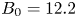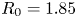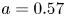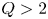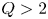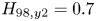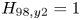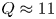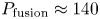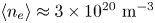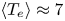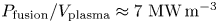105 results
Night-time/daytime Protein S100B serum levels in paranoid schizophrenic patients
- E. Diaz-Mesa, A. Morera-Fumero, L. Torres-Tejera, A. Crisostomo-Siverio, P. Abreu-Gonzalez, R. Zuñiga-Costa, S. Yelmo-Cruz, R. Cejas-Mendez, C. Rodriguez-Jimenez, L. Fernandez-Lopez, M. Henry-Benitez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S445-S446
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
S100B is a calcium-binding astrocyte-specific cytokine, that is considered a biomarker of neurodegeneration; which may be involved in the imbalance of the inflammatory response observed in several brain disorders, including major depression and schizophrenia. Two meta-analyses have reported higher serum levels of S100B in patients with schizophrenia respect to healthy controls.
Different studies have described circadian and seasonal variations of biological variables, such as melatonin or cortisol. It has been reported that there is not circadian rhythm of S100B blood levels in healthy subjects. However, it is not known whether there are circadian oscillations in S100B blood concentrations in patients with schizophrenia.
ObjectivesThe aim of this study is to describe S100B serum levels in patients with schizophrenia and to analyse whether they follow a circadian rhythm.
MethodsOur sample consists in 47 patients in acute phase and stabilized status. Blood samples were collected at 12:00 and 00:00 hours by venipuncture. Serum levels of Protein S100B were measured three times: at admission, discharge and three months after discharge. Protein S100B was measured by means of ELISA (Enzyme-linked immunosorbent assay) techniques.
Results12:00 24:00 P ADMISSION 132,95±199,27 85,85±121,44 0,004 DISCHARGE 73,65±71,744 75,80±123,628 0,070 CONTROL 43,49±34,60 40,14±23,08 0,47 P global P Admission Vs. Discharge P Admission Vs. Control P Discharge Vs. Control 0,97 There is a significance difference between 12:00 and 24:00 at admission for the Protein S100B.However, these difference did not occur at discharge and at three months after discharge.It can be interpreted as there is a circadian rhythm of Protein S100B when the patient has got a psychotic outbreak and disappears at discharge and when is psychopathologically stable.
ConclusionsWith respect to our results we can hypothesize that schizophrenic patients in acute relapse present circadian S100B rhythm that is not present when the patients are clinically stable.Furthermore, the decrease of serum protein S100B levels at discharge is indicative of a reduction of the cerebral inflammation, thus it can be a biomarker of cerebral inflammation and this reduction can be the effect of the treatment. Finally, its circadianity could be a guide of this process and clinical improvement.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
PALIPERIDONE PALMITATE 6-MONTH FORMULATION FOR THE TREATMENT OF SCHIZOPHRENIA: A 4-MONTH FOLLOW-UP STUDY
- S. L. Romero Guillena, G. Rodriguez Menendez, A. I. Florido Puerto, A. S. Fernández Flores
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1086-S1087
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Relapse prevention is critical because psychopathology and functionality can worsen in patients with schizophrenia because the repeated episodes and we have strong evidence of antipsychotics efficacy for relapse prevention, but nonadherence rates in patients with schizophrenia are very high, even in comparison with other illness. The literature speaks of average rates of 42% in schizophrenia. For that, long-acting injectable antipsychotics (LAIs) are considered important treatment option, but they are underutilized (Taipale et al. Schizophrenia Bulletin 2017; 44, 1381–1387) (Garcia et al. J Clin Psychopharmacol 2016; 36(4)355-371).
There is extensive clinical trial evidence for the use of paliperidone palmitate 1-month (PP1M) and paliperidone palmitate 3-month (PP3M) formulations for maintaining treatment continuity and preventing relapses and risk of hospitalizations in patients with schizophrenia. (Najarian et al. Int J Neuropsychopharmacol 2022; 25(3) 238-251).
