736 results
A case of steroid induced psychosis in a patient with mediastinal lymphoma
- B. Orgaz Álvarez, M. Velasco Santos, P. Ibáñez Mendoza, Á. de Vicente Blanco, G. García Cepero
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S317
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are a key part of many cancer treatment regimens and neuropsychiatric side effects have long been recognised. Steroid-induced psychosis is a disorder classified under substance or medication-induced psychosis in the Diagnostic and Statistical Manual of Mental Disorder, 5th edition. Management strategies include treatment with antipsychotic medication and reducing corticosteroid dosage.
ObjectivesTo describe the case of steroid induced psychosis in a patient with mediastinal lymphoma and provide a concise literature review.
MethodsClinical case report and brief literature review.
Results27-year-old male with a diagnosis of Stage IV Primary Mediastinal Lymphoma according to the Ann Arbor classification was admitted to the Haematology ward for chemotherapy treatment (R-DA EPOCH). Two days after admission the patient developed acute psychotic symptoms consisting of thought block, kinaesthetic hallucinations, and delusions. Prior to admission, the patient had been on corticosteroid treatment for two months (up to 8mg/day of dexamethasone), with a significant dose increase (up to 200mg/day of prednisone) at the beginning of chemotherapy treatment two days prior to symptom development. The patient had no personal or family history of mental health issues, no substance misuse and had not received any psychopharmacological treatment prior to admission.
Medical evaluations including a cranial CT scan, an MRI, EEG, blood tests and lumber puncture were all within normal parameters, discounting organic or metastatic causes for the symptoms.
Considering a potential episode of steroid-induced psychosis, the patient was started on olanzapine at a dosage of 10mg per day. The patient exhibited a positive response, with symptoms alleviating within 24 hours of the initial dose. In terms of corticosteroid therapy, haematologists adjusted the prednisone regimen to 100mg per day, and due to the encouraging progress, the olanzapine dosage was subsequently reduced to 5mg per day.
ConclusionsThis case underscores the importance of considering the possibility of steroid induced psychosis as a differential diagnosis specially in patients on high dose steroids presenting with psychotic symptoms. A multidisciplinary approach is crucial to ensure optimum treatment and care.
Disclosure of InterestNone Declared
Empathy as a predictor of burnout syndrome in health professionals of the Colombian Caribbean
- E. P. Ruiz Gonzalez, M. N. Muñoz Argel, A. M. M. Romero Otalvaro, M. G. Garcia Castañeda, M. C. Crespi
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S591
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Empathy is an essential skill in the doctor-patient relationship since it contributes to improve aspects of health care and patient satisfaction. Nevertheless, burnout research projects have been developed in recent years.
ObjectivesTo examine the predictive capacity that empathy has on burnout syndrome in health professionals.
MethodsA non-experimental, cross-sectional design was proposed. The type of study was correlational-descriptive since it was sought out to explore a functional relation through the prognosis of a criterion variable. Sample: 200 (100 female and 100 male).
ResultsFirst, the variance of cognitive and Affective Empathy was dug out in the emotional exhaustation criterion scale. Results accounted for 15% of variability in emotional exhaustation. (Corrected R 2 = .15, F = 17,56, p = 0,00). The best predictor of emotional exhaustation refers to Cognitive Empathy. (B = -.27, p = 0.00). It does not seem that Affective Empathy acts as a predictor variable of Emotional Exhaustation. (Table 1).
Table 1 Multiple linear regression analysis considering Emotional Exhaustation as a criterion.
TECA Corrected R2 F B p Cognitive Empathy .15 17,5 -.27** 0,00 Affective Empathy -.14 .13 The predictive capacity of Empathy in relation to Depersonalization was estimated (Corrected R 2 = .20, F = 25,4, p = 0.00). Cognitive and affective empathy were included as predictor variables and MBI as a criterion variable (Table 2). On one hand, the best predictor of Depersonalization is the Cognitive Empathy. On the other hand, regarding Affective Empathy, it does not act as a predictor of Depersonalization.
Table 2 Multiple linear regression analysis considering Depersonalization as a criterion.
TECA Corrected R2 F B p Cognitive Empathy .20 25,4 -.32** 0,00 Affective Empathy -.15 .84 Lastly, the predictive capacity of Empathy in relation to Personal Achievement was figured out. (Corrected R 2 = .19, F = 23,4, p = 0.00). Cognitive Empathy is the best predictor for Personal Fulfillment (Table 3).
Table 3 Multiple linear regression analysis considering Personal Fullfilment as a criterion.
TECA Corrected R2 F β p Cognitive Empathy .20 25,4 .43** 0,00 Affective Empathy .00 .96 ConclusionsIt was noticed that through a linear multiple regression analysis, the variable that best explains Emotional Exhaustation is Cognitive Empathy. Those results are replicated for Depersonalization and Personal Fullfilment.
Disclosure of InterestNone Declared
Descriptive study of suicidal behavior in adult population attended in an emergency department during a one-year period and comparative study with the following annual period
- M. GARCÍA MORENO, A. DE COS MILAS, L. BEATOBE CARREÑO, A. IZQUIERDO DE LA PUENTE, P. DEL SOL CALDERON, R. DE ARCE CORDON
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S783-S784
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most frequent psychiatric emergency. About 1% of all deaths are due to suicide so around 700,000 people commit suicide each year. Suicide attempt is more frequent in women (3:1) while completed suicide is more frequent in men (4:1). Most suicides occur in the 35-64 age range. The severity of a suicide attempt is assessed in terms of method, potential lethality, rescuability and impulsivity. A previous suicide attempt is the main risk factor for suicide behavior. The majority (more than 90%) of suicide behavior are related to an underlying psychopathology, mainly depression and substance abuse, especially alcohol. However, there are also numerous cases of impulsive attempts in the context of life stressors.
ObjectivesTo analyze sociodemographic and clinical characteristics of adult patients with suicidal behavior attended in the emergency department during a one-year period. To study the stability of the data obtained in the following annual period
MethodsA retrospective review of the population over 18 years attended in the emergency department during 2022 because of suicidal behavior, was carried out. Data collection for the year 2023 is in progress in order to be able to carry out a comparative study between both annual periods.
Results562 patients over 18 years were attended in the emergency department of our hospital due to suicide behavior during 2022. 383 of these patients were women (68.1%) and 179 men (31.9%). with an average age of 38.6 and 42.2 years respectively. The age range between 18 and 25 years accounted for 28.5% of the total cases. The most frequent suicidal behavior was medication overdose with a total of 307 (54.6%), being more frequent in women than in men (2.6:1). The second most frequent reason for attention was suicidal ideation without suicide attempt, with a total of 212 patients (37.7%). 371 patients were discharged home from the emergency department (66%) and 191 required a longer observation in hospital environment. We are awaiting to complete data collection for 2023 to establish a comparison with those described above.
ConclusionsAccording to our study, suicidal behavior in adult population is more frequent in women than in men. The most frequent age range in both genders was between 18 and 25 years old. The method most frequently used was medication overdose and suicidal ideation without a suicide attempt was the second most frequent reason of attention. Our patients mostly presented diagnoses of personality disorder, depression and substance use disorder.
