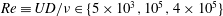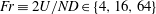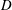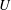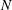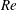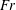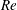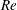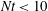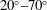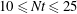17 results
Internal gravity wave radiation from a stratified turbulent wake
- K. L. Rowe, P. J. Diamessis, Q. Zhou
-
- Journal:
- Journal of Fluid Mechanics / Volume 888 / 10 April 2020
- Published online by Cambridge University Press:
- 11 February 2020, A25
-
- Article
- Export citation
-
The near-field energetics and directional properties of internal gravity waves (IGWs) radiated from the turbulent wake of a sphere towed through a linearly stratified fluid are investigated using a series numerical experiments. Simulations have been performed for an initial Reynolds number
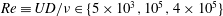 $Re\equiv UD/\unicode[STIX]{x1D708}\in \{5\times 10^{3},10^{5},4\times 10^{5}\}$ and internal Froude number
$Re\equiv UD/\unicode[STIX]{x1D708}\in \{5\times 10^{3},10^{5},4\times 10^{5}\}$ and internal Froude number 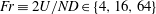 $Fr\equiv 2U/ND\in \{4,16,64\}$, defined using body-based scales –
$Fr\equiv 2U/ND\in \{4,16,64\}$, defined using body-based scales – 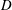 $D$, the sphere diameter;
$D$, the sphere diameter; 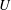 $U$, the tow speed; and
$U$, the tow speed; and 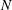 $N$, the Brunt–Väisälä frequency. Snapshots of temporally evolving wake flow fields are sampled over the full wake evolution. The energy extracted from the wake through internal wave radiation is quantified by computing the total wave power emitted through a wake-following elliptic cylinder. The total time-integrated wave energy radiated is found to increase with
$N$, the Brunt–Väisälä frequency. Snapshots of temporally evolving wake flow fields are sampled over the full wake evolution. The energy extracted from the wake through internal wave radiation is quantified by computing the total wave power emitted through a wake-following elliptic cylinder. The total time-integrated wave energy radiated is found to increase with 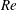 $Re$ and decrease with
$Re$ and decrease with 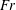 $Fr$. The peak radiated wave power occurs at early times, near to the onset of buoyancy control, and is found to be approximately unchanged in magnitude as
$Fr$. The peak radiated wave power occurs at early times, near to the onset of buoyancy control, and is found to be approximately unchanged in magnitude as 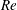 $Re$ is increased. For the two higher
$Re$ is increased. For the two higher 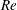 $Re$ considered, at late times, IGWs continue to be emitted – accounting for a distinct increase in total radiated wave energy. The most powerful IGWs are radiated out of the wake at a wide range of angles for
$Re$ considered, at late times, IGWs continue to be emitted – accounting for a distinct increase in total radiated wave energy. The most powerful IGWs are radiated out of the wake at a wide range of angles for 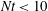 $Nt<10$, at
$Nt<10$, at 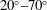 $20^{\circ }{-}70^{\circ }$ to the horizontal for
$20^{\circ }{-}70^{\circ }$ to the horizontal for 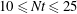 $10\leqslant Nt\leqslant 25$, and nearly parallel to the horizontal late in the non-equilibrium regime of wake evolution. Internal wave radiation is found to be an important sink for wake kinetic energy after
$10\leqslant Nt\leqslant 25$, and nearly parallel to the horizontal late in the non-equilibrium regime of wake evolution. Internal wave radiation is found to be an important sink for wake kinetic energy after 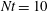 $Nt=10$, suggesting wave radiation cannot be neglected when modelling stratified turbulent wakes in geophysical and ocean engineering applications.
$Nt=10$, suggesting wave radiation cannot be neglected when modelling stratified turbulent wakes in geophysical and ocean engineering applications.
