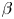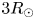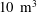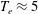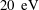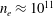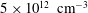15 results
311 Rib Fractures in Geriatric Trauma: A Review of 1,037 Cases at a Single Level I Trauma Center
- Forest Sheppard, Joseph D. Mack, Carolyne Falank, Bryan C Morse, Daniel C Cullinane, Joseph F Rappold, Julianne Ontengco, David Ciraulo
-
- Journal:
- Journal of Clinical and Translational Science / Volume 6 / Issue s1 / April 2022
- Published online by Cambridge University Press:
- 19 April 2022, pp. 54-55
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: Rib fractures are common traumatic thoracic injuries and are associated with high rates of morbidity and mortality. In those age ≥ 65, the rate of these complications double. This study sought to identify the extent to which injury-related predictors influence clinical outcomes in geriatric patients with rib fractures. METHODS/STUDY POPULATION: A retrospective 5-year review was performed of a single Level 1 Trauma center registry. Geriatric patients (≥65 years of age) diagnosed with rib fractures from January 1, 2014 to December 31, 2019 were included. The primary outcome of interest was in-hospital mortality. Secondary outcomes included hospital and intensive care unit length of stay (HLOS and ICU LOS, respectively) and discharge disposition, as a surrogate for loss of independence. Further, subgroup analysis based on number of rib fractures (i.e. <4 and ≥4 rib fractures) was performed. RESULTS/ANTICIPATED RESULTS: 2,134 adult trauma patients were admitted with at least one rib fracture. Of these, 1,037 (49%) were ≥ 65 years old. This cohort had a mean age of 78.6 years old, injury severity score (ISS) of 11.4, HLOS of 7.4 days and 29% required ICU care with mean ICU LOS of 1.9 days. Only 36% were discharged home compared to 64% who were discharged to a care facility and thus had a loss of independence. Overall mortality was 6.3%. Compared to survivors, non-survivors had a higher ISS (19.3 vs. 10.8, p = < 0.0001) and longer ICU LOS (7.1 vs. 6.5 days, p = 0.04). Analysis based on number of rib fractures showed that those with ≥4 rib fractures had significantly higher mortality (8% vs. 4%, p = 0.008), longer HLOS (8.7 vs. 6.1 days, p < 0.0001), longer ICU LOS (2.6 vs. 1.3 days, p < 0.0001), and significantly lower discharge to home (32% vs. 39%, p = 0.02). DISCUSSION/SIGNIFICANCE: To our knowledge, this is the largest single-center study of geriatric patients with rib fractures. In this study, the observed mortality in patients ≥65 years of age was 6.3% which represents a lower mortality rate than historically reported. Despite this, only 36% were able to be discharged directly to home.
Laminar and turbulent plasmoid ejection in a laboratory Parker Spiral current sheet
- Ethan E. Peterson, Douglass A. Endrizzi, Michael Clark, Jan Egedal, Kenneth Flanagan, Nuno F. Loureiro, Jason Milhone, Joseph Olson, Carl R. Sovinec, John Wallace, Cary B. Forest
-
- Journal:
- Journal of Plasma Physics / Volume 87 / Issue 4 / August 2021
- Published online by Cambridge University Press:
- 05 August 2021, 905870410
-
- Article
- Export citation
-
Quasi-periodic plasmoid formation at the tip of magnetic streamer structures is observed to occur in experiments on the Big Red Ball as well as in simulations of these experiments performed with the extended magnetohydrodynamics code, NIMROD. This plasmoid formation is found to occur on a characteristic time scale dependent on pressure gradients and magnetic curvature in both experiment and simulation. Single mode, or laminar, plasmoids exist when the pressure gradient is modest, but give way to turbulent plasmoid ejection when the system drive is higher, which produces plasmoids of many sizes. However, a critical pressure gradient is also observed, below which plasmoids are never formed. A simple heuristic model of this plasmoid formation process is presented and suggested to be a consequence of a dynamic loss of equilibrium in the high-$\beta$
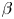 region of the helmet streamer. This model is capable of explaining the periodicity of plasmoids observed in the experiment and simulations, and produces plasmoid periods of 90 minutes when applied to two-dimensional models of solar streamers with a height of $3R_\odot$
region of the helmet streamer. This model is capable of explaining the periodicity of plasmoids observed in the experiment and simulations, and produces plasmoid periods of 90 minutes when applied to two-dimensional models of solar streamers with a height of $3R_\odot$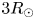 . This is consistent with the location and frequency at which periodic plasma blobs have been observed to form by Large Angle and Spectrometric Coronograph and Sun Earth Connection Coronal and Heliospheric Investigation instruments.
