25 results
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
Searching for bridges between psychopathology and real-world functioning in first-episode psychosis: a network analysis from the OPTiMiSE trial
- F. Dal Santo, E. Fonseca-Pedrero, M. P. García-Portilla, L. González-Blanco, P. A. Sáiz, S. Galderisi, G. M. Giordano, J. Bobes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S262-S263
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Network analysis has been used to explore the interplay between psychopathology and functioning in psychosis, but no study has used dedicated statistical techniques to focus on the bridge symptoms connecting these domains.
ObjectivesThe current study aims to estimate the network of depressive, negative, and positive symptoms, general psychopathology, and real-world functioning in people with first-episode schizophrenia or schizophreniform disorder, focusing on bridge nodes.
MethodsBaseline data from the OPTiMiSE trial were analysed. The sample included 446 participants (age 40.0±10.9 years, 70% males). The network was estimated with a Gaussian graphical model (GGM), using scores on individual items of the Positive and Negative Syndrome Scale (PANSS), the Calgary Depression Scale for Schizophrenia (CDSS), and the Personal and Social Performance (PSP) scale. Stability, strength centrality, expected influence (EI), predictability, and bridge centrality statistics were computed. The top 20% scoring nodes on bridge strength were selected as bridge nodes.
ResultsNodes from different rating scales assessing similar psychopathological and functioning constructs tended to cluster together in the estimated network (Fig. 1). The most central nodes (EI) were Delusions, Emotional Withdrawal, Depression, and Depressed Mood. Bridge nodes included Depression, Conceptual Disorganisation, Active Social Avoidance, Delusions, Stereotyped Thinking, Poor Impulse Control, Guilty Feelings, Unusual Thought Content, and Hostility. Most of the bridge nodes belonged to the general psychopathology subscale of the PANSS. Depression (G6) was the bridge node with the highest value.
Image:
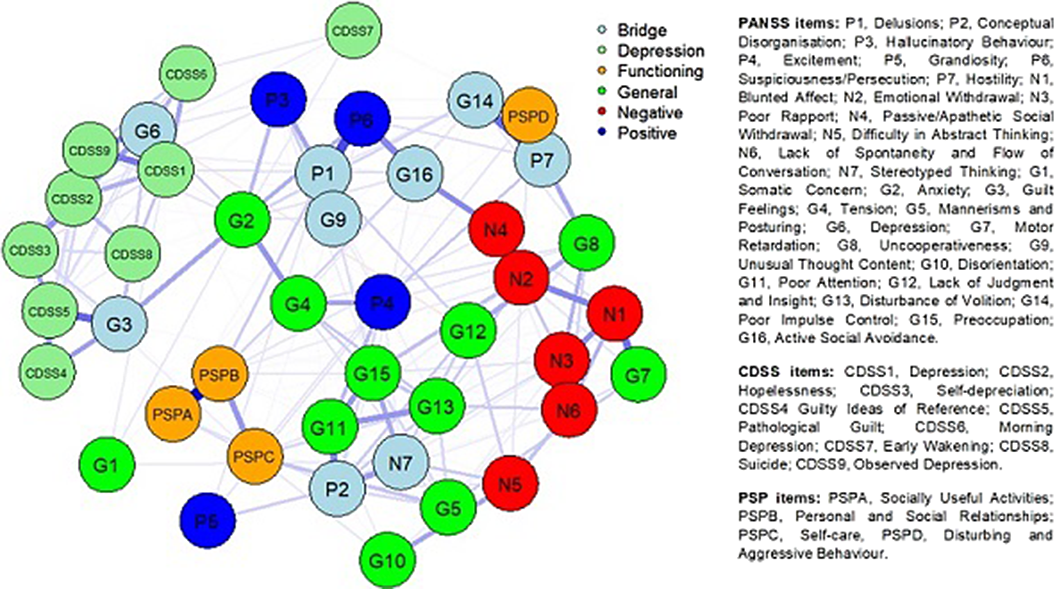 Conclusions
ConclusionsThe current study provides novel insights for understanding the complex phenotype of psychotic disorders and the mechanisms underlying the development and maintenance of comorbidity and functional impairment after psychosis onset.
Disclosure of InterestNone Declared
Gut permeability and low-grade inflammation in bipolar disorder
- M. Couce, G. Paniagua, L. González-Blanco, A. García-Fernández, C. Martínez-Cao, P. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S385-S386
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Systemic inflammation has been increasingly related to bipolar disorder -BD- (Tanaka et al. Neurosci Res 2017;115 59-63). Intestinal bacterial translocation has been postulated as one of the causes of this inflammation (Nguyen et al. J Psychiatr Res 2018;99 50-61). A possible pathway is through the lipopolysaccharide, which is presented to CD14 through lipopolysaccharide binding protein (LBP) leading to a release of systemic inflammatory markers like C-reactive protein (CPR) (Funda et al. Infect Immun 2001;69 3772-81).
Objectives1) Describe gut permeability in patients with BD through the determination of intestinal inflammatory markers (LBP, sCD14) in plasma; 2) Analyze variables associated with intestinal inflammation.
MethodsCross-sectional study of 38 patients with BD [mean age=45.50 (SD=10.93; range 23-68); males=15 (39.5%)], recruited from mental health outpatient clinics in Oviedo (Spain).
Assessment: Pro-inflammation biomarkers [CRP (mg/dL), Erythrocyte Sedimentation Rate (ESR) (mm/h), Neutrophil/Lymphocyte, Monocyte/Lymphocyte, Platelet/Lymphocyte and Systemic Immune Inflammation Indexes]. Indirect markers of intestinal bacterial translocation [LBP, soluble CD14 (sCD14)]. Dichotomous variables were created for LBP, considering LBP ≥15 μg/dL as increased gut permeability; and for CPR, considering CRP≥0.3 as systemic inflammation. Metabolic syndrome [ATPIII criteria: glucose, HDL, triglycerides (mg/dl), arterial pressure (mmHg), abdominal circumference (cm)], body mass index (BMI) (kg/m2), smoking, cannabis or alcohol use.
