- BAPEN
British Association for Parenteral and Enteral Nutrition
- DH
Department of Health
- ‘MUST’
‘Malnutrition Universal Screening Tool’
- NHS
National Health Service
The magnitude and distribution of malnutrition and their relevance to policies
Malnutrition remains an under-recognised and under-treated clinical and public health problem, with adverse clinical and financial consequences. In 2007, it was estimated that the public expenditure on disease-related malnutrition in the UK was in excess of £13×109(Reference Elia, Stratton, Elia and Russell1), corresponding to about 10% of the expenditure on health and social care. Most of the malnutrition exists in the community. In 2007 at a given point in time, it was estimated that about 98% of the malnutrition (affecting over 3 million subjects in the UK, according to Malnutrition Universal Screening Tool (‘MUST’) criteria of medium+high risk of malnutrition) occurred outside the hospital environment, 5% in care homes and the remainder in the community (2–3% in sheltered housing)(Reference Elia and Russell2).
Policies in hospitals
Although only about 2% of malnutrition in the UK is found in hospitals, many of the policies to combat malnutrition have tended to focus on the hospital environment. This is because policies in a relatively small number of institutions are generally easier to establish, monitor and inspect than in a large number of institutions or homecare. It is noteworthy that in the UK there are at least 10-fold fewer hospitals than care homes. Thus several reports on malnutrition, such as the 2003 Council of Europe Resolution on malnutrition(3), the 2003 report from Quality Improvement Scotland on Food, Fluid and Nutritional Care(4), and the 2009 report from the Republic of Ireland(5), have focused only on hospitals. One of the most consistent recommendations is to screen patients on admission to hospital, so that malnutrition does not go unrecognised and untreated.
There are other reasons why policies for detection and treatment of malnutrition have focused on the hospital environment. One of these is that hospital care is expensive, accounting for up to about 40% of total estimated public expenditure on malnutrition in health and social care(Reference Elia, Stratton and Russell6), and so policies that reduce the demand for expensive hospital stays would be welcomed. Another reason is that there is a perception that most of the malnutrition originates in hospital and the food provided there. In fact, most malnutrition originates in the community and it is the single most important reason for its presence in hospital(Reference Russell and Elia7). However, although only about one in 50 malnourished subjects is found in hospital, the flux of patients through hospitals is much greater than that through care homes and sheltered housing in combination, despite there being 6-fold fewer subjects in hospitals (approximately 200 000 hospital beds in the UK in 2007). To put this into perspective, consider the UK as a whole, which has a population of about 60 million. The number of hospital admissions in 2007 was estimated to be over 12 million (Department of Health Statistics England, Scotland, Northern Ireland and Wales) and, since about 28% of these admissions(Reference Russell and Elia8, Reference Russell and Elia9) (approximately 3·4 million) are thought to involve subjects at risk of malnutrition, an important opportunity exists to identify and treat malnutrition (although this may involve the same patient more than once). In this way, treatment initiated in hospital may continue in the community. If malnutrition is not identified, clinically effective and cost-effective treatments may be denied to patients both in hospital and after discharge from hospital. Similar considerations can be applied to hospital outpatients. In 2007 there were about 63 million outpatient attendances in UK(Reference Elia, Stratton, Elia and Russell1), with an estimated prevalence of malnutrition of 10% or more (16–20% according to recent studies involving the use of ‘MUST’ in surgical, medical, gastrointestinal and other outpatient clinics)(Reference Rust, Cawood and Stratton10–Reference Collins, Stratton and Kurukulaaratchy12). Despite these considerations, policies to screen for malnutrition in hospital outpatient clinics are generally less prevalent than in hospital wards. Policies for both inpatients and outpatients are important from both a clinical and a public health perspective.
