3293860 results
Evidence-Informed Approach to De-Prescribing of Atypical Antipsychotics (AAP) in the Management of Behavioral Expressions (BE) in Advanced Neurocognitive Disorders (NCD): Results of a Retrospective Study
- A. S. Luthra, R. LinBin Gao, P. Carducci, J. Sue, S. Remers
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S68-S69
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Diagnosis of behaviors in advanced neurocognitive disorders (aNCD) is one of exclusion, and the framework has been laid out in DSM-V. However, clinical assessments in aNCD become increasingly unreliable, and commonly used psychometric tools for clinical assessments lack reliability and validity, thereby making outcomes unreliable. Consequently, the syndromic and symptom management approaches for behaviors in aNCD behaviors have yielded poor results. To address this, the focus has shifted towards understanding the ‘meaning’ of behaviors in aNCD, recognizing them as a ‘mode of communication’. To date, there are no existing frameworks to ascribe ‘meaning’ to behaviors in aNCD.
ObjectivesLuBAIR™ paradigm is the first step in offering such a framework for understanding the ‘purpose’ and ‘meaning’ of behaviors in NCD. The ‘meaning’ ascribed to each behavioral category was used to guide the use of atypical antipsychotics in their management. De-prescribing was attempted on patients who qualified to enter this retrospective study. De-prescribing was defined as successful if individuals were completely withdrawn from AAP and remained off them for 60 days without the re-emergence of behaviors.
MethodsThe data collected on the second occasion, in the successful and failed de-prescribed groups, were compared in this retrospective study. MANOVA, Chi-Square paired t-test statistical analyses were used to detect the differences in the behavioral categories between the two cohorts. Cohen d was used to measure effect size.
ResultsPatients who did not have Mis-Identification and Goal-Directed Expressions were more likely to successfully de-prescribe: X2 (1, N = 40) = 29.119 p < 0.0001 and X2 (1, N = 40) = 32.374, p < 0.0001, respectively. Alternatively, the same behavioral categories were more likely present in patients who failed de-prescribing: MANOVA and paired t-test (p < 0.0001). Atypical antipsychotics, in their role as an antipsychotic and mood stabilizer, may be used to manage Mis-Identification and Goal-Directed Expressions, respectively.
ConclusionsLuBAIR paradigm has the potential to guide the development of specific behavioral care plans and the use of AAP in managing individual behavioral categories. AAP use can be justified for managing Misidentification and Goal-Directed Expressions. Vocal expressions may warrant the use of AAP, pending further study. The LuBAIR paradigm offers guidance for de-prescribing AAP for all other behavioral categories in the LuBAIR Inventory. This study is also a preliminary step in validating the psychological theories used to support the individual categories. This workshop will educate the participants on the LuBAIR paradigm and its application in developing person-centered interventions for behaviors in a NCD.
Disclosure of InterestNone Declared
Use of low-dose Aripiprazole to lower the antipsychotic medication - induced hyperprolactinemia.
- P. Argitis, A. Karampas, M. Peyioti, T. Koukouras, M. Demetriou, S. Karavia, Z. Chaviaras
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S623
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hyperprolactinemia (HPL) is a condition associated with disturbing consequences. Antipsychotic medications are one of the main causes of nontumoral hyperprolactinemia. Prolactin release in the hypothalamic tuberoinfundibular tract is increased through dopaminergic inhibition, which occurs more frequently with high- potency typical antipsychotics (40%–90%). Less commonly than typical antipsychotics, atypical antipsychotics can also result in hyperprolactinemia. In the presence of symptoms, clinicians frequently struggle with the decision of whether to stop using the suspected offending agent, lower the dosage, switch to another medication, or even add a full or partial dopamine agonist to the patient's current treatment. The issue is exacerbated by the fact that finding a suitable agent for each patient is sometimes a challenging task.
ObjectivesDue to the partial D2 receptor agonistic activity of aripiprazole, there is enough dopaminergic tone to continue the inhibition of prolactin release. Aripiprazole has been recommended in literature either as an adjunctive treatment in low doses or as a switch in therapy.
MethodsIn the Psychiatric clinic of the General Hospital of Corfu, a low-dose (5mg/day) of aripiprazole is being used as adjunctive therapy in patients with antipsychotic-induced hyperprolactinemia. More specifically in total 42 subjects, 19 male and 22 female, with a mean prolactin level of 862ng/ml, were introduced to the prior therapy. We whereupon conducted prolactin measurements to evaluate the response at the first, the third, and the sixth month of treatment.
ResultsOf the 42 subjects, 38 responded with an average reduction of prolactin to the level of 530ng/ml (mean reduction 38,5%).
ConclusionsHaving noticed the beneficial effect of low-dose Aripiprazole in patients with antipsychotic-induced hyperprolactinemia, we consider it appropriate that the literature recommendations concerning this additional use of aripiprazole should not be overlooked in clinical practice.
Disclosure of InterestNone Declared
Projective technique “Bird’s Nest Drawing” in child clinical psychology
- M. Zvereva, N. Zvereva, A. Sergienko, S. Strogova, D. Klak, E. Antonova, E. Balakireva
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S463-S464
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The “Bird’s Nest Drawing” technique is one of expressive drawing projective techniques. In Russia it has been used since the 2020s. We suggest the pilot version of using this projective technique in child clinical psychology. There were investigated the cognitive and emotional components of performance by children with different types of ontogenesis.
Purpose: pilot application of the technique of “Bird’s Nest Drawing” (BND) in the psychological diagnosis of children with different types of ontogenesis.
Objectives69 children and adolescents 6-17 years old (28 male), examined at the Mental Health Research Center. 1. hospital patients (11-16 years old, 18 persons) diagnoses F20.8, F21.4, 2) outpatient clients with psychological diagnostics (7-16 years old, 45 persons), most of them have psychiatric diagnoses and some of them came for a consultation independently of doctors (there were family and behavior problems). 3) children conceived with the help of assisted reproductive technologies (IVF) - participants in a program for studying cognitive and emotional-personal development (5-13 years old, 8 people). Control group of normal children (14 persons).
