273 results
Mental health research in South America: Psychiatrists and psychiatry trainees’ perceived resources and barriers
- Rodrigo Ramalho, Vanessa Chappe, Lisette Alvarez, Gianfranco C.A. Argomedo-Ramos, Guillermo Rivera Arroyo, Graciela L. Bonay, Javiera C. Libuy Mena, Miguel A. Cuellar Hoppe, Domenica N. Cevallos-Robalino, Jairo M. Gonzalez-Diaz
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 10 / 2023
- Published online by Cambridge University Press:
- 02 October 2023, e66
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
As mental health issues continue to rise in Latin America, the need for research in this field becomes increasingly pressing. This study aimed to explore the perceived barriers and resources for research and publications among psychiatrists and psychiatry trainees from nine Spanish-speaking countries in South America. Data was collected through an anonymous online survey and analyzed using descriptive methods and the SPSS Statistical package. In total, 214 responses were analyzed. Among the participating psychiatrists, 61.8% reported having led a research project and 74.7% of them reported having led an academic publication. As for the psychiatry trainees, 26% reported having conducted research and 41.5% reported having published or attempted to publish an academic paper. When available, having access to research training, protected research time and mentorship opportunities were significant resources for research. Further support is needed in terms of funding, training, protected research time and mentorship opportunities. However, despite their efforts to participate in the global mental health discussion, Latin American psychiatrists and psychiatry trainees remain largely underrepresented in the literature.
Water footprint of representative agricultural crops on volcanic islands: the case of the Canary Islands
- Noelia Cruz-Pérez, Juan C. Santamarta, Carlos Álvarez-Acosta
-
- Journal:
- Renewable Agriculture and Food Systems / Volume 38 / 2023
- Published online by Cambridge University Press:
- 04 August 2023, e36
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The Canary Islands are a Spanish archipelago, where the greatest water demand comes from agriculture. Being an outermost European region that receives a large number of tourists per year, the need for greater food sovereignty becomes more important. It is vital to undertake studies on the water footprint (WF) of the main crops, in order to identify the irrigation practices of local farmers and establish recommendations for water saving through improvement of these practices. The results of this study show that the average WF for bananas in the Canary Islands is 340.80 m3 t−1 ± 34.07 and for avocadoes is 1741.94 m3 t−1 ± 286.16. The WF models proposed can explain 92 and 86% of the total variance of the WF for banana and avocado crops, respectively. The WF of both crops can be reduced, and this work can be a starting point for improvement. Farmers will face a change in temperature and water availability due to climate change; useful water saving strategies for local farmers can now be made based on estimation of the WF with yield and net needs data.
Proinflammatory activation profile in circulating monocytes in patients with a major depressive episode
- L. Grendas, R. Alvarez Casiani, A. Arena, M. Penna, F. Hunter, A. Olaviaga, C. Prokopez, V. Tifner, A. Armesto, A. Carrera Silva, A. Errasti, F. Daray
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S993-S994
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mood Disorder (MD) affects more than 300 million people globally, and its etiology is unknown. In recently published data, MD has been correlated with inflammation and the immune system. Circulating monocytes have been proposed to play a role in the pathophysiology of depression.
ObjectivesTo determine if there is a specific activation profile of monocytes in patients with MD that differentiates them from healthy control (HC).
MethodsStudy Design: Case-control study matched by sex and age. The study was approved by IRB and carried out in three hospitals in Argentina.Participants between 18 and 55 years old from both genders, were evaluated by psychiatrists using the International Psychiatry Interview (MINI) to diagnose Mood Disorder (MD), and the Hamilton Depression Rating Scale (HADRS) to define active disease (AD), non-active disease (NAD) or healthy control (HC). The three monocyte subtypes were directly stained and analyzed in a drop of 100 uL of blood sample based on our validated monocyte cocktail including CD11b, HLA-DR, CD86, CD14 and CD16 expression by flow cytometry. To define normality Kolmogorov-Smirnov test was employed. A parametric T-test with Welch´s correction was employed for normal distribution and a non-parametric Mann Whitney test was used when comparing populations that do not pass the normality test.
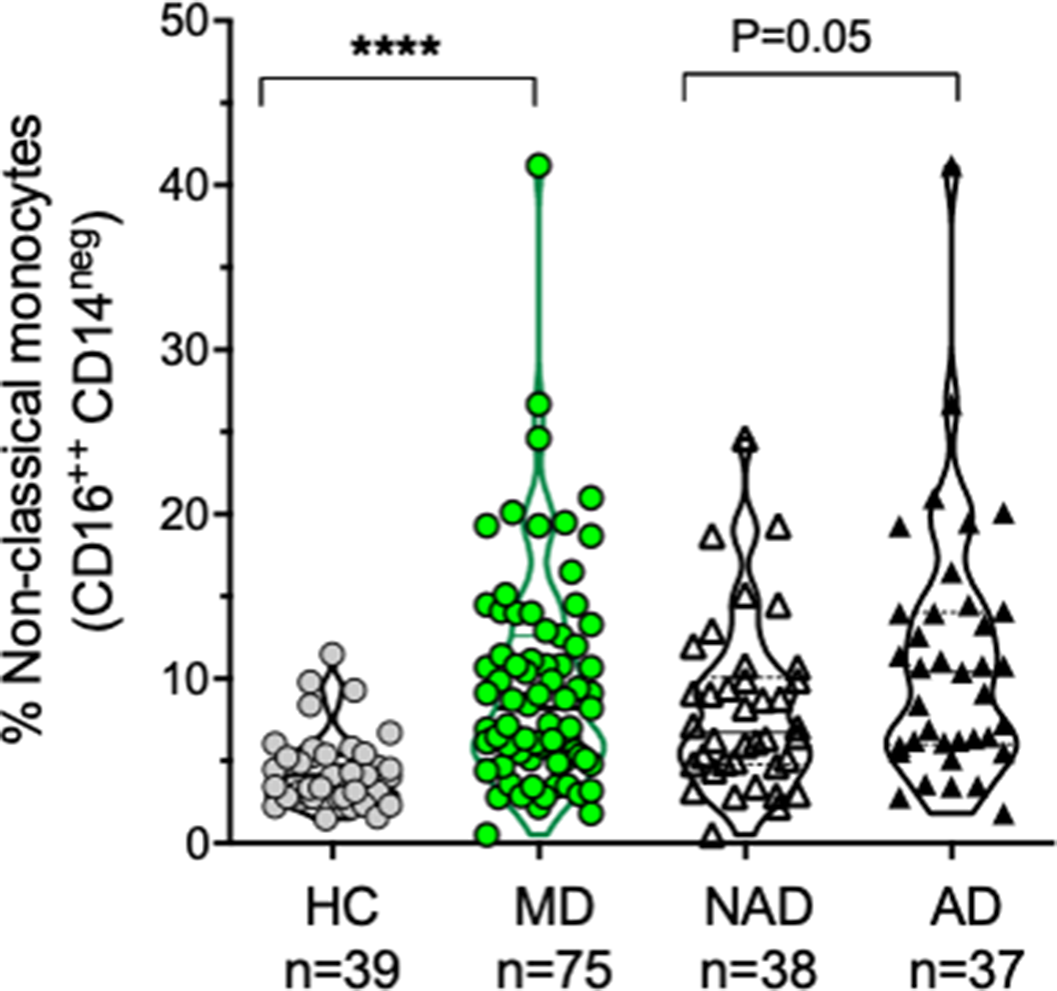
ResultsThe sample characteristics were shown in Table 1. Patients with AD (Hamilton >7) (n: 37), patients with NAD (Hamilton <7) (n: 38), and HC (n: 39) were recruited. The percentage of classical monocytes decreased in AD vs NAD (p=0.04), both AD, and NAD have significantly lower levels of classical monocytes than HC (****p<0.001) (Image 1). The percentage of intermediate monocytes is higher in AD vs NAD (p=0.05), both AD, and NAD have significantly higher levels of intermediate monocytes than HC (****p<0.001) (Image 2). The percentage of non-classical monocytes is higher in AD vs NAD (p=0.05), both AD, and NAD have significantly higher levels of non-classical monocytes than HC (****p<0.001) (Image 3).
