should be dismissed altogether in favour of results from UBAs and CBAs showing some positive results of CTOs (Reference MustafaMustafa 2015b). The dangers of relying on non-randomised methods are, however, illustrated by two studies from Valencia, Spain, conducted by the same team of researchers. Both were 2-year follow-ups of the same sample, but they reported contrasting results: the UBA study found positive hospital admission outcomes (Reference Castells-Aulet, Hernández-Viadel and Asensio-PascualCastells-Aulet 2013), whereas the CBA study (conducted to overcome the methodological weakness of the UBA) found no difference in admissions between CTO patients and matched controls (Reference Castells-Aulet, Hernández-Viadel and Jiménez-MartosCastells-Aulet 2015).
Issues of attrition, protocol violations and crossovers are undoubtedly limitations of the RCTs (as with most pragmatic trials). However, it is highly unlikely that all of the RCTs and meta-analyses would have resulted in false-negative findings (Reference Heun, Dave and RowlandsHeun 2016). Given the exceptionally clear nature of these findings, reservations do not give cause for concern in the way they would have if the results had been approaching statistical significance (Reference SzmuklerSzmukler 2015).
Should we give up on RCT-level evidence?
Some suggest that CTO implementation is so dependent on its context that evidence from one place cannot be generalised to another and that quasi-experimental and naturalistic studies represent the best way to assess effectiveness of such complex interventions (Reference Swanson and SwartzSwanson 2014). We would argue the opposite. Context-dependent factors, including preferential access to services such as case management and assertive community treatment for patients on CTOs (interventions that have solid evidence bases on their own), make it essential to isolate any independent effect of CTOs from the effects of these other interventions (Reference BurnsBurns 2014). It is hard to see how this could be achieved without randomisation.
Is it coercion or good care that has effect?
Improved outcomes are, by and large, observed only when patients also receive additional intensive services (Reference Morrissey, Desmarais and DominoMorrissey 2014), so cannot be confidently attributed to the CTO. In all three RCTs, patients in both arms were given case management. In the US trials, this represented an addition to standard care, and clinical improvements were observed in the whole sample (CTOs and controls). Improvements were not found in the English trial, where case management was standard care for both the CTO and the control groups before and during the trial. This would suggest that it is the enhanced services that have effect, not coercion.
What is the way forward regarding CTOs?
Very similar legislation for CTOs has been introduced across many jurisdictions. Reference Sjöström, Zetterberg and MarkströmSjöström and colleagues (2011) suggest that, when CTOs were introduced in the absence of good evidence, decision-making appeared ‘to rest upon a paradoxical mix of accepting medical expertise and relying on gut feeling’. The evidence base is much more substantive, and clear, now than when CTOs were first developed, but even so, the intuitive ‘logic’ of CTOs – if you compel patients to engage in treatment they get better – seems hard to shake off.
Where improvements are observed, it seems to be a result of good clinical follow-up, not coercion. This is crucial for service development. Whether in contexts where intensive services are provided routinely (such as in the UK and Australia), or where such services may be contingent on CTOs (such as in some states in the USA), policy makers need to know that it is the services, not coercion, that help patients. A lack of investment in community services cannot be compensated for by increased reliance on CTOs.
The evidence that CTOs do not have the effect assumed in their stated purposes is now strong. This makes the continued use of CTOs problematic for a number of reasons, including:
-
• clinically – the intervention does not have the intended effect of reducing hospital admissions and improving patients’ clinical condition
-
• ethically – restricting patients’ autonomy when they gain no clinical benefit from it is difficult to justify
-
• legally – clinicians are obliged to use the least restrictive alternative
-
• economically – the time and costs associated with the administration of CTOs might be better spent on patient care (Reference Heun, Dave and RowlandsHeun 2016)
-
• professionally – it is unedifying for psychiatrists to be observed continuing with an ineffective intervention in the face of the evidence.
Calls for a reappraisal of CTO practice have been made by clinicians and researchers (Reference KiselyKisely 2015; Reference DawsonDawson 2016; Reference Heun, Dave and RowlandsHeun 2016), by the Parliamentary Committee evaluating the 2007 changes to the Mental Health Act (House of Commons Health Committee 2013) and, most recently, by the Mental Health Taskforce (2016). It has also been suggested that CTOs should only be used for patients who chose them in a form of advanced directive (Reference SzmuklerSzmukler 2015). At the same time, clinicians are faced with a constant pressure to reduce bed use, differing opinions within multidisciplinary mental health teams, and the views of outside agencies (social services, housing services, etc.) and family members. The solution in the UK setting, where receipt of other services does not hinge on the CTO, should be simple, however: continue as before CTOs were introduced – it is just as effective.
Conclusions
Across the industrialised world, CTOs seems to be the favoured mechanism to ensure that care is delivered to non-adherent psychosis patients outside of hospital. Despite differences in legal frameworks and rationales, CTOs oblige patients to adhere to treatment plans. A large number of non-randomised outcome studies show discrepant results. Even if we disregard methodological weaknesses, the discrepancies are striking, with some reporting benefits where many others report none. On the other hand, all analyses of randomised data find no benefit to CTOs, with the exception in one study of a reduced likelihood of falling victim to crime. No other clinical or social benefits have been identified. We believe that this gives serious cause for concern and that the time is ripe to think alternatively about how we seek to help those whose lives are made exceptionally difficult by severe mental illness.
MCQs
Select the single best option for each question stem
-
1 Why have CTOs been introduced into legislation in about 75 jurisdictions worldwide?
-
a They have been shown to be effective and to benefit patients
-
b They give better results than treating patients voluntarily
-
c Services are increasingly expected to be delivered in the community
-
d They represent better value for money
-
e They improve the therapeutic alliance.
-
-
2 What is not among the criteria for placing a patient on a CTO in England and Wales?
-
a It is necessary for the person's health or safety that he/she receives treatment
-
b Without being on a CTO the patient may not obtain housing from the local authority
-
c The patient is not adherent and is likely to relapse rapidly without medication
-
d During relapse the patient may be a threat to other people
-
e Treatment can continue in the community without the person being detained in hospital.
-
-
3 Which of the following does not characterise the typical patient on a CTO?
-
a A diagnosis of schizophrenia
-
b Aged between 35 and 50
-
c Lack of insight
-
d In unskilled employment
-
e Long history of repeated admissions.
-
-
4 What methodology to investigate CTO effectiveness can best support evidence-based practice?
-
a Observing the effect on your patients or your colleagues’ patients
-
b Comparing patients’ outcomes before and after being on a CTO
-
c Randomising patients to be on a CTO or not and comparing outcomes
-
d Listening to the views of patients and their families
-
e Finding matched controls to patients on a CTO and comparing outcomes over time.
-
-
5 Which of the following outcomes is the only one shown to be affected by CTOs in research strong enough to indicate causality?
-
a Readmission to hospital
-
b Duration of admission
-
c Use of community services
-
d Improved adherence to medication
-
e Being a victim of crime.
-
MCQ answers

| 1 | c | 2 | b | 3 | d | 4 | c | 5 | e |





eLetters
No eLetters have been published for this article.