41 results
4 Evaluating Plasma GFAP for the Detection of Alzheimer’s Disease Dementia
- Madeline Ally, Henrik Zetterberg, Kaj Blennow, Nicholas J. Ashton, Thomas K. Karikari, Hugo Aparicio, Michael A. Sugarman, Brandon Frank, Yorghos Tripodis, Ann C. McKee, Thor D. Stein, Brett Martin, Joseph N. Palmisano, Eric G. Steinberg, Irene Simkina, Lindsay Farrer, Gyungah Jun, Katherine W. Turk, Andrew E. Budson, Maureen K. O’Connor, Rhoda Au, Wei Qiao Qiu, Lee E. Goldstein, Ronald Killiany, Neil W. Kowall, Robert A. Stern, Jesse Mez, Michael L. Alosco
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 408-409
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Blood-based biomarkers represent a scalable and accessible approach for the detection and monitoring of Alzheimer’s disease (AD). Plasma phosphorylated tau (p-tau) and neurofilament light (NfL) are validated biomarkers for the detection of tau and neurodegenerative brain changes in AD, respectively. There is now emphasis to expand beyond these markers to detect and provide insight into the pathophysiological processes of AD. To this end, a reactive astrocytic marker, namely plasma glial fibrillary acidic protein (GFAP), has been of interest. Yet, little is known about the relationship between plasma GFAP and AD. Here, we examined the association between plasma GFAP, diagnostic status, and neuropsychological test performance. Diagnostic accuracy of plasma GFAP was compared with plasma measures of p-tau181 and NfL.
Participants and Methods:This sample included 567 participants from the Boston University (BU) Alzheimer’s Disease Research Center (ADRC) Longitudinal Clinical Core Registry, including individuals with normal cognition (n=234), mild cognitive impairment (MCI) (n=180), and AD dementia (n=153). The sample included all participants who had a blood draw. Participants completed a comprehensive neuropsychological battery (sample sizes across tests varied due to missingness). Diagnoses were adjudicated during multidisciplinary diagnostic consensus conferences. Plasma samples were analyzed using the Simoa platform. Binary logistic regression analyses tested the association between GFAP levels and diagnostic status (i.e., cognitively impaired due to AD versus unimpaired), controlling for age, sex, race, education, and APOE e4 status. Area under the curve (AUC) statistics from receiver operating characteristics (ROC) using predicted probabilities from binary logistic regression examined the ability of plasma GFAP to discriminate diagnostic groups compared with plasma p-tau181 and NfL. Linear regression models tested the association between plasma GFAP and neuropsychological test performance, accounting for the above covariates.
Results:The mean (SD) age of the sample was 74.34 (7.54), 319 (56.3%) were female, 75 (13.2%) were Black, and 223 (39.3%) were APOE e4 carriers. Higher GFAP concentrations were associated with increased odds for having cognitive impairment (GFAP z-score transformed: OR=2.233, 95% CI [1.609, 3.099], p<0.001; non-z-transformed: OR=1.004, 95% CI [1.002, 1.006], p<0.001). ROC analyses, comprising of GFAP and the above covariates, showed plasma GFAP discriminated the cognitively impaired from unimpaired (AUC=0.75) and was similar, but slightly superior, to plasma p-tau181 (AUC=0.74) and plasma NfL (AUC=0.74). A joint panel of the plasma markers had greatest discrimination accuracy (AUC=0.76). Linear regression analyses showed that higher GFAP levels were associated with worse performance on neuropsychological tests assessing global cognition, attention, executive functioning, episodic memory, and language abilities (ps<0.001) as well as higher CDR Sum of Boxes (p<0.001).
Conclusions:Higher plasma GFAP levels differentiated participants with cognitive impairment from those with normal cognition and were associated with worse performance on all neuropsychological tests assessed. GFAP had similar accuracy in detecting those with cognitive impairment compared with p-tau181 and NfL, however, a panel of all three biomarkers was optimal. These results support the utility of plasma GFAP in AD detection and suggest the pathological processes it represents might play an integral role in the pathogenesis of AD.
5 Antemortem Plasma GFAP Predicts Alzheimer’s Disease Neuropathological Changes
- Madeline Ally, Henrik Zetterberg, Kaj Blennow, Nicholas J. Ashton, Thomas K. Karikari, Hugo Aparicio, Michael A. Sugarman, Brandon Frank, Yorghos Tripodis, Brett Martin, Joseph N. Palmisano, Eric G. Steinberg, Irene Simkina, Lindsay Farrer, Gyungah Jun, Katherine W. Turk, Andrew E. Budson, Maureen K. O’Connor, Rhoda Au, Wei Qiao Qiu, Lee E. Goldstein, Ronald Killiany, Neil W. Kowall, Robert A. Stern, Jesse Mez, Bertran R. Huber, Ann C. McKee, Thor D. Stein, Michael L. Alosco
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 409-410
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Blood-based biomarkers offer a more feasible alternative to Alzheimer’s disease (AD) detection, management, and study of disease mechanisms than current in vivo measures. Given their novelty, these plasma biomarkers must be assessed against postmortem neuropathological outcomes for validation. Research has shown utility in plasma markers of the proposed AT(N) framework, however recent studies have stressed the importance of expanding this framework to include other pathways. There is promising data supporting the usefulness of plasma glial fibrillary acidic protein (GFAP) in AD, but GFAP-to-autopsy studies are limited. Here, we tested the association between plasma GFAP and AD-related neuropathological outcomes in participants from the Boston University (BU) Alzheimer’s Disease Research Center (ADRC).
