73 results
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
TrackAnalyzer: A Fiji/ImageJ toolbox for a holistic analysis of tracks
- Ana Cayuela López, Eva M. García-Cuesta, Sofía R. Gardeta, José Miguel Rodríguez-Frade, Mario Mellado, José Antonio Gómez-Pedrero, Carlos Oscar S. Sorzano
-
- Journal:
- Biological Imaging / Volume 3 / 2023
- Published online by Cambridge University Press:
- 11 October 2023, e18
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Current live-cell imaging techniques make possible the observation of live events and the acquisition of large datasets to characterize the different parameters of the visualized events. They provide new insights into the dynamics of biological processes with unprecedented spatial and temporal resolutions. Here we describe the implementation and application of a new tool called TrackAnalyzer, accessible from Fiji and ImageJ. Our tool allows running semi-automated single-particle tracking (SPT) and subsequent motion classification, as well as quantitative analysis of diffusion and intensity for selected tracks relying on the graphical user interface (GUI) for large sets of temporal images (X–Y–T or X–Y–C–T dimensions). TrackAnalyzer also allows 3D visualization of the results as overlays of either spots, cells or end-tracks over time, along with corresponding feature extraction and further classification according to user criteria. Our analysis workflow automates the following steps: (1) spot or cell detection and filtering, (2) construction of tracks, (3) track classification and analysis (diffusion and chemotaxis), and (4) detailed analysis and visualization of all the outputs along the pipeline. All these analyses are automated and can be run in batch mode for a set of similar acquisitions.
Is social media important in adolescents with eating disorders?
- B. Martínez-Núñez, D. S. Cohen, R. Encinas-Encinas, A. Paniagua-Velasco, D. A. Gómez-Guimaraes, C. García-López, B. Muchada-López, M. Faya-Barrios, M. Graell-Berna
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S522-S523
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Eating disorders (ED) are complex entities of multicausal etiology that mainly affect adolescents and young women. For this reason, EDs frequently cause medical and psychological complications that can cause potentially irreversible developmental sequelae during adolescence.
96% of Spanish youth (15-29 years old) use daily Internet. In addition, 83% use Social Networks. Internet could be a good way to spread information through social media, websites, providing material and means to achieve the body culture purpose.
As we have seen in various papers, social media can influence and trigger the development of EDs.
ObjectivesThe objetives of the study are to analyse the preferred social network by adolescents diagnosed with eating disorders, as well as to measure characteristic and time-use of these networks.
MethodsWe decided to undergo a transversal study to analyse the use of social media. For that, we developed a survey to reflect the use of the main social networks (Instagram, Facebook, Snapchat, Twitter, YouTube and Reddit) in adolescents diagnosed with eating disorders in Spain, who are in outpatient treatment in a specialised ED unit.
ResultsThe total number of adolescents interviewed was 65; of these 96.9% were females and 3.1% males. The mean age was 14.8 years.
The preferred social network was Instagram (54%), followed by TikTok (34%) and YouTube (6%).
Most of the patients interviewed (68%) admitted checking Instagram daily, and 31% reflected spending between 1-3 hours/day. None of the adolescents reported using Facebook or Reddit.
The majority of adolescents (89%) admitted having ignored friend requests while 12% reflected the importance of having a high number of followers as a way of external validation, getting more ‘likes’ and getting to know more people.
ConclusionsThe obtained results reinforce the need of exploring and taking into account the use of Social Media in adolescents with ED and how it may influence their pathology. There is a need for further prospective research in this field.
Disclosure of InterestNone Declared
Alternative initiations with 6-monthly paliperidone palmitate. A retrospective study
- S. Benavente López, S. Bolaño Mendoza, A. Parra González, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S488-S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
6-monthly paliperidone palmitate features an initiation regimen through 1-monthly paliperidone palmitate or 3-monthly paliperidone palmitate. Some patients do not have sufficient adherence to treatment and it is necessary at the clinical level to start directly with 6-monthly paliperidone palmitate. There is little clinical experience with these alternative initiations and through this work those that have been carried out for 12 months at the Hospital Universitario Infanta Elena are exposed.
ObjectivesThe main objective of the study is to describe the alternative initiations performed with 6-monthly paliperidone palmitate in routine clinical practice, having opted for a regimen different from the standard for clinical reasons.
MethodsA retrospective selection of patients will be made through non-probabilistic consecutive sampling, including all patients who have been administered 6-monthly paliperidone palmitate with a start different from the standard during the last 4 months. To do this, the electronic medical record will be used, first selecting the patients who have started 6-monthly paliperidone palmitate through the anonymized digital records and, later, including in the study only those who have followed an alternative initiation pattern. The variables studied will be the following: age, sex, diagnosis, dose of paliperidone palmitate, initiation regimen, consumption of toxic substances, absenteeism from 6-monthly paliperidone palmitate, and visits to the emergency room and admissions.
ResultsThe study included a total of 20 patients (n: 20). 80% of the patients were male and 20% were female. The mean age was 39.7 years. 75% of the patients had an associated substance use disorder. The following alternate starting schedules were performed with biannual paliperidone palmitate: monthly paliperidone palmitate on days 1 and 8, and 6-monthly paliperidone palmitate on day 38 (n: 11); monthly paliperidone palmitate 150 mg together with semi-annual paliperidone palmitate both on day 1 (n: 5); biannual paliperidone palmitate on day 1 supplemented with oral paliperidone for 45 days (n:4). A total of 0 visits to the emergency department and 0 admissions were observed after the 6-monthly paliperidone palmitate regimen.
