10 results
P154: Mild Behavioral Impairment (MBI) in a sample of general population aged > 55: associations with degree of cognitive impairment.
- P Gracia-García, R López-Antón, C de la Cámara, J Santabárbara, E Lobo, A Lobo
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, p. 219
-
- Article
-
- You have access Access
- Export citation
-
Objective:
The present study aims to determine the prevalence estimates of MBI and specific MBI domains in a large sample of the general population, by degree of cognitive impairment (CI).
Method:A representative community sample of individuals aged 55+ (n=4803) (ZARADEMP Study) was studied. MBI, and specific MBI domains, were assessed according to ISTAART-AA MBI criteria, using the Geriatric Mental State (GMS). In accordance with these criteria, clinically significant anxiety, depression, and dementia were excluded. For the standardized degree of CI Perneczky et al. ́s criteria were applied: normal (MMSE 30), questionable (MMSE 26-29), mild CI (MMSE 21-25), moderate-severe CI (MMSE <21).
Results:The prevalence of MBI, and specifically the domain Decrease Motivation (DM), increased progressively and significantly by degree of CI, the differences being significant between all cognitive groups. After control by age and education, DM was 2- and 4.5-times more frequent in subjects with mild CI (10.6%) and moderate-severe CI (18.3%), respectively, than in cognitive normal (5.8%). Affective Dysregulation (AD) was 1.7-times more frequent in mild CI (26.4%) (vs 20.4% in normal). Impulsive Dyscontrol (ID) was 2- and 7.9-times more frequent in mild CI (8%) and moderate-severe CI (23.5%) than in cognitive normal (4.7%). And Abnormal Perception and Thoughts (APT) was 6-times more frequent in moderate-severe CI (10%) (vs 1.4% in cognitive normal).
Conclusion:Our results confirm an increase of MBI prevalence across the spectrum of CI. However, each specific domain of MBI shows a different pattern of association with CI. Our results support the relevance of studying MBI domains independently.
The Line between Psychosis and Schizotypy: a case report
- L. Huerga García, E. Hernández Padrón, N. Casanova Gracia, N. Torres Nieves, P. Gómez Pérez, F. Garcia Gómez-Pamo, J.J. Dorta Gonzalez, J.F. Dorta González
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S437
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since Kraepelin and Bleuler, schizotypy was understood as a mild expression of psychosis, a latent form with the same trajectory but different severity. They pointed characteristics such as being eccentric, unreasonable, supersticious or hipersensitive, interpersonal aversiveness (often related to suspiciousness and expectation of rejection), ambivalence, anhedonia,… and psychosis-like features that don’t usually lead to help-seeking.
ObjectivesTo do a case review
MethodsWe report a case of a 17 years old boy with a childhood trauma history who started psychiatric consultations a year and a half ago because his “usual” (as his mother referred) strange behaviour got worse, which was perceived by his
ENT specialist. During the appointments, the patient showed suspiciousness, odd speech, inappropriate affect, tendency to social withdrawal, obsessive ruminations with sexual content and occasional perceptual experiences (such as depersonalization, derealization and auditory hallucinations).
ResultsPsychosis and schizotypy are linked historically and phenomenologically, which is evidenced by their placement in non-affective psychosis in the ICD-10 and DSM-5, and it is known that the direct observation (by clinicians or family members) during the childhood and adolescence are key for a correct diagnosis. In fact, this construct reflects a phenotypic expression of vulnerability to schizophrenia, and during childhood or adolescence it may be understood as an early mental risk state.
ConclusionsIn contrast to models of psychosis that mainly rely on positive features and assume a progression of them, the positive traits of schizotypy seem to be beneficial and related to a “benign or happy schizotypy” according to the articles we reviewed.
DisclosureNo significant relationships.
OCD and ASD Diagnosis: a case review
- L. Huerga García, E. Hernández Padrón, N. Casanova Gracia, N. Torres Nieves, P. Gómez Pérez
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S392
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It’s well known the challenge of differential diagnosis between Obssesive compulsive disorder and autism since their symptoms (intrusive, recurrent thoughts and repetitive behaviours) often overlap.
