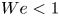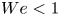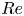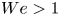47 results
On the shapes of liquid curtains flowing from a non-vertical slot
- Alessandro Della Pia, Michael G. Antoniades, Eleni S. Ioannidis, Zoe A. Wejko, Nathaniel S. Barlow, Matteo Chiatto, Steven J. Weinstein, Luigi de Luca
-
- Journal:
- Journal of Fluid Mechanics / Volume 974 / 10 November 2023
- Published online by Cambridge University Press:
- 26 October 2023, A18
-
- Article
- Export citation
-
A theoretical and experimental investigation of two-dimensional (2-D) liquid curtains (gravitationally thinning liquid sheets) is provided under conditions where the curtain issues from a thin slot whose centreline is inclined with respect to the vertical. This analysis is motivated in part by recent works where it has been proposed that oblique liquid curtains (those exiting a non-vertical slot) may bend upwards against gravity when the relevant Weber number at the slot is less than unity (
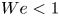 $We <1$). By contrast, Weinstein et al. (J. Fluid Mech., vol. 876, 2019, R3) have proposed that such
$We <1$). By contrast, Weinstein et al. (J. Fluid Mech., vol. 876, 2019, R3) have proposed that such 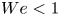 $We<1$ curtains must be vertical and downward falling regardless of the inclination of the slot. Under low-Reynolds-number (
$We<1$ curtains must be vertical and downward falling regardless of the inclination of the slot. Under low-Reynolds-number (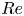 $Re$) conditions typical of liquid film coating operations, our experiments show that the curtain shape follows the classic ballistic (parabolic) trajectory in the supercritical regime (
$Re$) conditions typical of liquid film coating operations, our experiments show that the curtain shape follows the classic ballistic (parabolic) trajectory in the supercritical regime (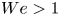 $We>1$). In subcritical conditions (
$We>1$). In subcritical conditions (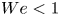 $We<1$), experiments show that the downward-falling curtain is vertical except in a relatively small region near the slot, where the combined effects of viscosity and surface tension induce the so-called teapot effect. These experimental results are confirmed by 2-D numerical simulations, which predict the curtain behaviour ranging from highly viscous (
$We<1$), experiments show that the downward-falling curtain is vertical except in a relatively small region near the slot, where the combined effects of viscosity and surface tension induce the so-called teapot effect. These experimental results are confirmed by 2-D numerical simulations, which predict the curtain behaviour ranging from highly viscous (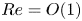 $Re = O(1)$) to nearly inviscid conditions. The one-dimensional (1-D) inviscid model of Weinstein et al. is recast in a different form to facilitate comparisons with the 2-D model, and 1-D and 2-D results agree favourably for supercritical and subcritical conditions. Despite the large parameter range explored, we have found no evidence that upward-bending curtains exist in an oblique configuration.
$Re = O(1)$) to nearly inviscid conditions. The one-dimensional (1-D) inviscid model of Weinstein et al. is recast in a different form to facilitate comparisons with the 2-D model, and 1-D and 2-D results agree favourably for supercritical and subcritical conditions. Despite the large parameter range explored, we have found no evidence that upward-bending curtains exist in an oblique configuration.
Molecular phylogenetic analysis of Neodiplostomum and Fibricola (Digenea, Diplostomidae) does not support host-based systematics
- Tyler J. Achatz, Eric E. Pulis, Ethan T. Woodyard, Thomas G. Rosser, Jakson R. Martens, Sara B. Weinstein, Alan Fecchio, Chris T. McAllister, Carlos Carrión Bonilla, Vasyl V. Tkach
-
- Journal:
- Parasitology / Volume 149 / Issue 4 / April 2022
- Published online by Cambridge University Press:
- 19 January 2022, pp. 542-554
-
- Article
- Export citation
-
Fibricola and Neodiplostomum are diplostomid genera with very similar morphology that are currently separated based on their definitive hosts. Fibricola spp. are normally found in mammals, while Neodiplostomum spp. typically parasitize birds. Previously, no DNA sequence data was available for any member of Fibricola. We generated nuclear ribosomal and mtDNA sequences of Fibricola cratera (type-species), Fibricola lucidum and 6 species of Neodiplostomum. DNA sequences were used to examine phylogenetic interrelationships among Fibricola and Neodiplostomum and re-evaluate their systematics. Molecular phylogenies and morphological study suggest that Fibricola should be considered a junior synonym of Neodiplostomum. Therefore, we synonymize the two genera and transfer all members of Fibricola into Neodiplostomum. Specimens morphologically identified as Neodiplostomum cratera belonged to 3 distinct phylogenetic clades based on mitochondrial data. One of those clades also included sequences of specimens identified morphologically as Neodiplostomum lucidum. Further study is necessary to resolve the situation regarding the morphology of N. cratera. Our results demonstrated that some DNA sequences of N. americanum available in GenBank originate from misidentified Neodiplostomum banghami. Molecular phylogentic data revealed at least 2 independent host-switching events between avian and mammalian hosts in the evolutionary history of Neodiplostomum; however, the directionality of these host-switching events remains unclear.
