49 results
Mental Health and Addictions in Pregnancy: Feasibility and Acceptability of a Computerized Clinical Pathway and Prevalence Rates
- R. Carmona Camacho, J. Chamorro Delmo, M. Alvaro Navidad, N. Lopez Carpintero, N. Estrella Sierra, R. Guimaraes de Oliveira, M. Olhaberry Huber, L. Mata Iturralde, R. Álvarez García, E. Baca Garcia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S66-S67
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental Health problems and substance misuse during pregnancy constitute a serious social problem due to high maternal-fetal morbidity (Cook et al, 2017; JOCG, 39(10) ,906-915) and low detection and treatment rates (Carmona et al. Adicciones. 2022;34(4):299-308)
ObjectivesOur study aimed to develop and test the feasibility and acceptability of a screening and treatment clinical pathway in pregnancy, based on the combination of e-Health tools with in-person interventions and, secondly, describe the prevalence of mental illness and substance use problems in this population.
Methods1382 pregnant women undergoing her first pregnancy visit were included in a tailored clinical pathway and sent a telematic (App) autoapplied questionnaire with an extensive battery of measures (WHO (Five) Well-Being [WHO-5],Patient Health Questionnaire [PHQ-9], General Anxiety Disorder [GAD-7], Alcohol Use Disorders Identification Test [AUDIT], Drug Abuse Screening Test [DAST], Columbia Suicide Severity Rating Scale [C-SSRS] and specifically designed questions on self-harm and psychopharmacological drugs).
Patients who did not respond to the questionnaire on their own received a counseling call.
Based on the screening results, patients were classified into five groups according to severity (Figure 1) and assigned a specific action pathway (Figure 2) that included a range of intervention intensity that goes from an individual psychiatric appointment to no intervention.
ResultsOf the 1382 women included in the clinical pathway, 565(41%) completed the evaluation questionnaires. Of these, 205 (36%) were screened as positive (Grades III,IV or V. Table 1) and 3(0.5%) were classified as needing urgent care. Of the patients offered on-line groups (100), 40% (40) were enrolled in them.
Table 1: Grade distribution of those screened as positives
Grade III 97 (17,2%) Grade IV 105 (18,6%) Grade V 3 (0,5%) Concerning prevalence rates, 73 (12,9%) patients endorsed at least moderate anxiety according to GAD-7 (≥10), 65 (11,5%) endorsed at least moderate depression according to PHQ-9 (≥ 10), 17 were positive on DAST (3%) and 63 (11%) patients scored above the threshold in AUDIT-C(≥ 3) for alcohol use.
Image:
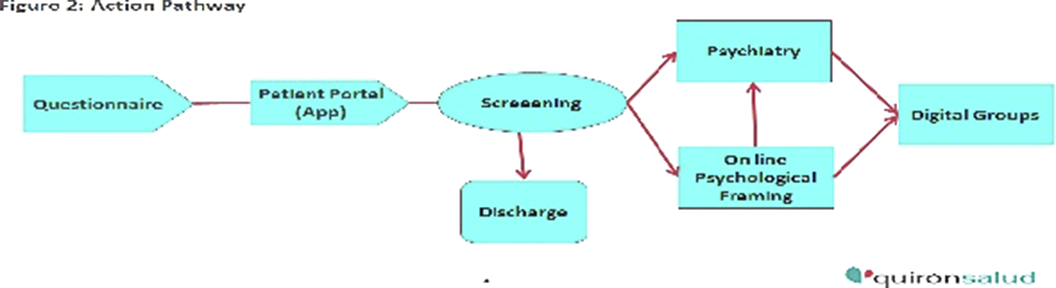
Image 2:
 Conclusions
ConclusionsHigh prevalence rates suggest that effective detection and treatment mechanisms should be integrated into usual care. The use of standardized clinical pathways can help with this aim, allowing better clinical management and referral to treatment, but still face challengues to increase retention. The use of e-health tools offers the opportunity to improve accessibility and therapeutic outcomes through online interventions.
Disclosure of InterestNone Declared
Differences in adherence to treatment, relapses and healthcare costs between delusional disorder and paranoid personality disorder
- R. Álvarez-García, S. Abascal-Peiró, A. Gonzalo de Miguel, C. Blanco-Londono, A. Martinez-Pillado, L. Mata-Iturralde, E. Baca-Garcia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S128
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Limited information is available regarding the clinical features, optimal treatment and prognosis of Paranoid Personality Disorder (PPD) and Delusional Disorder (DD). This is partly due to the low prevalence of cases and poor patient insight. The difference between DD and PPD has been questioned in the literature, as some studies have described them as a continuum, highlighting the role of specific personality traits in the transition to clinical delusions.
Nonadherence to pharmacological treatment is one of the most challenging aspects. This further leads to relapses, increased use of emergency psychiatric services, psychiatric admissions, longer periods of hospitalization, and an increased cost of illness to healthcare systems.
ObjectivesThe primary goal of this study is to compare the differences between DD and PPD in terms of medication adherence, relapses, lost to follow-up, and costs. Other aims of this study are to analyze the differences in these variables between patients who are adequately adherent and patients who are not
MethodsAn observational, retrospective, and multicenter descriptive epidemiological study was conducted. Patients were selected from four public departments of psychiatry in Madrid, providing an area of roughly one million people. All patients were older than 18 years-old, diagnosed with DD or PPD from 2005 to 2022. Data were extracted from electronic medical records and from electronic prescribing program used in the public health system.The study was approved by the Hospital Fundación Jiménez Díaz Ethics Committee.
Results1227 individuals diagnosed with DD (974 patients,79,3%) or PPD (253 patients, 20.61%). 23.81% (232 patients) of the DD-group did not take out the prescribed medication of the pharmacy, and 16.6% (42 patients) of the PPD-group were considered non-adherent.
Adherent patients had greater follow-up (4.02 vs 2.89 years) and shorter hospital stays (5.15 vs 8.6 days, p<0.05) compared to non-adherent patients. DD patients doubled the average hospitalization stay compared to the PPD group (6.7 vs 2.96 days, p<0.01).
Regarding costs: DD had higher hospitalization costs than PDD (1164 vs 488 euros per year) and higher total costs than PDD (2180 vs 1528 euros per year, p<0.05). The costs were also higher in non-adherent than in adherent patients (2570 vs 1895 euros per year, p<0.05)
ConclusionsOur sample of 1227 DD and PPD patients followed from 2005-2022 is, to our knowledge, one of the largest collected to date. We found sociodemographic and clinical differences between the DD and the PPD group. We also found differences between adherent and non-adherent patients, highlighting that non-adherence is associated with longer mean stay of hospitalization and more costs, both hospitalization and total direct healthcare costs. We have also found association between non-adherence and risk of psychotic relapse.