Table 1. General characteristics of the sample
Active disease Non-active disease Healty control n 37 38 39 Age (SD) 42.95 (11.78) 42 (12.02) 40.67 (11.42) Women (%) 76.3 64.9 76.9 BD I 15.8 54.1 0.0 BD II 26.3 5.4 0.0 BD (non specified) 0.0 2.7 0.0 MDD 57.9 37.8 0.0 HAM-D 17 items mean (SD) 14.13 (4.89) 3.11 (2.35) 0.49 (0.85) Image:
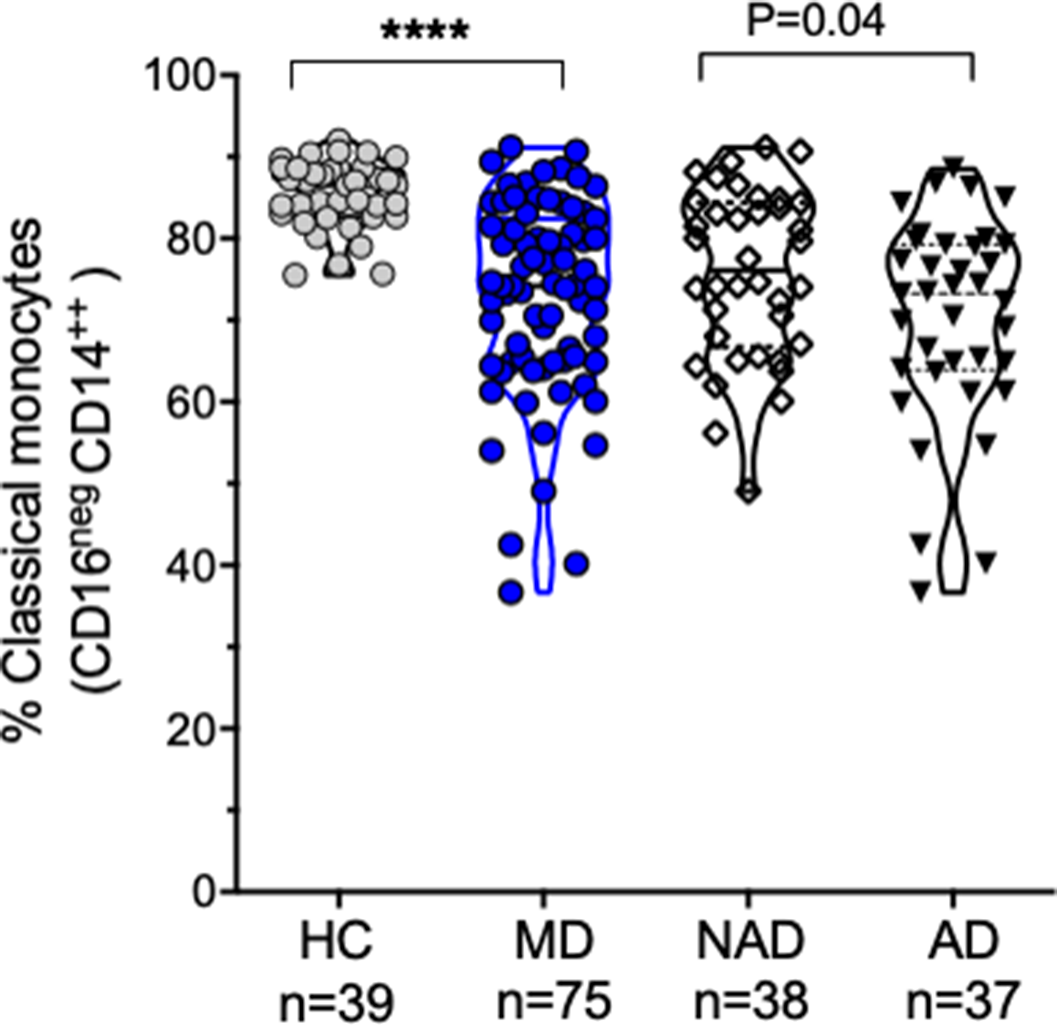
Image 2:
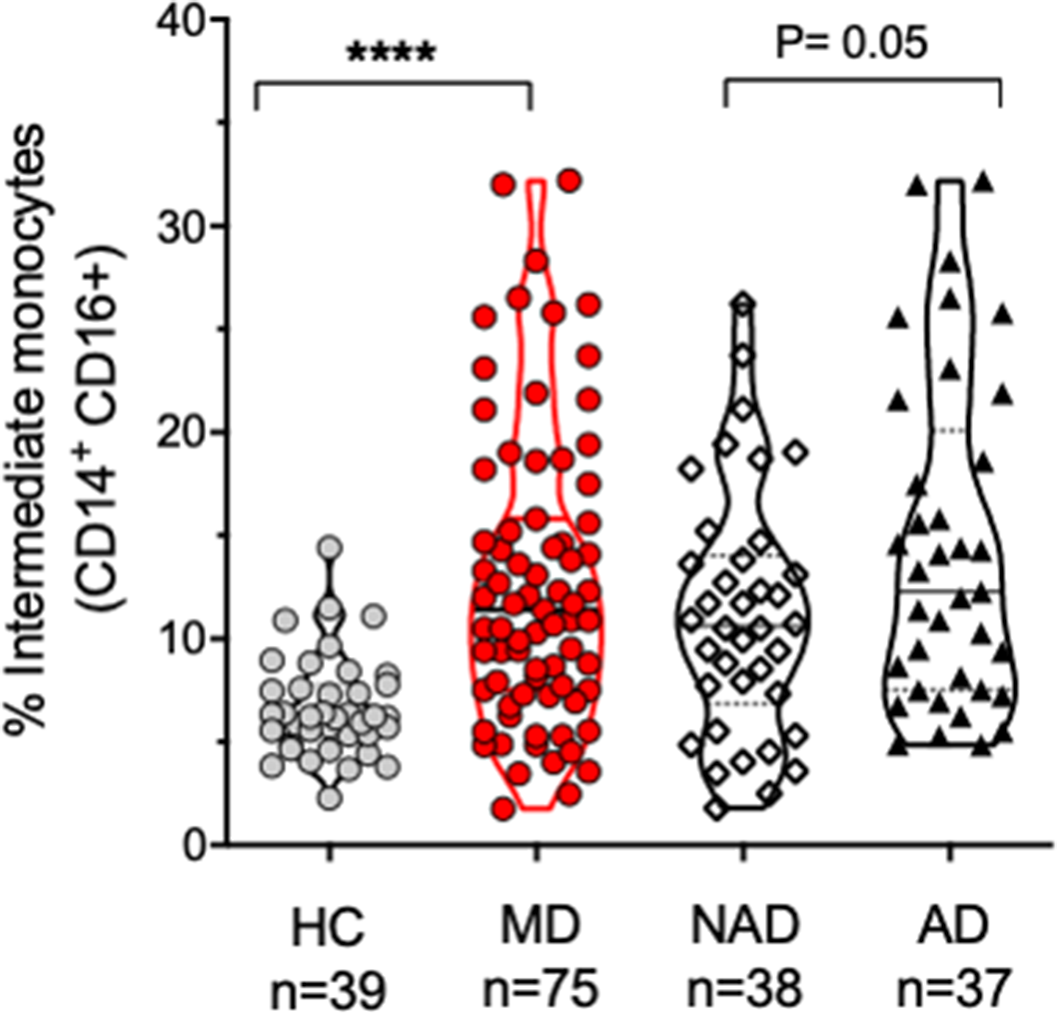
Image 3:
 Conclusions
ConclusionsWhile comparing percentages of three different monocyte subsets, clear differences in their distribution among the control and patient groups were appreciated. After comparing the subset frequencies between active patients (AD) and patients who were in remission (NAD), significant differences among the subsets were found although without reaching values of the HC, indicating that even patients in remission show an activated monocyte profile.
Disclosure of InterestNone Declared
Clinical characteristics and functional improvement of patients admitted to a Child and Adolescent Autism Spectrum Disorders (ASD) Day Therapeutic Unit
- A. Alvarez, N. Santamaria, V. Bote, C. Lamborena, R. Medina, J. A. Monreal, B. Sanchez, A. Hervas
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S713
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The ASD Day Therapeutic Unit of the HUMT is an interdisciplinary reference center specialized in ASD, for the care of children and adolescents with this pathology, that offers care by programs with the aim of achieving functionality altered.
ObjectivesThe main objective of this study is to know the clinical characteristics of the patients admitted to our center and to offer preliminary data on the functional improvement achieved in a pilot program that works by processes.
MethodsThis is a prospective clinical study of patients with ASD, treated at the ASD Day Therapeutic Unit of the Hospital Universitario Mutua Terrassa (HUMT), since februay 2022 till nowadays. We compare the clinical improvement and functionality acquired through the evaluation through various scales: Conners scale, SRS, BRIEF and CBCL.
ResultsOur sample is made up of 19 patients with ASD who are admitted to the HUMT ASD Day Hospital. 13 belonged to the intensive care program, 5 to recovery of low-functioning functionality, and 1 to the differential diagnosis program. 84.21% (n=16) have preserved cognitive capacity. The median age is 13.1 years. 73.7% of the sample are men.
