160 results
The association of adverse childhood experiences with long-term outcomes of psychosis: a 21-year prospective cohort study after a first episode of psychosis
- Victor Peralta, Elena García de Jalón, Lucía Moreno-Izco, David Peralta, Lucía Janda, Ana M. Sánchez-Torres, Manuel J. Cuesta, SEGPEPs group
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 30 May 2024, pp. 1-10
-
- Article
- Export citation
-
Background
Evidence suggests a possible relationship between exposure to childhood adversity (CA) and functional impairment in psychosis. However, the impact of CA on long-term outcomes of psychotic disorders remains poorly understood.
MethodsTwo hundred and forty-three patients were assessed at their first episode of psychosis for CA and re-assessed after a mean of 21 years of follow-up for several outcome domains, including symptoms, functioning, quality of life, cognitive performance, neurological dysfunction, and comorbidity. The unique predictive ability of CA exposure for outcomes was examined using linear regression analysis controlling for relevant confounders, including socioeconomic status, family risk of schizophrenia, and obstetric complications.
ResultsThere were 54% of the patients with a documented history of CA at mild or higher levels. CA experiences were more prevalent and severe in schizophrenia than in other psychotic disorders (p < 0.001). Large to very large effect sizes were observed for CA predicting most role functioning variables and negative symptoms (ΔR2 between 0.105 and 0.181). Moderate effect sizes were observed for positive symptoms, personal functioning, impaired social cognition, impaired immediate verbal learning, poor global cognition, internalized stigma, poor personal recovery, and drug abuse severity (ΔR2 between 0.040 and 0.066). A dose–response relationship was observed between levels of CA and severity of outcome domains.
ConclusionOur results suggest a strong and widespread link between early adversity exposure and outcomes of psychotic disorders. Awareness of the serious long-term consequences of CA should encourage better identification of those at risk and the development of effective interventions.
Influence of Silica Content on the Surface Charge Characteristics of Allophanic Clays
- A. Gonzales-Batista, J. M. Hernandez-Moreno, E. Fernandez-Caldas, A. J. Herbillon
-
- Journal:
- Clays and Clay Minerals / Volume 30 / Issue 2 / April 1982
- Published online by Cambridge University Press:
- 02 April 2024, pp. 103-110
-
- Article
- Export citation
-
The surface and charge characteristics of 6 allophanic clays originating from a climatosequence of Andisols have been studied by titration, ion retention, surface area, and reactivity measurements. Several properties of these clays, such as the pH of zero charge, the magnitude of the surface area, and the reactivity of structural hydroxyl groups, appear to be governed by their chemical composition, especially by their silica content. A similar relationship between the above properties and silica content also exists for synthetic aluminosilicate gels (often quoted in the literature as possible models of allophanes), despite their different structure to the natural clays. An explanation is that as desilication proceeds, octahedral polymeric units of aluminum progressively individualize in both the synthetic and natural samples. The surface areas of the aUophanic clays, based on the slope of the titration curve at pH 7, are closely related to the amounts of structural hydroxyl that can react with fluoride at about the same pH. The permanent negative charges are always very low, even for silica-rich, allophane-bearing samples. It is therefore suggested that all of these clays should be virtually free of tetrahedral aluminum.
Dietary intake of dicarbonyl compounds and changes in body weight over time in a large cohort of European adults
- Charlotte Debras, Reynalda Cordova, Ana-Lucia Mayén, Kim Maasen, Viktoria Knaze, Simone J. P. M. Eussen, Casper G. Schalkwijk, Inge Huybrechts, Anne Tjønneland, Jytte Halkjær, Verena Katzke, Rashmita Bajracharya, Matthias B. Schulze, Giovanna Masala, Valeria Pala, Fabrizio Pasanisi, Alessandra Macciotta, Dafina Petrova, Jazmin Castañeda, Carmen Santiuste, Pilar Amiano, Conchi Moreno-Iribas, Yan Borné, Emily Sonestedt, Ingegerd Johansson, Anders Esberg, Elom Kouassivi Aglago, Mazda Jenab, Heinz Freisling
-
- Journal:
- British Journal of Nutrition / Volume 131 / Issue 11 / 14 June 2024
- Published online by Cambridge University Press:
- 22 February 2024, pp. 1902-1914
- Print publication:
- 14 June 2024
-
- Article
- Export citation
-
Dicarbonyl compounds are highly reactive precursors of advanced glycation end products (AGE), produced endogenously, present in certain foods and formed during food processing. AGE contribute to the development of adverse metabolic outcomes, but health effects of dietary dicarbonyls are largely unexplored. We investigated associations between three dietary dicarbonyl compounds, methylglyoxal (MGO), glyoxal (GO) and 3-deoxyglucosone (3-DG), and body weight changes in European adults. Dicarbonyl intakes were estimated using food composition database from 263 095 European Prospective Investigation into Cancer and Nutrition–Physical Activity, Nutrition, Alcohol, Cessation of Smoking, Eating Out of Home in Relation to Anthropometry participants with two body weight assessments (median follow-up time = 5·4 years). Associations between dicarbonyls and 5-year body-weight changes were estimated using mixed linear regression models. Stratified analyses by sex, age and baseline BMI were performed. Risk of becoming overweight/obese was assessed using multivariable-adjusted logistic regression. MGO intake was associated with 5-year body-weight gain of 0·089 kg (per 1-sd increase, 95 % CI 0·072, 0·107). 3-DG was inversely associated with body-weight change (–0·076 kg, −0·094, −0·058). No significant association was observed for GO (0·018 kg, −0·002, 0·037). In stratified analyses, GO was associated with body-weight gain among women and older participants (above median of 52·4 years). MGO was associated with higher body-weight gain among older participants. 3-DG was inversely associated with body-weight gain among younger and normal-weight participants. MGO was associated with a higher risk of becoming overweight/obese, while inverse associations were observed for 3-DG. No associations were observed for GO with overweight/obesity. Dietary dicarbonyls are inconsistently associated with body weight change among European adults. Further research is needed to clarify the role of these food components in overweight and obesity, their underlying mechanisms and potential public health implications.
