Original Article
Cost-effectiveness analysis of whole-genome sequencing during an outbreak of carbapenem-resistant Acinetobacter baumannii
- Thomas M. Elliott, Patrick N. Harris, Leah W. Roberts, Michelle Doidge, Trish Hurst, Krispin Hajkowicz, Brian Forde, David L. Paterson, Louisa G. Gordon
-
- Published online by Cambridge University Press:
- 13 December 2021, e62
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Whole-genome sequencing (WGS) shotgun metagenomics (metagenomics) attempts to sequence the entire genetic content straight from the sample. Diagnostic advantages lie in the ability to detect unsuspected, uncultivatable, or very slow-growing organisms.
Objective:To evaluate the clinical and economic effects of using WGS and metagenomics for outbreak management in a large metropolitan hospital.
Design:Cost-effectiveness study.
Setting:Intensive care unit and burn unit of large metropolitan hospital.
Patients:Simulated intensive care unit and burn unit patients.
Methods:We built a complex simulation model to estimate pathogen transmission, associated hospital costs, and quality-adjusted life years (QALYs) during a 32-month outbreak of carbapenem-resistant Acinetobacter baumannii (CRAB). Model parameters were determined using microbiology surveillance data, genome sequencing results, hospital admission databases, and local clinical knowledge. The model was calibrated to the actual pathogen spread within the intensive care unit and burn unit (scenario 1) and compared with early use of WGS (scenario 2) and early use of WGS and metagenomics (scenario 3) to determine their respective cost-effectiveness. Sensitivity analyses were performed to address model uncertainty.
Results:On average compared with scenario 1, scenario 2 resulted in 14 fewer patients with CRAB, 59 additional QALYs, and $75,099 cost savings. Scenario 3, compared with scenario 1, resulted in 18 fewer patients with CRAB, 74 additional QALYs, and $93,822 in hospital cost savings. The likelihoods that scenario 2 and scenario 3 were cost-effective were 57% and 60%, respectively.
Conclusions:The use of WGS and metagenomics in infection control processes were predicted to produce favorable economic and clinical outcomes.
Poster Presentation
Antibiotic Stewardship
Analysis of Recurrent Urinary Tract Infection Management in Outpatient Settings Reveals Opportunities for Antibiotic Stewards
- Marissa Valentine-King, Barbara Trautner, Roger Zoorob, George Germanos, Jason Salemi, Kalpana Gupta, Larissa Grigoryan
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s34
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Studies of antibiotic prescribing choice and duration have typically excluded women with recurrent UTI (rUTI), yet the Infectious Disease Society of America (IDSA) UTI treatment guidelines are applicable to recurrent and sporadic cystitis. We sought to better understand prescribing practices among uncomplicated rUTI patients in terms of choice of drug, duration of therapy, and the risk factors for receiving guideline-discordant therapy. Methods: We performed a retrospective database study by extracting electronic health record data from adults seen at academic primary care, internal medicine, or urology practices between November 2016 and December 2018. Inclusion criteria included having ≥2 or ≥3 International Classification of Diseases Tenth Edition (ICD-10) cystitis codes recorded within a 6- or 12-month period, respectively. We excluded patients with ICD-10 codes indicating any structural or functional genitourinary comorbidities, interstitial cystitis, vaginosis, compromised immune systems, or pregnancy in the prior year. Patients were also excluded if they had signs or symptoms of pyelonephritis at presentation. Results: Overall, 232 patients presented for 597 outpatient visits. Most were married (52.2%), non-Hispanic white (62.9%), and female (92.2%), with a median age of 58 years (IQR, 41–68). Only 21% of visits with an antibiotic prescribed for treatment consisted of a first-line therapy agent prescribed for the recommended duration. In terms of antibiotic choice, these agents were prescribed in 58.4% of scenarios, which primarily included nitrofurantoin (37.8%) and trimethoprim-sulfamethoxazole (TMP-SMX) (20.3%). Guideline-discordant choices of fluoroquinolones (28.8%), and β-lactams (11.2%) were the second and third most commonly prescribed drug categories, respectively. Multinomial logistic regression identified age (OR, 1.02; 95% CI, 1.002–1.04) or having a telephone visit (OR, 3.17; 95% CI, 1.54–6.52) as independent risk factors for receiving a β-lactam. The duration exceeded the 3-day guideline recommendation in 87.6% of fluoroquinolones and 73% of TMP-SMX (73%) prescriptions, and 61% of nitrofurantoin prescriptions exceeded the recommended 5-day duration. Multiple logistic regression analysis revealed that seeking care at a urology clinic (OR, 2.81; 95% CI, 1.59–5.17) served as an independent factor for therapy duration exceeding guideline recommendations. Conclusions: This retrospective study revealed shortcomings in prescribing practices in the type and duration of therapy for rUTI. rUTI as well as sporadic UTI are important targets for outpatient antibiotic stewardship interventions.
Funding: This investigator-initiated research study was funded by Rebiotix Inc, a Ferring Company.
Disclosures: None
Concise Communication
Implementation of a surgical site infection prevention bundle: Patient adherence and experience
