127 results
Unraveling a Psychiatric Puzzle: Corticosteroid-Induced Psychosis in Addison’s Disease. A case report
- F. Mayor Sanabria, M. Fernández Fariña, M. E. Expósito Durán, C. E. Regueiro Martín-Albo, C. Arroyo Del Val, M. Paz Otero, Í. Alberdi Páramo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S490
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The spectrum of neuropsychiatric adverse effects of corticosteroids ranges from unspecific symptoms to structured psychotic or affective episodes. We present the case of a 30-year-old woman admitted to our hospital due to behavioral alterations, coinciding with the initiation of treatment with corticosteroid boluses as part of a chemotherapy regimen for gastric adenocarcinoma. She had a previous diagnose of Addison’s disease, undergoing treatment with supplemental corticosteroids.
Objectives1) To describe the clinical particularities of this case, focusing on the psychopathological aspects and their correlation with the corticoid treatment.
2) To review the available literature regarding the clinical characteristics and management of corticosteroid-induced psychosis, with special interest in patients with adrenal insufficiency that require long term steroid supplementation.
MethodsA review of the patient’s clinical history and complementary tests were carried out. Likewise, we reviewed the available literature in relation to the clinical presentation of corticosteroid-induced psychosis and its pharmacological management.
ResultsThe patient was admitted to our hospital due to acute behavioural alterations, which temporally coincided with the 4th cycle of FOLFOX chemotherapy and corticosteroid boluses. She presented with incoherent speech, with non sequitur answers and glossolalia, as well as dysphoric affect and purposeless behavior. She presented a favorable clinical course after the initiation of treatment with antipsychotics and temporary suspension of corticosteroid treatment.
Manic symptoms are the most common presentation of “corticosteroid-induced psychosis”, with the key characteristic being the temporal association with the corticosteroids administration. Although the discontinuation of steroids generally results in a sudden decrease in symptoms, additional treatment with antipsychotics such as haloperidol or olanzapine might be required for a symptomatic control. In patients with adrenal insufficiency, long-term treatment with lithium or anti-seizure treatments are effective strategies in relapse prevention when a higer steroid dose is required.
Conclusions- Corticosteroid-induced psychosis is a well described clinical phenomenon, that usually presents with manic symptoms rather than psychotic experiences.
- Progressive discontinuation of corticosteroid treatment usually results in complete cessation of symptoms, but additional psychopharmacological treatment might be required, especially in patients with adrenal insufficiency undergoing long-term corticosteroid treatment.
- This case outlines the psychopathological richness in the presentation of corticosteroid-induced psychosis, and illustrates the challenges in the pharmacological management in patients with adrenal insufficiency.
Disclosure of InterestNone Declared
Concurrent mood pathology in patients with autism spectrum disorder (ASD). A case report.
- C. Díaz Mayoral, M. Martín de Argila Lorente, E. Arroyo Sánchez, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S382
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mood disorders in patients with ASD (Autism Spectrum Disorder) have a significant impact on their well-being. Major depression and bipolar disorder are among the most common co-occurring psychiatric diagnoses in autism. Prevalence estimates range from 10-50% for depression and approximately 5% for bipolar disorder. These figures are markedly higher than those reported in the general population.
The diagnosis of these disorders in patients with autism poses several challenges: mood problems may be “overshadowed” by the diagnosis itself, symptoms vary between individuals and may present “atypically” (psychomotor agitation, regression, reduced self-care, and severe irritability). The use of assessment tools based largely on criteria developed and validated in the general population is common.
ObjectivesA case of a patient diagnosed with ASD and co-occurring mood disorder is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 20-year-old patient with a diagnosis of severe autism spectrum disorder was referred to the emergency department for behavioral disturbances based on episodes of heteroaggressiveness and self-aggressiveness, with a daily frequency, in the last 2 months. His parents attribute this decompensation to the introduction of Sertraline and changes in his routine, which has implied less stimulation. Having ruled out underlying organic pathology, given that her father refers to frequent episodes of crying and abandonment of leisure activities of his liking, we suspect a mood disorder.
In hospitalization, Sertraline was withdrawn and Valproic Acid was introduced. Likewise, Risperidone dose was increased, already prescribed in outpatient care. Progressively, a notable improvement was observed.
ConclusionsCurrent clinical recommendations on the use of selective serotonin reuptake inhibitors (SSRIs) for mood problems are largely based on evidence from typically developing groups. However, it has been shown that some individuals with autism show different neural responses to pharmacological challenge compared to neurotypical individuals. In addition, the use of SSRIs in ASD may result in increased adverse side effects, such as agitation, impulsivity, hyperactivity, stereotypy, and insomnia, and it has been suggested that they should therefore only be considered on a “case-by-case” basis. A systematic review reported that mood stabilizers (Lithium, Valproic Acid) are preferable to atypical antipsychotics, which are associated with a large number of side effects.
Because of the lack of strong evidence on the efficacy of pharmacologic interventions and issues regarding safety and side effects, risperidone and aripiprazole are among the few medications approved by the FDA for the treatment of irritability in people with autism. More research aimed at effective medications to treat mood problems in ASD needs to be advocated.
Disclosure of InterestNone Declared
Manic episode with psychotic symptoms in a patient with Pseudologia Fantastica of years of evolution. A case report
- C. Díaz Mayoral, E. Arroyo Sánchez, P. Setién Preciados, M. Martín de Argila Lorente
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S766-S767
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pseudologia Fantastica (PF) also called “mythomania” is a disorder centred on the tendency of the sufferer to distort reality through constant lies. These patients find it difficult to moderate their sense of self and their self-esteem. Therefore, they display significant grandiosity, which seems to defend them from intense psychological disturbance, pretending to counteract deep feelings of unworthiness, emptiness and alienation.