MethodsBird’s Nest Drawing (D.Kaiser, 2003, Kuftyak, 2021) - clinical expert assessment of the drawing parameters (size, location, quality, compliance with instructions) and the emotional component (color, self-assessment of the drawing).
ResultsTable 1. Frequency of different indicators of BND in compared groups of children.
Groups N Central place High Quality of drawing Nest out of tree birds /eggs Different colors Safety of nest High Assessment by participants High positive emotional expression Assessment by experts Hospital patients 18 (4 m) 12 4 10 4 10** 4 13** 5** Outpatient clients 45 (22 m) 38 13 19 17 32 10 25** 17 Children IVF 8 (2 m_ 7 2 4 3 6** 1 6 3 Normal children 14(6 m) 14 3 7 4 12** 4 13** 11** ** - significance of the differences (p≤0,05 by φ criterion).
Based on the data obtained, it can be noted that the most different between groups turned out to be an indicator for using different colors, subject’s assessment his picture and emotional expression assessment of picture by experts. Other parameters are similar: please of drawing,
DiscussionWe have obtained our own resalts about BND method in children with different type of ontogenesis. These data are similar to D.Kaiser and E.Kuftyak in opportunity of good diagnostic practice of BND method in children and adolescents with different type of ontogenesis in scientific
ConclusionsBND method is a good test for child clinical psychology as a projective one. Restrictions of this investigation - small groups, simple parameters for assessment. We plan to continue this work with more clinical (diagnosis, syndrome et cetera) and sex and age characteristics.
Disclosure of InterestNone Declared
ADHD in a women during (peri)menopause: missed diagnoses and cardiac complaints
- J. S. Kooij
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S800
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
(Abstract for the accepted case-based workshop by the NDAL section at EPA)
Women with ADHD are underdiagnosed in mental health care, and although ADHD starts in early childhood, the symptoms and impairment of women with ADHD may only be recognised for the first time during (peri)menopause.
ObjectivesThe relationship between decreasing levels of estrogen and the interaction with dopamine function in the brain in women with ADHD will be discussed and illustrated by a clinical case vignet of Mary, age 54.
MethodsMary presents with a history of repeated burnout episodes, mood swings, lifetime difficulty concentrating, planning and organising daily life, restlessness, sleep problems, and cardiac complaints.Mary has been working hard her whole life to overcome all difficulties, but her problem is she can never stop, leading to getting burnout several times. This time she is exhausted and can no longer cope; she is visiting the cardiologist for palpitations, hypertension and a recent myocardial infarction.
ResultsAfter a positive screening for ADHD, based on her lifetime symptoms of inattention, restlessness and impulsivity, as well as mood swings, she is referred to a psychiatrist for assessment of ADHD, mood and sleep problems. The pathophysiology behind this cluster of disorders during (peri)menopause, as well as the treatment options will be discussed based on Mary’s case.
ConclusionsBoth ADHD in women, (peri)menopausal mood disorders as well as the heart complaints in women during menopause are underrecognised and undertreated, leading to unneccesary suffering and cardiac death in women. It is time for psychiatry to join forces with cardiology and gynaecology for better recognition, sharing knowledge and multidisciplinary treatment of women with mental disorders such as ADHD during menopausal transition (see www.h3-netwerk.nl).
Disclosure of InterestNone Declared
An integrative, systemic day-clinic approach for the treatment of psychiatric disorders in young adults: a detailed study of two cases
- U. Altunoez, A. Osiak, M. Anthoff, G. Rietig, M. Bald, S. Akbas, I. T. Graef-Calliess
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S601
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 75% of the psychiatric disorders arise before the age of 30. Adolescence and young adulthood pose numerous developmental challenges like identity development, educational and occupational concerns, gaining autonomy and boundary-setting skills. The adolescent crises, which can involve a broad spectrum of psychiatric symptoms, demands a multidisciplinary approach to diagnosis and treatment.
ObjectivesOur goal is to present a best practice example of an interdisciplinary day clinic through two case presentations, aiming improving innovative strategies for assessment/treatment of psychiatric disorders in young adulthood.
MethodsVia two comprehensive case presentations, we will introduce a psychotherapeutic day-clinic concept from a psychiatric training hospital in Germany.
ResultsThe day clinic’s interdisciplinary team uses therapeutic approaches like dynamic, cognitive-behavioral, and systemic therapy to understand young adults beyond just their symptoms. Milieu-therapeutic methods, family constellations, socio-therapeutic approaches and non-verbal therapies are incorporated into our concept.
Case 1: A 20-year-old male patient, previously diagnosed with schizophrenia, was referred due to symptoms of living in an unreal world with perceived magical abilities and family conflicts. In the evaluation the features of high-functioning autism spectrum disorder (ASD) were more prominent than the psychotic symptoms. Developmental history and diagnostic tools yielded the diagnosis of ASD. Magical abilities in an unreal world appears to align more closely with repetitive/restrictive patterns of behavior, hereby we excluded in the follow-up the diagnosis of schizophrenia. Psychoeducation, social-skills-training and family interventions helped him to comprehend his strengths and discover a clearer direction in his life.
Case 2: Another 20-year-old male patient was referred with depressive symptoms, a sense of emptiness and self-mutilation. Following routine evaluation, we employed systemic methods (genogram constellations) to gain deeper insight into the patient’s psychopathology. His mother’s migration history from Thailand, coupled with unfulfilled aspirations, echoed in his recurring thought: “Where are my roots?” During follow-up, we recognized his passive stance toward therapeutic change, addressed through a systemic intervention known as ‘taking the side of non-change.’ This shifted his position from resistance to openness. Non-verbal approaches, family interventions, and corrective in-vivo experiences significantly contributed to his stabilization.
ConclusionsSpecialized psychiatric centers tailored to the unique needs of young adults play a critical role in evaluating, diagnosing, and treating psychiatric crises during this developmental stage. Achieving this requires the implementation of interdisciplinary holistic therapeutic approaches.