Participants and Methods:This sample included 45 participants from the BU ADRC who had a plasma sample within 5 years of death and donated their brain for neuropathological examination. Most recent plasma samples were analyzed using the Simoa platform. Neuropathological examinations followed the National Alzheimer’s Coordinating Center procedures and diagnostic criteria. The NIA-Reagan Institute criteria were used for the neuropathological diagnosis of AD. Measures of GFAP were log-transformed. Binary logistic regression analyses tested the association between GFAP and autopsy-confirmed AD status, as well as with semi-quantitative ratings of regional atrophy (none/mild versus moderate/severe) using binary logistic regression. Ordinal logistic regression analyses tested the association between plasma GFAP and Braak stage and CERAD neuritic plaque score. Area under the curve (AUC) statistics from receiver operating characteristics (ROC) using predicted probabilities from binary logistic regression examined the ability of plasma GFAP to discriminate autopsy-confirmed AD status. All analyses controlled for sex, age at death, years between last blood draw and death, and APOE e4 status.
Results:Of the 45 brain donors, 29 (64.4%) had autopsy-confirmed AD. The mean (SD) age of the sample at the time of blood draw was 80.76 (8.58) and there were 2.80 (1.16) years between the last blood draw and death. The sample included 20 (44.4%) females, 41 (91.1%) were White, and 20 (44.4%) were APOE e4 carriers. Higher GFAP concentrations were associated with increased odds for having autopsy-confirmed AD (OR=14.12, 95% CI [2.00, 99.88], p=0.008). ROC analysis showed plasma GFAP accurately discriminated those with and without autopsy-confirmed AD on its own (AUC=0.75) and strengthened as the above covariates were added to the model (AUC=0.81). Increases in GFAP levels corresponded to increases in Braak stage (OR=2.39, 95% CI [0.71-4.07], p=0.005), but not CERAD ratings (OR=1.24, 95% CI [0.004, 2.49], p=0.051). Higher GFAP levels were associated with greater temporal lobe atrophy (OR=10.27, 95% CI [1.53,69.15], p=0.017), but this was not observed with any other regions.
Conclusions:The current results show that antemortem plasma GFAP is associated with non-specific AD neuropathological changes at autopsy. Plasma GFAP could be a useful and practical biomarker for assisting in the detection of AD-related changes, as well as for study of disease mechanisms.
“Asking for help, quite a challenge”. Time from onset of symptoms to consultation with a psychiatrist
- T. Jiménez Aparicio, M. Fernández Lozano, M. Merizalde Torres, E. Domínguez Guerra, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S469-S470
