3294077 results
ACOMPANYA’M a novel multimodal intervention plan
- I. Insa Pineda, I. Rueda Bárcena, C. Lamborena Ramos, F. de Pedro Melgarejo, A. Planas Bas, T. Prieto Toribio, E. Lujan Lujan, M. Ribas Siñol
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S597-S598
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Residential Educational Therapeutic Unit Accompany from Hospital Sant Joan de Déu Barcelona, is a device integrated into the public health network, intended for the comprehensive care of children and adolescents under 18 years of age who suffer from an illness complex mental disorder, at serious risk of becoming chronic and generating significant disabilities at a functional, cognitive and emotional level. It was a result from a joint venture between the Department of Social Rights and the Department of Health. The device was created to respond to the increase in behavioral problems and mental health disorders of children underguardianship.
ObjectivesGeneral Objective
To improve the quality of life in the physical, mental and social spheres of vulnerable children and adolescents with serious complex mental pathology through a biopsychosocial and community care model that integrates health, social, family and educational care and which is aimed at the recovery of the person’s life project.
Specific Objectives
To offer intensive intervention, personalized and in a co-responsible manner, that is to say, that integrates the therapeutic, education, social services and child protection teams.
Promote the community and social reintegration avoiding stigmatization and social exclusion.
Improve the intra-family relationship and the burden perceived by caregivers.
Decrease the number of renunciations of parental authority of a minor.
MethodsThe unit has a capacity for 28 beds: 23 places for children/adolescents underguardianship of the administration and 5 places for cases that are at risk of family claudication due to their therapeutic and educational needs.
There are 5 coexisting therapeutic units. The apartments are referred as ‘homes’ and their organization is designed to encourage the active participation of residents with the professionals who attend them.
The Unit has a multidisciplinary team made up of the following professionals: Psychyatrists, Nurses, clinical psychologists, Social Workers, Educational worker, nursing assistants, administrative.
Results- 110 children and adolescents have been taken care, with an average cumulative stay of 13 months. In all cases in which the family had the guardianship of the patient, family claudication has been avoided There is a 36% discharge of those patients under guardian that have returned to their original family home 100% of the cases have been linked to an educational center adapted to their needs or to a training project
Image:
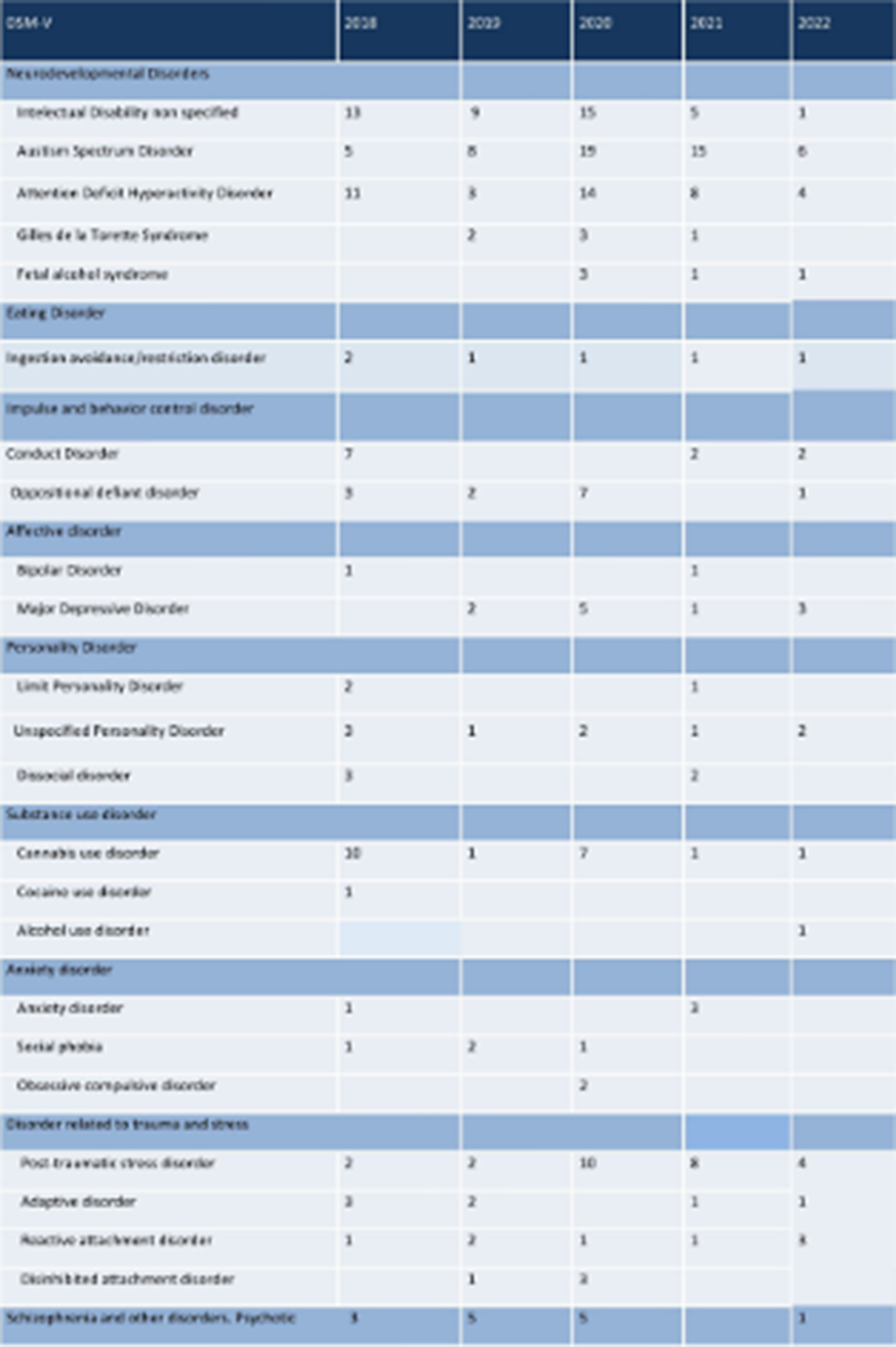
Image 2:
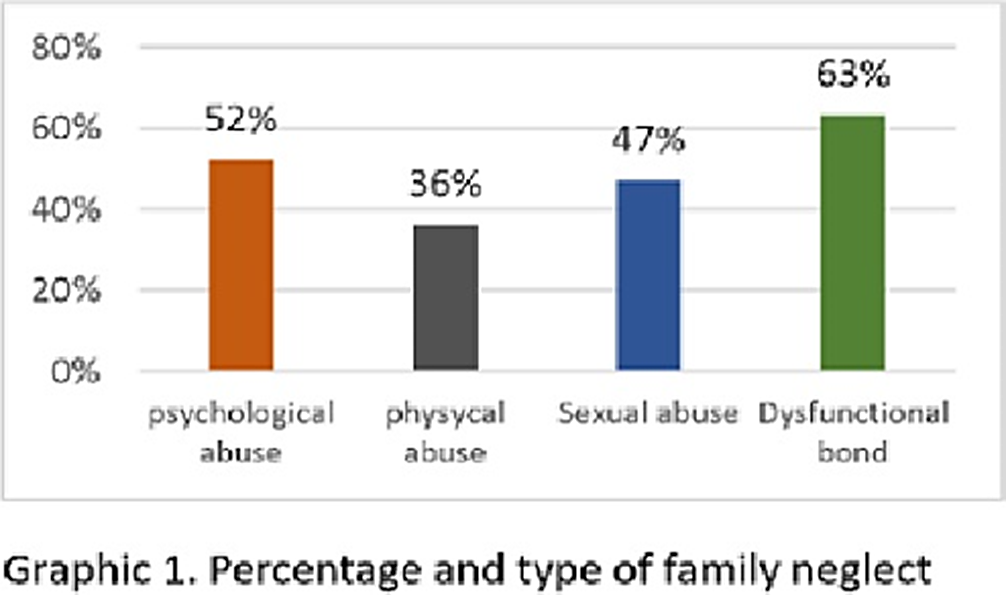 Conclusions
ConclusionsOverall, the care model implemented by the population served in the Acompanya’m unit is positively evaluated. Since it provides an intensive and personalized care, treatment and intervention for children suffering from a serious mental disorder of high complexity. A comprehensive, personalized, interdisciplinary approach is offered, coordinated and co-responsible with educational, protection and social services.
Disclosure of InterestNone Declared
Abnormal Neural Activation in Attention-Deficit/Hyperactivity Disorder: A Meta-Analysis of Functional Magnetic Resonance Imaging Studies
- G. Zamora, C. Baten, A. M. Klassen, J. H. Shepherd, A. Catchpole, E. Davis, I. Dillsaver, C. E. Hunt, E. Johnson-Venegas, P. Hamilton, M. D. Sacchet, E. Woo, J. A. Miller, D. W. Hedges, C. H. Miller
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S72-S73
