3294077 results
Use of Long-Acting Injectables in Borderline Personality Disorder: What Do We Know?
- E. D. S. Almeida, J. Abreu, R. P. Vaz, J. Martins, F. Cunha, I. Santos, N. Castro, R. P. Andrade, E. Monteiro
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S119
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotherapy serves as the foundation of care for individuals with borderline personality disorder (BPD), with pharmacotherapy being regarded as a supplementary measure to be considered when necessary. In clinical practice, however, most of BPD patients receive medication.
A major problem in the treatment of BPD is the lack of compliance derived from the pathological impulsivity of BPD patients. The use of long-acting antipsychotics (LAI) may be an option.
ObjectivesThis work aims to address the use of long-acting injectables in borderline personality disorder.
MethodsNon-systematic review of literature using the PubMed ® database, based on terms “Borderline Personality Disorder” and “Long-acting antipsychotics”. Only six articles were found.
ResultsSeveral studies have shown promising results in the treatment of Borderline Personality Disorder (BPD) with long-acting injectable (LAI) antipsychotics. A six-month study using IM risperidone demonstrated significant improvement, while LAI Aripiprazole also exhibited positive outcomes in individuals with BPD and Substance Abuse. Additionally, Palomares et al. (2015) found that palmitate paliperidone LAI reduced impulsive-disruptive behaviors and enhanced overall functioning in BPD patients. Carmona et al. (2021) compared oral and LAI antipsychotics and concluded that LAIs may have a role to play in the management of BPD.
ConclusionsTreatment with LAIs may play an important role in clinical and functional improvement in BPD patients.
Disclosure of InterestNone Declared
The possible role of platelet APP processing in the pathophysiology of Alzheimer’s Disease
- R. Gurrieri, M. G. Carbone, A. Arone, S. Palermo, D. Marazziti, A. Gemignani
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S316
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Alzheimer’s disease (AD) stands as the most prevalent form of dementia. Alzheimer’s Disease is acknowledged to have a complex origin, a gradual neurodegenerative progression, and a wide-ranging clinical profile marked primarily by progressive memory loss, cognitive decline, and various functional impairments that significantly diminish the quality of life: Key characteristics of AD encompass the presence of amyloid plaques, which are characterized by the pathological accumulation of insoluble β-amyloid (Aβ) aggregates within the brain tissue and blood vessel walls.Several reports have indicated the existence of cerebral abnormalities within platelets in individuals afflicted by AD.
ObjectivesThe objective of this investigation was to review studies investigating the metabolism of APP in platelets among individuals with AD to identify potential dependable peripheral indicators leading to novel approaches to its management and treatment.
MethodsA systematic review according to the PRISMA guidelines was carried out, by accessing the PubMed database up to June 2023. The authors screened the titles and the abstracts of all the potentially relevant papers on the basis of a strict list of exclusion and inclusion criteria.
ResultsA total of thirty-two studies were included. The evidence points towards the observation that AD individuals exhibit various modifications in platelet APP processing when compared to matched healthy controls, that are frequently associated with the severity of cognitive impairment and functional independence. The majority of the evidence supports changes in platelet ADAM-10 activity, β-secretase activity, APP ratio, a state of heightened platelet activation or hyper-responsiveness, and a potential release of platelet APP via vesicular mechanisms, which may ultimately contribute to Aβ production.
ConclusionsPlatelets offer a promising peripheral model for detecting and evaluating molecular changes associated with AD, as they hold the potential to provide vital insights into the development of an effective diagnostic tool and open doors to innovative therapeutic approaches.
Disclosure of InterestNone Declared
Methylomic signature of lithium response in bipolar disorder
- C. Bourdon, C. Courtin, F. Bellivier, B. Etain, C. Marie-Claire
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S218-S219
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is a chronic and severe psychiatric disorder, characterized by the alternance of episodes of (hypo)-mania and major depression. Lithium (Li) is the first-line treatment for BD but unfortunately response to Li is highly variable: after at least two consecutive years of treatment, only a fraction of patients receiving Li will display significant improvement in the frequency and/or severity of mood recurrences. This interindividual variability of treatment response is difficult to predict, in the bipolar disorder context. This could be determined by genetic factors still misidentified by available genetic studies. In addition, no clinical or biological markers are available to reliably define eligibility criteria for a lithium treatment in bipolar disorder. A consequence is a long process of therapeutic trials (18-24 months) to phenotype Li response, delaying the stabilization.
ObjectivesTo identify objective biomarkers of the prophylactic response to lithium in order to improve patient care and propose therapeutic alternatives to patients who do not respond to lithium.
MethodsUsing a genome-wide methylomic approach, and then logistic regressions incorporating as covariates the different types of treatments, we were able to identify differentially methylated regions (DMRs) whose methylation difference between responders and non-responders was not impacted by co-prescribed treatments. Then, we used Methylation Specific High-Resolution Melting (MS-HRM), a PCR based method than can be implemented in any medical laboratory at low cost and with minimal equipment, to estimate methylation proportion of 9 DMRs in 61 samples of bipolar patients.
ResultsIn the sample of 61 individuals with BD, the 9 MS-HRM-measured DMRs combined with clinical variables (age, sex, cigarette smoking status, lifetime number of hospitalizations, age at onset of BD, polarity at onset, psychotic symptoms at onset, family history of BD, lifetime alcohol/cannabis misuse, panic disorders, Li prescribed as the first mood stabilizer (vs 2nd or 3rd choice)) correctly classified 83,6% of individuals as good or non-responders (n=61, prophylactic response phenotype defined using the “Alda” scale). Excluding the partial responders, the percentage of correctly classified individuals is as high as 100% (n=43, 18 non responders and 25 responders). The AUC are respectively AUC=0.913 and AUC=1.0.
ConclusionsThe MS-HMR method allow to identify the response status of individuals with BD with 9 DMR. These DMRs discriminate good from non-responders and can be used in combination with clinical variables.
Disclosure of InterestNone Declared
The COVID-19 pandemic as a traumatic experience in the general population
- T. Mastelić, V. Višić, T. Borovina Marasović, N. Rančić, D. Vukorepa, M. Milanović, Ž. Kralj, E. Burilović, M. Pernat, K. Glavičić, M. Baković, A. Sabljar, S. Kozina, D. Lasić, M. Mavar, T. Glavina
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S499-S500
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The COVID-19 pandemic has significantly affected everyday life in most countries of the world. Researches conducted in 2020 showed that COVID-19 was a traumatic experience for 18-60% of respondents in the general population, depending on the country where the research is conducted. Researches for later periods are rare, although we can expect significant changes. We found only one study from 2023 on this topic, although not on the general population.
ObjectivesThat is why we were interested in what the situation is like after 3 years of the pandemic, when we have been living without non-pharmacological anti-pandemic measures for almost a year.
MethodsThe research was conducted at the beginning of 2023. 48 respondents who were not treated psychiatrically or are medical workers were surveyed, because it was shown that these groups were exposed to a greater risk of impaired mental health during the COVID-19 pandemic. To assess the level of traumatic experience, i.e. the risk of developing PTSD as a consequence of the COVID-19 pandemic, we used the Impact of Event Scale With Modifications for COVID-19 (IES-COVID19). A score on that scale of 27 to 34 indicates a clinically significant level of trauma, i.e. there is a 75% chance of developing PTSD. A result of 35 and above suggests that it is necessary to seek professional help.
ResultsOur research included 19 (39.6%) men and 29 (60.4%) women. The average age of the respondents is 60.4 years. 29 (60.4%) respondents know that they have recovered from COVID-19. 2 (4.2%) subjects were treated in the hospital due to COVID-19. 8 (16.7%) respondents have a traumatic experience of the COVID-19 pandemic. 5 (10.4%) respondents are in the category of clinically significant level of trauma, while 3 (6.3%) respondents are in the category that should seek professional help. The group traumatized by COVID-19 does not have significantly more respondents who recovered from COVID-19 (p=0.510) nor does it differ in terms of gender representation (p=0.984).