Notable characteristics include: normal or above average IQ, absence of formal thought disorder, poor sense of identity, poor sexual adjustment, low frustration tolerance, strong dependency needs and narcissism. The phenomenon of “imposture” (the person’s claim of achievement or having connections to famous or influential people) is frequent. The patient’s history often shows that one or both parents were experienced as rejecting figures. They are more likely to be involved in legal problems and 20% receive some form of psychiatric treatment.
The aetiology and pathogenesis of this disorder requires consideration of developmental disturbances, personal history and current life stressors.
ObjectivesA case of a patient with PF is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsWe admitted a 47-year-old man to the Acute Hospitalisation Unit for a suspected “psychotic episode with clinical mania”.
He presented manic and psychotic symptoms, with delusional ideation of months of evolution, megalomaniacal and fantastic discourse, centred on his work with high-ranking government officials and other implausible events. Multiple academic, work and personal life failures, with a diagnosis of depression 15 years earlier.
During admission, he constantly confirms his history. He tends to present a rationalising discourse and a minimising attitude towards behavioural alterations. He appears cooperative and docile at certain times, while at others he is irritable, complaining and threatening.
As for medication, olanzapine was initially prescribed at a dose of 20 mg per day, which was reduced to 10 mg given the psychopathological improvement and the difficulties of adherence.
On discharge, the presumptive diagnosis was “delusional disorder and probable personality disorder with narcissistic traits, with a history of PF, which in recent months has presented a manic episode with psychotic symptoms”.
ConclusionsTheir management poses challenges in terms of engaging with treatment and building a therapeutic alliance. It is important to assess the social and legal implications. Ensuring that they have stable relationships and adequate social supports is essential for successful treatment. Further exploration and research into this disorder is needed to better understand its manifestations and psychiatric consequences.
Disclosure of InterestNone Declared
Late Onset Bipolar Disorder (LOBD): a case report
- M. Martín De Argila Lorente, B. Franco Lovaco, B. Rabinovici, C. Díaz Mayoral, G. E. Toapanta Yanza
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S635-S636
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Bipolar disorder (BD) in the elderly patient may present as the evolution of illness initiated earlier in life or as a new-onset entity. Therefore, two groups of patients are distinguished: “late onset” (LOBD) when the first mania occurs in old age and “early onset” in elderly patients with long-standing history. BD in elderly patients (≥60 years) constitutes 25% of all BD cases. Specific aspects of older age bipolar disorder (OABD) are somatic and psychiatric comorbidity, impaired cognition and age-related psychosocial functioning. The management of BD in the elderly is complex given the high sensitivity of these patients to pharmacological side effects, particularly of psychotropic drugs.
ObjectivesThe case of a patient with LOBD is presented, followed by a theoretical review of the subject.
MethodsA case is presented with a bibliographic review.
ResultsA 76-year-old woman who had no prior history of mental health issues until March 2023 when she was initially admitted to a geriatric hospitalization unit for manifesting manic symptoms. She was readmitted in July 2023 due to worsening depressive symptoms that included a declining mood, passive thoughts of death, deterioration in self-care, weight loss, insomnia, constipation, and dry mouth despite recent changes in her medications. She was on treatment with escitalopram (which was gradually discontinued and replaced with mirtazapine), quetiapine, lormetazepam, and lorazepam. Imaging tests showed chronic ischemic lesions in her brain and a small meningioma, the rest of the test were normal.
The initial diagnostic hypothesis was a bipolar depressive episode, and her treatment was adjusted accordingly. She was started on lithium, and her quetiapine dosage was increased, along with the anxiolytic lorazepam. Due to the persistence of depressive symptoms, including low mood, anhedonia, apathy, and negative thoughts, she was also prescribed antidepressant medication (venlafaxine and mirtazapine). Her condition gradually improved, with better eating and sleep patterns, increased participation in activities, and reduced somatic complaints and anxiety.
As she continued to experience somnolence and decreased morning energy, her antipsychotic medication was switched from quetiapine to lurasidone. The dose of lithium was decreased due to tremors in her extremities, although they remained within the therapeutic range. Despite these adjustments, her mood significantly improved, and she showed no signs of worsening or psychotic symptoms, leading to her discharge.
ConclusionsSummarizing different studies, LOBD who develop mania for the first time at an advanced age (≥ 50 years) constitute 5-10% of all BD. It is important to perform a thorough differential diagnosis, as an organic substrate and diverse etiologies may be present. Current guidelines recommend that first-line treatment of OABD should be similar to that of BD in young patients, with careful use of psychotropic drugs.
Disclosure of InterestNone Declared
Euthanasia and assisted suicide in people with mental disorders: a case report
- M. Martin De Argila Lorente, B. Franco Lovaco, M. González Guembe, M. Fresnillo Palomera, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S575
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Until 2020, only Belgium, Luxembourg, Switzerland, and the Netherlands legalized euthanasia and assisted suicide in Europe. Spain joined this list in March 2021 with the Euthanasia Regulation Law. However, the practice of euthanasia and assisted suicide in individuals with severe mental disorders is complex due to potential cognitive and decision-making challenges. Psychiatrists play a vital role in evaluating such requests.
Objectiveshe case of a patient with recurrent depressive disorder requesting euthanasia is presented, followed by a theoretical review of the subject.
MethodsA case is presented with a bibliographic review.
