59 results
Challenges in Managing Antipsychotic-Induced Hyperprolactinemia: A Case Study and Clinical Considerations for Aripiprazole Integration
- J. Garde Gonzalez, P. Herrero Ortega, A. Oliva Lozano, M. A. Morillas Romerosa, M. N. P. Soler
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S127
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Current guidelines for managing antipsychotic-induced hyperprolactinemia recommend the use of aripiprazole, either as a substitute or in combination with the primary antipsychotic. However, there have been reported cases of exacerbated psychotic symptoms when introducing aripiprazole after chronic treatment with another antipsychotic.
ObjectivesWe present a case of a patient with unspecified schizophrenia spectrum disorder receiving amisulpride, who developed worsened psychotic symptoms following the introduction of aripiprazole to treat hyperprolactinemia. We also review this phenomenon and its clinical management in the literature.
MethodsClinical case report and brief literature review.
ResultsMs. G, a 54-year-old woman diagnosed with unspecified schizophrenia spectrum disorder, was on amisulpiride 400mg/day and had remained asymptomatic for months. During a follow-up, she complained of mastalgia and had a prolactin level of 71.7 ng/mL. Following clinical guidelines, aripiprazole was added at 10mg/day. Within a month, anxiety and sleep disturbances escalated, followed by the reappearance of psychotic symptoms. Aripiprazole was discontinued, amisulpride reinstated, achieving stability. Subsequently, hyperprolactinemia was managed using metformin.
Antipsychotic-induced hyperprolactinemia is common, especially with first-generation antipsychotics, causing various symptoms in both genders. Long-term consequences may include weight gain, reduced bone density, and potentially increased breast cancer risk, among others.
Aripiprazole is an atypical antipsychotic with a partial agonist effect on dopamine D2 and D3 receptors. This means that aripiprazole will act as a functional D2-antagonist under hyperdopaminergic conditions, but a functional D2-agonist under hypodopaminergic conditions. This property of aripiprazole may contribute to counteract ‘prolactin-raising’ agents, acting as a D2 agonist, potentially reducing prolactin rise.
Chronic use of presynaptic D2/D3 antagonist (amisulpiride) might create a hypodopaminergic environment and hypersensitivity to dopamine agonists, possibly explaining worsened symptoms with aripiprazole introduction.
To prevent adverse outcomes when adding or switching to aripiprazole, gradual reduction of the previous antipsychotic (amisulpride) and high-dose aripiprazole initiation (30-40 mg/day) can help.
ConclusionsAntipsychotic-induced hyperprolactinemia is a serious issue that deserves our attention. While aripiprazole is recommended by several guidelines to treat it, introducing it to patients on chronic antipsychotic treatment may lead to a worsening of psychotic symptoms. Caution is recommended when combining aripiprazole with potent D2 receptor blockers. To mitigate this effect, gradual dose reduction of the previous antipsychotic and high-dose aripiprazole initiation are crucial.
Disclosure of InterestNone Declared
The relationship between sleep problems and suicidality in Bipolar Disorder: a Systematic Review and a Meta-analysis
- C. Possidente, M. Bort, M. De Prisco, V. Oliva, G. Fico, L. Bracco, C. Sommerhoff, L. Montejo, A. Murru, E. Vieta
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S77
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is a multifaceted illness encompassing mood, energy, cognitive and biorhythms alterations. Sleep disturbances are common in prodromic, acute and inter-episodic phases of BD. Suicidality presents a known association with sleep disturbances. However, their interplay in BD remains intricate and not fully elucidated.
ObjectivesThe aim of the present systematic review (SR) and meta-analysis (MA) is to summarise the available evidence and to provide an estimate of the association between sleep disturbances and suicidality, defined as presence of suicide ideation, behaviour and suicide attempts, in patients with BD.
MethodsWe conducted a comprehensive literature search following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines across PubMed, PsycINFO, and SCOPUS databases. We included all studies reporting an association between sleep problems and suicidal behaviour in BD patients. No language restriction was imposed. Effect sizes were calculated as odds ratio (OR) for dichotomic variables, standard mean difference (SMD) for continuous outcomes, and Spearman’s coefficient (r) for correlations. Heterogeneity was assessed using the I2 statistic. Global inconsistency was evaluated using the Q statistics with the corresponding p-value.
ResultsThe initial search yielded 911 unique abstracts, of which 62 underwent full-text screening. Fourteen publications were included, comprising twelve cross-sectional and two longitudinal studies. The total sample consisted of 19,601 subjects diagnosed with BD, of which 51.76% were females and 69.52% had a diagnosis of BD type 1. We found that people with BD and sleep disturbances tend to have higher suicidality, both current (SMD=0.79, 95%CI=0.53, 1.05) and lifetime (OR=1.8; 95%CI=1.41, 2.55), when compared with people with BD and no sleep disturbances. Additionally, patients with BD and a history of suicide attempts tend to have more sleep problems (OR=1.37, 95%CI=1.21, 1.55). Moreover, a positive correlation exists between suicidality and poor sleep quality measured by the Pittsburgh Sleep Quality Index (PSQI) (r= 0.24, 95%CI=0.10, 0.36). No heterogeneity was found, except in the subanalysis of correlation (I2=66.67%, Q p-value=0.01).
ConclusionsOur SRMA outlines a positive relation between sleep disturbances and suicidality in patients with BD. The small number of included studies and the scarcity of longitudinal studies, preventing the inference of a causal relationship, represent the major limitations of this study. Also, studies with objective measures of sleep alterations are currently lacking. The prompt recognition, objective measurement, and treatment of sleep alterations could be crucial in averting or reducing suicidal attempts in BD.
Disclosure of InterestC. Possidente: None Declared, M. Bort: None Declared, M. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: Fellowship from “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), L. Bracco: None Declared, C. Sommerhoff: None Declared, L. Montejo: None Declared, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672, PI22/00840) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER), E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/ 00805, PI21/00787) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdireccio ́n General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357; the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151).
Cognitive reserve in Older Adults with Bipolar Disorder and its relationship with cognitive performance and psychosocial functioning
- L. Montejo, C. Torrent, S. Martín, A. Ruiz, M. Bort, G. Fico, V. Oliva, M. De Prisco, J. Sanchez-Moreno, E. Jimenez, A. Martinez-Aran, E. Vieta, B. Sole
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S324-S325
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cognitive reserve (CR) refers to the ability of the brain to cope with damage or pathology. In bipolar disorder (BD), it has been seen that the effects of the disease may potentially reduce CR, thus compromising cognitive outcomes. This concept takes on special relevance in late life in BD, due to the increased risk of cognitive decline because of the accumulative effects of the disease and the potential effects of aging. Therefore, we believe that CR may be a protective factor against cognitive decline in older adults with bipolar disorder (OABD).
ObjectivesThe aim of this study was to study the CR in OABD compared with healthy controls (HC) and to analyze its association with psychosocial functioning and cognitive performance.
MethodsA sample of euthymic OABD, defined as patients over 50 years old, and HC were included. CR was assessed using the CRASH scale. Differences in demographic, clinical, and cognitive variables between patients and HC were analyzed by t-test or X2 as appropriated. Lineal simple and multiple regressions analyses were used to study the association of CR and several clinical variables with functional and cognitive performance.
ResultsA total of 83 participants (42 OABD and 41 HC) were included. Compared to HC, OABD exhibited poorer cognitive performance (p<0.001), psychosocial functioning (p<0.001) and lower CR (p<0.001). Within the patient’s group, the linear simple regression analysis revealed that CR was associated with psychosocial functioning (β=-2.16; p=0.037), attention (β= 3.03; p=0.005) and working memory (β = 2.98; p=0.005) while no clinical factors were associated. Age and CR were associated with processing speed and verbal memory, but after applying multiple regression model, only the effect of age remained significant (β =-2.26; p= 0.030, and β =-2.23; p= 0.032 respectively). CR, age, and number of episodes were related to visual memory, but the multiple regression showed that only age (β = -2.37; p= 0.023) and CR (β = 3.99; p<0.001) were associated. Regarding executive functions only the number of manic episodes were significant. CR and age at onset were associated with visuospatial ability, but multiple regression only showed association of CR (β =2.23; p=0.032). Other clinical factors such as number of depressive or hypomanic episodes, illness duration, admissions, type of BD, and psychotic symptoms were not associated.
ConclusionsTo the best of our knowledge, this is the first report that studies the CR in a sample of OABD. We demonstrated that OABD had lower CR than HC. Importantly, we observed that CR was associated with cognitive and psychosocial functioning in OABD, even more than disease-related factors. These results suggest the potential protector effect of CR against cognitive impairment, supporting that improving modifiable factors associated with the enhancement of CR can prevent cognitive decline.
Disclosure of InterestL. Montejo: None Declared, C. Torrent Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00344) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER), S. Martín: None Declared, A. Ruiz: None Declared, M. Bort: None Declared, G. Fico Grant / Research support from: Fellowship from “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), V. Oliva: None Declared, M. De Prisco: None Declared, J. Sanchez-Moreno Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00060) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER),, E. Jimenez Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00060)integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER),, A. Martinez-Aran: None Declared, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/ 00805, PI21/00787) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIIISubdireccio ́n General de Evaluacio ́n and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357; the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151)., B. Sole: None Declared
Diagnostic Challenges in Affective Disorders: Delirious Mania - A Case Report and Literature Review.
- P. Herrero Ortega, A. Oliva Lozano, J. Garde González, M. A. Morillas Romerosa
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S438
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Affective disorders exhibit diverse clinical manifestations, and one distinctive subtype is delirious mania. Despite its exclusion from formal diagnostic manuals, delirious mania frequently emerges in everyday clinical practice. Recognizing it within the realm of differential diagnosis is crucial. Delirious mania is characterized by acute onset of excitement, grandiosity, emotional lability, delusions, and insomnia typical of mania, combined with disorientation and altered consciousness characteristic of delirium. Some authors consider delirious mania as a variant of classic bipolar disorder, while others associate it with catatonia. Additionally, some link it to underlying medical or neuropsychiatric causes.
ObjectivesTo describe the clinical case of a patient with delirious mania and emphasize the importance of recognizing this as a potencial diagnosis in patients with abrupt alterations in mental state.