ConclusionsAlternative initiations with 6-monthly paliperidone palmitate may be a useful and safe clinical alternative in patients with very low adherence who, due to clinical needs, require starting 6-monthly paliperidone palmitate earlier in order to guarantee adherence.
Disclosure of InterestNone Declared
Clinical experiences with 6-monthly paliperidone palmitate after 12 months of use. A retrospective study
- S. Benavente López, A. Parra González, S. Bolaño Mendoza, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S488
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIA) have provided a significant improvement in the treatment of schizophrenia. Although there is already significant clinical experience with paliperidone palmitate, it is important to evaluate the clinical response of patients to this new 6-monthly presentation, so descriptive studies based on real clinical evidence can be very useful for this purpose.
ObjectivesThe main objective of the study is to describe the use of 6-monthly paliperidone palmitate in routine clinical practice, providing variables that objectify the evolution such as the number of admissions and visits to the emergency room.
MethodsRetrospective descriptive study with a sample selected by non-probabilistic consecutive sampling, retrospective type, in a time interval of 12 months (n=40). The patients selected were all those who received 6-monthly paliperidone palmitate treatment, with a diagnosis of schizophrenia, in 12 months of use at Hospital Universitario Infanta Elena. A descriptive analysis was performed. Mean and standard deviation were calculated for quantitative variables and N and percentage for categorical variables.
ResultsA total of 40 administrations of 6-monthly paliperidone palmitate were performed in the study. None of the patients presented adverse reactions related to the administration of the drug, not reporting local pain or inflammation of the puncture area, except for the characteristic discomfort of an intramuscular puncture. Regarding the efficacy of 6-monthly paliperidone palmitate, none of the patients presented a psychotic decompensation after its administration, maintaining psychopathological stability after the change. The switch to 6-monthly paliperidone palmitate was made from both 1-monthly paliperidone palmitate and 3-monthly paliperidone palmitate, both showing the same efficacy. Regarding tolerability, all the patients who were administered 6-monthly paliperidone palmitate were previously treated with the monthly and quarterly presentation of the same molecule, having presented good tolerability to it, maintaining said tolerability after treatment. change to 6-monthly paliperidone palmitate, with no adverse reaction being recorded after the change. The adherence presented by the patients was very good, performing 100% of the administrations of 6-monthly paliperidone palmitate
Conclusions6-monthly paliperidone palmitate may be an effective and well-tolerated treatment for the treatment of schizophrenia. In the present study, the use of said LAIA in a group of 40 patients is objectified, showing excellent efficacy and tolerability. All study patients were already stable with the 1-monthly and 3-monthly paliperidone palmitate formulations, maintaining said psychopathological stability when switching to the 6-monthly paliperidone palmitate formulation, with excellent adherence and adverse effect profile .
Disclosure of InterestNone Declared
Clinical experiences with 6-monthly paliperidone palmitate beyond the diagnosis of schizophrenia. A retrospective study
- S. Benavente López, S. Bolaño Mendoza, A. Parra González, A. Lara Fernández, A. Herencias Nevado, E. Baca García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotics (LAIA) are used in diagnoses other than schizophrenia. Over the last two decades, LAIAs have been developed with less administration frequency, going from 2-weekly presentations to 6-monthly presentations. The 6-monthly paliperidone palmitate has recently been released, allowing a reduction in the frequency of administration compared to the 1-monthly presentation and the 3-monthly presentation. Descriptive studies based on real clinical evidence can be very useful to assess clinical outcomes.
ObjectivesThe main objective of the study is to describe the use of 6-monthly paliperidone palmitate in patients with schzophrenia, providing variables that objectify the evolution such as the number of psychotic decompensations.
MethodsRetrospective descriptive study with a sample selected by non-probabilistic consecutive sampling, retrospective type, in a time interval of 10 month (n=80). The patients selected were all those who received 6-monthly paliperidone palmitate treatment from after 10 months of use at Hospital Universitario Infanta Elena. A descriptive analysis was performed. Mean and standard deviation were calculated for quantitative variables and N and percentage for categorical variables.
ResultsA total of 80 administrations of 6-monthly paliperidone palmitate were performed in the study. None of the patients presented adverse reactions related to the administration of the drug, not reporting local pain or inflammation of the puncture area, except for the characteristic discomfort of an intramuscular puncture. Regarding the efficacy of 6-monthly paliperidone palmitate, none of the patients presented a psychotic decompensation after its administration, maintaining psychopathological stability after the change. The switch to 6-monthly paliperidone palmitate was made from both 1-monthly paliperidone palmitate and 3-monthly paliperidone palmitate, both showing the same efficacy. Regarding tolerability, all the patients who were administered 6-monthly paliperidone palmitate were previously treated with the monthly and quarterly presentation of the same molecule, having presented good tolerability to it, maintaining said tolerability after treatment. change to 6-monthly paliperidone palmitate, with no adverse reaction being recorded after the change. The adherence presented by the patients was very good, performing 100% of the administrations.
Conclusions6-monthly paliperidone palmitate may be an effective and well-tolerated treatment for the treatment of schizophrenia and other diagnoses such as bipolar disorder or borderline personality disorder. According to objective data, 6-monthly paliperidone palmitate could be an effective and well-tolerated treatment as an alternative to monthly and quarterly presentations of the same molecule. Longitudinal studies must be carried out to confirm this hypothesis.
