421 results
The Portuguese version of the Screen for Disordered Eating: Validity and reliability in the perinatal period
- A. T. Pereira, R. Lima, J. M. Pinto, D. Pereira, A. Macedo, C. Marques, A. I. Araújo, B. Barbosa, C. Pinto Gouveia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S308-S309
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Despite the increased knowledge about the prevalence and consequences of eating disorders (ED), they continue to be underdiagnosed and undertreated. Being more common in women of childbearing age, the perinatal period may play a decisive role in the incidence and course of these pathologies. The Screen for Disordered Eating (SDE) was developed for the screen of ED in primary care.
ObjectivesOur aim was to analyze the psychometric properties of the Portuguese Version of SDE in women during the perinatal period.
MethodsParticipants were 346 women with a mean age of 31.68 of years old (± 4.061; range: 18-42). 160 were pregnant (second or third trimester) and 186 were in the post-partum (mean baby´s age=4.37 months (± 2.87; range: 1-12). They answered an online survey including the Portuguese version of the SDE and of the Eating Disorder Examination – Questionnaire (EDE-Q-7).
ResultsConfirmatory Factor Analysis showed that the unidimensional model presented good fit indexes in pregnancy (), post-partum () and considering both – perinatal period (χ2/df=2.0335; RMSEA=.0547, p<.001; CFI=0.9976 TLI=0.9939, GFI=0.9906). The Cronbach’s alfa were ≥ 0.65. All the items contributed to the internal consistency and presented high internal validity. Pearson correlations between SDE and EDE-Q-7 total scores were significant (p<.001) positive and high in pregnancy (.639), postpartum (.583) and the perinatal period (.617).
ConclusionsThe Portuguese version of SDE has shown good validity (construct and concurrent) and internal consistency. As such, SDE might be a useful tool to screen ED in women during the perinatal period.
Disclosure of InterestNone Declared
The Portuguese short version of the Eating Disorder Examination Questionnaire: Validity and Reliability in men across multiple ages
- A. Silva, A. Macedo, C. Marques, M. J. Brito, A. T. Pereira, C. Coelho
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S563
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Eating Disorder Examination Questionnaire short version (EDE-Q7) presented better psychometric properties than the Fairburn’s 28-items original version, not only in girls (Machado et al. 2018), but also in older women (Pereira et al. 2021; Pereira et al. 2022). It comprises 7 items in three subscales: Dietary Restraint/DR; Shape and Weight Overvaluation/SWO and Body Dissatisfaction/BD. In a more recent clinical study in men (Laskowski et al. 2023) the factors associated with body concerns and dissatisfaction weren’t fully represented in the questionnaire, possibly indicating differences in body ideals, specially relating to musculature.
ObjectivesWe aimed to analyze the psychometric properties of the Portuguese version of EDE-Q7 in males.
MethodsParticipants were 227 male individuals with a mean age of 30.41 years (±13.96; range: 14-73 years). They answered an online survey including the Portuguese versions of the Screen for Disordered Eating/SDE; the Body Image Concern Inventory/BICI and the Muscle Dysmorphia subscale of the Eating Disorder Assessment for Men/DM-EDAM.
ResultsConfirmatory Factor Analysis showed that the second order model presented good fit (χ2/df=2.437; RMSEA=.0794; CFI=.986 TLI=.974, GFI=.967). Cronbach’s alpha was .856 for the total, .876 for DR and .917 for SWO and .900 for BD. All items contributed to internal consistency and presented high internal validity. Pearson’s correlations of EDE-Q7 with BICI (.465), DM-EDAM (.384) and SDE (.361) were significant (p<.001) and moderate.
ConclusionsAlso in men, the Portuguese version of EDE-Q7 demonstrates good validity (construct and convergent) and reliability.
Disclosure of InterestNone Declared
Between Delusions and Borders: Diagnosing Delusional Disorder in Migratory Contexts
- L. M. Carrasqueira, M. D. Pereira, I. Marques, M. Silva, C. Laureano
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S613
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The mental health of immigrants is a significant, yet often overlooked, aspect of public health. This case study highlights the intersection of migration and mental health, focusing on a patient with delusional disorder. It is particularly relevant for psychiatrists due to the unique challenges in diagnosing and treating mental health conditions in migrant populations, who often face cultural, linguistic, and systemic barriers in accessing care.
ObjectivesThe primary objective of this case study is to elucidate the diagnostic and clinical challenges encountered in managing delusional disorder in a migrant patient. The case study presented aims to provide insights into how delusional beliefs can precipitate and perpetuate the process of migration.
MethodsThe case study was developed through comprehensive psychiatric interviews during the patient’s stay in a Psychiatric Inpatient Unit, supplemented by a targeted literature review on PubMed using “delusion disorder” and “immigration” as keywords.
ResultsThe patient, a 44-year-old Indian male, was a functional young adult until 2007 when he began exhibiting symptoms of delusional disorder. His delusions progressively evolved from local scenarios to national and eventually to a global scale. The initial delusions were focused on personal and professional conspiracies within his home country, leading to his first internal migration. As the condition worsened, his delusions expanded, fueling a belief in a widespread conspiracy that transcended national borders. This escalation of delusional beliefs became the primary motivation for the patient’s international migration. He changed countries four times, each move driven by an attempt to escape the perceived threats and conspiracies associated with his delusional disorder. The patient’s journey through various countries was a direct result of the intensifying nature of his condition.
ConclusionsThis case study accentuates the profound impact that a delusional disorder can have as a driver and catalyst of international migration, influencing the individual’s decision-making process and shaping the migratory experiences. It emphasizes the necessity for psychiatrists to consider the unique socio-cultural contexts of migrant patients in diagnosis and treatment. The case study advocates for a comprehensive treatment approach, integrating psychiatric care with a nuanced understanding of the migrant’s experiences and challenges. This multifaceted approach is crucial in addressing the complex needs of patients with delusional disorder in migrant populations.
Disclosure of InterestNone Declared
Clinical Insights into Antipsychotics and Rifampicin Interaction: A Case Report
- P. Abreu, C. Ferreira dos Santos, M. Pereira, M. Vieira Lisboa, M. Cameira, M. Rebelo Soares
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S700-S701
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Antipsychotics are the primary class of drugs used to manage schizophrenia. These medications help control and reduce the severity of these symptoms, allowing individuals with schizophrenia to better function. On the other hand, rifampicin, used as treatment for tuberculosis, is a powerful inducer of several drug-metabolizing enzymes which have the potential to decrease the plasma levels of antipsychotics. Therefore, the presence of multiple pharmacokinetic interactions can alter how antipsychotics are metabolized, leading to a notable clinical impact when these medications are administered concurrently.