Paliperidone palmitate 6-month (PP6M) formulation is a presentation that provides a dosing interval of once every six months. It is the first and only antipsychotic to be administered twice a year.
ObjectivesThe principal aim of this study was to evaluate the effectiveness, safety, and tolerability of the PP6M in people with non-acute schizophrenia in a naturalistic psychiatric outpatient setting
MethodsSample: 22 patients diagnosed with schizophrenia (DSM 5 criteria) that started treatment with PP6M after being stabilized with PP1M (N:10) or PP3M (N:12) (the treatment dose was not changed in the four months before study inclusion)
The mean dose of PP6M was 822.727 mg
Bimonthly, the following evaluations were performed during a follow-up period of 4 months:
The Clinical Global Impression-Schizophrenia scale (CGI-SCH)
Treatment adherence, concomitant medication, adverse events and the number of hospitalizations and emergency visits
Efficacy values: Percentage of patients who remained free of admissions at the end of 4months of follow-up.
Other evaluation criteria: Percentage of patients who never visited the emergency department at the end of 4 months of follow-up, average change from baseline visit to the final evaluation as assessed by score obtained on the following scale: GSI-SCH, treatment adherence rate and tolerability.
ResultsThe percentage of patients who remained free of admissions at the end of the 4 months was 100% and the percentage of patients who never visited the emergency department at the end of 4 months was 100 %
Mean variations from baseline scores at 4 months were: (-0.21 ±0.31) on the GCI-SCH.
The rate of adherence to treatment with PP6M after 4 months was 100%.
Tolerability was good. None of the patients experienced an adverse event.
ConclusionsIn our study, we found that short-term treatment with paliperidone palmitate 6-month formulation is effective and well tolerated in clinical practice conditions
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
“Keeping an eye on amylase”. Side effects of antidepressants
- T. Jiménez Aparicio, G. Medina Ojeda, A. Rodríguez Campos, L. Rodríguez Andrés, C. Vallecillo Adame, C. De Andrés Lobo, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. J. Mateos Sexmero, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M. P. Pando Fernández, P. Martínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Both in consultations with the general practitioner and with the psychiatrist, antidepressants are one of the most used drugs (1). These have multiple indications, and there are different groups according to their mechanism of action. In relation to this case, we are going to talk about Venlafaxine, a dual-type antidepressant, that is, it inhibits the reuptake of serotonin and norepinephrine. One of the most common side effects is digestive discomfort, which usually resolves after a few weeks (2). However, we should not ignore these symptoms, since they can hide something more serious.
ObjectivesPresentation of a clinical case on a patient who presented an increase in pancreatic amylase after starting treatment with Venlafaxine.
MethodsBibliographic review including the latest articles in Pubmed on side effects of antidepressant treatment, and more specifically at the gastrointestinal level (in this case we will talk about pancreatitis).
ResultsWe present the case of a 49-year-old woman, who was hospitalized 2 years ago, due to a first depressive episode. During this admission, psychopharmacological treatment was started for the first time, on that occasion with a selective serotonin reuptake inhibitor (SSRI), treatment of first choice (3). The patient had no side effects at that time, but the response was very modest, so it was decided to replace that antidepressant with Venlafaxine (with dual action), up to 150mg. The depressive symptoms improved markedly, however the patient began to feel digestive discomfort (which at first did not seem to be of great importance). A general analysis was performed, in which an increase in lipase (978 U/L) and amylase (528 U/L) was detected. An echoendoscopy, an abdominal scan, and a magnetic resonance cholangiography were performed; Pancreatitis secondary to drugs was suspected (a severe condition). Luckily, no significant lesions were found in the tests, and the levels of amylase and lipase decreased when Venlafaxine treatment was withdrawn (without reaching the normal range). The patient was discharged and continued to attend consultations. In the last control, amylase had dropped to 225 U/L. His abdominal pain disappeared. Treatment with Vortioxetine (a multimodal antidepressant) was started, however the amylase levels continue to be monitored, and the patient continues to see the gastroenterologist.