Disclosure of InterestNone Declared
Impact of COVID-19 pandemic on psychiatric emergency care in a general hospital
- J. M. Rodríguez Capilla, A. Rubio Carramiñana, S. Vega Castellote, S. López Fernández, I. Arilla Herrera, J. M. Almenara Galdeano, A. Mora Prat, M. Campillo Benito, J. Albero Garcia, A. Valderrey Ratia, A. Grau Peñas, C. Pastor Fernández, M. Moreno Monzó, J. Guitart Gil, J. Martínez Raga, C. Knecht
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S405-S406
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The SARS-CoV-2 pandemic has produced an unprecedented clinical situation, causing a direct and indirect impact on the physical and mental health of the population. In Spain, between March 15 and June 21 of 2020, it was decreed a home confinement that caused the interruption of the daily life of millions of people. However, there are few studies that analyze the changes produced in psychiatric care in the Emergency Department (ED).
ObjectivesTo analyze the changes produced in psychiatric emergencies, subanalysing paediatric population, during the first year of the pandemic (COV1/Y-COV1) compared to the previous year (NOCOV/Y-NOCOV1). To analyze the clinical features of patients attended during the lockdown period of the pandemic (LOCK) and compare it to the period of the pandemic after the lockdown (NOLOCK).
MethodsThrough the registry of computerized medical records, patients who attended the psychiatric hospital emergency department between 03/01/2019 and 02/28/2021 were identified. We also identified all attendances from 15/03 to 21/06 in 2019 and in 2020 to obtain variables from the lockdown period.
ResultsDuring period of this study, 2694 psychiatric visits made in the ED (1744 patients - 54.3% women, and 69.5% were between 25 and 64 years-), 1537 in NOCOV and 1157 in COV1. Significant differences were found between COV1 and NOCOV in sociodemographic variables, such as employment status and number of offspring. At a clinical level, in COV1, we observed an increase in attendance due to heteroaggressive behaviors, mania, insomnia and problems due to substance use. An increase in the prescription and/or modification of treatment was observed (59.3% vs 54.3%). During COV1, in terms of discharge follow-up in the month following the ED visit, telematic assistance increased (11.4% vs. 5.3%). During the period of study, 282 ED attendances were performed, 153 in Y-NOCOV and 129 in Y-COV1. At a clinical level, during Y-COV1, a decrease in attendances related to substance use was found significant. The sub-analysis carried out for LOCK and NOLOCK yields similar data to those obtained in the COV1 vs. NOCOV1 comparison. During lockdown, the face-to-face follow-up in the month following the ED was significantly lower (39,5% vs 57,1%) regarding telematic follow-up (24,4% vs 5,8%) In this period, an increase of adolescents without previous mental health follow-up was observed (44% LOCK vs. 22% NOLOCK).
ConclusionsOur work supports the hypothesis that the COVID-19 pandemic caused a change in psychiatric care in the ED. It also shows how lockdown changed the attendance in psychiatric emergencies, and also in the later community care attendance. Changes are detected in emergency care for adolescents during the pandemic compared to the previous year. Strikingly, our study does not reflect a quantitative increase in the demand. It would be of interest to continue collecting data after the time of the present project.
Disclosure of InterestNone Declared
Tobacco use in first-episode psychosis, a multinational EU-GEI study
- T. Sánchez-Gutiérrez, E. Rodríguez-Toscano, L. Roldán, L. Ferraro, M. Parellada, A. Calvo, G. López, M. Rapado-Castro, D. La Barbera, C. La Cascia, G. Tripoli, M. Di Forti, R. M. Murray, D. Quattrone, C. Morgan, J. van Os, P. García-Portilla, S. Al-Halabí, J. Bobes, L. de Haan, M. Bernardo, J. L. Santos, J. Sanjuán, M. Arrojo, A. Ferchiou, A. Szoke, B. P. Rutten, S. Stilo, G. D'Andrea, I. Tarricone, EU-GEI WP2 Group, C. M. Díaz-Caneja, C. Arango
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 7265-7276
-
- Article
- Export citation
-
Background
Tobacco is a highly prevalent substance of abuse in patients with psychosis. Previous studies have reported an association between tobacco use and schizophrenia. The aim of this study was to analyze the relationship between tobacco use and first-episode psychosis (FEP), age at onset of psychosis, and specific diagnosis of psychosis.
MethodsThe sample consisted of 1105 FEP patients and 1355 controls from the European Network of National Schizophrenia Networks Studying Gene–Environment Interactions (EU-GEI) study. We assessed substance use with the Tobacco and Alcohol Questionnaire and performed a series of regression analyses using case-control status, age of onset of psychosis, and diagnosis as outcomes and tobacco use and frequency of tobacco use as predictors. Analyses were adjusted for sociodemographic characteristics, alcohol, and cannabis use.
ResultsAfter controlling for cannabis use, FEP patients were 2.6 times more likely to use tobacco [p ⩽ 0.001; adjusted odds ratio (AOR) 2.6; 95% confidence interval (CI) [2.1–3.2]] and 1.7 times more likely to smoke 20 or more cigarettes a day (p = 0.003; AOR 1.7; 95% CI [1.2–2.4]) than controls. Tobacco use was associated with an earlier age at psychosis onset (β = −2.3; p ⩽ 0.001; 95% CI [−3.7 to −0.9]) and was 1.3 times more frequent in FEP patients with a diagnosis of schizophrenia than in other diagnoses of psychosis (AOR 1.3; 95% CI [1.0–1.8]); however, these results were no longer significant after controlling for cannabis use.
ConclusionsTobacco and heavy-tobacco use are associated with increased odds of FEP. These findings further support the relevance of tobacco prevention in young populations.
Unplanned Pregnancy in women with mental disorder
- A. Roca Lecumberri, E. Gelabert, A. Torres Giménez, E. Solé, S. Andrés-Perpiñá, E. Roda, C. Lopez, C. Naranjo, L. Garcia-Esteve
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S331-S332
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Few studies have investigated the level of planning of pregnancy among women with mental disorder and associated risk factors.
