89 results
Liquor for breakfast, fighting against alcohol consumption
- N. Navarro Barriga, P. Marqués Cabezas, M. B. Arribas Simón, B. Rodríguez Rodríguez, C. Alario Ruiz, G. Guerra Valera, A. Aparicio Parras, M. J. Mateos Sexmero, M. Fernández Lozano, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, M. P. Pando Fernández, M. D. L. A. Guillén Soto, T. Jimenez Aparicio, M. D. C. Vallecillo Adame, C. De Andrés Lobo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S408-S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful consumption of alcohol is known for how tortuous its management can be in mental health, encouraging introspection of it as a serious problem is perhaps the main key to starting to battle against its damaging influence on the development of a functional and full life.
ObjectivesTo describe a clinical case showing an unpredictible complication in an alcohol detoxification process.
Methods54-year-old man, native of Cádiz, widowed for half a decade, without children. He resides with his parents in the family home. Currently unemployed for approximately a year. He has previously worked in the IT sector. As a notable somatic history, we found long-established arterial hypertension and a total hip replacement. He has been under irregular follow-up with a mental health team for anxiety-depressive symptoms in the context of grief. He goes to the emergency service brought by his family to begin the detoxification process in the hospital setting. He acknowledges ethanol consumption since he was widowed, which began when he awakes; quantities that ranged between one or up to three bottles of distilled liquor per day, generally consumption is in the home environment. A little less than a year ago, he began to isolate himself in his room and abandon his self-care, eating increasingly insufficient food intake, refusing to receive professional care to quit the habit, mainly because he did not recognize it as disruptive.
The patient was admitted to hospital with symptoms suggestive of withdrawal, making it extremely difficult to control blood pressure levels. On the third day of admission to the acute care unit, fever peaks, blood pressure levels well below normal parameters, and compromised level of consciousness began to be evident.
ResultsBlood tests were performed that, together with the clinical picture, suggested imminent septic shock, so critical care was contacted for transfer and stabilization. A germ of probable urinary etiology sensitive to a broad spectrum of antibiotics was isolated in blood cultures, and the medication of the detoxification process was progressively optimized. Once clinical stability was achieved at all levels, an inpatient cessation resource was managed, which the patient accepted and considered suitable for his complete recovery.
ConclusionsA holistic approach to the alcoholic patient is important, since serious problems of an organic nature often arise. This is why a multidisciplinary intervention is necessary, as well as a holistic approach to care, involving both classic pharmacology and assiduous long-term psychotherapeutic intervention.
Disclosure of InterestNone Declared
From schizotypy to psychosis: is it a natural continuum?
- M. A. Andreo Vidal, M. B. Arribas Simón, M. Calvo Valcárcel, M. P. Pando Fernández, P. Martínez Gimeno, M. D. L. Á. Guillén Soto, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, C. De Andrés Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, Ó. Martín Santiago, A. Monllor Lazarraga, M. Ríos Vaquero, L. Rojas Vázquez, L. Sobrino Conde, A. Apario Parra, G. Lorenzo Chapatte
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S658-S659
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal personality is a condition suffered by 4% of the population. It is defined by presenting interpersonal, behavioral and perceptual features similar to the clinical features of psychotic disorders, such as schizophrenia, in less intensity and dysfunctionality, but at risk of reaching psychosis.
ObjectivesPresentation of a clinical case about a patient with premorbid schizotypal personality traits presenting with an acute psychotic episode.
MethodsLiterature review on association between schizotypal personality and psychosis.
ResultsA 57-year-old woman with a history of adaptive disorder due to work problems 13 years ago, currently without psychopharmacological treatment, goes to the emergency room brought by the emergency services due to behavioral alteration. She reports that “her husband and son wanted to sexually abuse her”, so she had to run away from home and has been running through the streets of the town without clothes and barefoot.
Her husband relates attitude alterations and extravagant behaviors of years of evolution, such as going on diets of eating only bread for 40 days or talking about exoteric and religious subjects, as believing that the devil got inside her husband through a dental implant. He reports that these behaviors have been accentuated during the last month. She has also created a tarot website, and has even had discussions with several users. She is increasingly suspicious of him, has stopped talking to him and stays in his room all day long, with unmotivated laughter and soliloquies.
It was decided to admit him to Psychiatry and risperidone 4 mg was started. At the beginning, she was suspicious and reticent in the interview. As the days went by, communication improved, she showed a relaxed gesture and distanced herself from the delirious ideation, criticizing the episode.