Policies in care homes
There are also policies to identify and treat malnutrition in care homes. In England, standard 8.9 of the National Minimum Standards for Care Homes for Older People states(13): ‘Nutritional screening is undertaken on admission and subsequently on a periodic basis, a record maintained of nutrition including weight gain or loss, and appropriate action taken.’ The same standard is used in Wales (where it is referred to as standard 15.9)(14). In Scotland the ‘National Care Standards for older people in care homes’ requires that patients’ nutritional state is regularly assessed and reviewed (standard 14.6)(15). Thus, standard 14.6 states: ‘You can be confident that the provider is aware of your nutritional state and will, with your agreement, arrange for this to be regularly assessed and reviewed. This assessment will take account of any changes in your health.’ The standard is used by the Care Commission when inspecting care homes to ensure that they comply with the Regulation of Care Act 2001 (Scotland). In Northern Ireland, the first of ten standards for nurses (‘Get your 10 a day!’(16)) concerns nutritional screening: ‘All patients admitted to hospital are screened for risk of malnutrition (this standard, along with the nine other standards, are intended for use in all inpatient facilities in Health and Social Care Trusts).’
Appropriate regulation and inspection of care homes can be difficult, not least because the number of registered care homes is large. In England alone, on 31 March 2007, there were 18 577 care homes with 441 958 places(17). How does one ensure appropriate and uniform standards? How does one implement appropriate education and training in nutrition to various types of staff working in care homes, when currently there are no agreed educational reference standards? What roles should e-learning modules play and how should these be recognised, approved and coordinated? Recent e-learning modules include those produced by the Core Learning Unit (of the Department of Health (DH)) or organisations such as the British Association for Parenteral and Enteral Nutrition (BAPEN; BAPEN's interactive e-learning module on nutritional screening for healthcare in the community (expected to be released in 2010 to complement the existing e-learning module for hospital workers)). There is a need to consider the role of such modules in an overarching educational policy across healthcare workers. One such policy has been proposed by National Health Service (NHS) Scotland(18) with the ‘MUST’ framework as a central theme.
Policies in the community
The difficulties in establishing and enforcing policies on nutrition in the community, especially for free-living individuals, are also substantial and in many respects greater than those in sheltered housing, care homes and hospitals. This is partly because affected individuals may not seek advice about their health until their malnutrition becomes severe and partly because affected individuals may be difficult to contact since they are widely dispersed in the community, often living in small family units or even alone. Government policies in recent years have tended to shift care from hospitals and care homes to the community. For example, the number of hospital beds has been progressively decreasing, and the number of people financially supported in care homes (England) has fallen by 24 400 (9%) in the 4 years since March 2003(17). This means that the needs of those remaining in care homes are greater. Older people move into care homes later in life when their needs have become greater. In the meantime, much responsibility is to be placed on individuals and families (informal carers) who report that they receive insufficient support. This raises a number of questions. For example, does patient–carer involvement represent a beneficial and/or desirable change or shrugging off of statutory responsibility? How can appropriate education and training in prevention and treatment of malnutrition be delivered to those involved in home care, including patients and informal carers? The need for informal carers has been emphasised by the government in its report Carers at the heart of 21st-century families and communities (19). The charity Carers UK estimated that in the UK there are 6 million informal carers (10% of the general population), who provide support worth £87×109 per year(20). The DH has made a commitment to make available £4·7×106 per year to train, empower and enable carers (face-to-face training and distance learning)(21), as part of its programme of Caring with Confidence. This is a good start, but the funding is inadequate to deal properly with the major task at hand. BAPEN's report Combating Malnutrition: Recommendations for Action (Reference Elia and Russell2) draws attention to the need for much more education and training of carers involved in nutritional care.
The system of nutritional care in the community has a number of shortcomings. For example, the first of a three-tier system in Operational Plans (2008/9–2010/11) (22) proposed by the DH (England) concerns mandatory national requirements. The second tier relates to national priorities. At a local level, Primary Care Trusts produce plans for agreement and sign-off by their Strategic Health Authority. However, malnutrition does not feature in either of these two tiers. The third tier concerns choice, prioritisation and enforcement of healthcare activities by the Primary Care Trust in consultation with local partners. Nutritional care should feature prominently in this tier but it seems likely that it will do so only patchily unless considerable effort is put into improving awareness and practice, along the lines suggested by patient–carer representatives(Reference Elia and Smith23) and healthcare professionals(Reference Elia and Russell2, 24). There is a need for commissioners and providers of healthcare to appreciate the prevalence of malnutrition, its causes and consequences and the importance of nutritional care, so that appropriate nutritional support can escalate up the priority ladder. Incentivisation schemes exist within hospital and community services to encourage provision of high-quality care. Examples involving Commissioning for Quality and Innovation in hospital include schemes aiming to reduce the incidence of pressure ulcers and Clostridium difficile infection, to improve the care of inpatients with diabetes and to improve the responsiveness to personal needs of patients and patient-reported outcomes, such as those associated with knee replacements and hernia operations. Examples of the Quality and Outcomes Framework in the community include indicators aiming to improve clinical care in patients with CHD, hypertension diabetics, obesity and hypertension, standards or records, and information and patient experience. However, none appear to have been used to specifically improve nutritional care in primary or secondary care. Thus, commissioners are not holding providers to account for delivering high-quality nutritional care. There is a lack of commissioning guidelines on nutritional care and a lack of awareness of needs of different patient populations(Reference Elia and Russell2). Policies to address these issues would be welcomed, especially since plans to address the economic downturn in the next period aim to save £15–20×109 during 2011–2014 through improved efficiency in an integrated scheme of care that is closer to home(25).