- Stacey Hockett Sherlock, Daniel Suh, Eli Perencevich, Heather Schacht Reisinger, Judy Streit, Amy Frank, Gosia Clore, Madeline Ohl, Dina Speicher, Loreen Herwaldt, Marin L. Schweizer
-
- Published online by Cambridge University Press:
- 10 December 2021, e63
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We evaluated barriers and facilitators to patient adherence with a bundled intervention including chlorhexidine gluconate (CHG) bathing and decolonizing Staphylococcus aureus nasal carriers in a real-world setting. Survey data identified 85.5% adherence with home use of CHG as directed and 52.9% adherence with home use of mupirocin as directed.
Poster Presentation
Antibiotic Stewardship
Blood Culture Utilization at Six Southeastern US Hospitals
- Bobby Warren, Rebekah Moehring, Michael Yarrington, Deverick Anderson, Christopher Polage
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s34-s35
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Group Name: Duke Center for Antimicrobial Stewardship and Infection Prevention
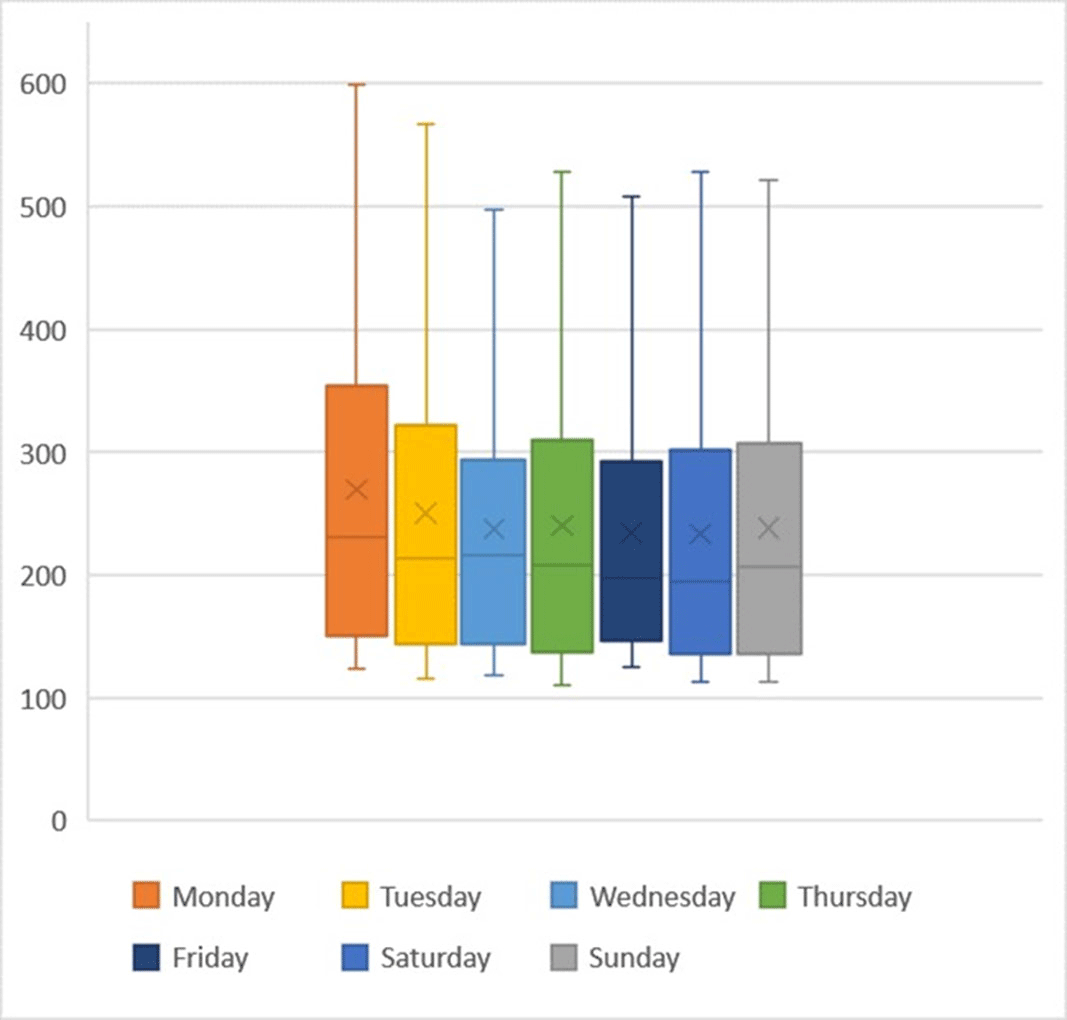
Background: Blood cultures are an essential diagnostic test, but over- and underutilization may cause harm. Methods: We analyzed blood culture utilization at 6 hospitals in the southeastern United States including 1 academic hospital (A) and 5 community hospitals (B–F) from May 2019 to April 2020. We measured blood culture utilization rate (BCUR) per 1,000 patient days and blood cultures per encounter. We counted blood cultures by laboratory accession number and measured utilization per 1,000 patient days and encounter. A likely contaminant was defined as 1 of 2 blood cultures collected in the same calendar day positive for a common skin commensal (CSC), as defined by the NHSN, and not identified from subsequent cultures. A likely pathogen was defined as a culture with a pathogen not on the CSC list or a CSC not meeting the contaminant definition. Hospital-level BCUR included samples for culture collected in the emergency department (ED) and inpatient areas divided by inpatient days. Results: The analysis included 117,897 blood cultures and 662,723 patient days with a median BCUR of 209.7 per hospital and median blood culture per encounter of 2 (Table 1). One community hospital (C) demonstrated a substantially higher BCUR than others. Cultures were frequently collected in the ED (54%; range, 36%–78%); most encounters with cultures in the ED were subsequently admitted to an inpatient unit (84%; range, 73%–89%). Higher BCURs were observed in intensive care and oncology units. The proportion of first blood cultures drawn after initiation of antibiotics was 6% (range, 3%–9%. Mondays had higher BCURs than other days of the week (Figure 1). The average BCUR by month was 176.1 (range, 164.3–181.4) with no seasonal patterns observed. Overall, 7.7% (range, 4.5%–9.1%) of blood cultures identified a likely pathogen and 2.1% (range, 1.3%–3.2%) identified a likely contaminant. The 3 hospitals with BCURs >200 also had contaminant rates >2% and >60% ED cultures. Conclusions: Blood culture utilization varied by hospital, unit, and day of the week. We observed higher rates of likely contaminants among hospitals with higher BCURs and ED culture rates. Comparisons may assist in identifying opportunities to optimize practice around blood-culture ordering and collection.
Funding: No
Disclosures: None
Table 1. 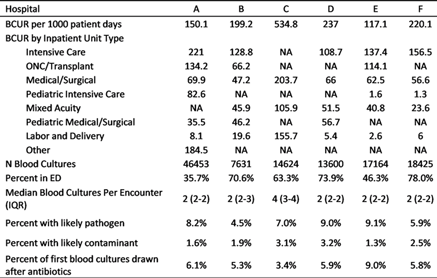
Figure 1.
Original Article
Current antimicrobial prescription at outpatient dentistry centers and clinics in tertiary-care hospitals in Tokyo, Japan: A multicenter cross-sectional study
- Yasuaki Tagashira, Masao Horiuchi, Atsushi Kosaka, Takuya Washino, Mikihiro Horiuchi, Shutaro Murakami, Itoe Tagashira, Hitoshi Honda
-
- Published online by Cambridge University Press:
- 13 December 2021, e64
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Antimicrobial administration is necessary before specific dental procedures to prevent postprocedural infections and complications and antimicrobials are sometimes indicated for the treatment of odontogenic infections. However, antimicrobials are commonly misused by dentists.
Methods:This cross-sectional study was conducted at 4 public, tertiary-care hospitals in Tokyo, Japan, from June to July 2019. We included patients who received an antimicrobial prescription at the outpatient dentistry center or clinic at each participating hospital. The indications for antimicrobial prescription were (1) antimicrobial prescriptions for prophylaxis (APPs) or (2) antimicrobial prescriptions for treatment (APTs). Prescribing patterns were described in terms of antimicrobial choice, timing, and dosages for APPs and APTs.
Results:During the study period, 1,772 patients received an antimicrobial prescription. Among them 1,439 (81.2%) were APPs and 333 (18.8%) were APTs. The most common aim of APP was to prevent local infections and complications following tooth extraction (n = 1,244, 86.4%). The proportion of appropriate APPs was only 0.8% (12 of 1,439). Among 1,439 total APPs, 171 (11.9%) were unnecessary, 32 (2.2%) were inappropriate, and 1,224 (85.1%) were suboptimal. Whereas 101 (30.3%) of 333 APTs were appropriate, the remaining 97 instances (29.1%) were unnecessary, 86 (26.7%) were inappropriate, and 46 (13.8%) were suboptimal.
Conclusion:Inappropriate antimicrobial prescriptions were common among dentists in Japan. Understanding the differences in the current antimicrobial prescribing patterns for prophylaxis and treatment is critically important for implementing an effective antimicrobial stewardship program in dentistry.
