697 results
Factors associated with clinician willingness to adopt HPV self-sampling and self-testing for cervical cancer screening
- Luke Brennan, Tiwaladeoluwa Adekunle, Monica Kasting, Michele R. Forman, Victoria Champion, Natalia M. Rodriguez
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e118
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background:
Cervical cancer screening rates in the USA fall behind national targets, requiring innovation to circumvent screening barriers. Cervical cancer screening where human papillomavirus (HPV) testing is performed on vaginal samples collected by the patients themselves (self-sampling) are effective and acceptable, and patient-operated rapid HPV tests (self-testing) are currently under development. It is unclear why there is ambivalence toward HPV self-sampling and self-testing among clinicians, an important stakeholder group. We conducted a mixed convergent quantitative and qualitative study to identify the factors influencing clinicians’ attitudes toward self-sampling and self-testing.
Methods:A survey of Midwest clinicians distributed by professional group media and a market research firm between May and November 2021 was analyzed (n = 248) alongside in-depth interviews with Midwest clinicians from professional groups (n = 23). Logistic regression models examined willingness to support self-sampling and self-testing across respondent characteristics.
Results:We report that family practice physicians and those in rural areas were more willing to adopt HPV self-sampling (adjusted OR (aOR) = 3.16 [1.43–6.99]; aOR = 2.17 [1.01–4.68]). Clinician willingness to support self-testing was positively associated with current use of self-testing for other conditions and negatively associated with performing 10 or more monthly cervical cancer screenings (aOR = 2.02 [1.03–3.95], aOR = 0.42 [0.23–0.78]). Qualitative data contextualize how clinical specialty and experience with self-sampling and self-testing for other conditions inform clinician perspectives.
Conclusion:These data suggest clinician populations most accepting of initiatives to implement self-sampling and self-testing for cervical cancer screening and highlight that experience with other forms of self-testing could facilitate more widespread adoption for cervical cancer.
Characterization of MoS2 films via simultaneous grazing incidence X-ray diffraction and grazing incidence X-ray fluorescence (GIXRD/GIXRF)
- Mark A. Rodriguez, Tomas F. Babuska, John Curry, James J. M. Griego, Mike T. Dugger, Steven R. Larson, Alex Mings
-
- Journal:
- Powder Diffraction , First View
- Published online by Cambridge University Press:
- 13 September 2024, pp. 1-9
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Physical vapor deposited (PVD) molybdenum disulfide (nominal composition MoS2) is employed as a thin film solid lubricant for extreme environments where liquid lubricants are not viable. The tribological properties of MoS2 are highly dependent on morphological attributes such as film thickness, orientation, crystallinity, film density, and stoichiometry. These structural characteristics are controlled by tuning the PVD process parameters, yet undesirable alterations in the structure often occur due to process variations between deposition runs. Nondestructive film diagnostics can enable improved yield and serve as a means of tuning a deposition process, thus enabling quality control and materials exploration. Grazing incidence X-ray diffraction (GIXRD) for MoS2 film characterization provides valuable information about film density and grain orientation (texture). However, the determination of film stoichiometry can only be indirectly inferred via GIXRD. The combination of density and microstructure via GIXRD with chemical composition via grazing incidence X-ray fluorescence (GIXRF) enables the isolation and decoupling of film density, composition, and microstructure and their ultimate impact on film layer thickness, thereby improving coating thickness predictions via X-ray fluorescence. We have augmented an existing GIXRD instrument with an additional X-ray detector for the simultaneous measurement of energy-dispersive X-ray fluorescence spectra during the GIXRD analysis. This combined GIXRD/GIXRF analysis has proven synergetic for correlating chemical composition to the structural aspects of MoS2 films provided by GIXRD. We present the usefulness of the combined diagnostic technique via exemplar MoS2 film samples and provide a discussion regarding data extraction techniques of grazing angle series measurements.
Esketamine in resistant depression: a case report
- L. Carrión Expósito, G. Chauca Chauca, R. Galan Armenteros, M. Rodriguez Lopez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S540-S541
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder is a common psychiatric condition affecting around 264 million people worldwide (WHO: Depression Fact Sheet. [Apr;2021]). Despite pharmacological advances, many patients still do not respond to antidepressant treatment or do so partially.
It is estimated that only 50-70% of patients respond to the initial antidepressant treatment according to the STAR-D study. 15% percent of cases do not respond significantly to various pharmacological and psychotherapeutic attempts (Rush AJ et. STAR*D report. al Am J Psychiatry). The current consensus places resistant depression for a practical approach in one that has been treated with two different antidepressant strategies in adequate doses and time and has not been remitted (Souery D et el, Treatment-resistant depression. J Clin Psychiatry 2006). We present a clinical case of a patient with Major Depressive Disorder, resistant to several therapeutic lines, in which intranasal esketamine was initiated.
ObjectivesThe main objective is to report the result of treatment with esketamine in a clinical case.
MethodsThis work analyze the clinical evolution and reponse of a 62-year-old patient after initiating intranasal esketamine.
This is a patient with a single depressive episode, with no personal psychiatric history of interest that, after exhausting several options of pharmacological and non-pharmacological treatment.
Regulated psychotherapy based on cognitive behavioral therapy was carried out along with different pharmacological strategies according to the recommendations of the main clinical guidelines: antidepressant dose increase, antidepressant change, combination of several antidepressants and potentiation with another drug. We measured clinical changes with MADRS Scale (Montgomery-Asberg Depression Rating Scale) at diferent times.
ResultsFrom the fifth administration of esketamine the patient presented a clear improvement. At three months, the score on the MADRS scale improved markedly and at 6 months, the patient reported euthymia.
Score MADRS:
- Basal 46
- 3 Months 14
- 6 Months 1
As for the adverse effects, the patient presented in all administrations very mild dizziness.
ConclusionsThe use of esketamine is a new therapeutic approach, being fast, safe and well tolerated in patients with depression who do not respond to other treatments (Sapkota A et al. Efficacy and Safety of Intranasal Esketamine in Treatment-Resistant Depression in Adults: A Systematic Review. Cureus.2021 Aug 21;13(8)). In our patient has proven to be effective and fast.
Disclosure of InterestNone Declared
Differences in clinical variables of cervical cancer in women with schizophrenia
- F. Casanovas, F. Dinamarca, S. Oller, A. Trabsa, L. Martínez-Sadurní, R. Rodríguez-Seoane, N. Zabaleta, L. M. Martin, V. Perez-Sola, A. I. Ruiz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S318
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is associated with a reduced life expectancy, not only because of suicide, but also medical causes such as cancer. Standardized mortality for cancer is higher in patients with schizophrenia, specially for lung, breast and colorectal locations (Ni et al, 2019). Other less frequent tumor locations have not been deeply studied.
Thir mortality gap could be related to a delayed diagnosis due to several reasons, such as lower inclusion in screening programs (Solmi et al, 2019). Since cervical cancer has a very efficient screening technique, women with schizophrenia and cervical cancer could have a worse prognosis because of a delayed diagnosis. However, there is a lack of research in this tumor location.
ObjectivesTo analyze clinical differences in women with cervical cancer with and without a diagnosis of schizophrenia.
