3082 results
Reduced MMN-indexed auditory change detection in a non-clinical high schizotypy sample
- Jenna N. Bissonnette, T-Jay Anderson, Lauren Ross, Ashley M. Francis, Kaitlyn Napier, N. Will Shead, Derek J. Fisher
-
- Journal:
- Personality Neuroscience / Volume 7 / 2024
- Published online by Cambridge University Press:
- 26 September 2024, e10
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Schizotypal traits include abnormalities in cognition, behavior, and interpersonal relationships that are similar, yet less severe than psychotic symptomology. It is estimated that approximately 5% of the general population displays psychotic symptoms and experiences that can be considered schizotypal in nature, but there is little research examining the neurological correlates of these traits. The mismatch negativity (MMN) event-related potential is an objective measure of auditory change detection derived from electroencephalography. The current study contributes to the limited body of evidence examining the neurobiological underpinnings of schizotypy in a non-clinical sample using the MMN. Participants were recruited from the general population and divided into high and low-schizotypy groups for comparison. Individuals with high schizotypal traits displayed reduced MMN amplitudes in response to frequency and location deviants, and longer MMN latencies in response to location deviants. Specific sub-traits of schizotypy were uniquely related to frequency and location amplitudes, suggesting the previously reported inconsistencies in the literature may be due to diverse samples and differing deviant tone types. Finally, impulsivity and sensation-seeking likely contributed to the slower processing seen in location deviance detection. Ultimately, the current results provide evidence that the neurobiological abnormalities seen in clinical populations of schizotypal personality disorder and psychosis also extend to non-clinical populations.
Magnetite nanoparticles are metastable biogeobatteries in consecutive redox cycles driven by microbial Fe oxidation and reduction
- Part of
- T. Bayer, N. Jakus, A. Kappler, J. M. Byrne
-
- Journal:
- Geo-Bio Interfaces / Volume 1 / 2024
- Published online by Cambridge University Press:
- 25 September 2024, e3
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Iron (Fe) minerals play a crucial role in biogeochemical cycles due to their ubiquity in nature, high adsorption capacity and redox activity towards many other elements. Mixed-valent Fe minerals are unique since they contain Fe(II) and Fe(III). For example, magnetite (Fe(II)Fe(III)2O4) nanoparticles (MNPs) can affect the availability and mobility of nutrients and contaminants. This is due to the high surface area to volume ratio and the presence of Fe(II) and Fe(III), allowing redox transformation of (in‑)organic contaminants. Recent studies have shown that magnetite can serve as an electron source and sink for Fe(II)-oxidizing and Fe(III)-reducing microorganisms, storing and releasing electrons; thus, it functions as a biogeobattery. However, the ability of MNPs to act as biogeobatteries over consecutive redox cycles and the consequences for mineral integrity and identity remain unknown. Here, we show MNPs working as biogeobatteries in two consecutive redox cycles over 41 days. MNPs were first oxidized by the autotrophic nitrate-reducing Fe(II)-oxidizing culture KS and subsequently reduced by the Fe(III)-reducing Geobacter sulfurreducens. In addition to reduced magnetite, we identified the Fe(II) mineral vivianite after reductions, suggesting partial reductive dissolution of MNPs and re-crystallization of Fe2+ with phosphate from the growth medium. Measurements of the Fe(II)/Fe(III) ratio revealed microbial oxidation and reduction for both the first redox cycle (oxidation: 0.29±0.014, reduction: 0.75±0.023) and the second redox cycle (oxidation: 0.30±0.015, reduction: 1.64±0.10). Relative changes in magnetic susceptibility (∆κ in %) revealed greater changes for the second oxidation (–8.7±1.99%) than the first (–3.9±0.19%) but more minor changes for the second reduction (+14.29±0.39%) compared to the first (+25.42±1.31%). Our results suggest that MNPs served as biogeobatteries but became less stable over time, which has significant consequences for associated contaminants, nutrients and bioavailability for Fe-metabolizing microorganisms.
Exploring the associations of food and financial insecurity and food assistance with breastfeeding practices among first-time mothers
- Junia N de Brito, Jessica K Friedman, Sydney T Johnson, Jerica M Berge, Susan M Mason
-
- Journal:
- Public Health Nutrition / Volume 27 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 06 September 2024, e160
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
Social determinants of health (SDoH), such as food and financial insecurity and food assistance, are potentially modifiable factors that may influence breastfeeding initiation and duration. Knowledge gaps exist regarding the relationship between these SDoH and infant feeding practices. We explored the relationships of food and financial insecurity and food assistance with the continuation of breastfeeding at four months postpartum among mothers and whether race and ethnicity modified these associations.
Design:Mothers retrospectively reported food and financial insecurity and receipt of food assistance (e.g. Women, Infants and Children and Supplemental Nutrition Assistance Program) during pregnancy with their first child and infant feeding practices (exclusive/mostly breastfeeding v. exclusive/mostly formula feeding) following the birth of their first child. Sociodemographic-adjusted modified Poisson regressions estimated prevalence ratios and 95 % CI.
Setting:Minneapolis-St. Paul, Minnesota.
Participants:Mothers who participated in the Life-course Experiences And Pregnancy study (LEAP) (n 486).
Results:Ten percent of mothers reported food insecurity, 43 % financial insecurity and 22 % food assistance during their pregnancies. At four months postpartum, 63 % exclusively/mostly breastfed and 37 % exclusively/mostly formula-fed. We found a lower adjusted prevalence of breastfeeding at four months postpartum for mothers who reported experiencing food insecurity (0·65; 0·43–0·98) and receiving food assistance (0·66; 0·94–0·88) relative to those who did not. For financial insecurity (aPR 0·92; 0·78, 1·08), adjusted estimates showed little evidence of an association.
Conclusions:We found a lower level of breastfeeding among mothers experiencing food insecurity and using food assistance. Resources to support longer breastfeeding duration for mothers are needed. Moreover, facilitators, barriers and mechanisms of breastfeeding initiation and duration must be identified.
Liquor for breakfast, fighting against alcohol consumption
- N. Navarro Barriga, P. Marqués Cabezas, M. B. Arribas Simón, B. Rodríguez Rodríguez, C. Alario Ruiz, G. Guerra Valera, A. Aparicio Parras, M. J. Mateos Sexmero, M. Fernández Lozano, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, M. P. Pando Fernández, M. D. L. A. Guillén Soto, T. Jimenez Aparicio, M. D. C. Vallecillo Adame, C. De Andrés Lobo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S408-S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful consumption of alcohol is known for how tortuous its management can be in mental health, encouraging introspection of it as a serious problem is perhaps the main key to starting to battle against its damaging influence on the development of a functional and full life.