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the biggest challenges for primary care professionals is to know when it is appropriate to request a consultation with a psychiatrist. A complete medical history should be performed to detect anxious-depressive symptoms, as well as to determine the intensity, the trigger, time of evolution, and the functional repercussion (1). It is also important that the patient is able to express his or her symptoms and ask for help. The concept of “Alexitimia” refers to the difficulty of expressing feelings verbally, and is a frequent symptom in depressive patients (2).
In mild cases and with little repercussion, the physician himself can initiate treatment and follow up (3). However, on other occasions, it will be advisable to request a consultation with psychiatry.
ObjectivesThe main objective is to observe the time that elapses from the onset of symptoms until consultation with the Mental Health team is finally requested. Some preliminary results can already be obtained from this data collection.
MethodsWe have decided to carry out a descriptive study, collecting different variables from patients attending a first Psychiatry consultation.
ResultsIn a total sample of 208 patients, the majority (67%) were between 31 and 60 years old. Following the DSM-V criteria (4), patients were classified into groups according to their disorder: Adaptive, depressive, or other. These data were cross-referenced (Figure 1).
Subsequently, the time elapsed from the onset of symptoms (referred by the patients) was collected, until the referral to Psychiatry was processed. In order to make a comparison, average time (in days) was calculated for the different groups according to their age and diagnosis.
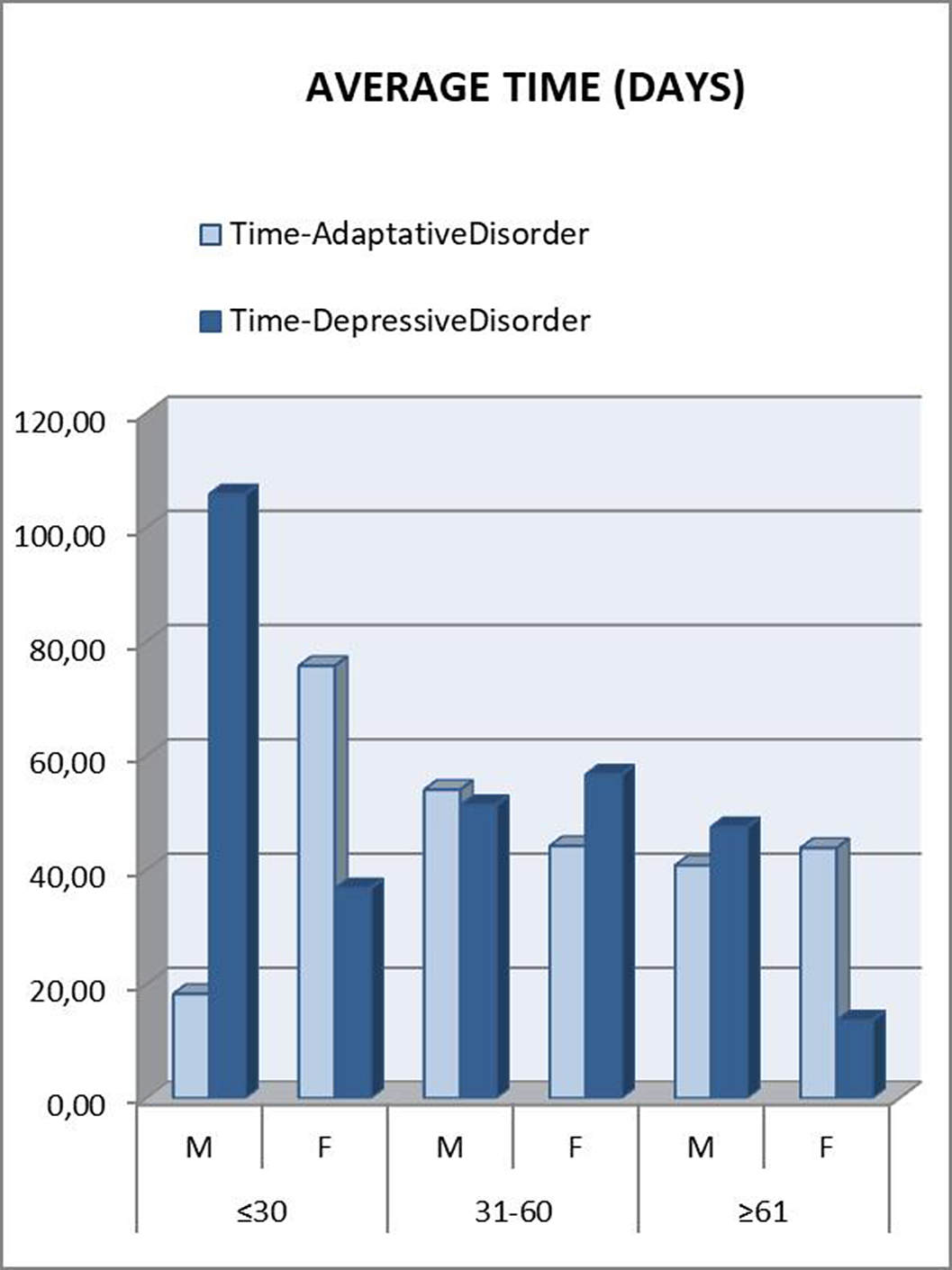
Those patients under 30 years were referred to psychiatry later. A downward trend was seen as the age range increased. In the “younger than 30” and “between 31 and 60” groups, patients who met criteria for Depressive Disorder took longer to be referred, which was striking considering that they are usually considered as more severe patients (Figure 2). This can be attributed to a greater difficulty in expressing their emotions (alexithymia), as another depressive symptom. Disaggregating these data by gender, the patients who clearly took the longest to be referred were men under 30 years old with a final diagnosis of Depressive Disorder (Figure 3). This gender difference is consistent with the social impact of alexithymia according to some articles (5).
Image:
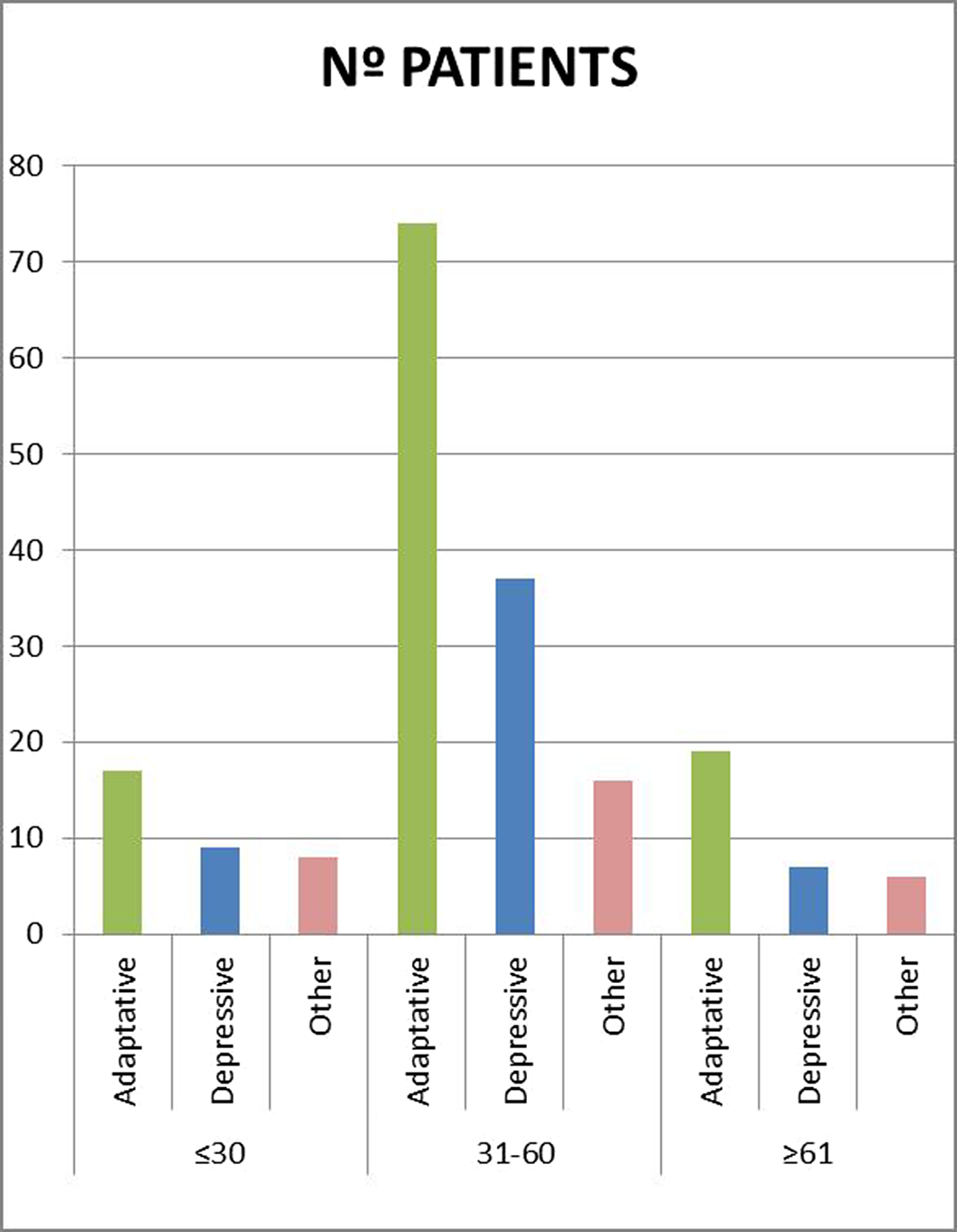
Image 2:
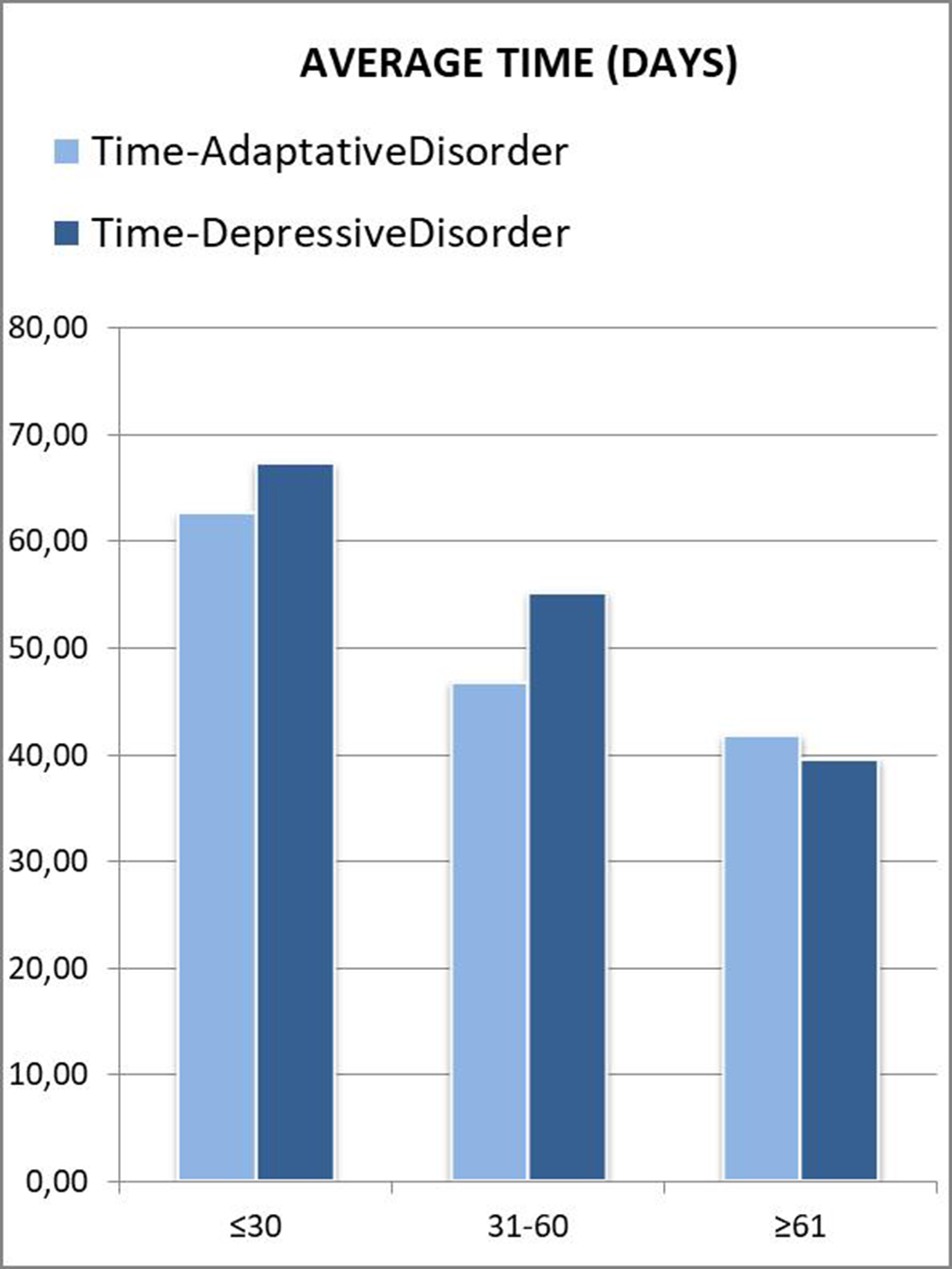
Image 3:
 Conclusions
