91 results
“Helping us by helping you”: Pro bono consulting and graduate student training
- Manuel F. Gonzalez, Lauren Offermann, Nicole A. Alonso, Jennifer D. Bragger, Valerie I. Sessa, Mele Kramer
-
- Journal:
- Industrial and Organizational Psychology / Volume 16 / Issue 4 / December 2023
- Published online by Cambridge University Press:
- 22 November 2023, pp. 468-472
-
- Article
- Export citation
Traumatic stress symptoms among Spanish healthcare workers during the COVID-19 pandemic: a prospective study
- Ana Portillo-Van Diest, Gemma Vilagut, Itxaso Alayo, Montse Ferrer, Franco Amigo, Benedikt L. Amann, Andrés Aragón-Peña, Enric Aragonès, Ángel Asúnsolo Del Barco, Mireia Campos, Isabel Del Cura-González, Meritxell Espuga, Ana González-Pinto, Josep M. Haro, Amparo Larrauri, Nieves López-Fresneña, Alma Martínez de Salázar, Juan D. Molina, Rafael M. Ortí-Lucas, Mara Parellada, José M. Pelayo-Terán, Aurora Pérez-Zapata, José I. Pijoan, Nieves Plana, Teresa Puig, Cristina Rius, Carmen Rodríguez-Blázquez, Ferran Sanz, Consol Serra, Iratxe Urreta-Barallobre, Ronald C. Kessler, Ronny Bruffaerts, Eduard Vieta, Víctor Pérez-Solá, Jordi Alonso, Philippe Mortier, MINDCOVID Working Group
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 32 / 2023
- Published online by Cambridge University Press:
- 09 August 2023, e50
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aim
To investigate the occurrence of traumatic stress symptoms (TSS) among healthcare workers active during the COVID-19 pandemic and to obtain insight as to which pandemic-related stressful experiences are associated with onset and persistence of traumatic stress.
MethodsThis is a multicenter prospective cohort study. Spanish healthcare workers (N = 4,809) participated at an initial assessment (i.e., just after the first wave of the Spain COVID-19 pandemic) and at a 4-month follow-up assessment using web-based surveys. Logistic regression investigated associations of 19 pandemic-related stressful experiences across four domains (infection-related, work-related, health-related and financial) with TSS prevalence, incidence and persistence, including simulations of population attributable risk proportions (PARP).
ResultsThirty-day TSS prevalence at T1 was 22.1%. Four-month incidence and persistence were 11.6% and 54.2%, respectively. Auxiliary nurses had highest rates of TSS prevalence (35.1%) and incidence (16.1%). All 19 pandemic-related stressful experiences under study were associated with TSS prevalence or incidence, especially experiences from the domains of health-related (PARP range 88.4–95.6%) and work-related stressful experiences (PARP range 76.8–86.5%). Nine stressful experiences were also associated with TSS persistence, of which having patient(s) in care who died from COVID-19 had the strongest association. This association remained significant after adjusting for co-occurring depression and anxiety.
ConclusionsTSSs among Spanish healthcare workers active during the COVID-19 pandemic are common and associated with various pandemic-related stressful experiences. Future research should investigate if these stressful experiences represent truly traumatic experiences and carry risk for the development of post-traumatic stress disorder.
Cannabis use in different mental disorders: a descriptive study in a psychiatric hospital
- B. Samso, A. López Fariña, C. González Navarro, L. Morado San Segundo, A. Bilbao Idarraga, U. López Puentes, R. F. Lopez Brokate, T. Ruiz de Azua Aspizua, U. Ortega Pozas, C. Arán Cisneros, E. Garnica de Cos, I. Alonso Salas
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S334-S335
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the last decade, the prevalence of THC use is increasing among adolescents and adults. There is also strong evidence to suggest that cannabis use is associated with psychiatric comorbidities. The strongest evidence is found between cannabis use and psychotic disorder. However, the literature shows that those who have used cannabis in the past or for a large part of their lives are at higher risk of mood disorders, anxiety, personality disorder or other drug use than those who do not use cannabis in a harmful way.
ObjectivesTo provide an overview of the association between cannabis use and the different mental pathologies presented by the patients admitted during the study period. To describe the prevalence of THC use in the study according to the mental pathology presented by the patient.
MethodsA retrospective observational descriptive study was developed for 3 months, of all patients admitted to the acute unit of the psychiatric hospital. No exclusion criteria were included.
ResultsDuring the period of study 172 patients were admitted to the hospital, classified according to the main diagnosis we have: 49 patients suffer from schizophrenia, 26 bipolar affective disorder, 20 with depressive disorder, 20 with personality disorder, 19 with substance use disorder, 18 with other unspecified disorders and 20 patients with no known previous diagnosis. The prevalence of THC use in the study sample according to diagnosis, would be schizophrenia 16%, Bipolar affective disorder 19%, Depressive disorder 5%, Personality disorder 45%, Substance use disorder 21%, Unspecified disorders 11% and patients with no known previous diagnosis 10%.
ConclusionsThe results obtained in the study in terms of THC use are in agreement with those obtained in the literature. In our study, we observed that cannabis use is associated with psychotic disorders as well as with mood, personality and substance abuse disorders. Given that the frequency of use has increased and there is a strong association with different comorbid psychiatric diagnoses, guidance on modifications in medication strategies might be necessary.
Disclosure of InterestNone Declared
Adherence to psychiatric medications and diagnosis
- C. González Navarro, A. Bilbao Idarraga, I. Alonso Salas, L. Morado San segundo, A. López Fariña, U. López Puentes, B. Samsó Martínez, R. F. Lopez Brokate, T. Ruiz de Azua Aspizua, E. M. Garnica de Cos, U. Ortega Pozas
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S240-S241
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients with mental disorders frequently become non-adherent during their long term prescribed treatment. This situation frequently triggers clinical worsening and hospital admission. Therefore, non-adherence may result in poorer long term clinical outcomes and has economic implications for health-care providers (Carlos De las Cuevas et al. Neuropsychopharmacol Hung 2021; 23(4):347-362).
Objectives- To describe the adherence to oral and long acting injectable treatment in the sample of patients that were admitted to the short stay hospital unit during the period of study.
- To describe the adherence to treatment amongst psychiatric diagnosis in the sample of study.
