3294077 results
Concurrent Gender Dysphoria/Incongruence and Autism Spectrum Disorder, a literature review
- N. Clementi
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S479
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies have found that ASD (Autism Spectrum Disorder) and GD (Gender Dysphoria by DSM-V)/GI (Gender Incongruence by ICD-11) tend to co-occur, and in recent years the interest and publications on this comorbidity has increased rapidly.
ObjectivesTo review the prevalence of ASD in individual with a diagnosis of GD/GI.
To better tailor and improve care offered in the National Health Service (NHS) Gender Identity Clinics (GICs) throughout the UK.
MethodsSystematic literature review was conducted via Pub Med, MEDLINE and PsycINFO by the author, for all English-language articles published between 2018 and 2023, containing keywords as ASD, GD (Gender Dysphoria), GI (Gender Incongruence), transgender, autistic traits, autism, gender diversity, gender variance.
ResultsRate of people with ASD appear to be higher in people accessing Gender Identity Clinics (GICs) than in the general population. Results from this literature review show increased prevalence of GD and GI in ASD population.
ConclusionsThis comorbidity has highlighted the importance of better tailor transgender healthcare services for people with neurodevelopmental conditions and neurodiversity, to avoid delay in ASD individuals accessing care and gender affirming medical treatments. Services should strive to provide an effective and equitable service. It is also important to better identify potential barriers for ASD people in accessing gender care. Literature also shows the people with ASD have more difficulties in communicating and describing their gender narrative and to express their wishes for gender treatments. Symptoms including problems in communications and social skills, obsession and rigidity can also impact their assessment of GD/GI in gender identity services. Some studies showed that for individuals who have concurrent ASD and GD/GI, assessment in GICs may be extended to better review their wishes for gender identity and for gender affirming treatment. Further research is needed to better investigate and understand factors explaining the relationship between ASD and gender diversity. There is still limited research in the real life experiences of gender diverse and autistic people. There is also a need to improve Gender reassignment protocol nationally to better care for individual with ASD and GD/GI throughout GICs in the UK.
Disclosure of InterestNone Declared
Assessing the Impact of the Different Psychiatric Disorders on the Profiles of Psychiatric Hospitalization: A descriptive study in a Greek Hospital
- G. N. Porfyri, P. Papadopoulou, M. V. Karakasi, A. Vlachaki
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S573
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The prevalence of psychiatric re-admission ranges from 15% to 60%, escalating even more in the first year after admission, affecting the patients’ quality of life. Furthermore, the diagnosis of psychotic or affective disorders represents a risk factor of psychiatric re-admission, highlighting the diagnosis impact to the “profile” of psychiatric hospitalization.
ObjectivesTo compare the different “Hospitalization Profiles” in association to the patients’ diagnostic categories.
MethodsOverall, 1,633 records of psychiatry inpatients were examined retrospectively throughout the 10-year records of the Psychiatry Department of Papanikolaou General Hospital in northern Greece. The research was conducted between 2013 and August 2023. The sample was divided into subgroups according to gender, diagnoses - according to the International Classification of Diseases (ICD-10)-, and year of hospitalization. A bivariate analysis was performed to examine relationships between the variables: (a.) place of residence; (b.) age; (c.) type of admission; (c.) hospitalization duration; (d.) number of lifetime hospitalizations; (e.) lifetime prosecutor’s orders for coercive examination; (f.) lifetime suicide attempts.
ResultsDevelopmental disorders (F80-89) stood for the youngest average age of hospitalization (26 years) and lowest average hospitalization duration (7 days). Neurodegenerative disorders (F00-09) represented the diagnostic category with the oldest mean age of hospitalization (66 years). Intellectual disorders (F70-79) yielded the longest average hospitalization duration (21 days). Patients with intellectual disorders were found to be facing homelessness at a higher rate (4.76%) than patients of any other diagnostic entity (p=0.096). Psychotic and substance use disorder patients obtained equivalently (p=0.18) the highest rates of coercive hospitalizations (63% and 71%, respectively); compared to other diagnostic categories (p=0.0008). Dual diagnosis and anxiety disorders projected equivalently (p=0.9) the highest rate of premature voluntary discharge (6.9% and 6.4%, respectively). Dual diagnosis, personality disorders, and affective disorders also recorded the highest rates of suicidality (11-15%; with no significant statistical difference among the three diagnostic entities p>0.1) among hospitalized patients of all diagnostic categories (p<0.05).
ConclusionsInterestingly, the study’s results reveal the pathologies of the Greek society, with the most representative example being this of patients suffering from intellectual disorders simultaneously presenting the highest risk of homelessness. Further studies are needed, focusing on the sub-populations of psychiatric patients as well as their status in terms of social security, health care providing, quality of life and life expectancy.
Disclosure of InterestNone Declared
Pregnancy enhances facial recognition of anger: Transition from early to late pregnancy
- F. Minami, R. Iwata, H. Nishida, S. Kudo, M. Yamagishi, K. Kamiya, M. Mimura, J. Hirano, B. Yamagata
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S809
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pregnancy and the postpartum period involve several physiological adaptations crucial for offspring care. Recent research has highlighted reproduction-related brain plasticity in human mothers. Associations with aspects of maternal caregiving suggest adaptive changes that facilitate a woman’s transition to motherhood. However, the dynamic changes that affect a woman’s brain are not merely adaptive, and they likely confer a vulnerability for the mental disorders. To elucidate the pathophysiology of psychiatric problems that occur during the perinatal period, gaining insights into the physiological changes in brain function due to pregnancy is crucial.