Disclosure of InterestNone Declared
Association between loneliness in childhood and first-episode psychosis
- C. M. Díaz-Caneja, L. Donaire, V. Cavone, Á. Andreu-Bernabeu, J. González-Peñas, M. Díaz-Marsá, R. Rodríguez-Jiménez, Á. Ibáñez, E. Baca-García, J. C. Leza, M. F. Bravo-Ortiz, J. L. Ayuso-Mateos, C. Arango
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S88-S89
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Evidence from observational and genetic studies suggests a bidirectional relationship between loneliness and psychosis. To our knowledge, no previous study has assessed the association between loneliness in childhood and first-episode psychosis (FEP).
ObjectivesWe aimed to assess the association between loneliness in childhood and the odds of FEP and clinical variables of interest (i.e., diagnosis and clinical and functional severity) in FEP and to explore gender differences in this association.
MethodsThis was an observational, case-control study, based on the AGES-CM cohort, a longitudinal prospective study including patients with FEP ages 7-40, their first-degree relatives, and an age- and sex-matched sample of controls in seven university hospitals in the region of Madrid. We assessed loneliness in childhood with the question “Have you ever felt lonely for more than 6 months before the age of 12” and objetive social isolation with the peer relationships item from the childhood subscale of the Premorbid Adjustment Scale. We conducted logistic and linear regression analyses to assess the association between childhood loneliness and i) the odds of presenting a FEP and ii) clinical variables of interest (diagnosis and scores on positive, negative, general, depressive, and manic symptoms and functioning), while adjusting for demographic variables.
ResultsThe study sample comprised 285 patients with FEP (32.6% female, age 24.50 ± 6.2 years) and 546 controls (48.7% female, age 25.93 ± 5.5 years). Loneliness in childhood was associated with increased odds of FEP (adjusted odds ratio; aOR: 2.17, 95% CI [1.40-3.51], p=.002). This association remained significant after controlling for objective social isolation in childhood (aOR:2.70, IC 95% [1.58-4.62], p<.001).
The effect of the association was stronger in females (aOR:4.74, 95% CI [2.23-10.05], p<.001) than in males (aOR:1.17, IC 95% [0.63-2.19], p=.623). In females with FEP, loneliness in childhood was significantly associated with increased odds of receiving a diagnosis of other psychosis (aOR:0.155, 95% CI [0.048-0.506], p=.002) relative to an SSD diagnosis. In the FEP sample, loneliness in childhood was associated with greater severity of positive and affective symptoms and worse functioning.
ConclusionsLoneliness in childhood is associated with increased odds of FEP and clinical variables of interest. This suggests the potential role of this phenotype as an early risk marker for psychosis that could help guide targeted interventions.
Disclosure of InterestC. Díaz-Caneja Grant / Research support from: Instituto de Salud Carlos III (PI17/00481, PI20/00721, JR19/00024), European Union, Consultant of: Angelini, L. Donaire: None Declared, V. Cavone: None Declared, Á. Andreu-Bernabeu: None Declared, J. González-Peñas: None Declared, M. Díaz-Marsá: None Declared, R. Rodríguez-Jiménez: None Declared, Á. Ibáñez: None Declared, E. Baca-García: None Declared, J. C. Leza: None Declared, M. F. Bravo-Ortiz: None Declared, J. L. Ayuso-Mateos: None Declared, C. Arango Grant / Research support from: Madrid Regional Government (R&D activities in Biomedicine S2022/BMD-7216 AGES 3-CM), Instituto de Salud Carlos III, European Union, Consultant of: Acadia, Angelini, Biogen, Boehringer, Gedeon Richter, Janssen Cilag, Lundbeck, Medscape, Menarini, Minerva, Otsuka, Pfizer, Roche, Sage, Servier, Shire, Schering Plough, Sumitomo Dainippon Pharma, Sunovion and Takeda
Factors associated with first suicide attempt vs. re-attempt in children and adolescents: A systematic review and meta-analysis
- S. Abascal-Peiró, A. Alacreu-Crespo, I. Peñuelas-Calvo, B. Ezquerra-de la Cruz, L. Jiménez-Muñoz, E. Baca-García, A. Porras-Segovia
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S584
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide among children, adolescents and young adults is a major health problem, as it represents the fourth leading cause of death among people aged 15-29 (WHO, 2022). A recent study showed that the years of potential life lost (YPLL) due to suicide in 2018 were 1,344,552, which is very close to the 1,591,487 YPLL caused by COVID-19 in the year 2020 (Porras-Segovia et al, 2021). In the recent years, there is a growing interest in suicide prevention research in differentiating attempter profiles in terms of lifetime suicide attempts. Specifically, studies suggest that there may be meaningful differences concerning risk factors between patients with a history of one versus multiple suicide attempts. Multiple attempters (MA) show more suicidal ideation, depressive symptoms and hopelessness than single attempters (SA) (Esposito et al, 2003; Goldston et al, 1998).
ObjectivesWe aimed to answer the question ‘What are the factors associated with attempting suicide for the first time and are they different from the factors associated with re-attempting suicide in children and adolescents?’
MethodsWe conducted a systematic literature search in four databases. Article selection and data extraction according to a predefined protocol, including bias risk assessment, were performed by independent peer reviewers. Due to the different way to present data in the studies effect sizes were pre-calculated to standard mean differences (SMD). Random effects model was used to calculate the pooled effect size for all meta-analysis. Publication bias was assessed using funnel plots.
Results14 studies were included in the systematic review, and 13 in the meta-analysis. Original articles used in the meta-analysis included a total of 4286 participants of whom 1579 were multiple suicide-attempters and 2707 single suicide attempters.
MAs showed significantly higher proportion of anxiety disorders (SMD = 0.387, 95%CI [0.09, 0.68], p < 0.022), alcohol abuse disorder (SMD = 0.382, 95%CI [0.07, 0.70], p < 0.036) and substance abuse disorder (SMD = 0.526, 95%CI [0.21, 0.84], p <0.013) than SAs. Mean depression severity was higher among MAs than SAs (SMD = 0.515, 95%CI [0.17, 0.86], p < 0.011). MAs showed higher impulsivity (SMD = 0.28, 95%CI [-0.03, 0.60], p < 0.068) and aggressiveness (SMD = 0.688, 95%CI [0.42, 0.96], p < 0.00) than SAs. Hopelessness (SMD = 0.482, 95%CI [0.06, 0.91], p < 0.03) and suicidal ideation (SMD = 0.399, 95%CI [0.34, 0.46], p < 0.007) was significantly higher in MA.
ConclusionsOn the basis of the current results, multiple attempters may represent a distinct patient population in terms of being a more severe clinical profile. This can provide the basis of stronger suicide prevention and vigilance programs focused in this suicidal phenotype.
Disclosure of InterestNone Declared
Alternative initiations with 6-monthly paliperidone palmitate. A retrospective study
- S. Benavente López, S. Bolaño Mendoza, A. Parra González, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S488-S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
6-monthly paliperidone palmitate features an initiation regimen through 1-monthly paliperidone palmitate or 3-monthly paliperidone palmitate. Some patients do not have sufficient adherence to treatment and it is necessary at the clinical level to start directly with 6-monthly paliperidone palmitate. There is little clinical experience with these alternative initiations and through this work those that have been carried out for 12 months at the Hospital Universitario Infanta Elena are exposed.
