100 results
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
Searching for bridges between psychopathology and real-world functioning in first-episode psychosis: a network analysis from the OPTiMiSE trial
- F. Dal Santo, E. Fonseca-Pedrero, M. P. García-Portilla, L. González-Blanco, P. A. Sáiz, S. Galderisi, G. M. Giordano, J. Bobes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S262-S263
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Network analysis has been used to explore the interplay between psychopathology and functioning in psychosis, but no study has used dedicated statistical techniques to focus on the bridge symptoms connecting these domains.
ObjectivesThe current study aims to estimate the network of depressive, negative, and positive symptoms, general psychopathology, and real-world functioning in people with first-episode schizophrenia or schizophreniform disorder, focusing on bridge nodes.
MethodsBaseline data from the OPTiMiSE trial were analysed. The sample included 446 participants (age 40.0±10.9 years, 70% males). The network was estimated with a Gaussian graphical model (GGM), using scores on individual items of the Positive and Negative Syndrome Scale (PANSS), the Calgary Depression Scale for Schizophrenia (CDSS), and the Personal and Social Performance (PSP) scale. Stability, strength centrality, expected influence (EI), predictability, and bridge centrality statistics were computed. The top 20% scoring nodes on bridge strength were selected as bridge nodes.
ResultsNodes from different rating scales assessing similar psychopathological and functioning constructs tended to cluster together in the estimated network (Fig. 1). The most central nodes (EI) were Delusions, Emotional Withdrawal, Depression, and Depressed Mood. Bridge nodes included Depression, Conceptual Disorganisation, Active Social Avoidance, Delusions, Stereotyped Thinking, Poor Impulse Control, Guilty Feelings, Unusual Thought Content, and Hostility. Most of the bridge nodes belonged to the general psychopathology subscale of the PANSS. Depression (G6) was the bridge node with the highest value.
Image:
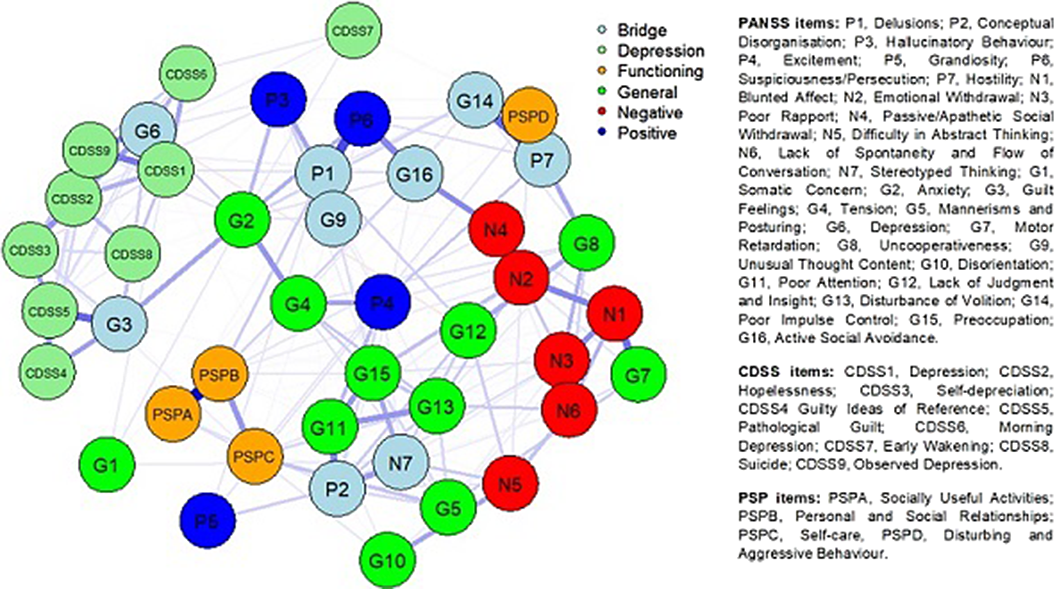 Conclusions
ConclusionsThe current study provides novel insights for understanding the complex phenotype of psychotic disorders and the mechanisms underlying the development and maintenance of comorbidity and functional impairment after psychosis onset.
Disclosure of InterestNone Declared
Analysis of the predictive potential of good clinical response of plasma levels of clozapine in patients with resistant schizophrenia in an area of southern Spain
- L. I. Muñoz-Manchado, F. González-Saiz, J. I. Pérez-Revuelta, N. Laherrán-Cantera, R. J. Pardo-Velasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Resistant schizophrenia is a schizophrenia subtype characterized by a non-ability to respond to an appropriate antipsychotic treatment in dosage and duration by the patients. These patients show a lower prognostic and symptomatology. The unique drug which has shown efficacy for resistant schizophrenia treatment is clozapine, which is effective in suicide and aggressive behaviour prevention too. Whereas clozapine has numerous and serious adverse effects such as agranulocytosis risk. Because of this, and for guaranteeing an accurate diagnosis of resistant schizophrenia, distinguishing this from pseudo-resistance due to a poor tracing of schizophrenia, clozapine’s plasmatic levels monitoring is recommended in Spain by many clinical practise-guidelines.
ObjectivesThis studio has the objective of determining if altered clozapine’s plasmatic levels have predictive potential of therapeutical response and answering what clinical and sociodemographic variables are associated to these anormal plasmatic levels.
MethodsIn this work, a cross-sectional observational study was carried out in which clinical and sociodemographic data obtained by the Mental Health Unit of the Jerez de la Frontera University Hospital were collected within the research project entitled: "Role of social cognition as a factor psychosocial functioning of the schizophrenic patient” (ECOFUN), of all the participating patients (in total the sample was 141 patients, of which 40 are in treatment with clozapine).
ResultsThe sample of patients has a mean age of 44 years and medium-high educational levels. The vast majority are men and do not currently consume substances of abuse, and when this consumption occurs, tobacco and alcohol are the most consumed substances. Their total scores on the PANSS and Markova Barrios scales are generally very disparate, but with average values of 55 and 16. It has been obtained as results that there is no significant statistical correlation between the plasma levels of clozapine and the values of the PANSS scale and its subscales in the patients. On the other hand, patients treated with clozapine would present clinical and sociodemographic characteristics practically identical to those of patients treated with other antipsychotics, especially their values on the PANSS scale. In addition, plasma levels of clozapine are correlated, although not significantly, with an improvement in the positive symptomatology of schizophrenia.
ConclusionsAs a conclusion, unusually higher values of clozapine are correlated significantly with lower values in positive symptomatology in schizophrenia, but plasmatic levels are not correlated significantly with values of PANSS scale.