ObjectivesTo describe a clinical case showing an unpredictible complication in an alcohol detoxification process.
Methods54-year-old man, native of Cádiz, widowed for half a decade, without children. He resides with his parents in the family home. Currently unemployed for approximately a year. He has previously worked in the IT sector. As a notable somatic history, we found long-established arterial hypertension and a total hip replacement. He has been under irregular follow-up with a mental health team for anxiety-depressive symptoms in the context of grief. He goes to the emergency service brought by his family to begin the detoxification process in the hospital setting. He acknowledges ethanol consumption since he was widowed, which began when he awakes; quantities that ranged between one or up to three bottles of distilled liquor per day, generally consumption is in the home environment. A little less than a year ago, he began to isolate himself in his room and abandon his self-care, eating increasingly insufficient food intake, refusing to receive professional care to quit the habit, mainly because he did not recognize it as disruptive.
The patient was admitted to hospital with symptoms suggestive of withdrawal, making it extremely difficult to control blood pressure levels. On the third day of admission to the acute care unit, fever peaks, blood pressure levels well below normal parameters, and compromised level of consciousness began to be evident.
ResultsBlood tests were performed that, together with the clinical picture, suggested imminent septic shock, so critical care was contacted for transfer and stabilization. A germ of probable urinary etiology sensitive to a broad spectrum of antibiotics was isolated in blood cultures, and the medication of the detoxification process was progressively optimized. Once clinical stability was achieved at all levels, an inpatient cessation resource was managed, which the patient accepted and considered suitable for his complete recovery.
ConclusionsA holistic approach to the alcoholic patient is important, since serious problems of an organic nature often arise. This is why a multidisciplinary intervention is necessary, as well as a holistic approach to care, involving both classic pharmacology and assiduous long-term psychotherapeutic intervention.
Disclosure of InterestNone Declared
Narcissistic predispositions of self-harm in young women with and without depression
- O. U. Vorontsova, T. I. Medvedeva, O. M. Boyko, S. N. Enikolopov, S. O. Kuznetsova
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S657
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Diagnostic criteria for narcissistic personality disorder primarily focus on grandiosity and significance. In psychotherapeutic work, it is important to distinguish two subtypes of pathological narcissism: narcissistic grandiosity and narcissistic vulnerability. One of the manifestations of narcissistic traits is unstable or unformed self-esteem, manifested in attempts to conform to ideals. A part of modern society perceives the female body as an object that “needs to be looked at”. Self-objectification refers to a learned pattern of self-assessment of the importance of one’s body and appearance compared to other aspects of the self. Self-observation and comparison of oneself with others is one of the manifestations of self-objectification. With acts of auto aggression, the body becomes a tool or a means to solve psychological problems. In order for this to become possible, the ability to objectify your body “to look at it from the outside” plays an important role.
ObjectivesAnalysis of the relationship between non-suicidal self-injurious behavior and narcissistic personality traits in young women with depression and young women without a psychiatric diagnosis.
MethodsТhe study included 49 women divided into two groups. The first group included 24 patients with depression undergoing inpatient treatment (mean age 18.4). The second group included 25 healthy subjects (mean age 18 years). The methods: The answer to the question “Sometimes I purposely injure myself” was used as an indicator of self-harm (NSSI) (five-point Likert scale); “Ich structure test” (ISTA); “Physical Appearance Comparison Scale-Revised” (PACS-R).
ResultsIn the clinical group, a significant association of severity of NSSI with indicators of “deficit narcissism” was revealed (Spearman r=,534*). Correlations were found between the severity of NSSI and PACS-R (r=,344**). In the clinical group, there was no connection between “Comparison with others” and narcissistic traits. In a group of healthy subjects, significant associations of NSSI severity with “destructive narcissism” (,572**) and PACS-R (,576**) were revealed. In the clinical group, the severity of NSSI is associated with a more serious pathology - the lack of formation of “normal” narcissism, and in the healthy group it is more likely to be deformed narcissism. Self-objectification and comparison of oneself with others in the clinical group is not associated with manifestations of narcissistic traits, such connections are demonstrated in the group of healthy young women.
ConclusionsIt is shown that in the clinical group of depressed young women, the severity of self-harming behavior is associated with “deficit narcissism”, and in healthy young women, first of all, with “destructive narcissism” with an increased need to compare themselves with others.
Disclosure of InterestNone Declared
Sex differences in diagnostic stability in first episode psychosis after 1-year follow-up
- B. Jiménez-Fernández, A. Toll-Privat, D. Bergé-Baquero, N. V. Motta-Rojas, M. Delgado-Marí, T. Legido-Gil, L. Martínez-Sarduní, T. Legido-Gil, J. Cuevas-Esteban, A. Mané-Santacana
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S470-S471
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Diagnostic stability is a controversial issue in first episode psychosis (FEP) due to heterogenous symptoms and unclear affective symptoms. Differencing affective and non-affective psychoses is important as treatment strategies are different. Initial affective symptomatology has low specificity for predicting the subsequent diagnosis of affective psychosis. Sex has proven to be relevant for clinical and functional outcomes but it remains unclear how sex may contribute to diagnosis switch of FEP.
ObjectivesTo determine the role of sex in diagnostic stability in a sample of FEP after 1-year follow-up.
MethodsDiagnoses of FEP patients from Hospital del Mar of Barcelona were assessed at baseline and 1 year after. Univariate analyses was perfomed for all diagnoses and dichotomic variable (affective/non-affective). Logistic regression model was perfomed to know which variables predict diagnosis switch.
Results256 patients were enrolled. No differences were found at baseline between completers and non-completers (Table 1). No significant differences between men and women at baseline diagnosis were found, neither all diagnoses (p=0.274) nor the dichotomic variable affective/non-affective (p=0.829) (Table 2AB). Significant differences were found at 1-year follow-up between men and women, for all diagnoses (p=0.043) and the dichotomic variable (p=0.039). Sex was the only variable that predicted diagnosis switch (Figure 1), PANSS, CDSS, YMRS, GAF and cannabis did not.