ObjectivesAlthough it has been hypothesized that pregnancy enhances social cognitive functions in mothers to adapt to the offspring care, there are few reports to support this hypothesis. This study aims to investigate whether social cognitive functions change during the first pregnancy, with a focus on maternal adaptation to offspring care.
MethodsThe study included a first pregnancy group and a never-pregnant control group. We conducted a prospective study comparing pregnant women between two-time points (T1, T2); at less than 21 weeks of gestation [T1] and those after 30 weeks of gestation [T2]. To assess the effects of pregnancy and gestational age (< 21 weeks or 30 weeks or more), both the control (never-pregnant) group and pregnant group were evaluated at two time points with similar intervals. The Emotion Recognition Task [ERT] of the Cambridge Neuropsychological Test Automated Battery (CANTAB) was performed to examine the emotion recognition of six basic emotions in facial expressions. We analyzed a cohort of 26 participants in the pregnant group and 25 in the control group. We performed a two-way repeated measures analysis of variance with pregnancy status and gestational period (T1, T2) as independent variables.
ResultsSignificant interactions between group and time points (T1, T2) were observed only for Unbiased Hit Rate Anger (p<0.01); facial recognition accuracy for anger increased with the progression of pregnancy. There were no significant interactions for Unbiased Hit Rate Sadness, Happiness, Fear, Disgust, or Surprise.
ConclusionsThis is the first study to demonstrate that facial recognition of anger enhances with the progression of pregnancy, utilizing never-pregnant women as a never-pregnant control group. The results of this study contribute to the physiological effects of pregnancy on the brain and cognitive function and have potential for further study of perinatal mental health problems.
Disclosure of InterestNone Declared
Psychiatric disorder in prolonged post-concussive syndrom : clinical assessment, physiopathology and management review of the literature
- I. Bouguerra, A. Touiti, A. Hajri, A. Maamri, H. Zalila
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S497
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
According to the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), post concussive syndrome (PCS) is given a diagnosis of either major or mild neurocognitive disorder (NCD) due to traumatic brain injury TBI. However Persistent post-concussion symptoms (PPCS) are more complex, and typically involve multidisciplinary assessment and management. The symptoms are varied, non-specific and the therapeutic process is defiant for psychiatrist.
ObjectivesTo investigate the semiology of persistent post-concussion syndrome (PPCS) and the therapeutic challenges it poses.
MethodsA literature review was made on Pubmed, Google Scholar and Cochrane library using keywords: “post-concussive syndrome”,”psychiatric disorder”, “depression”,”post-traumatic stress disorder”,”treatment”, “physiopathology”.
ResultsThe physiopathology of persistent PCS is controversy.The Symptoms are due to the Concept of “Symptom Generators” which results from the alterations in neurophysiology and neuropathology secondary to the injury, and pre- or post-injury psychological factors physiological concussion. The Global cerebral metabolic disturbance, the autonomic nervous system dysfunction and the cerebral blood flow dysregulation induce biochemical cascade,excitotoxic reaction and immunotoxicity.
Clinical diagnoses associated with PPCS are:Major depressive disorder,Post traumatic stress disorder,Anxiety disorder,Substance abuse disorder,Psychotic disorder and Antisocial personality disorder. For the non pharmacological management: A systematically early information and a graded physical exercise in addition to other treatment are essential.
Antidepressant, benzodiazepine and mood-stabilizer are the most recommended treatments for psychiatric symptoms. Atypical neuroleptics are indicated in delirant disorder, behavior disorder and antisocial personality disorder.Some studies suggest the methylphenidate and biperiden to treat several cognitive impairment and severe behavior disorder.
Conclusions(PPCS) is far from being a subjective complaint by patients. It is a complex clinical entity that groups symptoms that overlap with other psychiatric diagnoses, such as depression, post-traumatic stress disorder, and mood disorders. Early neuropsychiatric assessment and personalized pharmacological and psychotherapeutic treatment are essential factors in the prognosis of the disease.
Disclosure of InterestNone Declared
Pros and cons of alternative therapy omega-3 fatty acids during pregnancy and lactation for mental problems
- L. Boronin, I. Nastas
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S803
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Fatty acids omega-3 are irreplaceable. They stabilize cell membranes, nerve impulses, homeostasis, immune reactions, the birth process, the psycho-emotional state of the fetus-mother dyad. Correlations between adequate dietary intake of omega-3 and cognitive health have been described in detail. According to the literature, docosahexaenoic acid is associated with the synthesis of serotonin, dopamine, acetylcholine, glutamate, neuroprotective and anti-apoptotic action, has antidepressant effect. Omega-3 makes up 60% of neuronal membrane phospholipids. Under clinical aspect,according to publications, fish oil reduces the risk of preterm birth by 44%.
ObjectivesThe aim is to study the risks and benefits of using omega-3 during pregnancy and lactation in patients with mental disorders.
MethodsComparative analysis of evidence-based scientific publications for the use of omega-3 fatty acids in pregnancy and lactation.
ResultsThe body level of omega-3 depends on the quantitative intake from food, as well as gene polymorphism and age. For pregnant and lactating women are recommended 200-300 mg per day or about 300 g per week from food. Deficiency of omega-3 (protectins) affects the processes of myelination, neurogenesis, synaptogenesis, the metabolism of neurotransmitters, cell differentiation, neuronal migration and inflammatory responses.