Need to establish accurate and reliable information
Prevalence of malnutrition and malnutrition-related mortality in English and Scottish hospitals
In order to formulate appropriate policies on malnutrition it is important to have an appreciation of the magnitude of the problem, in both clinical and financial terms. Following ministerial questions in the House of Commons (in 2008 and in the first quarter of 2009), the government released figures on the prevalence of malnutrition on admission and discharge from hospital and on the incidence of malnutrition-related deaths in English hospitals. Fig. 1 shows a 2-fold increase in the number of admission and discharge episodes of malnutrition between 1997–1998 and 2007–2008. These results, based on Hospital Episode Statistics(26), used a combination of codes from the International Classification of Diseases (ICD-10 codes(27)) to identify ‘malnutrition’ (E40–E46 and O25: kwashiorkor, nutritional marasmus, marasmic kwashiorkor, unspecified severe protein-energy malnutrition, protein-energy malnutrition of moderate and mild degrees, retarded development following protein-energy malnutrition, unspecified protein malnutrition and malnutrition in pregnancy). A separate DH release in response to further ministerial questions in the House of Commons indicated a continued growth in the number of reported admission and discharge episodes of malnutrition (3377 and 4392, respectively, when 5-month data for the period April–August 2008 are extrapolated to the whole year). In addition to malnutrition, the DH also provided data on the prevalence of nutritional anaemias and other nutritional deficiencies, with similar general trends, although the absolute numbers are very different. Table 1 shows the data for the year 2007/08. When the data are combined and presented as a single combined entity, there is confusion as to what they really represent. The media raised concerns about the 2-fold increase in the prevalence of malnutrition on admission and discharge from hospital over the 10-year period, as well as criticisms about the way the National Health Service has been handling the malnutrition problem. An editorial in the British Medical Journal used such data to fuel these concerns(Reference Lean and Wiseman28).

Fig. 1. Number of malnutrition admission (•) and discharge episodes (○) in National Health Service hospitals between 1997–8 and 2007–8 (from Hospital Episode Statistics, The NHS Information Centre for health and social care). The results are for annual periods starting from the year indicated.
Table 1. Admission and discharge episodes of malnutrition, nutritional anaemias and other deficienciesFootnote *
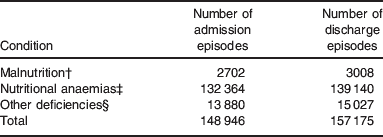
* Hospital Episode Statistics, The National Health Service Information Centre for health and social care.
† See text for codes used to define malnutrition.
‡ Fe deficiency anaemias (D50), vitamin B12 deficiency anaemias (D51), folate deficiency anaemias (D52) and other nutritional anaemias (D53).
§ Deficiencies of vitamin A (E50) thiamin (E51), niacin (E52), other group B vitamins (E53), ascorbic acid (E54), other vitamin deficiencies (E56) as well as dietary deficiencies of Ca (E58), Se (E59), other nutritional elements (E61) and other nutritional deficiencies (E63).