ConclusionsGastrointestinal side effects are very common when taking antidepressant treatment, and in most cases they do not usually represent a serious problem.
However, it is described in the scientific literature that in some cases, acute pancreatitis secondary to some drugs, including Venlafaxine, can occur (4). In order to detect it, it is necessary to perform a blood test and sometimes also other complementary tests.
For its treatment, the fundamental thing is to withdraw the causing drug, trying to find other alternatives, and carry out a control to monitor possible complications
Disclosure of InterestNone Declared
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Personality disorders and Juvenil Myoclonic Epilepsy
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S668
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a high comorbidity between psychiatric disorders and juvenile myoclonic epilepsy (JME), observed in up to 58% of these patients; specifically, mood disorders, anxiety and personality disorders (PD). In some patients with PD there are nonspecific alterations in the EEG, which nevertheless sometimes involve pathology. The presence of personality disorders along with JME has been repeatedly described. Previous studies have emphasized the difficulties in treating patients with JME, which have been attributed to some specific psychiatric, psychological and psychosocial characteristics.
ObjectivesDescribing distinctive personality traits in JME
MethodsReview of scientific literature based on a relevant clinical case.
Results19-year-old woman, single. Psychiatric history since she was 12 due to anxiety-depressive symptoms, after being diagnosed with JME. 4 admissions in Psychiatry, with a variety of diagnoses: eating disorder, attention deficit hyperactivity disorder and borderline personality disorder. The evolution of both disorders has been parallel, presenting epileptic seizures due to irregular therapeutic adherence together with pseudo-seizures, which made difficult their differential diagnosis. In addition, he has had frequent visits to the emergency room for suicide attempts and impulsive behaviors.
ConclusionsIn 1957, for the first time, distinctive personality traits were described in patients with JME: lack of control and perseverance, emotional instability, variable self-concept and reactive mood, which have been confirmed in subsequent studies. It is believed as epilepsy progresses, patients tend to develop symptoms of depression, anxiety, social problems, and attention deficit. Therefore, these patients have difficulty in following medical recommendations, especially precautions regarding precipitating factors for seizures.
DisclosureNo significant relationships.
Sleep Disorders and Dual Disorders
- L. Fernandez Mayo, D. Baño Rodrigo, E. Barbero García, M. Agujetas Rodriguez, I. Falcón Torres, V. De Antonio Pérez, C. Medina Sanchez, M. Serrano García
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S466
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
While it is well known that there is an interaction between sleep disorders and substance abuse, it is certainly more complex than was previously thought. The effects on sleep depend on the substance used, but it has been shown that both during use and in withdrawal periods consumers have various sleep problems, and basically more fragmented sleep. We know that sleep problems must be taken into account to prevent addiction relapses.
ObjectivesTo explain the different sleep disorders caused by substances such as alcohol and cannabis
MethodsAs an example of this, two cases are introduced: the first one, a 17-year-old boy, who is diagnosed with ADHD with daily cannabis use since the age of 14. As a result of reducing consumption, he presents an episode of sleep paralysis that he had not previously had. The second one is a 50-year-old man diagnosed with a personality disorder and with dependence on cannabis and alcohol for years. He currently has abstinence from alcohol for months and maintains daily cannabis use. However, he has long-standing sleep pattern disturbances and frequent depersonalization phenomena at night.
ResultsAlcohol at low doses has no clear effects on sleep architecture. At higher doses it decreases sleep latency, as well as awakenings. In chronic alcoholic patients, a decrease in deep slow sleep, and more fragmented sleep have been found. Cannabis withdrawal reduces sleep quality, increases latency, and produces strange dreams.
ConclusionsThere is a positive relationship both between having a substance use disorder and suffering from a sleep disorder.
DisclosureNo significant relationships.