ObjectivesWe report a case of a 14 years old boy diagnosed of ASD who was hospitalized for the first time due to difficult management of repetitive behaviours that made him incapable of doing basic activities without help. To interrupt them led to anxiety, aggressive responses and to insistence on sameness behaviours. Only with this information and with the literature research we made, anyone could tell the problem was probably an ASD symptom. However, during his evolution it was difficult to know whether this behaviour was due to ASD or OCD: after adjusting the medication, and when he started trusting his therapists, he told us about a theory he believed so he could explain the uncomfortable ideas that crossed his mind more than often, so he used those behaviours as an anxiety-reduction technique. This new situation was the fuel to make the present review.
MethodsTo report a case.
ResultsThe results are included in the “conclusions” section.
ConclusionsAlthough there is an ongoing debate concerning the nature of the symptoms in ASD versus those observed in OCD, there are commonly used criteria to differentiate them according to the articles we reviewed:
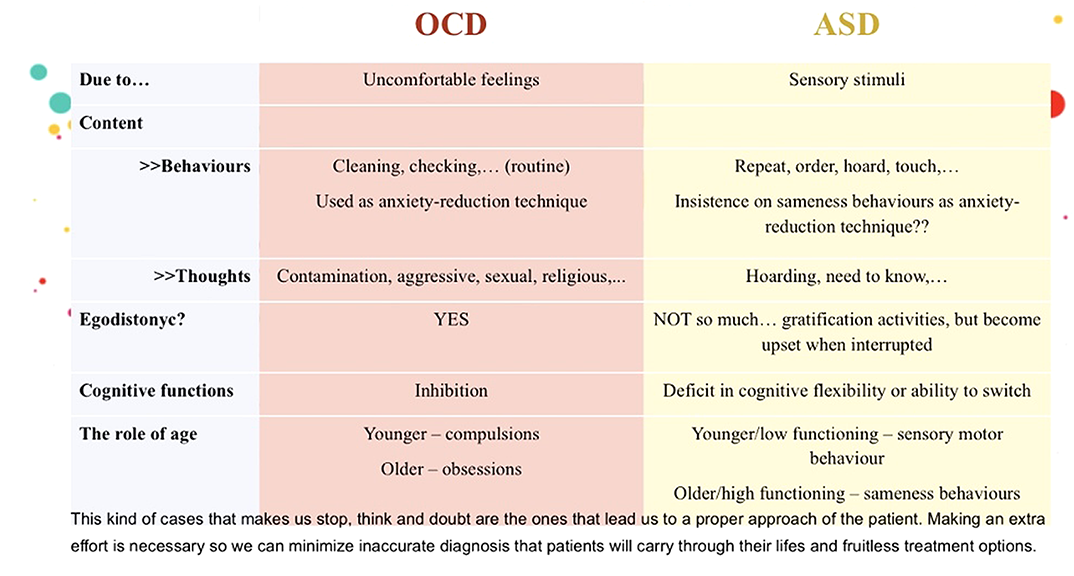 Disclosure
DisclosureNo significant relationships.
P03-154 - Serum Levels of S100B Proteins as a Marker of Positive Psychopathology in Schizophrenic Inpatients
- A.L. Morera-Fumero, E. Diaz-Mesa, P. Abreu-Gonzalez, M. Henry, A. Jimenez-Sosa, J. Garcia-Valdecasas-Campelo, A. Intxausti, L. Fernandez-Lopez, S. Yelmo, R. Gracia-Marco
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E1124
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Introduction
Schizophrenia is a chronic disease. Several etiopathogenic aetiologies have been posed, among them the existence of cerebral inflammation. S100B is a calcium-binding protein, mainly produced and secreted by astrocytes, that mediates the interaction among glial cells and between glial cells and neurons. Serum S100B levels have been proposed as a peripheral marker of brain inflammation.
ObjectivesThe aim of this research is to study if the serum level of the protein S100B has relationship with positive psychopathology.
Methods31 paranoid schizophrenic inpatients (22 male and 9 female, 36.7±10.3 years) meeting DSM-IV criteria participated in the study. Blood was sampled by venipuncture at 12:00 and 24:00 hours. Blood extractions were carried out during the first 48 hours after hospital admission. Psychopathology was assessed by the Positive and Negative Syndrome Scale (PANSS). Serum S100B levels were measured by sandwich ELISA techniques.
