22 results
Factors influencing healthcare personnel decision making to work with respiratory symptoms during the COVID-19 pandemic
- Rachel Meyer, Michael Kessler, Daniel Shirley, Linda Stevens, Fauzia Osman, Nasia Safdar
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s57-s58
-
- Article
-
- You have access Access
- Open access
- Export citation
-
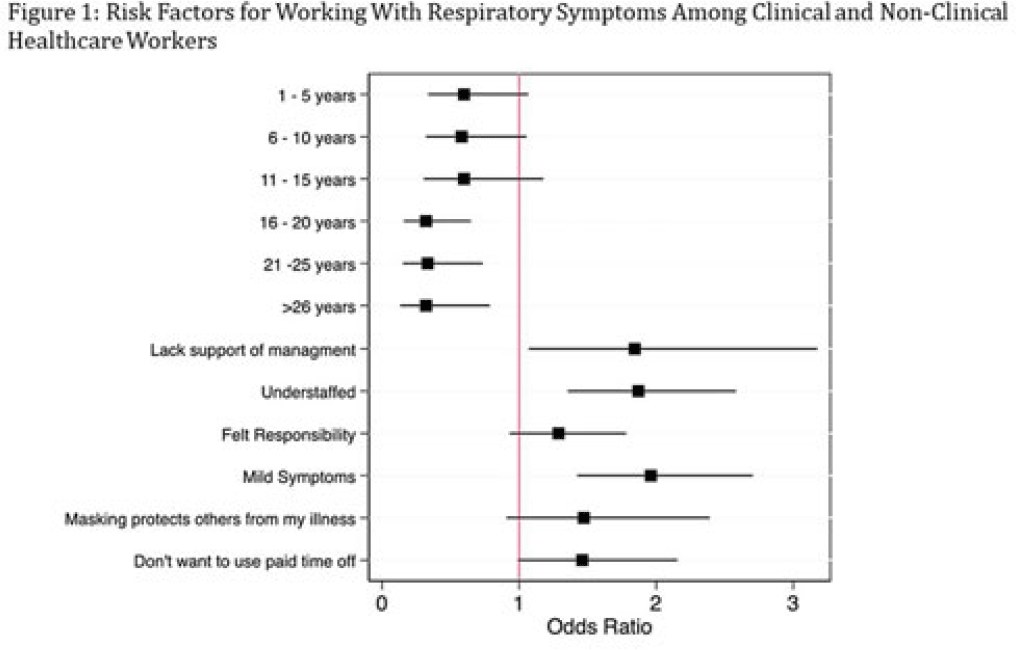
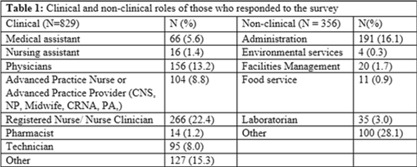
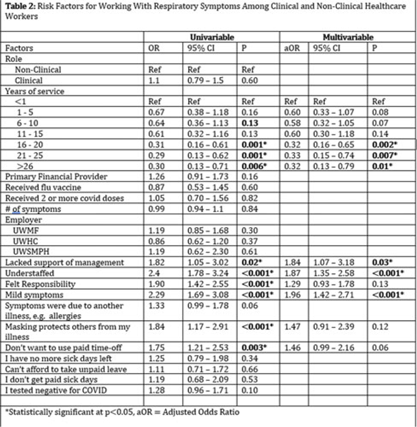
Background: Amid the COVID-19 pandemic, healthcare systems were stretched thin, with staffing shortages posing substantial challenges. Limiting spread of COVID-19 among healthcare professionals (HCP) is paramount to preventing exacerbation of such shortages, but strategies are highly dependent on HCP self-screening for symptoms and isolating when present. We examined HCP perceptions of barriers and factors that facilitate staying home when experiencing respiratory symptoms. Methods: At an academic tertiary-care referral center, in inpatient and ambulatory settings, we conducted an anonymous electronic survey between March 11, 2022, and April 12, 2022. Using logistic regression analysis, we analyzed predictors of employees reporting to work with respiratory symptoms using STATA and SAS software. Results: In total, 1,185 individuals including 829 clinical staff and 356 nonclinical staff responded to the survey. When excluding participants who reported working “remotely” (N = 381) and those who reported being unsure of whether they had worked with symptoms (N = 14), the prevalence of working with respiratory symptoms was 63%. There was no significant difference between clinical and nonclinical staff (OR, 1.1; 95% CI, 0.8–1.5; P = .60). Increasing number of years of service was protective against working with symptoms, achieving statistically significance in multivariable analysis after 16 years. Compared to those having worked <1 year, the odds ratios of working with symptoms were 0.32 (95% CI, 0.16–0.65; P = .002), 0.33 (95% CI, 0.15–0.74; P = .007), and 0.32 (95% CI, 0.13–0.79; P = .007) for those working 16–20 years, 21–25 years, and ≥26 years, respectively. More than half of HCP who worked with symptoms identified being understaffed (56.9%), having mild symptoms (55.3%), and sense of responsibility (55.1%) as reasons to work with respiratory symptoms. The following barriers, or reasons to work with symptoms, were more commonly identified as significant by those who worked with symptoms compared to those who did not: being understaffed (OR, 1.87; 95% CI, 1.35–2.58; P ≤ .001), having mild symptoms (OR, 1.96; 95% CI, 1.42–2.71; P < .001), and lack of support from management (OR, 1.84; 95% CI, 1.07–3.18; P = .03). Conclusions: Working with respiratory symptoms is prevalent in clinical and nonclinical HCP. Those with fewer years of work experience appear to be more susceptible to misconceptions and pressures to work despite respiratory symptoms. Messaging should stress support from leadership and the significance of even mild respiratory symptoms and should emphasize responsibility to patients and colleagues to stay home with respiratory symptoms. Strategies to ensure adequate staffing and sick leave may also be high yield.