MethodsClinical case report and literature review.
ResultsA 61-year-old female patient with a history of a unique depressive episode over 20 years ago, treated with Carbamazepine up to 750 mg, is admitted to the Emergency Room with acute symptoms consistent in global disorientation, agressive behavior, mutism, bradyphrenic and repetitive incoherent speech, along with visual hallucinations, all of which had developed over a few days. The gradual withdrawal of Tegretol over an 8-month period preceded her admission to the ER.
Relevant medical tests, including cranial CT, EEG, blood tests, and urine analysis, were conducted during her ER stay, all of which yielded normal results. Neurological evaluation ruled out acute neurological pathology, leading to her subsequent admission to the Psychiatry department. Throughout her admission, the patient exhibited irritability and expressed derogatory comments filled with offensive language. She gradually became more expansive, with her thought content becoming megalomaniac in a delirious range. Her speech was incoherent, verbose and had loose associations.
Treatment was reintroduced with Carbamazepine up to 600 mg/day and Olanzapine up to 20 mg/day, resulting in a rapid and comprehensive improvement of her symptoms, ultimately leading to the complete resolution of her condition.
ConclusionsThis case highlights the concept of delirious mania, characterized by alterations in attention, orientation, memory, confusion, behavioral and thought fluctuations, and psychomotor disturbances which can manifest abruptly, as observed in this patient. This clinical case underscores the significance of considering delirious mania in the differential diagnosis of patients with abrupt alterations in mental state, particularly those of advanced age with a history of affective episodes. A global understanding of this condition is essential for its timely recognition and appropriate management.
Disclosure of InterestNone Declared
Interplay of Environmental Factors, Genetic Susceptibility, and Sleep Disturbances predict Bipolar Disorder’s Relapses: preliminary results from a pilot study
- M. Bort, G. Fico, V. Oliva, M. de Prisco, L. Bracco, C. Possidente, M. Y. Rivas, V. Ruiz, L. Montejo, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S251
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Predicting acute affective episodes in individuals with Bipolar Disorder (BD) remains a clinical challenge. Specific environmental stressors, including air pollution, noise, and temperature variations might worsen affective symptoms or sleep in the general population, but their role in BD relapses is often overlooked. Indeed, they might exacerbate BD by perturbing circadian rhythms – fundamental aspects of BD.
ObjectivesWe thereby present the protocol of this pilot study and future preliminary data. We aim to longitudinally assess sleep alterations, mood fluctuations, and environmental exposure to several factors (air pollutants, climate, noise, artificial light-at-night, green space access) in patients with BD and to check the association of these variables with BD relapses.
MethodsIn this pilot study, we will recruit 40 patients with BD in a 6-month prospective study. Patients were assessed during baseline, at 3 and 6 months. Data recollected will consist of a subjective (questionnaires) and objective (through meteorological stations) evaluation of physical environmental factors around the home residence; clinical assessment of mood and circadian rhythms, and continuous tracking of sleep-wake patterns, energy, and movement using actigraphy.
ResultsExpected results will show that exposure to a worse environment (higher pollution, noise, light exposure, climate) will be associated with worse BD outcomes (i.e., relapse, mood symptoms, sleep alterations).
ConclusionsWe will be sharing preliminary data from our ongoing study, offering insights into early patterns and findings that shed light on our objectives.
Disclosure of InterestNone Declared
Sex differences in neurocognitive performance in older adults with bipolar disorder
- S. Martín-Parra, C. Torrent, A. Ruiz, M. Bort, G. Fico, V. Oliva, M. D. Prisco, J. Sanchez-Moreno, E. Jimenez, A. Martinez-Aran, E. Vieta, B. Sole, L. Montejo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S440
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years, research has focused on the older adults with bipolar disorder (OABD), aged 50 years and over, a constantly growing population due to the increased of life expectancy. Actually, some authors suggest that these individuals constitute a distinct subtype with a specific and different needs such as seen in epidemiologic, clinical and cognitive features. Further research has revealed significant differences between females and males with BD in clinical and cognitive variables in middle-aged and young patients, but this topic among OABD population remains unclear.
ObjectivesThe aim of this study is to identify the distinctive profile in clinical, functional and neurocognitive variables between females and males in OABD.
MethodsA sample of OABD and Healthy Controls (HC) were included. Euthymic patients or in partial remission were included. Neurocognition was measured with a battery of tests that included premorbid intelligence quotient, working memory, verbal and visual memory, processing speed, language and executive functions. Independent t-test and Chi-squared test analysis were performed as appropriated.
ResultsAccording to the analysis, statistically significant differences were seen between females and males. A more impaired cognitive profile is observed in women. They performed worse in the subscales of Arithmetic (F= 6.728, p = <0.001), forward digits (F= 0.936, p= 0.019) and Total Digits (F= 1.208, p= 0.019) of the WAIS-III, in the Stroop Color Word Test, color reading (F= 0.130, p= < 0.001), in the Continuous Performance Test, block change measure (F= 2.059, p= 0.037), in the Rey-Osterrieth Complex Figure-copy (F= 0.005, p= 0.029) and in the Boston Naming Test (F= 0.011, p= 0.024). Nor significant differences were found in clinical neither in psychosocial functioning variables.
ConclusionsIn view of the following results, and since no differences were observed between women and men in terms of clinical and functional outcomes, it could be said that the differences observed in cognition cannot be explained by disease-related factors. Furthermore, these results highlight the need to develop a gender-specific cognitive interventions in OABD population. In this way, we could have an impact on the course of the illness to reach a better quality of life.
Disclosure of InterestS. Martín-Parra: None Declared, C. Torrent Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00344) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIIISubdireccion General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), A. Ruiz: None Declared, M. Bort: None Declared, G. Fico Grant / Research support from: Fellowship from “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), V. Oliva: None Declared, M. Prisco: None Declared, J. Sanchez-Moreno Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00060) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), E. Jimenez Grant / Research support from: Spanish Ministry of Science and Innovation (PI20/00060) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdireccion General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), A. Martinez-Aran: None Declared, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/ 00805, PI21/00787) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357; the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), B. Sole: None Declared, L. Montejo: None Declared
Peduncular Hallucinosis: Clinical characteristics, etiology, and a case report
- J. Garde Gonzalez, A. Oliva Lozano, P. Herrero Ortega, M. A. Morillas Romerosa
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S260
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Visual hallucinations are a relatively common neurological complaint. Peduncular hallucinosis (PH) stands out as a distinct entity, characterized by complex visual hallucinations resulting from structural lesions in the brainstem or diencephalon.
ObjectivesWe aim to provide an overview of the clinical features, etiological factors, and management strategies associated with PH, incorporating a unique case study.
MethodsClinical case report and brief literature review.
ResultsClinical Characteristics: PH is marked by detailed, colorful, vivid, and occasionally emotionally charged visual hallucinations. These hallucinations encompass people, animals, or objects and may be mistaken for reality. While primarily visual, they may occasionally involve other sensory modalities. Crucially, patients with PH maintain insight, distinguishing it from primary psychotic disorders.
Etiological Factors: PH is most commonly associated with structural brainstem lesions, particularly in the midbrain. Potential instigators encompass ischemic strokes, vascular anomalies, tumors and infections. Disruption of the reticular activating system in the brainstem is implicated in the pathogenesis. Advanced imaging techniques have unveiled cases with subtle presentations, broadening our comprehension of PH.
Pathogenesis: PH may involve the disturbance of serotonergic inhibitory pathways and the reticular activating system. A plausible link with hypnagogic hallucinations hints at a mechanism related to rapid REM sleep transitions.
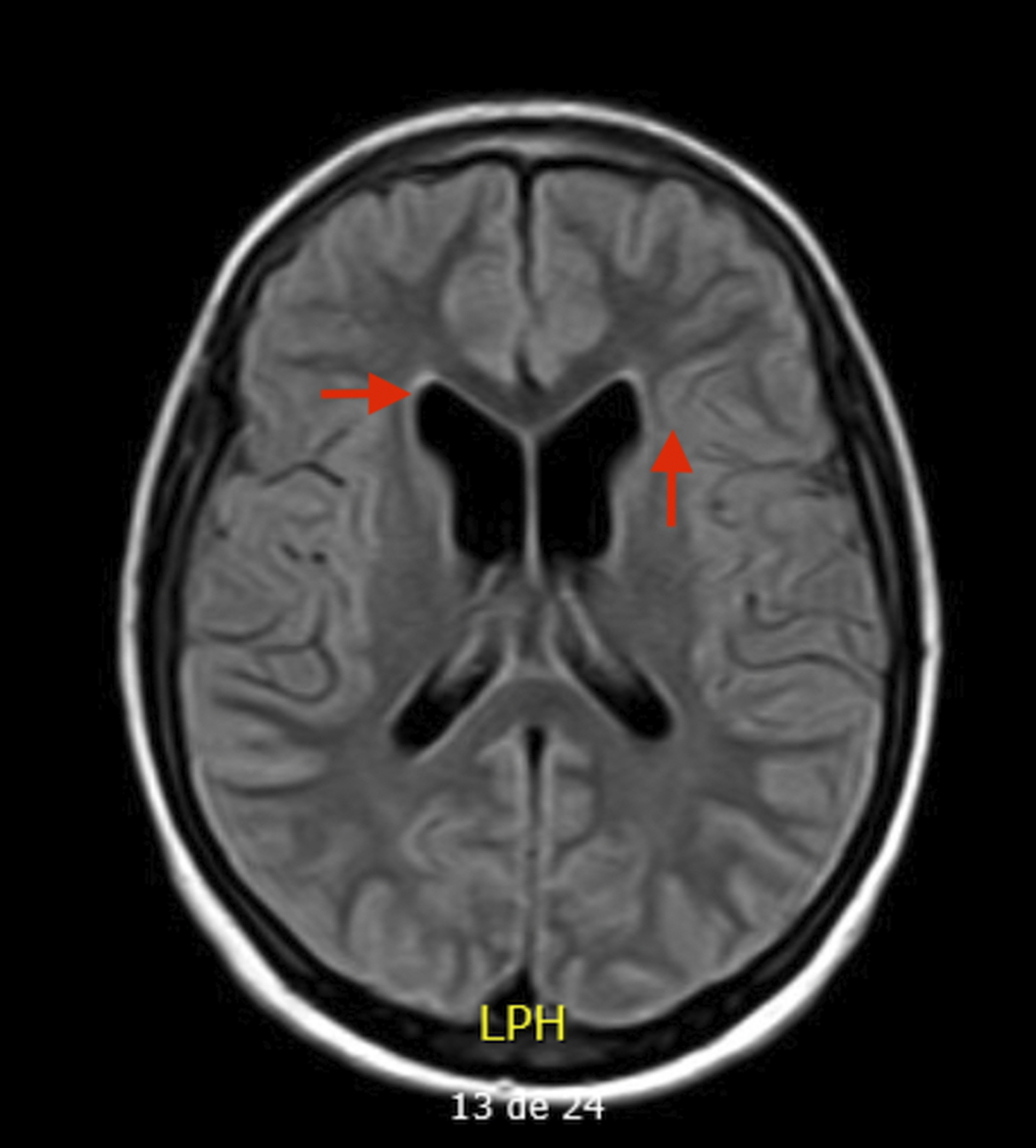
Case Report: Mr. J., a 30-year-old patient, suffered recurrent mesencephalic strokes attributed to Sneddon’s syndrome, ADA-2 deficiency, and protein C deficiency, leading to malacic lesions in the hemimesencephalon and right hemipons. He experienced complex visual hallucinations, primarily geometric patterns and animals, mainly at night. Importantly, he maintained insight into their hallucinatory nature. Mr. J. also had diplopia, visual impairment, recurrent headaches, and left hemiparesis.
