221 results
The association of adverse childhood experiences with long-term outcomes of psychosis: a 21-year prospective cohort study after a first episode of psychosis
- Victor Peralta, Elena García de Jalón, Lucía Moreno-Izco, David Peralta, Lucía Janda, Ana M. Sánchez-Torres, Manuel J. Cuesta, SEGPEPs group
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 30 May 2024, pp. 1-10
-
- Article
- Export citation
-
Background
Evidence suggests a possible relationship between exposure to childhood adversity (CA) and functional impairment in psychosis. However, the impact of CA on long-term outcomes of psychotic disorders remains poorly understood.
MethodsTwo hundred and forty-three patients were assessed at their first episode of psychosis for CA and re-assessed after a mean of 21 years of follow-up for several outcome domains, including symptoms, functioning, quality of life, cognitive performance, neurological dysfunction, and comorbidity. The unique predictive ability of CA exposure for outcomes was examined using linear regression analysis controlling for relevant confounders, including socioeconomic status, family risk of schizophrenia, and obstetric complications.
ResultsThere were 54% of the patients with a documented history of CA at mild or higher levels. CA experiences were more prevalent and severe in schizophrenia than in other psychotic disorders (p < 0.001). Large to very large effect sizes were observed for CA predicting most role functioning variables and negative symptoms (ΔR2 between 0.105 and 0.181). Moderate effect sizes were observed for positive symptoms, personal functioning, impaired social cognition, impaired immediate verbal learning, poor global cognition, internalized stigma, poor personal recovery, and drug abuse severity (ΔR2 between 0.040 and 0.066). A dose–response relationship was observed between levels of CA and severity of outcome domains.
ConclusionOur results suggest a strong and widespread link between early adversity exposure and outcomes of psychotic disorders. Awareness of the serious long-term consequences of CA should encourage better identification of those at risk and the development of effective interventions.
TwinsMX: Exploring the Genetic and Environmental Influences on Health Traits in the Mexican Population
- Brisa García-Vilchis, Talia V. Román-López, Diego Ramírez-González, Xanat J. López-Camaño, Vanessa Murillo-Lechuga, Xóchitl Díaz-Téllez, C. Itzamná Sánchez-Moncada, Ian M. Espinosa-Méndez, Diego Zenteno-Morales, Zaida X. Espinosa-Valdes, Sofia Pradel-Jiménez, Andrea Tapia-Atilano, Ana V. Zanabria-Pérez, Federica Livas-Gangas, Oscar Aldana-Assad, Ulises Caballero-Sánchez, César A. Dominguez-Frausto, Miguel E. Rentería, Alejandra Medina-Rivera, Sarael Alcauter, Alejandra E. Ruiz-Contreras
-
- Journal:
- Twin Research and Human Genetics / Volume 27 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 03 May 2024, pp. 85-96
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
TwinsMX registry is a national research initiative in Mexico that aims to understand the complex interplay between genetics and environment in shaping physical and mental health traits among the country’s population. With a multidisciplinary approach, TwinsMX aims to advance our knowledge of the genetic and environmental mechanisms underlying ethnic variations in complex traits and diseases, including behavioral, psychometric, anthropometric, metabolic, cardiovascular and mental disorders. With information gathered from over 2800 twins, this article updates the prevalence of several complex traits; and describes the advances and novel ideas we have implemented such as magnetic resonance imaging. The future expansion of the TwinsMX registry will enhance our comprehension of the intricate interplay between genetics and environment in shaping health and disease in the Mexican population. Overall, this report describes the progress in the building of a solid database that will allow the study of complex traits in the Mexican population, valuable not only for our consortium, but also for the worldwide scientific community, by providing new insights of understudied genetically admixed populations.
Additive effects of a family history of schizophrenia spectrum disorders and an environmental risk score for the outcome of patients with non-affective first-episode psychosis
- Manuel J. Cuesta, Elena García de Jalón, Ana M. Sánchez-Torres, Gustavo J. Gil-Berrozpe, Lidia Aranguren, Gerardo Gutierrez, Asier Corrales, Amalia Zarzuela, Berta Ibañez, Víctor Peralta, PEPsNa Group
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 20 March 2024, pp. 1-9
-
- Article
- Export citation
-
Background:
First-episode psychotic disorders comprise a heterogeneous phenotype with a complex etiology involving numerous common small-effect genetic variations and a wide range of environmental exposures. We examined whether a family of schizophrenia spectrum disorder (FH-Sz) interacts with an environmental risk score (ERS-Sz) regarding the outcome of patients with non-affective first episode psychosis (NAFEP).
Methods:We included 288 patients with NAFEP who were evaluated after discharge from an intensive 2-year program. We evaluated three outcome measures: symptomatic remission, psychosocial functioning, and personal recovery. We analyzed the main and joint associations of a FH-Sz and the ERS-Sz on the outcomes by using the relative excess risk due to interaction (RERI) approach.
Results:A FH-Sz showed a significant association with poor symptomatic remission and psychosocial functioning outcomes, although there was no significant interaction between a FH-Sz and the ERS-Sz on these outcomes. The ERS-Sz did not show a significant association with poor symptomatic remission and psychosocial functioning outcomes, even though the magnitude of the interaction between ERS-Sz and FH-Sz with the later outcome was moderate (RERI = 6.89, 95% confidence interval −16.03 to 29.81). There was no association between a FH-Sz and the ERS-Sz and personal recovery.
Conclusions:Our results provide further empirical support regarding the contribution of FH-Sz to poor symptomatic remission and poor psychosocial functioning outcomes in patients with NAFEP.