ObjectivesThe purpose of this study was to determine the associated factors to UP and psychopathological consequences.
MethodsA cross sectional study was conducted at the Perinatal Mental Health Unit of the Hospital Clínic in Barcelona. The total sample comprised 675 consecutive pregnant women with diagnosis of mental disorder (DSM-IV criteria), seen between January 2006 and December 2018. Clinical, psychometric and socio-demographic variables were collected at the first visit. Pregnancy planning was assessed by a question “Was this pregnancy planned?” with three possible answers: 1) Yes, it was planned and has been well received; 2) No, it was not planned but it has been well received; and 3) No, it was an accident. Response 1 was coded as “planned pregnancy” and responses 2 and 3 as “Unplanned Pregnancy”.
Results38.4% of the sample had an UP. Younger age, lower levels of education, Latin-American population, multiparity, financials problems and poor relationship with the partner were associated with UP in women with mental disorder. The mean EPDS and STAI scores and the presence of self-harming thoughts were significantly higher in women with UP.
ConclusionsUP was associated with more depressive and anxious symptoms and more self-harming thoughts. It is necessary to promote reproductive health care for women with mental disorders and to take into account their reproductive life plan, especially in those with risk factors described.
DisclosureNo significant relationships.
Multifamily therapy in first episodes of psychosis: a pilot study
- I. García Del Castillo, S. López García, A. Pérez Balaguer
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S783-S784
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Multifamily interventions have shown to reduce the risk of relapse of psychotic symptoms in first episodes of psychosis (FEPs) but are not frequently implemented in specific treatment programs. We have develop a pilot study for the implementation of the interfamily therapy in FEPs within a Mental Health Centre in the Community of Madrid.
ObjectivesThe aims were to examine: relapses (measured as re-hospitalization), duration of re-hospitalizations and voluntary versus involuntary re-hospitalizations during participation in MFG compared with the previous year.
Methods21 subjects participated in a MFG during 12 months, 11 participants with a diagnosis of psychosis and 10 family members. Interfamily therapy works as a new model of interactive psychoeducation among families where they share their own experiences and look for comprehension and solutions all together.
ResultsOur clinical experience in an interfamily therapy intervention over 12 months has led us to identify a high degree of participation and acceptance by users and their families, and we have observed a lower relapse rate, with fewer of psychiatric admissions and of shorter duration among patients during the year of participation in the MFG compared to the year before treatment.
ConclusionsMFG has been well accepted by both patients and their families, with a high degree of participation.The results observed in our experience of MFG treatment are consistent with the findings of previous studies that support the reduction of the relapse rate, the number of hospitalizations and their duration when family interventions are incorporated into treatment in recent-onset psychosis, especially in a multi-family group format.
DisclosureNo significant relationships.
Factors associated to stigma in mental health workers of Castilla y Leon. The role of burnout and work motivation
- J.M. Pelayo-Terán, Y. Zapico-Merayo, M.E. Garcia Llamas, S. Vega-García, C. López-Zapico, M.R. Villa-Carcedo, Á. Álvaro-Prieto
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S689-S690
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Stigma is one of the most important barriers to help-seeking, treating maintenance and recovery for people suffering mental disorders. These attitudes, when present in mental health workers, may have a negative effect on the quality of health care.
Objectivesto evaluate the levels of stigma in a representative sample of mental health workers and to explore potential modifiable factors associated to stigma attitudes.
MethodsAn online survey was conducted on the mental health workers of Castilla y León (Spain, 2409164 habs) while projecting the 2022 Mental Health Humanization plan in order to asses educational skills, burnout (Maschlach MBI), Professional Quiality of life (CVP-35) and Stigma attitudes (Mental Illness: Cinician’s Attitudes Scales, MICA4) together with sociodemographic and work position variables.