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Attention-deficit/hyperactivity disorder (ADHD) is a highly prevalent psychiatric condition that frequently originates in early development and is associated with a variety of functional impairments. Despite a large functional neuroimaging literature on ADHD, our understanding of the neural basis of this disorder remains limited, and existing primary studies on the topic include somewhat divergent results.
ObjectivesThe present meta-analysis aims to advance our understanding of the neural basis of ADHD by identifying the most statistically robust patterns of abnormal neural activation throughout the whole-brain in individuals diagnosed with ADHD compared to age-matched healthy controls.
MethodsWe conducted a meta-analysis of task-based functional magnetic resonance imaging (fMRI) activation studies of ADHD. This included, according to PRISMA guidelines, a comprehensive PubMed search and predetermined inclusion criteria as well as two independent coding teams who evaluated studies and included all task-based, whole-brain, fMRI activation studies that compared participants diagnosed with ADHD to age-matched healthy controls. We then performed multilevel kernel density analysis (MKDA) a well-established, whole-brain, voxelwise approach that quantitatively combines existing primary fMRI studies, with ensemble thresholding (p<0.05-0.0001) and multiple comparisons correction.
ResultsParticipants diagnosed with ADHD (N=1,550), relative to age-matched healthy controls (N=1,340), exhibited statistically significant (p<0.05-0.0001; FWE-corrected) patterns of abnormal activation in multiple brains of the cerebral cortex and basal ganglia across a variety of cognitive control tasks.
ConclusionsThis study advances our understanding of the neural basis of ADHD and may aid in the development of new brain-based clinical interventions as well as diagnostic tools and treatment matching protocols for patients with ADHD. Future studies should also investigate the similarities and differences in neural signatures between ADHD and other highly comorbid psychiatric disorders.
Disclosure of InterestNone Declared
Impulsivity as a predictor factor of health-related risk-taking
- A. Megías-Robles, L. Moreno-Ríos, R. Megías-Robles, A. Martínez-Estrella, M. A. Torres
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S652
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a broad consensus that risk taking is largely determined by risk perception. However, previous literature has shown numerous examples of situations associated with potential health risks where our decisions are not made in accordance with the level of perceived risk.
ObjectivesThe aim of the present research was to investigate the role of impulsivity in the explanation of the discordance observed between risk perception and risk-taking in health-related domains.
MethodsThe sample consisted of 612 participants (Mage = 23.54, 73,2% women). All participants were assessed for levels impulsivity and levels of risk perception and risk-taking propensity in contexts related to health.
ResultsResults revealed that higher levels of impulsivity were significantly related to a lower tendency to perceive and take risks in the health domain. Most important for our objectives, we observed that the relationship with impulsivity was significantly stronger for risk taking than for risk perception. Moreover, impulsivity significantly predicted risk taking propensity when controlling for risk perception.
ConclusionsThese findings suggest that, in the health-related domains, impulsivity can differentially affect risk perception and risk taking, thus, offering a possible explanation for the inconsistencies observed in the previous literature.
