Early-stage obesity is evident in children of preschool age(1, Reference Blair, Thompson and Black2) and many obese children and adolescents already show signs of metabolic change(Reference Cali and Caprio3). Furthermore, in New Zealand, the prevalence of overweight and obesity defined by BMI is significantly higher in Māori (40 %) and Pacific (60 %) children compared with their European counterparts (24 %)(1). Higher rates are also found in more deprived areas(1, 4), and in girls, compared with boys, from 10 years of age(1, 4). Early-onset obesity, exacerbated by these disparities, is believed to contribute to the diabetes epidemic(Reference Foster, Linder and Baranowski5), and to a potential decline in population life expectancy(Reference Olshansky, Passaro and Hershow6).
The Waikato region of New Zealand comprises 7·9 % of the country's land mass, has higher levels of deprivation and a higher proportion of Māori children than the national average(7). The Waikato District Health Board provides health care in the middle of the North Island of New Zealand to a total population of 360 000, including over 77 000 between 0 and 14 years old. The birth cohort is approximately 5600 per annum, which includes 40·9 % Māori and 48·5 % New Zealand Europeans(Reference Craig, Anderson and Jackson8).
In 2004, following a recommendation of the Child Health Advisory Group (ChildWATCH), the Waikato District Health Board invested in the development and implementation of an evaluated school-based intervention called Project Energize. Project Energize was contracted to the Regional Sports Trust (Sport Waikato) as a through-school programme to improve childhood obesity and cardiovascular risk factors in primary school children. The intervention was delivered by ‘Energizers’ employed by Sport Waikato(9), who each supported between eight and ten schools. Each Energizer worked with their schools to improve the health of their students by facilitating within-school changes and accessing regional initiatives to improve children's physical activity and nutrition.
The 2004–2006 trial was designed to compare changes in blood pressure (BP) and body composition in children who attended Energize schools with children in control schools(Reference Graham, Appleton and Rush10). The trial also aimed to identify predictors of increase in body fat and BP over 2 years in relation to age, sex, ethnicity, rurality and social deprivation.
Methods
Project Energize is a programme that aims to improve child health, through a range of school-based interventions and a full description of the methodology has been published elsewhere(Reference Graham, Appleton and Rush10). Briefly, the initial evaluation of the project was of a longitudinal design from 2004 to 2006, with schools (n 124) randomised with stratification by rurality and socio-economic status (SES) as either a control (n 62) or to receive the intervention (n 62). The evaluation sampled children who were 5 or 10 years of age, before programme commencement. The evaluation was approved by the Waikato (now Northern Y) Ethics Committee and both the usual carer and the child provided signed informed consent before any measurements were made. The present study was conducted according to the guidelines laid down in the Declaration of Helsinki. The trial was registered in the Australasian Clinical Trials Registry ACTRN12610000132044.
Physical measurements
In each of the last quarters of 2004 and 2006, height (portable height scale PE087; Mentone Education Centre, Victoria, Australia) and weight (portable electronic scale TIHD316; Wedderburn, Auckland, New Zealand) were measured to ± 0·5 cm and ± 0·5 kg, respectively. Bioelectrical impedance analysis (ImpediMed Single Frequency 50 Hz Bioimpedance Analyser, Imp-DF50; Impedimed, Brisbane, QLD, Australia) and resting BP (Omron Auto Blood Pressure monitor T8; Omron Healthcare, Kyoto, Japan) were measured to ± 5·0 Ω and ± 10 mmHg. All measures were recorded twice, and a third measure was taken where the pre-defined criterion detailed above was exceeded. Exact age was recorded as the difference between date of birth and date of measurement. The measurement teams were trained in all measurements and blind to the allocation of the school at baseline and follow-up.
Percentage of body fat (%BF) was calculated from impedance data, using equations previously established for New Zealand children of similar age and ethnic grouping(Reference Rush, Puniani and Valencia11) and BMI was calculated as kg/m2. BMI standard deviation score (SDS) was calculated using the British 1990 reference population(Reference Cole, Freeman and Preece12), %BF SDS using the McCarthy–Cole fat centiles(Reference McCarthy, Cole and Fry13) and BP SDS using the Jackson BP centiles(Reference Jackson, Thalange and Cole14), determined from representative surveys from Great Britain. Age- and sex-specific SDS allows comparisons to be made between intervention and control children without further adjustment. The British reference values were used due to a substantial portion of New Zealand people, including Māori having some British ancestry and because there are no comparable New Zealand tables. Cole criteria were used to define overweight and obesity(Reference Cole, Flegal and Nicholls15).