Table 1. Baseline characteristics of participants
Completers (n=188) Non-completers (n=68) p Women (n, %) 71 (37.8) 30 (44.1) 0.111 Age (M, IQR) 24 (20-28) 22 (20-28) 0.899 Cannabis use (M, IQR) 5.5 (0-18) 7 (0-21) 0.231 DUP (M, IQR) 45 (12.5-130) 36 (11.25-115.75) 0.213 PANSS (m, sd) 44.55 (10.17) 40.93 (10.42) 0.761 CDSS (M, IQR) 2 (0-7) 3 (0-5.5) 0.199 YMRS (m, sd) 19 (9.64) 17.6 (9.15) 0.845 GAF (M, IQR) 30 (25-50) 30 (25-35) 0.114 TABLE 2A and 2B. Diagnosis comparison (n, %)
Baseline 1-year follow-up Men Women Total Men Women Total Psychosis NOS 69 (59) 39 (54.9) 108 (57.4) 28 (23.9) 10 (14.1) 38 (20.2) Schizophreniform disorder 22 (18.8) 16 (22.5) 38 (20.2) 14 (12 9 (12.7) 23 (12.2) Induced psychosis 4 (3.4) 0 (0) 4 (2.1) 15 (12.8) 4 (5.6) 19 (10.1) Affective psychosis 17 (14.5) 9 (12.7) 26 (13.8) 24 (20.5) 25 (35.2) 49 (26.1) Schizophrenia 0 (0) 0 (0) 1 (0.4) 30 (25.6) 14 (19.7) 44 (23.4) Brief psychotic disorder 5 (4.3) 7 (9.9) 12 (6.4) 6 (5.1) 8 (11.3) 14 (7.4) Baseline 1-year follow-up Men Women Total Men Women Total Affective psychosis 17 (14.5) 9 (12.7) 26 (13.8) 24 (20.5) 25 (35.2) 49 (26.1) Non-affective psychosis 100 (85.5) 62 (87.3) 162 (86.2) 93 (79.5) 46 (64.8) 139 (73.9) Image:
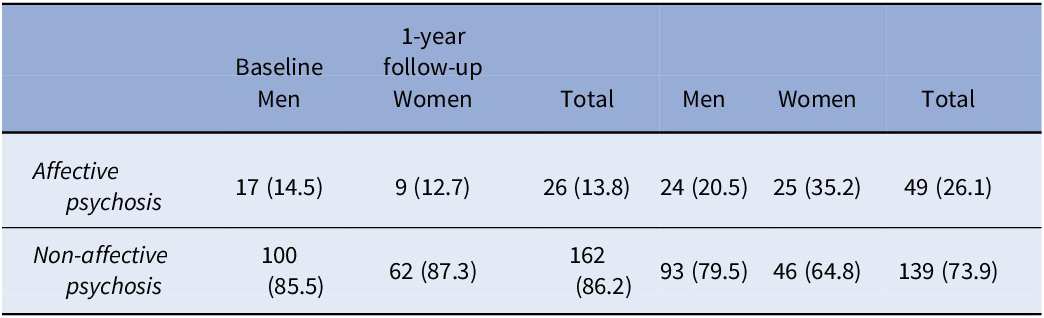 Conclusions
ConclusionsSex has proven to be the main predictor of switching initial diagnosis of FEP.
Disclosure of InterestNone Declared
The amount of drunk days and its relationships with other characteristics of alcoholic behavior of the respondents
- V. Kuzminov, I. Linskiy, O. Minko, M. Denisenko, T. Tkachenko, V. Zadorozhny, N. Malykhina, O. Minko, R. Lakinskiy, O. Vasilyeva, B. Herasymov, D. Herasymov, O. Yurchenko
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S411
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Alcohol abuse is a multifaceted problem. Its harmful effects on the individual have been more studied. Less studied is the influence of a drinking person on his microsocial environment. Having an abusing person in his space makes it interesting to study the influence of some quantitative and qualitative indicators of his alcohol consumption on the microsocial environment.
Objectives1532 people were examined during 2018-2022, who belonged to three comparison groups: patients with alcohol dependence (AD) (401 people); healthy relatives of AD patients (725 people); representatives of the general population comparable with the representatives of the first two age groups (406 people).
MethodsThe main research instruments were the questionnaire of the international research consortium “GENAHTO” (Gender, Alcohol, and Harms to Others), as well as the Alcohol Use Disorders Identification Test (AUDIT). The obtained data were processed by methods of mathematical statistics (variance, correlation and regression analysis).
ResultsAn algorithm for regression analysis in conditions of high dispersion of the initial data has been developed. Using this algorithm, it was shown that the regression dependence of the main characteristics of alcohol behavior on the frequency of DD is non-linear, while for typical and maximum doses of alcohol it is optimally described by polynomials of the second degree, and for the severity of disorders due to alcohol use (AU), the time spent on AU, as well as self-assessment of the negative impact of AU by respondents on their environment - by polynomials of the third degree. It was found that for men (on average) to reach the border of risky-dangerous AU (according to the criteria of the AUDIT test), a lower frequency of DD is sufficient than for women, which indicates a greater vulnerability of men (compared to women) to the formation of disorders due to AU.
ConclusionsIt was established that for men (on average) to reach the limit of risky and dangerous (according to the criteria of the AUDIT test), a lower frequency (2-3 times a week) is enough than for women (3-4 times a week), which once again indicates greater vulnerability of men (compared to women) to the formation of due to psychological problems and mental disorders.
Disclosure of InterestNone Declared
Neurophysiological evidence of motor preparation dysfunction to inner speech in schizophrenia
- L. K.-H. Chung, A. W. Harris, O. Griffiths, B. N. Jack, M. E. Le Pelley, K. M. Spencer, A. R. Barreiros, A. W. Harrison, N. Han, S. Libesman, D. Pearson, R. B. Elijah, S. S.-M. Chan, G. H.-C. Chong, S. H.-W. So, T. J. Whitford
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S243
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Auditory verbal hallucinations (AVHs) in schizophrenia have been suggested to arise from failure of corollary discharge mechanisms to correctly predict and suppress self-initiated inner speech. However, it is unclear whether such dysfunction is related to motor preparation of inner speech during which sensorimotor predictions are formed. The contingent negative variation (CNV) is a slow-going negative event-related potential that occurs prior to executing an action. A recent meta-analysis has revealed a large effect for CNV blunting in schizophrenia. Given that inner speech, similar to overt speech, has been shown to be preceded by a CNV, the present study tested the notion that AVHs are associated with inner speech-specific motor preparation deficits.
ObjectivesThe present study aimed to provide a useful framework for directly testing the long-held idea that AVHs may be related to inner speech-specific CNV blunting in patients with schizophrenia. This may hold promise for a reliable biomarker of AVHs.