Results193 workers completed completed the survey. Stigma Attitude values of the sample were low (MICA4: 31.71; SD:7.3) and burnout were low or medium (medium Emotional Exhaustion: 19.22; SD8.89; low Depersonalization: 4.91; SD:3.61; Medium Personal Accomplishment: 34,17; 6.3). In the linear regression (R2=0.249; F:11,527; p<0,001), a lower Stigma was predicted by psychologist (Beta:0,207; p=0,003) or psychiatrist position (Beta:0,204; 0,005), Self-efficacy assessed by the item “I am qualified” in the CVP-35 (Beta:-10,144; p=0,023), and a higher stigma was predicted by nurse assistant position (Beta: -0.230; p=0.001), Depersonalization Burnout dimension (Beta:0,351; p<0,001) and years of service (Beta:0.148; p=0,023)
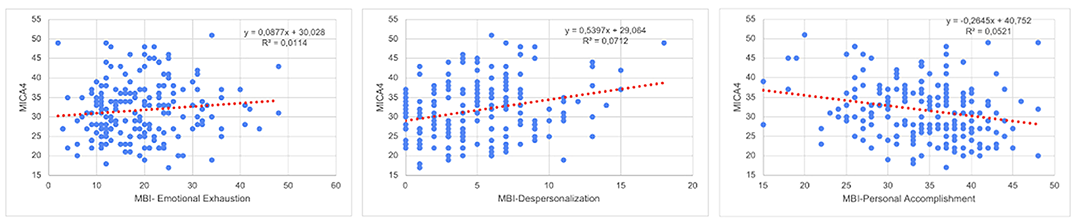
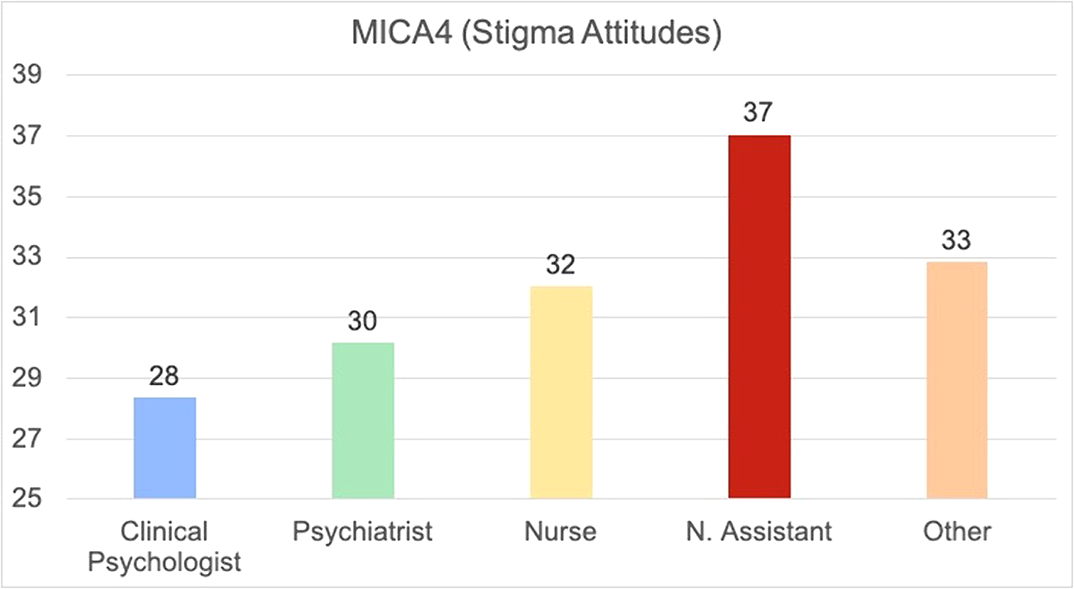 Conclusions
ConclusionsSome groups of mental workers are more vulnerable to develop stigma attitudes. These, may be increased by fatigue and burnout. Future interventions should determine if reducing burnout and increasing capacitation may be effective in stigma eradication
DisclosureNo significant relationships.
Levetirazetam psychosis
- C. Vilella Martín, M.Á. Alonso De La Torre López, P. García Vázquez, I. Gonzalez Rodríguez, S. Nuñez Sevillano, A. Serrano García
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S775
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Levetirazetam is an antiepileptic drug with psychiatric adverse reactions. It includes psychosis, paranoia or hallucinations. The frequency is less than 1%.
ObjectivesTo describe and study a case of Psychosis produced by Levetirazetam
MethodsRetrospective review of clinical records and complementary test, including psychiatry, electrophysiology and neurology. Diagnosis schales such as Salamanca Questionnaire were used as suport.
ResultsA 42-year-old woman diagnosed with tuberous sclerosis and undergoing treatment with levetirazetam acudes to the emergency department for behavioral disorders. She has presented an episode of aggression against a relative threatening him with a kitchen knife. The family reports that since the change in antiepilepticus 1 month ago, the patient has presented strange behaviors. Te Patient is conscious, uncooperative. Barely Approachable. Suspicious of her surroundings, with psychomotor restlessness, self-reference ideas and sparse speech. Auditory hallucinations seem to be present, as well as depressed and irritable mood. Psychic and somatic anxiety is found. Levetirazetam is discontinued, being replaced by valproic acid. Risperidone is started at a 3 mg dose. Treatment is well tolerated, and clinical stability is achived. Cluster A personality traits are found. Complementary test Blood and Urine simples, Imaging tests (CT and MRI), electroencephalogram and Electrocardiogram show no alterations
ConclusionsLevetirazetam can cause psychiatric adverse effects. it is important to make a proper diagnosis before a first psychotic outbreak in later life. Drugs that can produce psychiatric side effects should be identified and patients should be inform.
DisclosureNo significant relationships.
Pending challenges to e-mental health in the COVID-19 era: Acceptability of a smartphone-based ecological momentary assessment application among patients with schizophrenia spectrum disorders
- J.-D. Lopez-Morinigo, B.-E. Maria Luisa, A. Porras-Segovia, A. Sánchez-Escribano Martínez, P.-J. Escobedo-Aedo, V. González Ruiz-Ruano, L. Mata-Iturralde, L. Muñoz-Lorenzo, S. Sánchez-Alonso, A. Artés-Rodríguez, E. Baca-Garcia
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S343
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Concerns have been raised about ecological momentary assessment (EMA) acceptability among patients with schizophrenia spectrum disorders (SSD), which is of major relevance during the e-Mental health-focused COVID-19 pandemic.
ObjectivesTo investigate i) the levels of adherence to a passive smartphone-based EMA tool, the Evidence-Based Behavior (eB2), among SSD patients; and ii) putative predictors of this.
MethodsSample: SSD (F20-29-ICD10) outpatients, age 18-64, without financial incentives, recruited over 17/06/2019-11/03/2020 at the Hospital Universitario Fundación Jiménez Díaz (Madrid, Spain). Those who accepted the eB2 installation -users- and those who did not -non-users- were compared in sociodemographic, clinical, premorbid adjustment, neurocognitive, psychopathological, insight and metacognitive variables by a multivariable binary logistic regression model.
ResultsSample (N=77): n=41 males; age: 47.69±9.76 years, n=24 users (31.2%). n=14 users (70%) had the eB2 installed at follow-up (median=14.50 weeks).