Disclosure of InterestNone Declared
Differential diagnosis between frontotemporal dementia and bipolar disorder, review and case report
- M. García Moreno, A. De Cos Milas, L. Beatobe Carreño, P. Del Sol Calderón, A. Izquierdo de la Puente
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S639
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dementia can present with psychiatric symptoms even before the cognitive impairment, which makes difficult to establish an adequate diagnosis. There have described symptoms of this type in vascular dementia, frontotemporal dementia, Alzheimer disease and Lewy bodies dementia. Frontotemporal dementia has a prevalence of 9-20% and it`s the third in frequency among degenerative dementia. It appears before the age of 65 years old and is more common in men. Two variants have been described, linguistic and behavioral. The behavioral one has usually an initial psychiatric presentation, with behavioral disorders, disinhibition and personality changes. Therefore it`s important to make an adequate differential diagnosis with late onset bipolar disorder.
ObjectivesTo review about frontotemporal dementia and its differential diagnosis with late onset bipolar disorder.
MethodsWe carry out a literature review about frontotemporal dementia and its differential diagnosis with late onset bipolar disorder, accompanied by a clinical description of one patient with behavioral disturbance and language disorder.
ResultsA 59-year-old female was admitted to the short-term hospitalization unit from the emergency department due to behavior disorder. She had no relevant personal or familiar psychiatric history up to two years before when she received diagnosis of bipolar disorder. She presented behavioral disorganization, psychomotor restlessness, verbal aggressiveness, verbiage, insomnia and decreased intake. Psychopathological examination became difficult due to her language disorder since she presented an incoherent speech with paraphasias and loss of the common thread. Neurological study guided diagnosis to frontotemporal dementia even though they left the psychopharmacological treatment to our discretion. Olanzapine 5 mg twice a day was initiated, and behavioral improvement was observed. However, the patient maintained a significant functional impairment.
ConclusionsPsychiatric presentation is frequent in dementia, even before cognitive failures which makes essential an exhaustive differential diagnosis. It`s important to consider the diagnosis of frontotemporal dementia in those patients who debut with behavioral disturbance in the 50s. Psychopharmacological treatment is only symptomatic so functional recovery should not be expected.
Disclosure of InterestNone Declared
Relation between biomarkers and suicide attempts in patients with schizophrenia
- A. Garcia Fernandez, C. Martínez-Cao, M. Couce-Sánchez, L. González-Blanco, P. Sáiz, P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S125
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
An increased risk of suicide has been reported by psychiatric patients, including schizophrenia1. Numerous evidence suggests alterations in the grade of pro-inflammatory impact on suicidal behavior2, and this relation has been shown in patients with mood or anxious disorders3,4. However, the grade of inflammation impact suicidal behavior in patients with schizophrenia has hardly been investigated.
ObjectivesIdentify peripheral blood biomarkers of suicidal behavior in patients with schizophrenia, including inflammatory and lipid profile parameters.
MethodsSecondary analysis of a cross-sectional study. Sample: 254 patients with schizophrenia, aged 18-72. Assessments: ad-hoc demographic and clinical questionnaire, PANSS, CDS, CAINS, PSP. Inflammatory and lipid parameters: C-reactive protein (PCR), interleukin 6 (IL-6); high-density lipoprotein cholesterol (HDL-C), low density lipoprotein cholesterol (LDL-C), total cholesterol (TC), triglyceridaemia (TG). Statistical analysis: Correlations, T Student, U Mann-Withney and lineal regression.
ResultsMean age: 40.49 (13.10). Men: 64.2%.
No statistically significant differences were found between patients with suicide attempts and those without in any of the inflammatory or lipid parameters (p>0.05). However, differences were found in terms of suicide attempts (yes/no) in the PANSS negative (T=-2.217; p=0.028) and PANSS general psychopathy (T=-4.224; p< 0.001), in depressive symptoms (T =-6.967; p< 0.001), and the MAP subscale of the CAINS (T= -3.741; p<0.001).
Among patients with suicide attempts (n=42; 16.52% of the sample) (mean=1.90; sd=1.73; Range:1-7), statistically significant correlations were found with PCR (r=0.309; p=0.046), but not with cytokines and lipid parameters. On the other hand, no correlations were found with age, sex, length of illness, and any of the clinical scales.
A multiple linear regression was performed considering the number of suicide attempts as the dependent variable and as independent variables, age, sex, and those that were significant in the bivariate analysis (PCR).
A predictive model was found that explains 9.60% of the variance of number of suicide attempts (F = 4.224; p < 0.001). The variable that entered the model was PCR (β= 0.309; p=0.046).
ConclusionsThe increase in inflammation (manifested by the elevation of PCR) is related to an increase in the number of suicides. On the contrary, no correlations were found with lipid parameters or interleukins.
Disclosure of InterestNone Declared
Mania and alzheimer disease, review and case report
- M. Garcia Moreno, A. De Cos Milas, L. Beatobe Carreño, P. Del Sol Calderón, A. Izquierdo de la Puente
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S638-S639
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There are numerous organic causes that can be related to affective symptoms such as neurological, metabolic, infectious and pharmacological. Neurological conditions associated to affective symptoms include vascular lesions, tumors, infections, seizures and dementia. Within cognitive impairment conditions, depressive symptoms are more frequent in vascular dementia and Alzheimer disease, and behavioral or manic symptoms in frontotemporal dementia although we cannot rule out less common associations.
ObjectivesTo review about organic mania due to dementia
MethodsWe carry out a literature review about organic mania accompanied by a clinical description of one patient with manic symptoms and cognitive impairment.
ResultsA 80-year-old male was admitted to the short-term hospitalization unit from the emergency department due to maniform symptoms. He had believed for weeks that he was millionaire and capable to cure all the diseases in the world, reason for which he had given away many of his belongings and had tried to register the patent for his invent. He also had future plans to invest all the money he earned from the patent in the construction of roads in Latin America. He had not previous history of mental illness. Neurological study concluded a diagnosis of Alzheimer disease. It was treated as a manic episode with a mood stabilizer and antipsychotic, with partial resolution of the condition.
ConclusionsIt is common to find depressive symptoms in cognitive disorders. Although manic symptoms are much more frequent in frontotemporal dementia or other organic disorders, we can also find them in patients with Alzheimer disease. Since there is no specific curative treatment for this disease, concomitant psychopharmacological treatment is recommended if manic symptoms appear.
Disclosure of InterestNone Declared
Short-chain fatty acids in schizophrenia: are they affected by a depressive state?
- M. Couce-Sánchez, G. Paniagua, L. González-Blanco, A. García-Fernández, C. Martínez-Cao, C. Sabater, A. Margolles, J. Bobes, M. P. García-Portilla, P. Sáiz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S765-S766
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Short-chain fatty acids (SCFA) are bacterial metabolites that, within microbiome-gut-brain axis, make a promising research line on etiopathology of mental diseases like schizophrenia (SZ) and major depression disorder. Besides, depressive symptoms are frequent clinical features of SZ.