. This is consistent with the location and frequency at which periodic plasma blobs have been observed to form by Large Angle and Spectrometric Coronograph and Sun Earth Connection Coronal and Heliospheric Investigation instruments.
Safety of Using a Combinatorial Pharmacogenomic Test for Patients with Major Depressive Disorder in the GUIDED trial
- Sagar V. Parikh, Gabriela K. Khazanov, Michael E. Thase, Anthony J. Rothschild, Boadie W. Dunlop, Charles DeBattista, Charles R. Conway, Brent P. Forester, Richard C. Shelton, Matthew Macaluso, James Li, Kunbo Yu, Michael R. Jablonski, Stephanie Meek, John F. Greden
-
- Journal:
- CNS Spectrums / Volume 26 / Issue 2 / April 2021
- Published online by Cambridge University Press:
- 10 May 2021, pp. 169-170
-
- Article
-
- You have access Access
- Export citation
-
Background
Pharmacogenomic testing has emerged to aid medication selection for patients with major depressive disorder (MDD) by identifying potential gene-drug interactions (GDI). Many pharmacogenomic tests are available with varying levels of supporting evidence, including direct-to-consumer and physician-ordered tests. We retrospectively evaluated the safety of using a physician-ordered combinatorial pharmacogenomic test (GeneSight) to guide medication selection for patients with MDD in a large, randomized, controlled trial (GUIDED).
Materials and MethodsPatients diagnosed with MDD who had an inadequate response to ≥1 psychotropic medication were randomized to treatment as usual (TAU) or combinatorial pharmacogenomic test-guided care (guided-care). All received combinatorial pharmacogenomic testing and medications were categorized by predicted GDI (no, moderate, or significant GDI). Patients and raters were blinded to study arm, and physicians were blinded to test results for patients in TAU, through week 8. Measures included adverse events (AEs, present/absent), worsening suicidal ideation (increase of ≥1 on the corresponding HAM-D17 question), or symptom worsening (HAM-D17 increase of ≥1). These measures were evaluated based on medication changes [add only, drop only, switch (add and drop), any, and none] and study arm, as well as baseline medication GDI.
ResultsMost patients had a medication change between baseline and week 8 (938/1,166; 80.5%), including 269 (23.1%) who added only, 80 (6.9%) who dropped only, and 589 (50.5%) who switched medications. In the full cohort, changing medications resulted in an increased relative risk (RR) of experiencing AEs at both week 4 and 8 [RR 2.00 (95% CI 1.41–2.83) and RR 2.25 (95% CI 1.39–3.65), respectively]. This was true regardless of arm, with no significant difference observed between guided-care and TAU, though the RRs for guided-care were lower than for TAU. Medication change was not associated with increased suicidal ideation or symptom worsening, regardless of study arm or type of medication change. Special attention was focused on patients who entered the study taking medications identified by pharmacogenomic testing as likely having significant GDI; those who were only taking medications subject to no or moderate GDI at week 8 were significantly less likely to experience AEs than those who were still taking at least one medication subject to significant GDI (RR 0.39, 95% CI 0.15–0.99, p=0.048). No other significant differences in risk were observed at week 8.