ConclusionsIn recent years, there has been increasing interest in understanding the association between schizotypy and serious mental disorder. Several theories understand schizotypy as a natural continuum of personality that reveals genetic vulnerability and that can lead to psychotic disorder when added to precipitating factors. Other theories define schizotypy as a “latent schizophrenia” where symptoms are contained and expressed in less intensity.
Around 20% evolves to paranoid schizophrenia or other serious mental disorders. It is complex to distinguish between those individuals in whom schizotypy is a prodrome and those in whom it is a stable personality trait. To date, studies applying early psychotherapeutic or pharmacological interventions have had insufficient and contradictory results, and the follow-up and treatment of these individuals could be a stress factor and a stigma. Some studies are looking for reliable markers of evolution to schizophrenia in order to establish adequate protocols for detention, follow-up and treatment.
Disclosure of InterestNone Declared
“God speaks to me through a dove”. The evidence of clozapine in treatment-refractory psychosis
- B. Rodríguez Rodríguez, P. Marqués Cabezas, M. Queipo de Llano de La Viuda, N. Navarro Barriga, G. Guerra Valera, M. B. Arribas Simón, C. Alario Ruiz, M. J. Mateos Sexmero, M. Fernández Lozano, P. Marínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal, M. P. Pando Fernández, A. Monllor Lazarraga, M. Ríos Vaquero, G. Lorenzo Chapate, L. Rojas Vázquez, C. De Andrés Lobo, T. Jiménez Aparicio, M. D. C. Vallecillo Adame
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is an atypical antipsychotic synthesised in 1958. It was withdrawn from the market in the 1970s due to the appearance of agranulocytosis, but was reintroduced due to strong evidence of its efficacy and superiority over other antipsychotics in treatment-resistant schizophrenia.
ObjectivesTo describe the adequate response to clozapine in treatment-refractory psychosis.
MethodsReview of the scientific literature based on a relevant clinical case.
ResultsA 16-year-old woman was admitted to a psychiatric inpatient unit for psychotic symptoms and behavioural disorders. She lives with her father and older sister; she has not been in contact with her mother, who lives in another country, for several years. She attends secondary school, with poor academic performance. Maternal diagnosis of schizophrenia. She started using cannabis two years ago, with a progressive increase up to 20 grams per week. He reports the onset of a feeling of strangeness a year ago, with progressive isolation in his room, referring to delirious ideation of harm towards classmates and people from his town, self-referentiality and delirious interpretations of religious mystical content (“God speaks to me through a dove”). He comments on the phenomenon of theft and thought-reading. Soliloquies and unmotivated laughter are observed.
ConclusionsTreatment was started with risperidone, progressively increasing the dose up to optimisation, without achieving a decrease in positive symptoms, but with the appearance of excessive sedation and sialorrhoea. It was combined with aripiprazole up to 20mg, maintained for a couple of weeks, without significant clinical improvement. Given the failure of two lines of therapy, it was decided to change to clozapine up to a dose of 75mg, with adequate tolerance and response, achieving a distancing of the delirious ideation. Regular haematological controls were performed, with no alterations in haemogram or troponins.
Disclosure of InterestNone Declared
Psychiatry resident physician duty hours, resting times and European Working Time Directive compliance in Spain
- J. P. Carrasco Picazo, D. A. Sánchez Martínez, P. Estrella Porter, R. Ruiz-Montero, A. H. Aginagalde Llorente, E. García-Camacho, J. Navarro, A. Cerame del Campo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S393-S394
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a growing interest in understanding the impact of duty hours and resting times on training outcomes and the well-being of resident physicians. Psychiatry resident’s duty hours in Spain comprise a regular working schedule of 37.5h per week and a minimum of 4 mandatory on-call shifts. The most recent duty hours regulations in Spain were transposed from the European Working Time Directive (EWTD). According to Spanish Law, doctors cannot work for more than 48h per week and need to have resting times per day (at least 12h), per week (at least 36h) as well as annual leave (at least a month). However, there is practically no data on this situation in psychiatry resident physicians.
ObjectivesOur aim is firstly, to describe the number of shifts performed by psychiatry resident physicians in Spain. Secondly, to describe compliance with the daily and weekly rests compared to those set in national and European law. Finally, to analyse the difference by demographic variables (gender and year of residency), in both the number of on-call duty shifts and compliance with rests.
MethodsA descriptive cross-sectional study was designed through an online survey adapted from the existing literature. The target population were Spanish psychiatry resident physicians undergoing PGT who started their specialist training during the years 2018–2021. The survey was disseminated through the Spanish regional medical councils to all active psychiatry resident physicians by mail as well as through informal communication channels. The study was authorised by the Spanish Medical Organization’s General Assembly which is the highest ethical and deontological body of physicians in Spain.