Statistical analyses: t-Student test, multiple linear regression analyses.
ResultsAverage LBP was 14.60 μg/dL (SD=6.4) and 15 patients (39.5%) had increased gut permeability. Moreover, average CPR was 0.40 mg/dL (SD=0.58) and 16 patients (47.1%) showed systemic inflammation. There were no patients with increased levels of sCD14.
Associations were found between LBP and CPR (r=0.357; p=0.032), cannabis use in the last month (t=-2.293; p=0.029), BMI (r=0.433; p=0.008) and abdominal obesity (t=3.006; p=0.005); but no with age or sex.
Subsequently, a multiple linear regression model for LBP was calculated with variables previously mentioned, and age (based on expert criteria). The overall regression was statistically significant (R2=0.49, F=9.273, p<0.001). It was found that CPR, abdominal obesity, and cannabis use in the last month significantly predicted LBP levels (table 1).
Table 1. Multiple linear regression analyses to LBP B SE β t p CPR 4.842 1.529 0.439 3.167 0.004 Abdominal obesity 4.810 1.849 0.362 2.601 0.014 Cannabis use -5.048 2.273 -0.296 -2.221 0.034 ConclusionsMore than one third of patients with BD had increased gut permeability. Almost 50% had systemic inflammation. Intestinal permeability was directly related to abdominal obesity and systemic inflammation, but inversely related to cannabis use.
Disclosure of InterestNone Declared
The response to unfolded proteins in schizophrenia and bipolar disorder
- C. Cachán, I. M. Valle, Y. Potes, A. González Rubio, N. Menéndez Coto, D. López Fanjul, I. Vega Naredo, B. Caballero, P. Saiz, J. Bobes, P. García Portilla, A. Coto Montes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S636-S637
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia (SCH) and bipolar disorder (BD) are severe mental disordes, which have high incidence (Whiteford et al. Lancet 2013; 381 1575-86) and are the main causes of diasibility in young people (WHO 2022; https://www.who.int/news-room/fact-sheets/detail/mental-disorders).
Psycological stress appears in different mental disorders, and this is directly related to oxidative stress (Moller et al. Chem Biol Interact. 1996; 102 17-36)(Pupic-Bakrac et al. 2020; Psychiatr Danub. 32 412-9). Oxidative stress causes reticulum edoplasmic stress (ER stress) and this produces high levels of misfolded proteins. Defective proteins are degraded by the proteasome, but but when the density of misfolded proteins exceeds the capacity of the proteosome, the Unfolded and Misfolded Protein Response (UPR) is triggered through three main pathways: Inositol-requiring enzyme 1α (IRE1α); transcription factor 6 alpha (ATF6α) and protein kinase RNA-Like ER kinase (PERK), trying to recover normal protein synthesis capacity (Bermejo-Millo et al. 2018; Mol Neurobiol. 55 7973-86) (González-Blanco et al. 2022; J Cachexia Sarcopenia Muscle 13 919-31).
ObjectivesCharacterizing ER stress and UPR in SCH and BD.
MethodsWe studied ER stress and UPR in peripheral blood mononuclear cells (PBMC) from 50 patients with SCH and an equal number of patients with BD compared to their corresponding controls in order to achieve our objectives.
Western Blot assay were performed following classical procedure () and the results was normalized to Ponceau as loanding control (Nie et al. 2017; BiochemByophys Resp 12 10-13) (Sander et al. 2019; Anal Biochem 575 44-53). Proteasome activity was assessed using Proteasome Activity Assay Kit (ab107921, Abcam, Cambridge, UK).
ResultsER stress was evaluated with BiP/GRP78. Our results showed significantly increased expression in SCH (p<0,01) and BD (p<0,05), being more increased in SCH. Proteasome activity was increased in SCH and BD, being only statistically significant in SQZ (p<0,05). UPR study showed IRE1a cascade significantly activated in SCH (p<0,001) and only slight increased in BD showed without statistical differences. ATF6a pathway is measured by cleavage to active protein (50-kDa). Results showed higher expression in SCH than in BD and controls (p<0,001). In addition, PERK pathway showed higher statistical levels of p-eIF2a/eiF2a ratio in SCH than in BD and control respectively (p<0,05 and p<0,01).
ConclusionsOur results showed a greater alteration in SCH than in BD at the level of protein synthesis, which implies a greater toxicity at the cellular level and, therefore, a clear risk for the survival of cells in this pathology.
Disclosure of InterestNone Declared
SOD and CAT as potential preliminary biomarkers for the differential diagnosis of schizophrenia and bipolar disorder in the first episode of psychosis
- C. Cachán-Vega, E. Antuña, C. García-González, J. C. Bermejo-Millo, F. Baena-Huerta, L. González-Blanco, B. Caballero, I. Vega-Naredo, J. Bobes, M. P. García-Portilla, A. Coto-Montes, Y. Potes
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S449-S450
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia (SCH) and bipolar disorder (BD) are severe mental disorders which lead to psychotic, affective and cognitive symptoms and often cause a progressive functional deterioration of the individual. The current diagnosis of SCH and BD essentially depends on clinical observation that often leads to misdiagnosis and the introduction of non-specific treatments. Therefore, an early detection and intervention are determinant for a better prognosis. Improving outcomes of a First Episode of Psychosis (FEP) depends mainly on the identification of reliable and discriminatory biomarkers between both disorders.
ObjectivesGiven that oxidative stress has been tightly involved in multiple metal disorders, the major goal of this work was to characterize oxidative alterations in order to identify potential biomarkers which allow the differential diagnosis in an early stage.