ConclusionThese data indicate that patient safety in the combinatorial pharmacogenomic test-guided care arm was no worse than TAU in the GUIDED trial. Moreover, combinatorial pharmacogenomic-guided medication selection may reduce some safety concerns. Collectively, these data demonstrate that combinatorial pharmacogenomic testing can be adopted safely into clinical practice without risking symptom degradation among patients.
FundingMyriad Neuroscience/Assurex Health
Response to the Specialist Cheesemakers Association on ‘Microbiological quality of raw drinking milk and unpasteurised dairy products: results from England 2013–2019’
- J. McLauchlin, H. Aird, E. Forester, F. Jørgensen, C. Willis
-
- Journal:
- Epidemiology & Infection / Volume 149 / 2021
- Published online by Cambridge University Press:
- 19 April 2021, e112
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Facing the change together: reflections of coping and resilience from American geriatric psychiatrists during COVID-19
- Carmen Black Parker, Malcolm P Forbes, Ipsit V Vahia, Brent P Forester, Dilip V Jeste, Charles F Reynolds
-
- Journal:
- International Psychogeriatrics / Volume 32 / Issue 10 / October 2020
- Published online by Cambridge University Press:
- 23 July 2020, pp. 1107-1111
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Microbiological quality of raw drinking milk and unpasteurised dairy products: results from England 2013–2019
- Part of
- J. McLauchlin, H. Aird, A. Elliott, E. Forester, F. Jørgensen, C. Willis
-
- Journal:
- Epidemiology & Infection / Volume 148 / 2020
- Published online by Cambridge University Press:
- 14 May 2020, e135
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The aim of this study was to review microbiology results from testing >2500 raw drinking milk and dairy products made with unpasteurised milk examined in England between 2013 and 2019. Samples were collected as part of incidents of contamination, investigation of infections or as part of routine monitoring and were tested using standard methods for a range of both pathogens and hygiene indicators. Results from testing samples of raw cow's milk or cheese made from unpasteurised milk for routine monitoring purposes were overall of better microbiological quality than those collected during incident or investigations of infections. Results from routine monitoring were satisfactory for 62% of milks, 82% of cream, 100% of ice-cream, 51% of butter, 63% of kefir and 79% of cheeses, with 5% of all samples being considered potentially hazardous. Analysis of data from cheese demonstrated a significant association between increasing levels of indicator Escherichia coli with elevated levels of coagulase positive staphylococci and decreased probability of isolation of Shiga toxin-producing E. coli. These data highlight the public health risk associated with these products and provide further justification for controls applied to raw drinking milk and dairy products made with unpasteurised milk.
150 HAM-D6 Outcomes in a Randomized, Controlled Trial Evaluating the Utility of Combinatorial Pharmacogenomics in Depression
- Boadie W. Dunlop, Sagar V. Parikh, Maitrey Patel, Anthony J. Rothschild, Michael E. Thase, Charles DeBattista, Charles R. Conway, Brent P. Forester, Richard C. Shelton, Matthew Macaluso, James Li, Krystal Brown, Lisa Brown, Michael R. Jablonski, John F. Greden
-
- Journal:
- CNS Spectrums / Volume 25 / Issue 2 / April 2020
- Published online by Cambridge University Press:
- 24 April 2020, pp. 295-296
-
- Article
-
- You have access Access
- Export citation
-
Background:
The Genomics Used to Improve DEpresssion Decisions (GUIDED) trial assessed outcomes associated with combinatorial pharmacogenomic (PGx) testing in patients with major depressive disorder (MDD). Analyses used the 17-item Hamilton Depression (HAM-D17) rating scale; however, studies demonstrate that the abbreviated, core depression symptom-focused, HAM-D6 rating scale may have greater sensitivity toward detecting differences between treatment and placebo. However, the sensitivity of HAM-D6 has not been tested for two active treatment arms. Here, we evaluated the sensitivity of the HAM-D6 scale, relative to the HAM-D17 scale, when assessing outcomes for actively treated patients in the GUIDED trial.