Results55 responses were obtained, of which 61.82% identified as females. The mean number of on-call shifts in the last 3 months was 14.05. This mean was highest in women 14,32 and in the cohort of 2020 15.46 (first year of residency). Among the resident physicians surveyed, 66.07% exceeded the 48h per week limit set by the EWTD and 7% of them did not rest after a 24-h on-call shift. Furthermore, 22% of respondents did not have a day-off after a Saturday on-call shift. The mean working hours when not resting after an on-call-shift were 7 hours. The comparison by gender and year of residency of the main variables can be seen in figures 1 and 2 respectively.
Image:
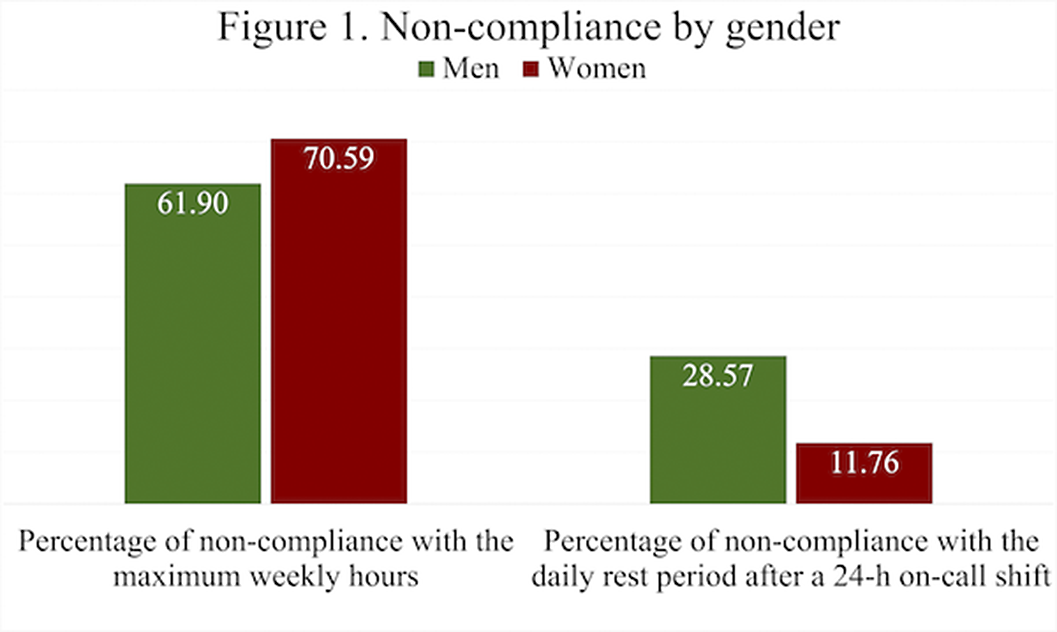
Image 2:
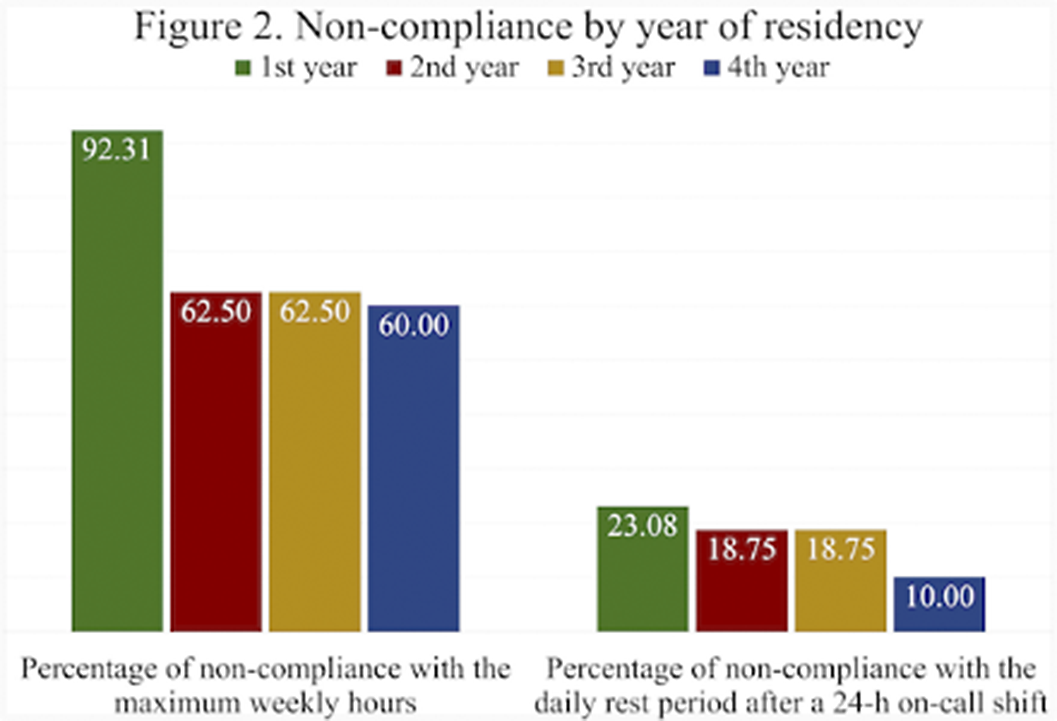 Conclusions
ConclusionsPsychiatry resident physicians in Spain greatly exceed the established 48 h/week EWTD limit. Likewise, non-compliance with labour regulations regarding mandatory rest after on-call duty and minimum weekly rest periods are observed. Differences can be seen by gender and year of residency. The situation described could potentially create a high-risk situation for the health and psychosocial well-being of resident physicians, hinder learning outcomes and could lead to suboptimal patient care.