MethodsWe carried out a retrospective cohort analysis with adult patients from the cancer registry of Hospital del Mar diagnosed between 1997 and 2021. The information was crossed with the Minimum Basic Data Set (MBDS) to identify those cancer patients with a diagnosis of schizophrenia using International Classification of Diseases (ICD) 9 codes 295*. The sociodemographic variables were age and sex. The clinical oncological variables included tumor location, place of first conultation, stage, first treatment intention, vital status and place of decease. We used t-student for continuous data and Chi-squared test for categorical variables. We performed a post-hoc analysis using Bonferroni correction for multiple comparisons to identify specifically which categories were significantly different between groups.
ResultsWe identified 13 women with schizophrenia and cervical cancer, and 1354 women with cervical cancer without schizophrenia. The proportion of this location was higher in the schizophrenia group (8% of all cancers vs. 4.4%; p=0.03). The proportion of diagnoses through screening programm was significantly lower (7.7% vs 14.6%; p=0.04). There was a trend of fewer diagnoses in situ in patients with schizophrenia (30.8% vs 55.6%) and less radical intention as first treatment option (15.4% vs 3.5%) but without statistical significance in both cases. There was a higher proportion of deceased patients in the group with schizophrenia (46.2% vs 15% p=0.002), and also a higher proportion of deaths outside hospital facilities (30.8% vs 6.6%; p=0.003).
Image:
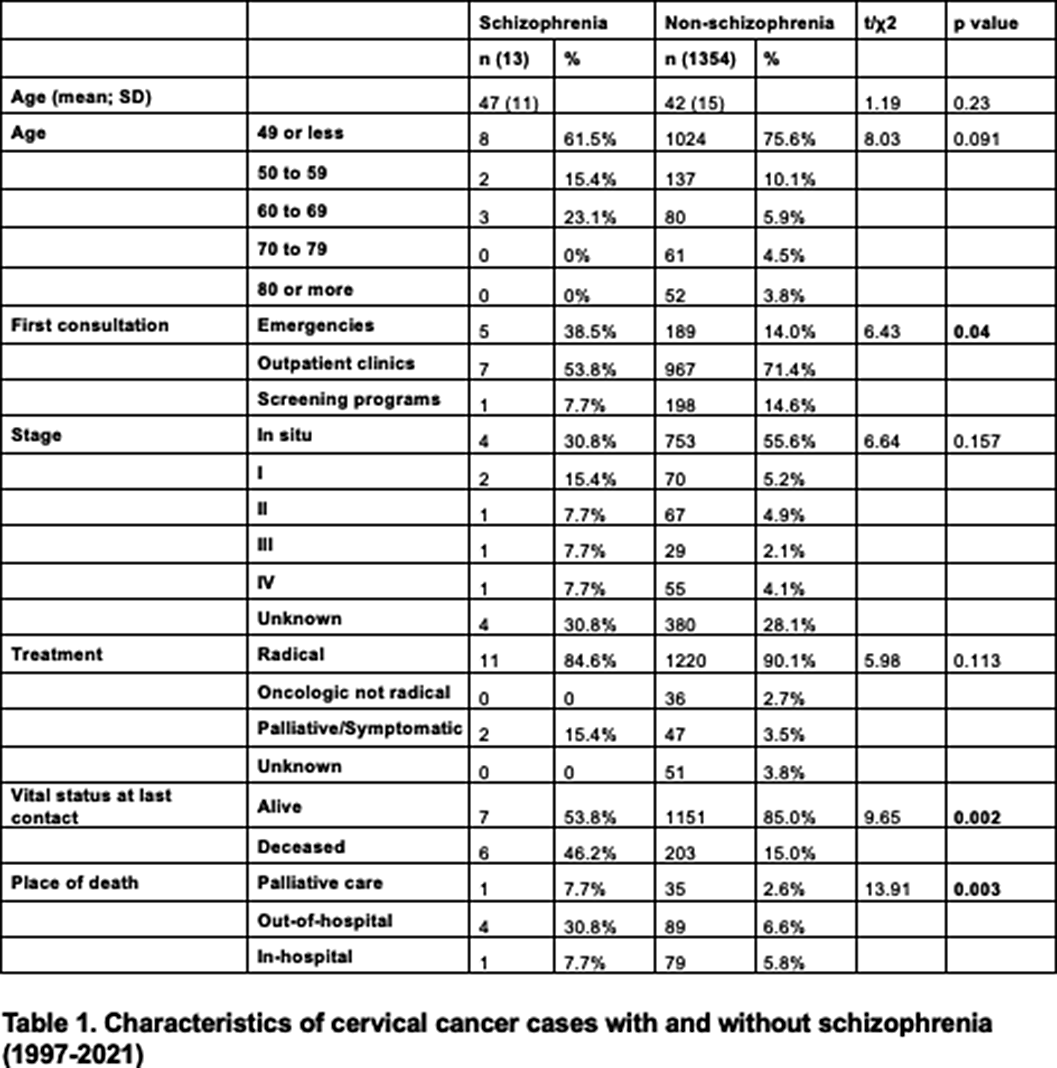 Conclusions
ConclusionsWomen with schizophrenia receive less diagnoses of cervical cancer through screening programs and more in emergency facilities, which could lead to more advanced stages and fewer indication of radical treatments. This ultimately leads to a higher proportion of deaths, and more frequently outside of hospital facilities.
Our data supports the idea that the increased mortality for cancer is related to a delayed diagnosis. Women with schizophrenia need special care to ensure their inclusion in early detection programs for cancer.
Disclosure of InterestNone Declared
Bipolar disorder, Deafness and Culturality in Psychiatric Home Hospitalization: A Clinical Case
- J. Marti Bonany, G. De Iturbe Catania, R. Romar Navia, D. Tolosa Merlos, C. Montserrat Diez, E. Pechuan Martínez, R. Rodriguez Seoane, L. Gil Martinez, D. Garcia Hernandez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S435
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health in the deaf community is a complex issue. Challenges in diagnosis and treatment arise from a lack of experienced interpreters and difficulties in translating Sign Language to spoken language. Deaf individuals, due to auditory limitations, are more vulnerable to abuse, increasing their risk of mental health disorders, including bipolar affective disorder (BPAD). BPAD is a prevalent, debilitating condition with varied prevalence estimates. Managing it is tough due to its lifelong, unpredictable nature. A new approach called Psychiatric Home Hospitalization Unit aims to provide acute mental health care at home as an alternative to hospitalization.
ObjectivesTo show the management of severe bipolar disorder with comorbidity from a Psychiatric Home Hospitalization Unit
MethodsA clinical case of bipolar disorder with deafness attended at the Psychiatric Home Hospitalization Unit of our hospital is presented.
ResultsA 24-year-old deaf woman borned in Pakistan and later moving to Catalonia, she faced educational challenges but ultimately completed her studies with sign language support. Afterward, she struggled to find suitable employment, and her family had a history of bipolar disorder.
She exhibited a sudden change in behavior, characterized by irritability, paranoia, and distrust. Communication was challenging due to her speech difficulties, but assessments using sign language and observation were conducted. Her physical examination was normal, but her speech was disorganized and pressured, suggesting possible auditory hallucinations and thought disturbances. She was hospitalized and diagnosed with bipolar disorder with psychotic features.