ConclusionsThere are many probably mechanisms of action of omega-3, namely: Enhances peroxisomal oxidation, reduces the synthesis of triglycerides in the liver; inhibits plasma acyltransfrerase. Omega-3 acts on phospholipids of the cell membranes of the nervous system and retina, their adequate functioning, improve psychomotor development of newborns. It was found the effect of decreasing the levels of cytokines and depressive symptoms, as well the risk of food allergies and depression. In conclusion, in adequate doses, omega-3 fatty acids seems to be useful in deficiencies and for prophylactic purposes in pregnancy and lactation.
Keywordsomega- 3 fatty acids, pregnancy, lactation, mental disorders.
Disclosure of InterestNone Declared
What link between violence against women and self-esteem?
- M. Abdelkefi, R. Feki, A. Turki, I. Gassara, N. Smaoui, S. Omri, N. Charfi, L. Zouari, J. Ben Thabet, M. Maalej Bouali, M. Maalej
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S804
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Violence against women is a public health problem worldwide and a violation of human rights. It affects women’s lives due to its potential short-, medium- or long-term physical and psychological consequences.
ObjectivesThe aim of our study is to explore the link between violence against women and self-esteem.
MethodsA descriptive cross-sectional study was conducted from March to August 2023 among Tunisian women consulting in three health care centers in Sfax, Tunisia. We have included women victims of violence (psychological, physical, sexual, and economic). We have used a semi-structured interview and the Rosenberg scale to determine the quality of self-esteem.
ResultsAmong one hundred interviewed women, fifty-four women who had reported being violence victims were included in our study. The mean age of the participants was 44 years with the majority being married (87 %). Only 29.6% had a high school level and 51.9% had a profession. A total of 29.6% had a low socioeconomic status.
We found that 79.6% are victims of domestic violence (57.4% being victims of spousal violence). Psychological violence seemed to be the most frequent type (59.3%).
Almost all those who were abused (90.6%) experienced psychological (emotional) violence.
The mean score of the Rosenberg self-esteem scale was 31.54.
Self-esteem was very low in 16.7%, low in 37%, medium in 18.5%, and high in 27.8% of the women.
A statistically significant association was found between being a victim of spousal violence and low self-esteem (p=0.032). The semi-structured interview demonstrates that women with low self-esteem are more likely to accept violence.
ConclusionsThese results justify the implementation of screening and support programs for women victims of violence to improve their self-esteem.
Disclosure of InterestNone Declared
The impact of climate change on mental health
- A. Heinz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S1
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
Climate change has a profound impact on mental health, supported by meta analytic evidence. For every degree temperature increase, there is a statistical increase in mental health problems by about 0.9%. The direct association between catastrophic events such as hurricanes or flooding and traumatization or negative mood states is evident. However, there are also interactions between pollution or heat islands in urban contexts and stress associated mental disorders, and there are indirect interactions e.g. between loss of agricultural space, poverty, displacement and mental health challenges. We provide an overview regarding direct and indirect effects of climate change on mental health and discuss possible interventions on the health care system.
Disclosure of InterestNone Declared
Text4Hope: An e-Mental Health Tool for Mitigating Psychological Symptoms among Young Adults
- A. Belinda, R. Shalaby, W. Vuong, S. Surood, A. Greenshaw, A. Gusnowski, Y. Wei, V. I. O. Agyapong
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S61
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Chronic stress, anxiety, and depression can interfere with young adults’ everyday function, academic achievement, and interpersonal relationships. Interventions aimed at preventing the deterioration or possibly onset of these mental disorders among young people are timely.
ObjectivesTo assess the impact of a supportive text messaging program (Text4Hope) on the psychological well-being of young adults.
MethodsThis study adopted both longitudinal and naturalistic controlled trial designs. Longitudinal study: compared baseline and 6th week outcomes in the same group of young adult subscribers. Naturalistic controlled study: compared clinical parameters in two groups of Text4Hope young adult subscribers: (i) intervention group (IG), subscribers who received once-daily supportive text messages for 6-weeks and completed 6th-week evaluation between 26 April and 12 July 2020, and (ii) control group (CG), subscribers who joined Text4Hope the same time frame, completed a baseline survey and were yet to receive text messages. The prevalence and severity of moderate-high stress, anxiety, and depression was measured using standardized scales. Inferential statistics, including the t-test, McNemar test, chi-square, and binary logistic regression analyses, were used to evaluate the differences in the prevalence and severity of the psychological symptoms.
ResultsLongitudinal study: subscribers who completed both the baseline and 6th-week surveys, had significant reduction in the prevalence of moderate-high stress (8%) and likely GAD (20%) from baseline to six weeks. The largest reduction in mean scores was for the GAD-7 scale (18.4%). Naturalistic study: significantly lower prevalence for likely Moderate Depressive Disorder (25.2%) and suicidal thoughts/thoughts of self-harm (48.4%), with a small effect size in the IG compared to CG.