Voices change my name
- C. Vallecillo Adame, T. Jiménez Aparicio, C. De Andrés Lobo, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, B. Rodríguez Rodríguez, M. Fernández Lozano, M.J. Mateos Sexmero, N. Navarro Barriga, N. De Uribe Viloria, G. Medina Ojeda, L. Rodriguez Andrés
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S801
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the clinical case of a patient where the psychotic clinic coexists with gender dysphoria. This scenario can be the result of a change in gender identity derived from the psychotic process or appear independently of it.
ObjectivesWe want to explain the importance of knowing how to act with a patient in whom these two processes coexist.
Methods20-year-old woman, with no history of mental health. She comes to the emergency department for behavioral alteration. The family observes strange behaviors, unmotivated laughter, soliloquies and aggressive episodes. Abandonment of studies, hobbies and radical physical change. Delusions of prejudice and self-referential delusions. Possible phenomena of echo and diffusion of the thought. Auditory hallucinations talking to her in male gender, since then she presents doubts about her sexual identity and manifests her desire to change sex. Altered judgment of reality.
ResultsDuring admission, we started treatment with an antipsychotic with good tolerance and she was referred to mental health team, where psychopharmacological treatment was adjusted with good response. In the following medical appointments the psychotic clinic disappeared at the same time that sexual identification was completely restored and made a critique of the behavior and experiences.
ConclusionsThis case highlights the importance of assessing the chronology of symptoms, the patient’s criticality, the response to antipsychotic treatment and the need to exclude the psychotic background of the desire for gender reassignment before making a therapeutic decision.
DisclosureNo significant relationships.
Suicidal behaviour and cognition: A systematic review with special focus on prefrontal deficits
- J. Fernández-Sevillano, A. González-Pinto, J. Rodríguez-Revuelta, S. Alberich-Mesa, L. González-Blanco, I. Zorrilla-Martínez, Á. Velasco, P. López-Pena, I. Abad-Acebedo, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S584
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicidal behaviour and cognition: A systematic review with special focus on prefrontal deficits Introduction: Suicide is a major health concern worldwide, thus, identifying risk factors would enable a more comprehensive understanding and prevention of this behaviour. Neuropsychological alterations could lead to difficulties in interpreting and managing life events resulting in a higher risk of suicide.
ObjectivesObjective: Bibliographic review about the influence of neuropsychological deficits on suicidal behaviour.
MethodsMethod: A systematic literature search from 2000 to 2020 was performed in Medline (Pubmed), Web of Science, SciELO Citation Index, PsycInfo, PsycArticles and Cochrane Library databases regarding studies comparing cognition of attempters versus non-attempters that share same psychiatric diagnosis. Results: 1.885 patients diagnosed with an Affective Disorder (n = 1512) and Schizophrenia/ Schizoaffective Disorder (n = 373) were included.
ResultsIn general comparison, attention was found to be clearly dysfunctional. Regarding diagnosis, patients with Schizophrenia and previous history of suicidal behaviour showed a poorer performance in executive function. Patients with current symptoms of an Affective Disorder and a previous history of suicidal attempt had poorer performance in attention and executive function. Similarly, euthymic affective patients with history of suicidal behaviour had worse decision-making, attention and executive function performance compared to euthymic non-attempters.
ConclusionsPatients who have attempted suicide have a poorer neuropsychological functioning than non-attempters with a similar psychiatric disorder in attention and executive function. These alterations increase vulnerability for suicide.
Conflict of interestJessica Fernández-Sevillano is beneficiary of the Pre-PhD Training Programme of the Basque Government. Dr. Gonzalez-Pinto has received grants and served as consultant, advisor or CME speaker for the following entities: Almirall, AstraZeneca, Bristol-Myers
Attempted suicide and pregnancy in COVID-19´s times
- M.O. Solis, L. Soldado Rodriguez, S.S. Sánchez Rus, M. ValverDe Barea, S. Jimenez Fernandez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S270
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pregnancy is a special risk factor for suicide attempts among females (Andrew E. Czeizel et al. 2011). Situational factors such as the novel coronavirus (COVID-19) have also been reported to impact on individual’s mental health.