During her initial hospitalization, she received lithium, olanzapine, clotiapine and benzodiacepines. After discharge, she continued treatment through a home hospitalization service during almost 4 month. During follow-up she presented a course with high affective instability, rapid cycling alternating brief periods of stability with other presenting manic and mixed features with high disorganization.
Due to the rapid cycling pattern Valproic acid was considered. Valproic acid was introduced up to 700 mg/d (97.1 mcg/mL). Treatment with lithium carbonate 800 mg/d (0.91 mEq/L) was maintained. Previous antipsychotic regimen was changed to quetiapine 400mg/d, olanzapine 5mg/d. Her condition improved significantly with the adjusted treatment regimen. She was discharged to an outpatient service.
ConclusionsDiagnosing and treating bipolar affective disorder (BPAD) in a deaf and mute patient posed unique challenges. The rapid mood cycling pattern and complexity of her case made treatment challenging. Family information and interpreter support were vital. Cultural factors were considered, and home hospitalization was crucial in managing symptoms that lasted over four months.
Disclosure of InterestNone Declared
Relationship between different PANSS cognitive factors and cognition assessed with MCCB in patients with first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, Á. Sánchez-Cabezudo, M. Scala, L. García-Fernández, L. Sánchez-Pastor, D. Rentero, I. Martínez-Gras, M. Caballero, J. M. Espejo-Saavedra, A. Nuñez-Doyle, O. Jiménez-Rodríguez, A. I. Aparicio-León, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S292-S293
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Positive and Negative Syndrome Scale (PANSS) has been used as a universal instrument for clinical assessment of psychopathology in schizophrenia. Different studies have analyzed the factorial structure of this scale and have suggested a five-factor model: positive, negative, excited, depressive, and cognitive/disorganized factors. Two of the most used models are the Marder´s solution and the Wallwork´s one.
ObjectivesThe aim of this work was to study the correlations of the two cognitive factors (Marder and Wallwork) with a cognitive assessment performed with a standard cognitive battery, in a sample of patients with first psychotic episode of schizophrenia.
MethodsSeventy four patients with first psychotic episode of schizophrenia (26.9, SD:7.8 years old; 70.3% male) were included. The cognitive assessment was performed with the MATRICS Consensus Cognitive Battery (MCCB). The MCCB present seven cognitive domains: Speed of processing, Working memory, Attention/Vigilance, Verbal Learning, Visual Learning, Reasoning and Problem Solving, and Social cognition). Pearson correlations were performed between MCCB scores and Marder´s PANSS cognitive factor (P2, N5, G5, G10, G11, G13, G15) and Wallwork´s one (P2, N5, G11).
ResultsCorrelation between MCCB scores and cognitive factors of Marder and Wallwork can be seen in the table.
Marder´s cognitive factor Wallwork´s cognitive factor Speed of processing r = -0.461; p<0.001 r = -0.455; p<0.001 Attention/Vigilance r = -0.414; p<0.001 r = -0.415; p<0.001 Working memory r = -0.449; p<0.001 r = -0.468; p<0.001 Verbal Learning r = -0.511; p<0.001 r = -0.405; p<0.001 Visual Learning r = -0.252; p=0.024 r = -0.254; p=0.029 Reasoning and Problem Solving r = -0.244; p=0.036 r = -0.272; p=0.019 Social cognition r = -0.268; p=0.024 r = -0.202; p=0.091 ConclusionsBoth PANSS cognition factors show a moderate correlations with Speed of processing, Working memory, Attention/Vigilance and Verbal Learning assessed by MCCB. More discrete correlations were found with Visual Learning, Reasoning and Problem Solving, and with Social cognition (in fact, non-significant correlation with Wallwork´s cognitive factor was found).
Acknowledgements. This study has been funded by Instituto de Salud Carlos III (ISCIII) through the project PI19/00766 and co-funded by the European Union.
Disclosure of InterestNone Declared
Clinical experience with once-monthly risperidone ISM in a mental health center. A retrospective study.
- A. Merino Iglesias, N. Rodríguez Ortega, L. Montero Quer, M. R. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S749
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics have undergone a great development in recent years, becoming useful tools to facilitate therapeutic adherence. Once-monthly risperidone ISM is a new way of treatment which has been commercialized in Spain since September 2022.
ObjectivesIn this study we will analyze our clinical experience with this treatment, especially in terms of tolerance and efficacy, during its first year of widespread use.
MethodsLongitudinal retrospective study of monhtly risperidone users in a mental health center in the Autonomous Community of Madrid (Spain), between September 2022 and September 2023.
A sample of 13 patients was selected, collecting both sociodemographic (age, gender) and clinical variables (diagnosis, dose, time elapsed, number of hospital readmissions, adverse effects and monotherapy or combined use). A descriptive analysis of the collected data was then carried out.
ResultsMonthly risperidone was used in 13 patients: 15% (n=2) were women, and 85% (n=11) were male. The mean age of the patients was 43.6 years. The most frequent diganosis of these patients was “psychotic disorders” (84,6%, n= 11), with other diagnoses such as schizoaffective disorder (7,7%, n=1) and obsessive compulsive disorder (7,7%, n=1).
The doses used of risperidone were 100mg every month in 61,5% of patients (n=8) and 75mg in 38,5% of patients (n=5). The mean time since the first administration was 4.35 months.
Concerning monotherapy, 84,6% (n=11) of patients on monthly risperidone were on antipsychotic monotherapy, while 15,4% (n=2) required more than one antipsychotic. Among the switches made to monthly risperidone, 69,2% (n=9) were previously treated with oral risperidone, 15,4% (n=2) were treated with once-biweekly risperidone long-acting injectable, 7,9% (n=1) with oral paliperidone and 7,9% with aripiprazole monthly injectable.
During the study period, hospital readmissions for psychiatric descompensations occurred in one patient (7,9%, n=1), while the rest of the patients (92,1%, n=12) did not present decompensations that required psychiatric admission.
Moderate or severe effects occurred in one patient (7,9%, n=1), in the form of acute dystonia, which led to the interruption of injectable treatment. The rest of the patients (92,1%, n=12)) did not present severe adverse effects. Minor adverse effects appeared in 3 patients (25%); these adverse effects were already present in the previous treatment with oral risperidone and did not condition the suspension of the treatment.
ConclusionsIn the sample analyzed, once-monthly Risperidone ISM had reasonable tolerance levels. Also, it´s shown to be effective in preventing psychotic decompensations and hospital admissions.
Therefore, this new injectable of monthly risperidone represents a therapeutic alternative to consider in order to guarantee therapeutic adherence and improve the quality of life of patients with psychotic symptoms.
Disclosure of InterestNone Declared
Depression: Biological Non-Pharmacological Interventions. A Review.
- F. A. Rodríguez Batista, S. Trufero Miguel, R. Bordón Guerra, A. R. Neyra del Rosario
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S538-S539
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder stands as one of the most significant mental health issues in the general population. It impacts the patients’ quality of life and increases both morbidity and mortality. Response and tolerability to available pharmacological treatments are often inefficient, sometimes requiring extended periods to achieve acceptable remission through combinations or augmentations. Non-pharmacological approaches constitute an element in the therapeutic options for this mental disorder. In recent years, there has been a growing interest in non-pharmacological biological treatment interventions. Among the principal ones are Electroconvulsive Therapy (ECT), Transcranial Magnetic Stimulation (TMS), Deep Brain Stimulation (DBS), and Vagus Nerve Stimulation (VNS).