ConclusionsAt the beginning of the COVID-19 pandemic, there were discussions about whether it can even be classified as a traumatic experience and whether we can talk about PTSD as a consequence of the pandemic. With this time lag, it seems that in part of the population we are finding PTSD symptoms that are a consequence of the pandemic, but to a lesser extent than research at the beginning of the pandemic suggested. Certainly, additional research is needed on this topic. Also, it is necessary to examine risk factors for possible prevention, as well as therapeutic possibilities.
Disclosure of InterestNone Declared
Motives for MDMA Use: A Comparative Study with Alcohol and Cannabis
- D. Zullino, L. Penzenstadler, S. Rothen, F. Seragnnoli, A. S. Girardet, G. Calzada, G. Thorens
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S418-S419
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
While research on drug use motives has primarily focused on widely used substances like alcohol, tobacco, and cannabis, understanding the motivations behind MDMA use is crucial for developing targeted therapeutic, preventive, and harm reduction strategies.
ObjectivesThe objective of this study is to present the findings of an online survey that evaluates the motives behind the use of 3,4-methylenedioxymethamphetamine (MDMA) and draws comparisons between these motives and those for alcohol and cannabis consumption.
MethodsData were collected through an online survey, available in both English and French, with 99 participants. The survey included five sections, including a substance abuse screening test (ASSIST) and the Pahnke-Richards Mystical Experience Questionnaire. The primary focus was on motives for MDMA use, assessed using an adapted version of the Marijuana Motives Measure (MMM), comparing them with alcohol and cannabis motives.
ResultsThe most reported motive for MDMA use was enhancement, followed by expansion motives. Social motives were the third most common, while coping motives ranked fourth, and conformity was the least common motive. Comparisons with alcohol and cannabis use motives revealed differences in motives for each substance. MDMA showed a unique pattern of motives.
ConclusionsEnhancement emerged as the most prevalent motive for MDMA use, consistent with previous research on MDMA motive use. Expansion motives, which involve altering perceptions and increasing self-awareness, ranked second, reflecting the growing interest in MDMA-assisted therapy for conditions like PTSD. Surprisingly, social motives were less common for MDMA compared to alcohol and cannabis, suggesting unique social dynamics associated with MDMA use. Conformity motives were also less significant for MDMA users, possibly due to the age of initiation and user maturity.
Understanding the motives behind MDMA use is essential for designing effective interventions and harm reduction strategies. The distinct motives for MDMA, as compared to alcohol and cannabis, highlight the need for tailored approaches to address its use. Further research should explore the complex interplay of motives, age of initiation, social context, and cultural factors to inform comprehensive strategies related to MDMA use.
Disclosure of InterestNone Declared
Cardiovascular risk associated with chronic treatment of paliperidone, olanzapine, risperidone and aripiprazole
- A. L. Montejo, C. Bermejo, J. Matías, T. Martín, J. Matías-Polo, Y. Santana, J. López-López, R. de Alarcón, J. M. Acosta
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S209
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Weight gain, QT interval prolongation, and dyslipidemias associated with the chronic use of some antipsychotic medications can explain a higher prevalence of cardiovascular risk in these psychiatric population. The D’Agostino Index include some factors such as age, total cholesterol, high-density lipoproteins, systolic blood pressure increased, antihypertensive treatment, smoking, and diabetes, to estimate an individual’s risk (low, moderate or severe) of developing a cardiovascular event through a period of 10 years or throughout the patient’s lifetime.
ObjectivesTo compare the degree of cardiovascular risk using the D’Agostino Index, among different antipsychotic medications.
MethodsAn estimation of cardiovascular risk (low, moderate, or high) was performed with the D´Agostino index in a sample of 144 patients (82 men and 62 women) mean age 45,2 +/- 10.13. All patients were treated for at least one year at a therapeutic dose and adhered to their treatment regimen correctly. Subjects with some relevant pre-existing unstable heart disease were excluded. All patients previously provided informed consent and were of legal age. Clinical data on medical history, concomitant medications, and risk factors were collected. A completed physical exam, waist circumference, lab sample, a lifestyle scale, and an evaluation of vital signs in accordance with European Society of Hypertension were evaluated. Statistical analysis was carried out using the statistical software SPSS version 26.0. A significance level α=0.05 was considered throughout the study.
ResultsThe four most consumed antipsychotics were risperidone 9.72% (n=14), paliperidone 25.7% (n=37), olanzapine 14.6% (n=21), and aripiprazole 34.7% (n=50). Descriptively, it was observed that the drugs most associated with moderate or high risks were paliperidone (37.8%) and olanzapine (33.3%), risperidone (28.6 %). Aripiprazol (22%) was the less associated compound with moderate/high cardiovascular risk.
ConclusionsSubjects treated with olanzapine and paliperidone showed a higher association with cardiovascular risk. Predicting cardiovascular risk could provide individual benefits by enabling lifestyle modifications, pharmacological treatment changes, or closer monitoring to reduce cardiovascular risk.
Disclosure of InterestA. Montejo Grant / Research support from: This study has been funded by the Instituto de Salud Carlos III (ISCIII) through the project PI19/1596 and co-funded by the European Union., C. Bermejo: None Declared, J. Matías: None Declared, T. Martín: None Declared, J. Matías-Polo: None Declared, Y. Santana: None Declared, J. López-López: None Declared, R. de Alarcón: None Declared, J. Acosta: None Declared
Gender differences in the association of dementia symptoms severity and hospital anxiety
- K. Bosak, S. Vuk Pisk, M. Grah, P. Folnegović Grošić, Ž. Bajić, V. Grošić
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S218
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Symptoms of anxiety can worsen cognitive decline in people with dementia, and symptoms of dementia and fears of further cognitive decline can cause anxiety. Advanced dementia is not necessarily associated with a loss of emotion, which means that people may still experience anxiety, but their ability to cope in a healthy way is reduced. The problem is exacerbated by the fact that hospital care alone can contribute to the severity of anxiety symptoms due to change in routine of daily activities, unfamiliar surroundings, uncertainty about health status, prognosis and various medical procedures. There are differences between women and men in the prevalence, course and manifestation of both dementia and anxiety disorders.
ObjectivesTo examine whether there are differences between women and men in the association of hospital anxiety with eight symptoms of dementia: difficulties with memory, orientation, judgement, problem solving, fulfilling social obligations, daily activities at home and with hobbies, or personal care, in patients with mild to moderate dementia.
MethodsA cross-sectional study was conducted at Sveti Ivan Psychiatric Clinic in Zagreb in June 2023. The target population were hospitalised patients diagnosed with dementia, both genderes, aged 60-90 years, without psychotic disorder. Anxiety during hospitalisation was measured using the anxiety subscale of the Hospital Anxiety and Depression Scale (HADS-A), and the severity of dementia symptoms was measured using the Dementia Assessment Instrument (CDR). The hypothesis was tested using Wald test of differences between women and men in unstandardised linear regression coefficients of the HADS-A on individual dementia symptoms, after adjustment for age, education, presence of a married or stable non-marital partner and duration of current hospitalisation.
ResultsWe enrolled 65 women and 35 men of comparable age. There were significant gender-related differences in the association between hospital anxiety and difficulties with judgement (P = 0.01), fulfilling social obligations (P < 0.001), difficulties with home and hobbies (P = 0.02), and personal care (P = 0.00). In women, more pronounced difficulties with judgement and with home and hobbies were associated with higher anxiety, and in men the presence of these two symptoms of dementia was associated with lower anxiety. Difficulties with fulfilling social obligations are associated with lower anxiety in women and higher anxiety in men. Difficulties with personal care were associated with lower anxiety in both genders, but this effect was stronger in men.