MethodsThe study was carried out on samples from 49 subjects (14 women and 35 men), divided into four groups: a control group of 10 individuals not previously diagnosed with any serious mental disorder, 17 patients who had presented a FEP, 12 patients diagnosed with SCH and 10 patients diagnosed with BP. Biochemical analysis were conducted in erythrocyte fraction to characterize the cellular oxidative damage by measuring lipid peroxidation (LPO) levels and the antioxidant defense system by the evaluation of catalase (CAT) and superoxide dismutase (SOD) activities.
ResultsIn the present work, we observed a significant increase in LPO levels in both SCH and BD disorders that was not neutralized by the antioxidant defense. It was found that SCH patients, despite exhibiting greater activities of SOD and CAT compared to BD individuals, also showed significantly higher levels of oxidative damage. The differential oxidative profile observed between SCH and BD individuals allowed to perform an individually analysis of patients diagnosed with FEP. Although it was not possible to identify the type of psychotic disorder of all the patients with FEP, the results obtained showed that while several individuals exhibited an oxidative prolife similar to that observed in SCH patients, other individuals presented a prolife very similar to that found in patients with BD.
ConclusionsThe current work reveals that LPO is a potential indicator of worse prognosis after being differentially modified in both SCH and BD. Moreover, SOD and CAT have been identified, by presenting an opposite profile between patients with SCH and BD, as potential preliminary biomarkers for a discriminatory diagnosis in an early stage of the disorder.
Disclosure of InterestNone Declared
Resistant depression. Clinical manifestations and diagnosis. Purposely a case
- S. M. Bañón González, N. Ogando Portilla, O. Sobrino cabra, B. Gamo Bravo, F. García Sánchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S844
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The term “depression” can be used in different senses: it can be a syndrome, a mood state, a mental disorder, and all of them are distinct clinical conditions…There are no pathognomonic features of bipolar/unipolar depression. A good medical history is the most important component of the evaluation. We have to use clinical variables and differential epidemiology for a correct diagnosis.
ObjectivesThey both analyze clinical, psychopathological and epidemiological characteristics of resistant depression and they review causes, incidence, prevalence, diagnostic, therapeutic tools and the importance of maintaining the treatment, because the abandonment of the treatment is a good predictor of possible relapses.
MethodsA literature Review of the last five years concerning resistant depression has been done: prevalence, incidence, pathogenesis and its relationship with other psychiatric disorders encoded in DSM-V.
ResultsUnipolar major depression (major depressive disorder) is characterized by a history of one or more major depressive episodes and no previous history of mania or hypomania symptoms. A major depressive episode is presented with five or more of the following nine symptoms for at least two consecutive weeks; at least one of them must be either a depressed mood or a loss of interest or pleasure. In addition, the symptoms must cause significant distress or psychosocial impairment, and not be a direct result of a substance or general medical condition.
ConclusionsSymptoms of unipolar depression in adults can overlap with symptoms of other psychiatric and general medical disorders. Unipolar depression needs to be distinguished from these other disorders to prevent inappropriate treatment.
Disclosure of InterestNone Declared
An empirical staging model for schizophrenia using machine learning
- M.-C. Clara, F. Sánchez-Lasheras, A. García-Fernández, L. González-Blanco, P. A. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S626-S627
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the great challenges still to be achieved in schizophrenia is the development of a staging model that reflects the progression of the disorder. The previous models suggested have been developed from a theoretical point of view and do not include objective variables such as biomarkers, physical comorbidities, or self-reported subjective variables (Martinez-Cao et al. Transl Psychiatry 2022; 12(1) 1-11).
ObjectivesDevelop a multidimensional staging model for schizophrenia based on empirical data.
MethodsNaturalistic, cross-sectional study. Sample: 212 stable patients with Schizophrenia (F20). Assessments: ad hoc questionnaire (demographic and clinical information); psychopathology: PANSS, CDS, OSQ, CGI-S; functioning: PSP; cognition: MATRICS; laboratory tests: C-Reactive Protein (CRP), IL-1RA, IL-6, Platelets/Lymphocytes (PLR), Neutrophils/Lymphocytes (NLR), and Monocytes/Lymphocytes (MLR) ratios. Statistical analysis: Variables selection was performed with an ad hoc algorithm developed for this research. The referred algorithm makes use of genetic algorithms (GA) to select those variables that show the best performance for the patients classification according to their global CGI-S. The objective function of the GA maximizes the individuals correct classification of a support vector machines (SVM) model that employs as input variables those given by the GA (Díez-Díaz et al. Mathematics 2021; 9(6) 654). Models performance was assessed with the help of 3-fold cross-validation and these process was repeated 10,000 times for each one of the models assessed.
ResultsMean age(SD): 39.5(13.54); men: 63.5%; secondary education: 59.50%. Most patients in our sample had never been married (74.10%), and more than a third received disability benefits due to schizophrenia (37.70%). The mean length of the disease was 11.98(12.02) years. The best SVM model included the following variables: 1)Clinical: number of hospitalizations, positive, negative, depressive symptoms and general psychopathology; 2)Cognition: speed of processing, visual learning and social cognition; 3)Functioning: PSP total score; 4)Biomarkers: PLR, NLR and MLR. This model was executed again 100,000 times applying again 3-fold cross-validation. In 95% of the algorithm executions more than a 53.52% of the patients were classfied in the right CGI-S category. On average the right classification was of 61.93%. About specificity and sensitivity the average values obtained were of 0.85 and 0.64 respectively.
ConclusionsOur staging model is a robust method that appropriately distributes patients according to the severity of the disorder. Highlights the importance of clinical, functional and cognitive factors to classify patients. Finally, the inflammatory parameters PLR, NLR and MLR have also emerged as potential biomarkers for staging schizophrenia.