Disclosure of InterestNone Declared
Gut permeability and low-grade inflammation in bipolar disorder
- M. Couce, G. Paniagua, L. González-Blanco, A. García-Fernández, C. Martínez-Cao, P. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S385-S386
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Systemic inflammation has been increasingly related to bipolar disorder -BD- (Tanaka et al. Neurosci Res 2017;115 59-63). Intestinal bacterial translocation has been postulated as one of the causes of this inflammation (Nguyen et al. J Psychiatr Res 2018;99 50-61). A possible pathway is through the lipopolysaccharide, which is presented to CD14 through lipopolysaccharide binding protein (LBP) leading to a release of systemic inflammatory markers like C-reactive protein (CPR) (Funda et al. Infect Immun 2001;69 3772-81).
Objectives1) Describe gut permeability in patients with BD through the determination of intestinal inflammatory markers (LBP, sCD14) in plasma; 2) Analyze variables associated with intestinal inflammation.
MethodsCross-sectional study of 38 patients with BD [mean age=45.50 (SD=10.93; range 23-68); males=15 (39.5%)], recruited from mental health outpatient clinics in Oviedo (Spain).
Assessment: Pro-inflammation biomarkers [CRP (mg/dL), Erythrocyte Sedimentation Rate (ESR) (mm/h), Neutrophil/Lymphocyte, Monocyte/Lymphocyte, Platelet/Lymphocyte and Systemic Immune Inflammation Indexes]. Indirect markers of intestinal bacterial translocation [LBP, soluble CD14 (sCD14)]. Dichotomous variables were created for LBP, considering LBP ≥15 μg/dL as increased gut permeability; and for CPR, considering CRP≥0.3 as systemic inflammation. Metabolic syndrome [ATPIII criteria: glucose, HDL, triglycerides (mg/dl), arterial pressure (mmHg), abdominal circumference (cm)], body mass index (BMI) (kg/m2), smoking, cannabis or alcohol use.
Statistical analyses: t-Student test, multiple linear regression analyses.
ResultsAverage LBP was 14.60 μg/dL (SD=6.4) and 15 patients (39.5%) had increased gut permeability. Moreover, average CPR was 0.40 mg/dL (SD=0.58) and 16 patients (47.1%) showed systemic inflammation. There were no patients with increased levels of sCD14.
Associations were found between LBP and CPR (r=0.357; p=0.032), cannabis use in the last month (t=-2.293; p=0.029), BMI (r=0.433; p=0.008) and abdominal obesity (t=3.006; p=0.005); but no with age or sex.
Subsequently, a multiple linear regression model for LBP was calculated with variables previously mentioned, and age (based on expert criteria). The overall regression was statistically significant (R2=0.49, F=9.273, p<0.001). It was found that CPR, abdominal obesity, and cannabis use in the last month significantly predicted LBP levels (table 1).
Table 1. Multiple linear regression analyses to LBP B SE β t p CPR 4.842 1.529 0.439 3.167 0.004 Abdominal obesity 4.810 1.849 0.362 2.601 0.014 Cannabis use -5.048 2.273 -0.296 -2.221 0.034 ConclusionsMore than one third of patients with BD had increased gut permeability. Almost 50% had systemic inflammation. Intestinal permeability was directly related to abdominal obesity and systemic inflammation, but inversely related to cannabis use.
Disclosure of InterestNone Declared
The response to unfolded proteins in schizophrenia and bipolar disorder
- C. Cachán, I. M. Valle, Y. Potes, A. González Rubio, N. Menéndez Coto, D. López Fanjul, I. Vega Naredo, B. Caballero, P. Saiz, J. Bobes, P. García Portilla, A. Coto Montes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S636-S637
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia (SCH) and bipolar disorder (BD) are severe mental disordes, which have high incidence (Whiteford et al. Lancet 2013; 381 1575-86) and are the main causes of diasibility in young people (WHO 2022; https://www.who.int/news-room/fact-sheets/detail/mental-disorders).
Psycological stress appears in different mental disorders, and this is directly related to oxidative stress (Moller et al. Chem Biol Interact. 1996; 102 17-36)(Pupic-Bakrac et al. 2020; Psychiatr Danub. 32 412-9). Oxidative stress causes reticulum edoplasmic stress (ER stress) and this produces high levels of misfolded proteins. Defective proteins are degraded by the proteasome, but but when the density of misfolded proteins exceeds the capacity of the proteosome, the Unfolded and Misfolded Protein Response (UPR) is triggered through three main pathways: Inositol-requiring enzyme 1α (IRE1α); transcription factor 6 alpha (ATF6α) and protein kinase RNA-Like ER kinase (PERK), trying to recover normal protein synthesis capacity (Bermejo-Millo et al. 2018; Mol Neurobiol. 55 7973-86) (González-Blanco et al. 2022; J Cachexia Sarcopenia Muscle 13 919-31).
ObjectivesCharacterizing ER stress and UPR in SCH and BD.
MethodsWe studied ER stress and UPR in peripheral blood mononuclear cells (PBMC) from 50 patients with SCH and an equal number of patients with BD compared to their corresponding controls in order to achieve our objectives.
Western Blot assay were performed following classical procedure () and the results was normalized to Ponceau as loanding control (Nie et al. 2017; BiochemByophys Resp 12 10-13) (Sander et al. 2019; Anal Biochem 575 44-53). Proteasome activity was assessed using Proteasome Activity Assay Kit (ab107921, Abcam, Cambridge, UK).
ResultsER stress was evaluated with BiP/GRP78. Our results showed significantly increased expression in SCH (p<0,01) and BD (p<0,05), being more increased in SCH. Proteasome activity was increased in SCH and BD, being only statistically significant in SQZ (p<0,05). UPR study showed IRE1a cascade significantly activated in SCH (p<0,001) and only slight increased in BD showed without statistical differences. ATF6a pathway is measured by cleavage to active protein (50-kDa). Results showed higher expression in SCH than in BD and controls (p<0,001). In addition, PERK pathway showed higher statistical levels of p-eIF2a/eiF2a ratio in SCH than in BD and control respectively (p<0,05 and p<0,01).