ResultsCorrelations between serum levels of S100B protein and PANSS positive scores are shown in the following table. The first figure corresponds to the Pearson's correlation coefficient, while the figure in brackets corresponds to its statistical significance.
S100B Total Positive Score Delusions Conceptual disorganization Hallucinations Hyperactivity Grandiosity Suspiciousness/ persecution Hostility 12:00 0.354 (0.051) 0.210 (0.249) 0.291 (0.106) 0.412 (0.019) -0.128 (0.486) 0.274 (0.135) 0.010 (0.957) 0.026 (0.887) 24:00 0.462 (0.009) 0.266 (0.141) 0.446 (0.011) 0.345 (0.053) -0.148 (0.419) 0.486 (0.006) 0.064 (0.728) 0.013 (0.942) [panss]
ConclusionsSerum levels of S100B protein may be used as a biological marker of positive psychopathology in paranoid schizophrenia.Acknowledgement
Circadian rhythm of malondialdehyde formation in healthy subjects
- A.L. Morera, P. Abreu, M. Henry, A. Garcia-Hernandez, F. Guillen-Pino, A. Intxausti, A. Orozco, E. Díaz-Mesa, F. Trujillo, J. Monzon, C.D. Díaz-Melian, R. Gracia
-
- Journal:
- European Psychiatry / Volume 22 / Issue S1 / March 2007
- Published online by Cambridge University Press:
- 16 April 2020, p. S316
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Malondialdehyde (MDA) is a common biologic marker of oxidative stress used in psychiatric research. Data regarding MDA levels in healthy subjects are controversial. One factor affecting MDA levels may stem from the existence of a circadian rhythm of MDA formation. The objective of this study consists of investigating whether MDA formation has a circadian rhythm of formation in healthy human subjects.
Methods:The sample was comprised by 9 healthy male subjects. None of them had a history of medical or neurological disease and routine laboratory parameters were normal. The study was carried out in accordance with the Helsinki Declaration and all subjects gave written informed consent before their inclusion. Blood samples were extracted at 12:00 and 2:00 in December 2004. The same routine was followed during the two experimental sessions. Serum MDA was determined by the thiobarbituric acid reactive substance (TBARS) according to the method of Ohkaba et al (1979).
Results:The sample was comprised by 9 male healthy subjects (age 33.0±11.7). There were significant differences in MDA levels between 12:00 and 2:00 (2.33±1.01 vs. 1.58±0.48, p<0.015).
Conclusions:MDA has a circadian rhythm of formation with higher levels at 12:00 than 2:00. This variation in circadian MDA levels of formation should be accounted when researching in this field.
757 – Individual Items Scores vs. Total Scores of the Schizophrenia Syndrome on Purpose of the Relationships with the Total Antioxidant Capacity
- E. Diaz Mesa, A. Morera Fumero, P. Abreu Gonzalez, M. Henry Benitez, L. Fernandez Lopez, S. Yelmo Cruz, P. Delgado Garcia, R. Gracia Marco
-
- Journal:
- European Psychiatry / Volume 28 / Issue S1 / 2013
- Published online by Cambridge University Press:
- 15 April 2020, 28-E253
-
- Article
-
- You have access Access
- Export citation
-
Introduction:
Relationships between total antioxidant capacity (TAC) and psychopathology in schizophrenia is controversial. Different methodological approaches may be a bias factor.
Objective:The aim of this research is to analyze the relationship between psychopathology as individual items and psychopathology as syndromes with the serum TAC concentration in schizophrenic patients.
Methods:20 DSM-IV paranoid schizophrenic outpatients were recruited from the psychiatric outpatient's clinic of the University Hospital of the Canary Islands. the severity of schizophrenia symptoms was measured with the Positive and Negative Syndrome Scale (PANSS). Blood samples were collected at 12:00 and 00:00 hours. Relationships between quantitative variables were assessed with the Pearson's correlation coefficient.