P052: Breaking down the pieces: A scoping review exploring the components of image ordering interventions and trends in their outcomes in pediatric emergency medicine
- L. Gaudet, L. Krebs, M. Carr, M. Kruhlak, A. Hall, K. Mahoney, B. Sevcik, B. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 21 / Issue S1 / May 2019
- Published online by Cambridge University Press:
- 02 May 2019, pp. S81-S82
- Print publication:
- May 2019
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Clinicians treating children in the emergency department (ED) are especially concerned with the efficacy and safety of imaging. Interventions to limit imaging have been proposed to maximize benefits and avoid risks; however, the types and effectiveness of interventions employed in pediatric EDs have not been examined in detail. Methods: Electronic databases and grey literature were systematically searched by a medical librarian. Comparative studies of ED-based interventions reporting computed tomography (CT), radiography (XR), or ultrasound (US) outcomes were included. Interventions introducing new imaging equipment or personnel to the ED, ED diversion strategies, and pre-admission protocols were excluded. At least two independent reviewers assessed each study for inclusion based on pre-defined criteria and extracted data. Disagreements were resolved through consensus. Descriptive results are reported. Results: Overall, 38 pediatric studies were included. Most (66%) interventions implemented two or more components; the most common intervention components were clinical guidelines or pathways (87%) and education or information (66%). Studies were categorized by presentation type: traumatic (n = 27); non-traumatic (n = 19), or combined ‘all-comers’ (n = 2). Included studies reported 62 imaging outcomes (CT = 29; XR = 20; US = 13). Among traumatic studies, 26 imaging outcomes were reported; CT was the most commonly reported outcome (CT = 15; XR = 9; US = 1). Of the CT outcomes, 33% reported significant decreases and five decreased but were either not significant or did not report significance. XR significantly decreased in 44% (4/9). In the non-traumatic studies, the most common imaging outcome remained CT (12 outcomes); 58% of which reported significant decreases. XR was the second most frequent outcome, with 63% reporting significant reductions. Combined success of the interventions to reduce CT and XR was 60%. Reported changes in ordering were less consistent in US. Conclusion: Multifaceted passive interventions have been implemented to reduce imaging in pediatric EDs. Most reported some success changing ordering practices, specifically among patients with non-trauma presentations. Future research exploring relationships between intervention content, effectiveness, and fidelity may provide insight into how to develop more effective interventions to change image ordering in the ED and guide which presentations to target.
P008: Hereditary Angioedema Rapid Triage Tool (HAE-RT): translating clinical research into clinical practice
- S. Betschel, E. Avilla, S. Waserman, J. Badiou, K. Binkley, R. Borici-Mazi, J. Hebert, L. Howlett, A. Kanani, P. Keith, G. Lacuesta, W. Yang, A. Rowe, P. Waite
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, p. S59
- Print publication:
- May 2018
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Hereditary angioedema (HAE) patients (both diagnosed and undiagnosed) commonly present to the emergency department (ED). Presenting symptoms (swelling and pain) may be erroneously attributed to common allergic and gastrointestinal conditions resulting in major delays in diagnosis and appropriate treatment. No published tools currently exist for HAE screening and management in undiagnosed disease. The overall goal of the study was to develop a HAE-RT tool for ED settings. Methods: A two-phase mixed methods approach was used to develop the HAE-RT Tool including: Phase 1: A Delphi Study [HAE specialists (N=9) and National Patient Advocacy Group Members (N=3)] was conducted to reach consensus (80% agreement) on predictor variables to include. Phase 2: A retrospective chart review was conducted to assess the predictive findings of the predictor variables. A convenient sample of patients presenting with angioedema (with and without HAE) between January 2012 January 2017 were included in the study. Results: Of the 12 experts invited, 9 (75%) participated in the Delphi study. Of 8 HAE-specific predictive variables, 4 reached consensuses including: (1) recurrent angioedema; (2) absence of urticaria; (3) past recurrent abdominal pain/swelling; (4) response to allergic therapy. The retrospective study included 85 patients (N=46 with HAE; N=39 non-HAE; overall 72% female). HAE patients were significantly more likely to have a family history of HAE (72% vs 0%; P<0.0001); previous recurrent angioedema (96%; P<0.009); present with no hives (91%; P<0.036); previous recurrent abdominal pain (80%; P<0.0001); and only 2% responded positively to allergy treatments (P<0.0001). Conclusion: Our study emphasizes the importance of key stakeholder involvement and feedback to facilitate the prioritization of important information that must be included in the design of an HAE-RT tool. The next step is to observe the effect of the HAE-RT tool on patient triage in the ED.