Disclosure of InterestNone Declared
Endocrine biomarkers related to sleep-wake cycle and sleep disturbances in patients with bipolar disorder: A systematic review
- L. Gonzalez-Blanco, C. Moya Lacasa, S. Jiménez-Fernández, M. Valtueña, C. Martinez-Cao, A. García Fernández, P.A. Saiz, M.P. Garcia-Portilla, J. Bobes, L. Gutierrez Rojas
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S360
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Sleep and circadian disturbances have been widely studied in patients with bipolar disorder (BD) (Duarte Faria et al., 2015; Gonzalez, 2014). However, there is no clear evidence about the role of peripheral biomarkers of circadian cycle in this population.
ObjectivesThis systematic review aims to identify potential endocrine biomarkers of circadian rhythm in blood and study their relationship with sleep problems in BD.
MethodsAn electronic search of Pubmed and PsycoInfo databases were performed. It includes articles about the topic from 1991 to 2021. The search strategy was: (“Peripheral biomarkers” OR “biological markers” OR biomarker OR cortisol OR melatonin OR orexin OR hypocretin) AND (blood OR serum OR plasma) AND (“sleep-wake” OR “circadian rhythm” OR sleep OR insomnia) AND “bipolar”.
Results92 records were obtained after excluding duplicates. Only five studies met the inclusion criteria (n = 499; BD = 125; unipolar depression = 148; schizophrenia = 80; controls = 146). The endocrine parameters analyzed were: cortisol (3 studies), melatonin (1 study) and orexin-A (1 study). Overall, no significant associations between these biomarkers and sleep disturbances, assessed with subjective (psychometric evaluation) and/or objective (polysomnography) measures, were detected.
ConclusionsThis systematic review highlights the lack of studies that explores the role of endocrine biomarkers related to circadian function in the pathophysiology of sleep disturbances in BD.
DisclosureNo significant relationships.
Mental Health Home Care program to pacients with Serious Mental Disorders
- S.M. Bañón González, N. Ogando Portilla, C. Montalvo Vico, F. Garcia Sánchez, M. Gutiérrez Rodríguez, R. Gutiérrez Labrador
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S627
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Mental Health Home Care is a program whose main objective is to provide care to people with a Serious Mental Disorders with difficulties to maintain continuity of treatment and link between the different resources. It is a program that guarantees continuity of care and facilitates the link between the different rehabilitation resources. It carries out a multidisciplinary approach to the difficulties of the patient and the family.
ObjectivesBoth analyze clinical, psychopathological and epidemiological characteristics of Serius Mental Disorders and review causes, incidence, prevalence, diagnostic, therapeutic tools and the importance of maintaining the treatment and rehabilitation in Serius Mental Disorders, because the abandonment of the treatment is a predictor of relapses.
MethodsReview of the impact literature for the last five years concerning Serius Mental Disorder: prevalence, incidence, pathogenesis and its relationship with other psychiatric disorders encoded in DSM-V.
ResultsThe program is made up of a Psychiatrist, a Clinical Psychologist, a Mental Health Nurse and two Nursing Auxiliary Care, two Social Workers and two Occupational Therapists.The responsible professional presents the patient at the program meetings. The program’s multidisciplinary team proposes an individualized treatment plan for the patient and family in the patient’s environment.
ConclusionsThe objective and areas of global intervention is to provide comprehensive psychiatric, psychological, social and rehabilitative support in patients with difficulty in linking to other resources, keeping the patient in a normalized community context, improving treatment compliance and making appropriate use of standardized mental health services.
DisclosureNo significant relationships.
Insomnia associated with neutrophil/lymphocyte ratio in female patients with schizophrenia
- G. Paniagua, L. González-Blanco, F. Dal Santo, C. Martínez-Cao, C. Moya-Lacasa, M. Valtueña-García, E. Martín Gil, L. García-Alvarez, P.A. Saiz, M.P. García-Portilla, J. Bobes
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S806
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Worse sleep quality and increased inflammatory markers in women with schizophrenia (Sch) have been reported (Lee et al. 2019). However, the physiological mechanisms underlying the interplay between sleep and the inflammatory pathways are not yet well understood (Fang et al. 2016).
ObjectivesAnalyze the relationship between Neutrophil/Lymphocyte (NLR), Monocyte/Lymphocyte (MLR) and Platelet/Lymphocyte (PLR) ratios, and insomnia in Sch stratified by sex.
MethodsFinal sample included 176 Sch patients (ICD-10 criteria) [mean age: 38.9±13.39; males: 111(63.1%)]. Assessment: PANSS, Calgary Depression Scale (CDSS), and Oviedo Sleep Questionnaire (OSQ) to identify a comorbid diagnosis of insomnia based on ICD-10. Fasting counting blood cell were performed to calculate ratios. Statistics: U Mann-Whitney, logistic regression.
ResultsInsomnia as comorbid diagnosis was present in 22 Sch (12.5%) with no differences between sex [14 males (12.6%), 8 females (12.3%)], neither in their age. Female patients with insomnia showed increased NLR [2.44±0.69 vs. 1.88±0.80, U=122.00 (p=0.034)]. However, no differences in PLR and MLR were found, neither in any ratio in males. Regression models using insomnia as dependent variable and covariates (age, PANSS-positive, PANSS-negative, CDSS) were estimated. Females: presence of insomnia was associated with NLR [OR=3.564 (p=0.032)], PANSS-positive [OR=1.263 (p=0.013)] and CDSS [OR=1.198 (p=0.092)]. Males: only PANSS-positive [OR=1.123 (p=0.027)] and CDSS scores [OR=1.220 (p=0.005)] were associated with insomnia.
ConclusionsNLR represent an inflammatory marker of insomnia in Sch but only in female patients. Improving sleep quality in these patients could help to decrease their inflammatory response.
DisclosureNo significant relationships.
Orexins in the clinical course of bipolar disorder
- C. Moya-Lacasa, M. Valtueña-García, E. Martín Gil, L. González-Blanco, M.P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S623
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Orexins are involved in the regulation of circadian rhythms which play an important role in mood regulation(1,2), and are hypothesised to be associated with major depressive disorder(3). However, scarce studies analyse their relationship with bipolar disorder (BD).