Disclosure of InterestNone Declared
Lithium withdrawal and relapse in bipolar disorder when kidney function deteriorates
- C. De Andrés-Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, A. Rodríguez Campos, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano, M. Calvo Valcárcel, M. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, L. Rojas Vázquez, G. Lorenzo Chapatte, M. Ríos Vaquero, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S427-S428
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium was the first mood stabilizer and today continues to be a first-line treatment in the treatment of bipolar disorder despite its adverse effects, which make it important to monitor blood levels and control kidney function.
ObjectivesPresentation of a case of litium withdrawal and relapse in bipolar disorder. Literature review relating to the risk of relapse when lithium treatment is interrupted.
MethodsWe present a clinical case of a patient who suffers a deterioration in renal function that requires the withdrawal of lithium and who consequently suffers a relapse. We conducted a bibliographic research of articles in Pubmed on this topic.
ResultsA 49-year-old male, with a history of multiple admissions to UHB since the age of 18 with a diagnosis of bipolar disorder and treatment with lithium. Decompensations towards the manic pole have always been related to interruptions in lithium treatment. On several occasions when the patient was feeling well emotionally, he believed himself to be “cured” and abandoned the treatment, triggering a manic episode, showing verbal aggression, increased self-esteem and delusional ideation of harm. Remission was usually achieved with the reintroduction of lithium and the addition of high-dose quetiapine. Between episodes, constant overvalued ideas of economic scarcity seemed to persist, which were accentuated in the form of delusional ideas of ruin in depressive decompensations. After 7 years of stability, control analysis showed blood litemia of 2.2 mEq/L with deterioration of kidney function and generalized tremor was observed, without improvement after serum therapy. He was admitted for dialysis and lithium was suspended. Treatment with valproate was started and a consultation scheduled in a week to adjust the dose. The patient did not attend that consultation and was admitted three days later to Psychiatry Hospitalization showing a challenging attitude, evident dysphoric mood, accelerated speech, with derailments and echolalia. Delusional ideation of harm with auditory hallucinations. Insomnia and hyporexia. Chronic renal failure persisted.
ConclusionsLithium is a very effective drug but with a narrow therapeutic range that requires adequate monitoring due to the possible consequences of its use at different organs and systems of the body. when lithium is found in the blood at toxic levels with deterioration of kidney function and glomerular filtration fails to recover, lithium treatment should be suspended. Sudden withdrawal of lithium significantly increases the risk of relapse due to rebound effect. More than 50% of patients experience a recurrence within 10 weeks of withdrawal.
Disclosure of InterestNone Declared
Delusional parasitosis: the importance of a multidisciplinary approach
- M. Calvo Valcárcel, G. Guerra Valera, M. A. Andreo Vidal, O. Martín Santiago, M. Lorenzo Hernando, M. P. Pando Fernández, P. Martinez Gimeno, M. D. L. Á. Guillén Soto, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, C. De Andrés Lobo, M. D. C. Vallecillo Adame, T. Jimenez Aparicio, A. Monllor Lazarraga, M. Ríos Vaquero, L. Rojas Vázquez, L. Sobrino Conde, A. Aparicio Parra, G. Lorenzo Chapatte
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S750
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Delusional parasitosis, also known as delusional infestation or Ekbom’s syndrome, is a rare psychotic disorder characterized by the false belief that a parasitic skin infestation exists, despite the absence of any medical evidence to support this claim. These patients often see many physicians, so a multidisciplinary approach among clinicians is important. Many patients refuse any treatment due to their firm belief that they suffer from an infestation, not a psychiatric condition, so it is crucial to gain the trust of these patients.