ConclusionsIt is important that primary care physicians know how to take a complete history in those patients with symptoms of anxiety and depression.
In many cases, patients themselves have difficulties expressing their emotions and feelings (alexithymia), which may be another symptom of their discomfort.
This may lead to a delay in the time until referral to a psychiatry is requested, and therefore a worsening of symptoms.
Disclosure of InterestNone Declared
Euthanasia and psychiatric patients: a Spanish glance to the Dutch experience
- P. Albarracin, F. Mayor, M. Aparicio, E. Herrero
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S874
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The recent approval of euthanasia in the Spanish legal code and its posible extension to psychiatric patients opens an unprecedented scenario in the Iberian country. We analize the experience of the Netherlands, a country where euthanasia has been in practice for over two decades, in order to foresee epidemiological trends that could be replicated in Spain.
ObjectivesTo review the legislation on euthanasia in Spain and the Netherlands, as well as the epidemiological data regarding euthanasia applicants affected by mental health conditions in the Netherlands, to predict future epidemiological trends in a similar population in Spain.
MethodsWe studied the legislation on euthanasia in Spain and the Netherlands, as well as the directives of the Regional Commisions for Euthanasia in the Netherlands to analize differences and similarities between the legal codes on both countries. We also sought epidemiological data regarding the application of euthanasia on psychiatric patients in the Netherlands, gathering data from seven articles in English language obtained through a search in PubMed using the MeSH terms “Euthanasia” AND “Netherlands” and “Psychiatry”.
ResultsEuthanasia on psychiatric patients in the Netherlands has been a practice on the rise during the last decade, despite the elevated proportion of rejected applications and the high survival rate of this patients in later longitudinal studies. Affective disorders and personality disorders stand out as major psychiatric causes between the applicants. The Spanish legislation bears important resemblance to its Dutch predecessor, but also significant differences.
ConclusionsThe available data on the application of euthanasia on mental health patients in the Netherlands show an in increasing trend regarding the execution of this practice, specially on patients who gather distinct clinical features. The data provided by the Dutch experience could have some replication in Spain, as well as anticipate possible future ethical conflicts regarding the application of this service.