ObjectivesThe objective is to share valuable clinical experiences and insights to aid healthcare providers in making informed decisions when faced with the challenge of co-administering antipsychotics with rifampicin, ultimately ensuring the safety and efficacy of treatment for their patients.
MethodsIt will be discussed a case of a 41-year-old woman with the diagnosis of schizophrenia under treatment with paliperidone palmitate and clozapine who had a sudden relapse after starting treatment for latent tuberculosis with rifampicin as a framework for a literature review based off Pubmed.
ResultsThe antituberculosis drug rifampicin induces drug-metabolizing enzymes in the liver, having the greatest effects on the expression of cytochrome P450 (CYP3A4) and therefore can lead to a decrease in the plasma levels of antipsychotic medications that also rely on these pathways for clearance. In this particular case, although specific data on clozapine and paliperidone concentrations were not reported, fluctuations in symptomatology following rifampicin introduction were probably explained by an inducing effect of this drug on their metabolism. So, when initiating rifampicin treatment and when discontinuing it, clinicians should carefully assess the dosages of any concomitant medications that may potentially interact with rifampicin. To ensure effective therapy during rifampicin treatment, it is crucial to monitor both the patient’s clinical response and their blood drug concentrations, making dosage adjustments as necessary.
ConclusionsThis case report offers valuable guidance to clinicians on safely and effectively managing drug interactions between antipsychotic medications and rifampicin, ensuring the well-being of their patients during treatment. The co-administration of these medications lacks robust clinical evidence, and notably, there is insufficient data regarding its impact on plasma antipsychotic levels, a crucial factor in determining clinical effectiveness.
Disclosure of InterestNone Declared
Prevalence of psychiatric disorders in patients with craniofacial malformations - a statistical analysis
- G. Pereira Bernd, V. Dall Agnol Bouvier, T. Brusa da Costa Linn, I. Cho de Almeida, B. de Oliveira de Marchi, L. Guinter Muccillo, C. G. Menezes Chaves Barcellos, C. Paz Portinho, M. V. Martins Collares
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S483-S484
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Craniofacial malformations have long been associated with a heightened risk of psychiatric disorders. Understanding this link is crucial, as it can inform early intervention and support for affected individuals, enhancing their overall well-being. Research in this area aims to shed light on the prevalence and nature of these disorders within the craniofacial population, ultimately improving healthcare and quality of life for affected individuals.
ObjectivesThis study aims to establish a comprehensive understanding of the relationship between craniofacial malformations and psychiatric disorders. Specifically, our objectives include: assessing prevalence, identifying risk factors, evaluating impact and informing clinical practice. This research aims to improve the holistic care and mental well-being of individuals with craniofacial malformations, contributing to a more comprehensive approach in the field of psychiatry.
MethodsThis cross-sectional study was conducted at a prominent referral hospital named Hospital de Clínicas de Porto Alegre during the month of August 2023.
Participant Selection: Patients with craniofacial malformations of all ages and both genders.
Data Collection: We conducted structured interviews with participants to gather demographic information, medical history, and details of their craniofacial conditions.
Medical Records Review: Medical records were reviewed to corroborate craniofacial diagnoses and identify any comorbid conditions.
Statistical Analysis: Data were analyzed using appropriate statistical techniques to assess the association between craniofacial malformations and psychiatric disorders.
Ethical Considerations: The study adhered to all ethical guidelines, with informed consent obtained from participants or their legal guardians. Ethical approval was obtained from the hospital’s Institutional Review Board.
Data Handling: Confidentiality and data security were ensured throughout the study, with all data anonymized to protect participant privacy.