Poster Presentation
Antibiotic Stewardship
Outpatient Antibiotic Use for Common Infectious Diagnoses: Patterns in Telehealth During the Emergence of COVID-19
- Brigid Wilson, Taissa Bej, Sunah Song, Janet M Briggs, Richard Banks, Robin Jump, Federico Perez, Ukwen Akpoji
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s35-s36
-
- Article
-
- You have access Access
- Open access
- Export citation
-
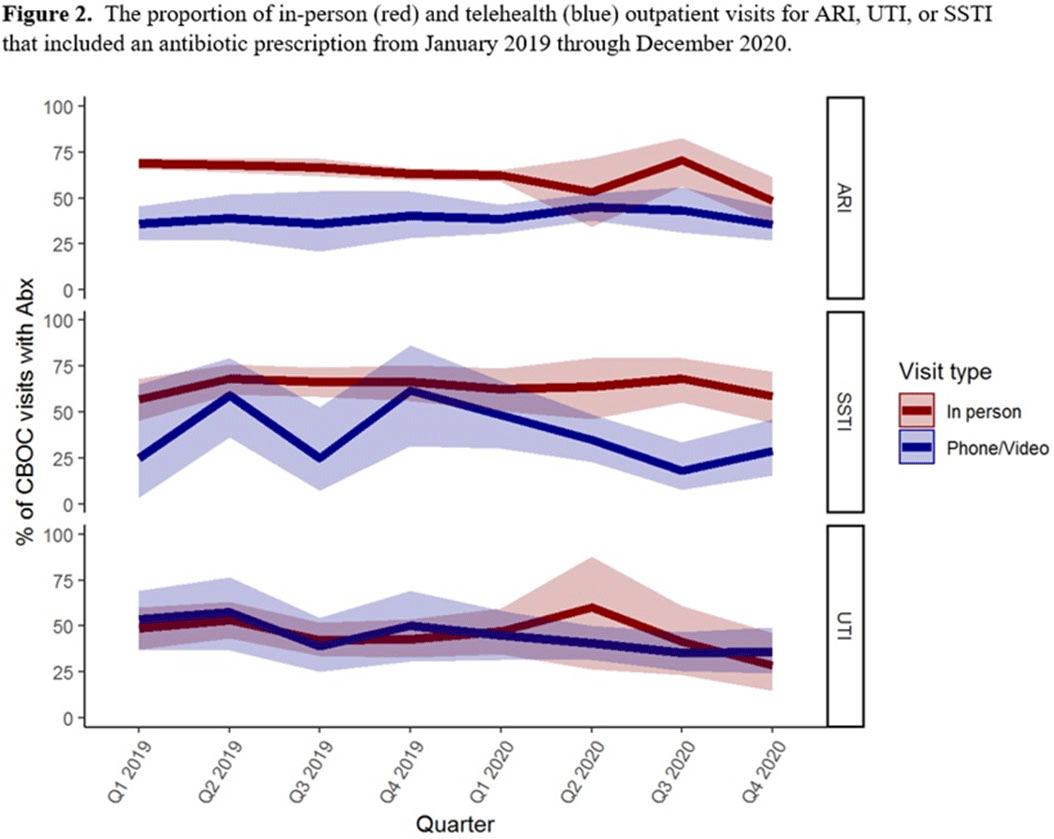
Background: The influence of increased use of telehealth during the emergence of COVID-19 on antibiotic prescriptions in outpatient settings is unknown. The VA Northeast Ohio Healthcare System has 13 community-based outpatient clinics (CBOCs) that provide primary and preventive care. We assessed changes in antibiotic prescriptions that occurred as care shifted from in-person to telehealth visits. Methods: Using VHA administrative databases, we identified all primary care CBOC visits between January 1, 2019, and December 31, 2020, that included a diagnosis for an acute respiratory infection (ARI), a urinary tract infection (UTI), or a skin or soft-tissue infection (SSTI), excluding visits with >1 of these diagnoses or with additional infectious diagnoses (eg, pneumonia, influenza). We summarized the proportion of telehealth visits and the proportion of patients prescribed antibiotics at quarterly intervals. We specifically assessed outpatient visits from April to December 2019 compared to the same months in 2020 to account for seasonality while analyzing diagnosis and antibiotic trends in the emergence of the COVID-19 pandemic. Results: The patients receiving care in April–December 2019 compared to April–December 2020 were similar (Table 1). From April through December 2019, 90% of CBOC primary care visits with a diagnosis for ARI, UTI, or SSTI were in-person, and antibiotics were prescribed at 63%, 46%, and 65% of visits in either modality, respectively (Figure 1). From April through December 2020, only 33% of CBOC primary care visits for ARI, UTI, and SSTI were in person, and antibiotics were prescribed at 46%, 38%, and 47% of visits in either modality, respectively. Comparing April–December in 2019 and 2020, the number of CBOC visits for ARI fell by 76% (2,152 visits to 509 visits), with a more modest decline of 20% and 35% observed for UTI and SSTI visits. In-person visits for ARIs and SSTIs were more likely than telehealth visits to result in an antibiotic prescription (Figure 2). Conclusions: Among the CBOCs at our healthcare system, an increase in the proportion of telehealth visits and a reduction in ARI diagnoses occurred after the emergence of COVID-19. In this setting, we observed a reduction in the proportion of visits for ARIs, UTIs, and SSTIs that included an antibiotic prescription.
Funding: Merck
Disclosures: None
Table 1. 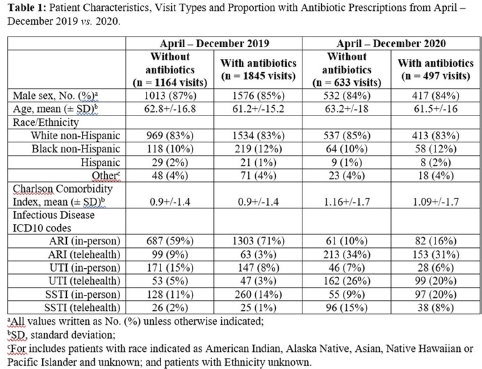
Figure 1.
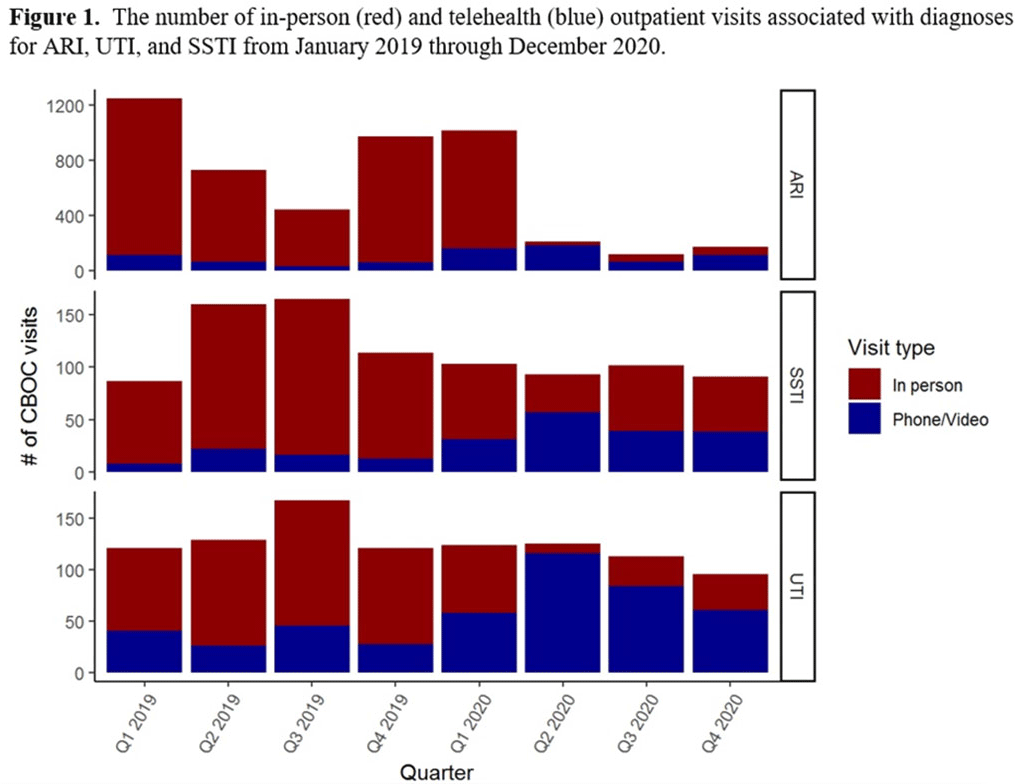
Figure 2.
Concise Communication
Sources of exposure identified through structured interviews of healthcare workers who test positive for severe acute respiratory coronavirus virus 2 (SARS-CoV-2): A prospective analysis at two teaching hospitals
- Chanu Rhee, Meghan A. Baker, Robert Tucker, Diane Griesbach, Dinah McDonald, Sarah A. Williams, Karen Fiumara, Andrew Resnick, Michael Klompas, for the CDC Prevention Epicenters Program
-
- Published online by Cambridge University Press:
- 15 December 2021, e65
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We interviewed 1,208 healthcare workers with positive SARS-CoV-2 tests between October 2020 and June 2021 to determine likely exposure sources. Overall, 689 (57.0%) had community exposures (479 from household members), 76 (6.3%) had hospital exposures (64 from other employees including 49 despite masking), 11 (0.9%) had community and hospital exposures, and 432 (35.8%) had no identifiable source of exposure.
