82 results
Factors influencing subcanopy leaf and stolon exposure and associated absorption and translocation of herbicides in semidormant zoysiagrass
- Jordan M. Craft, Navdeep Godara, Clebson G. Gonçalves, Shawn D. Askew
-
- Journal:
- Weed Science / Volume 72 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 17 November 2023, pp. 59-67
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Turfgrass managers are concerned about zoysiagrass (Zoysia japonica Steud.) injury from nonselective herbicide treatment during winter dormancy. Research was conducted to assess factors affecting spray penetration into semidormant ‘Meyer’ zoysiagrass canopies and to evaluate absorption and translocation of [14C]glyphosate and [14C]glufosinate into green leaves and subtending stolons. Absorption of [14C]glyphosate and [14C]glufosinate was up to four times greater in stolons than in leaves. Zoysiagrass leaves treated with [14C]glufosinate had more rapid 14C absorption than those treated with [14C]glyphosate. More 14C translocated out of the treated area following [14C]glyphosate treatment compared with [14C]glufosinate and moved more readily from stolon to leaves than from leaves to stolon. When extended-range, flat-fan spray tips (XR) were positioned 61 cm above zoysiagrass, 73% and 11% of recovered colorant was extracted from dormant vegetation in the upper and lower canopy levels. Turbo TeeJet® spray tips (TTI) deposited fewer droplets into the upper canopy and more droplets into the middle and lower canopy regardless of position above the turf surface. Increasing pressure from 103 to 414 kPa increased droplet velocities from XR and TTI nozzles and decreased droplet diameters of XR nozzles. Droplet diameters were also substantially increased when using TTI nozzles compared with XR nozzles. Droplet diameter and associated mass were more determinant of turfgrass canopy penetration than droplet velocity. At 60 L ha−1 of carrier volume, 23% of colorant reached the lower canopy level, and this quantity increased by 2.3% per additional 100 L ha−1. When carrier volume was reduced from 584 to 60 L ha−1, 48% less colorant was delivered to the lower canopy level. Given that subcanopy stolons are always present and absorb more glyphosate and glufosinate than leaves, practices such as avoiding induction-type nozzles, raising spray height, and reducing spray volume can reduce herbicide delivery and potential injury to semidormant zoysiagrass.
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
Specific treatment for alcohol use disorder reduces relapse after psichiatric hospitalization
- O. Martin-Santiago, J. I. Goncalves-Cerejeira, G. Guerra-Valera, M. Calvo-Valcarcel, P. Martinez-Gimeno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S565
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients with an alcohol use disorder frequently relapse after various efforts to quit. Admission to hospital units is a possible start to stop drinking alcohol and reach abstinence. Among the pharmacological strategies to quit this addiction are specific drugs, such as disulfiram or namelfen, which are widely studied. Hospitalized patients frequently initiate these medications to control addiction, but little is known about their efficacy after discharge in this group.
ObjectivesThe aim is to determine whether the initiation of treatment with specific drugs for alcohol use disorder could help to maintain alcohol abstinence after admission to a General Hospital Psychiatric Ward. In addition, we want to check those factors associated with a higher rate of relapse in consumption.
MethodsWe conducted a retrospective cross-sectional study of a group of patients admitted in 2018 to a psychiatric hospitalization ward due to alcohol use disorder and who expressed their desire to stop drinking. At the time of admission, we recorded sociodemographic data, consumption of other substances and alcohol family history. Patients initialized specific treatments to reduce and control alcohol consumption if they wanted. Twenty-four months after discharge, we acquired the number of relapses through new admissions, emergency room visits or outpatient follow-up data.