We observed that 89% of patients admitted to our unit presented comorbid symptoms with ADHD. more than 78.9% present isolation, anxiety/depression, altered thinking and attention difficulties. 13/19 present a SEVERE RANGE of affectation upon admission, in social area. Facing discharge, the CBCL shows us a general improvement in behavior and comorbidity in the total scale. The SRS shows us an improvement in social awareness, social communication, social motivation, repetitive behavior and stereotypes and in the total score.
ConclusionsSpecific interventions in social skills, autonomy, social understanding, daily routines, and sensory integration in patients with ASD improve core symptoms, as well as associated behavior.
Specific interventions and working on social relationships during admission improve comorbidity derived from ASD.
More studies are needed to specify the most efficient interventions to improve the quality of life in children and teenagers with ASD.
Disclosure of InterestNone Declared
Biomarkers and clinical predictors of long-term course in obsessivecompulsive disorder: A prospective cohort study
- S. López-Rodriguez, P. Alonso Ortega, C. Segalàs Cosi, E. Real Barrero, S. Bertolín Triquell, C. Soriano Mas, Á. Carracedo Alvarez, J. M. Menchón Magriña
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S231
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The purpose of the research project is to analyze the long-term evolution of obsessive-compulsive disorder (OCD) from of a study of a cohort of patients prospectively followed over a period ranging from 5 to 20 years, treated for according to therapeutic guidelines mediating serotonin reuptake inhibitors (IRS) and drug enhancers (antipsychotics) and cognitive behavioral therapy and evaluated in a standardized manner.
ObjectivesTo assess the long-term course of Obsessive-Compulsive Disorder (OCD) in a cohort of patients treated according to current clinical guidelines; to analyse possible prognostic factors associated with the long-term course of the disorder including clinical and sociodemographic variables, as well as genetic and neuroimaging biomarkers, and their interaction, and finally to study neuroanatomical and functional cerebral connectivity changes after 15 years of treatment in a subsample of patients.