MethodsHallucinating (n=52) and non-hallucinating (n=45) patients with schizophrenia, along with matched healthy controls (n=42), participated in a novel electroencephalographic (EEG) paradigm. In the Active condition, they were asked to imagine a single phoneme at a cue moment while, precisely at the same time, being presented with an auditory probe. In the Passive condition, they were asked to passively listen to the auditory probes. The amplitude of the CNV preceding the production of inner speech was examined.
ResultsHealthy controls showed a larger CNV amplitude (p = .002, d = .50) in the Active compared to the Passive condition, replicating previous results of a CNV preceding inner speech. However, both patient groups did not show a difference between the two conditions (p > .05). Importantly, a repeated measure ANOVA revealed a significant interaction effect (p = .007, ηp2 = .05). Follow-up contrasts showed that healthy controls exhibited a larger CNV amplitude in the Active condition than both the hallucinating (p = .013, d = .52) and non-hallucinating patients (p < .001, d = .88). No difference was found between the two patient groups (p = .320, d = .20).
ConclusionsThe results indicated that motor preparation of inner speech in schizophrenia was disrupted. While the production of inner speech resulted in a larger CNV than passive listening in healthy controls, which was indicative of the involvement of motor planning, patients exhibited markedly blunted motor preparatory activity to inner speech. This may reflect dysfunction in the formation of corollary discharges. Interestingly, the deficits did not differ between hallucinating and non-hallucinating patients. Future work is needed to elucidate the specificity of inner speech-specific motor preparation deficits with AVHs. Overall, this study provides evidence in support of atypical inner speech monitoring in schizophrenia.
Disclosure of InterestNone Declared
The SLC6A1 Mutation Schizophrenia case — A Comprehensive Case Study With iPSC Generation
- V. Mikhailova, N. Kondratyev, M. Alfimova, V. Kaleda, T. Lezheiko, M. Ublinsky, V. Ushakov, I. Lebedeva, A. Galiakberova, A. Artyuhov, E. Dashinimaev, V. Golimbet
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S764-S765
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The main finding of a large-scale collaborative study (Rees et al. Nat Neurosci 2020;23(2) 179-184), which focused on de novo mutations in schizophrenia, was the discovery of an enrichment of these mutations in the SLC6A1 gene. This gene encodes the gamma-aminobutyric acid (GABA) transporter GAT1, thereby encouraging further research into novel schizophrenia targets within the GABA pathway. However, the gene was not highlighted in recent schizophrenia genetic studies, while typically pathogenic SLC6A1 mutations result in epilepsy, motor dysfunction, autistic spectrum disorder (ASD) and developmental delay. The absence of genetic replication for SLC6A1’s involvement in schizophrenia and the differing clinical spectrum for SLC6A1 mutations led us to study in depth one of the only three original probands from the Rees et al. 2020 study.
ObjectivesIn our comprehensive case study, we delved deep into the relationship between the SLC6A1 mutation and schizophrenia.
MethodsOur subject, a patient who first presented with acute mania symptoms at age 15 and was later diagnosed with schizophrenia, carried the SLC6A1 Arg211Cys mutation. Over a detailed 25-year follow-up, we conducted an array of assessments and tests, including cognitive testing, personality assessments, EEG, and 1H-MRS.
ResultsNotably, we discovered abnormal GABA levels, potentially indicating a dysfunction in GABA reuptake, adding a new layer of complexity to our understanding. Further analysis revealed a significant correlation between the patient’s clinical picture and a polygenic background, rather than the SLC6A1 mutation. Despite having a high polygenic risk score for bipolar disorder, the dominant features of his condition were more representative of schizophrenia. Interestingly, neither the patient nor his father, who also showed a higher BP PRS, had a diagnosis of bipolar disorder. The pathogenic significance of the mutation warrants investigation in cells of neuronal origin. We generated induced pluripotent stem cells (iPSC) from the patient and his parents. This approach provides us with a platform for future investigations into the pathogenic significance of the mutation in neuronal cells. The Human Pluripotent Stem Cell Registry accession numbers of those cells are MHRCCGi001-A (patient), MHRCCGi005-A (mother) and MHRCCGi004-A (father).
ConclusionsIn the presented case the clinical picture is rather explained by the polygenic background than by the SLC6A1 Arg211Cys mutation. The study is supported by Russian Science Foundation, grant 21-15-00124 (https://rscf.ru/project/21-15-00124)
Disclosure of InterestNone Declared
A man stitches his mouth in the context of a personality disorder
- A. Monllor Lazarraga, P. Marques Cabezas, L. Rojas Vazquez, M. Rios Vaquero, G. Lorenzo Chapatte, T. Jimenez Aparicio, C. De Andres Lobo, C. Vallecillo Adame, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodriguez Rodriguez, M. Fernandez Lozano, M. A. Andreo Vidal, M. Calvo Valcarcel, M. P. Pando Fernandez, P. Martinez Gimeno, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S654-S655
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 28 year old patient will be presented. This paramilitary man was brought to the Emergency Room due to an autolytic attempt with Benzodiazepines, along with a mouth suture, in the context of a soon to be resolved problematic ankle osteosynthesis procedure. The patient claimed to be suffering pain, furthermore struggling due to the fact he could not be working due to his ankle issue. Language barrier was a problem during the interview.
ObjectivesThe objetives of this case is to try to explain the issues that may arise in patients with personality disorders in the context of an autolytic attempt
MethodsThis patient will be presented, along with systematic bibliography review of the topic.
ResultsThe following results were extracted upon the attention given to this patient which was admitted to the Psychiatric Unit.
First of all, the mouth stitches were removed, along with a petition for toxicological analysis. The results gave positive for cannabis and benzodiazepines. The patient was also brought previously this year with another autolytic attempt, this time on cocaine consumption too. Furthermore, a thorough review was made of the other autolytic attempts, including those which happened in his country of origin. The patient has hundreds of small cuts among his arms, from previews cuts made in the past. Furthermore, subcutaneous wounds were auto inflicted in the ER, with a small blade.
Among the whole interview, it was clear he had a personality disorder, with high impulsivity levels and lack of control once the situation overflows.
We also tried to understand the outcome of suturing his mouth. The patient referred his acts of impulsiveness due to his overwhelming situation of both having no job at this moment and the pain he was suffering due to his ankle procedure.
The patient was admitted to our Unit due to the high risk he could repeat this act. Upon arrival, the same day he was admitted, the patient asked if he had to stay at the unit. When explaining the following already told event, furthermore insisting in the possibility of been evaluated by the Traumatology team, he proceeded to try and hang himself with his medical-hospital clothing.