Results:There was a significant correlation between the PANSS positive subscale and the nocturnal TAC levels (r=0.527, p< 0.02). the PANSS negative subscale was not correlated with TAC concentrations. Item by item scores of the positive and negative PANSS correlations with nocturnal and diurnal TAC levels revealed that only item 6 (suspicion) of the positive PANSS subscale was significantly correlated with the nocturnal TAC concentrations (r=0,491, p< 0.03). Only item 3 (poor contact) of the negative PANSS subscale was also significantly correlated with the nocturnal TAC concentrations (r=0,516, p< 0.02).
Conclusions:We strongly recommend analyzing not only global scores of psychopathology but individual items scores when researching on biological markers in schizophrenia.
Acknowledgement:This study was partly supported by a grant (PI: 08/115) of the Fundacion Canaria de Investigacion y Salud (FUNCIS).
Disclosure statement:None of the authors have conflict of interest to disclose.
Staging cognitive impairment and incidence of dementia
- J. Santabárbara, R. Lopez-Anton, P. Gracia-García, C. De-la-Cámara, D. Vaquero-Puyuelo, E. Lobo, G. Marcos, L. Salvador-Carulla, T. Palomo, N. Sartorius, A. Lobo
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 25 / Issue 6 / December 2016
- Published online by Cambridge University Press:
- 15 October 2015, pp. 562-572
-
- Article
- Export citation
-
Aims.
In a background of interest in staging models in psychiatry, we tested the validity of a simple staging model of cognitive impairment to predict incident dementia.
Method.A large community sample of adults aged ≥55 years (N = 4803) was assessed in the baseline of a longitudinal, four-wave epidemiological enquiry. A two-phase assessment was implemented in each wave, and the instruments used included the Mini-Mental Status Examination (MMSE); the History and Aetiology Schedule and the Geriatric Mental State-AGECAT. For the standardised degree of cognitive impairment Perneczky et al's MMSE criteria were applied. A panel of psychiatrists diagnosed cases of dementia according to DSM-IV criteria, and cases and sub-cases of dementia were excluded for the follow-up waves. Competing risk regression models, adjusted by potential confounders, were used to test the hypothesised association between MMSE levels and dementia risk.
Results.Out of the 4057 participants followed up, 607 (14.9%) were classified as ‘normal’ (no cognitive impairment), 2672 (65.8%) as ‘questionable’ cognitive impairment, 732 (18.0%) had ‘mild’ cognitive impairment, 38 (0.9%) had ‘moderate’ cognitive impairment and eight (0.2%) had ‘severe’ impairment.
Cognitive impairment was associated with risk of dementia, the risk increasing in parallel with the level of impairment (hazard ratio: 2.72, 4.78 and 8.38 in the ‘questionable’, ‘mild’ and ‘moderate’ level of cognitive impairment, respectively).
Conclusions.The documented gradient of increased risk of dementia associated with the severity level of cognitive impairment supports the validity of the simple staging model based on the MMSE assessment.
