Original Articles
Hand Hygiene with Soap and Water Is Superior to Alcohol Rub and Antiseptic Wipes for Removal of Clostridium difficile
- Matthew T. Oughton, Vivian G. Loo, Nandini Dendukuri, Susan Fenn, Michael D. Libman
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 939-944
-
- Article
- Export citation
-
Objective.
To evaluate common hand hygiene methods for efficacy in removing Clostridium difficik.
Design.Randomized crossover comparison among 10 volunteers with hands experimentally contaminated by nontoxigenic C. difficile.
Methods.Interventions included warm water with plain soap, cold water with plain soap, warm water with antibacterial soap, antiseptic hand wipes, alcohol-based handrub, and a control involving no Intervention. All interventions were evaluated for mean reduction in colony-forming units (CFUs) under 2 contamination protocols: “whole hand” and “palmar surface.” Results were analyzed according to a Bayesian approach, by using hierarchical models adjusted for multiple observations.
Results.Under the whole-hand protocol, the greatest adjusted mean reductions were achieved by warm water with plain soap (2.14 log10 CFU/mL [95% credible interval (Cri), 1.74-2.54 log10 CFU/mL]), cold water with plain soap (1.88 log10 CFU/mL [95% Cri, 1.48-2.28 log10 CFU/mL), and warm water with antibacterial soap (1.51 log10 CFU/mL [95% Cri, 1.12-1.91 logu, CFU/mL]), followed by antiseptic hand wipes (0.57 log10 CFU/mL [95% Cri, 0.17-0.96 log10 CFU/mL]). Alcohol-based handrub (0.06 log10 CFU/mL [95% CrI, -0.34 to 0.45 log10 CFU/mL]) was equivalent to no Intervention. Under the palmar surface protocol, warm water with plain soap, cold water with plain soap, and warm water with antibacterial soap again yielded the greatest mean reductions, followed by antiseptic hand wipes (26.6, 26.6, 26.6, and 21.9 CFUs per plate, respectively), when compared with alcohol-based handrub. Hypothenar (odds ratio, 10.98 [95% Cri, 1.96-37.65]) and thenar (odds ratio, 6.99 [95% Cri, 1.25-23.41]) surfaces were more likely than fingertips to remain heavily contaminated after handwashing.
Conclusions.Handwashing with soap and water showed the greatest efficacy in removing C. difficile and should be performed preferentially over the use of alcohol-based handrubs when contact with C. difficile is suspected or likely.
Commentary
New Approaches to Decontamination of Rooms After Patients Are Discharged
- John M. Boyce
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 515-517
-
- Article
- Export citation
Original Articles
Closed-Hub Systems with Protected Connections and the Reduction of Risk of Catheter-Related Bloodstream Infection in Pediatric Patients Receiving Intravenous Prostanoid Therapy for Pulmonary Hypertension
- D. Dunbar Ivy, Michelle Calderbank, Brandie D. Wagner, Susan Dolan, Ann-Christine Nyquist, Michael Wade, William M. Nickels, Aimee K. Doran
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 823-829
-
- Article
- Export citation
-
Background.
Intravenous prostanoids (epoprostenol and treprostinil) are effective therapies for pulmonary arterial hypertension but carry a risk of catheter-related bloodstream infection (CR-BSI). Prevention of CR-BSI during long-term use of indwelling central venous catheters is important.
Objective.To evaluate whether using a closed-hub system and waterproofing catheter hub connections reduces the rate of CR-BSI per 1,000 catheter-days.
Design.Single-center open observational study (January 2003-December 2008).
Patients.Pediatric patients with pulmonary arterial hypertension who received intravenous prostanoids.
Methods.In July 2007, CR-BSI preventive measures were implemented, including the use of a closed-hub system and the waterproofing of catheter hub connections during showering. Rates of CR-BSI before and after implementing preventive measures were compared with respect to medication administered and type of bacterial infection.
Results.Fifty patients received intravenous prostanoid therapy for a total of 41,840 catheter-days. The rate of CR-BSI during the study period was 0.51 infections per 1,000 catheter-days for epoprostenol and 1.38 infections per 1,000 catheter-days for treprostinil, which differed significantly (P < .01 ). CR-BSIs caused by gram-negative pathogens occurred more frequently with treprostinil than with epoprostenol (0.91 infections per 1,000 catheter-days vs 0.08 infections per 1,000 catheter-days; P <.01). Patients treated with treprostinil after the implemented changes had a significant decrease in CR-BSI rate (1.95 infections per 1,000 catheter-days vs 0.19 infections per 1,000 catheter-days; P <.01).