Disclosure of InterestNone Declared
Regional Inequalities in Diagnosis and Therapies in Greece regarding Autism Spectrum Disorders
- R. Kouznetsov, P. Angelopoulos, S. Moulinos, A. Andrianopoulou, I. Dimakos, P. Gourzis, E. Jelastopulu
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S112
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Autism spectrum disorders (ASD) represent a major public health concern on a global scale. The increasing prevalence of ASD worldwide, coupled with the arising demand for treatments, underscores its important role in the public mental health discourse. Ensuring the equitable integration of children with ASD and their families into all aspects of society becomes an imperative task, in order to eradicate the stigma associated with the broad spectrum of autism, encompassing both visible and concealed dimensions.
ObjectivesThe primary objective of this study was to determine the crude prevalence of ASD in Greece nationwide, while also examining regional disparities in both prevalence and therapies. The study spanned a three-year period from February 2019 to February 2022 and relied on retrospective data sourced from the Greek National Organization for Healthcare Services Provision (EOPYY).
MethodsEOPYY provided de-identified data, including information such as sex, age, diagnosis, and treatment for each child, facilitated by hashed social security numbers. Statistical analysis of the dataset was performed using the open-source statistical program R.
ResultsA total of 18,245 children aged 2 -17 years were diagnosed with ASD in Greece, representing a nationwide crude prevalence rate of 1.16%. Regional disparities were evident, with prevalence rates ranging from 0.49% in the North Aegean to 1.57% in Crete. Over the three-year study period, a total of 15,328,327 non-medical therapies were prescribed, corresponding to an annual average of 264 therapies per child. Statistically significant differences between the thirteen regions in Greece were observed, ranging from 230 to 323 annual therapies per child.
ConclusionsOur findings align Greece’s ASD prevalence with the global estimate of 1 in 100 children, as per the World Health Organization. Disparities between rural and urban areas in Greece may be attributed to differences in diagnostic procedures and the availability and accessibility of specialized services for autistic individuals. Thus, the establishment of a national surveillance system for ASD is recommended to enhance our understanding of the autism spectrum, monitor changes in prevalence, and identify potential contributing factors to autism conditions. Furthermore, these evidence-based results offer invaluable insights for crafting policies concerning healthcare, education, and employment for individuals with ASD in order to ensure the development of people with autism, their wellbeing, and a good quality of life.
Disclosure of InterestNone Declared
Illness-Related Domestic Violence Experiences of Individuals Diagnosed with Obsessive Compulsive Disorder: A Qualitative Study
- Z. Bayram, M. C. Aktaş, H. Gundogdu
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S633
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Obsessions and compulsions often focus on routine life actions such as consuming, bathing and living in public, so the disorder interferes with the social, family and occupational functioning of both the individual and their caregiver. In OCD, caregivers are often involved in the ritual behaviors of the individual, either by providing avoidance or by assisting in ritual behaviors. Individuals with OCD are often exposed to aggression from family members because of these behaviors. Research has shown that individuals with OCD may experience illness-related domestic violence. In the literature review on the subject, there were no qualitative studies examining the experiences of individuals diagnosed with OCD towards domestic violence caused by the symptoms of the disease. A mix-method study conducted by aimed to explore the illness-related domestic violence experiences of individuals diagnosed with OCD. The study utilized both quantitative and qualitative methods to gather data from individuals with OCD. The findings of the study revealed that a significant number of individuals with OCD reported experiencing domestic violence related to their illness. This study highlights the importance of addressing the issue of domestic violence in individuals with OCD and the need for appropriate interventions and support.
ObjectivesThis study was planned to examine the experiences of individuals diagnosed with OCD regarding domestic violence caused by the symptoms of the disease in Turkey.
MethodsThe sample of the study was determined by purposive sampling method. The study was conducted with individuals diagnosed with OCD who were being treated in the psychiatric clinics of two university hospitals. The study used mixed methods and was planned in two phases. In the first stage, Socio-Demographic Data Form and Yale-Brown Obsession Compulsion Scale were used. After reviewing the results of these scales, individual in-depth interviews were conducted with 20 patients who had a history of domestic violence and scored above 16 on the Yale Brown Obsessions and Compulsions Scale. Data saturation was deemed to have been reached and data collection was terminated.
ResultsThe analysis of the data is still ongoing in detail by the researchers. The findings and relational implications of the study will be presented.
ConclusionsIt is thought that the results of the study will provide a basis for further research and intervention programs and contribute to the literature by determining the types of violence experienced by individuals diagnosed with OCD from family members due to the disease, how patients feel in the face of the problems they experience and how they cope with it. In addition, the results of the study are expected to help intervention programs to be developed for families to strengthen treatment adherence.
Disclosure of InterestNone Declared
Domestic violence in Tunisian women during pregnancy and anxiety: which association?
- R. Jbir, L. Aribi, I. Chaari, S. Mohamed, G. Fatma, M. Ines, N. Messedi, J. Aloulou
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Domestic violence is a major public health problem. The situation is alarming in Arab countries: the prevalence of domestic violence is 39.3% in Saudi Arabia, 55% in Morocco and 62.2% in Egypt.
In Tunisia, a national survey carried out by the national family planning office in 2010, published in July 2011, drew attention for the first time to the frequency of this phenomenon in Tunisia and the recurrent nature of this form of violence. Unfortunately, few studies have focused on domestic violence during pregnancy and its impact on the mental health of expectant mothers.
ObjectivesTo study the prevalence of domestic violence during pregnancy among Tunisian women consulting in the context of medical expertise and its association with anxiety.
MethodsOur study was descriptive and analytical cross-sectional, carried out with women examined in the context of medical expertise following domestic violence at ‘Hedi Chaker hospital’,Sfax , from May 2021 until January 2022.
An anonymous survey was asked to these ladies, it included a section for collecting socio-demographic data.
The HADS questionnaire was used to screen for anxiety.
Results122 responses was collected. The average age of victims was 35.66 ± 9.94 years.
All the women in our population study were married, and each one was a victim of at least one form of violence. The majority (86.1%) had children. Most of them had secondary (44.3%) or university (31.1%) level education.
More than half of the women (63.9%) had no occupation.
Sixty-five women (53.3%) were assaulted during pregnancy, 43% of whom suffered from complications of varying severity.
Different consequences on pregnancy were reported with decreasing prevalence: 16.9% hospitalization in a gynecological ward, 13.8% abortion, 6.2% fetal death in utero and premature delivery in 4.6% of cases.
