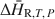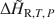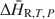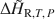17 results
Isothermal measurement of heats of hydration in zeolites by simultaneous thermogravimetry and differential scanning calorimetry
- Philip S. Neuhoff, Jie Wang
-
- Journal:
- Clays and Clay Minerals / Volume 55 / Issue 3 / June 2007
- Published online by Cambridge University Press:
- 01 January 2024, pp. 239-252
-
- Article
- Export citation
-
A calorimetric method for determining isothermal partial and integral heats of hydration reactions (${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$
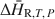 and ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$
and ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$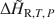 , respectively) in zeolites and other mineral hydrates is presented. The method involves immersing a dehydrated sample in a humid gas stream under isothermal conditions within a thermal analysis device that records simultaneous differential scanning calorimetric (DSC) and thermogravimetric analysis (TGA) signals. Monitoring changes in sample mass (corresponding to extent of reaction progress) coincident with a quantitative measurement of heat flow allows for direct detection of ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$
, respectively) in zeolites and other mineral hydrates is presented. The method involves immersing a dehydrated sample in a humid gas stream under isothermal conditions within a thermal analysis device that records simultaneous differential scanning calorimetric (DSC) and thermogravimetric analysis (TGA) signals. Monitoring changes in sample mass (corresponding to extent of reaction progress) coincident with a quantitative measurement of heat flow allows for direct detection of ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$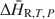 as a function of the extent of hydration, which can be integrated to determine ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$
as a function of the extent of hydration, which can be integrated to determine ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$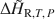 . In addition, it eliminates uncertainties associated with imprecise knowledge of the starting and final states of a sample during hydration. Measurement under isothermal conditions removes uncertainties associated with heat capacity effects that complicate interpretations of DSC measurements of dehydration heats conducted under traditional scanning temperature conditions. Example experiments on the zeolites natrolite, analcime and chabazite are used to illustrate strategies for quantifying ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$
. In addition, it eliminates uncertainties associated with imprecise knowledge of the starting and final states of a sample during hydration. Measurement under isothermal conditions removes uncertainties associated with heat capacity effects that complicate interpretations of DSC measurements of dehydration heats conducted under traditional scanning temperature conditions. Example experiments on the zeolites natrolite, analcime and chabazite are used to illustrate strategies for quantifying ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$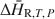 and ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$
and ${\rm{\Delta }}{\tilde H_{{\rm{R,}}T,\,P}}$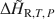 and minimizing errors associated with baseline uncertainties. Results from this method agree well with previously published values determined by other calorimetric techniques and regression of phase equilibrium data. In the case of chabazite, the results allowed detailed measurements of the variation in ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$
and minimizing errors associated with baseline uncertainties. Results from this method agree well with previously published values determined by other calorimetric techniques and regression of phase equilibrium data. In the case of chabazite, the results allowed detailed measurements of the variation in ${\rm{\Delta }}{\bar H_{{\rm{R,}}T,\,P}}$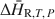 for energetically different water types encountered progressively as the sample absorbed water. This technique complements and in many cases improves the quality of thermodynamic data obtained through phase equilibrium observations and other calorimetric techniques.
for energetically different water types encountered progressively as the sample absorbed water. This technique complements and in many cases improves the quality of thermodynamic data obtained through phase equilibrium observations and other calorimetric techniques.
Sustained benefit of cognitive behaviour therapy for health anxiety in medical patients (CHAMP) over eight years: randomised controlled trial – CORRIGENDUM
- P. Tyrer, D. Wang, M. Crawford, S. Dupont, S. Cooper, S. Nourmand, V. Lazarevic, A. Philip, H. Tyrer
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 10 / July 2021
- Published online by Cambridge University Press:
- 03 June 2020, p. 1723
-
- Article
-
- You have access Access
- HTML
- Export citation
Sustained benefit of cognitive behaviour therapy for health anxiety in medical patients (CHAMP) over 8 years: a randomised-controlled trial
- P. Tyrer, D. Wang, M. Crawford, S. Dupont, S. Cooper, S. Nourmand, V. Lazarevic, A. Philip, H. Tyrer
-
- Journal:
- Psychological Medicine / Volume 51 / Issue 10 / July 2021
- Published online by Cambridge University Press:
- 16 March 2020, pp. 1714-1722
-
- Article
- Export citation
-
Background
Health anxiety is an under-recognised but a frequent cause of distress. It is particularly common in general hospitals.
MethodsWe carried out an 8-year follow-up of medical out-patients with health anxiety (hypochondriasis) enrolled in a randomised-controlled trial in five general hospitals in London, Middlesex and Nottinghamshire. Randomisation was to a mean of six sessions of cognitive behaviour therapy adapted for health anxiety (CBT-HA) or to standard care in the clinics. The primary outcome was a change in score on the Short Health Anxiety Inventory, with generalised anxiety and depression as secondary outcomes. Of 444 patients aged 16–75 years seen in cardiology, endocrinology, gastroenterology, neurology and respiratory medicine clinics, 306 (68.9%) were followed-up 8 years after randomisation, including 36 who had died. The study is registered with controlled-trials.com, ISRCTN14565822.
ResultsThere was a significant difference in the HAI score in favour of CBT-HA over standard care after 8 years [1.83, 95% confidence interval (CI) 0.25–3.40, p = 0.023], between group differences in generalised anxiety were less (0.54, 95% CI −0.29 to 1.36), p = 0.20, ns), but those for depression were greater at 8 years (1.22, 95% CI 0.42–2.01, p < 0.003) in CBT-HA than in standard care, most in standard care satisfying the criteria for clinical depression. Those seen by nurse therapists and in cardiology and gastrointestinal clinics achieved the greatest gains with CBT-HA, with greater improvement in both symptoms and social function.
ConclusionsCBT-HA is a highly long-term effective treatment for pathological health anxiety with long-term benefits. Standard care for health anxiety in medical clinics promotes depression. Nurse therapists are effective practitioners.
Confidence intervals for the duration of a mass extinction
- Steve C. Wang, Aaron E. Zimmerman, Brendan S. McVeigh, Philip J. Everson, Heidi Wong
-
- Journal:
- Paleobiology / Volume 38 / Issue 2 / Spring 2012
- Published online by Cambridge University Press:
- 08 April 2016, pp. 265-277
-
- Article
- Export citation
-
A key question in studies of mass extinctions is whether the extinction was a sudden or gradual event. This question may be addressed by examining the locations of fossil occurrences in a stratigraphic section. However, the fossil record can be consistent with both sudden and gradual extinctions. Rather than being limited to rejecting or not rejecting a particular scenario, ideally we should estimate the range of extinction scenarios that is consistent with the fossil record. In other words, rather than testing the simplified distinction of “sudden versus gradual,” we should be asking, “How gradual?”
In this paper we answer the question “How gradual could the extinction have been?” by developing a confidence interval for the duration of a mass extinction. We define the duration of the extinction as the time or stratigraphic thickness between the first and last taxon to go extinct, which we denote by Δ. For example, we would like to be able to say with 90% confidence that the extinction took place over a duration of 0.3 to 1.1 million years, or 24 to 57 meters of stratigraphic thickness. Our method does not deny the possibility of a truly simultaneous extinction; rather, in this framework, a simultaneous extinction is one whose value of Δ is equal to zero years or meters.
We present an algorithm to derive such estimates and show that it produces valid confidence intervals. We illustrate its use with data from Late Permian ostracodes from Meishan, China, and Late Cretaceous ammonites from Seymour Island, Antarctica.