ResultsA sample of 36 patients (28 men) admitted to a psychiatric hospitalization ward was analyzed. At discharge, 17 accepted specific pharmacological treatments to reduce alcohol consumption. After a follow-up period of 24 months, 70.8% relapsed compared to 94.7% who did not accept treatment (χ2=4.001, DF=1, p=0.045, OR=0.13). There were no differences between the two groups in age, gender, amount of alcohol consumed, follow-up modality at discharge or if it was their first detoxification attempt. However, those who did not accept the specific pharmacological treatment consumed other drugs (41.1% vs 5.8%, χ2= 5.888, DF=1, p=0.015), had other history of mental disorder (64.7% vs 23.5%, χ2= 5.845, FD=1, p=0.015) and a higher proportion of relatives with alcohol consumption (81.8% vs 42.8%, χ2= 3.896, FD=1, p=0.048) more frequently. The time (in days) to relapse was faster in this group of patients (200.8 vs 402.7 , Z=-2.5413, p=0.005).
ConclusionsAccepting drug-specific treatment for alcohol use can be helpful for many patients who want to achieve alcohol abstinence. Among the factors that prevent the acceptance of this treatment is the consumption of other substances, comorbidity with another mental pathology and family history, which may involve genetic factors that favour addiction. This group of patients could benefit from a specific pharmacological treatment, although other psychosocial factors may also help.
Disclosure of InterestNone Declared
Chronic obstructive pulmonary disease and comorbid psychiatric disorders: preliminary results of an 8-year retrospective study using real data
- G. Santos, A. R. Ferreira, M. Gonçalves-Pinho, A. Freitas, L. Fernandes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S513-S514
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Chronic obstructive pulmonary disease (COPD) is the third leading cause of mortality worldwide. In Portugal, it is estimated to afflict 14.2% of the population over the age of 45 and is one of the most common causes of morbidity, with a significant social impact and excessive expenses. Moreover, COPD is associated with high levels of psychological distress and diverse psychiatric disorders that heighten the disease burden as they are associated with increased risk of exacerbations and frequent hospitalizations. Despite this overview, psychiatric conditions remain understudied compared to comorbid general medical conditions, and few studies have assessed their effect on COPD hospitalization outcomes.
ObjectivesThis study aimed to describe the occurrence of a vast array of psychiatric comorbid diagnoses in COPD hospitalizations and to understand their impact on hospitalization outcomes.
MethodsA retrospective observational study was conducted. All inpatient episodes from 2008 to 2015 of patients with at least 40 years and a primary diagnosis of COPD (ICD-9-CM codes 491.x, 492.x and 496) were selected from a national administrative database that included all hospitalizations in mainland public hospitals. From these sampled episodes, secondary psychiatric diagnoses were identified (ICD-9-CM codes 290.x-319.x). Age at hospitalization, sex, psychiatric comorbidities, length of stay (LoS) in days, admission type and date, destination after discharge, in-hospital mortality and hospital charges were analyzed.
ResultsFrom a total of 66,661 COPD hospitalizations, 17,652 (26.5%) corresponded to episodes with a secondary psychiatric diagnosis. Patients with a comorbid psychiatric diagnosis were on average younger at admission (70.3 vs. 75.9 years, p<0.001), had a longer median LoS (9.89 vs. 9.33 days, p<0.001) and higher urgent admission rates (96.2% vs. 95.7%, p=0.009). There was also a significant association between discharge destination and psychiatric diagnoses (p<0.001).
ConclusionsThese findings suggest that mental disorders have an adverse and quantifiable impact on COPD hospitalization outcomes. With this in mind, to provide optimal treatment for patients with both conditions, psychiatric disorders should become a matter of routine evaluation and follow-up.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
Paraffin gauze bolus as tissue compensator in photon irradiation for mycosis fungoides – regarding a case study
- André M. Pires, Fátima Borges, Anabela G. Dias, Lencart Joana, Marisa Matos, Joana Gonçalves
-
- Journal:
- Journal of Radiotherapy in Practice / Volume 22 / 2023
- Published online by Cambridge University Press:
- 28 February 2023, e82
-
- Article
- Export citation
-
Introduction:
Total skin electron beam therapy is a treatment option in patients with mycosis fungoides (MF) affecting a significant amount of the body surface. For patients with involvement of soles and interdigital folds, however, this approach is ineffective, requiring alternatives such as localised radiotherapy (RT). Although electron beams are well suited for superficial lesions, on irregular surfaces it provides inadequate tumour coverage and excess dose variance, requiring photon irradiation with tissue compensation.