Long-term diagnostic stability, predictors of diagnostic change, and time until diagnostic change of first-episode psychosis: a 21-year follow-up study
- David Peralta, Lucía Janda, Elena García de Jalón, Lucía Moreno-Izco, Ana M. Sánchez-Torres, Manuel J. Cuesta, Victor Peralta, SEGPEPs Group
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 7 / May 2024
- Published online by Cambridge University Press:
- 21 November 2023, pp. 1329-1338
-
- Article
- Export citation
-
Background
Although diagnostic instability in first-episode psychosis (FEP) is of major concern, little is known about its determinants. This very long-term follow-up study aimed to examine the diagnostic stability of FEP diagnoses, the baseline predictors of diagnostic change and the timing of diagnostic change.
MethodsThis was a longitudinal and naturalistic study of 243 subjects with FEP who were assessed at baseline and reassessed after a mean follow-up of 21 years. The diagnostic stability of DSM-5 psychotic disorders was examined using prospective and retrospective consistencies, logistic regression was used to establish the predictors of diagnostic change, and survival analysis was used to compare time to diagnostic change across diagnostic categories.
ResultsThe overall diagnostic stability was 47.7%. Schizophrenia and bipolar disorder were the most stable diagnoses, with other categories having low stability. Predictors of diagnostic change to schizophrenia included a family history of schizophrenia, obstetric complications, developmental delay, poor premorbid functioning in several domains, long duration of untreated continuous psychosis, spontaneous dyskinesia, lack of psychosocial stressors, longer duration of index admission, and poor early treatment response. Most of these variables also predicted diagnostic change to bipolar disorder but in the opposite direction and with lesser effect sizes. There were no significant differences between specific diagnoses regarding time to diagnostic change. At 10-year follow-up, around 80% of the diagnoses had changed.
ConclusionsFEP diagnoses other than schizophrenia or bipolar disorder should be considered as provisional. Considering baseline predictors of diagnostic change may help to enhance diagnostic accuracy and guide therapeutic interventions.
Review of a sample of episodes of forced medication in an area of southern Spain
- L. I. Muñoz-Manchado, J. M. Mongil-Sanjuan, J. I. Pérez-Revuelta, C. M. Robledo Casal, J. M. Villagrán-Moreno
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1067
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Forced medication is one of the most frequently used coercive measures in acute mental health units. It is a practice that can lead to physical, psychological and psychopathological consequences. Therefore, it is necessary to implement measures to reduce its use. In this sense, it is interesting to study the variables that can be associated with its use, and thus take measures accordingly.
ObjectivesThis study attempts to identify the number of forced medication episodes between July 2017 and December 2018 treated in the catchment area of the Mental Health Service at Jerez Hospital. As a secondary objective, it pursues to identify the factors that conducted to the use of forced medication with the intention of being able to reduce the use of these measures.
MethodsA descriptive and retrospective study has been developed reviewing the total number of episodes of forced medication. Patients admitted and discharged from hospital between July 2017 and December 2018 treated in the Mental Health Service at Jerez Hospital. Data were extracted from medical records.
ResultsThe total number of episodes of forced medication identified was 330. In these episodes, the average age was 41 years, with a predominance of 74% of the male gender. The most used route in the episodes was intramuscular (94.8%), in addition, more than 50% needed the association of two drugs, the most used were haloperidol and olanzapine. The 32.7% of the episodes also required the use of mechanical restraint and 44.2% required the presence of security service.
Image:
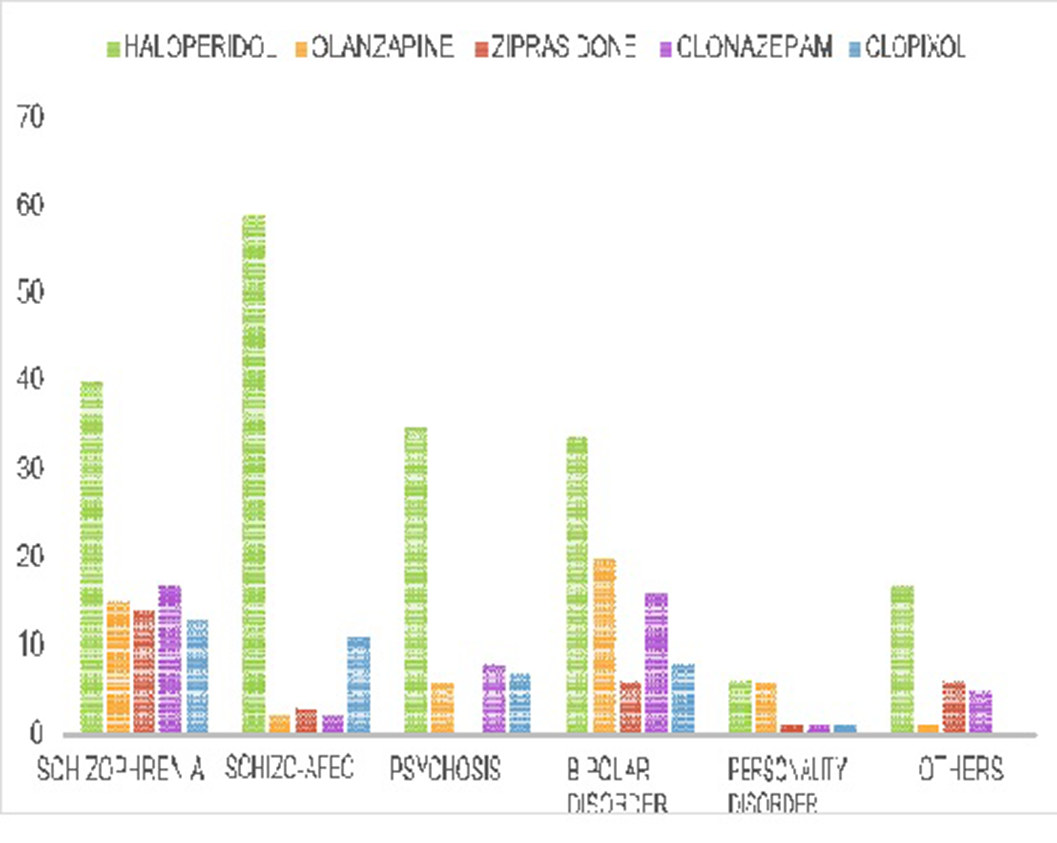 Conclusions
ConclusionsWe present the descriptive analysis of a further study currently been conducted in hour hospital which means to stablish predictive factors for the use of forced medication. We therefore intend to create patient profile, as well as new measures specifically directed to these factors with which to diminish the use of forced medication.
