9 results
Bioenergetic changes and mitochondrial dysfunction in mania versus euthymia in bipolar disorder type I
- A. Giménez-Palomo, M. Guitart-Mampel, G. Garrabou, X. Alsina-Restoy, A. Meseguer, L. Colomer, G. Roqué, F. J. García-García, E. Tobías, J. Moisés, M. Valentí, E. Vieta, I. Pacchiarotti
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S692-S693
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Current evidence has hypothesized the involvement of mitochondrial dysfunction during the acute episodes of BD compared to symptomatic remission. So far, no studies have compared mitochondrial and bioenergetic functions both in-vivo (respiratory parameters) and ex-vivo (cellular respiration) in different phases of the disease in the same individuals.
ObjectivesThis multidisciplinary pilot study aims at assessing bioenergetic and mitochondrial intra-individual differences between manic and euthymic states.
MethodsFour patients with a manic episode admitted to our acute psychiatric ward were recruited. Bioenergetic parameters were measured at admission (T0) and after symptomatic remission (T1).
At admission (T0) and before discharge (T1), HAMD and YMRS total scores were obtained. For the assessment of cellular respiration, polymorphonuclear cells were obtained by a Ficoll density gradient centrifugation procedure. To determine oxygen consumption (at T0 and T1), a million of living peripheral blood mononuclear cells (PBMC) were used. High-resolution respirometry was performed at 37°C by polarographic oxygen sensors in a two-chamber Oxygraph-2k system.
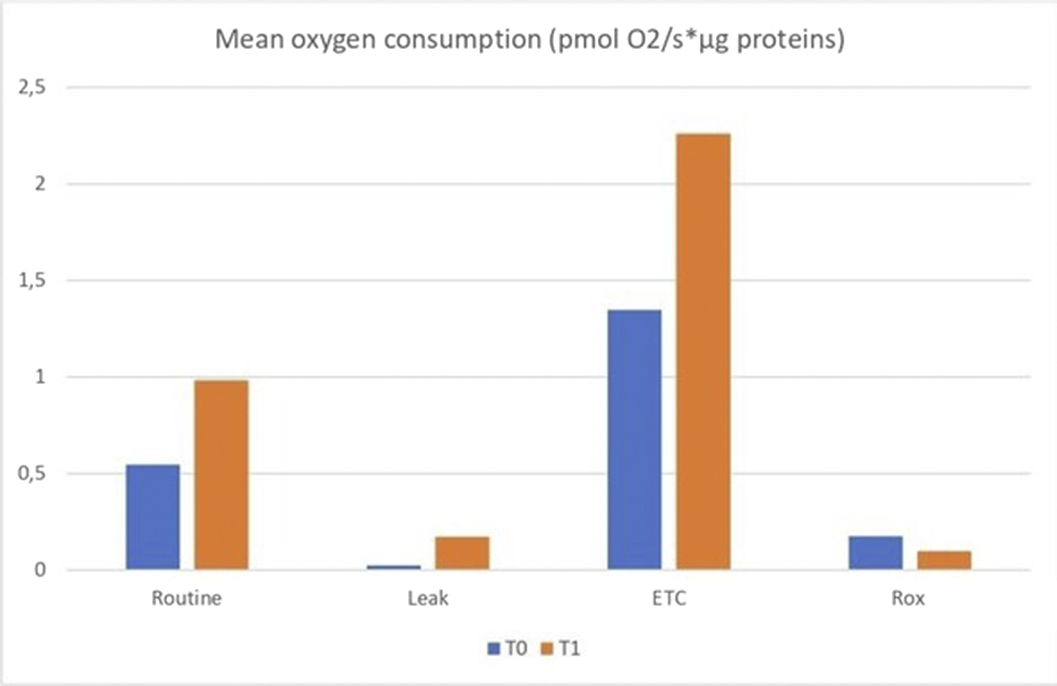
Specific oxygen uptakes (Routine: basal oxygen consumption; Proton Leak: oxygen consumption not coupled to ATP synthesis; and ETC: maximal capacity of the electron transport chain) rates were obtained using mitochondrial chain inhibitors and uncouplers. Oxygen consumption was normalized for protein concentration. Results are expressed as picomoles of oxygen per millilitre (pmol O2/s*μg prot).
Also, a constant work rate exercise test was performed on a cycle ergometer and basal and effort respiratory variables were measured.
Statistical analysis was performed with the SPSS v. 25.0 and GraphPad. Results were expressed as means and SD. Nonparametric tests (Mann–Whitney, Pearson) were used to determine differences (significant at p value <0.05).