Conclusion.The closed-hub system and the maintenance of dry catheter hub connections significantly reduced the incidence of CR-BSI (particularly infections caused by gram-negative pathogens) in patients receiving intravenous treprostinil.
A Qualitative Exploration of Reasons for Poor Hand Hygiene Among Hospital Workers Lack of Positive Role Models and of Convincing Evidence That Hand Hygiene Prevents Cross-Infection
- V. Erasmus, W. Brouwer, E. F. van Beeck, A. Oenema, T. J. Daha, J. H. Richardus, M. C. Vos, J. Brug
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 415-419
-
- Article
- Export citation
-
Objective.
To study potential determinants of hand hygiene compliance among healthcare workers in the hospital setting.
Design.A qualitative study based on structured-interview guidelines, consisting of 9 focus group interviews involving 58 persons and 7 individual interviews. Interview transcripts were subjected to content analysis.
Setting.Intensive care units and surgical departments of 5 hospitals of varying size in the Netherlands.
Participants.A total of 65 nurses, attending physicians, medical residents, and medical students.
Results.Nurses and medical students expressed the importance of hand hygiene for preventing of cross-infection among patients and themselves. Physicians expressed the importance of hand hygiene for self-protection, but they perceived that there is a lack of evidence that handwashing is effective in preventing cross-infection. All participants stated that personal beliefs about the efficacy of hand hygiene and examples and norms provided by senior hospital staff are of major importance for hand hygiene compliance. They further reported that hand hygiene is most often performed after tasks that they perceive to be dirty, and personal protection appeared to be more important for compliance that patient safety. Medical students explicitly mentioned that they copy the behavior of their superiors, which often leads to noncompliance during clinical practice. Physicians mentioned that their noncompliance arises from their belief that the evidence supporting the effectiveness of hand hygiene for prevention of hospital-acquired infections is not strong.
Conclusion.The results indicate that beliefs about the importance of self-protection are the main reasons for performing hand hygiene. A lack of positive role models and social norms may hinder compliance.
Influx of Multidrug-Resistant, Gram-Negative Bacteria in the Hospital Setting and the Role of Elderly Patients With Bacterial Bloodstream Infection
- Aurora Pop-Vicas, E. Tacconelli, Stefan Gravenstein, Bing Lu, Erika M. C. D'Agata
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 325-331
-
- Article
- Export citation
-
Background.
Multidrug-resistant (MDR) gram-negative bacteria are reported increasingly frequently among isolates recovered from elderly patients. The clinical epidemiology of bloodstream infection (BSI) due to MDR gram-negative bacteria among elderly patients is unknown.
Objective.To characterize the clinical epidemiology of BSI due to MDR gram-negative bacteria among elderly patients at hospital admission in an effort to provide a greater understanding of these serious infections and ultimately to improve patient outcomes.
Design.Case-control study.
Setting.Tertiary care hospital in Boston, Massachusetts.
Patients.Patients 65 years of age and older.
Methods.From 1999 to 2007, computerized medical records were reviewed for BSI due to MDR gram-negative bacteria within 48 hours of hospital admission. Risk factors for BSI due to these bacteria were identified.
Results.MDR gram-negative bacteria were recovered from 61 (8%) of 724 elderly patients with BSI caused by gram-negative bacteria. Over the
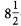 -year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9]; P = .006), presence of an invasive device (OR, 6.0 [95% CI, 1.5–23.5]; P = .01), severe sepsis (OR, 7.9 [95% CI, 1.7–37.1]; P = .009), and delayed initiation of effective therapy (OR, 12.8 [95% CI, 3.9–41.1]; P<.001).Conclusion.
-year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9]; P = .006), presence of an invasive device (OR, 6.0 [95% CI, 1.5–23.5]; P = .01), severe sepsis (OR, 7.9 [95% CI, 1.7–37.1]; P = .009), and delayed initiation of effective therapy (OR, 12.8 [95% CI, 3.9–41.1]; P<.001).Conclusion.The 16-fold increase in BSI due to MDR gram-negative bacteria at hospital admission among elderly patients, especially among those who resided in long-term care facilities prior to admission, contributes further to the expanding body of evidence that these patients are the main reservoirs of MDR gram-negative bacteria. Given their contribution to the influx of antimicrobial-resistant bacteria in the hospital setting, infection control interventions that target this high-risk group need to be considered.
Editorial
Methicillin-Resistant Staphylococcus aureus Decolonization “Yes, We Can,” But Will It Help?
