9 results
Colonization with extended-spectrum cephalosporin-resistant Enterobacterales (ESCrE) in hospitalized patients in Botswana
- Naledi Betsi Mannathoko, Mosepele Mosepele, Robert Gross, Rachel Smith, Ashley Styczynski, Leigh Cressman, Melissa Richard-Greenblatt, Laurel Glaser, Kevin Alby, Anne Jaskowiak, Kgotlaetsile Sewawa, Laura Cowden, Dimpho Otukile, Giacomo Paganotti, Margaret Mokomane, Warren Bilker, Ebbing Lautenbach
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s81
-
- Article
-
- You have access Access
- Open access
- Export citation
-
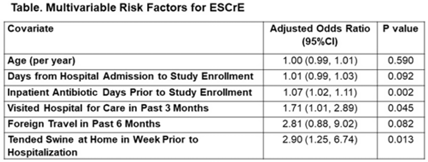
Background: The epidemiology of extended-spectrum cephalosporin-resistant Enterobacterales (ESCrE) in hospitalized patients in low- and middle-income countries (LMICs) is poorly described. Although risk factors for ESCrE clinical infection have been studied, little is known of the epidemiology of ESCrE colonization. Identifying risk factors for ESCrE colonization, which can predispose to infection, is therefore critical to inform antibiotic resistance reduction strategies. Methods: This study was conducted in 3 hospitals located in 3 districts in Botswana. In each hospital, we conducted ongoing surveillance in sequential units hospitalwide. All participants had rectal swabs collected which were inoculated onto chromogenic media followed by confirmatory testing using MALDI-TOF MS and VITEK-2. Data were collected via interview and review of the inpatient medical record on demographics, comorbidities, antibiotic use, healthcare exposures, invasive procedures, travel, animal contact, and food consumption. Participants with ESCrE colonization (cases) were compared to noncolonized participants (controls) using bivariable and multivariable analyses to identify risk factors for ESCrE colonization. Results: Enrollment occurred from January 15, 2020, to September 4, 2020, and 469 participants were enrolled. The median age was 42 years (IQR, 31–58) and 320 (68.2%) were female. The median time from hospital admission to date of sampling was 5 days (IQR, 3–12). There were 179 cases and 290 controls (ie, 38.2% of participants were ESCrE colonized). Independent risk factors for ESCrE colonization were a greater number of days on antibiotic, recent healthcare exposure, and tending swine prior to hospitalization. (Table). Conclusions: ESCrE colonization among hospitalized patients was common and was associated with several exposures. Our results suggest prior healthcare exposure may be important in driving ESCrE. The strong link to recent antibiotic use highlights the potential role of antibiotic stewardship interventions for prevention. The association with tending swine suggests that animal husbandry practices may play a role in community exposures, resulting in colonization detected at the time of hospital admission. These findings will help to inform future studies assessing strategies to curb further emergence of hospital ESCrE in LMICs.