ResultsIn our study, we assessed 132 different patients, comprising 62 females and 70 males. The youngest patient was 2 months old, while the oldest was 56 years old. The mean age of the patients was 16.22 years, with a median of 9 years, a harmonic mean of 18 years, and a standard deviation of 15.23 years.
Among the patients, 24 exhibited psychiatric disorders, evenly split between 12 males and 12 females. Their average age was 16.21 years, with a median of 10 years, a harmonic mean of 6.13, and a standard deviation of 14.57. The youngest patient with evidence of a psychiatric disorder was 2 years old.
Image:
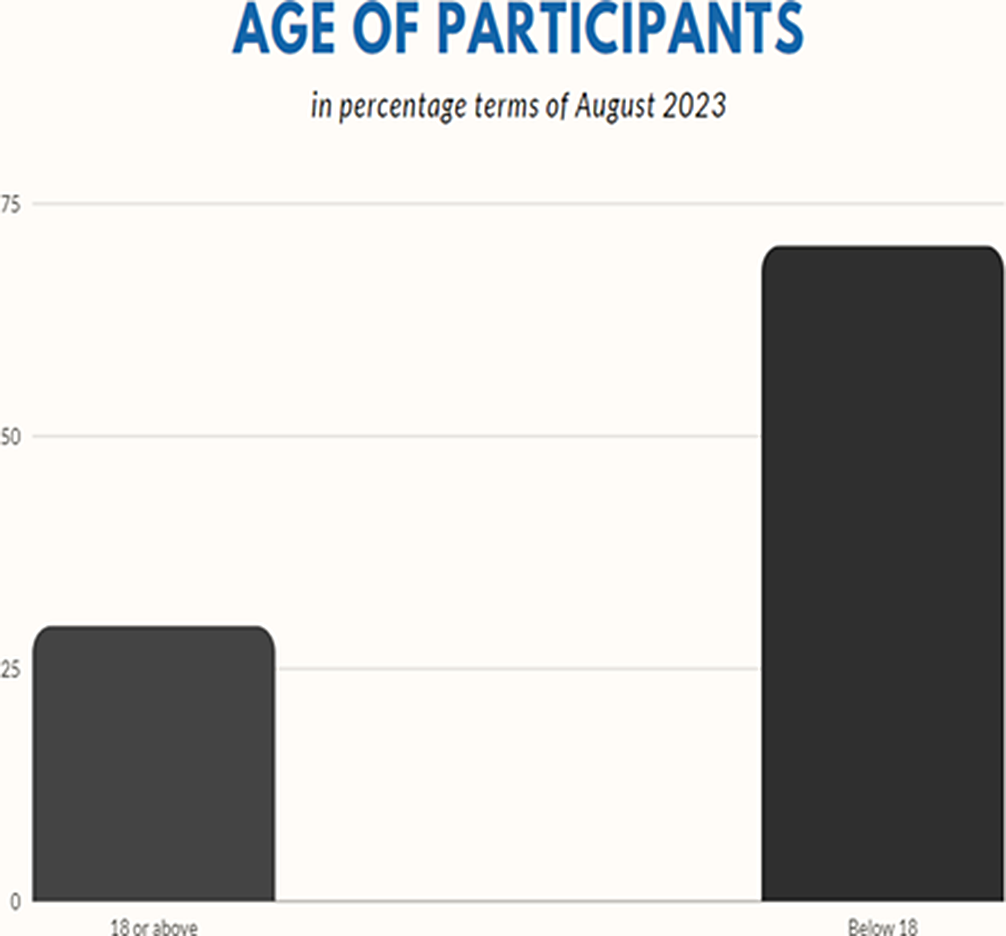
Image 2:
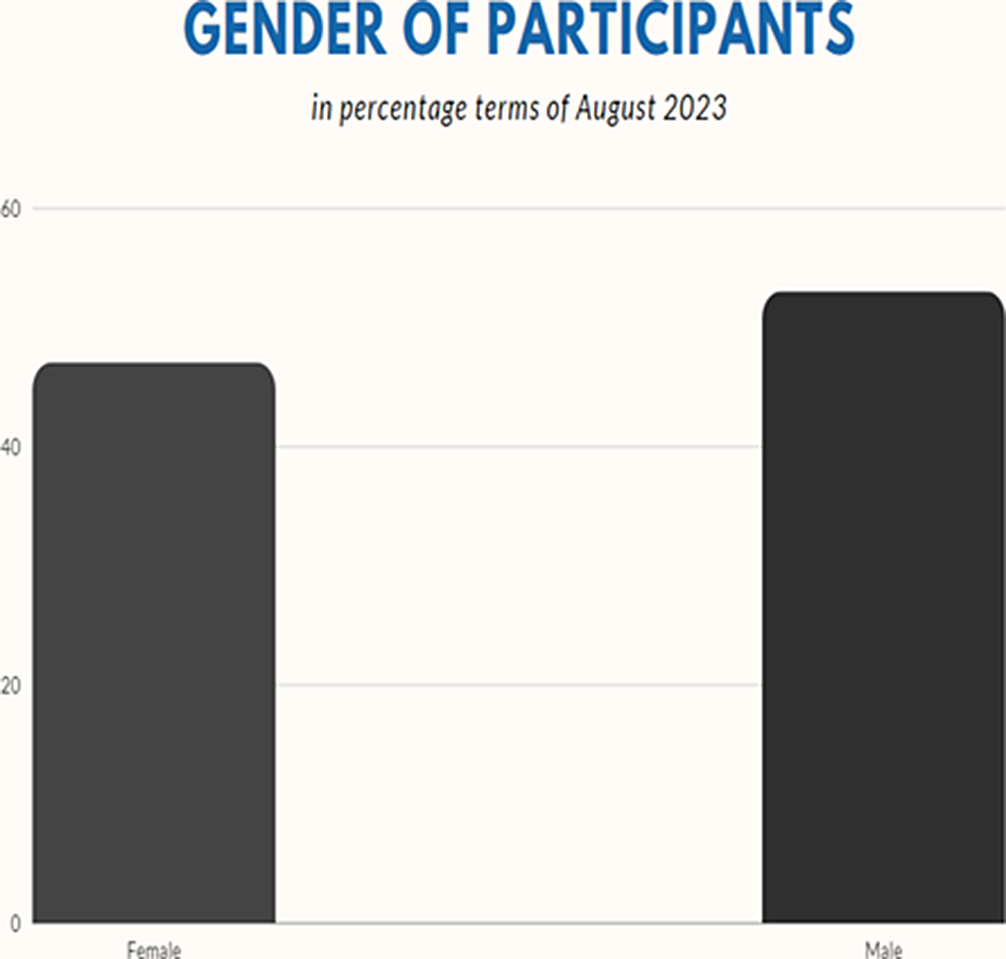 Conclusions
ConclusionsOur study underscores the prevalence of psychiatric disorders among craniofacial patients, which seems to be greater than the general population, emphasizing the need for integrated care that considers both medical and psychological aspects, thus enhancing the overall well-being of these individuals.
Disclosure of InterestNone Declared
Our old friend lithium and encephalopathy: a case report
- M. P. Cameira, C. F. dos Santos, M. Pereira, M. V. Lisboa, M. R. Soares, P. Abreu
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S432-S433
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium is a well-established mood stabilizer used in the management of bipolar disorder, that is generally well-tolerated; however, it is associated with rare but potentially severe neurological side effects. Lithium-induced encephalopathy is characterized by a spectrum of symptoms, ranging from subtle cognitive deficits to severe manifestations such as altered mental status to overt delirium, seizures and coma. Risk factors include advanced age, concomitant medication and underlying renal impairment. This symptoms do not consistentely correlate with lithium concentrations.
ObjectivesThis abstract aims to provide an overview of the clinical characteristics, underlying mechanisms, and management of lithium-induced encephalopathy.
MethodsWe discuss a case of a 62-years-old woman diagnosed with bipolar disorder under treatment with lithium and olanzapine, without recent changes of posology. She presented to emergency department with subacute and fluctuating neuropsychiatric symptoms, including confusion, disorientation in time and space, complex visual hallucinations, delusional ideas, alteration in memory and logic thinking, dysarthria and dyspraxia. Neuroimaging showed no structural abnormalities, blood tests were normal and serum lithium levels were within the therapeutic range (0.8 mEq/L). Upon discontinuation of lithium, the patient exhibited a gradual resolution of symptoms. We conducted a comprehensive search of medical databases, including PubMed, to identify relevant articles related to lithium encephalopathy published up to September 2023.
ResultsThis case challenges the conventionally established threshold of elevated serum lithium levels in the development of encephalopathy. The underlying pathophysiology is complex and multifactorial, with proposed mechanisms including alterations in neurotransmitter balance, oxidative stress, mitochondrial dysfunction and individual susceptibility to idiosyncratic reactions. Early diagnosis is challenging, necessitating a high clinical suspicion, neuroimaging and exclusion of other etiologies. Management strategies involve discontinuation of lithium, even when serum lithium levels are within the therapeutic range, supportive care, and, in severe cases, hemodialysis to reduce lithium levels rapidly.
ConclusionsClinicians should maintain a high index of suspicion of lithium-induced encephalopathy, especially in patients presenting with neurological symptoms while on lithium treatment. Early recognition and intervention are essential for minimizing morbidity and preventing potentially irreversible neurological damage. Further research is needed to better understand the precise mechanisms underlying it, risk factors and to refine treatment strategies.
Disclosure of InterestNone Declared
Validity and reliability of the Eating Disorder Examination-Questionnaire-7 Portuguese version in the perinatal period
- A. T. Pereira, R. Lima, D. Pereira, J. M. Pinto, B. Barbosa, A. I. Araújo, C. Marques, A. Macedo, C. Pinto Gouveia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S110
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The EDE-Q-7 Portuguese version presented good reliability and validity in Portuguese women fro the general population (Pereira et al. 2022).