Image:
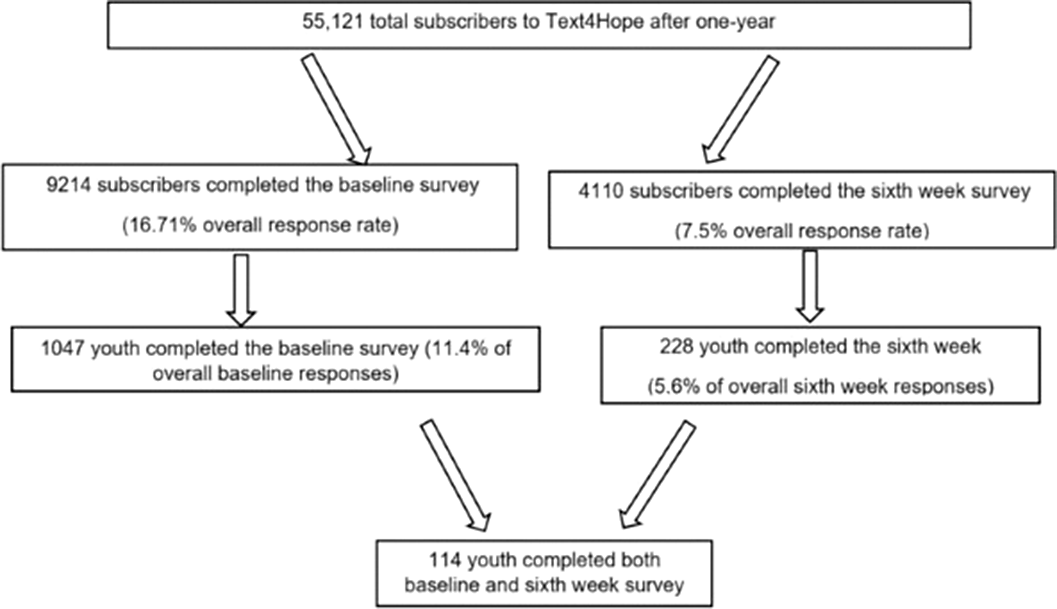 Conclusions
ConclusionsTheText4Hope program has been demonstrated as an effective e-mental health tool for mental health support for young adult subscribers. This is particularly encouraging, as young adults have already adapted to SMS text messaging and texting. Therefore, this mode of intervention can be used to supplement existing treatments for psychological problems impacting young adults. In addition, the cost effectiveness and easy scalability of supportive text message interventions mean that policymakers and governments can quickly implement similar programs as part of national youth suicide prevention strategies.
Disclosure of InterestNone Declared
The Delicate Balance: Aptitude of Physicians with Psychiatric diseases
- N. Khaterchi, G. Bahri, I. Youssef, M. Mersni, H. Ben Said, D. Brahim, N. Mechergui, M. Methni, C. Ben Said, N. Bram, N. Ladhari
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S825
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The delicate balance between the need to ensure quality patient care and the reality of physicians dealing with psychiatric diseases poses a major challenge within the medical field. This issue raises fundamental ethical, legal, and medical questions, highlighting the complexity of decision-making regarding professional aptitude for practitioners affected by mental disorders.
ObjectivesTo examine the impact of psychiatric diseases on the medical aptitude of physicians.
MethodsThis was a retrospective descriptive study that focused on physicians with psychiatric diseases referred to the occupational pathology clinic at Charles Nicolle Hospital in Tunis for medical evaluations of their work aptitude between January 1, 2021, and September 15, 2023.
ResultsDuring the study period, we collected data from 20 patients. The mean age was 38 ± 11 years, with a sex-ratio (F/M)of 4.5. Five examined physicians had family histories of psychiatric disorders. Medical specialties were the most represented (N=17), including three general practitioners, two family medicine practitioners, and two anesthesiologists. The study population included 10 residents, eight hospital assistants, and two medical interns. The most common psychiatric diagnosis was depression (N=7), followed by bipolar disorder (N=5). The medical treatment prescribed was combinations of antidepressants and anxiolytics in seven cases, antipsychotics in five cases, and antidepressants in two cases. Medication adherence was noted in 10 physicians. Fourteen physicians had taken long-term sick leave, with an average duration of 203 days. Five physicians were declared fit to continue their regular professional activities, seven physicians were declared fit with restrictions on night work, and one physician was declared fit with workplace accommodations.
ConclusionsThis study highlights the challenges surrounding the medical aptitude of physicians with psychiatric diseases. However, it is imperative to promote mental health awareness and to implementsupport measures to ensure both compassion for physicians and patient safety.
Disclosure of InterestNone Declared
The Detached Mindfulness approach to anxiety disorders in an Italian mental health service
- F. Raffone, E. Pessina, A. Martini, P. Giunnelli, A. Massa, E. Carbone, M. Russo, V. Martiadis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S383-S384
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anxiety disorders are one of the most common mental illnesses, and a consistent increase was observed after the COVID-19 pandemic. Mindfulness refers to a process that leads to a mental state characterized by nonjudgmental awareness of the present experience. Mindfulness can be considered both a skill and a practice. The stronger is the ability to adopt a mindful state, the less suffering one will experience. While Mindfulness-based Psychotherapies have shown efficacy in their treatment, they have not yet been thoroughly studied in Italian public mental health services. In Detached Mindfulness, negative thoughts are acknowledged and avoided by turning them into actions using a standardized, time-limited, metacognitive intervention.
ObjectivesThe purpose of this study is to examine the efficacy and cost-effectiveness of Detachment Mindfulness for twelve patients with Generalized Anxiety Disorder (GAD) not being treated pharmacologically.
MethodsWe enrolled 12 patients diagnosed with GAD according to DSM-V in an 8-session program of Detached Mindfulness Psychotherapy (once a week). The Generalized Anxiety Disorder - 7 Scale (GAD-7) and the Kellner Symptom Questionnaire (SQ) were used to assess anxiety symptoms at baseline (T0), after 4 sessions (T1), and at the end of treatment (T2). The Client Satisfaction Questionnaire (CSQ-8) was used to assess treatment satisfaction.