Disclosures: None
370 Epicardial adipose tissue and cardiometabolic health in youth-onset type 2 diabetes undergoing vertical sleeve gastrectomy
- Part of
- Tyler Dobbs, Megan Kelsey, Melanie Cree-Green, Amy Baumgartner, Alex Bailey, Susan Gross, Laura Pyle, Thomas Inge, Petter Bjornstad, Kristen Nadeau
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: The goal of this study is to investigate the potential independent relationship between epicardial adipose tissue (EAT) and cardiometabolic health in youth-onset type 2 diabetes (T2D) and explore changes in EAT as a potential mediator of changes in cardiometabolic health in response to vertical sleeve gastrectomy (VSG). METHODS/STUDY POPULATION: We will assess glycemic control, insulin sensitivity and secretion in youth with T2D before and 3 months after VSG. Fasting labs, anthropometrics, and a 4-hour, frequently sampled liquid mixed meal tolerance test (45g carbohydrates, 14g fat, and 14g protein) were performed. Calculations included glucose, insulin, and GLP-1 area under the curve (AUC), Matsuda Index, HOMA-IR, and oral disposition index (DI). These cardiometabolic outcomes will then be assessed for associations between total EAT volume, measured from cardiac MRI. RESULTS/ANTICIPATED RESULTS: Previous studies have shown that individuals with obesity have higher EAT than lean controls, and adults with T2D have even higher EAT than obese controls. Therefore, we anticipate that our participants will have higher volume of EAT than what has been reported in the literature and that they will have worsening cardiometabolic outcomes without MBS. Our anticipated results will include: Weight and BMI, hemoglobin A1c, diabetes medications, Matsuda Index, HOMA-IR, DI, and glucose and insulin AUC during an MMTT. Cardiac MRI's are being analyzed and will give total EAT volume and will be analyzed for correlations with the cardiometabolic outcomes of body composition, aortic stiffness, blood pressure, cardiac structure and function, as well as lipid panel and insulin sensitivity. DISCUSSION/SIGNIFICANCE: This study is the first to specifically assess EAT in adolescents with T2D. The assessment of EAT will be done with gold-standard MRI and correlated with cardiometabolic health assessed by gold-standard methods. Together, the results will give insight into EAT as a potential independent cardiometabolic risk factor in adolescents undergoing VSG.
Decreased hospital readmissions after programmatic strengthening of an outpatient parenteral antimicrobial therapy (OPAT) program
- Gaurav Agnihotri, Alan E. Gross, Minji Seok, Cheng Yu Yen, Farah Khan, Laura M. Ebbitt, Cassandra Gay, Susan C. Bleasdale, Monica K. Sikka, Andrew B. Trotter
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 21 February 2023, e33
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To determine whether a structured OPAT program supervised by an infectious disease physician and led by an OPAT nurse decreased hospital readmission rates and OPAT-related complications and whether it affected clinical cure. We also evaluated predictors of readmission while receiving OPAT.
Patients:A convenience sample of 428 patients admitted to a tertiary-care hospital in Chicago, Illinois, with infections requiring intravenous antibiotic therapy after hospital discharge.
Methods:In this retrospective, quasi-experimental study, we compared patients discharged on intravenous antimicrobials from an OPAT program before and after implementation of a structured ID physician and nurse-led OPAT program. The preintervention group consisted of patients discharged on OPAT managed by individual physicians without central program oversight or nurse care coordination. All-cause and OPAT-related readmissions were compared using the χ2 test. Factors associated with readmission for OPAT-related problems at a significance level of P < .10 in univariate analysis were eligible for testing in a forward, stepwise, multinomial, logistic regression to identify independent predictors of readmission.
Results:In total, 428 patients were included in the study. Unplanned OPAT-related hospital readmissions decreased significantly after implementation of the structured OPAT program (17.8% vs 7%; P = .003). OPAT-related readmission reasons included infection recurrence or progression (53%), adverse drug reaction (26%), or line-associated issues (21%). Independent predictors of hospital readmission due to OPAT-related events included vancomycin administration and longer length of outpatient therapy. Clinical cure increased from 69.8% before the intervention to 94.9% after the intervention (P < .001).
Conclusion:A structured ID physician and nurse-led OPAT program was associated with a decrease in OPAT-related readmissions and improved clinical cure.
Brain-derived neurotrophic factor, depressive symptoms and somatic comorbidity in patients with coronary heart disease
- Mira Tschorn, Stella Linnea Kuhlmann, Nina Rieckmann, Katja Beer, Laura Grosse, Volker Arolt, Johannes Waltenberger, Wilhelm Haverkamp, Jacqueline Müller-Nordhorn, Rainer Hellweg, Andreas Ströhle
-
- Journal:
- Acta Neuropsychiatrica / Volume 33 / Issue 1 / February 2021
- Published online by Cambridge University Press:
- 24 September 2020, pp. 22-30
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Depression and coronary heart disease (CHD) are highly comorbid conditions. Brain-derived neurotrophic factor (BDNF) plays an important role in cardiovascular processes. Depressed patients typically show decreased BDNF concentrations. We analysed the relationship between BDNF and depression in a sample of patients with CHD and additionally distinguished between cognitive-affective and somatic depression symptoms. We also investigated whether BDNF was associated with somatic comorbidity burden, acute coronary syndrome (ACS) or congestive heart failure (CHF).