ObjectivesThe aim of our study was to analyse the psychometric properties of the EDE-Q-7 in a sample of Portuguese women during the perinatal period.
MethodsParticipants were 346 women with a mean age of 31.68 of years old (± 4.061; range: 18-42). 160 were pregnant (second or third trimester) and 186 were in the post-partum (mean baby´s age=4.37 months (± 2.87; range: 1-12). They answered an online survey including the Portuguese version of the EDE-Q-7 and of the Screen for Disordered Eating/SDE.
ResultsConfirmatory factor analysis (CFA) presented adequate fit, in pregnancy (χ2/df=; RMSEA=, p<.001; CFI=; TLI=; GFI=), postpartum (χ2/df=; RMSEA=, p<.001; CFI=; TLI=; GFI=) and considering both – perinatal period (χ2/df=2.7998; RMSEA=.0722, p<.001; CFI=.9709; TLI=.9444; GFI=.9761). The Cronbach’s alpha coefficients were >0.90 for the total and approximately .70 for the three factors - Dietary restraint, Shape/weight overvaluation and Body dissatisfaction. All the items contributed to the internal consistency and presented high internal consistency. Pearson correlations between factors and total scores were significant, positive and high, as well as between the EDE-Q-7 measures and SDE (>.60 with the total; >.40 with the factors), in pregnancy, postpartum and considering both periods.
ConclusionsPresented sound psychometric properties across the perinatal period, the EDE-Q-7 and can be very useful to evaluate the presence and severity of eating disorders symptoms in women in pregnancy and post-partum.
Disclosure of InterestNone Declared
Muscle dysmorphia subscale of eating disorder assessment for men: validity and reliability of the Portuguese version in men across multiple ages
- A. Silva, A. Macedo, M. J. Brito, C. Marques, A. T. Pereira, M. Bajouco
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S563-S564
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Although symptom presentation varies by gender, almost all eating disorder/ED instruments have been developed and validated on females. The Eating Disorder Assessment for Men (EDAM; Stanford & Lemberg 2012) is a male specific self-report measure, composed of four sub-scales, proved to be useful to assess gender differences in ED presentations (Nagata et al. 2021). The MD comprises 5 items about the overwhelming concern with muscularity and the false perception of having an underdeveloped body.
ObjectivesHaving already valid measures of body image and eating behaviors in men, we now aim to analyze the psychometric properties of the Portuguese version of MD, in order to have a quick and rigorous measure of this specific construct.
MethodsParticipants were 227 male individuals (mean age=30.41 years±13.96; range: 14-73 years). They answered an online survey including the preliminary DM and the Portuguese validated versions of the Eating Disorder Examination Questionnaire (EDE-Q7) and the Body Image Concern Inventory (BICI).
ResultsConfirmatory Factor Analysis showed that the unidimensional model presented good fit indexes (χ2/df=.6829; RMSEA=.0000; CFI=1.00 TLI=1.01, GFI=.995). Cronbach’s alfa was .891; all the items contributed to the internal consistency and had high internal validity. Pearson correlations of DM with EDE-Q7 and BICI were significant (p<.001) and moderate-high, respectively,.384 and .522.
ConclusionsThe Portuguese preliminary version of DM-EDAM demonstrated validity (construct and convergent) and reliability. can be used for clinical and research purposes, namely in an ongoing project we have in progress, about body image, disordered eating, gender and age.
Disclosure of InterestNone Declared
Understanding the Occurrence of Psychiatric Disorders in Epilepsy in Brazil: An Epidemiological Investigation
- L. Bardini Goulart, A. Roloff Krüger, G. Moreno Xavier, G. Fiorio Grando, J. Michelon, L. F. Alves Nascimento, J. Adames, A. T. Konzen, G. Pereira Bernd, C. Fontes Augusto, H. Wolmeister, I. Fachinetto Thoen, Y. de França, P. H. Filipin Von Muhlen, F. J. Carvalho da Costa, V. Kayser, P. H. Paesi Dutra, R. Rahal de Albuquerque, T. Garcia Furtado, G. Macelaro, A. C. Castelo, H. Vieira Rodrigues, E. Rockenbach Fidélis, D. Crusius, E. Guidugli, M. F. Valentim de Paula, Y. Marques Loureiro, E. Paiva Borsa, L. de Paula e Souza, G. Ferreira Cruz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S98
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Epilepsy is one of the most common serious brain illness, with symptoms influenced by multiple risk factors and a strong genetic predisposition, rather than having a single expression and cause¹. Neuropsychiatric symptoms in epilepsy can encompass manifestations such as mood alterations, anxiety, sleep disturbances, psychosis, and behavioral disorders. While the motor and sensory manifestations of epileptic seizures are widely recognized, neuropsychiatric symptoms accompanying epilepsy are often underestimated. Therefore, it is essential to understand the most prevalent epidemiological profile of these patients to improve the diagnosis and management of these symptoms.
ObjectivesOur goal was to evaluate the neuropsychiatric behavior of epilepsy patients in Brazilian over the past 3 years through hospitalization data in order to outline an epidemiological and behavioral profile.
MethodsA cross-sectional, descriptive, retrospective, and quantitative study was conducted on hospitalizations of individuals simultaneously diagnosed with epilepsy, schizotypal and delusional disorders, and mood disorders in all five regions of Brazil (South, Southeast, Midwest, North, and Northeast) between February 2020 and December 2022. Data from January 2020 were not available. The data used were collected through the Department of Health Informatics of the Brazilian Unified Health System (DATASUS) in the “Hospital Information System of SUS” section, gathering information regarding the nature of care, age range, gender, and ethnicity of the patients.
ResultsThe analysis covers the years 2020 to 2022, totaling 503,045 hospitalizations. In 2022, the highest number of cases occurred (≈ 37.55%), followed by 2021 (≈ 33.62%) and 2020 (≈ 28.81%). Urgent hospitalizations represented ≈ 90.85% of the total. The most affected age group was 30 to 39 years old (≈ 18.30%). Men were more affected than women (≈ 52.03% and ≈ 47.96%, respectively), and Caucasians accounted for ≈ 36.07% of the hospitalizations. The average length of stay was 19.1 days, and the mortality rate was 1.4%.
ConclusionsThus, there is a gradual and annual increase in the number of hospitalizations during the observed period. While there is a minimal disparity between the affected genders, it is evident that the profile of male, caucasian, and adult patients is the most prevalent. Moreover, the predominantly urgent nature of hospitalizations points to an alarming scenario regarding this issue. From the analysis of the data obtained in the study, there is a clear need for interventions capable of reducing the prevalence of hospitalizations for neuropsychiatric symptoms in epilepsy patients in Brazil.