Contributors
-
- By Mitchell Aboulafia, Frederick Adams, Marilyn McCord Adams, Robert M. Adams, Laird Addis, James W. Allard, David Allison, William P. Alston, Karl Ameriks, C. Anthony Anderson, David Leech Anderson, Lanier Anderson, Roger Ariew, David Armstrong, Denis G. Arnold, E. J. Ashworth, Margaret Atherton, Robin Attfield, Bruce Aune, Edward Wilson Averill, Jody Azzouni, Kent Bach, Andrew Bailey, Lynne Rudder Baker, Thomas R. Baldwin, Jon Barwise, George Bealer, William Bechtel, Lawrence C. Becker, Mark A. Bedau, Ernst Behler, José A. Benardete, Ermanno Bencivenga, Jan Berg, Michael Bergmann, Robert L. Bernasconi, Sven Bernecker, Bernard Berofsky, Rod Bertolet, Charles J. Beyer, Christian Beyer, Joseph Bien, Joseph Bien, Peg Birmingham, Ivan Boh, James Bohman, Daniel Bonevac, Laurence BonJour, William J. Bouwsma, Raymond D. Bradley, Myles Brand, Richard B. Brandt, Michael E. Bratman, Stephen E. Braude, Daniel Breazeale, Angela Breitenbach, Jason Bridges, David O. Brink, Gordon G. Brittan, Justin Broackes, Dan W. Brock, Aaron Bronfman, Jeffrey E. Brower, Bartosz Brozek, Anthony Brueckner, Jeffrey Bub, Lara Buchak, Otavio Bueno, Ann E. Bumpus, Robert W. Burch, John Burgess, Arthur W. Burks, Panayot Butchvarov, Robert E. Butts, Marina Bykova, Patrick Byrne, David Carr, Noël Carroll, Edward S. Casey, Victor Caston, Victor Caston, Albert Casullo, Robert L. Causey, Alan K. L. Chan, Ruth Chang, Deen K. Chatterjee, Andrew Chignell, Roderick M. Chisholm, Kelly J. Clark, E. J. Coffman, Robin Collins, Brian P. Copenhaver, John Corcoran, John Cottingham, Roger Crisp, Frederick J. Crosson, Antonio S. Cua, Phillip D. Cummins, Martin Curd, Adam Cureton, Andrew Cutrofello, Stephen Darwall, Paul Sheldon Davies, Wayne A. Davis, Timothy Joseph Day, Claudio de Almeida, Mario De Caro, Mario De Caro, John Deigh, C. F. Delaney, Daniel C. Dennett, Michael R. DePaul, Michael Detlefsen, Daniel Trent Devereux, Philip E. Devine, John M. Dillon, Martin C. Dillon, Robert DiSalle, Mary Domski, Alan Donagan, Paul Draper, Fred Dretske, Mircea Dumitru, Wilhelm Dupré, Gerald Dworkin, John Earman, Ellery Eells, Catherine Z. Elgin, Berent Enç, Ronald P. Endicott, Edward Erwin, John Etchemendy, C. Stephen Evans, Susan L. Feagin, Solomon Feferman, Richard Feldman, Arthur Fine, Maurice A. Finocchiaro, William FitzPatrick, Richard E. Flathman, Gvozden Flego, Richard Foley, Graeme Forbes, Rainer Forst, Malcolm R. Forster, Daniel Fouke, Patrick Francken, Samuel Freeman, Elizabeth Fricker, Miranda Fricker, Michael Friedman, Michael Fuerstein, Richard A. Fumerton, Alan Gabbey, Pieranna Garavaso, Daniel Garber, Jorge L. A. Garcia, Robert K. Garcia, Don Garrett, Philip Gasper, Gerald Gaus, Berys Gaut, Bernard Gert, Roger F. Gibson, Cody Gilmore, Carl Ginet, Alan H. Goldman, Alvin I. Goldman, Alfonso Gömez-Lobo, Lenn E. Goodman, Robert M. Gordon, Stefan Gosepath, Jorge J. E. Gracia, Daniel W. Graham, George A. Graham, Peter J. Graham, Richard E. Grandy, I. Grattan-Guinness, John Greco, Philip T. Grier, Nicholas Griffin, Nicholas Griffin, David A. Griffiths, Paul J. Griffiths, Stephen R. Grimm, Charles L. Griswold, Charles B. Guignon, Pete A. Y. Gunter, Dimitri Gutas, Gary Gutting, Paul Guyer, Kwame Gyekye, Oscar A. Haac, Raul Hakli, Raul Hakli, Michael Hallett, Edward C. Halper, Jean Hampton, R. James