Disclosure of InterestNone Declared
Cumulative trauma exposure comparison between non-refugee immigrants and locals with psychotic disorder
- A. Trabsa Biskri, A. Mané, L. González, J. M. Ginés, F. Casanovas, A. Moreno, B. Amann, V. Pérez Sola
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S62
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A significant global increase in immigration has been reported due to humanitarian crisis around the world. Trauma exposure related to migration process is usually multiple and maintained in long-term which could provoke a cumulative effect. Moreover, several meta-analysis describe increased risk for psychosis in immigrant population. Despite this increase, there is a lack of research in non-refugee immigrants specially within those with psychotic disorder.
ObjectivesThe aim of the study is to describe and compare cumulative lifetime trauma between immigrants and locals with psychotic disorder.
MethodsPatients who have presented, according to DSM-V criteria, one or more non-affective psychotic episodes, were recruited in Acute and Chronic inpatients units at Hospital del Mar (Barcelona) from November 2019 to June 2021, leading to a total sample of 199 patients. Demographic characteristics of patients, clinical data and main pharmacological treatment were recorded through a questionnaire. Database information was completed with electronic medical records. Cumulative trauma Scale was used as instrument to assess lifetime trauma exposure frequency and distress. Comparative analysis was performed with IBM SPSS Statistics (Chicago INC) using Chi-Square Test for qualitative variables and t-Student test for continuous variables. Covariate adjustment with demographic and clinical variables was performed by ANOVA test. Study received local ethics committee approval “CEIC” (No. 2019/8398/I).
ResultsFrom a total of 198 patients, 99 (50%) were immigrants and 99 (50%) locals. Immigrants were exposed on average 3 times more to lifetime traumatic events (16.12) when compared to locals (5.39). Likewise, distress intensity caused by trauma exposure had a mean of 97.13 in immigrants compared to 27.24 in locals. Traumatic events more present in immigrants’ group were “uprooting” (82.8%), “physical abuse” (76.8%), racial discrimination (74.7%), threat of death (74.7%) and life-threatening to close friend (72.2%) and in local group was school failure (42.4%), serious disease (38.4%), accidents (36.4%), physical abuse (36.4%) and interpersonal relationship rejection (36.4%).
ConclusionsAccording to our results there are important differences in cumulative traumatic events between immigrants and locals with psychotic disorder. Immigrants showed three times more lifetime traumatic events than locals. Likewise, immigrants presented significant higher level of distress caused by lifetime trauma and the nature of traumatic events was more severe. These results should be considered in order to offer better assessment and treatment to this population considering this comorbidity.
Disclosure of InterestNone Declared
Effect of aripiprazole once-monthly 400mg (AOM400) on hospitalisation prevention and use of healthcare resources in schizophrenia patients, a study based on real clinical practice on schizophrenia: AMBITION Study
- V. Sanchez-Gistau, M. J. Moreno, S. Gómez-Lus, A. Sicras Mainar, B. Crespo-Facorro
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S494
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a large and increasing burden for patients from early stages of the disease. Long-acting injectable antipsychotics (LAIs), like aripiprazole once-monthly 400 mg (AOM400), have demonstrated an improvement in treatment adherence compared to oral formulations, with a consequent reduction in time to remission and risk of relapse.
ObjectivesThis study aims to compare the hospitalisation rate in individuals with schizophrenia who started their treatment with AOM400 or atypical oral antipsychotics (OA) in a real-world setting in Spain.
MethodsThis is an observational and retrospective study based on the electronic medical records of the BIG-PAC database. Adults diagnosed with schizophrenia who initiated treatment with AOM400 or atypical OA (olanzapine, risperidone, paliperidone, aripiprazole or asenapine) from 01/01/2017 to 31/12/2019 were included. A 1:1 propensity score matching (PSM) was conducted to match individuals from both cohorts. Healthcare resource use and treatment persistence (with AOM400 or OA) were also analysed after 12 months.
ResultsAfter the PSM, 1,017 individuals with similar baseline characteristics were included in each cohort (total population: 2,024 individuals). At index date (treatment initiation) patients were 41.4 years (standard deviation, SD: 10.6), 54.6% were male and had received 1.6 (SD: 0.9) previous antipsychotic treatments. During the follow-up period, the AOM400 cohort had a 40% lower risk of hospitalisation than the OA cohort (hazard ratio, HR: 0.60 [95% confidence interval, CI: 0.49 – 0.74]). The median time to the first hospitalisation was longer in individuals with AOM400 compared to those with OA (197 compared to 174 days; p<0.004), whereas median length of hospital stay were shorter (6 and 11 days for AOM400 and OA, respectively; p<0.001). The AOM400 cohort also required fewer visits to primary care, specialized care and emergency rooms than the OA cohort (p≤0.005). After 12 months, the AOM cohort was more persistent than the OA cohort (64.9% compared to 53.7%; p<0.001).
ConclusionsAOM400 reduces the number and duration of hospitalisations and improves treatment persistence compared to atypical OA. Our results suggest that the use of AOM400 may reduce the burden of schizophrenia in Spain.
Disclosure of InterestNone Declared
Smoking treatments for patients with mental illness: case presentation and a brief literature review
- F. Garcia Sanchez, M. Gutierrez Rodriguez, C. Moreno Menguiano, M. A. Corral Alonso, J. J. Vazquez Vazquez, S. M. Bañon Gonzalez, V. Voces Domingo, J. A. Casado de la Hera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S756
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Smoking prevalence in patients with mental illness ranges between two to 4 times higher than general population. This higher prevalence has a multifactorial origin, and some of the possible causes are still unknown.
They have a higher prevalence of tobacco-associated diseases and higher mortality.
Additionally, these patients have greater difficulty in treating and quitting smoking.
A relationship has been found between severity of mental illness and smoking. Risk of suicide seems to be higher in patients with higher tobacco consumption. Schizophrenia is the mental illness that has been most closely related to smoking, with a prevalence close to 90%.