- Jan Kluytmans, Stephan Harbarth
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 633-635
-
- Article
-
- You have access Access
- Export citation
Original Articles
Daily Hazard of Acquisition of Methicillin-Resistant Staphylococcus aureus Infection in the Intensive Care Unit
- Caroline Marshall, Denis Spelman, Glenys Harrington, Emma McBryde
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 125-129
-
- Article
- Export citation
-
Objective.
Increasing length of hospital stay is associated with methicillin-resistant Staphylococcus aureus (MRSA) acquisition. The exact risk of becoming colonized with MRSA on a given day has not been clearly elucidated. We determined the hazard of MRSA acquisition in relation to the length of time spent in an intensive care unit in which only standard precautions were used for MRSA-colonized and MRSA-infected patients.
Methods.This study took place at a tertiary referral hospital intensive care unit in which patients were screened for MRSA at hospital admission, at hospital discharge, and twice weekly during intensive care unit stay. We analyzed the hazard of MRSA acquisition by using a statistical smoothing kernel for hazard with a width of 5 days. Patients were stratified according to age, sex, medical unit, and length of hospital stay.
Results.Of the patients who were at risk of colonization or infection, 12.8% acquired MRSA. The mean length of stay in the intensive care unit was 7.2 days. The daily hazard of acquiring MRSA was less than 1% at admission to the intensive care unit and increased linearly to more than 2% risk per day by day 12, followed by a leveling out of risk.
Conclusions.The daily hazard of acquiring MRSA is not constant. This has implications for studies that assume a constant hazard in their analysis and should be considered.
Validation of Statewide Surveillance System Data on Central Line–Associated Bloodstream Infection in Intensive Care Units in Australia
- Emma S. McBryde, Judy Brett, Philip L. Russo, Leon J. Worth, Ann L. Bull, Michael J. Richards
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1045-1049
-
- Article
- Export citation
-
Objective.
To measure the interobserver agreement, sensitivity, specificity, positive predictive value, and negative predictive value of data submitted to a statewide surveillance system for identifying central line-associated bloodstream infection (BSI).
Design.Retrospective review of hospital medical records comparing reported data with gold standard according to definitions of central line–associated BSI.
Setting.Six Victorian public hospitals with more than 100 beds.
Methods.Reporting of surveillance outcomes was undertaken by infection control practitioners at the hospital sites. Retrospective evaluation of the surveillance process was carried out by independent infection control practitioners from the Victorian Hospital Acquired Infection Surveillance System (VICNISS). A sample of records of patients reported to have a central line-associated BSI were assessed to determine whether they met the definition of central line–associated BSI. A sample of records of patients with bacteremia in the intensive care unit during the assessment period who were not reported as having central line–associated BSI were also assessed to see whether they met the definition of central line-associated BSI.
Results.Records of 108 patients were reviewed; the agreement between surveillance reports and the VICNISS assessment was 67.6% (κ = 0.31). Of the 46 reported central line–associated BSIs, 27 were confirmed to be central line–associated BSIs, for a positive predictive value of 59% (95% confidence interval [CI], 43%–73%). Of the 62 cases of bacteremia reviewed that were not reported as central line–associated BSIs, 45 were not associated with a central line, for a negative predictive value of 73% (95% CI, 60%–83%). Estimated sensitivity was 35%, and specificity was 87%. The positive likelihood ratio was 3.0, and the negative likelihood ratio was 0.72.
Discussion.The agreement between the reporting of central line–associated BSI and the gold standard application of definitions was unacceptably low. False-negative results were problematic; more than half of central line–associated BSIs may be missed in Victorian public hospitals.
Patients' Beliefs and Perceptions of Their Participation to Increase Healthcare Worker Compliance with Hand Hygiene
- Yves Longtin, Hugo Sax, Benedetta Allegranzi, Stéphane Hugonnet, Didier Pittet
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 830-839
-
- Article
- Export citation
-
Background.
Research suggests that patients could improve healthcare workers' compliance with hand hygiene recommendations by reminding them to cleanse their hands.
Objective.To assess patients' perceptions of a patient-participation program to improve healthcare workers' compliance with hand hygiene.
Design.Cross-sectional survey of patient knowledge and perceptions of healthcare-associated infections, hand hygiene, and patient participation, defined as the active involvement of patients in various aspects of their health care.
Setting.Large Swiss teaching hospital.