According to the HADS, seventy-six of women surveyed (62.3%) had anxiety symptoms.
Anxiety was significantly associated with exposure to violence during pregnancy (p=0.03).
ConclusionsOur results showed a significant incidence of domestic violence during pregnancy and a significant association with anxiety.
Different actions must be taken towards these anxious women such as: Identify a “referent” in maternity wards to screen for domestic violence and directing women to structures and shelters that can help and, above all, protect them.
Disclosure of InterestNone Declared
Unipolar and Bipolar Depression : Which Differences?
- M. Turki, A. Labyadh, W. Abid, N. Halouani, S. Ellouz, J. Aloulou
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S438-S439
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depression is a common mental disorder whose management remains delicate, given the trans-nosographic nature of this syndrome. Two common types of depression are bipolar and unipolar depression. Although they share many similar symptoms, several differences between the two pathologies are suggested in prior studies.
ObjectivesWe aimed to compare the disease characteristics and evolution of unipolar and bipolar depressed patients.
MethodsWe conducted a retrospective descriptive and analytical study among medical records of 167 patients hospitalized for a depressive episode (DE) at the Psychiatry “B” Department, Hedi Chaker University Hospital (Sfax, Tunisia), during the period between 2015 and 2017. Patients were divided into two groups according to DSM-5 criteria: those with bipolar disorder I or II (bipolar depression) versus those with major depressive disorder (unipolar depression).
ResultsThe mean age of our patients was 37.6 years, with a female predominance (sex-ration F/M =1.7). The age of onset of the disease was earlier in bipolar depressed patients (29.36 versus 31.89), without a significant relationship. Family psychiatric history was significantly more prevalent in bipolar disorder patients (73.5% versus 37.3%; p<0.001). Bipolar patients are more likely to be unemployed (65.3% versus 50.8%), but without a significant relationship.
Bipolar patients were more likely to be hospitalized for suicide attempts (44.9% versus 35.6%; p=0.2).
ConclusionsDistinguishing between major depressive disorder and bipolar disorder is important because there are differences in the optimal management of these conditions.
Disclosure of InterestNone Declared
The opportunity for e-mental health to overcome stigma and discrimination
- K. Subramaniam, A. Greenshaw, A. Thapliyal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S549-S550
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many with mental illness do not seek treatment, often due to stigma; be it public, self, or institutional type. To improve outcomes, stigma needs addressing.
ObjectivesUnderstand the opportunity for e-mental health to help overcome stigma and, to provide an expert opinion to foster its adoption.
MethodsWe conducted literature searches using the terms ((mental health) AND ((stigma) OR (discrimination))) AND (((((digital tools) OR (digital services)) OR (healthcare apps)) OR (digital solutions)) OR (digital technology)), limited to 2007 – 2023, identifying 223 citations, 9 of which were relevant for this evaluation, including 4 systematic reviews (Table 1).
ResultsLiterature reports suggest that e-mental health may be useful for addressing stigma and reducing the treatment gap. While it was not consistently as good as face-to-face services, e-mental health tools were frequently shown to be effective in reducing stigma, improving mental health literacy, and increasing help-seeking behaviors. Tools included web-based breathing, meditation, and CBT; suicide prevention apps; and online videos and games. Experts from a 2022 global Think Tank session convened by eMHIC, opined and emphasised that embracing e-mental health must not leave people behind nor reinforce inequality and that structural barriers must first be acknowledged and overcome. Creating a shared understanding of the challenge and of terminology is essential, as is codesigning any solution together with people with lived experience.
Table 1. Systematic literature reviews
Study Interventions Findings SLR + meta-analysis, 9 studies, n=1916 (Goh et al. Int J Ment Health Nu 2021;30:1040–1056) - Web-based program
- MIDonline
- AboutFace
- BluePages
- MoodGYM
- MHFA eLearning
- Beyond Silence
Online vs offline: similarly effective for reducing public stigma SLR, healthcare setting (Pospos,et al. Acad Psychiatry 2018;42:109–120) - Breath2Relax
- Headspace
- Meditation Audios
- MoodGYM
- Stress Gym
- Virtual Hope Box
- Stay Alive
Identified tools provide a starting point to mitigate burnout, depression, and suicidality SLR, 13 interventions for stigma (Johnson, et al. Indian J Psychol Med 2021;44:332–340) - Web-based, psychoeducation interventions
- Online games
- Mobile app
Most interventions increased help-seeking SLR + meta-analysis, 9 RCTs, n=1832 (Rodriguez-Rivas, et al. JMIR Serious Games. 2022; 10:e35099) - Video games
- Virtual reality
- Videoconferencing and online chat
Interventions had a consistent effect on reducing public stigma ConclusionsPublished data suggest that e-mental health is promising to reduce stigma and discrimination, with the potential to foster help-seeking and treatment engagement. Adoption requires attention to derailers and must foster inclusivity. There is an imperative to adopt e-mental health, especially evidence-based solutions.
Disclosure of InterestK. Subramaniam Employee of: Employee of Viatris, A. Greenshaw: None Declared, A. Thapliyal: None Declared
Psychosomatic relationships between the state of mental health and the level of vital threat of dermatological disease
- M. Markova, T. Abdriakhimova, H. Skrebtsova, M. Chemerys
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S370-S371
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
According to the literature, 25-60% of dermatological patients have mental disorders. In the case of oncodermatological disease, the patient is under the influence of two stressogenic factors – existential experiences and social discomfort from the manifestations of the disease, which imprints on the patient’s mental health and promotes the development of mental maladaptation (MM).
ObjectivesTo study the features of mental state in patients with dermatological diseases with different levels of vital threat.
MethodsThe examination included the use of clinical-psychological, psychodiagnostic and psychometric research methods.
Results120 dermatological patients were examined: 60 patients with non-vital dermatological diseases (L82, A63.0, D18.0, L80), and 60 patients with dermatological diseases posing a vital threat (C43, C44, D04).
The identification of clinical signs of MM proved their presence in 70 (58.4%) people in the total sample. Among patients with non-vital diseases, the signs of MM were established in 33 (55.0%), among the patients with vital diseases – in 37 (61.7%). So, among patients with dermatological diseases, there are both psychologically adapted and maladapted individuals, regardless of the vitality/non-vitality of the pathological process.
