14 results
Three-day antibiotic duration in patients with pneumonia: A sixty-eight–hospital cohort
- Valerie Vaughn, Lindsay Petty, David Ratz, Elizabeth McLaughlin, Tawny Czilok, Jennifer Horowitz, Anurag Malani, Danielle Osterholzer, Scott Flanders, Tejal Gandhi
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, p. s22
-
- Article
-
- You have access Access
- Open access
- Export citation
-
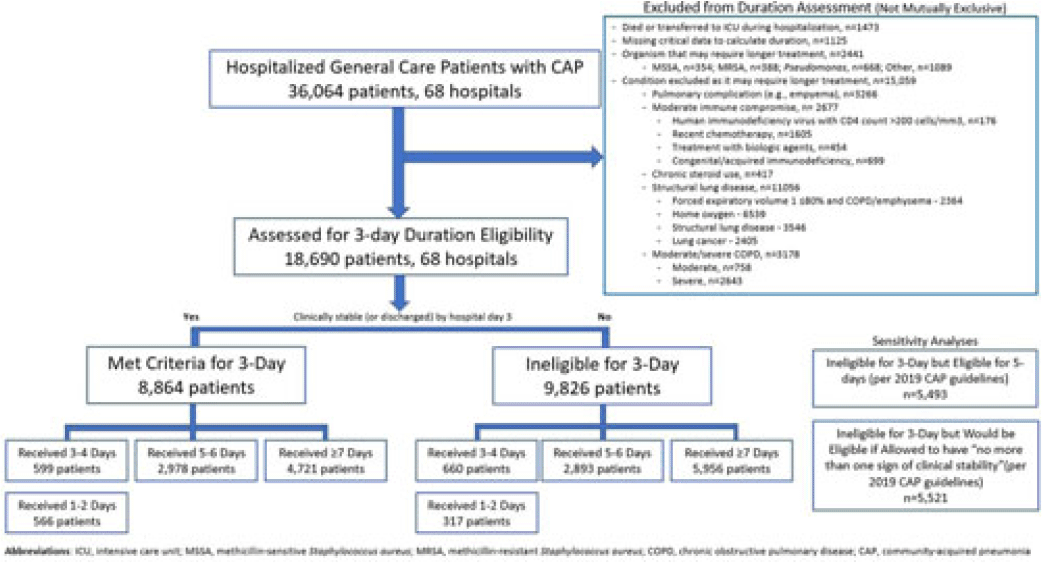
Background: Since 2019, community-acquired pneumonia (CAP) guidelines have recommended hospitalized patients be treated until clinical “stability and for no less than 5 days.” However, randomized trials have reported that, in patients who stabilize by hospital day 3, very short antibiotic durations (eg, 3 days) are noninferior to longer durations. How these trial results relate to real-world practice is unknown. Methods: Using a 68-hospital cohort study of hospitalized, general-care adults with CAP, we aimed to (1) quantify the percentage of patients who—according to trial criteria—qualify for a 3-day antibiotic duration, (2) quantify the percentage who actually received a 3-day duration, and (3) assess 30-day outcomes. Patients were considered to have CAP if they had a pneumonia discharge diagnosis and met clinical criteria for CAP. Patients with concomitant infections (including COVID-19), admission to intensive care, or severe immunocompromise were not included. Results: Between February 23, 2017, and August 3, 2022, 36,064 patients with CAP were included. Of those, 48.2% (9,826 of 36,064) were excluded due to a condition or organism ineligible for the 3-day treatment (Fig. 1). Of the 18,690 patients remaining, 52.6% (9,826) were unstable on day 3 and thus were ineligible for the 3-day treatment. Therefore, of all 36,064 patients, only 8,864 (24.6%) would be eligible under trial criteria for a 3-day treatment. Notably, 5,493 (55.9%) of 9,826 patients unstable on day 3 would be eligible for 5 days of treatment under national guidelines. In practice, use of 3–4-day treatment was rare, occurring in 599 (6.8%) of 8,864 patients eligible for a 3-day treatment versus 660 (6.7%) of 9,826 patients unstable on day 3 (P = .945). Use of 3–4-day treatment increased over time and comorbidities that could mimic CAP or a negative procalcitonin were more common in patients who received a 3–4-day treatment whereas specific symptoms of CAP were less common (Fig. 2). After adjustments, patients eligible for a 3-day duration who received a 3–4 day treatment versus a ≥5-day treatment had higher 30-day mortality (aOR, 1.87; 95% CI, 1.32–2.64) and readmission (aOR, 1.35; 95% CI, 1.17–1.56). Conclusions: Across 68 hospitals, <25% of patients hospitalized with CAP would be eligible for a 3-day antibiotic treatment. Though increasing over time, there was little use of 3–4-day treatments and, when prescribed, outcomes were worse, potentially due to CAP misdiagnosis. Given the small number of patients eligible for 3-day treatment, and the potential harm with too-short durations, it may be prudent to focus on increasing the use of 5-day treatments.