ResultsThe GAD-7 score showed consistent reductions in generalized anxiety symptoms after Detached Mindfulness treatment (mean decrease of -42% at the end of the program). As measured by SQ, patients also reported improvement in physical well-being, relaxation, and somatic symptoms significantly respect to baseline. As for treatment satisfaction, ten out of twelve patients rated their treatment as satisfactory. As reported by patients, mindfulness can become a powerful and effective means to relate to one’s own internal experiences such as anxiety or fear, learning to recognize them, staying with them and avoiding their consequences.
ConclusionsThese results showed that detached mindfulness was an effective and cost-effective intervention for GAD, given the short amount of time it requires and the ease with which it can be implemented. For its extensive use in the public mental health system to be further supported, studies on larger populations are needed.
Disclosure of InterestNone Declared
Body dysmorphia in a 23 year old patient with obsessive compulsive disorder: a case report
- P. Setién Preciados, E. Arroyo Sánchez, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S629
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Body dysmorphic disorder (BDD) was considered an anxiety disorder in the DSM-IV, but in the DSM-V was added to the obsessive-compulsive and related disorders category. BDD is a psychiatric disorder characterised by an excessive, persistent, and distressful preoccupation with a perceived defect in appearance. These perceived defects are slight and are unnoticed by others. People with BDD usually have poor insight and are preoccupied with a perceived physical defect which causes them to check on it repeatedly. This leads to an impairment in psychosocial functioning, depression, and an increase in suicide risk.
ObjectivesReview how dismorphophobia (BDD) and obsessive compulsive syndrome intersect, the differences they present in symptomatology, prevalence and treatment.
MethodsPresentation of a patient’s case and review of existing literature, in regards to body dysmorphic syndrome and its similarities and differences with respect to obsessive compulsive syndrome.
ResultsThere are common features between both disorders, which are genetic overlap, physical past traumatic events, sex ratio, trait of perfectionism and body image disturbance.
Studies have found the prevalence of BDD in patients with OCD in a large patient sample was 8.7% to 15% compared to 3% in non-OCD.
The risk of comorbidity of OCD-BDD is three times higher in samples with a primary diagnosis of BDD compared to those with a primary diagnosis of OCD with 27.5% and 10.4%, respectively.
BDD as well as OCD must be managed with pharmacological and psychotherapy treatment. A selective serotonin reuptake inhibitor is the recommended first-line medication for BDD, even if appearance beliefs are delusional in nature.
Serotonin reuptake inhibitor (SRI) doses and trial durations are similar to those used for OCD; higher doses and a longer treatment trial are recommended than those typically used for depression and most other disorders. Cognitive-behavioral therapy that is specifically tailored to BDD is the psychosocial treatment of choice. Simply treating BDD as if it were OCD is not recommended.
ConclusionsThere are limitations included a restricted number of studies overall, an absence of studies comparing biological parameters, and the frequent inclusion of participants with comorbid body dysmorphic disorder and obsessive-compulsive disorder. The current nosological status of body dysmorphic disorder is somewhat tenuous and requires further investigation, with particular focus on dimensional, biological and aetiological elements.
Disclosure of InterestNone Declared
Cariprazine efficacy in a 40-year untreated case of a woman with predominantly negative symptoms of psychosis: A case report
- A. Mara, S. Myriknas
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S753-S754
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies have demonstrated the unfavorable and neurotoxic effects of untreated psychosis (UP) on the brain. An estimated 10 to 12 cc of brain tissue could be potentially damaged due to neuroinflammation and oxidative stress when a first episode of psychosis goes untreated. Other studies have found a correlation between the duration of untreated psychosis (DUP) and treatment resistance or nonresponse. Evidence-based schizophrenia treatment mainly relies upon the use of first and second-generation antipsychotics, without solid evidence that the former is superior to the latter regarding the treatment of negative symptoms. Both groups, however, can come with a risk of side effects. Cariprazine, a third-generation antipsychotic, represents a safe and effective treatment, targeting both the positive and negative symptoms of schizophrenia.
ObjectivesTo report a clinical case of a woman with an extreme DUP with predominantly negative symptoms of schizophrenia and highlight the favorable outcome cariprazine monotherapy had on her global functioning.
MethodsWe report a clinical case of a 58-year-old woman with a history of a 40-year UP successfully treated with 4,5mg of cariprazine. The woman was brought involuntarily for psychiatric assessment at the emergency department with a clinical image of catatonic stupor and predominantly negative symptoms of psychosis. Her total PANSS score at admission was 129. The negative subscale score was 49. She was initially treated with 3mg cariprazine and 10mg olanzapine and was gradually left on 4,5mg cariprazine monotherapy with an adjunctive 30mg mirtazapine.
ResultsThe patient was dismissed after 47 days of hospitalization. Cariprazine was effective in targeting both the cognitive and affective symptoms of long-standing UP. In the long-term, cariprazine also improved remnant delusional ideas of somatic and persecutory types, enhancing the patient’s social life, ensuring her support network, and assisting her integration into the community. The patient did not report any side effects, and her blood test results were within the normal range.
ConclusionsNot all cases of schizophrenia are dramatic at presentation - some can have a chronic and insidious course predominated by negative symptoms. UP can lead to disastrous consequences for the patient’s biopsychosocial well-being, leading to future treatment resistance and disability. Although such cases of untreated psychosis seem to be from the past, we should be conscious of their existence and treat them with a patient-personalized and symptom-centered approach. Cariprazine was successful and effective in treating this patient with a remarkable course of UP.