ConclusionsOur results showed a greater alteration in SCH than in BD at the level of protein synthesis, which implies a greater toxicity at the cellular level and, therefore, a clear risk for the survival of cells in this pathology.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
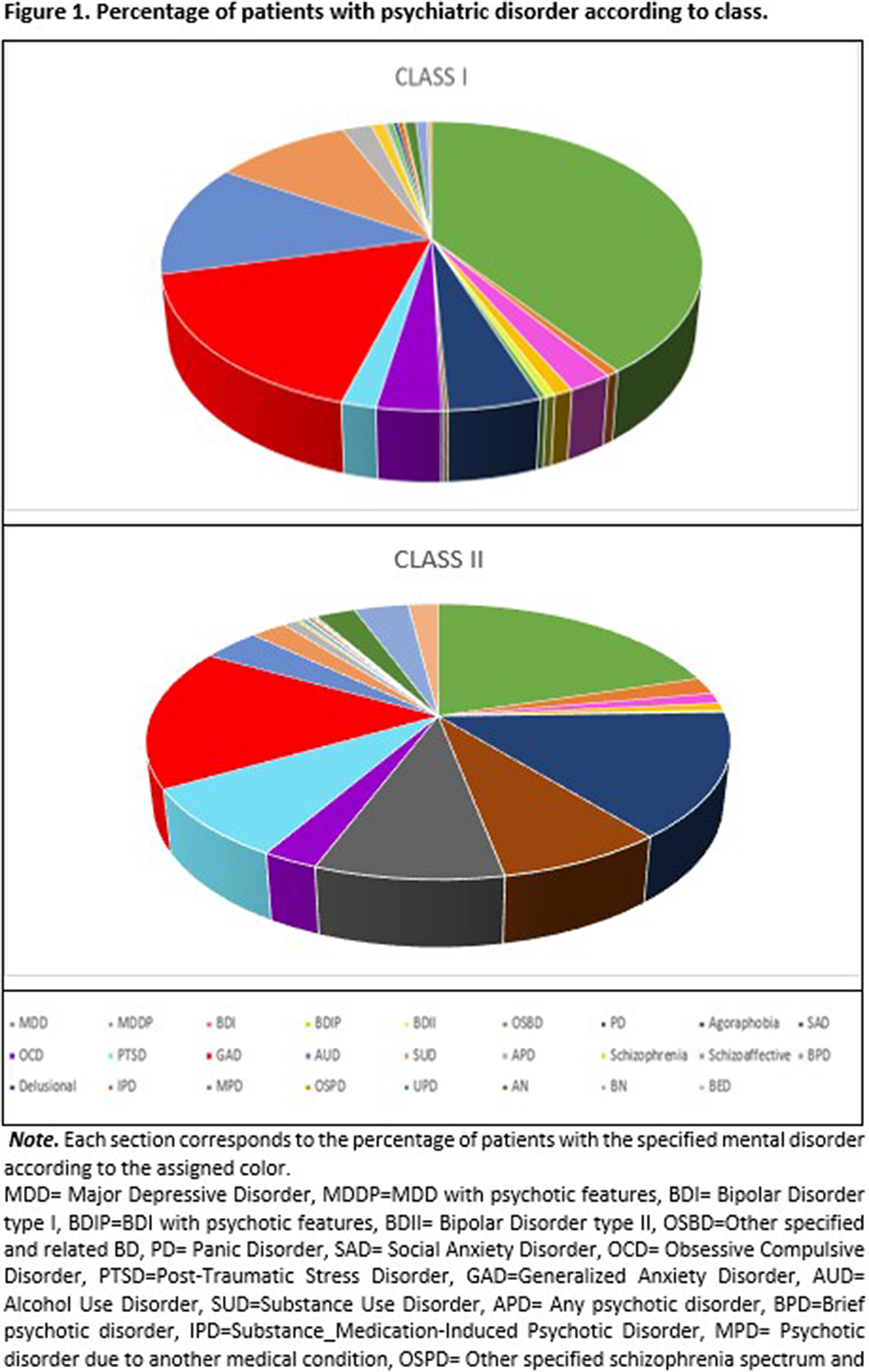 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
An empirical staging model for schizophrenia using machine learning
- M.-C. Clara, F. Sánchez-Lasheras, A. García-Fernández, L. González-Blanco, P. A. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S626-S627
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the great challenges still to be achieved in schizophrenia is the development of a staging model that reflects the progression of the disorder. The previous models suggested have been developed from a theoretical point of view and do not include objective variables such as biomarkers, physical comorbidities, or self-reported subjective variables (Martinez-Cao et al. Transl Psychiatry 2022; 12(1) 1-11).
ObjectivesDevelop a multidimensional staging model for schizophrenia based on empirical data.
MethodsNaturalistic, cross-sectional study. Sample: 212 stable patients with Schizophrenia (F20). Assessments: ad hoc questionnaire (demographic and clinical information); psychopathology: PANSS, CDS, OSQ, CGI-S; functioning: PSP; cognition: MATRICS; laboratory tests: C-Reactive Protein (CRP), IL-1RA, IL-6, Platelets/Lymphocytes (PLR), Neutrophils/Lymphocytes (NLR), and Monocytes/Lymphocytes (MLR) ratios. Statistical analysis: Variables selection was performed with an ad hoc algorithm developed for this research. The referred algorithm makes use of genetic algorithms (GA) to select those variables that show the best performance for the patients classification according to their global CGI-S. The objective function of the GA maximizes the individuals correct classification of a support vector machines (SVM) model that employs as input variables those given by the GA (Díez-Díaz et al. Mathematics 2021; 9(6) 654). Models performance was assessed with the help of 3-fold cross-validation and these process was repeated 10,000 times for each one of the models assessed.
ResultsMean age(SD): 39.5(13.54); men: 63.5%; secondary education: 59.50%. Most patients in our sample had never been married (74.10%), and more than a third received disability benefits due to schizophrenia (37.70%). The mean length of the disease was 11.98(12.02) years. The best SVM model included the following variables: 1)Clinical: number of hospitalizations, positive, negative, depressive symptoms and general psychopathology; 2)Cognition: speed of processing, visual learning and social cognition; 3)Functioning: PSP total score; 4)Biomarkers: PLR, NLR and MLR. This model was executed again 100,000 times applying again 3-fold cross-validation. In 95% of the algorithm executions more than a 53.52% of the patients were classfied in the right CGI-S category. On average the right classification was of 61.93%. About specificity and sensitivity the average values obtained were of 0.85 and 0.64 respectively.
ConclusionsOur staging model is a robust method that appropriately distributes patients according to the severity of the disorder. Highlights the importance of clinical, functional and cognitive factors to classify patients. Finally, the inflammatory parameters PLR, NLR and MLR have also emerged as potential biomarkers for staging schizophrenia.