LO55: Role of n-terminal pro brain natriuretic peptide (NT Pro-BNP) in emergency department syncope risk stratification: a multicenter study
- V. Thiruganasambandamoorthy, M. L.A. Sivilotti, A. D. McRae, I. G. Stiell, M. Mukarram, L. Huang, K. Arcot, G. A. Wells, B. H. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 20 / Issue S1 / May 2018
- Published online by Cambridge University Press:
- 11 May 2018, p. S26
- Print publication:
- May 2018
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Two published studies reported natriuretic peptides can aid in risk-stratification of Emergency Department (ED) syncope. We sought to assess the role of N-Terminal pro Brain Natriuretic Peptide (NT pro-BNP) to identify syncope patients at risk for serious adverse events (SAE) within 30 days of the ED visit, and its value above that of the Canadian Syncope Risk Score (CSRS). Methods: We conducted a multicenter prospective cohort study at 6 large Canadian EDs from Nov 2011 to Feb 2015. We enrolled adults who presented within 24-hours of syncope and excluded those with persistent altered mentation, obvious seizure, and intoxication. We collected patient characteristics, nine CSRS predictors (includes troponin), ED management and NT pro-BNP levels. Adjudicated serious adverse events (SAE) included death, cardiac SAE (arrhythmias, myocardial infarction, serious structural heart disease) and non-cardiac SAE (pulmonary embolism, severe hemorrhage and procedural interventions within 30-days). We used two tailed t-test and logistic regression analysis. Results: Of the 1359 patients (mean age 57.2 years, 54.7% females, 13.3% hospitalized) enrolled, 148 patients (10.9%; 0.7% deaths, 7.9% cardiac SAE including 6.1% arrhythmia) suffered SAE within 30-days. The mean NT pro-BNP values, when compared to the patients with no SAE (499.8ng/L) was significantly higher among the 56 patients who suffered SAE after ED disposition (3147ng/L, p=0.001), and among the 35 patients with cardiac SAE after ED disposition (2016.2ng/L, p=0.02). While there was a trend to higher levels among patients who suffered arrhythmia after the ED visit, it was not statistically significant (1776.4ng/L, p=0.07). In a model with CSRS predictors, the adjusted odds ratio for NT pro-BNP was 8.0 (95%CI 1.8, 35.9) and troponin was 3.8 (95%CI 1.7, 8.8). The addition of NT pro-BNP did not significantly improve the classification performance (p=0.76) with areas under the curves for CSRS was 0.91 (95%CI 0.88, 0.95) and CSRS with NT pro-BNP was 0.92 (95%CI 0.88, 0.95). Conclusion: In this multicenter study, mean NT pro-BNP levels were significantly higher among ED syncope patients who suffered SAE including cardiac SAE after ED disposition. Though NT pro-BNP was a significant independent predictor of SAE after ED disposition, it did not improve accuracy in ED syncope risk-stratification when compared to CSRS. Hence, we do not recommend NT pro-BNP measurement for ED syncope management.
LO31: Identification of high risk factors associated with 30 day serious adverse events among syncope patients transported to the emergency department by emergency medical services
- L. Yau, M.A. Mukarram, S. Kim, K. Arcot, K. Thavorn, M. Taljaard, M. Sivilotti, B.H. Rowe, V. Thiruganasambandamoorthy
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S38
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: The majority of syncope patients transported to the emergency department (ED) by emergency medical services (EMS) are low-risk with very few suffering serious adverse events (SAE) within 30-days and over 50% are diagnosed with vasovagal syncope. These patients can potentially be diverted by EMS to alternate pathways of care (primary care or syncope clinic) if appropriately identified. We sought to identify high-risk factors associated with SAE within 30-days of ED disposition as a step towards developing an EMS clinical decision tool. Methods: We prospectively enrolled adult syncope patients who were transported to 5 academic EDs by EMS. We collected standardized variables at EMS presentation from history, clinical examination and investigations including ECG and ED disposition. We also collected concerning symptoms identified and EMS interventions. Adjudicated SAE included death, myocardial infarction, arrhythmia, structural heart disease, pulmonary embolism, hemorrhage and procedural interventions. Multivariable logistic regression was used for analysis. Results: 990 adult syncope patients (mean age 58.9 years, 54.9% females and 16.8% hospitalized) were enrolled with 137 (14.6%) patients suffering SAE within 30-days of ED disposition. Of 42 candidate predictors, we identified 5 predictors that were significantly associated with SAE on multivariable analysis: ECG abnormalities [OR=1.77; 95%CI 1.36-2.48] (non-sinus rhythm, high degree atrioventricular block, left bundle branch block, ST-T wave changes or Q waves), cardiac history [OR=2.87; 95%CI 1.86-4.41] (valvular or coronary heart disease, cardiomyopathy, congestive heart failure, arrhythmias or device insertions), EMS interventions or concerning symptoms [OR=4.88; 95%CI 3.13- 7.62], age >50 years [OR=3.18; 95%CI 1.68-6.02], any abnormal vital signs [OR=1.58; 95%CI 1.03-2.42] (any EMS systolic blood pressure >180 or <100 mmHg, heart rate <50 or >100/minute, respiratory rate >25/minute, oxygen saturation <91%). [C-statistic: 0.81; Hosmer Lemeshow p=0.30]. Conclusion: We identified high-risk factors that are associated with 30-day SAE among syncope patients transported to the ED by EMS. This will aid in the development of a clinical decision tool to identify low-risk patients for diversion to alternate pathways of care.