Poster Presentation
Antibiotic Stewardship
Antimicrobial Stewardship Standards and Patient Safety: A Case Study in Blood Culture Contamination
- Connie Schaefer
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s36
-
- Article
-
- You have access Access
- Open access
- Export citation
-
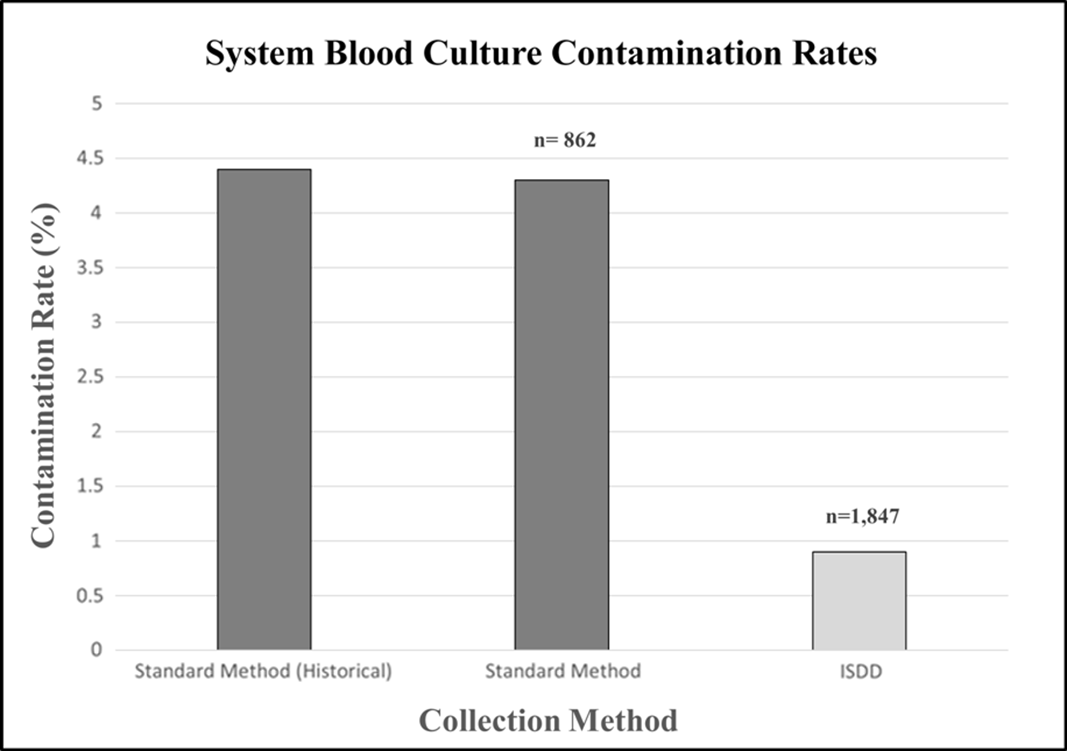
Background: Blood culture is a crucial diagnostic tool for healthcare systems, but false-positive results drain clinical resources, imperil patients with an increased length of stay (and associated hospital-acquired infection risk), and undermine global health initiatives when broad-spectrum antibiotics are administered unnecessarily. Considering emerging technologies that mitigate human error factors, we questioned historically acceptable rates of blood culture contamination, which prompted a need to promote and trial these technologies further. In a 3-month trial, 3 emergency departments in a midwestern healthcare system utilized an initial specimen diversion device (ISDD) to draw blood cultures to bring their blood culture contamination rate (4.4% prior to intervention) below the 3% benchmark recommended by the Clinical & Laboratory Standards Institute. Methods: All emergency department nursing staff received operational training on the ISDD for blood culture sample acquisition. From June through August 2019, 1,847 blood cultures were drawn via the ISDD, and 862 were drawn via the standard method. Results: In total, 16 contamination events occurred when utilizing the ISDD (0.9%) and 37 contamination events occurred when utilizing the standard method (4.3%). ISDD utilization resulted in an 80% reduction in blood culture contamination from the rate of 4.4% rate held prior to intervention. Conclusions: A midwestern healthcare system experienced a dramatic reduction in blood culture contamination across 3 emergency departments while pilot testing an ISDD, conserving laboratory and therapeutic resources while minimizing patient exposure to unnecessary risks and procedures. If the results obtained here were sustained and the ISDD utilized for all blood culture draws, nearly 400 contamination events could be avoided annually in this system. Reducing unnecessary antibiotic use in this manner will lower rates of associated adverse events such as acute kidney injury and allergic reaction, which are possible topics for further investigation. The COVID-19 pandemic has recently highlighted both the importance of keeping hospital beds available and the rampant carelessness with which broad-spectrum antibiotics are administered (escalating the threat posed by multidrug-resistant organisms). As more ambitious healthcare benchmarks become attainable, promoting and adhering to higher standards for patient care will be critical to furthering an antimicrobial stewardship agenda and to reducing treatment inequity in the field.
Funding: No
Disclosures: None
Figure 1.
Original Article
Changes in outpatient antibiotic prescribing for acute respiratory illnesses, 2011 to 2018
- Laura M. King, Sharon V. Tsay, Lauri A. Hicks, Destani Bizune, Adam L. Hersh, Katherine Fleming-Dutra
-
- Published online by Cambridge University Press:
- 17 December 2021, e66
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objectives:
To describe acute respiratory illnesses (ARI) visits and antibiotic prescriptions in 2011 and 2018 across outpatient settings to evaluate progress in reducing unnecessary antibiotic prescribing for ARIs.
Design:Cross-sectional study.
Setting and patients:Outpatient medical and pharmacy claims captured in the IBM MarketScan commercial database, a national convenience sample of privately insured individuals aged <65 years.
Methods:We calculated the annual number of ARI visits and visits with oral antibiotic prescriptions per 1,000 enrollees overall and by age category, sex, and setting in 2011 and 2018. We compared these and calculated prevalence rate ratios (PRRs). We adapted existing tiered-diagnosis methodology for International Classification of Diseases, Tenth Revision, Clinical Modification (ICD-10-CM) codes.
Results:In our study population, there were 829 ARI visits per 1,000 enrollees in 2011 compared with 760 ARI visits per 1,000 enrollees in 2018. In 2011, 39.3% of ARI visits were associated with ≥1 oral antibiotic prescription versus 36.2% in 2018. In 2018 compared with 2011, overall ARI visits decreased 8% (PRR, 0.92; 99.99% confidence interval [CI], 0.92–0.92), whereas visits with antibiotic prescriptions decreased 16% (PRR, 0.84; 99.99% CI, 0.84–0.85). Visits for antibiotic-inappropriate ARIs decreased by 9% (PRR, 0.91; 99.99% CI, 0.91–0.92), and visits with antibiotic prescriptions for these conditions decreased by 32% (PRR, 0.68; 99.99% CI, 0.67–0.68) from 2011 to 2018.
Conclusions:Both the rate of antibiotic prescriptions per 1,000 enrollees and the percentage of visits with antibiotic prescriptions decreased modestly from 2011 to 2018 in our study population. These decreases were greatest for antibiotic-inappropriate ARIs; however, additional reductions in inappropriate antibiotic prescribing are needed.