Disclosure of InterestNone Declared
Mental and Behavioral Disorders Associated with the Use of Psychoactive Substances and Alcohol: An Epidemiological Analysis in Southern Brazil
- L. Bardini, A. Roloff Krüger, G. Moreno Xavier, G. Fiorio Grando, J. Michelon, L. F. Alves Nascimento, J. Adames, A. T. Konzen, G. Pereira Bernd, C. Fontes Augusto, H. Wolmeister, I. Fachinetto Thoen, Y. de França, P. H. Filipin Von Muhlen, F. J. Carvalho da Costa, V. Kayser, P. H. Paesi Dutra, R. Rahal de Albuquerque, T. Garcia Furtado, G. Macelaro, A. C. Castelo, H. Vieira Rodrigues, E. Rockenbach Fidélis, D. Crusius, E. Guidugli, M. F. Valentim de Paula, Y. Marques Loureiro, E. Paiva Borsa, L. de Paula e Souza, G. Ferreira Cruz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Neuropsychiatric disorders are the leading cause of disability worldwide, as seen in cases such as depression, anxiety, bipolar mood disorder and schizophrenia, which can be developed or exacerbated by the use of psychoactive substances. Most mental disorders have an early onset, often leading to early and/or permanent disability, increasing the need and cost of healthcare. Therefore, it is necessary to improve the identification of the epidemiological profile of these cases in the South of Brazil in order to enhance the diagnosis and reduce the costs associated with managing these disorders.
ObjectivesThe present study aimed to analyze statistical data regarding hospitalizations related to mental disorders caused by the use of psychoactive substances and alcohol in the southern region of Brazil, highlighting the pathological scenario and identifying the most prevalent profiles of these disorders in this region.
MethodsA cross-sectional, descriptive, retrospective, and quantitative study was conducted on hospitalizations of individuals diagnosed with mental and behavioral disorders due to the use of psychoactive substances and alcohol in the states of the Southern region of Brazil (Paraná, Santa Catarina, and Rio Grande do Sul) between February 2020 and December 2022. Data of January 2020 were not available. The data used were collected through the Department of Health Informatics of the Brazilian Unified Health System (DATASUS) in the “Hospital Information System of SUS” section, gathering information regarding the nature of the care, age range, gender, and ethnicity of the patients.
ResultsThe study covers the years 2020 to 2022, indicating a total of 81,608 hospitalizations, with the year 2022 having the highest number of cases (≈ 37.13%), followed by 2021 (≈ 33.30%) and 2020 (≈ 29.55%). The states with the highest number of hospitalizations were Rio Grande do Sul (≈ 54.90%), Paraná (≈ 29.29%), and Santa Catarina (≈ 15.79%). Urgent hospitalizations accounted for ≈ 87.29% of the total. The most affected age group was 30 to 39 years old (≈ 25.61%). Men were more affected than women (≈ 81.70% and ≈ 18.28%, respectively). Caucasians accounted for ≈ 64.29% of the hospitalizations. The average length of stay was 20.8 days, and the mortality rate was 0.32%.
ConclusionsThere is a clear increase in the number of hospitalizations related to mental disorders caused by the use of psychoactive substances in the period from 2020 to 2022 in the southern region of Brazil, with the highest number of cases in the state of Rio Grande do Sul. The most affected population consisted of Caucasian men aged 30 to 39 years old. Furthermore, these results may be related to the increasing trend of psychoactive substance use among the Brazilian population and also the COVID-19 pandemic, which led to a period of underreporting due to social isolation.
Disclosure of InterestNone Declared
The relationship between mental-health-related stigma among psychiatrists and country indicators across Europe
- D. Őri, P. Szocsics, T. Molnár, L. Bankovska Motlova, O. Kazakova, S. Mörkl, M. Wallies, M. Abdulhakim, S. Boivin, K. Bruna, C. Cabaços, E. A. Carbone, E. Dashi, G. Grech, S. Greguras, I. Ivanovic, K. Guevara, S. Kakar, K. Kotsis, I. M. I. Klinkby, J. Maslak, S. Matheiken, A. Mirkovic, N. Nechepurenko, A. Panayi, A. T. Pereira, E. Pomarol-Clotet, S. Raaj, P. Rus Prelog, J. Soler-Vidal, R. Strumila, F. Schuster, H. Kisand, A. Reim, G. Ahmadova, M. Vircik, H. Yilmaz Kafali, N. Grinko, Z. Győrffy, S. Rózsa
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S62-S63
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health-related stigma occurs not only within the public community but is also an issue among healthcare professionals. The relationship between national culture and provider stigma remains yet to be empirically attested.
ObjectivesWe performed a cross-sectional multicentre study across 32 European countries to investigate the attitudes of psychiatrists towards patients with mental health problems. We aimed to examine the relationship of attitude with country-specific indicators.
MethodsWe measured stigmatizing attitudes using the Opening Minds Stigma Scale for Health Care Providers (OMS-HC) within an online survey among specialists and trainees in general adult, child and adolescent psychiatry. Its total score was correlated with the Human Development Index (HDI), the Democracy Index (DI), the Social Progress Index (SPI), the number of psychiatrists per 100,000 people, and the Hofstede dimensions. Latent class analysis was done to find subgroups of countries according to the stigmatizing attitudes of psychiatrists and the six Hofstede dimensions.
ResultsAltogether, n=4245 participants completed the survey. The total score of the OMS-HC significantly correlated with the long-term orientation (r=0.453, p=0.015) and indulgence dimensions (r=-0.629, p<0.0001) and with the HDI (r=-0.503, p=0.005), DI (r=-0.418, p=0.024), SPI (r=-0.348, p=0.040). The latent class analysis separated high- and low-stigma countries. High stigma was associated with high power distance and uncertainty scores.
ConclusionsFindings from this study not only expand knowledge of factors related to stigmatizing attitudes of healthcare professionals, but also enlighten the cultural aspects of the stigma that could contribute to the further development of anti-stigma programs.