In dermatological patients with signs of MM, the clinical picture is dominated by anxious (mainly in patients with non-vital diseases) and depressive (mainly in patients with vital diseases) radicals. Auxiliary psychopathological constructs are represented by manifestations of somatization, obsessive-compulsive symptoms, interpersonal sensitivity, and phobic anxiety. Affective symptoms are most pronounced in patients with MM and vital diseases, it is less pronounced in patients with non-vital pathology.
The presence and intensity of maladaptive pathopsychological-affective reactions in patients with dermatological pathology are not clearly associated with the vitality of the dermatological process, but are based on mechanisms of the mutual influence of biological predisposition and psychological and psychosocial factors, the mosaic combination of which determines the individual’s resource capabilities for constructive acceptance the fact of the presence of a dermatological disease and the development of an adequate strategy for its mastery, regardless of the severity of the disease.
ConclusionsThese patterns should be considered when developing treatment measures and rehabilitation for patients with dermatological pathology.
Disclosure of InterestNone Declared
Cognitive complaints in schizophrenia:relationship with clinical symptoms, stigma and insight
- S. Ajmi, M. Bouhamed, R. Ouali, S. Hentati, I. Feki, R. Sallemi, J. Masmoudi
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S757
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In addition to the classic clinical symptoms, patients with schizophrenia suffer from cognitive difficulties, self-stigma and poor insight.
ObjectivesThis study aims to evaluate the impact of stigma, symptom severity, and insight on subjective cognitive complaints in patients with schizophrenia.
MethodsThis is a cross-sectional, descriptive and analytical study carried out on 72 stabilized patients followed at the post-cure psychiatry consultation ‘A’ at the CHU Hédi Chaker in Sfax diagnosed with schizophrenia according to the DSM 5 criteria.
We used the schedule for the Assessment of Insight–Expanded Version(SAI-E) to assess clinical insight, The Internalized Stigma of Mental Illness (ISMI) scale for the assessment of internalized stigma, the Subjective Scale to Investigate Cognition in Schizophrenia (SSTICS) scale to determine subjective cognitive complaints and the Positive and Negtive Syndroms Scale (PANSS) to assess positive and negatives symptoms.
ResultsThe average age of the patients was 46.83 ± 11.6 years, with a sex ratio (M/F) of 2. In our study, 48.5% of the patients were single, 52.8years,% were smokers and 23 6% consumed alcohol. The level of education did not exceed the primary level for 44.4% of the patients. The average age of disease onset was 24.56 ± 5, 82. Our participants had an average score of 25 on the SSTICS total score and 20.1 on the SAI-E. The median ISMI total score and PANSS total score were 2.45 and 46respectively
The predominant negative symptoms(p=0.003), stigma(p=0.009), and insight (p<10-3)were significant factors associated with increased cognitive complaints.
ConclusionsIn schizophrenia, the combination of cognitive difficulties, self-stigma with a low insight makes the management of these patients more difficult.
Disclosure of InterestNone Declared
Evaluation of adherence to treatment in patients with anxious-depressive syndrome.
- T. Jiménez Aparicio, M. Fernández Lozano, M. Merizalde Torres, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S674-S675
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Treatment-resistant depression can pose a major challenge to mental health professionals, both in identifying cases and in devising consequent therapeutic strategies (1). However, it is not uncommon that the lack of response to antidepressant treatment is actually due to non-adherence to it in many cases (2).
ObjectivesIn this context, it would be interesting to know the rate of abandonment of antidepressant treatment in patients with anxious-depressive symptomatology, since the patient’s evolution may depend entirely on this.
MethodsTo this end, the psychiatry service of the Hospital Clínico Universitario de Valladolid has collected data on adult patients who come for a first consultation in the mental health team, referred for presenting symptoms of anxiety and depression.
These data have been recorded over the last 2 years, including different socio-demographic and clinical variables. Subsequently, a descriptive analysis was carried out, the preliminary results of which are presented below.
ResultsWe started from a sample of 222 patients at the present time: 69 men and 153 women, which is in accordance with previous data on the prevalence of anxiety disorders and depression by gender (3).
Antidepressant treatment was prescribed (from psychiatry or primary care) in 80% of them. A review 6 months later showed that up to 1/3 of these patients (34%) had abandoned treatment on their own before completing this period, as can be seen in the first graph (image 1), which is contemplated in several guidelines and recommendations in the scientific literature (4). No major differences were observed between genders for treatment indication or treatment abandonment.
On the other hand, 61% of the patients in the sample had been treated with benzodiazepines. Among them, up to 74% were still taking these drugs 6 months later (image 2). This result is striking, since in reality, the duration of treatment with benzodiazepines should be much shorter, according to the latest reviews (5).
Finally, cross-checking these data, it was observed that for 116 patients (52% of the total) the initial treatment included antidepressants and benzodiazepines. At 6 months, 18 of these patients (16%) had voluntarily discontinued the antidepressant, but continued with benzodiazepines.