P01-246 - Self Esteem and Self Evaluation During Adolescence. The Contribution of the Rey-Weinstein
- M. Schweitzer, G. Weinstein, N. Puig-Verges
-
- Journal:
- European Psychiatry / Volume 25 / Issue S1 / 2010
- Published online by Cambridge University Press:
- 17 April 2020, 25-E452
-
- Article
-
- You have access Access
- Export citation
-
Numerous studies have focused on concepts of self esteem during the period of adolescence, but studies about self portrayal or self image are less frequent. They find their sources in the theories of the contemporary psychoanalytical schools about narcissism and “the Self”concept.
The reference to the “Self” is more frequently found in Anglo-Saxon studies. The focus is on the links between “The Self” and subjective experience as well as construction of personal identity in relation with developmental psychopathology. The construction of personal identity is due to a very complex process: the person has to figure up his own physical and psychic features and at the same time has to live in social interaction.
In reference to a developmental and psychogenetic approach, the interactions between the “Self” and the group will play an important role during the period of adolescence. It is necessary to focus on the identity process in reference with parental psychopathology and environment.
The contribution of the Rey- Weinstein test is focussed precisely on this double approach:
André Rey whose concerns were mainly on development and construction of personality created this test, modernized by G. Weinstein, both authors aiming to explore the field of
self image. By doing the test, the adolescent is asked to self evaluate himself on physical, intellectual, social and psychic features and to figure up how he would be evaluated by people surrounding him.
Projection of fears and desires, various levels of identifications sustain the self evaluation process and create a specific dynamic during the assessment.
In this clinical interactive prospect, the Rey Weinstein self evaluation test and in addition the
N. PUIG VERGES AND G.WEINSTEIN self portrait test contribute to the explore the self evaluation process and allow the adolescent to understand the way he lives, the way he builds his self experience and his own identity.
S10.02 - A Pet imaging study of the effects of modafinil and topiramate on brain mechanisms underlying cue-induced cocaine craving and dependence in cocaine-dependent and methadone maintained cocaine-dependent patients
- A. Weinstein, L. Karila, M. Sanchez, W. Lowenstein, G. Lambert, I. Herman, N. Freedman, R. Mishani, H. Atlan, R. Chisin
-
- Journal:
- European Psychiatry / Volume 23 / Issue S2 / April 2008
- Published online by Cambridge University Press:
- 16 April 2020, p. S16
-
- Article
-
- You have access Access
- Export citation
-
Although no pharmacological treatment has proved to be highly effective for reducing cocaine dependence, several medications have been tested over the last decade and have shown promising efficacy. Modafinil (Provigil), known as a treatment for day time sleepiness, and Topiramate (Topamax), an anti-epileptic medication also prescribed for migraine, have been shown to be effective in controlled clinical trials. We have recently started a major study utilizing Positron Emission Tomography (PET) brain imaging to monitor the progress of pharmacotherapy with modafinil or topiramate in cocaine-dependent and methadone-maintained cocaine-dependent patients. Patients will be assessed before treatment, and again after 4 weeks of pharmacotherapy. The aims of the project are to study effects of the two medications on cocaine dependence and craving, and on dopamine binding in the brain. At each assessment session, patients will undergo PET with [11C] raclopride to image the dopamine receptor DRD2. To trigger craving, patients will then be exposed to a videotape showing cocaine use; a questionnaire will be used to record their subjective responses, and a second PET scan will be performed with [18F] fluorodeoxyglucose (FDG) to image cerebral glucose metabolism during craving. This protocol was designed to enable us to study changes resulting from pharmacotherapy on dopamine binding in the brain, and on craving as reflected both in subjective measures and regional cerebral glucose metabolism. In addition, we will investigate the association between subjective measures of craving for cocaine and the level of dopamine DRD2 receptor occupancy in the brain before and after treatment. Notwithstanding the complexity of the clinical and therapeutic reality characterizing cocaine dependence, we hope to present preliminary evidence for the relative efficacy of these two promising medications in treatment for cocaine. dependence. This evidence could also elucidate the brain mechanisms underlying cocaine craving and dependence in cocaine-dependent patients.