Methods:We present the case of a patient with extensive cutaneous MF with skin lesions spread over both lower limbs and treated on these affected areas with photon beam RT. Long sheets of paraffin gauze dressings were used to create a 0·5-cm-thick bolus. The patient received a single fraction of 8 Gy. In vivo dosimetry using Gafchromic films was performed.
Results:After 3 months, a complete response was achieved. In this case, paraffin gauze bolus proved to be an inexpensive, convenient, effective and flexible method for irregular superficial cancer irradiations.
Conclusion:Paraffin gauze bolus is a suitable option for irregular contours.
My stomach is full
- M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, N. De Uribe Viloria, G. Guerra Valera, T. Jiménez Aparicio, C. Vallecillo Adame, C. De Andrés Lobo, I. Santos Carrasco, J. Gonçalves Cerejeira, N. Navarro Barriga, M.J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S583
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is an eating behavior disorder that is often related to various personality factors. The relationship between obsessive compulsive disorder and eating Disorders has been highlighted.
ObjectivesTo present a clinical case of a patient with eating disorder and gastric bezoar, secondary to compulsive hair ingestion.
MethodsBibliographic review of articles published in relation to the comorbidity of these disorders, based on articles published in the last 5 years in Pubmed.
Results26-year-old female. Diagnosis of restrictive anorexia nervosa. She was admitted to the hospital on two occasions for nutritional disorders. In the last admission, she reported greater anxiety and significant weight loss. She reports that she has limited her food intake, but she does feel thin and is unable to eat for fear of gaining weight. Ruminative thoughts about her body image. During admission, the patient expressed a sensation of fullness, nausea and vomiting, later observing in abdominal X-ray and gastroscopy, the presence of a gastric trichobezoar, which was finally resolved conservatively.
ConclusionsTrichotillomania is observerd in 1 in 2000 people, trichophagia is even less frequent. According to DSM- V, these disorders are grouped within obsessive-compulsive spectrum disorders. A Trichobezoar is a conglomerate that can be found in the stomach or intestine, composed mainly of hair, previously ingested. Trichotillomania can be associated with anorexia nervosa, especially in patients with obsessive personality traits, which occurs frequently. The gastric slowing that patients with anorexia often present is a factor that favors the formation of the bezoar
DisclosureNo significant relationships.
Alcohol abuse among women: a review with a gender perspective
- J. Gonçalves Cerejeira, I. Santos Carrasco, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S820
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful use of alcohol is an important risk factor for the health of the population around the world. The incidence of alcohol dependence in women is increasing and both its consumption pattern and its consequences have unique characteristics.
ObjectivesTo present a literature review focused on alcohol use disorder with a gender perspective.
MethodsLiterature review.
Results- Women use to start using alcohol sooner than men and this seems to be a risk factor to become addicted. - Due to physiological and psychological factors women experience more negative health effects from excessive alcohol use than men and it occurs at lower levels of use. - Psychiatric comorbidity associated with alcohol abuse such as anxiety and depression is more common in women and this in turn worsens the alcohol use disorder. - Alcohol consumption increases the vulnerability of women on several levels, including an increased risk of physical abuse.
ConclusionsAlcohol abuse among women deserves special attention and a specific intervention focused on the gender perspective.
DisclosureNo significant relationships.
Something inside my head
- T. Jiménez Aparicio, G. Medina Ojeda, C. De Andrés Lobo, C. Vallecillo Adame, J. Gonçalves Cerejeira, I. Santos Carrasco, G. Guerra Valera, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, N. Navarro Barriga, M. Fernández Lozano, B. Rodríguez Rodríguez, M.J. Mateos Sexmero, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Electroconvulsive therapy (ECT) is a medical treatment for those patients with high suicide risk or refractory psychiatric disorders. It is currently a safe technique, and its effectiveness has been widely demonstrated.
ObjectivesPresentation of a clinical case about a patient with drug-resistant delusional disorder and high suicide risk, who eventually received ECT treatment.
MethodsBibliographic review including the latest articles in Pubmed about ECT procedure, effects and use.