ResultsAn 89-year-old man with a history of one prior brief psychiatric hospitalization for depression three years ago was admitted after attempting suicide with an overdose of medication. He reports depressive symptoms of several years of evolution. Medical tests came back normal, but he had a urinary catheter due to voiding issues. He was initially on a medication regimen of amitriptyline, clomethiazole, and fluvoxamine. Despite his depressive state, he maintained his cognitive and decision-making abilities. Medication adjustments were made, including discontinuing amitriptyline and switching fluvoxamine to amitriptyline. His depressive symptoms worsened after three days, leading to the addition of trazodone to his treatment. He also developed urinary symptoms and was diagnosed with a urinary tract infection and metastatic prostate cancer during urological evaluation. Emotionally, he became more apathetic, anergic, and anhedonic, frequently expressing a desire for euthanasia, even with medication changes. Hyponatremia led to the discontinuation of duloxetine and the introduction of venlafaxine. To address anxiety and sleep problems, clomethiazole was replaced with mirtazapine. Upon learning of his cancer diagnosis, his mood deteriorated further, along with increased anxiety and continued mentions of euthanasia. Lorazepam was introduced, and he was informed of his right to request euthanasia after discussing therapeutic options with urology. Following this consultation, the patient became calmer, stopped expressing thoughts of death, and began making short-term plans, including the possibility of receiving palliative care at home upon discharge.
ConclusionsEuthanasia and assisted suicide in severe mental disorders are complex due to ethical and medical challenges. Patients must understand their condition, prognosis, and have decision-making capacity. Assessing their suffering is crucial. Coexisting mental and organic issues complicate the request’s origin. In SMD, determining irreversibility is tricky, as these are often chronic, non-terminal conditions. Exhausting treatment options is essential before considering euthanasia, despite patient treatment refusal. Limited research underscores the need for more studies.
Disclosure of InterestNone Declared
ADHD and BPD, two disorders for the same patient? Psychopathological dimensions and other cross-cutting factors in ADHD and BPD: a pragmatic review
- M. D. P. Paz-Otero, E. Lozano-Bori, S. Puyal-González, J. Sánchez-Rodríguez, F. Mayor-Sanabria, M. Fernández-Fariña, Í. Alberdi-Páramo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S657
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The relationship between Borderline Personality Disorder and Attention Deficit Hyperactivity Disorder has been highlighted in different studies over the last few years, with an estimated prevalence of around 15-35% of ADHD in adult patients diagnosed with BPD and a 7.4 times higher risk of developing BPD in patients diagnosed with ADHD.
ObjectivesTo conduct a pragmatic review of the recent literature on the relationship between ADHD and BPD, so that it serves as a starting point for an in-depth study of the sociodemographic, clinical and cross-sectional dimensional factors of both disorders.
MethodsA bibliographic review of scientific articles published in recent years, in English and Spanish, extracted from the MEDLINE database, which delve into the relationship between BPD and ADHD, will be carried out. In addition, the common psychopathological dimensions, such as impulsivity or emotional dysregulation, as well as the weight of other dimensional factors related to both disorders, will be studied.
ResultsThe results of the selected articles will be grouped, for a better understanding, in the following sections:
- Clinical factors and shared comorbidities.
- Psychopathological dimensions: impulsivity and emotional dysregulation.
- Other common dimensional factors.
ConclusionsThere are common symptoms and etiological or perpetuating factors, as well as comorbidities shared in both conditions, which in many cases make the correct diagnosis and, therefore, the appropriate therapeutic approach to these patients, quite difficult. Taking into account the differential characteristics of BPD and ADHD, it is possible to create different profiles that allow a precise approach to both disorders in those cases in which they coexist in the same patient.
Disclosure of InterestNone Declared
Addressing negative symptoms of schizophrenia in a Psychosis Day Hospital: a case report
- F. Mayor Sanabria, E. M. Fernández Fonollosa, C. M. Gil Sánchez, A. Fuentes Merlos, E. X. González Vivero, S. Puyal González, M. Fernández Fariña, B. Serván Rendon-Luna
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S729-S730
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms are present in more than two thirds of schizophrenic patients throughout the evolution of the disorder. These include symptoms related to reduced motivation or pleasure, such as avolition, anhedonia and asociality, and reduced expressivity, including alogia and blunted affect.
We present the case of a 24-year-old man who was admitted to our Psychosis Day Hospital after several psychotic episodes, presenting with prominent negative symptomatology that was imbued with mystical delusional beliefs.
Objectives1) To describe the clinical particularities of this case, focusing on the improvement of negative symptoms during the course of treatment at our Day Hospital.
2) To review the available evidence regarding the pharmacological and psychotherapeutic management of negative symptoms of schizophrenia.
MethodsA review of the patient’s clinical history and complementary tests were carried out. Likewise, we reviewed the available literature in relation to the management of negative symptoms of schizophrenia in an ambulatory setting.
ResultsThe patient was admitted to our Day Hospital after four psychiatric hospitalizations due to mystical delusions, ideas of grandiosity and hyper-spirituality, along with prominent negative symptoms at the moment of inclusion at our centre, including social withdrawal, diminished affective response, lack of interest in the academic sphere and poor social drive. Although previous positive symptoms were present in a lesser degree, the patient interpreted the presence of the negative symptoms described above as a “punishment” or “test” from spiritual creatures.
Management of negative symptoms represents a major unmet need in schizophrenia. Modest effect size evidence for pharmacological approaches favours the use of antipsychotic in monotherapy and augmentation of antipsychotic treatment with other agents, such as antidepressants. Scarce evidence regarding psychotherapeutic approaches to these symptoms points to the use of cognitive behaviour therapy and social skills training.
Conclusions- Clinical identification and characterization of negative symptoms is crucial when treating patients with schizophrenia, as these are associated with important disability and poorer functional outcomes.
- Differentiation of primary and secondary negative symptoms is a key aspect in the evaluation and management of schizophrenic patients.
- This case outlines the coexistence of positive and negative symptoms, and illustrates the challenges in the pharmacological and psychotherapeutic management of these symptoms at a Psychosis Day Hospital.