Association between malaria incidence and meteorological factors: a multi-location study in China, 2005–2012
- J. XIANG, A. HANSEN, Q. LIU, M. X. TONG, X. LIU, Y. SUN, S. CAMERON, S. HANSON-EASEY, G. S. HAN, C. WILLIAMS, P. WEINSTEIN, P. BI
-
- Journal:
- Epidemiology & Infection / Volume 146 / Issue 1 / January 2018
- Published online by Cambridge University Press:
- 17 December 2017, pp. 89-99
-
- Article
-
- You have access Access
- HTML
- Export citation
-
This study aims to investigate the climate–malaria associations in nine cities selected from malaria high-risk areas in China. Daily reports of malaria cases in Anhui, Henan, and Yunnan Provinces for 2005–2012 were obtained from the Chinese Center for Disease Control and Prevention. Generalized estimating equation models were used to quantify the city-specific climate–malaria associations. Multivariate random-effects meta-regression analyses were used to pool the city-specific effects. An inverted-U-shaped curve relationship was observed between temperatures, average relative humidity, and malaria. A 1 °C increase of maximum temperature (Tmax) resulted in 6·7% (95% CI 4·6–8·8%) to 15·8% (95% CI 14·1–17·4%) increase of malaria, with corresponding lags ranging from 7 to 45 days. For minimum temperature (Tmin), the effect estimates peaked at lag 0 to 40 days, ranging from 5·3% (95% CI 4·4–6·2%) to 17·9% (95% CI 15·6–20·1%). Malaria is more sensitive to Tmin in cool climates and Tmax in warm climates. The duration of lag effect in a cool climate zone is longer than that in a warm climate zone. Lagged effects did not vanish after an epidemic season but waned gradually in the following 2–3 warm seasons. A warming climate may potentially increase the risk of malaria resurgence in China.
Pseudo-outbreak of Mycobacterium gordonae Following the Opening of a Newly Constructed Hospital at a Chicago Medical Center
- Kavitha Prabaker, Chethra Muthiah, Mary K. Hayden, Robert A. Weinstein, Jyothirmai Cheerala, Mary L. Scorza, John Segreti, Mary A. Lavin, Barbara A. Schmitt, Sharon F. Welbel, Kathleen G. Beavis, Gordon M. Trenholme
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 36 / Issue 2 / February 2015
- Published online by Cambridge University Press:
- 18 December 2014, pp. 198-203
- Print publication:
- February 2015
-
- Article
- Export citation
-
OBJECTIVE
To identify the source of a pseudo-outbreak of Mycobacterium gordonae
DESIGNOutbreak investigation.
SETTINGUniversity Hospital in Chicago, Ilinois.
PATIENTSHospital patients with M. gordonae-positive clinical cultures.
METHODSAn increase in isolation of M. gordonae from clinical cultures was noted immediately following the opening of a newly constructed hospital in January 2012. We reviewed medical records of patients with M. gordonae-positive cultures collected between January and December 2012 and cultured potable water specimens in new and old hospitals quantitatively for mycobacteria.