ResultsOne patient was a man and three patients were women, with a mean age of 28 years old. HAMD initial and final mean scores were 11.0 and 7.0, and mean YMRS scores were 21.5 and 7.0 respectively.
Results from mitochondrial oxygen consumption revealed that mean basal oxygen consumption tended to be higher in T1 (0.98±0.45) than in T0, and maximal respiratory capacity was significantly increased in T1 (2.26±0.33; p=0.028) compared to T0.
Mean lactate levels and pH levels were similar in T0 and T1. Scales scores were not correlated to different pH or lactate changes after the effort task. Higher initial oxygen consumption was significantly correlated to higher maximal capacity (p<0.05) in T0 and T1.
Image:
 Conclusions
ConclusionsOur preliminary results suggest that mania could imply lower oxygen consumption capacity, which should be confirmed in future studies. A bigger study is planned to determine changes in bioenergetic patterns and capacity for aerobic response in manic and depressive episodes.
Disclosure of InterestNone Declared
Unplanned Pregnancy in women with mental disorder
- A. Roca Lecumberri, E. Gelabert, A. Torres Giménez, E. Solé, S. Andrés-Perpiñá, E. Roda, C. Lopez, C. Naranjo, L. Garcia-Esteve
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S331-S332
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Few studies have investigated the level of planning of pregnancy among women with mental disorder and associated risk factors.
ObjectivesThe purpose of this study was to determine the associated factors to UP and psychopathological consequences.
MethodsA cross sectional study was conducted at the Perinatal Mental Health Unit of the Hospital Clínic in Barcelona. The total sample comprised 675 consecutive pregnant women with diagnosis of mental disorder (DSM-IV criteria), seen between January 2006 and December 2018. Clinical, psychometric and socio-demographic variables were collected at the first visit. Pregnancy planning was assessed by a question “Was this pregnancy planned?” with three possible answers: 1) Yes, it was planned and has been well received; 2) No, it was not planned but it has been well received; and 3) No, it was an accident. Response 1 was coded as “planned pregnancy” and responses 2 and 3 as “Unplanned Pregnancy”.
Results38.4% of the sample had an UP. Younger age, lower levels of education, Latin-American population, multiparity, financials problems and poor relationship with the partner were associated with UP in women with mental disorder. The mean EPDS and STAI scores and the presence of self-harming thoughts were significantly higher in women with UP.
ConclusionsUP was associated with more depressive and anxious symptoms and more self-harming thoughts. It is necessary to promote reproductive health care for women with mental disorders and to take into account their reproductive life plan, especially in those with risk factors described.
DisclosureNo significant relationships.
Mother-Baby Day Hospital (MBDH): preliminary results of effectiveness of multidisciplinary intensive intervention for women with postpartum affective/anxiety disorder
- E. Gelabert, A. Torres Giménez, S. Andrés-Perpiñá, C. Naranjo, E. Roda, L. Garcia-Esteve, A. Roca Lecumberri
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S331
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women experiencing postpartum mental illness have unique needs. Psychiatric Mother Baby Units (MBUs) can provide specialist in-patient care for mothers without separation from their baby. Since 2018, an innovative Mother-Baby Day Hospital (MBDH) have been developed and implemented in a public hospital in Spain, directed at the intensive, integral, and multidisciplinary treatment.
ObjectivesThe aim of the present study was to obtain preliminary data regarding its effectiveness in postpartum women with affective and anxiety disorders.
MethodsThirty-three mothers and their babies with affective or anxiety disorders attended to MBDH CLINIC-BCN participated in the study. All women were assessed at admission, discharge, and 3 months follow-up. Primary outcomes were depression (EPDS) and anxiety symptoms (STAI-S), mother-infant bonding (PBQ) and functional impairment (HoNOs).
ResultsAt discharge, 100% of women no longer met the full criteria for the main diagnosis (PSR≥5). Significant improvements from admission to discharge were achieved in depression and anxiety symptoms, mother infant bonding and functional impairment. Clinical significance was also calculated. After treatment, mothers had greater autonomy for care their babies. Similar results were observed at 3 months follow-up. The MBDH was rated by mothers as an excellent quality program and they would recommend it.
ConclusionsThis study found that multidisciplinary intervention at MBDH for postpartum women with affective or anxiety disorders is effective, not only for maternal psychopathology but also for maternal care and bonding. It is imperative to develop specialized devices that integrate the care of the dyad by professionals specialized in perinatal mental health.
DisclosureNo significant relationships.
Dissociative disorder following preeclampsia: A case report
- A. Giménez Palomo, M.L. Imaz, I. Pacchiarotti, A. Roca, E. Solé, L. Garcia-Esteve
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S650
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Preeclampsia is a new-onset hypertension with new-onset proteinuria after 20 weeks gestation. Scarce evidence regarding psychiatric effects of preeclampsia is available.