Disclosure of InterestNone Declared
Neutrophil-to-lymphocyte ratio, platelet-to-lymphocyte ratio, and monocyte-to-lymphocyte ratio in depressed patients with suicidal behavior: A systematic review
- A Velasco, A Lengvenyte, J Rodriguez-Revuelta, L Jimenez-Treviño, P Courtet, MP Garcia-Portilla, J Bobes, PA Sáiz
-
- Journal:
- European Psychiatry / Accepted manuscript
- Published online by Cambridge University Press:
- 16 April 2023, pp. 1-25
-
- Article
-
- You have access Access
- Open access
- Export citation
Trends in the incidence of hospital-treated suicide attempts during the COVID-19 pandemic in Oviedo, Spain
- J. Fernandez-Fernandez, L. Jiménez-Treviño, E. Seijo-Zazo, F. Sánchez Lasheras, M. P. García-Portilla, P. A. Sáiz, J. Bobes
-
- Journal:
- European Psychiatry / Volume 66 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 03 February 2023, e23
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
The potential impact of the COVID-19 pandemic on suicidal behavior has generated predictions anticipating an increase in suicidal tendencies. The aim of this research is to study its influence on the incidence of hospital-treated suicide attempts throughout the year 2020 in Oviedo, Spain.
MethodsData were collected on all patients admitted to the emergency department of Central University Hospital of Asturias in Oviedo for attempted suicide during 2020. Incidence rates were calculated for three lockdown periods. Suicide attempt trends in 2020 were compared with a non-COVID-19 year (2009) to avoid seasonal variations bias. Chi-square and Fisher’s exact tests were performed. The influence of COVID-19 incidence in Oviedo was analyzed using Spearman’s correlation coefficient.
ResultsThe cumulative incidence rate of attempted suicide per 100,000 person-years was 136.33 (pre-lockdown), 115.15 (lockdown), and 90.25 (post-lockdown) in adults (over 19 years old), and 43.63 (pre-lockdown), 32.72 (lockdown), and 72.72 (post-lockdown) in adolescents (10–19 years old). No association was found with COVID-19 incidence rates (Spearman’s rho −0.222; p = 0.113). Comparing the years 2020 and 2009, statistically significant differences were observed in adolescents (Fisher’s exact test; p = 0.024), but no differences were observed in adults (chi-square test = 3.0401; p = 0.218).
ConclusionsHospital-treated suicide rates attempted during the COVID-19 outbreak in Oviedo, Spain showed a similar trend compared with a non-COVID-19 year. In contrast, the number of adolescents hospital-treated for attempted suicide increased during lockdown, suggesting more vulnerability to COVID-19 restrictions after the initial lockdown period in this age group.
Altered Executive Function in Suicide Attempts
- J. Fernández, S. Alberich, I. Zorrilla, I. González-Ortega, M.P. López, V. Pérez-Solà, E. Vieta, A.M. González-Pinto, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S124
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Executive function organizes and directs behaviour but alterations in this cognitive domain can lead to inaccurate perception, interpretation and response to environmental information, which could be a risk factor for suicide.
ObjectivesTo explore executive function performance of depressed recent suicide attempters in comparison to depressed past suicide attempters, depressed non-attempters and healthy controls.
Methods96 participants from the Psychiatry Department of the Araba University Hospital-Santiago were recruited as follows: 20 patients with a recent suicide attempt (<30days) diagnosed with a Major Depressive Disorder (MDD), 33 MDD patients with history of attempted suicide, 23 non-attempter MDD patients and 20 healthy controls. All participants underwent a clinical interview and neuropsychological assessment on executive function with the Wisconsin Sorting Card Test. Backward multiple regressions were performed adjusting for significant confounding variables. For group comparisons ANOVA test and Bonferroni post hoc test were performed with p<0.05 significance level.
ResultsPatient groups did not differ regarding severity of depression. All patient groups performed significantly worse than healthy controls on executive function. Adjusted comparisons between patient groups indicated that recent suicide attempters had a poorer performance in this cognitive domain in comparison to both depressed lifetime attempters and depressed non-attempters (B=0.296, p=0.019 and B=0.301, p=0.028 respectively).
ConclusionsExecutive function performance is altered in recent suicide attempts. As impaired executive function can be a risk factor for suicide, preventive interventions on suicide should focus on its assessment and rehabilitation.
DisclosureNo significant relationships.
Endocrine biomarkers related to sleep-wake cycle and sleep disturbances in patients with bipolar disorder: A systematic review
- L. Gonzalez-Blanco, C. Moya Lacasa, S. Jiménez-Fernández, M. Valtueña, C. Martinez-Cao, A. García Fernández, P.A. Saiz, M.P. Garcia-Portilla, J. Bobes, L. Gutierrez Rojas
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S360
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Sleep and circadian disturbances have been widely studied in patients with bipolar disorder (BD) (Duarte Faria et al., 2015; Gonzalez, 2014). However, there is no clear evidence about the role of peripheral biomarkers of circadian cycle in this population.
ObjectivesThis systematic review aims to identify potential endocrine biomarkers of circadian rhythm in blood and study their relationship with sleep problems in BD.
MethodsAn electronic search of Pubmed and PsycoInfo databases were performed. It includes articles about the topic from 1991 to 2021. The search strategy was: (“Peripheral biomarkers” OR “biological markers” OR biomarker OR cortisol OR melatonin OR orexin OR hypocretin) AND (blood OR serum OR plasma) AND (“sleep-wake” OR “circadian rhythm” OR sleep OR insomnia) AND “bipolar”.
Results92 records were obtained after excluding duplicates. Only five studies met the inclusion criteria (n = 499; BD = 125; unipolar depression = 148; schizophrenia = 80; controls = 146). The endocrine parameters analyzed were: cortisol (3 studies), melatonin (1 study) and orexin-A (1 study). Overall, no significant associations between these biomarkers and sleep disturbances, assessed with subjective (psychometric evaluation) and/or objective (polysomnography) measures, were detected.
ConclusionsThis systematic review highlights the lack of studies that explores the role of endocrine biomarkers related to circadian function in the pathophysiology of sleep disturbances in BD.
DisclosureNo significant relationships.
Orexins and bipolar disorder: A review
- C. Moya Lacasa, L. Gonzalez-Blanco, C. Martinez-Cao, C.M. Alvarez-Vazquez, E. Martin-Gil, A. García Fernández, P.A. Saiz, J. Bobes, M.P. Garcia-Portilla
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S400
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is a chronic deteriorating illness which has a strong impact on functionality. In the past few years, orexins have gained importance as possible biomarkers of circadian rhythms, affected in BD. Up to this date, we have not found any bibliographical review evaluating the association of orexins and BD.