ObjectivesThe main objective of the study is to describe the alternative initiations performed with 6-monthly paliperidone palmitate in routine clinical practice, having opted for a regimen different from the standard for clinical reasons.
MethodsA retrospective selection of patients will be made through non-probabilistic consecutive sampling, including all patients who have been administered 6-monthly paliperidone palmitate with a start different from the standard during the last 4 months. To do this, the electronic medical record will be used, first selecting the patients who have started 6-monthly paliperidone palmitate through the anonymized digital records and, later, including in the study only those who have followed an alternative initiation pattern. The variables studied will be the following: age, sex, diagnosis, dose of paliperidone palmitate, initiation regimen, consumption of toxic substances, absenteeism from 6-monthly paliperidone palmitate, and visits to the emergency room and admissions.
ResultsThe study included a total of 20 patients (n: 20). 80% of the patients were male and 20% were female. The mean age was 39.7 years. 75% of the patients had an associated substance use disorder. The following alternate starting schedules were performed with biannual paliperidone palmitate: monthly paliperidone palmitate on days 1 and 8, and 6-monthly paliperidone palmitate on day 38 (n: 11); monthly paliperidone palmitate 150 mg together with semi-annual paliperidone palmitate both on day 1 (n: 5); biannual paliperidone palmitate on day 1 supplemented with oral paliperidone for 45 days (n:4). A total of 0 visits to the emergency department and 0 admissions were observed after the 6-monthly paliperidone palmitate regimen.
ConclusionsAlternative initiations with 6-monthly paliperidone palmitate may be a useful and safe clinical alternative in patients with very low adherence who, due to clinical needs, require starting 6-monthly paliperidone palmitate earlier in order to guarantee adherence.
Disclosure of InterestNone Declared
Clinical experiences with 6-monthly paliperidone palmitate after 12 months of use. A retrospective study
- S. Benavente López, A. Parra González, S. Bolaño Mendoza, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S488
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIA) have provided a significant improvement in the treatment of schizophrenia. Although there is already significant clinical experience with paliperidone palmitate, it is important to evaluate the clinical response of patients to this new 6-monthly presentation, so descriptive studies based on real clinical evidence can be very useful for this purpose.
ObjectivesThe main objective of the study is to describe the use of 6-monthly paliperidone palmitate in routine clinical practice, providing variables that objectify the evolution such as the number of admissions and visits to the emergency room.
MethodsRetrospective descriptive study with a sample selected by non-probabilistic consecutive sampling, retrospective type, in a time interval of 12 months (n=40). The patients selected were all those who received 6-monthly paliperidone palmitate treatment, with a diagnosis of schizophrenia, in 12 months of use at Hospital Universitario Infanta Elena. A descriptive analysis was performed. Mean and standard deviation were calculated for quantitative variables and N and percentage for categorical variables.
ResultsA total of 40 administrations of 6-monthly paliperidone palmitate were performed in the study. None of the patients presented adverse reactions related to the administration of the drug, not reporting local pain or inflammation of the puncture area, except for the characteristic discomfort of an intramuscular puncture. Regarding the efficacy of 6-monthly paliperidone palmitate, none of the patients presented a psychotic decompensation after its administration, maintaining psychopathological stability after the change. The switch to 6-monthly paliperidone palmitate was made from both 1-monthly paliperidone palmitate and 3-monthly paliperidone palmitate, both showing the same efficacy. Regarding tolerability, all the patients who were administered 6-monthly paliperidone palmitate were previously treated with the monthly and quarterly presentation of the same molecule, having presented good tolerability to it, maintaining said tolerability after treatment. change to 6-monthly paliperidone palmitate, with no adverse reaction being recorded after the change. The adherence presented by the patients was very good, performing 100% of the administrations of 6-monthly paliperidone palmitate
Conclusions6-monthly paliperidone palmitate may be an effective and well-tolerated treatment for the treatment of schizophrenia. In the present study, the use of said LAIA in a group of 40 patients is objectified, showing excellent efficacy and tolerability. All study patients were already stable with the 1-monthly and 3-monthly paliperidone palmitate formulations, maintaining said psychopathological stability when switching to the 6-monthly paliperidone palmitate formulation, with excellent adherence and adverse effect profile .
Disclosure of InterestNone Declared
Clinical experiences with 6-monthly paliperidone palmitate beyond the diagnosis of schizophrenia. A retrospective study
- S. Benavente López, S. Bolaño Mendoza, A. Parra González, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIA) are used in diagnoses other than schizophrenia. Over the last two decades, LAIAs have been developed with less administration frequency, going from 2-weekly presentations to 6-monthly presentations. The 6-monthly paliperidone palmitate has recently been released, allowing a reduction in the frequency of administration compared to the 1-monthly presentation and the 3-monthly presentation. Descriptive studies based on real clinical evidence can be very useful to assess clinical outcomes.
ObjectivesThe main objective of the study is to describe the use of 6-monthly paliperidone palmitate in patients with schzophrenia, providing variables that objectify the evolution such as the number of psychotic decompensations.
MethodsRetrospective descriptive study with a sample selected by non-probabilistic consecutive sampling, retrospective type, in a time interval of 10 month (n=80). The patients selected were all those who received 6-monthly paliperidone palmitate treatment from after 10 months of use at Hospital Universitario Infanta Elena. A descriptive analysis was performed. Mean and standard deviation were calculated for quantitative variables and N and percentage for categorical variables.
ResultsA total of 80 administrations of 6-monthly paliperidone palmitate were performed in the study. None of the patients presented adverse reactions related to the administration of the drug, not reporting local pain or inflammation of the puncture area, except for the characteristic discomfort of an intramuscular puncture. Regarding the efficacy of 6-monthly paliperidone palmitate, none of the patients presented a psychotic decompensation after its administration, maintaining psychopathological stability after the change. The switch to 6-monthly paliperidone palmitate was made from both 1-monthly paliperidone palmitate and 3-monthly paliperidone palmitate, both showing the same efficacy. Regarding tolerability, all the patients who were administered 6-monthly paliperidone palmitate were previously treated with the monthly and quarterly presentation of the same molecule, having presented good tolerability to it, maintaining said tolerability after treatment. change to 6-monthly paliperidone palmitate, with no adverse reaction being recorded after the change. The adherence presented by the patients was very good, performing 100% of the administrations.
Conclusions6-monthly paliperidone palmitate may be an effective and well-tolerated treatment for the treatment of schizophrenia and other diagnoses such as bipolar disorder or borderline personality disorder. According to objective data, 6-monthly paliperidone palmitate could be an effective and well-tolerated treatment as an alternative to monthly and quarterly presentations of the same molecule. Longitudinal studies must be carried out to confirm this hypothesis.