Disclosures: None
Risk Factors and outcomes associated with inappropriate empiric broad-spectrum antibiotic use in hospitalized patients with community-acquired pneumonia
- Tejal Gandhi, Lindsay Petty, Valerie Vaughn, Anurag Malani, David Ratz, Tawny Czilok, Jennifer Horowitz, Elizabeth McLaughlin, Lisa Dumkow, Stephanie Burdick, Danielle Osterholzer, Mariam Younas, Steven Bernstein, Scott Flanders
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s31-s32
-
- Article
-
- You have access Access
- Open access
- Export citation
-
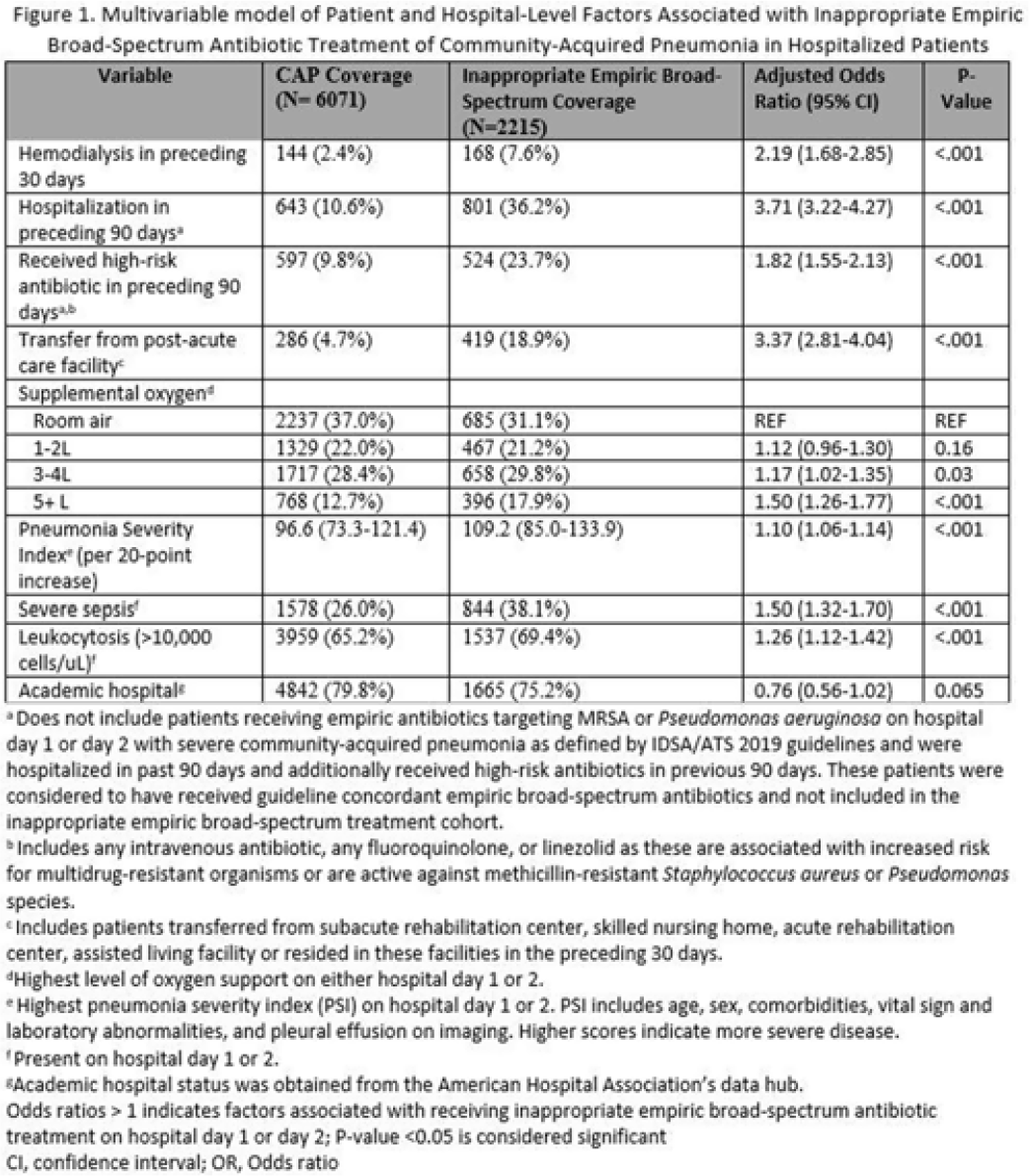
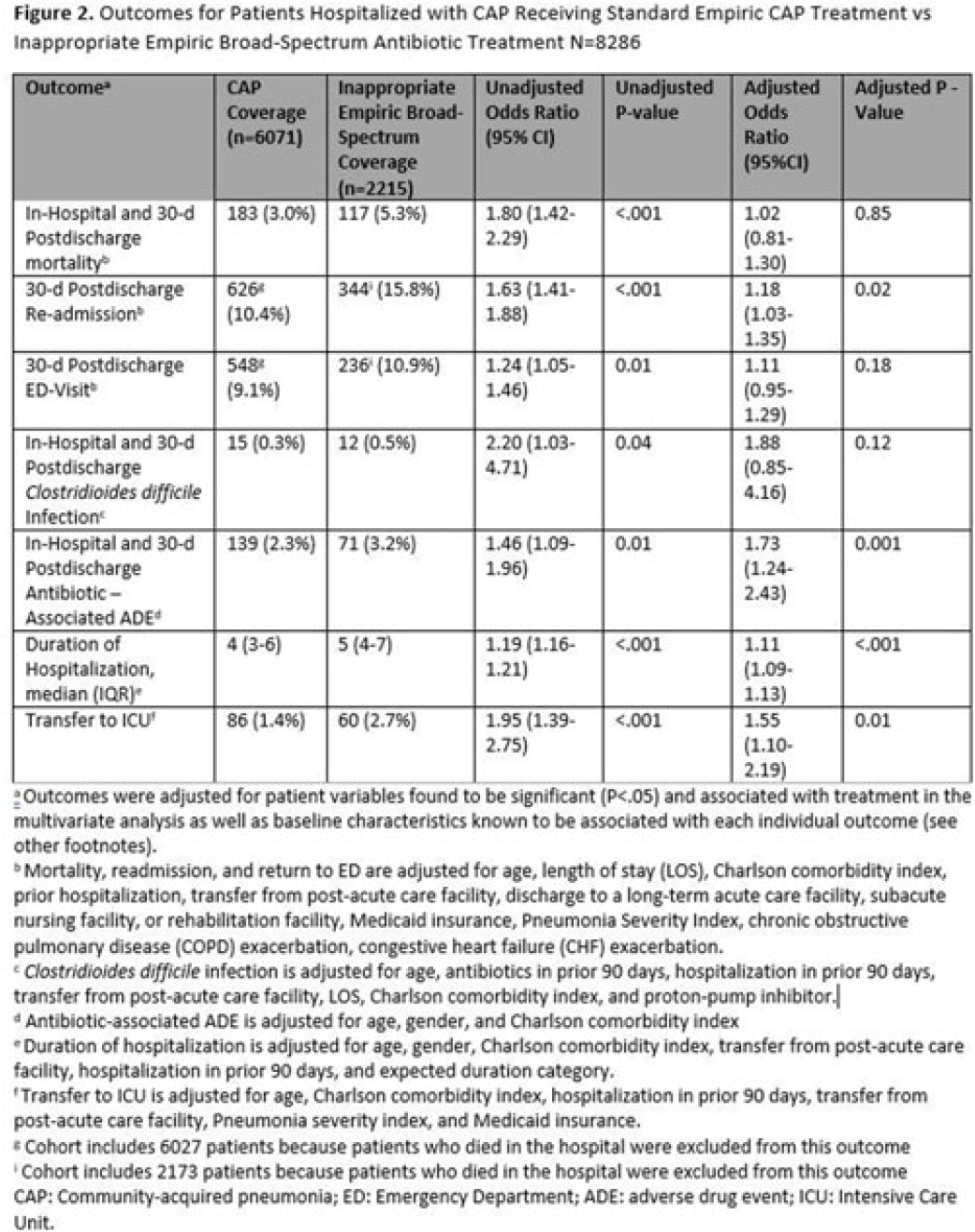
Background: Inappropriate broad-spectrum antibiotic use targeting methicillin-resistant Staphylococcus aureus (MRSA) and Pseudomonas aeruginosa can result in increased adverse events, antibiotic resistance, and Clostridioides difficile infection. In 2019, revised ATS/IDSA community-acquired pneumonia (CAP) guidelines removed healthcare-associated pneumonia (HCAP) as a clinical entity and modified patient factors warranting empiric broad-spectrum antibiotic (BSA) use. As a result, most patients hospitalized with CAP should receive empiric antibiotics targeting standard CAP pathogens. Based on revised guidelines, we evaluated predictors and outcomes associated with inappropriate BSA use among hospitalized patients with CAP. Methods: Between November 2019 and July 2022, trained abstractors collected data on non-ICU adult medical patients admitted with CAP at 67 Michigan hospitals who received either an inappropriate empiric BSA on hospital day 1 or 2 or a standard CAP regimen. Inappropriate empiric BSA use was defined as use of an anti-MRSA or anti-pseudomonal antibiotic in a patient eligible for standard CAP coverage per IDSA guidelines. Patients with immune compromise, moderate or severe chronic obstructive pulmonary disease (COPD), pulmonary complication, or guideline-concordant treatment with