ObjectivesExamine the effect of COVID-19 and its association with mental health and attempt suicide risk in pregnant population.
MethodsA cross-sectional study that includes 113 pregnant women from Spain, through an anonymous, voluntary and multiple response type online survey which included questions about socio demographic aspects, COVID-19’s aspects and mental health.
ResultsOf the 112 pregnant patients surveyed, only 2 reported suicidal ideation. The age of the respondents was 32 and 33 years, both of whom were in the 2nd trimester of pregnancy. Both report that it was the first pregnancy and affirm a worsening of their economic situation since the beginning of the COVID-19 pandemic. One of them did not have a partner / marriage and was living with a relative, in turn this respondent was unemployed. Both responded that they were “always” worried about the possible outcome of the COVID-19 pandemic and that their fears had increased, being difficult to control and let them pass. It is very relevant that both agree that they “never” felt that the professionals who carried out the pregnancy controls asked or inquired about their current state of mental health.
ConclusionsAntepartum suicidal ideation is an important and common complication of pregnancy, specially in COVID-19’s times, healthcare professionals who follow pregnancy should detect high-risk suicidal patients and be able to carry out a suicide prevention program.
Impact of early use of long acting paliperidone (1 and 3 monthly) in a first-episode psychosis sample
- P. Gil Lopez, J.M. Rodriguez, L. Garcia Fernandez, E. Fernandez Martin, N. Fernandez Gayoso, V. Sanchez Estevez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S811
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Relapse prevention is a key objetive for patients with a First Episode Psychosis (FEP) and the low adherence to antipsychotic (AP) treatment is the main reason for relapse after a FEP.
ObjectivesThere are no clear recommendations about the early use of long-acting injectables (LAIs) in FEP. We review the impact on hospitalization rates of the early use (earlier than 1 year after the inclusion in our Early Intervention Service “Lehenak”) of LAI paliperidone in a FEP sample.
MethodsWe evaluated in a naturalistic study a sample (N=384) of patients with a FEP. We carried out a mirror-design study to compare the numer of hospitalizations before and after the introduction of LAI paliperidone (1 and 3 monthly) in early users (<1 year) vs late users (>1 year).
ResultsA total of 384 FEP patients with LAI paliperidone were assessed.
Early Paliperidone LAI (n=201) Late Paliperidone LAI (n=173) Within groups comparisons t (p) Hospitalizations pre-LAI mirror period (media, standard deviation) 1.76 (1.97) 2.22 (2.60) 1,87 (0.06) Days in hospital pre-LAI mirror period 21.42 (28.28) 28.02 (38.27) 1.87 (0.06) Hospitalizations post-LAI mirror period 0.68 (1.61) 0.80 (1.74) 0.73 (0.46) Days in hospital post-LAI mirror period 15.17 (40.58) 18.78 (45.24) 0.81 (0.42) ConclusionsThere was no difference between the early and late introduction of LAI Paliperidone in the number of hospitalizations after treatament. There was a trend to present more previous hospitalizations and days in hospital in late users. This could support an earlier use of paliperidone LAI to prevent an excess of hospitalizations due to late introduction.
DisclosureThe presenting author has received honouraria for lectures or advisory boards from Janssen, Otsuka, Lundbeck and Angelini in the last five years.
Effect of long-acting injectable paliperidone 3 monthly and aripiprazol 1 monthly on hospitalization rate in a first-episode psychosis
- P. Gil Lopez, J.M. Rodriguez Sanchez, L. Garcia Fernandez, V. Sanchez Estevez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S812
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIs) can reduce relapse and hospitalization risk but they are not widely used in first psychotic episode (FEP) patientes.
ObjectivesTo examine the effcacy of two of the most used second generation LAI antipsychotics (paliperione 3 monthly and aripiprazol 1 monthly) to reduce hospitalization rates.