Disclosure of InterestNone Declared
Miss attending risk factors in gynecological prenatal care among pregnant women at risk for dual pathology
- I. Caro-Cañizares, R. Carmona Camacho, C. Vidal Mariño, N. Lopez Carpintero, E. Baca Garcia
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S320
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Access to adequate healthcare is the best means we have for detecting and preventing complications during pregnancy and childbirth. Identifying and preventing factors that can interfere with this access become essential (Gulliford et al., 2002). Mother dual pathology during pregnancy is a condition with severe consequences (Cosp & Ontano, 2009). However there is scarce literature regarding barriers to obstetric care among women at risk for dual pathology.
ObjectivesThe main objective was to explore healthcare access barriers among pregnant women at risk for dual pathology.
MethodsFramed in a broader research (The WOMAP project) 2014 adult pregnant women less than 26 weeks of pregnancy were screened in five hospitals in Madrid (Spain) between 2016-2019. If the screening test (AC-Ok scale) identified the presence of dual pathology during the last month, women were included in the clinical trial and assessed with a more extensive battery (compound by PHQ-9; GAD-7; PCL-5; AUDIT; DAST; and Fagerström Test) and a semi-structured interview.
Results163 women at risk for dual pathology were assessed. Of them, 152 (93,2%) referred to having attended all scheduled appointments. Socioeconomic level (0.184, p=0.024), depression (-0.174, p=0.034), post-traumatic stress symptoms (-0.214, p=0.011) and alcohol reporting (-0.259, p=0.045) were significantly correlated with attendance level.
ConclusionsWomen with more severe symptoms of dual pathology are at higher risk for misatending obstetrical appointments. Social criticism, even subtle or unintentional, related to dual pathology during pregnancy could be restraining these women to attend properly. Thus, care providers should pay attention to women’s mental health and alcohol abuse to prevent miss-attention.
DisclosureNo significant relationships.
E-health treatments for Dual Disorders on pregnancy