ObjectivesThe aim of this work is reviewing the current bibliography referring to smoking treatments for patients with mental illness
MethodsA literature search using electronic manuscripts available in PubMed database published during the last ten years and further description and discussion of a single-patient clinical case
ResultsThe treatment of tobacco dependence in patients with mental illnesses is sometimes waited until there is psychiatric stability, which can take a long time in those cases with more severe mental disorders, which can have negative physical and psychiatric consequences.
The combined treatment of cognitive behavioral therapy and pharmacological treatment is the most effective approach. Nicotine replacement therapy can be useful, while combined use of antidepressants or anxiolytics is also recommended.
Bupropion has shown efficacy. In patients with schizophrenia it does not seem to worsen positive symptomatology, but improving the negative one. It should not be used in patients with bipolar disorder or bulimia.
Varenicline has shown efficacy in the general population, but limitations were established in patients with mental illness, although it is the drug that has shown greater efficacy. However, is not currently available in our country.
Cytisine is a drug with limited number of studies in the psychiatric population but it may be a reasonable treatment alternative.
ConclusionsThe prevalence of tobacco use in patients with mental illness is higher than the general population, especially in paranoid schizophrenia. The consequences on physical health and the evolution of psychiatric illness are very relevant. Based on above, a multidisciplinary and coordinated management involving psychiatrists and other specialists in the treatment of these patients should be desirable.
Disclosure of InterestNone Declared
Impact of COVID-19 pandemic on psychiatric emergency care in a general hospital
- J. M. Rodríguez Capilla, A. Rubio Carramiñana, S. Vega Castellote, S. López Fernández, I. Arilla Herrera, J. M. Almenara Galdeano, A. Mora Prat, M. Campillo Benito, J. Albero Garcia, A. Valderrey Ratia, A. Grau Peñas, C. Pastor Fernández, M. Moreno Monzó, J. Guitart Gil, J. Martínez Raga, C. Knecht
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S405-S406
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The SARS-CoV-2 pandemic has produced an unprecedented clinical situation, causing a direct and indirect impact on the physical and mental health of the population. In Spain, between March 15 and June 21 of 2020, it was decreed a home confinement that caused the interruption of the daily life of millions of people. However, there are few studies that analyze the changes produced in psychiatric care in the Emergency Department (ED).
ObjectivesTo analyze the changes produced in psychiatric emergencies, subanalysing paediatric population, during the first year of the pandemic (COV1/Y-COV1) compared to the previous year (NOCOV/Y-NOCOV1). To analyze the clinical features of patients attended during the lockdown period of the pandemic (LOCK) and compare it to the period of the pandemic after the lockdown (NOLOCK).
MethodsThrough the registry of computerized medical records, patients who attended the psychiatric hospital emergency department between 03/01/2019 and 02/28/2021 were identified. We also identified all attendances from 15/03 to 21/06 in 2019 and in 2020 to obtain variables from the lockdown period.
ResultsDuring period of this study, 2694 psychiatric visits made in the ED (1744 patients - 54.3% women, and 69.5% were between 25 and 64 years-), 1537 in NOCOV and 1157 in COV1. Significant differences were found between COV1 and NOCOV in sociodemographic variables, such as employment status and number of offspring. At a clinical level, in COV1, we observed an increase in attendance due to heteroaggressive behaviors, mania, insomnia and problems due to substance use. An increase in the prescription and/or modification of treatment was observed (59.3% vs 54.3%). During COV1, in terms of discharge follow-up in the month following the ED visit, telematic assistance increased (11.4% vs. 5.3%). During the period of study, 282 ED attendances were performed, 153 in Y-NOCOV and 129 in Y-COV1. At a clinical level, during Y-COV1, a decrease in attendances related to substance use was found significant. The sub-analysis carried out for LOCK and NOLOCK yields similar data to those obtained in the COV1 vs. NOCOV1 comparison. During lockdown, the face-to-face follow-up in the month following the ED was significantly lower (39,5% vs 57,1%) regarding telematic follow-up (24,4% vs 5,8%) In this period, an increase of adolescents without previous mental health follow-up was observed (44% LOCK vs. 22% NOLOCK).
ConclusionsOur work supports the hypothesis that the COVID-19 pandemic caused a change in psychiatric care in the ED. It also shows how lockdown changed the attendance in psychiatric emergencies, and also in the later community care attendance. Changes are detected in emergency care for adolescents during the pandemic compared to the previous year. Strikingly, our study does not reflect a quantitative increase in the demand. It would be of interest to continue collecting data after the time of the present project.
Disclosure of InterestNone Declared
Syndrome of inappropiate antidiuretic hormone secretion (SIADH) secondary to sertraline: case report and literature review
- C. Cardenes-Moreno, S. Yelmo-Cruz, I. Perez-Sagaseta, J. J. Tascon-Cervera, J. Dorta-Gonzalez, A. Crisostomo-Siverio, L. Torres-Tejera, M. Paniagua-Gonzalez, S. Canessa, M. R. Cejas-Mendez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S556
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Currently, in addition to their frequent use in community medicine, the use of antidepressants is a fundamental pillar of pharmacological treatments used in psychiatry. Due to this frequent use, we must be aware of the possible side effects, in particular the SIADH produced in this clinical case by SSRIs. There are already described cases of this association including other antidepressants and many different types of drugs.
ObjectivesTo review the current literature on the management of this pathology when it is secondary to the use of frequently used drugs such as SSRIs.
MethodsWe report the case of a 64-year-old woman hospitalised in the psychiatric department for malnutrition secondary to unspecified eating disorder (ED). During admission, treatment with sertraline was started with ascending doses up to 100mg, subsequently producing slight edema with the following analytical results: plasma Na: 123 mEq/L (135-145), plasma osmolarity: 250 mOsm/kg (275-300), urinary Na: 174 mEq/L (>40), fulfilling diagnostic criteria for SIADH.
Afterwards, we reduced sertraline until discontinuation and started treatment with water restriction and urea (30 grams/24 hours) during admission and after discharge. During admission, we observed disappearance of the edema and partial improvement of the analytical values (Na:131 mEq/L), which were normalised with home treatment of daily urea.
ResultsThe precise prevalence of SIADH from the use of SSRIs is unknown, it is known that patients older than 65 are at higher risk of developing severe hyponatraemia in the first 5 weeks after initiation. Similarly, treatment with water and urea restriction, together with discontinuation of SSRIs, appears to be sufficient.