ResultsWe present a 45-year-old man, who visited different doctors several times by reporting he had the feeling of “having a brain tumor or a vascular disorder”, so he requested imaging tests (computed tomography and magnetic resonance). These tests were absolutely normal, but he kept thinking something was wrong, and eventually attempted suicide by hanging (his family founded him before it was too late). The patient was admitted to hospital, and started psychopharmacological treatment, with minimal response. He desperately insisted that he had “something inside his head”. At this point, it was proposed to start ECT, and the patient accepted. After 6 bilateral ECT sessions, he was visibly more relaxed and less worried, and he no longer presented autolytic ideation. He was still a little bit suspicious about the feeling of having a neurological disease. Currently, the patient runs a follow-up consultation.
ConclusionsElectroconvulsive therapy is a safe and effective technique for those patients with high suicide risk. It may be useful to perform imaging tests in certain cases, for detecting intracranial pressure, acute hemorrhage, tumors… A follow-up of these patients must be performed
DisclosureNo significant relationships.
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Personality disorders and Juvenil Myoclonic Epilepsy
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S668
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a high comorbidity between psychiatric disorders and juvenile myoclonic epilepsy (JME), observed in up to 58% of these patients; specifically, mood disorders, anxiety and personality disorders (PD). In some patients with PD there are nonspecific alterations in the EEG, which nevertheless sometimes involve pathology. The presence of personality disorders along with JME has been repeatedly described. Previous studies have emphasized the difficulties in treating patients with JME, which have been attributed to some specific psychiatric, psychological and psychosocial characteristics.
ObjectivesDescribing distinctive personality traits in JME
MethodsReview of scientific literature based on a relevant clinical case.
Results19-year-old woman, single. Psychiatric history since she was 12 due to anxiety-depressive symptoms, after being diagnosed with JME. 4 admissions in Psychiatry, with a variety of diagnoses: eating disorder, attention deficit hyperactivity disorder and borderline personality disorder. The evolution of both disorders has been parallel, presenting epileptic seizures due to irregular therapeutic adherence together with pseudo-seizures, which made difficult their differential diagnosis. In addition, he has had frequent visits to the emergency room for suicide attempts and impulsive behaviors.
ConclusionsIn 1957, for the first time, distinctive personality traits were described in patients with JME: lack of control and perseverance, emotional instability, variable self-concept and reactive mood, which have been confirmed in subsequent studies. It is believed as epilepsy progresses, patients tend to develop symptoms of depression, anxiety, social problems, and attention deficit. Therefore, these patients have difficulty in following medical recommendations, especially precautions regarding precipitating factors for seizures.
DisclosureNo significant relationships.
Covid-19 pandemic and suicidal risk among adolescents
- J. Gonçalves Cerejeira, C. Vallecillo Adame, S. Uribe, I. Santos Carrasco, T. Jiménez Aparicio, C. De Andrés Lobo, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S436
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Covid-19 pandemic has had a significant impact on the mental health of adolescents. Several descriptive studies and systematic reviews have shown an increase in suicide rates in this age group.
Objectives- To present a literary review on the impact of the Covid-19 pandemic on the mental health and suicidal behavior of adolescents around the world. - To present data on admission rates due to suicidal behavior during the first year of the Covid-19 pandemic in a Spanish child-adolescent psychiatric hospitalization unit.
Methods- We will present a literature review and a retrospective cross-sectional study on admission rates for suicidal behavior in a child-adolescent psychiatric hospitalization unit. - Admission rates for suicidal behavior during the year prior to the pandemic will be compared with rates relative to the first year of the pandemic.
Results- We have found a significant increase in admission rates for suicidal behavior during the year of the pandemic. Similar results have been found in different studies and meta-analyzes. - The socio-demographic characteristics of the patients are quite similar in the two periods of time analyzed, but the reference to intra-family problems has been more frequent in the year of the pandemic.
ConclusionsOur data is in line with other studies suggesting that the Covid-19 pandemic has had a strong impact on teenage suicidal behavior.
DisclosureNo significant relationships.