- R. Carmona Camacho, N. Lopez Carpintero, I. Caro-Cañizares, L. Albarracin García, E. Baca Garcia, M. Sanchez Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S92-S93
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dual pathology during pregnancy, described as the co-occurrence of substance use and mental health problems, is one of the leading preventable causes of maternal and perinatal mortality and morbidity; however, effective and accessible treatments are lacking.
ObjectivesAs part of the WOMAP(Woman Mental Health and Addictions on Pregnancy) initiative, our study aimed to evaluate the effectiveness of an e-health-based psychotherapeutic program compared to enhanced usual care.
MethodsThis effectiveness clinical trial was conducted between 2016-2020 in 5 hospitals in the Madrid (Spain) metropolitan area. 2014 pregnant women under 26 weeks of pregnancy were screened. Eligible participants(n=120) were those who screened positive for co-occurring symptoms (AC-OK screener) and were not receiving specialized behavioral treatment. Participants were assessed in depth at baseline, 2,4,8 and 12 months(PHQ-9;GAD-7;PCL-5;AUDIT;DAST;Fagerström) and randomized to the usual care control group(n=38) or to two groups of a 10-session pregnancy-adapted psychotherapeutic program, one delivered by App/internet(n=41) and one by telephone(n=41). Intent-to-treat analyses assessed effectiveness.
ResultsStatistically significant effects of the intervention were found for mental health symptoms in the telephone group as compared to the control and App/internet groups, with an improvement effect starting earlier (2 months) and lasting longer (figures 1-3). Regarding substance use, due to the lack of other substances consumption, only smoking and alcohol cessation rates were analyzed. Patients in the App/internet and telephone groups discontinued significantly more, earlier and for a longer period compared to the control group(figures 4-5).
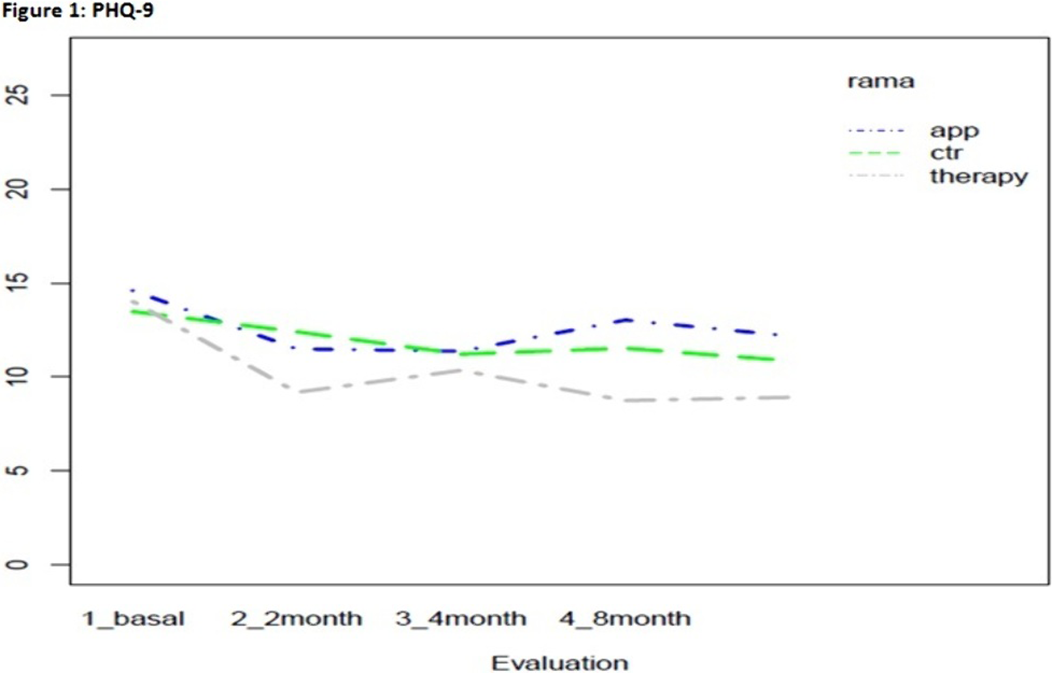
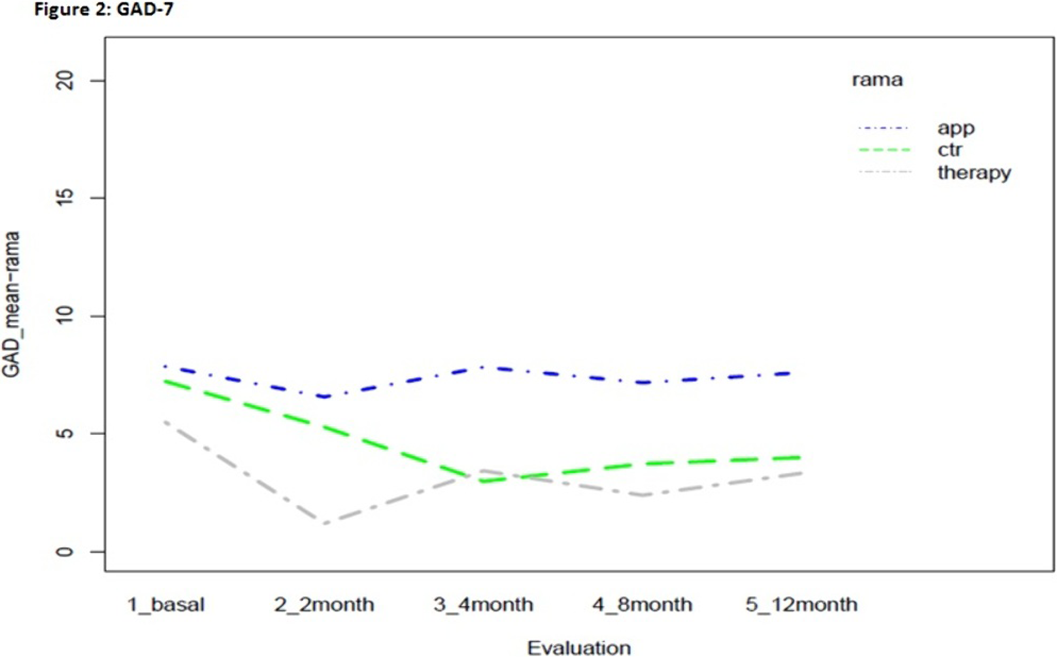
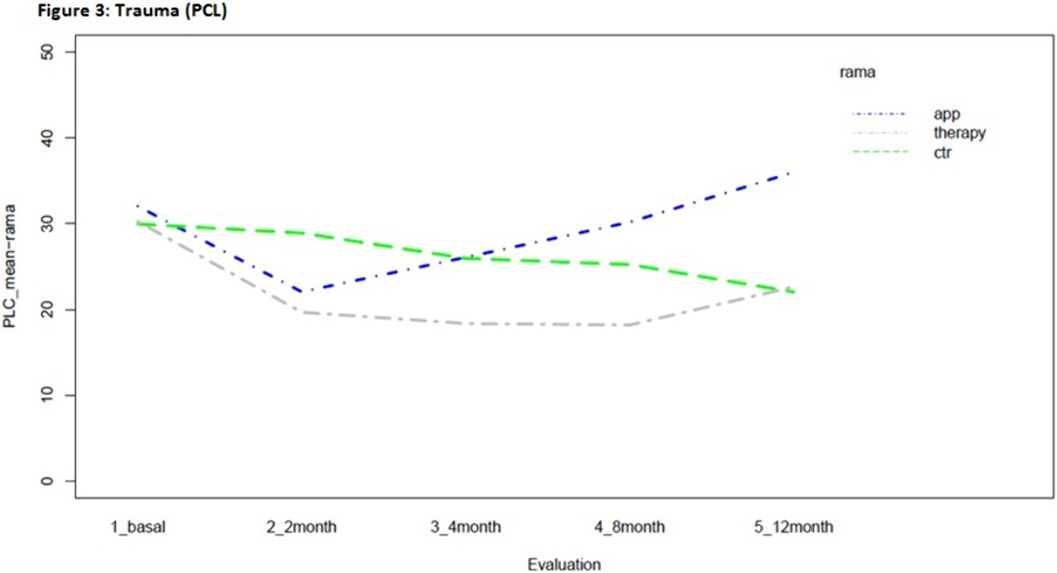
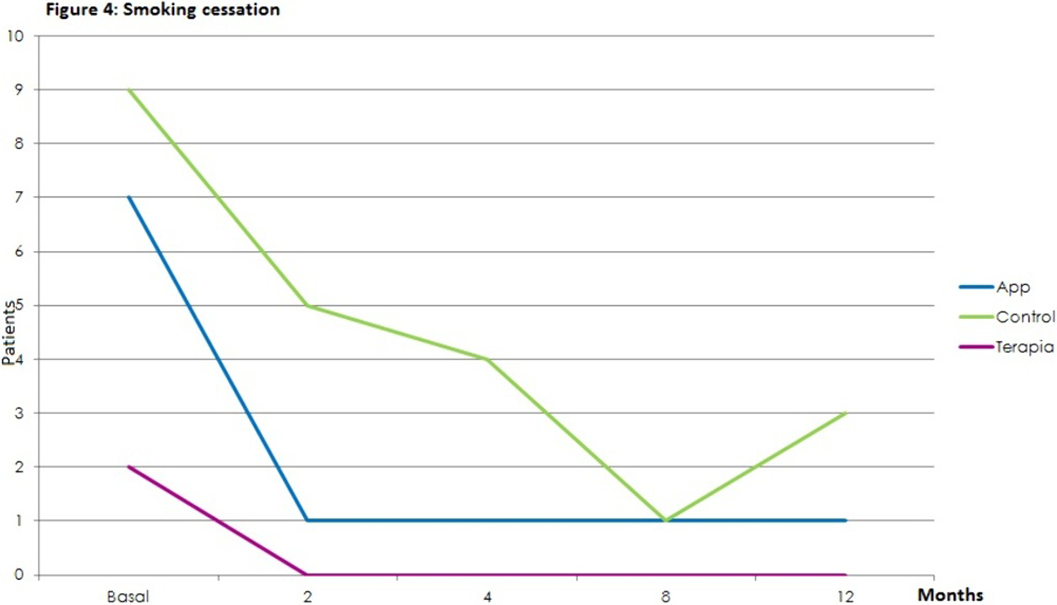
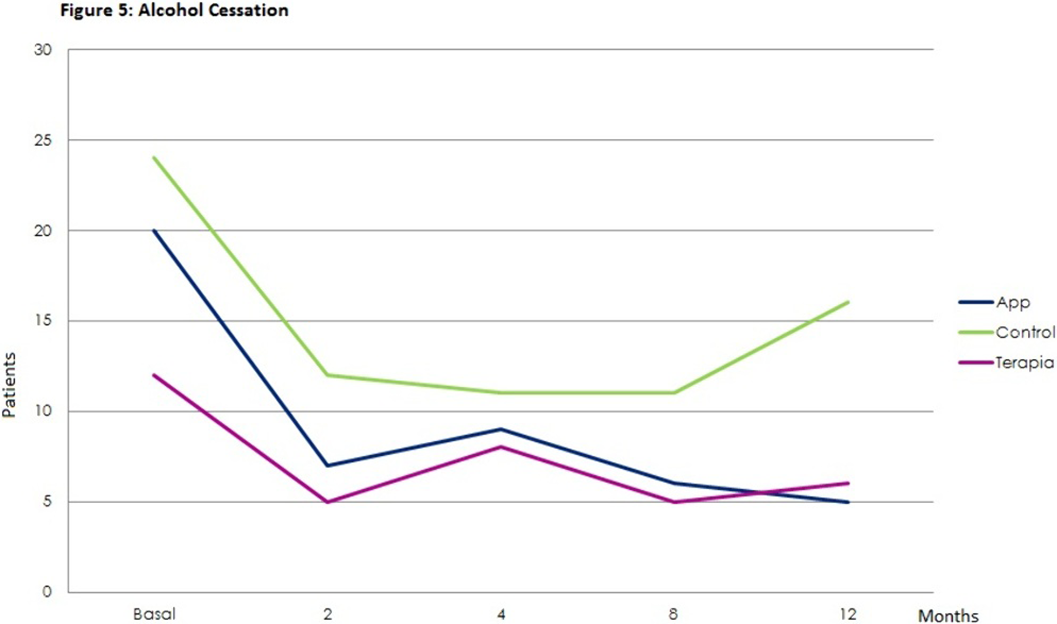 Conclusions
ConclusionsE-health psychotherapeutic programs could benefit pregnant women with dual disorders. An App/internet implementation could only be useful if focused solely on substances.