BSA were excluded. Data collected included comorbidities, antibiotic use and hospitalizations in the preceding 90 days, cultures in the preceding year, signs or symptoms of pneumonia, hospital characteristics, and 30-day postdischarge patient outcomes. Data were collected through chart review and patient phone calls. Predictors of inappropriate empiric BSA were evaluated using logistic general estimating equation (GEE) models, accounting for hospital-level clustering. We assessed the effect of inappropriate empiric BSA (vs standard CAP therapy) on 30-day patient outcomes using logistic GEE models controlling for predictors associated with the outcome and probability of treatment. Results: Of 8,286 included patients with CAP, 2,215 (26.7%) were empirically treated with inappropriate BSA. The median BSA treatment was 3 days (IQR, 2.5). After adjustments, factors associated with inappropriate empiric BSA treatment included hospitalization or treatment with high-risk antibiotics in preceding 90 days, transfer from a postacute care facility, hemodialysis, support with ≥3 L supplemental oxygen, severe sepsis, leukocytosis, and higher pneumonia severity index (Fig. 1). After adjustments, patients with inappropriate empiric BSA treatment had higher readmissions 30 days after discharge, more transfers to the intensive care unit, more antibiotic-associated adverse events, and longer hospitalizations (Fig. 2). Conclusions: Patients hospitalized with CAP often received inappropriate BSA as empiric coverage, and this inappropriate antibiotic selection was associated with worse patient outcomes. To improve patient outcomes, stewardship efforts should focus on reducing inappropriate BSA use in patients hospitalized for CAP with historic HCAP risk factors or severe CAP without other guideline-directed indications for BSA.
Financial support. H.M.S. initiative is underwritten by Blue Cross and Blue Shield of Michigan.