Disclosure of InterestNone Declared
Prevalence and patterns of post-traumatic stress disorder in victims of intimate partner violence
- F. Tabib, F. Guermazi, R. Masmoudi, D. Mnif, I. Feki, I. Baati, J. Masmoudi
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S665-S666
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
It’s a well-known fact that violence, particularly repetitive violence or violence lasting several years, as is often the case with intimate partner violence (IPV), has a severe psycho-traumatic impact. Although not all women are affected to the same degree or in the same way, post-traumatic stress disorder (PTSD) is the most common mental health consequence of IPV.
ObjectivesTo assess the psycho-traumatic impact of IPV on female victims. To study the factors associated with PTSD among these women.
MethodsWe conducted a descriptive and analytical cross-sectional observational study, carried out over a 10-month period from March 2021 to December 2021, among female victims of IPV consulting psychiatric emergencies at UHC Hédi Chaker, Sfax, Tunisia for medical expertise at the request of the court. We studied the PTSD in these women using the Post Traumatic Stress Disorder Checklist Scale (PCLS).
ResultsThe total number of participants was 120 with an average age of 37.27 years. The majority had secondary education or less (62.5%), were professionally active (53.3%), and were financially dependent on their partners (26.7%). As for the women’s clinical characteristics, 19.2% were under psychiatric care, 15% had attempted suicide and 10% had a history of childhood abuse. Regarding the couple’s profile, marriage was arranged in 58.3% of cases, and the average duration of marriage was 12.34 years, exceeding 10 years in 44.2% of cases.
The impact reported by our women was 100% psychological and 96.7% familial. As a result, 75.8% had sought help from family and friends, and 55.8% had decided to separate from their partners.
According to the PCLS scale, 78.3% of female victims showed PTSD with a positive score > 44. It was associated with a higher number of suicide attempts (p=0.04), a marriage duration exceeding 10 years (p=0.02), help-seeking (p=0.001), and divorce (p=0.014).
ConclusionsPTSD is a particularly serious psychiatric condition. However, its impact remains insufficiently understood and taken into account in medical, psychological, social, and legal care. Knowing the psycho-traumatic consequences of violence is absolutely essential to better protect, support, and care for victims.
Disclosure of InterestNone Declared
Association between loneliness in childhood and first-episode psychosis
- C. M. Díaz-Caneja, L. Donaire, V. Cavone, Á. Andreu-Bernabeu, J. González-Peñas, M. Díaz-Marsá, R. Rodríguez-Jiménez, Á. Ibáñez, E. Baca-García, J. C. Leza, M. F. Bravo-Ortiz, J. L. Ayuso-Mateos, C. Arango
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S88-S89
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Evidence from observational and genetic studies suggests a bidirectional relationship between loneliness and psychosis. To our knowledge, no previous study has assessed the association between loneliness in childhood and first-episode psychosis (FEP).
ObjectivesWe aimed to assess the association between loneliness in childhood and the odds of FEP and clinical variables of interest (i.e., diagnosis and clinical and functional severity) in FEP and to explore gender differences in this association.
MethodsThis was an observational, case-control study, based on the AGES-CM cohort, a longitudinal prospective study including patients with FEP ages 7-40, their first-degree relatives, and an age- and sex-matched sample of controls in seven university hospitals in the region of Madrid. We assessed loneliness in childhood with the question “Have you ever felt lonely for more than 6 months before the age of 12” and objetive social isolation with the peer relationships item from the childhood subscale of the Premorbid Adjustment Scale. We conducted logistic and linear regression analyses to assess the association between childhood loneliness and i) the odds of presenting a FEP and ii) clinical variables of interest (diagnosis and scores on positive, negative, general, depressive, and manic symptoms and functioning), while adjusting for demographic variables.
ResultsThe study sample comprised 285 patients with FEP (32.6% female, age 24.50 ± 6.2 years) and 546 controls (48.7% female, age 25.93 ± 5.5 years). Loneliness in childhood was associated with increased odds of FEP (adjusted odds ratio; aOR: 2.17, 95% CI [1.40-3.51], p=.002). This association remained significant after controlling for objective social isolation in childhood (aOR:2.70, IC 95% [1.58-4.62], p<.001).
The effect of the association was stronger in females (aOR:4.74, 95% CI [2.23-10.05], p<.001) than in males (aOR:1.17, IC 95% [0.63-2.19], p=.623). In females with FEP, loneliness in childhood was significantly associated with increased odds of receiving a diagnosis of other psychosis (aOR:0.155, 95% CI [0.048-0.506], p=.002) relative to an SSD diagnosis. In the FEP sample, loneliness in childhood was associated with greater severity of positive and affective symptoms and worse functioning.
ConclusionsLoneliness in childhood is associated with increased odds of FEP and clinical variables of interest. This suggests the potential role of this phenotype as an early risk marker for psychosis that could help guide targeted interventions.
Disclosure of InterestC. Díaz-Caneja Grant / Research support from: Instituto de Salud Carlos III (PI17/00481, PI20/00721, JR19/00024), European Union, Consultant of: Angelini, L. Donaire: None Declared, V. Cavone: None Declared, Á. Andreu-Bernabeu: None Declared, J. González-Peñas: None Declared, M. Díaz-Marsá: None Declared, R. Rodríguez-Jiménez: None Declared, Á. Ibáñez: None Declared, E. Baca-García: None Declared, J. C. Leza: None Declared, M. F. Bravo-Ortiz: None Declared, J. L. Ayuso-Mateos: None Declared, C. Arango Grant / Research support from: Madrid Regional Government (R&D activities in Biomedicine S2022/BMD-7216 AGES 3-CM), Instituto de Salud Carlos III, European Union, Consultant of: Acadia, Angelini, Biogen, Boehringer, Gedeon Richter, Janssen Cilag, Lundbeck, Medscape, Menarini, Minerva, Otsuka, Pfizer, Roche, Sage, Servier, Shire, Schering Plough, Sumitomo Dainippon Pharma, Sunovion and Takeda
First episode psychosis in a young person with a diagnosis of Autistic Spectrum Disorder: A Case report
- P. Raghvani, C. Inogbo, V. Damle
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S456
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic disorders are significant comorbidities in young people with Autistic Spectrum Disorder (ASD). Evidence suggests that ASD & psychosis present with overlapping clinical features & cognitive symptoms leading to misdiagnosis (Trevisan et al. Front.Psych 2020;11:548). Clinicians encounter diagnostic dilemma during assessment of psychosis in adolescents with ASD.