Unlocking archaeological data online via the PEPAdb (Prehistoric Europe's Personal Adornment Database) initiative for Open Science
- Galo Romero-García, Daniel Sánchez-Gómez, José Á. Garrido-Cordero, José M. Martínez-Blanes, Ana C. Sousa, Carlos P. Odriozola
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
PEPAdb (Prehistoric Europe's Personal Adornment Database) is a long-term, open-ended project that aims to improve access to archaeological data online. Its website (https://pepadb.us.es) publishes and analyses datasets about prehistoric personal adornment, drawing on the results of various research projects and bibliographic references.
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
41 Concussion History, Physical Activity, and Athletic Status Predict Subjective but not Objective Executive Functioning
- Madeline M. Doucette, Juan P. Sanchez, Ryan E. Rhodes, Mauricio A. Garcia-Barrera
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 914-915
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Factors such as physical activity and sports participation may have a positive effect on executive functioning. However, people involved in sports are at a higher risk of experiencing a concussion, which may have a detrimental effect. Previous research has yet to investigate those combined negative and positive effects while also utilizing a comprehensive assessment of executive function. This study aims precisely to examine the effects of physical activity, athletic status and concussion history on subjective (e.g., questionnaire) and objective measures (e.g., latent variables) of three well-established components of executive function (i.e., inhibiting, shifting, and updating) in young adults.
Participants and Methods:247 Canadian university students (ages 18 - 25; 83% female) completed a remote assessment of executive function involving nine computerized tasks and a behavioural self-report, in addition to demographic questionnaires and items assessing weekly physical activity, athletic status, and concussion history. A linear regression analysis was used to assess the effects of the predictor variables (age, sex, concussion history, physical activity and athletic status) on subjective reporting of executive functioning using the Executive Function Index. Furthermore, structural equation modelling (SEM) was used to predict objective executive function using a three-factor model (shifting, updating, inhibition).
Results:The three-factor measurement model of executive function fit the data adequately: x2 = 26.10, df = 17, p = 0.07, CFI = 0.97, TLI = 0.95, RMSEA = 0.05 [90% CI: 0.00-0.09], SRMR = 0.04. Then, the three-factor SEM of executive function also fit the data adequately: X2 = 66.38, df = 51, p = 0.07, CFI = 0.95, TLI = 0.93, RMSEA = 0.04 [90% CI: 0.00-0.06], SRMR = 0.05. Using SEM, no direct relationship was found between the factors of executive function and the predictor variables (i.e., age, physical activity, concussion history, and athletic status). Sex was significantly related to inhibition (b = 0.52, p = 0.02), such that males had greater inhibition. For the regression, physical activity (b = 0.09, p < .01), concussion history (b = 3.29, p < .05) and athletic status (b = -4.01, p < .05) were found to be significant predictors for the Executive Function Index.
Conclusions:Concussion history, physical activity, and athletic status were all predictive of subjective but not objective measures of executive function. Interestingly, these findings align with previous research that demonstrated performance-based executive function measures often do not align with self-report measures, which may suggest they are complementary but measure slightly different aspects of the underlying executive function construct. Mixed findings in the extant literature regarding sex differences and executive function require continued research to understand better the relationship and mechanisms behind the sex differences in inhibition. In summary, these findings offer support for the differentiation between subjective and objective measures of executive function when investigating their relationship with physical activity, sport participation, concussion history, age and sex.
Difficulties during delivery, brain ventricle enlargement and cognitive impairment in first episode psychosis
- Ana Costas-Carrera, Norma Verdolini, Clemente Garcia-Rizo, Gisela Mezquida, Joost Janssen, Isabel Valli, Iluminada Corripio, Ana M. Sanchez-Torres, Miquel Bioque, Antonio Lobo, Ana Gonzalez-Pinto, Marta Rapado-Castro, Eduard Vieta, Helena De la Serna, Anna Mane, Alexandra Roldan, Nicolas Crossley, Rafael Penades, Manuel J. Cuesta, Mara Parellada, Miquel Bernardo, PEPs group
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 7 / May 2024
- Published online by Cambridge University Press:
- 28 November 2023, pp. 1339-1349
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Patients with a first episode of psychosis (FEP) display clinical, cognitive, and structural brain abnormalities at illness onset. Ventricular enlargement has been identified in schizophrenia since the initial development of neuroimaging techniques. Obstetric abnormalities have been associated with an increased risk of developing psychosis but also with cognitive impairment and brain structure abnormalities. Difficulties during delivery are associated with a higher risk of birth asphyxia leading to brain structural abnormalities, such as ventriculomegaly, which has been related to cognitive disturbances.
MethodsWe examined differences in ventricular size between 142 FEP patients and 123 healthy control participants using magnetic resonance imaging. Obstetric complications were evaluated using the Lewis–Murray scale. We examined the impact of obstetric difficulties during delivery on ventricle size as well as the possible relationship between ventricle size and cognitive impairment in both groups.
ResultsFEP patients displayed significantly larger third ventricle size compared with healthy controls. Third ventricle enlargement was associated with diagnosis (higher volume in patients), with difficulties during delivery (higher volume in subjects with difficulties), and was highest in patients with difficulties during delivery. Verbal memory was significantly associated with third ventricle to brain ratio.
ConclusionsOur results suggest that difficulties during delivery might be significant contributors to the ventricular enlargement historically described in schizophrenia. Thus, obstetric complications may contribute to the development of psychosis through changes in brain architecture.