The patient was treated with antipsychotics. Along with Lormetazepam at night. At the end of the hospitalization, and after been evaluated by the Psychiatrist of this Unit, the patient was also treated with Lithium due to its effectiveness in the treatment of autolytic attempts.
ConclusionsPersonality disorders are one of the psychiatric pathologies that prevail with greater frequency in autolytic attempts 1. Additionally, it should be taken into account the possible ongoing consumption of psychoactive drugs that could also derive in psychopathological decompensation. On top of the following, the use of antipsychotic treatment is indicated for the managing of conduction altercations 2, besides Lithium being a great option in managing suicidal temptations 3.
Disclosure of InterestNone Declared
From schizotypy to psychosis: is it a natural continuum?
- M. A. Andreo Vidal, M. B. Arribas Simón, M. Calvo Valcárcel, M. P. Pando Fernández, P. Martínez Gimeno, M. D. L. Á. Guillén Soto, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, C. De Andrés Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, Ó. Martín Santiago, A. Monllor Lazarraga, M. Ríos Vaquero, L. Rojas Vázquez, L. Sobrino Conde, A. Apario Parra, G. Lorenzo Chapatte
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S658-S659
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal personality is a condition suffered by 4% of the population. It is defined by presenting interpersonal, behavioral and perceptual features similar to the clinical features of psychotic disorders, such as schizophrenia, in less intensity and dysfunctionality, but at risk of reaching psychosis.
ObjectivesPresentation of a clinical case about a patient with premorbid schizotypal personality traits presenting with an acute psychotic episode.
MethodsLiterature review on association between schizotypal personality and psychosis.
ResultsA 57-year-old woman with a history of adaptive disorder due to work problems 13 years ago, currently without psychopharmacological treatment, goes to the emergency room brought by the emergency services due to behavioral alteration. She reports that “her husband and son wanted to sexually abuse her”, so she had to run away from home and has been running through the streets of the town without clothes and barefoot.
Her husband relates attitude alterations and extravagant behaviors of years of evolution, such as going on diets of eating only bread for 40 days or talking about exoteric and religious subjects, as believing that the devil got inside her husband through a dental implant. He reports that these behaviors have been accentuated during the last month. She has also created a tarot website, and has even had discussions with several users. She is increasingly suspicious of him, has stopped talking to him and stays in his room all day long, with unmotivated laughter and soliloquies.
It was decided to admit him to Psychiatry and risperidone 4 mg was started. At the beginning, she was suspicious and reticent in the interview. As the days went by, communication improved, she showed a relaxed gesture and distanced herself from the delirious ideation, criticizing the episode.
ConclusionsIn recent years, there has been increasing interest in understanding the association between schizotypy and serious mental disorder. Several theories understand schizotypy as a natural continuum of personality that reveals genetic vulnerability and that can lead to psychotic disorder when added to precipitating factors. Other theories define schizotypy as a “latent schizophrenia” where symptoms are contained and expressed in less intensity.
Around 20% evolves to paranoid schizophrenia or other serious mental disorders. It is complex to distinguish between those individuals in whom schizotypy is a prodrome and those in whom it is a stable personality trait. To date, studies applying early psychotherapeutic or pharmacological interventions have had insufficient and contradictory results, and the follow-up and treatment of these individuals could be a stress factor and a stigma. Some studies are looking for reliable markers of evolution to schizophrenia in order to establish adequate protocols for detention, follow-up and treatment.
Disclosure of InterestNone Declared
Conversive and Factitious disorders: Differential diagnosis based on a case report
- M. Fernandez Lozano, B. Rodriguez Rodriguez, N. Navarro Barriga, M. J. Mateos Sexmero, C. Alario Ruiz, L. Rodriguez Andrés, G. Medina Ojeda, T. Jimenez Aparicio, C. Vallecillo Adame, C. De Andres Lobo, M. A. Andreo Vidal, P. Martínez Gimeno, M. Calvo Valcarcel, M. P. Pando Fernández, L. Rojas Vazquez, M. Rios Vaquero, G. Lorenzo Chapatte, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S444
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Conversive disorder is characterised by the presence of one or more involuntary neurological symptoms that are not due to a clear medical pathology. On the other hand, consciously simulated illnesses fall into two diagnostic categories: factitious disorders and malingering, which are differentiated by both the motivation for the behaviour and the awareness of that motivation. Factitious disorder behaviours are motivated by an unconscious need to assume the sick role, whereas malingering behaviours are consciously driven to achieve external secondary gains.
ObjectivesStudy of the differences between conversion disorder and factitious disorder and their repercussions from a case of difficult diagnosis.
MethodsBibliographic review of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 14-year-old male patient. Adoptive parents. Studying in high school. Social difficulties since childhood. He comes to the emergency department on several occasions referring stereotyped movements and motor tics in the four extremities with left cervical lateralization. Increase of these symptoms in the last month, so it was decided to admit him to the pediatric hospital. After observation and study of the patient’s movements with normal complementary tests he should return home. The following day he returned to the emergency department after an episode of dizziness, mutism and emotional block. It was decided to admit him to Psychiatry for behavioral observation and differential diagnosis.
ConclusionsIn the assessment of patients it is essential to make an appropriate diagnosis taking into account the patient’s symptomatology and the patient’s background and life context. Conversion disorder is the unintentional production of neurological symptom, whereas malingering and factitious disorder represent the voluntary production of symptoms with internal or external incentives. They have a close history and this has been frequently confounded. Practitioners are often confronted to medically unexplained symptoms; they represent almost 30% of neurologist’s consultation. The first challenge is to detect them, and recent studies have confirmed the importance of “positive” clinical bedside signs based on incoherence and discordance. Multidisciplinary therapy is recommended with behavioral cognitive therapy, antidepressant to treat frequent comorbid anxiety or depression, and physiotherapy. Factitious disorder and malingering should be clearly delineated from conversion disorder. Factitious disorder should be considered as a mental illness and more research on its physiopathology and treatment is needed, when malingering is a non-medical condition encountered in medico-legal cases.
Disclosure of InterestNone Declared
“God speaks to me through a dove”. The evidence of clozapine in treatment-refractory psychosis
- B. Rodríguez Rodríguez, P. Marqués Cabezas, M. Queipo de Llano de La Viuda, N. Navarro Barriga, G. Guerra Valera, M. B. Arribas Simón, C. Alario Ruiz, M. J. Mateos Sexmero, M. Fernández Lozano, P. Marínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal, M. P. Pando Fernández, A. Monllor Lazarraga, M. Ríos Vaquero, G. Lorenzo Chapate, L. Rojas Vázquez, C. De Andrés Lobo, T. Jiménez Aparicio, M. D. C. Vallecillo Adame
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is an atypical antipsychotic synthesised in 1958. It was withdrawn from the market in the 1970s due to the appearance of agranulocytosis, but was reintroduced due to strong evidence of its efficacy and superiority over other antipsychotics in treatment-resistant schizophrenia.