MethodsProspective, descriptive, and observational study of a cohort of OCD patients, receiving treatment at the Department of Psychiatry of Hospital de Bellvitge since 1998, according to a standardized protocol. Follow-up period ranges from 5 (n=423), to 10 (n= 247) and 15 years (123). Baseline clinical and sociodemographic assessment, long-term evolution and information on treatments provided are available for the whole sample. Data on whole exome sequencing is available for 300 of the patients included in the cohort and baseline structural neuroimaging and cerebral functional connectivity has been analysed in 168 subjects. To expand the analysis of genetic biomarkers, we propose the study of de novo variants through exome analysis of 50 trios (patient and both parents) selected among those subjects that have reached 15 years of follow-up (25 trios with patients within the “long-term remission” group and 25 trios with patients with chronic OCD). De novo variants detected in the trio analysis will be replicated in the rest of the sample. A structural and resting state MRI will be obtained in a subsample of 100 patients recruited among those who have completed a minimum follow-up period of 15 years, to assess cerebral changes associated with the long-term course of the disorder.
Resultsin the current moment the recruitment period of the study has ended and all the data is being statistically analysed in order to provide solid results in a short period of time.
ConclusionsThe identification of those factors associated with an increased risk of chronic disease is an element essential to offer personalized treatment to our patients and improve their prognosis, emphasizing the intensive use of those therapeutic strategies for which we can predict a better response and modifying to the extent of, if possible, environmental factors or factors of access to treatment that contribute to perpetuate obsessive symptoms.
Disclosure of InterestNone Declared
TRANVIA: A program for continuum mental health assistance in transition period
- L. Pérez Gómez, A. González Álvarez, M. A. Reyes Cortina, E. Lanza Quintana, N. Álvarez Alvargonzález, C. Rodríguez Turiel, E. Lago Machado, J. J. Martínez Jambrina
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S728
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Transition between adolescence and adulthood represents the most important challenge for personal development and involves several transformations: physical, psychological and social. It is a complex age bracket, concurring the transition from youth psychiatric units to adult ones, with an increased risk for the appearance of mental disorders and risky behaviours. TRANVIA program, developed in Avilés, provides psychiatric assistance to patients between 15 and 25 years old, diagnosed with a severe psychiatric disorder or with an increased risk of having one.
ObjectivesOur objectives are: ensuring clinical continuity assistance, promoting communication among professionals and the empowerment of our patients to improve their functionality and quality of life.
MethodsDescriptive study including patients involved in TRANVIA program from November 2019 to November 2021.
ResultsDuring this two-years period there have been 44 referrals to the program, 11 of them were rejected for failure to comply with diagnostic criteria. In November 2021 there were 33 patients included in the TRANVIA program with an average age of 17 years old (range: 15-22). 70% of them were men and 30% women. All of them had psychiatric assistance from different sources: youth mental health units, neuropediatrics… About 75% of the patients were diagnosed with autistic spectrum disorder and approximately three-quarters of the sample needed pharmacological treatment. Risperidone was the most prescribed drug. We have also developed other assistance alternatives as home-based care, relaxation sessions, social worker interventions and coordination with schools.
ConclusionsTRANVIA program has allowed us to provide continual attention to vulnerable patients that shift from youth psychiatric units to adult ones. Patients that meet inclusion criteria were enrolled independently the type of assistance they have previously received. Accessibility and flexibility were our priority. During the described period there was only one dropout, three patients required psychiatric hospitalization and two others visited the emergency department. There have been no cases of completed suicide.
Disclosure of InterestNone Declared
An interesting clinical case. New therapies in Dissociative Identity Disorder.
- P. García Vázquez, E. Seijo Zazo, C. Vilellla Martin, A. Serrano García, C. M. Franch Pato, E. Martína Gil, C. Alvarez Vazquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S970-S971
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dissociative identity disorder (DID) also referred as multiple personality disorder is a chronic post-traumatic condition. It is characterized according to DSM-5 by “disruption of identity characterized by two or more distinct personality states”, with “marked discontinuity in sense of self… accompanied by related alterations in affect, behavior, consciousness, memory, perception, cognition, and/or sensory-motor functioning.”
ObjectivesHere, we present a case of a 33-year-old Caucasian female with no psychiatric history until 2 years ago, privately. The patient is admitted to the Psychiatry Service due to worsening. During admission, consultations are made to the Neurology Service and the Neurophysiology Service, who request an electroencephalogram, an MRI and a brain scan, resulting in normality.
After discharge, she returns home with her parents, and the crisis become more frequent and of longer duration. She acknowledges that during these periods she is dominated by her alternate personality, which she is unaware of until her family informs her. This personality is a demon, who verbally assaults and even physically threatens her surroundings, and can hardly be controlled by the prayers of her family.
MethodsDespite psychopharmacological treatment, as well as the cognitive-behavioral therapy carried out by the patient for more than two years, there was no improvement. Once she comes to the consultation, it is decided to carry out a therapy guided by the central Rogerian attitudes, originating a process of empathic resonance of the therapist, which influences the experience of the patient. Three main interventions are carried out, the awareness of the disease, the regulation of the intensity of this experience, to maintain the attention and the exploration of what guides the change. After carrying out this intervention, the patient is currently asymptomatic.
ResultsCurrently, there are not evidence-based treatment guidelines. The most common approach is individual psychodynamic psychotherapy according to practice-based guidelines initiated by the International Society for the Study of Trauma and Dissociation.
To handle the present case, we used a model with two pillars, the patient’s commitment and the investigation of microprocesses within a process of experiential exploration, in which the therapist is a facilitator of reflective attention and experimental awareness.
ConclusionsThe torpid evolution suffered by the patient, with little clinical improvement to the interventions carried out, and the absence of evidence on the treatment, led to a therapeutic approach focused on the empathic resonance process of the therapist, with good results.
Disclosure of InterestNone Declared
Sexual dysfunction induced by psychotropic drugs: a narrative review.
- C. Álvarez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1096
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One fairly common side effect of psychopharmaceuticals is sexual dysfunction. They can influence various aspects of sexual function, including lubrication, desire, ejaculation, and orgasmic intensity… This may worsen mental health conditions and make it challenging for patients to adhere to the Treatment. We’ll examine how these drugs affect the area of sexual activity.
ObjectivesTo emphasise how different antipsychotics and antidepressants may affect sexual function.
MethodsWe conducted a narrative review about the available literature on the subject. Articles were selected based on their clinical relevance.