ObjectivesThe aim of this paper is to review the current available literature to expand our knowledge about biological non-pharmacological treatment in depression, particularly ECT, TMS, DBS, and VNS.
MethodsA qualitative review was conducted over the last 5 years, using the Medline database through PubMed. We selected studies in English or Spanish that met the objectives of the review, excluding references in other languages. The scientific evidence obtained was analyzed and synthesized.
ResultsThere is growing evidence in this area. TMS, whose place in clinical guidelines remains unclear, is a less available treatment but might be considered in patients with moderate to severe depression who cannot receive pharmacological treatment. DBS, which shows good results in treatment-resistant major depressive disorder, achieves response rates greater than 50%. VNS has accumulated studies since its approval for treatment-resistant depression, showing some latency of response but demonstrating improvement persistence for at least two years, although some studies have not clearly shown a benefit. We also found studies demonstrating the effectiveness and favorable cost-benefit balance of ECT.
ConclusionsThis review highlights the importance of increasing knowledge in these types of treatments. They have shown significant progress in recent years. We have a better understanding and use of the technique of ECT, while newer options have gained evidence in effectiveness over these years, with improvements facilitating their use in patients with treatment-resistant depression.
Disclosure of InterestNone Declared
Changing our way of working for a greater integration of mental health patients: The evolution of the Zamora’s Assertive Community Treatment over the last 10 years
- L. Vicente Rodriguez, L. Giménez Robert, L. Carrascal Laso, V. Saez Enguidanos, R. S. Gamonal Limcaoco, M. A. Franco Martin
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S222-S223
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since its beginning in the 1970s in Wisconsin, Assertive Community Treatment (ACT), has been adopted by numerous hospitals worldwide. It improves outcomes for people who are most at-risk of psychiatric hospitalization. The main goal is to provide a global attention with a focus on promoting maximum autonomy and facilitating integration into society. In 2012, the Health Care Complex of Zamora, Spain, adopted this pioneering approach to Mental Health. The main efforts were focused on creating a community network for individuals with severe mental disorders. It embraced a biopsychosocial model of intervention aimed at facilitating patient recovery, giving them tools to create a new life project based on their own autonomy.
ObjectivesThe primary objective of this study was to assess the progress of the Assertive Community Treatment (ACT) since its introduction at the Health Care Complex of Zamora, with a specific focus on analyzing the number of hospitalizations as the dependent variable.
MethodsA quantitative analysis about psychiatry number of hospitalizations was conducted using the database of the Zamora’s Psychiatry Hospitalization Unit. SPSS Statistics for Windows was used to calculate statistical values related to number of hospitalization. The dataset covers de period from 2010 to 2017.
ResultsThe implementation of ACT has resulted in a significant reduction in hospitalizations reaching up to 75% in the Psychiatry Service of Zamora. It has been revealed a decrease from 17107 hospitalizations registered in 2011 to a total reduction to 4869 stances in 2013. A consistent trend in the reduction of hospitalizations has been observed (figure 1).A restructuration of the Hospitalization Unit was performed in order to implement de community model and reduce hospitalizations. Removal of more than 50% of the beds was developed.Besides, there has been implemented a community subunit with the objective of regaining their autonomy after a psychiatric exacerbation.
Image:
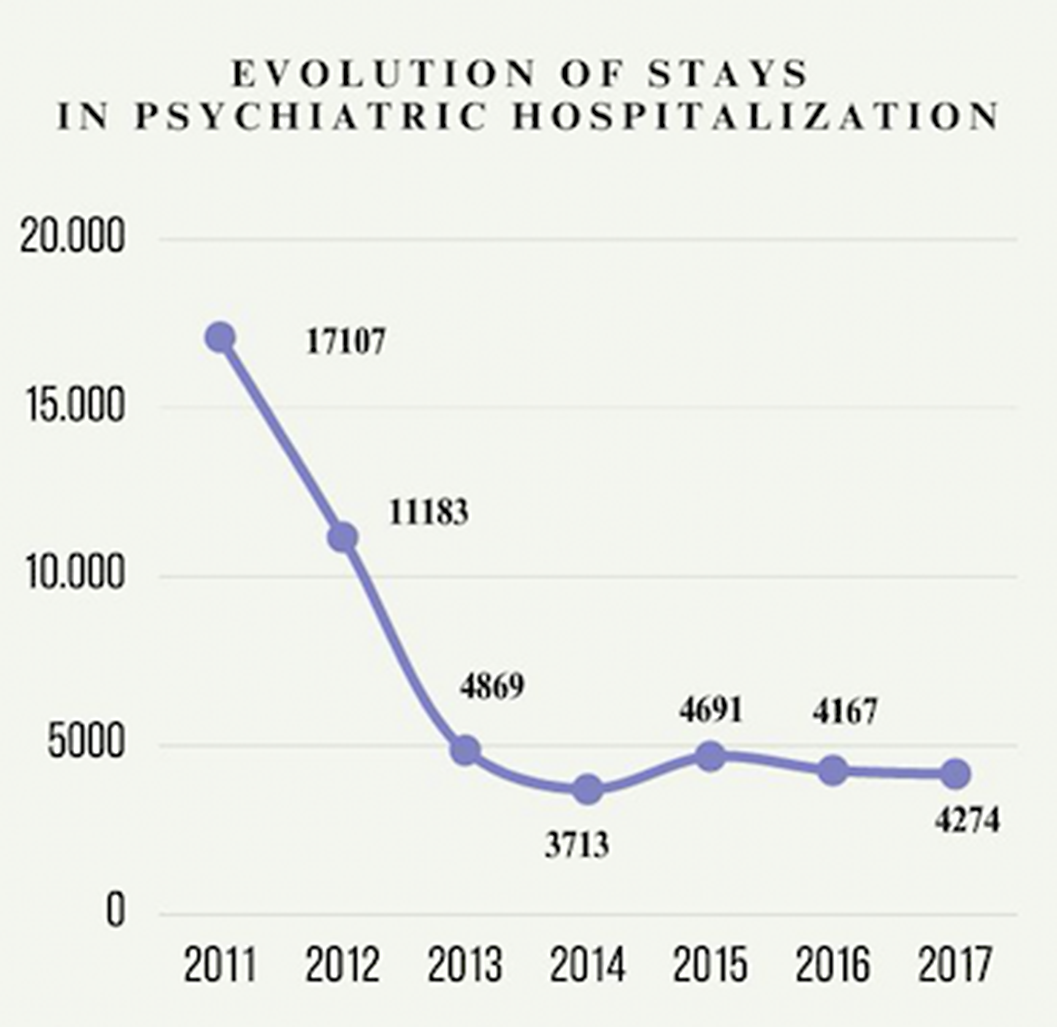 Conclusions
ConclusionsGetting hospitalized in a Psychiatry Unit can have many different socio-laboral consequences. The ACT model has demonstrated a significative reduction in hospitalizations and it has evolved into a support network dedicated the integration of individuals that are usually left behind by society. Moreover, it presents itself as a positive cost-benefit intervention.ACT allows us to envision a future with fewer hospitalization and greater integration of mental health patients into modern society.