Long-term diagnostic stability, predictors of diagnostic change, and time until diagnostic change of first-episode psychosis: a 21-year follow-up study
- David Peralta, Lucía Janda, Elena García de Jalón, Lucía Moreno-Izco, Ana M. Sánchez-Torres, Manuel J. Cuesta, Victor Peralta, SEGPEPs Group
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 7 / May 2024
- Published online by Cambridge University Press:
- 21 November 2023, pp. 1329-1338
-
- Article
- Export citation
-
Background
Although diagnostic instability in first-episode psychosis (FEP) is of major concern, little is known about its determinants. This very long-term follow-up study aimed to examine the diagnostic stability of FEP diagnoses, the baseline predictors of diagnostic change and the timing of diagnostic change.
MethodsThis was a longitudinal and naturalistic study of 243 subjects with FEP who were assessed at baseline and reassessed after a mean follow-up of 21 years. The diagnostic stability of DSM-5 psychotic disorders was examined using prospective and retrospective consistencies, logistic regression was used to establish the predictors of diagnostic change, and survival analysis was used to compare time to diagnostic change across diagnostic categories.
ResultsThe overall diagnostic stability was 47.7%. Schizophrenia and bipolar disorder were the most stable diagnoses, with other categories having low stability. Predictors of diagnostic change to schizophrenia included a family history of schizophrenia, obstetric complications, developmental delay, poor premorbid functioning in several domains, long duration of untreated continuous psychosis, spontaneous dyskinesia, lack of psychosocial stressors, longer duration of index admission, and poor early treatment response. Most of these variables also predicted diagnostic change to bipolar disorder but in the opposite direction and with lesser effect sizes. There were no significant differences between specific diagnoses regarding time to diagnostic change. At 10-year follow-up, around 80% of the diagnoses had changed.
ConclusionsFEP diagnoses other than schizophrenia or bipolar disorder should be considered as provisional. Considering baseline predictors of diagnostic change may help to enhance diagnostic accuracy and guide therapeutic interventions.
Coronavirus disease 2019 is associated with long-term depressive symptoms in Spanish older adults with overweight/obesity and metabolic syndrome
- Sangeetha Shyam, Carlos Gómez-Martínez, Indira Paz-Graniel, José J. Gaforio, Miguel Ángel Martínez-González, Dolores Corella, Montserrat Fitó, J. Alfredo Martínez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque, Dora Romaguera, José López-Miranda, Ramon Estruch, Francisco J. Tinahones, José Manuel Santos-Lozano, J. Luís Serra-Majem, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín Sánchez, Xavier Pintó, María Ortiz Ramos, Josep Vidal, Maria Mar Alcarria, Lidia Daimiel, Emilio Ros, Fernando Fernandez-Aranda, Stephanie K. Nishi, Oscar García Regata, Estefania Toledo, Jose V. Sorli, Olga Castañer, Antonio Garcia-Rios, Rafael Valls-Enguix, Napoleon Perez-Farinos, M. Angeles Zulet, Elena Rayó-Gago, Rosa Casas, Mario Rivera-Izquierdo, Lucas Tojal-Sierra, Miguel Damas-Fuentes, Pilar Buil-Cosiales, Rebeca Fernández-Carrion, Albert Goday, Patricia J. Peña-Orihuela, Laura Compañ-Gabucio, Javier Diez-Espino, Susanna Tello, Ana González-Pinto, Víctor de la O, Miguel Delgado-Rodríguez, Nancy Babio, Jordi Salas-Salvadó
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 3 / February 2024
- Published online by Cambridge University Press:
- 05 September 2023, pp. 620-630
-
- Article
- Export citation
-
Background
The coronavirus disease 2019 (COVID-19) has serious physiological and psychological consequences. The long-term (>12 weeks post-infection) impact of COVID-19 on mental health, specifically in older adults, is unclear. We longitudinally assessed the association of COVID-19 with depression symptomatology in community-dwelling older adults with metabolic syndrome within the framework of the PREDIMED-Plus cohort.
MethodsParticipants (n = 5486) aged 55–75 years were included in this longitudinal cohort. COVID-19 status (positive/negative) determined by tests (e.g. polymerase chain reaction severe acute respiratory syndrome coronavirus 2, IgG) was confirmed via event adjudication (410 cases). Pre- and post-COVID-19 depressive symptomatology was ascertained from annual assessments conducted using a validated 21-item Spanish Beck Depression Inventory-II (BDI-II). Multivariable linear and logistic regression models assessed the association between COVID-19 and depression symptomatology.
ResultsCOVID-19 in older adults was associated with higher post-COVID-19 BDI-II scores measured at a median (interquartile range) of 29 (15–40) weeks post-infection [fully adjusted β = 0.65 points, 95% confidence interval (CI) 0.15–1.15; p = 0.011]. This association was particularly prominent in women (β = 1.38 points, 95% CI 0.44–2.33, p = 0.004). COVID-19 was associated with 62% increased odds of elevated depression risk (BDI-II ≥ 14) post-COVID-19 when adjusted for confounders (odds ratio; 95% CI 1.13–2.30, p = 0.008).
ConclusionsCOVID-19 was associated with long-term depression risk in older adults with overweight/obesity and metabolic syndrome, particularly in women. Thus, long-term evaluations of the impact of COVID-19 on mental health and preventive public health initiatives are warranted in older adults.