ObjectivesTo describe a case of a pregnant 24 year-old patient with a premature cesarean section in context of severe preeclampsia and dissociative symptoms.
MethodsPatient referred to a third-level hospital for cesarean section due to a severe preeclampsia at week 32, in whom magnesium sulfate, labetalol perfusion and betamethasone are started. In the puerperium period only labetalol up to 300 mg/6h is maintained.
ResultsDue to the appearance of pulsating headache and photophobia, a computerized tomography is conducted, showing bilateral insular and occipital hypodensity related to vasogenic edema. High blood pressure is maintained (177/121 mmHg) despite antihypertensive treatment. A magnetic resonance imaging and an ophthalmologic exam do not show significant abnormalities and blood pressure is stabilized with treatment. However, the patient refers new-onset auditory imperative hallucinations and suicide thoughts, being referred to our Acute Psychiatric Ward for clinical assessment and intervention. Treatment with risperidone 2 mg is started. The day after her admission, she does not refer psychotic symptoms, explaining depersonalization symptoms in the previous 5 days, seeing herself having to choose a knife to commit suicide. After discharge, she maintains reiterative dreams in which she falls down from a building, not presenting dissociative symptoms during the day.
ConclusionsFurther evidence regarding psychiatric effects of preeclampsia is needed in order to study the consequences of edema and pharmacological treatment. Blood pressure and psychiatric symptoms monitoring after preeclampsia should also be considered.
DisclosureNo significant relationships.
Neonatal and infant outcomes of clozapine exposure in pregnancy: A consecutive case series
- M.L. Imaz, S. Lera, B. Sureda, A. Roca, S. Andres, A. Giménez Palomo, E. Solé, A. Torres, L. Garcia-Esteve
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S479
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is a second-generation antipsychotic agent approved for treatment-resistant schizophrenia and risk reduction of recurrent suicidal behavior in schizophrenia and schizoaffective disorder. Given the known negative consequences of relapse of severe mental disorders for both mother and infant, the maintenance of clozapine during pregnancy is recommended.1 Studies of pregnancy regarding to clozapine have demonstrated a heterogenous range of neonatal and infant complications.2
ObjectivesTo evaluate neonatal and infants outcomes of clozapine exposure in pregnancy.
MethodsWe report three cases of infants exposed to clozapine politherapy throughout pregnancy. The dose range for all women on clozapine was 200-600 mg/day. Infants were evaluated between 4-6 months of chronological age with the Bayley-III infant development scale (BSID-III)3 and with the Alarme Détresse Bébé Scale (ADBB)4 for the detection of early-signs of withdrawal.
ResultsWomen remained stable during pregnancy but presented obesity and gestational diabetes. Clozapine Newborn were born to term by caesarean section due to breech presentation (N=2) or instrumental delivery due to loss of fetal well-being (N=1). They presented normal weight (3500-3800 gr). Two presented Apgarmin1-5 9/10 and one Apgarmin1-5 6/8 which showed lethargy and low alertness during the first weeks of life. All showed normal capacity for sociability, reciprocity and development of language and communication. However, one baby had scores in the low normal zone for cognition and another for motor skills.
ConclusionsThe infant’s risks of clozapine exposure during pregnancy should be discussed with women and weighed against those associated with other treatments and/or with untreated severe mental illness.
Prevalence of ADHD in chronic fatigue syndrome
- N. Sáez Francàs, J. Alegre, N. Calvo Piñero, J.A. Ramos Quiroga, E. Ruiz, B. Olivares, E. García Gíménez, M. Casas
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1574
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Chronic Fatigue Syndrome (CFS) is characterized by severe fatigue associated with pain, sleep disturbance, attentional impairment and headaches. Evidence points towards a prominent role for Central Nervous System in its pathogenesis, and alterations in serotoninergic and dopaminergic neurotransmission have been described.
Attention-deficit Hyperactivity Disorder (ADHD) courses with inattention, impulsivity, and hyperactivity. It affects children and persists into adulthood in 50% of patients. Dopamine transporter abnormalities lead to impaired neurotransmission of catecholaminergic frontal-subcortical-cerebellar circuits.
ObjectivesTo describe the prevalence of ADHD in a sample of CFS patients, and the clinical implications of the association.
AimsTo study the relationship between CFS and ADHD.