MethodsIt was a retrospective observational study with a duration of three months. Data was collected from all patients admitted to the short stay hospital unit during the period of study and there were no specific exclusion criteria. Descriptive statistics were performed. To assess the adherence to pharmachological treatment the patient report, the family report and the pharmacy dispensation according to the existent informatic prescription platform was considered. Regarding the long acting injectable treatment the formulary of administration in the clinical history was checked.
ResultsDuring the period of study 172 patients were admitted to the short stay hospital unit. Of those, 146 patients had a previous pharmacologic prescription. Data of treatment was not possible to obtain in 7 patients. In the sample of study, 83.5% were on oral and 16.5% on long acting injectable treatment. The general adherence to treatment in the sample was 61.87%. In the oral treatment group the adherence was 58.4% and in the long acting injectable treatment group was 65.2%.
Amongst the different psychiatric diagnoses the outcomes of adherence to treatment were: 60.4% in schizophrenia and related psychosis, 62.5% in bipolar disorder, 78.6% in depression, 58.3% in personality disorders and 62% in addictive disorders.
ConclusionsIn our descriptive study adherence to treatment was higher in the long acting injectable treatment group, agreeing with the existent scientific literature.
The results of adherence for schizophrenia and bipolar disorder are similar to the ones found in scientific literature but differ from the ones for depression, being higher in our sample (Judit Lazary et al. Neuropsychopharmacol Hung 2021;23(4): 347-362). Moreover, in scientific literature it is found a similar prevalence of adherence across diagnosis (for schizophrenia, bipolar disorder and depression) whereas in our sample patients with depression showed a different and higher adherence to treatment (Judit Lazary et al. Neuropsychopharmacol Hung 2021;23(4): 347-362). In our sample, patients with personality disorders had the lowest adherence to treatment.
Disclosure of InterestNone Declared
Acute mutism in a young female. A case report of a 20-year-old female who presents a 3-month mutism
- A. Gonzalez-Mota, A. Gonzalez-Gil, C. Martin-Gomez, J. A. Benito-Sanchez, I. M. Peso-Navarro, L. Fernandez-Alonso
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 20-year-old female presents with a progressive 3-month mutism, hyporexia (20kg weight loss), abulia, anhedonia, apathy, social isolation,seeking company of her parents even at night, bradypsychia, sialorrhea, psychomotor slowdown and hypomimia. She is hospitalized in the Psychiatric Brief Hospitalization Unit (PBHU).Her parents relate the beginning of this symptomatology to a breakup and gender violence,which the patient confirms during the interview by eye/cephalic movements and single words jotted down.
ObjectivesThe objective of this study is to describe the evolution of the patient during her hospitalization in the PBHU of Salamanca and to look into the available bibliography about mutism related to stress and sialorrhea.
MethodsWe carried out a follow-up of the hospitalization of the patient and a structured search in PubMed with the keywords “mutism”,“sialorrhea” and “stress” in the last 10 years in English,Spanish and French.
ResultsFew or no articles where found.Therefore, the articles about mutism and stress were analyzed, which focused mostly in selective mutism. Regarding fear,the response to cope with the threat(fight, flight, freeze) is mediated by the autonomic system. The “Polyvagal Theory” speaks about the vagus nerve participating in emotion regulation (social communication and mobilization). Dissociation, in this context,has adaptive and defensive purposes and its threshold can be reduced by repeated stress situations.Long-term alteration of the autonomic nervous system has been described in selective mutism.This malfunction can be related to an elevated production of saliva due to the activation of the parasympathetic in the salivary glands, causing sialorrhea in our patient.
The patient began treatment with sertraline 100mg and risperidone 2mg with the aim of its antidepressive and major tranquilizer effects, she also began individual and family psychotherapy, we assured her sleep and intakes and she began to progressively recover her speech and mobility,identifying a possible trigger for the symptomatology: a physical beating of gender violence after her breakup.
ConclusionsDissociation and “freeze” response can be a maladaptative mechanism to fear.The malfunction of the autonomic nervous system can explain the disconnection,poor gaze,low facial and body expression and inability to speak.
Disclosure of InterestNone Declared
Alcohol consumption and cardiovascular risk: a descriptive study in a psychiatric short stay unit
- C. González Navarro, I. Alonso Salas, L. Morado San segundo, A. López Fariña, A. Bilbao Idarraga, U. López Puentes, B. Samsó Martínez, R. F. Lopez Brokate, T. Ruiz de Azua Aspizua, E. M. Garnica de Cos, U. Ortega Pozas
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S754
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients with mental disorders have a decreased life expectancy, being the main reason the cardiovascular disease. An important proportion of patients present a comorbid drug consumption. Amongst drugs, alcohol is the most frequent, and it is associated with a higher cardiovascular risk. The metabolic syndrome is one of the most employed tools to assess cardiovascular risk.
Objectives- To describe the demographic characteristics of the patients with an active alcohol consumption that were admitted to the hospital during the period of study.
- To describe the prevalence of metabolic syndrome in the sample, according to the Adult Treatment Panel III (ATP-III) criteria.
MethodsRetrospective observational study of three months duration. Data was collected from all patients admitted to the hospital during the period of study, with no specific exclusion criteria. Descriptive statistics were performed.
ResultsDuring the period of study 172 patients were admitted to the hospital (56.4% women and 43.6% men). A 44.8% presented alcohol consumption (25% sporadically, 6.4% weekly and 13.4% daily). Amongst women, 1% presented daily and 1% weekly consumption. Amongst men, 21.3% presented daily and 5.3% weekly consumption.
The prevalence of metabolic syndrome in the study sample was 29.11%. In the alcohol consumption group, the prevalence was 24.7% and differed according to the pattern of consumption: 43.5% in the daily consumption group, 27.3% in the weekly and 14% in the sporadically consumption group.
ConclusionsOn the one hand, in the sample of study a higher percentage of men present an active alcohol consumption, compared to women. It is remarkable the high percentage of daily alcohol consumption amongst men in our sample.
On the other hand, the prevalence of metabolic syndrome in our sample is similar to the one found in scientific literature regarding patients with mental disorders. It is noteworthy in our sample the increased prevalence of metabolic syndrome found in patients with a daily alcohol consumption, and a decreased prevalence in those with a sporadic pattern.
Disclosure of InterestNone Declared
What do we know about lithium associated hypercalcemia?