Discontinuation of Systematic Surveillance and Contact Precautions for Vancomycin-Resistant Enterococcus (VRE) and Its Impact on the Incidence of VRE faecium Bacteremia in Patients with Hematologic Malignancies
- Nikolaos G. Almyroudis, Ryosuke Osawa, George Samonis, M. Wetzler, Eunice S. Wang, Philip L. McCarthy, Jr., Brahm H. Segal
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 37 / Issue 4 / April 2016
- Published online by Cambridge University Press:
- 11 January 2016, pp. 398-403
- Print publication:
- April 2016
-
- Article
- Export citation
-
OBJECTIVE
To study the effect of discontinuation of systematic surveillance for vancomycin-resistant Enterococcus (VRE) and contact isolation of colonized patients on the incidence of VRE bacteremia
SETTINGA hematology-oncology unit with high prevalence of VRE colonization characterized by predominantly sporadic molecular epidemiology
PARTICIPANTSInpatients with hematologic malignancies and recipients of hematopoietic stem cell transplantation
METHODSThe incidence of VRE bacteremia was measured prospectively during 2 different 3-year time periods; the first during active VRE surveillance and contact precautions and the second after discontinuation of these policies. We assessed the collateral impact of this policy change on the incidence of bacteremia due to methicillin-resistant Staphylococcus aureus (MRSA) and Clostridium difficile infection even though we maintained contact precautions for these organisms. Incidence of infectious events was measured as number of events per 1,000 patients days per month. Time series analysis was used to evaluate trends.
RESULTSThe incidence of VRE bacteremia remained stable after discontinuation of VRE surveillance and contact precautions. The incidence of MRSA bacteremia and Clostridium difficile infection for which we continued contact precautions also remained stable. Aggregated antibiotic utilization and nursing hours per patient days were similar between the 2 study periods.
CONCLUSIONActive surveillance and contact precautions for VRE colonization did not appear to prevent VRE bacteremia in patients with hematologic malignancies and recipients of hematopoietic stem cell transplantation with high prevalence of VRE characterized by predominantly sporadic molecular epidemiology.
Infect. Control Hosp. Epidemiol. 2016;37(4):398–403
26 - Photovoltaic retinal prosthesis for restoring sight to the blind
- from Part V - Bionics
-
- By Daniel Palanker, Stanford University, Yossi Mandel, Bar Ilan University, Keith Mathieson, University of Strathclyde, James Loudin, Stanford University, Georges Goetz, Stanford University, Philip Huie, Stanford University, Lele Wang, University of California, San Diego, Theodore I. Kamins, Stanford University, Richard Smith, University of California, Santa Cruz, James S. Harris, Stanford University, Alexander Sher, University of California, Santa Cruz
- Edited by Sandro Carrara, École Polytechnique Fédérale de Lausanne, Krzysztof Iniewski
-
- Book:
- Handbook of Bioelectronics
- Published online:
- 05 September 2015
- Print publication:
- 06 August 2015, pp 325-338
-
- Chapter
- Export citation
-
Summary
Introduction
Age-related macular degeneration (AMD) is one of the leading causes of blindness in the developed world, with an incidence of 1:500 in patients aged 55–64, and 1:8 in patients over 85 [1]. Retinitis pigmentosa (RP) is an inherited disease blinding about 1 in every 4000 individuals much earlier in life [2]. In both of these conditions the photoreceptor layer degenerates, while the inner retinal neurons survive to a large extent [3–5]. Electrically activating these neurons provides an alternative route for visual information and raises hope for the restoration of sight to the blind.
In a normal retina, photoreceptors convert light into neural signals that are processed by inner retinal neurons, leading to generation of action potentials in the retinal ganglion cells (RGCs). These signals travel to the brain through the optic nerve and serve as the basis for visual perception. Electrical stimulation of the retina with microelectrodes can also produce action potentials in RGCs, creating spatially patterned percepts of light called phosphenes. Indeed, recent clinical trials with retinal prosthetic electrode arrays have restored visual acuity to subjects blinded by retinal degeneration up to 20/1200 using epiretinal placement (facing the ganglion cell side) [6], and up to 20/550 with subretinal implantation [7]. While this serves as an important proof of concept with clinically useful implications, existing retinal prosthesis designs have a number of shortcomings.
Contributors
-
- By Linda S. Aglio, Cyrus Ahmadi Yazdi, Syed Irfan Qasim Ali, Caryn Barnet, Jessica Bauerle, Felicity Billings, Evan Blaney, Beverly Chang, Christopher Chen, Zinaida Chepurny, Hyung Sun Choi, Allison Clark, Lauren J. Cornella, Lisa Crossley, Michael D’Ambra, Galina Davidyuk, Whitney de Luna, Manisha S. Desai, Sukumar P. Desai, Kelly G. Elterman, Michaela K. Farber, Iuliu Fat, Jaida Fitzgerald, Devon Flaherty, John A. Fox, Gyorgy Frendl, Rejean Gareau, Joseph M. Garfield, Andrea Girnius, Laverne D. Gugino, J. Tasker Gundy, Carly C. Guthrie, Lisa M. Hammond, M. Tariq Hanifi, James Hardy, Philip M. Hartigan, Thomas Hickey, Richard Hsu, Mohab Ibrahim, David Janfaza, Yuka Kiyota, Suzanne Klainer, Benjamin Kloesel, Hanjo Ko, Bhavani Kodali, Vesela Kovacheva, J. Matthew Kynes, Robert W. Lekowski, Joyce Lo, Jeffrey Lu, Alvaro A. Macias, Zahra M. Malik, Erich N. Marks, Brendan McGinn, Jonathan R. Meserve, Annette Mizuguchi, Srdjan S. Nedeljkovic, Ju-Mei Ng, Michael Nguyen, Olutoyin Okanlawon, Jennifer Oliver, Krishna Parekh, Jessica Patterson, Christian Peccora, Pete Pelletier, Sujatha Pentakota, James H. Philip, Marc Philip T. Pimentel, Timothy D. Quinn, Elizabeth M. Rickerson, Susan L. Sager, Julia Serber, Shaheen Shaikh, Stanton Shernan, David Silver, Alissa Sodickson, Pingping Song, George P. Topulos, Agnieszka Trzcinka, Richard D. Urman, Rosemary Uzomba, Joshua Vacanti, Assia Valovska, Michael Vaninetti, Scott W. Vaughan, Kamen Vlassakov, Christopher Voscopoulos, Emily L. Wang, Laura Westfall, Zhiling Xiong, Stephanie Yacoubian, Dongdong Yao, Martin Zammert, Maksim Zayaruzny, Jose Luis Zeballos, Natthasorn Zinboonyahgoon, Jie Zhou
- Edited by Linda S. Aglio, Robert W. Lekowski, Richard D. Urman
-
- Book:
- Essential Clinical Anesthesia Review
- Published online:
- 05 February 2015
- Print publication:
- 08 January 2015, pp xi-xvi
-
- Chapter
- Export citation
Detection of human taeniases in Tibetan endemic areas, China
- TIAOYING LI, XINGWANG CHEN, TETSUYA YANAGIDA, HAO WANG, CHANGPING LONG, YASUHITO SAKO, MUNEHIR OKAMOTO, YUNFEI WU, PATRICK GIRAUDOUX, FRANCIS RAOUL, AGATHE NKOUAWA, MINORU NAKAO, PHILIP S. CRAIG, AKIRA ITO
-
- Journal:
- Parasitology / Volume 140 / Issue 13 / November 2013
- Published online by Cambridge University Press:
- 18 July 2013, pp. 1602-1607
-
- Article
- Export citation
-
Detection of taeniasis carriers of Taenia solium is essential for control of cysticercosis in humans and pigs. In the current study, we assessed the positive detection rate of a self-detection tool, stool microscopy with direct smear and coproPCR for taeniasis carriers in endemic Tibetan areas of northwest Sichuan. The self-detection tool through questioning about a history of proglottid expulsion within the previous one year showed an overall positive detection rate of more than 80% for Taenia saginata, T. solium and T. asiatica. The positive detection rate was similar for T. saginata and T. solium. In 132 taeniid tapeworm carriers, 68 (51·5%) were detected by microscopy and 92 (69·7%) were diagnosed by coproPCR. A combination of microscopy and coproPCR increased the positive detection rate to 77·3%. There remained 10 cases (7·6%) coproPCR negative but microscopy positive. Due to the high cost and complicated process, coproPCR is required for the identification of Taenia species only when necessary, though it had a significant higher positive detection rate than microscopy. Combined use of self-detection and stool microscopy are recommended in community-based mass screening for taeniases in this Tibetan area or in other situation-similar endemic regions.