RESULTSOf 30 patients with M. gordonae-positive clinical cultures, 25 (83.3%) were housed in the new hospital; of 35 positive specimens (sputum, bronchoalveolar lavage, gastric aspirate), 32 (91.4%) had potential for water contamination. M. gordonae was more common in water collected from the new vs. the old hospital [147 of 157 (93.6%) vs. 91 of 113 (80.5%), P=.001]. Median concentration of M. gordonae was higher in the samples from the new vs. the old hospital (208 vs. 48 colony-forming units (CFU)/mL; P<.001). Prevalence and concentration of M. gordonae were lower in water samples from ice and water dispensers [13 of 28 (46.4%) and 0 CFU/mL] compared with water samples from patient rooms and common areas [225 of 242 (93%) and 146 CFU/mL, P<.001].
CONCLUSIONSM. gordonae was common in potable water. The pseudo-outbreak of M. gordonae was likely due to increased concentrations of M. gordonae in the potable water supply of the new hospital. A silver ion-impregnated 0.5-μm filter may have been responsible for lower concentrations of M. gordonae identified in ice/water dispenser samples. Hospitals should anticipate that construction activities may amplify the presence of waterborne nontuberculous mycobacterial contaminants.
Infect Control Hosp Epidemiol 2014;00(0): 1–6
About the authors
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp xviii-xxii
-
- Chapter
- Export citation
7 - Multiple test results
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 165-208
-
- Chapter
- Export citation
-
Summary
Even though the diagnostic radiologist examines black-and-white images, the information that is derived from the images is hardly ever black-and-white.
M.G. Myriam HuninkIntroduction
In the previous chapters we focused on dichotomous test results, e.g., fecal occult blood is either present or absent. Test results can conveniently be dichotomized, and thinking in terms of dichotomous test results is generally helpful. Distinguishing patients with and without the target disease is useful for the purpose of subsequent decision making because most medical actions are dichotomous. In reality, however, most test results have more than two possible outcomes. Test results can be categorical, ordinal, or continuous. For example, categories of a diagnostic imaging test may be defined by key findings on the images. These categories may be ordered (intuitively) according to the observer’s confidence in the diagnosis, based on the findings. As an example, abnormalities seen on mammography are commonly reported as definitely malignant, probably malignant, possibly malignant, probably benign, or definitely benign. As we shall see later in this chapter, it makes sense to order the categories (explicitly) according to increasing likelihood ratio (LR). Some test results are inherently ordinal, e.g., the five categories of a Papanicolaou smear (test for cervical cancer) are ordinal. Results of biochemical tests are usually given on a continuous scale, which may be reduced to an ordinal scale by grouping the test results. Thus, a test result on a continuous scale can be considered a result on an ordinal scale with an infinite number of very narrow categories. Scores from prediction models are on an ordinal scale if there are a finite number of possible scores, and on a continuous scale if there are an infinite number of scores. When test results are categorical, ordinal, or continuous, we have to consider many test results Ri, where i can be any value from two (the case we have considered in Chapter 5 and Chapter 6, T+ and T−) up to any number of categories. Interpretation of a test result on an ordinal scale can be considered a generalization of the situation of dichotomous test results.
2 - Managing uncertainty
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 29-52
-
- Chapter
- Export citation
-
Summary
Much of medical training consists of learning to cope with pervasive uncertainty and with the limits of medical knowledge. Making serious clinical decisions on the basis of conflicting, incomplete, and untimely data is routine.
J.D. McCueIntroduction
Much of clinical medicine and health care involves uncertainties: some reducible, but some irreducible despite our best efforts and tests. Better decisions will be made if we are open and honest about these uncertainties, and develop skills in estimating, communicating, and working with such uncertainties. What types of uncertainty exist? Consider the following example.
Needlestick injury:
It has been a hard week. It is time to go home when you are called to yet another heroin overdose: a young woman has been found unconscious outside your clinic. After giving intravenous (IV) naloxone (which reverses the effects of heroin), you are accidentally jabbed by the needle. After her recovery, despite your reassurances, the young woman flees for fear of the police. As the mêlée settles, the dread of human immunodeficiency virus (HIV) infection begins to develop. You talk to the senior doctor about what you should do. She is very sympathetic, and begins to tell you about the risks and management. The good news is that, even if the patient was HIV-positive, a needlestick injury rarely leads to HIV infection (about 3 per 1000). And if she was HIV-positive then a basic two-drug regime of antivirals such as zidovudine (AZT) plus lamivudine are likely to be able to prevent most infections (perhaps 80%).