ObjectivesTo discuss the clinical challenges in the assessment & treatment of young people with ASD & comorbid psychosis.
MethodsA case report of a young girl with ASD & comorbid psychotic illness.
ResultsA young girl with ASD was admitted to CAMHS inpatient Unit with unusual beliefs & perceptual disturbances. She reported hearing the voice of ‘Hydrogis’ who was talking to her about his girlfriend. She made a voodoo doll & tried to set it on fire, as she believed that this would kill the girlfriend. She also heard voices of characters from a TV show, discussing her in third person. She absconded from home due to the distress associated. She attempted suicide by tying a ligature. She was seen responding to external stimuli, laughing incongruously & was thought disordered. Despite never being to USA, she spoke in American accent. She lacked insight & struggled to differentiate reality from fantasy. The aim of admission was to determine if the symptoms were part of ASD or a psychotic disorder. She had medication free assessment but continued to be very distressed. We commenced Aripiprazole which was optimised. She responded well to the treatment & was discharged to the care of Early Intervention in Psychosis team with partial remission of symptoms.
ConclusionsHistorically psychotic illnesses & ASD were thought to be closely linked. Research suggest that they are two separate disorders with specific onset, progress, signs & symptoms. ASD might be misdiagnosed as psychosis as difficulties in communication may resemble thought disorder, ‘melt down’ may mimic catatonia & difficulties in recognising others’ intentions may mimic paranoia. Our patient was experiencing first episode psychosis in late adolescence. This age of onset is consistent with research findings. A study to differentiate between ASD & psychosis found that positive symptoms like hallucinations & delusions were suggestive of psychosis while odd emotional gestures, stereotyped speech & restricted interests indicated ASD. Our patient predominantly had positive symptoms of delusions, hallucinations & thought disorder, hence our diagnosis of psychotic episode. In some cases, it is difficult to differentiate childhood fantasies from delusional beliefs (Ribolsi et al. Front.Psych 2022;13:768586). Bleuler explains that children with ASD replace imperfect realities with imaginations & hallucinations but Michael Rutter claims that autistic children lack fantasy. There are varying views on this subject & this is the challenge we faced when treating this young person.
Disclosure of InterestNone Declared
Exploring Exercise Intervention as a Therapeutic Catalyst within the Mental Health and Addiction Program in Nova Scotia: A Proof-of-Concept Study
- S. Obeng Nkrumah, R. da Luz Dias, E. Eboreime, B. Agyapong, S. Sridharan, V. I. O. Agyapong
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S826
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Many mental health conditions, including anxiety, mood disorders, and depression, can be effectively treated at a relatively low cost. Exercise interventions can be a therapeutic strategy, but even though exercise has consistently been shown to improve physical health, cognitive function, and psychological well-being, as well as reduce depression and anxiety symptoms, this intervention is often neglected in mental health care services.
ObjectivesThe study aims to assess the feasibility of incorporating an Exercise Intervention Program (EIP) as a therapeutic pathway within the Mental Health and Addictions Program (MHAP) in Nova Scotia, as well as to evaluate the effectiveness of the program on mental health outcomes and incremental costs, and the patient acceptability and satisfaction with the program.
MethodsThis proof-of-concept study has a pragmatic, prospective, controlled observational design with an embedded one-phase qualitative component. Patients with a primary diagnosis of depression or anxiety attending the Rapid Assessment and Stabilization Program (RASP, Halifax, Nova Scotia, Canada) will be offered to receive 60-minute exercise sessions three times per week, per 12 weeks. Patients with similar mental health conditions that have opted to wait for Cognitive Behavioral Therapy (CBT) with the community provider and declined from the EIP will be part of the control group. A certified recreational therapist will conduct the EIP. Participants of both groups (EIP and control condition) will be assessed at baseline and then weekly for four weeks, six weeks and then at 12 weeks post-enrollment. Primary outcomes include differences in the mean change in functional (well-being, resilience, and recovery) and symptom variables (depression, anxiety, and suicidal risk), which will be assessed through online validated scales/questionnaires. Service variables (patient acceptance and satisfaction) and health care utilization (crisis calls, emergency department visits, hospital admissions and readmissions, length of stay for each admission) will comprise the secondary outcomes.
ResultsThe results of the study will provide information about the effectiveness of EIP in the treatment of anxiety and depression compared to those only wait-listed to receive CBT or counselling from a CMHA provider. The study will also inform about the acceptability and satisfaction of the EIP, as well as the incremental cost-effectiveness of the intervention compared to the control condition.
ConclusionsThis proof-of-concept study will demonstrate the effectiveness of EIP as an adjunctive or alternative therapeutic option for the treatment of anxiety and depression in patients seeking mental health support from the MHAP in Nova Scotia.
Disclosure of InterestNone Declared
Reactivation of trauma in an inadequately structured person
- V. V. Jovanovska
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S667
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The person is constantly exposed to various types of psychosocial stress, and what will be the course and outcome of the reaction, in addition to other factors, primarily depends on the structure of the person (cognitive, conative, affective and somatic characteristics).
ObjectivesPresentation of a case of an inadequately structured person (a 29-year-old girl) who experiences an emotional loss, thus reactivating a trauma experienced many years ago (content-like emotional loss). The activation of traumatic memory as a center for generating a complex of pathological symptoms is provoked due to the personal structural inability of a person to legally reorganize, reintegrate and absorb stress.
MethodsFor a complete psychological exploration of an organization, personality dynamics, symptoms, defenses, motives, goals, values, interpersonal relationships, etc. I have applied: MMPI-202, NEO PI-R, Millon’s test, PIE, ZS and Azinger aggression scale.