ConclusionsThere are differences between women and men in the association between anxiety during hospital treatment and the severity of individual dementia symptoms. These differences are present in difficulties with judgement, fulfilling social obligations, home, hobbies and personal care.
Disclosure of InterestNone Declared
Peculiarities of the first time diagnosed mental disorders formationin after the coronavirus disease COVID-19
- N. O. Maruta, V. Y. Fedchenko, T. V. Panko, I. O. Yavdak
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S519
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The world community is only at the beginning of awareness of the peculiarities of the formation, course and outcome of the psychopathological consequences of the impact of the SARS-CoV-2 pandemic.
ObjectivesTo investigate the clinical and anamnestic features and their influence on the formation of psychopathological consequences in patients with first diagnosed mental disorders who have experienced COVID-19 and were exposed to the stressors of the SARS-CoV-2 pandemic.
Methods97 patients with first diagnosed mental disorders who have experienced COVID-19 and were exposed to the stressors of the SARS-CoV-2 pandemic were examined (F 32.0-32.2 – 34 patients, F 40-45 – 32 patients, F 06.3-06.6 – 31 patients). Clinical-psychopathological, clinical-amnestic methods, including information about the experienced coronavirus disease COVID-19, the impact of the stressors of the SARS-COV-2 pandemic, and methods of statistical analysis were applied.
ResultsThe conducted research made it possible to identify the phenomenological structure of mental disorders that develop after the coronavirus disease COVID-19. This structure includes depressive disorders (35.05%), neurotic, stress-related and somatoform disorders (32.99%), as well as mental disorders of organic genesis (31.96%). An important result of the study was the determination of the heterogeneity of mental pathology in the context of the influence of stressogenic factors of the pandemic and other psychogenies. In this aspect, all mental and behavioral disorders must be divided into 3 variants of pathology, which differ in the mechanisms of formation: caused by the pathoplastic factors of COVID-19 and the patient’s personal reactions to the disease; related to the psychogenic effects of the stressors of the SARS-COV-2 pandemic; with a combined mechanism of influence of pathoplastic and psychogenic factors. Certain diagnostic and phenomenological regularities characteristic of each of the options are defined. The influence of pathoplastic factors and personal reactions to the disease is associated with the formation of depressive disorders. Pandemic stressors most often cause the development of neurotic, stress-related and somatoform disorders. Under the influence of combined factors, disorders of organic genesis are formed to a greater extent. The initial manifestations of pathology also differ with different formation mechanisms: when pathoplastic factors predominate, asthenia, depression and sleep disturbances prevail; with leading psychogenic influences – anxiety and tension; when the above factors are combined - asthenia, stress and cognitive disorders.
ConclusionsThe significance of the obtained data lies in the possibility of studying the role of the psychopathological consequences of COVID-19 in the genesis of mental disorders.
Disclosure of InterestNone Declared
Impact of Antidepressant Treatment on Fibronectin Levels in Patients with Depression and Chronic Heart Failure
- A. K. Sikora, S. Fedorov
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S95-S96
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Inflammation has emerged as a critical factor in the pathophysiology of both depression and chronic heart failure (HF). Chronic heart failure, a complex clinical syndrome, is often accompanied by a state of heightened inflammation, with elevated levels of proinflammatory markers. Likewise, depression, a prevalent comorbidity in HF patients, has been intricately linked to inflammation, with evidence suggesting a bidirectional relationship.
ObjectivesThis study aimed to evaluate the effect of antidepressant treatment on plasma fibronectin levels in patients with comorbid depression and chronic heart failure.
MethodsWe enrolled a total of 113 patients with HF, all of whom had comorbid depression. The patients were divided into two groups based on the antidepressant treatment they received: Group 1 (n = 78) received vortioxetine, and Group 2 (n = 35) received sertraline. Before initiating treatment and after 6 months, we measured fibronectin levels in the patients’ plasma.
ResultsThe study revealed a significant difference in the effects of the two antidepressants on fibronectin levels. Patients treated with vortioxetine demonstrated a substantial reduction in fibronectin levels post-treatment, with an approximate threefold decrease compared to the pre-treatment levels (pre-treatment value ± standard deviation) μg/ml to (post-treatment value ± standard deviation) μg/ml, (p<0.05). Conversely, patients treated with sertraline experienced a comparatively lesser reduction in fibronectin levels, with a change from (pre-treatment value ± standard deviation) μg/ml to (post-treatment value ± standard deviation) μg/ml (p<0.05).
ConclusionsThis study highlights the considerable impact of vortioxetine on fibronectin levels in patients with comorbid depression and chronic heart failure, resulting in a significant reduction. In contrast, sertraline’s effect on fibronectin levels, while present, is notably less pronounced. The study emphasizes the potential therapeutic benefit of vortioxetine in cardiac remodeling associated with depression in patients with chronic heart failure, underscoring the need for further research and exploration.
Disclosure of InterestNone Declared
A Challenging Conundrum; Learning Disability, Schizophrenia and Autism - a Case Report
- F. Rouhani, G. Aperis, S. Digpal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S145-S146
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychiatric disorders are common in patients with learning disabilities. There are also patients with the triad of autism, schizophrenia and learning disability. Patients with this background can be admitted to general hospitals for psychiatric or non-psychiatric reasons.
We are presenting a case who had a very complicated clinical course and her discharge planning was challenging.
ObjectivesThe objective of this work was to show the challenges in the investigation, medical management, and discharge planning of the patients with concomitant learning disability, schizophrenia and autism.
MethodsWe scrutinized the patient’s casenotes, including blood results and all relevant imaging. We paid a particular attention to all the entries from the psychiatry team, general medical doctors, oncologists, learning disability team and discharge planners.
ResultsThe lady had a protracted 4-month inpatient admission throughout which she was physically and verbally aggressive to hospital staff. She was deemed to lack capacity for hospital admission and treated in her best interests under Mental Capacity Act (MCA), frequently requiring sedation with Haloperidol and Lorazepam. Following consultation with the local Psychiatrist her medications were altered to: Risperidone 2 mg BD, Diazepam 5 mg OM, 5 mg afternoon and 10 mg evening, Procyclidine 5 mg BD, Chlorpromazine 25 mg BD, Promethazine 25 mg OD PRN, and Midazolam 10 mg buccal PRN.
A change in her clinical condition was noted by the Psychiatry team; increased agitation, confusion and dysarthria. A repeat blood test was advised, due to patient refusal this took weeks to achieve despite the use of buccal Midazolam following Anaesthesiologist advice. Although blood tests were not significantly deranged, she was treated for presumed urinary tract infection with a course of antibiotics. A urine sample was unobtainable.
She reported right breast pain and underwent a mammogram. This showed a hypoechoic lesion 8x7x9 mm. Following consultation with a Breast Surgeon and Oncologist, Letrozole was replaced with Tamoxifen. The Psychiatric team concluded that the clinical deterioration with dysarthria was related to anxiety, associated with Autistic patients. The movement disorder was deemed secondary to antipsychotics exacerbated by stress and anxiety.
The patient’s discharge planning was complex. She was declined by numerous care homes. At time of writing, she remains an inpatient.
ConclusionsThe management of patients with a triad of Learning Disability, Schizophrenia and Autism is extremely difficult, particularly within an acute medical setting. Physical deterioration could be related to medication adverse effects or change in environment. Anxiety and stress are linked to these conditions. The challenging behaviour that these patients often have will make discharge planning very difficult as specialised care homes to accommodate these unique patients are very limite
Disclosure of InterestNone Declared
Psychological intervention online for adolescent: acceptability of Online Emotional Self-Regulation Improvement program
- C. López Soler, A. Martínez, V. Fernandez, M. Castro, J. L. Vicente
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S554
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Given that child and adolescent mental health has been affected by several factors in recent years, such as the distance between home and specialized centers that provide psychological care to children, the lack of care resources, or the lockdown caused by the COVID-19 pandemic, online psychological treatments are becoming increasingly common among the child and adolescent population, although it is necessary to develop this type of treatment for children at psychosocial risk, since these have been developed mostly for the general population. To this aim, the Online Emotional Self-Regulation Improvement program (Mejora de la Auto-regulación para Menores, Online MAM@) was developed.