It is important to emphasize that the city of Zamora possesses unique characteristics that have facilitated the adaptation of this model. Not only are the rental prices for housing usually affordable, but the city’s small size, which easy walking, allows for easy access to Community Mental Health resources and services.
Disclosure of InterestNone Declared
Gender diversity and autism spectrum disorder in child and youth population
- P. R. Rodríguez, M. M. Grimal, E. E. M. Castellano, F. A. R. Batista, N. M. Pérez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S465
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interest in the co-occurrence of gender dysphoria and autism spectrum disorder has gained prominence in recent years. Gender dysphoria refers to the distress experienced when there is an incongruence between gender identity and sex assigned at birth. On the other hand, autism spectrum disorder is characterized by difficulties in communication and social interaction, as well as restrictive and repetitive patterns of behavior.
ObjectivesThe aim of this paper is to review the current available literature in order to expand our knowledge about gender identity and dysphoria in the population with autism spectrum disorder.
MethodsA qualitative review was conducted over the last 20 years, using the Medline database through PubMed. Combinations of MeSH terms related to gender identity and people with autism spectrum disorder were used, selecting those studies in English, French or Spanish that met the objectives of the review, excluding references in other languages. The scientific evidence obtained was analyzed and synthesized.
ResultsThe development of gender identity of people with autism spectrum disorder can be a complex process. Comparing the general population with the population with autism spectrum disorder, a higher prevalence of gender dysphoria has been evidenced in the population with autism spectrum disorder, and within this group when segmented by gender, greater in women than in men.
ConclusionsThis review highlights the importance of increasing knowledge about sexuality and gender dysphoria in people with autism spectrum disorder in order to facilitate the development, understanding and acceptance of their gender identity and sexual orientation of these people.
Disclosure of InterestNone Declared
Secondary Trauma by Internet Content Moderation: a Case Report
- L. Martinez-Sadurni, F. Casanovas, C. Llimona, D. Garcia, R. Rodriguez-Seoane, J. I. Castro
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S666
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years, a global debate has emerged regarding the protection of Internet users from exposure to harmful content. Content moderation is defined as the organized practice of filtering user-generated content posted on internet, social networks, and media to determine the appropriateness of the content for a site, locality, or jurisdiction. The growing volume of this content along with the psychological impact of this activity have promoted the application of automated approaches based on artificial intelligence and machine-learning. However, the changing characteristics of content, as well as the cultural differences that influence its appropriateness, mean that human moderation of Internet content currently continues to exist. Psychological effects of this activity such as symptoms of post-traumatic stress disorder (PTSD) could represent an example of secondary trauma.
ObjectivesOur aim is to describe a clinical case of post-traumatic stress disorder presenting with specific traumatic exposure idiosyncrasy that could lead to a better consequence characterization of a recent social phenomena such as internet content moderation.
MethodsWe expose the clinical case of a woman with emotional distress who was reffered to our outpatient psychiatric unit in Barcelona in 2022 after five years working as an internet content moderator.
ResultsWe describe the case of a 35-year-old woman without relevant medical, toxicologic or psychiatric record that presents to our out-patient psychiatric clinic with post-traumatic stress disorder after five years of working as an internet content moderator and being exposed to visual traumatic content such as sexual assault and paedophilia. The clinical presentation consisted with one year of recurrent daily panic attacks, intrusive images about the traumatic exposure, intrusive thoughts, insomnia, vivid nightmares, avoidance of exposure to her son, distrust of the environment and intense fear for her son security. The disorder interfered in her capacity to work. The patient received psychological treatment and ISRS (Sertraline) was prescribed, however only partial response was reached with persistence of the majority of symptoms.
ConclusionsThe presented case suggests a temporal and symptom content relationship between the described work exposure and the appearance of emotional distress in a patient without PTSD history. Although previous evidence of secondary trauma in people exposed to indirect traumatic experiences has been reported, for example in healthcare professionals, the exposure to alien trauma through digital exposure as a workactivity is yet to be specifically examined. It is necessary to expand knowledge on the clinical expression of this phenomenon due to the observed recurrence of anxious and depressive symptomatology related to repeated exposure to traumatic content.
Disclosure of InterestNone Declared
“They say I’m crazy, but I’ve lived through hell.”
- N. Molina Pérez, J. Pereira López, M. I. Santana Ortiz, P. Rivero Rodríguez, A. R. N. Del Rosario, M. M. Grimal, V. Acosta Pérez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S524
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Migration has been present in the evolution of human beings throughout history. Economic inequalities give rise to a permanent flow of people trying to improve their lives. In addition, there are people who are forced to seek asylum or refuge due to wars or political violence. Therefore, the migratory flow, gives rise to a clinical scenario in which, the arrival of immigrant people demands an adaptation of the psychiatric paradigm.
ObjectivesThe objective of this paper is to review the international scientific literature published on the impact of the migration process on mental health.
MethodsWe propose a review of the international scientific literature published in recent years on psychiatry and migration.
We present the case of a 27-year-old male, diagnosed with paranoid schizophrenia, who arrived in the Canary Islands after a 2-year migration process from his country of origin (Senegal).
ResultsThe limits between normality and pathology of certain types of behavior vary from one culture to another.
In the case of a patient with a mental disorder who has undergone a migration process, an approach based on the cultural formulation of the case should be made, taking into account the process of adaptation to the culture of the host country, as well as the impact of the culture of origin on the patient’s interpretation of his or her psychopathology.
ConclusionsCulture can influence the acceptance or rejection of a diagnosis and treatment, affecting the course of the disease and recovery.
Therefore, understanding the cultural context in which the disease is experienced is essential for a good diagnostic evaluation and effective clinical management.
Disclosure of InterestN. Molina Pérez: None Declared, J. Pereira López: None Declared, M. I. Santana Ortiz: None Declared, P. Rivero Rodríguez: None Declared, A. R. Del Rosario Grant / Research support from: Jansen Pharmaceuticals, Inc., Consultant of: Jansen Pharmaceuticals, Inc.; Lundbeck, Inc., Employee of: Universidad de Las Palmas de Gran Canaria, Speakers bureau of: Jansen Pharmaceuticals, Inc.; Lundbeck, Inc.; Otsuka Pharmaceutical Co.; Pfizer Inc.; Esteve Pharmaceuticals, S.A.; AstraZeneca Pharmaceuticals LP.; Angelini Pharma S.L.U.; Laboratorios Farmacéuticos ROVI SA., M. Grimal: None Declared, V. Acosta Pérez: None Declared
Mental health impact of fentanyl abuse, a case report
- G. Lorenzo - Chapatte, G. Guerra Valera, P. Marqués Cabezas, L. R. Vázquez, M. Ríos Vaquero, A. Monllor Lazarraga, M. P. Pando Fernández, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, B. Rodríguez Rodríguez, N. Navarro Barriga, M. J. Mateos Sexmero, M. Fernández Lozano, T. Jiménez Aparicio, C. De Andrés-Lobo, M. D. C. Vallecillo Adame, M. D. L. Á. Guillén Soto, L. Sobrino Conde, A. Aparicio Parras
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years, there has been an increase in the prevalence of illicit use of fentanyl and other opioids in the United States population. This has led to an increase in medical, psychopathological and abuse-associated comorbidity, an increase in deaths and a decrease in the age of consumption, and has become a serious emerging problem in young people.