ObjectivesTo review published literature in relation to the associaton of orexins and BD.
MethodsA bibliographical search was conducted in PubMed. Inclusion criteria were a) the study evaluated orexins in plasma or cerebrospinal fluid, and b) patients with BD were included within the subjects of study.
Reference lists of the articles that met inclusion criteria were also examined.
ResultsTen articles were retrieved from the initial search. Only three met inclusion criteria and another one was selected from the reference list examination. One study observed significantly higher levels of orexin A in plasma of BD patients versus depression and controls. Other found higher concentration of orexin A of unipolar and bipolar depression versus controls, but this result was not statistically significant. Another one did not find differences in orexin A concentration between mania, depression and controls. The remaining study detected significantly lower concentration of orexin A in BD versus depression, schizophrenia and controls.
ConclusionsDespite being heterogenous, the results point out there are differences in orexin levels in BD when compared to other diagnostic groups or controls. This sets a starting point to focus research on this subject and continue analyzing the role of orexins as biomarkers in BD.
DisclosureNo significant relationships.
The prescriber’s guide to classic MAO inhibitors (phenelzine, tranylcypromine, isocarboxazid) for treatment-resistant depression
- Vincent Van den Eynde, Wegdan R. Abdelmoemin, Magid M. Abraham, Jay D. Amsterdam, Ian M. Anderson, Chittaranjan Andrade, Glen B. Baker, Aartjan T.F. Beekman, Michael Berk, Tom K. Birkenhäger, Barry B. Blackwell, Pierre Blier, Marc B.J. Blom, Alexander J. Bodkin, Carlo I. Cattaneo, Bezalel Dantz, Jonathan Davidson, Boadie W. Dunlop, Ryan F. Estévez, Shalom S. Feinberg, John P.M. Finberg, Laura J. Fochtmann, David Gotlib, Andrew Holt, Thomas R. Insel, Jens K. Larsen, Rajnish Mago, David B. Menkes, Jonathan M. Meyer, David J. Nutt, Gordon Parker, Mark D. Rego, Elliott Richelson, Henricus G. Ruhé, Jerónimo Sáiz-Ruiz, Stephen M. Stahl, Thomas Steele, Michael E. Thase, Sven Ulrich, Anton J.L.M. van Balkom, Eduard Vieta, Ian Whyte, Allan H. Young, Peter K. Gillman
-
- Journal:
- CNS Spectrums / Volume 28 / Issue 4 / August 2023
- Published online by Cambridge University Press:
- 15 July 2022, pp. 427-440
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This article is a clinical guide which discusses the “state-of-the-art” usage of the classic monoamine oxidase inhibitor (MAOI) antidepressants (phenelzine, tranylcypromine, and isocarboxazid) in modern psychiatric practice. The guide is for all clinicians, including those who may not be experienced MAOI prescribers. It discusses indications, drug-drug interactions, side-effect management, and the safety of various augmentation strategies. There is a clear and broad consensus (more than 70 international expert endorsers), based on 6 decades of experience, for the recommendations herein exposited. They are based on empirical evidence and expert opinion—this guide is presented as a new specialist-consensus standard. The guide provides practical clinical advice, and is the basis for the rational use of these drugs, particularly because it improves and updates knowledge, and corrects the various misconceptions that have hitherto been prominent in the literature, partly due to insufficient knowledge of pharmacology. The guide suggests that MAOIs should always be considered in cases of treatment-resistant depression (including those melancholic in nature), and prior to electroconvulsive therapy—while taking into account of patient preference. In selected cases, they may be considered earlier in the treatment algorithm than has previously been customary, and should not be regarded as drugs of last resort; they may prove decisively effective when many other treatments have failed. The guide clarifies key points on the concomitant use of incorrectly proscribed drugs such as methylphenidate and some tricyclic antidepressants. It also illustrates the straightforward “bridging” methods that may be used to transition simply and safely from other antidepressants to MAOIs.
Association between the Prime Diet Quality Score and depressive symptoms in a Mediterranean population with metabolic syndrome. Cross-sectional and 2-year follow-up assessment from PREDIMED-PLUS study
- Naomi Cano-Ibáñez, Lluis Serra-Majem, Sandra Martín-Peláez, Miguel Ángel Martínez-González, Jordi Salas-Salvadó, Maria Dolores Corella Piquer, Camille Lassale, José Alfredo Martínez Hernandez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque Lopez, Dora Romaguera, José López-Miranda, Ramon Estruch, Ana María Gómez-Pérez, José Manuel Santos-Lozano, Fernando Fernández-Aranda, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín, Xavier Pintó Sala, Miguel Delgado-Rodríguez, Pilar Matía Martín, Josep Vidal, Jersy J. Cárdenas, Lidia Daimiel Ruiz, Emilio Ros, Pilar Buil-Cosiales, Nerea Becerra-Tomás, Carmen Saiz, Miguel-Ángel Muñoz-Perez, Itziar Abete, Lucas Tojal-Sierra, Olga Fernández-Barceló, Andrea Bernabé-Casanova, Jadwiga Konieczna, Antonio García-Ríos, Rosa Casas, Maria Rosa Bernal-López, José Lapetra, Estefanía Toledo, Carlos Gómez-Martínez, Oscar Coltell, Mireia Malcampo-Manrúbia, María Angeles Zulet, Carolina Sorto-Sánchez, Alfredo Gea, José Luis Hernández-Fleta, Olga Castañer Niño, Almudena Sánchez-Villegas
-
- Journal:
- British Journal of Nutrition / Volume 128 / Issue 6 / 28 September 2022
- Published online by Cambridge University Press:
- 29 October 2021, pp. 1170-1179
- Print publication:
- 28 September 2022
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The burden of depression is increasing worldwide, specifically in older adults. Unhealthy dietary patterns may partly explain this phenomenon. In the Spanish PREDIMED-Plus study, we explored (1) the cross-sectional association between the adherence to the Prime Diet Quality Score (PDQS), an a priori-defined high-quality food pattern, and the prevalence of depressive symptoms at baseline (cross-sectional analysis) and (2) the prospective association of baseline PDQS with changes in depressive symptomatology after 2 years of follow-up. After exclusions, we assessed 6612 participants in the cross-sectional analysis and 5523 participants in the prospective analysis. An energy-adjusted high-quality dietary score (PDQS) was assessed using a validated FFQ. The cross-sectional association between PDQS and the prevalence of depression or presence of depressive symptoms and the prospective changes in depressive symptoms were evaluated through multivariable regression models (logistic and linear models and mixed linear-effects models). PDQS was inversely associated with depressive status in the cross-sectional analysis. Participants in the highest quintile of PDQS (Q5) showed a significantly reduced odds of depression prevalence as compared to participants in the lowest quartile of PDQS (Q1) (OR (95 %) CI = 0·82 (0·68, 0·98))). The baseline prevalence of depression decreased across PDQS quintiles (Pfor trend = 0·015). A statistically significant association between PDQS and changes in depressive symptoms after 2-years follow-up was found (β (95 %) CI = −0·67 z-score (–1·17, −0·18). A higher PDQS was cross-sectionally related to a lower depressive status. Nevertheless, the null finding in our prospective analysis raises the possibility of reverse causality. Further prospective investigation is required to ascertain the association between PDQS and changes in depressive symptoms along time.