Methods:The following variables were assessed for 225 hospitalised patients with CHD: BDNF concentrations, depression [Patient Health Questionnaire-9 (PHQ-9)], somatic comorbidity (Charlson Comorbidity Index), CHF, ACS, platelet count, smoking status and antidepressant treatment.
Results:Regression models revealed that BDNF was not associated with severity of depression. Although depressed patients (PHQ-9 score >7) had significantly lower BDNF concentrations compared to non-depressed patients (p = 0.04), this was not statistically significant after controlling for confounders (p = 0.15). Cognitive-affective symptoms and somatic comorbidity burden each closely missed a statistically significant association with BDNF concentrations (p = 0.08, p = 0.06, respectively). BDNF was reduced in patients with CHF (p = 0.02). There was no covariate-adjusted, significant association between BDNF and ACS.
Conclusion:Serum BDNF concentrations are associated with cardiovascular dysfunction. Somatic comorbidities should be considered when investigating the relationship between depression and BDNF.
Contributors
-
- By J. William Allwood, Eleni T. Bairaktari, Jean-Pierre Bellocq, Malika A. Benahmed, Hanne Christine Bertram, Zaver M. Bhujwalla, Ulrich Braumann, Juan Casado-Vela, Marta Cascante, Arancha Cebrián, Albert Chen, Man Ho Choi, Bong Chul Chung, Yuen-Li Chung, Morten Rahr Clausen, Patrick J. Cozzone, Ralph J. DeBerardinis, Julien Detour, Santiago Díaz-Moralli, Warwick B. Dunn, Karim Elbayed, Udo Engelke, Teresa W.-M. Fan, Ana M. Gil, Kristine Glunde, Markus Godejohann, Teresa Gómez del Pulgar, Royston Goodacre, Angelina Goudswaard, Gonçalo Graça, Richard W. Gross, Herbert H. Hill, Ralph E. Hurd, Alessio Imperiale, Kimberly A. Kaplan, Neil L. Kelleher, Michael A. Kiebish, Ann M. Knolhoff, Christina E. Kostara, Juan Carlos Lacal, Andrew N. Lane, Martin O. Leach, Norbert W. Lutz, Elizabeth Maher, Craig R. Malloy, Isaac Marin-Valencia, Laura Menchén, Bruce Mickey, Fanny Mochel, Éva Morava, François-Marie Moussallieh, Izzie J. Namer, Peter Nemes, Ioanna Ntai, Geoffrey S. Payne, Marie-France Penet, Martial Piotto, Stanislav S. Rubakhin, Elsa Sánchez-López, A. Dean Sherry, Bindesh Shrestha, Jonathan V. Sweedler, Akos Vertes, Mark R. Viant, Ralf J. M. Weber, Ron Wehrens, Ron A. Wevers, Catherine L. Winder, David S. Wishart, Kui Yang, Yi-Fen Yen
- Edited by Norbert W. Lutz, Jonathan V. Sweedler, University of Illinois, Urbana-Champaign, Ron A. Wevers
-
- Book:
- Methodologies for Metabolomics
- Published online:
- 05 January 2013
- Print publication:
- 21 January 2013, pp viii-xii
-
- Chapter
- Export citation
Dietary fatty acid intake, its food sources and determinants in European adolescents: the HELENA (Healthy Lifestyle in Europe by Nutrition in Adolescence) Study
- Krishna E. Vyncke, Lars Libuda, Tineke De Vriendt, Luis A. Moreno, Myriam Van Winckel, Yannis Manios, Frederic Gottrand, Denes Molnar, Barbara Vanaelst, Michael Sjöström, Marcela González-Gross, Laura Censi, Kurt Widhalm, Nathalie Michels, Chantal C. Gilbert, Christos Xatzis, Magdalena Cuenca García, Fátima Pérez de Heredia, Stefaan De Henauw, Inge Huybrechts, on behalf of the HELENA consortium
-
- Journal:
- British Journal of Nutrition / Volume 108 / Issue 12 / 28 December 2012
- Published online by Cambridge University Press:
- 28 February 2012, pp. 2261-2273
- Print publication:
- 28 December 2012