Unfortunately, the HIV status of the young woman who had overdosed is unknown. Since she was not a patient of your clinic, you are uncertain about whether she is infected, but think that it is possible since she is an IV drug user. The Centers for Disease Control and Prevention (CDC) guidelines (1) suggest: ‘If the exposure source is unknown, use of post-exposure prophylaxis should be decided on a case-by-case basis. Consider the severity of exposure and the epidemiologic likelihood of HIV.’ What do you do?
Dedication
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp v-vi
-
- Chapter
- Export citation
11 - Estimation, calibration, and validation
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 334-355
-
- Chapter
- Export citation
-
Summary
Essentially, all models are wrong, but some are useful.
George E. P. BoxIntroduction
As discussed in Chapter 8, ‘good decision analyses depend on both the veracity of the decision model and the validity of the individual data elements.’ The validity of each individual data element relies on the comprehensiveness of the literature search for the best and most appropriate study or studies, criteria for selecting the source studies, the design of the study or studies, and methods for synthesizing the data from multiple sources. Nonetheless, Sir Michael David Rawlins avers that ‘Decision makers have to incorporate judgements, as part of their appraisal of the evidence, in reaching their conclusions. Such judgements relate to the extent to which each of the components of the evidence base is “fit for purpose.” Is it reliable?’(1) Because the integration of a multitude of these ‘best available’ data elements forms the basis for model results, some individuals refer to decision analyses as black boxes, so this last question applies particularly to the overall model predictions. Consequently, assessing model validity becomes paramount. However, prior to assessing model validity, model construction requires attention to parameter estimation and model calibration. This chapter focuses on parameter estimation, calibration, and validation in the context of Markov and, more generally, state-transition models (Chapter 10) in which recurrent events may occur over an extended period of time. The process of parameter estimation, calibration, and validation is iterative: it involves both adjustment of the data to fit the model and adjustment of the model to fit the data.
Parameter estimation
Survival analysis involves determining the probability that an event such as death or disease progression will occur over time. The events modeled in survival analysis are called ‘failure’ events, because once they occur, they cannot occur again. ‘Survival’ is the absence of the failure event. The failure event may be death, or it may be death combined with a non-fatal outcome such as developing cancer or having a heart attack, in which case the absence of the event is referred to as event-free survival. Commonly used methods for survival analysis include life-table analysis, Kaplan–Meier product limit estimates, and Cox proportional hazards models. A survival curve plots the probability of being alive over time (Figure 11.1).
3 - Choosing the best treatment
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 53-77
-
- Chapter
- Export citation
-
Summary
Firstly, do no (net) harm.
(adapted from) HippocratesIntroduction
Some treatment decisions are straightforward. For example, what should be done for an elderly patient with a fractured hip? Inserting a metal pin has dramatically altered the management: instead of lying in bed for weeks or months waiting for the fracture to heal while blood clots and pneumonia threatened, the patient is now ambulatory within days. The risks of morbidity and mortality are both greatly reduced. However, many treatment decisions are complex. They involve uncertainties and trade-offs that need to be carefully weighed before choosing. Tragic outcomes may occur no matter which choice is made, and the best that can be done is to minimize the overall risks. Such decisions can be difficult and uncomfortable to make. For example, consider the following historical dilemma.
Benjamin Franklin and smallpox
Benjamin Franklin argued implicitly in favor of the application to individual patients of probabilities based on previous experience with similar groups of patients. Before Edward Jenner’s discovery in 1796 of cowpox vaccination for smallpox, it was known that immunity from smallpox could be achieved by a live smallpox inoculation, but the procedure entailed a risk of death. When a smallpox epidemic broke out in Boston in 1721, the physician Zabdiel Boylston consented, at the urging of the clergyman Cotton Mather, to inoculate several hundred citizens. Mather and Boylston reported their results (1):
Out of about ten thousand Bostonians, five thousand seven hundred fifty-nine took smallpox the natural way. Of these, eight hundred eighty-five died, or one in seven. Two hundred eighty-six took smallpox by inoculation. Of these, six died, or one in forty-seven.