Multivariable binary logistic regression model on ‘user’ as outcome β SE Wald p OR 95% CI Age -0.075 0.038 3.910 0.048 0.928 0.861-0.999 Education level -0.967 1.289 0.563 0.453 0.380 0.030-4.755 Early adolescence premorbid adjustment -0.285 0.110 6.695 0.010 0.752 0.606-0.933 Trail Making Test A -0.030 0.025 1.488 0.222 0.970 0.924-1.018 Trail Making Test B -0.005 0.010 0.278 0.598 0.995 0.976-1.014 Cognitive Insight 0.062 0.061 1.043 0.307 1.064 0.944-1.200 X2=25.296,df=6,p<0.001. Nagelkerke-R2=44.7%. Correctly classified: 76.9%, users:54.5%, non-users:88.4%.
ConclusionsAcceptability of a smartphone-based EMA application among SSD patients was low. Age (young) and good premorbid adjustment predicted acceptability. e-Mental Health methods need to be tailored for patients with SSD. Otherwise, these highly vulnerable individuals may be neglected by e-health-based services in the post-COVID-19 years ahead.
Schizoaffective disorder: Nosological controversies and absence of specific treatment guidelines
- M. Valtueña García, R. Combina Fescina, A. Vázquez González, C. Ludwig, A. González Suarez, J. López Fernández, C. Huergo Lora, S. Ocio León, L. Lago García
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S540
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizoaffective disorder is a psychotic disorder of controversial nosological entity. Affective symptomatology and psychotic features of varying intensity coexist simultaneously in him throughout evolution. The lack of consensus on the existence of this entity determines its diagnostic delay and the absence of specific treatment guidelines.
ObjectivesTo review the diagnostic criteria for schizoaffective disorder and the published scientific evidence on the efficacy and safety of the different therapeutic options available. To analyze the efficacy of a multidisciplinary treatment plan implemented in an intensive follow-up program, presenting the evolution of a clinical case.
MethodsTo review the psychiatric history and psychopathological evolution of a patient diagnosed with schizoaffective disorder from the beginning of an intensive follow-up program in a day center to the present. Review the existing scientific evidence on the usefulness of the treatments used in this nosological entity.
ResultsThis is a longitudinal and retrospective study of a clinical case in which the areas for improvement are analyzed before implementing a multidisciplinary therapeutic program and the favorable results obtained today. Currently, the patient is euthymic and attenuated and chronic positive and negative symptoms persist that do not interfere with his functionality.
ConclusionsFrom the implementation of an individualized, personalized and multidisciplinary maintenance treatment plan, an overall improvement in psychopathological stability and functional recovery is observed. Among the psychopharmacological options in this patient, Paliperidone Long Acting Injection (PLAI) stands out for its long-term efficacy and safety.
Assessment of hospitalizations in schizophrenia patients treated with paliperidone 1-monthly (PP1M), paliperidone 3-monthly (PP3M), aripiprazole once-monthly (AOM) and other oral antipsychotics (OAP) in clinical practice
- L. Gutiérrez Rojas, S. Sánchez Alonso, M. García Dorado, P. Lopez
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S539
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It has been shown that long-acting treatments can significantly improve adherence, control symptom, and reduce the risk of relapse compared to oral drugs. However, limited real world evidence is available as to whether there are differences among the various formulations marketed.
ObjectivesThis study aims to assess the impact on several prognosis variables of PP1M,PP3M,AOM and OAP drugs.
MethodsAll adults (≥18 years) with schizophrenia who were initiated on PP1M, PP3M, AOM, or OAP treatment (chlorpromazine,levomepromazine,fluphenazine,haloperidol,ziprasidone,zuclopenthixol,olanzapine,quetiapine,asenapine,amisulpride, risperidone,aripiprazole,paliperidone) between 2017 and 2018 were identified in IQVIA’s database(1.8M of inhabitants from 4 Spanish areas). The rate of hospitalizations, emergency room visits, and treatment persistence was calculated using the Kaplan-Meier method. Survival curves were compared using the log-rank test (Sidak-adjustment),and Cox´s Hazard Ratios (HR) were used for the comparison between groups.
ResultsData from 2275 patients were analyzed (PP1M= 387;PP3M=490;AOM=75;OAP=1323).The mean age of patients was 46.8(14.95) years, and 62.9% were male. The hospitalization rate at 12 months was significantly lower (p<0.01) for PP3M (8.3%) than for AOM (21.2%), PP1M (22.1%),and OAP (29.4%).When compared with PP3M use, the HRs were 2.17 for PP1M, 2.22 for AOM,and 2.90 for OAP. Emergency room visits rate at 12 months was also significantly lower (p<0. 01) for PP3M (23%) than for PP1M (36.9%), OAP (43.5%),and AOM (46.2%). Persistence rates were higher for PP3M (91%) than for any other treatment (p<0.01).
ConclusionsOur results outline that patients treated with PP3M experienced fewer relapses and decompensations compared to all other treatments analyzed, which might help improve the prognosis and quality of life of patients.
Conflict of interestThis study was sponsored by Janssen. M. García and P. López are employees of Janssen.
Relationship between suicide attempts of repetition and dependence to the cocaine: Report of clinical case
- M. Valtueña García, L. Lago García, R. Combina Fescina, A. Vázquez González, C. Ludwig, A. González Suarez, J. López Fernández, C. Huergo Lora, S. Ocio León, R. Arias Martino
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S645-S646
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
People with borderline personality disorder are at higher risk of repeating suicidal behavior. At the same time, numerous publications have demonstrated the relationship between cocaine dependence and suicide attempts of repetition.
ObjectivesReview the relationship between cocaine addiction, borderline personality disorder and repeated suicide attempts. Present through a clinical case the effectiveness of a comprehensive and multidisciplinary therapeutic plan with different mental health devices.