MP27: Costs of emergency syncope care in Canada
- S. Kim, O. Cook, L. Yau, M.A. Mukarram, K. Arcot, A. Ishimwe, K. Thavorn, M. Taljaard, M. Sivilotti, B.H. Rowe, V. Thiruganasambandamoorthy
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S74
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Syncope is a common emergency department (ED) presentation and constitutes 1% of all ED visits, approximately 160,000 visits annually across Canada. Lack of standardized syncope care has economic and cost implications. Currently, emergency medical services (EMS) is over utilized, variations in ED management exist and a substantial proportion (46.5%) are hospitalized for cardiac monitoring. Our previous studies have proposed ways to reduce health care utilization through development of EMS clinical decision tool, ED risk scores and remote cardiac monitoring. We sought to: 1) Estimate costs associated with syncope care in the pre-hospital, ED and inpatient settings; and 2) Determine potential cost savings if the proposed alternate strategies were adopted. Methods: A prospective cohort study was conducted in five Canadian EDs from 2010-2014. We enrolled adult (≥16 years) syncope patients and excluded those with prolonged loss of consciousness, mental status changes, seizure, significant trauma, or alcohol/illicit drug abuse. Demographics, medical history, mode of arrival, EMS time points, reasons for hospitalization, ED and inpatient length of stay, final ED diagnosis and any serious adverse event within 30 days of index visit were collected. Descriptive and inferential statistics were used. Results: Out of 4,064 patients enrolled, 67.3% were transported to the ED by EMS and the average cost per event was $262.78 (range at study sites: $156.43-$553.03). The average cost per ED visit was $267.98 (range: $174.66-$374.95). 12.9% of the patients were admitted and the average of cost per admission was $9,886.15 (range: $9,715.23-$10,277.98). Syncope is associated with an estimated total annual cost of $257 million. In Canada, we estimate that diverting low-risk patients will save $5 million in the pre-hospital setting and $15 million in the ED annually, and implementing a remote cardiac monitoring strategy will save $50 million annually. Conclusion: It is estimated that the proposed strategies will save $70 million annually. This is likely an underestimation as cost savings due to reduction in investigations related to diversion of ED patients, reduction in ED length of stay and hospitalization are unaccounted. Adoption of similar strategies will likely lead to significantly higher cost savings in countries with higher resource utilization for syncope management.
LO98: Optimal length of observation for emergency department patients with syncope: a time to event analysis
- V. Thiruganasambandamoorthy, M. Sivilotti, M.A. Mukarram, C. Leafloor, K. Arcot, G.A. Wells, B.H. Rowe, A. Krahn, L. Huang, M. Taljaard
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S62
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Concern for occult serious conditions leads to variations in ED syncope management [hospitalization, duration of ED/inpatient monitoring including Syncope Observation Units (SOU) for prolonged monitoring]. We sought to develop evidence-based recommendations for duration of ED/post-ED ECG monitoring using the Canadian Syncope Risk Score (CSRS) by assessing the time to serious adverse event (SAE) occurrence. Methods: We enrolled adults with syncope at 6 EDs and collected demographics, time of syncope and ED arrival, CSRS predictors and time of SAE. We stratified patients as per the CSRS (low, medium and high risk as ≤0, 1-3 and ≥4 respectively). 30-day adjudicated SAEs included death, myocardial infarction, arrhythmia, structural heart disease, pulmonary embolism or serious hemorrhage. We categorized arrhythmias, interventions for arrhythmias and death from unknown cause as arrhythmic SAE and the rest as non-arrhythmic SAE. We performed Kaplan-Meier analysis using time of ED registration for primary and time of syncope for secondary analyses. Results: 5,372 patients (mean age 54.3 years, 54% females, and 13.7% hospitalized) were enrolled with 538 (10%) patients suffering SAE (0.3% died due to an unknown cause and 0.5% suffered ventricular arrhythmia). 64.8% of SAEs occurred within 6 hours of ED arrival. The probability for any SAE or arrhythmia was highest within 2-hours of ED arrival for low-risk patients (0.65% and 0.31%; dropped to 0.54% and 0.06% after 2-hours) and within 6-hours for the medium and high-risk patients (any SAE 6.9% and 17.4%; arrhythmia 6.5% and 18.9% respectively) which also dropped after 6-hours (any SAE 0.99% and 2.92%; arrhythmia 0.78% and 3.07% respectively). For any CSRS threshold, the risk of arrhythmia was highest within the first 15-days (for CSRS ≥2 patients 15.6% vs. 0.006%). ED monitoring for 2-hours (low-risk) and 6-hours (medium and high-risk) and using a CSRS ≥2 cut-off for outpatient 15-day ECG monitoring will lead to 52% increase in arrhythmia detection. The majority (82.2%) arrived to the ED within 2-hours (median time 1.1 hours) and secondary analysis yielded similar results. Conclusion: Our study found 2 and 6 hours of ED monitoring for low-risk and medium/high-risk CSRS patients respectively, with 15-day outpatient ECG monitoring for CSRS ≥2 patients will improve arrhythmia detection without the need for hospitalization or observation units.