Disclosure of InterestNone Declared
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Evolution of Electroconvulsive Therapy during the COVID-19 pandemic in the Regional ECT Unit of the Region of Murcia
- M.A. Cutillas Fernández, M.L. Medina Garrido, M. López Villaescusa, E. Bermudez Larrosa, C. Martínez Milán, E. Aparicio Castro
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S522-S523
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Covid-19 was declared a global pandemic by the WHO on 11 March 2020. From the beginning, the pandemic posed a challenge to the different health systems around the world, which were forced to prioritise and distribute their resources as efficiently as possible. During the period between 11 March 2020 and 28 April 2021, the Regional ECT Unit of the Region of Murcia remained closed.
Objectives- Determine the clinical status of patients on maintenance ECT in the Regional ECT Unit during the Covid-19 pandemic.
- Prioritise resumption of treatment in those who were clinically decompensated or at risk
- Understand the consequences of discontinuation of maintenance ECT for these patients.
MethodsA longitudinal descriptive study was conducted during the month of May 2020.
ResultsThirty-seven patients were contacted by telephone. On the first call, a total of 15 patients were unstable or at risk of decompensation.
Prior to the second call, CT was administered preferentially to a total of 8 patients and programmed to 2. On the second call, a total of 11 patients were at risk of decompensation.
ConclusionsThe closure of the Regional ECT Unit had negative consequences for patients undergoing maintenance treatment. Electroconvulsive therapy is an essential part of the treatment of psychiatric patients both in acute episodes and in relapse prevention.
DisclosureNo significant relationships.
Bed for three
- C. Vallecillo Adame, T. Jiménez Aparicio, C. De Andrés Lobo, M. Queipo De Llano De La Viuda, G. Guerra Valera, A. Gonzaga Ramírez, I. Santos Carrasco, J. Gonçalves Cerejeira, C. Capella Meseguer, E. Rodríguez Vázquez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S767-S768
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Charles Bonnet syndrome (CBS) is characterized by the presence of visual hallucinations without other sensory-perceptual disturbances or evidence of organic mental disorder nor functional psychosis.
ObjectivesReview differential diagnosis of BCS, searching articles in Pubmed.
Methods62-year-old woman, undergoing treatment with Sertraline and psychotherapy for three months because of anxious-depressive synthoms. Pathological myopia and retinal detachment in 2012, blind left eye, retaining 33% vision in the right eye. She comes to the emergency room feeling really anxious, she says that for a year now she has had the feeling that her husband is cheating on her with another woman, and she claims with certainty that she sees a woman in her bed at night, as well as flashes of light evidencing her presence. She has also begun to hear voices through the telephone wires. She and her family deny memory loss or other cognitive impairments. We performed a Nuclear Magnetic Resonance with normal results. Family claims good conygal relation until these synthoms began and no signs of cognitive impairment.
ResultsThe patient lives as real these hallucinations which haven´t appeared during admission. We started treatment with an antipsychotic and a benzodiazepine, with great improvement of anxiety and development of some insight. Executive impairment was observed.
ConclusionsThe results obtained, make us think that, although our patient has an important visual loss, it is more a psychiatric pathology. Here lies the importance of a multidisciplinary approach among ophthalmologists, neurologists and psychiatrists in order to avoid misdiagnosis and that the patient can benefit from proper treatment.
DisclosureNo significant relationships.
Capgras syndrome. Where to find it?
- I.D.L.M. Santos Carrasco, J. Gonçalves Cerejeira, E. Rodríguez Vázquez, C. Capella Meseguer, M. Queipo De Llano De La Viuda, G. Guerra Valera, A. Gonzaga Ramírez, C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, A. Pérez Escudero
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S474-S475
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Capgras syndrome, where patients have the conviction that one or more close people have been replaced by a “double,” is the most prevalent delusional misidentification syndrome. It appears in psychiatric illness and organic brain damage. It seems to be due to damage of bifrontal and right limbic and temporal regions, mainly in the right hemisphere.
ObjectivesTo review the pathologies associated to Capgras Syndrome and the relevance of the differential diagnosis
Methods53-year-old female was admitted due to great sadness, crying, social withdrawal and severe paranoid concerns over the last month. Follow-up in Mental Health since 2014, because of anxious depression. After her mother’s death, she felt being followed because of old faults. Since then, low dosis of antipsychotics were used. Now she is afraid of being harmed in relation to petty thefts she committed over 15 years ago. In recent days, she has been noticing small details indicating that her family members have been impersonated by strangers, showing anguish regarding their whereabouts.
ResultsDuring her admission, high doses of antidepresants and paliperidone 6 mg/day were used with the complete disappearance of Capgras Syndrome and her anguish. Mild guilty thoughts were present after her discharge. That is why she was diagnosed with psychotic depression.
ConclusionsCapgras syndrome can be encountered in primary psychiatric diagnosis (particularly in schizophrenia and mood disorders) – where an organic element may exist in about a third of all cases – or secondary to organic disorders or medication-induced, through to overt organic brain damage, particularly in neurodegenerative disease.
Toothache
- E. Rodríguez Vázquez, C. Capella Meseguer, J. Gonçalves Cerejeira, I. Santos Carrasco, G. Guerra Valera, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, C. Vallecillo Adame, T. Jiménez Aparicio, C. De Andrés Lobo, A. Pérez Escudero
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S650
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental retardation (RM) is defined as by a deficient intellectual capacity as well as by alterations of the adaptive capacity that are externalized in two or more functional areas (Personal autonomy, Communication, Orientation in the environment, Work and Free time).
ObjectivesPresent a patient with a severe behavioural disturbance with an associated intellectual deficit, who remained hospitalized for 2 months and after observing an oral alteration her symptoms improved.