MethodsTo review the psychopathological evolution of a patient with a diagnosis of borderline personality disorder; dependence to the cocaine; Harmful alcohol consumption and suicidal behavior from the beginning of follow-up in mental health services to the present. Review the existing scientific evidence on the relationship between cocaine addiction and repeated suicide attempts. Analyze the eficacy of the different treatments available.
ResultsThis is a longitudinal and retrospective study of the psychiatric history and evolution of a clinical case since the implementation of an individualized therapeutic program and the favorable results obtained. Intensive outpatient follow-up was carried out for high suicide risk and hospitalization in a psychiatric hospitalization unit, day care centre and therapeutic community.
ConclusionsAt present, the patient remains in abstinence with remission of suicidal ideation. The literature has shown the usefulness of intensive mental health follow-up programs to achieve remission of suicidal ideation and maintain abstinence from illegal substances.
DisclosureNo significant relationships.
Examining the independent and joint effects of genomic and exposomic liabilities for schizophrenia across the psychosis spectrum
- L.-K. Pries, G. A. Dal Ferro, J. van Os, P. Delespaul, G. Kenis, B. D. Lin, J. J. Luykx, A. L. Richards, B. Akdede, T. Binbay, V. Altınyazar, B. Yalınçetin, G. Gümüş-Akay, B. Cihan, H. Soygür, H. Ulaş, E. Şahin Cankurtaran, S. Ulusoy Kaymak, M. M. Mihaljevic, S. Andric Petrovic, T. Mirjanic, M. Bernardo, G. Mezquida, S. Amoretti, J. Bobes, P. A. Saiz, M. Paz García-Portilla, J. Sanjuan, E. J. Aguilar, J. L. Santos, E. Jiménez-López, M. Arrojo, A. Carracedo, G. López, J. González-Peñas, M. Parellada, N. P. Maric, C. Atbaşoğlu, A. Ucok, K. Alptekin, M. Can Saka, Genetic Risk and Outcome of Psychosis (GROUP) investigators, C. Arango, M. O'Donovan, S. Tosato, B. P. F. Rutten, S. Guloksuz
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 29 / 2020
- Published online by Cambridge University Press:
- 17 November 2020, e182
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Psychosis spectrum disorder has a complex pathoetiology characterised by interacting environmental and genetic vulnerabilities. The present study aims to investigate the role of gene–environment interaction using aggregate scores of genetic (polygenic risk score for schizophrenia (PRS-SCZ)) and environment liability for schizophrenia (exposome score for schizophrenia (ES-SCZ)) across the psychosis continuum.
MethodsThe sample consisted of 1699 patients, 1753 unaffected siblings, and 1542 healthy comparison participants. The Structured Interview for Schizotypy-Revised (SIS-R) was administered to analyse scores of total, positive, and negative schizotypy in siblings and healthy comparison participants. The PRS-SCZ was trained using the Psychiatric Genomics Consortiums results and the ES-SCZ was calculated guided by the approach validated in a previous report in the current data set. Regression models were applied to test the independent and joint effects of PRS-SCZ and ES-SCZ (adjusted for age, sex, and ancestry using 10 principal components).
ResultsBoth genetic and environmental vulnerability were associated with case-control status. Furthermore, there was evidence for additive interaction between binary modes of PRS-SCZ and ES-SCZ (above 75% of the control distribution) increasing the odds for schizophrenia spectrum diagnosis (relative excess risk due to interaction = 6.79, [95% confidential interval (CI) 3.32, 10.26], p < 0.001). Sensitivity analyses using continuous PRS-SCZ and ES-SCZ confirmed gene–environment interaction (relative excess risk due to interaction = 1.80 [95% CI 1.01, 3.32], p = 0.004). In siblings and healthy comparison participants, PRS-SCZ and ES-SCZ were associated with all SIS-R dimensions and evidence was found for an interaction between PRS-SCZ and ES-SCZ on the total (B = 0.006 [95% CI 0.003, 0.009], p < 0.001), positive (B = 0.006 [95% CI, 0.002, 0.009], p = 0.002), and negative (B = 0.006, [95% CI 0.004, 0.009], p < 0.001) schizotypy dimensions.
ConclusionsThe interplay between exposome load and schizophrenia genetic liability contributing to psychosis across the spectrum of expression provide further empirical support to the notion of aetiological continuity underlying an extended psychosis phenotype.
Can metacognitive interventions improve insight in schizophrenia spectrum disorders? A systematic review and meta-analysis
- Javier-David Lopez-Morinigo, Olesya Ajnakina, Adela Sánchez-Escribano Martínez, Paula-Jhoana Escobedo-Aedo, Verónica González Ruiz-Ruano, Sergio Sánchez-Alonso, Laura Mata-Iturralde, Laura Muñoz-Lorenzo, Susana Ochoa, Enrique Baca-García, Anthony S David
-
- Journal:
- Psychological Medicine / Volume 50 / Issue 14 / October 2020
- Published online by Cambridge University Press:
- 14 October 2020, pp. 2289-2301
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Patients with schizophrenia spectrum disorders (SSD) tend to lack insight, which is linked to poor outcomes. The effect size of previous treatments on insight changes in SSD has been small. Metacognitive interventions may improve insight in SSD, although this remains unproved.
MethodsWe carried out a systematic review and meta-analysis of randomized controlled trials (RCTs) to examine the effects of metacognitive interventions designed for SSD, namely Metacognitive Training (MCT) and Metacognitive Reflection and Insight Therapy (MERIT), on changes in cognitive and clinical insight at post-treatment and at follow-up.