ResultsAll SSRI antidepressants carry a considerable risk of sexual dysfunction. According to some research, escitalopram and paroxetine may pose the greatest risk among this group. Similar risks of sexual issues exist with SNRIs. Bupropion, on the other hand, has a lot of evidence demonstrating low or no risk. Agomelatine, mirtazapine, and moclobemide also have a minor impact on sexual performance.
Hyperprolactinemia has been specifically linked to sexual impairment in antipsychotic medication, hence antipsychotics that cause hyperprolactinemia such as haloperidol, risperidone, paliperidone, and amisulpride are more likely to induce sexual disturbances. Aripiprazole, quetiapine, and ziprasidone have been demonstrated to be less or not connected to sexual dysfunction.
ConclusionsAlthough sexual dysfunction is not an unusual side effect of psychiatric medications, it is frequently underdiagnosed. Sexuality needs to be explored by therapists because it may affect patient’s treatment compliance and well-being. It’s critical to understand how each psychotropic drugs can impair sexual function in order to select the best option based on the individual traits of each person.
Disclosure of InterestNone Declared
Parental Alienation Syndrome (PAS). Psychological and legal implications
- M. Arrieta Pey, S. Rubio Corgo, A. Álvarez Astorga, A. M. Delgado Campos, C. Díaz Gordillo, A. C. Castro Ibáñez, M. Á. Álvarez de Mon González
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S729-S730
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The first definition of PAS, enunciated by Richard Gardner in 1985, refers to a disorder originating in the context of legal conflicts related to child custody. Its main characteristic would be a smear campaign by the child towards a parent, in the absence of plausible arguments. In this context, the child would experience an oppositional and dichotomous feeling towards his or her parents. In recent years, the presence of PAS has become increasingly important, both in the legal and health fields, largely due to the controversy and debate surrounding its approval and recognition, and there is currently no consensus on the matter.
ObjectivesThe main objective of this work is to examine the current state of PAS in depth in the different fields in which it is emerging: the medical-scientific and legal spheres. The current controversies and debate, both scientific and legal, will be developed. Research will be carried out on the origin of the concept and its evolution, its symptomatic presentation, the neuropsychological consequences in minors, the role and legal value of expert reports, as well as the existing evaluation methods for the assessment of PAS.
MethodsAn extensive literature review was carried out on the subject in question, extracting information mainly from scientific articles, but also from legislative documents, manuals and books.
ResultsThere are currently no specific laws regulating PAS in European countries. According to Article 10.2 of the Spanish Constitution, norms related to fundamental rights shall be interpreted according to the Universal Declaration of Human Rights. As a direct consequence of the chronic psychological stresses experienced by children, adaptive disorders may appear, often characterised by symptoms of anxiety and depression. In addition, a multitude of neuropsychological consequences have been observed not only in the affected child, but also in the adult he or she will become.
ConclusionsCurrently, there is a fervent debate about the validity and recognition of PAS as a diagnostic entity, spanning different disciplines, ranging from health to social and legal. In Europe, professionals in the scientific field have not reached an agreement regarding the approval of PAS. On the one hand, there are those for whom PAS is a verified phenomenon; on the other hand, there are those who flatly reject the existence of this phenomenon. The latter consider PAS an unscientific construct, referring to it as “court syndrome” or “patriarchal alienation syndrome”.
Disclosure of InterestNone Declared
Use of paliperidone palmitate half-yearly release in patients diagnosed with psychotic disorder: profile and satisfaction of use
- P. Andres-Olivera, A. Alvarez, M. D. L. A. Garzon, R. Gonzalez, C. Roncero, P. Jesús
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S638
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The lack of insight can be present among patients with a diagnosis of schizophrenia, which often results in lack of adherence to pharmacological treatments1 and, subsequently, in treatment discontinuation and relapses2. This vicious pattern leads to further clinical deterioration, impaired functioning, and reduced quality of life 3. There is a plethora of evidence supporting the fact that long-acting injectable and depot antipsychotics can increase adherence to treatment, reduce the risk of discontinuation and hospital admissions4. It is also known that low fluctuations between peaks and lows in plasma drug levels could be related to a better tolerability profiles5. A new paliperidone palmitate prolonged release formulation, which is administered twice annually, has been approved as maintenance treatment for patients with schizophrenia who are already stable on the monthly or quarterly prolonged release paliperidone palmitate6.
ObjectivesWe aimed to evaluate the transition of monthly and quarterly paliperidone palmitate to the new six-monthly formulation and patients’ satisfaction with it in a real-world clinical setting.
MethodsWe collected a basic epidemiologic questionnaire, responses to a query about local pain after administration, and the Drugs Attitude Inventory (DAI).
ResultsA total of 21 patients from an outpatient clinic for severe mental disorders with a long evolution of their disease in Salamanca, Spain, were included. All of them had a DSM5-TR diagnosis of Schizophrenia. Sixteen were male and 5 female. The mean age was 42.6 years. 14 were receiving quartlery paliperidone palmitate (10 with high doses (525 mg) and 4 with moderate doses (350 mg)) and 7 were on monthly injections (6 with high doses (150 mg) and 1 with a moderate dose (100 mg)). Those receiving moderate doses of quarterly or monthly paliperidone palmitate were administered 700 mg of six-monthly paliperidone palmitate; 1000 mg were injected to those with higher doses. The mean score on the DAI scale was 8. Only one patient reported an increase in local pain after the injection, and another reported dissatisfaction with the administration in the gluteus instead of the deltoid muscle. The first administration of the new formulation in our site was on June 26th; to date none of these patients have required hospital admission due to relapse.
ConclusionsSix-monthly prolonged release paliperidone palmitate seems to be an effective maintenance treatment for schizophrenia. In addition, this new formulation is well received and tolerated by patients previously on monthly or quarterly formulations of the same drug.
Disclosure of InterestNone Declared
Chronic disease (CD) during transition from child to adult.Psychopathological consequences and coping strategies
- S. Rubio Corgo, M. Arrieta Pey, A. M. Matas Ochoa, M. I. Duran Cristobal, E. Perez Vicente, A. Delgado Campos, C. Diaz Gordillo, A. C. Castro Ibañez, A. Alvarez Astorga, P. Alcindor Huelva
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S745
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
CD is characterized by at least three features: its duration is prolonged, it does not resolve spontaneously and it is rarely completely cured. Approximately 10-15% of young people have CD. Adolescents with CD often have emotional and behavioral problems.