Disclosures: None
Patterns, predictors, and patient-reported reasons for antidepressant discontinuation in the WHO World Mental Health Surveys
- Alan E. Kazdin, Meredith G. Harris, Irving Hwang, Nancy A. Sampson, Dan J. Stein, Maria Carmen Viana, Daniel V. Vigo, Chi-Shin Wu, Sergio Aguilar-Gaxiola, Jordi Alonso, Corina Benjet, Ronny Bruffaerts, José Miguel Caldas-Almeida, Graça Cardoso, Elisa Caselani, Stephanie Chardoul, Alfredo Cía, Peter de Jonge, Oye Gureje, Josep Maria Haro, Elie G. Karam, Viviane Kovess-Masfety, Fernando Navarro-Mateu, Marina Piazza, José Posada-Villa, Kate M. Scott, Juan Carlos Stagnaro, Margreet ten Have, Yolanda Torres, Cristian Vladescu, Ronald C. Kessler
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 14 September 2023, pp. 67-78
-
- Article
- Export citation
-
Background
Despite their documented efficacy, substantial proportions of patients discontinue antidepressant medication (ADM) without a doctor's recommendation. The current report integrates data on patient-reported reasons into an investigation of patterns and predictors of ADM discontinuation.
MethodsFace-to-face interviews with community samples from 13 countries (n = 30 697) in the World Mental Health (WMH) Surveys included n = 1890 respondents who used ADMs within the past 12 months.
Results10.9% of 12-month ADM users reported discontinuation-based on recommendation of the prescriber while 15.7% discontinued in the absence of prescriber recommendation. The main patient-reported reason for discontinuation was feeling better (46.6%), which was reported by a higher proportion of patients who discontinued within the first 2 weeks of treatment than later. Perceived ineffectiveness (18.5%), predisposing factors (e.g. fear of dependence) (20.0%), and enabling factors (e.g. inability to afford treatment cost) (5.0%) were much less commonly reported reasons. Discontinuation in the absence of prescriber recommendation was associated with low country income level, being employed, and having above average personal income. Age, prior history of psychotropic medication use, and being prescribed treatment from a psychiatrist rather than from a general medical practitioner, in comparison, were associated with a lower probability of this type of discontinuation. However, these predictors varied substantially depending on patient-reported reasons for discontinuation.
ConclusionDropping out early is not necessarily negative with almost half of individuals noting they felt better. The study underscores the diverse reasons given for dropping out and the need to evaluate how and whether dropping out influences short- or long-term functioning.