ObjectivesTo describe the adequate response to clozapine in treatment-refractory psychosis.
MethodsReview of the scientific literature based on a relevant clinical case.
ResultsA 16-year-old woman was admitted to a psychiatric inpatient unit for psychotic symptoms and behavioural disorders. She lives with her father and older sister; she has not been in contact with her mother, who lives in another country, for several years. She attends secondary school, with poor academic performance. Maternal diagnosis of schizophrenia. She started using cannabis two years ago, with a progressive increase up to 20 grams per week. He reports the onset of a feeling of strangeness a year ago, with progressive isolation in his room, referring to delirious ideation of harm towards classmates and people from his town, self-referentiality and delirious interpretations of religious mystical content (“God speaks to me through a dove”). He comments on the phenomenon of theft and thought-reading. Soliloquies and unmotivated laughter are observed.
ConclusionsTreatment was started with risperidone, progressively increasing the dose up to optimisation, without achieving a decrease in positive symptoms, but with the appearance of excessive sedation and sialorrhoea. It was combined with aripiprazole up to 20mg, maintained for a couple of weeks, without significant clinical improvement. Given the failure of two lines of therapy, it was decided to change to clozapine up to a dose of 75mg, with adequate tolerance and response, achieving a distancing of the delirious ideation. Regular haematological controls were performed, with no alterations in haemogram or troponins.
Disclosure of InterestNone Declared
Relation between the first psychotic episode in schizophrenia patients and IL-1β plasma levels – Serbian population study
- N. M. Stojanovic, S. Tošić Golubović, S. Vujić, N. Stefanović, G. Nikolić, A. Todorović, A. Vrućinić, M. Petković, M. Simonović, P. Randjelovic, T. Jevtović Stoimenov
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S388
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
According to immunological theories of schizophrenia prenatal and postnatal exposure to pathogens may contribute to the etiopathogenesis, suggesting that chronically activated immune system cells (macrophages and T lymphocytes) constantly secrete proinflammatory cytokines which affect the development and function of central nervous system.
ObjectivesIn the present work we aimed to evaluate IL-1β plasma levels in schizophrenic patients during their first psychotic episode and to compare the obtained results to those from healthy subjects.
MethodsPlasma was obtained from 32 drug-naive schizophrenic patients, without history of substance abuse or addiction, immediately after their admission to the medical ward, while the control samples were obtained from 20 healthy volunteers.
ResultsLevels of IL-1β were measured using ELISA assay, which measures IL-1β protein in a range from 7.81 to 500 pg/ml. Results revealed that the levels of IL-1β in patients with first psychotic episode were not increased and were below the limit of detection in all studied samples. The same was found in the samples belonging to the control group.
ConclusionsThese data contribute to the poll of knowledge and a still unresolved dogma about the etiopathogenesis of schizophrenia since the results obtained by some studies are also questioning this marker. Thus, whether or not an increase of IL-1β is congenital, acquired during the prodromal phase or absent until the time of first psychotic episode has not yet been investigated.
Disclosure of InterestNone Declared
Persistent COVID an differential diagnosis with depression symptoms
- B. Arribas Simon, M. J. Mateos-Sexmero, O. Martin-Santiago, P. Andres-Olivera, B. Rodriguez-Rodriguez, P. Martinez-Gimeno, N. Navarro-Barriga, T. Jimenez-Aparicio, M. Andreo-Vidal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S502
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 48-year-old woman, a nurse, referred from the Internal Medicine department for evaluation of depressive symptoms and accompanying somatic presentation following COVID-19. The aim is to highlight a recently emerging condition that we are increasingly encountering in our clinics, which can complicate the diagnosis of an underlying affective disorder
ObjectivesDiagnosed with COVID-19, confirmed by a positive PCR test, 6 months ago following an infection in the workplace. The clinical picture consisted of mild symptoms, with a ten-day course and apparent resolution at the time of hospitalization. She returned to her work activities and gradually began to report fluctuating symptoms, including headaches, mild shortness of breath, fatigue, as well as a tingling sensation in the upper extremities, especially in the hands. Additionally, she described feelings of restlessness, depressive mood, and intense fatigue. In additional tests: (CT-Scan) there are signs of mild bilateral lower lung fibrosis.
MethodsTreatment with Duloxetine was initiated for a case of depressive symptoms with accompanying physical symptoms. The differential diagnosis considered Major Depressive Disorder, Single Episode, and Adjustment Disorder with Depressed Mood.”
ResultsWe are facing a clear case of depressive clinic that may have endogenous features, if we adhere to criteria such as those in the DSM-5, as it would meet the criteria for Major Depressive Disorder, Single Episode. However, we have a clearly identified trigger, so we also need to perform a differential diagnosis, primarily with Adjustment Disorder with Depressed Mood: here, the symptoms appear within 3 months following the stressful agent (in this case, SARS-CoV-2 infection). Unlike Major Depressive Episode, once the agent has ceased, the symptoms do not persist beyond 6 months (which we do not know because the physical symptoms causing disability have not disappeared).In addition to purely psychiatric diagnoses that we are accustomed to, we must consider a new diagnostic entity that is becoming more prevalent as the pandemic progresses, namely “long-covid” or persistent COVID.These are generally middle-aged women who, several months after infection, continue to manifest a multifactorial complex of symptoms. These symptoms persist over time, not only the classical ones but also many others that can appear during the ongoing course of the disease.
ConclusionsBeyond the purely psychiatric diagnoses we are accustomed to, we must also consider a new diagnostic entity that is becoming more prevalent as the pandemic continues to advance: Persistent COVID or ‘long-COVID.’ Generally, this condition affects middle-aged women who, several months after contracting the virus, continue to exhibit a multifactorial complex of symptoms. The most common symptoms include fatigue/asthenia (95.91%); general discomfort (95.47%); headaches (86.53%); and low mood (86.21%)
Disclosure of InterestNone Declared
Anxiety and subjective assessment of cognitive functions after COVID-19.