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Dietary fatty acids (FA) play a role in several (patho)physiological processes at any age, and different FA have different effects on lipid status and health outcome. The present study aims to describe the FA intake and its main food sources in a population of healthy European adolescents and to assess the variation in intake as a function of non-dietary factors. FA intake was assessed with 24 h recall interviews in 1804 adolescents aged 12·5–17·5 years. Usual intakes were calculated using the multiple source method. Multilevel analyses, adjusting for study centre, were used to investigate the influence of non-dietary factors. The mean total fat intake was 33·3 (sd 1·2) % of total energy intake (%E). The mean SFA intake was 13·8 (sd 1·2) %E, with 99·8 % of the population exceeding the recommendations. SFA was mainly delivered by meat and cake, pies and biscuits. In most adolescents, the PUFA intake was too low, and 35·5 % of the population did not achieve the minimum recommended intake for α-linolenic acid (ALA). The main determinants of FA intake in the present study population were age and sex, as well as physical activity in the male subgroup. No contributions of body composition, socio-economic status or sexual maturation to the variance in FA intake were observed. In conclusion, the most important public health concerns regarding FA intake in this adolescent population were the low intake of ALA and the high intake of SFA, mainly seen in the younger-aged boys. In this group the major contributor to SFA was meat.
6 - In defense of virtue
- from Part II - Humanitarian NGOs
- Edited by Peter A. Gourevitch, University of California, San Diego, David A. Lake, University of California, San Diego, Janice Gross Stein, University of Toronto
-
- Book:
- The Credibility of Transnational NGOs
- Published online:
- 05 June 2012
- Print publication:
- 12 January 2012, pp 137-164
-
- Chapter
- Export citation
-
Summary
Humanitarian organizations, like most virtuous organizations, help us live an ethical life. It is often impossible practically, or prohibitively expensive, to do the right thing on our own. Many of us are deeply concerned about human suffering in places like Darfur, but cannot directly help these distant strangers. Instead the most that we can do is support humanitarian agencies that have the desire and the capacity to act in ways that are consistent with our values. By supporting humanitarian organizations we turn them into our ethical agents. We contribute to humanitarian organizations because we believe both in what they stand for and that they can and will do what they promise.
What happens to virtuous organizations when beliefs about their values and their effectiveness are shaken or can no longer be sustained by faith, when their legitimacy and their credibility are questioned? For much of their history humanitarian organizations were credible in large part because they were legitimate, a legitimacy based largely on their social purpose. Acting in the name of humanity and according to universal principles, they were helping the world’s most vulnerable populations. Yet over the last several decades the “virtue” of humanitarian organizations has been challenged; whether their actions are truly consistent with the values of the international community – a question of legitimacy – and whether they can credibly carry out their stated goals – an issue of credibility – came into question.