Disclosure of InterestNone Declared
A longitudinal study of conversational remembering in WhatsApp group messages before, during, and after COVID-19 lockdown
- Part of
- Lucas M. Bietti, Eric Mayor
-
- Journal:
- Memory, Mind & Media / Volume 2 / 2023
- Published online by Cambridge University Press:
- 30 November 2023, e5
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Conversational remembering entails that people engage in recalling past experiences, which may themselves have been shared. Conversational remembering comes with social benefits for the person telling the narrative and the one receiving it (e.g., developing and strengthening friendships, fostering entertainment, and consolidating group identity). COVID-19 lockdowns have significantly affected social interaction, including face-to-face interactions where conversational remembering occurs. The aim of this study was to explore how WhatsApp group messages supported conversational remembering in a large group of friends living in Buenos Aires where a complete lockdown was established between 19 March 2020 and 6 November 2020. To accomplish such aim, we conducted a mixed-methods longitudinal study. The data consisted of 32,810 WhatsApp group messages collected over a period of 700 consecutive days, from 13 April 2019 to 13 March 2021. Our study shows that WhatsApp group messages enabled group members to keep connected during the COVID-19 lockdown period. This occurred by remembering together situations, events, and actions associated with the group's identity. The use of WhatsApp group messages may have represented an adaptive collective behaviour in response to changes in global social norms.
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
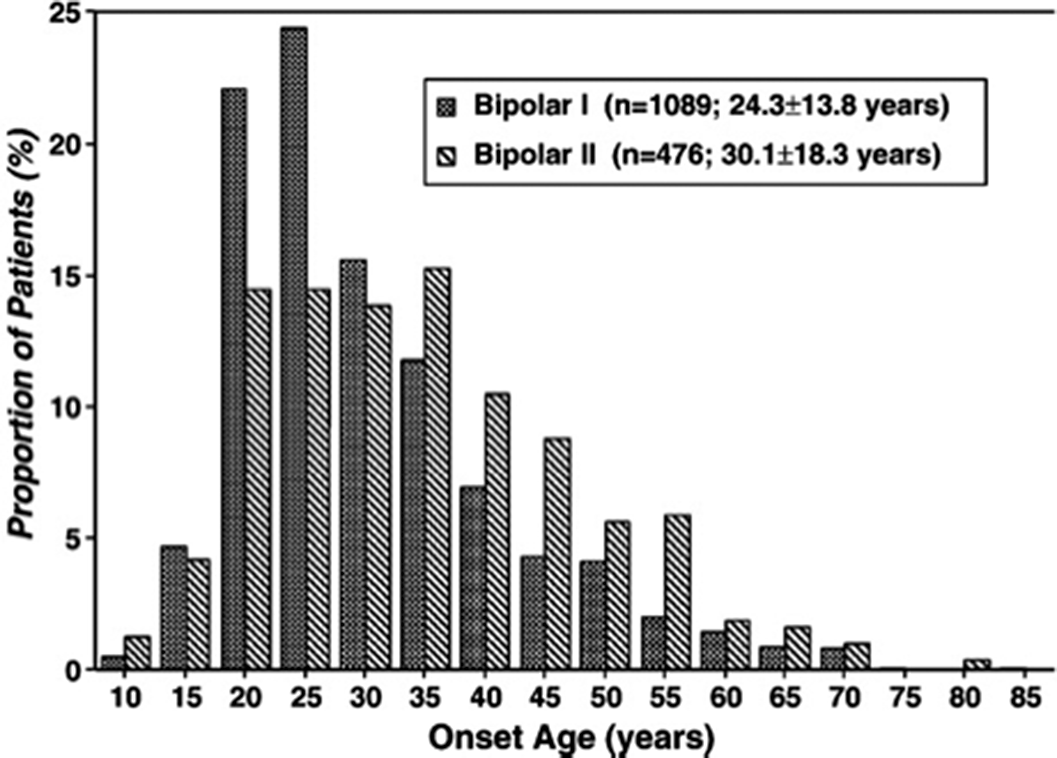
Image 2:
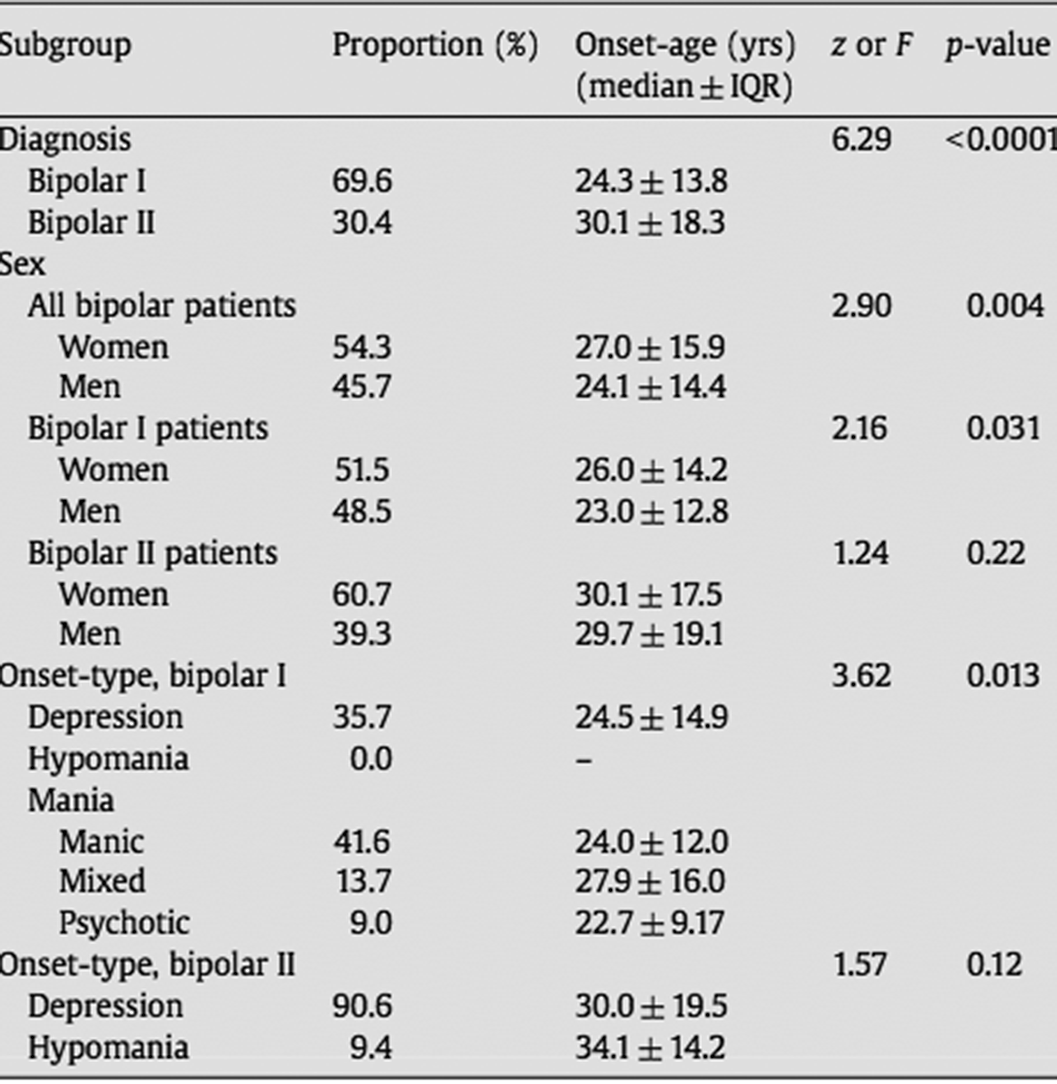 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
Euthanasia and psychiatric patients: a Spanish glance to the Dutch experience
- P. Albarracin, F. Mayor, M. Aparicio, E. Herrero
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S874
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The recent approval of euthanasia in the Spanish legal code and its posible extension to psychiatric patients opens an unprecedented scenario in the Iberian country. We analize the experience of the Netherlands, a country where euthanasia has been in practice for over two decades, in order to foresee epidemiological trends that could be replicated in Spain.
ObjectivesTo review the legislation on euthanasia in Spain and the Netherlands, as well as the epidemiological data regarding euthanasia applicants affected by mental health conditions in the Netherlands, to predict future epidemiological trends in a similar population in Spain.
MethodsWe studied the legislation on euthanasia in Spain and the Netherlands, as well as the directives of the Regional Commisions for Euthanasia in the Netherlands to analize differences and similarities between the legal codes on both countries. We also sought epidemiological data regarding the application of euthanasia on psychiatric patients in the Netherlands, gathering data from seven articles in English language obtained through a search in PubMed using the MeSH terms “Euthanasia” AND “Netherlands” and “Psychiatry”.