ResultsThe result is an inadequately structured person of the avoidant type: introverted, vulnerable, disturbingly self-centered, constantly alert to prevent his impulses and affectional compunctions from leading to a repetition of pain and suffering experienced in the past, denying his feelings to maintain interpersonal distance, sensitive, helpless in an aggressive environment, low self-esteem and self-confidence, with weak capacities to overcome stress, etc. Anxiety and depressive symptoms are dominant. Manifest symptomatology is elaborated.
ConclusionsIn a person with an inadequate structure, there is an increased vulnerability, therefore applying an exploratory approach to people with a stressful condition in daily professional practice is a necessary need in order to more effectively, comprehensively treat the current and previously memorized stressful reactions with an emphasis on the highly personalized response to stress.
Disclosure of InterestNone Declared
Emergence of lobed wakes during the sedimentation of spheres in viscoelastic fluids
- Stylianos Varchanis, Eliane Younes, Simon J. Haward, Amy Q. Shen
-
- Journal:
- Journal of Fluid Mechanics / Volume 992 / 10 August 2024
- Published online by Cambridge University Press:
- 27 August 2024, A14
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The motion of rigid particles in complex fluids is ubiquitous in natural and industrial processes. The most popular toy model for understanding the physics of such systems is the settling of a solid sphere in a viscoelastic fluid. There is general agreement that an elastic wake develops downstream of the sphere, causing the breakage of fore-and-aft symmetry, while the flow remains axisymmetric, independent of fluid viscoelasticity and flow conditions. Using a continuum mechanics model, we reveal that axisymmetry holds only for weak viscoelastic flows. Beyond a critical value of the settling velocity, steady, non-axisymmetric disturbances develop peripherally of the rear pole of the sphere, giving rise to a four-lobed fingering instability. The transition from axisymmetric to non-axisymmetric flow fields is characterized by a regular bifurcation and depends solely on the interplay between shear and extensional properties of the viscoelastic fluid under different flow regimes. At higher settling velocities, each lobe tip is split into two new lobes, resembling fractal fingering in interfacial flows. For the first time, we capture an elastic fingering instability under steady-state conditions, and provide the missing information for understanding and predicting such instabilities in the response of viscoelastic fluids and soft media.
Sociodemographic profile and prescribing pattern of antipsychotic medication in patients with Schizophrenia
- A. Palushaj, V. Kola
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S242
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a complex psychiatric disorder that changes the patient’s life by influencing how they think, behave, express emotions, percept reality and their interpersonal relationships.
ObjectivesThe aim of this study was to evaluate sociodemographic and therapeutic factors that act as risk and protective factors in the clinical outcomes of patients diagnosed with schizophrenia.
MethodsThis was an observational retrospective study including patients diagnosed with schizophrenia, treated at the “Xhavit Gjata” Psychiatric Hospital, Tirane, Albania, who were discharged between May 1- October 30, 2022. The follow-up period was six months. Data on further hospitalizations during the follow-up were obtained from the Department of Statistics, QSUT, and confirmed by family members for hospitalizations in other psychiatric hospitals in the country. Univariate and multivariate analyses were conducted to identify potential factors associated with emergency room stays, length of stay, and time until the next admission.
ResultsA total of 158 patients were included in the study, 63 women and 95 men (p=0.03). The average age of the patients was 42.9 years, with women averaging 45.3 years and men 40.6 years (p=0.01). 43.7% of them had elementary education. The average age of disorder onset was 24.7 years. Haloperidol was the ambulatory therapy used in 54.3% of patients, while atypical antipsychotics were used in 75.1% of patients. The most commonly used atypical antipsychotic was Risperidone in 34.1% of patients, followed by Olanzapine in 17% of cases. Depo antipsychotics were used in 35.1% of patients. Clozapine was administered to 29.3% of patients, where 12.8% for the first time. 54.2% of patients starting Clozapine for the first time had three or more admissions. Clozapine was more frequently used in men, showing a significant difference from women (p=0.05). In 44.7% of cases, monotherapy was prescribed. The average hospital stay was 21.9 days, ranging from 2-68 days. Living with a family member, male gender, and being “married” helped reduce the length of hospital stay. In the 6-month follow-up period, 31.4% were re-hospitalized. Significant factors affecting the reduction of time spent outside the hospital until the next hospitalization were social problems, the number of previous hospitalizations, civil status “not married,” living arrangements, negative symptoms, and alcohol use (nearly significant). Protective factors included Clozapine, which reduced the prevalence of hospitalization by 57% compared to patients not taking it. Additionally, the use of Clozapine and Haloperidol increased the time spent outside the hospital.
ConclusionsSocial and family support, positive compliance, and antipsychotic therapy such as Clozapine serve as protective factors for patients diagnosed with schizophrenia.
Disclosure of InterestNone Declared
The Most Iniquitous Lobby: The Committee for Constitutional Government and the Shaping of American Politics, 1937–1955
- Alex McPhee-Browne
-
- Journal:
- Journal of Policy History / Volume 36 / Issue 3 / July 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. 281-307
-
- Article
-
- You have access Access
- HTML
- Export citation
-
This article examines the Committee for Constitutional Government, a conservative organization that spearheaded a novel form of mass-based mobilization and direct-mail propaganda to counter New Deal reforms from 1937 to the late 1950s. I argue that the members of the committee offered a supple and variegated response to New Deal liberalism, one with deep roots in the American past. Organizationally, the committee differed from other conservative groups of the period in the vastly greater reach of its propaganda, the small-donor financial base of its operations, and its extensive cultivation of a grassroots movement committed to right-wing reform. The committee was a critical political actor from 1937 to 1955, systematically shaping legislation and countering the trend toward social democracy in America. The ultimate result of its campaigns was to retard the growth of the administrative state and help formulate a cogent conservative critique of reformist liberalism.