Transmission ecosystems of Echinococcus multilocularis in China and Central Asia
- PATRICK GIRAUDOUX, FRANCIS RAOUL, EVE AFONSO, ISKENDER ZIADINOV, YURONG YANG, LI LI, TIAOYING LI, JEAN-PIERRE QUÉRÉ, XIAOHUI FENG, QIAN WANG, HAO WEN, AKIRA ITO, PHILIP S. CRAIG
-
- Journal:
- Parasitology / Volume 140 / Issue 13 / November 2013
- Published online by Cambridge University Press:
- 05 June 2013, pp. 1655-1666
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
From continental to regional scales, the zoonosis alveolar echinococcosis (AE) (caused by Echinococcus multilocularis) forms discrete patches of endemicity within which transmission hotspots of much larger prevalence may occur. Since the late 80s, a number of hotspots have been identified in continental Asia, mostly in China, wherein the ecology of intermediate host communities has been described. This is the case in south Gansu, at the eastern border of the Tibetan plateau, in south Ningxia, in the western Tian Shan of Xinjiang, and in the Alay valley of south Kyrgyzstan. Here we present a comparative natural history and characteristics of transmission ecosystems or ecoscapes. On this basis, regional types of transmission and their ecological characteristics have been proposed in a general framework. Combining climatic, land cover and intermediate host species distribution data, we identified and mapped 4 spatially distinct types of transmission ecosystems typified by the presence of one of the following small mammal ‘flagship’ species: Ellobius tancrei, Ochotona curzoniae, Lasiopodomys brandtii or Eospalax fontanierii. Each transmission ecosystem had its own characteristics which can serve as a reference for further in-depth research in the transmission ecology of E. multilocularis. This approach may be used at fine spatial scales to characterize other poorly known transmission systems of the large Eurasian endemic zone, and help in consideration of surveillance systems and interventions.
Contributors
-
- By Aakash Agarwala, Linda S. Aglio, Rae M. Allain, Paul D. Allen, Houman Amirfarzan, Yasodananda Kumar Areti, Amit Asopa, Edwin G. Avery, Patricia R. Bachiller, Angela M. Bader, Rana Badr, Sibinka Bajic, David J. Baker, Sheila R. Barnett, Rena Beckerly, Lorenzo Berra, Walter Bethune, Sascha S. Beutler, Tarun Bhalla, Edward A. Bittner, Jonathan D. Bloom, Alina V. Bodas, Lina M. Bolanos-Diaz, Ruma R. Bose, Jan Boublik, John P. Broadnax, Jason C. Brookman, Meredith R. Brooks, Roland Brusseau, Ethan O. Bryson, Linda A. Bulich, Kenji Butterfield, William R. Camann, Denise M. Chan, Theresa S. Chang, Jonathan E. Charnin, Mark Chrostowski, Fred Cobey, Adam B. Collins, Mercedes A. Concepcion, Christopher W. Connor, Bronwyn Cooper, Jeffrey B. Cooper, Martha Cordoba-Amorocho, Stephen B. Corn, Darin J. Correll, Gregory J. Crosby, Lisa J. Crossley, Deborah J. Culley, Tomas Cvrk, Michael N. D'Ambra, Michael Decker, Daniel F. Dedrick, Mark Dershwitz, Francis X. Dillon, Pradeep Dinakar, Alimorad G. Djalali, D. John Doyle, Lambertus Drop, Ian F. Dunn, Theodore E. Dushane, Sunil Eappen, Thomas Edrich, Jesse M. Ehrenfeld, Jason M. Erlich, Lucinda L. Everett, Elliott S. Farber, Khaldoun Faris, Eddy M. Feliz, Massimo Ferrigno, Richard S. Field, Michael G. Fitzsimons, Hugh L. Flanagan Jr., Vladimir Formanek, Amanda A. Fox, John A. Fox, Gyorgy Frendl, Tanja S. Frey, Samuel M. Galvagno Jr., Edward R. Garcia, Jonathan D. Gates, Cosmin Gauran, Brian J. Gelfand, Simon Gelman, Alexander C. Gerhart, Peter Gerner, Omid Ghalambor, Christopher J. Gilligan, Christian D. Gonzalez, Noah E. Gordon, William B. Gormley, Thomas J. Graetz, Wendy L. Gross, Amit Gupta, James P. Hardy, Seetharaman Hariharan, Miriam Harnett, Philip M. Hartigan, Joaquim M. Havens, Bishr Haydar, Stephen O. Heard, James L. Helstrom, David L. Hepner, McCallum R. Hoyt, Robert N. Jamison, Karinne Jervis, Stephanie B. Jones, Swaminathan Karthik, Richard M. Kaufman, Shubjeet Kaur, Lee A. Kearse Jr., John C. Keel, Scott D. Kelley, Albert H. Kim, Amy L. Kim, Grace Y. Kim, Robert J. Klickovich, Robert M. Knapp, Bhavani S. Kodali, Rahul Koka, Alina Lazar, Laura H. Leduc, Stanley Leeson, Lisa R. Leffert, Scott A. LeGrand, Patricio Leyton, J. Lance Lichtor, John Lin, Alvaro A. Macias, Karan Madan, Sohail K. Mahboobi, Devi Mahendran, Christine Mai, Sayeed Malek, S. Rao Mallampati, Thomas J. Mancuso, Ramon Martin, Matthew C. Martinez, J. A. Jeevendra Martyn, Kai Matthes, Tommaso Mauri, Mary Ellen McCann, Shannon S. McKenna, Dennis J. McNicholl, Abdel-Kader Mehio, Thor C. Milland, Tonya L. K. Miller, John D. Mitchell, K. Annette Mizuguchi, Naila Moghul, David R. Moss, Ross J. Musumeci, Naveen Nathan, Ju-Mei Ng, Liem C. Nguyen, Ervant Nishanian, Martina Nowak, Ala Nozari, Michael Nurok, Arti Ori, Rafael A. Ortega, Amy J. Ortman, David Oxman, Arvind Palanisamy, Carlo Pancaro, Lisbeth Lopez Pappas, Benjamin Parish, Samuel Park, Deborah S. Pederson, Beverly K. Philip, James H. Philip, Silvia Pivi, Stephen D. Pratt, Douglas E. Raines, Stephen L. Ratcliff, James P. Rathmell, J. Taylor Reed, Elizabeth M. Rickerson, Selwyn O. Rogers Jr., Thomas M. Romanelli, William H. Rosenblatt, Carl E. Rosow, Edgar L. Ross, J. Victor Ryckman, Mônica M. Sá Rêgo, Nicholas Sadovnikoff, Warren S. Sandberg, Annette Y. Schure, B. Scott Segal, Navil F. Sethna, Swapneel K. Shah, Shaheen F. Shaikh, Fred E. Shapiro, Torin D. Shear, Prem S. Shekar, Stanton K. Shernan, Naomi Shimizu, Douglas C. Shook, Kamal K. Sikka, Pankaj K. Sikka, David A. Silver, Jeffrey H. Silverstein, Emily A. Singer, Ken Solt, Spiro G. Spanakis, Wolfgang Steudel, Matthias Stopfkuchen-Evans, Michael P. Storey, Gary R. Strichartz, Balachundhar Subramaniam, Wariya Sukhupragarn, John Summers, Shine Sun, Eswar Sundar, Sugantha Sundar, Neelakantan Sunder, Faraz Syed, Usha B. Tedrow, Nelson L. Thaemert, George P. Topulos, Lawrence C. Tsen, Richard D. Urman, Charles A. Vacanti, Francis X. Vacanti, Joshua C. Vacanti, Assia Valovska, Ivan T. Valovski, Mary Ann Vann, Susan Vassallo, Anasuya Vasudevan, Kamen V. Vlassakov, Gian Paolo Volpato, Essi M. Vulli, J. Matthias Walz, Jingping Wang, James F. Watkins, Maxwell Weinmann, Sharon L. Wetherall, Mallory Williams, Sarah H. Wiser, Zhiling Xiong, Warren M. Zapol, Jie Zhou