LO95: A prospective evaluation of mild traumatic brain injuries in a working population in Edmonton, AB
- L. Gaudet, L. Eliyahu, J. Lowes, J. Beach, M. Mrazik, G. Cummings, K. Latoszek, L. Carroll, B.R. Holroyd, B.H. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S61
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Patients with mild traumatic brain injury (mTBI) frequently present to the emergency department (ED); however, wide variation in diagnosis and management has been demonstrated in this setting. Sub-optimal mTBI management can contribute to post-concussion syndrome (PCS), affecting vocational outcomes like return to work. This study documented the work-related events, ED management, discharge advice, and outcomes for employed patients presenting to the ED with mTBI. Methods: Adult (>17 years) patients presenting to one of three urban EDs in Edmonton, Alberta with Glasgow coma scale score ≥13 within 72 hours of a concussive event were recruited by on-site research assistants. Follow-up calls ascertained outcomes, including symptoms and their severity, advice received in the ED, and adherence to discharge instructions, at 30 and 90 days after ED discharge. Dichotomous variables were analyzed using chi-square testing; continuous variables were compared using t-tests or Mann-Whitney tests, as appropriate. Work-related injury and return to work outcomes were modelled using logistic or linear regression, as appropriate. Results: Overall, 250 patents were enrolled; 172 (69%) were employed at the time of their injury and completed at least one follow-up. The median age was 37 years (interquartile range [IQR]: 24, 49.5), both sexes were equally represented (48% male), and work-related concussions were uncommon (16%). Work-related concussion was related to manual labor jobs and self-reported history of attention deficit disorder. Patients often received advice to avoid sports (81%) and/or work (71%); however, the duration of recommended time off varied. Most employed patients (80%) missed at least one day of work (median=7 days; IQR: 3, 14); 91% of employees returned to work by 90 days, despite 41% reporting persistent symptoms. Increased days of missed work were linked to divorce, history of sleep disorder, and physician’s advice to avoid work. Conclusion: While work-related concussions are uncommon, most employees who sustain a mTBI at any time miss some work. Many patients experience mTBI symptoms past 90 days, which has serious implications for workers’ abilities to fulfill their work duties and risk of subsequent injury. Workers, employers, and the workers compensation system should take the necessary precautions to ensure that workers return to work safely and successfully following a concussion.
P057: Diagnosis for mild traumatic brain injury in three Canadian emergency departments: missed opportunities
- L. Gaudet, L. Eliyahu, J. Lowes, J. Beach, M. Mrazik, G. Cummings, K. Latoszek, L. Carroll, B.R. Holroyd, B.H. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue S1 / May 2017
- Published online by Cambridge University Press:
- 15 May 2017, p. S97
- Print publication:
- May 2017
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Patients with mild traumatic brain injury (mTBI) often present to the emergency department (ED). Incorrect diagnosis may delay appropriate treatment and recommendations for these patients, prolonging recovery. Notable proportions of missed mTBI diagnosis have been documented in children and athletes, while diagnosis of mTBI has not been examined in the general adult population. Methods: A prospective cohort study was conducted in one academic (site 1) and two non-academic (sites 2 and 3) EDs in Edmonton, Canada. On-site research assistants enrolled adult (>17 years) patients presenting within 72 hours of the injury event with clinical signs of mTBI and Glasgow comma scale score ≥13. Patient demographics, injury characteristics, and ED flow information were collected by chart review. Physician-administered questionnaires and patient interviews documented the recommendations given by emergency physicians at discharge. Bi-variable comparisons are reported using Pearson’s chi-square tests, Student’s t-tests or Mann-Whitney tests, as appropriate. Multivariate analyses were performed using logistic regression methods. Results: Overall, 130/250 enrolled patients were female, and the median age was 35. Proportions of successfully diagnosed mTBI varied significantly across study sites (Site 1: 89%; Site 2: 73%, Site 3: 53%; p>0.001). Patients without a diagnosis were less likely to receive a recommendation to follow-up with their family physician (OR=0.08; 95% CI: 0.03, 0.21) or advice about return to work (OR=0.17; 95% CI: 0.08, 0.04) or physical activity (OR=0.08; 95% CI: 0.04, 0.17). Patients with missed diagnoses had longer ED stays (median=5.0 hours; IQR: 3.8, 7.0) compared with diagnosed mTBI patients (median=3.9 hours; IQR: 3.0, 5.3). In the adjusted model, patients presenting to non-academic centers had reduced likelihood of mTBI diagnosis (Site 2: OR=0.21; 95% CI: 0.08, 0.58; Site 3: OR=0.07; 95% CI: 0.02, 0.24). Conclusion: The diagnostic accuracy of physicians assessing patients presenting with symptoms of mTBIs to these three EDs is suboptimal. The rates of missed diagnosis vary among EDs and were associated with length of ED stay. Closer examination of institutional factors, including diagnosis processes and personnel factors such as physician training, is needed to identify effective strategies to heighten the awareness of mTBI presentations.