Reactive anxiety and depression due to functional loss followed his recurrent strokes. Initially, antipsychotics were used to manage sensory-perceptual disturbances, but were later discontinued due to reduced interference with daily functioning. Antidepressant and psychological therapy was continued throughout the follow-up to address mood symptoms.
ConclusionsPeduncular hallucinosis is an intriguing phenomenon characterized by complex visual hallucinations. Understanding its clinical features, etiology, and possible mechanisms is essential for accurate diagnosis and management. This case report emphasizes PH’s clinical aspects and the importance of a multidisciplinary approach, including pharmacological intervention and psychological support. Understanding its features, causes, and management is essential for accurate care. Further research is needed to improve our comprehension and optimize treatment strategies.
Disclosure of InterestNone Declared
Severe Hyperhidrosis Secondary to Bupropion Use and Treatment. A case report.
- A. Oliva Lozano, J. Garde Gonzalez, M. A. Morillas Romerosa, P. Herrero Ortega
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hyperhidrosis, the excessive and uncontrollable sweating, is a well-documented side effect of various medications. Among these, bupropion, a commonly prescribed antidepressant and smoking cessation aid, has been associated with the development of severe hyperhidrosis in a subset of patients. This clinical report aims to shed light on a compelling case of severe hyperhidrosis induced by bupropion use and the subsequent treatment strategies employed
The patient under discussion is a 42-year-old female with a history of recurrent major depressive disorder and a previous favorable response to selective serotonin reuptake inhibitors (SSRIs). Due to side effect concerns and a desire to quit smoking, she was transitioned to bupropion, a norepinephrine-dopamine reuptake inhibitor (NDRI), at a standard therapeutic dose of 150 mg daily.
Approximately four weeks after initiating bupropion therapy, the patient began experiencing debilitating symptoms of excessive sweating, particularly affecting her palms, soles, and axillae. The profuse sweating episodes occurred throughout the day and night, significantly impairing her quality of life, social interactions, and occupational functioning. No previous history of hyperhidrosis was reported, and physical examinations revealed no underlying medical conditions or dermatological issues.
ObjectivesTo aknowledge the importance of recognizing and addressing medication-induced side effects within the realm of psychiatry and an early implementation of patient-centered treatment.
MethodsClinical case report and a brief literature review.
ResultsThe treatment of hyperhidrosis secondary to bupropion use presents a challenging clinical scenario that requires a delicate balance between managing the distressing side effect and ensuring the continued efficacy of psychiatric therapy. Given the rarity of severe hyperhidrosis as a side effect of bupropion, there is a limited body of evidence guiding treatment strategies. Gradual withdrawal in the dose of bupropion was initiated, with careful monitoring of depressive symptoms to prevent relapse, switching to Duloxetine 90mg daily, with adecuate efectiveness.In this particular case, the combination of medication adjustment and psychological support led to a significant reduction in hyperhidrosis symptoms. The patient reported improved social interactions, enhanced self-esteem, and restored occupational functioning. Importantly, her depressive symptoms remained well-managed, underscoring the success of the treatment strategy.
ConclusionsThis clinical report highlights the importance of a patient-centered approach when addressing rare medication-induced side effects within the field of psychiatry. Bupropion withdrawal and regular follow-up showed effective in the treatment of the simptoms. Future research may provide additional insights and treatment options for cases like this, further enhancing patient care and outcomes.
Disclosure of InterestNone Declared
Identifying digital biomarkers of illness activity and treatment response in bipolar disorder with a novel wearable device (TIMEBASE): protocol for a pragmatic observational clinical study
- Gerard Anmella, Filippo Corponi, Bryan M. Li, Ariadna Mas, Marina Garriga, Miriam Sanabra, Isabella Pacchiarotti, Marc Valentí, Iria Grande, Antoni Benabarre, Anna Giménez-Palomo, Isabel Agasi, Anna Bastidas, Myriam Cavero, Miquel Bioque, Clemente García-Rizo, Santiago Madero, Néstor Arbelo, Andrea Murru, Silvia Amoretti, Anabel Martínez-Aran, Victoria Ruiz, Yudit Rivas, Giovanna Fico, Michele De Prisco, Vincenzo Oliva, Aleix Solanes, Joaquim Radua, Ludovic Samalin, Allan H. Young, Antonio Vergari, Eduard Vieta, Diego Hidalgo-Mazzei
-
- Journal:
- BJPsych Open / Volume 10 / Issue 5 / September 2024
- Published online by Cambridge University Press:
- 01 August 2024, e137
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Bipolar disorder is highly prevalent and consists of biphasic recurrent mood episodes of mania and depression, which translate into altered mood, sleep and activity alongside their physiological expressions.
AimsThe IdenTifying dIgital bioMarkers of illnEss activity and treatment response in BipolAr diSordEr with a novel wearable device (TIMEBASE) project aims to identify digital biomarkers of illness activity and treatment response in bipolar disorder.
MethodWe designed a longitudinal observational study including 84 individuals. Group A comprises people with acute episode of mania (n = 12), depression (n = 12 with bipolar disorder and n = 12 with major depressive disorder (MDD)) and bipolar disorder with mixed features (n = 12). Physiological data will be recorded during 48 h with a research-grade wearable (Empatica E4) across four consecutive time points (acute, response, remission and episode recovery). Group B comprises 12 people with euthymic bipolar disorder and 12 with MDD, and group C comprises 12 healthy controls who will be recorded cross-sectionally. Psychopathological symptoms, disease severity, functioning and physical activity will be assessed with standardised psychometric scales. Physiological data will include acceleration, temperature, blood volume pulse, heart rate and electrodermal activity. Machine learning models will be developed to link physiological data to illness activity and treatment response. Generalisation performance will be tested in data from unseen patients.
ResultsRecruitment is ongoing.
ConclusionsThis project should contribute to understanding the pathophysiology of affective disorders. The potential digital biomarkers of illness activity and treatment response in bipolar disorder could be implemented in a real-world clinical setting for clinical monitoring and identification of prodromal symptoms. This would allow early intervention and prevention of affective relapses, as well as personalisation of treatment.
Characterization and drug release of benzalkonium chloride-loaded organo-palygorskite or organo-montmorillonite
- Héctor A. Lobato-Aguilar, Wilberth A. Herrera-Kao, Santiago Duarte-Aranda, Fernando J. Aguilar-Pérez, Andrés I. Oliva-Arias, Víctor Rejón-Moo, José M. Baas-López, Jorge A. Uribe-Calderón, José M. Cervantes-Uc
-
- Journal:
- Clay Minerals / Volume 58 / Issue 2 / June 2023
- Published online by Cambridge University Press:
- 21 July 2023, pp. 102-112
-
- Article
- Export citation
-
This study examined the incorporation of benzalkonium chloride into palygorskite and montmorillonite, assessing their potential as drug carriers. The aim was to evaluate the use of both clay minerals as viable options for antibacterial drug delivery. Various amounts (0.5, 1.0 and 2.0 times the cation-exchange capacity) of benzalkonium chloride were incorporated into both clay minerals, and the resulting materials were characterized using Fourier-transform infrared spectroscopy, thermogravimetric analysis, X-ray diffraction and elemental analysis using both CHNS-O elemental analysis and energy-dispersive X-ray spectroscopy. The Fourier-transform infrared spectroscopy and elemental analysis results indicate that benzalkonium chloride was incorporated successfully into the clay minerals. The X-ray diffraction traces of organo-montmorillonite indicate that the d-value increased as benzalkonium chloride content increased, confirming the intercalation of benzalkonium chloride within the montmorillonite interlayer space. By contrast, this behaviour was not observed for palygorskite. For the benzalkonium chloride-release studies, an initial burst release was found within the first 5 h, followed by a sustained release of benzalkonium chloride during the remaining testing time (24 h). Drug-release profiles were similar for modified palygorskite or montmorillonite during the testing time (24 h). Both clay minerals modified with benzalkonium chloride are promising materials for use as antibacterial fillers for several applications, including in the dental care industry.
Group psychotherapy for patients with first-episode psychosis: Effect on the clinical status and use of resources
- P. Herrero Ortega, A. Oliva Lozano, J. Garde González, C. Bayón-Pérez, R. Mediavilla, M. P. Vidal-Villegas, B. Rodríguez-Vega, S. Cebolla, E. Román, E. V. Pérez Pérez, M. F. Bravo-Ortiz, O. B. O. AGES-Mind Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S635-S636
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorders carry several economical, psychological and social consequences, both at individual and community levels. Early intervention programs after first-episode psychosis which combine pharmacological and psychosocial strategies are aimed at reducing symptoms, lowering costs in the use of health and non-health care resources and improving overall functioning. AGES-Mind study is based on manualized psychotherapeutic interventions for people with first-psychosis episodes.