Evaluation of an experiential training program in patient-centered outcomes and comparative effectiveness research for diverse researcher communities and health care organizations
- Dedra S. Buchwald, Megan H. Rogers, Barbara A. Rose, Brian W. Bresnahan, Beth Devine, Linda LeResche, Lonnie A. Nelson, Donald L. Patrick, Danielle C. Lavallee, Michelle M. Garrison, Andrew A. White, Larry G. Kessler
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue 1 / 2023
- Published online by Cambridge University Press:
- 15 March 2023, e81
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background/Objective:
The goal of the Patient-Centered Outcomes Research Partnership was to prepare health care professionals and researchers to conduct patient-centered outcomes and comparative effectiveness research (CER). Substantial evidence gaps, heterogeneous health care systems, and decision-making challenges in the USA underscore the need for evidence-based strategies.
Methods:We engaged five community-based health care organizations that serve diverse and underrepresented patient populations from Hawai’i to Minnesota. Each partner nominated two in-house scholars to participate in the 2-year program. The program focused on seven competencies pertinent to patient-centered outcomes and CER. It combined in-person and experiential learning with asynchronous, online education, and created adaptive, pragmatic learning opportunities and a Summer Institute. Metrics included the Clinical Research Appraisal Inventory (CRAI), a tool designed to assess research self-efficacy and clinical research skills across 10 domains.
Results:We trained 31 scholars in 3 cohorts. Mean scores in nine domains of the CRAI improved; greater improvement was observed from the beginning to the midpoint than from the midpoint to conclusion of the program. Across all three cohorts, mean scores on 52 items (100%) increased (p ≤ 0.01), and 91% of scholars reported the program improved their skills moderately/significantly. Satisfaction with the program was high (91%).
Conclusions:Investigators that conduct patient-centered outcomes and CER must know how to collaborate with regional health care systems to identify priorities; pose questions; design, conduct, and disseminate observational and experimental research; and transform knowledge into practical clinical applications. Training programs such as ours can facilitate such collaborations.
Antidepressant use and risk of adverse outcomes: population-based cohort study
- Narinder Bansal, Mohammed Hudda, Rupert A. Payne, Daniel J. Smith, David Kessler, Nicola Wiles
-
- Journal:
- BJPsych Open / Volume 8 / Issue 5 / September 2022
- Published online by Cambridge University Press:
- 13 September 2022, e164
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Antidepressants are one of the most widely prescribed drugs in the global north. However, little is known about the health consequences of long-term treatment.
AimsThis study aimed to investigate the association between antidepressant use and adverse events.
MethodThe study cohort consisted of UK Biobank participants whose data was linked to primary care records (N = 222 121). We assessed the association between antidepressant use by drug class (selective serotonin reuptake inhibitors (SSRIs) and ‘other’) and four morbidity (diabetes, hypertension, coronary heart disease (CHD), cerebrovascular disease (CV)) and two mortality (cardiovascular disease (CVD) and all-cause) outcomes, using Cox's proportional hazards model at 5- and 10-year follow-up.
ResultsSSRI treatment was associated with decreased risk of diabetes at 5 years (hazard ratio 0.64, 95% CI 0.49–0.83) and 10 years (hazard ratio 0.68, 95% CI 0.53–0.87), and hypertension at 10 years (hazard ratio 0.77, 95% CI 0.66–0.89). At 10-year follow-up, SSRI treatment was associated with increased risks of CV (hazard ratio 1.34, 95% CI 1.02–1.77), CVD mortality (hazard ratio 1.87, 95% CI 1.38–2.53) and all-cause mortality (hazard ratio 1.73, 95% CI 1.48–2.03), and ‘other’ class treatment was associated with increased risk of CHD (hazard ratio 1.99, 95% CI 1.31–3.01), CVD (hazard ratio 1.86, 95% CI 1.10–3.15) and all-cause mortality (hazard ratio 2.20, 95% CI 1.71–2.84).
ConclusionsOur findings indicate an association between long-term antidepressant usage and elevated risks of CHD, CVD mortality and all-cause mortality. Further research is needed to assess whether the observed associations are causal, and elucidate the underlying mechanisms.