ObjectivesTo assess the acceptability of the Online Emotional Self-Regulation Improvement program, by the adolescent.
MethodsThe intervention program was applied to a total of n = 32 children (n = 17 girls) between 11 and 15 years of age. The program consists of 7 target emotions to be worked on, and the acceptance, usability, usefulness, enjoyment of each module and barriers to use by the children were assessed with an adaptation of the Venkatesh and Davis scale. These measures were taken post-test, once the intervention module was completed. The program was applied online for five weeks by the children, and their regular therapists contacted them to provide them with weekly access codes and reminders in case they were not completing the modules.
ResultsIt was observed that the best rated module was the anger module, the most useful module was the sadness module, the module considered to have the highest usability was the fear module, and the most enjoyed module was the sadness module, although all the modules had very high scores above the average and no significant differences were found in the rating of the modules between sexes. As for the most common barriers to use among the children, problems were found with the completion of the intervention, since they often forgot to access the web, and these did not apply what they had learned outside the intervention program.
ConclusionsThe Online Emotional Self-Regulation Improvement program is the first program developed in Spanish language for adolescents at psychosocial risk, and may represent a breakthrough to consolidate these programs in the national scene and bring the therapeutic possibilities for adolescents to the same level as in other parts of the world. Focusing on future versions of the program, it would be advisable to reduce its length and incorporate activities outside the treatment program to guarantee a generalization of what is learned in the intervention program in everyday life situations.
Disclosure of InterestNone Declared
Seeing like an asset manager
- Brett Christophers
-
- Journal:
- Finance and Society / Volume 10 / Issue 2 / August 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. 205-208
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Asset managers have assumed a position of unprecedented power and influence in the control of essential infrastructures of social life, with broadly negative ramifications. But as the commentaries assembled here all insist, it did not – and does not – have to be this way. In this reply, I discuss the potential, as I see it, for the world to be otherwise, offering a rather pessimistic prognosis.
Ultrastructural analysis of synapses and mitochondria in the hippocampus of depressed patiens
- A. Sebők-Tornai, D. Csabai, C. Szekeres-Paraczky, Z. Maglóczky, M. Simon, C. A. Stockmeier, B. Czéh
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S362-S363
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is a common multifactorial disorder, but the exact pathophysiology is still unknown. in vivo and post-mortem studies document volumetric and cellular changes in the hippocampus of depressed patients. Chemical synapses are key functional units of the central nervous system and earlier studies found reduced number of synapses in the prefrontal cortex of depressed patients (Kang HJ et al. Nature Medicine 2012;18(9):1413-1417). Mitochondria are intracellular powerhouses generating chemical energy for cellular biochemical reactions. Recent findings suggest that individuals with impaired mitochondrial function may be vulnerable to develop psychopathologies.
ObjectivesWe investigated synapses and mitochondria in post-mortem hippocampal samples from psychiatric patients.
MethodsThe three study groups were: 1) MDD patients (n=11); 2) patients with alcohol dependence (n=8) and 3) controls (n=10). Controls were individuals who accidentally deceased and had no neuropsychiatric disorders. Three sub-regions of the hippocampus (dentate gyrus, CA3 and CA1 areas were investigated. Ultrathin sections were examined, and photomicrographs were taken for further analysis using a JEOL JEM 1400 FLASH transmission electron microscope. Systematic quantitative analysis was conducted with the Neurolucida system using unbiased counting principles.
ResultsWe could not detect any differences in synapse and mitochondria densities between the patients and controls subjects.
ConclusionsOur preliminary data suggest that despite our expectations hippocampal synapse and mitochondrial densities are rather constant parameters which are not easily affected by psychopathology or alcohol consumption. Potential methodical limitations may also explain this negative finding.
FUNDING:
This research was founded by the Hungarian Brain Research Program 3 and by the TKP2021-EGA-16 project. A.S.T. was supported by the ÚNKP-23-3-I New National Excellence program of the Ministry for Culture and Innovation from the source of the National Research, Development and Innovation Fund.
Disclosure of InterestNone Declared
Mitochondrial respiratory capacity in patients with acute episodes of bipolar disorder compared with clinical remission
- A. Giménez-Palomo, M. Guitart-Mampel, A. Meseguer, M. Valentí, L. Bracco, H. Andreu, E. Vieta, G. Garrabou, I. Pacchiarotti
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S80-S81
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) is a chronic and recurrent disease characterized by acute mood episodes alternated with periods of euthymia. The available literature postulates that a biphasic dysregulation of mitochondrial bioenergetics might be observed in BD.
ObjectivesWe aimed to explore differences in in vivo mitochondrial respiration (1) intra-individually: longitudinally within patients during an acute mood episode of BD and after clinical remission, and (2) inter-individually: between patients with BD on depressive or manic episodes and healthy controls (HC).
MethodsPatients admitted to our acute psychiatric ward with a manic episode or bipolar depression were recruited. Different mitochondrial oxygen consumption rates (OCRs) were assessed during the acute episode (T0) and after clinical remission (T1) in one million of peripheral blood mononuclear cells (PBMC): Routine, Leak, ETC and Rox. They were measured as picomoles of oxygen per million cells (pmol O2/million). This experiment was also conducted in HC. High-resolution respirometry was performed at 37°C by polarographic oxygen sensors in a two-chamber Oxygraph-2k system. Manic and depressive symptoms were assessed using standardized psychometric scales. Oxygen consumption capacity was compared (1) intra-individually, during acute episodes and after clinical remission, and (2) inter-individually, during acute manic and depressive episodes, and in HC. Statistical analyses were performed with SPSS, GraphPad and R Statistics.
Results20 patients with BD (15 manic, 5 depressed) and 10 HC were included. A significant increase in the maximal oxygen consumption capacity (ETC) was observed in clinical remission (27.4 ± 17.4) compared to the acute episodes (21.1 ± 11.7, p = 0.001), which remained significant after subtracting Rox from the other rates (p = 0.001). At T1, patients admitted with a manic episode tended to show higher mean ETC (31.2 ± 18.7) compared with T0 (24.1 ± 12.0, p = 0.074); the tendency persisted after Rox subtraction (p = 0.076). Patients admitted with a depressive episode also showed higher ETC means in T1 (16.3 ± 3.8) compared to T0 (12.1 ± 3.4), but there were not significant differences (p = 0.231). When HC, manic and depressive patients at T0 were compared between them, significant differences were observed in ETC (H =8.5; p =0.014) and Rox (H =13.8; p = 0.001). After Rox deduction, differences in ETC remained (H =11.7; p = 0.003). Individuals with bipolar depression showed lower ETC rates (12.1 ± 3.4) than those with a manic episode (24.1 ± 12.0; t = -3.5, p = 0.003), which was also found after Rox deduction (p = 0.001).
ConclusionsIn both manic and depressive episodes in BD, mitochondrial respiration might be reduced and increase after clinical remission. Further studies with larger samples will allow to confirm these results and also to identify potential mitochondrial state-dependent biomarkers.
Disclosure of InterestA. Giménez-Palomo Grant / Research support from: AGP is supported by a Rio Hortega 2021 grant (CM21/00094) from the Spanish Ministry of Health financed by ISCIII and cofinanced by Fondo Social Europeo Plus (FSE+)., M. Guitart-Mampel: None Declared, A. Meseguer: None Declared, M. Valentí: None Declared, L. Bracco: None Declared, H. Andreu: None Declared, E. Vieta: None Declared, G. Garrabou: None Declared, I. Pacchiarotti: None Declared
Relationship between MASC scores and diagnosis in a sample of children and adolescents in Spain
- C. Canga-Espina, C. Vidal-Androher, A. Diez-Suarez, C. Maestro-Martin, M. Vallejo-Valdivielso
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S462-S463
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anxiety is one of the most common Mental Health diagnosis in underage population. We decided to study if there was any variable that would lead us to a specific diagnosis, using the MASC questionnaire (Multidimensional Anxiety Scale for Children).