ObjectivesThe aim of the study was to evaluate the effect of a group psychotherapeutic intervention on the clinical status and use of clinical resources in a sample of patients with first-episode psychosis at 12 and 24 months after the beginning of the intervention. This cohort will be compared to patients with first-psychosis episodes without group psychotherapeutic intervention.
MethodsLongitudinal, observational, retrospective study on a cohort of N=46 patients with first-episode psychosis within the last 5 years. Two groups of 23 patients each were formed. The participants of one of those groups received group psychotherapy in the context of the AGES-Mind study and the other group received treatment as usual without group intervention. Non-exposed patients were matched by age, gender and time elapsed since first-episode psychosis with those exposed to the intervention. Sociodemographic data, clinical status and use of clinical resources outcome variables were assessed.
ResultsNo significant differences were found in clinical status and use of resources between participants and non-participants in the psychotherapeutic group intervention after 12 and 24 months.
ConclusionsAfter controlling for potentially confounding variables as sociodemographic, age and time since first-episode, participating in a group psychotherapeutic program does not seem to improve clinical variables or use of resources. Further studies with larger samples would be necessary to explore other variables, such as symptoms, satisfaction with the intervention or social functioning.
Disclosure of InterestNone Declared
AGESMind clinical trial: SocialMIND® results at 16 weeks
- M. P. Vidal-Villegas, A. Abad Pérez, P. Herrero Ortega, A. Oliva Lozano, J. Garde González, J. Andreo-Jover, A. Muñoz-Sanjosé, R. Mediavilla, B. Rodríguez-Vega, G. Lahera, Á. Palao-Tarrero, C. Bayón-Pérez, M. F. Bravo-Ortiz
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S480-S481
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Early intervention on a first psychotic episode is fundamental for a more favorable prognosis, and it usually combines pharmacological treatment, which mainly affects positive psychotic symptoms, with interventions that can improve the rest of the symptoms and associated problems such as deterioration in social functioning (Harvey & Penn, 2010; Fusar-Poli, McGorry & Kane, 2017). While Mindfulness is gaining more and more prominence in the field of psychotherapy (Chan et al., 2019; Cillesen et al., 2019), social cognition and social functioning are being researched as key targets on which to intervene after a first psychotic episode (Green, Horan & Lee, 2015).
SocialMIND® is a mindfulness-based social cognition training tailor-made to improve social functioning in people who have suffered a first psychotic episode within the last five years. It is currently being compared with a group Psychoeducational Multicomponent Intervention (PMI) in a Randomized Controlled Trial (RCT) (Mediavilla et al., 2019). Both group psychotherapies include 17 sessions delivered over a 9 month period: 8 weekly sessions, 4 biweekly sessions and 5 monthly sessions.
The results of SocialMIND® at 8 weeks showed improvements in social cognition and social functioning, specifically on affective social cognition and self-care (Mediavilla et al., 2021).
ObjectivesTo evaluate the efficacy of SocialMIND® in improving social functioning, measured by the Personal and Social Functioning (PSP) scale 16 weeks after starting the intervention, in people who have suffered a first psychotic episode in the last 5 years.
MethodsRandomized, controlled pilot trial (use of a psychoeducational multicomponent intervention or PMI as active comparator) of two parallel groups (SocialMIND® and PMI) with a 1:1 ratio using a blind evaluator.
ResultsNo statistically significant differences were found in the social functioning variable between the two treatment arms. Intragroup differences are observed in other secondary variables studied (social cognition) 16 weeks after starting the interventions.
ConclusionsSocialMIND® has not been shown to be more effective than a PMI in improving social functioning at 16 weeks after starting the intervention in people who have suffered a first psychotic episode in the five years prior to being included in the study.
Disclosure of InterestNone Declared
Meta-analysis of the variability in the individual response to pharmacological treatments for mania in bipolar disorder
- G. Anmella, M. De Prisco, V. Oliva, M. Sanabra, L. Fortea, M. Ortuño, G. Fico, A. Murru, E. Vieta, D. Hidalgo-Mazzei, A. Solanes, J. Radua
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S84
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many studies have investigated whether there exist predictors of good response to antimanic drugs in bipolar disorder (BD). However, these factors predict response or only indicate benign illness course.
ObjectivesTo shed some light on the topic, we tested whether the response to antimanic drugs showed any variability beyond that expected by the effects of illness course and placebo.
MethodsWe included all double-blind, placebo-controlled RCTs of oral pharmacotherapies targeting adult patients with acute bipolar mania from 1991 to 2020. The primary outcome was the variance of the improvement in manic symptoms in treated individuals compared to placebo. The effect size was the log variability ratio (logVR). We performed a random-effects meta-analysis, including assessments of heterogeneity, sensitivity/cumulative/subgroup analyses, and meta-regression.
Results42 RCTs (46 comparisons) from a total of 8,438 BD patients with acute mania (53.7% male, mean age=39.3; 5,563 treatment/2,875 control groups) were included in the analysis. Individuals in active treatment groups did not show variability in the response beyond that observed in individuals under placebo (VR=1; 95% C.I.=0.97,1.03; p-value=0.97). No heterogeneity was detected between the studies (I2=0%; tau2=0%; Q=29.21; df=45; p-value=0.97). Results were similar in the leave-one-out/cumulative/subgroup analyses. Meta-regression did not show influences by age, sample size, sex, severity of manic symptoms at baseline, or clinical features (rapid cycling, mixed or psychotic features).
ConclusionsThis meta-analysis shows no evidence of differences in the individual response to treatments. These findings suggest that the average treatment effect is a reasonable assumption for the individual BD patient with acute mania. The presented article adds evidence to the equivalent results in schizophrenia-spectrum disorders, clinical high-risk state for psychosis, and major depressive disorder, not supporting classification in responders vs. non-responders. However, these findings should be balanced with results from other fields supporting such classification.
Disclosure of InterestNone Declared
Is emotion dysregulation correlated to depressive and manic symptoms of bipolar disorder? Results from a systematic review and network meta-analysis
- V. Oliva, M. De Prisco, G. Fico, A. Murru, M. Fornaro, A. Serretti, J. Radua, E. Vieta
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S275-S276
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion dysregulation (ED) is a multidimensional construct involving the lack of awareness, understanding and acceptance of emotions, a reduced access to adaptive and appropriate strategies to modulate the intensity or duration of emotional responses, and the inability to control behaviors in accordance with desired goals when experiencing negative emotions. ED is outlined in the general population and several psychiatric disorders, including bipolar disorder (BD), and influences its clinical course and management, quality of life, and daily social functioning.
ObjectivesThe objective of this systematic review was to examine the correlations between maladaptive (i.e., positive and negative rumination, negative focus, risk taking behaviors, suppression, and dampening) and adaptive (i.e., cognitive reframing, adaptive coping, and acceptance) strategies of emotion regulation (ER) and depressive and manic symptoms of BD.
MethodsWe searched the literature from inception to April 12, 2022, and included studies focusing on ER/ED assessed with a validated scale. We conducted multiple pairwise meta-analyses for correlations between ED dimension (or overall ED) and the measures of depressive and manic symptoms of BD, and separate Bayesian network meta-analyses to examine which aspects of emotion regulation were most closely associated with depressive and manic symptoms of BD. The Pearson’s r coefficients were adjusted using sample-size weights and Fisher’s r-to-z transformed was conducted.
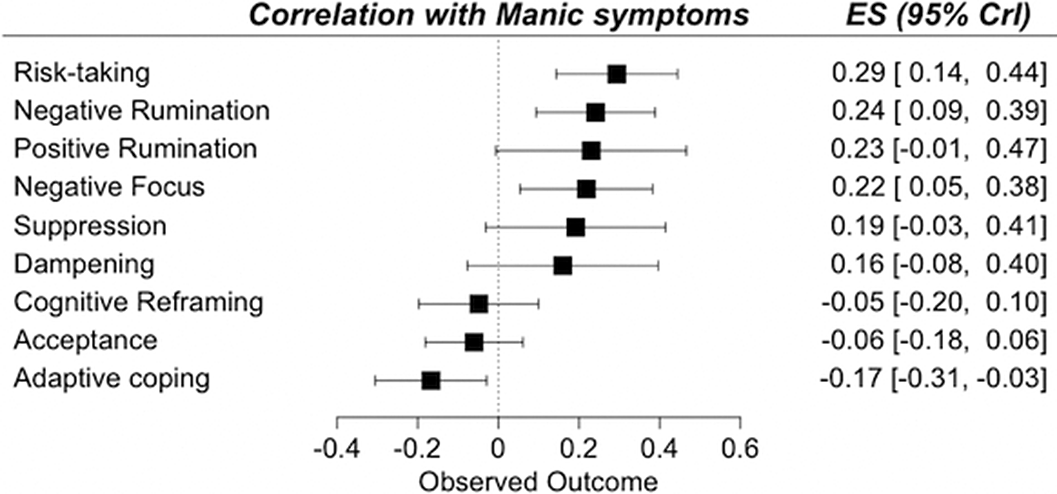
ResultsA total of 13,826 records was identified and, after duplicate removal and title/abstract evaluation, 442 were explored at the full text. Sixteen studies were finally included. Results from pairwise meta-analyses are shown in Figure 1, results from network meta-analyses in Figure 2 and 3. Both depressive and manic BD symptomatology were found to be related to maladaptive ER strategies, with the only difference of positive rumination, associated only to manic symptoms. Negative rumination and risk-taking behaviors were the strategies more correlated to both manic and depressive symptoms, as confirmed by both pairwise metanalyses and network metanalyses. On the other hand, depressive symptomatology appeared more correlated with decreased adaptive strategies than manic symptomatology.