Objectives- Describe fecal SCFA concentrations in SZ patients.
- Analyze differences in SCFA depending on:
- Depression.
- Clinical severity, antipsychotics and antidepressants, comorbidities (pro-inflammatory state/obesity/metabolic syndrome [MetS]), lifestyle.
MethodsCross-sectional study of 67 outpatients [mean age=43.52±12.42, range=22-67; males=40 (59.7%)] with diagnosis (DSM-5) of SZ recruited from their mental health clinics in Oviedo (Spain).
- Assessment:
- Fecal SCFA (gas chromatography;μg/mL).
- Plasmatic C-reactive protein (CPR;mg/dL).
- PANSS, Calgary Depression (CDS), International Physical Activity (IPAQ), Mediterranean Diet Adherence (MEDAS).
- Toxic habits (alcohol use/smoking/cannabis).
- Chlorpromazine equivalent doses (CPZ-ED), use of antidepressants.
- MetS (ATP-III), body mass index (BMI; kg/cm2).
- Statistics: Spearman correlation, U Mann-Whitney, ANCOVA.
Results14 patients showed clinical depression (CDS≥5). There were no differences in age or sex between groups. 36 patients (53.7%) showed systemic low-grade inflammation (CPR≥0.3mg/dL) and 32 (30.8%) MetS.Table 1 shows fecal SCFA levels by depressive state. Means (SD) are ahown.
Table 1 CDS≤4 CDS≥5 Total U Mann-Whitney (p-value) Acetate 21.449(12.823) 12.911(7.189) 19.665(12.328) 221.000(0.021) Propanoate 9.170(6.819) 6.848(6.036) 8.685(6.687) 268.500(0.114) Butyrate 8.529(6.436) 7.875(8.232) 8.392(6.787) 320.000(0.432) Total SCFA 39.148(23.770) 31.415(24.526) 36.742(23.549) 250.000(0.062) Correlations were found in Age with Butyrate (r=-0.248,p=0.043) and weekly alcohol units with Propanoate (r=0.250,p=0.041) plus trend to significance with Butyrate (r=0.232,p=0.059). It also showed a trend towards statistical relation for CPZ-ED with Propanoate (r=-0.253,p=0.039) and Total SCFA (r=-0.253,p=0.039). We found no correlation in SCFA with MetS, CGI, PANSS-N, BMI, IPAQ, MEDAS and other toxic habits.
ANCOVA was performed to Acetate and Total SCFA using depression state as independent variable and Age and CPZ-ED as covariates. There was a trend towards statistical significance for Acetate (F=3.937,p=0.052,η2=0.059) whereas Total SCFA showed no difference (F=1.350,p=2.250,η2=0.021).
ConclusionsThere seems to be lower levels of fecal Acetate in SZ patients with depressive symptoms, considering age and antipsychotic intake. In our sample there was no relation between SFCA and clinical severity, lifestyle, comorbidities or antidepressant use.
Disclosure of InterestNone Declared
Descriptive study of adolescents hospitalized in the Psychiatric Unit of a hospital in Madrid, Spain
- P. Del Sol Calderon, A. Izquierdo de la Puente, R. Fernández, M. García Moreno, L. Mallol, I. Palanca
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S102
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
An increase in suicidal behavior among the adolescent population is reflected in the literature and in clinical practice. According to a study of suicidal behavior and mental health by the Spanish ANAR Foundation, the number of cases with suicidal behavior has experienced an accentuated growth in the period 2012-2022 (1,921.3%), highlighting the increase produced in the post-COVID-19 period, between 2020 and 2022 (128%)
ObjectivesTo analyze the reasons for admission to the short hospitalization unit. To describe the sociodemographic characteristics of hospitalized adolescents.
MethodsDescriptive observational study of the sample of adolescents admitted to the inpatient psychiatric unit of the Hospital Universitario Puerta de Hierro between January 1, 2023 and June 30, 2023. It is carried out through the information obtained in the clinical history of the patients.
ResultsDuring this period of time 113 adolescents were admitted, 80.2% were female. The mean age was 15.16 years. The main reason for admission was autolytic ideation, occurring in 33.3% of the patients. The second most frequent reason for admission was suicide attempt (29.7%) and behavioral disturbance (17.1%) was the third most frequent. Of the methods used in suicide attempts, drug overeating stands out among the methods used in suicide attempts. (75.8%), followed by attempted hanging (12.1%) or cutting (12.1%).
Image:
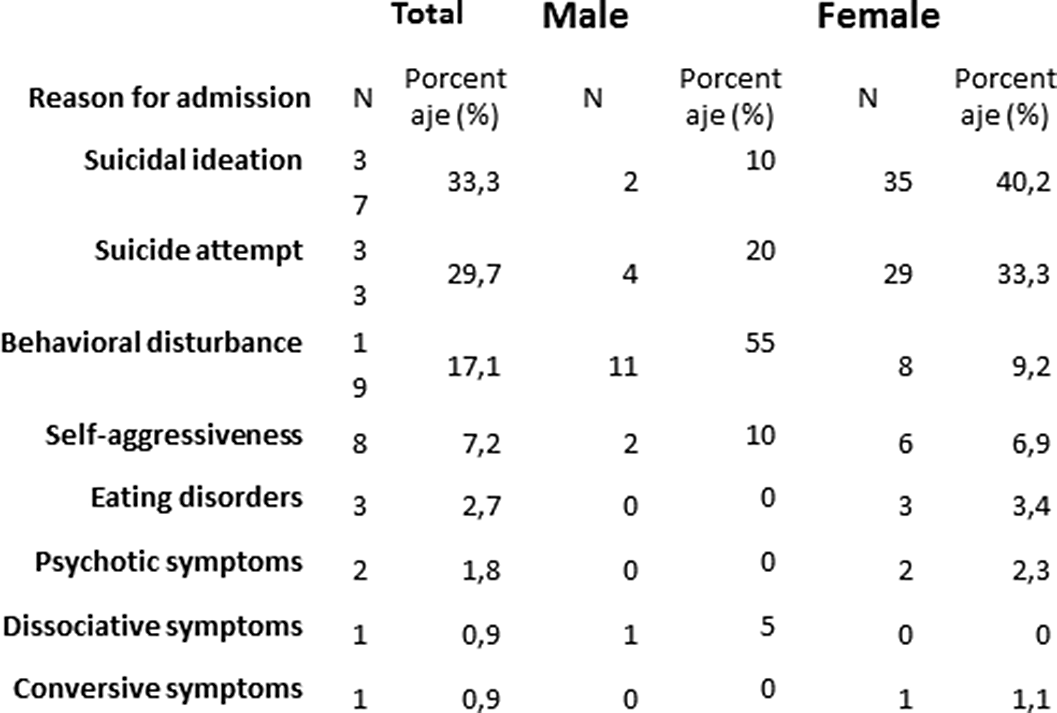 Conclusions
ConclusionsThe results corroborate what is reported in the scientific literature, where self-harm and self-injury attempts have increased and are the most frequent reasons for admission. This shows that suicide is a public health problem of the first order, where prevention and early intervention programs are necessary.