Hankinson, K. R. Hanley, Russell Hardin, Robert M. Harnish, William Harper, David Harrah, Kevin Hart, Ali Hasan, William Hasker, John Haugeland, Roger Hausheer, William Heald, Peter Heath, Richard Heck, John F. Heil, Vincent F. Hendricks, Stephen Hetherington, Francis Heylighen, Kathleen Marie Higgins, Risto Hilpinen, Harold T. Hodes, Joshua Hoffman, Alan Holland, Robert L. Holmes, Richard Holton, Brad W. Hooker, Terence E. Horgan, Tamara Horowitz, Paul Horwich, Vittorio Hösle, Paul Hoβfeld, Daniel Howard-Snyder, Frances Howard-Snyder, Anne Hudson, Deal W. Hudson, Carl A. Huffman, David L. Hull, Patricia Huntington, Thomas Hurka, Paul Hurley, Rosalind Hursthouse, Guillermo Hurtado, Ronald E. Hustwit, Sarah Hutton, Jonathan Jenkins Ichikawa, Harry A. Ide, David Ingram, Philip J. Ivanhoe, Alfred L. Ivry, Frank Jackson, Dale Jacquette, Joseph Jedwab, Richard Jeffrey, David Alan Johnson, Edward Johnson, Mark D. Jordan, Richard Joyce, Hwa Yol Jung, Robert Hillary Kane, Tomis Kapitan, Jacquelyn Ann K. Kegley, James A. Keller, Ralph Kennedy, Sergei Khoruzhii, Jaegwon Kim, Yersu Kim, Nathan L. King, Patricia Kitcher, Peter D. Klein, E. D. Klemke, Virginia Klenk, George L. Kline, Christian Klotz, Simo Knuuttila, Joseph J. Kockelmans, Konstantin Kolenda, Sebastian Tomasz Kołodziejczyk, Isaac Kramnick, Richard Kraut, Fred Kroon, Manfred Kuehn, Steven T. Kuhn, Henry E. Kyburg, John Lachs, Jennifer Lackey, Stephen E. Lahey, Andrea Lavazza, Thomas H. Leahey, Joo Heung Lee, Keith Lehrer, Dorothy Leland, Noah M. Lemos, Ernest LePore, Sarah-Jane Leslie, Isaac Levi, Andrew Levine, Alan E. Lewis, Daniel E. Little, Shu-hsien Liu, Shu-hsien Liu, Alan K. L. Chan, Brian Loar, Lawrence B. Lombard, John Longeway, Dominic McIver Lopes, Michael J. Loux, E. J. Lowe, Steven Luper, Eugene C. Luschei, William G. Lycan, David Lyons, David Macarthur, Danielle Macbeth, Scott MacDonald, Jacob L. Mackey, Louis H. Mackey, Penelope Mackie, Edward H. Madden, Penelope Maddy, G. B. Madison, Bernd Magnus, Pekka Mäkelä, Rudolf A. Makkreel, David Manley, William E. Mann (W.E.M.), Vladimir Marchenkov, Peter Markie, Jean-Pierre Marquis, Ausonio Marras, Mike W. Martin, A. P. Martinich, William L. McBride, David McCabe, Storrs McCall, Hugh J. McCann, Robert N. McCauley, John J. McDermott, Sarah McGrath, Ralph McInerny, Daniel J. McKaughan, Thomas McKay, Michael McKinsey, Brian P. McLaughlin, Ernan McMullin, Anthonie Meijers, Jack W. Meiland, William Jason Melanson, Alfred R. Mele, Joseph R. Mendola, Christopher Menzel, Michael J. Meyer, Christian B. Miller, David W. Miller, Peter Millican, Robert N. Minor, Phillip Mitsis, James A. Montmarquet, Michael S. Moore, Tim Moore, Benjamin Morison, Donald R. Morrison, Stephen J. Morse, Paul K. Moser, Alexander P. D. Mourelatos, Ian Mueller, James Bernard Murphy, Mark C. Murphy, Steven Nadler, Jan Narveson, Alan Nelson, Jerome Neu, Samuel Newlands, Kai Nielsen, Ilkka Niiniluoto, Carlos G. Noreña, Calvin G. Normore, David Fate Norton, Nikolaj Nottelmann, Donald Nute, David S. Oderberg, Steve Odin, Michael O’Rourke, Willard G. Oxtoby, Heinz Paetzold, George S. Pappas, Anthony J. Parel, Lydia Patton, R. P. Peerenboom, Francis Jeffry Pelletier, Adriaan T. Peperzak, Derk Pereboom, Jaroslav Peregrin, Glen Pettigrove, Philip Pettit, Edmund L. Pincoffs, Andrew Pinsent, Robert B. Pippin, Alvin