Image:
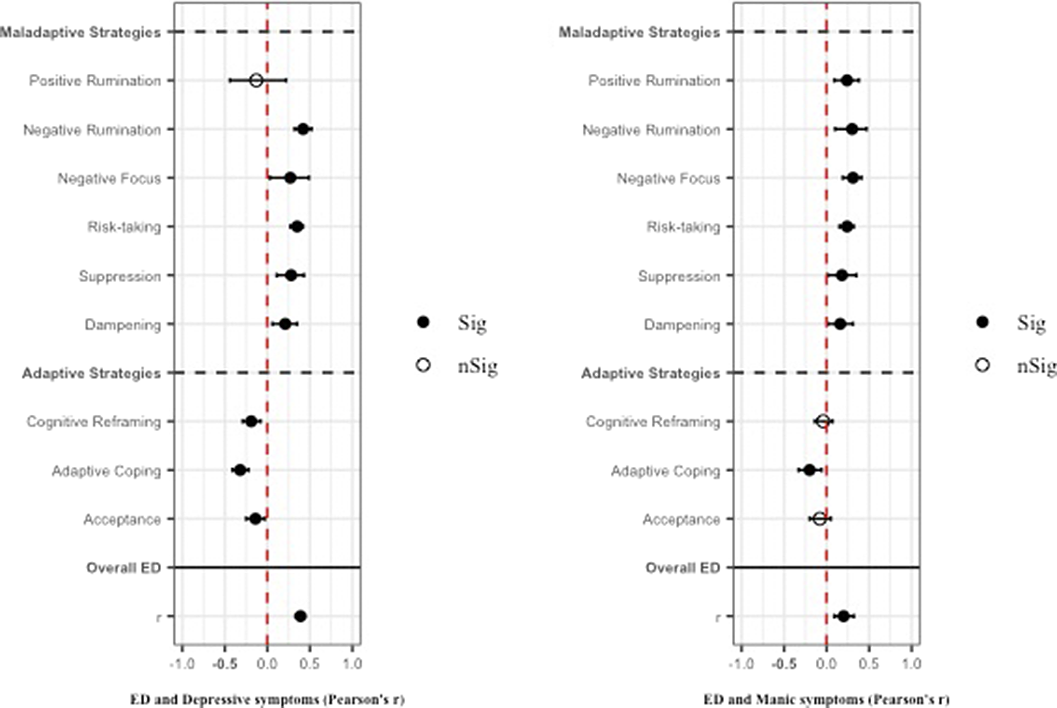
Image 2:
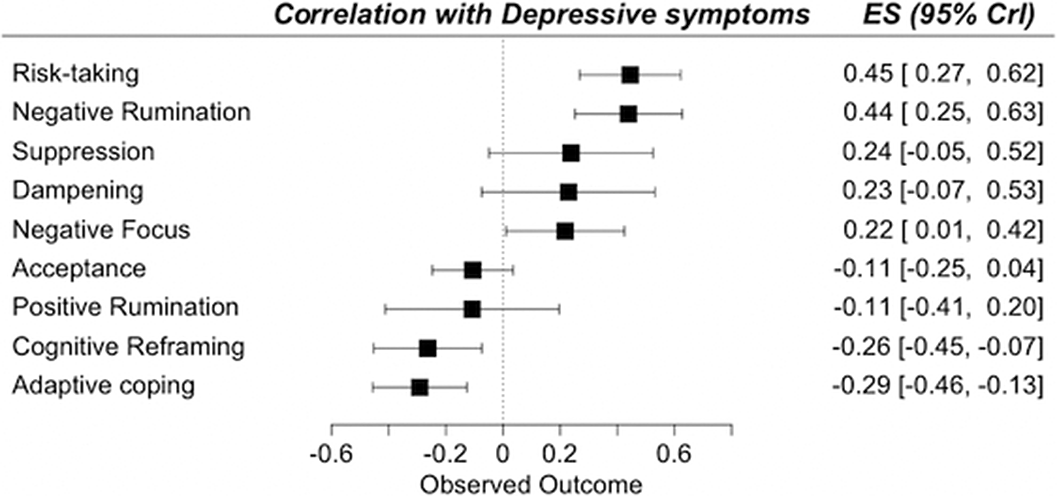
Image 3:
 Conclusions
ConclusionsED has a significant correlation with BD symptomatology, therefore it should be explicitly considered during clinical assessment, diagnosis, and intervention on BD, and specific treatments should be implemented. More studies, and with longitudinal design, are needed to better explore these associations and their causal direction. In addition, future studies should mainly focus on the complex interactions between cognitive, social, and cultural aspects, and biological correlates to improve knowledge on a topic that is still poorly investigated.
Disclosure of InterestV. Oliva: None Declared, M. De Prisco: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda, M. Fornaro: None Declared, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris
Does bipolar disorder differ from other mental illnesses in terms of emotion dysregulation? A systematic review and meta-analysis
- M. De Prisco, V. Oliva, G. Fico, J. Radua, I. Grande, N. Roberto, G. Anmella, D. Hidalgo-Mazzei, M. Fornaro, A. de Bartolomeis, A. Serretti, E. Vieta, A. Murru
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S571-S572
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Emotion regulation (ER) is the ability to assess, monitor, or modify emotional reactions to achieve a goal (Gross. Psychological inquiry 2015; 26 1-26). When ER strategies are rigidly or maladaptively applied, emotional dysregulation (ED) can occur (Thompson. Development and psychopathology 2019; 31 805-815). ED is common in people diagnosed with bipolar disorder (BD), but it can also be described in other clinical populations given its transdiagnostic nature. Numerous aspects of ED have been described in BD (De Prisco et al. Neuroscience & Biobehavioral Reviews 2022; 104914), but it is unclear whether these manifest similarly in other conditions such as major depressive disorder (MDD) or borderline personality disorder (BPD), or whether they are specific to BD.
ObjectivesThe objective of this systematic review and meta-analysis is to examine the literature comparing BD with other psychiatric disorders in terms of ED, focusing on those studies using validated clinical tools.
MethodsA systematic search from inception to April 28th, 2022, was conducted exploring the PubMed/MEDLINE,EMBASE, Scopus, and PsycINFO databases. Those studies providing quantitative data on ED in people diagnosed with BD and compared with clinical groups were eligible for inclusion. No restriction about age, sample size, or language were applied. Random effect meta-analyses were conducted, and effect sizes were calculated as standardized mean differences (SMD).
ResultsA total of 3,239 records was identified and, after duplicate removal and title/abstract evaluation, 112 were explored at the full text. Twenty-nine studies were finally included, and it was possible to perform a meta-analysis with twenty-two (145 comparisons) of them. Only studies comparing BD with MDD, and BPD provided sufficient data to perform a meta-analysis. People with BD did not differ from people with MDD in most of the comparisons considered. However, BD patients presented higher positive rumination (two comparisons: SMD=0.46; CI=0.27, 0.64; p=8.5e-07; I2=0%; and SMD=0.34; CI=0.15, 0.52; p=2.7e-04; I2=0%) and risk-taking behaviors (SMD=0.48; CI=0.27, 0.69; p=8.11e-06; I2=0%). In contrast, people with BPD displayed an overall higher degree of ED (SMD=-1.22; CI=-1.94, -0.5; p=9.1e-04; I2= 90.7) and used fewer adaptive ER strategies. Additionally, higher levels of self-blaming (SMD=-0.80; CI=-1.11, -0.50; p=2.68e-07; I2=0) and impulsive behavior (SMD=-0.76; CI=-0.89, -0.63; p=5.4e-29; I2=0) were observed.