Disclosures: None
Commentaries
- Daniel Goldrich, Peter G. Snow, Raymond Tanter, Anthony Leeds, Irving Louis Horowitz, Sandra Powell, Raymond Tanter
-
- Journal:
- Latin American Research Review / Volume 3 / Issue 2 / Spring 1968
- Published online by Cambridge University Press:
- 24 October 2022, pp. 67-88
-
- Article
-
- You have access Access
- Export citation
Pharmacist gender and physician acceptance of antibiotic stewardship recommendations: An analysis of the reducing overuse of antibiotics at discharge home intervention
- Part of
- Valerie M. Vaughn, Daniel L. Giesler, Daraoun Mashrah, Adamo Brancaccio, Katie Sandison, Emily S. Spivak, Julia E. Szymczak, Chaorong Wu, Jennifer K. Horowitz, Linda Bashaw, Adam L. Hersh
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 44 / Issue 4 / April 2023
- Published online by Cambridge University Press:
- 07 June 2022, pp. 570-577
- Print publication:
- April 2023
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To assess association of pharmacist gender with acceptance of antibiotic stewardship recommendations.
Design:A retrospective evaluation of the Reducing Overuse of Antibiotics at Discharge (ROAD) Home intervention.
Setting:The study was conducted from May to October 2019 in a single academic medical center.
Participants:The study included patients receiving antibiotics on a hospitalist service who were nearing discharge.
Methods:During the intervention, clinical pharmacists (none who had specialist postgraduate infectious disease residency training) reviewed patients on antibiotics and led an antibiotic timeout (ie, structured conversation) prior to discharge to improve discharge antibiotic prescribing. We assessed the association of pharmacist gender with acceptance of timeout recommendations by hospitalists using logistic regression controlling for patient characteristics.
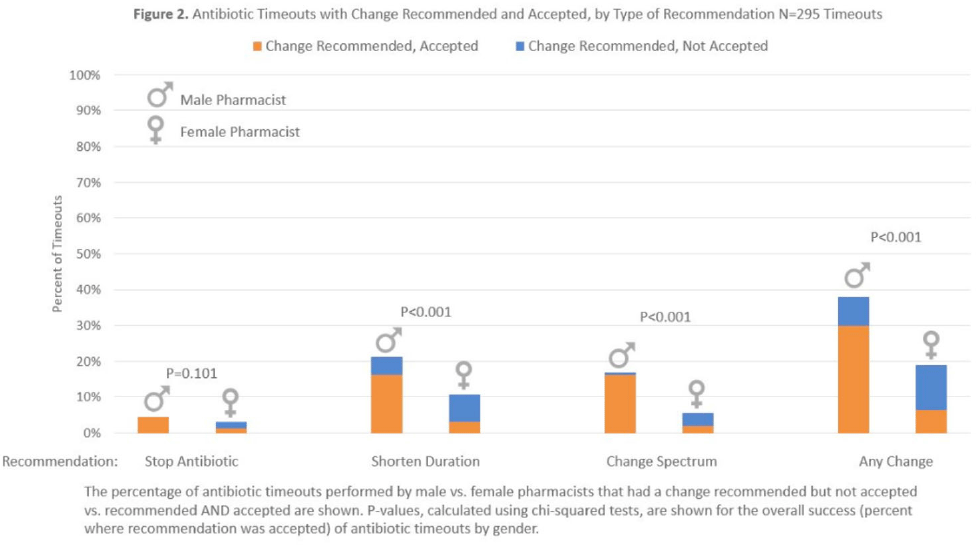
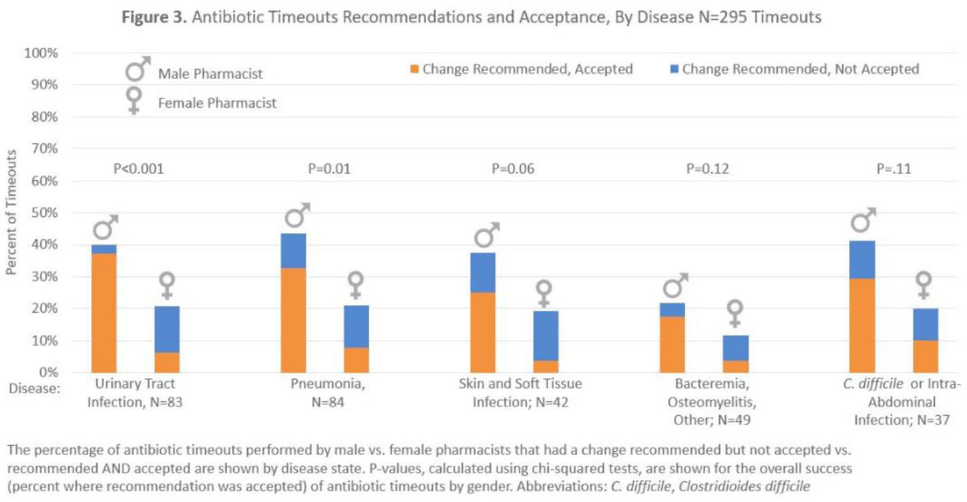
Results:Over 6 months, pharmacists conducted 295 timeouts: 158 timeouts (53.6%) were conducted by 12 women, 137 (46.4%) were conducted by 8 men. Pharmacists recommended an antibiotic change in 82 timeouts (27.8%), of which 51 (62.2%) were accepted. Compared to male pharmacists, female pharmacists were less likely to recommend a discharge antibiotic change: 30 (19.0%) of 158 versus 52 (38.0%) of 137 (P < .001). Female pharmacists were also less likely to have a recommendation accepted: 10 (33.3%) of 30 versus 41 (8.8%) of 52 (P < .001). Thus, timeouts conducted by female versus male pharmacists were less likely to result in an antibiotic change: 10 (6.3%) of 158 versus 41 (29.9%) of 137 (P < .001). After adjustments, pharmacist gender remained significantly associated with whether recommended changes were accepted (adjusted odds ratio [aOR], 0.10; 95%confidence interval [CI], 0.03–0.36 for female versus male pharmacists).