Results.Of 194 patients who participated, most responded that they would not feel comfortable asking a nurse (148 respondents [76%]) or a physician (150 [77%]) to perform hand hygiene, and 57 (29%) believed that this would help prevent healthcare-associated infections. In contrast, an explicit invitation from a healthcare worker to ask about hand hygiene doubled the intention to ask a nurse (from 34% to 83% of respondents; P < .001) and to ask a physician (from 30% to 78%; P < .001). In multivariate analysis, being nonreligious, having an expansive personality, being concerned about healthcare-associated infections, and believing that patient participation would prevent healthcare-associated infections were associated with the intention to ask a nurse or a physician to perform hand hygiene (P < .05). Being of Jewish, Eastern Orthodox, or Buddhist faith was associated also with increased intention to ask a nurse (P < .05), compared with being of Christian faith.
Conclusions.This study identifies several sociodemographic characteristics associated with the intention to ask nurses and physicians about hand hygiene and underscores the importance of a direct invitation from healthcare workers to increase patient participation and foster patient empowerment. These findings could guide the development of future hand hygiene-promotion strategies.
Variability in the Hawthorne Effect With Regard to Hand Hygiene Performance in High- and Low-Performing Inpatient Care Units
- Erol Kohli, Judy Ptak, Randall Smith, Eileen Taylor, Elizabeth A. Talbot, Kathryn B. Kirldand
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 222-225
-
- Article
- Export citation
-
Objective.
To determine the impact of known observers on hand hygiene performance in inpatient care units with differing baseline levels of hand hygiene compliance.
Design.Observational study.
Setting.Three inpatient care units, selected on the basis of past hand hygiene performance, in a hospital where hand hygiene observation and feedback are routine.
Participants.Three infection control practitioners (ICPs) and a student intern observed hospital staff.
Methods.Beginning in late 2005, the 3 ICPs, who were well known to the hospital staff, performed frequent, regular observations of hand hygiene in all 3 inpatient care units of the hospital, as part of routine surveillance. During the study period (January-May 2007), a student intern who was unknown to the hospital staff also performed observations of hand hygiene in the 3 inpatient care units. The rates of hand hygiene compliance observed by the 3 ICPs were compared with those observed by the student intern.
Results.The 3 ICPs observed 332 opportunities for hand hygiene during 15 observation periods, and the student intern observed 355 opportunities during 19 observation periods. The overall rate of hand hygiene compliance observed by the ICPs was 65% (ie, in 215 of the 332 opportunities, the performance of proper hand hygiene by hospital staff was observed), and the overall rate of hand hygiene compliance observed by the student intern was 58% (ie, in 207 of the 355 opportunities, the performance of proper hand hygiene by hospital staff was observed) (P = .1). Both the ICPs and the student intern were able to distinguish between inpatient care units with a high rate of hand hygiene compliance (hereafter referred to as high-performing units) and those with a low rate (hereafter referred to as low-performing units). However, in the 2 high-performing units, the ICPs observed significantly higher compliance rates than did the student intern, whereas in the low-performing unit, both the ICPs and the student intern measured similarly low rates of hand hygiene compliance.
Conclusions.Recognized observers are associated with higher rates of hand hygiene compliance, even in a healthcare setting where such observations have become routine. This effect (ie, the Hawthorne effect) is more pronounced in high-performing units and insignificant in low-performing units. The use of unrecognized observers may be important for verifying high performance but is probably unnecessary for documenting poor performance. Moreover, the Hawthorne effect may be a useful tool for sustaining and improving hand hygiene compliance.
Commentary
Article Commentary
The Graying of Methicillin-Resistant Staphylococcus aureus
- Kyle J. Popovich, Robert A. Weinstein
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 9-12
-
- Article
- Export citation
Original Articles
Mixture Model to Assess the Extent of Cross-Transmission of Multidrug-Resistant Pathogens in Hospitals
- Rafael T. Mikolajczyk, Göran Kauermann, Ulrich Sagel, Mirjam Kretzschmar
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 730-736
-
- Article
- Export citation
-
Objective.
Creation of a mixture model based on Poisson processes for assessment of the extent of cross-transmission of multidrug-resistant pathogens in the hospital.
Methods.We propose a 2-component mixture of Poisson processes to describe the time series of detected cases of colonization. The first component describes the admission process of patients with colonization, and the second describes the cross-transmission. The data set used to illustrate the method consists of the routinely collected records for methicillin-resistant Staphylococcus aureus (MRSA), imipenem-resistant Pseudomonas aeruginosa, and multidrug-resistant Acinetobacter baumannii over a period of 3 years in a German tertiary care hospital.
Results.For MRSA and multidrug-resistant A. baumannii, cross-transmission was estimated to be responsible for more than 80% of cases; for imipenem-resistant P. aeruginosa, cross-transmission was estimated to be responsible for 59% of cases. For new cases observed within a window of less than 28 days for MRSA and multidrug-resistant A. baumannii or 40 days for imipenem-resistant P. aeruginosa, there was a 50% or greater probability that the cause was cross-transmission.