Image:
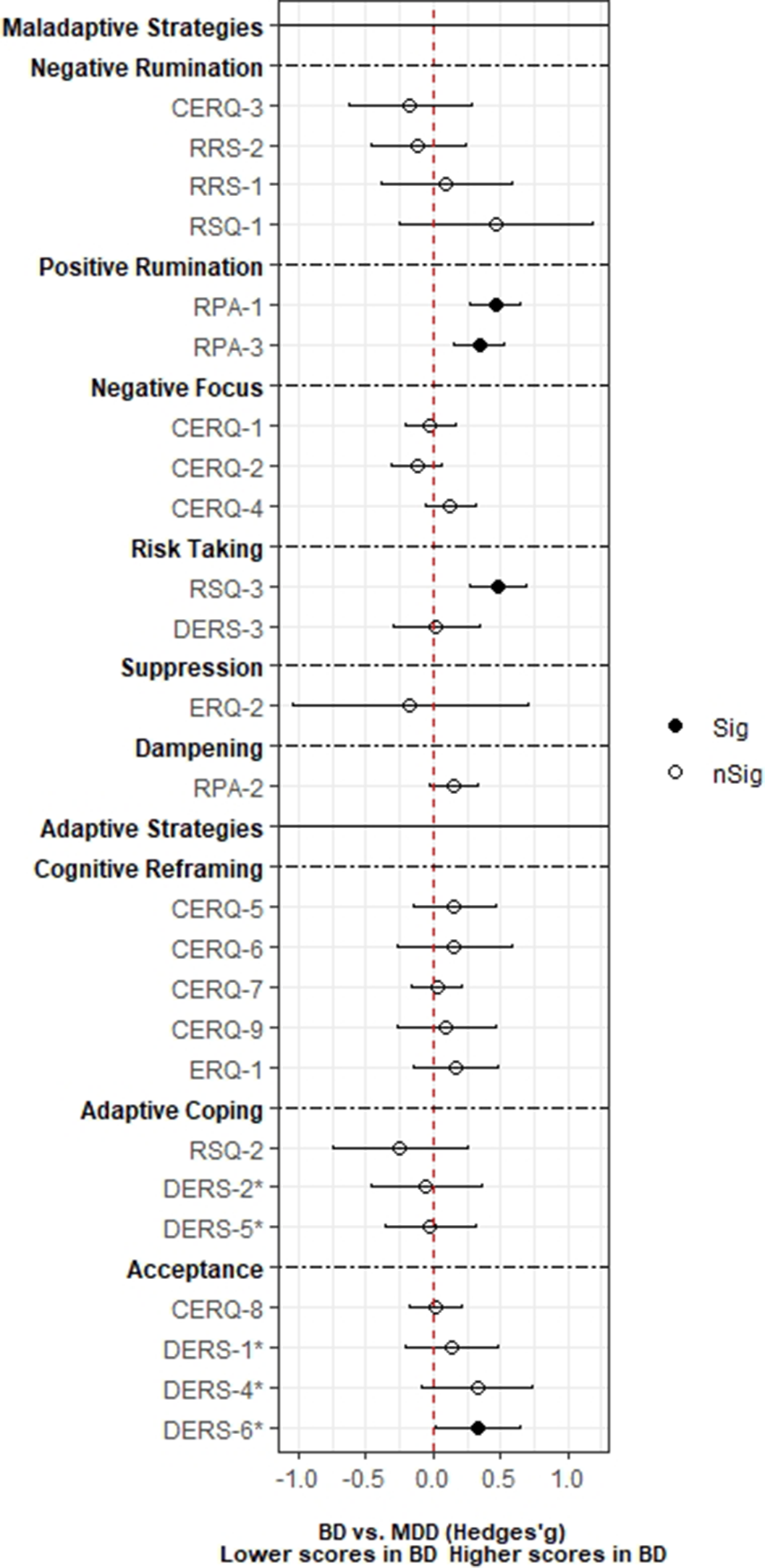
Image 2:
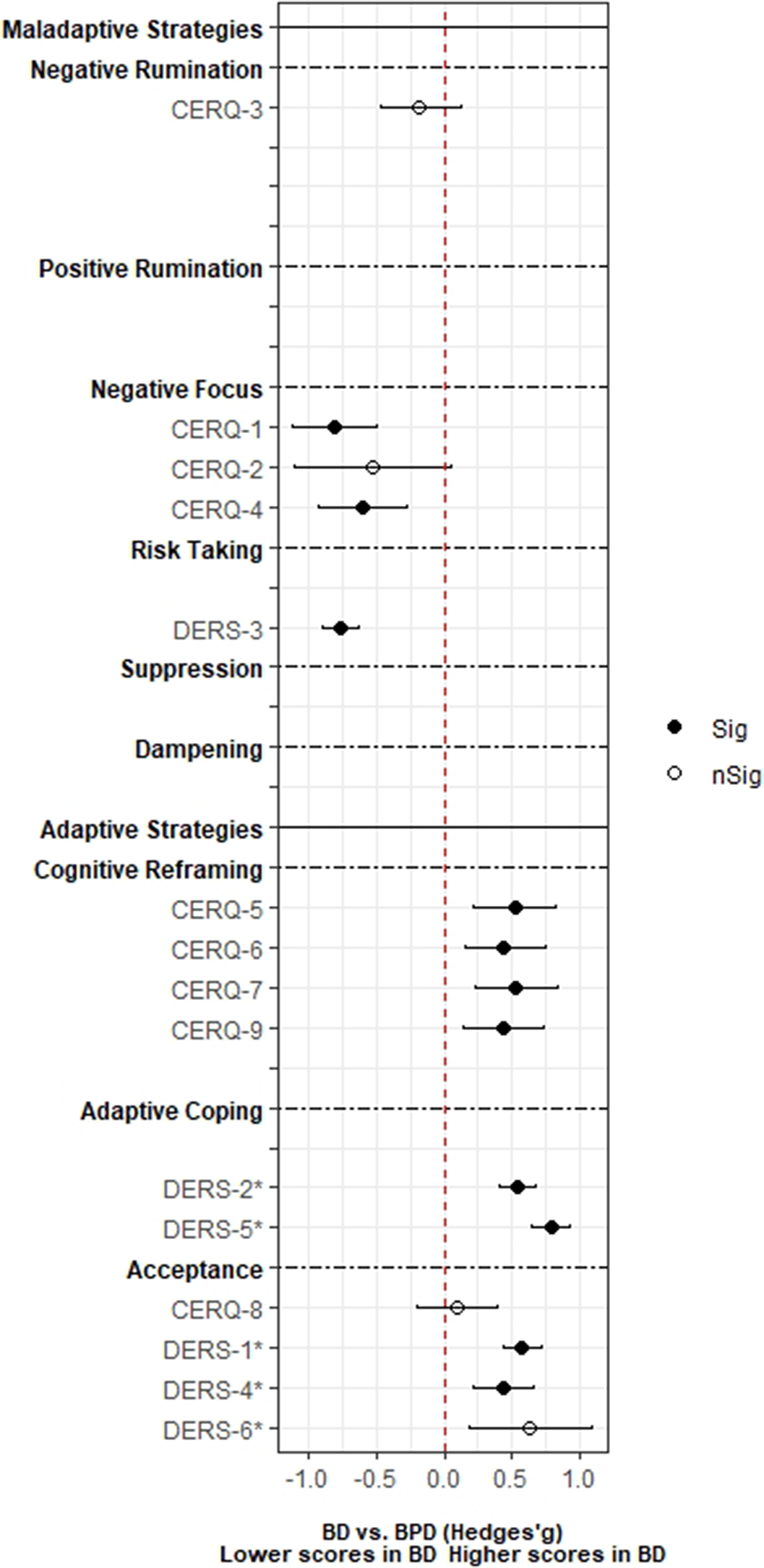 Conclusions
ConclusionsED is a trans-diagnostic construct that spans a continuum of different psychiatric disorders. Outlining the specific clinical features of one disorder versus another may help future research to increase our knowledge of these issues and develop new treatment strategies to reduce the clinical burden of these patients.
Disclosure of InterestM. De Prisco: None Declared, V. Oliva: None Declared, G. Fico Grant / Research support from: “La Caixa” Foundation (ID 100010434 - fellowship code LCF/BQ/DR21/11880019), Consultant of: Angelini, Janssen-Cilag and Lundbeck, J. Radua Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00394, CPII19/00009) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER) and the Instituto de Salud Carlos III, I. Grande Grant / Research support from: Spanish Ministry of Science and Innovation (MCIN) (PI19/00954) integrated into the Plan Nacional de I+D+I and cofinanced by the ISCIII-Subdirección General de Evaluación y el Fondos Europeos de la Unión Europea (FEDER, FSE, Next Generation EU/Plan de Recuperación Transformación y Resiliencia_PRTR ); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); and the the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), CERCA Programme / Generalitat de Catalunya as well as the Fundació Clínic per la Recerca Biomèdica (Pons Bartran 2022-FRCB_PB1_2022), Consultant of: ADAMED, Angelini, Casen Recordati, Ferrer, Janssen Cilag, and Lundbeck, Lundbeck-Otsuka, Luye, SEI Healthcare, N. Roberto: None Declared, G. Anmella Grant / Research support from: Rio Hortega 2021 grant (CM21/00017) from the Spanish Ministry of Health financed by the Instituto de Salud Carlos III (ISCIII) and co-financed by the Fondo Social Europeo Plus (FSE+), Consultant of: Janssen-Cilag, Lundbeck, Lundbeck/Otsuka, and Angelini, D. Hidalgo-Mazzei Grant / Research support from: Juan Rodés JR18/00021 granted by the Instituto de Salud Carlos III (ISCIII), M. Fornaro: None Declared, A. de Bartolomeis Consultant of: Janssen, Lundbeck, and Otsuka and lecture fees for educational meeting from Chiesi, Lundbeck, Roche, Sunovion, Vitria, Recordati, Angelini and Takeda; he has served on advisory boards for Eli Lilly, Jansen, Lundbeck, Otsuka, Roche, and Takeda, Chiesi, Recordati, Angelini, Vitria, A. Serretti Consultant of: Abbott, Abbvie, Angelini, AstraZeneca, Clinical Data, Boehringer, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Innovapharma, Italfarmaco, Janssen, Lundbeck, Naurex, Pfizer, Polifarma, Sanofi, Servier, and Taliaz, E. Vieta Grant / Research support from: Spanish Ministry of Science and Innovation (PI18/00805, PI21/00787) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER); the Instituto de Salud Carlos III; the CIBER of Mental Health (CIBERSAM); the Secretaria d’Universitats i Recerca del Departament d’Economia i Coneixement (2017 SGR 1365), the CERCA Programme, and the Departament de Salut de la Generalitat de Catalunya for the PERIS grant SLT006/17/00357. Thanks the support of the European Union Horizon 2020 research and innovation program (EU.3.1.1. Understanding health, wellbeing and disease: Grant No 754907 and EU.3.1.3. Treating and managing disease: Grant No 945151), Consultant of: AB-Biotics, AbbVie, Angelini, Biogen, Boehringer-Ingelheim, Celon Pharma, Dainippon Sumitomo Pharma, Ethypharm, Ferrer, Gedeon Richter, GH Research, Glaxo-Smith Kline, Janssen, Lundbeck, Medincell, Novartis, Orion Corporation, Organon, Otsuka, Rovi, Sage, Sanofi-Aventis, Sunovion, Takeda, and Viatris, A. Murru Grant / Research support from: Spanish Ministry of Science and Innovation (PI19/00672) integrated into the Plan Nacional de I+D+I and co-financed by the ISCIII-Subdirección General de Evaluación and the Fondo Europeo de Desarrollo Regional (FEDER), Consultant of: Angelini, Idorsia, Lundbeck, Pfizer, Takeda
Superior mesenteric artery syndrome: when vomiting are not voluntary
- M. A. Morillas Romerosa, A. Oliva Lozano, P. Herrero Ortega, J. Garde Gonzalez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S851
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Superior mesenteric artery syndrome is a gastro-vascular disorder in which the third and final portion of the duodenum is compressed between the abdominal aorta and the overlying superior mesenteric artery. This rare, potentially life-threatening syndrome is typically caused by an angle of 6°–25° between the abdominal aorta and the superior mesenteric artery, in comparison to the normal range of 38°–56°, due to a lack of retroperitoneal and visceral fat (mesenteric fat). In addition, the aortomesenteric distance is 2–8 millimeters, as opposed to the typical 10–20. However, a narrow superior mesenteric artery angle alone is not enough to make a diagnosis with no symptoms.
Symptoms are fullness and epigastric tightness after meals, nausea and vomiting (often bilious) and pain in the middle of the abdomen that improves with the prone or knees flexed to the chest. The diagnosis is supported by imaging tests (esophagogastroduodenal transit or CT) showing dilation and stasis proximal to AMS in the third duodenal portion.
Relief from vomiting with feeding through a enteral probe placed beyond the obstruction to the proximal jejunum supports diagnosis.