Antidepressant use in low- middle- and high-income countries: a World Mental Health Surveys report
- Alan E. Kazdin, Chi-Shin Wu, Irving Hwang, Victor Puac-Polanco, Nancy A. Sampson, Ali Al-Hamzawi, Jordi Alonso, Laura Helena Andrade, Corina Benjet, José-Miguel Caldas-de-Almeida, Giovanni de Girolamo, Peter de Jonge, Silvia Florescu, Oye Gureje, Josep M. Haro, Meredith G. Harris, Elie G. Karam, Georges Karam, Viviane Kovess-Masfety, Sing Lee, John J. McGrath, Fernando Navarro-Mateu, Daisuke Nishi, Bibilola D. Oladeji, José Posada-Villa, Dan J. Stein, T. Bedirhan Üstün, Daniel V. Vigo, Zahari Zarkov, Alan M. Zaslavsky, Ronald C. Kessler, the WHO World Mental Health Survey collaborators
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 4 / March 2023
- Published online by Cambridge University Press:
- 23 September 2021, pp. 1583-1591
-
- Article
- Export citation
-
Background
The most common treatment for major depressive disorder (MDD) is antidepressant medication (ADM). Results are reported on frequency of ADM use, reasons for use, and perceived effectiveness of use in general population surveys across 20 countries.
MethodsFace-to-face interviews with community samples totaling n = 49 919 respondents in the World Health Organization (WHO) World Mental Health (WMH) Surveys asked about ADM use anytime in the prior 12 months in conjunction with validated fully structured diagnostic interviews. Treatment questions were administered independently of diagnoses and asked of all respondents.
Results3.1% of respondents reported ADM use within the past 12 months. In high-income countries (HICs), depression (49.2%) and anxiety (36.4%) were the most common reasons for use. In low- and middle-income countries (LMICs), depression (38.4%) and sleep problems (31.9%) were the most common reasons for use. Prevalence of use was 2–4 times as high in HICs as LMICs across all examined diagnoses. Newer ADMs were proportionally used more often in HICs than LMICs. Across all conditions, ADMs were reported as very effective by 58.8% of users and somewhat effective by an additional 28.3% of users, with both proportions higher in LMICs than HICs. Neither ADM class nor reason for use was a significant predictor of perceived effectiveness.
ConclusionADMs are in widespread use and for a variety of conditions including but going beyond depression and anxiety. In a general population sample from multiple LMICs and HICs, ADMs were widely perceived to be either very or somewhat effective by the people who use them.
Dissecting the heterogeneity of posttraumatic stress disorder: differences in polygenic risk, stress exposures, and course of PTSD subtypes
- Laura Campbell-Sills, Xiaoying Sun, Karmel W. Choi, Feng He, Robert J. Ursano, Ronald C. Kessler, Daniel F. Levey, Jordan W. Smoller, Joel Gelernter, Sonia Jain, Murray B. Stein
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 15 / November 2022
- Published online by Cambridge University Press:
- 05 May 2021, pp. 3646-3654
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Definition of disorder subtypes may facilitate precision treatment for posttraumatic stress disorder (PTSD). We aimed to identify PTSD subtypes and evaluate their associations with genetic risk factors, types of stress exposures, comorbidity, and course of PTSD.
MethodsData came from a prospective study of three U.S. Army Brigade Combat Teams that deployed to Afghanistan in 2012. Soldiers with probable PTSD (PTSD Checklist for Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition ≥31) at three months postdeployment comprised the sample (N = 423) for latent profile analysis using Gaussian mixture modeling and PTSD symptom ratings as indicators. PTSD profiles were compared on polygenic risk scores (derived from external genomewide association study summary statistics), experiences during deployment, comorbidity at three months postdeployment, and persistence of PTSD at nine months postdeployment.
ResultsLatent profile analysis revealed profiles characterized by prominent intrusions, avoidance, and hyperarousal (threat-reactivity profile; n = 129), anhedonia and negative affect (dysphoric profile; n = 195), and high levels of all PTSD symptoms (high-symptom profile; n = 99). The threat-reactivity profile had the most combat exposure and the least comorbidity. The dysphoric profile had the highest polygenic risk for major depression, and more personal life stress and co-occurring major depression than the threat-reactivity profile. The high-symptom profile had the highest rates of concurrent mental disorders and persistence of PTSD.
ConclusionsGenetic and trauma-related factors likely contribute to PTSD heterogeneity, which can be parsed into subtypes that differ in symptom expression, comorbidity, and course. Future studies should evaluate whether PTSD typology modifies treatment response and should clarify distinctions between the dysphoric profile and depressive disorders.