MethodsA descriptive study of a clinical case
Results54-year-old woman, single. You have a moderate intellectual disability. In January 2019, she began mental health consultations with a diagnosis of adjustment disorder, on treatment with aripiprazole 5 mg/day, mirtazapine 15 mg/day, lorazepam 0.5 mg/day and dipotassium clorazepate 10 mg/day. Went to the emergency room with mutism, hyporesponsiveness and refuse to intake, having lost 25 kg in 6 months. Abdominal and thoracic CT and upper gastrointestinal endoscopy without significant findings. Consultation with otorhinolaryngology, dermatology, traumatology without significant findings. Odontostomatology consultation: Deep cavities are observed, so it is necessary to carry out extractions of the pieces in poor condition. After this intervention, the patient returns to accept oral intake.
ConclusionsPeople with intellectual disabilities have a wide range of medical problems that in many cases are directly associated with the underlying disease or syndrome and, in others, with poor physical health due to problems in basic self-care skills or the ability to express verbally. Usually, the first manifestation of pain is an alteration in behaviour, which must be taken into account when making a differential diagnosis.
DisclosureNo significant relationships.
¡ I see presenters in my house !
- M. Queipo De Llano, E. Rodríguez Vázquez, C. Capella Meseguer, J. Gonçalves Cerejeira, I. Santos Carrasco, G. Guerra Valera, A. Gonzaga Ramírez, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S412
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Charles Bonnet syndrome (CBS) is characterized by the presence of visual hallucinations, generally complex, which occurs in patients with alterations in the visual pathway. The majority of affected patients are elderly. It appears in 15% of people with visual loss, predominantly in the 80-year-old female gender.
ObjectivesTo present a clinical case of a patient with visual hallucinations and a possible diagnosis of Charles Bonnet syndrome. Highlight the importance of an adequate differential diagnosis.
MethodsBibliographic review of the treatment and diagnosis of CBS, from articles published in the last 5 years in Pubmed.
ResultsWoman, 80 years old. No ophthalmological history except those associated with advanced age. She goes to the emergency room due to the presence of visual hallucinosis, in the form of “television presenters” of whom she makes partial criticism, being aware most of the time of their unreality. Hallucinations are not accompanied by anxiety or significant affective repercussions. Discarded delirium, intoxication by substances or drugs that cause the condition. Currently under follow-up to rule out other causes.
ConclusionsThe diagnosis of SCB requires a multidisciplinary approach between neurologists, psychiatrists and ophthalmologists in order to avoid erroneous diagnoses. The differential diagnosis should be made with pathologies such as Lewy body dementia, Parkinson’s disease, delirium, substance intoxication, migraine aura, and metabolic encephalopathy, among others. It is important to involve the family in the treatment of the syndrome to reinforce the recognition of the unreality of these hallucinations in the patients. Antipsychotic treatment can be effective only if the condition is extremely distressing.
Comorbid anorexia nervosa and schizophrenia
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, C. Capella Meseguer, E. Rodríguez Vázquez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S243-S244
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Although schizophrenia and anorexia nervosa are very different disorders, when they occur in the same patient it can be difficult to distinguish whether the alterations in body image are due to psychotic symptoms or correspond to a comorbid eating disorder. It is also relevant to know how they can interact with each other.
ObjectivesPresentation of a clinical case of anorexia nervosa in the context of a patient with a previous diagnosis of paranoid schizophrenia.
MethodsBibliographic review of the relationship between schizophrenia and alterations in the perception of body image by searching for articles in Pubmed.
ResultsWe present a 48-year-old woman who resides with her mother and a sister. Diagnosed with paranoid schizophrenia and eating disorder. She had previously been admitted to hospital twice. Since 2004, she has been followed up in mental health consultations. The patient reports constant weight changes. A year ago she began to feel overweight and began to restrict her intake and to exercise, having lost 20 kg. She reports psychotic symptoms in the past, that she now denies. Various scales show moderate impact of weight on personal perception of psychosocial adjustment, an impulse to thinness and a significant distortion of body image, perceiving herself as heavier than she is and wishing she was lighter.
ConclusionsIn schizophrenia, confusion in bodily experiences and states is not uncommon. The possible interactions between the symptoms of schizophrenia and anorexia nervosa complicate the adequate care of these patients. Further research on comorbidity of these two disorders is necessary.
The ugliest woman un the world
- M. Queipo De Llano, C. Capella Meseguer, E. Rodríguez Vázquez, I. Santos Carrasco, J. Gonçalves Cerejeira, G. Guerra Valera, A. Gonzaga Ramírez, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S611
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The main feature of body dysmorphic disorder (BDD) is impairing preoccupation with a physical defect that appears slight or non-existent to others.
ObjectivesTo draw an overview of BDD through a clinical case of a patient with BDD and autolytic ideation, which improved after an adequate diagnosis and an early pharmacological and psychotherapeutic approach.
MethodsBibliographic review of the treatment and diagnosis of BDD, from articles published in the last 5 years in Pubmed.
Results18-year-old woman diagnosed with depression and obsessive ideation, which started at the age of 11, after a comment at school. The patient believes that she has intenseunder-eye bags or dark circles, this has caused her to abandon all activity and self-isolate at home. Symptoms included recurring obsessive and intruding thoughts related to the supposed defect, ritualized behaviors of hours of duration aiming toit through makeup, and autolytic ideation. Therapeutic approach combined psychopharmacological and psychotherapeutic treatments, obtaining gradual improvement of symptomatology and disappearance of the autolytic ideation.
ConclusionsThe disorder is severe, which is reflected in high rates of suicide attempts. Differential diagnosis between obsessive and delirious dysmorphophobia is essential for improving outcomes; the egodystonic nature of the symptom, awareness of illness and obsessive personality traits facilitate the diagnosis. A multidisciplinary approach involving psychiatrists and clinical psychologists is necessary for a correct diagnosis and early treatment of this pathology, as well as recognition by dermatologists, surgeons and medical aesthetic professionals, where these patients go with the aim of finding solutions to their problem.