- Edited by Charles Vacanti, Scott Segal, Pankaj Sikka, Richard Urman
-
- Book:
- Essential Clinical Anesthesia
- Published online:
- 05 January 2012
- Print publication:
- 11 July 2011, pp xv-xxviii
-
- Chapter
- Export citation
Contributors
-
- By Dag Aarsland, Adrià Arboix, Carlos Bazán, James T. Becker, Sylvie Belleville, Kevin M. Biglan, Sandra E. Black, Mariana Blanco, Rémi W. Bouchard, Bruce J. Brew, David J. Burn, Leonardo Caixeta, Richard Camicioli, Paulo Caramelli, Neil Cashman, Nicholas W. S. Davies, Yan Deschaintre, Rachel S. Doody, Bruno Dubois, Uwe Ehrt, Stephane Epelbaum, Ryan V. V. Evans, Joseph M. Ferrara, Bruno Franchi, Morris Freedman, Anders Gade, Serge Gauthier, Marta Grau-Olivares, Matthew E. Growdon, Will Guest, Marie Christie Guiot, Shahul Hameed, Mirna Lie Hosogi-Senaha, Ging-Yuek Robin Hsiung, Masamichi Ikawa, Rajive Jassal, Vesna Jelic, Peter Johannsen, Edward S. Johnson, Mary M. Kenan, Bert-Jan Kerklaan, Benjamin Lam, Gabriel C. Léger, Gabriel Leonard, Emilie Lepage, Irene Litvan, Oscar L. Lopez, Ian R. A. Mackenzie, Mario Masellis, Fodi Massoud, Paige Moorhouse, John C. Morris, Taim Muayqil, Yannick Nadeau, Inger Nennesmo, Jørgen E. Nielsen, Ricardo Nitrini, Sven-Eric Pålhagen, Robert Perry, Gerald Pfeffer, Machiel Pleizier, Steffen Plickert, Gil D. Rabinovici, Philippe H. Robert, Lothar Resch, Gustavo C. Román, Maxime Ros, Pedro Rosa-Neto, Aiman Sanosi, Philip Scheltens, Christian Schmidt, Eric Schmidt, Jean-Paul Soucy, Jette Stokholm, David Summers, Rawan Tarawneh, Louis Verret, Huali Wang, Bengt Winblad, Makoto Yoneda, Xin Yu, Inga Zerr
- Edited by Serge Gauthier, McGill University, Montréal, Pedro Rosa-Neto, McGill University, Montréal
-
- Book:
- Case Studies in Dementia
- Published online:
- 16 May 2011
- Print publication:
- 21 April 2011, pp viii-xiv
-
- Chapter
- Export citation
The global burden of mental disorders: An update from the WHO World Mental Health (WMH) Surveys*
- Ronald C. Kessler, Sergio Aguilar-Gaxiola, Jordi Alonso, Somnath Chatterji, Sing Lee, Johan Ormel, T. Bedirhan Üstün, Philip S. Wang
-
- Journal:
- Epidemiologia e Psichiatria Sociale / Volume 18 / Issue 1 / March 2009
- Published online by Cambridge University Press:
- 11 April 2011, pp. 23-33
-
- Article
- Export citation
-
Aims - The paper reviews recent findings from the WHO World Mental Health (WMH) surveys on the global burden of mental disorders. Methods - The WMH surveys are representative community surveys in 28 countries throughout the world aimed at providing information to mental health policy makers about the prevalence, distribution, burden, and unmet need for treatment of common mental disorders. Results - The first 17 WMH surveys show that mental disorders are commonly occurring in all participating countries. The inter-quartile range (IQR: 25th-75th percentiles) of lifetime DSM-IV disorder prevalence estimates (combining anxiety, mood, externalizing, and substance use disorders) is 18.1–36.1%. The IQR of 12-month prevalence estimates is 9.8–19.1%. Prevalence estimates of 12-month Serious Mental Illness (SMI) are 4–6.8% in half the countries, 2.3–3.6% in one-fourth, and 0.8–1.9% in one-fourth. Many mental disorders begin in childhood-adolescence and have significant adverse effects on subsequent role transitions in the WMH data. Adult mental disorders are found to be associated with such high role impairment in the WMH data that available clinical interventions could have positive cost-effectiveness ratios. Conclusions - Mental disorders are commonly occurring and often seriously impairing in many countries throughout the world. Expansion of treatment could be cost-effective from both employer and societal perspectives
Contributors
-
- By Shamsuddin Akhtar, Greg Albert, Sidney Allison, Muhammad Anwar, Haruo Arita, Amanda Barker, Mary Hanna Bekhit, Jeanna Blitz, Tyson Bolinske, David Burbulys, Asokumar Buvanendran, Gregory Cain, Keith A. Candiotti, Daniel B. Carr, Derek Chalmers, John Charney, Rex Cheng, Roger Chou, Keun Sam Chung, Anna Clebone, Frederick Conlin, Susan Dabu-Bondoc, Tiffany Denepitiya-Balicki, Jeanette Derdemezi, Anahat Kaur Dhillon, Ho Dzung, Juan Jose Egas, Stephen M. Eskaros, Zhuang T. Fang, Claudia R. Fernandez Robles, Victor A. Filadora, Ellen Flanagan, Dan Froicu, Allison Gandey, Nehal Gatha, Boris Gelman, Christopher Gharibo, Muhammad K. Ghori, Brian Ginsberg, Michael E. Goldberg, Jeff Gudin, Thomas Halaszynski, Martin Hale, Dorothea Hall, Craig T. Hartrick, Justin Hata, Lars E. Helgeson, Joe C. Hong, Richard W. Hong, Balazs Horvath, Eric S. Hsu, Gabriel Jacobs, Jonathan S. Jahr, Rongjie Jaing, Inderjeet Singh Julka, Zeev N. Kain, Clinton Kakazu, Kianusch Kiai, Mary Keyes, Michael M. Kim, Peter G. Lacouture, Ryan Lanier, Vivian K. Lee, Mark J. Lema, Oscar A. de Leon-Casasola, Imanuel Lerman, Philip Levin, Steven Levin, JinLei Li, Eric C. Lin, Sharon Lin, David A. Lindley, Ana M. Lobo, Marisa Lomanto, Mirjana Lovrincevic, Brenda C. McClain, Tariq Malik, Jure Marijic, Joseph Marino, Laura Mechtler, Alan Miller, Carly Miller, Amit Mirchandani, Sukanya Mitra, Fleurise Montecillo, James M. Moore, Debra E. Morrison, Philip F. Morway, Carsten Nadjat-Haiem, Hamid Nourmand, Dana Oprea, Sunil J. Panchal, Edward J. Park, Kathleen Ji Park, Kellie Park, Parisa Partownavid, Akta Patel, Bijal Patel, Komal D. Patel, Neesa Patel, Swati Patel, Paul M. Peloso, Danielle Perret, Anthony DePlato, Marjorie Podraza Stiegler, Despina Psillides, Mamatha Punjala, Johan Raeder, Siamak Rahman, Aziz M. Razzuk, Maggy G. Riad, Kristin L. Richards, R. Todd Rinnier, Ian W. Rodger, Joseph Rosa, Abraham Rosenbaum, Alireza Sadoughi, Veena Salgar, Leslie Schechter, Michael Seneca, Yasser F. Shaheen, James H. Shull, Elizabeth Sinatra, Raymond S. Sinatra, Neil Singla, Neil Sinha, Denis V. Snegovskikh, Dmitri Souzdalnitski, Julie Sramcik, Zoreh Steffens, Alexander Timchenko, Vadim Tokhner, Marc C. Torjman, Co T. Truong, Nalini Vadivelu, Ashley Vaughn, Anjali Vira, Eugene R. Viscusi, Dajie Wang, Shu-ming Wang, J. Michael Watkins-Pitchford, Steven J. Weisman, Ira Whitten, Bryan S. Williams, Jeremy M. Wong, Thomas Wong, Christopher Wray, Yaw Wu, Anthony T. Yarussi, Laurie Yonemoto, Bita H. Zadeh, Jill Zafar, Martha Zegarra, Keren Ziv