Methods:Outpatients (N=1,298) diagnosed with MDD and an inadequate treatment response to >1 psychotropic medication were randomized into treatment as usual (TAU) or combinatorial PGx-guided (guided-care) arms. Combinatorial PGx testing was performed on all patients, though test reports were only available to the guided-care arm. All patients and raters were blinded to study arm until after week 8. Medications on the combinatorial PGx test report were categorized based on the level of predicted gene-drug interactions: ‘use as directed’, ‘moderate gene-drug interactions’, or ‘significant gene-drug interactions.’ Patient outcomes were assessed by arm at week 8 using HAM-D6 and HAM-D17 rating scales, including symptom improvement (percent change in scale), response (≥50% decrease in scale), and remission (HAM-D6 ≤4 and HAM-D17 ≤7).
Results:At week 8, the guided-care arm demonstrated statistically significant symptom improvement over TAU using HAM-D6 scale (Δ=4.4%, p=0.023), but not using the HAM-D17 scale (Δ=3.2%, p=0.069). The response rate increased significantly for guided-care compared with TAU using both HAM-D6 (Δ=7.0%, p=0.004) and HAM-D17 (Δ=6.3%, p=0.007). Remission rates were also significantly greater for guided-care versus TAU using both scales (HAM-D6 Δ=4.6%, p=0.031; HAM-D17 Δ=5.5%, p=0.005). Patients taking medication(s) predicted to have gene-drug interactions at baseline showed further increased benefit over TAU at week 8 using HAM-D6 for symptom improvement (Δ=7.3%, p=0.004) response (Δ=10.0%, p=0.001) and remission (Δ=7.9%, p=0.005). Comparatively, the magnitude of the differences in outcomes between arms at week 8 was lower using HAM-D17 (symptom improvement Δ=5.0%, p=0.029; response Δ=8.0%, p=0.008; remission Δ=7.5%, p=0.003).
Conclusions:Combinatorial PGx-guided care achieved significantly better patient outcomes compared with TAU when assessed using the HAM-D6 scale. These findings suggest that the HAM-D6 scale is better suited than is the HAM-D17 for evaluating change in randomized, controlled trials comparing active treatment arms.
Funding Acknowledgements:Assurex Health, Inc.
49 Combinatorial Pharmacogenomics to Guide Treatment Selection for Major Depressive Disorder: A Large, Blinded, Randomized Controlled Trial
- John F. Greden, Anthony J. Rosthschild, Michael Thase, Boadie W. Dunlop, DMH Charles DeBattista, Charles R. Conway, Brent P. Forester, Francis M. Mondimore, Richard C. Shelton, James Li, Alexa Gilbert, Lindsey Burns, Michael Jablonski, Bryan Dechairo, Sagar Parikh
-
- Journal:
- CNS Spectrums / Volume 24 / Issue 1 / February 2019
- Published online by Cambridge University Press:
- 12 March 2019, pp. 202-203
-
- Article
-
- You have access Access
- Export citation
-
Background
Major depressive disorder (MDD) is a leading cause of disease burden worldwide, with lifetime prevalence in the United States of 17%. Here we present the results of the first prospective, large-scale, patient- and rater-blind, randomized controlled trial evaluating the clinical importance of achieving congruence between combinatorial pharmacogenomic (PGx) testing and medication selection for MDD.
Methods1,167 outpatients diagnosed with MDD and an inadequate response to ≥1 psychotropic medications were enrolled and randomized 1:1 to a Treatment as Usual (TAU) arm or PGx-guided care arm. Combinatorial PGx testing categorized medications in three groups based on the level of gene-drug interactions: use as directed, use with caution, or use with increased caution and more frequent monitoring. Patient assessments were performed at weeks 0 (baseline), 4, 8, 12 and 24. Patients, site raters, and central raters were blinded in both arms until after week 8. In the guided-care arm, physicians had access to the combinatorial PGx test result to guide medication selection. Primary outcomes utilized the Hamilton Depression Rating Scale (HAM-D17) and included symptom improvement (percent change in HAM-D17 from baseline), response (50% decrease in HAM-D17 from baseline), and remission (HAM-D17<7) at the fully blinded week 8 time point. The durability of patient outcomes was assessed at week 24. Medications were considered congruent with PGx test results if they were in the ‘use as directed’ or ‘use with caution’ report categories while medications in the ‘use with increased caution and more frequent monitoring’ were considered incongruent. Patients who started on incongruent medications were analyzed separately according to whether they changed to congruent medications by week8.