Toward measuring effective treatment coverage: critical bottlenecks in quality- and user-adjusted coverage for major depressive disorder
- Daniel Vigo, Josep Maria Haro, Irving Hwang, Sergio Aguilar-Gaxiola, Jordi Alonso, Guilherme Borges, Ronny Bruffaerts, Jose Miguel Caldas-de-Almeida, Giovanni de Girolamo, Silvia Florescu, Oye Gureje, Elie Karam, Georges Karam, Viviane Kovess-Masfety, Sing Lee, Fernando Navarro-Mateu, Akin Ojagbemi, Jose Posada-Villa, Nancy A. Sampson, Kate Scott, Juan Carlos Stagnaro, Margreet ten Have, Maria Carmen Viana, Chi-Shin Wu, Somnath Chatterji, Pim Cuijpers, Graham Thornicroft, Ronald C. Kessler
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 10 / July 2022
- Published online by Cambridge University Press:
- 20 October 2020, pp. 1948-1958
-
- Article
- Export citation
-
Background
Major depressive disorder (MDD) is a leading cause of morbidity and mortality. Shortfalls in treatment quantity and quality are well-established, but the specific gaps in pharmacotherapy and psychotherapy are poorly understood. This paper analyzes the gap in treatment coverage for MDD and identifies critical bottlenecks.
MethodsSeventeen surveys were conducted across 15 countries by the World Health Organization-World Mental Health Surveys Initiative. Of 35 012 respondents, 3341 met DSM-IV criteria for 12-month MDD. The following components of effective treatment coverage were analyzed: (a) any mental health service utilization; (b) adequate pharmacotherapy; (c) adequate psychotherapy; and (d) adequate severity-specific combination of both.
ResultsMDD prevalence was 4.8% (s.e., 0.2). A total of 41.8% (s.e., 1.1) received any mental health services, 23.2% (s.e., 1.5) of which was deemed effective. This 90% gap in effective treatment is due to lack of utilization (58%) and inadequate quality or adherence (32%). Critical bottlenecks are underutilization of psychotherapy (26 percentage-points reduction in coverage), underutilization of psychopharmacology (13-point reduction), inadequate physician monitoring (13-point reduction), and inadequate drug-type (10-point reduction). High-income countries double low-income countries in any mental health service utilization, adequate pharmacotherapy, adequate psychotherapy, and adequate combination of both. Severe cases are more likely than mild-moderate cases to receive either adequate pharmacotherapy or psychotherapy, but less likely to receive an adequate combination.
ConclusionsDecision-makers need to increase the utilization and quality of pharmacotherapy and psychotherapy. Innovations such as telehealth for training and supervision plus non-specialist or community resources to deliver pharmacotherapy and psychotherapy could address these bottlenecks.
Like a Bat Out of…. the Hospital? Development of a Bat Capture and Testing Protocol Prompted by Two Nosocomial Encounters
- Michael Kessler, Daniel Shirley, Laura Anderson, Nasia Safdar
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 41 / Issue S1 / October 2020
- Published online by Cambridge University Press:
- 02 November 2020, p. s314
- Print publication:
- October 2020
-
- Article
-
- You have access Access
- Export citation
-
Background: In the state of Wisconsin, 3%–4% of bats submitted for rabies testing are positive. Inpatient bat encounters at 2 affiliated healthcare facilities at nearly the same time were brought to the attention of the infection prevention and control (IPC) team. The first bat was captured in a patient room and was submitted for testing. Postexposure prophylaxis (PEP) was initiated for 1 patient before the bat testing results came back negative. The second bat was found in a transplant unit hallway and was released before we could request testing. We observed significant variations in responses, including decision to administer PEP and submission of bats for rabies testing. The IPC team developed a protocol to minimize unnecessary PEP, to prevent nosocomial rabies infection from bat exposure, and to limit associated panic. Methods: A systematic literature review of multiple databases was performed. A search of nonscientific articles using Google was also performed to assess unpublished inpatient bat encounters. A workgroup was established including IPC staff, physicians, and facilities management. The county animal services department and the state public health department veterinarian were consulted to aid in development of a protocol. Results: Literature review yielded a single report of a bat discovered in a neonatal intensive care unit (NICU). A lack of protocol resulted in PEP administration to 7 neonates without observed exposure after the bat was released instead of being submitted for testing. Of the first 100 articles retrieved via Google search of “bat in hospital,” 9 pertained to nosocomial discovery of bats in 5 different states over the past 7 years. Encounters included infestations requiring unit shutdowns and PEP administration. One tertiary-care referral center reported 10 encounters per year but did not elaborate on associated procedures. The county animal services staff assisted in training maintenance and engineering services (MES) personnel on how to secure bats for testing and helped develop a “bat kit” with protective gear and equipment to do so safely. In the new protocol, an inpatient bat encounter prompts personnel to capture the bat and begin an investigation into known or potential occult exposure. Known or potential exposures merit submission of the bat for rabies testing, the results of which guide PEP recommendations. All encounters are investigated for point of entry or roost. Conclusions: Inpatient bat encounters are not uncommon. Encounters should prompt systematic assessment for exposures and an investigation of the root cause. Following a protocol may limit unnecessary PEP administration, prevent nosocomial transmission of rabies from bat to patient, and attenuate associated anxiety.