Suicidal behaviour and cognition: A systematic review with special focus on prefrontal deficits
- J. Fernández-Sevillano, A. González-Pinto, J. Rodríguez-Revuelta, S. Alberich-Mesa, L. González-Blanco, I. Zorrilla-Martínez, Á. Velasco, P. López-Pena, I. Abad-Acebedo, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S584
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicidal behaviour and cognition: A systematic review with special focus on prefrontal deficits Introduction: Suicide is a major health concern worldwide, thus, identifying risk factors would enable a more comprehensive understanding and prevention of this behaviour. Neuropsychological alterations could lead to difficulties in interpreting and managing life events resulting in a higher risk of suicide.
ObjectivesObjective: Bibliographic review about the influence of neuropsychological deficits on suicidal behaviour.
MethodsMethod: A systematic literature search from 2000 to 2020 was performed in Medline (Pubmed), Web of Science, SciELO Citation Index, PsycInfo, PsycArticles and Cochrane Library databases regarding studies comparing cognition of attempters versus non-attempters that share same psychiatric diagnosis. Results: 1.885 patients diagnosed with an Affective Disorder (n = 1512) and Schizophrenia/ Schizoaffective Disorder (n = 373) were included.
ResultsIn general comparison, attention was found to be clearly dysfunctional. Regarding diagnosis, patients with Schizophrenia and previous history of suicidal behaviour showed a poorer performance in executive function. Patients with current symptoms of an Affective Disorder and a previous history of suicidal attempt had poorer performance in attention and executive function. Similarly, euthymic affective patients with history of suicidal behaviour had worse decision-making, attention and executive function performance compared to euthymic non-attempters.
ConclusionsPatients who have attempted suicide have a poorer neuropsychological functioning than non-attempters with a similar psychiatric disorder in attention and executive function. These alterations increase vulnerability for suicide.
Conflict of interestJessica Fernández-Sevillano is beneficiary of the Pre-PhD Training Programme of the Basque Government. Dr. Gonzalez-Pinto has received grants and served as consultant, advisor or CME speaker for the following entities: Almirall, AstraZeneca, Bristol-Myers
Insomnia associated with neutrophil/lymphocyte ratio in female patients with schizophrenia
- G. Paniagua, L. González-Blanco, F. Dal Santo, C. Martínez-Cao, C. Moya-Lacasa, M. Valtueña-García, E. Martín Gil, L. García-Alvarez, P.A. Saiz, M.P. García-Portilla, J. Bobes
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S806
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Worse sleep quality and increased inflammatory markers in women with schizophrenia (Sch) have been reported (Lee et al. 2019). However, the physiological mechanisms underlying the interplay between sleep and the inflammatory pathways are not yet well understood (Fang et al. 2016).
ObjectivesAnalyze the relationship between Neutrophil/Lymphocyte (NLR), Monocyte/Lymphocyte (MLR) and Platelet/Lymphocyte (PLR) ratios, and insomnia in Sch stratified by sex.
MethodsFinal sample included 176 Sch patients (ICD-10 criteria) [mean age: 38.9±13.39; males: 111(63.1%)]. Assessment: PANSS, Calgary Depression Scale (CDSS), and Oviedo Sleep Questionnaire (OSQ) to identify a comorbid diagnosis of insomnia based on ICD-10. Fasting counting blood cell were performed to calculate ratios. Statistics: U Mann-Whitney, logistic regression.
ResultsInsomnia as comorbid diagnosis was present in 22 Sch (12.5%) with no differences between sex [14 males (12.6%), 8 females (12.3%)], neither in their age. Female patients with insomnia showed increased NLR [2.44±0.69 vs. 1.88±0.80, U=122.00 (p=0.034)]. However, no differences in PLR and MLR were found, neither in any ratio in males. Regression models using insomnia as dependent variable and covariates (age, PANSS-positive, PANSS-negative, CDSS) were estimated. Females: presence of insomnia was associated with NLR [OR=3.564 (p=0.032)], PANSS-positive [OR=1.263 (p=0.013)] and CDSS [OR=1.198 (p=0.092)]. Males: only PANSS-positive [OR=1.123 (p=0.027)] and CDSS scores [OR=1.220 (p=0.005)] were associated with insomnia.
ConclusionsNLR represent an inflammatory marker of insomnia in Sch but only in female patients. Improving sleep quality in these patients could help to decrease their inflammatory response.
DisclosureNo significant relationships.
The mediating role of impulsivity in the relationship between suicidal behaviour and early traumatic experiences in depressed subjects
- F. Dal Santo, J.J. Carballo, Á. Velasco, L. Jiménez-Treviño, J. Rodríguez-Revuelta, C. Martínez-Cao, I. Irene Caro-Cañizares, L. De La Fuente-Tomás, I. Menéndez-Miranda, L. González-Blanco, M.P. García-Portilla, J. Bobes, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S583
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depressed patients with early traumatic experiences may represent a clinically distinct subtype with worse clinical outcome. Since early traumatic experiences alter the development of systems that regulate the stress response, certain personality features may influence coping strategies, putting individuals with depression and a history of early traumatic experiences at greater risk of suicidal behaviour.
ObjectivesTo determine whether impulsivity mediates the relationship between early traumatic experiences and suicidal behaviour in patients with major depressive disorder (MDD).
MethodsThe sample included 190 patients [mean age (SD)=53.71 (10.37); females: 66.3%], with current MDD. The Childhood Trauma Questionnaire-Short Form (CTQ-SF), the List of Threatening Experiences (LTE), and the Barratt Impulsiveness Scale-11 (BIS-11) were used to assess childhood and adulthood adverse life events and impulsivity. We developed mediation models by bootstrap sampling methods.