However, all the above actions are probably unjustified and potentially misleading because the statistics are grossly inadequate for reasons detailed below. BAPEN's two Nutrition Screening Week Surveys undertaken in 2007(Reference Russell and Elia8) and 2008(Reference Russell and Elia9), both of which involved the collection of data based on ‘MUST’(Reference Elia29), found that 28% of patients were at risk of malnutrition on admission to hospital, and most of these (78%) were at high risk of malnutrition, requiring active treatment. Given that there are over 10 million admissions to English hospitals each year (10·7 million admissions in 2006–2007(30)), it is estimated, as a first-order approximation, that about 3 million of these would have been malnourished or at risk of malnutrition. The estimated prevalence of malnutrition based on DH statistics is not only less than 1% of the BAPEN estimate, but also implausible for other reasons. For example, a secondary analysis of DH data for the year 2006–2007 by one of the authors (M.E.) revealed no reports of malnutrition in 77 of 279 trusts (28%) on admission and about 38% among those trusts (n 205) that responded to this question, which is inconceivable. Similarly, on discharge from hospital, no malnutrition was identified in 74 of 279 trusts (27%) and about 35% among those trusts that responded to this question (n 211). These results are not robust and are consistent with a lack of awareness about malnutrition among registrants. Indeed it can be argued that the 2-fold increase in prevalence of malnutrition over time may simply reflect an increase in awareness of the problem and improved documentation, especially since this has been the goal of many organisations and agencies including the DH. The media response to such data included criticisms of the NHS and of the DH statistics on malnutrition-related mortality (see later). Unreliable figures that grossly underestimate the true prevalence of malnutrition are of no help when formulating national policies. In contrast, data on representative samples that use the same consistent criteria to identify and monitor the effects of interventions on malnutrition would be much more useful.
A second set of statistics released by the government on 1 April 2009 revealed a diagnosis of malnutrition on the death certificates of 242 patients who died in English NHS hospitals in 2007 (this being the highest of 11 annual figures between 1997 and 2007, which ranged from 169 to 242, with an average of 210 per year)(31). The results are shown in Fig. 2. From 1997 the diagnoses on the death certificates were defined using ICD-9 codes(32) (260–269 (malnutrition) and E904.1 (effects of hunger)) and from 2001 they were defined using ICD-10 codes(27) (E40–E46 (malnutrition) and T73.0 (effects of hunger)), which means that the number of deaths from each cause before 2001 are not entirely comparable with those obtained after 2001. Deaths were included when one of these conditions was mentioned anywhere on the death certificate. This included anything that contributed towards the death, and this did not necessarily mean that it led to death directly (e.g. mild or moderate protein-energy malnutrition (E44) would qualify). However, the prevalence of malnutrition among those dying in hospital is likely to have been 2–3 orders of magnitude higher. According to the Office of National Statistics(33) the annual death rate in England and Wales between 2004 and 2007 ranged from 504 052 to 514 250 (93–94% occurring in England and 6–7% in Wales). Since about 50–55% of deaths at all ages occur in NHS hospitals(34), it can be calculated that about 0·25 million people die in NHS hospitals each year, in agreement with estimates based on Hospital Episode Statistics. For example, for the year 1999–2000, 253 799 deaths were identified in English hospitals(Reference Dixon, Shaw and Frankel35), a figure that is probably an underestimate because it did not include newborns, people who died before being formally admitted to hospital and some long-term patients who were probably admitted before the study period. Nevertheless, these considerations are sufficient to show that only about 0·1% of patients dying in hospital had a diagnosis of malnutrition on their death certificates. This seems unrealistic since inpatient prevalence of malnutrition is probably over 30%(Reference Russell and Elia8, Reference Russell and Elia9) and malnutrition contributes to morbidity and mortality in many different ways(Reference Stratton, Green and Elia36). Thus, if it is assumed that malnutrition is present in a third of the patients dying in hospital each year (about 0·25 million total deaths), then malnutrition would have affected about 83 000 of these. This last figure is likely to be an underestimate for at least three reasons: people who die tend to be older (85% of deaths in English hospitals have been reported to occur in those aged >65 years and 55% in those aged ≥75 years(Reference Dixon, Shaw and Frankel35)), and older patients are more likely to be malnourished than the average patient(Reference Russell and Elia8, Reference Russell and Elia9); the ward prevalence of malnutrition (point prevalence) tends to be higher than the admission prevalence, mainly because those without malnutrition are discharged more quickly, leaving a greater proportion of malnourished individuals on the wards; and the presence of malnutrition predisposes to death(Reference Stratton, Green and Elia36), which means that those that die are more likely to be malnourished. Therefore, a tentative annual figure of up to 100 000 hospital deaths in association with malnutrition (disease-related malnutrition) can be proposed. Although there is a difference between dying directly from malnutrition and dying with malnutrition, neither the government nor BAPEN data have distinguished between the two, and it may be difficult to do so since malnutrition is both a cause and consequence of disease and vice versa. The case mix in this respect may differ substantially between registrations on death certificates and registrations in the BAPEN national surveys(Reference Russell and Elia8, Reference Russell and Elia9), but the contrast between the number of deaths associated with the former (200–250) and the latter (about 100 000) is so striking that a number of potential explanations should be considered. These include lack of awareness about malnutrition, inconsistencies in registration of malnutrition on death certificates and use of an inadequate reporting system.