We present the case of an 18-year-old woman from the United States who recently settled in Spain and started a follow-up in Mental Health due to opioid and other substance abuse problems.
ObjectivesTo address the growing problem surrounding the illicit use of fentanyl and opioids as drugs of abuse based on the presentation of the clinical case mentioned above.
MethodsBibliographic search and description of a clinical case of a patient under follow-up by Mental Health at the “Hospital Clínico Universitario de Valladolid”.
ResultsAn 18-year-old woman from the United States who has been living with her father in Spain since the summer of 2023, having moved to Spain due to problems related to substance abuse.
With no previous medical or surgical history and with a history of follow-up in Mental Health in her country of origin for depressive symptomatology, dysfunctional personality traits and abuse of different toxic substances since adolescence.
After a brief and erratic follow-up in Psychiatry for anxious-depressive symptoms reactive to a complex and conflictive relationship with his mother and marked academic difficulties during the first years of adolescence, at the age of 15 he started using cannabis and alcohol, thus beginning a period marked by relationships with marginalized sectors of the population, substance abuse and school failure.
As his cannabis consumption intensified, he began to consume fentanyl prescribed to his mother, as well as other opioids to which he had access illegally, for which reason he had to be admitted twice to detoxification centers without results, which is why his family finally decided to move him to Spain.
ConclusionsIn recent years, fentanyl abuse has become a serious public health problem that is mainly centered in the young population.
High levels of impulsivity and lack of frustration tolerance predispose to the use of illicit substances for elusive purposes.
Substance abuse carries with it not only an important organic comorbidity, but also a marked socio-familial and economic repercussion.
Disclosure of InterestNone Declared
Meta-analysis of generalization reliability of the Montreal Cognitive Assessment (MoCA) questionnaire in cognitive impairment
- R. Fernández Fernández, Á. Izquierdo de la Puente, P. del Sol Calderón, M. Vizcaíno da Silva, A. Rodríguez Rodríguez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S640
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dementia is a syndrome of high prevalence and health impact. The Montreal Cognitive Assessment (MoCA) questionnaire is a screening tool whose use has increased in recent years, especially in cases of mild cognitive impairment. Some studies suggest that its ability to detect cognitive impairment, especially in early or mild stages, seems to be greater than gold-standard instruments (Ciesielska et al., 2016).
ObjectivesWe have performed a meta-analysis of reliability generalization to see if different adaptations and use in different contexts show consistent results.
MethodsWe performed a literature search in PyscINFO and Medline with the terms “Cognitive impairment” AND “internal consistency” AND “Cronbach”, using the following inclusion criteria:
1. Be a study in which the MoCA scale was applied to a population sample.
2. Studies published in the last 10 years.
3. Studies that provide the reliability coefficient or sufficient data to calculate them.
4. Be written in English or Spanish.
We have limited our study to the last 10 years and the English language has given us a total of 19 results in Medline and 132 results in PsycINFO. Subsequently, we completed this search by snowball sampling.
A random effects model was assumed for the statistical calculations and the transformation of our values using the Hakstian and Whalen (1976) proposal. Statistical analysis was performed with the MAJOR package of the Janovi program, based on the R environment.
ResultsWe obtained a mean reliability for the transformed test scores of 0.42 (95% CI: 0.38 - 0.45), as well as high heterogeneity measured by Cochran’s Q statistic and the I2 index, which is attributed after analysis of moderating variables to the geographical adaptation of the questionnaire and the type of patient on whom it is applied. Our Funnel Plot graph indicates that we do not appear to have committed a publication bias.
ConclusionsOur meta-analysis shows high heterogeneity, mainly explained by the population of origin, both geographically (continent) and clinically (presence of primary cognitive impairment or not), with special incidence in those with impairment secondary to other pathologies, mainly neurological. However, we should consider the high probability that we have not included important variables in our analysis that could increase the explanatory power of our model.
Disclosure of InterestNone Declared
Comparison of PTSD prevalence between immigrants and locals with psychotic disorders
- A. Trabsa Biskri, A. Mané, R. Rodríguez, N. Zabaleta, L. Martínez, F. Casanovas, I. Ezquiaga, T. Legido, V. Pérez, B. Amann, A. Moreno
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S97
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Due to the global humanitarian crisis, there has been a significant increase in global immigration.(1)
The migration process typically involves multiple trauma exposures that are sustained over time(2), which may result in an impact on the mental health of these individuals(3), such as posttraumatic stress disorder(3). A recent meta-analysis estimated that 25% of migrants had PTSD(15), which is significantly higher than the 0.2% to 3.8 percent prevalence data found for the general population(4). In addition, a number of meta-analyses indicate an increased risk of psychosis among immigrants(5). Despite this rise, there is a gap in trauma research in non-refugee immigrants, particularly those with psychotic disorders.
ObjectivesTo describe and compare PTSD diagnosis between immigrants and locals recruited from mental health services in Barcelona.
MethodsPatients who have presented, according to DSM-V criteria, one or more non-affective psychotic episodes, were recruited in Acute and Chronic inpatients units at Hospital del Mar (Barcelona) from November 2019 to June 2021, leading to a total sample of 199 patients.
Demographic characteristics of patients, clinical data and main pharmacological treatment were recorded through a questionnaire. Database information was completed with electronic medical records. Global Assessment of Posttraumatic Stress Questionnaire (EGEP-5) was used as an instrument to assess PTSD diagnosis, main trauma nature and PTSD symptoms. Comparative analysis was performed with IBM SPSS Statistics (Chicago INC) using Chi-Square Test for qualitative variables and t-Student test for continuous variables. Covariate adjustment with demographic and clinical variables was performed by ANOVA test. Study received local ethics committee approval “CEIC” (No. 2019/8398/I).
ResultsFrom the total sample of 199 individuals, 98 were immigrants and 98 locals. From the total sample 39 individuals (19.69%) presented PTSD. 32.3% of the immigrants with psychotic disorders presented PTSD compared to 7.1% of the locals with psychotic disorders (F1=19.9, p=0.00). Most traumatic events related to PTSD in immigrants were: “murder of relatives” (33.1%), Physical violence (21.9%) and Terrorism (15.6%) in locals were: “physical violence” (28.6%). Immigrants and locals with psychotic disorders showed similar averages of symptoms, except for avoidance symptoms where locals showed a mean of 5.1 compared to a mean of 3.5 in the immigrant group. Finally, immigrants showed one more functionality affected area by PTSD (5.1) when compared to locals (4) (F7=3.9, p=0.05).
ConclusionsAccording to our results there are important differences in PTSD prevalence between immigrants and locals with psychotic disorders. These findings ought to be taken into consideration for programs that are both clinically and sociopolitically tailored to improve assessment and treatment for this population.