Conclusions:Antibiotic stewardship recommendations made by female clinical pharmacists were less likely to be accepted by hospitalists. Gender bias may play a role in the acceptance of clinical pharmacist recommendations, which could affect patient care and outcomes.
The effect of gender bias on acceptance of antibiotic stewardship recommendations by clinical pharmacists
- Valerie Vaughn, Daniel Giesler, Adamo Brancaccio, Daraoun Mashrah, Katie Sandison, Chaorong Wu, Jennifer Horowitz, Linda Bashaw, Adam Hersh
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 2 / Issue S1 / July 2022
- Published online by Cambridge University Press:
- 16 May 2022, pp. s67-s68
-
- Article
-
- You have access Access
- Open access
- Export citation
-
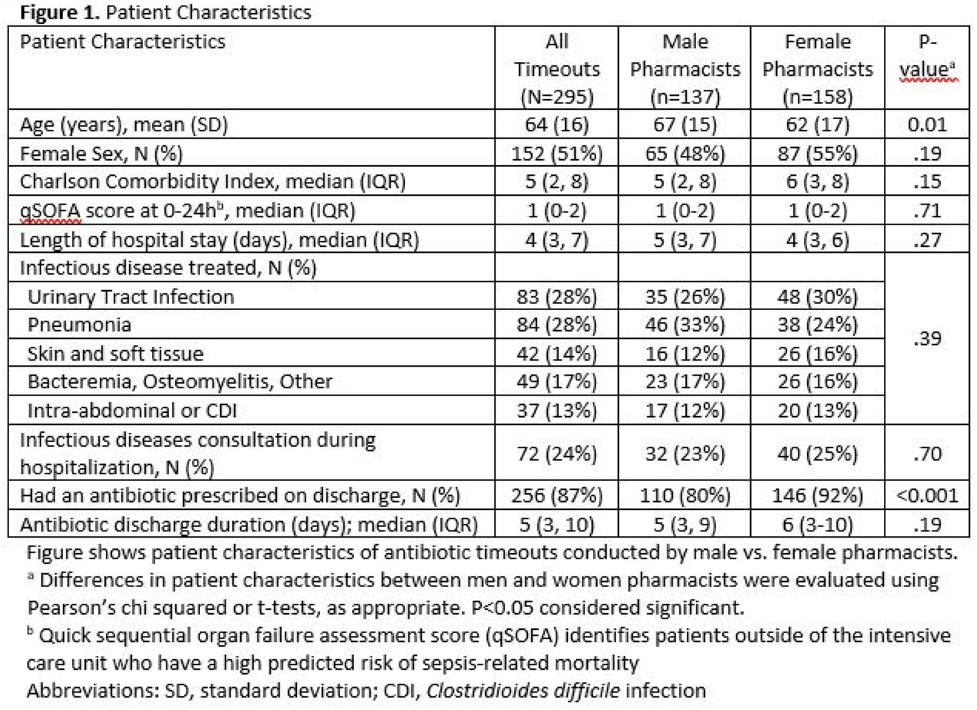
Background: Clinical pharmacists are a critical part of antibiotic stewardship. Stewardship often relies on relationships and persuasion, which may be affected by gender bias. Thus, we aimed to assess the association of sex with the acceptance of antibiotic stewardship recommendations. Methods: Between May and October 2019, medicine pharmacists at single hospital reviewed patients on antibiotics and–when a discharge was anticipated–led an antibiotic discussion (or “timeout”) prior to discharge. To explore differences in antibiotic timeout effectiveness by gender, we assessed the association of pharmacist sex with suggestion and acceptance of antibiotic changes using logistic regression controlling for patient characteristics. We also assessed whether hospitalist sex was associated with or moderated the effect of pharmacist sex on acceptance of timeout recommendations. Results: Between May 1, 2019, and October 31, 2019, pharmacists conducted 295 timeouts (patient characteristics in Fig. 1). Overall, 54% of timeouts were conducted by 12 female pharmacists and the remaining 46% were conducted by 8 male pharmacists. Overall, 82 (29%) of 295 timeouts resulted in a pharmacist recommending an antibiotic change, and male pharmacists were more likely to recommend a change: 52 (38%) of 137 versus 30 (19%) 158 (P Conclusions: In this discharge antibiotic intervention, timeouts conducted by women were less likely to result in an antibiotic change than those conducted by men. The difference in effectiveness resulted both from female pharmacists being less likely to recommend a change and from hospitalists being less likely to accept recommendations from a female pharmacist. These findings suggest that gender bias may play a role acceptance of antibiotic stewardship recommendations, which could affect antibiotic use, pharmacist job satisfaction, and patient outcomes.
Funding: None
Disclosures: None
Roundtable - Mark Greif , The Age of the Crisis of Man: Thought and Fiction in America, 1933–1973 (Princeton, NJ: Princeton University Press, 2014, £19.95). Pp. 434. isbn 978 0 6911 4639 3.