ResultsEuthanasia on psychiatric patients in the Netherlands has been a practice on the rise during the last decade, despite the elevated proportion of rejected applications and the high survival rate of this patients in later longitudinal studies. Affective disorders and personality disorders stand out as major psychiatric causes between the applicants. The Spanish legislation bears important resemblance to its Dutch predecessor, but also significant differences.
ConclusionsThe available data on the application of euthanasia on mental health patients in the Netherlands show an in increasing trend regarding the execution of this practice, specially on patients who gather distinct clinical features. The data provided by the Dutch experience could have some replication in Spain, as well as anticipate possible future ethical conflicts regarding the application of this service.
Disclosure of InterestNone Declared
Moria or Mania? Manic symptoms as the clinical manifestation of glioblastoma recurrence: a case report
- F. Mayor Sanabria, M. E. Expósito Durán, M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. Paz Otero, I. Alberdi Páramo, B. Rodado León
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S520
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Up to 50% of patients with brain tumors experience psychiatric symptoms, and rates up to 80% have been reported in malignant neoplasms such as glioblastoma multiforme (GBM). Still, clinical presentation as mania-like syndromes is a rare phenomenon, mainly occurring when frontal structures are compromised.
We present the case of a 42-year-old woman who was admitted to our hospital due to manic symptoms coinciding with a recurrence of a bifrontal GBM, for which she underwent surgery 5 months prior.
Objectives1) To describe the clinical particularities of this case, focusing on the differential diagnosis.
2) To review the association between manic symptoms and frontal dysfunction caused by brain tumors, with special interest on GBM.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, we reviewed the available literature in relation to manic symptoms related to brain tumors.
ResultsThe patient’s GBM recurrence presented with late onset symptoms of mania, including euphoric mood, increased spending, ideas of grandiosity and hyper-religiosity. She had no previous psychiatric history but, interestingly, she had an extensive affective burden in her family, with 4 consummated suicides. However, she also presented other clinical signs, such as disorientation, perseveration, mild memory impairment and stereotyped motor behaviors, that pointed to relevant frontal lobe dysfunction, suggesting Moria as a possible contribution for the symptoms described.
Manic symptoms in the context of brain tumors appear in 7-15% of patients with psychiatric symptoms, usually associated with right frontal dysfunction (75% of cases). Bifrontal affectation, such as this patient, is only described in 6% of cases. Although fast growing, malignant tumors have been associated with higher rates of psychiatric symptoms, no correlation has been described between these and brain tumor histology.
Conclusions- The presence of atypical manic symptoms, such as those presented in this case, should raise clinical concern for secondary mania.
- Moria shares similarities with mania, including mood elevation, tendency to hilarity or hyper-sexuality, that may hinder diagnosis of patients with frontal dysfunction.
- This case outlines the difficulties in making a differential diagnosis in patient with both manic and neurological signs, and highlights the implication of frontal structures in the development of manic symptoms.