Funding: None
Disclosures: None
1 - Neuroimaging in Personality Disorders
- from Part I - Etiology
- Edited by Carl W. Lejuez, University of Kansas, Kim L. Gratz, University of Toledo, Ohio
-
- Book:
- The Cambridge Handbook of Personality Disorders
- Published online:
- 24 February 2020
- Print publication:
- 07 May 2020, pp 3-19
-
- Chapter
- Export citation
-
Summary
This chapter focuses on advancements in the understanding of personality pathology gained from structural and functional neuroimaging studies. It draws from the literature on the most widely researched personality disorders including schizotypal, borderline, and antisocial personality disorder. Prominent findings in schizotypal personality disorder include abnormalities in temporal and frontal lobe volumes, decreased structural connectivity of temporal lobe regions, and inefficient recruitment of brain areas during task performance. In borderline personality disorder, neuroimaging findings are characterized by aberrant volume and activity of limbic and prefrontal brain areas that suggest diminished top-down control of affective responsivity. Studies in antisocial personality disorder reveal reduced volume in prefrontal and temporal lobe structures, white matter structure compromise, and altered brain network functional connectivity. Significant challenges in studying this complex population and limitations of current methodology are discussed. Suggestions for future directions of research in this field are provided.
1c - Illustrating the Value of Neuroimaging Studies Using the Example of Affect Regulation: Author Rejoinder to Commentaries on Neuroimaging in Personality Disorders
- from Part I - Etiology
- Edited by Carl W. Lejuez, University of Kansas, Kim L. Gratz, University of Toledo, Ohio
-
- Book:
- The Cambridge Handbook of Personality Disorders
- Published online:
- 24 February 2020
- Print publication:
- 07 May 2020, pp 27-28
-
- Chapter
- Export citation
-
Summary
This rejoinder uses the neuroimaging literature on affect regulation to exemplify how integration of complementary methods suggested by the commentaries could advance neurobiological understanding of personality disorders. It illustrates progressive insights gained from incorporating multiple sources of evidence including neuroimaging, genetics, and behavioral data associated with affect regulation. It also demonstrates the use of brain pattern activation analysis in addition to studying individual regions of interest to better understand the complex relationships between biological genotype, brain activity, and behavioral phenotype. The ways in which neuroimaging can serve as an endophenotype to bridge the gap between genes and distant phenotypes are highlighted.
Patterns of care and dropout rates from outpatient mental healthcare in low-, middle- and high-income countries from the World Health Organization's World Mental Health Survey Initiative
- Daniel Fernández, Daniel Vigo, Nancy A. Sampson, Irving Hwang, Sergio Aguilar-Gaxiola, Ali O. Al-Hamzawi, Jordi Alonso, Laura Helena Andrade, Evelyn J. Bromet, Giovanni de Girolamo, Peter de Jonge, Silvia Florescu, Oye Gureje, Hristo Hinkov, Chiyi Hu, Elie G. Karam, Georges Karam, Norito Kawakami, Andrzej Kiejna, Viviane Kovess-Masfety, Maria E. Medina-Mora, Fernando Navarro-Mateu, Akin Ojagbemi, Siobhan O'Neill, Marina Piazza, Jose Posada-Villa, Charlene Rapsey, David R. Williams, Miguel Xavier, Yuval Ziv, Ronald C. Kessler, Josep M. Haro
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 12 / September 2021
- Published online by Cambridge University Press:
- 28 April 2020, pp. 2104-2116
-
- Article
- Export citation
-
Background
There is a substantial proportion of patients who drop out of treatment before they receive minimally adequate care. They tend to have worse health outcomes than those who complete treatment. Our main goal is to describe the frequency and determinants of dropout from treatment for mental disorders in low-, middle-, and high-income countries.