- ADAM KELLY, WILL NORMAN, RICHARD H. KING, ROBERT GENTER, DANIEL HOROWITZ
-
- Journal:
- Journal of American Studies / Volume 51 / Issue 1 / February 2017
- Published online by Cambridge University Press:
- 24 January 2017, pp. 255-266
- Print publication:
- February 2017
-
- Article
- Export citation
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Contributors
-
- By Rony A. Adam, Gloria Bachmann, Nichole M. Barker, Randall B. Barnes, John Bennett, Inbar Ben-Shachar, Jonathan S. Berek, Sarah L. Berga, Monica W. Best, Eric J. Bieber, Frank M. Biro, Shan Biscette, Anita K. Blanchard, Candace Brown, Ronald T. Burkman, Joseph Buscema, John E. Buster, Michael Byas-Smith, Sandra Ann Carson, Judy C. Chang, Annie N. Y. Cheung, Mindy S. Christianson, Karishma Circelli, Daniel L. Clarke-Pearson, Larry J. Copeland, Bryan D. Cowan, Navneet Dhillon, Michael P. Diamond, Conception Diaz-Arrastia, Nicole M. Donnellan, Michael L. Eisenberg, Eric Eisenhauer, Sebastian Faro, J. Stuart Ferriss, Lisa C. Flowers, Susan J. Freeman, Leda Gattoc, Claudine Marie Gayle, Timothy M. Geiger, Jennifer S. Gell, Alan N. Gordon, Victoria L. Green, Jon K. Hathaway, Enrique Hernandez, S. Paige Hertweck, Randall S. Hines, Ira R. Horowitz, Fred M. Howard, William W. Hurd, Fidan Israfilbayli, Denise J. Jamieson, Carolyn R. Jaslow, Erika B. Johnston-MacAnanny, Rohna M. Kearney, Namita Khanna, Caroline C. King, Jeremy A. King, Ira J. Kodner, Tamara Kolev, Athena P. Kourtis, S. Robert Kovac, Ertug Kovanci, William H. Kutteh, Eduardo Lara-Torre, Pallavi Latthe, Herschel W. Lawson, Ronald L. Levine, Frank W. Ling, Larry I. Lipshultz, Steven D. McCarus, Robert McLellan, Shruti Malik, Suketu M. Mansuria, Mohamed K. Mehasseb, Pamela J. Murray, Saloney Nazeer, Farr R. Nezhat, Hextan Y. S. Ngan, Gina M. Northington, Peggy A. Norton, Ruth M. O'Regan, Kristiina Parviainen, Resad P. Pasic, Tanja Pejovic, K. Ulrich Petry, Nancy A. Phillips, Ashish Pradhan, Elizabeth E. Puscheck, Suneetha Rachaneni, Devon M. Ramaeker, David B. Redwine, Robert L. Reid, Carla P. Roberts, Walter Romano, Peter G. Rose, Robert L. Rosenfield, Shon P. Rowan, Mack T. Ruffin, Janice M. Rymer, Evis Sala, Ritu Salani, Joseph S. Sanfilippo, Mahmood I. Shafi, Roger P. Smith, Meredith L. Snook, Thomas E. Snyder, Mary D. Stephenson, Thomas G. Stovall, Richard L. Sweet, Philip M. Toozs-Hobson, Togas Tulandi, Elizabeth R. Unger, Denise S. Uyar, Marion S. Verp, Rahi Victory, Tamara J. Vokes, Michelle J. Washington, Katharine O'Connell White, Paul E. Wise, Frank M. Wittmaack, Miya P. Yamamoto, Christine Yu, Howard A. Zacur
- Edited by Eric J. Bieber, Joseph S. Sanfilippo, University of Pittsburgh, Ira R. Horowitz, Emory University, Atlanta, Mahmood I. Shafi
-
- Book:
- Clinical Gynecology
- Published online:
- 05 April 2015
- Print publication:
- 23 April 2015, pp viii-xiv
-
- Chapter
- Export citation
Use of vitamin D supplements during infancy in an international feeding trial
- Eveliina Lehtonen, Anne Ormisson, Anita Nucci, David Cuthbertson, Susa Sorkio, Mila Hyytinen, Kirsi Alahuhta, Carol Berseth, Marja Salonen, Shayne Taback, Margaret Franciscus, Teba González-Frutos, Tuuli E Korhonen, Margaret L Lawson, Dorothy J Becker, Jeffrey P Krischer, Mikael Knip, Suvi M Virtanen, , Thomas Mandrup-Poulsen, Elias Arjas, Åke Lernmark, Barbara Schmidt, Jeffrey P. Krischer, Hans K. Åkerblom, Mila Hyytinen, Mikael Knip, Katriina Koski, Matti Koski, Eeva Pajakkala, Marja Salonen, David Cuthbertson, Jeffrey P. Krischer, Linda Shanker, Brenda Bradley, Hans-Michael Dosch, John Dupré, William Fraser, Margaret Lawson, Jeffrey L. Mahon, Mathew Sermer, Shayne P. Taback, Dorothy Becker, Margaret Franciscus, Anita Nucci, Jerry Palmer, Minna Pekkala, Suvi M. Virtanen, Jacki Catteau, Neville Howard, Patricia Crock, Maria Craig, Cheril L. Clarson, Lynda Bere, David Thompson, Daniel Metzger, Colleen Marshall, Jennifer Kwan, David K. Stephure, Daniele Pacaud, Wendy Schwarz, Rose Girgis, Marilyn Thompson, Shayne P. Taback, Daniel Catte, Margaret L. Lawson, Brenda Bradley, Denis Daneman, Mathew Sermer, Mary-Jean Martin, Valérie Morin, Lyne Frenette, Suzanne Ferland, Susan Sanderson, Kathy Heath, Céline Huot, Monique Gonthier, Maryse Thibeault, Laurent Legault, Diane Laforte, Elizabeth A. Cummings, Karen Scott, Tracey Bridger, Cheryl Crummell, Robyn