ObjectivesThe comprehensive review of this clinical case aims to investigate Ekbom syndrome, from a historical, clinical and therapeutic perspective.
MethodsLiterature review based on delusional parasitosis.
ResultsA 65-year-old woman comes to the psychiatry consultation referred by her primary care physician concerned about being infested by insects that she perceives through scales on her skin for the last three months. She recognizes important impact on her functionality. She is also convinced that her family is being infected too. As psychiatric history she recognizes alcohol abuse in the past (no current consumption) and an episode of persecutory characteristics with a neighbor, more than ten years ago. On psychopathological examination, she shows delusional ideation of parasitosis, with high behavioral repercussions, cenesthetic and cotariform hallucinations, as well as feelings of helplessness and anger. Treatment with Pimozide was started and the patient was referred to dermatology for evaluation, a plan she accepted. Her primary care physician and dermatology specialist were informed about the case and the treatment plan. In the recent reviews, the patient is calmer, however, despite the corroboration of dermatology and in the absence of organic lesions in cranial CT, she is still unsatisfied with the results, remaining firm in her conviction of infestation. It was decided to start treatment with atypical neuroleptics (Aripiprazole), with progressive recovery of her previous functionality.
ConclusionsDespite the increase in the number of studies in recent years, there are still few studies on this type of delirium. The female:male ratio varies in the bibiliography (between 2:1 and 3:1). The onset is usually insidious, generally appearing as a patient who comes to his primary care physician convinced of having parasites in different skin locations. It is usual to observe scratching lesions or even wounds in search of the parasite. In the past, the most used and studied treatment was Pimozide. Currently the treatment of choice is atypical neuroleptics due to their lower side effects. The latest reviews on the prognosis of this disorder show data with percentages of complete recovery between 51% and 70%, and partial responses between 16.5% and 20%. Finally, for a good diagnosis and therapeutic management, it is important to achieve a multidisciplinary approach.
Disclosure of InterestNone Declared
From adjustment disorder to schizotypal personality disorder
- C. De Andrés-Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, A. Rodríguez Campos, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano, M. Calvo Valcárcel, M. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, L. Rojas Vázquez, G. Lorenzo Chapatte, M. Ríos Vaquero, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S652-S653
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Individuals with schizotypal personality disorder are characterized by tendencies to magical thinking, unusual perceptions, discomfort in social situations, and restricted affect. It is frecuent that they have social anxiety and have difficulty in understanding the motivations and thoughts of others.
ObjectivesPresentation of a case of a patient who was first diagnosed with adjustment disorder, but on a closer study, was discovered to have a schizotypal personality disorder.
MethodsWe conducted a bibliographic review by searching for articles about schizotypal personality disorder and theory of mind in Pubmed.
ResultsWe present the case of a 39-year-old woman, diagnosed with adjustment disorder after a conflict at work with a colleague that caused her anxiety-depressive symptoms. In consultations, the patient shows verbiage without expansiveness or euphoria, with rambling speech. She expresses feelings of indignation and injustice, she is irritable, with contained anger. She refers that she prefers to be distrustful of others because she does not understand their intentions. Her thoughts are very rigid, which leads her to have avoidant and phobic attitudes, having no relationships of friendship throughout her life.
A neuropsychological evaluation is carried out, resulting in a surprising WAIS with a TIC of 128. However, the Mayer‐Salovey‐Caruso Emotional Intelligence Test (MSCEIT) shows difficulties in Perception, Comprehension and Emotional Management
Considering the patient’s symptomatology as a whole, it is noteworthy:
– Sustained social isolation throughout their life history
– Superficiality of interpersonal relationships
– Distrust and slight self-referentiality. Deficit in inferring the feelings and thoughts of others
– Peculiar speech with ideas of magical content, superstitions and rituals…
Which together supported a diagnosis of schizotypal personality disorder and generalized anxiety disorder. From this point we started to work on her self-esteem, modification of irrational beliefs and cognitive distortions, interpersonal communication and metacognitive therapy, with good results.
ConclusionsThe type of schizotypal patients who come to consultations most frequently are the actively isolated/timorous profile due to their intense social anxiety and difficulties in understanding and adapting to the social world around them. Initial therapy should be empathic support. The theory of mind is the ability to infer the other’s mental states and therefore predict their behavior, this ability being diminished in the schizotypal patient. Mentalization tasks, metacognitive therapy, cognitive flexibility training, social skills training, and promoting self-worth are useful. On some occasions it may be necessary to start psychopharmacological treatment to control anxiety and unusual perceptions when they cause discomfort.