ResultsAt week 8, symptom improvement for individuals in the guided-care arm was not significantly different than TAU (27.2% versus 24.4%, p=0.11). However, individuals in the guided-care arm were more likely than those in TAU to achieve remission (15% versus 10%; p<0.01) and response (26% versus 20%; p=0.01). Remission rates, response rates, and symptom reductions continued to improve in the guided-treatment arm until the 24week time point. Congruent prescribing increased to 91% in the guided-care arm by week 8. Among patients who were taking one or more incongruent medication at baseline, those who changed to congruent medications by week 8 demonstrated significantly greater symptom improvement (p<0.01), response (p=0.04), and remission rates (p<0.01) compared to those who persisted on incongruent medications.
ConclusionsCombinatorial PGx testing improves short- and long-term response and remission rates for MDD compared to standard of care. In addition, prescribing congruency with PGx-guided medication recommendations is important for achieving symptom improvement, response, and remission for MDD patients.
Funding Acknowledgements: This study was supported by Assurex Health, Inc.
GD02: An international consensus study to identify quality indicators for ambulatory emergency care
- S. Berthelot, E. Lang, M. Émond, M. Mallet, H. T. Stelfox, R. Lavergne, F. Légaré, L. Bissonnette, S. Blais, J-C Forest, E. Mercier, C. Guimont, L. Moore
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, pp. S62-S63
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Redirecting low acuity patients from emergency departments to primary care walk-in clinics has been identified as a priority by many health authorities. Promoting family physicians for the management of ambulatory patients with urgent health concerns reflects the assumption that primary care facilities can offer high-quality and more affordable ambulatory emergency care. However, no performance assessment framework has been developed for ambulatory emergency care and consequently, quality of care provided in these alternate settings has never been formally compared. Primary objective: To identify structure, process and outcome indicators for ambulatory emergency care. Methods: We will identify and develop quality indicators (QIs) for ambulatory emergency care using a RAND/UCLA Appropriateness Method (RAM) composed of three different steps. First, we will perform a scoping literature review to inventory 1) all previously recommended QIs assessing care provided to ambulatory emergency patients in the ED or the primary care settings; 2) all conditions evaluated with the retrieved QIs; and 3) all outcomes measured by the same QIs. Second, a steering committee composed of the research team and of international experts in performance assessment in emergency and primary care will be presented with the lists of QI-related conditions and outcomes. They will be asked to identify potential outcome indicators for ambulatory emergency care by generating any relevant combinations of one condition and one outcome (e.g. acute asthma exacerbation/re-consultation). Committee members will be given the latitude to use and pair any conditions or outcomes not included in the lists as long as they think the resulting indicators are compatible with the study objectives. Using a structured nominal group approach, they will combine their suggestions and refine the list of potential QIs. This list of potential outcome indicators composed of pairs “condition/outcome” will be merged with the list of already published QIs identified during the literature review. Third, as per the RAM standards, we will assemble an international multidisciplinary panel (n=20) of patients, emergency and primary care providers, researchers and decision makers, after recommendations from international emergency and primary care associations, and from the Canadian Strategy for Patient-Oriented Research (SPOR) Support Units. Through iterative rounds of ratings using both web-based survey tools and videoconferencing, panelists will independently assess all candidate QIs. They will be asked to rate on a nine-level scale to what extent each QI is a relevant and useful measure of ambulatory emergency care quality. From one round to the next, QIs with a median panelist rating score of one to three will be excluded. Those with a median score of seven or more will be automatically included in the final list. QIs with median score of four to six will be retained for future deliberations among the panelists. Rounds of ratings will be conducted until all QIs are classified. Impact: The QIs identified will be used to develop a performance assessment framework for ambulatory emergency care. This will represent an essential step toward testing the assumption that EDs and primary care walk-in clinics provide equivalent care quality to low acuity patients.