- N. Laherrán Cantera, R. Palacios - Garrán, A. Sanchez-Guerra Alonso, C. Gutiérrez Santaló, L. I. Muñoz-Manchado
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S577
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium associated with hypercalcemia may mimic a psychiatric condition and be confused for a relapse of bipolar disorder. The etiology seems to be due to a reduced sensitivity of the parathyroid cells to calcium, altering the parathyroid hormone (PTH) response. Lithium as an essential monovalent cation has some structural similarity to calcium (Ca) and can interact with protein receptors. This leads to changes in the inhibitory configuration of PTH and increased serum calcium concentrations, rising the threshold necessary to suppress hormone secretion.
Lithium-induced hyperparathyroidism (HIL) is the main cause of hypercalcemia in these patients.
ObjectivesBased on a clinical case of lithium-associated hypercalcemia in a patient with bipolar disorder, review the existing literature and state the needs for periodic monitoring protocols.
MethodsCase report and bibliographical review.
ResultsA 38-year-old woman, diagnosed with bipolar affective disorder at the age of 18, has been treated with lithium during which she developed secondary tubulointerstitial nephropathy as an adverse effect. Recently, she requested medical evaluation for constitutional syndrome associated with deterioration of general condition with loss of strength and difficulty in walking. Analytically, mild hypercalcemia was detected, and the study was extended to include Ca and PTH.
Chronic lithium therapy often develops mild hypercalcemia (approximately 10 to 20 percent of patients taking lithium), most likely due to increased secretion of PTH. Lithium can also unmask previously unrecognized mild hyperparathyroidism in patients with adenomas within a few years of starting therapy or induce parathyroid hyperplasia with a chronic use.
The hypercalcemia usually, but not always, subsides when the lithium is stopped. Normalization of serum calcium is more likely to occur one to four weeks post-lithium withdrawal in patients with a relatively short duration of lithium use. It is less likely in patients receiving lithium for more than 10 years.
Regarding the case to be presented, a review of the literature is carried out and the need to propose periodic calcium monitoring protocols is exposed.
ConclusionsRecommendations include determination of serum calcium every 6 months, urinary calcium and creatinine every 12 months, and bone mineral density monitoring every 1 to 3 years. Regular analytical monitoring including total calcium, PTH and vitamin D, would identify patients with a tendency to hypercalcemia so that appropriate measures could be taken. So as chronic treatment with lithium can develop mild hypercalcemia, I consider it necessary to develop periodic monitoring protocols for this adverse effect.
Disclosure of InterestNone Declared
Tobacco and hypertension: a descriptive study in a psychiatric short care unit
- I. Alonso Salas, A. Lopez Fariña, C. Gonzalez Navarro, A. Bilbao Idarraga, L. Morado San Segundo, U. Lopez Puentes, R. Lopez Brokate, T. Ruiz de Azua Aspizua, E. M. Garnica de Cos, U. Ortega Pozas, B. Samsó Martinez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S954-S955
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients affected by mental disorders are known to have a decreased life expectancy.
One of the main reasons are cardiovascular diseases. It is known that tobacco and hypertension are risk factors to develop them. WHO estimates that hypertension is diagnosed and treated in less than half of adults with hypertension, and even less in patients with severe mental illness.
ObjectivesTo describe the demographic characteristics of patients with tobacco comsumption and hypertension admitted to a short-term hospitalization unit.
MethodsA three-month retrospective observational study. Data were collected by interviewing incoming patients and performing a blood pressure measurement, with no exclusion criteria.
ResultsOf 172 patients admitted, 100 were smokers of whom 49 were men and 51 were women. Among the smokers, a total of 18 patients were diagnosed with hypertension and 79 were not diagnosed. Within the group of patients not diagnosed with hypertension, elevated blood pressure was recorded in 5 of them. A total of 67 patients were non-smokers, 23 of whom were male and 44 female. Among the non-smokers, 19 were diagnosed with hypertension and 48 were not, despite which elevated blood pressure levels were recorded in 4 of them. No data were collected from 5 patients.
ConclusionsThe prevalence of smokers in our sample was 58%. The prevalence of patients diagnosed with hypertension was 21,51% which is coherent with the existent literature. We did not find a higher percentage of hypertensive patients among the smokers admitted. There were patients who suffered from hypertension and were not diagnosed or treated previously.
Disclosure of InterestNone Declared
Thyroid disorders in psychiatric patients: a descriptive study in a psychiatric hospital
- U. López, L. Morado San Segundo, C. González Navarro, I. Alonso Salas, A. López Fariña, A. Bilbao Idarraga, B. Samsó Martínez, R. F. López Brokate, E. M. Garnica de Cos, T. Ruiz de Azua Aspizua, U. Ortega Pozas
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S471
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Thyroid disorders can present with psychiatric symptons similar to depression, and, at the same time, certain treatments, like litio, can cause changes in thyroid function. Given, therefore, the importance for the treatment and care of patients, the study of thyroid function is one of the parametres that should be requested in patients with psychiatric pathology.
ObjectivesTo study the frequency of thyroid disorders in patients who where admitted to a psychiatric short stay unit.
MethodsRetrospective descriptive observational study is carried out in the acute stay unit of a psychiatric hospital. As a sample, all patients admitted to the unit over a period of three months. During admission, their sociodemographic data, the treatment they receive and their diagnosis are recorded. Secondly, blood test are performed whith differents parameters, including TSH values.
ResultsIn the total sample of 172 patients, 8 of them have TSH abnormalities. 7 of them, all women, present hypothyroidism values.
A single male patient presented values of hyperthryroidism.
ConclusionsAccording to the present study, 4,6% of the patients present alterations at the TSH at admission, although except in one case, the values were not markedly altered.
The thyroid study at admission allows detecting cases of altered TSH that are amenable to treatment and monitoring.
Disclosure of InterestNone Declared
Under-diagnosis of alcohol abuse: a descriptive study in a psychiatric hospital
- A. Lopez Fariña, U. López Puentes, I. Alonso Salas, C. Gonzalez Navarro, A. Bilbao Idarraga, L. Morado Sansegundo, U. Ortega Pozas, C. Aran Cisneros, B. Samso Martinez, R. F. Lopez Brokate, T. Ruiz de Azua Aspizua, E. M. Garnica De Cos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S333
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Incidence of alcohol abuse in our country is high, although it is still under-diagnosed and under-treated. The WHO estimates that a total of 3.3 million deaths worldwide per year are related to alcohol consumption.