Disclosure of InterestNone Declared
Mental health impact of fentanyl abuse, a case report
- G. Lorenzo - Chapatte, G. Guerra Valera, P. Marqués Cabezas, L. R. Vázquez, M. Ríos Vaquero, A. Monllor Lazarraga, M. P. Pando Fernández, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, B. Rodríguez Rodríguez, N. Navarro Barriga, M. J. Mateos Sexmero, M. Fernández Lozano, T. Jiménez Aparicio, C. De Andrés-Lobo, M. D. C. Vallecillo Adame, M. D. L. Á. Guillén Soto, L. Sobrino Conde, A. Aparicio Parras
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years, there has been an increase in the prevalence of illicit use of fentanyl and other opioids in the United States population. This has led to an increase in medical, psychopathological and abuse-associated comorbidity, an increase in deaths and a decrease in the age of consumption, and has become a serious emerging problem in young people.
We present the case of an 18-year-old woman from the United States who recently settled in Spain and started a follow-up in Mental Health due to opioid and other substance abuse problems.
ObjectivesTo address the growing problem surrounding the illicit use of fentanyl and opioids as drugs of abuse based on the presentation of the clinical case mentioned above.
MethodsBibliographic search and description of a clinical case of a patient under follow-up by Mental Health at the “Hospital Clínico Universitario de Valladolid”.
ResultsAn 18-year-old woman from the United States who has been living with her father in Spain since the summer of 2023, having moved to Spain due to problems related to substance abuse.
With no previous medical or surgical history and with a history of follow-up in Mental Health in her country of origin for depressive symptomatology, dysfunctional personality traits and abuse of different toxic substances since adolescence.
After a brief and erratic follow-up in Psychiatry for anxious-depressive symptoms reactive to a complex and conflictive relationship with his mother and marked academic difficulties during the first years of adolescence, at the age of 15 he started using cannabis and alcohol, thus beginning a period marked by relationships with marginalized sectors of the population, substance abuse and school failure.
As his cannabis consumption intensified, he began to consume fentanyl prescribed to his mother, as well as other opioids to which he had access illegally, for which reason he had to be admitted twice to detoxification centers without results, which is why his family finally decided to move him to Spain.
ConclusionsIn recent years, fentanyl abuse has become a serious public health problem that is mainly centered in the young population.
High levels of impulsivity and lack of frustration tolerance predispose to the use of illicit substances for elusive purposes.
Substance abuse carries with it not only an important organic comorbidity, but also a marked socio-familial and economic repercussion.
Disclosure of InterestNone Declared
Psychopharmacological management in patients with Di George syndrome
- L. Rojas Vázquez, P. Marqués Cabezas, G. Lorenzo Chapatte, M. Ríos Vaquero, A. Monllor Lazarraga, M. P. Pando Fernández, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano, N. Navarro Barriga, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, L. Sobrino Conde, M. D. L. Á. Guillén Soto, A. Aparicio Parra
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S455
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It is widely described in the scientific literature that patients who suffer from some type of congenital syndrome such as Di George Syndrome are more likely to present some type of psychopathological alteration during their development that may require intervention and treatment by infant and juvenile mental health teams in coordination with neuropediatrics (1). On this occasion, we will present the clinical case of a patient who regularly attends psychiatry consultations for management of anxious symptoms with impulse control deficits associated with intellectual disability, diagnosed since childhood with tetralogy of Fallot and later with Di George syndrome. In this type of case, treatment is usually considered taking into account possible comorbidities at the organic level (since there may be cardiological involvement, which can be an added difficulty when taking into account the adverse effects of some psychotropic drugs) (2).
ObjectivesThis is followed by the presentation of the clinical case, which can serve to exemplify this type of case and clarify any doubts that may arise regarding treatment.
MethodsPresentation of the clinical case and review of updated scientific literature on the subject.
ResultsPatient who first came to the infantile-junior consultations at the age of 8 years due to delay in the acquisition of verbal language and impulsivity. The patient had a history of pediatric follow-up since birth for different physical symptoms that finally led to the diagnosis of Di George syndrome.
Given the difficulties he presented both at home and at school, different psychometric tests were performed and it was determined that it could be beneficial to initiate treatment with extended-release methylphenidate. Prior to treatment, psychomotor restlessness (without aggressiveness) and difficulty in concentration prevailed, which improved significantly after upward adjustment of the dose to a guideline corresponding to his age and weight. It was not necessary in this case to administer other treatments (the possibility of starting Aripiprazole in case of episodes of agitation was considered, but it was not necessary). The patient has continued to be monitored by cardiology to assess the possible side effects of the treatment (since it can increase heart rate and blood pressure (3), but so far no complications have been detected).