ObjectivesTo evaluate the relationship of orexin-A and the clinical course of BD
Methods95 BD patients were tested for serum orexin-A. The clinical course was analysed through number of depressive, manic/mixed episodes. HDRS and YMRS were used to assess severity of current episode. Statistics: Spearman correlations, U Mann-Whitney, linear regression analysis.
ResultsMean age was 50.03 (SD=12.87) and 64.2% were women. 63.2% had BD-type I. Mean number of manic, depressive and mixed episodes was 2.32 (SD=3.07), 7.28 (SD=12.37), and 3.01 (SD=9.06), respectively. Mean age of onset was 26.09 (SD=10.50). Mean concentration of orexin-A was 21.78 pg/ml (SD=15.41), with no differences in sex, body mass index, age at onset or presence of insomnia(ICD-10). A correlation with age was observed; r=0.24 (p=0.019). No association was identified between orexin-A and severity of current episode. In relation to clinical course, no correlation was found with manic or mixed episodes. However, a negative correlation was identified between orexin-A levels and number of depressive episodes; r=-0.36 (p=0.001). When linear regression (orexin-A as dependent variable) was used to control for age, only this covariate (B=0.304) entered in the model (R2=0.067, F=6.045, p=0.015).
ConclusionsNo relationship between orexin-A and number of manic/mixed episodes were detected. The association of orexin-A with number of depressive episodes dissappeared when age was controlled.
DisclosureNo significant relationships.
COVID-19 psychological impact in patients with depressive disorder: Differences based on their age
- E. Martín Gil, M. Valtueña-García, L. González-Blanco, F. Dal Santo, C. Moya-Lacasa, C. Álvarez Vázquez, C. Martínez-Cao, L. García-Alvarez, M.P. García-Portilla, P.A. Saiz, J. Bobes
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S674-S675
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
COVID-19 pandemic and lockdown have provoked a considerable psychological impact in Spain. Some studies have reported greater psychological impact in the younger population. To date, no previous study has focused on depressive disorder (DD) patients based on their age.
ObjectivesTo describe the psychological impact on DD according to age.
MethodsCross-sectional study of an online survey available from 19 to 26 March 2020. Out of a total of 21207 respondents, 608 (2.9%) reported suffering from DD (mean age ±SD = 41.2 years±14.07 [18-82], 80.6% women). The subsample (608) was divided according to age, “youngsters” <45 (57.4%)/ “elders” ≥45. DASS-21 and IES scales were employed. Statistical analyses: Chi-square, t-Student test.
ResultsBoth groups did not differ (p>0.05) in sex, having COVID-19 symptoms, having family/friends infected, or income changes. While youngsters were single more frequently (68.8% vs 14.3%, χ² = 179.7, p<0.001), elders had somatic illness more frequently (64.8% vs 39.7% χ² =30.401, p<0.001). Youngsters obtained higher scores in depression (4.69 vs 4.1, T=5.413, p<0.001), anxiety (2.86 vs 1.97, T=5.249, p<0.001) and stress (4.48 vs 3.17, T=6.355, p<0.001) DASS-21 subscales, as in intrusive (3.42 vs 3.05, T=1.984, p=0.048) and avoidant (4.64 vs 4.11, T=3.056, p=0.002) IES scores.
ConclusionsDespite the group of elders with depression being more vulnerable to severe COVID-19 disease and presenting more frequently somatic comorbidities, younger depressive patients suffered more from depressive, anxiety, stress and avoidant symptoms and intrusive thoughts, in line with previous reports in the general population.
DisclosureNo significant relationships.
Examining the association between exposome score for schizophrenia and functioning in schizophrenia, siblings, and healthy controls: Results from the EUGEI study
- Gamze Erzin, Lotta-Katrin Pries, Jim van Os, Laura Fusar-Poli, Philippe Delespaul, Gunter Kenis, Jurjen J. Luykx, Bochao D. Lin, Alexander L. Richards, Berna Akdede, Tolga Binbay, Vesile Altınyazar, Berna Yalınçetin, Güvem Gümüş-Akay, Burçin Cihan, Haldun Soygür, Halis Ulaş, Eylem Şahin Cankurtaran, Semra Ulusoy Kaymak, Marina M. Mihaljevic, Sanja Andric-Petrovic, Tijana Mirjanic, Miguel Bernardo, Gisela Mezquida, Silvia Amoretti, Julio Bobes, Pilar A. Saiz, Maria Paz García-Portilla, Julio Sanjuan, Eduardo J. Aguilar, Jose Luis Santos, Estela Jiménez-López, Manuel Arrojo, Angel Carracedo, Gonzalo López, Javier González-Peñas, Mara Parellada, Nadja P. Maric, Cem Atbaşoğlu, Alp Ucok, Köksal Alptekin, Meram Can Saka, Genetic Risk and Outcome of Psychosis (GROUP) investigators, Celso Arango, Micheal C. O’Donovan, Bart P. F. Rutten, Sinan Guloksuz
-
- Journal:
- European Psychiatry / Volume 64 / Issue 1 / 2021
- Published online by Cambridge University Press:
- 19 March 2021, e25
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
A cumulative environmental exposure score for schizophrenia (exposome score for schizophrenia [ES-SCZ]) may provide potential utility for risk stratification and outcome prediction. Here, we investigated whether ES-SCZ was associated with functioning in patients with schizophrenia spectrum disorder, unaffected siblings, and healthy controls.
MethodsThis cross-sectional sample consisted of 1,261 patients, 1,282 unaffected siblings, and 1,525 healthy controls. The Global Assessment of Functioning (GAF) scale was used to assess functioning. ES-SCZ was calculated based on our previously validated method. The association between ES-SCZ and the GAF dimensions (symptom and disability) was analyzed by applying regression models in each group (patients, siblings, and controls). Additional models included polygenic risk score for schizophrenia (PRS-SCZ) as a covariate.