The Wisconsin Plasma Astrophysics Laboratory
- Part of
- C. B. Forest, K. Flanagan, M. Brookhart, M. Clark, C. M. Cooper, V. Désangles, J. Egedal, D. Endrizzi, I. V. Khalzov, H. Li, M. Miesch, J. Milhone, M. Nornberg, J. Olson, E. Peterson, F. Roesler, A. Schekochihin, O. Schmitz, R. Siller, A. Spitkovsky, A. Stemo, J. Wallace, D. Weisberg, E. Zweibel
-
- Journal:
- Journal of Plasma Physics / Volume 81 / Issue 5 / October 2015
- Published online by Cambridge University Press:
- 07 August 2015, 345810501
-
- Article
- Export citation
-
The Wisconsin Plasma Astrophysics Laboratory (WiPAL) is a flexible user facility designed to study a range of astrophysically relevant plasma processes as well as novel geometries that mimic astrophysical systems. A multi-cusp magnetic bucket constructed from strong samarium cobalt permanent magnets now confines a
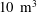 $10~\text{m}^{3}$, fully ionized, magnetic-field-free plasma in a spherical geometry. Plasma parameters of
$10~\text{m}^{3}$, fully ionized, magnetic-field-free plasma in a spherical geometry. Plasma parameters of 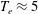 $T_{e}\approx 5$ to
$T_{e}\approx 5$ to 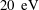 $20~\text{eV}$ and
$20~\text{eV}$ and 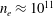 $n_{e}\approx 10^{11}$ to
$n_{e}\approx 10^{11}$ to 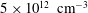 $5\times 10^{12}~\text{cm}^{-3}$ provide an ideal testbed for a range of astrophysical experiments, including self-exciting dynamos, collisionless magnetic reconnection, jet stability, stellar winds and more. This article describes the capabilities of WiPAL, along with several experiments, in both operating and planning stages, that illustrate the range of possibilities for future users.
$5\times 10^{12}~\text{cm}^{-3}$ provide an ideal testbed for a range of astrophysical experiments, including self-exciting dynamos, collisionless magnetic reconnection, jet stability, stellar winds and more. This article describes the capabilities of WiPAL, along with several experiments, in both operating and planning stages, that illustrate the range of possibilities for future users.
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Harmonic resonant filters for power electronics
- G. Daveau, Ch. Joubert, F. Forest
-
- Journal:
- The European Physical Journal - Applied Physics / Volume 40 / Issue 1 / October 2007
- Published online by Cambridge University Press:
- 21 September 2007, pp. 113-117
- Print publication:
- October 2007
-
- Article
- Export citation
-
The object of this work is to report a passive filter structure dedicated for power applications. The structure is based on a series combination of elementary notch filters resonating at harmonic frequencies of a base frequency (switching frequency of a converter). A calculation of values of the components used for a given performance is presented. In addition, energy study comparing the behavior of this new structure with that of a traditional LC filter shows that the same performances can be achieved with the 50% volume reduction.