DisclosureNo significant relationships.
Lithium toxicity. A case report
- E. Rodríguez Vázquez, C. Capella Meseguer, I. Santos Carrasco, J. Gonçalves Cerejeira, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. De Andrés Lobo, T. Jiménez Aparicio, C. Vallecillo Adame
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S651
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium is widely used in the treatment of the bipolar disorder. Once introduced, it is necessary to carry out an adequate control of the therapeutic range, since it is potentially toxic, and can affect various organs.
ObjectivesTo present the case of a patient suffering from lithium poisoning and to review the symptoms of lithium poisoning.
MethodsA descriptive study of a clinical case and review of the literature
Results49-year-old woman, married. Diagnosed with bipolar disorder. She went to the emergency room due to a low level of consciousness, kidney failure, trembling of the limbs, hyperthermia and leukocytosis. In the last two weeks, the patient has reduced her intake of food, not water, finding herself more and more shaky and less reactive. Lithium in blood at admission 1.71, so conventional dialysis was performed with a progressive decrease into 0.65. On examination, he is practically mutist, bradypsychia with a significant response latency. Clinical judgment: Accidental lithium poisoning.
ConclusionsThe primary site of toxicity is the central nervous system and clinical manifestations vary from asymptomatic supratherapeutic drug concentrations to clinical toxicity such as confusion, ataxia, or seizures. Severe lithium neurotoxicity occurs almost exclusively in the context of chronic therapeutic administration of lithium and rarely results from acute ingestion of lithium, even in patients currently taking lithium. As such it is an iatrogenic illness, occurring in patients who have identifiable clinical risk factors: nephrogenic diabetes insipidus, older age, abnormal thyroid function and impaired renal function.
DisclosureNo significant relationships.
They are not real patients
- T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Queipo De Llano De La Viuda, G. Guerra Valera, A. Gonzaga Ramírez, J. Gonçalves Cerejeira, I. Santos Carrasco, C. Capella Meseguer, E. Rodríguez Vázquez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S688
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive depressive disorder (or depressive pseudodementia) is a condition defined by functional impairment, similar to dementias or other neurodegenerative disorders, in the context of psychiatric patients. It is important to consider a differential diagnosis in patients with cognitive impairment.
ObjectivesPresentation of a clinical case of a patient with depression with psychotic symptoms who presents cognitive impairment.
MethodsBibliographic review of the differential diagnosis between cognitive depressive disorder and real dementia by searching for articles in PubMed.
ResultsWe present a 51-year-old woman, previously diagnosed with adjustment disorder (with mixed anxiety and depressed mood) and unspecific anxiety disorder, who was admitted to the hospital due to delusional ideation of harm and Capgras syndrome, ensuring that her relatives had been replaced and the rest of the patients were not real patients, but actors who conspired against her. The MRI (Magnetic Resonance Imaging) was strictly normal (tumors or acute injuries as stroke or hemorrhage were discarded), and a MoCA (Montreal Cognitive Assesment) test was performed to screen any cognitive impairments (obtaining a score of 19/30, with language fluency and abstraction particularly affected). It would be convenient to repeat the test when this episode and the psychotic symptoms are resolved or improved.
Conclusions1. Some patients may have cognitive impairment in the context of a mood disorder. 2. A differential diagnosis and follow-up of these patients should be performed to assess prognosis, reversibility and treatment. 3. Depressive cognitive impairment may precede the development and establishment of a dementia or neurodegenerative picture.
DisclosureNo significant relationships.
Green synthesis of silver nanoparticles with phytosterols and betalain pigments as reducing agents present in cactus Myrtillocactus geometrizans.
- Isaac Lucas-Gómez, Gabriela Carrasco-Torres, Daniel Bahena-Uribe, Jaime Santoyo-Salazar, Eduardo Fernández-Martínez, Isabel Sánchez-Crisóstomo, José. A. Pescador-Rojas, José E. Aparicio-Burgos
-
- Journal:
- MRS Advances / Volume 5 / Issue 63 / 2020
- Published online by Cambridge University Press:
- 25 November 2020, pp. 3361-3369
- Print publication:
- 2020
-
- Article
- Export citation
-
In the current work, we compared the green synthesis of silver nanoparticles (AgNP) using plant extracts, a promising methodology against the use of chemical reducers, such as oleic acid and oleylamine. The advantages of green synthesis are one-step method, economic and ecological while the advantages of classic synthesis methods are high nanoparticle performance, homogeneity in size and smaller average sizes. With this work we want to demonstrate that plant extracts with specific mixtures of chemical compounds can obtain smaller average sizes with greater homogeneity in nanoparticles compared to the use of classical synthesis. Myrtillocactus geometrizans was used as a polar plant extract, which was selected by the chemical components contained in the extract. Phytosterols, oleic acid and betalains contained in Myrtillocactus geometrizans are biomolecules responsible for the reduction and stability of AgNP below 5 nm. TEM analysis of the green synthesis of nanoparticles revealed the formation of spherical particles with an average diameter of 5 nm and with preferential crystallographic directions of the silver plane [111].
Contribution of multivariate analysis to the correlation of some properties of kaolin with its mineralogical and chemical composition
- E. Galan, P. Aparicio, I. Gonzalez, A. Miras
-
- Journal:
- Clay Minerals / Volume 33 / Issue 1 / March 1998
- Published online by Cambridge University Press:
- 09 July 2018, pp. 65-75
-
- Article
- Export citation
-
According to multivariate analysis, the following were established (a) kaolinite crystallinity index (KCI) values determined by XRD are highly correlated to one another and seemingly influenced by kaolin impurities; (b) kaolin minerals are concentrated mainly in the fractions <4 µm; (c) the kaolin surface area as determined by the BET (nitrogen adsorption) method is more markedly affected by kaolin impurities than by kaolin minerals themselves; (d) BET surfaces increase when kaolinite crystallinity decreases; (e) brightness is inversely correlated with kaolin impurities; (f) the more ordered the kaolinite and the greater the proportion in the <4 µm fraction of the kaolin, the greater the brightness; and (g) KCI values are particle size-distribution dependent for sedimentary-residual kaolins. The correlations obtained were better when kaolins were selected according to their origin because the kaolin minerals and their impurities, particle size-distribution and texture were more alike. The industrial properties of kaolin can not be predicted from other basic properties such as mineralogy, KCI, etc., because they are intricately related to one another.