ObjectivesThe main objective is to describe the pattern of alcohol consumption in a sample of patients who are admitted to our psychiatric hospital for different reasons, relating with previous diagnoses.
MethodsA retrospective observational descriptive study was carried out in the acute care unit of the psychiatric hospital, after approval of the corresponding protocol by the ethics committee. All patients admitted to this unit during a three-month period were taken as a sample. During admission, sociodemographic data, drug use, treatment type and time and previous diagnoses were collected.
ResultsOut of 172 patients, 81 reported being abstemious, 45 declared occasional consumption, 11 weekly and 22 daily consumption. There is no data about 13 patients. Among those who reported daily alcohol consumption, 59% had a previous diagnosis of Substance Use Disorder (SUD), 23% a previous diagnosis of Schizophrenia, 13.5% of Bipolar Disorder and finally 4.5% of Depressive Disorder. All the patients with a previous diagnosis of SUD reported consumption of more than 10 SDUs/day, the group with Schizophrenia stated less than 5 SDUs/day, of the group with T. Bipolar between 7-10 SDUs/day and with T. Depressive 5 SDUs/day.
ConclusionsThe results obtained are consistent with the literature in relation to the under-diagnosis of alcohol use disorder, taking into account that 40% of patients in the sample with daily alcohol consumption previously had not such a diagnosis and it was not recorded in their medical history. For this reason, and for the sake of being able to treat them, it is essential to question all patients about alcohol consumption, whatever the reason for their admission.
Disclosure of InterestNone Declared
Survey on helminths of bats in the Yucatan Peninsula: infection levels, molecular information and host–parasite networks
- Wilson I. Moguel-Chin, David I. Hernández-Mena, Marco Torres-Castro, Roberto C. Barrientos-Medina, Silvia F. Hernández-Betancourt, M. Cristina MacSwiney G., Luis García-Prieto, Víctor M. Vidal-Martínez, Celia Isela Selem-Salas, Jesús Alonso Panti-May
-
- Journal:
- Parasitology / Volume 150 / Issue 2 / February 2023
- Published online by Cambridge University Press:
- 29 November 2022, pp. 172-183
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Helminth species of Neotropical bats are poorly known. In Mexico, few studies have been conducted on helminths of bats, especially in regions such as the Yucatan Peninsula where Chiroptera is the mammalian order with the greatest number of species. In this study, we characterized morphologically and molecularly the helminth species of bats and explored their infection levels and parasite–host interactions in the Yucatan Peninsula, Mexico. One hundred and sixty-three bats (representing 21 species) were captured between 2017 and 2022 in 15 sites throughout the Yucatan Peninsula. Conventional morphological techniques and molecular tools were used with the 28S gene to identify the collected helminths. Host–parasite network analyses were carried out to explore interactions by focusing on the level of host species. Helminths were found in 44 (26.9%) bats of 12 species. Twenty helminth taxa were recorded (7 trematodes, 3 cestodes and 10 nematodes), including 4 new host records for the Americas. Prevalence and mean intensity of infection values ranged from 7.1 to 100% and from 1 to 56, respectively. Molecular analyses confirmed the identity of some helminths at species and genus levels; however, some sequences did not correspond to any of the species available on GenBank. The parasite–host network suggests that most of the helminths recorded in bats were host-specific. The highest helminth richness was found in insectivorous bats. This study increases our knowledge of helminths parasitizing Neotropical bats, adding new records and nucleotide sequences.
Pediatric complex regional pain syndrome: a review
- A.M. Matas Ochoa, R. Martinez De Velasco, S. Bravo Herrero, I. Moreno Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S477
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Complex regional pain syndrome (CRPS) is a chronic localized pain condition that can have a significant impact on the quality of life. It affects children and adolescents as well as adults, but is more common among adolescent girls.
ObjectivesTo present up-to-date clinical information regarding CRPS in pediatric population.
MethodsA review of recent literature.
ResultsIn contrast to adults, CRPS appears after an initial event that is typically a minor trauma and occurs more frequently in the lower extremity than in the upper extremity. This syndrome is characterized by spontaneous or stimuli-induced pain, which is disproportionate to the actual incident trauma/stimulus, in the presence of a wide variety of autonomic and motor disturbances. The exact mechanism of CRPS is unknown, although several different mechanisms have been suggested. In many cases, CRPS follows a relatively minor trauma, in some cases, no previous injury was recalled and there are psychological factors implicated. It has been found a high prevalence of anxiety and depression in patients with CRPS and it is considered stress has an important role in inducing or perpetuating CRPS. Standard care consists of a multidisciplinary approach with the implementation of intensive physical therapy in conjunction with psychological counseling; in some patients, pharmacological treatments may help to reduce pain.
ConclusionsA multidisciplinary approach with psychological and psychiatric counseling are needed for effective management of CRPS. Further research in targeting specific mechanisms involved in the pathophysiology of CRPS should lead to prevention of this condition.
DisclosureNo significant relationships.
Building bridges between body and mind: liaison psychiatry
- S. Bravo Herrero, I. Moreno Alonso, M.J. Sánchez Artero, A.M. Matas Ochoa
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S472-S473
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
As liaison psychiatrists, it is very important to mantein a good relationship with other medical specialties in order to obtain the best result for our patients. Most of the times, the somatic process affects direct or indirectly to mental healt and vice versa, so our cooperation is extremely important for the patient’s welbeing.
ObjectivesWith this study we try to find special considerations and necesities of every specialty that count on us in our hospital. We have design this batebase with the aim of discovering which are the main problems that suffer the admitted patients, which doubts face our colleagues when evaluate mental health patients, etc. Thus, our team could help other physicians properly or so we could stablish a proper liaison in order to make things easier.
MethodsA database has been created with all the patients evaluated by our liaison psychiatry team during half a year. We have taken into account sex, age, referral specialist, mental health diagnosis (after our evaluation), previous mental health follow-up, if they are on psycopharmacology treatment, if they requiere psycopharmacology treatment and if they requiere follow-up once discharged.
Results22,9% were kid/adolescent patients. 25,8% were elderly people (>70 yo). 47% were men (of which, 6% were trans men), 53% were women. 22,9% suffered from adjustment disorder, 14,1% had no acute mental health problem, 11,76% presented substance abuse. Main petitions were made from Internal Medicine (30%)
ConclusionsWith this information we can explore other specialists’ and admitted patients’ needs and concerns and focus our effort in solving them.
DisclosureNo significant relationships.