- Edited by Raymond S. Sinatra, Jonathan S. Jahr, University of California, Los Angeles, School of Medicine, J. Michael Watkins-Pitchford
-
- Book:
- The Essence of Analgesia and Analgesics
- Published online:
- 06 December 2010
- Print publication:
- 14 October 2010, pp xi-xviii
-
- Chapter
- Export citation
Contributors
-
- By Rose Teteki Abbey, K. C. Abraham, David Tuesday Adamo, LeRoy H. Aden, Efrain Agosto, Victor Aguilan, Gillian T. W. Ahlgren, Charanjit Kaur AjitSingh, Dorothy B E A Akoto, Giuseppe Alberigo, Daniel E. Albrecht, Ruth Albrecht, Daniel O. Aleshire, Urs Altermatt, Anand Amaladass, Michael Amaladoss, James N. Amanze, Lesley G. Anderson, Thomas C. Anderson, Victor Anderson, Hope S. Antone, María Pilar Aquino, Paula Arai, Victorio Araya Guillén, S. Wesley Ariarajah, Ellen T. Armour, Brett Gregory Armstrong, Atsuhiro Asano, Naim Stifan Ateek, Mahmoud Ayoub, John Alembillah Azumah, Mercedes L. García Bachmann, Irena Backus, J. Wayne Baker, Mieke Bal, Lewis V. Baldwin, William Barbieri, António Barbosa da Silva, David Basinger, Bolaji Olukemi Bateye, Oswald Bayer, Daniel H. Bays, Rosalie Beck, Nancy Elizabeth Bedford, Guy-Thomas Bedouelle, Chorbishop Seely Beggiani, Wolfgang Behringer, Christopher M. Bellitto, Byard Bennett, Harold V. Bennett, Teresa Berger, Miguel A. Bernad, Henley Bernard, Alan E. Bernstein, Jon L. Berquist, Johannes Beutler, Ana María Bidegain, Matthew P. Binkewicz, Jennifer Bird, Joseph Blenkinsopp, Dmytro Bondarenko, Paulo Bonfatti, Riet en Pim Bons-Storm, Jessica A. Boon, Marcus J. Borg, Mark Bosco, Peter C. Bouteneff, François Bovon, William D. Bowman, Paul S. Boyer, David Brakke, Richard E. Brantley, Marcus Braybrooke, Ian Breward, Ênio José da Costa Brito, Jewel Spears Brooker, Johannes Brosseder, Nicholas Canfield Read Brown, Robert F. Brown, Pamela K. Brubaker, Walter Brueggemann, Bishop Colin O. Buchanan, Stanley M. Burgess, Amy Nelson Burnett, J. Patout Burns, David B. Burrell, David Buttrick, James P. Byrd, Lavinia Byrne, Gerado Caetano, Marcos Caldas, Alkiviadis Calivas, William J. Callahan, Salvatore Calomino, Euan K. Cameron, William S. Campbell, Marcelo Ayres Camurça, Daniel F. Caner, Paul E. Capetz, Carlos F. Cardoza-Orlandi, Patrick W. Carey, Barbara Carvill, Hal Cauthron, Subhadra Mitra Channa, Mark D. Chapman, James H. Charlesworth, Kenneth R. Chase, Chen Zemin, Luciano Chianeque, Philip Chia Phin Yin, Francisca H. Chimhanda, Daniel Chiquete, John T. Chirban, Soobin Choi, Robert Choquette, Mita Choudhury, Gerald Christianson, John Chryssavgis, Sejong Chun, Esther Chung-Kim, Charles M. A. Clark, Elizabeth A. Clark, Sathianathan Clarke, Fred Cloud, John B. Cobb, W. Owen Cole, John A Coleman, John J. Collins, Sylvia Collins-Mayo, Paul K. Conkin, Beth A. Conklin, Sean Connolly, Demetrios J. Constantelos, Michael A. Conway, Paula M. Cooey, Austin Cooper, Michael L. Cooper-White, Pamela Cooper-White, L. William Countryman, Sérgio Coutinho, Pamela Couture, Shannon Craigo-Snell, James L. Crenshaw, David Crowner, Humberto Horacio Cucchetti, Lawrence S. Cunningham, Elizabeth Mason Currier, Emmanuel Cutrone, Mary L. Daniel, David D. Daniels, Robert Darden, Rolf Darge, Isaiah Dau, Jeffry C. Davis, Jane Dawson, Valentin Dedji, John W. de Gruchy, Paul DeHart, Wendy J. Deichmann Edwards, Miguel A. De La Torre, George E. Demacopoulos, Thomas de Mayo, Leah DeVun, Beatriz de Vasconcellos Dias, Dennis C. Dickerson, John M. Dillon, Luis Miguel Donatello, Igor Dorfmann-Lazarev, Susanna Drake, Jonathan A. Draper, N. Dreher Martin, Otto Dreydoppel, Angelyn Dries, A. J. Droge, Francis X. D'Sa, Marilyn Dunn, Nicole Wilkinson Duran, Rifaat Ebied, Mark J. Edwards, William H. Edwards, Leonard H. Ehrlich, Nancy L. Eiesland, Martin Elbel, J. Harold Ellens, Stephen Ellingson, Marvin M. Ellison, Robert Ellsberg, Jean Bethke Elshtain, Eldon Jay Epp, Peter C. Erb, Tassilo Erhardt, Maria Erling, Noel Leo Erskine, Gillian R. Evans, Virginia Fabella, Michael A. Fahey, Edward Farley, Margaret A. Farley, Wendy Farley, Robert Fastiggi, Seena Fazel, Duncan S. Ferguson, Helwar Figueroa, Paul Corby Finney, Kyriaki Karidoyanes FitzGerald, Thomas E. FitzGerald, John R. Fitzmier, Marie Therese Flanagan, Sabina Flanagan, Claude Flipo, Ronald B. Flowers, Carole Fontaine, David Ford, Mary Ford, Stephanie A. Ford, Jim Forest, William Franke, Robert M. Franklin, Ruth Franzén, Edward H. Friedman, Samuel Frouisou, Lorelei F. Fuchs, Jojo M. Fung, Inger Furseth, Richard R. Gaillardetz, Brandon Gallaher, China Galland, Mark Galli, Ismael García, Tharscisse Gatwa, Jean-Marie Gaudeul, Luis María Gavilanes del Castillo, Pavel L. Gavrilyuk, Volney P. Gay, Metropolitan Athanasios Geevargis, Kondothra M. George, Mary Gerhart, Simon Gikandi, Maurice Gilbert, Michael J. Gillgannon, Verónica Giménez Beliveau, Terryl Givens, Beth Glazier-McDonald, Philip Gleason, Menghun Goh, Brian Golding, Bishop Hilario M. Gomez, Michelle A. Gonzalez, Donald K. Gorrell, Roy Gottfried, Tamara Grdzelidze, Joel B. Green, Niels Henrik