ResultsTwelve RCTs, including 10 MCT RCTs (n = 717 participants) and two MERIT trials (n = 90), were selected, totalling N = 807 participants. Regarding cognitive insight six RCTs (n = 443) highlighted a medium effect of MCT on self-reflectiveness at post-treatment, d = 0.46, p < 0.01, and at follow-up, d = 0.30, p < 0.01. There was a small effect of MCT on self-certainty at post-treatment, d = −0.23, p = 0.03, but not at follow-up. MCT was superior to controls on an overall Composite Index of cognitive insight at post-treatment, d = 1.11, p < 0.01, and at follow-up, d = 0.86, p = 0.03, although we found evidence of heterogeneity. Of five MCT trials on clinical insight (n = 244 participants), which could not be meta-analysed, four of them favoured MCT compared v. control. The two MERIT trials reported conflicting results.
ConclusionsMetacognitive interventions, particularly Metacognitive Training, appear to improve insight in patients with SSD, especially cognitive insight shortly after treatment. Further long-term RCTs are needed to establish whether these metacognitive interventions-related insight changes are sustained over a longer time period and result in better outcomes.
A replication study of JTC bias, genetic liability for psychosis and delusional ideation
- Cécile Henquet, Jim van Os, Lotta K. Pries, Christian Rauschenberg, Philippe Delespaul, Gunter Kenis, Jurjen J. Luykx, Bochao D. Lin, Alexander L. Richards, Berna Akdede, Tolga Binbay, Vesile Altınyazar, Berna Yalınçetin, Güvem Gümüş-Akay, Burçin Cihan, Haldun Soygür, Halis Ulaş, Eylem S. Cankurtaran, Semra U. Kaymak, Marina M. Mihaljevic, Sanja S. Petrovic, Tijana Mirjanic, Miguel Bernardo, Gisela Mezquida, Silvia Amoretti, Julio Bobes, Pilar A. Saiz, Maria P. García-Portilla, Julio Sanjuan, Eduardo J. Aguilar, Jose L. Santos, Estela Jiménez-López, Manuel Arrojo, Angel Carracedo, Gonzalo López, Javier González-Peñas, Mara Parellada, Nadja P. Maric, Cem Atbaşoğlu, Alp Ucok, Köksal Alptekin, Meram C. Saka, Celso Arango, Michael O'Donovan, Bart P.F. Rutten, Sinan Gülöksüz
-
- Journal:
- Psychological Medicine / Volume 52 / Issue 9 / July 2022
- Published online by Cambridge University Press:
- 13 October 2020, pp. 1777-1783
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
This study attempted to replicate whether a bias in probabilistic reasoning, or ‘jumping to conclusions’(JTC) bias is associated with being a sibling of a patient with schizophrenia spectrum disorder; and if so, whether this association is contingent on subthreshold delusional ideation.
MethodsData were derived from the EUGEI project, a 25-centre, 15-country effort to study psychosis spectrum disorder. The current analyses included 1261 patients with schizophrenia spectrum disorder, 1282 siblings of patients and 1525 healthy comparison subjects, recruited in Spain (five centres), Turkey (three centres) and Serbia (one centre). The beads task was used to assess JTC bias. Lifetime experience of delusional ideation and hallucinatory experiences was assessed using the Community Assessment of Psychic Experiences. General cognitive abilities were taken into account in the analyses.
ResultsJTC bias was positively associated not only with patient status but also with sibling status [adjusted relative risk (aRR) ratio : 4.23 CI 95% 3.46–5.17 for siblings and aRR: 5.07 CI 95% 4.13–6.23 for patients]. The association between JTC bias and sibling status was stronger in those with higher levels of delusional ideation (aRR interaction in siblings: 3.77 CI 95% 1.67–8.51, and in patients: 2.15 CI 95% 0.94–4.92). The association between JTC bias and sibling status was not stronger in those with higher levels of hallucinatory experiences.
ConclusionsThese findings replicate earlier findings that JTC bias is associated with familial liability for psychosis and that this is contingent on the degree of delusional ideation but not hallucinations.
P01-369 - Prevalence and Predictor Factors of Neuropsychiatric Symptoms in Institutionalized Patients Diagnosed with Dementia
- A. Robles Castiñeiras, S. Reinoso Hermida, G. Díaz Grávalos, A. López González, A. García Caballero
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E577
-
- Article
-
- You have access Access
- Export citation
-
Objective
To estimate the prevalence and severity of neuropsychiatric symptoms in patients with dementia in nursing homes, assessing their association with certain factors that may promote or prevent its occurrence.
MethodsA cross-sectional study was carried out. We included all elderly diagnosed with degenerative, vascular, or mixed dementia, stage 4 to 7 of the GDS, and residents in 6 nursing homes in the province of Ourense (Spain). The assessment of symptoms was performed using the Neuropsychiatric Inventory - Nursing Home (NPI-NH) test. A sample size of 120 individuals was determined to be necessary.
ResultsWe included 212 cases, with an average age of 85.7 (SD = 6.7) years. The prevalence of neuropsychiatric symptoms was 84.4%. The most common symptom was apathy, followed by agitation and delirium, the least frequent were euphoria and hallucinations. The symptom that produced most occupational disruption was agitation. Multivariate analysis showed that a higher score on the NPI-NH was associated with the use of neuroleptics, both typical and atypical, and with a higher score on the Reisberg Scale. Negative association was demonstrated with the number of days of institutionalization and the diagnosis of vascular dementia.
ConclusionsPatients with dementia in nursing homes in our area have a high frequency of neuropsychiatric symptoms that are associated with neuroleptic use and decreases as the patient remains institutionalized for longer. Patients diagnosed with vascular dementia have lower scores on the NPI-NH test.