5 - Interpreting diagnostic information
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 118-144
-
- Chapter
- Export citation
-
Summary
The interpretation of new information depends on what was already known about the patient.
Harold SoxDiagnostic information and probability revision
Physicians have at their disposal an enormous variety of diagnostic information to guide them in decision making. Diagnostic information comes from talking to the patient (symptoms, such as pain, nausea, and breathlessness), examining the patient (signs, such as abdominal tenderness, fever, and blood pressure), and from diagnostic tests (such as blood tests, X-rays, and electrocardiograms (ECGs)) and screening tests (such as Papanicolaou smears for cervical cancer or cholesterol measurements).
Physicians are not the only ones that have to interpret diagnostic information. Public policy makers in health care are equally concerned with understanding the performance of diagnostic tests. If, for example, a policy maker is considering a screening program for lung cancer, he/she will need to understand the performance of the diagnostic tests that can detect lung cancer in an early phase of the disease. In public policy making, other types of ‘diagnostic tests’ may also be relevant. For example, a survey with a questionnaire in a population sample can be considered analogous to a diagnostic test. And performing a trial to determine the efficacy of a treatment is in fact a ‘test’ with the goal of getting more information about that treatment.
list of Abbreviations
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp xvi-xvii
-
- Chapter
- Export citation
6 - Deciding when to test
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 145-164
-
- Chapter
- Export citation
-
Summary
Before ordering a test ask: What will you do if the test is positive? What will you do if the test is negative? If the answers are the same, then don’t do the test.
Poster in an Emergency DepartmentIntroduction
In the previous chapter we looked at how to interpret diagnostic information such as symptoms, signs, and diagnostic tests. Now we need to consider when such information is helpful in decision making. Even if they reduce uncertainty, tests are not always helpful. If used inappropriately to guide a decision, a test may mislead more than it leads. In general, performing a test to gain additional information is worthwhile only if two conditions hold: (1) at least one decision would change given some test result, and (2) the risk to the patient associated with the test is less than the expected benefit that would be gained from the subsequent change in decision. These conditions are most likely to be fulfilled when we are confronted with intermediate probabilities of the target disease, that is, when we are in a diagnostic ‘gray zone.’ Tests are least likely to be helpful either when we are so certain a patient has the target disease that the negative result of an imperfect test would not dissuade us from treating, or, conversely, when we are so certain that the patient does not have the target disease that a positive result of an imperfect test would not persuade us to treat. These concepts are illustrated in Figure 6.1, which divides the probability of a disease into three ranges:
do not treat (for the target disease) and do not test, because even a positive test would not persuade us to treat;
test, because the test will help with treatment decisions or with follow-up; and
treat and do not test, because even a negative test would not dissuade us from treating.
Treat implies patient management as if disease is present and may imply initiating medical therapy, performing a therapeutic procedure, advising a lifestyle or other adjuvant intervention, or a combination of these. Do not treat implies patient management as if disease is absent and usually means risk factor management, lifestyle advice, self-care and/or watchful waiting.
1 - Elements of decision making in health care
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 1-28
-
- Chapter
- Export citation
-
Summary
And take the case of a man who is ill. I call two physicians: they differ in opinion. I am not to lie down and die between them: I must do something.
Samuel JohnsonIntroduction
How are decisions made in practice, and can we improve the process? Decisions in health care can be particularly awkward, involving a complex web of diagnostic and therapeutic uncertainties, patient preferences and values, and costs. It is not surprising that there is often considerable disagreement about the best course of action. One of the authors of this book tells the following story (1):
Being a cardiovascular radiologist, I regularly attend the vascular rounds at the University Hospital. It’s an interesting conference: the Professor of Vascular Surgery really loves academic discussions and each case gets a lot of attention. The conference goes on for hours. The clinical fellows complain, of course, and it sure keeps me from my regular work. But it’s one of the few conferences that I attend where there is a real discussion of the risks, benefits, and costs of the management options. Even patient preferences are sometimes (albeit rarely) considered.