Contributors
-
- By Aakash Agarwala, Linda S. Aglio, Rae M. Allain, Paul D. Allen, Houman Amirfarzan, Yasodananda Kumar Areti, Amit Asopa, Edwin G. Avery, Patricia R. Bachiller, Angela M. Bader, Rana Badr, Sibinka Bajic, David J. Baker, Sheila R. Barnett, Rena Beckerly, Lorenzo Berra, Walter Bethune, Sascha S. Beutler, Tarun Bhalla, Edward A. Bittner, Jonathan D. Bloom, Alina V. Bodas, Lina M. Bolanos-Diaz, Ruma R. Bose, Jan Boublik, John P. Broadnax, Jason C. Brookman, Meredith R. Brooks, Roland Brusseau, Ethan O. Bryson, Linda A. Bulich, Kenji Butterfield, William R. Camann, Denise M. Chan, Theresa S. Chang, Jonathan E. Charnin, Mark Chrostowski, Fred Cobey, Adam B. Collins, Mercedes A. Concepcion, Christopher W. Connor, Bronwyn Cooper, Jeffrey B. Cooper, Martha Cordoba-Amorocho, Stephen B. Corn, Darin J. Correll, Gregory J. Crosby, Lisa J. Crossley, Deborah J. Culley, Tomas Cvrk, Michael N. D'Ambra, Michael Decker, Daniel F. Dedrick, Mark Dershwitz, Francis X. Dillon, Pradeep Dinakar, Alimorad G. Djalali, D. John Doyle, Lambertus Drop, Ian F. Dunn, Theodore E. Dushane, Sunil Eappen, Thomas Edrich, Jesse M. Ehrenfeld, Jason M. Erlich, Lucinda L. Everett, Elliott S. Farber, Khaldoun Faris, Eddy M. Feliz, Massimo Ferrigno, Richard S. Field, Michael G. Fitzsimons, Hugh L. Flanagan Jr., Vladimir Formanek, Amanda A. Fox, John A. Fox, Gyorgy Frendl, Tanja S. Frey, Samuel M. Galvagno Jr., Edward R. Garcia, Jonathan D. Gates, Cosmin Gauran, Brian J. Gelfand, Simon Gelman, Alexander C. Gerhart, Peter Gerner, Omid Ghalambor, Christopher J. Gilligan, Christian D. Gonzalez, Noah E. Gordon, William B. Gormley, Thomas J. Graetz, Wendy L. Gross, Amit Gupta, James P. Hardy, Seetharaman Hariharan, Miriam Harnett, Philip M. Hartigan, Joaquim M. Havens, Bishr Haydar, Stephen O. Heard, James L. Helstrom, David L. Hepner, McCallum R. Hoyt, Robert N. Jamison, Karinne Jervis, Stephanie B. Jones, Swaminathan Karthik, Richard M. Kaufman, Shubjeet Kaur, Lee A. Kearse Jr., John C. Keel, Scott D. Kelley, Albert H. Kim, Amy L. Kim, Grace Y. Kim, Robert J. Klickovich, Robert M. Knapp, Bhavani S. Kodali, Rahul Koka, Alina Lazar, Laura H. Leduc, Stanley Leeson, Lisa R. Leffert, Scott A. LeGrand, Patricio Leyton, J. Lance Lichtor, John Lin, Alvaro A. Macias, Karan Madan, Sohail K. Mahboobi, Devi Mahendran, Christine Mai, Sayeed Malek, S. Rao Mallampati, Thomas J. Mancuso, Ramon Martin, Matthew C. Martinez, J. A. Jeevendra Martyn, Kai Matthes, Tommaso Mauri, Mary Ellen McCann, Shannon S. McKenna, Dennis J. McNicholl, Abdel-Kader Mehio, Thor C. Milland, Tonya L. K. Miller, John D. Mitchell, K. Annette Mizuguchi, Naila Moghul, David R. Moss, Ross J. Musumeci, Naveen Nathan, Ju-Mei Ng, Liem C. Nguyen, Ervant Nishanian, Martina Nowak, Ala Nozari, Michael Nurok, Arti Ori, Rafael A. Ortega, Amy J. Ortman, David Oxman, Arvind Palanisamy, Carlo Pancaro, Lisbeth Lopez Pappas, Benjamin Parish, Samuel Park, Deborah S. Pederson, Beverly K. Philip, James H. Philip, Silvia Pivi, Stephen D. Pratt, Douglas E. Raines, Stephen L. Ratcliff, James P. Rathmell, J. Taylor Reed, Elizabeth M. Rickerson, Selwyn O. Rogers Jr., Thomas M. Romanelli, William H. Rosenblatt, Carl E. Rosow, Edgar L. Ross, J. Victor Ryckman, Mônica M. Sá