Gregersen, Cristina Grenholm, Herbert Griffiths, Eric W. Gritsch, Erich S. Gruen, Christoffer H. Grundmann, Paul H. Gundani, Jon P. Gunnemann, Petre Guran, Vidar L. Haanes, Jeremiah M. Hackett, Getatchew Haile, Douglas John Hall, Nicholas Hammond, Daphne Hampson, Jehu J. Hanciles, Barry Hankins, Jennifer Haraguchi, Stanley S. Harakas, Anthony John Harding, Conrad L. Harkins, J. William Harmless, Marjory Harper, Amir Harrak, Joel F. Harrington, Mark W. Harris, Susan Ashbrook Harvey, Van A. Harvey, R. Chris Hassel, Jione Havea, Daniel Hawk, Diana L. Hayes, Leslie Hayes, Priscilla Hayner, S. Mark Heim, Simo Heininen, Richard P. Heitzenrater, Eila Helander, David Hempton, Scott H. Hendrix, Jan-Olav Henriksen, Gina Hens-Piazza, Carter Heyward, Nicholas J. Higham, David Hilliard, Norman A. Hjelm, Peter C. Hodgson, Arthur Holder, M. Jan Holton, Dwight N. Hopkins, Ronnie Po-chia Hsia, Po-Ho Huang, James Hudnut-Beumler, Jennifer S. Hughes, Leonard M. Hummel, Mary E. Hunt, Laennec Hurbon, Mark Hutchinson, Susan E. Hylen, Mary Beth Ingham, H. Larry Ingle, Dale T. Irvin, Jon Isaak, Paul John Isaak, Ada María Isasi-Díaz, Hans Raun Iversen, Margaret C. Jacob, Arthur James, Maria Jansdotter-Samuelsson, David Jasper, Werner G. Jeanrond, Renée Jeffery, David Lyle Jeffrey, Theodore W. Jennings, David H. Jensen, Robin Margaret Jensen, David Jobling, Dale A. Johnson, Elizabeth A. Johnson, Maxwell E. Johnson, Sarah Johnson, Mark D. Johnston, F. Stanley Jones, James William Jones, John R. Jones, Alissa Jones Nelson, Inge Jonsson, Jan Joosten, Elizabeth Judd, Mulambya Peggy Kabonde, Robert Kaggwa, Sylvester Kahakwa, Isaac Kalimi, Ogbu U. Kalu, Eunice Kamaara, Wayne C. Kannaday, Musimbi Kanyoro, Veli-Matti Kärkkäinen, Frank Kaufmann, Léon Nguapitshi Kayongo, Richard Kearney, Alice A. Keefe, Ralph Keen, Catherine Keller, Anthony J. Kelly, Karen Kennelly, Kathi Lynn Kern, Fergus Kerr, Edward Kessler, George Kilcourse, Heup Young Kim, Kim Sung-Hae, Kim Yong-Bock, Kim Yung Suk, Richard King, Thomas M. King, Robert M. Kingdon, Ross Kinsler, Hans G. Kippenberg, Cheryl A. Kirk-Duggan, Clifton Kirkpatrick, Leonid Kishkovsky, Nadieszda Kizenko, Jeffrey Klaiber, Hans-Josef Klauck, Sidney Knight, Samuel Kobia, Robert Kolb, Karla Ann Koll, Heikki Kotila, Donald Kraybill, Philip D. W. Krey, Yves Krumenacker, Jeffrey Kah-Jin Kuan, Simanga R. Kumalo, Peter Kuzmic, Simon Shui-Man Kwan, Kwok Pui-lan, André LaCocque, Stephen E. Lahey, John Tsz Pang Lai, Emiel Lamberts, Armando Lampe, Craig Lampe, Beverly J. Lanzetta, Eve LaPlante, Lizette Larson-Miller, Ariel Bybee Laughton, Leonard Lawlor, Bentley Layton, Robin A. Leaver, Karen Lebacqz, Archie Chi Chung Lee, Marilyn J. Legge, Hervé LeGrand, D. L. LeMahieu, Raymond Lemieux, Bill J. Leonard, Ellen M. Leonard, Outi Leppä, Jean Lesaulnier, Nantawan Boonprasat Lewis, Henrietta Leyser, Alexei Lidov, Bernard Lightman, Paul Chang-Ha Lim, Carter Lindberg, Mark R. Lindsay, James R. Linville, James C. Livingston, Ann Loades, David Loades, Jean-Claude Loba-Mkole, Lo Lung Kwong, Wati Longchar, Eleazar López, David W. Lotz, Andrew Louth, Robin W. Lovin, William Luis, Frank D. Macchia, Diarmaid N. J. MacCulloch, Kirk R. MacGregor, Marjory A. MacLean, Donald MacLeod, Tomas S. Maddela, Inge Mager, Laurenti Magesa, David G. Maillu, Fortunato Mallimaci, Philip Mamalakis, Kä Mana, Ukachukwu Chris Manus, Herbert Robinson Marbury, Reuel Norman Marigza, Jacqueline Mariña, Antti Marjanen, Luiz C. L. Marques, Madipoane Masenya (ngwan'a Mphahlele), Caleb J. D. Maskell, Steve Mason, Thomas Massaro, Fernando Matamoros Ponce, András Máté-Tóth, Odair Pedroso Mateus, Dinis Matsolo, Fumitaka Matsuoka, John D'Arcy May, Yelena Mazour-Matusevich, Theodore Mbazumutima, John S. McClure, Christian McConnell, Lee Martin McDonald, Gary B. McGee, Thomas McGowan, Alister E. McGrath, Richard J. McGregor, John A. McGuckin, Maud Burnett McInerney, Elsie Anne McKee, Mary B. McKinley, James F. McMillan, Ernan McMullin, Kathleen E. McVey, M. Douglas Meeks, Monica Jyotsna Melanchthon, Ilie Melniciuc-Puica, Everett Mendoza, Raymond A. Mentzer, William W. Menzies, Ina Merdjanova, Franziska Metzger, Constant J. Mews, Marvin Meyer, Carol Meyers, Vasile Mihoc, Gunner Bjerg Mikkelsen, Maria Inêz de Castro Millen, Clyde Lee Miller, Bonnie J. Miller-McLemore, Alexander Mirkovic, Paul Misner, Nozomu Miyahira, R. W. L. Moberly, Gerald Moede, Aloo Osotsi Mojola, Sunanda Mongia, Rebeca Montemayor, James Moore, Roger E. Moore, Craig E. Morrison O.Carm, Jeffry H. Morrison, Keith Morrison, Wilson J. Moses, Tefetso Henry Mothibe, Mokgethi Motlhabi, Fulata Moyo, Henry Mugabe, Jesse Ndwiga Kanyua Mugambi, Peggy Mulambya-Kabonde, Robert Bruce Mullin, Pamela Mullins Reaves, Saskia Murk Jansen, Heleen L. Murre-Van den Berg, Augustine Musopole, Isaac M. T. Mwase, Philomena Mwaura, Cecilia Nahnfeldt, Anne Nasimiyu Wasike, Carmiña Navia Velasco, Thulani Ndlazi, Alexander Negrov, James B. Nelson, David G. Newcombe, Carol Newsom, Helen J. Nicholson, George W. E. Nickelsburg, Tatyana Nikolskaya, Damayanthi M. A. Niles, Bertil Nilsson, Nyambura Njoroge, Fidelis Nkomazana, Mary Beth Norton, Christian Nottmeier, Sonene Nyawo, Anthère Nzabatsinda, Edward T. Oakes, Gerald O'Collins, Daniel O'Connell, David W. Odell-Scott, Mercy Amba Oduyoye, Kathleen O'Grady, Oyeronke Olajubu, Thomas O'Loughlin, Dennis T. Olson, J. Steven O'Malley, Cephas N. Omenyo, Muriel Orevillo-Montenegro, César Augusto Ornellas Ramos, Agbonkhianmeghe E. Orobator, Kenan B. Osborne, Carolyn Osiek, Javier Otaola Montagne, Douglas F. Ottati, Anna May Say Pa, Irina Paert, Jerry G. Pankhurst, Aristotle Papanikolaou, Samuele F. Pardini, Stefano Parenti, Peter Paris, Sung Bae Park, Cristián G. Parker, Raquel Pastor, Joseph Pathrapankal, Daniel Patte, W. Brown Patterson, Clive Pearson, Keith F. Pecklers, Nancy Cardoso Pereira, David