Disclosure of InterestD. Őri Grant / Research support from: Research grant form the Fulbright Association, P. Szocsics: None Declared, T. Molnár: None Declared, L. Bankovska Motlova: None Declared, O. Kazakova: None Declared, S. Mörkl: None Declared, M. Wallies: None Declared, M. Abdulhakim: None Declared, S. Boivin: None Declared, K. Bruna: None Declared, C. Cabaços: None Declared, E. A. Carbone: None Declared, E. Dashi: None Declared, G. Grech: None Declared, S. Greguras: None Declared, I. Ivanovic: None Declared, K. Guevara: None Declared, S. Kakar: None Declared, K. Kotsis: None Declared, I. Klinkby: None Declared, J. Maslak: None Declared, S. Matheiken: None Declared, A. Mirkovic: None Declared, N. Nechepurenko: None Declared, A. Panayi: None Declared, A. Pereira: None Declared, E. Pomarol-Clotet: None Declared, S. Raaj: None Declared, P. Rus Prelog: None Declared, J. Soler-Vidal: None Declared, R. Strumila: None Declared, F. Schuster: None Declared, H. Kisand: None Declared, A. Reim: None Declared, G. Ahmadova: None Declared, M. Vircik: None Declared, H. Yilmaz Kafali: None Declared, N. Grinko: None Declared, Z. Győrffy: None Declared, S. Rózsa: None Declared
Scale for Body Image Concerns During the Perinatal Period – Adaptation and validation
- A. T. Pereira, B. Barbosa, R. Lima, A. I. Araújo, C. Marques, D. Pereira, A. Macedo, C. Pinto Gouveia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S159-S160
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The perinatal period may intensify weight and body image concerns. Due to its specifics, the traditional body image scales are inaccurate in the perinatal period (Fuller-Tyszkiewicz et al. 2013). The Body Image Concerns During Pregnancy (Uçar et al. 2018) was developed to measures this cognitive-emotional variable in pregnancy.
ObjectivesTo analyze the psychometric properties of the Portuguese adapted (both for pregnancy and postpartum) version of the Body Image Concerns during the Perinatal Period (BICPP), namely its construct validity and the internal consistency.
MethodsA sample of 346 women recruited through social media and Family Health Units, assessed in the second trimester of pregnancy (mean gestational age=28.11±7.67 weeks) and after delivery (baby’s age 4.37±2.87 months), completed a survey including the Portuguese BICPP.
The total sample was randomly divided into two sub-samples: sample A (n=173) was used to perform an exploratory factor analysis/EFA; sample B (n=173) to perform a confirmatory factor analysis/CFA.
ResultsEFA resulted in four components. CFA revealed that the second-order model with four factors presented good fit indexes (X2/df=2.4141; CFI=.9195; GFI=.948; TLI=.9028; GFI=.8181; RMSEA=.0807). BICPP Cronbach alphas was α=.936; for F1 Concern about future weight and image, F2 Concern with the new body image, F3 Social avoidance and concern and F4 Concern with appearance were .922, .930, .809, .807, respectively.
ConclusionsThis psychometric study provides evidence for the validity and reliability of the Portuguese version of BIC-Perinatal Period, which will be used in an ongoing research project on the relationship between eating, depressive and anxiety disorders in the perinatal period.
Disclosure of InterestNone Declared
Prevalence of Low Self-Esteem Among Patients Treated in the Craniofacial Surgery Department of an international Reference Hospital
- G. Pereira Bernd, V. Dall Agnol Bouvier, T. Brusa da Costa Linn, I. Cho de Almeida, B. de Oliveira de Marchi, L. Guinter Muccillo, C. G. Menezes Chaves Barcellos, C. Paz Portinho, M. V. Martins Collares, R. Ribas Leite
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S484-S485
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Craniofacial surgery is a specialized field that addresses congenital and acquired deformities of the head and face. While the physical outcomes of craniofacial surgery are well-documented, less attention has been given to the psychological well-being of adult patients. This abstract aims to explore self-esteem issues among adult patients treated at the Craniofacial Surgery Sector of HCPA (Hospital de Clínicas de Porto Alegre), where a substantial proportion of adult patients have reported self-esteem problems.
Objectives1. To assess the prevalence of self-esteem issues among adult patients (≥18 years old) attending the HCPA Craniofacial Surgery Sector.
2. To examine potential contributing factors to self-esteem problems in this specific patient population.
3. To evaluate the impact of self-esteem on the mental health and psychosocial functioning of adult craniofacial surgery patients.
4. To propose recommendations for psychosocial support and intervention strategies tailored to the needs of adult patients in this context.
MethodsThis cross-sectional study involved 132 adult patients who had undergone or were scheduled for craniofacial surgery at HCPA. Participants reported self-esteem issues in their talk with the hospital’s physicians, and their medical records were reviewed to collect demographic and clinical data. Additionally, participants provided information about their mental health status and psychosocial functioning.
ResultsAmong the 39 adult patients included in the study, 37 (94.9%) reported experiencing self-esteem issues, such as lack of confidence or feeling unattractive. The most commonly reported contributing factors were visible facial differences, social interactions, and prior surgical experiences. Patients with lower self-esteem had a higher likelihood of reporting symptoms of depression and anxiety and reported lower overall psychosocial functioning compared to those with higher self-esteem.
ConclusionsThis reveals a strikingly high prevalence of self-esteem issues among adult patients attending the Craniofacial Surgery Sector at HCPA. These findings underscore the importance of recognizing and addressing the psychological well-being of adult craniofacial surgery patients. Comprehensive psychosocial support, including counseling, peer support, and interventions to enhance self-esteem, should be integrated into the care of these patients. By addressing self-esteem concerns, healthcare providers can improve the mental health and overall quality of life of adult craniofacial surgery patients.
Disclosure of InterestNone Declared
Epidemiological analysis of hospitalizations for Schizophrenia, Schizotypal Disorders and Delirium in Rio Grande do Sul over the last 5 years
- L. Bardini, A. Roloff Krüger, G. Moreno Xavier, G. Fiorio Grando, J. Michelon, L. F. Alves Nascimento, J. Adames, A. T. Konzen, G. Pereira Bernd, C. Fontes Augusto, H. Wolmeister, I. Fachinetto Thoen, Y. de França, P. H. Filipin Von Muhlen, F. J. Carvalho da Costa, V. Kayser, P. H. Paesi Dutra, R. Rahal de Albuquerque, T. Garcia Furtado, G. Macelaro, A. C. Castelo, H. Vieira Rodrigues, E. Rockenbach Fidélis, D. Crusius, E. Guidugli, M. F. Valentim de Paula, Y. Marques Loureiro, E. Paiva Borsa, L. de Paula e Souza, G. Ferreira Cruz
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S390-S391
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In recent years, mental health has gained prominence in public health, prompting thorough investigations into psychiatric condition trends. This study conducts a comprehensive epidemiological analysis of hospitalizations for Schizophrenia, Schizotypal, and Delirium Disorders in Rio Grande do Sul (RS) over the past five years. By revealing these patterns, it enhances our understanding of regional mental health dynamics and offers insights for intervention strategies, resource planning, and improved mental healthcare. The ultimate goal is to advance more effective and accessible mental healthcare in RS and beyond.
ObjectivesThis study aims to analyze the prevalence and epidemiological profile of hospitalizations due to psychiatric disorders to assist in the diagnosis and outcome of affected patients.