Rêgo, Nicholas Sadovnikoff, Warren S. Sandberg, Annette Y. Schure, B. Scott Segal, Navil F. Sethna, Swapneel K. Shah, Shaheen F. Shaikh, Fred E. Shapiro, Torin D. Shear, Prem S. Shekar, Stanton K. Shernan, Naomi Shimizu, Douglas C. Shook, Kamal K. Sikka, Pankaj K. Sikka, David A. Silver, Jeffrey H. Silverstein, Emily A. Singer, Ken Solt, Spiro G. Spanakis, Wolfgang Steudel, Matthias Stopfkuchen-Evans, Michael P. Storey, Gary R. Strichartz, Balachundhar Subramaniam, Wariya Sukhupragarn, John Summers, Shine Sun, Eswar Sundar, Sugantha Sundar, Neelakantan Sunder, Faraz Syed, Usha B. Tedrow, Nelson L. Thaemert, George P. Topulos, Lawrence C. Tsen, Richard D. Urman, Charles A. Vacanti, Francis X. Vacanti, Joshua C. Vacanti, Assia Valovska, Ivan T. Valovski, Mary Ann Vann, Susan Vassallo, Anasuya Vasudevan, Kamen V. Vlassakov, Gian Paolo Volpato, Essi M. Vulli, J. Matthias Walz, Jingping Wang, James F. Watkins, Maxwell Weinmann, Sharon L. Wetherall, Mallory Williams, Sarah H. Wiser, Zhiling Xiong, Warren M. Zapol, Jie Zhou
- Edited by Charles Vacanti, Scott Segal, Pankaj Sikka, Richard Urman
-
- Book:
- Essential Clinical Anesthesia
- Published online:
- 05 January 2012
- Print publication:
- 11 July 2011, pp xv-xxviii
-
- Chapter
- Export citation
The glial modulatory drug AV411 attenuates mechanical allodynia in rat models of neuropathic pain
- Annemarie Ledeboer, Tongyao Liu, Jennifer A. Shumilla, John H. Mahoney, Sharmila Vijay, Matthew I. Gross, Joseph A. Vargas, Lance Sultzbaugh, Mark D. Claypool, Laura M. Sanftner, Linda R. Watkins, Kirk W. Johnson
-
- Journal:
- Neuron Glia Biology / Volume 2 / Issue 4 / November 2006
- Published online by Cambridge University Press:
- 26 February 2007, pp. 279-291
- Print publication:
- November 2006
-
- Article
- Export citation
-
Controlling neuropathic pain is an unmet medical need and we set out to identify new therapeutic candidates. AV411 (ibudilast) is a relatively nonselective phosphodiesterase inhibitor that also suppresses glial-cell activation and can partition into the CNS. Recent data strongly implicate activated glial cells in the spinal cord in the development and maintenance of neuropathic pain. We hypothesized that AV411 might be effective in the treatment of neuropathic pain and, hence, tested whether it attenuates the mechanical allodynia induced in rats by chronic constriction injury (CCI) of the sciatic nerve, spinal nerve ligation (SNL) and the chemotherapeutic paclitaxel (Taxol¯). Twice-daily systemic administration of AV411 for multiple days resulted in a sustained attenuation of CCI-induced allodynia. Reversal of allodynia was of similar magnitude to that observed with gabapentin and enhanced efficacy was observed in combination. We further show that multi-day AV411 reduces SNL-induced allodynia, and reverses and prevents paclitaxel-induced allodynia. Also, AV411 cotreatment attenuates tolerance to morphine in nerve-injured rats. Safety pharmacology, pharmacokinetic and initial mechanistic analyses were also performed. Overall, the results indicate that AV411 is effective in diverse models of neuropathic pain and support further exploration of its potential as a therapeutic agent for the treatment of neuropathic pain.