Disclosure of InterestNone Declared
Examining the effect of family-based intervention programs used in psychosis on the disease: a systematic review
- Z. Kutlutürk, M. C. Aktaş, C. H. Ayhan
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S290
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychosis is a complex mental health condition that can have a significant impact on individuals and their families. Family-based intervention programs have been developed to provide support and education to both individuals with psychosis and their families. These programs aim to improve clinical and family outcomes, reduce relapse rates, and enhance the overall well-being of individuals and their families . This study examined the effect of family-based intervention programs used in psychosis on the disease by synthesizing evidence from a systematic review of relevant studies.Family interventions have shown promising results in improving clinical and family outcomes in long-standing psychosis (Sadath et al., 2015). These interventions focus on improving relationships through problem-solving and enhancing the understanding of the illness and its treatment (Kuipers et al., 2010).
ObjectivesThe aim of this study was to evaluate the effect of intervention programs implemented for the families of individuals diagnosed with psychosis on the course of the disease.
MethodsThe study was conducted between August and September 2023 in 3 databases (PubMed, Cochrane Library, Science Direct) using the keywords “psychosis”, “family interventions”, “family in psychosis”. These databases were preferred because they contain a significant amount of evidence-based literature in the field of biomedical sciences and psychology. Studies conducted between 2013 and 2023, whose full texts were accessed and written in Turkish and English were included in the study.
ResultsAs of September 2023, 16 national and international research articles on the subject have been reached and the literature review continues. When the literature review is finalized, all study results will be presented together.
ConclusionsThis review provides an overview of the effects of intervention programs implemented for the families of individuals diagnosed with psychosis on the course of the disease and solution suggestions. Family-based intervention programs have shown promise in improving clinical and family outcomes in psychosis. These programs focus on enhancing relationships, providing education, and reducing relapse rates. However, the implementation of family interventions in routine clinical services can be challenging due to various barriers. Peer support programs have emerged as a valuable addition to family interventions, providing a supportive environment for families to share their experiences and support one another. Future research should focus on addressing barriers to implementation and further exploring the benefits of peer-driven family support services in early intervention programs for psychosis.
Disclosure of InterestNone Declared
Thai Habitus in Contemporary Society: Paving the Way for Tackling Inequality
- Sirima Thongsawang, Boike Rehbein, Supang Chantavanich
-
- Journal:
- TRaNS: Trans-Regional and -National Studies of Southeast Asia , First View
- Published online by Cambridge University Press:
- 27 August 2024, pp. 1-26
-
- Article
- Export citation
-
This paper examines the habitus of contemporary Thailand based on the concepts developed by Pierre Bourdieu and their operationalisation to Thai society developed by Boike Rehbein's principles, which explain how contemporary habitus is linked to social inequality and mobilisation participation. Thailand has two key social structures: precapitalist and capitalist. Both create and reproduce different types of habitus. The paper used a mixed-methods research approach to analyse social inequality and challenges in Thailand since 2019. Data collection was conducted during the years between 2021 and 2022 from 400 surveys and fifteen qualitative interviews. The paper proposes eight habitus types rooted in Thai social structures with seven characteristics for explaining contemporary Thai society. The pre-capitalist structure generates the following habitus types: subsistential, traditionalist, and powerful (phuyai). The capitalist structure generates the following types: desperate, individualist, aspirant, and content creator. Between these two structures is the conformist. All habitus types share some characteristics. Authoritarianism is the fundamental trait of the predominant habitus types in Thai society, which are interconnected with social structures, thereby reflecting the consequences of social inequality and mobilisations. The demographic most affected by social inequality is the desperate group, but a more significant habitus for mobilisation participation is that of content creator, which is considerably small now but is likely to increase. Traditionalist and conformist groups are less likely to protest and, to a lesser degree, this is true of the subsistential and powerful types. Moreover, rationales of being affected by social inequality and reacting differently are distinct characteristics of each type, and socio-economic positions interplayed with social media influences.
Diagnosing Trauma-related Dissociative Disorders in Hungary: The Development of the Hungarian Version of MID (MID-HU)
- Z. Boytha, Á. Münnich, J. Molnár
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S374
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The recognition, diagnostics and treatment of dissociative disorders (DD) in Hungary is currently in its infancy. According to international researches the prevalence of dissociative disorders is similar to that of the major psychiatric disorders (bipolar disorder, schizophrenia, etc.). Due to the lack of valid diagnostic tools no data is available regarding the prevalence of dissociative disorders in Hungary so far.
ObjectivesTo fill this gap within our profession; to provide a complex diagnostic tool; developing the hungarian version of the Multidimensional Dissociation Questionnaire (MID-HU)
Methods341 people participated in our study classified into four groups: (1) healthy controls (n=88), (2) patients from private practice diagnosed with DD and all those participants who have DD according to their MID results (n=103), (3) hospitalized psychiatric (mixed sample, n=60) and (4) SUD patients (n=89). The questionnaire package contained the hungarian version of the Multidimensional Inventory of Dissociation (MID-HU), the Dissociative Experience Scale (DES), the Traumatic Antecendents Questionnaire (TAQ), the Self-Report Version of the Dissociative Disorders Interview Schedule (DDIS-SR) and additional questions. Now we present the first results regarding the adaptation process of the hungarian MID (MID-HU).