Poster Presentation
Antibiotic Stewardship
Minimal Mortality Among Veterans with Urine Cultures Positive for Group B Streptococcus
- Nicole Mongilardi, Robin Jump, Federico Perez, Taissa Bej, Janet M Briggs, Richard Banks, Brigid Wilson, Sunah Song
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s36-s37
-
- Article
-
- You have access Access
- Open access
- Export citation
-
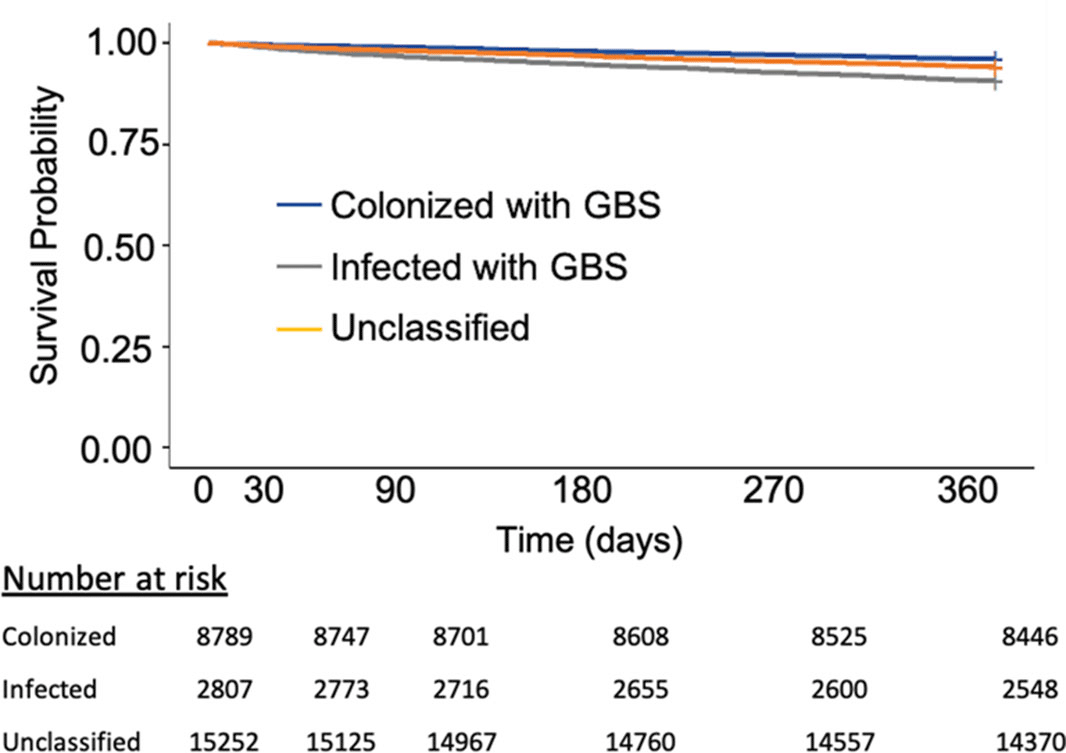
Background: Group B Streptococcus (GBS) can cause life-threating invasive infections, yet GBS is also a normal component of the intestinal and genitourinary tract. Although it is regarded as a potential urinary pathogen, the morbidity and mortality associated with recovery of GBS from urine cultures of nonpregnant adults is not well understood. We evaluated characteristics and mortality among nonpregnant adults with urine cultures that grew GBS. Methods: Using administrative data from the Veterans’ Healthcare Administration (VHA), we conducted a retrospective cohort study of VA healthcare system users from January 1, 2008, through December 31, 2017, with monomicrobial urine cultures growing ≥100,000 colony-forming units of GBS. Urinary tract infection (UTI) cases were defined as urinalysis positive for leukocyte esterase and pyuria (≥10 white blood cells), an International Classification of Diseases (ICD) code for UTI, and an antibiotic prescription. Cases with colonization were defined as negative for leukocyte esterase and pyuria, no ICD code for UTI, and no antibiotic prescription. Cases not meeting either definition were deemed unclassifiable. We compared demographics, comorbidities, and all-cause mortality among these 3 groups. Results: Over the 10-year study period, 26,848 veterans had 30,740 urine cultures positive for GBS. Applying the definitions above, there were 2,807 cases of infection, 8,789 cases of colonization, and 15,252 cases that were unclassifiable. Patients with a GBS UTI were slightly older compared to those who were colonized, with a higher Charlson comorbidity index and greater burden of chronic renal disease (Table 1). Individuals with infection versus colonization had 30-day mortality rates of 1% and 0%, respectively, and 1-year mortality rates of 9% and 4%, respectively (Figure 1). Conclusions: The association of a greater burden of illness among veterans who met our definition of UTI compared to colonization might be more reflective of providers’ responses to patients with chronic medical conditions rather than a difference in GBS as a cause of UTI. Overall, the prospect of a urine culture that grows GBS does not appear to be associated with adverse long-term outcomes.
Funding: No
Disclosures: None
Table 1. 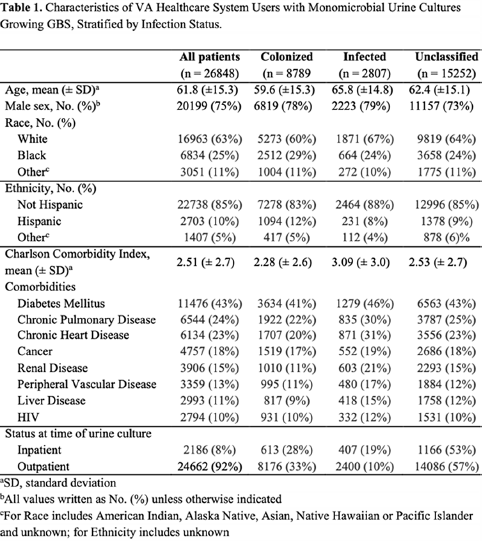
Figure 1.
Original Article
A retrospective analysis of community-onset bloodstream infections at a tertiary-care academic hospital in South Africa. Are current empiric antimicrobial practices appropriate?
- Vinitha Alex, Trusha Nana, Vindana Chibabhai
-
- Published online by Cambridge University Press:
- 21 December 2021, e67
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Community-onset bloodstream infection (CO-BSI) is associated with substantial morbidity and mortality. Knowledge of locally prevalent pathogens and antimicrobial susceptibility patterns can promptly guide appropriate empiric therapy and improve outcomes.
Objectives:We sought to determine the epidemiology of CO-BSI, the blood culture positivity rate and the contamination rate. We also sought to establish appropriateness of current empiric antimicrobial therapy practices.
Methods:We retrospectively analyzed blood cultures taken from January 2015 to December 2019 at the emergency departments (EDs) of a tertiary-care academic hospital in South Africa using extracted laboratory data.
Results:The overall positivity rate of blood cultures taken at the EDs was 15% (95% confidence interval [CI], 0.15–0.16) and the contamination rate was 7% (95% CI, 0.06–0.07). Gram-positive bacteria predominated in the pediatric cohort: neonates, 52 (54%) of 96; infants, 57 (52%) of 109; older children, 63 (61%) of 103. Methicillin-susceptible Staphylococcus aureus was the predominant pathogen among older children: 30 (35%) of 85. Escherichia coli was the most common pathogen isolated among adults and the elderly: 225 (21%) of 1,060 and 62 (29%) of 214, respectively. Among neonates, the susceptibility of E. coli and Klebsiella pneumoniae to the combination of ampicillin and gentamicin was 17 (68%) of 25. Among adults, the susceptibility of the 5 most common pathogens to amoxicillin-clavulanate was 426 (78%) of 546 and their susceptibility to ceftriaxone was 481 (85%) of 565 (P = .20). The prevalence of methicillin-resistant S. aureus, extended-spectrum β-lactamase–producing and carbapenem-resistant Enterobacterales were low among all age groups.
Conclusions:Review of blood culture collection techniques is warranted to reduce the contamination rate. High rates of resistance to currently prescribed empiric antimicrobial agents for CO-BSI warrants a re-evaluation of local guidelines.
Poster Presentation
Antibiotic Stewardship
Assessing Baccalaureate Nursing Students’ Antibiotic Stewardship Knowledge Using Virtual Standardized Patient Simulations
- Mary Lou Manning, Monika Pogorzelska-Maziarz, David Jack, Lori Wheeler
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s37
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: According to the Centers for Disease Control and Prevention, the single most important factor leading to the development of antibiotic resistance (AMR) is the use of antibiotics. Studies indicate that up to 50% of hospitalized patients receive at least 1 antibiotic, half of which are inappropriate. The outpatient setting accounts for >60% of antibiotic use and over half of these prescriptions are inappropriate. Antibiotic stewardship programs improve appropriate antibiotic use, reduce AMR, decrease complications of antibiotic use, and improve patient outcomes. Building a nursing workforce with necessary AMR and antibiotic stewardship knowledge and skill is critical. Nursing graduates can translate knowledge into practice, promoting the judicious use of antibiotics to keep patients safe from antibiotic harm. Methods: Third-year baccalaureate nursing students enrolled in a fall 2020 health promotion course at an urban university affiliated with an academic medical center participated. Students received a 3-hour lecture on antibiotics, AMR and antibiotic stewardship nursing practices and actively engaged in antibiotic stewardship simulations using standardized patient (SP) encounters. The SP participants were specifically trained for these activities. Simulations included a 30-minute brief before and a 60-minute briefing after the activities. All activities occurred via video conferencing. Case scenarios, developed by the authors, focused on penicillin-allergy delabeling of an adolescent prior to elective surgery and appropriate use of antibiotics in managing pediatric urinary tract infections and acute otitis media (AOM). Before-and-after tests were used to assess the impact on AMR and antibiotic stewardship knowledge. Results: Over a period of 4 days, all enrolled students (n = 165) participated in 1 three-hour virtual simulation session. Using Zoom video conferencing with multiple breakout rooms, the activities were easily managed. During the simulations, students often struggled with reading an antibiogram and applying the concept of “watchful waiting” in AOM management. Significant differences were found in before-and-after test results, with significant improvement in students’ general and specific knowledge and awareness of antibiotics (P < .01). During the debriefing sessions, students reported increased awareness related to their role in advancing the judicious use of antibiotics. Conclusions: Initially, we planned to conduct in-person SP simulations. Due to the COVID-19 pandemic, faculty and students demonstrated remarkable flexibility and resilience as we successfully converted to a virtual format. Virtual lecture and SP simulations, followed by debriefing, was an effective approach to educate baccalaureate nursing students about AMR and their role in antibiotic stewardship. Areas for course content improvement were identified.