ResultsES-SCZ was associated with the GAF dimensions in patients (symptom: B = −1.53, p-value = 0.001; disability: B = −1.44, p-value = 0.001), siblings (symptom: B = −3.07, p-value < 0.001; disability: B = −2.52, p-value < 0.001), and healthy controls (symptom: B = −1.50, p-value < 0.001; disability: B = −1.31, p-value < 0.001). The results remained the same after adjusting for PRS-SCZ. The degree of associations of ES-SCZ with both symptom and disability dimensions were higher in unaffected siblings than in patients and controls. By analyzing an independent dataset (the Genetic Risk and Outcome of Psychosis study), we replicated the results observed in the patient group.
ConclusionsOur findings suggest that ES-SCZ shows promise for enhancing risk prediction and stratification in research practice. From a clinical perspective, ES-SCZ may aid in efforts of clinical characterization, operationalizing transdiagnostic clinical staging models, and personalizing clinical management.
Examining the independent and joint effects of genomic and exposomic liabilities for schizophrenia across the psychosis spectrum
- L.-K. Pries, G. A. Dal Ferro, J. van Os, P. Delespaul, G. Kenis, B. D. Lin, J. J. Luykx, A. L. Richards, B. Akdede, T. Binbay, V. Altınyazar, B. Yalınçetin, G. Gümüş-Akay, B. Cihan, H. Soygür, H. Ulaş, E. Şahin Cankurtaran, S. Ulusoy Kaymak, M. M. Mihaljevic, S. Andric Petrovic, T. Mirjanic, M. Bernardo, G. Mezquida, S. Amoretti, J. Bobes, P. A. Saiz, M. Paz García-Portilla, J. Sanjuan, E. J. Aguilar, J. L. Santos, E. Jiménez-López, M. Arrojo, A. Carracedo, G. López, J. González-Peñas, M. Parellada, N. P. Maric, C. Atbaşoğlu, A. Ucok, K. Alptekin, M. Can Saka, Genetic Risk and Outcome of Psychosis (GROUP) investigators, C. Arango, M. O'Donovan, S. Tosato, B. P. F. Rutten, S. Guloksuz
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 17 November 2020, e182
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Psychosis spectrum disorder has a complex pathoetiology characterised by interacting environmental and genetic vulnerabilities. The present study aims to investigate the role of gene–environment interaction using aggregate scores of genetic (polygenic risk score for schizophrenia (PRS-SCZ)) and environment liability for schizophrenia (exposome score for schizophrenia (ES-SCZ)) across the psychosis continuum.
MethodsThe sample consisted of 1699 patients, 1753 unaffected siblings, and 1542 healthy comparison participants. The Structured Interview for Schizotypy-Revised (SIS-R) was administered to analyse scores of total, positive, and negative schizotypy in siblings and healthy comparison participants. The PRS-SCZ was trained using the Psychiatric Genomics Consortiums results and the ES-SCZ was calculated guided by the approach validated in a previous report in the current data set. Regression models were applied to test the independent and joint effects of PRS-SCZ and ES-SCZ (adjusted for age, sex, and ancestry using 10 principal components).
ResultsBoth genetic and environmental vulnerability were associated with case-control status. Furthermore, there was evidence for additive interaction between binary modes of PRS-SCZ and ES-SCZ (above 75% of the control distribution) increasing the odds for schizophrenia spectrum diagnosis (relative excess risk due to interaction = 6.79, [95% confidential interval (CI) 3.32, 10.26], p < 0.001). Sensitivity analyses using continuous PRS-SCZ and ES-SCZ confirmed gene–environment interaction (relative excess risk due to interaction = 1.80 [95% CI 1.01, 3.32], p = 0.004). In siblings and healthy comparison participants, PRS-SCZ and ES-SCZ were associated with all SIS-R dimensions and evidence was found for an interaction between PRS-SCZ and ES-SCZ on the total (B = 0.006 [95% CI 0.003, 0.009], p < 0.001), positive (B = 0.006 [95% CI, 0.002, 0.009], p = 0.002), and negative (B = 0.006, [95% CI 0.004, 0.009], p < 0.001) schizotypy dimensions.
ConclusionsThe interplay between exposome load and schizophrenia genetic liability contributing to psychosis across the spectrum of expression provide further empirical support to the notion of aetiological continuity underlying an extended psychosis phenotype.
Evidence, and replication thereof, that molecular-genetic and environmental risks for psychosis impact through an affective pathway
- Jim van Os, Lotta-Katrin Pries, Margreet ten Have, Ron de Graaf, Saskia van Dorsselaer, Philippe Delespaul, Maarten Bak, Gunter Kenis, Bochao D. Lin, Jurjen J. Luykx, Alexander L. Richards, Berna Akdede, Tolga Binbay, Vesile Altınyazar, Berna Yalınçetin, Güvem Gümüş-Akay, Burçin Cihan, Haldun Soygür, Halis Ulaş, Eylem Şahin Cankurtaran, Semra Ulusoy Kaymak, Marina M. Mihaljevic, Sanja Andric Petrovic, Tijana Mirjanic, Miguel Bernardo, Gisela Mezquida, Silvia Amoretti, Julio Bobes, Pilar A. Saiz, María Paz García-Portilla, Julio Sanjuan, Eduardo J. Aguilar, José Luis Santos, Estela Jiménez-López, Manuel Arrojo, Angel Carracedo, Gonzalo López, Javier González-Peñas, Mara Parellada, Nadja P. Maric, Cem Atbaşoğlu, Alp Ucok, Köksal Alptekin, Meram Can Saka, Celso Arango, Michael O'Donovan, Bart P. F. Rutten, Sinan Guloksuz
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 10 / July 2022
- Published online by Cambridge University Press:
- 19 October 2020, pp. 1910-1922
-
- Article
- Export citation
-
Background
There is evidence that environmental and genetic risk factors for schizophrenia spectrum disorders are transdiagnostic and mediated in part through a generic pathway of affective dysregulation.