Horace Perkins, Pheme Perkins, Edward N. Peters, Rebecca Todd Peters, Bishop Yeznik Petrossian, Raymond Pfister, Peter C. Phan, Isabel Apawo Phiri, William S. F. Pickering, Derrick G. Pitard, William Elvis Plata, Zlatko Plese, John Plummer, James Newton Poling, Ronald Popivchak, Andrew Porter, Ute Possekel, James M. Powell, Enos Das Pradhan, Devadasan Premnath, Jaime Adrían Prieto Valladares, Anne Primavesi, Randall Prior, María Alicia Puente Lutteroth, Eduardo Guzmão Quadros, Albert Rabil, Laurent William Ramambason, Apolonio M. Ranche, Vololona Randriamanantena Andriamitandrina, Lawrence R. Rast, Paul L. Redditt, Adele Reinhartz, Rolf Rendtorff, Pål Repstad, James N. Rhodes, John K. Riches, Joerg Rieger, Sharon H. Ringe, Sandra Rios, Tyler Roberts, David M. Robinson, James M. Robinson, Joanne Maguire Robinson, Richard A. H. Robinson, Roy R. Robson, Jack B. Rogers, Maria Roginska, Sidney Rooy, Rev. Garnett Roper, Maria José Fontelas Rosado-Nunes, Andrew C. Ross, Stefan Rossbach, François Rossier, John D. Roth, John K. Roth, Phillip Rothwell, Richard E. Rubenstein, Rosemary Radford Ruether, Markku Ruotsila, John E. Rybolt, Risto Saarinen, John Saillant, Juan Sanchez, Wagner Lopes Sanchez, Hugo N. Santos, Gerhard Sauter, Gloria L. Schaab, Sandra M. Schneiders, Quentin J. Schultze, Fernando F. Segovia, Turid Karlsen Seim, Carsten Selch Jensen, Alan P. F. Sell, Frank C. Senn, Kent Davis Sensenig, Damían Setton, Bal Krishna Sharma, Carolyn J. Sharp, Thomas Sheehan, N. Gerald Shenk, Christian Sheppard, Charles Sherlock, Tabona Shoko, Walter B. Shurden, Marguerite Shuster, B. Mark Sietsema, Batara Sihombing, Neil Silberman, Clodomiro Siller, Samuel Silva-Gotay, Heikki Silvet, John K. Simmons, Hagith Sivan, James C. Skedros, Abraham Smith, Ashley A. Smith, Ted A. Smith, Daud Soesilo, Pia Søltoft, Choan-Seng (C. S.) Song, Kathryn Spink, Bryan Spinks, Eric O. Springsted, Nicolas Standaert, Brian Stanley, Glen H. Stassen, Karel Steenbrink, Stephen J. Stein, Andrea Sterk, Gregory E. Sterling, Columba Stewart, Jacques Stewart, Robert B. Stewart, Cynthia Stokes Brown, Ken Stone, Anne Stott, Elizabeth Stuart, Monya Stubbs, Marjorie Hewitt Suchocki, David Kwang-sun Suh, Scott W. Sunquist, Keith Suter, Douglas Sweeney, Charles H. Talbert, Shawqi N. Talia, Elsa Tamez, Joseph B. Tamney, Jonathan Y. Tan, Yak-Hwee Tan, Kathryn Tanner, Feiya Tao, Elizabeth S. Tapia, Aquiline Tarimo, Claire Taylor, Mark Lewis Taylor, Bishop Abba Samuel Wolde Tekestebirhan, Eugene TeSelle, M. Thomas Thangaraj, David R. Thomas, Andrew Thornley, Scott Thumma, Marcelo Timotheo da Costa, George E. “Tink” Tinker, Ola Tjørhom, Karen Jo Torjesen, Iain R. Torrance, Fernando Torres-Londoño, Archbishop Demetrios [Trakatellis], Marit Trelstad, Christine Trevett, Phyllis Trible, Johannes Tromp, Paul Turner, Robert G. Tuttle, Archbishop Desmond Tutu, Peter Tyler, Anders Tyrberg, Justin Ukpong, Javier Ulloa, Camillus Umoh, Kristi Upson-Saia, Martina Urban, Monica Uribe, Elochukwu Eugene Uzukwu, Richard Vaggione, Gabriel Vahanian, Paul Valliere, T. J. Van Bavel, Steven Vanderputten, Peter Van der Veer, Huub Van de Sandt, Louis Van Tongeren, Luke A. Veronis, Noel Villalba, Ramón Vinke, Tim Vivian, David Voas, Elena Volkova, Katharina von Kellenbach, Elina Vuola, Timothy Wadkins, Elaine M. Wainwright, Randi Jones Walker, Dewey D. Wallace, Jerry Walls, Michael J. Walsh, Philip Walters, Janet Walton, Jonathan L. Walton, Wang Xiaochao, Patricia A. Ward, David Harrington Watt, Herold D. Weiss, Laurence L. Welborn, Sharon D. Welch, Timothy Wengert, Traci C. West, Merold Westphal, David Wetherell, Barbara Wheeler, Carolinne White, Jean-Paul Wiest, Frans Wijsen, Terry L. Wilder, Felix Wilfred, Rebecca Wilkin, Daniel H. Williams, D. Newell Williams, Michael A. Williams, Vincent L. Wimbush, Gabriele Winkler, Anders Winroth, Lauri Emílio Wirth, James A. Wiseman, Ebba Witt-Brattström, Teofil Wojciechowski, John Wolffe, Kenman L. Wong, Wong Wai Ching, Linda Woodhead, Wendy M. Wright, Rose Wu, Keith E. Yandell, Gale A. Yee, Viktor Yelensky, Yeo Khiok-Khng, Gustav K. K. Yeung, Angela Yiu, Amos Yong, Yong Ting Jin, You Bin, Youhanna Nessim Youssef, Eliana Yunes, Robert Michael Zaller, Valarie H. Ziegler, Barbara Brown Zikmund, Joyce Ann Zimmerman, Aurora Zlotnik, Zhuo Xinping
- Edited by Daniel Patte, Vanderbilt University, Tennessee
-
- Book:
- The Cambridge Dictionary of Christianity
- Published online:
- 05 August 2012
- Print publication:
- 20 September 2010, pp xi-xliv
-
- Chapter
- Export citation
25 - Hurricane Katrina
- from Part Six - Case Studies
- Edited by Yuval Neria, Columbia University, New York, Sandro Galea, University of Michigan, Ann Arbor, Fran H. Norris
-
- Book:
- Mental Health and Disasters
- Published online:
- 07 May 2010
- Print publication:
- 20 July 2009, pp 419-440
-
- Chapter
- Export citation
-
Summary
This chapter deals with disaster mental health research in children, and systematically examines the extant literature, focusing on methodological issues. Children represent the ideal age group to study in order to gain insight into the etiology of psychopathology in the aftermath of disaster. Any postdisaster child assessment should necessarily involve a two-step process, including a detailed characterization of the child's exposure and the possible related reactions. The chapter proposes a three-category disaster typology based on the distribution of different types of disaster exposures. The chapter focuses on reports of reactions related to posttraumatic stress disorder (PTSD) in children after mass traumatic events, with studies being reviewed within the context of the proposed typology. Psychiatric disorders observed in children after large-scale traumatic events include a range of disorders, with PTSD and depression being the most commonly assessed.