A cross-sectional descriptive study to assess the impact of the “open door” policy on patient satisfaction
- M. Campillo, J. Marti, L. Rius, S. Garcia Fernandez, M. Olivero, G. Sanchez Tomico, G. Brusco-Passalaqua, E. Pechuan, T. Vates, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S910
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Since the beginning of the modern psychiatry the acute units have established a “locked door” policy. Some studies show that this condition may increase patient’s discomfort and affect the perception of health quality of care (Boyer L, 2009, Eur Psychiatry Dec;24(8):540-9). Lately, several European countries such as Germany, Switzerland and Spain are starting to implement the “open-door” policy but its impact on patient’s satisfaction is still unknown (Hochstrasser, L, Frontiers in Psychiatry, 9(57). https://doi.org/10.3389/fpsyt.2018.00057) .
ObjectivesTo help characterize the advantages of the “open-door” policy implemented in an acute inpatient psychiatric unit in order to assess the patient’s view of it.
MethodsThis is a descriptive observational study carried out at an inpatient psychiatric unit. Data were collected after the implementation of the open door policy on June 2019, assessing the patient satisfaction of 31 subjects who completed the SATISPSY-22 scale at the time of discharge. Results are described using the average and its standard deviation.
ResultsResults show scores in all items above 50 points, being the care team and the quality of care the most valued ones with 82 and 79 points respectively. The overall score is above 65 points (Fig. 1).
Image:
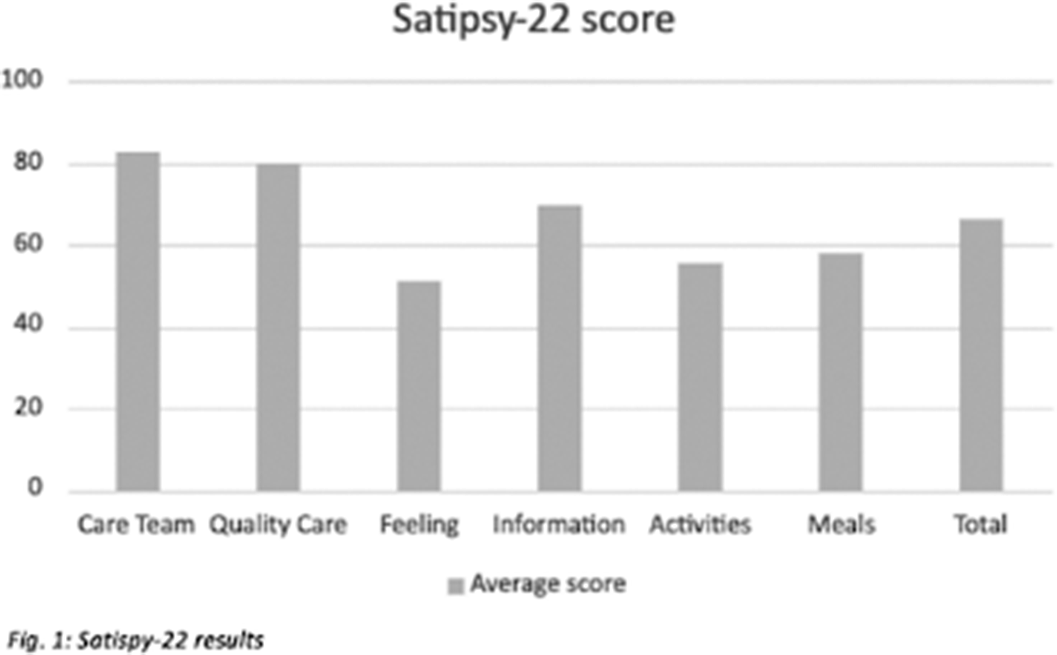 Conclusions
ConclusionsIn line with previous studies, our data suggests that the main impact of the “open-door” policy implementation is on patients’ perception of the care, being Quality of care and satisfaction with the Staff the items with highest scores. This could be explained by patients trusting more in the Care team, which would help enhance the therapeutic relationship improving therapeutic adherence, treatment adequacy and the outcome. Nevertheless, the Feeling related to hospitalisation was found to be the item with the lowest score. This could mean strategies should focus on improving patient’s insight regarding their clinical state and their need to be admitted. Our study supports the hypothesis that open-door policy in acute psychiatric units is seen positively by patients and that further research should be carried.
Disclosure of InterestNone Declared
Differential diagnosis of late onset psychotic symptoms. A case report.
- J. Sánchez Rodríguez, S. Puyal González, M. Paz Otero, E. Lozano Bori, A. García Recio
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1063
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a sixty-seven-year-old woman who is examined for the first time in the emergency room because of a nine-month clinical picture that involves psychotic symptoms. The patient exhibits persecutory delusions that started after she shared some private information on social media. These symptoms also entail emotional distress and behavioral disturbances. She has never experienced hallucinations, but she does present delusional interpretations of the environment. Her clinical history reveals abnormalities of premorbid personality, including paranoid and immature features.
Objectives(1) We will be carrying out a differential diagnosis of late onset psychotic symptoms. We will as well be exploring the concept of Paraphrenia and analyzing its differential features in order to stablish the most suitable diagnosis for the case.
(2) The relationship between abnormalities in premorbid personality and psychotic symptoms will be covered, reviewing the available literature on this matter, and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, considering her biography, the testimony of her family and the complementary tests performed during the hospitalization period.
A bibliographic review of the available scientific literature will also be developed involving disorders that could explain psychotic symptoms in the elderly, as well as the term Paraphrenia, which describes specific features in a psychotic episode but is not included in the diagnostic manuals.
Results(1) The symptomatology that our patient exhibits may be considered atypical given the late stage of its onset and its specific features.
(2) The case could be explained under the category of Delusional Disorder. From a psychopathological point or view, it could also fit under de diagnosis of Paraphrenia as described by Ravindran et al.