Disclosure of InterestNone Declared
Suicidality and social cognition: the association between hypomentalizing and suicide lethality
- J. Andreo-Jover, K. March, E. Fernández-Jiménez, J. Fernandez Fernandez, A. Garcia Fernandez, M. P. Lopez Peña, M. Ruiz Veguilla, B. Crespo Facorro, N. Garrido Torres, A. Cebria, I. Grande, N. Roberto, W. Ayad-Ahmed, A. Pemau Gurumeta, A. Garcia Ramos, M. Diaz-Marsa, M. F. Bravo-Ortiz, A. Palao-Tarrero, V. Perez-Sola
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S183
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide attempts (SA) leading to highly lethal consequences have been associated with heightened suicide planning (Barker et al., 2022), along with deficits in social cognition (Levi-Belz et al., 2022). Hypomentalizing, characterized by excessive uncertainty regarding mental states, may contribute to heightened social withdrawal and an increased risk of SA (Nestor & Sutherland, 2022). Although certain studies have identified a connection between hypomentalizing profiles and self-harm (Badoud et al., 2015), research into the lethality of SA remains limited.
ObjectivesThis study aimed to explore the association between hypomentalizing and SA lethality.
MethodsOur study encompassed a cohort of 1,371 patients who committed a SA. We conducted assessments of mentalizing using the RFQ-8 instrument, and evaluations of suicidal ideation and behavior employing the CSRSS questionnaire. Demographic and clinical characteristics were compared using the T-student and Chi-square tests. To investigate the relationship between hypomentalizing and the SA lethality, we employed logistic regression models.
ResultsDescriptive date are presented in Table 1. Our results show that hypomentalizing do not predict a higher SA lethality. Additionally, hypomentalizing increased the risk of SA planning (p≤0.001, B=-0.182), and SA planning predicted a higher SA lethality (see Table 2).
Table 1. Means Comparison for low and high lethality (N=1371)
Low lethality N=539 High lethality N=832 p value Effect size Age, mean (SD) 38.65 (15.65) 41.91 (15.37) ≤0.001 -0.209a Female sex, N (%) 392 (72.7) 571 (68.6) 0.116 0.044b Educational years, mean (SD) 12.45 (2.99) 12.43 (3.41) 0.890 0.0076a Employed, N (%) 220 (41.2) 332 (40) 0.692 0.012b Suicide Ideation, N (%) 475 (88.1) 742 (89.2) 0.541 0.016b Suicide Planning, N (%) 159 (39.2) 400 (58.1) ≤0.001 0.183b Number of attempts, mean (SD) 3.28 (5.48) 3.63 (5.74) 0.269 -0.169a RFQ, mean (SD) 4.68 (1.27) 4.56 (1.32) 0.087 0.095a Table 2. Logistic regression analyses for high SA lethality (N=1371).
Univariate analysis Multivariate analysis OR p value OR p value Age 1.014 (1.007-1.021) ≤0.001 1.014 (1.005-1.022) 0.001 Female sex 0.820 (0.646-1.042) 0.105 Educational years 0.998 (0.965-1.031) 0.890 Employed 0.952 (0.763-1.187) 0.660 Suicide ideation 1.111 (0.790-1.562) 0.545 Suicide planning 2.150 (1.674-2.761) ≤0.001 2.183 (1.697-2.808) ≤0.001 Number SA 1.012 (0.990-1.034) 0.277 RFQ 0.929 (0.854-1.011) 0.088 ConclusionsWhile the association between hypomentalizing and high SA lethality was not significant, a discernible trend toward such relationship can be noted. Further studies examining the moderating effects of planning in the association between hypomentalizing and SA lethality are required.
Disclosure of InterestNone Declared
Drug-induced psychosis and intravenous drug use in chemsex context
- J. Curto Ramos, A. Rodríguez Laguna, P. Barrio, L. Ibarguchi, A. García, I. Azqueta, H. Dolengevich Segal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S413
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies have called atention to the mental health disorders associated with chemsex -the intentional use of drugs before or during sexual intercourse GBMSM (gay, bisexual and men who have sex with men) population-. Sexualized intravenous drug use is also known as slam or slamsex. There are few studies that analyze the mental health differences between intravenous drug users compared to non-intravenous drug users in chemsex context.
ObjectivesWe aim to analyze the relationship between the practice of slamsex and the development of drug-induced psychosis.
MethodsA cross-sectional descriptive analysis of a sample of users attended by the non-governmental organization Apoyo Positivo in the program “Sex, Drugs and You” between 2016-2019 was performed.
ResultsWe included 217 participants. Drug-induced psychosis was found in 80 participants. Drug-induced psychosis was significantly higher in the intravenous drug use group compared to the non-intravenous drug use group (p<0.05).
ConclusionsPrevious studies have reported that MSM who practiced chemsex were more likely to experience from different mental health disorders, being psychosis one of the most frequent psychiatric diagnoses. In our study, drug-induced psychosis was higher in participants who engaged in intravenous drug use. Further studies analyzing the relationship between slamsex and drug-induced psychosis are needed.
Disclosure of InterestNone Declared
Transcranial Magnetic Stimulation and its Efficacy in Alleviating Depressive Symptoms in Patients with Suicidal Ideation
- A. Moleon, M. Martín-Bejarano, P. Alvarez de Toledo, I. Perez, J. Narbona, M. García-Ferriol, R. Perea, J. M. Oropesa, J. Torres
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S181
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a global public health issue. According to the latest available data from the National Institute of Statistics, 4,003 people died by suicide in 2021, reaching a new historical high. Approximately 90% of suicide victims suffer from one or more severe psychiatric disorders, and there is a documented 20-fold higher risk of suicide in individuals with affective disorders compared to healthy subjects (Abdelnaim et al., 2020). Repetitive transcranial magnetic stimulation (rTMS) has been established as an effective alternative or complementary treatment option for patients with depressive disorders, but little is known about its effects on suicide risk.
ObjectivesTo assess the efficacy of rTMS in reducing depressive symptoms in patients with suicidal ideation and behaviors.
MethodsPopulation and Methods: A retrospective analysis was conducted on a sample of 28 psychiatric patients (23 females; mean age 49.36 ± 16.23) with suicidal ideation identified by item 3 (suicidality) of the Hamilton Depression Rating Scale (HDRS), who were treated with rTMS. All patients received a minimum of 30 sessions, consisting of the application of a high-frequency (>10Hz) or intermittent theta burst stimulation (TBS) over the left dorsolateral prefrontal cortex (DLPFC) at an intensity of 120% of the resting motor threshold (RMT), and repeated low-frequency pulses (1Hz) or continuous TBS over the right DLPFC with an intensity of 110% of the RMT.