Objectives1. Describe the prevalence of the different anxiety disorders and the differences in its prevalence according to sex. 2. Examine possible differences and associtions between MASC questionnaire scores and a specific anxiety diagnosis.
MethodsThis is a descriptive, observational, retrospective, quantitative study with data from patients between June 2016 and 2023. Inclusion criteria: 3-18 year-old-spanish-speakers who met criteria for a ICD-11 disorder. Exclusion criteria: absence of legal representatives, intellectual disability. Variables: sex, ICD-11 diagnosis, MASC’s subscales (Physical Symptoms, Harm Avoidance, Social Anxiety and Separation Anxiety) and CGI. Statistical analyzes were performed with STATA-15 program, using as independent variables MASC questionnaire and dependent one Anxiety Diagnosis.
ResultsThe sample contains 1024 patients. Figure 1 shows the distribution of Anxiety Disorders: Unspecified Anxiety Disorder (47%), Separation Anxiety Disorder (23%), Simple Phobias (9%) and Social Anxiety Disorder (7%). Figure 2 represents the distribution by sex, with the differences being statistically significant (p<0.05) for all anxiety disorders, meaning that girls have higher prevalence of all anxiety disorders. Figure 3 shows how age correlates significantly and directly with all the subscales, meaning the older the patients are the higher the scores. We also found that boys have lower scores and a lower percentage of alteration in all subscales. CGI scale also correlates positively with all the subscales, specially with Physical Symptoms. All these data have been adjusted.
Image:
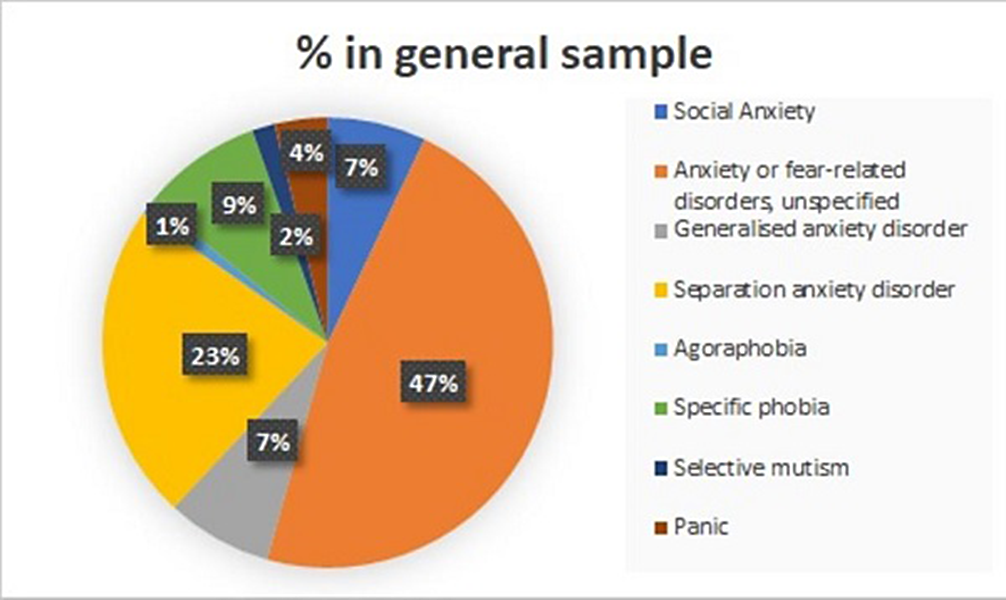
Image 2:
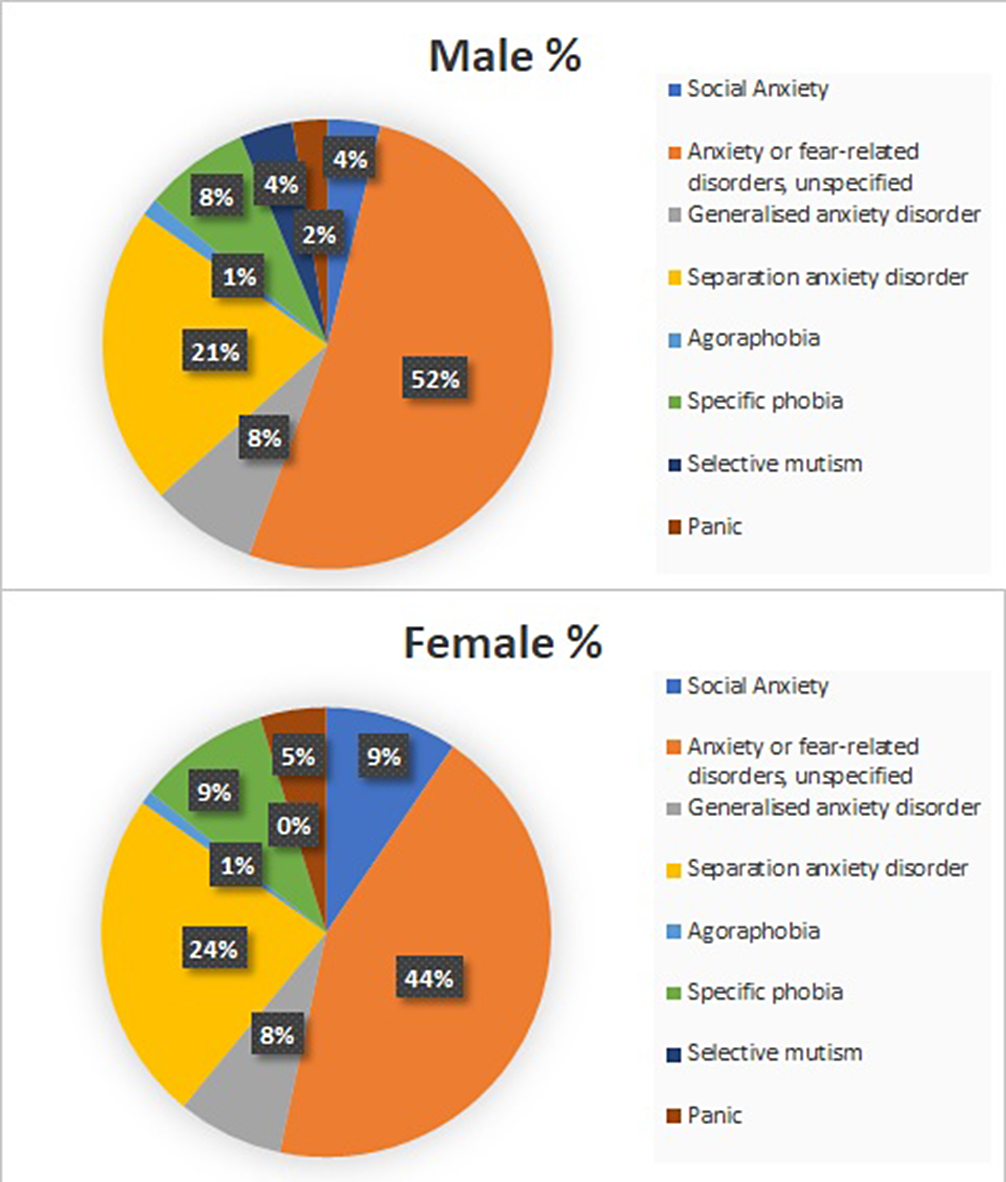
Image 3:
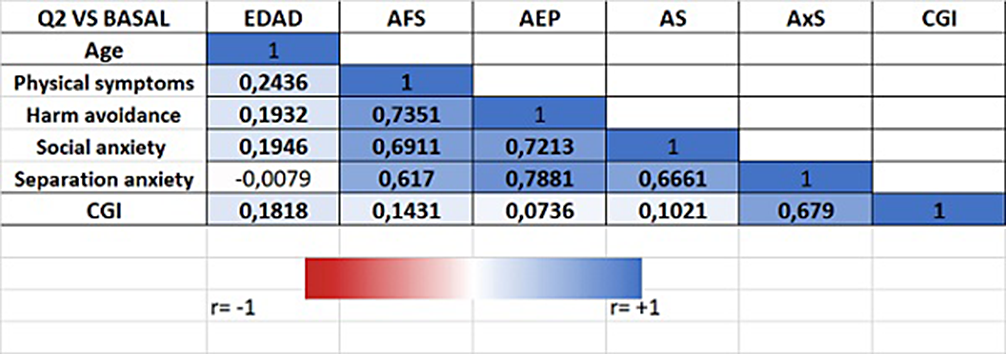 Conclusions
ConclusionsAnxiety disorders are the most common form of Mental Disorder in young people (lobal prevalence of 6.5%, Rapee et al.2023). Prevalence for specific Anxiety Disorders in underage population are less reliable, because of the unequal age of samples (Rapee et al.2023). Separation Anxiety disorder is the most prevalent among children (La Maison et al., 2018), while Social Anxiety disorder is among adolescents (Lawrence et al.2015). We did not categorized our sample, being Separation Anxiety disorder the most frequent followed by Social Anxiety. We observed a correlation between some subscales and a specific diagnosis: the risk of presenting a Social Anxiety disorder is multiplied by 1.08 for each point of increase in that subscale and the risk of presenting a Separation Anxiety disorder is multiplied by 1.05 for each increase of 1 point in Separation Anxiety subscale. However, the diagnosis of Simple Phobia decreases with the increase in scores in all subscales, maybe due to the fact that there are not many items that specifically evaluate fears.