ResultsThe mean age of the participants was 36 years, 61,6% were female and 38,4% male.
The MID-HU has strong internal consistency: the alpha coefficients for the 14 facet scales were 0.88 or higher. The alpha coefficients for the 23 dissociation diagnostic scales ranged from 0,74-0,95; 9 were excellent (0,90 or above), 10 were good (0,80 or above), and 4 were fair (0,70 or above). The test-retest correlation of the Mean MID-HU scores is good (0,87). Factor analysis of the MID-HU extracted one main factor: dissociation. The mean MID-HU scores correlated with mean DES scores (0,87), indicating a good convergent validity. We found significant differences between the healthy control group and the dissociatve group in the mean DES (control: 9,5, dissociative: 27,6, Sig:<0,001), mean MID (control: 2,5, dissociative: 27, Sig: <0,001), the 23 dissociative diagnostics scales of the MID, 14 facet scales of the MID, and all diagnostics scales of the DDIS (using Mann-Whitney).
ConclusionsThe MID-HU seems to be a valid instrument, that can differentiate between DD patients and healthy people.
Disclosure of InterestNone Declared
Understanding females with attention deficit and hyperactivity disorder
- O. Kilic
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S36
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
The predominant association of attention deficit and hyperactivity disorder (ADHD) with males, often leads to underdiagnosis or misdiagnosis in females. Recent studies have highlighted marked differences between genders in the manifestation, symptoms, and outcomes of ADHD. Understanding these differences is essential for accurate identification, diagnosis, and tailored interventions for affected individuals, particularly females. TThe multifaceted nature of ADHD demands a nuanced examination of its impact on females, considering how societal expectations, hormonal influences, and a range of symptom presentations may contribute to the variation in the manifestation of this disorder across genders. This presentation aims to contribute to a more comprehensive understanding of ADHD, fostering improved recognition and tailored strategies to support both males and females who suffer from this condition.
Disclosure of InterestNone Declared
Explanation of the personality factor with the Enneagram in the selection of the specialty branch of the intern doctors
- B. Özen, E. Ilgin, E. Akça, A. Özercan, P. Seçgin, Ö. Yanartaş
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S658
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Personality characteristics have an important place in the choices of interns who are at the stage of deciding how their profession will be shaped in the future. While the Big 5 personality model has been widely used in evaluating the personality traits factor in career planning, the Enneagram has increased in popularity in recent years. In this study, it was aimed to investigate how senior medical students evaluate their professional future between these choices and the students’ personality types.
ObjectivesForms and scales were presented to 221 interns who agreed to participate in our study and were studying in their final year in the 2022-2023 period at three different faculties, two state universities and one private university in the Marmara Region in Turkey.
MethodsThe sociodemographic data form, Enneagram Personality Types and Subtypes Inventory, and Positive Future Expectation Scale, prepared by the researchers and containing questions about the factors that may be effective in choosing medical specialization, obtained through a face-to-face pilot interview with ten students and literature review, were applied to the participants. Participants answered the forms and scales via ‘Google forms’.
Results211 out of 221 participants, who did not constitute outliers, were included in the analysis. The mean age of the participants was 24.43 (S.E= 0.11)
In terms of Enneagram typologies, Type 2 (39.3%) exhibited the highest prevalence, followed by Type 1 (13.3%), Type 6 (11.8%), and Type 7 (8.5%).
Furthermore, a statistically significant relationship was found between specialization area and Enneagram types (Fisher exact <.001, p< .001). Post-hoc examinations highlighted specific associations, such as the relationship between Type 3 and Cardiovascular Surgery, Orthopedics and Traumatology; Type 4 and Pneumology, Psychiatry; Type 5 and PRC, Type 6 and Infectious Diseases, Neurology, Medical Microbiology; Type 7 and Cardiology; Type 8 and Pediatrics, Medical Biochemistry; and Type 9 and Family Medicine, Radiology, Psychiatry, Medical Pathology.
ConclusionsWhen the results are evaluated, the highest rate of type 2 and type 1 of the Enneagram typology in senior medical faculty students supports the fact that the medical profession consists of responsible and principled people who love helping others. It is compatible with the character traits of people with type 9 who avoid stress and conflict, preferring the department to have a low workload, and turning to family medicine, radiology, psychiatry and medical pathology departments, which are estimated to have relatively fewer working hours and emergency applications.
Our study suggests that this scale be used more widely, as the Enneagram typology, which is used in many professional and career choices, shows results compatible with the participants’ preferences in choosing a medical specialty.
Disclosure of InterestNone Declared
Urinary retention induced by psychotropics: A case report
- E. Smaoui, D. Mnif, N. Reguaieg, F. Guermazi, S. Sakka, I. Baati, J. Masmoudi
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S693-S694
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Neurological bladder is considered a functional disability that has a significant impact on the quality of life and psychological state of patients. Psychotropic drugs, in turn, can worsen the urinary dysfunction caused by this disease.
ObjectivesOur objective is to illustrate, through the case of a patient suffering from a neurological bladder decompensated by the treatment of a characterized depressive episode, the link between these two pathologies.