(3) Pathological personality traits were assessed in premorbid personality which included paranoid and immature features.
ConclusionsIt could be useful to review the concept of the “paranoid spectrum” as proposed by some authors regarding some patient’s psychotic symptoms that don’t exactly fit any of the nowadays diagnostic categories. “Paraphrenia” could be understood as a distinct clinical entity for patients who show psychotic disorders but keep affective warmth and lack though deterioration and grossly disorganized behavior.
Most patients with late life paranoid psychoses have abnormal premorbid personalities, most usually of schizoid or paranoid type. There’s a decent amount of consensus in viewing the premorbid personality as having been abnormal as an early marker of impending psychosis.
Reformulating the way we approach diagnosis of psychotic symptoms of late onset could help us identify vulnerable patients on a premorbid stage and better classify and understand atypical entities.
Disclosure of InterestNone Declared
Characteristics of patients admitted to a Psychiatric Home Hospitalization Unit and burden felt by caregivers
- J. Marti-Bonany, O. Garcia, D. Tolosa, R. Romar, G. Mateu, D. Garcia, R. Sanchez, M. G. Hurtado, M. Campillo, C. Monserrat, M. Roldan
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S901
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Severe mental illnesses characterized by periods of relapse that require intensive resource management. Caregivers of schizophrenia and bipolar disorder patients feel a considerable burden of care (Tanna et al. Ind Psychiatry J 2021, 30(2):299-304).
The main objective of Hospital at home for psychiatric patients is to provide intense care to patients with severe mental disorders at home as an alternative to acute admission (Alba et al. Rev Psiquiatr Salud Ment. 2019, 12 (4) 207-212).
ObjectivesThe aim of this study is to describe the characteristics of patients attended at the Psychiatric Home Hospitalization Unit of our hospital (HAD-CAEM) and to assess the of burden of care that caregivers feel while giveing care to this patients.
MethodsData were collected retrospectively at admission and discharge of all patients treated at HAD-CAEM between August 2018 to March 2022. Incomes of patients who met DSM-5 criteria for schizophrenia, bipolar disorder and major depressive disorder. Severity of disease and patient’s level of functionality was evaluated with the global assessment of functioning scale (GAF) and the Clinical Global Impression Scale (CGI). Burden Caregivers was evaluated with The Zarit Caregiver Burden Scale (ZCBS). Statistical analysis was performed by using SPSS program.
Results109 patients were included in the study. 49.5% were women. The mean age was 48 years (SD 18.47 years). 44% met criteria for schizophrenia, 25.7% for depressive disorder, and 30.3% for bipolar disorder. Most of them lived with their own family (47.7%); had secondary education (51.4%) and were unemployed (33%). 81% had a history of at least one admission to an acute psychiatric unit.
The mean duration of admission in HAD-CAEM was 33.8 days (SD 15.72 days), with a mean follow-up of 8.75 visits (SD 3.58 visits).
The mean CGI severity item at admission was 4.36 and there was an improvement at the time of discharge according to the CGI improvement item (mean CGI-I=2.43).
The GAF scale on admission was 46.74 (SD 11.2) and on discharge 64.24 (SD 13.85), showing an improvement of 17.5 points at discharge (p<0.001).
The mean ZCBS of the sample was 48.21 (SD 15.11). Mean ZCBS in Schizophrenia group (n=22) was 46.13 (SD 16.53), in depressive group (n=18) was 43.61 (SD 12.89) and for bipolar group (n=17) was 55.76 (SD 13.19). A statistical test is performed with ANOVA, showing significant differences between groups (p=0.039). Post-hoc analyzes show significant differences between bipolar disorder group and the depressive disorder group (p=0.04). No significant differences are found between the other groups.
ConclusionsCaregivers of schizophrenia, depressive and bipolar disorder patients feel a considerable burden of care. ZCBS was administered to the caregivers on the last day of admission, when the patient presented clinical and functional improvement. More studies are needed to support these results.
Disclosure of InterestNone Declared
Effect of psychotherapy on peripheral BDNF concentration levels in patients with bipolar disorder. A systematic review
- M. Valtueña García, L. Rubio Rodríguez, L. Sánchez-Pastor, I. Martínez-Gras, R. Rodríguez-Jiménez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S706
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotherapy is a treatment of proven efficacy in bipolar disorder (BD), but little is known about the molecular and cellular mechanisms that it produces in the brain. Brain-derived neurotrophic factor (BDNF) is thought to be important in neuroplasticity and could be increased by psychopharmaceuticals and psychotherapy in BD patients, but evidence in the literature is limited.
ObjectivesTo analyze the scientific studies that relate psychotherapies with the increase in BNDF levels in patients with BD.
MethodsSystematic review with PRISMA recommendations in PUBMED and Web of Science in July 2022. The search was performed using the combination of keywords “bipolar disorder” AND (“BDNF” OR “Brain Derived Neurotrophic Factor”) AND “psychotherapy”.
ResultsWith the initial search, 839 studies were obtained, finally 8 articles were analyzed. The available literature supports the role of psychotherapy in increasing BNDF in patients with BD.
ConclusionsBDNF could be a biomarker of therapeutic efficacy in BD. Psychotherapy increases BDNF levels. No differences were found between the different types of psychotherapies. More studies are needed to determine the mechanisms by which psychotherapies produce molecular changes in the brain.