Image:
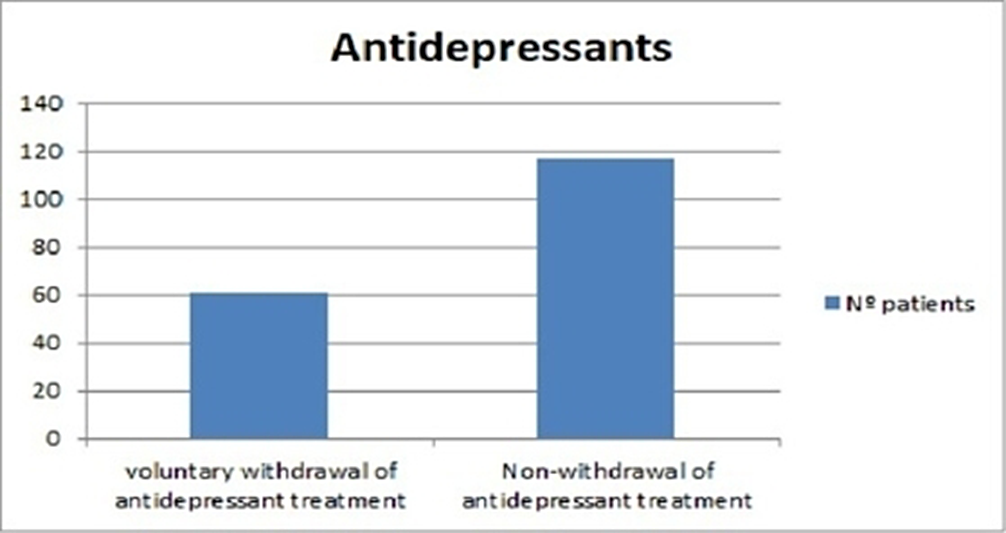
Image 2:
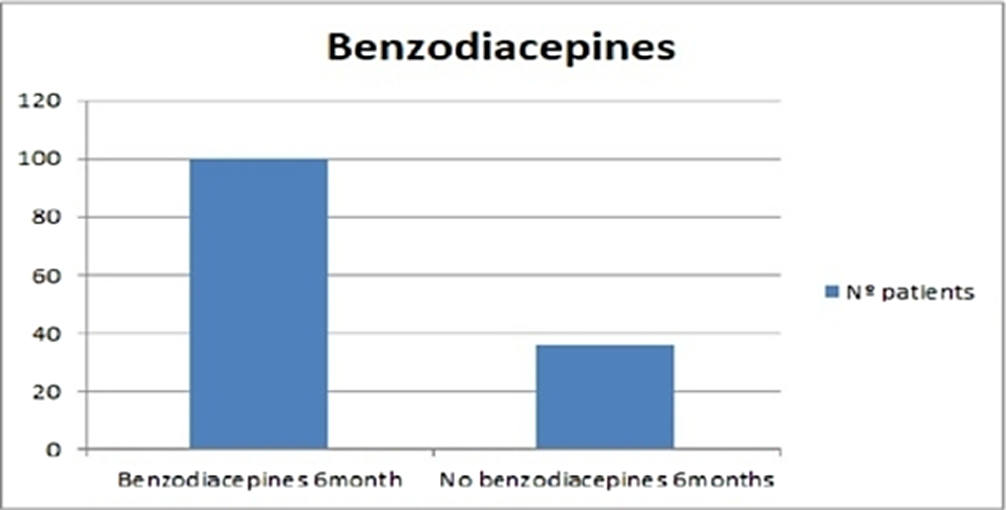 Conclusions
ConclusionsIt is very important to review adherence to treatment in all patients, especially in those cases in which the persistence of symptoms makes us think of a possible resistant depression. For this reason, it would be advisable to try to establish an adequate doctor-patient relationship that allows trust in the therapist and communication between both and leads to a favorable evolution.
Disclosure of InterestNone Declared
Marion Turner. The Wife of Bath: A Biography Princeton: Princeton University Press, 2023. Pp. 336. $29.95 (cloth).
- Karla Taylor
-
- Journal:
- Journal of British Studies , First View
- Published online by Cambridge University Press:
- 27 August 2024, pp. 1-2
-
- Article
- Export citation
Experience in the Psychotherapeutic Treatment of Eating Disorders in Children and Adolescents: A Brief Approach and EMDR Outcomes
- L. López Gómez-Miguel, L. Herranz Núñez, L. Santolaya López, F. Benavides Rivero, A. Privado Aranda, M. González San José
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S460
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
This study is based on our experience at public hospitals and private clinics of Toledo and Madrid, where we have addressed the treatment of children and adolescents presenting with Eating Disorders (EDs). Our intervention focuses on the application of brief psychotherapy, with particular emphasis on the effectiveness of Eye Movement Desesitization and Reprocessing (EMDR) in these cases.
ObjectivesThe primary objective of this study is to determine the benefits of applying EMDR in cases of pediatric and adolescent EDs in comparison to other psychotherapeutic techniques.
MethodsOver a period of one year, brief psychotherapy sessions were conducted with children and adolescents diagnosed with EDs. An integrative approach was used, combining family sistemic therapy, cognitive-behavioural therapy techniques, and brief psychodynamic approaches, along with EMDR sessions. Pre and post treatment assessments were conducted to measure changes in symptoms and patients’ quality life.
ResultsThe results obtained reveal significant improvements in patient symptomatology, including a notable reduction in food-anxiety, dietary restriction and compensatory behaviours. Furthermore, improvements were observed in body image perception and patiends’ overall quality of life. Incidence of relapse cases was minimal.
ConclusionsOur experience suggests that the application of a brief psychotherapy approach, combined with EMDR sessions, can be highly effective in treating children and adolescents with EDs. Early intervention and individualized adaptation of therapies are essential for achieving positive and lasting outcomes in this patient group. These findings underscore the importance of considering integrative approaches in the care of EDs in young population.
Disclosure of InterestNone Declared
Do antidepressants lead to weight-increase? Antidepressant therapy and long-term changes in body mass index, waist circumference and fat mass - A prospective, population-based study
- M.-P. Strippoli, M. Preisig
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S24-S25
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Abstract
The presentation will focus on long-term weight changes in patients with major depressive disorder who use antidepressants. Research studying weight change over periods of more than 12 months is scarce and the effects of depressive episodes and antidepressants on weight changes have rarely been assessed simultaneously. Using data of a prospective population-based CoLaus|PsyCoLaus study, data on the associations of antidepressant use prior to baseline and during a 5.5-year follow-up with changes in adiposity markers and multiple adjustments including for the effects of depressive episodes will be presented. The cohort included 2479 randomly selected 35 to 66 year-old white residents (mean age 49.9 years, 53.3% women) of an urban area who accepted the physical and psychiatric evaluations at baseline and follow-up (76.8% participation at the follow-up). Diagnostic information on mental disorders, treatment use including psychotropic drugs was elicited using a semi-structured interview. Independently of the effect of antidepressants used during the follow-up and the effects of depressive episodes, the number of any antidepressant compounds used prior to baseline was associated with lower increase of body mass index (BMI), whereas the use of antidepressants during the follow-up was associated with steeper increase in BMI and waist circumference. Within AD classes, the use of tricyclic AD (TCA) and selective serotonin reuptake inhibitor (SSRI) prior to baseline was associated with lower increase, the use of SSRI during follow-up was associated with steeper increases in BMI. Similarly, the use of SSRI prior to baseline was associated with lower increase, the use of TCA and SSRI during the follow-up was associated with steeper increase in waist circumference. Finally, the use of SSRI during follow-up was also associated with steeper increase in fat mass. The findings support unfavorable obesogenic effects of sustained treatment not only with TCAs but also with SSRIs, suggesting that the benefit of long-term administration of these AD classes should be carefully weighed against the potential risk of weight gain.