Thanks to psychotherapeutic and educational intervention, language acquisition was achieved, although to date he still requires support due to the difficulties he still presents.
ConclusionsIt is important to take into account the possible side effects of psychopharmacological treatment in patients with an associated congenital syndrome. Intensive and comprehensive follow-up by psychiatry and pediatrics (and later by their primary care physician) should be performed.
Disclosure of InterestNone Declared
Impulse phobias during pregnancy: a case report of a 37 year-old woman pregnant of her first child
- M. Ríos-Vaquero, G. Lorenzo-Chapatte, L. Rojas-Vázquez, A. Monllor-Lazarraga, L. Sobrino-Conde, M. J. Mateos-Sexmero, T. Jimenez-Aparicio, M. Calvo-Valcarcel, M. A. Andreo-Vidal, M. P. Pando-Fernández, P. Martínez-Gimeno, M. D. L. A. Guillen-Soto, B. Rodriguez-Rodriguez, N. Navarro-Barriga, M. Fernández-Lozano, A. Aparicio-Parras, M. D. C. Vallecillo-Adame, C. De Andres-Lobo, A. Rodríguez-Campos
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S801
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pregnancy and puerperium are two critical stages for women’s mental health due to the biological stress of pregnancy itself, as well as the emotional stress that surrounds this vital moment. (1) Debut and aggravation of psychiatric symptoms may occur, as well as relapse in women previously diagnosed with Severe Mental Disorder (SMD).
Symptoms of the anxious spectrum are the most frequent within the perinatal mental pathology, being impulse phobias an entity that appears in about 25% of women previously diagnosed with OCD and up to 10-15% of women without previous psychopathology (2)
ObjectivesExposing the importance of Perinatal Mental Health from the presentation of a clinical case.
MethodsReview of the literature available in PubMed. Presentation of the pathobiography and evolution of the patient.
ResultsOur case is about a 37-year-old woman, 30 weeks pregnant with her first child and history of having required admission to Psychiatry with subsequent follow-up in Mental Health for anxious-depressive symptoms with the presence of self-injurious ideas who, after two weeks with multiple life stressors, came to the Emergency Department for the presence of impulse phobias focused on pregnancy with significant internal anguish and ideas of death as a resolution to it, which is why it was decided to hospitalize her. During admission, and taking into account the patient’s gestational state, treatment was started with diluted Mirtazapine and Aripiprazole solution at minimal doses, which in this case were sufficient for symptom control.
The latest guidelines addressing psychopharmacology during pregnancy and lactation point to sertraline among the antidepressants and Lorazepam among the benzodiazepines as the safest drugs during pregnancy (3).
Conclusions- The exacerbation of anxious symptomatology and the presence of gestation-focused impulse phobias are frequent during pregnancy and their intensity increases as the time of delivery approaches.
- Sertraline, Lorazepam, Mirtazapine and Aripiprazole are safe drugs during pregnancy.
- In these women, a close and multidisciplinary follow-up by Psychiatry and Gynecology is advisable.
Disclosure of InterestNone Declared
Cuticular lipid profiles of selected species of cyclocephaline beetles (Melolonthidae, Cyclocephalini)
- Geanne Karla N. Santos, Daniela Maria do Amaral F. Navarro, Artur Campos D. Maia
-
- Journal:
- Bulletin of Entomological Research / Volume 114 / Issue 1 / February 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 124-133
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Neotropical cyclocephaline beetles, a diverse group of flower-loving insects, significantly impact natural and agricultural ecosystems. In particular, the genus Cyclocephala, with over 350 species, displays polymorphism and cryptic complexes. Lacking a comprehensive DNA barcoding framework, accessible tools for species differentiation are needed for research in taxonomy, ecology, and crop management. Moreover, cuticular hydrocarbons are believed to be involved in sexual recognition mechanisms in these beetles. In the present study we examined the cuticular chemical profiles of six species from the genus Cyclocephala and two populations of Erioscelis emarginata and assessed their efficiency in population, species, and sex differentiation. Overall we identified 74 compounds in cuticular extracts of the selected taxa. Linear alkanes and unsaturated hydrocarbons were prominent, with ten compounds between them explaining 85.6% of species dissimilarity. Although the cuticular chemical profiles efficiently differentiated all investigated taxa, only C. ohausiana showed significant cuticular profile differences between sexes. Our analysis also revealed two E. emarginata clades within a larger group of ‘Cyclocephala’ species, but they were not aligned with the two studied populations. Our research underscores the significance of cuticular lipid profiles in distinguishing selected cyclocephaline beetle species and contemplates their potential impact as contact pheromones on sexual segregation and speciation.