Conclusions.The proposed method offers a solution to assessing of the extent of cross-transmission, which can be of clinical use. The method can be applied using freely available software (the package FlexMix in R) and it requires relatively little data.
Survey Study of the Knowledge, Attitudes, and Expected Behaviors of Critical Care Clinicians Regarding an Influenza Pandemic
- Elizabeth L. Daugherty, Trish M. Perl, Lewis Rubinson, Andrew Bilderback, Cynthia S. Rand
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 1143-1149
-
- Article
- Export citation
-
Objective.
Intensive care units (ICUs) are potential high-risk areas for the transmission of respiratory viruses such as influenza. An influenza pandemic is expected to result in a dramatic surge of critically ill patients, and ICU healthcare workers (HCW) are likely to be at high risk of infection.
Objective.To characterize the knowledge, attitudes, and expected behaviors of ICU HCWs concerning the risk of and response to an influenza pandemic.
Design, Participants, and Setting.A survey was distributed to 292 HCWs (ie, internal medicine house staff, pulmonary and critical care fellows and faculty members, nurses, and respiratory care professionals) at 2 hospitals in Baltimore, Maryland.
Results.Of the 292 HCWs, 256 (88%) completed the survey. Just over one-half of the respondents believed there is at least a 45% chance of an influenza pandemic within the next 5 years. However, only 41% reported knowing how to protect themselves during an outbreak. Despite this common belief that a pandemic is likely in the near future, 59% of those surveyed reported only minimal knowledge of the risks of and protective strategies for an influenza pandemic, and 20% reported being unlikely to report to work during a pandemic or being unsure about whether they would do so. The odds of reporting to work varied on the basis of race and responsibility for child care.
Conclusions.ICU HCWs reported having minimal knowledge concerning the risk of and response to an influenza pandemic, even though more that one-half of HCWs expect that a pandemic will occur in the near future. This finding in a high-risk setting is of concern, given that lack of knowledge among HCWs may result in increased nosocomial transmission to HCWs and patients. Interventions to improve knowledge of pandemics and understanding of risks among ICU HCWs are essential.
Surgical Hand Antisepsis With Alcohol-Based Hand Rub Comparison of Effectiveness After 1.5 and 3 Minutes of Application
- Walter P. Weber, Stefan Reck, Uschi Neff, Ramon Saccilotto, Marc Dangel, Manfred L. Rotter, Reno Frei, Daniel Oertli, Walter R. Marti, Andreas F. Widmer
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 420-426
-
- Article
- Export citation
-
Objective.
Research has shown 1.5 minutes of surgical hand antisepsis with alcohol-based hand rub to be at least as effective under experimental conditions as the 3-minute reference disinfection recommended by European Norm 12791. The aim of the present study was to validate the effectiveness of 1.5 minutes of surgical hand antisepsis in a clinical setting by comparing the effectiveness of 1.5- and 3-minute applications of alcohol-based hand rub (45% vol/vol 2-propanol, 30% vol/vol 1-propanol, and 0.2% mecetronium ethylsulphate).
Design.Prospective crossover trial in which each surgeon served as his or her own control, with individual randomization to the 1.5-or the 3-minute group during the first part of the trial.
Setting.Basel University Hospital, Switzerland.
Participants.Thirty-two surgeons with different levels of postdoctoral training.
Methods.We measured the bactericidal effectiveness of 1.5 minutes and 3 minutes of surgical hand antisepsis with alcohol-based hand rub by assessing the mean (± SD) log10 number of colony-forming units before the application of hand rub (baseline), after the application of hand rub (immediate effect), and after surgery (sustained effect) so as to follow European Norm 12791 as closely as possible.
Results.The immediate mean (± SD) log10 reduction in colony-forming units (cfu) was 2.66 ±1.13 log10 cfu for the 1.5-minute group and 3.01 ±1.06 log10 cfu for the 3-minute group (P = .204). Similarly, there was no statistically significant difference between the 2 groups with respect to the sustained effect; the mean ( ± SD) log10 increase in bacterial density during surgery was 1.08 ± 1.13 log10 cfu for the 1.5-minute group and 0.95 ± 1.27 log10 cfu for the 3-minute group (P = .708). No adverse effects were recorded.
Conclusion.In this clinical trial, surgical hand antisepsis with alcohol-based hand rub resulted in a similar bacterial reduction, regardless of whether it was applied for 3 or 1.5 minutes, which confirms experimental data generated with healthy volunteers.