Houlden, Adriana Breen, George Carson, Sheila Kelly, Koravangattu Sankaran, Marie Penner, Richard A. White, Nancy King, James Popkin, Laurie Robson, Eva Al Taji, Irena Aldhoon, Pavla Mendlova, Jan Vavrinec, Jan Vosahlo, Ludmila Brazdova, Jitrenka Venhacova, Petra Venhacova, Adam Cipra, Zdenka Tomsikova, Petra Krckova, Pavla Gogelova, Ülle Einberg, Mall-Anne Riikjärv, Anne Ormisson, Vallo Tillmann, Päivi Kleemola, Anna Parkkola, Heli Suomalainen, Anna-Liisa Järvenpää, Anu-Maaria Hämälainen, Hannu Haavisto, Sirpa Tenhola, Pentti Lautala, Pia Salonen, Susanna Aspholm, Heli Siljander, Carita Holm, Samuli Ylitalo, Raisa Lounamaa, Anja Nuuja, Timo Talvitie, Kaija Lindström, Hanna Huopio, Jouni Pesola, Riitta Veijola, Päivi Tapanainen, Abram Alar, Paavo Korpela, Marja-Liisa Käär, Taina Mustila, Ritva Virransalo, Päivi Nykänen, Bärbel Aschemeier, Thomas Danne, Olga Kordonouri, Dóra Krikovszky, László Madácsy, Yeganeh Manon Khazrai, Ernesto Maddaloni, Paolo Pozzilli, Carla Mannu, Marco Songini, Carine de Beaufort, Ulrike Schierloh, Jan Bruining, Margriet Bisschoff, Aleksander Basiak, Renata Wasikowa, Marta Ciechanowska, Grazyna Deja, Przemyslawa Jarosz-Chobot, Agnieszka Szadkowska, Katarzyna Cypryk, Malgorzata Zawodniak-Szalapska, Luis Castano, Teba Gonzalez Frutos, Mirentxu Oyarzabal, Manuel Serrano-Ríos, María Teresa Martínez-Larrad, Federico Gustavo Hawkins, Dolores Rodriguez Arnau, Johnny Ludvigsson, Malgorzata Smolinska Konefal, Ragnar Hanas, Bengt Lindblad, Nils-Osten Nilsson, Hans Fors, Maria Nordwall, Agne Lindh, Hans Edenwall, Jan Aman, Calle Johansson, Margrit Gadient, Eugen Schoenle, Dorothy Becker, Ashi Daftary, Margaret Franciscus, Carol Gilmour, Jerry Palmer, Rachel Taculad, Marilyn Tanner-Blasiar, Neil White, Uday Devaskar, Heather Horowitz, Lisa Rogers, Roxana Colon, Teresa Frazer, Jose Torres, Robin Goland, Ellen Greenberg, Maudene Nelson, Holly Schachner, Barney Softness, Jorma Ilonen, Massimo Trucco, Lynn Nichol, Erkki Savilahti, Taina Härkönen, Mikael Knip, Outi Vaarala, Kristiina Luopajärvi, Hans-Michael Dosch
-
- Journal:
- Public Health Nutrition / Volume 17 / Issue 4 / April 2014
- Published online by Cambridge University Press:
- 24 June 2013, pp. 810-822
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objective
To examine the use of vitamin D supplements during infancy among the participants in an international infant feeding trial.
DesignLongitudinal study.
SettingInformation about vitamin D supplementation was collected through a validated FFQ at the age of 2 weeks and monthly between the ages of 1 month and 6 months.
SubjectsInfants (n 2159) with a biological family member affected by type 1 diabetes and with increased human leucocyte antigen-conferred susceptibility to type 1 diabetes from twelve European countries, the USA, Canada and Australia.
ResultsDaily use of vitamin D supplements was common during the first 6 months of life in Northern and Central Europe (>80 % of the infants), with somewhat lower rates observed in Southern Europe (>60 %). In Canada, vitamin D supplementation was more common among exclusively breast-fed than other infants (e.g. 71 % v. 44 % at 6 months of age). Less than 2 % of infants in the USA and Australia received any vitamin D supplementation. Higher gestational age, older maternal age and longer maternal education were study-wide associated with greater use of vitamin D supplements.
ConclusionsMost of the infants received vitamin D supplements during the first 6 months of life in the European countries, whereas in Canada only half and in the USA and Australia very few were given supplementation.
Same Time, Same Station: Creating American Television, 1948–1961. By James H. Baughman. Baltimore: Johns Hopkins University Press, 2007. xiii + 443 pp. Photographs, notes, index. Cloth, $35.00. ISBN: 0-8018-7933-7.
- Daniel Horowitz
-
- Journal:
- Business History Review / Volume 81 / Issue 4 / Winter 2007
- Published online by Cambridge University Press:
- 13 December 2011, pp. 814-817
- Print publication:
- Winter 2007
-
- Article
- Export citation
Better Living: Advertising, Media, and the New Vocabulary of Business Leadership. By William L. BirdJr Evanston, Ill.: Northwestern University Press, 1999. x + 288. Bibliography, figures, index, and notes. Cloth, $30.00. ISBN 0810115859.