Ostracodes as Hydrologic Indicators in Springs, Streams and Wetlands: A Tool for Environmental and Paleoenvironmental Assessment
- Alison J. Smith, Jesse W. Davis, Donald F. Palmer, Richard M. Forester, B. Brandon Curry
-
- Journal:
- The Paleontological Society Papers / Volume 9 / November 2003
- Published online by Cambridge University Press:
- 21 July 2017, pp. 203-222
- Print publication:
- November 2003
-
- Article
- Export citation
-
Although the majority of publications on extant nonmarine ostracode species in North America are concerned with lacustrine settings, many species that are potentially valuable as indicators of water quality changes live in non-lacustrine settings. Ostracode distributions in 157 springs, wetlands and streams in the United States are examined here in order to assess 1) species richness, 2) association with physical and chemical parameters of their habitats and 3) the presence of potentially useful biomonitors and environmental sentinels. The 157 non-lacustrine sites are a subset of a large database (North American Non-marine Ostracode Database: NANODe version 1) consisting of 611 mostly lacustrine sites with ostracode species, presence-absence data, hydrochemistry and climate data (Forester et al., in review). Of the 89 species represented in NANODe version 1, 51 species are found in springs, 59 species are found in wetlands and only 15 species are found in streams. Many species are found in at least two of these habitats and some in all three. Principal Components Analysis of these 157 sites indicates that 71% of the variance is explained by salinity (total ionic concentration), alkalinity and temperature, a result consistent with previously published analyses of natural water. Cluster analysis shows that spring species are most strongly tied to temperature, whereas wetlands and streams are most strongly tied to ionic composition. Three species are found to be potentially valuable biomonitors: Cavernocypris wardi in springs, Fabaeformiscandona rawsoni in wetlands and Physocypria globula in streams.
Numerical study of crystalline plasticity: measurements of the heterogeneities due to grain boundaries under small strains
- F. Barbe, S. Forest, S. Quilici, G. Cailletaud
-
- Journal:
- Revue de Métallurgie – International Journal of Metallurgy / Volume 100 / Issue 9 / September 2003
- Published online by Cambridge University Press:
- 17 November 2003, pp. 815-823
- Print publication:
- September 2003
-
- Article
- Export citation
-
A finite element 3D polycrystalline aggregate made of 216 grains is subjected to a mean axial deformation up to 1%. The heterogeneities inside the polycrystal are due to the crystallographic orientations of the grains - this appears at the scale of the mean responses per grain - and to the local interaction between neighbouring grains - this appears at the intragranular scale. The intragranular heterogeneity is measured as a function of the distance to the grain boundary, inside a single grain and for all the points of the microstructure. It is characterized by dispersions of the local responses due to grain boundaries. These measurements correspond to dispersions - variances -; the statistical errors have also been determined.
Diagnostic depressive symptoms of the mixed bipolar episode
- F. CASSIDY, E. AHEARN, E. MURRY, K. FOREST, B. J. CARROLL
-
- Journal:
- Psychological Medicine / Volume 30 / Issue 2 / March 2000
- Published online by Cambridge University Press:
- 01 March 2000, pp. 403-411
-
- Article
- Export citation
-
Background. There is not yet consensus on the best diagnostic definition of mixed bipolar episodes. Many have suggested the DSM-III-R/-IV definition is too rigid. We propose alternative criteria using data from a large patient cohort.
Methods. We evaluated 237 manic in-patients using DSM-III-R criteria and the Scale for Manic States (SMS). A bimodally distributed factor of dysphoric mood has been reported from the SMS data. We used both the factor and the DSM-III-R classifications to identify candidate depressive symptoms and then developed three candidate depressive symptom sets. Using ROC analysis we determined the optimal threshold number of symptoms in each set and compared the three ROC solutions. The optimal solution was tested against the DSM-III-R classification for cross-validation.
Results. The optimal ROC solution was a set, derived from both the DSM-III-R and the SMS, and the optimal threshold for diagnosis was two or more symptoms. Applying this set iteratively to the DSM-III-R classification produced the identical ROC solution. The prevalence of mixed episodes in the cohort was 13·9% by DSM-III-R, 20·2% by the dysphoria factor and 27·4% by the new ROC solution.
Conclusions. A diagnostic set of six dysphoric symptoms (depressed mood, anhedonia, guilt, suicide, fatigue and anxiety), with a threshold of two symptoms, is proposed for a mixed episode. This new definition has a foundation in clinical data, in the proved diagnostic performance of the qualifying symptoms, and in ROC validation against two previous definitions that each have face validity.