Ethnicity was recorded from parental reports and SES calculated via the use of school deciles, which were obtained from a national register(16). A scale from 1 to 10 was used; 1 being linked to the lowest 10 % of affluence and 10 with the highest 10 %.
Project Energize was underpinned by a number of essential elements, such as reducing the inequalities among ethnic groups, SES, sex and geography(17). The project was aligned with national and regional activities.
Intervention components
Sport Waikato was contracted by the Waikato District Health Board to deliver Project Energize. ‘Team Energize’ are either teachers or graduates in the fields of exercise and nutrition, or physical education, employed by Sport Waikato to support the delivery and development of the programme in each intervention school. Each of the eleven Team Energize staff (‘Energizers’) were allocated between six and eight schools each, by the team manager. At induction and throughout the 2 years, the ‘Energizers’ undertook combined training as a group in order to share experience, resources and skills. The philosophy adopted was that Team Energize act as agents of change, not as additional teaching staff. For example, Team Energize staff might have ‘modelled’ classes and support the usual class teacher. Classes modelled included fundamental movement skill training, ideas for ‘huff and puff’ fitness activities, modified games, and ball activities and sport-related games, where keeping children moving as much as possible throughout each session was the focus. Teachers requested and were provided with ideas for management and control of children during physical activity sessions. Energizers promoted active transport, lunchtime games, bike days and leadership training for students to be leaders of physical activities before and after school.
Energizers were also available to assist each school with a range of healthy-eating initiatives. These included canteen makeovers to remove pastry-based pies and ‘big cookies’ and add filled rolls, fruit and low-fat yogurt. Healthy fund raising was promoted with sales of water, milk, soup, bread rolls, fruit and non-food items instead of chocolate, sweets, sausages and sugary drinks. Support was also given to class teachers (by the Energizer) in the form of curriculum-based material, which provided information on the benefits of replacing of sugary drinks with water and milk, the importance of eating breakfast, and modelling the preparation of healthy lunches and snacks on a budget.
Nutrition ‘nuggets’ were also provided every week in the school newsletter. These included a series of thirty smart swaps (e.g. replacing instant noodles with baked beans, potato crisps with popcorn), lunch box makeovers to include sandwiches and fruit, and what are ‘everyday, sometimes and occasional’ foods. There was also a home–school link programme that provided opportunities for parents to attend three information-based sessions, which included a 45 min practical nutrition class. During the same weeks, all classes in the school received integrated nutrition lessons. Fridge magnets and laminated cards that reinforced the nutrition goals were provided to all children, and they were encouraged to put these on their fridges at home.
In addition to school children, the project offered assistance to teachers, parents and the local community. This was implemented through a range of activities, such as professional development and evenings with a dietitian to raise parents' awareness of healthier choices of food. Activities also targeted the local community through events such as gala open days and edible gardens. Control schools were given no additional resourcing or information; however, no restrictions were placed on initiatives they may have pursued for themselves.
Each school involved in the project worked with their Energizer to develop an individualised action plan based on the individual needs of the school. A Memorandum of Agreement fully described the delegated responsibilities of both the schools and Sport Waikato and that the school would participate in evaluation of the Project goals.
Statistics
Statistical analysis was undertaken using the JMP Statistical Discovery Software version 5.1 (SAS Institute, Inc., Cary, NC, USA), SAS version 9.1 (SAS Institute, Inc.), and StatsDirect version 2.5.7 (StatsDirect Limited, Altrincham Cheshire, UK). All data were analysed separately as either 5 or 10 years old. Results are presented as means and standard deviations. Between-group differences in anthropometric measurements were assessed by unpaired two-tailed t tests and analysed within sex and ethnicity. ANCOVA was used to evaluate changes in each age sample-standardised body composition (BMI and %BF SDS and BP scores) at 2 years, with adjustment for corresponding baseline values, programme group, rurality and school decile group. Deciles ranging from 1 to 5 were coded as 0, and those from 6 to 10 coded as 1. The data were clustered by school. Multivariate models were examined for interactions between intervention, rurality, ethnicity and sex using ANOVA.