Disclosure of InterestNone Declared
War and Migration – when Mental Health is left behind
- A. L. Ramos, H. Salgado
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S614
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Wars and armed conflicts are known to have devastating consequences for both physical and mental health of all the people involved. Studies have shown that conflict situations cause more mortality and disability than any major disease and, among the consequences of war, the impact on mental health of the civilian population is one of the most significant.
Forced migration, compelling people to become internally displaced or refugees who have fled to other countries, is responsible for additional physical and mental health problems. Regardless of the reasons for migration, the process itself can be a highly stressful life event, leading to a higher risk of psychiatric disorders. Refugees are particularly susceptible to mood and anxiety disorders, whose prevalence rates is almost twice as high as those found among non-refugee migrants.
ObjectivesSince 2022, with the progression of the conflict between Russia and Ukraine, and the establishment of a real war scenario, many Ukrainians were forced to leave their homeland, to ensure their survival and security. In Europe, many countries took in Ukrainian refugees and Portugal was no exception.
In the Psychiatry Inpatient Service of University Hospital Center of São João, there were admissions of Ukrainian refugees who already had a known mental disease - at that time decompensated - and also new cases, to date without follow-up by the specialty.
MethodsIn this work, we will carry out a bibliographical review on the impact of war and migration on mental health and the potential of proper medical approach, based on articles indexed in Pubmed, in the last 10 years.
Furthermore, we will present the cases of war refugees interned in our service between January 2022 and December 2023.
ResultsWe will describe the psychopathological features and also the sociofamilial circumstances of these patients, as well as explain the intervention and longitudinal support developed in these cases.
ConclusionsAs a conclusion, we point out the importance of approaching mental illness in light of the individual’s context, knowing that this context may contain the problem and also the solution. War and forced migration bring increased challenges to psychiatry and, in an increasingly globalized society, geographical, linguistic or cultural barriers cannot impose limits on our best and most appropriate medical treatment.
Disclosure of InterestNone Declared
Case Report and Literature review. Neuropsychiatry Manifestation of Frontal Lobe Neoplasm- Meningioma. Prevalence, Presentation and Pathogenesis
- U. Anyeji, O. Alli-Balogun
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S646
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Meningiomas are the most frequent primary brain tumor. Although most Meningiomas are benign, their location in the central nervous system can predict symptomatology which could result in significant morbidity and mortality. However, due to the slow-growing nature, meningiomas are usually asymptomatic, and diagnosis is often made incidentally on neuroimaging or at an autopsy. The incidence rate is 1.2-fold higher in Black Americans than White Americans. Neuropsychiatry manifestation might be only initial presentation; thus, psychiatrists are often the first to see these patients, and the correct diagnosis may be made only when the tumor has grown to a considerable size and begun to displace the brain.
ObjectivesThe aim of this study is to understand the biological basis of psychiatry symptoms in patients with Frontal Lobe meningiomas.
MethodsA review of literature and individual patient data analysis was conducted. The literature review was conducted on PubMed, Medline, MeSH, Google Scholar, and mount Sinai’s levy Library using the key words; meningioma, meningioma with psychiatric symptoms, psychosis, depression, neuropsychiatry manifestation of meningiomas.
ResultsThe review revealed that 88% of brain tumors and psychiatric symptoms are located in the frontal region. Meningiomas accounts for 13%-26% of intracranial tumors. There is a reported low incidence due to its slow growing nature and are usually asymptomatic. Incidence of meningiomas is predominant in females, and is attributed to hormonal factors, this is associated with estrogen and progestogen cycles. Reports shows that smoking has been linked to increase risk of meningiomas in men. Frontal lobe meningiomas may present with only psychological symptoms that resemble depression, anxiety states, hypomania and schizophrenia. Personality and mental status changes are also noted in Frontal lobe tumors. Left sided lesions are associated with inhibition of motor activity, impairment in motor and initiative aspect of speech, diminished generalization ability and general inertia of mental process.
ConclusionsGiven the absence of frank neurological symptoms, to help localize the lesion, most meningiomas are missed due to diagnostic overshadowing of the primary psychiatric illness. Peritumoral edema indicates the underlying mechanism and location of the lesion predicts symptomatology. Like our patient who is an 81-year-old male with no past psychiatry history, presenting to our comprehensive psychiatry emergency program with psychiatric manifestation as the initial presentation and subsequently with MRI suggestive of Right Frontal extra-axial meningioma. This study shows that primitive frontal lobe tumors are likely to be misdiagnosed as patients with such tumors are often referred first to psychiatrist. High index of suspicious is needed.
Disclosure of InterestNone Declared
Effects of light therapy in the anxious-depressive clinic
- M. T. Gonzalez Salvador, R. Gutierrez-Labrador, M. I. C. Gómez-Ulla, A. I. de la Puente
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S533
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major depressive disorder (MDD) is defined as a mental disorder of multifactorial etiology, which presents with mood disturbance, mainly sadness associated with loss of interest or pleasure. Light therapy (LT) is a therapeutic intervention consisting of daily exposure to a light source. This study aims to evaluate the effects of LT on anxious-depressive symptomatology and sleep in a sample of patients diagnosed with depression.
ObjectivesThis study aims to evaluate the effects of LT on anxious-depressive symptomatology and sleep in a sample of patients diagnosed with depression.
MethodsProspective case-control study, in which the cases are outpatients diagnosed with MDD and the controls are healthy individuals. Both groups underwent LT sessions and were assessed by means of validated scales, anxiety and depression symptoms before and after LT sessions, as well as changes in sleep patterns through a sleep measuring device.