ResultsResults: The results show a statistically significant improvement in depressive symptoms following rTMS intervention (p < 0.001). Furthermore, remission was observed in 46% of the sample (HDRS < 8).
ConclusionsDiscussion: In line with recent studies (Abdelnaim et al., 2020; Hines et al., 2022) and systematic reviews (Cui et al., 2022; Bozzay et al., 2020) on suicidal ideation in the context of psychiatric disorders, the findings of this study demonstrated that rTMS achieved satisfactory results in reducing depressive symptoms and suicidal ideation.
Conclusions: This clinical study indicates preliminary promise for the prevention of suicidal acts and underscores the need for more detailed and specific research on rTMS in the field of suicide.
Keywords: rTMS, neuromodulation, depression, suicide.
Disclosure of InterestNone Declared
Grading of Recommendations of psychological interventions in the rehabilitation of patients with schizophrenia
- R. Vazquez-Noguerol Mendez, S. Garcia Pineiro, P. G. S. Perez, M. Puime Miguez, C. Cinos Galan, M. J. Veiga Candan, M. Suarez Baldomir, M. Soriano Garcia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S741
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
As part of the intervention, patients with severe schizophrenia who are cared for in psychiatric rehabilitation units need psychological treatments. However, there is great variability within the psychotherapy alternatives that are proposed for rehabilitation in schizophrenia, and it is necessary to know which are the most efficient interventions in order to prioritize their inclusion in intervention programs.
ObjectivesTo know the level of evidence of the existing psychotherapy alternatives for the rehabilitation treatment in schizophrenia through the systematic review of recently published studies.
MethodsConsecutive systematic searches in the scientific literature were used in a sensitive and specific way, aimed at identifying the existence of documents in databases and clinical practice guidelines based on evidence of psychological treatment in schizophrenia. Psychosocial and social approaches and family members interventions were excluded, and the search was limited to the last 5 years. The PICO format has been used, and a subsequent critical reading using the AGREE II tool, considering the inclusion criteria of presenting a score >60% in 4 domains.
ResultsThe following interventions have been found to be therapeutically effective: Level 1B (Early intervention in Psychosis; Patient and Family psychoeducational intervention; Basic ando social skills training; Social cognition and Metakognition training; Cognitive Remediation; Cognitive Behavioral Individual Therapy; Assertive Community treatment; Supported employment). Level 2B (Family Problem Solving Therapy, Dynamic Psychotherapy; Cognitive Behavioral Group Therapy); Level 2C (Horticultural, Art, Music, Animals Therapies).
ConclusionsSeveral psychotherapy alternatives are proposed for rehabilitation in schizophrenia, with known level of evidenca in order to prioritize their inclusion in intervention programs.
Disclosure of InterestNone Declared
Psychiatry resident physician duty hours, resting times and European Working Time Directive compliance in Spain
- J. P. Carrasco Picazo, D. A. Sánchez Martínez, P. Estrella Porter, R. Ruiz-Montero, A. H. Aginagalde Llorente, E. García-Camacho, J. Navarro, A. Cerame del Campo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S393-S394
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a growing interest in understanding the impact of duty hours and resting times on training outcomes and the well-being of resident physicians. Psychiatry resident’s duty hours in Spain comprise a regular working schedule of 37.5h per week and a minimum of 4 mandatory on-call shifts. The most recent duty hours regulations in Spain were transposed from the European Working Time Directive (EWTD). According to Spanish Law, doctors cannot work for more than 48h per week and need to have resting times per day (at least 12h), per week (at least 36h) as well as annual leave (at least a month). However, there is practically no data on this situation in psychiatry resident physicians.
ObjectivesOur aim is firstly, to describe the number of shifts performed by psychiatry resident physicians in Spain. Secondly, to describe compliance with the daily and weekly rests compared to those set in national and European law. Finally, to analyse the difference by demographic variables (gender and year of residency), in both the number of on-call duty shifts and compliance with rests.
MethodsA descriptive cross-sectional study was designed through an online survey adapted from the existing literature. The target population were Spanish psychiatry resident physicians undergoing PGT who started their specialist training during the years 2018–2021. The survey was disseminated through the Spanish regional medical councils to all active psychiatry resident physicians by mail as well as through informal communication channels. The study was authorised by the Spanish Medical Organization’s General Assembly which is the highest ethical and deontological body of physicians in Spain.
Results55 responses were obtained, of which 61.82% identified as females. The mean number of on-call shifts in the last 3 months was 14.05. This mean was highest in women 14,32 and in the cohort of 2020 15.46 (first year of residency). Among the resident physicians surveyed, 66.07% exceeded the 48h per week limit set by the EWTD and 7% of them did not rest after a 24-h on-call shift. Furthermore, 22% of respondents did not have a day-off after a Saturday on-call shift. The mean working hours when not resting after an on-call-shift were 7 hours. The comparison by gender and year of residency of the main variables can be seen in figures 1 and 2 respectively.