Disclosure of InterestNone Declared
Results of anxiety disorders in a medical professional
- P. Sarantuya, B. Putev, T. Myatav
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S424
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anxiety is the most prevalent disease in the world. Symptoms of anxiety disorders affect everyone. The symptoms are worse after a long period of time and more severe disease than normal. A study was conducted to support the assumption that it is an opportunity to improve healthcare services.
Objectives1. Anxiety disorders of doctors and medical specialists of Selenge Province General Hospital
2. Determine the relationship between certain factors and certain factors of anxiety disorders
MethodsThe GAD7, SRQ20, and PHQ9, sleep system detection questionnaire methods issued by WHO for doctors of primary health care institutions were analyzed by analytical research snapshot model from 03.15 to 04.05, 2023.03.22. /1/01 was obtained and the survey was conducted.
ResultsIn the study, 23-65-year-olds received medical care, and the average life expectancy was 37.05 years. 30% (27) of the respondents did not have anxiety disorders, 36.67% (33) had mild anxiety disorders, 18.89% (17) had moderate anxiety disorders, and 14.44% (13) had severe health problems. 6.67% (6) of the respondents had no depression, 10% (9) had very mild depression and could cope on their own, 24.44% (22) had moderate depression and could cope, and 27.78% (25) with healthy depression. 24.44% (22) had major depressive disorder and 6.67% (6) had major depressive disorder. According to correlation analysis, GAD7 score with SRQ20 stress score r=0.76 and PHQ9 mood score with r=0. the inverse association was statistically significant at p=0.00. PHQ9 depression score had a strong effect on SRQ20 stress score r=0.74, p=0.00, and GAD7 score r =0.46, p=0.0000. r=-0.40, p=0.00 had a moderate inverse relationship with age, and r=-0.24, p=0.00 had a weak inverse relationship with age. In linear regression analysis, the GAD7 anxiety disorder score increased by 48.8% (p=0.00) when fixed at one, which was statistically significant. In logistic regression analysis, PHQ9 depression score increased by 35.08% (p=0.01) per entry. In composite logistic regression analysis, the PHQ9 depression score was statistically significant OR=4.07 (p=0.01) multiplied by one.
ConclusionsDoctors and medical professionals include psychological health research, testing, treatment, psychological counseling, and health care. Anxiety disorders are related to stress, depression, satisfaction, and age, while depressive disorders are anxiety disorders.
Disclosure of InterestNone Declared
Supervision an essential tool in medical (and psychiatric) training
- R. J. Van Der Gaag
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S793
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Supervision is an essentail tool in medical training and especially in psychiatry and psychotherapy. It emcopasses two distinct aspects namely: coaching in the workplace aimed at developping competences (pyramid of Miller) and on the other side a safe place to reflect on ones personal development as a professional. This mentoring should be distinguised from the personal training psychotherapy. The mentoring supervisor will take the doctor’s pledge as a starting point of professional development. But will also encourage the resident to become aware of elements of transference and counter transference in his/her clinical work, helping to foster empathy “maximal understanding with respect for professional distance. This, not only for the benefit of the patient and his/her security, but also in order to take care of one’s own health and developing a sound balance between work and private life.
Too often supervision is taken for granted once the resident has become a consultant. Along with examples of the techniques and the pitfalls of supervison, the presenters will plea for training and intervision as part of the development of the supervisor!
ObjectivesRaise awareness for the competences needed to become a valuable supervisor and the place supervision in its two aspects (coaching and place of reflection) should take in the training of medical doctors and especially psychiatrists
Methods- an inventory of the place of supervision in training in psychiatry throughout Europe
- looking into competences needed in order to develop a sound professional attitude
- looking into the competencies needed to become a valuable supervisor
Results- supervision is differently defined and given in training in psychiatry throughout Europe
- the competences needed in order to develop a sound professional attitude are defined in the Doctor’s Pledge (World Medical Association 2017) but should be refined according to the specialty with special attention to aspects of psychiatry alien to other specialities
- along with Teaching the Teachers - special trainings are available to become a supervisor
ConclusionsSupervision is an essential tool in medical/psychiatric training, but it needs to be taken seriously in terms of developing the competences needed but also maintaining them in intervision with the colleagues of the training staff
Disclosure of InterestNone Declared
Suicide planning type interventions as an evidence based alternative for no-suicide contracts
- A. Garbacka, M. Bzowska
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S777
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicidality is a common concern in psychiatric patients and one of the leading causes of death in adolescents and young adults. (Adolescent health. (2019, November 26) WHO). Some mental health professionals engage in a no-suicide contract with their patients. In this type of intervention, the patient usually agrees to not harm or kill himself/herself. There is an increasing body of evidence to support brief interventions, such as group of safety planning-type interventions (SPTIs) (McCabe et al. MC Psychiatry, 2018, May 3; 18(1)). Safety planning is derived from cognitive therapy and cognitive behavioral therapy used for suicide prevention.
ObjectivesOur objective was to summarize and critically analyze current evidence of effectiveness of SPTIs and no-suicide contracts in suicide prevention.
MethodsWe conducted a literature review to compare no-suicide contract to safety-planning interventions in suicide prevention.
ResultsAlthough no-suicide contracts may work for some individuals, there is not enough quantitative evidence to support such contracts as clinically effective tools. A recent meta-analysis has shown that SPTIs were associated with reductions in suicidal behaviors although no effect was identified with frequency of suicidal thoughts (Nuij et al. (2021, April 30). The British Journal of Psychiatry, 219 (2), 419–426).
ConclusionsBased on the evidence and straightforward implementation of SPTIs in different clinical settings it may to be a more effective alternative to no-suicide contracts.
Disclosure of InterestNone Declared
Clozapine-induced pyoderma gangrenosum. A case report
- M. Peyioti, P. Argitis, O. Pikou
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S146-S147
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is an atypical antipsychotic medication which is mainly used in cases of treatment-resistant schizophrenia. Although it has several advantages over other typical and atypical antipsychotic medication, such as fewer relapses and lowering the risk of tardive dyskinesia and suicide it also has a range of adverse effects which makes compliance an issue for many patients.