Contributors
-
- By Jennifer Alvarez, Ananda B. Amstadter, Metin Başoğlu, David M. Benedek, Charles C. Benight, George A. Bonanno, Evelyn J. Bromet, Richard A. Bryant, Barbara Lopes Cardozo, M. L. Somchai Chakkraband, Claude Chemtob, Roman Cieslak, Lauren M. Conoscenti, Joan M. Cook, Judith Cukor, Carla Kmett Danielson, JoAnn Difede, Charles DiMaggio, Anja J.E. Dirkzwager, Cristiane S. Duarte, Jon D. Elhai, Diane L. Elmore, Yael L.E. Errera, Julian D. Ford, Carol S. Fullerton, Sandro Galea, Freya Goodhew, Neil Greenberg, Lindsay Greene, Linda Grievink, Michael J. Gruber, Sumati Gupta, Johan M. Havenaar, Alesia O. Hawkins, Clare Henn-Haase, Kimberly Eaton Hoagwood, Christina W. Hoven, Sabra S. Inslicht, Krzysztof Kaniasty, Ronald C. Kessler, Rachel Kimerling, Richard V. King, Rolf J. Kleber, Jessica Mass Levitt, Brett T. Litz, Maria Livanou, Katelyn P. Mack, Paula Madrid, Shira Maguen, Paul Maguire, Donald J. Mandell, Charles R. Marmar, Andrea R. Maxwell, Shannon E. McCaslin, Alexander C. McFarlane, Thomas J. Metzler, Summer Nelson, Yuval Neria, Elana Newman, Thomas C. Neylan, Fran H. Norris, Carol S. North, Lawrence A. Palinkas, Benjaporn Panyayong, Maria Petukhova, Betty Pfefferbaum, Marleen Radigan, Beverley Raphael, James Rodriguez, G. James Rubin, Kenneth J. Ruggiero, Ebru Şalcıoğlu, Nancy A. Sampson, Arieh Y. Shalev, Bruce Shapiro, Laura M. Stough, Prawate Tantipiwatanaskul, Warunee Thienkrua, Phebe Tucker, J. Blake Turner, Robert J. Ursano, Bellis van den Berg, Peter G. van der Velden, Frits van Griensven, Miranda Van Hooff, Edward Waldrep, Philip S. Wang, Simon Wessely, Leslie H. Wind, C. Joris Yzermans, Heidi M. Zinzow
- Edited by Yuval Neria, Columbia University, New York, Sandro Galea, University of Michigan, Ann Arbor, Fran H. Norris
-
- Book:
- Mental Health and Disasters
- Published online:
- 07 May 2010
- Print publication:
- 20 July 2009, pp xi-xvi
-
- Chapter
- Export citation
Looking Backward, Looking Forward: MLA Members Speak
- April Alliston, Elizabeth Ammons, Jean Arnold, Nina Baym, Sandra L. Beckett, Peter G. Beidler, Roger A. Berger, Sandra Bermann, J.J. Wilson, Troy Boone, Alison Booth, Wayne C. Booth, James Phelan, Marie Borroff, Ihab Hassan, Ulrich Weisstein, Zack Bowen, Jill Campbell, Dan Campion, Jay Caplan, Maurice Charney, Beverly Lyon Clark, Robert A. Colby, Thomas C. Coleman III, Nicole Cooley, Richard Dellamora, Morris Dickstein, Terrell Dixon, Emory Elliott, Caryl Emerson, Ann W. Engar, Lars Engle, Kai Hammermeister, N. N. Feltes, Mary Anne Ferguson, Annie Finch, Shelley Fisher Fishkin, Jerry Aline Flieger, Norman Friedman, Rosemarie Garland-Thomson, Sandra M. Gilbert, Laurie Grobman, George Guida, Liselotte Gumpel, R. K. Gupta, Florence Howe, Cathy L. Jrade, Richard A. Kaye, Calhoun Winton, Murray Krieger, Robert Langbaum, Richard A. Lanham, Marilee Lindemann, Paul Michael Lützeler, Thomas J. Lynn, Juliet Flower MacCannell, Michelle A. Massé, Irving Massey, Georges May, Christian W. Hallstein, Gita May, Lucy McDiarmid, Ellen Messer-Davidow, Koritha Mitchell, Robin Smiles, Kenyatta Albeny, George Monteiro, Joel Myerson, Alan Nadel, Ashton Nichols, Jeffrey Nishimura, Neal Oxenhandler, David Palumbo-Liu, Vincent P. Pecora, David Porter, Nancy Potter, Ronald C. Rosbottom, Elias L. Rivers, Gerhard F. Strasser, J. L. Styan, Marianna De Marco Torgovnick, Gary Totten, David van Leer, Asha Varadharajan, Orrin N. C. Wang, Sharon Willis, Louise E. Wright, Donald A. Yates, Takayuki Yokota-Murakami, Richard E. Zeikowitz, Angelika Bammer, Dale Bauer, Karl Beckson, Betsy A. Bowen, Stacey Donohue, Sheila Emerson, Gwendolyn Audrey Foster, Jay L. Halio, Karl Kroeber, Terence Hawkes, William B. Hunter, Mary Jambus, Willard F. King, Nancy K. Miller, Jody Norton, Ann Pellegrini, S. P. Rosenbaum, Lorie Roth, Robert Scholes, Joanne Shattock, Rosemary T. VanArsdel, Alfred Bendixen, Alarma Kathleen Brown, Michael J. Kiskis, Debra A. Castillo, Rey Chow, John F. Crossen, Robert F. Fleissner, Regenia Gagnier, Nicholas Howe, M. Thomas Inge, Frank Mehring, Hyungji Park, Jahan Ramazani, Kenneth M. Roemer, Deborah D. Rogers, A. LaVonne Brown Ruoff, Regina M. Schwartz, John T. Shawcross, Brenda R. Silver, Andrew von Hendy, Virginia Wright Wexman, Britta Zangen, A. Owen Aldridge, Paula R. Backscheider, Roland Bartel, E. M. Forster, Milton Birnbaum, Jonathan Bishop, Crystal Downing, Frank H. Ellis, Roberto Forns-Broggi, James R. Giles, Mary E. Giles, Susan Blair Green, Madelyn Gutwirth, Constance B. Hieatt, Titi Adepitan, Edgar C. Knowlton, Jr., Emanuel Mussman, Sally Todd Nelson, Robert O. Preyer, David Diego Rodriguez, Guy Stern, James Thorpe, Robert J. Wilson, Rebecca S. Beal, Joyce Simutis, Betsy Bowden, Sara Cooper, Wheeler Winston Dixon, Tarek el Ariss, Richard Jewell, John W. Kronik, Wendy Martin, Stuart Y. McDougal, Hugo Méndez-Ramírez, Ivy Schweitzer, Armand E. Singer, G. Thomas Tanselle, Tom Bishop, Mary Ann Caws, Marcel Gutwirth, Christophe Ippolito, Lawrence D. Kritzman, James Longenbach, Tim McCracken, Wolfe S. Molitor, Diane Quantic, Gregory Rabassa, Ellen M. Tsagaris, Anthony C. Yu, Betty Jean Craige, Wendell V. Harris, J. Hillis Miller, Jesse G. Swan, Helene Zimmer-Loew, Peter Berek, James Chandler, Hanna K. Charney, Philip Cohen, Judith Fetterley, Herbert Lindenberger, Julia Reinhard Lupton, Maximillian E. Novak, Richard Ohmann, Marjorie Perloff, Mark Reynolds, James Sledd, Harriet Turner, Marie Umeh, Flavia Aloya, Regina Barreca, Konrad Bieber, Ellis Hanson, William J. Hyde, Holly A. Laird, David Leverenz, Allen Michie, J. Wesley Miller, Marvin Rosenberg, Daniel R. Schwarz, Elizabeth Welt Trahan, Jean Fagan Yellin
-
- Journal:
- PMLA / Publications of the Modern Language Association of America / Volume 115 / Issue 7 / December 2000
- Published online by Cambridge University Press:
- 23 October 2020, pp. 1986-2078
- Print publication:
- December 2000
-
- Article
- Export citation