Funding: No
Disclosures: None
How the COVID-19 Pandemic Affected Antimicrobial Prescribing Practices at a Tertiary-Care Healthcare System in Detroit, Michigan
- Angela Beatriz Cruz, Jennifer LeRose, Avnish Sandhu, Teena Chopra
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s37-s38
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Inappropriate antimicrobial use continues to threaten modern medicine. The ongoing pandemic likely exacerbated this problem because COVID-19 presents similarly to bacterial pneumonia, confusion exists regarding treatment guidelines, and testing turnaround times (TATs) are slow. Our primary object was to quantify antimicrobial use changes during the pandemic to rates before the crisis. A subanalysis within the COVID-19 cohort was completed based on SARS-CoV-2 status. Methods: The pre–COVID-19 period was January–May 2019 and the COVID-19 period was January–May 2020. Subanalyses were used to explore differences in antibiotics use between persons not under investigation (non-PUIs), SARS-CoV-2–negative PUIs, and SARS-CoV-2–positive PUIs. Non-PUI patients were those without respiratory symptoms and/or fever. The χ2 and Wilcoxon signed rank-sum tests were used for analysis. Results: During the 2019 and 2020 study periods, 7,909 and 7,283 patients received >1 antimicrobial, respectively (Figure 1). Overall, antibiotic therapy per 1,000 patient days increased from 633.1 before COVID-19 to 678.5 during COVID-19, a 7.2% increase (Table 1). Notably, broad-spectrum respiratory antibiotics demonstrated a significant increase between pre–COVID-19 and COVID-19 cohorts (p < 0.001). Of the 7,283 patients within the COVID-19 cohort, 34.7% (n = 2,532) were PUI and 13.8% (n = 1,002) of these patients tested SARS-CoV-2 positive. Again, broad-spectrum respiratory antibiotics use was significantly increased for COVID-19 patients (p < 0.001). Of note, the proportion of patients receiving respiratory antibiotics steadily decreased over time (R2 = 0.99). Conclusions: There was a significant increase in antibiotic use during the COVID-19 pandemic. Encouragingly, antimicrobial use decreased over time, likely due to (1) faster TATs, (2) real-time education to clinicians and subsequent de-escalation of unnecessary antimicrobials, and (3) development of treatment guidelines as new research emerged.
Funding: No
Disclosures: None
Figure 1.
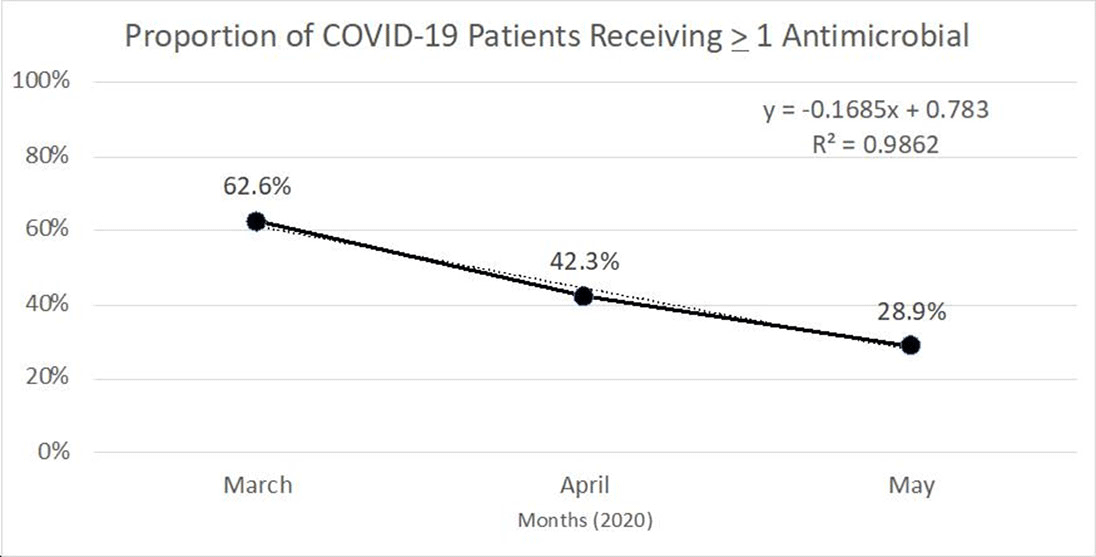
Table 1. 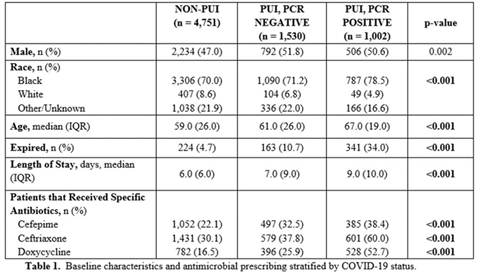
Original Article
Outpatient antifungal prescribing patterns in the United States, 2018
- Kaitlin Benedict, Sharon V. Tsay, Monina G. Bartoces, Snigdha Vallabhaneni, Brendan R. Jackson, Lauri A. Hicks
-
- Published online by Cambridge University Press:
- 22 December 2021, e68
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Widespread inappropriate antibiotic prescribing is a major driver of resistance. Little is known about antifungal prescribing practices in the United States, which is concerning given emerging resistance in fungi, particularly to azole antifungal agents.
Objective:We analyzed outpatient antifungal prescribing data in the United States to inform stewardship efforts.
Design:Descriptive analysis of outpatient antifungal prescriptions dispensed during 2018 in the IQVIA Xponent database.
Methods:Prescriptions were summarized by drug, sex, age, geography, and healthcare provider specialty. Census denominators were used to calculate prescribing rates among demographic groups.
Results:Healthcare providers prescribed 22.4 million antifungal courses in 2018 (68 prescriptions per 1,000 persons). Fluconazole was the most commonly prescribed drug (75%), followed by terbinafine (11%) and nystatin (10%). Prescription rates were higher among females versus males (110 vs 25 per 1,000 population) and adults versus children (82 vs 27 per 1,000 population). Prescription rates were highest in the South (81 per 1,000 population) and lowest in the West (48 per 1,000 population). Nurse practitioners and family practitioners prescribed the most antifungals (43% of all prescriptions), but the highest prescribing rates were among obstetrician-gynecologists (84 per provider).
Conclusions:Prescribing antifungal drugs in the outpatient setting is common, with enough courses dispensed for 1 in every 15 US residents in 2018. Fluconazole use patterns suggest vulvovaginal candidiasis as a common indication. Regional prescribing differences could reflect inappropriate use or variations in disease burden. Further study of higher antifungal use in the South could help target antifungal stewardship practices.