Results81 (42.6%) patients had previous suicide attempts (SA). CTQ-SF-Total and BIS-11-Total scores were higher in MDD patients with previous SA. Correlation analyses revealed significant correlations between the CTQ-SF-Total and BIS-11-Total, CTQ-SF-Total and HDRS-Total, and BIS-11-Total and HDRS-Total scores. Regression models found that CTQ-SF-Total, BIS-11-Total, and HDRS-Total scores were associated with SA. Mediation analyses further revealed the association between CTQ-SF-Total and SA was mediated by the indirect effect of the BIS-11-Total score (b=0.007, 95% CI=0.001, 0.015), after controlling for sex, HDRS-Total, and LTE-Total.
ConclusionsImpulsivity could mediate the influence of childhood trauma on suicidal behaviour. This will help understand the role of risk factors in suicidal behaviour and aid in the development of prevention interventions focused on modifiable mediators when risk factors are non-modifiable.
Association of traumatic events in childhood, impulsivity and decision-making with previous suicide attempt and/or current suicidal ideation in adult patients with major depressive disorder
- A. Roman, J. Rodríguez-Revuelta, F. Dal Santo, L. García-Alvarez, L. De La Fuente-Tomás, C. Martínez-Cao, L. Jiménez-Treviño, L. González-Blanco, M.P. García-Portilla, J. Bobes, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicidal behavior has a great impact on world public health. The literature describes the possible existence of an association between neurobiological, clinical and cognitive factors in suicidal behavior.
ObjectivesTo determine the possible relationship between clinical variables (history of abuse/maltreatment in childhood), psychopathology (impulsivity traits) and cognitive (decision-making) with a history of suicide attempt and/or current suicidal idea in patients with major depressive disorder.
MethodsCross-sectional study in a sample of adult patients with major depressive disorder in which two types of comparisons are made. In the first case, two groups were compared based on the presence or absence of history of suicide attempt. In the second case, two groups were compared based on the presence or absence of suicidal ideation in the same sample of patients. Finally, sociodemographic, clinical and cognitive variables were evaluated in that population sample.
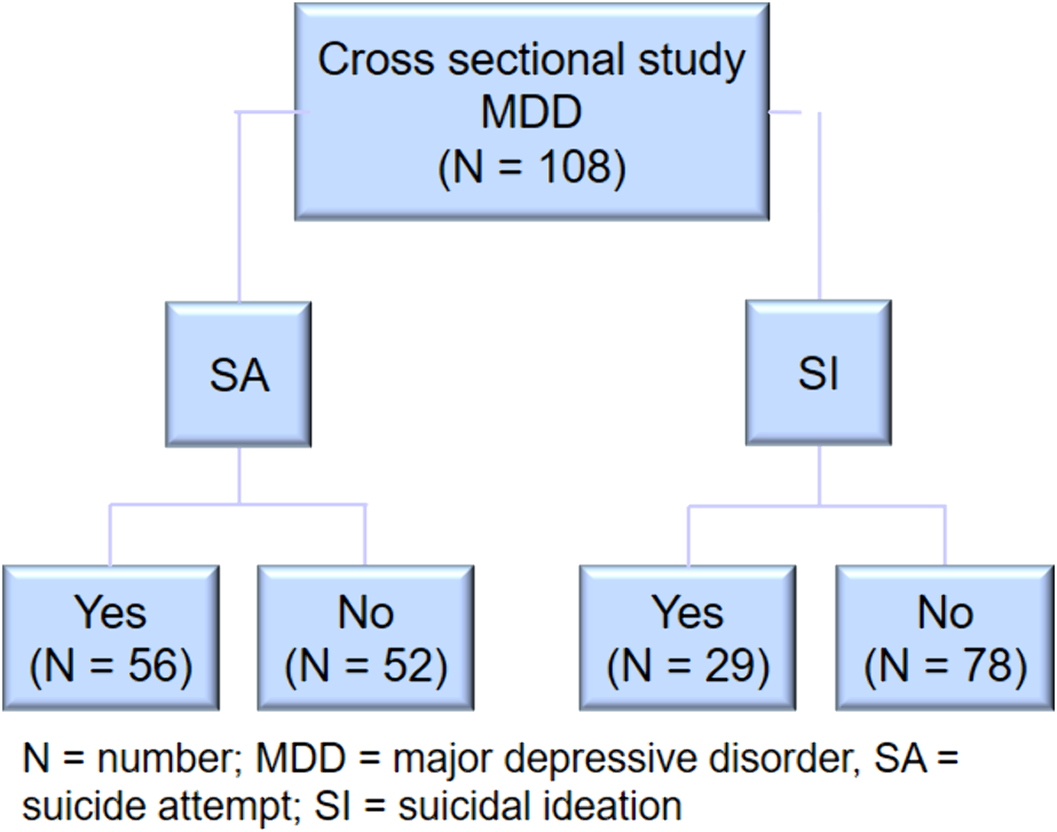 Results
ResultsWhen the joint influence of sociodemographic, clinical and cognitive characteristics are present, it can be said that being single/divorced/separated, a history of sexual abuse in childhood and an alteration in decision-making, specifically a lower number of choices of deck D in the IGT test, are associated with a higher probability of a personal history of suicide attempt. While a higher score on the Barrat impulsivity scale is associated with a greater probability of presenting current suicidal ideation once the influence of sociodemographic, clinical and cognitive variables has been taken into account.
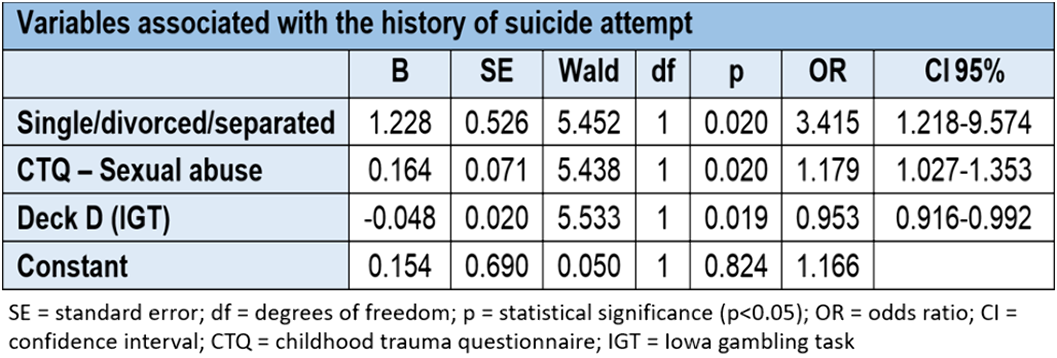
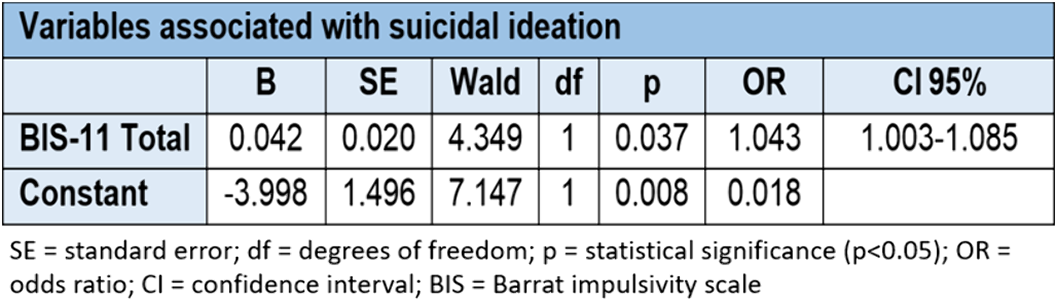 Conclusions
ConclusionsDifferent sociodemographic, clinical and cognitive factors are associated with the presence of a history of suicide attempt and/or current suicidal ideation.