Clinical predictors of hepatic complications in Anorexia Nervosa
- S. Villa, I. Sánchez, F. Fernandez-Aranda, N. Custal, J. Menchón, P. Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S386
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hepatic ones are some of the most described somatic complications in anorexia nervosa (AN) affected patients. They can be due to malnutrition, which is the more usual thing, or due to re-feeding. The first one can lead to more marked elevations of the hepatic enzymes, especially alanine-aminotransferase (ALT). It’s been also described the relation between a sharply decreased body mass index (BMI) and this kind of complications, but there are still to determine more predictors.
ObjectivesIdentifying clinical predictors of hepatic complications in AN.
MethodsWe analysed data from 71 AN affected patients hospitalized at Bellvitge Hospital from January 2016 to October 2021. We used IBM SPSS Statistics 22 to do all the statistics in this work.
ResultsThe medium age of the sample was 27.66 years with 10.8 years of evolution of AN. The medium BMI was 13.88. 33.80% of them had some sort of hepatic enzymes elevation, two of them a several one. AST, ALT and ALP were significantly more elevated in those patients with lower BMI. GGT was significantly more elevated in patients with more years of disorder development. We didn’t identify correlation between any purgative method and hepatic alterations.
ConclusionsThe elevation of ALT, AST and ALP seems to be related with the BMI of the patients, while the elevation of the GGT turns out to be related to the time of evolution of the eating disorder. Purgative methods don’t seem to be related to the development of hepatic alterations in AN.
DisclosureNo significant relationships.
Prevalence of depression in Europe using two different PHQ-8 scoring methods
- J. Arias De La Torre, G. Vilagut, A. Ronaldson, A. Serrano-Blanco, J. Valderas, V. Martín, A. Dregan, I. Bakolis, J. Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S299
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The prevalence of depression based on the Patient Health Questionnaire-8 (PHQ-8) may vary depending on the scoring method.
Objectives1) To describe the prevalence of depression in Europe using two PHQ-8 scoring methods. 2) To identify the countries with the highest prevalence according to each method.
MethodsData from 27 countries included in the European Health Survey (EHIS-2) for the year 2014/2015 were used (n=258,888). All participants who completed the PHQ-8 were included. The prevalence of depression and its 95% Confidence Interval (95%CI) were calculated overall for the whole of Europe and for each country using a PHQ-8≥10 cut-off point and the PHQ-8 algorithm scoring method. Weights derived from the complex sample design were considered for their calculation.
ResultsThe overall prevalence of depression for all Europe was lower using the PHQ-8>=10 cut-off point (6.38%, 95%CI 6.24-6.52) than the PHQ-8 algorithm (7.01%, 95%CI, 6.86-7.16). Using the PHQ-8≥10 cut-off point, the highest prevalence was observed in Iceland (10.33%, 95%CI, 9.33-11.32), Luxembourg (9.74%, 95%CI, 8.76-10.72) and Germany (9.24%, 95%CI, 8.82-9.66). Using the PHQ-8 algorithm the highest rates were observed in Hungary (10.99%, 95%CI,10.14-11.84), Portugal (10.63%, 95%CI, 9.96-11.29) and Iceland (9.80%, 95%CI, 8.77-10.83).
ConclusionsThere is variability in the prevalence of depression rates in Europe according to the PHQ-8 scoring method. These findings suggest the necessity of identify the method of choice for each country comparing with a gold standard measure (clinical diagnosis). Countries with consistent higher prevalence of depression based on PHQ-8 regardless of scoring method deserve further study.
DisclosureThis work has been funded by CIBERESP (ESP21PI05)
E-health treatments for Dual Disorders on pregnancy
- R. Carmona Camacho, N. Lopez Carpintero, I. Caro-Cañizares, L. Albarracin García, E. Baca Garcia, M. Sanchez Alonso
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S92-S93
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dual pathology during pregnancy, described as the co-occurrence of substance use and mental health problems, is one of the leading preventable causes of maternal and perinatal mortality and morbidity; however, effective and accessible treatments are lacking.
ObjectivesAs part of the WOMAP(Woman Mental Health and Addictions on Pregnancy) initiative, our study aimed to evaluate the effectiveness of an e-health-based psychotherapeutic program compared to enhanced usual care.
MethodsThis effectiveness clinical trial was conducted between 2016-2020 in 5 hospitals in the Madrid (Spain) metropolitan area. 2014 pregnant women under 26 weeks of pregnancy were screened. Eligible participants(n=120) were those who screened positive for co-occurring symptoms (AC-OK screener) and were not receiving specialized behavioral treatment. Participants were assessed in depth at baseline, 2,4,8 and 12 months(PHQ-9;GAD-7;PCL-5;AUDIT;DAST;Fagerström) and randomized to the usual care control group(n=38) or to two groups of a 10-session pregnancy-adapted psychotherapeutic program, one delivered by App/internet(n=41) and one by telephone(n=41). Intent-to-treat analyses assessed effectiveness.
ResultsStatistically significant effects of the intervention were found for mental health symptoms in the telephone group as compared to the control and App/internet groups, with an improvement effect starting earlier (2 months) and lasting longer (figures 1-3). Regarding substance use, due to the lack of other substances consumption, only smoking and alcohol cessation rates were analyzed. Patients in the App/internet and telephone groups discontinued significantly more, earlier and for a longer period compared to the control group(figures 4-5).