MethodsA cross-sectional, descriptive, retrospective, and quantitative study was conducted regarding hospitalizations for Schizophrenia, Schizotypal Disorders, and Delirium in the state of RS between January 2018 and November 2022. Data were collected from the Department of Informatics of the Brazilian Unified Health System (DATASUS) in the “Hospital Information System of SUS” section, focusing on the nature of care, age group, gender, and ethnicity of the patients. The information was aggregated over the five-year period based on the four mentioned descriptors and subsequently analyzed to establish a profile of hospitalizations during that period.
ResultsThe analysis spans from 2018 to 2022, encompassing a total of 28,345 hospitalizations. In 2019, there was the highest number of cases (22.21%), followed by 2018 (21.08%). Urgent care admissions constituted 85.34% of the total. The age group most affected was 35 to 39 years (11.8%). Men were more affected than women (60.18%), and the majority of hospitalizations were among the Caucasian ethnicity (75.12%). The average length of stay was 23.7 days, and the mortality rate stood at 0.26%.
ConclusionsThe increasing trend in hospitalizations, peaking in 2019, highlights the need for preventive measures. Urgent admissions (85.34%) underscore the demand for accessible mental health resources. Men in the 35 to 39 age group are disproportionately affected, suggesting specific risk factors. The predominance of Caucasian ethnicity emphasizes the need for culturally sensitive care. A longer average length of stay (23.7 days) underscores treatment complexity, while a low mortality rate (0.26%) signals effective medical care. In essence, these findings inform tailored mental health policies to enhance service quality and prioritize patient-centered approaches.
Disclosure of InterestNone Declared
The Portuguese version of the screen for disordered eating: validity and reliability in men across multiple ages
- A. T. Pereira, A. Silva, M. J. Brito, C. Marques, A. Araújo, A. Macedo, S. Renca
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S564
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Screen for Disordered Eating/SDE was created as a primary care screening method for eating disorders, including binge eating disorder (Maguen et al. 2018). The SDE comprises five items (yes/no answers), extracted from other validated self-reported questionnaires assessing eating psychopathology. Its validity and reliability has proved in a Portuguese psychometric study, that only included woman (Pereira et al. 2022). It psychometric properties have yet to be evaluated in men.
ObjectivesWe aim to assess the psychometric properties of the Portuguese version of SDE in males.
MethodsParticipants were 227 male individuals with a mean age of 30.41 years (±13.96; range: 14-73). They answered an online survey including the Portuguese preliminary versions of the seven-item Eating Disorder Examination Questionnaire/EDE-Q7; the Body Image Concern Inventory/BICI and the Muscle Dysmorphia subscale of the Eating Disorder Assessment for Men/DM-EDAM.
ResultsConfirmatory Factor Analysis showed good fit for the unidimensional model (χ2/df=1.483; RMSEA=.0460; CFI=.980 TLI=.961, GFI=.988). Cronbach’s alpha was .621 which although inferior to .7 can be explained by the small number of items and the fact that each one assesses different dimensions. All items contributed to the internal consistency and presented high internal validity. Pearson’s correlations of SDE with BICI (.317) and EDE-Q7 (.361) were significant and moderate. The correlation with DM-EDAM was non-significant, probably due to its focus on muscle dysmorphia, which is not included in SDE’s items.
ConclusionsThe Portuguese version of SDE demonstrated adequate validity (construct and convergent) and reliability.
Disclosure of InterestNone Declared
Prevalence of psychiatric and cognitive disorders in patients with Pierre-Robin sequence - a statistical analysis
- G. Pereira Bernd, V. Dall Agnol Bouvier, T. Brusa da Costa Linn, I. Cho de Almeida, B. de Oliveira de Marchi, L. Guinter Muccillo, C. G. Menezes Chaves Barcellos, C. Paz Portinho, M. V. Martins Collares
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S485
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Pierre-Robin sequence (PRS), characterized by micrognathia, glossoptosis, and cleft palate, has long been a subject of clinical interest. Recent research suggests a potential association between PRS and cognitive or psychiatric disorders. This study explores this intriguing connection, shedding light on the complex interplay between craniofacial anomalies and mental health.
ObjectivesThis study aims to establish a comprehensive understanding of the relationship between Pierre-Robin Sequence and psychiatric disorders. Specifically, our objectives include: assessing prevalence, evaluating impact and informing clinical practice. This research aims to improve the holistic care and mental well-being of individuals with craniofacial malformations, contributing to a more comprehensive approach in the field of psychiatry.
MethodsThis cross-sectional study was conducted at a prominent referral hospital named Hospital de Clínicas de Porto Alegre, an international reference in Pierre-Robin Sequence, during the month of August 2023.
Participant Selection: Patients with PRS. Inclusion criteria encompassed individuals of all ages and both genders.
Data Collection: Trained medical personnel conducted structured interviews with participants to gather demographic information, medical history, and details of their craniofacial conditions.
Medical Records Review: Medical records were reviewed to corroborate craniofacial diagnoses and identify any comorbid conditions.
Statistical Analysis: Data were analyzed using appropriate statistical techniques to assess the association between PRS and psychiatric disorders.
Ethical Considerations: The study adhered to all ethical guidelines, with informed consent obtained from participants or their legal guardians. Ethical approval was obtained from the hospital’s Institutional Review Board.
Data Handling: Confidentiality and data security were ensured throughout the study, with all data anonymized to protect participant privacy.
ResultsIn our study, we assessed 28 different patients with Pierre-Robin Sequence, comprising 13 females and 15 males. The youngest patient was 2 months old, while the oldest was 22 years old. The mean age of the patients was 4.75 years, with a median of 3 years and a standard deviation of 5.36 years.
Among the patients, 6 exhibited psychiatric disorders, split between 4 males and 2 females. Their average age was 10 years, with a median of 9 years and a standard deviation of 4.2. The youngest patient with evidence of a psychiatric disorder was 5 years old.
ConclusionsThis study underscores a concerning reality within the Pierre-Robin population, pointing to a high prevalence of psychiatric disorders. These findings highlight the urgent need for integrated care, emphasizing the importance of early psychiatric assessment and tailored interventions to enhance the overall well-being of individuals facing the challenges of PRS.
Disclosure of InterestNone Declared
Hydroxy-Chromium Smectite
- C. Volzone, A. M. Cesio, R. M. Torres Sánchez, E. Pereira
-
- Journal:
- Clays and Clay Minerals / Volume 41 / Issue 6 / December 1993
- Published online by Cambridge University Press:
- 28 February 2024, pp. 702-706
-
- Article
- Export citation
-
Hydroxy-chromium solutions were prepared from chromium nitrate solutions by adding NaOH with OH/Cr = 2.