Multicenter Study of the Impact of Community-Onset Clostridium difficile Infection on Surveillance for C. difficile Infection
- Erik R. Dubberke, Anne M. Butler, Bala Hota, Yosef M. Khan, Julie E. Mangino, Jeanmarie Mayer, Kyle J. Popovich, Kurt B. Stevenson, Deborah S. Yokoe, L. Clifford McDonald, John Jernigan, Victoria J. Fraser, Prevention Epicenters Program from the Centers for Disease Control and Prevention
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 518-525
-
- Article
- Export citation
-
Objective.
To evaluate the impact of cases of community-onset, healthcare facility (HCF)-associated Clostridium difficile infection (CDI) on the incidence and outbreak detection of CDI.
Design.A retrospective multicenter cohort study.
Setting.Five university-affiliated, acute care HCFs in the United States.
Methods.We collected data (including results of C. difficile toxin assays of stool samples) on all of the adult patients admitted to the 5 hospitals during the period from July I, 2000, through June 30, 2006. CDI cases were classified as HCF-onset if they were diagnosed more than 48 hours after admission or as community-onset, HCF-associated if they were diagnosed within 48 hours after admission and if the patient had recently been discharged from the HCF. Four surveillance definitions were compared: cases of HCF-onset CDI only (hereafter referred to as HCF-onset CDI) and cases of HCF-onset and community-onset, HCF-associated CDI diagnosed within 30, 60, and 90 days after the last discharge from the study hospital (hereafter referred to as 30-day, 60-day, and 90-day CDI, respectively). Monthly CDI rates were compared. Control charts were used to identify potential CDI outbreaks.
Results.The rate of 30-day CDI was significantly higher than the rate of HCF-onset CDI at 2 HCFs (P < .01 ). The rates of 30-day CDI were not statistically significantly different from the rates of 60-day or 90-day CDI at any HCF. The correlations between each HCF's monthly rates of HCF-onset CDI and 30-day CDI were almost perfect (ρ range, 0.94-0.99; P < .001). Overall, 12 time points had a CDI rate that was more than 3 standard deviations above the mean, including 11 time points identified using the definition for HCF-onset CDI and 9 time points identified using the definition for 30-day CDI, with discordant results at 4 time points (k = 0.794; P < .001).
Conclusions.Tracking cases of both community-onset and HCF-onset, HCF-associated CDI captures significantly more CDI cases, but surveillance of HCF-onset, HCF-associated CDI alone is sufficient to detect an outbreak.
Population-Based Surveillance of Clostridium difficile Infection in Manitoba, Canada, by Using Interim Surveillance Definitions
- Pascal J. Lambert, Myrna Dyck, Laura H. Thompson, Greg W. Hammond
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 945-951
-
- Article
- Export citation
-
Objective.
TO apply interim surveillance definitions of Clostridium difficile infection (CDI) cases to 1 year of data from the provincewide surveillance system of Manitoba, Canada, to determine the epidemiology of CDI incident cases in a population.
Methods.CDI cases were categorized with interim surveillance definitions developed by an ad hoc C. difficile surveillance working group. Incident cases recorded in the provincial CDI database between July 2005 and June 2006 were linked to the provincial hospitalization and nursing home databases and analyzed.
Results.One thousand six incident cases were identified over 1 year. Five hundred fifteen (51%) cases were associated with and began in a healthcare facility (HCF), whereas 275 (27%) were associated with and began in the community. An additional 131 (13%) cases were HCF associated but began in the community, while 85 (8%) were of indeterminate origin. Cases of HCF-associated CDI occurred in patients who were older than did cases of community-associated CDI (P < .0001). The provincial rate of community-onset cases was 23.4 per 100,000 person-years, and rates varied among geographic areas. HCF-associated CDI rates among the 10 largest hospitals varied from 0.5 to 8.4 per 10,000 patient-days. The time to CDI onset after hospital admission indicated that 25% of nosocomial cases began by the 8th day, and 50% began by the 17th day.
Conclusions.Although the majority of CDI cases were associated with exposure to a HCF, 40% of incident CDI began in the community. Populations with HCF- and community-associated CDI demonstrated significantly different age distributions. The wide variation of rates among HCFs requires explanation. The high percentage of incident cases in the community warrants increased study.
Impact of Finger Rings on Transmission of Bacteria During Hand Contact
- Mette Fagernes, Egil Lingaas
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 427-432
-
- Article
- Export citation
-
Objective.
To investigate the impact of finger rings on the transmission of bacteria from the hands of healthcare workers and the impact on the microflora on the hands of healthcare workers in clinical practice.