Cannabis use and cognitive impairment in schizophrenia
- M. Gonçalves, J. Romão, R. André, F. Félix, G. Andrade, R. Saraiva, E. Dornelles, E. Fernandes, M. Abreu, I. Chendo, F. Ismail
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S456-S457
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Neurocognitive deficits amongst patients with schizophrenia are considered one of schizophrenia’s central features. These deficits appear to be present from the first episode of psychosis (FEP) and certain cognitive impairments could be components of a genetic vulnerability to schizophrenia. Regarding research on cannabis and cognition in schizophrenia, different studies have assessed neurocognitive functions: memory, attention/vigilance, processing speed, verbal learning, executive functions, and verbal fluency.
ObjectivesThe aim is to do a review of recent findings concerning the association of cannabis use with cognition in schizophrenia.
MethodsA literature review was conducted using the PubMed search database.
ResultsPatients with schizophrenia and concomitant cannabis use are associated with worse performance in immediate verbal learning, and in some studies with worse working memory performance. There is an improvement of verbal memory when they cease the cannabis’ consumption. Regarding attention capacity and memory types assessed, the results are controversial. In FEP, heavy cannabis use during the previous year correlates with slower processing speed. Also, FEP-patients with cannabis use but no family history of psychosis perform worse in executive functions, while those with a family history of psychosis perform better.
ConclusionsThe studies of psychosis, cannabis and cognition differ in relevant aspects, which might be connected to the result variability. Therefore, before solid conclusions can be reached, it is important to carry out longitudinal studies to understand the changes in the cognitive variables, which can depend on the pattern of cannabis’ use (concurrent or prior to the FEP). Possible confounding variables that might be present should be acknowledged.
DisclosureNo significant relationships.
Traumatic brain injury, antisocial personality disorder and alcohol
- C. De Andrés Lobo, T. Jiménez Aparicio, C. Vallecillo Adame, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, N. De Uribe Viloria, G. Medina Ojeda
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S667
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Traumatic brain injury (TBI) can cause changes in the personality and behaviors. History of TBI has been associated with violent behavior and substance abuse.
ObjectivesPresentation of a clinical case of a patient with antisocial personality traits who suffered a TBI and abuses alcohol.
MethodsWe conducted a bibliographic review by searching for articles published the last 5 years in Pubmed
ResultsWe present the case of a 48-year-old male patient with a history of myoclonic epilepsy, who suffered a TBI in a car crash. During his stay at ICU antisocial and borderline personality traits were found. When he came to consultations, he presented signs of alcohol intoxication (verbiage with hasty and dysarthric speech, and psychomotor incoordination). He acknowledges daily alcohol intake, although he minimizes it. During the interview he is irritable, prone to anger when contradicted and boasts of episodes of heteroaggressiveness and violence that he has carried out in the past. He reports morning sickness and tremors, but does not accept that they may be due to alcohol withdrawal. There is no motivation for change.
ConclusionsIt has been determined that history of TBI is more frequent in individuals with antisocial personality. TBI has been linked to violent behaviors, poor inhibitory control, engaging in illegal acts and higher rates of substance abuse. However, the causal relationship between antisocial behavior and TBI has yet to be clarified, as the available evidence does not show which comes first. More research is needed in the future that takes into account the temporal sequence of events.
DisclosureNo significant relationships.
Migration and psychosis: the link between them
- C. De Andrés Lobo, T. Jiménez Aparicio, C. Vallecillo Adame, A. Gonzaga Ramírez, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S217
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Migrations are a source of stress for patients, which can have repercussions on their Mental Health. We present the case of a native Senegalese patient who presented a first psychotic episode.
ObjectivesPresentation of a clinical case of an immigrant patient with a psychotic disorder.
MethodsBibliographic review on migration and psychosis by searching for articles in Pubmed.
ResultsWe present the case of a patient of 20 years, a native of Senegal, who has been living in Spain for 3 months in a shelter home. He has no family or relations in Spain, and only speaks Wolof, presenting serious difficulties in communication with healthcare workers. He came to Hospital with his social worker because strange behaviors had been observed. He presented delusional ideation of self-referential and mystical-religious content, related to “the prophet” and “the need to fulfill a mission”. He also presented auditory hallucinations that he identified as of divine origin, and ordered him to perform behaviors such as picking hairs from the ground and various rituals. He acknowledges cannabis and alcohol use in the previous days. Paliperidone treatment was started. Throughout the admission, he begins to show concern for the state of his relatives in Senegal and the need to send them money.