MethodsWe evaluated in a naturalistic study a sample of patients (n=277) with a FEP. We carried out a mirror-design study to compare the number of hospitalizations and days in hospital before and after the introduction of LAI paliperidone (3 monthly) or LAI aripiprazol. In our Early Intervention Services (Lehenak) antipsychotic treatment is not protocolized and is established for each patient according to the psychiatrist criteria.
ResultsWe review the oucome of 277 FEP treated in our Early Intervention Service “Lehenak” with LAI paliperidone 3 monthly (n=156) or LAI Aripiprazol (n=121)
Pre LAI Mirror Period Post LAI Mirror Period Within group comparisons (paired t-test) t p Aripiprazol LAI number of Hospitalizations (mean, standard deviation) 2.31 (1.72) 0.73 (1.23) 17.4 (<0.001) Paliperidone LAI 3 monthly number of Hospitalizations number 0,68 (0.93) 0.15 (0.47) 4.62 (<0.001) Aripiprazol LAI Days in Hospital 30.26 (33.52) 17.02 (38.19) 2.93 (0.004) Paliperidone LAI 3 monthly Days in hospital 12.63 (24.23) 3.40 (14.18)) 7.5 (<0.001) ConclusionsBoth LAI paliperidone 3 monthly and LAI aripiprazol had a postive impact on hospitalIzation rate, decreasing them significantly after their introduction. These data also support a more extensive use of LAI paliperidone 3 monthly in FEP.
DisclosurePresenting author has received honouraria for lectures or advisory boards from Janssen, Otsuka, Lundbeck and Angelini in the last five years
Overview of the SPARC tokamak
- Part of
- A. J. Creely, M. J. Greenwald, S. B. Ballinger, D. Brunner, J. Canik, J. Doody, T. Fülöp, D. T. Garnier, R. Granetz, T. K. Gray, C. Holland, N. T. Howard, J. W. Hughes, J. H. Irby, V. A. Izzo, G. J. Kramer, A. Q. Kuang, B. LaBombard, Y. Lin, B. Lipschultz, N. C. Logan, J. D. Lore, E. S. Marmar, K. Montes, R. T. Mumgaard, C. Paz-Soldan, C. Rea, M. L. Reinke, P. Rodriguez-Fernandez, K. Särkimäki, F. Sciortino, S. D. Scott, A. Snicker, P. B. Snyder, B. N. Sorbom, R. Sweeney, R. A. Tinguely, E. A. Tolman, M. Umansky, O. Vallhagen, J. Varje, D. G. Whyte, J. C. Wright, S. J. Wukitch, J. Zhu, the SPARC Team
-
- Journal:
- Journal of Plasma Physics / Volume 86 / Issue 5 / October 2020
- Published online by Cambridge University Press:
- 29 September 2020, 865860502
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The SPARC tokamak is a critical next step towards commercial fusion energy. SPARC is designed as a high-field (
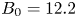 $B_0 = 12.2$ T), compact (
$B_0 = 12.2$ T), compact (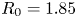 $R_0 = 1.85$ m,
$R_0 = 1.85$ m, 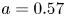 $a = 0.57$ m), superconducting, D-T tokamak with the goal of producing fusion gain
$a = 0.57$ m), superconducting, D-T tokamak with the goal of producing fusion gain 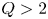 $Q>2$ from a magnetically confined fusion plasma for the first time. Currently under design, SPARC will continue the high-field path of the Alcator series of tokamaks, utilizing new magnets based on rare earth barium copper oxide high-temperature superconductors to achieve high performance in a compact device. The goal of
$Q>2$ from a magnetically confined fusion plasma for the first time. Currently under design, SPARC will continue the high-field path of the Alcator series of tokamaks, utilizing new magnets based on rare earth barium copper oxide high-temperature superconductors to achieve high performance in a compact device. The goal of 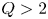 $Q>2$ is achievable with conservative physics assumptions (
$Q>2$ is achievable with conservative physics assumptions (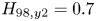 $H_{98,y2} = 0.7$) and, with the nominal assumption of
$H_{98,y2} = 0.7$) and, with the nominal assumption of 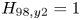 $H_{98,y2} = 1$, SPARC is projected to attain