Plantinga, Louis P. Pojman, Richard H. Popkin, John F. Post, Carl J. Posy, William J. Prior, Richard Purtill, Michael Quante, Philip L. Quinn, Philip L. Quinn, Elizabeth S. Radcliffe, Diana Raffman, Gerard Raulet, Stephen L. Read, Andrews Reath, Andrew Reisner, Nicholas Rescher, Henry S. Richardson, Robert C. Richardson, Thomas Ricketts, Wayne D. Riggs, Mark Roberts, Robert C. Roberts, Luke Robinson, Alexander Rosenberg, Gary Rosenkranz, Bernice Glatzer Rosenthal, Adina L. Roskies, William L. Rowe, T. M. Rudavsky, Michael Ruse, Bruce Russell, Lilly-Marlene Russow, Dan Ryder, R. M. Sainsbury, Joseph Salerno, Nathan Salmon, Wesley C. Salmon, Constantine Sandis, David H. Sanford, Marco Santambrogio, David Sapire, Ruth A. Saunders, Geoffrey Sayre-McCord, Charles Sayward, James P. Scanlan, Richard Schacht, Tamar Schapiro, Frederick F. Schmitt, Jerome B. Schneewind, Calvin O. Schrag, Alan D. Schrift, George F. Schumm, Jean-Loup Seban, David N. Sedley, Kenneth Seeskin, Krister Segerberg, Charlene Haddock Seigfried, Dennis M. Senchuk, James F. Sennett, William Lad Sessions, Stewart Shapiro, Tommie Shelby, Donald W. Sherburne, Christopher Shields, Roger A. Shiner, Sydney Shoemaker, Robert K. Shope, Kwong-loi Shun, Wilfried Sieg, A. John Simmons, Robert L. Simon, Marcus G. Singer, Georgette Sinkler, Walter Sinnott-Armstrong, Matti T. Sintonen, Lawrence Sklar, Brian Skyrms, Robert C. Sleigh, Michael Anthony Slote, Hans Sluga, Barry Smith, Michael Smith, Robin Smith, Robert Sokolowski, Robert C. Solomon, Marta Soniewicka, Philip Soper, Ernest Sosa, Nicholas Southwood, Paul Vincent Spade, T. L. S. Sprigge, Eric O. Springsted, George J. Stack, Rebecca Stangl, Jason Stanley, Florian Steinberger, Sören Stenlund, Christopher Stephens, James P. Sterba, Josef Stern, Matthias Steup, M. A. Stewart, Leopold Stubenberg, Edith Dudley Sulla, Frederick Suppe, Jere Paul Surber, David George Sussman, Sigrún Svavarsdóttir, Zeno G. Swijtink, Richard Swinburne, Charles C. Taliaferro, Robert B. Talisse, John Tasioulas, Paul Teller, Larry S. Temkin, Mark Textor, H. S. Thayer, Peter Thielke, Alan Thomas, Amie L. Thomasson, Katherine Thomson-Jones, Joshua C. Thurow, Vzalerie Tiberius, Terrence N. Tice, Paul Tidman, Mark C. Timmons, William Tolhurst, James E. Tomberlin, Rosemarie Tong, Lawrence Torcello, Kelly Trogdon, J. D. Trout, Robert E. Tully, Raimo Tuomela, John Turri, Martin M. Tweedale, Thomas Uebel, Jennifer Uleman, James Van Cleve, Harry van der Linden, Peter van Inwagen, Bryan W. Van Norden, René van Woudenberg, Donald Phillip Verene, Samantha Vice, Thomas Vinci, Donald Wayne Viney, Barbara Von Eckardt, Peter B. M. Vranas, Steven J. Wagner, William J. Wainwright, Paul E. Walker, Robert E. Wall, Craig Walton, Douglas Walton, Eric Watkins, Richard A. Watson, Michael V. Wedin, Rudolph H. Weingartner, Paul Weirich, Paul J. Weithman, Carl Wellman, Howard Wettstein, Samuel C. Wheeler, Stephen A. White, Jennifer Whiting, Edward R. Wierenga, Michael Williams, Fred Wilson, W. Kent Wilson, Kenneth P. Winkler, John F. Wippel, Jan Woleński, Allan B. Wolter, Nicholas P. Wolterstorff, Rega Wood, W. Jay Wood, Paul Woodruff, Alison Wylie, Gideon Yaffe, Takashi Yagisawa, Yutaka Yamamoto, Keith E. Yandell, Xiaomei Yang, Dean Zimmerman, Günter Zoller, Catherine Zuckert, Michael Zuckert, Jack A. Zupko (J.A.Z.)