In vitro antimicrobial and antibiofilm activity of phage cocktail against Mammaliicoccus sciuri, a causative agent of bovine mastitis
- Puthiya Maliyekkal Shahana Shirin, Archana Chandran, Pathiyarathvalappill Subrahmanian Surabhi, Ramachandran Latha Rathish, Mundakka Paramban Rahila
-
- Journal:
- Journal of Dairy Research , First View
- Published online by Cambridge University Press:
- 27 August 2024, pp. 1-6
-
- Article
- Export citation
-
In this research paper the in vitro antimicrobial and antibiofilm activity of phage cocktail against the coagulase negative Mammaliicoccus sciuri was investigated. Three M. sciuri isolates obtained from clinical bovine mastitis samples were characterized and identified by 16S rRNA gene sequencing. Bacteriophages with lytic activity against M. sciuri isolates were isolated from dairy farm effluents. Two typical phages were isolated using standard enrichment and plaque assay techniques, purified by polyethylene glycol precipitation, and morphologically characterized based on shape and size using transmission electron microscopy. This was followed by determination of host range using spot tests and stability to varying temperature, pH and UV treatment. The phage cocktail suppressed bacterial activity within 30 min of exposure. Crystal violet assay showed that the tested phages and their cocktail significantly reduced the biofilm biomass of all three M. sciuri strains compared to the untreated control in vitro within 24 h with a single dosing. Transmission electron micrography of the purified phage particle revealed an icosahedral head and a rigid contractile tail, characteristic of the class Caudoviricetes. The findings open new avenues in phage-based antimicrobial approaches for controlling contagious and teat skin opportunistic bacteria causing bovine mastitis.
Psychotherapies for generalized anxiety disorder in adults: systematic review and network meta-analysis of randomized-controlled trials
- D. Papola, C. Miguel Sanz, M. Mazzaglia, P. Franco, F. Tedeschi, S. A. Romero, A. R. Patel, G. Ostuzzi, C. Gastaldon, E. Karyotaki, M. Harrer, M. Purgato, M. Sijbrandij, V. Patel, T. A. Furukawa, P. Cuijpers, C. Barbui
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S50-S51
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Generalized anxiety disorder (GAD) is one of the most common mental disorders in adults. Psychotherapies are among the most recommended treatment choices for GAD, but which should be considered as first-line treatment still needs to be clarified.
ObjectivesTo examine the most effective and accepted psychotherapy for GAD both in the short and long-term, via a network meta-analysis.
MethodsWe searched MEDLINE, Embase, PsycINFO, and the Cochrane Register of Controlled Trials – CENTRAL, from database inception to January 1st, 2023, to find randomized controlled trials (RCTs) of psychotherapies for GAD. Eight psychotherapies (behaviour therapy, cognitive-behaviour therapy, cognitive restructuring, psychoeducation, psychodynamic therapy, relaxation therapy, supportive psychotherapy, and third-wave CBTs) were compared with each other and two control conditions (treatment as usual, waiting list). We followed Cochrane standards when extracting data and assessing data quality and used PRISMA guidelines for the reporting. We conducted random-effects model pairwise and network meta-analyses. We assessed risk of bias of individual studies through the second version of the Cochrane’s Risk of Bias tool and used the Confidence in Network Meta-Analysis (CINeMA) to rate certainty of evidence for meta-analytical results. Severity of GAD symptoms and acceptability of the psychotherapies were our outcomes of interest.
ResultsWe analysed data from 66 RCTs. Effect size estimates on data from 5,597 participants suggest third wave cognitive-behavioural therapies (standardized mean differences [SMDs] =-0.78; 95%CI=-1.19 to -0.37; certainty=moderate), cognitive-behavioural therapy (CBT) (SMD=-0.68; 95%CI=-1.05 to -0.32 certainty=moderate), and relaxation therapy (SMD=-0.54; 95%CI=-1.04 to -0.05; certainty=low) reduced generalized anxiety symptoms more than treatment as usual (TAU). Relative risks for all-cause discontinuation signalled no differences compared with TAU for all psychotherapies. When excluding studies at high risk of bias, relaxation therapy lost its superiority over TAU. When considering anxiety severity at three to twelve months after completion of the intervention only CBT remained significantly more efficacious than TAU (SMD=-0.58; 95%CI=-0.93 to -0.23).
Image:
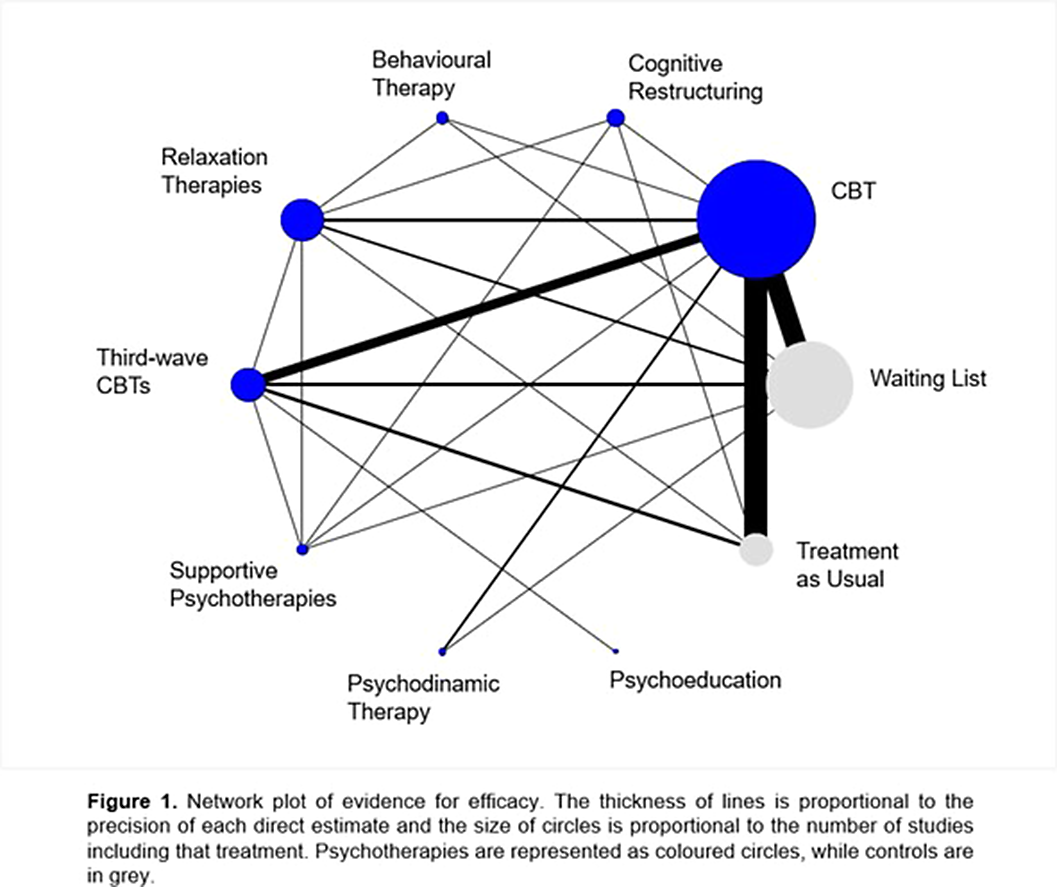 Conclusions
ConclusionsGiven the evidence for both acute and long-term efficacy, CBT may represent the reasonable first-line psychological treatment for GAD. Third-wave CBT and relaxation therapy have short-term efficacy and may also be offered. Results from this investigation should inform patients, clinicians, and guidelines. This project is funded by the European Union’s HORIZON EUROPE research programme under grant agreement No 101061648.