ConclusionsSSRIs can cause SIADH a reversible but potentially life-threatening pathology, and we need to be aware of this possibility especially in the older population and being able to handle it
Disclosure of InterestNone Declared
Fahr’s Disease: a case report of a patient with neuropsychiatric symptoms
- I. Perez-Sagaseta, S. Yelmo-Cruz, C. Cardenes-Moreno, L. Torres-Tejera, A. Crisostomo-Siverio, J. Dorta-Gonzalez, J. J. Tascon-Cervera, M. Paniagua-Gonzalez, S. Canessa, M. R. Cejas-Mendez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S769-S770
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Fahr’s disease (FD) is a rare disorder consisting of bilateral and symmetrical calcium deposits in basal ganglia and cerebral cortex. These lesions are associated with neurological and psychiatric symptoms such as a rigid hypokinetic syndrome, mood disorders and memory and concentration abnormalities. It can be idiopathic or secondary to endocrine disorders, infectious diseases or mitochondrial myopathies.
ObjectivesTo highlight the importance of considering organic causes when evaluating patients presenting atypical psychiatric symptoms and claim the role of neuroimaging.
MethodsCase report and non-systematic review of literature: sources obtained from Pubmed database.
ResultsA 69-year-old man, native of Syracuse (Italy), was admitted to the Psychiatry Unit in February 2022 presenting behavioural disturbances and irritability. In July 2021 he presented the same symptoms, being mistakenly diagnosed with Bipolar Disease type I. He has no previous psychiatric history. He started with changes in his personality, short-term memory loss, aggressiveness and disorganized behaviour at the age of 66. At admission he was talkative and hyperfamiliar, presenting delusions of grandiosity, exalted affectivity and insomnia. Neurological examination showed short-term memory problems, signs of frontal disinhibition and abnormal glabellar tap sign. Blood tests, CT brain and MRI were performed to rule out organic underlying causes. Neuro-imaging found bilateral and symmetric calcifications in globus pallidus, thalamus and corpus striatum, in favour of FD. Secondary causes (abnormalities in the PTH, vitamin disorders and infectious diseases such as HIV, brucellosis or neurosyphilis) where discarded, allowing us to conclude it was probably a primary case of FD. Valproate was started as a mood stabilizer and anticonvulsant. Genetic tests were indicated.
ConclusionsFD should be considered as a differential diagnosis in the evaluation of psychiatric symptoms, especially when atypical and/or presented with neurological symptoms. The role of neuro-imaging is essential.
Disclosure of InterestNone Declared
Visual hallucinations and age-related macular degeneration: case presentation and a brief literature review
- M. M. Gutiérrez Rodríguez, F. García Sánchez, M. Á. Corral Alonso, J. J. Vázquez Vázquez, C. Moreno Menguiano
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S936-S937
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
age-related macular degeneration (AMD) is an ocular disease involving central vision. It is one of the mainreasons of vision loss in people over 50. Seeing non-existing faces or shapes are described in AMD. Symtoms of visualhallucinations that occur as a result of vision loss is known as Charles Bonnet syndrome (CBS). These patients haveintact cognition, do not have hallucinations in any other sensory modalities, and retain insight into the unreal nature oftheir hallucinations.
Objectivesthe aim of this work is analizing ethiology, demographic characteristics, clinica features and treatment inpatients with AMD and visual hallucinations
Methodsa literature search using electronic manuscripts available in PubMed database published during the last ten years with further description and discussion of a single-patient clinical case.
Resultsin different studies in patients diagnosed with AMD, the reported prevalence ranges between 15 up to 39percent. Patients with more significant vision loss may be more likely to experience visual hallucinations. In large caseseries, mean age is 70 to 85 years. Hallucinations can last few minutes or several hours. On average, people experiencethese hallucinations on and off for about 3 years. Those who experience hallucinations tend to see multiple types ofimages, particularly people and faces.The diagnosis of CBS is made when visual hallucinations occur in patients withvision loss in the absence of psychosis, delirium, or other causes.
There is no specific treatment for CBS: optimal ocular care, education and differents techniques to manage hallucinations(changing your lighting conditions and environment, blinking frequently or moving your eyes side-to-side rapidly whilekeeping your head still…). Antidepressants, anticonvulsants, anxiolytics and low-dose of antipsychotics have been used for CBS with positiveeffects in previous reports, but the efficacy of these drugs in the treatment is somewhat questionable and should bereserved for those who exhibit high levels of distress and have not responded to conventional intervention.
Case report: 80-years old woman who presented with a 4 month history of hallucinations and legally blind from AMD. Aworkup for other pathological causes of visual hallucinations was negative.
ConclusionsCBS is an under-recognized and under-reported disorder that involves visual hallucinations in visuallyimpaired individuals. It requires a multidisciplinary approach from neurologists, psychiatrists, general practitioners andophthalmologists. New studies are needed in order to understand its clinical presentation and to improve its management.
Disclosure of InterestNone Declared
Clinician’s attitude towards clozapine prescription
- O. Brugue, M. Gonzalez, L. Moreno, C. Ivorra, R. Hernandez, S. Cepedello, J. Labad
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1013
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Current clinical guidelines recommend the use of clozapine for the treatment of refractory schizophrenia, present in up to a third of patients with this disease. Despite the evidence, the data point to low prescription, underdosing, and delayed initiation.
ObjectivesThe objective of the study is to elucidate which factors may interfere in clozpine prescription.
MethodsThis is a cross-sectional observational study, carried out using a survey designed specifically for it.
It was answered online by seventy psychiatrists affiliated with the Catalan Society of Psychiatry.
ResultsMore than half admitted having prescribed two or more antipsychotics without having previously ruled out pseudorefractoriness through depot treatment. 70% recognized the need for monitoring as the main prescription barrier, while the main reason for withdrawal was its adverse effects. The most alarming was considered agranulocytosis, with drooling, drowsiness and weight gain being the most reported.
Statistically significant differences (p=0.031) were found in relation to the years of experience and the device where clozapine was preferred to be started: <10 years in hospital, 10-20 years in partial hospitalization and >20 years outpatient office.
Statistically significant differences were observed in the preference of the device for its initiation depending on the usual work device: hospitalization (p<0.000) and partial hospitalization (p=0.046) preferred to schedule it from their respective devices, without any preference in consultations.