DisclosureNo significant relationships.
Pending challenges to e-mental health in the COVID-19 era: Acceptability of a smartphone-based ecological momentary assessment application among patients with schizophrenia spectrum disorders
- J.-D. Lopez-Morinigo, B.-E. Maria Luisa, A. Porras-Segovia, A. Sánchez-Escribano Martínez, P.-J. Escobedo-Aedo, V. González Ruiz-Ruano, L. Mata-Iturralde, L. Muñoz-Lorenzo, S. Sánchez-Alonso, A. Artés-Rodríguez, E. Baca-Garcia
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S343
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Concerns have been raised about ecological momentary assessment (EMA) acceptability among patients with schizophrenia spectrum disorders (SSD), which is of major relevance during the e-Mental health-focused COVID-19 pandemic.
ObjectivesTo investigate i) the levels of adherence to a passive smartphone-based EMA tool, the Evidence-Based Behavior (eB2), among SSD patients; and ii) putative predictors of this.
MethodsSample: SSD (F20-29-ICD10) outpatients, age 18-64, without financial incentives, recruited over 17/06/2019-11/03/2020 at the Hospital Universitario Fundación Jiménez Díaz (Madrid, Spain). Those who accepted the eB2 installation -users- and those who did not -non-users- were compared in sociodemographic, clinical, premorbid adjustment, neurocognitive, psychopathological, insight and metacognitive variables by a multivariable binary logistic regression model.
ResultsSample (N=77): n=41 males; age: 47.69±9.76 years, n=24 users (31.2%). n=14 users (70%) had the eB2 installed at follow-up (median=14.50 weeks).
Multivariable binary logistic regression model on ‘user’ as outcome β SE Wald p OR 95% CI Age -0.075 0.038 3.910 0.048 0.928 0.861-0.999 Education level -0.967 1.289 0.563 0.453 0.380 0.030-4.755 Early adolescence premorbid adjustment -0.285 0.110 6.695 0.010 0.752 0.606-0.933 Trail Making Test A -0.030 0.025 1.488 0.222 0.970 0.924-1.018 Trail Making Test B -0.005 0.010 0.278 0.598 0.995 0.976-1.014 Cognitive Insight 0.062 0.061 1.043 0.307 1.064 0.944-1.200 X2=25.296,df=6,p<0.001. Nagelkerke-R2=44.7%. Correctly classified: 76.9%, users:54.5%, non-users:88.4%.
ConclusionsAcceptability of a smartphone-based EMA application among SSD patients was low. Age (young) and good premorbid adjustment predicted acceptability. e-Mental Health methods need to be tailored for patients with SSD. Otherwise, these highly vulnerable individuals may be neglected by e-health-based services in the post-COVID-19 years ahead.
P03-37 - Testing A New Technique for the Rehabilitation of Schizophrenia and Other Psychoses Based on Viewing Fiction Films
- L. Caballero Martínez, M. Magariños, C. Pelaez, I. García del Castillo, R. Calero, I. Mateo, R. Diaz, E. Baca, C. Torre-Marin, M. Luz Chimeno de la Vega
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1147
-
- Article
-
- You have access Access
- Export citation
-
Fiction films offer unexplored opportunities of rehabilitation for schizophrenia and other psychoses. Schizophrenia produces deficits y distortions in the perception and comprehension of reality, also expressed in the perception and comprehension of films. After a year of an “ad hoc” experience, the following technique was developed:
1) Selecting a fiction film for its narrative, affective, cognitive and social cognitive content
2) Briefly presenting of the film to a group of 8-16 patients with diverse psychosis.
3) Screening of the film to the patients and the therapeutic team.
4) Summarizing of the plot by a patient. Group correcting of distortions and deficits caused by problems of attention and working memory, as well as positive, negative, affective and social cognitive symptoms (emotional perception, theory of mind, attributive style)
5) Selecting 1-2 sequences by each patient, and group commenting using the same technique.
6) Field recording of all the commentaries obtained.
7) Second screening of the film two days after, repeating points 2 to 6.
8) Comparing both field records.
An experimental study using this technique is presented. 8 patients with schizophrenia and other psychoses watched 4 fiction films (“The 39 Steps”, “Charade”, “M”, “The General”). The differences founded in both viewings by two external evaluators (using CGI and analogical scales of the main variables) are presented and commented. An evaluation of the perceived usefulness and satisfaction of the participants was included.
S09-02 - Diagnostic Stability of Psychiatric Disorders
- E. Baca-García, J. Lopez Castroman
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E109
-
- Article
-
- You have access Access
- Export citation
-
Diagnostic stability is the measure of the degree to which a diagnosis remains the same at subsequent assessments of the patient and constitutes a longitudinal validation of the original baseline diagnosis. Follow-up studies including evidence of diagnostic stability and diagnostic consistency over time have been proposed to test the validity of psychiatric diagnoses. Until this moment definitions for psychiatric diagnoses are based on expert opinion rather than on their biological basis, and the modest knowledge base regarding underlying etiologies has hindered the use of etiological factors in psychiatric classification systems. But it is assumed that the higher the diagnostic stability, the more likely is to reflect a consistent psychopathological or pathophysiological process. Being that the main clinical purpose of diagnosis, as a formulation, is to furnish the informational basis for planning and conducting clinical care, stability of a diagnosis gives a relevant base not only for prediction of the course and outcome of a disorder but also for effective planning and provision of treatment. The availability of longitudinal data, however, may cause significant fluctuations in diagnostic stability as changes in clinical presentation are seen. Thus, evolving longitudinal observations should lead to periodic updating of the comprehensive diagnostic formulation, and yet, despite the inherent problems derived from criteria based on cross-sectional observations, our diagnostic system relies on stable diagnoses. Accounting for the potentially harmful consequences of unsuitable treatment options or clinical interventions, the study of diagnostic stability remains an essential issue in psychiatry.
Patients with suicidal ideation in primary care: Clinical characteristics
- P. Martinez-Alfonso, P. Garcia-Parajua, J. Iglesias, L. de Ugarte, M. Magarinos, J.J. Carballo, L. Giner, E. Baca
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, pp. S327-S328
-
- Article
-
- You have access Access
- Export citation
-
Background and aims:
Up to 45% of individuals who commit suicide contact their Primary Care physician (PCP) the month before. The objective is to study clinical characteristics of patients presenting death and/or suicidal ideation (SI) in Primary Care.