Disclosure of InterestNone Declared
Association between loneliness in childhood and first-episode psychosis
- C. M. Díaz-Caneja, L. Donaire, V. Cavone, Á. Andreu-Bernabeu, J. González-Peñas, M. Díaz-Marsá, R. Rodríguez-Jiménez, Á. Ibáñez, E. Baca-García, J. C. Leza, M. F. Bravo-Ortiz, J. L. Ayuso-Mateos, C. Arango
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S88-S89
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Evidence from observational and genetic studies suggests a bidirectional relationship between loneliness and psychosis. To our knowledge, no previous study has assessed the association between loneliness in childhood and first-episode psychosis (FEP).
ObjectivesWe aimed to assess the association between loneliness in childhood and the odds of FEP and clinical variables of interest (i.e., diagnosis and clinical and functional severity) in FEP and to explore gender differences in this association.
MethodsThis was an observational, case-control study, based on the AGES-CM cohort, a longitudinal prospective study including patients with FEP ages 7-40, their first-degree relatives, and an age- and sex-matched sample of controls in seven university hospitals in the region of Madrid. We assessed loneliness in childhood with the question “Have you ever felt lonely for more than 6 months before the age of 12” and objetive social isolation with the peer relationships item from the childhood subscale of the Premorbid Adjustment Scale. We conducted logistic and linear regression analyses to assess the association between childhood loneliness and i) the odds of presenting a FEP and ii) clinical variables of interest (diagnosis and scores on positive, negative, general, depressive, and manic symptoms and functioning), while adjusting for demographic variables.
ResultsThe study sample comprised 285 patients with FEP (32.6% female, age 24.50 ± 6.2 years) and 546 controls (48.7% female, age 25.93 ± 5.5 years). Loneliness in childhood was associated with increased odds of FEP (adjusted odds ratio; aOR: 2.17, 95% CI [1.40-3.51], p=.002). This association remained significant after controlling for objective social isolation in childhood (aOR:2.70, IC 95% [1.58-4.62], p<.001).
The effect of the association was stronger in females (aOR:4.74, 95% CI [2.23-10.05], p<.001) than in males (aOR:1.17, IC 95% [0.63-2.19], p=.623). In females with FEP, loneliness in childhood was significantly associated with increased odds of receiving a diagnosis of other psychosis (aOR:0.155, 95% CI [0.048-0.506], p=.002) relative to an SSD diagnosis. In the FEP sample, loneliness in childhood was associated with greater severity of positive and affective symptoms and worse functioning.
ConclusionsLoneliness in childhood is associated with increased odds of FEP and clinical variables of interest. This suggests the potential role of this phenotype as an early risk marker for psychosis that could help guide targeted interventions.
Disclosure of InterestC. Díaz-Caneja Grant / Research support from: Instituto de Salud Carlos III (PI17/00481, PI20/00721, JR19/00024), European Union, Consultant of: Angelini, L. Donaire: None Declared, V. Cavone: None Declared, Á. Andreu-Bernabeu: None Declared, J. González-Peñas: None Declared, M. Díaz-Marsá: None Declared, R. Rodríguez-Jiménez: None Declared, Á. Ibáñez: None Declared, E. Baca-García: None Declared, J. C. Leza: None Declared, M. F. Bravo-Ortiz: None Declared, J. L. Ayuso-Mateos: None Declared, C. Arango Grant / Research support from: Madrid Regional Government (R&D activities in Biomedicine S2022/BMD-7216 AGES 3-CM), Instituto de Salud Carlos III, European Union, Consultant of: Acadia, Angelini, Biogen, Boehringer, Gedeon Richter, Janssen Cilag, Lundbeck, Medscape, Menarini, Minerva, Otsuka, Pfizer, Roche, Sage, Servier, Shire, Schering Plough, Sumitomo Dainippon Pharma, Sunovion and Takeda
Euthanasia - A Novel Intricacy for Psychiatry’s Purview?
- Í. Alberdi-Páramo, M. Pérez-Lombardo, J. Pemán-Rodríguez, J. E. Ibáñez Vizoso, R. Á. Baena Mures, L. Niell Galmés, J. Rodríguez Quijano, G. Montero-Hernández
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S332
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Numerous countries, notably within Europe, have sanctioned the practice of euthanasia. Extant legal frameworks meticulously define the extent, essence, and application of euthanasia, encompassing divergent characterizations, explications of entitlements, procedural modalities, and provisions for access. Nonetheless, the precise function of psychiatrists within these legislative contours remains conspicuously nebulous.
ObjectivesThe present inquiry undertakes a comprehensive evaluative review of the euthanasia phenomenon vis-à-vis the intricate tapestry of European legislative paradigms, with an emphasis on elucidating the multifaceted involvement of psychiatry within this evolving landscape.
MethodsA nuanced narrative review is undertaken, encapsulating the contemporary state-of-affairs, fundamental conceptual architectures, the tenets of the Spanish Organic Law 03/2021, and the pharmaceutic armamentarium deployed in the orchestration of euthanasic practices. Additionally, the methodological blueprint employed within a prominent tertiary healthcare institution situated in Madrid is meticulously expounded.
ResultsTo date, euthanasia has garnered legal imprimatur across diverse jurisdictions including, but not limited to, the Netherlands, Belgium, Colombia, Canada, Spain, and New Zealand. The ambit of assisted death and its application to the domain of mental infirmities is meticulously deconstructed. Within the overarching realm of foundational concepts, a rigorous delineation is rendered between euthanasia, medical succor in the throes of mortality, assisted self-termination, facilitated demise, provision of mortal release, judicious calibration of therapeutic enterprise, and the contours of palliative sedation. Distinction between the principal executor and the advisory consultant is rendered salient. The rubric of conscientious objection emerges as an inviolable entitlement of healthcare practitioners enmeshed in the provisionary matrix.
The enduring incumbency of the psychiatrist as a pivotal appraiser of cognitive and volitional faculties holds firm. The conspicuous influence of psychopathological constellations upon the contours of euthanasia eligibility precipitates cogent deliberation.
ConclusionsAs the frontiers of euthanasia expand to encompass an augmented array of legal jurisdictions, this study underscores the increasingly intricate role inhabited by psychiatrists in the matrix of evaluative assessments. The proclivity of mental maladies to exert a substantial gravitational pull upon determinations of eligibility for euthanasia accentuates the exigency for refined explication of roles and responsibilities within this evolving sphere, a clarion call resonant not only within the precincts of psychiatry but reverberating across the broader firmament of medical praxis.
Disclosure of InterestNone Declared
Assessing adherence to plant-rich dietary patterns using metabolic signatures of plant food metabolites
- Y. Li, Y. Xu, M. Le Sayec, T. D Spector, C. Menni, R. Gibson, A. Rodriguez-Mateos
-
- Journal:
- Proceedings of the Nutrition Society / Volume 83 / Issue OCE2 / June 2024
- Published online by Cambridge University Press:
- 03 July 2024, E202
-
- Article
-
- You have access Access
- Export citation
-
Diet is an important modifiable lifestyle factor for human health, and plant-rich dietary patterns are associated with lower risk of non-communicable diseases in numerous studies. However, objective assessment of plant-rich dietary exposure in nutritional epidemiology studies remains challenging. This study aimed to develop and evaluate metabolic signatures of the most widely used plant-rich dietary patterns using a targeted metabolomics method comprising of 108 plant food metabolites.