ConclusionsMultiple studies indicate that migrants are at higher risk of psychosis, specially those from countries where the majority of population was black, according to some series. The challenge lies in understanding the mechanisms underlying this increased incidence, taking into account psychosocial factors such as social isolation and trauma.
DisclosureNo significant relationships.
Psychosis: Risk Factors and Prognosis
- M. Fernández Lozano, I. Santos Carrasco, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Queipo De Llano De La Viuda, G. Guerra Valera, A. Gonzaga Ramírez, J. Gonçalves Cerejeira, O. Segurado Martín
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S313
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There are life events that may increase the possibilities of suffering some kind of Psychopathology. The most validated model for understanding the aetiology of psychosis is based on genetic and environmental risk factors and their interaction, likely involving epigenetic mechanisms. It is necessary to consider those events as risk factors for Mental Health.
ObjectivesStudy of risk and prognostic factors in psychosis.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 28-year-old male patient from Peru, currently living in Germany. History of sexual abuse in childhood. He started taking drugs at the age of 8. In the emergency department, he reports that since the beginning of the pandemic, after listening to a speech by the Pope, he begins to interpret signals about situations occurring around him. He begins to read about mystical-religious subjects, changes the style of music he listens to and recognises changes in his personality. He says for months he has been feeling watched, persecuted and expresed someone wants to kill him. He says hears voices and that they communicate with him through bodily sensations.
ConclusionsChildhood trauma, immigration and cannabis use are significantly associated with an increased risk of functional psychosis. A neurotic personality also independently contributes to this risk. The accumulation of these factors increases vulnerability to mental disorders and leads to a worse prognosis and evolution of these pathologies. These findings could help to improve the prevention of psychosis and the development of specific treatment strategies in this particular population.
DisclosureNo significant relationships.
Psicosis and suicide risk: who, when and why
- J. Gonçalves Cerejeira, I. Santos Carrasco, C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, G. Guerra Valera, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, O. Martin-Santiago
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S842-S843
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide rates in people diagnosed with a psychotic disorder can be up to 50 times higher than in the general population, with the lethality of attempts being significantly higher in this group, compared to people diagnosed with other psychiatric disorders. Furthermore, it is known that being male is associated with more serious suicide attempts and higher rates of completed suicides.
ObjectivesTo reflect on the increased risk of suicide associated with psychotic disorders.
MethodsCase report and literature review.
ResultsCase report 40-year-old male, recently diagnosed with Schizophreniform Disorder and currently with persistent positive symptoms. He was admitted to our psychiatric hospitalization unit due to a voluntary overdose of almost 100 tablets (antihypertensives, antiarrhythmics, and benzodiazepines) and alcohol. He admits taking the pills with the aim of committing suicide. Literature review: - Around 10% of people diagnosed with schizophrenia commit suicide. - In young patients diagnosed with schizophrenia, suicide is the leading cause of death. - Between 15 and 65% of patients diagnosed with schizophrenia have depressive symptoms such as hopelessness. - Depressive symptoms in these patients seem to be directly proportionally with awareness of the disease (stigma, awareness of its severity and a sudden decrease in quality of life and social integration). - The risk of suicide increases especially in the first 10 years of the disease.
ConclusionsPsychosis is an important risk factor of suicide and active preventive measures should be carried out in these patients.
DisclosureNo significant relationships.
Organic lesions and Psychiatry: “A sample on a pendant”
- T. Jiménez Aparicio, G. Medina Ojeda, C. De Andrés Lobo, C. Vallecillo Adame, J. Gonçalves Cerejeira, I. Santos Carrasco, G. Guerra Valera, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, M. Fernández Lozano, B. Rodríguez Rodríguez, M.J. Mateos Sexmero, N. Navarro Barriga, N. De Uribe Viloria
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S214-S215
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Brain lesions may induce psychiatric symptoms in some cases. Imaging tests are important to make a differential diagnosis, and therefore initiate an appropriate treatment.