Methods:195 patients attending their PCP were evaluated using systematic sampling in three Primary Care Centres. Patients completed the PHQ and a Life Changes Checklist. Demographic data, both psychiatric and medical conditions and treatments, visits to their PCP, and days out of work (last year) were also collected.
Results:24 patients had death or suicidal ideation for the previous two weeks (12,4%; IC95% 8,3-18,8%). Most of them (87,5%) had a mental disease, major depressive disorder (62,5%) and general anxiety disorder (50%). Patients with SI had more somatic symptoms (p<0,001), a greater number and score of recent life changes (p<0,001) and days out of work (last year) ((p=0,028) than the rest of the sample.
Compared to patients with any psychiatric disorder, patients with SI had more depressive symptoms (p<0,001) and a higher score in life changes in the 6-12 month period (p=0,044).
14 (58,3%) patients with SI had no previous psychiatric diagnosis and only 8 (33%) were receiving treatment.
Conclusions:In spite of a greater severity in depressive and other clinical characteristics of patients with SI most of them are not correctly detected and treated. Improving the rate of detection and treatment by the PCP of such patients would probably play a key role in the prevention of suicide.
P0201 - Primary versus secondary chronic insomnia in primary care
- M. Iza, P. Garcia-Parajua, B. Sanz-Aranguez, P. Martinez-Alfonso, L. Giner, M. Magariños, E. Baca
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, pp. S359-S360
-
- Article
-
- You have access Access
- Export citation
-
Background ans Aims:
Chronic insomnia (ChI) is a common condition in Primary Care (PC). Regardless that it's often related to psychiatric morbidity it appears to be a strong predictor of future depression and a disabling disorder by itself. The aim of this study was to measure and compare clinical and psychiatric characteristics of both patients with primary ChI and secondary ChI.
Methods:A random sample of 225 subjects older than 18 years old, from 3 PC Centres of the area of Madrid (Spain) was interviewed using the Oviedo Sleep Questionnaire, a semi-structured interview for sleep disorders. The subjects completed the Patient Health Questionnaire. Data about medical conditions, drug treatments, days of work lost (last year) and use of health care services (last 3 months), were also collected. Psychiatric and clinical characteristics between groups (primary vs secondary ChI) were compared.
Results:78 patients fulfilled criteria for ChI and 53 (67.9 %) of them were suffering from any psychiatric disorder (including subtreshold conditions). Patients with primary ChI compared to secondary insomnia patients had no significant differences in age, gender, use of health care resources and days of work lost. However, patients with secondary ChI compared to primary ChI had more somatic and depressive symptoms (U-Mann-Witney test; p=0.002 and p<0.001, respectively).
Conclussions:There is an important group of patients among PC attendees suffering primary ChI. Patients suffering primary ChI are comparable to patients with psychiatric disorders and insomnia in terms of days of work lost and use of health care resources.
Blood polyamine levels in drug-free schizophrenics
- C. Riaza Bermudo-Soriano, C. Vaquero-Lorenzo, M. Dîaz-Hernândez, M. Garda Dorado, P. Sânchez-Pâez, I. Durân Cristobal, R. Manzanero Estopinân, J. Gômez-Arnau, E. Baca-Garcîa, J. Pérez Piqueras, J. Sâiz Ruiz, A. Chinchilla Moreno
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 1492
-
- Article
-
- You have access Access
- Export citation
-
Background
Natural polyamines (putrescine, spermidine and spermine) are low molecular weight highly protonated aliphatic molecules that physiologically modulate NMDA, AMPA/kainate glutamatergic receptors and limbic dopaminergic neurotransmission. Previous studies had demonstrated that polyamine metabolism might be disrupted in schizophrenia, what could potentially be linked to glutamatergic dysfunction. In particular, polyamine levels in blood and fibroblast cultures from patients with schizophrenia had previously been found to be higher than in healthy controls. Indeed, a significant positive correlation between blood polyamine levels and severity of illness may exist.
MethodsIn order to test potential differences in blood polyamine levels between drug-free schizophrenia in-patients (n = 12), and healthy controls (n = 26, blood donors), spermidine (spd), spermine (spm), and spermidine/spermine index (spd/spm) were determined using HPLC after dansylation.
ResultsNo significant differences were found between groups (t = 0,974; df = 36; P = 0,337 for spd, t = l0, 52; df = 36; P = 0,959 for Spm, and, t = 0, 662; df = 36; P = 0,512 for spd/spm).
ConclusionsThough we couldn’t replicate previous findings suggesting disturbances in blood polyamine levels in schizophrenia, this issue may be a promising target. Future research should take into account possible factors such as sex, nutritional state, and stress.
P0084 - Characteristics of patients with undetected psychiatric pathology in primary care
- P. Garcia-Parajua, P. Martinez-Alfonso, M. Magariños, M. Iza, J. Iglesias, L. De Ugarte, E. Baca
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S327
-
- Article
-
- You have access Access
- Export citation
-
Background and Aims:
Previous data suggest that there is an important group of patients between primary care (PC) attendees suffering a psychiatric disorder that remain undetected. Our aim was to know data about this group of patients compared with patients without psychiatric pathology (PWP) and patients with already known psychiatric pathology (PKP).
Methods:A random sample of 225 subjects older than 18 years old, from 3 PC Centres of the area of Madrid (Spain) completed the Patient Health Questionnaire (PHQ). Data about medical and psychiatric conditions, drug treatments, days of work lost (last year) and use of health care services (last 3 months), were also collected. Psychiatric and clinical characteristics between groups were compared.
Results:50 (22,2%) patients were suffering a psychiatric condition according to PHQ but without recognition by their general practioner. This group of patients were younger than PWP and PKP (ANOVA; p=0,021 and p=0,013). They were suffering more depressive symptoms and somatic complaints than PWP (p<0,001 and p<0,001 respectively). In terms of days of work lost and use of health care services did not differ from PWP.
Conclusions:The results suggest that other reasons rather than the symptomathology (depresive symptoms, somatic complaints) may be important in the proccess of detection of mental health problems in PC. Both days of work lost and the number of visits to general practioner appear to be two determinant factors.
SAT-1 -1415T/C polymorphism and suicidal behavior
- C. Riaza Bermudo-Soriano, C. Vaquero-Lorenzo, E. Baca-García, M. Díaz-Hernández, J. Pérez-Piqueras, J. Sáiz-Ruiz
-
- Journal:
- European Psychiatry / Volume 26 / Issue S2 / March 2011
- Published online by Cambridge University Press:
- 16 April 2020, p. 812
-
- Article
-
- You have access Access
- Export citation
-
Background
A growing interest in the potential role of polyamines in stress, mood disorders and suicidal behavior has recently emerged. In particular, the expression of polyamine's rate-limiting catabolic enzyme (SAT-1, Spermidine/spermine N1-acetyltransferase-1) may be reduced in ventral prefrontal cortex and posterior cyngulate gyrus of patients who committed suicide. However, there is some controversy regarding the involvement of potential cis-acting loci controlling SAT-1 gene expression (rs6526342 or rs17286006) in suicidal behavior. Moreover, a significant association between SAT-1 rs1960264 SNP and anxiety disorders has been found in a male caucasian spanish sample.