Disclosure of InterestNone Declared
Cultural factors in depressive experience and its severity: A case report
- C. Regueiro Martín-Albo, F. Mayor Sanabria, E. Expósito Durán, M. Fernández Fariña, M. Navas Tejedor
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S816
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For a very long time, anthropologists and psychiatrists have studied how the symptomatology of mental diseases varies among cultures. Different social environments approach depression in different ways, and cultural practices and meanings influence how it develops. Culture also affects how symptoms are felt and described, how treatments are chosen, how patients and doctors interact, how likely it is that certain events, like suicide, will occur, and how professionals behave. As a result, all of these circumstances must be taken into consideration when approaching the diagnosis and management of depressive disorders. To illustrate the above, we present the case of a 31-year-old man, originally from Nigeria, who was admitted to the hospital after a suicide attempt by precipitation onto the subway tracks.
Objectives(1) To describe the clinical particularities of this case, focusing on the diagnostic difficulties we faced derived from intercultural contrasts (2) To review cross-cultural differences in the symptomatology and its implication on severity of depressive disorders.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, a bibliographic review of the available scientific literature was also performed in relation to transcultural depressive experiences and its severity.
ResultsThere is little evidence in favor of a direct link between sociocultural factors and severe depression, but we reviewed the arguments that look significant for further research. Depressive illnesses are found in all societies and their symptomatic expression varies culturally, particularly in terms of somatization and delusional ideas. Similarly, the social and individual representations of the disease depend on the culture, and some conceptual models can increase the effects of stigmatization. These cross-cultural variations could influence the care-seeking process and therefore modulate the evolution of the disease in the sense of greater severity.
ConclusionsAll societies experience depressive disorders, which exhibit symptoms that vary culturally, especially in terms of somatization and delusional beliefs.
The care-seeking process is affected by cross-cultural differences, and as a result, the disease’s progression may also be modulated in terms of increased severity.
When we ignore cultural factors in understanding, assessing, and treating depression, we are contributing to misdiagnosis and errors in patient management.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Application of family therapy in a case of anorexia nervosa
- C. Díaz Mayoral, I. Romero Gerechter, E. Arroyo Sánchez, M. Martín Velasco, A. Sanz Giancola, M. Martín de Argila
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S848
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anorexia nervosa is a behavioral mental disorder, characterized by body dysmorphia, an intense fear of gaining weight and behaviors that interfere with this, in addition to a restriction of food intake, associated usually with medical complications, even a considerable risk of death.
Several psychotherapeutic approaches have been used along last decades. Until relatively recently, parents have been recognized as part of the problem, but nowadays we involve them into the therapeutic process through family therapy based on a systemic approach, recommended in current published clinical guidelines and research findings, with consistent evidence, as the first-line treatment of patients with anorexia nervosa.
ObjectivesA case of a patient with anorexia nervosa, is presented followed by a theoretical review on the topic.
MethodsA case is presented with a bibliographic review.
ResultsA 24-yeard-old female was hospitalized for renutrition due to a significant weight loss and multiple physical symptoms. After 4 months without progress, the patient was transferred to the psychiatric ward.
Once there, physical stabilisation was achieved with family therapy and pharmacological treatment, based on progressive administration of Clomipramine, previously assessed by Cardiology, which improved rumination and obsessive behaviour. We conduct daily individual and weekly family interviews, working on family dynamics, emotional regulation strategies and more adaptive ways of communication. Likewise, several lines of action were found in the systemic work: peripheral father; maternal over-involvement; fraternal rivalry; difficulties of interaction between all of them, derived from “the role of the sick person” and intra-family communication around the illness. Finally, showed effectiveness in terms of an improvement in interpersonal relationships, greater assertiveness and an optimistic attitude with an active search for coping strategies.
ConclusionsHistorically, parents have been recognized by a causal factor in the pathogenesis of this disorder. Nevertheless, the abolition of the emphasis on family responsibility, motivated by a philosophic and evidence-based, has allowed us to see them as an essential resource in aiding the patient in the improvement process. This parental involvement has resulted in a relevant reduction in morbidity, as well as a significant decrease treatment attrition rates. It has been noted a re-establishment in other individual and family factors such as self-esteem, quality of life, and some aspects of the experiences of caregiving, and behavioral symptoms have been resolved.
Disclosure of InterestNone Declared
Visual hallucinosis and Linezolid use: A case report.
- M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. E. Expósito Durán, F. Mayor Sanabria, Í. Alberdi Páramo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1012
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 78-year-old man with multiple somatic pathologies and associated depressive symptoms, under treatment with Citalopram 10mg, who was admitted due to cholangitis secondary to biliary prosthetic obstruction.
Empirical antibiotic treatment with Meropenem and Linezolid was started, along with an increase in the dose of Citalopram to 20mg due to mood worsening. The patient begins with symptoms consisting of complex and polymorphic visual hallucinosis, without any affective or behavioral repercussions. He does not present another semiology of the psychotic sphere.
ObjectivesTo highlight the importance of knowing the different interactions and adverse effects of drugs for good clinical management.
MethodsWe collected the complete medical history of our patient and we carried out a review of the interactions and adverse effects described with the antibiotic drug Linezolid.
ResultsAs the onset of hallucinations was temporarily correlated with the use of medications, drug-induced hallucinations were suspected, resolving completely after 2 days after withdrawal of Linezolid treatment.
Linezolid is a nonselective inhibitor of MAO A and B, preventing the destruction of monoamine neurotransmitters like serotonin, dopamine, or norepinephrine. It has dopaminergic properties that may enhance the central nervous system effects of anticholinergics and co-prescription with serotonergic drugs increases the risk of serotonin syndrome.
ConclusionsThis case highlights the importance of taking into account drug interactions and adverse effects to reduce the risk of drug induced symptoms and optimize their management.