Image:
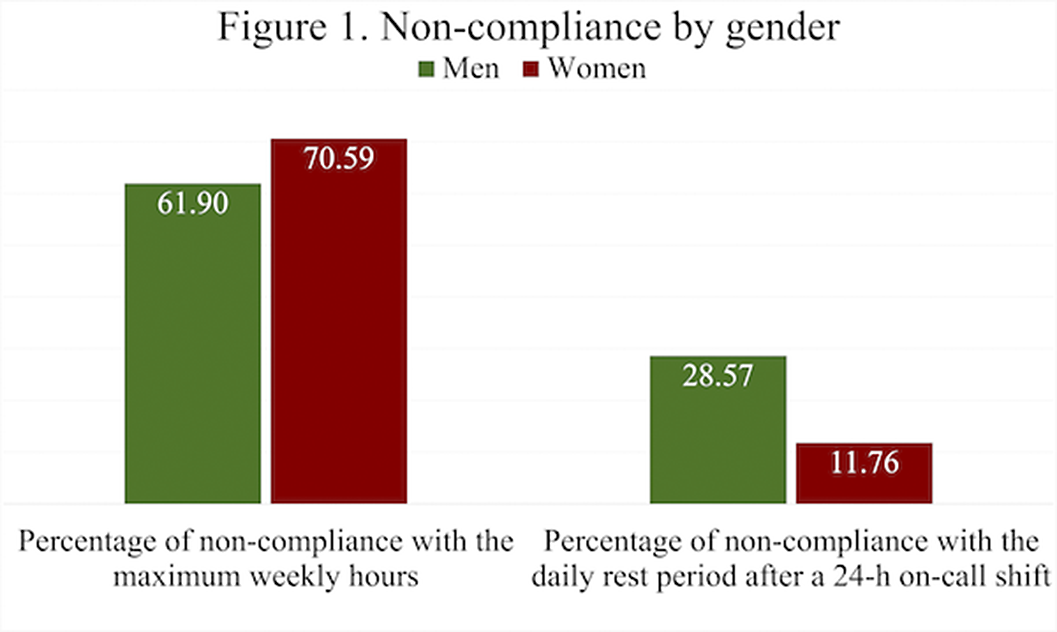
Image 2:
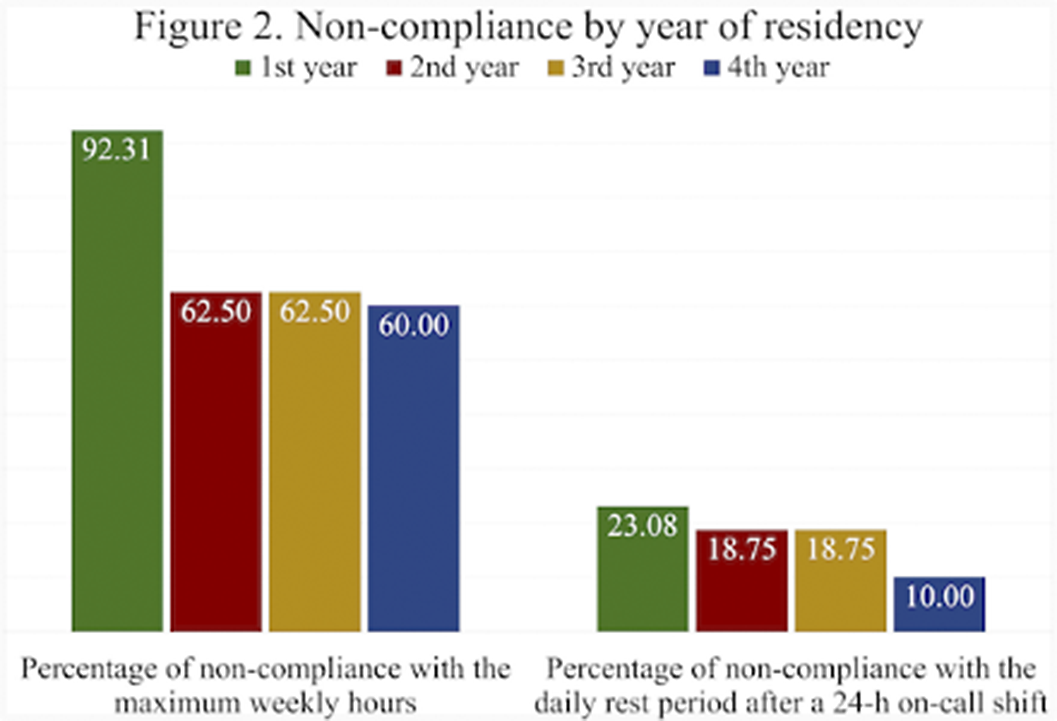 Conclusions
ConclusionsPsychiatry resident physicians in Spain greatly exceed the established 48 h/week EWTD limit. Likewise, non-compliance with labour regulations regarding mandatory rest after on-call duty and minimum weekly rest periods are observed. Differences can be seen by gender and year of residency. The situation described could potentially create a high-risk situation for the health and psychosocial well-being of resident physicians, hinder learning outcomes and could lead to suboptimal patient care.
Disclosure of InterestNone Declared
Use of aripiprazole long-acting injectable release as a stabiliser. About a case
- A. Izquierdo De La Puente, P. del Sol Calderón, R. Fernandez Fernandez, M. V. da Silva, M. Garcia Moreno
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S435-S436
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 56-year-old patient diagnosed with bipolar affective disorder type II, who remains stable, with no manifest episodes, thanks to aripiprazole 60mg daily.
ObjectivesThe aim is to carry out a brief review of the use of the drug as the only stabiliser in bipolar affective disorder.
MethodsA 56-year-old patient, who has been suffering from episodes of hypomania since the age of 40, with episodes of depression. After poor tolerance to the use of the usual stabilisers, and the impossibility of using antidepressants due to hypomanic swings, it was decided to start treatment with aripiprazole orally, up to a maximum of 60mg daily. Despite the fact that the patient, with this treatment, had no side effects and remained more stable psychopathologically, the patient did not comply adequately with the correct dosage, due to his rotating work shifts. This fact explained that although he acknowledged an improvement, he continued with episodes of depressive symptoms lasting several days followed by episodes of hypomanic characteristics.
ResultsFor this reason, it was decided to change treatment to aripiprazole long-acting injectable, in order to ensure linear blood levels of the drug. Initially, it was decided to prescribe 400mg every 28 days. However, after the first administration, 20 days later, the patient began to show dysphoric mood, with marked emotional lability, living in an egodystonic manner. For this reason, the dose was increased to 600mg on a monthly basis. Since then, after a year and a half with the same treatment, the patient has been stable and in line. There has been no further decompensation of the underlying psychopathology and no side effects.
ConclusionsAripiprazole in TAB is superior to placebo in type I patients, mainly affecting manic and mixed episodes, but not so much in depressive episodes. It has also been observed that it not only acts in the acute phases, but also has a stabilising function, preventing manic episodes.
One study showed that up to 65% of patients on oral aripiprazole in whom it was replaced by AOM remained clinically stable. In the same study, approximately 50% of those who completed 52 weeks of follow-up were able to maintain clinical stability.
Disclosure of InterestNone Declared
Understanding the Occurrence of Psychiatric Disorders in Epilepsy in Brazil: An Epidemiological Investigation
- L. Bardini Goulart, A. Roloff Krüger, G. Moreno Xavier, G. Fiorio Grando, J. Michelon, L. F. Alves Nascimento, J. Adames, A. T. Konzen, G. Pereira Bernd, C. Fontes Augusto, H. Wolmeister, I. Fachinetto Thoen, Y. de França, P. H. Filipin Von Muhlen, F. J. Carvalho da Costa, V. Kayser, P. H. Paesi Dutra, R. Rahal de Albuquerque, T. Garcia Furtado, G. Macelaro, A. C. Castelo, H. Vieira Rodrigues, E. Rockenbach Fidélis, D. Crusius, E. Guidugli, M. F. Valentim de Paula, Y. Marques Loureiro, E. Paiva Borsa, L. de Paula e Souza, G. Ferreira Cruz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S98
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Epilepsy is one of the most common serious brain illness, with symptoms influenced by multiple risk factors and a strong genetic predisposition, rather than having a single expression and cause¹. Neuropsychiatric symptoms in epilepsy can encompass manifestations such as mood alterations, anxiety, sleep disturbances, psychosis, and behavioral disorders. While the motor and sensory manifestations of epileptic seizures are widely recognized, neuropsychiatric symptoms accompanying epilepsy are often underestimated. Therefore, it is essential to understand the most prevalent epidemiological profile of these patients to improve the diagnosis and management of these symptoms.
ObjectivesOur goal was to evaluate the neuropsychiatric behavior of epilepsy patients in Brazilian over the past 3 years through hospitalization data in order to outline an epidemiological and behavioral profile.
MethodsA cross-sectional, descriptive, retrospective, and quantitative study was conducted on hospitalizations of individuals simultaneously diagnosed with epilepsy, schizotypal and delusional disorders, and mood disorders in all five regions of Brazil (South, Southeast, Midwest, North, and Northeast) between February 2020 and December 2022. Data from January 2020 were not available. The data used were collected through the Department of Health Informatics of the Brazilian Unified Health System (DATASUS) in the “Hospital Information System of SUS” section, gathering information regarding the nature of care, age range, gender, and ethnicity of the patients.