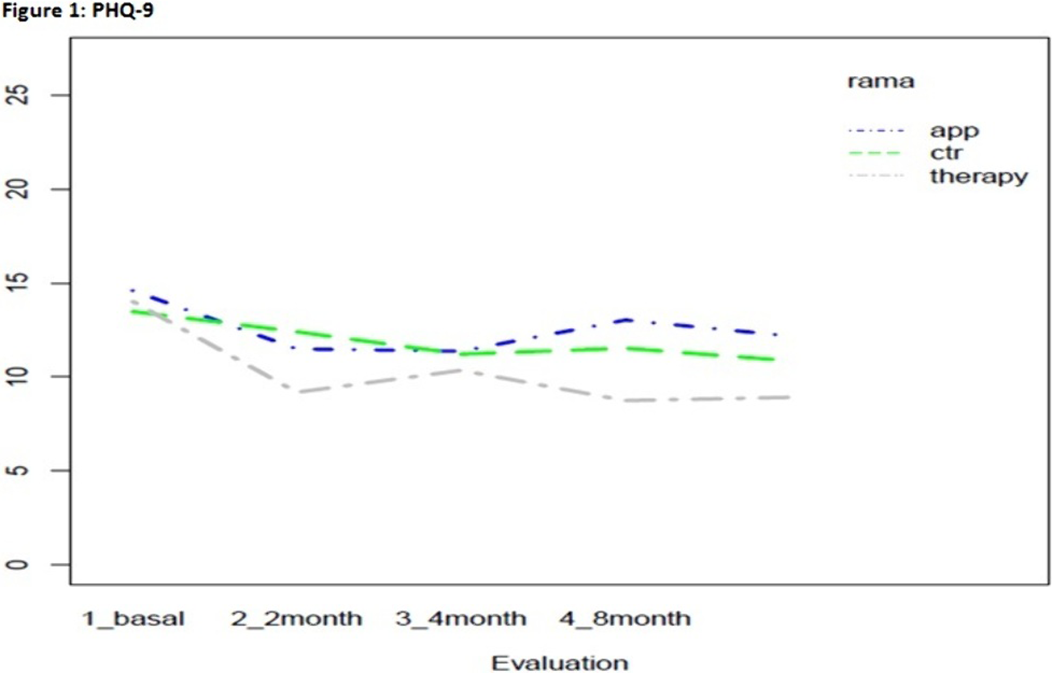
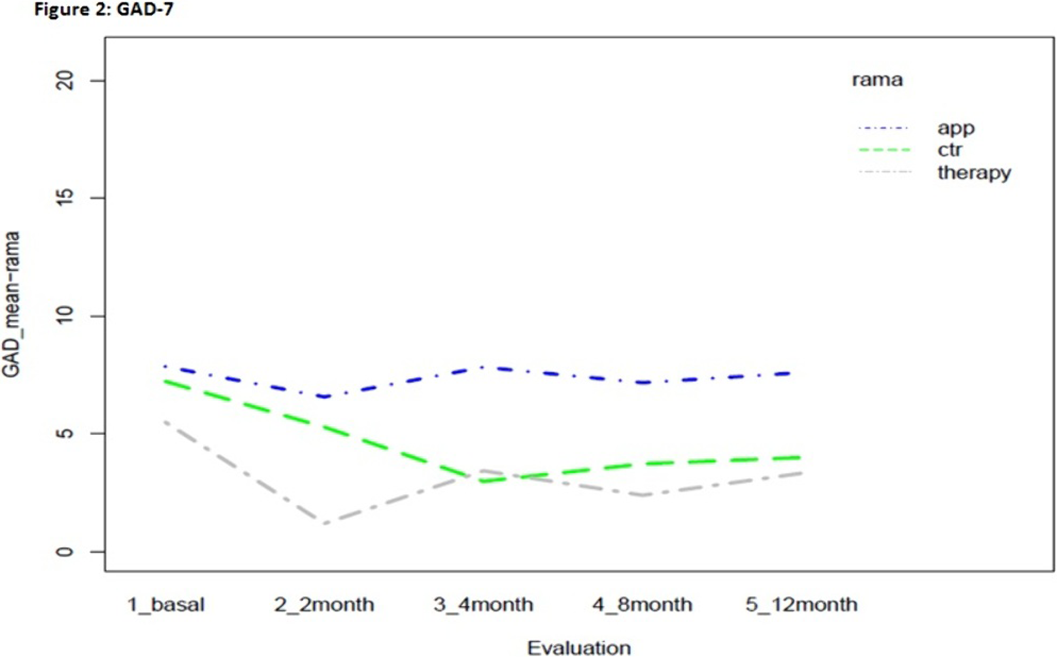
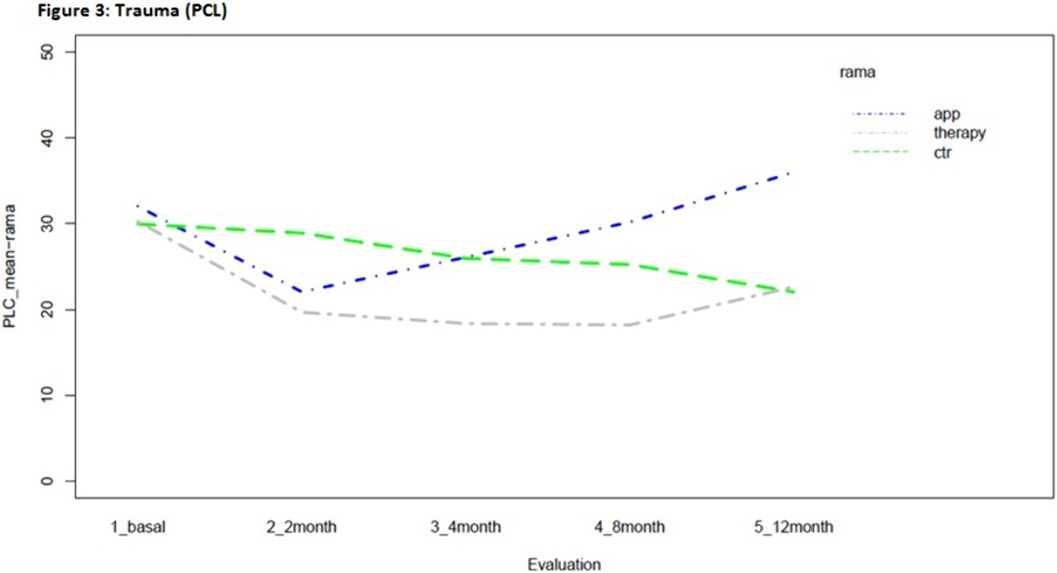
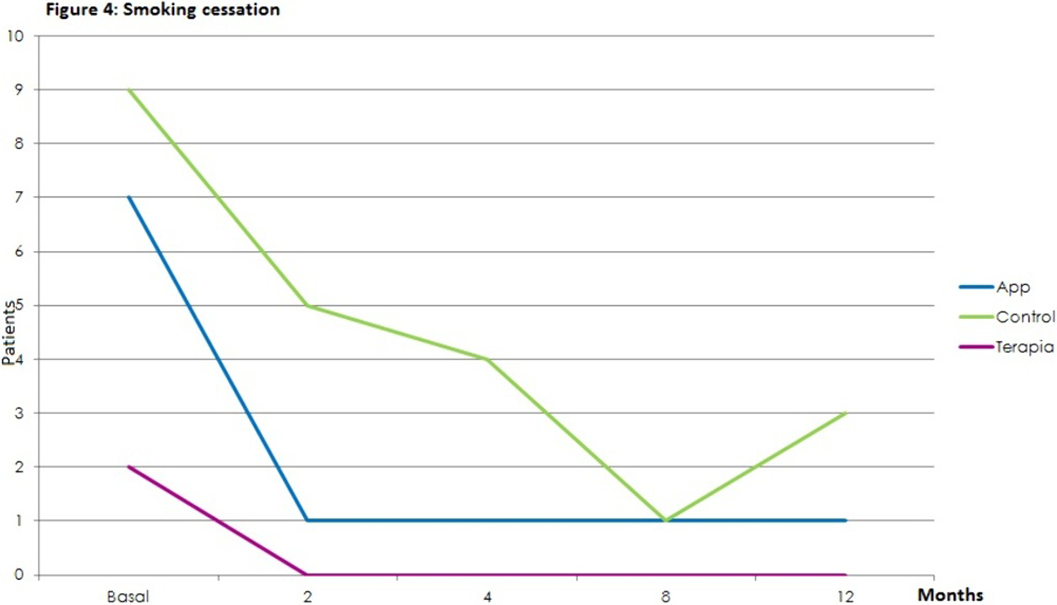
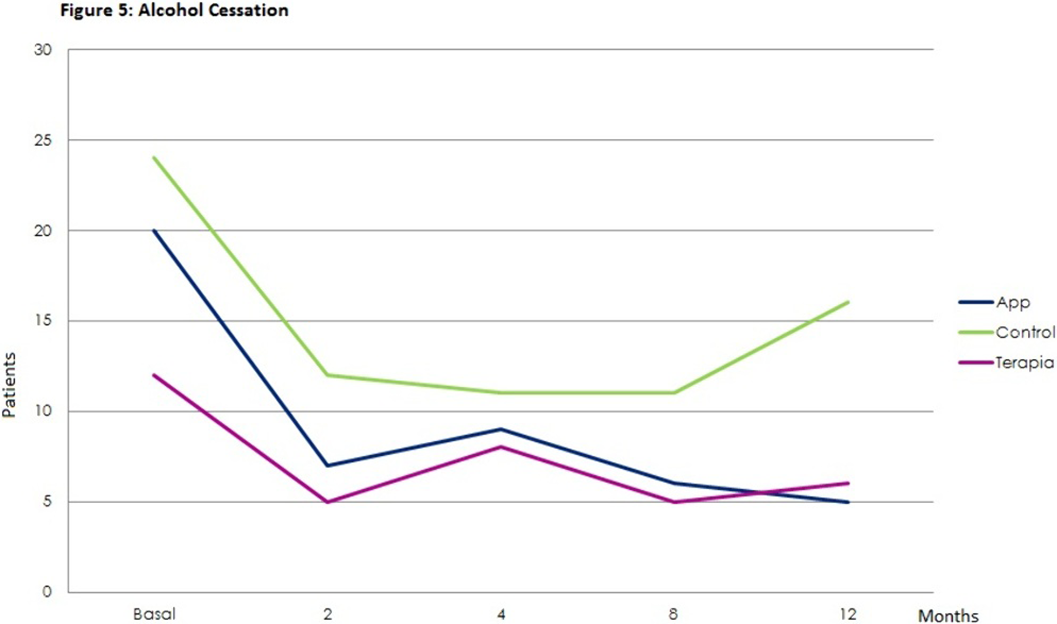 Conclusions
ConclusionsE-health psychotherapeutic programs could benefit pregnant women with dual disorders. An App/internet implementation could only be useful if focused solely on substances.
DisclosureNo significant relationships.
Neuropsychiatric phenotypes of anti-NMDAR encephalitis: a prospective study
- M. Espinola-Nadurille, M. Restrepo-Martínez, L. Bayliss, E. Flores-Montes, V. Rivas-Alonso, S. Vargas-Cañas, L. Hernández, I. Martínez-Juarez, A. Gonzalez-Aguilar, R. Solis-Vivanco, G. L. Fricchione, J. Flores-Rivera, J. Ramirez-Bermudez
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 9 / July 2023
- Published online by Cambridge University Press:
- 10 May 2022, pp. 4266-4274
-
- Article
- Export citation
-
Background
Patients with anti-N-methyl-d-aspartate (NMDA) receptor encephalitis (ANMDARE) show a wide range of behavioral abnormalities and are often mistaken for primary psychiatric presentations. We aimed to determine the behavioral hallmarks of ANMDARE with the use of systematic neuropsychiatric and cognitive assessments.