Fig. 2. Number of malnutrition-related deaths in hospitals of England between 1997 and 2007. The results are for registered deaths in each calendar year.
Following questions about malnutrition in the Scottish Parliament, the National Statistician (UK Statistics Authority) provided information on the prevalence of malnutrition on discharge from acute hospitals in Scotland and the incidence of malnutrition-related mortality in acute hospitals. Issues raised earlier about the accuracy of the results in England also apply to Scottish statistics(37, Reference MacDonnel38).
To avoid confusion and unnecessary criticisms of the NHS, it seems important to collect information on malnutrition in a more complete and systematic way. Such a system can also be used to assess the effectiveness of interventions. Current efforts by the DH to introduce the ‘MUST’ into a new NHS software system within the National Programme for IT in England could facilitate such a process. The use of a large number of different coding systems to define malnutrition, both within and between care settings, is not practical or particularly helpful in routine clinical practice.
Nutrition-related patient safety incidents
The National Patient Safety Agency reports on the number of nutrition-related safety incidents. A safety incident is ‘any unintended or unexpected incident which could have or did lead to harm for one or more patients receiving NHS care’. Examples include failure to undertake screening, failure to provide a special diet or provision of an incorrect nutritional treatment. The number of nutrition-related safety incidents in NHS hospitals was reported to increase from 15 473 in 2005 to 29 138 in 2007 (88% increase)(Reference Elia and Russell2). It is easy to reach incorrect conclusions by ascribing the rising incidence to deteriorating nutritional care. However, this explanation may be erroneous because the increasing number of reported patient safety incidents may have resulted from increased awareness about malnutrition, partly as a consequence of policies that have actively encouraged NHS staff to report such incidents. There may have also been a wider range of the types of incidents reported (change in case mix) since the remit of the National Patient Safety Agency for nutritional care appears to have widened to include incidents from identification of malnutrition through nutritional screening to implementation of appropriate care plans and follow-up and missed meals. It would therefore be valuable to evaluate critically the results to prevent unnecessary criticisms of the NHS.
Regulation and inspection
As the watchdog for hospital care in England, the Healthcare Commission, now incorporated into the Care Quality Commission, has been undertaking surveys on nutritional care of hospitalised patients. For example, for the years 2006 and 2007 it reported that 20% of patients did not get enough help from staff to enable them to eat their meals. These results were based on a patient survey(Reference Elia and Russell2). However, a separate survey involving self-assessment by NHS staff revealed a different picture, which is of some concern. The Commission inspects hospitals against two core standards on nutrition, one of which is standard C15b (‘Where food is provided healthcare organisations have systems in place to ensure that patients’ individual nutrition, personal and clinical dietary requirements are met, including the necessary help with feeding and access to food 24 hours a day’). Only 1·5% of Trusts reported a failure to meet this core standard and insufficient assurance was given in only another 1·6%(Reference Elia and Russell2). These results are so discordant from those obtained from the patient survey that questions arise about the validity of the answers. In 2009, Baroness Barbara Young, the first chair of the Care Quality Commission, admitted on BBC radio that the system she inherited from the Healthcare Commission to assess the performance of hospitals was ‘too simplistic’(Reference Hawkes39). Baroness Young also announced that she planned to stand down as chair of the Commission and she did so in February 2010. In the next period, it seems reasonable to assess critically the value of surveys and procedures used to regulate and inspect healthcare providers, especially since nutritional issues are expected to be become more prominent(40).