Disclosure of InterestNone Declared
Cannabis Use and Its Interaction with Anxiety Disorders
- F. Varino, T. Duarte, F. S. Silva, P. Froes, A. M. Fernandes, P. Baronet
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S423-S424
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cannabis use has been reported to cause a myriad of acute adverse reactions, including those linked to anxiety disorders, such as panic attacks and derealization. Notably, in the emergency department, anxiety makes up a significant proportion of the complaints related to cannabinoid consumption. Several reports show these symptoms can persist after the cessation of cannabis consumption. Consequently, some questions have arisen regarding the role of cannabinoids as precipitators for anxiety disorders in vulnerable individuals. Alternatively, it has been hypothesized that patients with anxiety disorders are more prone to using cannabis.
ObjectivesWe aim to understand whether there is an established relationship between anxiety disorders and cannabis use. Moreover, we intend to identify what are the factors which make an individual more likely to experience anxiety following cannabis consumption.
MethodsA search was conducted in the PubMed database using the MeSH terms “cannabis”, “panic disorder”, “anxiety”, “panic” and “generalized anxiety disorder”. Articles published in the last ten years were considered. Publications were selected after careful reading of their abstract. A non-systematic review of the selected articles was performed.
ResultsEight articles were included in this review. While a majority of these publications did not find a significant association between cannabis use and anxiety disorders, a small subset of analyzed articles found that cannabis use may increase anxiety severity in general, devoid of specific diagnostic association. Individuals who presented to the emergency department with anxiety complaints after cannabis use were likely to be young and to have ingested edible cannabis. History of psychiatric disease, especially substance use disorder, was common in this population.
ConclusionsMost available data suggest cannabis use is not clearly linked to anxiety disorders. However, information around this topic is scarce and heterogenous. Further research is needed focusing on the natural evolution of acute anxiety after cannabis use. Factors such as young age, presence of psychiatric comorbidities and consumption of edible cannabis appear to contribute to a significantly increased risk of experiencing acute anxiety after cannabis use.
Disclosure of InterestNone Declared
Cariprazine as adjunctive treatment of catatonia in schizoaffective disorder: a case report.
- D. Magalhaes, L. Fernandes
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S238
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Cariprazine is one of the most recent innovations in neuropsychopharmacology, with evidence for its efficacy in affective and psychotic spectrum disorders.
ObjectivesTo present a case that highlights cariprazine’s potential use outside the regulatory approved indications.
MethodsCase report using CARE guidelines and a narrative review.
ResultsWe present the case of a 41-year-old male readmitted to a psychiatric inpatient unit due to three months of mutism and withdrawal. At admission, the patient did not communicate verbally or in writing, but he complied with simple orders, and his consciousness remained unimpaired. He scored 11 points on the Bush-Francis Catatonia Rating Scale (BFCRS), indicating immobility, mutism, staring, withdrawal, ambitendency, and automatic obedience. We observed psychomotor retardation and indirect signs of a depressive mood, including the omega sign. His medical history included ongoing psychiatric treatment since the age of 30, with two prior admissions to an acute inpatient unit. At the time of admission, he was treated with olanzapine 20 mg/day, lorazepam 2 mg/day (recently downtitrated), venlafaxine 150 mg/day, and bupropion 150 mg/day. At the start of the current episode, the patient’s diagnosis was uncertain, with previous descriptions of psychotic, affective, and catatonic features. Due to suspicion of catatonia, we administered a high dose of lorazepam (8 mg/day), resulting in a partial response with a 4-point reduction in the BFCRS. We discontinued bupropion, increased venlafaxine to 225 mg, and switched from olanzapine to cariprazine using a taper, washout, and switch strategy. Psychotic symptoms briefly appeared when the patient was not taking a dopamine D2-receptor modulatory drug. We identified mild possible adverse drug reactions, including akathisia, transient insomnia, and daytime sleepiness. At a dose of 6 mg/day of cariprazine, we observed complete remission of catatonia (BFCRS=0) and significant improvement in affective and psychotic symptoms. The patient was discharged home with diagnoses of catatonia and schizoaffective disorder, prescribed 6mg/day of cariprazine, 225mg/day of venlafaxine, and 2,5mg/day of lorazepam. At the 6-month follow-up, the patient continues to exhibit clinical stability.
ConclusionsThis case emphasizes the safety and potential effectiveness of cariprazine in treating catatonia within the context of schizoaffective disorder. We consider that the partial agonist properties of cariprazine could theoretically reduce the risk of exacerbating catatonia, a risk typically associated with full D2-receptor antagonists. Other mechanisms of action, such as D3 partial agonism, may also contribute to the improvement or at least the non-aggravation of catatonic symptoms. Cariprazine’s mood-stabilizing properties make it a promising off-label choice for treating schizoaffective disorder, especially when catatonic features are present.