ResultsThe analysis covers the years 2020 to 2022, totaling 503,045 hospitalizations. In 2022, the highest number of cases occurred (≈ 37.55%), followed by 2021 (≈ 33.62%) and 2020 (≈ 28.81%). Urgent hospitalizations represented ≈ 90.85% of the total. The most affected age group was 30 to 39 years old (≈ 18.30%). Men were more affected than women (≈ 52.03% and ≈ 47.96%, respectively), and Caucasians accounted for ≈ 36.07% of the hospitalizations. The average length of stay was 19.1 days, and the mortality rate was 1.4%.
ConclusionsThus, there is a gradual and annual increase in the number of hospitalizations during the observed period. While there is a minimal disparity between the affected genders, it is evident that the profile of male, caucasian, and adult patients is the most prevalent. Moreover, the predominantly urgent nature of hospitalizations points to an alarming scenario regarding this issue. From the analysis of the data obtained in the study, there is a clear need for interventions capable of reducing the prevalence of hospitalizations for neuropsychiatric symptoms in epilepsy patients in Brazil.
Disclosure of InterestNone Declared
Major depressive episode in the elderly. Use of maintenance ECT: a case report.
- A. Izquierdo De La Puente, P. del Sol Calderón, R. Fernandez Fernandez, M. Garcia Moreno
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S641
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of an elderly patient with a severe depressive episode who, in order to maintain psychopathological stabilisation, receives ECT on an outpatient basis.
ObjectivesThe objective is to briefly review the use of ECT as a maintenance treatment for severe depression in the elderly.
MethodsPatient aged 76 years, multipathological, with a history of hypertension, DM and LBP. Femoral head fracture, myelodysplastic syndrome, severe osteoporosis with vertebral crushing, requiring rescue treatment with tramadol, and renal failure.
She came for consultation, reporting depressive symptoms of months’ duration, together with delusions of ruin and nihilism. Despite antidepressant and stabilising treatment with duloxetine at daily doses of 120mg, extended-release quetiapine 600mg, lorazepam 2.5mg and mirtazapine 45mg, the patient began to show negative behaviour towards accepting food, clinophilic behaviour and abandonment, which led to her being admitted to the short-term hospitalisation unit.
ResultsDue to the severity of the depressive symptomatology, it was decided to start ECT, administering a total of 12 sessions, which were effective, and outpatient follow-up was resumed. However, after a week, the patient again began to show marked apathy and abulia, as well as complete anorexia lasting more than 24 hours, which led to a new admission. It was then that it was decided to maintain the ECT treatment, on an outpatient basis, as maintenance treatment, together with pharmacological treatment.
ConclusionsECT is indicated in severe depression, with or without psychotic symptoms, with malnutrition and organic pathology. According to studies, it has a beneficial response of more than 60%. However, the rate of receiving depressive symptomatology in a severe episode is high, despite ECT, so studies and clinical practice recommend maintenance ECT. It is usual to start with weekly sessions, and progressively space them out to maintain the minimum that guarantees stability.
Disclosure of InterestNone Declared
Mental and Behavioral Disorders Associated with the Use of Psychoactive Substances and Alcohol: An Epidemiological Analysis in Southern Brazil
- L. Bardini, A. Roloff Krüger, G. Moreno Xavier, G. Fiorio Grando, J. Michelon, L. F. Alves Nascimento, J. Adames, A. T. Konzen, G. Pereira Bernd, C. Fontes Augusto, H. Wolmeister, I. Fachinetto Thoen, Y. de França, P. H. Filipin Von Muhlen, F. J. Carvalho da Costa, V. Kayser, P. H. Paesi Dutra, R. Rahal de Albuquerque, T. Garcia Furtado, G. Macelaro, A. C. Castelo, H. Vieira Rodrigues, E. Rockenbach Fidélis, D. Crusius, E. Guidugli, M. F. Valentim de Paula, Y. Marques Loureiro, E. Paiva Borsa, L. de Paula e Souza, G. Ferreira Cruz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Neuropsychiatric disorders are the leading cause of disability worldwide, as seen in cases such as depression, anxiety, bipolar mood disorder and schizophrenia, which can be developed or exacerbated by the use of psychoactive substances. Most mental disorders have an early onset, often leading to early and/or permanent disability, increasing the need and cost of healthcare. Therefore, it is necessary to improve the identification of the epidemiological profile of these cases in the South of Brazil in order to enhance the diagnosis and reduce the costs associated with managing these disorders.
ObjectivesThe present study aimed to analyze statistical data regarding hospitalizations related to mental disorders caused by the use of psychoactive substances and alcohol in the southern region of Brazil, highlighting the pathological scenario and identifying the most prevalent profiles of these disorders in this region.
MethodsA cross-sectional, descriptive, retrospective, and quantitative study was conducted on hospitalizations of individuals diagnosed with mental and behavioral disorders due to the use of psychoactive substances and alcohol in the states of the Southern region of Brazil (Paraná, Santa Catarina, and Rio Grande do Sul) between February 2020 and December 2022. Data of January 2020 were not available. The data used were collected through the Department of Health Informatics of the Brazilian Unified Health System (DATASUS) in the “Hospital Information System of SUS” section, gathering information regarding the nature of the care, age range, gender, and ethnicity of the patients.
ResultsThe study covers the years 2020 to 2022, indicating a total of 81,608 hospitalizations, with the year 2022 having the highest number of cases (≈ 37.13%), followed by 2021 (≈ 33.30%) and 2020 (≈ 29.55%). The states with the highest number of hospitalizations were Rio Grande do Sul (≈ 54.90%), Paraná (≈ 29.29%), and Santa Catarina (≈ 15.79%). Urgent hospitalizations accounted for ≈ 87.29% of the total. The most affected age group was 30 to 39 years old (≈ 25.61%). Men were more affected than women (≈ 81.70% and ≈ 18.28%, respectively). Caucasians accounted for ≈ 64.29% of the hospitalizations. The average length of stay was 20.8 days, and the mortality rate was 0.32%.
ConclusionsThere is a clear increase in the number of hospitalizations related to mental disorders caused by the use of psychoactive substances in the period from 2020 to 2022 in the southern region of Brazil, with the highest number of cases in the state of Rio Grande do Sul. The most affected population consisted of Caucasian men aged 30 to 39 years old. Furthermore, these results may be related to the increasing trend of psychoactive substance use among the Brazilian population and also the COVID-19 pandemic, which led to a period of underreporting due to social isolation.