Results11 cases and 18 controls were included in the study. Of the participants, 62.1% were female and 37.9% were male. The mean age of the sample was 54.03 □ 11.55 years. There were significant case differences in the pre and post LT scores of the depression scale. There were no significant differences in the changes in superficial, deep and total sleep and in the anxiety scale scores.
ConclusionsIn the sample analysed, LT has significant effects on the cases at the level of the depression scale.
Disclosure of InterestNone Declared
Typology of hyperthymic personalities with affective phases
- A. Barkhatova, A. Churkina, S. Sorokin
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S656-S657
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Modern authors characterize hyperthymic individuals as eloquent, humorous, self-confident, optimistic, energetic, liberated, sexually active, constantly planning and implementing their plans. Four or more of the listed characteristics indicate the individual’s involvement in the circle of hyperthymic people. Statistical data on the prevalence of hyperthymic is scarce, which is due to rare requests for help and the diagnosis of this condition not as a disease, but within the framework of characterological traits. Attempts to classify hyperthymics have been made more than once, but previously none of the authors divided them according to the presence of side character traits in the personality structure.
ObjectivesTo establish psychopathological types of hyperthymic individuals in whom affective states were formed.
MethodsThe sample consisted of 50 patients (42 women, 8 men) who were on inpatient or outpatient treatment at the clinic since 2019 to 2022. Patients were examined by clinical-psychopathological, clinical-anamnestic methods due to the presence of a phase affective state.
ResultsFour types of hyperthymic personalities have been identified: anxious-hyperthymic, hysterical-hyperthymic, schizoid-hyperthymic and standard hyperthymic. Anxious-hyperthymic type, 20% (n=10) characterized by a combination of increased activity, sociability with such traits as suspiciousness, perfectionism, meticulousness, exactingness, concern for one’s health and the desire to maintain a healthy lifestyle. Hysterical-hyperthymic type, 46% (n=23) includes both hyperthymic and hysterical traits in the form of increased emotionality, egocentrism, drama, and desire for recognition from others. In addition, patients in this group are characterized by increased concern about their appearance (bright clothes, makeup, tattoos). Schizoid-hyperthymic type, 10% (n=5). In addition to increased activity and emancipation, patients in this group are prone to fantasizing, overvalued hobbies, sthenicity, emotional poverty and rationalism. Standard type, 24% (n=12) are characterized by the presence of typical hyperthymic traits - optimism, energy, constant desire for productive activity, success in the chosen profession, rapid career growth, sociability, openness.
ConclusionsHyperthymic individuals with the development of affective phases are heterogeneous in their psychopathological structure and have features of the pathocharacterological structure that make it possible to distinguish anxious-hyperthymic, hysterical-hyperthymic, schizoid-hyperthymic and standard types. The developed classification of hyperthymia reveals the predominance of the hysterical-hyperthymic type (46%).
Disclosure of InterestNone Declared
The future of psychiatry and psychotherapy - An Early Career psychiatrist’s view
- F. H. Kraxner
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S819
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychiatry is one of the most fast developing and agile discipline within human medicine. But more work is necessary to complete these advances.
ObjectivesI address the following questions:
How does the future of psychiatry look in the eyes of early career psychiatrists?
What strengths, weaknesses opportunities and threats will come?
And what can we learn from different mental health systems and reagions?
MethodsOral or written statements to the raised questions followed optimally by a discussion
ResultsIn low- and middle-income countries, a vast majority of people with mental disorders do not receive adequate treatment. Even in high income countries, roughly a third of people with severe forms of mental illness are not receiving the appropriate therapy. Laws concerning mental health are outdated in different countries. The protection of the human rights of the mentally ill is still incomplete and imperfect. The emphasis on economic gain and the digitalization of medicine in recent years has not helped. And new technical advancements such as artifical intelligence are becoming more important.
ConclusionsMore discussion needs to be done on the identity and understanding of the psychiatric profession.
Disclosure of InterestNone Declared
Co-design of a digital violence prevention and management tool for psychiatric inpatient care: focus on supporting integration into electronic health record system
- T. Lantta, T. Rautiainen, M. Anttila, J. Anttila, M. Ameel
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S59
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Violence in psychiatric inpatient settings is a global challenge. Several methods have been developed and tested to help staff prevent the occurrence of violence on the wards. One novel and effective method is eDASA+APP, originating from Australian forensic psychiatric settings (Maguire et al. Int J Ment Health Nurs 2019; 281186-1197, Griffith et al. Psychiatr Serv 2021; 72 885-890). This electronic method contains an instrument (DASA) to assess the risk for imminent violence and includes evidence-based violence risk management methods for risk levels. It is important to ensure that this electronic intervention is integrated into daily clinical practice. This can be done in co-design between all that are involved e.g., staff and experts by experience, and by encouraging them to achieve a common goal and gain benefits by working together.
ObjectivesThis prevention gives an overview of how the Finnish version of eDASA+APP was co-designed with healthcare staff and experts by experience, focusing on integration into the electronic patient health record system. The presentation is part of a larger research project testing eDASA+APP in Finnish psychiatric inpatient care.
MethodsCo-design workshops focusing on three major themes: 1) identifying current practices and how eDASA+APP would fit in those, 2) producing a linguistically and culturally appropriate version of eDASA+APP, and 3) preferred use of eDASA+APP in an electronic patient health record system. Notes were kept during the workshops by researchers. Qualitative material were analysed with deductive content analysis. Results from the third theme are shared in this presentation.
ResultsStaff and experts by experience described that integration of eDASA+APP in electronic patient health record system is supported if it 1) brings clear and fast information to the staff about the violence risk of a patient, 2) is a visible measure that is concretely in sight in electronic patient health record system, 3) provides information about which violence prevention and management interventions have worked with a patient, 4) involves patient preferences, and 5) consist of joint decisions that have been agreed multi-professionally.
ConclusionsIntegration of eDASA+APP in the electronic patient health record system has the potential to succeed if it is realized in cooperation with staff and experts by experience, is technically easy to use, and the users have an understanding of its benefits to everyone involved.
Disclosure of InterestNone Declared