Integration of national nutrition policies
The healthcare systems of the four devolved nations (England, Scotland, Northern Ireland and Wales) have diverted. Therefore, national plans in one country do not necessarily reflect those of the other countries. Here, only a brief mention will be made of the Nutrition Action Plan for England(41), which spans all care settings. This policy has five main aims:
1. To raise awareness of the link between nutrition and good health and that malnutrition can be prevented.
2. To ensure accessible guidance is available across all sectors and that relevant guidance is appropriate and user-friendly.
3. To encourage nutritional screening for all people using health and social care services, paying particular attention to those groups that are known to be vulnerable.
4. To encourage provision and access to relevant training from front-line staff and managers on the importance of nutrition for good health and nutritional care.
5. To clarify standards and strengthen inspection and regulation.
It was recognised at the outset that appropriate implementation of this policy would not occur spontaneously, and so a Delivery Board was set up with five subcommittees, each addressing one of the five priority areas listed above. The Delivery Board, which was set up early in 2008, comprised multidisciplinary group of individuals, including senior DH officials involved in health and social care, experts (and also members of non-governmental organisations) with a special interest in nutritional care in health and social care and a patient representative. Targets were set and progress reports were sent to ministers. However, the achievements of the Delivery Board are difficult to evaluate. Nevertheless, interactions between different members of the DH, working with a multi-disciplinary professional workforce with interests in different care settings, as well as individuals involved in the prevention and treatment of disease, including a patient–carer representative, led to a greater understanding and appreciation of the breadth of nutrition in clinical care and public health, a greater appreciation of the problems faced by different groups of individuals, and how joined up thinking can help establish a more effective operational infrastructure. Some of the work of the Delivery Board can be illustrated using one or two examples associated with the activities of the Nutrition Screening Subcommittee, which has linked its actions to other national initiatives. The Nutrition Screening Week, organised and led by BAPEN, not only received support from the governments of England and Scotland, the Welsh assembly, and the Chief Nursing Officer for Northern Ireland, it was also actively promoted by a number of other agencies. In addition, the results were used by the DH to promote its policies. These activities coincided with the production of fact sheets by the National Patient Safety Agency, one of which focused on Nutritional Screening(42). It used an integrated approach (promoting use of the same screening tool (‘MUST’ as an example) across different care settings), as recommended by the Delivery Board, and the Malnutrition Action Group of BAPEN and by the Combating malnutrition Report(Reference Elia and Russell2). These activities include the development of software by the DH (Connecting for Health) to incorporate ‘MUST’ into new software designed for widespread use in the NHS, and the development of an e-learning programme on nutritional screening using ‘MUST’ in hospital (shortly to be followed by a module for healthcare workers in the community) by BAPEN and Greater Glasgow and Clyde NHS Trust partnership. These activities, which were on the Delivery Board's agenda, would probably have occurred anyway, but perhaps more slowly and in a less integrated, interactive manner and with less overall impact. Proposals have been put forward to continue the implementation process, which includes partnerships between governmental and non-governmental organisations to ensure appropriate delivery chains are established, as suggested in previous reports on nutritional care(Reference Elia and Russell2, 24). However, the government, whilst acknowledging the valuable work and the recommendations of the Delivery Board, which it planned to implement, also disbanded it at the end of February 2010. This has left a number of concerns about provision of a co-ordinated care service between and within settings and about the interface between clinical and public health nutrition.
In summary, since malnutrition is a common, costly and largely treatable condition (for evidence see extensive review by Stratton, Green & Elia(Reference Stratton, Green and Elia36) and the accompanying paper which focuses on oral nutrition supplements(Reference Stratton and Elia43)), it is imperative that there is a national policy to ensure that it is detected and treated appropriately and that it becomes embedded in routine practice. To help achieve this it is necessary to ensure appropriate education and training of all key healthcare professionals involved in the management of malnutrition and an integrated, accurate system for recording and auditing the management of this condition.
Acknowledgements
C. A. R. is an independent nutrition advisor and was Chair of BAPEN Nutrition Screening Week. M. E. and R. J. S. are affiliated to the University of Southampton (R. J. S. also works at Nutricia Ltd). The authors declare that there is no conflict of interest. M. E. drafted the paper and C. A. R. and R. J. S. discussed it and modified it.