A total of 218 healthy participants from the POLYNTAKE cohort were included, aged 51.5 ± 17.7 years, with 24h urine samples measured using ultra-high-performance liquid chromatography–mass spectrometry. The validation dataset employed three sample types to test the robustness of the signature, including 24h urine (ABP cohort, n = 88), plasma (POLYNTAKE cohort, n = 195), and spot urine (TwinsUK cohort, n = 198). Adherence to the plant-rich diet was assessed using a priori plant- rich dietary patterns. A combination of metabolites that evaluates the adherence and metabolic response to a specific diet was identified as metabolic signature. We applied linear regression analysis to select the metabolites significantly associated with dietary patterns (adjusting energy intake), and ridge regression to estimate penalized weights of each candidate metabolite. The correlation between metabolic signature and the dietary pattern was assessed by Spearman analysis (FDR < 0.05).
The metabolic signatures consisting of 42, 22, 35, 15, 33, and 33 predictive metabolites across different subclasses were found to be associated with adherence to Amended Mediterranean Score (A-MED), Original MED (O-MED), Dietary Approaches to Stop Hypertension (DASH), Mediterranean-DASH Intervention for Neurodegenerative Delay (MIND), healthy Plant-based Diet Index (hPDI) and unhealthy PDI (uDPI), respectively. The overlapping and distinct predictive metabolites across six dietary patterns predominantly consisted of phenolic acids (n = 38), including 14 cinnamic acids, 14 hydroxybenzoic acids, seven phenylacetic acids, and three hippuric acids. Six metabolites were included in all signatures, including two lignans: enterolactone-glucuronide, enterolactone-sulfate, and four phenolic acids: cinnamic acid, cinnamic acid-4'-sulfate, 2'- hydroxycinnamic acid, and 4-methoxybenzoic acid-3-sulfate. The established signatures were robustly correlated with dietary patterns in validation dataset (r = 0.13 - 0.40, FDR < 0.05).
We developed and evaluated a set of metabolic signatures that robustly reflected the adherence and metabolic response to plant-rich dietary patterns, suggesting the potential of these signatures to serve as an objective assessment of free-living eating habits.
Investigating nutritional status and body composition in children with cerebral palsy; the Eat, Sleep Play-CP study
- M. Copeland, R. Diaz-Rodriguez, N.S. Hill, F.E. Lithander, S.A. Williams
-
- Journal:
- Proceedings of the Nutrition Society / Volume 83 / Issue OCE1 / April 2024
- Published online by Cambridge University Press:
- 07 May 2024, E186
-
- Article
-
- You have access Access
- Export citation
-
Cerebral palsy (CP), or to use the Te Reo term “Hōkai Nukurangi”, is an umbrella name for a group of permanent neurodevelopmental disorders, affecting movement and posture(1), and is the most common childhood onset physical disability globally. The available literature on the nutritional status of children with CP describes high rates of malnutrition, however data appears to be skewed towards children of higher levels of impairment impacting functional independence. Less is known about the nutritional status of children with lower levels of impairment. The aim of the “Eat, Sleep, Play-CP” study was to evaluate total energy intake, total protein intake and the timing of protein intake in relation to physical activity for children with CP across all functional levels living in Aotearoa New Zealand. Children with CP aged 5-12 years were invited to participate in an observational assessment of dietary intake using parent reported 24-hour dietary recall (Intake 24) on three non-consecutive days, accompanied by a questionnaire capturing self-reported sleep and physical activity patterns. Body composition was assessed via whole body dual energy X-ray absorptiometry scan. Nine participants (6 males, median age: 10 years, n = 2 Māori), across Gross Motor Function Classification System levels I-IV, and Eating and Drinking Classification System levels I-III took part in the study. The median total energy intake was 7267kJ/d (range 5355-10731.96kJ/d), and median protein intake was 67g/d (range 49-111g/d). According to the Nutrient Reference Values for Australia and New Zealand (NRV)(2), 3 of the 9 participants (33%) were within the recommended range for energy intake according to their age and reported physical activity levels. Of the other 6, 4 were below and 2 were above the recommended ranges. All 9 met the recommended protein intake (NRV). Participants had a median percentage body fat of 40% (range 20-46%), and non-fat mass of 58% (range 52-76%). Five participants fell within the overweight or obese range for their age and sex, three of whom were within the recommended range of total energy daily intake according to NRVs. This outcome may indicate that for some children with CP, recommendations could be over-estimating the actual requirements. These early results may bring in to question current practice around guidance for energy intake requirements for children with CP and their whānau to support healthy body composition. Further investigations are needed to establish whether specific energy intake guidelines are required for children with CP.
More dietary advice may be needed to support healthy body composition for children with cerebral palsy in Aotearoa New Zealand
- R. Diaz-Rodriguez, M. Copeland, N.S. Hill, F.E. Lithander, S.A. Williams
-
- Journal:
- Proceedings of the Nutrition Society / Volume 83 / Issue OCE1 / April 2024
- Published online by Cambridge University Press:
- 07 May 2024, E168
-
- Article
-
- You have access Access
- Export citation
-
The available literature on the nutritional status of children with cerebral palsy (CP) worldwide has identified high rates of malnutrition, specifically undernutrition(1). However, there is a current lack of clear CP-specific dietary guidelines for children with CP across all functional levels. Standard reference tools such as estimated energy requirement (EER) and recommended dietary intake (RDI) may overestimate requirements in children with CP, especially those with reduced mobility and activity levels. Furthermore, for children with severe CP, body composition data indicates higher risks of obesity and obesity-related conditions(2). There can be a wide range of functional abilities, classifiable with tools such as the Gross Motor Function Classification System (GMFCS) and the Eating and Drinking Ability Classification System (EDACS). The majority of nutrition-related CP literature focuses on children requiring assistance for feeding (EDACS IV-V) with little information available for children with higher levels of functional independence. The aim of this study was to determine whether children with CP had received any prior dietary guidance for healthy body composition and to summarise the type of advice received. Children aged 5-12 years and their whānau were invited to participate in a study where a purpose-developed questionnaire captured their history of receiving tailored dietary recommendations for CP. Body composition was assessed via whole-body dual-energy X-ray absorptiometry scan. Nine participants (6 males, median age: 10y, n = 2 Māori), across GMFCS levels I-IV and EDACS levels I-III took part in the study. Out of 9 children, 5 (55%) indicated that their child had never received dietary advice, 3 of whom were classified as obese or overweight based on growth chart percentiles using their measures of body fat percentage, 1 was classified as underweight and 1 was within the healthy ranges. Of the 4 who had previously received advice, its nature was reported as in support of weight gain (n = 3), and weight loss (n = 1). All 4 received dietary advice from a dietitian and 1 reported some additional advice from a pediatrician and/or orthopedic doctor. Two of the children who had received dietary advice fell within a healthy body fat percentage based on the growth chart percentiles at the time of the study, while the other two were classified as overweight or obese. The results indicate the importance of developing clear dietary guidance for children with CP which may differ from that for typically developing children, particularly depending upon CP subtype diagnosis and functional level, in order to support healthy body composition.