Disclosure of InterestNone Declared
Brain correlates of recall of negative autobiographical memories in patients with schizophrenia
- L. Barbosa, A. Aquino-Servín, P. Fuentes-Claramonte, M. Á. García-León, A. Karuk, N. Jaurrieta, B. Hoyas-Galán, N. Ramiro-Sousa, C. Corte-Souto, P. McKenna, E. Pomarol-Clotet
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S619
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Autobiographical memory is known to be disturbed in schizophrenia. In addition, a leading theory of auditory hallucinations (AVH) is that they are intrusive – typically negative – autobiographical memories that are misinterpreted as perceptions.
ObjectivesThe aim of this study was to examine the brain functional correlates of recall of negatively emotionally valanced autobiographical memories in patients with schizophrenia, with a longer term aim of comparing patients with and without AVH.
Methods11 patients meeting DSM-5 criteria for schizophrenia or schizoaffective disorder and 10 age, sex and estimated premorbid IQ-matched healthy controls have so far taken part.
Participants underwent functional MRI in a 3T scanner while performing a task requiring them to recall autobiographical memories in response to individually tailored pairs of cue words. The cue words were based on autobiographical memories previously elicited in an interview with each patient and were designed to evoke the same memory. The cue words were presented in 10 20-second blocks interspersed with blocks where the subjects viewed cue words that did not evoke autobiographical memories. Brain activations were examined in three contrasts of interest: memory evoking words vs baseline, neutral words vs baseline and memory evoking vs neutral words.
Pre-processing and analysis were carried out with the FEAT module included in the FSL software. Statistical analysis was performed by means of a General Linear Model (GLM) approach.
ResultsIn the memory evoking vs baseline contrast the patients showed hypoactivation in the medial frontal cortex compared to the healthy controls (Figure 1). There were no differences in activation between the patients and the controls comparing the memory evoking and neutral cues.
Image:
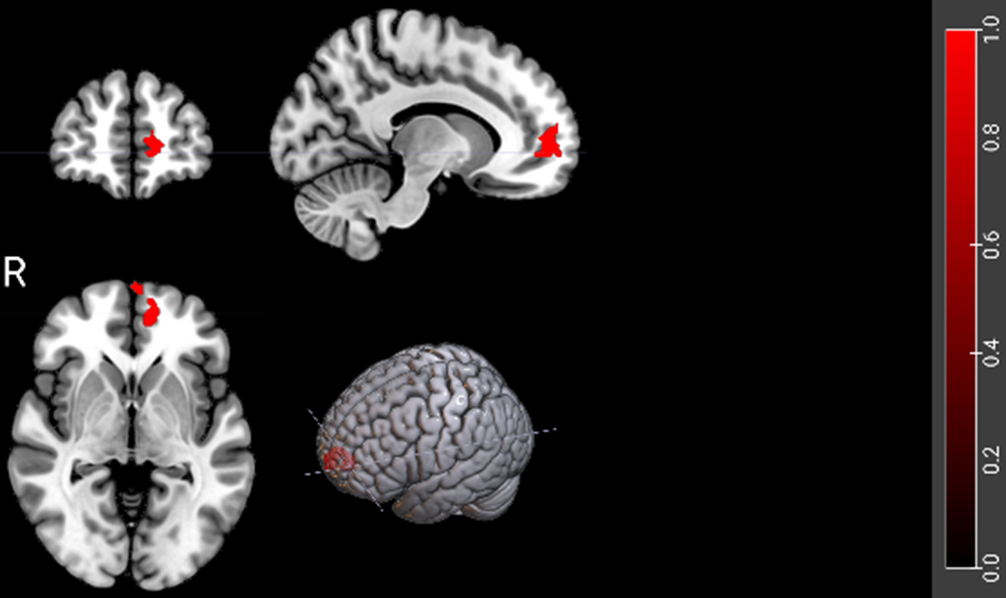 Conclusions
ConclusionsThe finding of hypoactivation in the medial frontal cortex compared to low level baseline in patients with schizophrenia suggests dysfunction in the default mode network, which is known to activate during recall of autobiographical memories.
These preliminary results suggest that recall of negative autobiographical memories in patients with schizophrenia is associated with reduced activity in the default mode network. A planned larger sample of patients and controls will be used to examine activations in patients with and without AVH.
Disclosure of InterestNone Declared
Suicidal behaviour and intravenous drug use in chemsex context
- J. Curto Ramos, A. Rodríguez Laguna, P. Barrio, L. Ibarguchi, A. García, I. Azqueta, H. Dolengevich Segal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S295
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies have called atention to the mental health disorders associated with chemsex --the intentional use of drugs before or during sexual intercourse GBMSM (gay, bisexual and men who have sex with men) population-. Sexualized intravenous drug use is also known as slam or slamsex. There are few studies that analyze the mental health differences between intravenous drug users compared to non-intravenous drug users in chemsex context.
ObjectivesTo describe the suicidal behaviour in a sample of users with sexualized drug use (chemsex) attended by the non-governmental organization Apoyo Positivo in the program “Sex, Drugs and You” and to compare the suicidal behaviour between intravenous drug users compared to non-intravenous drug users.
MethodsA cross-sectional descriptive analysis of a sample of users attended by the non-governmental organization Apoyo Positivo in the program “Sex, Drugs and You” between 2016-2019 was performed.
ResultsWe included 217 participants. 37 had attempted suicide at least once. The percentage of chemsex users who have attempted suicide were significantly higher in the intravenous drug use group compared to the non-intravenous drug use group (p<0.05).
ConclusionsPossible risk factors for suicidal behaviour among chemsex users include slamsex. Other possible risk factors previously described in other studies include adversities experienced due to one’s sexual orientation and an increased risk for HIV and other STI infections. Further studies analyzing the relationship between chemsex, slamsex and suicidal behaviour are needed.
Disclosure of InterestNone Declared
Vortioxetine as an effective drug in the treatment of depression in adolescents with long QT index. A case report
- P. Del Sol Calderon, A. Izquierdo de la Puente, R. Fernández, M. García Moreno
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S454-S455
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
This is a 13-year-old female patient admitted to the psychiatric unit active suicidal ideation.
Objectivesthe objective is to show through a clinical case how vortioxetine can be safe in adolescents.
MethodsCase report and literature review
ResultsShe has a history of daily consumption of at least 2 units of cannabis per day. She presents high emotional distress secondary to academic failure, consuming the substance as a coping strategy. Due to prohibition and control by her parents, the patient stopped taking the substance, presenting severe depressive symptoms, self-injury and suicide ideation. For this reason she is admitted to the inpatient psychiatric unit. The electrocardiogram performed on admission shows a corrected QT index of 524. Exploring physical symptoms, she recognized episodes of syncope and palpitations. Coordination was made with cardiology, who performed an echocardiogram with normal results and began follow-up with them without prescribing medication. It was agreed not to use drugs that could prolong the QT index. Evaluating the clinical situation, it was decided to start treatment with Vortioxetine up to 10 mg. With this treatment there was no worsening of the electrocardiogram and the patient’s mood improved, anxiety and ideas of death were remitted
ConclusionsThis work aims to show how vortioxetine has been effective and safe at the cardiological level in the case of moderate-severe depression in an adolescent with prolonged QT index
Disclosure of InterestNone Declared