MethodsRespondents from 13 low- or middle-income countries (N = 60 224) and 15 in high-income countries (N = 77 303) were screened for mental and substance use disorders. Cross-tabulations were used to examine the distribution of treatment and dropout rates for those who screened positive. The timing of dropout was examined using Kaplan–Meier curves. Predictors of dropout were examined with survival analysis using a logistic link function.
ResultsDropout rates are high, both in high-income (30%) and low/middle-income (45%) countries. Dropout mostly occurs during the first two visits. It is higher in general medical rather than in specialist settings (nearly 60% v. 20% in lower income settings). It is also higher for mild and moderate than for severe presentations. The lack of financial protection for mental health services is associated with overall increased dropout from care.
ConclusionsExtending financial protection and coverage for mental disorders may reduce dropout. Efficiency can be improved by managing the milder clinical presentations at the entry point to the mental health system, providing adequate training, support and specialist supervision for non-specialists, and streamlining referral to psychiatrists for more severe cases.
A low-fidelity, high-functionality, inexpensive ultrasound-guided nerve block model
- Daniel Micheller, Matthew J. Chapman, Michael Cover, Jonathan D. Porath, Nik Theyyunni, Ross Kessler, Robert Huang
-
- Journal:
- Canadian Journal of Emergency Medicine / Volume 19 / Issue 1 / January 2017
- Published online by Cambridge University Press:
- 01 August 2016, pp. 58-60
- Print publication:
- January 2017
-
- Article
-
- You have access Access
- HTML
- Export citation
Divorcing the puzzles: When group identities foster in-group cooperation
- Daniel Seewald, Stefanie Hechler, Thomas Kessler
-
- Journal:
- Behavioral and Brain Sciences / Volume 39 / 2016
- Published online by Cambridge University Press:
- 07 March 2016, e23
-
- Article
- Export citation
-
We argue that general social psychological mechanisms (e.g., common group identity) can account for prosocial behavior and cooperative norms without the need for punishing Big Gods. Moreover, prosocial religions often do not prevent conflict within their religious groups. Hence, we doubt whether Big Gods and prosocial religions are more effective than alternative identities in enhancing high-level cooperation.
The US National Comorbidity Survey: overview and future directions
- Ronald C. Kessler, James C. Anthony, Daniel G. Blazer, Evelyn Bromet, William W. Eaton, Kenneth Kendler, Marvin Swartz, Hans-Ulrich Wittchen, Shanyang Zhao
-
- Journal:
- Epidemiologia e Psichiatria Sociale / Volume 6 / Issue 1 / April 1997
- Published online by Cambridge University Press:
- 11 October 2011, pp. 4-16
-
- Article
-
- You have access Access
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
Who Supports Health Reform?
- David W. Brady, Daniel P. Kessler
-
- Journal:
- PS: Political Science & Politics / Volume 43 / Issue 1 / January 2010
- Published online by Cambridge University Press:
- 15 January 2010, pp. 1-6
- Print publication:
- January 2010
-
- Article
- Export citation
-
In this article, we report results from a new study that surveyed a large, national sample of American adults about their willingness to pay for health reform. As in previous work, we find that self-identified Republicans, older Americans, and high-income Americans are less supportive of reform. However, these basic findings mask three important features of public opinion. First, income has a substantial effect on support for reform, even holding political affiliation constant. Indeed, income is the most important determinant of support for reform. Second, the negative effects of income on support for reform begin early in the income distribution, at annual family income levels of $25,000 to $50,000. Third, although older Americans have a less favorable view of reform than the young, much of their opposition is due to dislike of large policy changes than to reform per se.