ObjectivesTo assess risk factors, derived psychiatric pathologies and coping strategies for a CD diagnosis in adolescence.
MethodsAn extensive literature review was carried out on the subject in question, extracting information mainly from scientific articles, manuals and books.
ResultsThe main risk factors are those related with the CD in question, physical sequelae, the need for long-term hospital admissions or the use of drugs whose side effects include affective or behavioral symptoms; those related to the personality traits of the affected child or adolescent. In addition, as far as the family is concerned, the presence of a low level of education, lack of support or communication, as well as the presence of psychiatric disorders or serious medical conditions in parents. Among the most frequent psychiatric disorders associated with CD are affective and anxiety disorders, adaptive disorders, somatoform disorders, eating disorders and behavioral disorders. Whatever the CD is, it generates high levels of stress and uncertainty in the patient and family, which must be dealt together from a flexible perspective, allowing child or adolescent to adapt to the changes, reorganize and facing them with adaptive patterns of behavior. For this, it will be essential to have adequate social and family support with relational style based on communication, trust and acceptance.
ConclusionsIn general, both adolescents with CD and their families have an adequate capacity to adapt to the repercussions and effects derived from the disease. Nevertheless, in case of possible emotional difficulties that may appear, a comprehensive and individualized approach to these adolescents and their families is necessary to provide them resources and coping strategies in different areas and contexts in which the disease debuts.The comprehensive therapeutic approach will consist of interventions at the individual and family level. Among the main objectives of these interventions are to achieve acceptance and adaptation to CD provinding adequate psychosocial support to enable them to cope with CD in the best possible way and to detect and address the emotional implications, even coexisting psychopathology.
Disclosure of InterestNone Declared
Extrapyramidal syndrome in psychotic depression: a case report.
- C. Álvarez, A. M. Gómez Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1049-S1050
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic depression is a subtype of major depression, with worst prognosis but underdiagnosed and undertreated. We introduce the case of a 75-year-old patient who is attended in the hospital presenting sorrow and behavioral disturbances. He also had delusions of ruin and surveillance through his phone, adding amnesia, dizziness, constipation, tremor and bradykinesia. He had suffered a limited depressive episode regarding his wife’s death.
ObjectivesTo highlight the importance of a correct differential diagnosis in psychotic depression to prescribe an adequate treatment that provides a better outcome for the patient.
MethodsA narrative search of the available literature on the subject through the presentation of a case.
ResultsThe presumptive diagnosis is Parkinson vs psychotic depression. After some weeks of treatment with venlafaxine and olanzapine, the absence of improvement and fluctuating symptoms orientates towards Parkinson. This is later excluded due to a normal DATSCAN. Therefore, the diagnosis of psychotic depression is made, explaining parkinsonism as secondary to psychotropics. Olanzapine and venlafaxine are retired, introducing clozapine because of its lower incidence of extrapyramidal symptoms. After two weeks, the symptoms disappear, recovering the patient his basal functionality.
ConclusionsDepression with psychotic symptoms can take several weeks to respond to treatment, requiring a proper organic screening. In our case, the slow response to treatment made the organic etiology as one of the main differential diagnoses, specifically Parkinson disease. It ruled out because of the absence of findings in the DATSCAN and the resolution of the extrapyramidal symptoms with the change of treatment.
Disclosure of InterestNone Declared
Psychosomatics and mentalization
- A. M. Delgado Campos, P. Alcindor Huelva, A. Alvarez Astorga, S. Rubio Corgo, E. Pérez Vicente, M. Arrieta Pey, C. Diaz Gordillo, P. Del Sol Calderón, A. C. Martín Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1024
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We have investigated the relationship between the Psychosomatic Classification method (Marty) and the Rorschach Test, with respect to the diagnosis of psychosomatic disorders, within the framework of the degree of mentalization measured by both.
ObjectivesA) To verify statistical coincidence with respect to the degree of mentalization (risk of generating psychosomatic disorders in a subject) between the Rorschach Test and the diagnostic technique Psychosomatic Classification, by P. Marty. B) To test the hypothesis: Patients diagnosed with infertility, whose degree of mentalization is good, will have a greater probability of achieving a successful pregnancy throught Assisted Reproduction Techniques.
MethodsTwo evaluation tools were used: a) Psychosomatic Classification based on the criteria established by this diagnostic method; b) The Rorschach test (based on the evaluation of 29 indicators, selected according to their greater relevance in the generation of somatic symptoms).
A sample of 120 patients (women) diagnosed infertility at the Assisted Reproduction Unit (U.R.A.) at Hospital Universitario 12 de Octubre in Madrid was recruited. The method of ‘statistical correlation of coincidence’ between the results of the two diagnostic instruments used was used. Once both tests had been assessed by the “inter-judge” method and the quantitative values of the selected items had been weighted, the KAPPA statistical method was applied to establish the “correlation of coincidence” between the results of the two assessment instruments.
ResultsConsidering that the KAPPA method takes values between “0" and ”1" and that between 0.6 and 0.8 the agreement or coincidence is considered good, and above 0.8 very good, the result applied to the hypothesis is 0’76 (’good’).
ConclusionsA) Using the Rorschach Test and P. Marty’s Psychosomatic Classification in a complementary manner, these two instruments together provide high reliability, with respect to the degree of mentalization (a subject’s risk of suffering psychosomatic disorders). B) The degree of mentalization has a significant impact on the success or failure in the application of Assisted Reproduction Techniques in infertile women.
Disclosure of InterestNone Declared
When magic happens. An interesting study of symptoms
- P. García Vázquez, C. Vilella Martin, E. Seijo Zazo, E. Gil Martín, C. Alvarez Vazquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S773
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Among the cases usually referred to Pain Clinics, the existence of cases of medically unexplained symptoms (MUS) is frequent, which are defined as those physical symptoms that present little or no basis that they respond to an underlying organic disease or that even when organic disease exists the symptoms are inconsistent or disproportionate to it.
ObjectivesThe main objective of this study is to know the proportion of patients who present MUS among those referred to a Pain Clinic. Secondarily, an attempt will be made to classify those patients with MUS in different diagnostic categories.
MethodsObservational study. All those patients referred to the Pain Unit of the Complejo Asistencial Universitario de León for 18 months were included in the study. All patients are evaluated in real clinical conditions, without any experimental control of variables, initially by a multidisciplinary team made up of Anesthesiologist, Psychiatrist and Rehabilitator and, in those who suspect a MUS condition, individually by part of psychiatry in order to confirm and characterize the syndrome.