Precipitating factors should be corrected first, whenever possible. Acute symptoms can be resolved with gastric decompression and intravenous fluids. Therefore, surgical correction should only be done in well-studied patients with chronic recurrent episodes of AMS syndrome. The most recommended surgical technique is a laparoscopic proximal duodenojejunostomy
ObjectivesTo describe a case of superior mesenteric artery syndrome and review in literature the organic complications and associated psychopathology of this disorder
MethodsClinical case report and brief review of literatura
Results17-year-old woman with a diagnosis of anorexia nervosa. Admitted for behavioral disorder, repeated self-harm and low mood. Presents a BMI of 16.6. Irregular rules. Progressive diet is started to which nutritional supplements are added with good initial tolerance. It presents a loss of 2kg and begins with nausea, vomiting and postprandial epigastralgia. Oral panendoscopy and abdominal ultrasound are performed showing possible mesenteric aortic clamp so naso-jejunal probe and exclusive enteral feeding is prescribed. She received enteral jejunal nutrition progressively with feedback syndrome prophylaxis that included parenteral vitamin B1. After a few days, oral supplementation began. He remained hemodynamically stable, with no signs of heart failure. It gained 3kg of weight up to 43.2kg, starting before discharge from the hospital successfully oral tolerance.
ConclusionsSuperior mesenteric artery syndrome is a serious complication in anorexia nervosa with a low incidence and an estimated mortality of 33%. A multidisplinar approach that addresses both the medical and psychological needs of these patients throughout their hospital stay is necessary.
Disclosure of InterestNone Declared
“Social functioning and use of rehabilitation resources in a group of people who experienced a first episode of psychosis and participated in a psychotherapeutic group program versus a control group”
- A. Oliva Lozano, J. Garde Gonzalez, P. Herrero Ortega, A. Muñoz-Sanjosé, Á. Palao-Tarrero, M. P. Vidal-Villegas, R. Mediavilla, P. Tarín Garrón, J. M. Pastor-Haro, Á. De Diego Gómez-Cornejo, M. F. Bravo-Ortiz, O. B. O. A.-M. Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S185
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorders have a huge impact on social functioning, which is the ability to stablish and maintain social activities such as interpersonal relationships and self-care activities of daily living. Research data support that the early intervention in people who have experienced a first episode of psychosis (FEP) -based on a multidisciplinary treatment including both psychopharmacological and psychosocial treatments-, has a relevant role in a favorable evolution. AGES-Mind study is based on manualized psychotherapeutic interventions for people with first-psychosis episodes.
ObjectivesTo describe the use of rehabilitation resources and social functioning in a group of people with FEP who were included in a psychotherapeutic group program versus a control group, at 12 and 24 months since the beginning of the intervention.
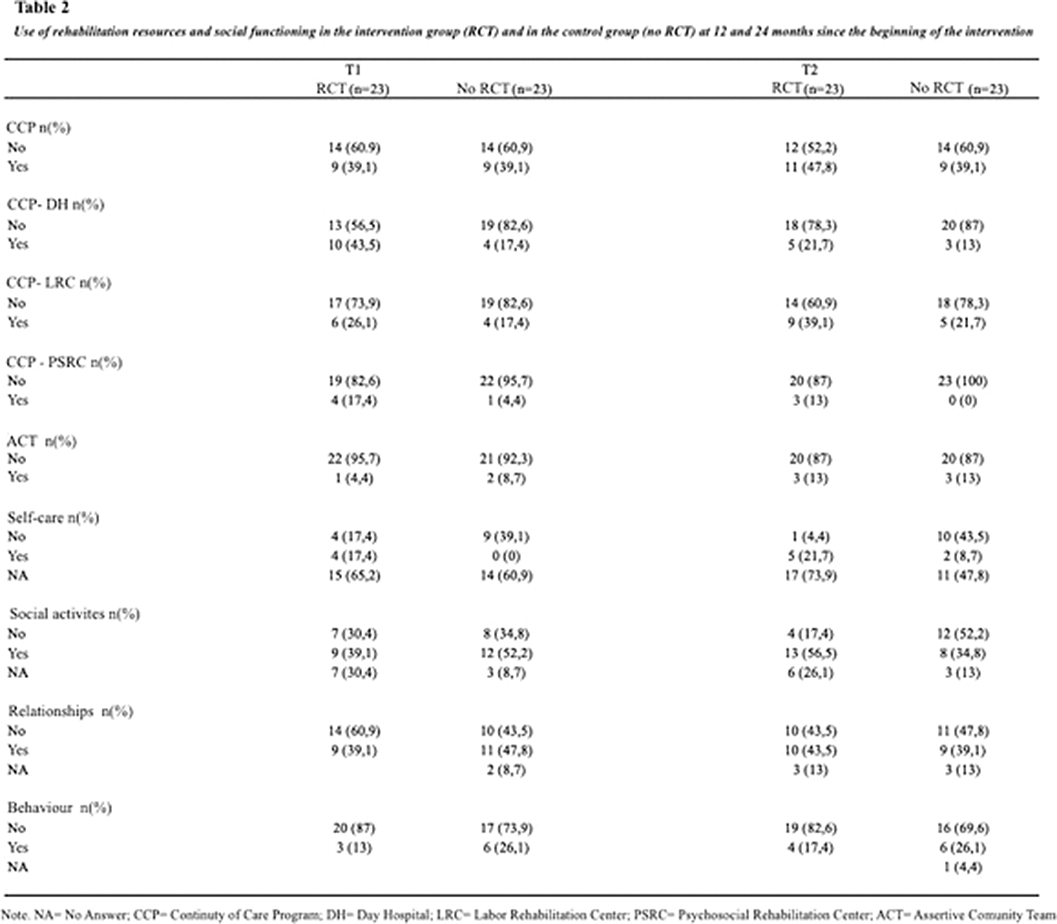
MethodsLongitudinal, analytical, observational, retrospective study on a cohort of 46 patients with first-episode psychosis within the last 5 years. 23 patients received group psychotherapy in the context of the AGES-Mind study and they were compared with 23 control patients who did not receive a group intervention (treatment as usual). Controls were matched by age, gender and time elapsed since the first episode of psychosis with those exposed to the intervention. Sociodemographic data, social functioning (self-care, social activities, social relationships, and behavior) and use of rehabilitation resources outcome variables were assessed.
ResultsSignificant differences were found regarding participation in social activities in the intervention group versus control group at 24 months. No significant differences were found in other dimensions of social functioning or in the use of rehabilitation resources.
Image:
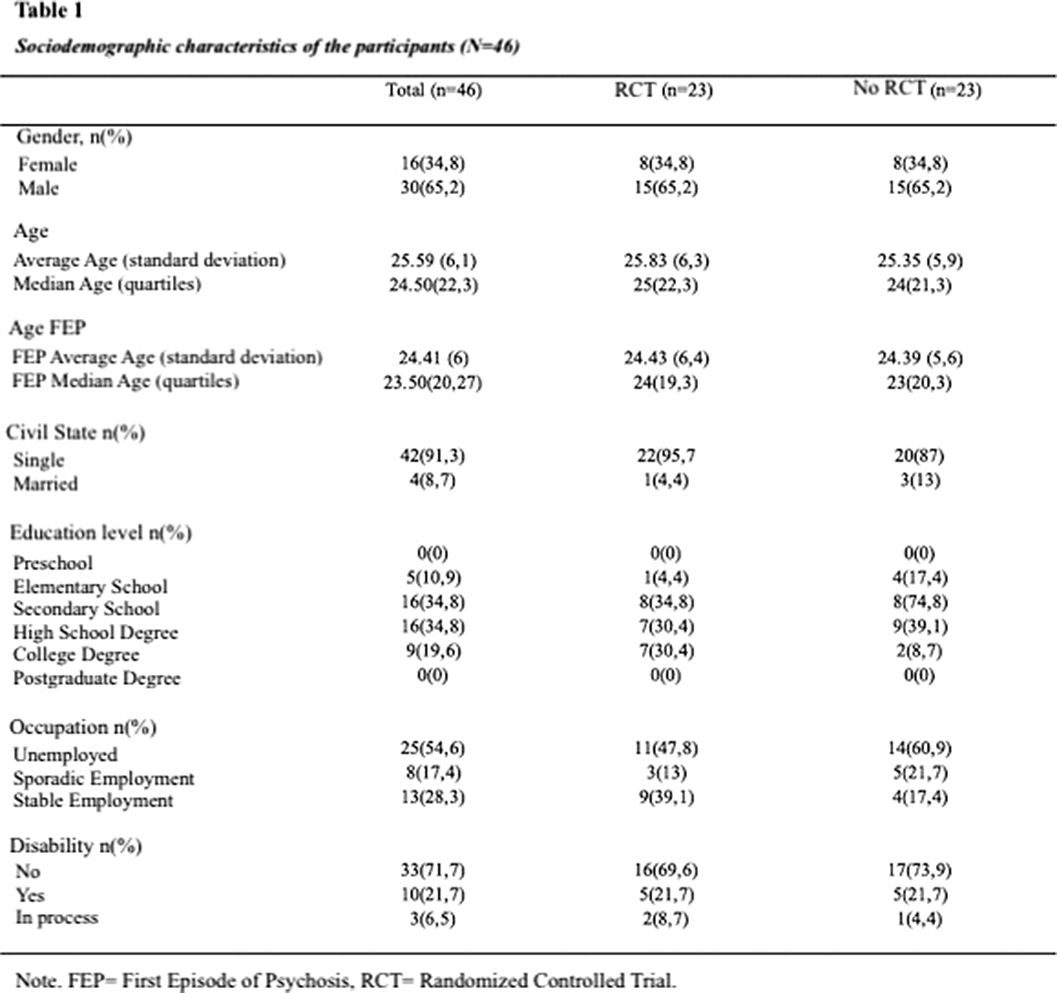
Image 2:
 Conclusions
ConclusionsFurther studies with larger sample sizes are needed in order to determine if the participation in group therapy leads to an improvement in social functioning and use of rehabilitation resources for people who have experienced a first episode of psychosis.
Disclosure of InterestNone Declared
“Unspecified organic personality and behavioral disorder due to brain damage from HHV-6 encephalitis in child. case report and literature review”
- A. Oliva Lozano, M. A. Morillas Romerosa, P. Herrero Ortega, J. Garde Gonzalez, B. Orgaz Álvarez, J. Curto Ramos, M. Alcamí Pertejo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S143-S144
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present a case of a 15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis.