Poster Presentation
Antibiotic Stewardship
Evaluation of Penicillin Allergy Prevalence and Antibiotic Prescribing Patterns for Patients within the Emergency Department
- Ashlyn Norris, Lindsay Daniels, Nikolaos Mavrogiorgos, Kalynn Northam, Mildred Kwan, Gary Burke, Renae Boerneke
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s38
-
- Article
-
- You have access Access
- Open access
- Export citation
-
As the point of entry into healthcare for many patients, the emergency department (ED) is an ideal setting in which to assess penicillin (PCN) allergies. An estimated 10% of the United States population has a reported PCN allergy; however, few studies have evaluated the prevalence and impact of PCN allergies on antibiotic selection within the ED. Patients with a documented PCN allergy are more likely to be exposed to costly alternative broad-spectrum antibiotics that have higher rates of adverse events, including C. difficile infections. We sought to determine the prevalence of PCN allergies within the UNC Medical Center ED. Key secondary outcomes included the percentage of patients with a documented PCN allergy who (1) received alternative antibiotics (carbapenems, aztreonam, fluoroquinolones, clindamycin, vancomycin), (2) received β-lactam antibiotics and experienced an allergic reaction during their ED visit, and/or (3) had received a β-lactam antibiotic during a past hospitalization or ED visit without their chart being appropriately updated. A retrospective evaluation included patients aged >18 years with a documented PCN allergy who were discharged from the ED between January 1, 2017, and December 31, 2019. Over the study period, there were 14,635 patient encounters with a documented PCN allergy that comprised 8,573 unique patients. The prevalence of PCN allergies was 14.3% for all ED encounters. PCN allergy–labeled patients received alternative antibiotics in 59.4% of ED encounters in which antibiotics were prescribed. Of the 454 β-lactam antibiotics (62 penicillins, 380 cephalosporins, 12 carbapenems) administered to PCN allergy-labeled patients within the ED, there were zero allergic reactions. Also, 18.6% of PCN allergy-labeled patients had received and tolerated a β-lactam antibiotic during prior hospitalizations or ED visits (1.7% penicillins, 14.4% cephalosporins, 2.6% carbapenems) without appropriate updated documentation to reflect β-lactam antibiotic tolerance. These findings confirm the utilization of non–β-lactam antibiotics in PCN allergy-labeled patients, highlighting the importance of accurate and updated allergy documentation in the electronic medical record. These findings also demonstrate the need for improved allergy documentation and protocols to proactively assess penicillin allergy labels while in the ED.
Funding: No
Disclosures: None
Concise Communication
Caregiver perspectives and preferences for acute otitis media management
- Holly M. Frost, Amy Keith, Thresia Sebastian, Timothy C. Jenkins
-
- Published online by Cambridge University Press:
- 22 December 2021, e69
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Surveyed caregivers of children in Denver, Colorado, with acute otitis media (AOM) preferred immediate antibiotics over delayed antibiotics or observation. Overall, 77% stated that they would immediately fill a prescription written as delayed. In contrast, 86% of caregivers favored whichever duration was recommended by the provider or the shortest duration necessary.
Original Article
Improving antimicrobial prescribing for upper respiratory infections in the emergency department: Implementation of peer comparison with behavioral feedback
- George F. Jones, Valeria Fabre, Jeremiah Hinson, Scott Levin, Matthew Toerper, Jennifer Townsend, Sara E. Cosgrove, Mustapha Saheed, Eili Y. Klein
-
- Published online by Cambridge University Press:
- 23 December 2021, e70
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To reduce inappropriate antibiotic prescribing for acute respiratory infections (ARIs) by employing peer comparison with behavioral feedback in the emergency department (ED).
Design:A controlled before-and-after study.
Setting:The study was conducted in 5 adult EDs at teaching and community hospitals in a health system.
Patients:Adults presenting to the ED with a respiratory condition diagnosis code. Hospitalized patients and those with a diagnosis code for a non-respiratory condition for which antibiotics are or may be warranted were excluded.
Interventions:After a baseline period from January 2016 to March 2018, 3 EDs implemented a feedback intervention with peer comparison between April 2018 and December 2019 for attending physicians. Also, 2 EDs in the health system served as controls. Using interrupted time series analysis, the inappropriate ARI prescribing rate was calculated as the proportion of antibiotic-inappropriate ARI encounters with a prescription. Prescribing rates were also evaluated for all ARIs. Attending physicians at intervention sites received biannual e-mails with their inappropriate prescribing rate and had access to a dashboard that was updated daily showing their performance relative to their peers.
Results:Among 28,544 ARI encounters, the inappropriate prescribing rate remained stable at the control EDs between the 2 periods (23.0% and 23.8%). At the intervention sites, the inappropriate prescribing rate decreased significantly from 22.0% to 15.2%. Between periods, the overall ARI prescribing rate was 38.1% and 40.6% in the control group and 35.9% and 30.6% in the intervention group.
Conclusions:Behavioral feedback with peer comparison can be implemented effectively in the ED to reduce inappropriate prescribing for ARIs.
Poster Presentation
Antibiotic Stewardship
Impact of an Inpatient Nurse-Initiated Penicillin Allergy Delabeling Questionnaire
- Lauren Dutcher, Hilary Bediako, Christina Harker, Aditi Rao, Kristen Sigafus, Keith Hamilton, Olajumoke Fadugba
-
- Published online by Cambridge University Press:
- 29 July 2021, pp. s38-s39
-
- Article
-
- You have access Access
- Open access
- Export citation
-
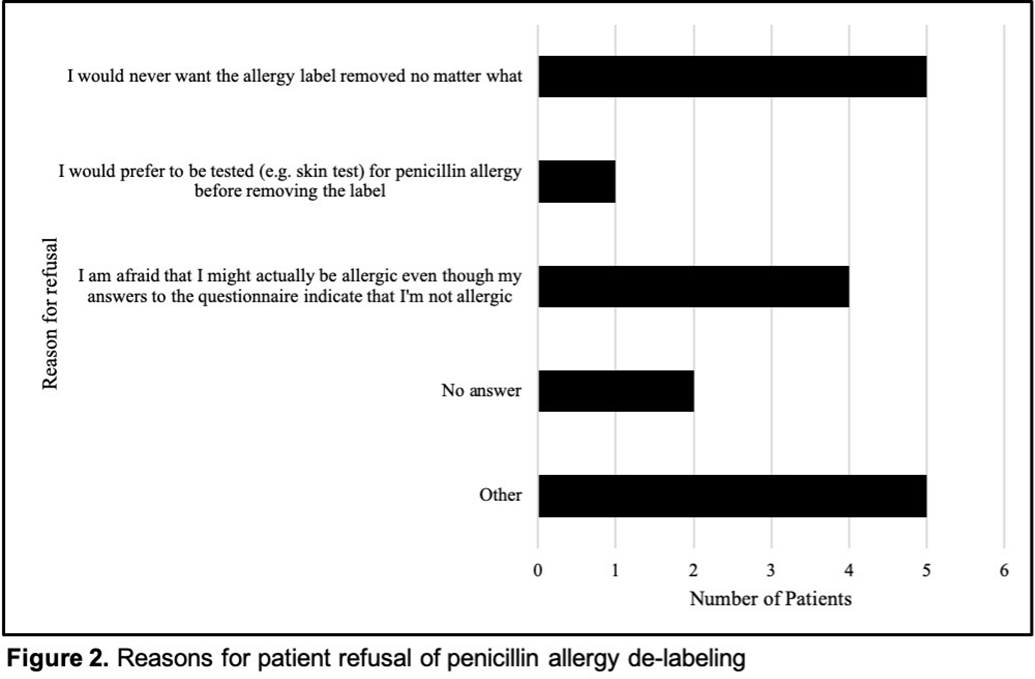
Background: Penicillin allergy is the most common drug allergy, with ~10% of all patients in the United States reporting a penicillin allergy. A penicillin allergy label is associated with the use of inappropriate or broad-spectrum antibiotics, worse patient outcomes, increased bacterial resistance, and increased healthcare costs, yet no studies have explored the unique role nurses may play in allergy delabeling through history taking as a part of broader antimicrobial stewardship efforts. Here, we describe the impact of using an inpatient nurse-initiated penicillin-allergy questionnaire. Methods: We implemented a nurse-driven intervention focused on penicillin allergy delabeling in inpatient noncritical care units (surgery, neurology, medicine, oncology, and cardiovascular medicine) at an academic hospital from July 9, 2019, to July 24, 2020. Patients with a penicillin allergy listed in the electronic health record (EHR) were identified and invited to participate. The intervention consisted of a questionnaire administered by nurses who elicited details of penicillin allergy history. If a patient was deemed eligible for penicillin allergy removal, nurses requested approval from both the patient as well as a physician member of the study team. Results: In total, 306 patients with a penicillin allergy label were identified in the EHR, of whom 242 patients were eligible for and agreed to participate in the delabeling interview (Figure 1). Of the 34 (14%) of 242 patients potentially eligible for delabeling by the questionnaire based on their history, the study physicians agreed with delabeling for 23 (68%) of 34 patients. Of these 34 patients, 18 (53%) agreed with delabeling (pending physician approval), and 16 (47%) of these 34 patients were ultimately delabeled. For those who declined delabeling, never wanting the label removed under any circumstance and uncertainty about accuracy of the survey results were common reasons for refusal (Figure 2). Additionally, for the 13 patients who refused delabeling, 9 patients did not want or were unsure about following up with an allergy specialist. Conclusions: The nurse-driven penicillin-allergy delabeling questionnaire is a no-cost intervention that can successfully identify patients to delabel. In this study, this measure resulted in the removal of 16 (7%) of 242 penicillin allergy labels. However, patients frequently opted to keep penicillin allergy labels, expressing uncertainty and fear of removal. Future work should explore optimal methods to engage nurses and patients in allergy delabeling, as well as the impact on antibiotic use and patient outcomes.