- Edited by Robert Audi, University of Notre Dame, Indiana
-
- Book:
- The Cambridge Dictionary of Philosophy
- Published online:
- 05 August 2015
- Print publication:
- 27 April 2015, pp ix-xxx
-
- Chapter
- Export citation
Degree of cognitive impairment and mortality: a 17-year follow-up in a community study
- J. Santabárbara, R. Lopez-Anton, G. Marcos, C. De-la-Cámara, E. Lobo, P. Saz, P. Gracia-García, T. Ventura, A. Campayo, L. Rodríguez-Mañas, B. Olaya, J. M. Haro, L. Salvador-Carulla, N. Sartorius, A. Lobo
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 24 / Issue 6 / December 2015
- Published online by Cambridge University Press:
- 06 June 2014, pp. 503-511
-
- Article
- Export citation
-
Background.
To test the hypothesis that cognitive impairment in older adults is associated with all-cause mortality risk and the risk increases when the degree of cognitive impairment augments; and then, if this association is confirmed, to report the population-attributable fraction (PAF) of mortality due to cognitive impairment.
Method.A representative random community sample of individuals aged over 55 was interviewed, and 4557 subjects remaining alive at the end of the first year of follow-up were included in the analysis. Instruments used in the assessment included the Mini-Mental Status Examination (MMSE), the History and Aetiology Schedule (HAS) and the Geriatric Mental State (GMS)-AGECAT. For the standardised degree of cognitive impairment Perneczky et al's MMSE criteria were applied. Mortality information was obtained from the official population registry. Multivariate Cox proportional hazard models were used to test the association between MMSE degrees of cognitive impairment and mortality risk. We also estimated the PAF of mortality due to specific MMSE stages.
Results.Cognitive impairment was associated with mortality risk, the risk increasing in parallel with the degree of cognitive impairment (Hazard ratio, HR: 1.18 in the ‘mild’ degree of impairment; HR: 1.29 in the ‘moderate’ degree; and HR: 2.08 in the ‘severe’ degree). The PAF of mortality due to severe cognitive impairment was 3.49%.
Conclusions.A gradient of increased mortality-risk associated with severity of cognitive impairment was observed. The results support the claim that routine assessment of cognitive function in older adults should be considered in clinical practice.
Molecular line probes of activity in galaxies
- C. Kramer, S. Aalto, R. Simon, S. García-Burillo, J. Graciá-Carpio, A. Usero, P. Planesas, A. Fuente, M. Krips
-
- Journal:
- European Astronomical Society Publications Series / Volume 31 / 2008
- Published online by Cambridge University Press:
- 04 October 2008, pp. 85-88
- Print publication:
- 2008
-
- Article
- Export citation
-
The use of specific tracers of the dense molecular gas phase can help to explore the feedback of activity on the interstellar medium (ISM) in galaxies. This information is a key to any quantitative assessment of the efficiency of the star formation process in galaxies. We present the results of a survey devoted to probe the feedback of activity through the study of the excitation and chemistry of the dense molecular gas in a sample of local universe starbursts and active galactic nuclei (AGNs). Our sample includes also 17 luminous and ultraluminous infrared galaxies (LIRGs and ULIRGs). From the analysis of the LIRGs/ULIRGs subsample, published in Graciá-Carpio et al. (2007), we find the first clear observational evidence that the star formation efficiency of the dense gas, measured by the LFIR/LHCN ratio, is significantly higher in LIRGs and ULIRGs than in normal galaxies. Mounting evidence of overabundant HCN in active environments would even reinforce the reported trend, pointing to a significant turn upward in the Kennicutt-Schmidt law around LFIR = 1011L๏. This result has major implications for the use of HCN as a tracer of the dense gas in local and high-redshift luminous infrared galaxies.