Results
Complete measurements for those who did not change school, and for whom time between measurements was more than 23 months were available for 1352 children, 926 were 5–7 years old and 426 were 10–12 years old (692 interventions and 660 controls; 895 Europeans, 349 Māori, 108 other; 686 boys, 666 girls), time between measurements averaged 742 (sd 24, range 694–817) days, 742 (sd 23, range 697–810) days for the intervention schools and 743 (sd 25, range 694–817) days for the control schools. Table 1 shows the numbers and proportions by demography of the intervention and control children who were measured in 2004 and 2006. The prevalence of overweight and obesity did not substantially change between 2004 and 2006.
Table 1 Proportions (%) of children measured by demography and obesity classification at baseline and after intervention
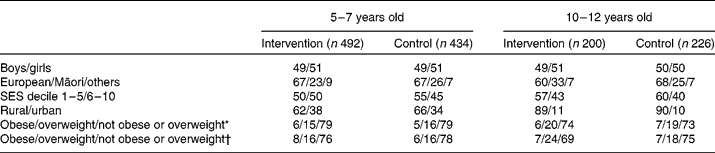
SES, socio-economic status.
* At baseline.
† After intervention(Reference Cole, Bellizzi and Flegal35).
The intervention and control groups in both samples had higher BMI SDS and %BF SDS than the reference populations and 12-year-olds had a higher score than 7-year-olds (Table 2). Systolic BP SDS in 7-year-olds was lower than the reference population and that of the 12-year-olds. Diastolic BP SDS in both samples was higher than the reference.
Table 2 Change in outcome variables in the 2-year intervention (intervention relative to control)
(Probability values and 95 % confidence intervals)
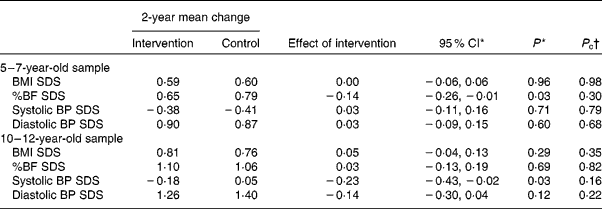
SDS, standard deviation score; %BF, percentage of body fat; BP, blood pressure.
* Adjusted for baseline measure, rurality and school decile (including interaction).
† P value corrected for the clustering of children by school.
The intervention was associated with a favourable outcome (slower gain in BP) for the 10–12-year sample for systolic BP SDS and to a lesser extent diastolic BP SDS. Percentage of BF SDS was also improved for the 5–7-year sample. When clustering by school was taken into account, the CI were widened (and the P value increased).
Subgroup analysis within age group by sex, ethnicity and Cole criteria showed similar patterns of change, with the largest effect of the intervention on %BF SDS in 7-year-old Europeans and on systolic and diastolic BP SDS in boys and 12-year-old Europeans (Table 3). Over 2 years, Māori children compared with Europeans had a non-significantly greater increase in BMI, %BF and BP than Europeans. Although there was a differential effect on BMI or systolic BP among normal weight, overweight and obese children, %BF was reduced significantly among normal-weight 7-year-olds and non-significantly (P = 0·07) among obese at age 12 years. The increase in diastolic BP was lower among overweight and obese at 7 years in the intervention group.
Table 3 Differences in outcome variables in the 2-year intervention (intervention relative to control, adjusted for confounding variables)
(Probability values and 95 % confidence intervals)

SDS, standard deviation score; %BF, percentage of body fat; BP, blood pressure.
* Adjusted for baseline measure, rurality and school decile (including interaction).
† P value corrected for the clustering of children by school.
The potential environmental confounders of SES (decile) and rurality were explored further. In relation to the change in %BF SDS in 7-year-olds, the intervention had a more favourable, but not statistically significant, effect in rural schools and schools of higher SES. These findings, while not statistically significant, could be important from a public health perspective. The outcome of interest in the 12-year-olds of the change in systolic BP SDS was non-significantly lower in rural children than urban (P = 0·08) and the intervention was marginally more effective in high-decile children compared with low-decile children (P = 0·09).