ObjectivesPresentation of a clinical case about a patient with psychiatric symptoms who presented an organic lesion.
MethodsBibliographic review including the latest articles in Pubmed about psychiatric symptoms induced by organic lesions.
ResultsWe present a 51-year-old male patient, with adequate previous functionality, who attended psychiatric consultations due to changes in his character, with delusional mystical and megalomaniac ideation, verbiage, hypoprosexia, memory loss and insomnia (diagnosed with Bipolar Disorder type II, hypomanic episode). Eventually, a brain computed tomography scan was performed, in which meningioma was visualized. The patient underwent surgery, and he asked to keep a sample of his tumor to always carry it with him on a pendant. Psychiatric symptoms induced by organic lesions are highly variable, depending on the location and size of the lesion, and they may be the first and/or only symptom of a meningioma (up to 21% according to various studies), so it is important to perform imaging tests in some cases. At this time, the patient is under follow-up, he has remained euthymic and stable, and he refuses to take psychopharmacological medication.
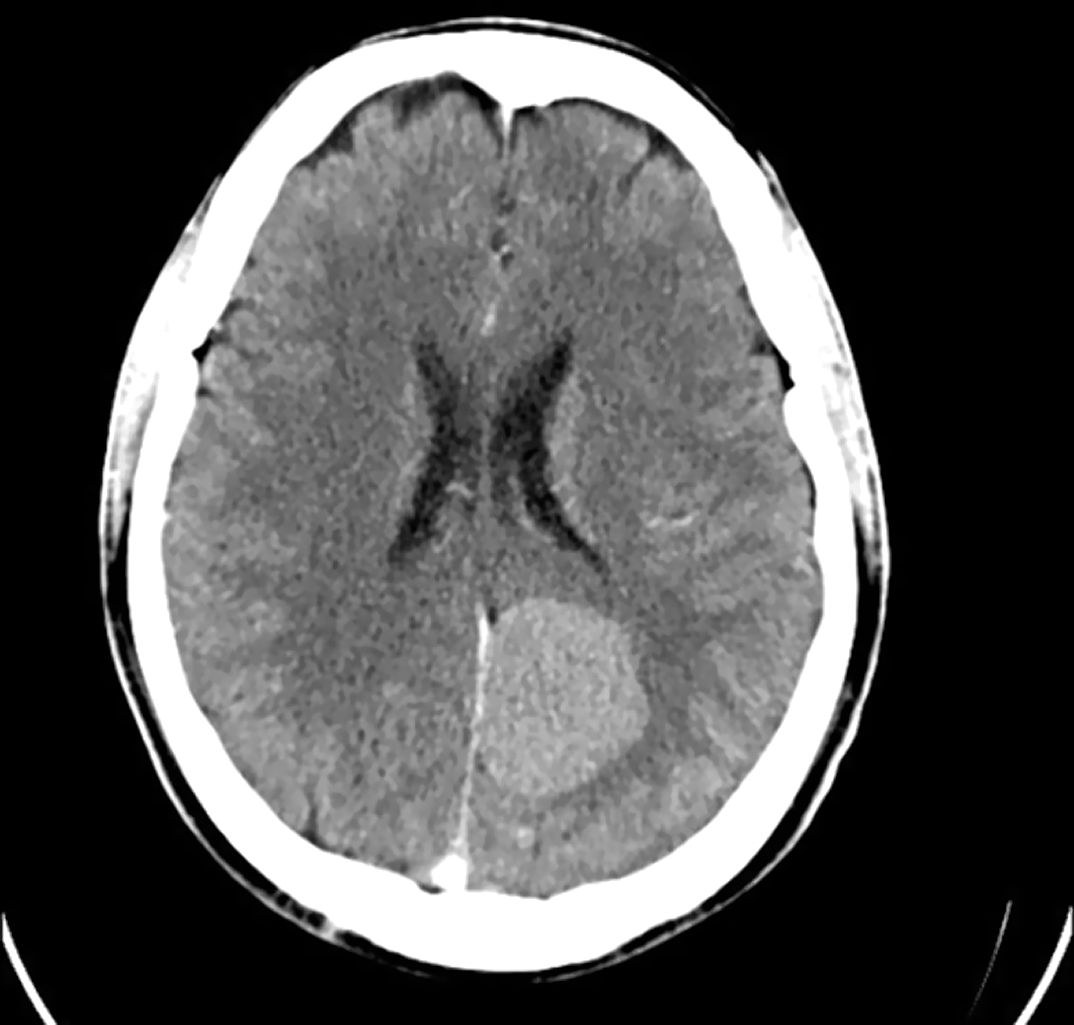 Conclusions
ConclusionsPsychiatric symptoms may be the first and/or only manifestation of an organic lesion in some cases. Neuroimaging tests (CT and MR) may be useful in the differential diagnosis. It is important to carry out an indiviualized treatment based on the patient’s pathology, which may include surgery and/or drugs.