DisclosureNo significant relationships.
COVID-19 psychological impact in patients with depressive disorder: Differences based on their age
- E. Martín Gil, M. Valtueña-García, L. González-Blanco, F. Dal Santo, C. Moya-Lacasa, C. Álvarez Vázquez, C. Martínez-Cao, L. García-Alvarez, M.P. García-Portilla, P.A. Saiz, J. Bobes
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S674-S675
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
COVID-19 pandemic and lockdown have provoked a considerable psychological impact in Spain. Some studies have reported greater psychological impact in the younger population. To date, no previous study has focused on depressive disorder (DD) patients based on their age.
ObjectivesTo describe the psychological impact on DD according to age.
MethodsCross-sectional study of an online survey available from 19 to 26 March 2020. Out of a total of 21207 respondents, 608 (2.9%) reported suffering from DD (mean age ±SD = 41.2 years±14.07 [18-82], 80.6% women). The subsample (608) was divided according to age, “youngsters” <45 (57.4%)/ “elders” ≥45. DASS-21 and IES scales were employed. Statistical analyses: Chi-square, t-Student test.
ResultsBoth groups did not differ (p>0.05) in sex, having COVID-19 symptoms, having family/friends infected, or income changes. While youngsters were single more frequently (68.8% vs 14.3%, χ² = 179.7, p<0.001), elders had somatic illness more frequently (64.8% vs 39.7% χ² =30.401, p<0.001). Youngsters obtained higher scores in depression (4.69 vs 4.1, T=5.413, p<0.001), anxiety (2.86 vs 1.97, T=5.249, p<0.001) and stress (4.48 vs 3.17, T=6.355, p<0.001) DASS-21 subscales, as in intrusive (3.42 vs 3.05, T=1.984, p=0.048) and avoidant (4.64 vs 4.11, T=3.056, p=0.002) IES scores.
ConclusionsDespite the group of elders with depression being more vulnerable to severe COVID-19 disease and presenting more frequently somatic comorbidities, younger depressive patients suffered more from depressive, anxiety, stress and avoidant symptoms and intrusive thoughts, in line with previous reports in the general population.
DisclosureNo significant relationships.
Examining the association between exposome score for schizophrenia and functioning in schizophrenia, siblings, and healthy controls: Results from the EUGEI study
- Gamze Erzin, Lotta-Katrin Pries, Jim van Os, Laura Fusar-Poli, Philippe Delespaul, Gunter Kenis, Jurjen J. Luykx, Bochao D. Lin, Alexander L. Richards, Berna Akdede, Tolga Binbay, Vesile Altınyazar, Berna Yalınçetin, Güvem Gümüş-Akay, Burçin Cihan, Haldun Soygür, Halis Ulaş, Eylem Şahin Cankurtaran, Semra Ulusoy Kaymak, Marina M. Mihaljevic, Sanja Andric-Petrovic, Tijana Mirjanic, Miguel Bernardo, Gisela Mezquida, Silvia Amoretti, Julio Bobes, Pilar A. Saiz, Maria Paz García-Portilla, Julio Sanjuan, Eduardo J. Aguilar, Jose Luis Santos, Estela Jiménez-López, Manuel Arrojo, Angel Carracedo, Gonzalo López, Javier González-Peñas, Mara Parellada, Nadja P. Maric, Cem Atbaşoğlu, Alp Ucok, Köksal Alptekin, Meram Can Saka, Genetic Risk and Outcome of Psychosis (GROUP) investigators, Celso Arango, Micheal C. O’Donovan, Bart P. F. Rutten, Sinan Guloksuz
-
- Journal:
- European Psychiatry / Volume 64 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 19 March 2021, e25
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
A cumulative environmental exposure score for schizophrenia (exposome score for schizophrenia [ES-SCZ]) may provide potential utility for risk stratification and outcome prediction. Here, we investigated whether ES-SCZ was associated with functioning in patients with schizophrenia spectrum disorder, unaffected siblings, and healthy controls.
MethodsThis cross-sectional sample consisted of 1,261 patients, 1,282 unaffected siblings, and 1,525 healthy controls. The Global Assessment of Functioning (GAF) scale was used to assess functioning. ES-SCZ was calculated based on our previously validated method. The association between ES-SCZ and the GAF dimensions (symptom and disability) was analyzed by applying regression models in each group (patients, siblings, and controls). Additional models included polygenic risk score for schizophrenia (PRS-SCZ) as a covariate.
ResultsES-SCZ was associated with the GAF dimensions in patients (symptom: B = −1.53, p-value = 0.001; disability: B = −1.44, p-value = 0.001), siblings (symptom: B = −3.07, p-value < 0.001; disability: B = −2.52, p-value < 0.001), and healthy controls (symptom: B = −1.50, p-value < 0.001; disability: B = −1.31, p-value < 0.001). The results remained the same after adjusting for PRS-SCZ. The degree of associations of ES-SCZ with both symptom and disability dimensions were higher in unaffected siblings than in patients and controls. By analyzing an independent dataset (the Genetic Risk and Outcome of Psychosis study), we replicated the results observed in the patient group.
ConclusionsOur findings suggest that ES-SCZ shows promise for enhancing risk prediction and stratification in research practice. From a clinical perspective, ES-SCZ may aid in efforts of clinical characterization, operationalizing transdiagnostic clinical staging models, and personalizing clinical management.