Kaolin fractal dimension. Comparison with other properties
- P. Aparicio, J . L. Pérez-Bernal, E. Galán, M. A. Bello
-
- Journal:
- Clay Minerals / Volume 39 / Issue 1 / March 2004
- Published online by Cambridge University Press:
- 09 July 2018, pp. 75-84
-
- Article
- Export citation
-
The fractal dimension values of several kaolins with different structural order and properties have been calculated from N2-adsorption isotherm data according to the Neimark method. All kaolins show a fractal regime in the same nitrogen relative pressure range, with fractal dimension values ranging between 2.38 and 2.57.
The correlation between fractal dimension and other kaolin characteristics (structural order of kaolinite, BET surface area, brightness and particle-size distribution) was determined. The correlation matrix shows that the fractal dimension (Ds) is highly correlated with the degree of structural order-disorder and is also moderately correlated with the particle-size distribution and brightness. No correlation was observed between BET and Ds, probably because the first is a measurement of the accessible surface while Ds represents the scaling properties of the area.
As Ds is a parameter easily calculated and related to the degree of surface heterogeneity, and well correlated with other kaolinite parameters, it can be used to estimate a set of kaolin technical properties for suitability of the kaolin in the paper industry.
Residence and fractionation of rare earth elements during kaolinization of alkaline peraluminous granites in NW Spain
- E. Galán, J. C. Fernández-Caliani, A. Miras, P. Aparicio, M. G. Márquez
-
- Journal:
- Clay Minerals / Volume 42 / Issue 3 / September 2007
- Published online by Cambridge University Press:
- 09 July 2018, pp. 341-352
-
- Article
- Export citation
-
A geochemical and mineralogical study has allowed us to address the factors controlling distribution pattern, residence and behaviour of rare earth elements (REE) during kaolinization of Variscan granitoids in NW Spain. Mineral composition of the deeply weathered samples is dominated by kaolinite, with minor amounts of quartz, muscovite-illite, alkaline feldspar and traces of resistant minerals (rutile, ilmenite, zircon and monazite). Variable amounts of Si, Na, Ca, K, Rb, Cs, Ba, U and P were lost from the weathering profile, as a result of feldspars, mica and apatite breakdown, whereas Al, Fe, Ti, Zr, Th, Hf and REE were concentrated in the residual kaolin. Chondrite-normalized REE patterns of the kaolins show an overall enrichment of light REE (LaN/SmN = 1.22–2.53), heavy REE depletion (GdN/YbN = 2.42–15.10) and a strong negative Eu anomaly (Eu/Eu* = 0.11–0.25), probably inherited from the parent granite. Nevertheless, the normalization to the parent granite reveals some REE fractionation and increasing positive Eu anomalies with advancing weathering, in response to the breakdown of feldspars. Different grain-size fractions show similar REE distribution patterns, but differ in concentration levels. Although the fine fractions are the most important REE reservoir, there is no positive correlation with clay mineralogy. The correlative behaviour among P2O5, Th and REE in the <2 mm fraction suggests that monazite plays a dominant role controlling the REE budget in the weathering profile.
A new kaolinite order index based on XRD profile fitting
- P. Aparicio, E. Galán, R. E. Ferrell
-
- Journal:
- Clay Minerals / Volume 41 / Issue 4 / December 2006
- Published online by Cambridge University Press:
- 09 July 2018, pp. 811-817
-
- Article
- Export citation
-
The determination of kaolinite order-disorder by X-ray diffraction is problematic due to overlapping peaks from associated kaolin minerals and X-ray amorphous phases. This paper presents a new index (Aparicio-Gala´n-Ferrell index — AGFI), measured on 02l and 11l reflections after decomposing individual peaks in the complex diffraction band in an effort to reduce interferences. The new index was tested with three kaolins, of varying structural order, and their admixtures containing different percentages of quartz, feldspar, illite, smectite, chlorite, halloysite and Fe hydroxides and silica gels. The AGFI is highly correlated with the percentage of low-defect kaolinite and the Hinckley Index. It is not as prone to interference by associated minerals and X-ray amorphous phases as other indices. The AGFI can be used to determine kaolinite order-disorder in a wide variety of kaolins and kaolinitic rocks; the only prerequisite is that the kaolinite content should be >10 wt.% in order for the results to be reproducible.
An application of profile fitting and CLAY++ for the quantitative representation (QR) of mixed-layer clay minerals
- P. Aparicio, R. E. Ferrell
-
- Journal:
- Clay Minerals / Volume 36 / Issue 4 / December 2001
- Published online by Cambridge University Press:
- 09 July 2018, pp. 501-514
-
- Article
- Export citation
-
Clay mineral quantification by XRD is difficult when mixed-layer clay minerals and discrete clay types are both present. New procedures for peak decomposition and pattern simulation offer increased opportunities to obtain mineral abundance estimates. This proposed methodological sequence, for quantitative representation (QR) of complex clay samples, involves: (1) determination of layer type, mixed-layer proportion and order (R); (2) simulation of XRD patterns using MULCALC, an adaptation of NEWMOD; and (3) interpretation of the clay assemblage by fitting the whole pattern with CLAY++, a statistical program. The product is a QR of individual phases or a summation of layer types. The absence of quantitative reference standards means results cannot be checked for accuracy, but the statistical fit is highly reproducible and less prone to operator error. The QRs may be obtained with simulated or actual reference mineral patterns in the database. Results for freshwater marsh samples illustrate the approach.