The level of experience and the most reported side effect were statistically significant: for the newest psychiatrists it was weight gain (p=0.031), without presenting differences in the rest of the groups.
ConclusionsClozapine is the psychoactive drug of choice in refractory schizophrenia, so efforts should be devoted to reducing prescription barriers, offering training on its management and innovating forms of monitoring to promote its use.
Disclosure of InterestNone Declared
Psychological trauma as a transdiagnostic risk factor for mental disorder: an umbrella meta‐analysis
- B. M. Hogg, I. Gardoki-Souto, A. Valiente-Gómez, A. Ribeiro Rosa, L. Fortea, J. Radua, B. L. Amann, A. Moreno-Alcázar
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S982-S983
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
This umbrella review is the frst to systematically examine psychological trauma as a transdiagnostic risk factor across psychiatric conditions.
ObjectivesThis review aimed to be the frst to evaluate whether psychological trauma fulflilled criteria as a transdiagnostic risk factor cutting across various diagnostic categories and spectra. Transdiagnosticity will be assessed against the framework of the TRANSD criteria (Fusar-Poli, World Psychiatry 2019; 18 361-362). The paper additionally aimed to analyse the association of psychopathology with specifc trauma type.
MethodsWe searched Pubmed, Scopus, and PsycNET databases from inception until 01/05/2021 for systematic reviews/meta-analyses evaluating the association between psychological trauma and at least one diagnosed mental disorder. We re-calculated the odds ratio (OR), then classifed the association as convincing, highly suggestive, suggestive, or weak, based on the number of cases and controls with and without psychological trauma, random-efects p value, the 95% conf- dence interval of the largest study, heterogeneity between studies, 95% prediction interval, small-study efect, and excess significance bias. Additional outcomes were the association between specifc trauma types and specific mental disorders, and a sensitivity analysis for childhood trauma. Transdiagnosticity was assessed using TRANSD criteria. The review was pre-registered in Prospero CRD42020157308 and followed PRISMA/MOOSE guidelines.
ResultsFourteen reviews met inclusion criteria, comprising 16,277 cases and 77,586 controls. Psychological trauma met TRANSD criteria as a transdiagnostic factor across diferent diagnostic criteria and spectra. There was highly suggestive evidence of an association between psychological trauma at any time-point and any mental disorder (OR=2.92) and between childhood trauma and any mental disorder
(OR=2.90). Regarding specifc trauma types, convincing evidence linked physical abuse (OR=2.36) and highly suggestive evidence linked sexual abuse (OR=3.47) with a range of mental disorders, and convincing evidence linked emotional abuse to anxiety disorders (OR=3.05); there were no data for emotional abuse with other disorders.
Image:
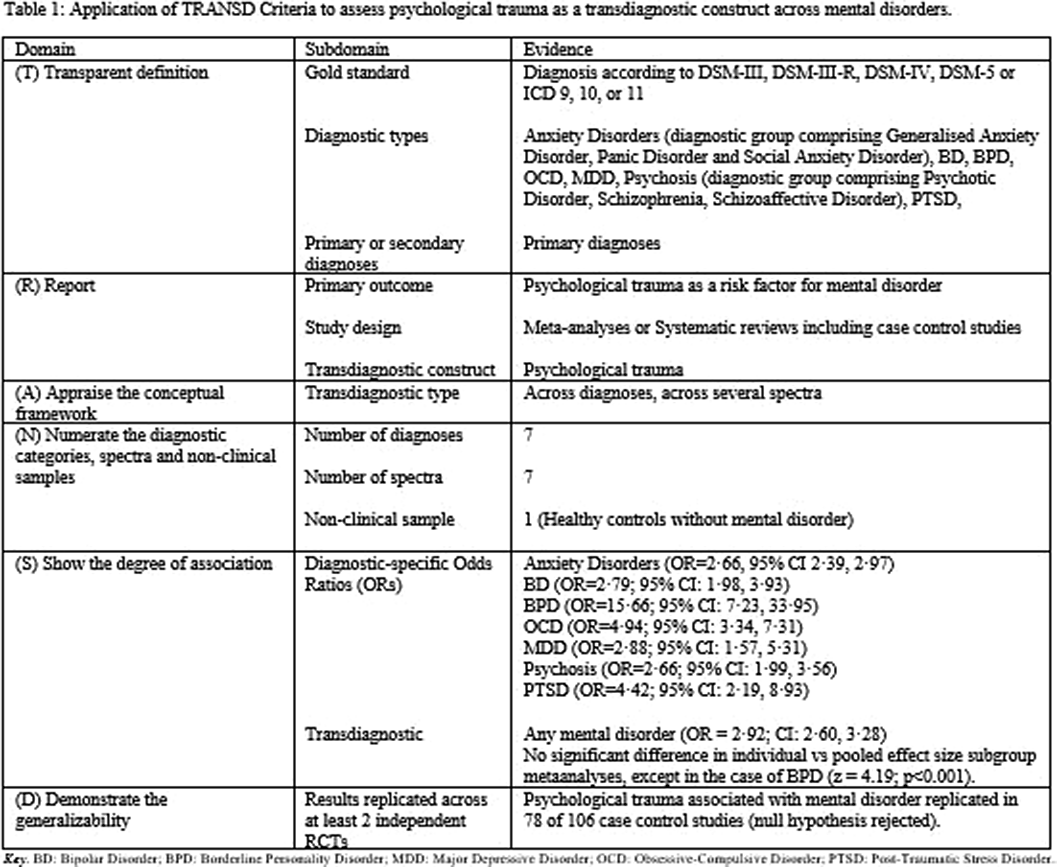
Image 2:
 Conclusions
ConclusionsThese fndings highlight the importance of preventing early traumatic events and providing trauma-informed care in early intervention and psychiatric services.
Disclosure of InterestNone Declared
Anorexia nervosa and Wernicke-Korsakoff syndrome: case report an literature review
- S. Yelmo-Cruz, J. J. Tascon-Cervera, I. Perez-Sagaseta, C. Cardenes-Moreno, L. Torres-Tejera, A. Crisostomo-Siverio, E. Diaz-Mesa, J. Dorta-Gonzalez, M. Paniagua-Gonzalez, S. Canessa, A. L. Morera-Fumero, M. R. Cejas-Mendez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S424
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Wenicke-Korsakoff syndrome (WKS) is a neurological disorder caused by thiamine deficiency. Wernicke Encephalopathy (WE) is the acute phase and the chronic phase is called Korsakoff-syndrome (KS).