Contributors
-
- By Kateri Berasi, Carol A. Boyer, Diane R. Brown, Robyn Lewis Brown, Tony N. Brown, Padraic J. Burns, Cleopatra Howard Caldwell, Daniel L. Carlson, Cheryl Corcoran, Manuela Costa, Stephen Crystal, Gary S. Cuddeback, William W. Eaton, Adrianne Frech, Virginia Aldigé Hiday, Stevan E. Hobfoll, Allan V. Horwitz, Robert J. Johnson, Verna M. Keith, Ronald C. Kessler, Corey L. M. Keyes, Jacinta P. Leavell, Harriet P. Lefley, Mary Clare Lennon, Laura Limonic, Bruce G. Link, Athena McLean, David Mechanic, Elizabeth G. Menaghan, Barret Michalec, John Mirowsky, Shirin Montazer, Joseph P. Morrissey, Carles Muntaner, Bernice A. Pescosolido, Christopher Peterson, Jo C. Phelan, Michael Polgar, Sarah Rosenfield, Catherine E. Ross, Ebony Sandusky, Jaime C. Sapag, Teresa L. Scheid, Mark F. Schmitz, Sharon Schwartz, Dena Smith, David T. Takeuchi, Peggy A. Thoits, R. Jay Turner, Edwina S. Uehara, Jerome C. Wakefield, James Walkup, Emily Walton, Blair Wheaton, David R. Williams, Kristi Williams
- Edited by Teresa L. Scheid, University of North Carolina, Charlotte, Tony N. Brown, Vanderbilt University, Tennessee
-
- Book:
- A Handbook for the Study of Mental Health
- Published online:
- 05 June 2012
- Print publication:
- 16 November 2009, pp xi-xiv
-
- Chapter
- Export citation
Surface Coatings Based on Polysilsesquioxanes: Grafting-from Approach Starting from Organic Polymers
- Daniel Kessler, Patrick Theato
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 1190 / 2009
- Published online by Cambridge University Press:
- 31 January 2011, 1190-NN10-02
- Print publication:
- 2009
-
- Article
- Export citation
-
Poly(methylsilsesquioxane) (PMSSQ) based hybrid materials are promising candidates to produce substrate-independent stable and adherent surface coatings. Usually these materials are synthesized by controlled radical polymerization from inorganic precursors. The presented synthetic pathway in here demonstrates how to graft PMSSQ networks from an endgroup-functionalized organic polymer and thus enlarges the range of accessible inorganic/organic hybrid coating materials.
5 - The Effects of the U.S. Malpractice System on the Cost and Quality of Care
-
- By David J. Becker, assistant professor, University of Alabama Birmingham's Department of Health Care Organization and Policy., Daniel P. Kessler, professor, Stanford University Graduate School of Business
- Edited by William M. Sage, Columbia University, New York, Rogan Kersh, Syracuse University, New York
-
- Book:
- Medical Malpractice and the U.S. Health Care System
- Published online:
- 10 December 2009
- Print publication:
- 12 June 2006, pp 84-92
-
- Chapter
- Export citation
-
Summary
In theory, the medical malpractice liability system operates according to the “negligence rule”: Doctors are responsible for the costs of injuries that they negligently cause. The negligence rule should lead doctors' private decisions about whether and how to practice medicine to reflect society's overall interests, by leading them to balance the benefits of medical care, the costs of precaution, and the costs of negligence.
Imperfections in markets for health care and the liability system, however, mean that the negligence rule may not provide incentives for appropriate medical care in practice. It may lead doctors to take insufficient precautions against medical injuries or may lead to “defensive medicine” – medical practice based on fear of legal liability rather than on patients' best interests.
This indeterminacy has led to an extensive empirical debate over tort policy. What are the effects of the medical liability system on the cost and quality of care? What reforms to the system have the potential to reduce cost and improve quality?
This chapter reviews existing research on these questions. The first section outlines why understanding the effects of the liability system on the cost and quality of care is an important empirical issue. The second section summarizes the empirical evidence about the effects of the system and the effects of conventional “tort reforms” – changes to state law that seek to reduce liability. In brief, the empirical evidence supports the hypothesis that the existing system encourages defensive medicine, and that tort reforms reduce its prevalence.
A posteriori error control for the Allen–Cahn problem: circumventing Gronwall's inequality
- Daniel Kessler, Ricardo H. Nochetto, Alfred Schmidt
-
- Journal:
- ESAIM: Mathematical Modelling and Numerical Analysis / Volume 38 / Issue 1 / January 2004
- Published online by Cambridge University Press:
- 15 February 2004, pp. 129-142
- Print publication:
- January 2004
-
- Article
- Export citation
-
Phase-field models, the simplest of which is Allen–Cahn's problem, are characterized by a small parameter ε that dictates the interface thickness. These models naturally call for mesh adaptation techniques, which rely on a posteriori error control. However, their error analysis usually deals with the underlying non-monotone nonlinearity via a Gronwall argument which leads to an exponential dependence on ε-2. Using an energy argument combined with a topological continuation argument and a spectral estimate, we establish an a posteriori error control result with only a low order polynomial dependence in ε-1. Our result is applicable to any conforming discretization technique that allows for a posteriori residual estimation. Residual estimators for an adaptive finite element scheme are derived to illustrate the theory.