- Daniel Horowitz
-
- Journal:
- Business History Review / Volume 73 / Issue 4 / Winter 1999
- Published online by Cambridge University Press:
- 08 March 2017, pp. 754-756
- Print publication:
- Winter 1999
-
- Article
- Export citation
7 - The Emigré as Celebrant of American Consumer Culture: George Katona and Ernest Dichter
- Edited by Susan Strasser, Charles McGovern, Smithsonian Institution, Washington DC, Matthias Judt, Martin Luther-Universität Halle-Wittenburg, Germany
-
- Book:
- Getting and Spending
- Published online:
- 05 January 2013
- Print publication:
- 13 November 1998, pp 149-166
-
- Chapter
- Export citation
-
Summary
With its adaptation of Marxism and its emphasis on the role of the mass media, the Frankfurt School has provided the most widely recognized analysis of consumer culture to come out of Europe in the 1930s and influence Americans in subsequent decades. Beginning in the 1940s, George Katona and Ernest Dichter celebrated what many leading emigre intellectuals were critiquing: the impact of consumer culture on American life. Katona (1901-81) relied on his surveys of consumer expectations carried out at the University of Michigan from 1946 to 1972 to assert that the optimistic and sensible American consumer would heroically prevent the nation from experiencing the inflation and instability that ravaged Europe in the years between the two world wars. Dichter (1907-91) made a handsome living in the United States helping corporations understand the psyche of consumers. In the process, he linked democracy with purchasing, redefined the roles of middle-class women, and promoted a distinctly antipuritanical vision.
Although the pictures drawn by Katona and Dichter of the American consumer differed in many respects, they shared a belief, shaped by their experiences in Europe and the United States, that American consumers were critical to the promotion of growth, democracy, and stability. They both gave a special importance in their analysis to the new middle class of salaried and professional employees and to the leadership of educated experts, social and behavioral scientists especially, as forces that would prevent fascism from coming to America.
Distant metastases in terminal head and neck cancer patients
- Yoav P. Talmi, Daniel Cotlear, Alexander Waller, Zeev Horowitz, Abraham Adunski, Yehuda Roth, Jona Kronenberg
-
- Journal:
- The Journal of Laryngology & Otology / Volume 111 / Issue 5 / May 1997
- Published online by Cambridge University Press:
- 29 June 2007, pp. 454-458
- Print publication:
- May 1997
-
- Article
- Export citation
-
With improved control of cancer above the clavicles, distant metastases (DM) are frequently more seen and are becoming a more common cause of morbidity and mortality. The present study defined the incidence of distant metastases in a cohort of terminal head and neck cancer patients (HNCP) and compared it to current reported data. The incidence of distant metastases in relation to the primary tumour was evaluated and their impact on survival was assessed. A retrospective survey of patient charts was made, based on the hospice database and original referring hospital charts. Data of 59 patients admitted to the hospice were evaluated. The incidence and location of locoregional and distant disease were studied and effects on survival analyzed.
The overall survival from diagnosis to demise was 42.7 months. Thyroid cancer was seen in 20.3 per cent of cases and squamous cell cancer was seen in 59.3 per cent. Distant metastases were found in 83 per cent and 48.6 per cent of patients respectively. Laryngeal cancer patients had a 54.5 per cent incidence of distant metastases. Locoregional disease was seen in 47 per cent of cases and 35.7 per cent of them had distant metastases while a 64.3 per cent incidence of distant metastases was found in cases without locoregional disease. Mean survival was 47.3 months with distant metastases vs 36.5 months without metastases. The difference was not statistically significant.
The incidence of distant metastases in squamous cell cancer in terminalHNCP was 48.6 per cent. This is the highest reported incidence of metastases in a clinical series. Patients without locoregional disease had almost a two-fold incidence of metastases. Survival was not affected by metastases in this series.
Double-Blind, Placebo-Controlled, Crossover Trial of Glycine Adjuvant Therapy for Treatment-Resistant Schizophrenia
- Uriel Heresco-Levy, Daniel C. Javitt, Marina Ermilov, Clara Mordel, Avraham Horowitz, Dalia Kelly
-
- Journal:
- The British Journal of Psychiatry / Volume 169 / Issue 5 / November 1996
- Published online by Cambridge University Press:
- 02 January 2018, pp. 610-617
- Print publication:
- November 1996
-
- Article
- Export citation
-
Background
It has been proposed that schizophrenia is associated with underactivity of brain glutamatergic neurotransmission, especially at the level of the N-methyl-D-aspartate (NMDA) subtype of glutamate receptor. Glycine potentiates NMDA receptor-mediated neurotransmission, indicating that it may serve as an effective therapeutic agent in the treatment of schizophrenia.
MethodEleven treatment-resistant patients with chronic schizophrenia completed a double-blind placebo-controlled, six-week, randomly assigned, crossover treatment trial of 0.8 g/kg body weight/day of glycine, added to their prior antipsychotic treatment.
ResultsGlycine was well tolerated, resulted in significantly increased serum glycine levels and induced a mean 36 (7%) reduction in negative symptoms (P < 0.0001). Significant improvments were also induced in depressive and cognitive symptoms. The greatest reduction in negative symptoms was registered in the patients who had the lowest baseline serum glycine levels.
ConclusionsThese results extend previous findings and suggest an additional approach to the pharmacotherapy of negative symptoms and cognitive deficits in schizophrenia.