ObjectivesTo review the current literature on the management of WKS in a patient with anorexia nervosa.
MethodsWe report the case of a 63-year-old woman admitted to the Psychiatry Unit after weight loss in the last 3 months (from 39 kg to 33,500 kg). She only made one meal a day. By exploration and analysis, neoplastic disease is ruled out (thoraco-abdomino-pelvic CT without pathological findings). She has maintained restrictive intakes for more than 30 years. A long-term anorexia nervosa (AN) is suspected, with a worsening of restrictive behavior in recent months. Upon admission, she has a weight of 33,500 kg and a BMI of 14,10. She has a left palpebral ptosis and an alteration of the anterograde memory as well as affectation of executive functions. Progressive oral diet is started, and due to the suspicion of a WKS, thiamine ev is started for a week and then continued with oral thiamine. Thiamine levels are extracted once the ev treatment has begun, so we do not have previous levels to know if they were decreased. Brain MRI shows bilateral hyperintensities in white matter and at supratentorial level in T2 and FLAIR. After a month and a half of admission, the patient has progressively regained weight, has managed to make adequate intakes and has improvement in memory.
ResultsAn adverse consequence of severe malnutrition in AN due to severe food restriction and purging behavior is thiamine deficiency, and also global cerebral atrophy and concomitant cognitive deficits can be found. Thiamine deficiency occurs in 38% of individuals with AN and is often unrecognized. WKS is caused by thiamine deficiency, and WE is the acute phase of this syndrome (presentation of triad can vary). The chronic phase is KS and consists in amnesia with confabulations. WKS typically develops after malnourishment in alcoholic patients but can be associated in nonalcoholic such as prolonged intravenous feeding, hyperemesis, anorexia nervosa, refeeding after starvation, thyrotoxicosis, malabsorption syndromes; hemodialysis; peritoneal dialysis; AIDS; malignancy. WKS is a clinical diagnosis, and no specific abnormalities have been found in cerebrospinal fluid, brain imaging or electroencephalograms. MRI has a sensitivity of 53%, but high specificity of 93%, and shows an increased signal in T2 and FLAIR sequences, bilaterally symmetrical in the paraventricular regions of the thalamus, the hypothalamus, mamillary bodies, the periaquedutal region, the floor of the fourth ventricle and midline cerebellum.
ConclusionsIf the disorder is suspected, thiamine should be initiated immediately in order to prevent irreversible brain damage, with an estimated mortality rate of about 20%, or to the chronic form of the WE in up to 85% of survivors
Disclosure of InterestNone Declared
Effect of polygenic risk score, family load of schizophrenia and exposome risk score, and their interactions, on the long-term outcome of first-episode psychosis
- M. J. Cuesta, S. Papiol, B. Ibañez, E. García de Jalón, A. M. Sánchez-Torres, G. J. Gil-Berrozpe, L. Moreno-Izco, A. Zarzuela, L. Fañanás, V. Peralta, SEGPEPs Group
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 14 / October 2023
- Published online by Cambridge University Press:
- 06 March 2023, pp. 6838-6847
-
- Article
- Export citation
-
Background
Consistent evidence supports the involvement of genetic and environmental factors, and their interactions, in the etiology of psychosis. First-episode psychosis (FEP) comprises a group of disorders that show great clinical and long-term outcome heterogeneity, and the extent to which genetic, familial and environmental factors account for predicting the long-term outcome in FEP patients remains scarcely known.
MethodsThe SEGPEPs is an inception cohort study of 243 first-admission patients with FEP who were followed-up for a mean of 20.9 years. FEP patients were thoroughly evaluated by standardized instruments, with 164 patients providing DNA. Aggregate scores estimated in large populations for polygenic risk score (PRS-Sz), exposome risk score (ERS-Sz) and familial load score for schizophrenia (FLS-Sz) were ascertained. Long-term functioning was assessed by means of the Social and Occupational Functioning Assessment Scale (SOFAS). The relative excess risk due to interaction (RERI) was used as a standard method to estimate the effect of interaction of risk factors.
ResultsOur results showed that a high FLS-Sz gave greater explanatory capacity for long-term outcome, followed by the ERS-Sz and then the PRS-Sz. The PRS-Sz did not discriminate significantly between recovered and non-recovered FEP patients in the long term. No significant interaction between the PRS-Sz, ERS-Sz or FLS-Sz regarding the long-term functioning of FEP patients was found.
ConclusionsOur results support an additive model of familial antecedents of schizophrenia, environmental risk factors and polygenic risk factors as contributors to a poor long-term functional outcome for FEP patients.
Significant early and long-term improvement of neuropsychiatry symptomatology in HCV-infected patients after viral eradication with DAA
- R. Martin-Santos, C. Bartrés, L. Nacar, R. Navinés, M. Cavero, S. Lens, S. Rodriguez-Tajes, J.C. Pariante, I. Horrillo, E. Muñoz-Moreno, N. Bargallo, L. Capuron, J. Meana, X. Forns, Z. Mariño
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S238-S239
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Chronic Hepatitis C infection is considered a systemic disease with extrahepatic manifestations, mainly neuropsychiatric symptoms, which is associated with a chronic low-grade inflammatory state. Hepatitis C virus (HCV) eradication is currently achieved in >98% of cases with oral direct-acting antivirals (DAA).
ObjectivesTo study potential clinical neuropsychiatric changes (mood, cognition, sleep, gastrointestinal, sickness, and motion) in HCV-infected patients after HCV eradication with DAA.
MethodsDesign: Cohort study. Subjects: 37 HCV-infected patients, aged<55 years old, with non-advanced liver disease receiving DAA; free of current mental disorder. 24 healthy controls were included at baseline. Assessment: -Baseline (BL) (socio-demographic and clinical variables, MINI-DSM-IV, and Neurotoxicity Scale (NRS), (mood, cognitive, sleep, gastrointestinal, sickness and motor dimensions). Follow-up: End-of-treatment, 12weeks-after and 48weeks-after DAA: NRS. Analysis: Descriptive and bivariate non-parametrical analysis.