Funding: No
Disclosures: None
Figure 1.
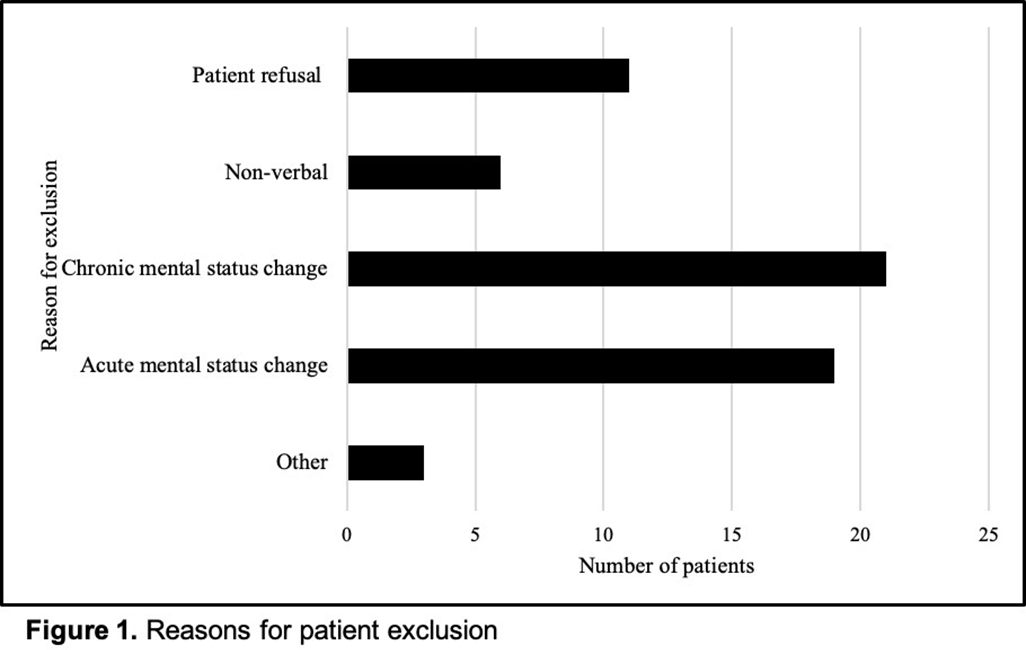
Figure 2.
Evaluation of Penicillin Allergies and an Allergy Assessment Pilot in the Emergency Department
- Ashlyn Norris, Kalynn Northam, Lindsay Daniels, Mildred Kwan, Gary Burke, Nikolaos Mavrogiorgos, Renae Boerneke
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s39
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Penicillin (PCN) allergy is one of the most frequently reported medication allergies, with ~10% of the US population reporting a PCN allergy. However, studies have shown that only 1% of the US population have a true IgE-mediated reaction to PCN. Delabeling and appropriately updating patient allergy profiles could decrease the use of alternative broad-spectrum antibiotics, rates of infectious complications [C. difficile, methicillin-resistant Staphylococcus aureus (MRSA), vancomycin-resistant Enterococcus (VRE)], antibiotic resistance, and overall healthcare cost. The emergency department (ED) is an important setting in which to assess PCN allergies and to delabel patients when appropriate because there are >130 million ED visits in the United States each year. We sought to determine the percentage of PCN allergy–labeled patients who could be delabeled through a PCN allergy assessment interview in an ED. Key secondary outcomes included the percentage of interviewed patients who could not be delabeled based on history alone but would be eligible for an amoxicillin oral challenge or a PCN skin test (PST). A prospective PCN allergy assessment pilot was performed for patients aged >18 years presenting to the UNC Medical Center ED between December 1 and December 17, 2020, with a documented PCN allergy. A pharmacist conducted penicillin allergy assessments on a convenience sample of patients presenting to the ED between 8 a.m. and 3 p.m. on weekdays. Based on patients’ reported and documented histories, charts were updated with the most accurate information and allergies were delabeled if appropriate. In total, 95 patients were assessed; 62 (65.3%) were interviewed and 15 (24.2%) were delabeled. In addition, 26 patients (41.9%) were deemed eligible for an oral amoxicillin challenge, 19 (30.6%) qualified for a PST, and 2 (3.2%) patients did not qualify for further assessment due to having a an IgE-mediated reaction in the past 5 years. Of the 15 patients who were delabeled, 6 (40.0%) received antibiotics during their admission: 4 (73.3%) of those patients received a penicillin and 2 (36.7%) received a cephalosporin, all without adverse reactions. Patient assessments took ~20 minutes to complete, including chart review, patient interview, and postinterview chart updating. The results from this pilot study demonstrate the impact of performing PCN allergy assessments in ED. Interdisciplinary opportunities should be explored to develop processes that will improve the efficiency and sustainability of PCN allergy assessments within the ED to allow this important stewardship intervention to continue.
Funding: No
Disclosures: None
Associations Between Patient Neighborhood Characteristics and Inappropriate Antimicrobial Use
- Joseph Engeda, Jane Kriengkauykiat, Erin Epson
-
- Published online by Cambridge University Press:
- 29 July 2021, p. s39
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Background: Antimicrobials are among the most commonly prescribed medications in US hospitals; an estimated 50% of hospitalized patients receive an antimicrobial. Research has shown that antimicrobial prescriptions to vary by patient- and hospital-level factors; however, disparities by patient neighborhood characteristics have not been examined. We evaluated associations between hospital and neighborhood indicators of socioeconomic status (SES) and antimicrobial use (AU) for gram-positive bacterial infections (GPBs), and broad-spectrum use for community-acquired infections (BSCAs) and hospital-onset infections (BSHOs). Methods: This analysis was conducted among 86 acute-care hospitals in California that submitted AU data via the NHSN in 2019. Hospital-level AU was measured as standardized antimicrobial administration ratios (SAARs) calculated by dividing observed antimicrobial use by risk-adjusted predicted antimicrobial use for GPB, BSCA, and BSHO antimicrobial groupings and categorized as binary (>1 or <1); SAARs >1 indicate potential inappropriate prescribing. California Office of Statewide Health Planning and Development 2018 data were used to obtain hospital characteristics and patient age, race or ethnicity, insurance, and comorbidities (defined by Charlson comorbidity index) for hospitalizations where AU may have been indicated, based on International Classification of Diseases Tenth Revision (ICD-10) diagnosis codes. The California Healthy Places Index (HPI) was used to obtain composite neighborhood SES indicators for each patient at the ZIP code level, measured as tertiles. Covariates were aggregated to the hospital level. Poisson regressions were used to evaluate the association between hospital and neighborhood SES indicators and SAAR scores, controlling for potential hospital-level confounders. Results: Among 86 hospitals included in the analysis, the mean patient age for hospitalizations where AU may have been indicated was 66 years, the proportion of white patients was 55%, and the mean proportion of Medi-Cal users was 19%. After adjusting for confounders including age, race or ethnicity, insurance status, comorbidities, and number of hospital beds; higher median values of patient SES had a protective effect against hospitals having GP SAAR scores > 1 (relative risk [RR], 0.68; 95% CI, 0.50–0.93) but was not significantly associated with hospitals having BSCA SAAR scores >1 (RR, 0.79; 95% CI, 0.62–1.02) or BSHO SAAR scores >1 (RR, 0.80; 95% CI, 0.61–1.04). Conclusions: Considering SES in addition to summary antimicrobial use scores such as SAARs may help identify populations potentially at risk for inappropriate AU; however, patient-level information is still necessary to evaluate appropriateness of antimicrobial prescribing.
Funding: No
Disclosures: None