And yet, I find there is something disturbing about the conference. The discussions always seem to go along the same lines. Doctor R. advocates treatment X because he recently read a paper that reported wonderful results; Doctor S. counters that treatment X has a substantial risk associated with it, as was shown in another paper published last year in the world’s highest-ranking journal in the field; and Doctor T. says that given the current limited health-care budget maybe we should consider a less expensive alternative or no treatment at all. They talk around in circles for ten to 15 minutes, each doctor reiterating his or her opinion. The professor, realizing that his fellows are getting irritated, finally stops the discussion. Practical chores are waiting; there are patients to be cared for. And so the professor concludes: ‘All right. We will offer the patient treatment X.’ About 30% of those involved in the decision-making process nod their heads in agreement; another 30% start bringing up objections which get stifled quickly by the fellows who really do not want an encore, and the remaining 40% are either too tired or too flabbergasted to respond, or are more concerned about another objective, namely their job security.
Contents
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp vii-vii
-
- Chapter
- Export citation
8 - Finding and summarizing the evidence
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 209-236
-
- Chapter
- Export citation
-
Summary
It is surely a great criticism of our profession that we have not organized a critical summary, by specialty or subspecialty, adapted periodically, of all relevant randomized controlled trials.
Archie CochraneIntroduction
Good decision analyses depend on both the veracity of the decision model and on the validity of the individual data elements. These elements may include probabilities (such as the pre-test probabilities, the sensitivity and specificity of diagnostic tests, the probability of an adverse event, and so on), estimates of effectiveness of interventions (such as the relative risk reduction), and the valuation of outcomes (such as quality of life, utilities, and costs). Often we lack the information needed for a confident assessment of these elements. Decision analysis, by structuring a decision problem, makes these gaps in knowledge apparent. Sensitivity analysis on these ‘soft’ numbers will also give us insight into which of these knowledge gaps is most likely to affect our decisions. These same gaps exist in less systematic decision making as well, but there is no convenient way to determine how our decisions should be affected. In this chapter we shall cover the basic methods for finding the best estimate for each of the different elements that may be included in a formal decision analysis or in less systematic decision making.
Sometimes, but not as often as one would like, the estimates one is looking for can be inferred from a published study or from a series of cases that someone has reported in the literature or recorded in a data bank. This is generally considered the most satisfactory way of assessing a probability, because it involves the use of quantitative evidence. Often we will have a choice of data sources, so it is useful to have some ‘rules’ to guide the choice of possible estimates. One helpful concept is the ‘hierarchy of evidence’ (see www.cebm.net) which explicitly ranks the available evidence; ‘perfect’ data will rarely be available, but we need to know how to choose the best from the available imperfect data. This choice will also need to be tempered by the practicalities and purpose of each decision analysis: what is feasible will differ with a range from the urgent individual patient decision to a national policy decision to fund an expensive new procedure.
4 - Valuing outcomes
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp 78-117
-
- Chapter
- Export citation
-
Summary
Values are what we care about. As such, values should be the driving force for our decision making. They should be the basis for the time and effort we spend thinking about decisions. But this is not the way it is. It is not even close to the way it is.
Ralph KeeneyIntroduction
Value judgments underlie virtually all clinical decisions. Sometimes the decision rests on a comparison of probability alone, such as the probability of surviving an acute episode of illness. In such cases, there is a single outcome measure – the probability of immediate survival – that can be averaged out to arrive at an optimal decision. In most cases, however, decisions between alternative strategies require not only estimates of the probabilities of the associated outcomes, but also value judgments about how to weigh the benefits versus the harms, and how to incorporate other factors like individual preferences for convenience, timing, who makes decisions, who else is affected by the decision, and the like. Consider the following examples.
Frontmatter
- M. G. Myriam Hunink, Erasmus Universiteit Rotterdam, Milton C. Weinstein, Harvard University, Massachusetts, Eve Wittenberg, Michael F. Drummond, University of York, Joseph S. Pliskin, Ben-Gurion University of the Negev, Israel, John B. Wong, Tufts University, Massachusetts, Paul P. Glasziou, Bond University, Queensland
-
- Book:
- Decision Making in Health and Medicine
- Published online:
- 05 October 2014
- Print publication:
- 16 October 2014, pp i-iv
-
- Chapter
- Export citation