Pyoderma gangrenosum (PG) is a rare neutrophilic dermatosis clinically characterized by painful pustules or nodules that rapidly evolve in ulcers with violaceous, undermined borders and raised periphery. The etiopathogenesis of the disease remains unclear, however PG is usually manifested in the setting of an underlying immune-mediated disease, more commonly inflammatory bowel disease, rheumatoid arthritis and haematological malignancies.
ObjectivesNevertheless, in the literature there are scarce reports of drug-induced PG.
MethodsWe present the case of a 56-year-old woman with a diagnosis of refractory schizophrenia on clozapine treatment for 4 months, who was admitted to the emergency department for a skin eruption localized on the trunk, genital area and extremities. The clinical examination revealed numerous, discrete erythematous macules, papules and plaques with central necrosis, and multiple, sharply marginated ulcers with undermined, red to purple border. Further physical examination disclosed no systemic findings and laboratory analyses and skin biopsy were performed.
ResultsOn work-up, white blood cell count and C-reactive protein (CRP) were elevated, while blood and pustule cultures were negative. Histologic examination revealed dermal necrosis and inflammation, features consistent with the diagnosis of PG. The pathergy test was positive.
Image:
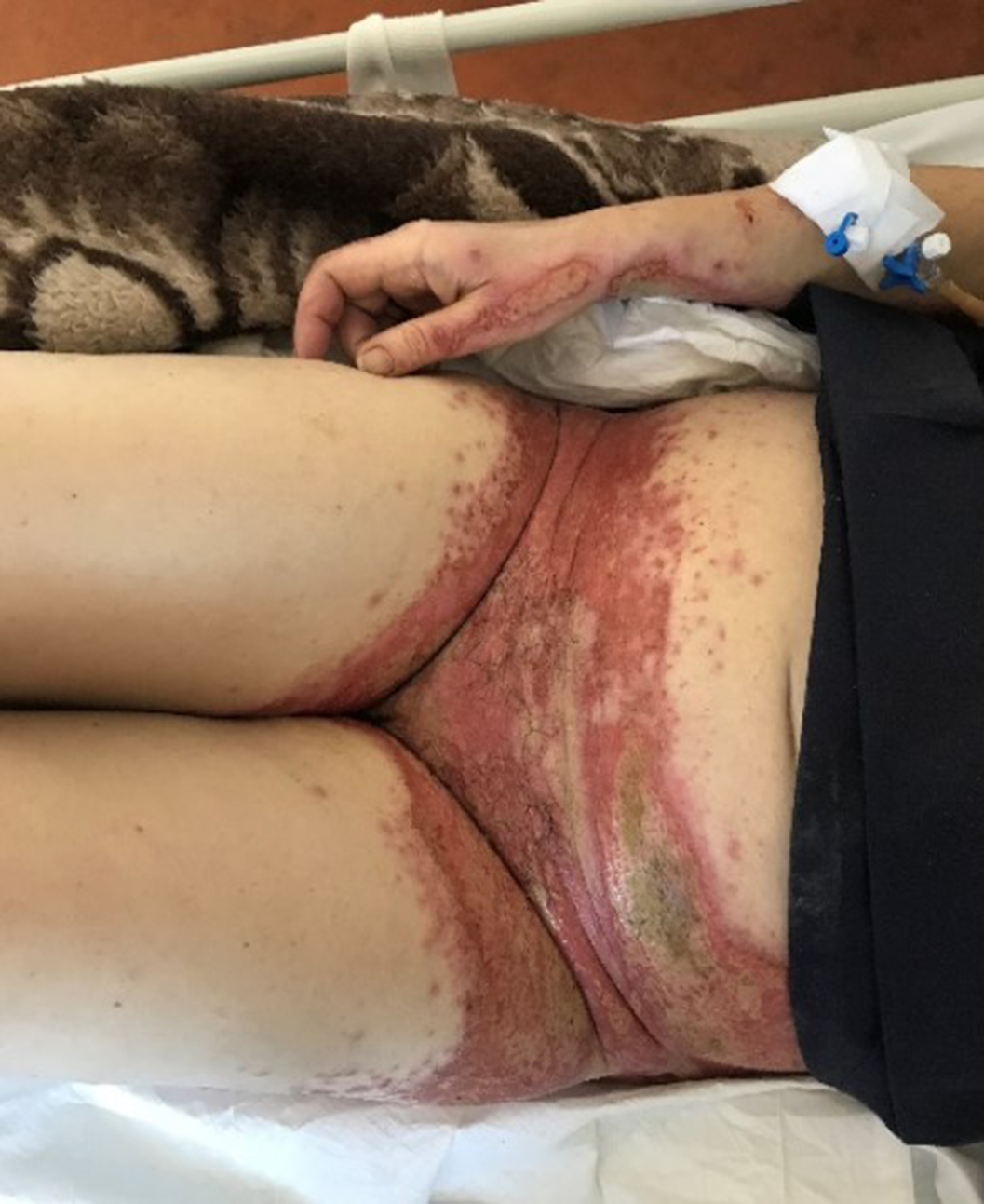
Image 2:
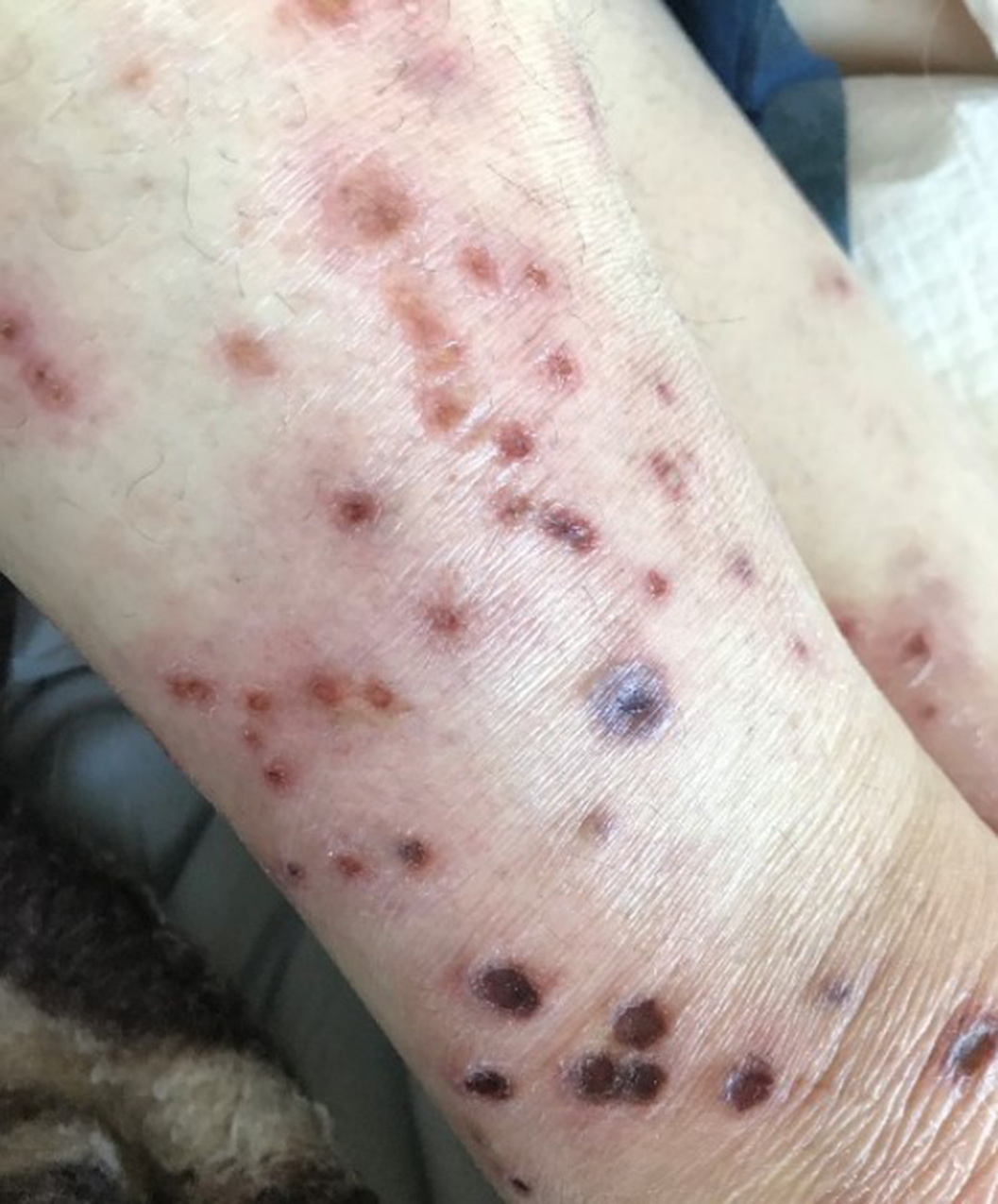
Image 3:
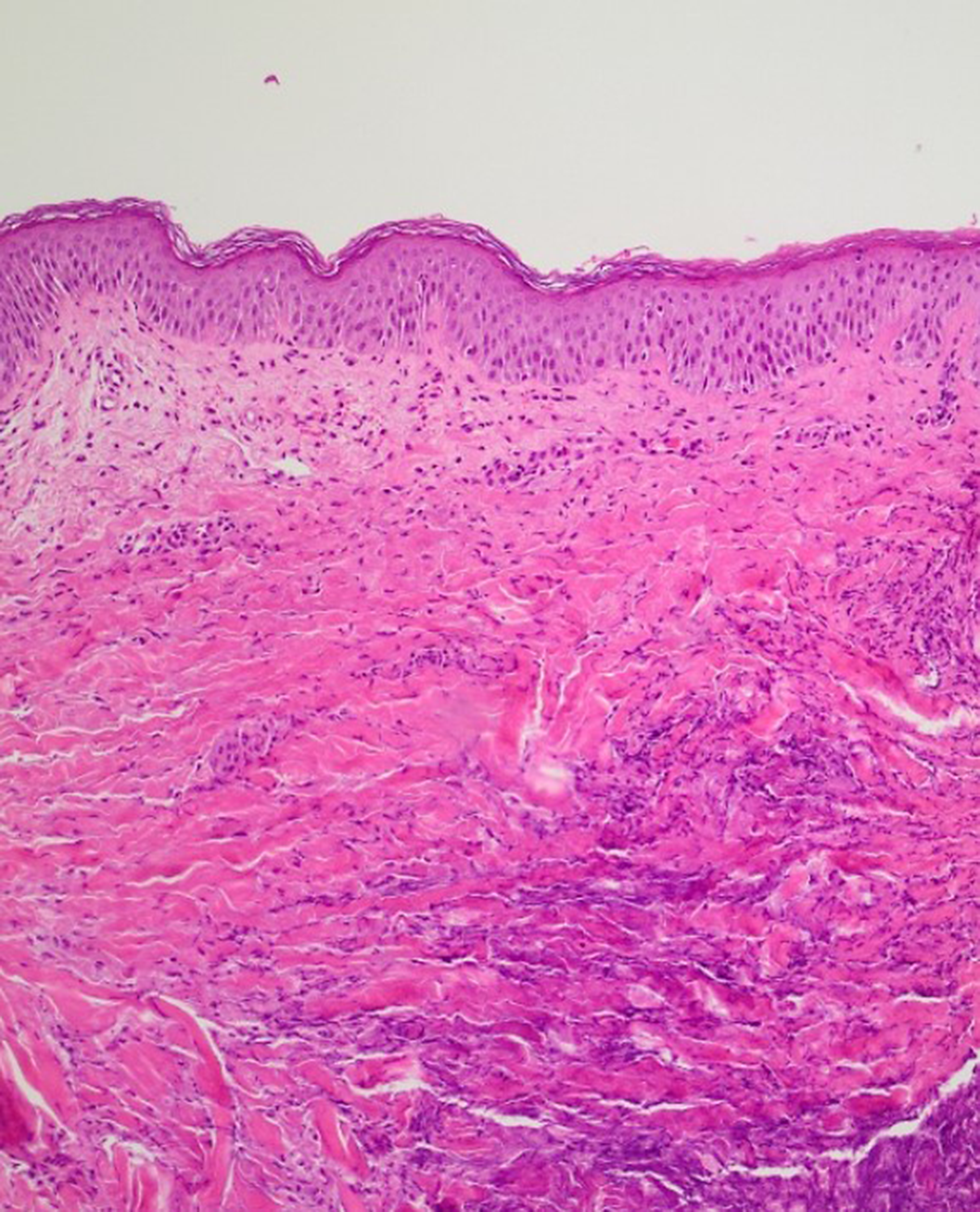 Conclusions
ConclusionsPyoderma gangrenosum is a rare autoinflammatory skin disorder of unknown etiology. The pathogenesis of the disease is not well understood, but drug-induced PG is considered to result from neutrophil dysfunction and dysregulation of the inflammatory response. Cases of drug-induced PG are rare and attributed to certain drugs. Clozapine is an antipsychotic medication for the treatment of refractory schizophrenia. It is suggested that clozapine alters plasma TNF-α levels and thus can modulate the inflammatory response. To date, a variety of adverse skin reactions (Stevens- Johnson syndrome, DRESS syndrome etc) have been previously described in the literature. However, to the best of our knowledge, this is the first case which strongly indicates the likely association between clozapine and drug-induced PG.
Disclosure of InterestNone Declared
Disconnecting from my heartbeat: About a case of derealization in a critically ill patient
- C. Alario Ruiz, M. S. Oscar, N. Navarro Barriga, R. R. Beatriz, R. V. Claudia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S420-S421