Discussion
This is the largest and most comprehensive through-school intervention for New Zealand children of mixed ethnicity from a large geographical area. Over 2 years, this evaluation of the effectiveness of Project Energize in 5–7 and 10–12-year-old children has shown that there is a trend for a reduced rate of rise in systolic BP and accumulation of body fat in children attending schools that received the intervention. Confounding has been reduced because the evaluation was of a randomised controlled trial but within subgroups, interpretation is limited because of the complexity of the demography of the schools. School size varied widely so the data were analysed with and without clustering, widening the CI but not changing the direction or mean population effect. Baseline measures, SES and geographical location were adjusted for in the main analysis. Subgroup analysis showed differences in response to intervention by age group, sex, ethnicity, body fat and interactions. The complexity of interpreting these findings also shows clearly the complexity of tackling the problem and the difficulty of objective measures of effectiveness in the short term. Evidence for favourable changes in anthropometry in other school-based interventions is accumulating(Reference Foster, Linder and Baranowski5, Reference Hollar, Lombardo and Lopez-Mitnik18–Reference Van Cauwenberghe, Maes and Spittaels20).
The changes observed in this evaluation took place over a short time period and, like similar findings relating to the temporal increase in BMI SDS(Reference Lazarus, Wake and Hesketh21), may translate into large differences in terms of population health as time progresses. In growing children, the proportion of fat may decrease and muscle increase without a change in BMI(Reference Singhal and Misra22), limiting the ability to infer that a change in BMI is a change in adiposity. We show that the increase in %BF was lower in 5–7-year-olds attending the intervention compared with the control schools, which may mean that there was increased muscle. Over 2 years, body size, body fat and BP have increased at a faster rate in our population and particularly in the Māori children than in the reference populations. However, in the long term, the small reduction in the trajectory of accrual of body fat and increase BP may play an important role in predicting future health outcomes of these children. The finding that there were no significant effects for change in BMI SDS and %BF SDS by treatment or ethnicity in the 10–12-year sample could be explained by this age group entering a life-stage that is not associated with an increasing prevalence of obesity(Reference Kimm, Glynn and Kriska23). Furthermore, in girls, increased body fat is associated with earlier pubertal changes and increased CVD risk factors(Reference Remsberg, Demerath and Schubert24), and Māori girls experience menses earlier than Europeans(25).
Some school-based interventions to reduce obesity have also been associated with improvements in BP(Reference Hollar, Messiah and Lopez-Mitnik26) and reductions in various indices of adiposity in those above the 85th centile(Reference Foster, Linder and Baranowski5), and we also found trends in improvement in %BF among overweight/obese children. Improvements associated with prevention programmes may provide some protection against chronic disease in the long term. A conceptual model(Reference Montani, Antic and Yang27) is that obesity, hypertension and cardiovascular risk are entwined in an amplification loop, each aggravating the effect of the other. This model does imply that an intervention positively having an impact on any one of the three elements is likely to have a significant impact on the presence and effect of the other elements, by disrupting the amplification loop.
Differences in risk factor patterns by sex and ethnicity in this intervention were also found, which supports studies undertaken elsewhere(Reference Hollar, Lombardo and Lopez-Mitnik18, Reference Hollar, Messiah and Lopez-Mitnik26, Reference Luepker, Perry and McKinlay28, Reference Webber, Osganian and Feldman29). Patterns of growth varied among ethnic groups. For the first time in New Zealand, the present longitudinal study has shown Māori children attending a primary school show, over 2 years, a tendency for greater increases in relative body size, body fat and BP than their European counterparts. Māori children are over-represented in the lower SES schools. This is important evidence to inform the focus and design of future school-based interventions aimed at New Zealand youth.
The strengths of the present study are its longitudinal design, school-based randomisation with matching of schools by size, rurality and decile, sample size (n 1352) and robust measures of body size, %BF and BP measured 2 years apart. It was also well controlled (with or without clustering, there was no bias in terms of intervention v. control) and the intervention programme was inclusive of the whole school and wider community (teachers and parents). Retention, while challenging, due to the mobile nature of the community (with children moving between the present out of programme and control schools, particularly older children moving to non-Energize intermediate schools) was reasonably successful overall when considering these constraints (see below). While this reduced the number of children available for repeated measurements, we restricted the analysis to only those children who had repeated measures available, and who had been in either a programme or control school for the duration. Children of differing ages and ethnicities were also considered, which adds to the study's complexity and as the study continues, its potential for additional impact cannot be ignored. The programme is cost-effective, the main costs are the salaries of the Energizers and team leader and the travel required to move between schools. We calculate that the average cost of the intervention for each child, each year, is less than $40 New Zealand and this could be improved by further efficiencies.