ObjectivesTo describe a case of an Unspecified Organic Personality and Behavioral Disorder secondary to brain damage from Human Herpes Virus-6 (HHV-6) Encephalitis in an 11 year-old childand to review recent literature, in order to improve clinical practice.
MethodsClinical case report and brief review of literature. A bibliographic research was made in the database PubMed, using the terms “Viral Encephalitis” AND “Neuropsychiatric symptoms”; “Viral Encephalitis” AND “Behavioral Disorder”; “Long-Term Neurological Morbidity” AND “Viral Encephalitis”.
Results15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis, secondary to immunosupression in the context of haematopoietic progenitor transplantation (HPT) at 11 years old. MRI showed supratentorial ventriculomegaly, atrophic changes in encephalon and right hippocampus with subcortical retraction secondary to previous encephalitis. Clinically, main changes appeared in behavior, presenting a serious frontal syndrome with high disinhibition, what implied severe social and academic difficulties. During the outpatient follow-up, the behavioural disorder is being pharmacologically treated with Risperidone 1,5mg per day with a partially favorable evolution. The patient presented intolerance to olanzapine, with an episode of low level of conciuosness after taking it.
Bibliographic research results indicate that the gold standard treatment for behavioral disturbances are antipsychotics. Risperdidone is proven save for treatment in children. Results point out also the importance of an early multidisciplinar intervention, involving family training, rehabilitation resources and curricular adaptations.
Image:
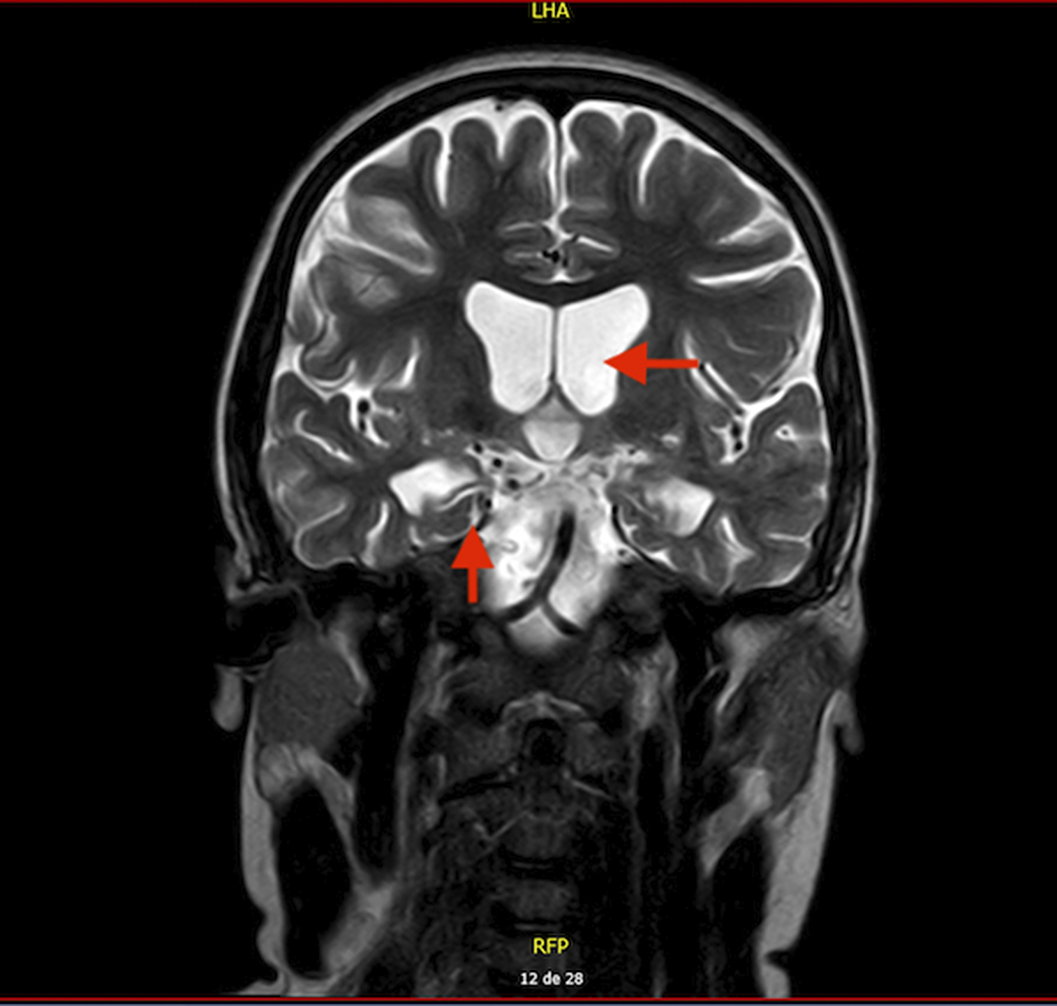
Image 2:
 Conclusions
ConclusionsViral encephalitis may have serious neuropsychiatric consequences, especially during childhood while the brain development is not finished. When the neurological damage affects the frontal lobes of the brain, behavioural and personality disturbances are expected and an early multidisciplinar intervention should be considered. Antypsichotics are the gold standard pharmacological treatment for behavioural disturbances. During the scholar period, special curricular adaptations should be done in order to reduce study-related stress.
Disclosure of InterestNone Declared
Sociodemographic and clinical characteristics of the population with a first psychotic episode attended in the mental health services of area 5 of Madrid (Spain)
- J. Garde González, P. Herrero Ortega, A. Oliva Lozano, I. I. Louzao Rojas, M. P. Vidal-Villegas, A. Muñoz-Sanjosé, M. P. Sánchez-Castro, G. Lahera, S. Sánchez Quílez, M. F. Bravo-Ortiz, O. B. O. A.-M. Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S443
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Risk of functional impairment and progression to chronic illness in people with a first episode of psychosis (FEP) has motivated early intervention programs, showing promising results. Defining the characteristics of people with FEP at local level enables the clinicians to adjust interventional models to the reality of the population. The area 5 of Madrid (Spain) is referred to La Paz University Hospital and it serves a catchment area of roughly 527,000 people.
ObjectivesWe aim to identify sociodemographic and clinical characteristics of patients in the area 5 of Madrid (Spain) who meet the criteria of FEP.
MethodsA descriptive retrospective study including 179 people (age range 18-40 years) who were attended in mental health services of La Paz University Hospital (area 5 of Madrid, Spain), between January 2019 and May 2020, having suffered a psychotic episode in the last five years.
ResultsThe average age of people with FEP was 29.32 years, with a higher proportion of men (62%). The mean duration of untreated psychosis (DUP) was 3.64 months and 47% of patients consume cannabis. We found disparities in DUP among the different districts in the area and we also observed differences depending on the district for inclusion in rehabilitation programs or psychotherapy. The following averages were obtained for the aggregate sample: 1.01 hospitalization/year, 1.42 emergency room visits/year, 1.81 years of illness and a mean dosage equivalent to olanzapine 6.75 mg/day. The incidence of psychosis in our area has been 7.01 cases per 100000 inhabitants/year.
ConclusionsThe incidence of psychosis has been as expected according to data recorded at previous studies in Spain. The results obtained in our sample have included a lower DUP and a higher use of cannabis than those described in the literature. We have also found differences when observing the inclusion of patients in different treatments (psychotherapy, rehabilitation), which may be related to the differences in the DUP by districts. Further exploration in this field is needed to draw causal conclusions.
Disclosure of InterestNone Declared
Non-schizophrenic psychotic disorders: Cycloid psychosis. Case report and literature review
- P. Herrero Ortega, J. Garde González, M. A. Morillas Romerosa, A. Oliva Lozano, J. Curto Ramos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S636
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cycloid psychosis is a clinical entity with defining traits which emerged from the Wernicke-Kleist-Leonhard school of psychiatry and has a long history in Europe. Leonhard distinguished three clinical forms: anxiety-happiness, confusion and motility psychosis. It is a condition with high clinical heterogeneity and favorable prognosis.
ObjectivesTo describe a case of cycloid psychosis and review in literature the heterogeneity of this phenomena and its clinical management.
MethodsClinical case report and brief review of literature.
Results57-year old male with previous diagnosis of paranoid schizophrenia and severe congenital hearing loss. Preserved autonomy and adequate real-life and interpersonal functioning. Along the past few years the patient has presented episodes of a significant clinical global worsening in context of mainly somatic symptoms (intestinal obstruction and volvulus) and minor stressful life events. On this occasion he appears in the emergency room with a new episode of abdominal pain and is admitted to Internal Medicine with presumptive diagnosis of intestinal volvulus. The patient gathered heterogeneous symptoms including disorientation, confusion, generalized tremor, gait disorder, profuse sweating, regressive and oppositional behaviors (refusal to eat or drink liquids) and sudden behavioral oscillations (from agitation to prostration). From the psychic point of view he showed thought blocking, mutism, significant anxiety, fear of death, delusional prejudice ideas and sensoperceptive disturbance which seemed otherwise related to previous sensorial problems. We introduced treatment with Olanzapine 30 mg and after 4 weeks, the patient suddenly showed a significant clinical improvement until the complete remission of the symptoms and restitution of his previous state. In coordination with his regular psychiatrist was proposed the controversial diagnosis of cycloid psychosis. Cycloid psychosis gather a few clinical features which differentiate it from other entities: acute onset, polymorphic symptomatology, global disturbance of psychic life, remitting and recurrent course and favorable prognosis. Regarding its clinical management no controlled studies have been conducted to this date of the treatment of this phenomena. According to literature ECT seems to be an effective treatment as well as low-doses of atypical antipsychotics. Some authors propose pharmacological maintenance treatment with mood stabilizers.
ConclusionsThe diagnosis of cycloid psychosis can be useful as well as necessary to describe certain patients with similar clinical features, recurrent course and favorable prognosis. Future studies on pharmacological approach would be useful to ensure the appropriate clinical management of these patients.
Disclosure of InterestNone Declared