MethodsIn order to test the potential association of SAT-1 -1415T/C SNP (rs1960264) with suicidal behavior, genotype frequencies for that SNP were compared between 193 suicidal attempters (126 female and 67 male) and 650 non-suicidal patients (314 female and 336 male) from an in-patient sample.
ResultsWe could not find a significant difference in the distribution of the genotypes for rs1960264 SNP between suicide attempters versus non-suicidal individuals (Linear-by-Linear association X2 = 0,203; df = 1; P = 0,652, females; Linear-by-Linear association X2 = 0,000; df = 1; P = 0,990, males). Neither could we demonstrate a relationship between rs1960264 genotype and past history of suicidal attempts (Linear-by-Linear association X2 = 2,966 ; df = 1; P = 0,085, females; Linear-by-Linear association X2 = 1,171; df = 1; P = 0,279, males).
ConclusionsAlthough we did not find a link between rs1960264 genotype and suicidal behavior, SAT-1 may be an interesting target to investigate the biology of this phenotype. Future studies should take into account other genetic polymorphisms at SAT-1, and definitively evaluate whether or not rs6526342 and rs1960264 have any functional implications.
Searching for Variables Associated with Familial Suicide Attempts Using Data Mining Techniques
- D. Saiz-Gonzalez, E. Baca-García, M. Perez-Rodriguez, I. Basurte Villamor, J. Saiz-Ruiz, J.M. Leiva-del Rio, M. De Prado Cumplido, R. Santiago-Mozos, A. Artes Rodriguez, J. De Leon
-
- Journal:
- European Psychiatry / Volume 24 / Issue S1 / January 2009
- Published online by Cambridge University Press:
- 16 April 2020, 24-E730
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Adoption, twin and family studies suggest that suicide behavior is familial and heritable. Both completed and attempted suicide appear to be transmitted in a familial form. Genetics and environment influences had been detected in various studies. But suicidal behavior suggests to be inherited independently from the mental disorders usually associated with it. While traditional statistics emphasizes inference and estimations, data mining emphasizes the fulfillment of a task such as classification, estimation, or knowledge discovery.
Objectives:The goal of this study was to determine in a large sample of suicide attempts which variables are associated with family history of attempted suicide.
Methods:In an emergency room, 539 adult suicide attempters were recruited. The two dichotomous dependent variables were family history of suicide attempt (10%) and of completed suicide (4%). Independent variables were 101 clinical variables explored with two data mining techniques: Random Forest and Forward Selection.
Results:A model for family history of completed suicide could not be developed. A classificatory model for family history of attempted suicide included the use of alcohol in the intent and family history of completed suicide, provide a sensitivity of 78.4%, a specificity of 98.7% and accuracy of 96.6%.
Conclusions:A classificatory model for family history of completed suicide could not be developed using data mining techniques. But it suggested that the use of alcohol in the intent and family history of completed suicide may be associated with familial attempted suicide.
Bordeline personality disorder in primary care: Characteristics and patterns of comorbidity
- M. Iza, L. Mata, J. Iglesias, L. de Ugarte, P. Garcia-Parajua, E. Baca
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, p. S175
-
- Article
-
- You have access Access
- Export citation
-
Background and aims:
Borderline personality disorder (BPD) seems to be a prevalent condition in Primary Care (PC) with high rates of comorbidity and health care use. The aim of this study is to describe the characteristics and patterns of comorbidity in patients with suspected BPD.
Methods:192 consecutive primary health care patients completed the IPDE screening questionnaire, CAGE and the Prime-MD patient questionnaire, and were interviewed by a general practitioner (GP) using the Prime-MD. Number of visits to the GP (last year), medical illnesses and treatments were also collected. “High Risk” of BPD group (RBPDg) was defined by scoring 4 or higher in the IPDE, and it was compared to patients without psychiatric morbidity and patients with any psychiatric disorder but not BPD's risk.
Results:39 (20,3%) patients fulfilled the condition of RBPDg. Compared to the group of patients without psychiatry pathology (n=110) RBPDg had a higher number of visits to their GP (last year) (p<0,001), more somatic complaints (p<0,001), a worse health perception (p<0,001) and higher rates of alcohol abuse or dependence (p=0,016).
In the RBPDg we found a high rate of axis I disorders, mainly major depressive disorder (MDD) (40,0%) and generalized anxiety disorder (33,3%). Furthermore, they had a lower level of education (p=0,03) and a higher rate of MDD (p=0,026) than patients with psychiatric pathology but without risk of BPD (n=43).
Conclusions:Borderline personality traits or disorder could be present in many depressive patients seen in PC. GP's knowledge about personality disorders needs to be improved
Consensus guideline for the evaluation of physical health in patients with schizophrenia
- J. Bobes, J. Saiz-Ruiz, M. Bernardo, M. Gutiérrez, M. Bousoño, J. Sanjuan, E. Baca-García, J. Mostaza, On Behalf of the Consensus Group of Experts in Physical Health in Patients with Schizophrenia
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, p. S105
-
- Article
-
- You have access Access
- Export citation
-
Background and aim
Patients with schizophrenia have a reduced life expectancy of 20% in comparison to the general population. They have a relative risk of 1.6 for all cause mortality. Recent innovations in antipsychotic treatment have improved the social integration of patients thanks to a better control of symptoms, however undesirable effects of medication may affect physical health.
ObjectiveTo develop a consensus document about the Evaluation of Physical Health of Patients with Schizophrenia along their life, and to propose recommendations for diagnostic and clinical interventions to manage modifiable risk factors which impact on quality of life and life expectancy.
MethodsA literature review was performed to identify diseases and/or risk factors potentially related to patient with schizophrenia.
A systematic review of the literature was performed to evaluate the morbid-morbidity of patients with schizophrenia in relation to the identified conditions. 25 psychiatrists and 8 experts from the different specialities participated in the consensus meeting to adapt the general population guidelines to the management of patients with schizophrenia.
ResultsThe literature review revealed that increased mortality in patients with schizophrenia is associated to respiratory diseases, cardiovascular diseases and cancer. Increased morbidity is associated to diabetes and metabolic syndrome, respiratory diseases, hepatitis, HIV and dyskinesia.
The resulting recommendations were submitted to the Spanish psychiatry medical societies for their validation.
ConclusionThe physical health of patients with schizophrenia requires specific monitoring and follow-up to guarantee that their life expectancy, quality of life and social functioning is similar to the general population.