The solutions were treated at 20°C and 60°C. The hydrolysis times were from 1 to 100 days. Polymeric species in hydrolyzed chromium solutions were followed by visible absorption spectra within the range 325–800 nm and by pH measurement. OH-Cr-smectite with high d(001) spacing (2.07 nm) was obtained when hydroxy-chromium solution was prepared at 60°C and with 1-day hydrolysis. When this sample was heated up to 350°C the basal spacing collapsed at 1.8 nm.
The samples were characterized by X-ray diffraction and N2 adsorption-desorption isotherms.
Mn–Fe-rich genthelvite from pegmatites associated with the Madeira Sn–Nb–Ta deposit, Pitinga, Brazil: new constraints on the magmatic-hydrothermal transition in the albite-enriched granite system
- Ingrid W. Hadlich, Artur C. Bastos Neto, Vitor P. Pereira, Nilson F. Botelho, Luiz H. Ronchi, Harold G. Dill
-
- Journal:
- Mineralogical Magazine / Volume 88 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 13 February 2024, pp. 111-126
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Genthelvite from pegmatite veins hosted by the albite-enriched granite (ca.1.8 Ga) corresponding to the Sn–Nb–Ta (F, REE, Li, Zr, U, Th) Madeira deposit, Amazonas, Brazil was studied. Genthelvite, the exclusive Be-bearing mineral within the deposit, occurs as massive crystals of up to 4.7 cm in size. Compositions are homogeneous within individual crystals, although there is moderate variation in the overall composition reflecting relatively limited substitutions within the helvine–genthelvite–danalite solid-solution series, with relatively high Zn contents (36.96 to 49.45 wt.% ZnO), lower Mn contents (0.61 to 3.03 wt.% MnO), and variable Fe contents (2.10 to 10.94 wt.% FeO), completing an existing compositional gap in this system. Genthelvite formed in an alkaline and subaluminous environment, under stable conditions within the late-evolved fluids, at relatively high temperature (>400°C), in a reducing environment. The extremely high concentration of fluorine in the magma and the crystallisation of magmatic galena resulted in an effective reduction of H2S fugacity. This resulted in the stabilisation of genthelvite during the transition from the late magmatic to early hydrothermal stages of the albite-enriched granite evolution. The variability in Fe content within genthelvite is associated primarily with localised variations in the mineral assemblage (e.g. the presence of riebeckite and polylithionite). Genthelvite was altered by low-temperature aqueous fluids rich in F which resulted in the incorporation of Fe, Mn, Mg, Pb, Ba, Na, K, U and REE into the Zn2+ structural site and the allocation of excess Si, Al, Ti and P in the IVSi and IVBe structural sites. The substantial content of U and REE substituting for Zn, together with Si substituting for Be, is charge balanced by the presence of vacancies at the A site.
FC23: Dementia and Triadic (Doctor-Patient-Carer) Interactions in Primary Care
- C. Balsinha, F. Barreiros, M.J. Marques, S. Dias, S. Iliffe, M. Gonçalves-Pereira
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 84-85
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Primary care visits of persons with dementia often bring together triads composed of patients, family carers and general practitioners (GPs), as previously discussed (1). Communication dynamics potentially affect dementia outcomes, not least because primary care is a health setting where these triad encounters often occur naturally. Our aim is to present further data from Portuguese primary care consultations with persons with dementia, their carers and GPs.
Methods:We refer to the conclusion of our study ‘Dementia in Primary Care: the Patient, the Carer and the Doctor in the Medical Encounter - Bayer Investigation Grant | NOVAsaúde Ageing 2018’ (1). Fieldwork was interrupted during the COVID-19 pandemic and resumed in 2022. Sixteen consultations with persons with dementia, their carers and GPs (purposive sampling) were audio- recorded and transcribed verbatim. Interactions were thematically analysed using NVIVO® software. The analytical framework combined codes derived from the transcripts with codes from the literature.
Results:Dementia-related content took up less than half of consultations’ time, despite their considerable length (as compared to the average in primary care). Most GPs assessments lacked breadth, although efforts towards positive attitudes were present. Themes specifically related to social health in dementia were not (or were poorly) covered. Frequently, carers facilitated GPs’ assessment of dementia consequences, but their own needs were neglected. Patients’ self-expression tended to be limited.
Discussion:Our findings suggest that doctor-patient interactions in many GPs’ consultations seemingly compromise patient-centred approaches. There are challenges regarding how to assess the biopsychosocial consequences of dementia in a context of fragmented care (2,3). Given the scarcity of evidence from live-recorded primary care consultations about triadic dynamics, our findings are important to guide further explorations.
P123: Cognitive Disorders and Impact on Caregivers: The COGCARE Study protocol
- M. Gonçalves-Pereira, B. Pedrosa, M. Braga, M.J. Marques, C. Balsinha, A. Verdelho, E. Albanese, for the COGCARE Study Group
-
- Journal:
- International Psychogeriatrics / Volume 35 / Issue S1 / December 2023
- Published online by Cambridge University Press:
- 02 February 2024, pp. 252-253
-
- Article
-
- You have access Access
- Export citation
-
Introduction and objectives:
Dementia is associated with a high burden of disease, impacting patients, families and society. Nevertheless, related epidemiological data is becoming outdated, given the difficulties of implementing costly and laborious fieldwork surveys. Data is also difficult to retrieve from health and social services’ information systems. Overall, we must improve the feasibility and validity of case definition regarding dementia and the assessment of caregivers’ consequences. The 10/66 Dementia Research Group diagnostic algorithm is a cross-culturally valid method(1). A ‘short 10/66’ was also validated(2), but not in Portugal. We intend to assess its feasibility and validity in Portuguese samples, using REDcap (a browser-based, metadata-driven software) in mobile devices. Additionally, we aim to assess dementia family caregivers’ subjective burden and psychological distress, contrasting primary care and hospital outpatient settings.
Methods:A multicentre mixed-methods study will be conducted on fifty dyads of older people with dementia and their caregivers, plus 150 dyads of ‘controls’ and their close family members, as informants. The ‘short 10/66’ will be administered. Dementia caregivers’ assessments include the Zarit Burden Interview and Self-report Questionnaire. Quantitative analyses will estimate the sensitivity and specificity of the ‘short 10/66’ dementia case definition. Semi-structured qualitative interviews will be conducted with participants and research assistants, exploring their experiences with the assessment process; thematic analysis will then be used.
Implications:We expect this study to facilitate the diagnosis of dementia and data collection in health/social services on a routine basis, which will potentially improve the feasibility and decrease the costs of epidemiological surveys and allow for prevalence monitoring in Portugal.