LO087: Emergency department patients’ connection to primary care providers: reasons for lack of connection
- L. Krebs, S.W. Kirkland, K. Crick, C. Villa-Roel, A. Davidson, B. Voaklander, B. Holroyd, E. Cross, T. Nikel, R. Chetram, S. Couperthwaite, G. Cummings, D. Voaklander, B.H. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 18 / Issue S1 / May 2016
- Published online by Cambridge University Press:
- 02 June 2016, p. S60
- Print publication:
- May 2016
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Some non-urgent/low-acuity Emergency Department (ED) presentations are considered convenience visits and potentially avoidable with improved access to primary care services. This study surveyed patients who presented to the ED and explored their self-reported reasons and barriers for not being connected to a primary care provider (PCP). Methods: Patients aged 17 years and older were randomly selected from electronic registration records at three urban EDs in Edmonton, Alberta (AB), Canada. Following initial triage, stabilization, and verbal informed consent, patients completed a 47-item questionnaire. Data from the survey were cross-referenced to a minimal patient dataset consisting of ED and demographic information. The questionnaire collected information on patient characteristics, their connection to a PCP, and patients' reasons for not having a PCP. Results: Of the 2144 eligible patients, 1408 (65.7%) surveys were returned and 1402 (65.4%) were completed. The majority of patients (74.4%) presenting to the ED reported having a family physician; however, the ‘closeness’ of the connection to their family physician varied greatly among ED patients with the most recent family physician visit ranging from 1 hour before ED presentation to 45 years prior. Approximately 25% of low acuity ED patients reported no connection with a family physician. Reasons for a lack of PCP connection included: prior physician retired, left, or died (19.8%), they had never tried to find one (19.2%), they had recently moved to Alberta (18.0%), and they were unable to find one (16.5%). Conclusion: A surprisingly high proportion of ED patients (25.6%) have no identified PCP. Patients had a variety of reasons for not having a family physician. These need to be understood and addressed in order for primary care access to successfully contribute to diverting non-urgent, low acuity presentations from the ED.
LO091: Non-urgent presentations to the emergency department: patients’ reasons for presentation
- L. Krebs, R. Chetram, S.W. Kirkland, T. Nikel, B. Voaklander, A. Davidson, B. Holroyd, E. Cross, C. Villa-Roel, K. Crick, S. Couperthwaite, C. Alexiu, G. Cummings, D. Voaklander, B.H. Rowe
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 18 / Issue S1 / May 2016
- Published online by Cambridge University Press:
- 02 June 2016, p. S61
- Print publication:
- May 2016
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Some low acuity Emergency Department (ED) presentations are considered non-urgent or convenience visits and potentially avoidable with improved access to primary care. This study explored self-reported reasons why non-urgent patients presented to the ED. Methods: Patients, 17 years and older, were randomly selected from electronic registration records at three urban EDs in Edmonton, Alberta (AB), Canada during weekdays (0700 to 1900). A 47-item questionnaire was completed by each consenting patient, which included items on whether the patient believed the ED was their best care option and the rationale supporting their response. A thematic content analysis was performed on the responses, using previous experience and review of the literature to identify themes. Results: Of the 2144 eligible patients, 1408 (65.7%) questionnaires were returned, and 1402 (65.4%) were analyzed. For patients who felt the ED was their best option (n = 1234, 89.3%), rationales included: safety concerns (n = 309), effectiveness of ED care (n = 284), patient-centeredness of ED (n = 277), and access to health care professionals in the ED (n = 204). For patients who felt the ED was not their best care option (n = 148, 10.7%), rationales included a perception that: access to health professionals outside the ED was preferable (n = 39), patient-centeredness (particularly timeliness) was lacking in the ED (n = 26), and their health concern was not important enough to require ED care (n = 18). Conclusion: Even during times when alternative care options are available, the majority of non-urgent patients perceived the ED to be the most appropriate location for care. These results highlight that simple triage scores do not accurately reflect the appropriateness of care and that understanding the diverse and multi-faceted reasons for ED presentation are necessary to implement strategies to support non-urgent, low acuity care needs.