Disclosure of InterestNone Declared
Smoking treatments for patients with mental illness: case presentation and a brief literature review
- F. Garcia Sanchez, M. Gutierrez Rodriguez, C. Moreno Menguiano, M. A. Corral Alonso, J. J. Vazquez Vazquez, S. M. Bañon Gonzalez, V. Voces Domingo, J. A. Casado de la Hera
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S756
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Smoking prevalence in patients with mental illness ranges between two to 4 times higher than general population. This higher prevalence has a multifactorial origin, and some of the possible causes are still unknown.
They have a higher prevalence of tobacco-associated diseases and higher mortality.
Additionally, these patients have greater difficulty in treating and quitting smoking.
A relationship has been found between severity of mental illness and smoking. Risk of suicide seems to be higher in patients with higher tobacco consumption. Schizophrenia is the mental illness that has been most closely related to smoking, with a prevalence close to 90%.
ObjectivesThe aim of this work is reviewing the current bibliography referring to smoking treatments for patients with mental illness
MethodsA literature search using electronic manuscripts available in PubMed database published during the last ten years and further description and discussion of a single-patient clinical case
ResultsThe treatment of tobacco dependence in patients with mental illnesses is sometimes waited until there is psychiatric stability, which can take a long time in those cases with more severe mental disorders, which can have negative physical and psychiatric consequences.
The combined treatment of cognitive behavioral therapy and pharmacological treatment is the most effective approach. Nicotine replacement therapy can be useful, while combined use of antidepressants or anxiolytics is also recommended.
Bupropion has shown efficacy. In patients with schizophrenia it does not seem to worsen positive symptomatology, but improving the negative one. It should not be used in patients with bipolar disorder or bulimia.
Varenicline has shown efficacy in the general population, but limitations were established in patients with mental illness, although it is the drug that has shown greater efficacy. However, is not currently available in our country.
Cytisine is a drug with limited number of studies in the psychiatric population but it may be a reasonable treatment alternative.
ConclusionsThe prevalence of tobacco use in patients with mental illness is higher than the general population, especially in paranoid schizophrenia. The consequences on physical health and the evolution of psychiatric illness are very relevant. Based on above, a multidisciplinary and coordinated management involving psychiatrists and other specialists in the treatment of these patients should be desirable.
Disclosure of InterestNone Declared
Patient satisfaction in an “open-door” acute inpatient psychiatric unit
- M. Campillo, L. Rius, S. Garcia, M. Olivero, G. Sanchez Tomico, M. Martinez Garcia, I. Garcia Velasco, C. Monserrat, A. Pratdesava, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S903
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Traditionally, psychiatric wards had established a “locked door” policy but secluded conditions may increase patient’s discomfort1 that could affect the perception of health quality of care2. Recently, the “open-door” policy is being adopted in several European countries but its impact on patient satisfaction remains unknown (Schreiber, LK. BMC Psychiatry. 2019 May 14;19(1):149). Since 2019 our psychiatric hospital has implemented the open-door policy.
ObjectivesThe aim of this study is to investigate the impact of the “open-door” policy on patient satisfaction during their stay in the acute inpatient unit of our psychiatric hospital.
MethodsThis is an observational study. Prior to the implementation of the open door policy 31 patient satisfaction data was collected between October 2018 to April 2019 and it was also assessed with 31 subjects between July to October 2019, after the implementation of the open “door-policy”. The inclusion criteria were being >18 years old, reading Spanish correctly and with a length of stay >72 hours. The patients with dementia disorder and intellectual disability where excluded from the study. We used the Satispsy-22-E scale, a self-administered questionnaire (Frías, V., et al. 2018. Psychiatry Res. Oct;268:8-14). It assesses patient’s experience of hospitalization through 22 items distributed into 6 dimensions. The score range is from 0 to 100. Differences in Satispsy-22-E scores were analysed by applying ANOVA using the IBM-SPSS (v. 25).