Results462 patients were evaluated in a multidisciplinary way. 174 (37.7%) were male and 288 (62.3%) females. The mean age was 59.06 + 16.30 years. After the multidisciplinary assessment, two groups of patients were formed, one of 313 patients (67.75%) in whom there was no suspicion of MUS and the other of 149 patients (32.25%) in whom the existence of a MUS condition was suspected and who were referred for evaluation by psychiatric interview. After the psychiatric interview, it is observed that psychopathological and social factors explain the painful condition in 23.7% of the cases. The diagnoses found were Somatoform Disorders and Central Sensitization (N = 49, 10.6%), Malingering (N = 23, 5%), Factitious Disorders (N =21, 4.5%) and Other Diagnoses (N = 38, 8.2%).
ConclusionsThe psychological and social factors are relevant to explain the condition of up to
23.7% of the patients referred to the pain unit.
Disclosure of InterestNone Declared
New insights into cerebellar dysfunction in patients with delusional disorder: A systematic review
- A. González- Rodríguez, A. Guàrdia, A. Alvarez, M. Natividad, C. Pagés, C. Ghigliazza, E. Román, B. Sánchez, J. A. Monreal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S372-S373
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The cerebellum has been implicated in cognitive, affective and motor functions, including emotion regulation, executive control and sensorimotor processing. In schizophrenia, cerebellar dysfunction has been associated with treatment resistance and clinical features. However, few studies have been focused on delusional disorder (DD).
ObjectivesOur main purpose was to review the evidence available on cerebellum abnormalities and dysfunctions in patients with DD.
MethodsA systematic review was conducted through PubMed, Scopus and ClinicalTrials.gov (inception-June 2022) according to the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) directives. The following search terms were used: cerebellum OR cerebellar AND (“delusional disorder” AND paranoia). Reference lists from included studies were hand-checked to find other potential relevant papers.
ResultsSix studies were included from a total of 119 retrieved records (PubMed: 52, Scopus: 66, ClinicalTrials.gov: 1). Study 1:Patients with DD somatic type (n=14) presented a decreased gray matter volume in cerebellar lobules compared to healthy controls (HC) (n=32, left lobule VIIIa) and non-somatic DD (n=18, lobule V). Cerebellar volumes did not seem to differ between HC and non-somatic DD. Study 2:Abnormalities of voluntary saccadic eye movements, linking frontal and cerebellar functions, were found in DD patients (n=34) compared to HC (n=40). Study 3: Abnormal smooth pursuit eye movements in DD (n=15) compared with HC (n=40) and similar to schizophrenia (n=40). Case reports (n=3): DD associated with Dandy-Walker variant (partial vermian hypoplasia), unruptured intracerebral aneurysm of basilar artery, and megacisterna magna.
ConclusionsCerebellar deficits in patients with DD has been reported, particularly in those presenting somatic delusional contents.
Disclosure of InterestNone Declared
GnRh agonists as precipitating components of psychiatric pathology. A case report.
- A. Guerrero Medina, J. S. García Eslava, A. C. Martín Rodriguez, L. Martinez Salvador, M. J. Alvarez Alonso, M. Aubareda Magriña
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1042-S1043
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
GnRh agonists are drugs used in various gynecological pathologies, among which is endometriosis. They act by stimulating GnRh receptors in the pituitary gland. This sustained and continuous stimulation of GnRh, will initially generate an increase in the release of luteinizing hormones and follicle-stimulating hormones, subsequently losing sensitivity to the receptors, internalizing them, and thus suppressing the release of these hormones, which would entail an ovarian suppression, thereby inhibiting the release of estrogens and progesterone. Psychiatric adverse effects have been described. Gonzalez-Rodriguez et al (Front Psychiatry 2020; 11:479), described this association with changes in mood, and the presence of a series of cases where the link between GnRh agonist and the possibility of presenting psychotic symptoms is observed. Wieck (Curr Top Behav Neurosci 2011;8:173-87), Frokjaer (J Neurosci Res 2020;98(7):1283-1292), Brzezinski-Sinai et al (Front Psychiatry 2020;11:693) reported that this association could be related with the relationship of the hypothalamic-pituitary-gonadal axis, hormonal fluctuation and its relationship with the dopaminergic regulation, a genetic component that would increase the predisposition to trigger psychiatric pathology in patients with greater sensitivity to hormonal fluctuations, and the loss of neuroprotection generated by the decrease of estrogens in the central nervous system. All of this in the context of multiple environmental and genetic factors that participate together in the appearance of the disease.
ObjectivesTo describe the importance of detecting the risk factors that can precipitate a psychotic episode, including the use of certain drugs, such as GnRh agonists.
MethodsWe describe a case of a 45 year old patient with endometriosis with multiple organ involvement who went to the emergency room due to behavioral changes in the context of a brief psychotic disorder with “ad-integrum” recovery.
ResultsA retrospective analysis of the case is conducted, observing an association between the introduction of GnRh agonists and the presentation of a first psychotic episode.
ConclusionsThe importance of this case lies in the limited evidence of this association in the literature, and the implication of these drugs in the triggering of psychiatric pathology, being an aspect to be considered by psychiatrists in their patient’s follow-up.
Disclosure of InterestNone Declared
Female infertility, Alexithymia and Stress
- A. M. Delgado Campos, P. Alcindor Huelva, A. Alvarez Astorga, S. Rubio Corgo, E. Pérez Vicente, M. Arrieta Pey, C. Diaz Gordillo, P. del Sol Calderón, A. C. Martín Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S648
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In this research the Paris School (I.P.S.O.), by P. Marty, is chosen as the theoretical and clinical basis of Psychosomatics. We work with the degree of mentalization (good, bad and uncertain) -obtained through Marty’s Psychosomatic Classification-, as a previous diagnosis and prognosis of 120 infertile women undergoing treatment at the Assisted Reproduction Unit (ARU) at Hospital Universitario 12 de Octubre in Madrid.
Objectivesa) To analyse the statistical coincidence between female infertility, stress and alexithymia syndrome. b) To verify the differences between psychosomatic disorders and other somatoform symptoms and syndromes (conversive and hypochondriac). c) To test the following hypothesis: subjects whose degree of mentalization is deficient, present high degree of alexithymia and stress.
Methods120 infertile women undergoing treatment with Assisted Reproduction Techniques were examined by means of psychodiagnostic tests.