LO083: Outcomes and resource utilization among syncope patients transported by emergency medical services
- L. Yau, M.A. Mukarram, S. Kim, K. Arcot, K. Thavorn, M. Taljaard, M. Sivilotti, B.H. Rowe, V. Thiruganasambandamoorthy
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 18 / Issue S1 / May 2016
- Published online by Cambridge University Press:
- 02 June 2016, pp. S58-S59
- Print publication:
- May 2016
-
- Article
-
- You have access Access
- Export citation
-
Introduction: Syncope accounts for 1% of all annual emergency department (ED) visits in Canada with only 10.3% suffering serious adverse event (SAE) within 30-days. However, 66% are transported to ED by Emergency Medical Services (EMS). Our objectives were to assess 30 day SAE among syncope patients transported by Emergency medical services (EMS), assess the need to develop an EMS clinical decision aid, and estimate anticipated health care savings by diverting patients from the ED to alternative care pathways. Methods: We conducted a prospective cohort study at four tertiary care EDs from Feb 2012 to Feb 2013. We included patients ≥16 years of age with syncope and who arrived to the ED via EMS. We collected patient demographics, medical history, 30 day SAE, EMS time points (call received, EMS arrival on scene, EMS departure from scene, time of transfer of care in the ED), critical EMS interventions, and ED length of stay. We assessed for the occurrence of any SAE (death, arrhythmia, other cardiac and non-cardiac conditions) within 30 days of ED disposition. We used descriptive analysis, unpaired two-tailed t-test and chi-square test. Ethics approval was obtained at all study sites. Results: Of 1,475 ED patients with syncope during the study period, 992 (67.3%) arrived by EMS. Mean times (SD) for EMS arrival to the scene, patient assessment at the scene and transfer of patient from scene to the ED were 10.1 (6.4), 18.9 (8.3), and 14.6 (11.5) minutes respectively. Only two patients had critical interventions enroute (pacing and defibrillation). Overall 138 (13.9%) patients suffered a SAE; 32 (3.2%) detected by EMS, 58 (5.8%) detected during ED evaluation, 48 (4.8%) after ED disposition. The average ED length of stay was 5.9(4.2) hours. Based on average of cost from two sites, we estimated that total cost of transporting syncope patients from the scene to the ED to be $4 million in Canada. The total cost of ED care for syncope patients transported by EMS in Canada was calculated at $21.5 million. Conclusion: A substantial proportion of patients arriving to the ED via EMS suffer no SAE within 30 days. Correspondingly, our results suggest a need for an EMS clinical decision aid to divert low-risk syncope patients to alternative care pathways such as family physicians or rapid access clinics. If developed and implemented, this tool can potentially reduce EMS burden, ED crowding, and reduce healthcare costs.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Factors affecting subjective memory complaints in the AIBL aging study: biomarkers, memory, affect, and age
- R. Buckley, M. M. Saling, D. Ames, C. C. Rowe, N. T. Lautenschlager, S. L. Macaulay, R. N. Martins, C. L. Masters, T. O'Meara, G. Savage, C. Szoeke, V. L. Villemagne, K. A. Ellis, Australian Imaging Biomarkers and Lifestyle Study of Aging (AIBL) Research Group
-
- Journal:
- International Psychogeriatrics / Volume 25 / Issue 8 / August 2013
- Published online by Cambridge University Press:
- 22 May 2013, pp. 1307-1315
-
- Article
- Export citation
-
Background:
The prognostic value of subjective memory complaints (SMCs) in the diagnosis of dementia of the Alzheimer's type is unclear. While some studies have found an association between SMCs and cognitive decline, many have found a stronger association with depression, which raises questions about their diagnostic utility.