Design.Our study had a nonequivalent control group posttest-only design (pre-experimental). Healthcare workers who wore finger ring(s) on 1 hand and no ring on the other hand (n = 100) and a control group of healthcare workers who did not wear any rings (n = 100) exchanged standardized hand shakes with an investigator wearing sterile gloves. Samples from the gloved hands of the investigators and the bare hands of the healthcare workers were thereafter obtained by the glove juice technique.
Setting.Two Norwegian acute care hospitals.
Participants.Healthcare workers (n = 200) during ordinary clinical work.
Results.A significantly higher bacterial load (odds ratio, 2.63 [95% confidence interval, 1.28-5.43]; P = .009) and a significantly higher number of bacteria transmitted (odds ratio, 2.43 [95% confidence interval, 1.44-4.13]; P = .001) were associated with ringed hands, compared with control hands. However, a multiple analysis of covariance revealed no statistically significant effect of rings alone. The prevalence of nonfermentative gram-negative bacteria (42% vs 26%) and Enterobacteriaceae (26% vs 13%) was also significantly higher among persons who wore rings than among persons who did not wear rings. However, no statistically significant differences in the incidence of transmission of these pathogens were detected after hand contact. The prevalence of Staphylococcus aureus and incidence of transmission of S. aureus were the same in both groups.
Conclusions.Wearing finger rings increases the carriage rate of nonfermentative gram-negative bacteria and Enterobacteriaceae on the hands of healthcare workers. However, no statistically significant differences in the incidence of transmission of nonfermentative gram-negative bacteria or Enterobacteriaceae were detected between the healthcare workers who wore rings and those who did not.
Recovery of Both Vancomycin-Resistant Enterococci and Methicillin-Resistant Staphylococcus aureus From Culture of a Single Clinical Specimen From Colonized or Infected Patients
- Sang Hoon Han, Bum Sik Chin, Han Sung Lee, Su Jin Jeong, Hee Kyung Choi, Chang Ki Kim, Chang Oh Kim, Dongeun Yong, Jun Yong Choi, Young Goo Song, Kyungwon Lee, June Myung Kim
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 130-138
-
- Article
- Export citation
-
Objective.
To describe the incidence of recovery of both vancomycin-resistant enterococci (VRE) and methicillin-resistant Staphylococcus aureus (MRSA) from culture of a single clinical specimen, to describe the clinical characteristics of patients from whom these specimens were recovered, and to identify the risk factors of these patients.
Design.A retrospective cohort and case-control study.
Setting.A tertiary care university hospital and referral center in Seoul, Korea.
Methods.We identified 61 case patients for whom a single clinical specimen yielded both VRE and MRSA on culture, and 122 control patients for whom any clinical specimen yielded only VRE on culture. The control patients were selected by matching 2 :1 with the case patients for age, sex, and first date of sampling that led to isolation of VRE or both VRE and MRSA among 1,536 VRE-colonized patients from January 1, 2003, through December 31, 2006. To identify patient risk factors for the recovery of both VRE and MRSA in a single clinical specimen, we performed univariate comparisons between the 2 groups and then multivariate logistic regression analysis.
Results.The incidence of recovery of both VRE and MRSA from culture of a single clinical specimen was 3.97% (for 61 of 1,536 VRE-colonized patients) over 4 years. Among these 82 single clinical specimens, the most common type was wound specimens (26.8%), followed by lower respiratory tract specimens (18.3%), urine specimens (17.1%), and catheter tips (15.9%). Of the 61 case patients, 14 (23.0%) had 2 or more single clinical specimens that yielded both VRE and MRSA on culture, and the longest interval from the first sampling that yielded both organisms to the last sampling that yielded both was 174 days. Independent patient risk factors for the presence of both VRE and MRSA in a single clinical specimen were chronic renal disease (odds ratio [OR], 7.00; P = .012), urinary catheterization (OR, 3.36; P = .026), and longer total cumulative duration of hospital stay within the previous year (OR, 1.03; P < .001).
Conclusion.We confirmed that the recovery of VRE and MRSA from a single clinical specimen occurs continually. Because prolonged cell-to-cell contact can facilitate transfer of vanA, close observation and surveillance for vancomycin-resistant S. aureus, especially among patients with risk factors for the recovery of both VRE and MRSA from a single clinical specimen, should be continued.