Diagnostic tools: P. Mary’s Psychosomatic Classification (P.C.) (semi-structured interview), as a means of diagnosing the degree of mentalization; T.A.S. (Toronto Alexithymia Scale); Battery of stress measurement questionnaires (H.A.D., PANAS. IRE, MCMQ).
The correlation of coincidence between the results of C.P. and the different Alexithymia and Stress questionnaires with the independent variable (success or failure of pregnancy in the selected subjects) has been studied, applying Spearman’s Correlation Coefficient.
ResultsWith respect to what was obtained in the Psychosomatic Classification:
- T.A.S. questionnaire yields a coefficient of [-0.48]. Therefore, there is a negative correlation between the degree of mentalization and the presence of alexithymia; in other words, as the degree of mentalization increases, the degree of alexithymia decreases and vice versa;
- There is positive correlation [0.39] between the results of Mentalization (Psychosomatic Classification) and the degree of stress; therefore, the existence of stress does not prevent better mentalization.
ConclusionsThe present research concludes: a) that people at risk for psychosomatic disorders have high scores on “alexithymia”; b) that patients at high risk for psychosomatic disorders do not necessarily suffer from “stress” situations; c) that there are many indicators in behavior and psychological functioning that differentiate psychosomatic disorders from conversive and hypochondriac disorders - both in their etiology and their development; d) there is a statistical correlation between female infertility and alexithymia; e) there is no statistical correlation between female infertility and stress.
Disclosure of InterestNone Declared
Assessment of beliefs and attitudes about electroconvulsive therapy posted on Twitter: An observational study
- L. de Anta, M. A. Alvarez-Mon, C. Donat-Vargas, F. J. Lara-Abelanda, V. Pereira-Sanchez, C. Gonzalez Rodriguez, F. Mora, M. A. Ortega, J. Quintero, M. Alvarez-Mon
-
- Journal:
- European Psychiatry / Volume 66 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 09 January 2023, e11
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Electroconvulsive therapy (ECT) is an effective and safe medical procedure that mainly indicated for depression, but is also indicated for patients with other conditions. However, ECT is among the most stigmatized and controversial treatments in medicine. Our objective was to examine social media contents on Twitter related to ECT to identify and evaluate public views on the matter.
MethodsWe collected Twitter posts in English and Spanish mentioning ECT between January 1, 2019 and October 31, 2020. Identified tweets were subject to a mixed method quantitative–qualitative content and sentiment analysis combining manual and semi-supervised natural language processing machine-learning analyses. Such analyses identified the distribution of tweets, their public interest (retweets and likes per tweet), and sentiment for the observed different categories of Twitter users and contents.
Results“Healthcare providers” users produced more tweets (25%) than “people with lived experience” and their “relatives” (including family members and close friends or acquaintances) (10% combined), and were the main publishers of “medical” content (mostly related to ECT’s main indications). However, more than half of the total tweets had “joke or trivializing” contents, and such had a higher like and retweet ratio. Among those tweets manifesting personal opinions on ECT, around 75% of them had a negative sentiment.
ConclusionsMixed method analysis of social media contents on Twitter offers a novel perspective to examine public opinion on ECT, and our results show attitudes more negative than those reflected in studies using surveys and other traditional methods.
Hysteria in neurology: a diagnostic approach to conversive disorder
- A. Sanz Giancola, I. Cuevas Iñiguez, C. Alvarez Garcia, M.D.C. Molina Liétor, M. Blanco Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S395
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Conversion disorder (a term that describes what was previously called hysteria) refers to motor or sensory symptoms, or both, that resemble a neurological disease, but that do not originate from or cannot be explained by a known physical disease.
ObjectivesTo find reliable tools that can guide the difficult diagnosis of conversion disorder.
MethodsBibliographic review
ResultsThe exact prevalence of the disorder is unknown. It is estimated that approximately 5% of referrals to neurology are for this disorder. Approximately one third of patients referred to the neurologist have symptoms that cannot be explained by an organic disease. Involuntary movements are the most common motor manifestations of the conversive syndrome, being tremor one of the most frequent manifestations. The first differential diagnosis of conversion disorder is neurological disease. It is currently not necessary for the diagnosis to assess whether or not the symptoms are produced intentionally, as the assessment of conscious intentionality is unreliable. The neurological examination is the fundamental tool for the diagnostic approach, being even more enlightening than the complementary tests. Hoover’s sign, Babinski’s combined leg flexion, plantar flexion of the ankle, tremor and its distraction and synchronisation manoeuvres, as well as the clinical differences between epileptic seizures and non-epileptic seizures of psychogenic origin, are some of the reliable tools for a correct diagnosis.
ConclusionsThe diagnosis of the disease should be one of exclusion. There must be clinical data showing clear evidence of incompatibility with a neurological disease and conversion symptoms do not correspond to known physiological mechanisms and anatomical pathways.
DisclosureNo significant relationships.
Proposal of a therapeutic algorithm for the psychopharmacological management of treatment-resistant depression
- A. Sanz Giancola, M.D.C. Molina Liétor, I. Cuevas Iñiguez, C. Alvarez Garcia, M. Blanco Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S567
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The lack of a standardised definition for the concept of TRD and an adequate criteria for therapeutic response make difficult the management of patients with MDD who do not achieve remission with one or more courses of treatment. All classifications suggested to define TRD are arbitrary, partially evidence-based, subordinated to the pharmacological findings of the time in which they are written and with serious inconsistencies, making it difficult to construct a universal and enduring diagnostic system.
ObjectivesConsidering that the most important goal in treating a patient with Major Depressive Disorder (MDD) should be remission and return to previous functionality, the search for a standardised, evidence-based classification system will allow timely and effective interventions leading to the reduction of this devastating condition.
MethodsBibliographic review
ResultsThe proposed therapeutic algorithm arises from the combination of several fundamental principles for the management of treatment-resistant depression: the different classification systems of the concept, as well as the concepts of response, relapse, recurrence and remission; the scientific evidence found in the current literature, routine clinical practice, knowledge of switching and augmentation strategies, the new pharmacological targets and neurobiological hypothesis discovered, without forgetting finally the different clinical profiles of depressive symptomatology and the specific indications of each antidepressant.
ConclusionsResistant depression is difficult to treat successfully and is not a uniform entity. Recently there has been a move to characterise treatment-resistant depression as ‘difficult-to-treat’ depression on the basis that the former description implies that depression treatments are normally effective and that non-response is therefore somehow abnormal.
DisclosureNo significant relationships.