MethodsWe report the case of Ms. M.W., aged 51, with a history of high blood pressure stabilized under nebivolol and a neurological bladder diagnosed 10 years ago with episodic pollakiuria, admitted to the psychiatric department for repeated suicide attempts. She had never used psychoactive substances and had no family psychiatric history. The patient presented depressive symptoms evolving for 5 months. The diagnosis of a characterized depressive episode with melancholic features was made and the patient was treated with sertraline. From the first intake of the drug, the patient presented acute urinary retention (UR) requiring the placement of a permanent bladder catheter. The urinary symptoms improved upon stopping the treatment. Sertraline was changed to olanzapine and escitalopram. The patient stopped the treatment after one month because of the worsening of urinary symptoms requiring the installation of a suprapubic catheter. The urinary problem, together with the cessation of treatment, were responsible for a worsening of psychiatric symptoms leading to multiple suicide attempts. Given the advanced stage of the neurological bladder demonstrated by the urodynamic tests, our patient was treated with paroxetine, quetiapine and oxazepam along with psychotherapeutic education. The evolution was characterized by improvement in psychiatric symptoms and the urinary symptoms were stable.
ResultsThe lack of improvement after treatment discontinuation could be explained by an underlying neurological bladder manifesting with pollakiuria. The current literature on UR induced by psychotropic treatments is quite rare limited in case reports. This effect occurs especially when selective serotonin reuptake inhibitors (SSRIs) are prescribed in combination with other antipsychotics. Unlike first generation antipsychotics, atypical antipsychotics have muscarinic receptor antagonist properties which can induce UR. Among atypical antipsychotics, olanzapine has been shown to have the greatest antimuscarinic effects. Regarding SSRIs, they are associated with a lower risk of UR than other antidepressants and sertraline had the highest risk of UR.
ConclusionsSSRIs can induce UR particularly in combination with atypical antipsychotics. Coordination of care across multiple specialties and understanding the side effects of psychotropic medications can enable faster diagnoses and adequate management.
Disclosure of InterestNone Declared
Evaluation of an App-based brief Cognitive Behavioral Therapy for individuals with Nonsuicidal Self-injury
- S. Kang, S. M. Zoh, J.-W. Hur
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S552
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Nonsuicidal self-injury (NSSI), the deliberate and direct destruction of one’s own body tissue without suicidal intent, has represented a significant public health concern among adolescents and young adults worldwide, yet they have limited access to evidence-based interventions. App-based digital therapy, with its advantages of high cost-effectiveness, accessibility, and user receptivity, could be an effective intervention for NSSI. We expected that the use of an app-based brief cognitive-behavioral therapy (CBT) would improve depressive symptoms and emotion dysregulation, the most prevalent symptoms among individuals with NSSI.
ObjectivesThis study aimed to evaluate the efficacy of a 3-week app-based brief CBT program focusing on cognitive distortion correction for individuals with NSSI.
MethodsA total of 34 participants who engaged in NSSI were included in the final analysis, with 18 individuals assigned to the ‘app group’ and 16 to the ‘waitlist group.’ The brief CBT program consisted of three quizzes designed to prompt the users to identify cognitive distortions embedded in a series of short scenarios, develop more realistic perspectives, and imagine advising to significant others. The app group was instructed to complete three quizzes per day for three weeks, while the waitlist group received no intervention.
ResultsBaseline and follow-up assessments of depression and emotion regulation were conducted. After the 3-week program, the app group showed a significant reduction in depressive symptoms (F = 8.30, P = .007) compared to the waitlist group. There was no group difference regarding emotion regulation.
ConclusionsDepression is a prominent symptom in individuals with NSSI. Our findings suggest that an app-based brief CBT intervention targeting cognitive distortions can effectively alleviate depression in individuals with NSSI. The results also highlight the need for digital interventions that are tailored and designed to improve emotion regulation in this population.
Disclosure of InterestNone Declared
Current Challenges and Future Directions of Research in Cell Phone Addiction
- O. Vasiliu
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S295-S296
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Behavioral addictions (BAs) are intensely explored during the last decades due to their impact on the quality of life, functionality, socio-economical negative consequences, and high risk of mental health negative consequences. BAs are new challenges for clinicians and researchers due to a lack of well-defined diagnostic criteria, very few available epidemiological data, and scarce information about efficient therapeutic interventions. Cell phone addiction (CPA) has been raising a significant interest for mental health specialists because of its increasing prevalence and potential long-term physical and mental complications. Therefore, an analysis of the available data about the main characteristics of this pathology seems granted.
ObjectivesThe main objective of this review was represented by the need to find relevant reports about the epidemiological, clinical, and therapeutic interventions in CPA.
MethodsA narrative review focused on the available treatments for food addiction was performed through a search in four electronic databases (PubMed, Cochrane, EMBASE, and Web of Science/Clarivate) using the paradigm “cell phone addiction” or “smartphone dependence” and “treatment” or “epidemiology” or “diagnostic criteria” or “risk factors.” No inferior time limit for published papers was established, and the superior limit was July 2023.
ResultsA relatively large number of papers regarding this topic were found (n=772), but after applying the inclusion and exclusion criteria, only 29 articles remained. Female gender and adolescents, but also high anxiety levels, insomnia, excessive Internet use, less physical activity, and a higher level of dependence have been correlated with CPA. Six validated scales have been identified as possible instruments for monitoring the CPA evolution. Different diagnostic criteria have been suggested, but they still lack clinical validation. Cognitive-behavioral therapy could be helpful, and smartphone applications that limit online time could also be efficient. Treatment of previously mentioned vulnerability factors is also recommended to obtain long-term favorable effects.
ConclusionsCPA is an increasingly explored BA, but validated diagnostic criteria are still missing. The treatment is also based on extrapolations from other addictions. Therefore large sample-based therapy trials are needed.
Disclosure of InterestNone Declared