ResultsTotal scores in Satispsy-22 are provided in Figure 1. We found that patient satisfaction was increased in the dimensions of “personal experience” and “food” (p<0.05). No significant differences were found in staff, quality of care, information, activity dimensions and Total score (Table 2).
Dimension F-Test Statistic Value Staff 1.402 p=0.241 Quality of Care 841 p=0.362 Personal Experience 4.071 p=0.048* Information 656 p=0.420 Activity 434 p=0.512 Food 4.507 p=0.037* TOTAL 3.645 p=0.61 Image:
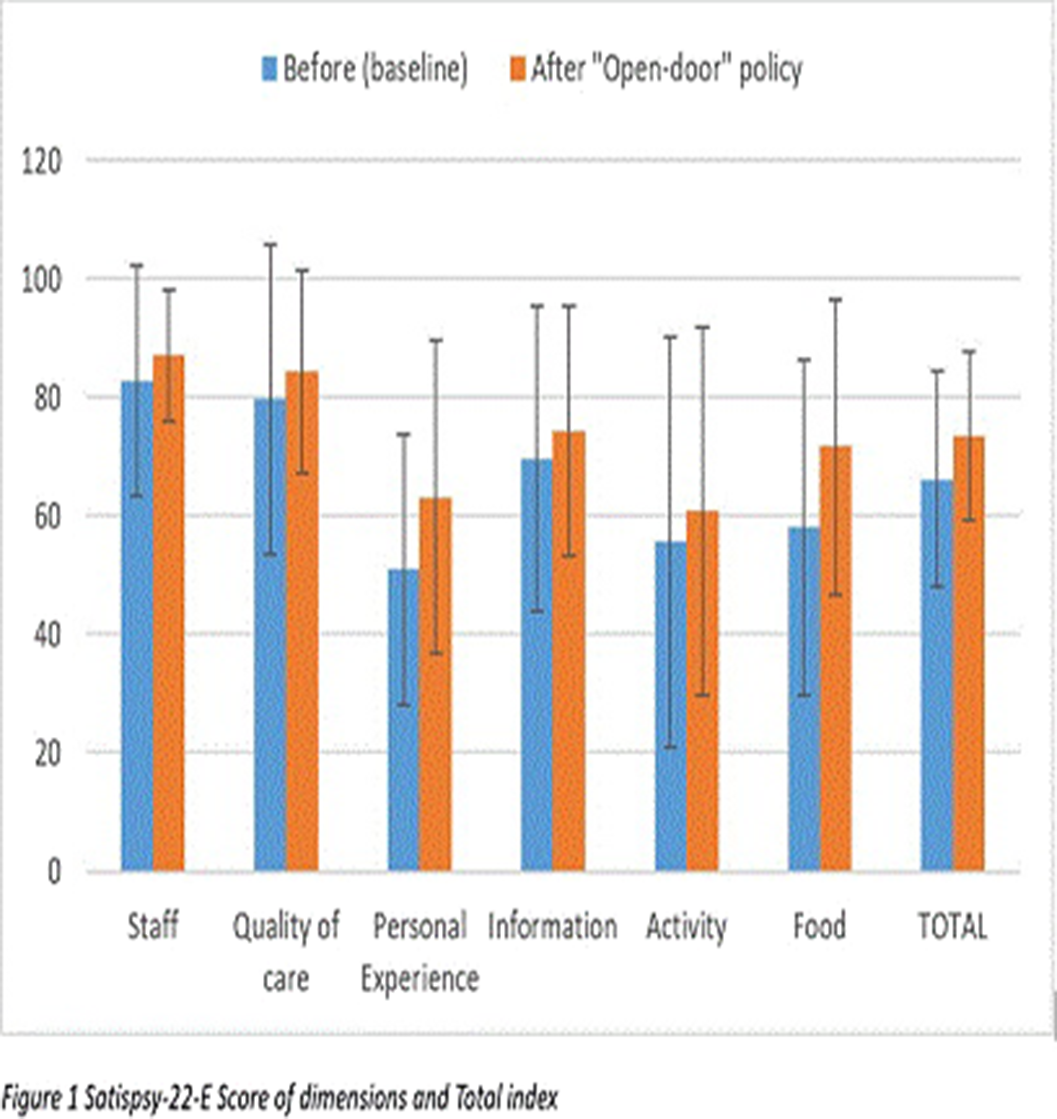 Conclusions
ConclusionsOur results provide preliminary evidence indicating that the open-door policy could have a positive impact on patient satisfaction, especially in relation to the personal experience on an acute inpatient psychiatric unit.
Disclosure of InterestNone Declared
Resistant depression. Clinical manifestations and diagnosis. Purposely a case
- S. M. Bañón González, N. Ogando Portilla, O. Sobrino cabra, B. Gamo Bravo, F. García Sánchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S844
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The term “depression” can be used in different senses: it can be a syndrome, a mood state, a mental disorder, and all of them are distinct clinical conditions…There are no pathognomonic features of bipolar/unipolar depression. A good medical history is the most important component of the evaluation. We have to use clinical variables and differential epidemiology for a correct diagnosis.
ObjectivesThey both analyze clinical, psychopathological and epidemiological characteristics of resistant depression and they review causes, incidence, prevalence, diagnostic, therapeutic tools and the importance of maintaining the treatment, because the abandonment of the treatment is a good predictor of possible relapses.
MethodsA literature Review of the last five years concerning resistant depression has been done: prevalence, incidence, pathogenesis and its relationship with other psychiatric disorders encoded in DSM-V.
ResultsUnipolar major depression (major depressive disorder) is characterized by a history of one or more major depressive episodes and no previous history of mania or hypomania symptoms. A major depressive episode is presented with five or more of the following nine symptoms for at least two consecutive weeks; at least one of them must be either a depressed mood or a loss of interest or pleasure. In addition, the symptoms must cause significant distress or psychosocial impairment, and not be a direct result of a substance or general medical condition.
ConclusionsSymptoms of unipolar depression in adults can overlap with symptoms of other psychiatric and general medical disorders. Unipolar depression needs to be distinguished from these other disorders to prevent inappropriate treatment.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
Delusions of body control: Psychopathological description of a case.
- C. M. Gil Sánchez, J. A. Salomón Martínez, E. Fernández García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S999-S1000
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A considerable number of patients with schizophrenia suffer from somatic passivity or delusions of control. So much so, that Schneider considered them as part of the first-rank symptoms.
In these cases, patients can think that feelings, impulses, thoughts, or actions are controlled or imposed by an external force.
ObjectivesThe objective is to make a psychopathological description of this symptomatology, based on a case report with Anomalous bodily experiences.
MethodsIn this study, we describe the case of a patient with disorder of self-experience. We have conducted a systematic review of the descriptions published to date, regarding this case.
ResultsWe present the case of a 21-year-old patient who had gone to the emergency services three times for somatic pathology (described as dysesthetic and algic sensations in the throat, stomach and testicles).
In the psychopathological exploration, a delusional narrative is observed, as he refers that these sensations are being provoked by external people, with the aim of harming him.
The patient reports that these people are causing an increase in salivation in his salivary glands, for which he spits repeatedly.
He explains that these people can control his organs using an influencing machine, which in this case consists of a microchip implanted at the retroauricular area, from which they give orders and insult him at the same time.
In this case, a good symptom response was achieved with intramuscular Aripiprazole.
ConclusionsIn the experiences of passivity, the patient experiences one event as if it were not his, but inserted into his self from the outside.