- T. I. Medvedeva, O. M. Boyko, S. N. Enikolopov, O. U. Vorontsova
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S264
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Wide circulation of the COVID-19 has led to the high occurrence of a longcovid in which the complaints of violations of cognitive functions and affective disorders often occur.
ObjectivesThe aim of this study was to assess the relation of anxiety and subjective appraisal of the states of cognitive functions.
MethodsThe data of 1233 respondents of internet-research who were divided into the four groups according to their COVID-19 status and the level of anxiety. Group 1 (didn’t have COVID before, low level of anxiety) – 689 people (mean age 40,6), group 2 (didn’t have COVID before, High level of anxiety) – 364 people (mean age 39,8), group 3 (had been ill COVID-19, low level of anxiety) – 102 people (mean age 41,2), group 4 (had been ill COVID-19, High level of anxiety) -130 people (mean age 35,5). Methods include the questions about the states of their cognitive functions (attention, memory, working capacity), a question about COVID-19 status. There are the results of comparing the groups that was carried out using the Kruskal-Wallis test. A pairwise comparison was carried out using the Mann-Whitney test for two groups of people who were not ill; two groups who were ill; two groups with a low level of anxiety; two groups with a high level of anxiety. To correct multiple comparisons, the adjusted significance level calculated by the formula (p = 1 - 0,9511/n) was used, which was p=0,017 for 4 pairwise comparisons.
ResultsResults are shown in table.
Group 1 Group 2 Group 3 Group 4 Trouble remembering things 0,50 0,99 0,77 1,30 (*2) (*1,*4) (*1,*4) (*2,*3) Feeling low in energy or slowed down 0,74 1,77 1,23 2,34 (*2,*3) (*1,*4) (*1,*4) (*2,*3) Having to do things very slowly to insure correctness 0,27 0,88 0,31 1,00 (*2) (*1) (*4) (*3) Difficulty making decisions 0,63 1,63 0,82 1,67 (*2) (*1) (*4) (*3) Your mind going blank 0,34 1,12 0,64 1,36 (*2,*3) (*1) (*1,*4) (*3) Trouble concentrating 0,58 1,55 0,72 1,86 (*2) (*1,*4) (*4) (*2,*3) Feeling everything is an effort 0,43 1,47 0,56 1,81 (*2) (*1,*4) (*4) (*2,*3) An entry in parentheses such as (2*) means that this group for this parameter statistically significant differs from group 2.
As indicated in the table, respondents with the high level of anxiety have higher levels of the subjective assessment of cognitive functions regardless of their COVID-19 status.
ConclusionsA possible explanation may be the disorganizing effect of anxiety on the cognitive functions. When combined with possible organic disorders caused by the transferred COVID-19, the most marked indicators of cognitive decline are observed. An effective rehabilitation of cognitive functions after COVID-19 requires to diagnose the level of anxiety and to seek psychological and psychiatric assistance for people with a high level of anxiety.
Disclosure of InterestNone Declared
Bipolar Disorder in Pregnancy: A Challenging Case Managed with Maintenance Electroconvulsive Therapy
- B. Arribas-Simon, M. J. Mateos-Sexmero, O. Martin-Santiago, P. Andres-Olivera, B. Rodriguez-Rodriguez, P. Martinez-Gimeno, N. Navarro-Barriga, T. Jimenez-Aparicio, P. Fernandez-Pando, M. Andreo-Vidal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S115-S116
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pregnancy is a high-risk period for major affective disorders and can lead to a destabilizing period for our patients. Standard pharmacological strategies must be carefully evaluated due to potential teratogenic or side effects. We present a case of bipolar disorder type I with challenging-to-control maniac episodes during pregnancy, which has required Electroconvulsive Therapy for its management.
ObjectivesPresenting maintenance electroconvulsive therapy (ECT) as a safe and effective therapeutic strategy during pregnancy, with the presentation of a case in which it has been administered every 3 weeks from the second trimester until the baby’s birth at 37 weeks
MethodsThis concerns a 28-year-old immigrant woman, married, with a 10-year-old child. She was diagnosed with bipolar disorder type I at the age of 16 when she experienced her first manic episode in her country of origin. Subsequently, during her first pregnancy, she required hospitalization for electroconvulsive therapy (ECT) treatment, with a positive response after a single session. She remained stable for several years without maintenance pharmacological treatment or follow-up until the ninth week of her second pregnancy when she experienced a manic episode requiring hospitalization.
ResultsShe was initially treated with Olanzapine and Lorazepam with a positive response, but three weeks later, she was readmitted with a similar episode. These decompensations occurred almost monthly, leading to the consideration of introducing mood stabilizers after the first trimester. However, due to the patient’s severe hyperemesis gravidarum, this stabilizing treatment was ruled out due to the difficulty in controlling its blood levels and the associated risk of intoxication. During the fifth admission at the 20th week of gestation, the decision was made to initiate ECT treatment, which yielded an excellent response and subsequent maintenance.
ConclusionsThe indications for electroconvulsive therapy (ECT) during pregnancy are the same as in the rest of adult patients. In individuals with a psychiatric history, it is possible for a relapse of mental illness to occur during pregnancy, although the risk is considerably higher during the postpartum period. ECT is considered an effective and safe treatment option in all three trimesters of pregnancy and the postpartum period. During the informed consent process, patients should be informed about the potential impact of ECT as well as alternative treatment options.
Disclosure of InterestNone Declared
Attachment disturbance in women with depressive spectrum disorder, its connection with hostility
- S. N. Enikolopov, O. U. Vorontsova, T. I. Medvedeva, O. M. Boyko, I. V. Oleichik
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S541-S542
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The results of the study of psychological factors of hostility in depression are presented. The topicality of the study is due to hostility considered, on the one hand, as a property of depression, and on the other hand, as a risk factor, associated with the likelihood of auto-aggressive behavior.
ObjectivesThe aim of the study was to analyze the relationship between hostility and attachment disorders in endogenous depression.
MethodsThe study involved 49 patients with depressive disorder (mean age 19,8±4,5). All patients were assessed using the Hamilton Depression Rating Scale (HDRS-17 mean 21,03±6,02). All completed the following methods: Revised Experiences in Close Relationships (ECR-R); Symptom Check List-90-Revised (SCL-90R); Aggression Questionnaire by Buss and Perry (BPAQ); I-structural test by G. Ammon (ISTA). According to the “depression” parameter of the SCL-90R, the group was divided into subgroups with high and medium severity of depression. Analysis of variance (ANOVA) or Mann-Whitney test were. Correlation analysis (Spearman) and stepwise multiple regression analysis were also used.