Disclosure of InterestNone Declared
A Machine Learning Model for Predicting Major Depressive Disorder Using Diffusion-Tensor Imaging Data
- J. H. Lee, D.-K. Lee
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S617-S618
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Major Depressive Disorder (MDD) stands as a prevalent psychiatric condition within the general population. Despite extensive research efforts, the identification of definitive diagnostic biomarkers for depressive disorders remains elusive. Currently, machine learning methods are gaining prominence in the diagnosis of medical illnesses.
ObjectivesThis study aims to construct a machine learning-based prediction model for Major Depressive Disorder (MDD) by harnessing diffusion tensor imaging (DTI) data.
MethodsThe DTI datasets comprising MDD (N=83) and Healthy Control (N=70) groups were procured from the cohort study of Anxiety and Depression conducted at the National Center for Mental Health in South Korea. A machine learning method using a decision tree algorithm was employed to select relevant brain regions and establish a robust diagnostic model. Features associated with white matter (WM) tracts were chosen through recursive feature elimination.
ResultsDemographic characteristics, including age, sex, and handedness, displayed no significant differences between the MDD and Healthy Control groups. However, the total score of the Beck Depression Inventory was notably higher in individuals with MDD compared to Healthy Controls. A diagnostic model was crafted using the decision tree algorithms to distinguish between the two groups. The model demonstrated the following classification performance metrics: accuracy (65.6% ± 8.5), sensitivity (66.6% ± 12.5), and specificity (64.7% ± 13.6). Furthermore, through recursive feature elimination, specific neuroanatomical features tied to brain structures such as the inferior cerebellar peduncle, posterior thalamic radiation, cingulum (hippocampus), uncinate fasciculus, and tapetum were identified.
ConclusionsDespite of limited performance of classification, a machine learning-based approach could provide insights into the development of a diagnostic model for MDD using neuroimaging data. Furthermore, these features, derived from DTI-derived data, may have implications for understanding the neural underpinnings of major depressive disorder.
Disclosure of InterestNone Declared
In People who Identify as Gender Minority People the Social Cure Model and in People who Identify as LGBTQ* People the Intragroup Status and Health Model might Explain the Link between Identity Centrality and Body Appreciation
- N. Komlenac, K. Stockburger, J. Birke, M. Hochleitner
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S557
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Sexual and gender minority (SGM) people are often found to have lower levels of body appreciation than do cis-heteronormative people.
ObjectivesThe current study utilizes the social cure model and the intragroup status and health model to investigate whether identification with a SGM social group and identity centrality (i.e., the degree to which a specific social identity is important to an individual) is linked to experiences of hostile behaviors because of a person’s looks or body and consequently, to body appreciation.
MethodsA cross-sectional online-questionnaire study was conducted with 1,680 German-speaking participants (49.2% cisgender women, 37.7% cisgender men, 9.0% non-binary, 4.1% transgender; Mage = 32.7, SD = 12.5). The Multidimensional and Multicomponent Measure of Social Identification, the Body Appreciation Scale-2, the Perceived Stigmatization Questionnaire and the Sociocultural Attitudes Towards Appearance Questionnaire-4, revised were used. A manifest path model was calculated.
ResultsPeople who identified as gender minority (GM) people and LGBTQ* people reported lower levels of body appreciation. Sexual minority (SM) individuals who identified with a social group other than LGBTQ* people reported levels of body appreciation similar to those of individuals who identified as women. Individuals who identified as GM people experienced fewer instances of hostile behaviors because of their looks or body the higher their level of identity centrality was. On the other hand, individuals who identified as LGBTQ* people more frequently encountered hostile behaviors because of their looks or body when their identity centrality was strong. Frequent experiences of hostile behaviors because of a person’s looks or body was linked to poor body appreciation in all social groups.
ConclusionsIdentity centrality might help alleviate experiences of discrimination, especially in people who identify as GM people, as the social cure model suggests. In line with the intragroup status and health model, individuals who strongly identify as LGBTQ* people might be more visible as SM people and experience more discrimination than do SM people who identify with another social group.
Disclosure of InterestNone Declared
Prevalence and Risk Factors of Burnout Among Medical Residents in Tunisia: A Cross-Sectional Study
- W. Haouari, S. Omri, A. Labyadh, I. Gassara, R. Feki, N. Charfi, J. Ben Thabet, M. B. Maalej, N. Smaoui, L. Zouari, M. Maalej
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S830
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The burnout syndrome is a blend of physical exhaustion and emotional fatigue that impairs an individual’s performance at work. In Tunisia, factors like working hours, the frequency of monthly shifts, and the physical and emotional abuse that physicians face from patients have collectively led to a significant incidence of burnout among medical professionals.
ObjectivesTo evaluate the prevalence of burnout syndrome among medical residents working in healthcare facilities in Tunisia and to pinpoint the contributing factors.
MethodsThis study is a descriptive cross-sectional survey conducted among medical residents completing their training in various healthcare facilities in Tunisia. The study employed an online self-administered questionnaire and assessed burnout across three dimensions: personal burnout, professional burnout, and relational burnout, using the Copenhagen Burnout Inventory (CBI).
ResultsA total of 50 physicians took part in the survey. Among them, 72% were female, 80% were single, and the average age at the time of the study was 27.72 years. Concerning their professional status, 84% worked in university hospitals, 16% specialized in surgery, 40% specialized in medicine, and 44% were family physicians. The majority were students from the Faculty of Medicine in Sfax (56%), with 30% in Monastir, 8% in Tunis, and 6% in Sousse. Regarding their work hours, more than 40 hours per week were reported by 32% of participants. According to the CBI scale, 12% of participants had scores indicating severe personal burnout, while 20% had scores indicating moderate personal burnout. Additionally,16% reported severe professional burnout, and 12% had scores suggesting severe relational burnout. In contrast, only 8% had scores indicating moderate relational burnout. The sociodemographic and professional factors that were studied, such as weekly working hours, monthly shifts, specialty, and workplace, did not show a significant correlation with the presence of burnout syndrome.
ConclusionsBurnout syndrome among medical resident physicians not only impacts their physical and mental well-being but also reduces their effectiveness and motivation at work. It is essential to introduce stress management strategies within hospitals to foster a healthier work-life balance.
Disclosure of InterestNone Declared