French National Program for Prevention of Healthcare-Associated Infections and Antimicrobial Resistance, 1992–2008: Positive Trends, But Perseverance Needed
- Jean Carlet, Pascal Astagneau, Christian Brun-Buisson, Bruno Coignard, Valérie Salomon, Béatrice Tran, Jean-Claude Desenclos, Vincent Jarlier, Benoît Schlemmer, Pierre Parneix, Bernard Regnier, Jacques Fabry, French National Program for Prevention of Healthcare-Associated Infections and Antimicrobial Resistance
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 737-745
-
- Article
- Export citation
-
Objective.
To describe the French program for the prevention of healthcare-associated infections and antibiotic resistance and provide results for some of the indicators available to evaluate the program. In addition to structures and process indicators, the 2 outcome indicators selected were the rate of surgical site infection and the proportion of methicillin-resistant Staphylococcus aureus (MRSA) isolates among the S. aureus isolates recovered.
Design.Descriptive study of the evolution of the national structures for control of healthcare-associated infections since 1992. Through national surveillance networks, process indicators were available from 1993 to 2006, surgical site infection rates were available from 1999 to 2005, and prevalence rates for MRSA infection were available from 2001 to 2007.
Results.A comprehensive national program has gradually been set up in France during the period from 1993 to 2004, which included strengthening of organized infection control activities at the local, regional, and national levels and developing large networks for surveillance of specific infections and antibiotic resistance. These achievements were complemented by instituting mandatory notification for unusual nosocomial events, especially outbreaks. The second phase of the program involved the implementation of 5 national quality indicators with public reporting. Surgical site infection rates decreased by 25% over a 6-year period. In France, the median proportion of MRSA among S. aureus isolates recovered from patients with bacteremia decreased from 33.4% to 25.7% during the period from 2001 to 2007, whereas this proportion increased in many other European countries.
Conclusions.Very few national programs have been evaluated since the Study on the Efficacy of Nosocomial Infection Control. Although continuing efforts are required, the French program appears to have been effective at reducing infection rates.
Clostridium difficile Infection in Ohio Hospitals and Nursing Homes During 2006
- Robert J. Campbell, Lynn Giljahn, Kim Machesky, Katie Cibulskas-White, Lisa M. Lane, Kyle Porter, John O. Paulson, Forrest W. Smith, L. Clifford McDonald
-
- Published online by Cambridge University Press:
- 02 January 2015, pp. 526-533
-
- Article
- Export citation
-
Context.
Healthcare data suggest that the incidence and severity of Clostridium difficile infection (CDI) in hospitals are increasing. However, the overall burden of disease and the mortality rate associated with CDI, including the contribution from cases of infection that occur in nursing homes, are poorly understood.
Objective.To describe the epidemiology, disease burden, and mortality rate of healthcare-onset CDI.
Methods.In 2006, active public reporting of healthcare-onset CDI, using standardized case definitions, was mandated for all Ohio hospitals and nursing homes. Incidence rates were determined and stratified according to healthcare facility characteristics. Death certificates that listed CDI were analyzed for trends.
Results.There were 14,329 CDI cases reported, including 6,376 cases at 210 hospitals (5,217 initial cases [ie, cases identified more than 48 hours after admission to a healthcare facility in patients who had not had CDI during the previous 6 months] and 1,159 recurrent cases [ie, cases involving patients who had had CDI during the previous 6 months]) and 7,953 cases at 955 nursing homes (4,880 initial and 3,073 recurrent cases). After adjusting for missing data, the estimated total was 18,200 cases of CDI, which included 7,000 hospital cases (5,700 initial and 1,300 recurrent cases) and 11,200 nursing homes cases (6,900 initial and 4,300 recurrent cases). The rate for initial cases was 6.4-7.9 cases/10,000 patient-days for hospitals and 1.7-2.9 cases/10,000 patient-days for nursing homes. The rate for initial cases in nursing homes decreased during the study (P < .001). Nonpediatric hospital status (P = .011), a smaller number of beds (P = .003), and location in the eastern or northeastern region of the state (P = .011) were each independently associated with a higher rate of initial cases in hospitals. Death certificates for 2006 listed CDI among the causes of death for 893 Ohio residents; between 2000 and 2006, this number increased more than 4-fold.
Conclusion.Healthcare-onset CDI represents a major public health threat that, when considered in the context of an increasing mortality rate, should justify a major focus on prevention efforts.

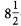 -year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9];
-year study period, the percentage of MDR gram-negative bacteria among bloodstream isolates increased from 2 (1%) of 199 to 34 (16%) of 216. Empiric therapy was ineffective for 38 (63%) of 60 patients with BSI caused by MDR gram-negative bacteria. The variables independently associated with BSI due to these bacteria were as follows: residency in a long-term care facility (odds ratio [OR], 4.9 [95% confidence interval {CI} 1.6–14.9];