Worth noting are some of the study's limitations. As we wanted to include specific subsets of children, particularly Māori, issues relating to over- and under-sampling bias cannot be avoided. The initial response was from 50 % of those invited. At 2 years later, 20 % of the younger children and 43 % of the older children were lost to follow up; the higher rate for the older children because many had moved on to high school. We intentionally sampled from schools by SES, and hence ethnicity, but attrition over time could not be avoided. Consequently, absolute numbers, particularly for Māori, fell below that required for significance. While the evaluation measurements were undertaken 2 years from the commencement of the intervention, the nature of the intervention process meant that it was able to be implemented only in a graduated way, reflecting the characteristics and capacities of individual schools. This led to a shorter duration of intervention implementation before endpoint measurements for lower-decile schools, where a higher proportion of Māori children attend. This, along with the relatively low absolute numbers of Māori children enrolled in the evaluation and subsequent lack of power, may account for the lack of demonstrated effect for Māori in subgroup analysis.
Direct measures of changes in activity levels and dietary habits were not made due to budget and time restraints. However, a ‘household questionnaire’ was answered by 618 carers (46 %) of the children in the present study and no important changes or differences between control and intervention were seen in their basic food pattern over time(30). Changes in schools were measured by a school stocktake(30), and it indicated that the Project was having an impact on the programme school environment and staff in terms of portion sizes of pies and cookies sold and availability of healthier options such as sandwiches and fresh fruit. Of the sixty-two intervention schools, fifty-six did report, however, that there had been a change in the children's knowledge of healthy eating and physical activity.
Children's behaviours outside of the school environment could also not be accounted for and we must acknowledge that the present study may not be truly representative of all children in all schools in the Waikato region of New Zealand. Control schools were not limited in any other initiatives that they may have wanted to undertake and at that time, the nationwide Healthy Eating Healthy Action Strategy with the ‘Mission On’ initiative targeted at young New Zealanders was introduced(Reference McLean, Hoek and Buckley31). This initiative was supported by social marketing, monitored food regulations and supplied fruit to low-SES schools. This awareness is likely to have affected the response of control schools in the school stocktake. Such external uncontrolled initiatives, unable to be controlled for in our evaluation, potentially reduce the discernable effect of Project Energize. Yet, despite these shortcomings, it is worth noting that the positive changes in the right direction for BP and %BF SDS still took place in the schools that received, in addition, the services of an Energizer to help them plan, implement and drive new initiatives. There are tremendous forces at play in an obesogenic environment(Reference Swinburn and Egger32) and (if demonstrated to be sustained in the longer term) any beneficial change in such an environment is laudable.
Conclusion
Project Energize supports studies elsewhere(Reference Hollar, Lombardo and Lopez-Mitnik18, Reference Hollar, Messiah and Lopez-Mitnik19, Reference Hollar, Messiah and Lopez-Mitnik26, Reference Taylor, McAuley and Barbezat33, Reference Taylor, McAuley and Barbezat34) that schools are important arenas to implement health promotion strategies to prevent overweight and obesity. Although this intervention programme, at best, has shown minor improvements in the health outcomes over 2 years, its potential long-term benefits cannot be ignored. Its continued implementation and exposure to other schools should also be explored.
Acknowledgements
E. R. contributed to the study conception and design, acquisition of the data, interpretation of the data, critical revision, drafting of the manuscript. P. R. contributed to the analysis and interpretation of the data, critical revision, approval of the final draft for submission. S. M. contributed to the study conception and design, acquisition of the data, critical revision, approval of the final draft for submission. T. C. contributed to the interpretation of the data, critical revision, approval of the final draft for submission. D. S. contributed to the study conception and design, interpretation of the data, critical revision, approval of the final draft for submission. D. G. contributed to the study conception and design, acquisition of the data, interpretation of the data, critical revision, approval of the final draft for submission. The authors report no conflicts of interest. The Waikato District Health Board funds the Project Energize programme and its evaluation. The Ministry of Health, New Zealand has contributed to evaluation funding.