In the case of somatic passivity, there is a belief that there are external influences acting on the body. In this case, there was probably a kinesthetic hallucination coupled with an experience of passivity.
Similar to other published cases, this patient complained of being controlled and impaired by some form of contemporary technology. Delusions of control are often associated with delusional explanations about how thought or body can be controlled, in this case, through a microchip.
Disclosure of InterestNone Declared
Visual hallucinations and age-related macular degeneration: case presentation and a brief literature review
- M. M. Gutiérrez Rodríguez, F. García Sánchez, M. Á. Corral Alonso, J. J. Vázquez Vázquez, C. Moreno Menguiano
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S936-S937
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
age-related macular degeneration (AMD) is an ocular disease involving central vision. It is one of the mainreasons of vision loss in people over 50. Seeing non-existing faces or shapes are described in AMD. Symtoms of visualhallucinations that occur as a result of vision loss is known as Charles Bonnet syndrome (CBS). These patients haveintact cognition, do not have hallucinations in any other sensory modalities, and retain insight into the unreal nature oftheir hallucinations.
Objectivesthe aim of this work is analizing ethiology, demographic characteristics, clinica features and treatment inpatients with AMD and visual hallucinations
Methodsa literature search using electronic manuscripts available in PubMed database published during the last ten years with further description and discussion of a single-patient clinical case.
Resultsin different studies in patients diagnosed with AMD, the reported prevalence ranges between 15 up to 39percent. Patients with more significant vision loss may be more likely to experience visual hallucinations. In large caseseries, mean age is 70 to 85 years. Hallucinations can last few minutes or several hours. On average, people experiencethese hallucinations on and off for about 3 years. Those who experience hallucinations tend to see multiple types ofimages, particularly people and faces.The diagnosis of CBS is made when visual hallucinations occur in patients withvision loss in the absence of psychosis, delirium, or other causes.
There is no specific treatment for CBS: optimal ocular care, education and differents techniques to manage hallucinations(changing your lighting conditions and environment, blinking frequently or moving your eyes side-to-side rapidly whilekeeping your head still…). Antidepressants, anticonvulsants, anxiolytics and low-dose of antipsychotics have been used for CBS with positiveeffects in previous reports, but the efficacy of these drugs in the treatment is somewhat questionable and should bereserved for those who exhibit high levels of distress and have not responded to conventional intervention.
Case report: 80-years old woman who presented with a 4 month history of hallucinations and legally blind from AMD. Aworkup for other pathological causes of visual hallucinations was negative.
ConclusionsCBS is an under-recognized and under-reported disorder that involves visual hallucinations in visuallyimpaired individuals. It requires a multidisciplinary approach from neurologists, psychiatrists, general practitioners andophthalmologists. New studies are needed in order to understand its clinical presentation and to improve its management.
Disclosure of InterestNone Declared
An empirical staging model for schizophrenia using machine learning
- M.-C. Clara, F. Sánchez-Lasheras, A. García-Fernández, L. González-Blanco, P. A. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S626-S627
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the great challenges still to be achieved in schizophrenia is the development of a staging model that reflects the progression of the disorder. The previous models suggested have been developed from a theoretical point of view and do not include objective variables such as biomarkers, physical comorbidities, or self-reported subjective variables (Martinez-Cao et al. Transl Psychiatry 2022; 12(1) 1-11).
ObjectivesDevelop a multidimensional staging model for schizophrenia based on empirical data.
MethodsNaturalistic, cross-sectional study. Sample: 212 stable patients with Schizophrenia (F20). Assessments: ad hoc questionnaire (demographic and clinical information); psychopathology: PANSS, CDS, OSQ, CGI-S; functioning: PSP; cognition: MATRICS; laboratory tests: C-Reactive Protein (CRP), IL-1RA, IL-6, Platelets/Lymphocytes (PLR), Neutrophils/Lymphocytes (NLR), and Monocytes/Lymphocytes (MLR) ratios. Statistical analysis: Variables selection was performed with an ad hoc algorithm developed for this research. The referred algorithm makes use of genetic algorithms (GA) to select those variables that show the best performance for the patients classification according to their global CGI-S. The objective function of the GA maximizes the individuals correct classification of a support vector machines (SVM) model that employs as input variables those given by the GA (Díez-Díaz et al. Mathematics 2021; 9(6) 654). Models performance was assessed with the help of 3-fold cross-validation and these process was repeated 10,000 times for each one of the models assessed.
ResultsMean age(SD): 39.5(13.54); men: 63.5%; secondary education: 59.50%. Most patients in our sample had never been married (74.10%), and more than a third received disability benefits due to schizophrenia (37.70%). The mean length of the disease was 11.98(12.02) years. The best SVM model included the following variables: 1)Clinical: number of hospitalizations, positive, negative, depressive symptoms and general psychopathology; 2)Cognition: speed of processing, visual learning and social cognition; 3)Functioning: PSP total score; 4)Biomarkers: PLR, NLR and MLR. This model was executed again 100,000 times applying again 3-fold cross-validation. In 95% of the algorithm executions more than a 53.52% of the patients were classfied in the right CGI-S category. On average the right classification was of 61.93%. About specificity and sensitivity the average values obtained were of 0.85 and 0.64 respectively.
ConclusionsOur staging model is a robust method that appropriately distributes patients according to the severity of the disorder. Highlights the importance of clinical, functional and cognitive factors to classify patients. Finally, the inflammatory parameters PLR, NLR and MLR have also emerged as potential biomarkers for staging schizophrenia.
Disclosure of InterestNone Declared