MethodsWe analysed to what degree the impact of schizophrenia polygenic risk (PRS-SZ) and childhood adversity (CA) on psychosis outcomes was contingent on co-presence of affective dysregulation, defined as significant depressive symptoms, in (i) NEMESIS-2 (n = 6646), a representative general population sample, interviewed four times over nine years and (ii) EUGEI (n = 4068) a sample of patients with schizophrenia spectrum disorder, the siblings of these patients and controls.
ResultsThe impact of PRS-SZ on psychosis showed significant dependence on co-presence of affective dysregulation in NEMESIS-2 [relative excess risk due to interaction (RERI): 1.01, p = 0.037] and in EUGEI (RERI = 3.39, p = 0.048). This was particularly evident for delusional ideation (NEMESIS-2: RERI = 1.74, p = 0.003; EUGEI: RERI = 4.16, p = 0.019) and not for hallucinatory experiences (NEMESIS-2: RERI = 0.65, p = 0.284; EUGEI: −0.37, p = 0.547). A similar and stronger pattern of results was evident for CA (RERI delusions and hallucinations: NEMESIS-2: 3.02, p < 0.001; EUGEI: 6.44, p < 0.001; RERI delusional ideation: NEMESIS-2: 3.79, p < 0.001; EUGEI: 5.43, p = 0.001; RERI hallucinatory experiences: NEMESIS-2: 2.46, p < 0.001; EUGEI: 0.54, p = 0.465).
ConclusionsThe results, and internal replication, suggest that the effects of known genetic and non-genetic risk factors for psychosis are mediated in part through an affective pathway, from which early states of delusional meaning may arise.
A replication study of JTC bias, genetic liability for psychosis and delusional ideation
- Cécile Henquet, Jim van Os, Lotta K. Pries, Christian Rauschenberg, Philippe Delespaul, Gunter Kenis, Jurjen J. Luykx, Bochao D. Lin, Alexander L. Richards, Berna Akdede, Tolga Binbay, Vesile Altınyazar, Berna Yalınçetin, Güvem Gümüş-Akay, Burçin Cihan, Haldun Soygür, Halis Ulaş, Eylem S. Cankurtaran, Semra U. Kaymak, Marina M. Mihaljevic, Sanja S. Petrovic, Tijana Mirjanic, Miguel Bernardo, Gisela Mezquida, Silvia Amoretti, Julio Bobes, Pilar A. Saiz, Maria P. García-Portilla, Julio Sanjuan, Eduardo J. Aguilar, Jose L. Santos, Estela Jiménez-López, Manuel Arrojo, Angel Carracedo, Gonzalo López, Javier González-Peñas, Mara Parellada, Nadja P. Maric, Cem Atbaşoğlu, Alp Ucok, Köksal Alptekin, Meram C. Saka, Celso Arango, Michael O'Donovan, Bart P.F. Rutten, Sinan Gülöksüz
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 9 / July 2022
- Published online by Cambridge University Press:
- 13 October 2020, pp. 1777-1783
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
This study attempted to replicate whether a bias in probabilistic reasoning, or ‘jumping to conclusions’(JTC) bias is associated with being a sibling of a patient with schizophrenia spectrum disorder; and if so, whether this association is contingent on subthreshold delusional ideation.
MethodsData were derived from the EUGEI project, a 25-centre, 15-country effort to study psychosis spectrum disorder. The current analyses included 1261 patients with schizophrenia spectrum disorder, 1282 siblings of patients and 1525 healthy comparison subjects, recruited in Spain (five centres), Turkey (three centres) and Serbia (one centre). The beads task was used to assess JTC bias. Lifetime experience of delusional ideation and hallucinatory experiences was assessed using the Community Assessment of Psychic Experiences. General cognitive abilities were taken into account in the analyses.
ResultsJTC bias was positively associated not only with patient status but also with sibling status [adjusted relative risk (aRR) ratio : 4.23 CI 95% 3.46–5.17 for siblings and aRR: 5.07 CI 95% 4.13–6.23 for patients]. The association between JTC bias and sibling status was stronger in those with higher levels of delusional ideation (aRR interaction in siblings: 3.77 CI 95% 1.67–8.51, and in patients: 2.15 CI 95% 0.94–4.92). The association between JTC bias and sibling status was not stronger in those with higher levels of hallucinatory experiences.
ConclusionsThese findings replicate earlier findings that JTC bias is associated with familial liability for psychosis and that this is contingent on the degree of delusional ideation but not hallucinations.
Trends in suicide in the elderly in Asturias (Spain)
- J Díaz-Suárez, B Lopez Garcia, P Gonzalez-G-Portilla, M Bousoño Garcia, R Hinojal Fonseca, J Bobes Garcia
-
- Journal:
- European Psychiatry / Volume 10 / Issue 7 / 1995
- Published online by Cambridge University Press:
- 16 April 2020, pp. 339-344
-
- Article
- Export citation
-
Data from elderly suicides was obtained from two previous studies of community suicides in two localities of Northern Spain, namely, Oviedo between 1983 and 1990, and Gijón between 1975 and 1986. Data from the two localities were obtained by the revision of court register cases. A retrospective study on elderly suicide (over 60 years of age) was carried out. Mean annual specific rates for the elderly in Oviedo for 1982–1991 were 37.7 (58.1 for men and 23.3 for women) and for those in Gijón for the period 1975–1986, 23.4 (40 for men and 11.5 for women). A marked increase was seen in the rates for Gijón from the first (1975–1978) to the last period (1983–1986). This was particularly marked in men. The greatest increase in the rate was seen in men over 75 from Gijón and in those between 1970–1974 from Oviedo. In contrast a decrease was seen in the 65–69 age group rates for both men and women. A tendency for the rates to increase was seen but no important increase for elderly suicides was evident.