ResultsAt high levels of depression, the indicators of “hostility”, “destructive” and “deficit aggression” are statistically significantly higher. The severity of depression significantly correlates with the severity of “anxiety” in attachment (close relationships), as well as with pathological “narcissism”, “destructive external self-delimitation”, “deficient internal self-delimitation”.
For the measure of depression, regression analysis showed that the regression model explained more than 76% of the variance, with the measures of “interpersonal sensitivity”, “deficit narcissism”, and “avoidance” in attachment making significant contributions. For the “hostility” the regression model explains about 62% of the variance, while a significant contribution is made, as in the analysis of “depression”, by the indicators of “interpersonal sensitivity” and “avoidance”, however, unlike “depression”, the contribution of the “destructive narcissism” is noted in contrast to the “deficit narcissism”.
ConclusionsWith severe depressive symptoms, indicators of hostility are increased. Hostility in depression is associated with factors caused by a violation of early interpersonal relationships (anxious attachment), which causes increased sensitivity in relations with others, “building a barrier” between oneself and the external environment perceived as hostile in the narcissistic pathology, problems in emotional regulation. One of the targets of psychotherapeutic work may be the ambivalence between desire for symbiotic dependence and the experienced hostility.
Disclosure of InterestNone Declared
Lithium withdrawal and relapse in bipolar disorder when kidney function deteriorates
- C. De Andrés-Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, A. Rodríguez Campos, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano, M. Calvo Valcárcel, M. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, L. Rojas Vázquez, G. Lorenzo Chapatte, M. Ríos Vaquero, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S427-S428
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium was the first mood stabilizer and today continues to be a first-line treatment in the treatment of bipolar disorder despite its adverse effects, which make it important to monitor blood levels and control kidney function.
ObjectivesPresentation of a case of litium withdrawal and relapse in bipolar disorder. Literature review relating to the risk of relapse when lithium treatment is interrupted.
MethodsWe present a clinical case of a patient who suffers a deterioration in renal function that requires the withdrawal of lithium and who consequently suffers a relapse. We conducted a bibliographic research of articles in Pubmed on this topic.
ResultsA 49-year-old male, with a history of multiple admissions to UHB since the age of 18 with a diagnosis of bipolar disorder and treatment with lithium. Decompensations towards the manic pole have always been related to interruptions in lithium treatment. On several occasions when the patient was feeling well emotionally, he believed himself to be “cured” and abandoned the treatment, triggering a manic episode, showing verbal aggression, increased self-esteem and delusional ideation of harm. Remission was usually achieved with the reintroduction of lithium and the addition of high-dose quetiapine. Between episodes, constant overvalued ideas of economic scarcity seemed to persist, which were accentuated in the form of delusional ideas of ruin in depressive decompensations. After 7 years of stability, control analysis showed blood litemia of 2.2 mEq/L with deterioration of kidney function and generalized tremor was observed, without improvement after serum therapy. He was admitted for dialysis and lithium was suspended. Treatment with valproate was started and a consultation scheduled in a week to adjust the dose. The patient did not attend that consultation and was admitted three days later to Psychiatry Hospitalization showing a challenging attitude, evident dysphoric mood, accelerated speech, with derailments and echolalia. Delusional ideation of harm with auditory hallucinations. Insomnia and hyporexia. Chronic renal failure persisted.
ConclusionsLithium is a very effective drug but with a narrow therapeutic range that requires adequate monitoring due to the possible consequences of its use at different organs and systems of the body. when lithium is found in the blood at toxic levels with deterioration of kidney function and glomerular filtration fails to recover, lithium treatment should be suspended. Sudden withdrawal of lithium significantly increases the risk of relapse due to rebound effect. More than 50% of patients experience a recurrence within 10 weeks of withdrawal.
Disclosure of InterestNone Declared
Psychiatrists’ Readiness for Digital Psychiatry in Pakistan: A Multicenter CrossSectional Study with Regression Analysis
- M. M. Adeel Riaz, T. Abrar, S. S. Tebha, H. Tariq, R. Fatima, M. Hamad, A. A. Khan, A. Ahadi, N. Ul Sabah, W. Rasool, K. Latif, M. Umar, I. Siddique, F. A. Nawaz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S548-S549
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The concept of digital psychiatry, encompassing technologies such as mental health apps, Virtual Reality (VR), Artificial Intelligence (AI), and telepsychiatry, emerges as a potential solution to bridge the existing gaps in the mental health system of Pakistan. However, one of the major barriers to the implementation of these technologies is hesitancy to adopt digital tools by psychiatrists.
ObjectivesThis study aims to explore the current understanding of digital psychiatry, the barriers faced by psychiatrists in its’ widespread implementation, and their willingness to adopt these services in clinical practice.
MethodsThis cross-sectional study surveyed psychiatrists’ knowledge, attitudes, and practices on digital psychiatry from 39 public hospitals across Pakistan using an online validated questionnaire from January to July 2023. Participants included psychiatry residents, fellows, and consultants practicing in Pakistan. Responses were analyzed with Raosoft software, Quirkos, and SPSS 26 using thematic analysis and correlation.
ResultsA total of 200 participants responded to the questionnaire, primarily in the age range of 20-30 years (56%). The gender distribution was 55% male (N = 111) and 45% female (N = 89). Among the professional roles, 23% were consultants, 7% were registrars, 54% were psychiatry residents, and 17% were medical officers. Respondents came from both rural (N = 148, 74%) and urban (N = 52, 26%) practice settings. Regarding telepsychiatry, 46% strongly agreed that they are familiar with telepsychiatry, while 58% agreed that telepsychiatry can save time and money. Additionally, 22% strongly agreed that it’s a viable approach for patient care. Concerning perspectives on Artificial Intelligence (AI) in digital psychiatry readiness, only 40% of participants had received AI training. However, 55% expressed interest in collaborating with international centers on AI-related projects. In terms of mental health apps, 62% of respondents reported limited familiarity with them. Nevertheless, 65% believed that these apps could potentially save time and money for psychiatric health systems. Lastly, concerning Virtual Reality (VR) in psychiatric care, 57% of participants were familiar with VR technology, but only 43% were acquainted with its applications in psychiatry. Notably, 71% did not view VR as a viable replacement for in-person psychiatric management.
ConclusionsThis is the first study conducted on understanding digital psychiatry in Pakistan’s healthcare system, which revealed multiple challenges to digital health competency among psychiatrists. This emphasizes on the need for formal training and funding towards resources to overcome obstacles in utilizing mental health technologies.
Disclosure of InterestNone Declared