MethodsThe initial sample consisted of 142 patients, of whom 9 were excluded because of severe psychopathology or incomplete evaluation. All the patients (age 49 ± 87; 94,7 women) received CFS diagnoses according to Fukuda criteria. ADHD was assessed with a diagnostic interview (CAADID), ADHD Rating Scale and the scale WURS, for childhood diagnose. The scales FIS-40, HAD, STAI and Pluthik Risk of Suicide (RS) were administrated.
Results38 patients (28,8%) were diagnosed of childhood ADHD (4 combined, 22 hyperactive-impulsive, 12 inattentive) and persisted into adulthood in 28 (21,1%; 5 combined, 4 hyperactive-impulsive, 19 inattentive). There were no differences in Fukuda criteria profile and FIS-40 between groups. ADHD patients scored higher in HAD-Anxiety (9,88 ± 4,82 vs. 12,57 ± 3,49; p = 0,007), HAD-Depression (9,69 ± 4,84 vs. 12,04 ± 4,53; p = 0,023), STAI-E (30,55 ± 14,53 vs. 38,41 ± 11,35; p = 0,012), and RS (6,13 ± 3,48 vs. 8,49 ± 3,07; p = 0,002).
ConclusionsADHD is frequent in CFS patients and it is associated with more severe clinical profile.
P0242 - Spanish validation of the Index of spouse abuse
- L.L. Garcia-Esteve, A. Torres Gimenez, P. Navarro, M.J. Tarragona, E. Gelabert, Z. Herreras, T. Echeverria, S. Subira, C. Ascaso
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S371
-
- Article
-
- You have access Access
- Export citation
-
Background and Aim:
To assess the psychometric properties of the Spanish version of the Index of Spouse Abuse (ISA), and validate it against external criteria of intimate partner violence (IPV).
Methods:A case control, transversal study was designed. Spanish version of the ISA was administered to 405 women (223 controls and 182 IPV cases). Spanish items weights were developed. Internal consistency was assessed through Cronbach's alfa, and factor structure by means of principal component analysis (PCA). Receiver operating characteristic (ROC) analysis was used to validate the ISA against external criteria.
Results:PCA analysis yielded two factors that accounted the 69% of variance, and reproduced partially the original factors: physical (ISA-P) and non-physical (ISA-NP). Internal consistency coefficients oscillated between 0,88 and 0,98. For the ISA global score, the AUC value for detecting IPV was 0,99; and 0,89 for detecting physical IPV. The optimal cut-off scores were 13 for detecting IPV, and 15 for detecting physical IPV. For the ISA subscales, 6 was the optimal cut-off score for the ISA-P, and 13 was the optimal cut-off for the ISA-NP.
Conclusions:The Spanish version of the ISA is a valid and reliable instrument for detecting and measuring the intensity of the IPV in Spanish women population.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Characterization of cardiopulmonary function and cardiac muscarinic and adrenergic receptor density adaptation in C57BL/6 mice with chronic Trypanosoma cruzi infection
- N. N. ROCHA, S. GARCIA, L. E. D. GIMÉNEZ, C. C. Q. HERNÁNDEZ, J. F. V. SENRA, R. S. LIMA, F. CYRINO, E. BOUSKELA, M. B. P. SOARES, R. RIBEIRO DOS SANTOS, A. C. CAMPOS DE CARVALHO
-
- Journal:
- Parasitology / Volume 133 / Issue 6 / December 2006
- Published online by Cambridge University Press:
- 18 September 2006, pp. 729-737
-
- Article
- Export citation
-
Circulating antibodies in chagasic patients interact with myocardial β adrenergic and muscarinic cholinergic receptors, triggering intracellular signals that alter cardiac function along the course of the disease. However, until now, experimental data in models of chronically infected chagasic mice linking the effects on myocardial β adrenergic and muscarinic receptors to cardiopulmonary dysfunction is lacking. Thus, we studied C57BL/6 mice 8 months after intraperitoneal injection of 100 trypomastigote forms of the Colombian strain of T. cruzi. Uninfected mice, matched in age, were used as controls. Histopathological analyses (inflammation and fibrosis) and radio-ligand binding assays for estimation of muscarinic and adrenergic receptor density were performed in myocardium tissue samples. When compared to controls, infected mice had electrical conduction disturbances, diastolic dysfunction, lower O2 consumption and anaerobic threshold. In addition, hearts of chronic chagasic mice had intense inflammation and fibrosis, and decreased β adrenergic and increased muscarinic receptor densities than normal controls. Our data suggest that chronic T. cruzi infection causes alterations in cardiac receptor density and fibrosis deposition which can be associated with cardiac conduction abnormalities, diastolic dysfunction and lower exercise capacity, associating for the first time all these functional and histopathological alterations in chagasic mice.