$H_{98,y2} = 1$, SPARC is projected to attain 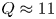 $Q \approx 11$ and
$Q \approx 11$ and 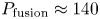 $P_{\textrm {fusion}} \approx 140$ MW. SPARC will therefore constitute a unique platform for burning plasma physics research with high density (
$P_{\textrm {fusion}} \approx 140$ MW. SPARC will therefore constitute a unique platform for burning plasma physics research with high density (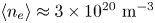 $\langle n_{e} \rangle \approx 3 \times 10^{20}\ \textrm {m}^{-3}$), high temperature (
$\langle n_{e} \rangle \approx 3 \times 10^{20}\ \textrm {m}^{-3}$), high temperature (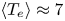 $\langle T_e \rangle \approx 7$ keV) and high power density (
$\langle T_e \rangle \approx 7$ keV) and high power density (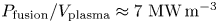 $P_{\textrm {fusion}}/V_{\textrm {plasma}} \approx 7\ \textrm {MW}\,\textrm {m}^{-3}$) relevant to fusion power plants. SPARC's place in the path to commercial fusion energy, its parameters and the current status of SPARC design work are presented. This work also describes the basis for global performance projections and summarizes some of the physics analysis that is presented in greater detail in the companion articles of this collection.
$P_{\textrm {fusion}}/V_{\textrm {plasma}} \approx 7\ \textrm {MW}\,\textrm {m}^{-3}$) relevant to fusion power plants. SPARC's place in the path to commercial fusion energy, its parameters and the current status of SPARC design work are presented. This work also describes the basis for global performance projections and summarizes some of the physics analysis that is presented in greater detail in the companion articles of this collection.
The prevalence of the metabolic syndrome in bipolar patients
- M.P. Garcia-Portilla, P.A. Saiz, I. Menendez, P. Sierra, L. Livianos, A. Benabarre, J. Perez, A. Rodriguez, J. Valle, F. Sarramea, R. Fernandez-Villamor, J.M. Montes, M.J. Muñiz
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, p. S252
-
- Article
-
- You have access Access
- Export citation
-
Background and aims:
Two studies to date have been published regarding the prevalence of the metabolic syndrome in bipolar patients. The unadjusted prevalence rates reported were 30% and 32%. The aim of this study was to evaluate the prevalence of the metabolic syndrome in a group of 142 bipolar patients from Spain.
Methods:Bipolar patients (ICD-10 criteria) from 11 centres in Spain were assessed cross-sectionally for metabolic syndrome according to the NCEP ATP III criteria.
Results:The mean age was 47.3 (SD 14.5), 51.1% were male. On average, patients were receiving 2.8 (SD 1.3) drugs for the treatment of their bipolar disorder. Ninety-one percent were receiving mood stabilizers, 63.4% antipsychotics and 29.6 antidepressants. Eighty-seven percent of the antipsychotics prescribed were atypicals. The overall prevalence of metabolic syndrome in our sample was 24.6% Fifty-seven percent of the sample met the criterion for abdominal obesity, 37.4% for met the criterion for hypertriglyceridemia, 36.4% for low HDL-cholesterol, 25.2% for high blood pressure and 12.5% for high fasting glucose. No statistically significant difference was found between with and without the metabolic syndrome for gender, illness status (acute versus in remission), CGI-S-BP scores and number of medications used. Patients taking tow mood stabilizers had significantly higher metabolic syndrome rates than patients taking one mood stabilizer and than patients without mood stabilizer treatment (40% versus 17.8% and 11.1% respectively, p .02).
Conclusions:The prevalence of the metabolic syndrome in bipolar patients is high. It appears to be higher than that estimated for the Spanish general population.