DisclosureNo significant relationships.
A narrative approach to trichotillomania
- J. Gonçalves Cerejeira, I. Santos Carrasco, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. De Andrés Lobo, T. Jiménez Aparicio
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Trichotillomania is an obsessive-compulsive spectrum disorder characterized by recurrent and uncontrolled hair pulling. This behavior causes significant anxiety as well as low self-esteem in people who suffer from this disorder. There is still no therapy of proven efficacy in the treatment of trichotillomania. Psychotropic drugs and cognitive behavioral psychotherapy have been tried in the management of this disease, but the relapse rate is high. Narrative therapy is an innovative type of postmodern psychotherapy and in our literary search we have not found data related to its use in the treatment of trichotillomania.
ObjectivesTo present a novel therapeutic approach to a highly resistant disorder, trichotillomania.
MethodsCase report and literature review.
ResultsWe present a case of a 39-year-old woman diagnosed with trichoticolomania twenty years earlier. She tried several types of psychotherapies for manage her hair-pulling problem, all related with relapse only a few days after finishing the sessions. We have carried out a total of 5 narrative therapy sessions spread over 3 months. No relapses have been observed during the subsequent 9-month follow-up period.
ConclusionsBased on our experience, we believe that Narrative Therapy is a good and still unexplored alternative for people diagnosed with trichotillomania.
DisclosureNo significant relationships.
Eating Disorders during the pandemic COVID-2019
- B. Rodríguez Rodríguez, I. Santos Carrasco, M. Fernández Lozano, M.J. Mateos Sexmero, N. Navarro Barriga, C. De Andrés Lobo, T. Jiménez Aparicio, C. Vallecillo Adame, G. Guerra Valera, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, J. Gonçalves Cerejeira, C. Valdivieso Burón
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S584
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Concerns about health and fitness during lockdown may serve as a trigger for eating disorders in vulnerable individuals. Other risk factors may also include increased use of social networks and comparison with beauty ideals. Isolation, loneliness and problems with emotional regulation may lead people to reduce food intake by giving them a greater sense of control.
ObjectivesEmphasise the relevance of the increase in the incidence of Eating Disorders (ED) cases during the pandemic.
MethodsReview of the scientific literature based on a relevant clinical case.
Results14-year-old female, residing with her mother. She reports that from the beginning of COVID-19 confinement she became obsessed with leading a healthier life, starting to restrict food, limiting fats and carbohydrates, and having also started compulsive physical activity (approximately 4 hours of aerobic exercise per day), without associated purging behaviours. She also acknowledges eating small amounts (although she minimises this aspect) and controlling all calories, stating that food and practices aimed at “staying healthy” now dominate her life. Her previous BMI was 18, with a current BMI of 11.7.
ConclusionsPatients suffering from ED, who often have poor knowledge of their illness and find social-emotional communication difficult, may delay seeking help. Studies suggest the relevance of identifying specific vulnerability factors among ED patients in confinement in order to develop preventive strategies and personalised treatment approaches.
DisclosureNo significant relationships.