MethodsA prospective study was conducted, with 160 patients admitted to the National Institute of Neurology and Neurosurgery of Mexico, who fulfilled criteria for possible autoimmune encephalitis and/or red flags along a time window of seven years. Cerebrospinal fluid (CSF) antibodies against the NR1 subunit of the NMDAR were processed with rat brain immunohistochemistry and cell-based assays with NMDA expressing cells. Systematic cognitive, neuropsychiatric, and functional assessments were conducted before knowing NMDAR antibodies results. A multivariate analysis was used to compare patients with and without definite ANMDARE according to antibodies in CSF.
ResultsAfter obtaining the CSF antibodies results in 160 consecutive cases, 100 patients were positive and classified as having definite ANMDARE. The most frequent neuropsychiatric patterns were psychosis (81%), delirium (75%), catatonia (69%), anxiety-depression (65%), and mania (27%). Cognition was significantly impaired. A total of 34% of the patients had a predominantly neuropsychiatric presentation without seizures. After multivariate analysis, the clinical hallmarks of ANMDARE consisted of a catatonia–delirium comorbidity, tonic-clonic seizures, and orolingual dyskinesia.
ConclusionsOur study supports the notion of a neurobehavioral phenotype of ANMDARE characterized by a fluctuating course with psychotic and affective symptoms, catatonic signs, and global cognitive dysfunction, often accompanied by seizures and dyskinesia. The catatonia–delirium comorbidity could be a distinctive neurobehavioral phenotype of ANMDARE.