EPA-0512 – Multidisciplinary Approach in Patients with Severe Pshychotic Illness
- N. Ogando Portilla, S. Gonzalez-Coloma, J. López Higes, I. Vidal Navarro, M. Martínez Cortés, P. García González, F. Del Olmo
-
- Journal:
- European Psychiatry / Volume 29 / Issue S1 / 2014
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Schizophrenia is a psychiatric disorder which involves chronic or recurrent psychosis and it is commonly associated with impairment in social and occupational functioning. Antipsychotic medications are a first-line treatment, however, most patients experience disabling impairment even after benefiting from antipsychotics, including positive and negative symptoms, cognitive deficits, poor social functioning and episodes of acute symptomatic relapse.
Methods:Systematic literature review in UpToDate and Pubmed.
Objectives:To identify the most relevant intervention areas of systematic rehabilitation in schizophrenia.
Clinical case:45 years old schizophrenic male who admitted in a Medium Stay Psychiatry Unit with severe behavioural impairment and psychotic symptoms. At least 10 hospitalizations and pronounced disability in basic life skills despite optimal treatment. Poor insight and compliance, frequent relapses, co-morbid substance abuse and difficult family support. Clozapine was added to his treatment with improvement in psychotic symptoms. A multidisciplinary intervention was also done and he was discharged home with important improvement in social skills, better insight and familiar functioning
Discussion:Despite following an adequate antipsychotic treatment, including Clozapine as the main medication in resistant schizophrenia, it is often partially effective with severe impairments in social and occupational functioning. Family-based interventions, cognitive behavioural therapy and social skills training, added to this medication seem to be essential in the systematic treatment of schizoprenia. It includes a multidisciplinary team and a specific length of time but it is based on the patient's status. Despite evidence of their efectiveness, the availability of these interventions varies widely, as does the availability of clinicians to provide them.
Differential Biomarkers of Negative Dimension in Schizophrenia
- M. Garcia-Portilla Gonzalez, L. García-Álvarez, E. Díaz-Mesa, P. Burón-Fernández, S. Al-Halabi, P.A. Sáiz, J. Bobes
-
- Journal:
- European Psychiatry / Volume 30 / Issue S1 / March 2015
- Published online by Cambridge University Press:
- 15 April 2020, p. 1
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Schizophrenia is not only a mental disorder but also has other components affecting the physical part of the body. Several studies have suggested that neuroinflammatory processes may play a role in schizophrenia pathogenesis, at least in a subgroup of patients.
AimsThis poster reported the preliminary results of a project aiming to find schizophrenia biomarkers. We present biological parameters and clinical variables of patients with schizophrenia according to the lab results and the clinical assessments.
MethodsCross-sectional, naturalistic study. Inclusion criteria: DSM-IV diagnosis of schizophrenia; age >17 years; and written informed consent given.
Results123 patients with schizophrenia. Mean age 40.75 (10.37), 67.5% males. There is relationship between homocysteine(oxidative stress) and psychopathology: PANSS [negative subscale 0.27 (p=0.003), general subscale 0.21 (p=0.028) and Marder factor 0.28 (p=0.003)], NSA [global score 0.24 (p=0.010), and some factors: communication 0.26 (p=0.005), affect 0.28 (p=0.002), motivation 0.30 (p=0.001) and motor retardation 0.27 (p=0.004)]; Functioning [(PSP total score -0.24 (p=0.011) and some PSP factors: work 0.30 (p=0.001), self-care 0.21 (p=0.022)]. However, there is no relationship between C-reactive protein(inflammation) and any clinical variable. On the other hand, there is relationship between: glucose and cognitive impairment; cholesterol and NSA motivation score, cognitive impairment and PSP (total score, self-care and work); triglycerides and HDRS (total score, melancholia factor and vitality factor), NSA motivation score and cognitive impairment.
ConclusionThe negative dimension of schizophrenia is associated with high homocysteine levels, which means an oxidative stress state. As well, a worse functioning level is associated with high homocysteine level.
1655 – Suicide Attempt Prediction In a Controlled Study Of Case Management In The Prevention Of Recurrent Suicidal Behaviour
- P. Burón, S. Al-Halabí, M. Garrido, J. Rodríguez-Revuelta, L. García-Álvarez, L. González-Blanco, P. García-Portilla, P.A. Sáiz, J. Bobes
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E933
-
- Article
-
- You have access Access
- Export citation
-
Introduction
Information about the perception of suicide attempters regarding prevention of their suicide attempt may be helpful in implementing preventive strategies.
AimTo examine:
(i) sociodemographic profile,
(ii) distribution of the Suicide Intent Scale, and
(iii) differences according to the gender in the sample of participants in a controlled study to determine the effectiveness of case management programme in the prevention of recurrent suicidal behaviour.
Method106 suicide attempters who attended the Emergency Room of the Hospital of Asturias from July- 2011 to October- 2012 were included in the study [33% males; mean age (SD)= 41.82 (13.16)]. Instruments: Ad hoc Sociodemographic- Questionnaire; Suicide Intent Scale (SIS); SAD-PERSON Scale; Medical Damage Scale; List of Threatening Experiences; Hamilton Depression Rating Scale.
ResultsProfile: 45-54 years old (30.4%), married (34%), with bachelor's degree (42.5%), unemployed (29.2%), with children (61.3%) and living with partner (34.9%). 36.2% of the sample had the intention to repeat at the time of the suicide attempt (SA), while 22.6% actually repeated it. The intention to repeat the SA was associated with the commission of SA at 12-months follow-up (p=.002). SIS data: mean total score (SD)=15.99(4.71); mean objective score (SD)=5.69(2.48); mean subjective score (SD)=10.28(3.29). Significant differences in SIS scores were found by gender (p=.007), men scoring higher. Repetition of the SA was related with higher scores (p=.002).
ConclusionsSA severity and its repetition at 12-months follow-up was related with the intention of repetition; nevertheless we didn’t find relation between the SA severity and the repetition of SA one year later.