The increase in resistance to antibiotic treatment allows us to anticipate that the use of Linezolid will increase in the coming years, and it is important to know its mechanism of action given the interactions with psychotropic drugs that we use in our usual clinical practice
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Cyclothymia, bipolar disorder and multiple sclerosis: A case report
- M. D. P. Paz Otero, E. Lozano Bori, J. Sánchez Rodríguez, S. Puyal González, M. Fernández Fariña, F. Mayor Sanabria, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S703-S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 49-year-old woman who was diagnosed with multiple sclerosis at the age of 19 and suffers from an affective disorder that has been evolving for years. This condition, for which she has been followed by psychiatry and psychology for more than ten years, consists of alternating periods of hypomania lasting weeks and phases in which frank depressive symptomatology predominates, with no phases of euthymia in between and with a predominance of severe deterioration of her functionality at both poles.
Objectives(1) We will review the term cyclothymia and explore the concept of “cyclothymic temperament” advocated by some authors, in order to be able to understand the dimension of the present case and reformulate its approach.
(2) The relationship between multiple sclerosis and bipolar spectrum disorders will be covered, reviewing the current knowledge in this regard and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, taking into account her life history, the complementary tests performed as well as the multiple therapeutic approaches tried over the last few years.
Likewise, a bibliographic review of the available scientific literature will be carried out in relation to the diagnosis of cyclothymia or bipolar disorder type II, the controversial term “cyclothymic temperament”, and the relationship that these diagnoses have with the diagnosis of Multiple Sclerosis.
Results(1) Our patient could fit into what many authors define as a cyclothymic temperament, fulfilling, in certain episodes, the criteria that the manuals propose for bipolar disorder type II.
(2) 2.1 The prevalence of bipolar affective disorder in MS is approximately twice as high as in the general population (rates of 0.3-2.4%). 2.2 Patients with MS have higher scores in cyclothymic and hyperthymic temperament than the control group. 2.3 Certain drugs generally used in BD also seem to have a beneficial effect on MS.
Image:
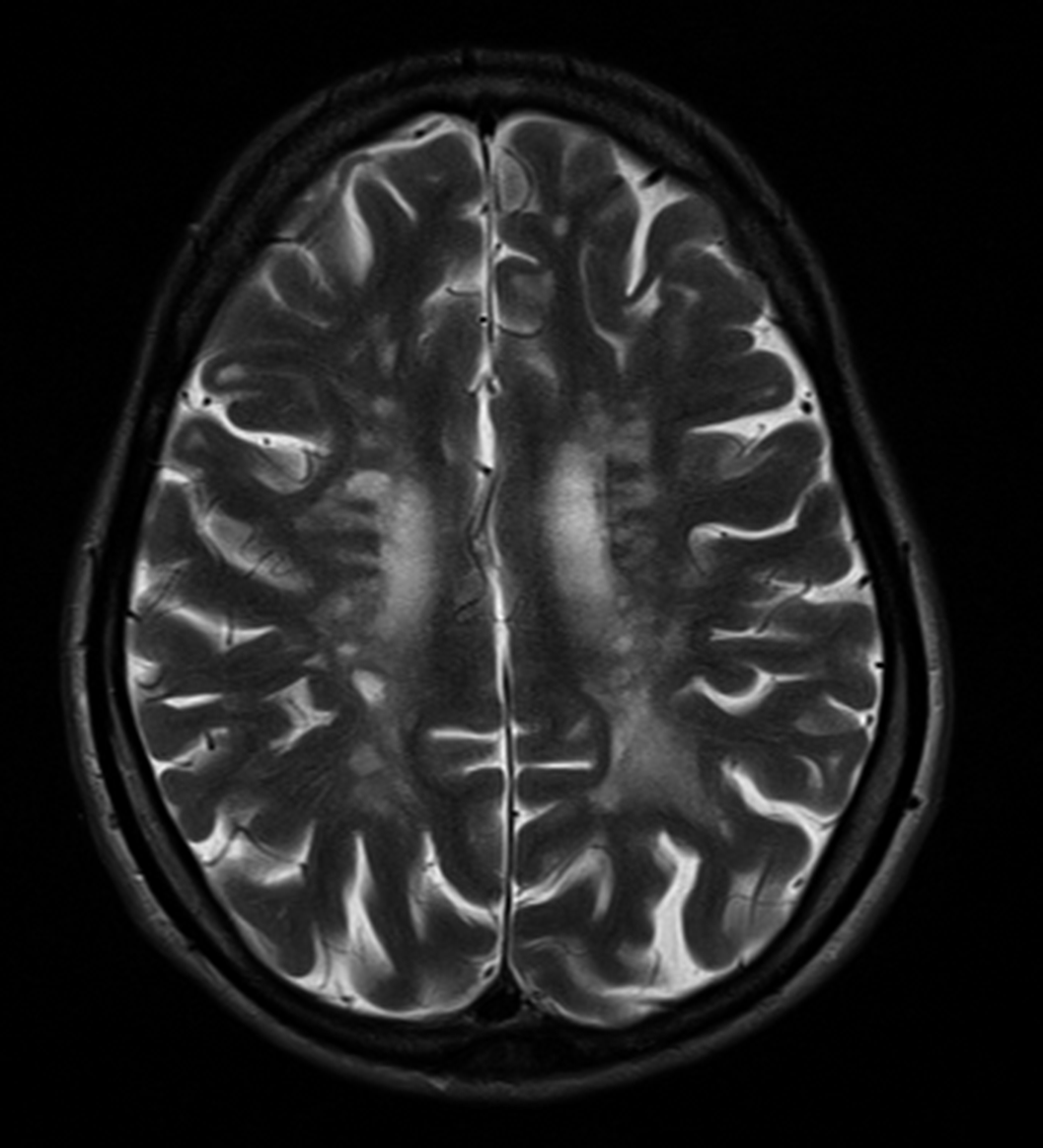
Image 2:
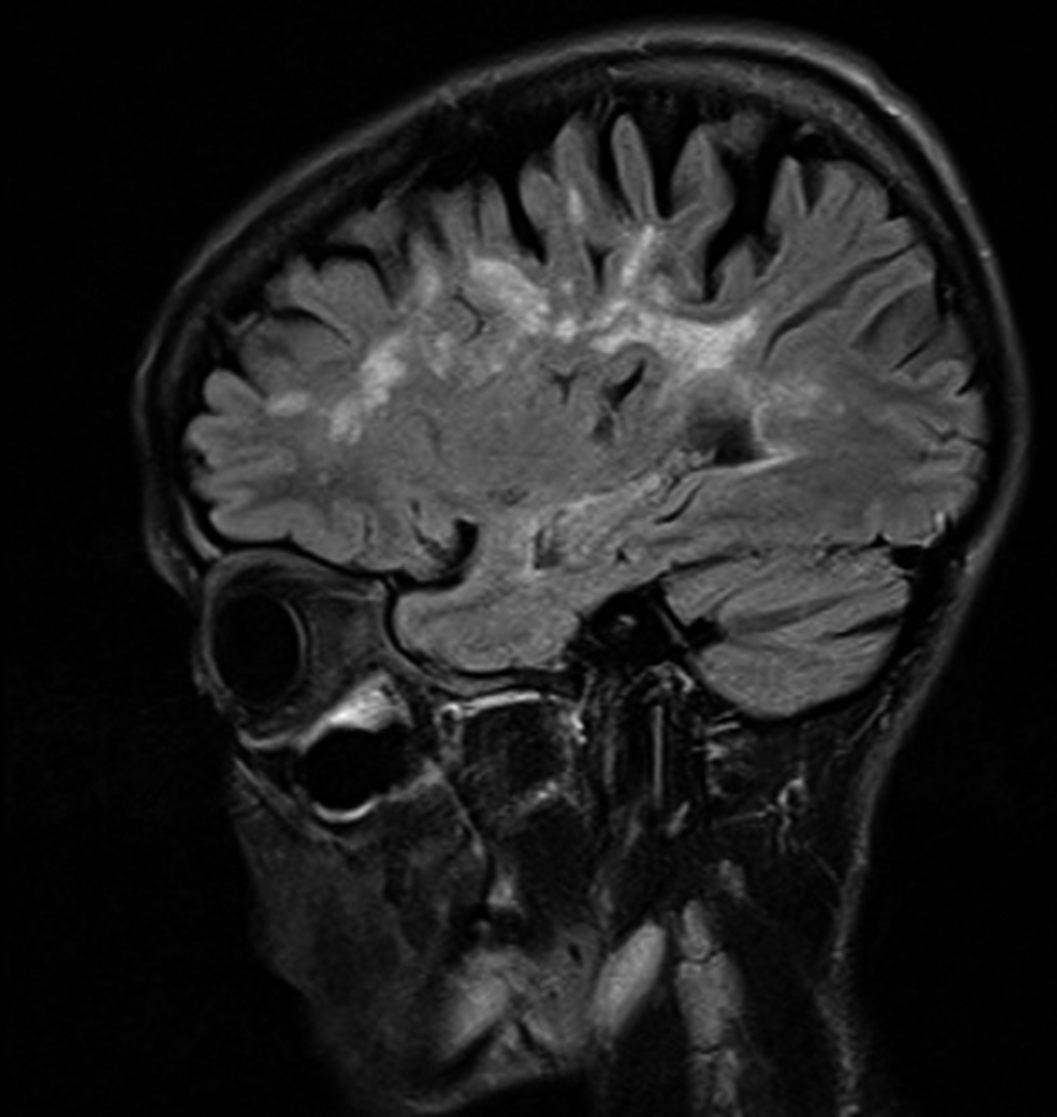 Conclusions
ConclusionsThe reformulation of the concept of cyclothymia would allow us to recognize in our patient a basic temperament of long evolution that would be the substrate on which different factors have subsequently influenced, such as antidepressant drugs or multiple sclerosis. In addition, it is necessary to know the association between BD and MS, in order to be able to offer an adequate treatment, contemplating some pharmacological options such as Lithium or some Atypical Antipsychotics, given the beneficial effect both for the affective disorder and for the neurological process.
Disclosure of InterestNone Declared
Reviewing the consistency of Dissociative Identity Disorder: a case report.
- E. Herrero Pellón, P. Albarracín Marcos, M. Huete Naval, R. Galerón Guzmán, F. Mayor Sanabria, A. Montes Montero
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S969
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 22-year-old patient who has been followed up in a daytime hospital for personality disorders since June 2022. Of note is the presence of multiple personalities (in total of more than 20 have been identified), each of which has distinct physical and psychological characteristics.
ObjectivesThe objective is to present a clinical case of dissociative identity disorder and to review the existence of scientific evidence supporting this diagnosis.
MethodsLiterature review of scientific papers over the last years and classic textbooks on the issue. We included references in English and Spanish languages.
ResultsNumerous studies support that dissociative disorders are the result of psychological traumas that generally begin in childhood. This is a difficult category to diagnose, since they present symptoms that also appear in other disorders such as those of the schizophrenic spectrum.
One or more dissociative parts of the subject’s personality avoid the traumatic memories while others become fixed to these traumatic experiences and manifest symptoms. In the case of our patient, there are dissociative episodes with subsequent amnesia and auditory, visual and olfactory hallucinations, as well as impulsive behaviors in the form of self-injury and a flattened affect, with significant emotional distancing.
Conclusions- The prevalence of dissociative identity disorder is higher than traditionally thought.
- Some theories develop how trauma essentially produces a degree of dissociation of the psychobiological systems that constitute the subject’s personality.
Disclosure of InterestNone Declared