Methods:We examined the cross-sectional association between SMC severity (as measured using the MAC-Q, a brief SMC questionnaire) and affect, memory, and Alzheimer's disease (AD) biomarkers (β-amyloid deposition and the apolipoprotein E ε4 (APOEε4) allele) in healthy elderly controls (HC; M = 78.74 years, SD = 6.7) and individuals with mild cognitive impairment (MCI; M = 72.74 years, SD = 8.8). We analyzed a subset of individuals drawn from the Australian Imaging Biomarkers and Lifestyle (AIBL) Study of Aging.
Results:SMCs were more severe in MCI patients than in HCs. SMC severity was related to affective variables and the interaction between age and group membership (HC/MCI). Within the HC group, SMC severity was related to affective variables only, while severity correlated only with age in the MCI group. SMCs were not related to cognitive variables or AD biomarkers.
Conclusion:SMCs were related to solely by poorer mood (greater depressive and anxious symptomatology) in the cognitively healthy elderly however mean levels were subclinical. This finding argues for the assessment of affective symptomatology in conjunction with cognitive assessment in elderly memory complainers. Future AIBL research will focus on assessing other AD biomarkers, such as brain atrophy and Aβ plasma markers, in relation to complaint severity. Once our 36-month follow-up data are collected, we propose to assess whether SMCs can predict future cognitive decline.
A christening party outbreak of haemorrhagic colitis and haemolytic uraemic syndrome associated with Escherichia coli O 157. H7
- R. L. Salmon, I. D. Farrell, J. G. P. Hutchison, D. J. Coleman, R. J. Gross, N. K. Fry, B. Rowe, S. R. Palmer
-
- Journal:
- Epidemiology & Infection / Volume 103 / Issue 2 / October 1989
- Published online by Cambridge University Press:
- 15 May 2009, pp. 249-254
-
- Article
-
- You have access Access
- Export citation
-
A point source outbreak of haemorrhagic colitis due to Escherichia coli O 157. H7 producing verocytotoxin (VT), took place following a christening party in Birmingham in June 1987. Twenty-six people were affected, six were admitted to hospital and one developed haemolytic uraemic syndrome: there were no deaths. VT + E. coli O 157. H7 was isolated from 13 (57%) of 23 faecal specimens from affected people and from 3 (9%) of 33 specimens from asymptomatic people. Free VT was detected in the faeces of one further asymptomatic person. Illness was associated with eating turkey-roll sandwiches (P < 0·001) suggesting that cold meats might be an important source of infection.
Rare genetically defined causes of dementia
- K. E. Novakovic, V. L. Villemagne, C. C. Rowe, C. L. Masters
-
- Journal:
- International Psychogeriatrics / Volume 17 / Issue s1 / September 2005
- Published online by Cambridge University Press:
- 08 September 2005, pp. S149-S194
-
- Article
- Export citation
-
Several genetic disorders, though rare, are associated or present with dementia. Developments in the field of genetics are contributing to clarify and expand our knowledge of the complex physiopathological mechanisms leading to neurodegeneration and cognitive decline. Disorders associated with misfolded and aggregated proteins and lipid, metal or energy metabolism are examples of the multifarious disease processes converging in the clinical features of dementia, either as its predominant feature, as in cases of Alzheimer's disease (AD) or frontotemporal dementia (FTD), or as part of a cohort of accompanying or late-developing symptoms, as in Parkinson's disease (PD) or amyotrophic lateral sclerosis with dementia (ALS-D). Awareness of these disorders, allied with recent advances in genetic, biochemical and neuroimaging techniques, may lead to early diagnosis, successful treatment and better prognosis.
Frequency Analysis of the RRc Variables of the MACHO Database for the LMC
- G. Kovács, C. Alcock, R. Allsman, D. Alves, T. Axelrod, A. Becker, D. Bennett, C. Clement, K. H. Cook, A. Drake, K. Freeman, M. Geha, K. Griest, D. W. Kurtz, M. Lehner, S. Marshall, D. Minniti, C. Nelson, B. Peterson, P. Popowski, M. Pratt, P. Quinn, A. Rodgers, J. Rowe, C. Stubbs, W. Sutherland, A. Tomaney, T. Vandehei, D. L. Welch, The MACHO Collaboration
-
- Journal:
- International Astronomical Union Colloquium / Volume 176 / 2000
- Published online by Cambridge University Press:
- 12 April 2016, pp. 313-314
- Print publication:
- 2000
-
- Article
-
- You have access Access
- Export citation
-
We present the first massive frequency analysis of the 1200 first overtone RR Lyrae stars in the Large Magellanic Cloud observed in the first 4.3 yr of the MACHO project. Besides the many new double-mode variables, we also discovered stars with closely spaced frequencies. These variables are most probably nonradial pulsators.