Mental impact of Covid-19 among Spanish healthcare workers. A large longitudinal survey
- J. Alonso, G. Vilagut, I. Alayo, M. Ferrer, F. Amigo, A. Aragón-Peña, E. Aragonès, M. Campos, I. del Cura-González, I. Urreta, M. Espuga, A. González Pinto, J. M. Haro, N. López Fresneña, A. Martínez de Salázar, J. D. Molina, R. M. Ortí Lucas, M. Parellada, J. M. Pelayo-Terán, A. Pérez Zapata, J. I. Pijoan, N. Plana, M. T. Puig, C. Rius, C. Rodriguez-Blazquez, F. Sanz, C. Serra, R. C. Kessler, R. Bruffaerts, E. Vieta, V. Pérez-Solá, P. Mortier, MINDCOVID Working group
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 31 / 2022
- Published online by Cambridge University Press:
- 29 April 2022, e28
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Longitudinal data on the mental health impact of the coronavirus disease 2019 (Covid-19) pandemic in healthcare workers is limited. We estimated prevalence, incidence and persistence of probable mental disorders in a cohort of Spanish healthcare workers (Covid-19 waves 1 and 2) -and identified associated risk factors.
Methods8996 healthcare workers evaluated on 5 May–7 September 2020 (baseline) were invited to a second web-based survey (October–December 2020). Major depressive disorder (PHQ-8 ≥ 10), generalised anxiety disorder (GAD-7 ≥ 10), panic attacks, post-traumatic stress disorder (PCL-5 ≥ 7), and alcohol use disorder (CAGE-AID ≥ 2) were assessed. Distal (pre-pandemic) and proximal (pandemic) risk factors were included. We estimated the incidence of probable mental disorders (among those without disorders at baseline) and persistence (among those with disorders at baseline). Logistic regression of individual-level [odds ratios (OR)] and population-level (population attributable risk proportions) associations were estimated, adjusting by all distal risk factors, health care centre and time of baseline interview.
Results4809 healthcare workers participated at four months follow-up (cooperation rate = 65.7%; mean = 120 days s.d. = 22 days from baseline assessment). Follow-up prevalence of any disorder was 41.5%, (v. 45.4% at baseline, p < 0.001); incidence, 19.7% (s.e. = 1.6) and persistence, 67.7% (s.e. = 2.3). Proximal factors showing significant bivariate-adjusted associations with incidence included: work-related factors [prioritising Covid-19 patients (OR = 1.62)], stress factors [personal health-related stress (OR = 1.61)], interpersonal stress (OR = 1.53) and financial factors [significant income loss (OR = 1.37)]. Risk factors associated with persistence were largely similar.
ConclusionsOur study indicates that the prevalence of probable mental disorders among Spanish healthcare workers during the second wave of the Covid-19 pandemic was similarly high to that after the first wave. This was in good part due to the persistence of mental disorders detected at the baseline, but with a relevant incidence of about 1 in 5 of HCWs without mental disorders during the first wave of the Covid-19 pandemic. Health-related factors, work-related factors and interpersonal stress are important risks of persistence of mental disorders and of incidence of mental disorders. Adequately addressing these factors might have prevented a considerable amount of mental health impact of the pandemic among this vulnerable population. Addressing health-related stress, work-related factors and interpersonal stress might reduce the prevalence of these disorders substantially. Study registration number: NCT04556565
Gut microbiota and its implications for psychiatry
- A. Matas Ochoa, A. Rodriguez Quiroga, R. Martinez De Velasco, P. Nava Garcia, C. Banzo Arguis, I. Moreno Alonso
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S471
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years there has been increasing interest in knowing the function of the microbiota, especially its role in the gut-brain axis. The microbiota is the set of millions of microorganisms that coexist in a symbiotic way in our body and are located in the digestive tract mainly. Numerous evidences show that the microbiota could modulate the information directed to the brain and therefore the pathogenic basis of numerous psychiatric and neurological disorders.
ObjectivesA better understanding of the microbiota and its interaction with the brain and mental health.
MethodsReview of recent literature about the implications of the gut microbiota in psychiatry.
ResultsThe connection between the microbiota and the central nervous system (gut-brain axis) occurs through the vagus nerve, the systemic pathway (through the release of hormones, metabolites and neurotransmitters) and the immune system (through the action of cytokines). Changes in the microbiota are associated not only with gastrointestinal diseases, but also with disorders such as depression, anxiety, autism, anorexia, attention deficit and hyperactivity, Alzheimer’s disease and Parkinson’s disease. As some research indicates, changes in diet and composition of the microbiota can reduce the risk of suffering these diseases or reduce their symptoms. Other therapeutic alternatives postulated are the use of probiotics or fecal microbiota transplantation.
ConclusionsDespite growing interest in the microbiota in the last few years, little is known about the mechanisms underlying this communication. More research is expected to contribute to the design of strategies that modulate the gut microbiota and its functions in order to improve mental health.
Levetirazetam psychosis
- C. Vilella Martín, M.Á. Alonso De La Torre López, P. García Vázquez, I. Gonzalez Rodríguez, S. Nuñez Sevillano, A. Serrano García
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S775
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Levetirazetam is an antiepileptic drug with psychiatric adverse reactions. It includes psychosis, paranoia or hallucinations. The frequency is less than 1%.
ObjectivesTo describe and study a case of Psychosis produced by Levetirazetam
MethodsRetrospective review of clinical records and complementary test, including psychiatry, electrophysiology and neurology. Diagnosis schales such as Salamanca Questionnaire were used as suport.
ResultsA 42-year-old woman diagnosed with tuberous sclerosis and undergoing treatment with levetirazetam acudes to the emergency department for behavioral disorders. She has presented an episode of aggression against a relative threatening him with a kitchen knife. The family reports that since the change in antiepilepticus 1 month ago, the patient has presented strange behaviors. Te Patient is conscious, uncooperative. Barely Approachable. Suspicious of her surroundings, with psychomotor restlessness, self-reference ideas and sparse speech. Auditory hallucinations seem to be present, as well as depressed and irritable mood. Psychic and somatic anxiety is found. Levetirazetam is discontinued, being replaced by valproic acid. Risperidone is started at a 3 mg dose. Treatment is well tolerated, and clinical stability is achived. Cluster A personality traits are found. Complementary test Blood and Urine simples, Imaging tests (CT and MRI), electroencephalogram and Electrocardiogram show no alterations
ConclusionsLevetirazetam can cause psychiatric adverse effects. it is important to make a proper diagnosis before a first psychotic outbreak in later life. Drugs that can produce psychiatric side effects should be identified and patients should be inform.
DisclosureNo significant relationships.