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
PEAKS AND VALLEYS: BIPOLAR DISORDER, RAPID CYCLERS AND ENERGY DRINKS CONSUMPTION
- M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martinez Gimeno, P. Pando Fernández, B. Rodriguez Rodriguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. D. C. Vallecillo Adame, T. Jimenez Aparicio, C. de Andres Lobo, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S702-S703
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar Disorder (BD) is considered a serious mental disorder characterized by a changing mood that fluctuates between two completely opposite poles. It causes pathological and recurrent mood swings, alternating periods of exaltation and grandiosity with periods of depression. We talk about rapid cyclers when four or more manic, hypomanic or depressive episodes have occurred within a twelve-month period. Mood swings can appear rapidly. Approximately half of the people with bipolar disorder may develop rapid cycling at some point.
ObjectivesPresentation of a clinical case about a patient with Bipolar Disorder with rapid cycling and poor response to treatment.
MethodsReview of the scientific literature based on a clinical case.
Results33-year-old male, single, living with his mother, under follow-up by mental health team since 2012. First debut of manic episode in 2010. The patient has filed multiple decompensations related to consumption of toxics (alcohol and cannabis). Currently unemployed. He attended to the emergency service in June 2022 accompanied by his mother, who reported that he was restless. The patient refers that he has interrupted the treatment during the vacations, having sleep rhythm disorder with abuse of caffeine drinks. Currently the patient does not recognize any consumption.The patient reports that during the village festivals he felt very energetic, occasionally consuming drinks rich in taurine and sugars, even having conflicts with people of the village. Finally, the patient was stabilized with Lithium 400 mg and Olanzapine. In September, the patient returned to the emergency service on the recommendation of his referral psychiatrist due to therapeutic failure. The only relevant finding we observed in the analytical determinations were low lithium levels (0.4 mEq/L). The transgression of sleep rhythms and the abuse of psychoactive substances required the admission of the patient to optimize the treatment (Clozapine, Lithium, Valproic Acid). At discharge, he is euthymic, has not presented behavioral alterations and is resting well. Finally, it was decided that the patient should go to the Convalescent Center to continue treatment and achieve psychopathological stability.
ConclusionsBipolar disorder is an important mental illness, having an incidence of 1.2%, being responsible for 20% of all mood disorders. Therefore, it is important to perform an adequate and individualized follow-up of each patient. Treatment with mood stabilizers tries to improve and prevent manic and depressive episodes, improving chronicity and trying to make the long-term evolution as good as possible, being important psychoeducation and psychotherapy.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
Identification of trema in first episode psychosis: a case report
- C. Alvarez Garcia, D. García Martínez, L. Nocete Navarro
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S789-S790
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The concept of trema refers to an initial phase in the psychotic process that is characterized by intense anguish, an experience of hostility and a feeling of imminent catastrophe. This situation engenders in the patient a sensation of being in a tunnel than can only lead to something terrible but ineffable.
ObjectivesTo illustrate the incipient phase of psychotic disorder though the presentation of a case.
MethodsA presentation of a clinical case.
ResultsA 29-year-old man attends the emergency department due to anxiety of one moth of evolution, that had debuted after a stressful event in the patient’s life such as loss of employment. He suffered from intense morning-predominance anguish, depersonalization episodes, insomnia, hallucinosis, cognitive blocks that occasioned him great anxiety and apragmatic behaviors. Besides, he had language alteration and autolytic ideation with previous autolytic gestures. After evaluation, he was diagnosed with psychotic episode. He was hospitalized, and treatment with olanzapine and lorazepam was started.
ConclusionsWith the exhibition of this case, we intended to point up the importance of a differential diagnosis with different disorders marked by anxiety as the main symptom. In our case, panic disorder should be taken in account as a differential diagnosis. Furthermore, as the evidence shows, the identification of prodromic phases in schizophrenia allows an early diagnosis and early intervention, improving the prognosis.
DisclosureNo significant relationships.
The unbearable limitations of solo science: Team science as a path for more rigorous and relevant research
- Alison Ledgerwood, Cynthia Pickett, Danielle Navarro, Jessica D. Remedios, Neil A. Lewis, Jr.
-
- Journal:
- Behavioral and Brain Sciences / Volume 45 / 2022
- Published online by Cambridge University Press:
- 13 May 2022, e81
-
- Article
- Export citation
-
Both early social psychologists and the modern, interdisciplinary scientific community have advocated for diverse team science. We echo this call and describe three common pitfalls of solo science illustrated by the target article. We discuss how a collaborative and inclusive approach to science can both help researchers avoid these pitfalls and pave the way for more rigorous and relevant research.