ResultsNRS total score and dimensions where different between cases and controls (.000) at baseline. NRS total score (.000) and mood (.000), cognition (.000), sleep (.002), gastrointestinal (.017), and sickness (.003), except motor dimension score (.130) showed significant longitudinal improvement.
ConclusionsHCV-infected patients with mild liver disease presented significantly worse scores for neurotoxicity symptomatology in all dimensions compared to healthy individuals. After HCV eradication with DAA, both at short and long follow-up a significant improvement of the NRS total score and each of the dimensions (except motor) were observed. However, they did not reach the values of healthy individuals, suggesting a not complete neuropsychiatric restoration in the period studied. Grant: ICIII-FIS:PI17/02297.(One way to make Europe) (RMS) and Gilead Fellowship-GLD17/00273 (ZM); and the support of SGR17/1798 (RMS)
DisclosureNo significant relationships.
Synthetic cathinone (α-pyrrolidinohexanophenone): an emerging threat
- V. Rosello-Molina, A. Hervas Aparisi, M. Simon Blanes, J. Tejera Nuñez, E. Moreno Soldado, I. Meri Abad, O. Sparano Ros, C. Ribera, M. Esteban, T. De Vicente Muñoz
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S470
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Alpha-pyrrolidinohexanophenone (α-PHP) is a synthetic cathinone with uneven distribution throughout the world. Its use is not uniformly regulated and its distribution is legal in some European countries. Easily accessible and available through different websites. Synthetic cathinones inhibit monoamine transporters which include dopamine, norepinephrine, and serotonin, resulting in increased neurotransmitter synaptic concentration. Ways of administration show wide range regarding latency period. Onset and appearance of symptoms as well as their duration and intensity may fluctuate. A decreasing order of latency (oral, inhaled, sublingual and intravenous) has been reported. α-PHP can result in the appearance of psychiatric symptoms, include among others, intoxication with sensory perception disturbances and α-PHP -induced psychotic episodes.
ObjectivesThe aim of our study was to assess the epidemiology, clinical and legal features regarding Alpha-pyrrolidinohexanophenone (α-PHP).
MethodsReview the current bibliography to upgrade the existing knowledge. -Present assorted cases with diverse clinical features. All cases include variability through psychopathological interview, symptoms assessment and treatment response according to rating scales (PANSS, YMRS). -Evaluate different treatment administration ways during acute phase and after hospital discharge.
ResultsDifferences were observed after hospitalization in the response using diverse rating scales. We used antipsychotics to treat intoxication with sensory perception disturbances and α-PHP -induced psychotic episodes. α-PHP had a negative impact on the quality of life of the patients.
Conclusionsα-PHP is a synthetic cathinone with potential risk to mental health and life of users. It is mandatory to implement common legislation all through the European Union to prevent its use and possible implications on population’s mental health.
DisclosureNo significant relationships.
Alcohol-induced psychotic disorder: a study of hospitalized patients in Lisbon
- V. Nogueira, I. Pereira, M. Moreno, J. Teixeira
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S119-S120
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
While alcohol-induced psychotic disorder (AIPD) is a well-recognised clinical disorder, relativery little is known about aspects such as epidemiology, course and treatment of the condition. Current evidence suggests AIPD can be clinically distinguised from alcohol-withdrawal delirium and schizophrenia. AIPD is associated with high comorbidity with other psychiatric disorders, high re-hospitalization and mortality rate, namely suicidal behaviour.
ObjectivesThe objetive of the study was to examine the correlates, clinical features, psycopathology, and short-term response in an inpatient sample with alcohol-induced psychotic disorder, predominant hallucinations (ICD-10 F10.52) admitted to Centro Hospitalar Psiquiátrico de Lisboa.
MethodsWe collected retrospectively data from all admitted patients to our Alcohol Unit between January 2010 and January 2020 with the diagnosis of AIPD. The exclusion criteria were: presence of preexisting psychotic disorder, delirium, or other substance use disorders. We characterized our sample in Demographic categories, Clinical categories, Treatment and Short-term course.
ResultsA total of 113 subjects were included in the study. The prevalance of alcoholic hallucinosis was found to be 1.3% of all patients who received inpatient treatment. Most individuals reported auditory hallucinations, that iniciated when they decrease their alcohol intake, and 1 in 4 had past episodes of AIPD.
ConclusionsThere are specific challenges in studiyng AIPD, such as the relatively rarity of the disorder, its often transient nature and high levels of comorbidity. A high degree of recurrence and morbidity indicates a need to prevent, and intervene early with an abstinent-oriented management goal.
DisclosureNo significant relationships.
That song in my head: a review on Musical Hallucinations
- F. Ramalheira, M. Conde Moreno, J. Romão, S. Vieira
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S708-S709
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hearing music inside our heads is frequent, however some hear it more vividly, constantly and involuntarily. Musical Hallucinations (MH), first described by Baillarger in 1846, are a complex type of auditory hallucination characterized by perception of melodies, music, or songs.
ObjectivesThis work aims to review the literature considering MH.
MethodsPubmed and Google Scholar search using MeSH term “musical hallucinations”
ResultsMH occurs in 0.16% of the population. They´re usually perceived as frightening or annoying. Proposed mechanisms include spontaneous activity triggered by sensory deprivation from hearing impairment, like in visual hallucinations in Charles Bonnet syndrome, and some authors even include MH as a subtype of this syndrome. Indeed, 60% of all patients with MH have hearing impairment or deafness. Other less frequent causes include focal brain lesions involving the auditory pathway and cortex, temporal epilepsy, metabolic or drug intoxication. Psychiatric conditions are uncommon but not impossible, especially in affective disorders. MH most frequently consist in familiar tunes, sometimes of personal significance, religious songs (especially in older patients), childhood songs, folk and popular songs from the radio - suggesting that musical perception is never unlearned but represents a “parasitic memory”, an unchangeable memory feature which can be experienced by relevant neuronal circuit stimulation. Most patients with MH were reported to have no extraordinary musical skills.
ConclusionsMH are rare and strongly associated with hearing loss, though investigation of other causes should be sought. Treating the underlying cause is important but remission is not guaranteed.
DisclosureNo significant relationships.