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depersonalization/derealization encompasses a series of symptoms that are difficult to describe by the patient, as well as complex to diagnose by the professional, and can go through multiple diagnoses prior to the diagnosis of certainty.
ObjectivesIt is proposed, through a clinical case, to know the characteristics of this disorder, evolution, differential diagnosis and therapeutic possibilities
Methods62-year-old male, history of harmful alcohol consumption and a previous admission to a psychiatric short hospitalization unit for self-injury (superficial cuts in the context of severe mental illness of his wife) post-transplantation who is required by ideas of death, anhedonia and lack of collaboration in patient, The day before the evaluation, refusal to take oral treatment, selective mutism. Pre-transplant evaluation where no psychopathological alteration was observed.
ResultsWhat is initially assessed and treated as a confusional episode of inactive type, through a correct psychopathological examination and with subsequent continuous interviews, with mood fluctuations throughout the admission, is subsequently oriented as an acute stress disorder, adaptive reaction with an anxious-depressive component and finally concluding that we are facing a dissociative disorder, highlighting the depersonalization/derealization on a dysfunctional personality base.
ConclusionsCharacteristic of depersonalization is the great difficulty in describing symptoms, the feeling of being disconnected from one’s own body, emotions and reality. The latest studies on etiopathogenesis with MRI show an inhibitory response on the limbic system by hyperactivation of the ventrolateral prefrontal cortex as well as a decrease in the autonomic response, the initial result being the attenuation of the processing of emotions. Among the differential diagnoses: post-anxiety illness disorder, major depressive episode, other dissociative disorders, panic disorder, psychotic disorder, substance-induced disorder There are several partially effective treatments, although the results so far are poor. SSRIs, quetiapine and naltrexone have been tried. Partial efficacy with lamotrigine together with SSRIs and, if high levels of anxiety coexist, SSRIs together with clonazepam. There are studies where psychodynamic psychotherapy, behavioral therapy and hypnosis have obtained partially effective results.
Disclosure of InterestNone Declared







