87 results
Ten new insights in climate science 2023
- Mercedes Bustamante, Joyashree Roy, Daniel Ospina, Ploy Achakulwisut, Anubha Aggarwal, Ana Bastos, Wendy Broadgate, Josep G. Canadell, Edward R. Carr, Deliang Chen, Helen A. Cleugh, Kristie L. Ebi, Clea Edwards, Carol Farbotko, Marcos Fernández-Martínez, Thomas L. Frölicher, Sabine Fuss, Oliver Geden, Nicolas Gruber, Luke J. Harrington, Judith Hauck, Zeke Hausfather, Sophie Hebden, Aniek Hebinck, Saleemul Huq, Matthias Huss, M. Laurice P. Jamero, Sirkku Juhola, Nilushi Kumarasinghe, Shuaib Lwasa, Bishawjit Mallick, Maria Martin, Steven McGreevy, Paula Mirazo, Aditi Mukherji, Greg Muttitt, Gregory F. Nemet, David Obura, Chukwumerije Okereke, Tom Oliver, Ben Orlove, Nadia S. Ouedraogo, Prabir K. Patra, Mark Pelling, Laura M. Pereira, Åsa Persson, Julia Pongratz, Anjal Prakash, Anja Rammig, Colin Raymond, Aaron Redman, Cristobal Reveco, Johan Rockström, Regina Rodrigues, David R. Rounce, E. Lisa F. Schipper, Peter Schlosser, Odirilwe Selomane, Gregor Semieniuk, Yunne-Jai Shin, Tasneem A. Siddiqui, Vartika Singh, Giles B. Sioen, Youba Sokona, Detlef Stammer, Norman J. Steinert, Sunhee Suk, Rowan Sutton, Lisa Thalheimer, Vikki Thompson, Gregory Trencher, Kees van der Geest, Saskia E. Werners, Thea Wübbelmann, Nico Wunderling, Jiabo Yin, Kirsten Zickfeld, Jakob Zscheischler
-
- Journal:
- Global Sustainability / Volume 7 / 2024
- Published online by Cambridge University Press:
- 01 December 2023, e19
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Non-technical summary
We identify a set of essential recent advances in climate change research with high policy relevance, across natural and social sciences: (1) looming inevitability and implications of overshooting the 1.5°C warming limit, (2) urgent need for a rapid and managed fossil fuel phase-out, (3) challenges for scaling carbon dioxide removal, (4) uncertainties regarding the future contribution of natural carbon sinks, (5) intertwinedness of the crises of biodiversity loss and climate change, (6) compound events, (7) mountain glacier loss, (8) human immobility in the face of climate risks, (9) adaptation justice, and (10) just transitions in food systems.
Technical summaryThe Intergovernmental Panel on Climate Change Assessment Reports provides the scientific foundation for international climate negotiations and constitutes an unmatched resource for researchers. However, the assessment cycles take multiple years. As a contribution to cross- and interdisciplinary understanding of climate change across diverse research communities, we have streamlined an annual process to identify and synthesize significant research advances. We collected input from experts on various fields using an online questionnaire and prioritized a set of 10 key research insights with high policy relevance. This year, we focus on: (1) the looming overshoot of the 1.5°C warming limit, (2) the urgency of fossil fuel phase-out, (3) challenges to scale-up carbon dioxide removal, (4) uncertainties regarding future natural carbon sinks, (5) the need for joint governance of biodiversity loss and climate change, (6) advances in understanding compound events, (7) accelerated mountain glacier loss, (8) human immobility amidst climate risks, (9) adaptation justice, and (10) just transitions in food systems. We present a succinct account of these insights, reflect on their policy implications, and offer an integrated set of policy-relevant messages. This science synthesis and science communication effort is also the basis for a policy report contributing to elevate climate science every year in time for the United Nations Climate Change Conference.
Social media summaryWe highlight recent and policy-relevant advances in climate change research – with input from more than 200 experts.
Coronavirus disease 2019 is associated with long-term depressive symptoms in Spanish older adults with overweight/obesity and metabolic syndrome
- Sangeetha Shyam, Carlos Gómez-Martínez, Indira Paz-Graniel, José J. Gaforio, Miguel Ángel Martínez-González, Dolores Corella, Montserrat Fitó, J. Alfredo Martínez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque, Dora Romaguera, José López-Miranda, Ramon Estruch, Francisco J. Tinahones, José Manuel Santos-Lozano, J. Luís Serra-Majem, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín Sánchez, Xavier Pintó, María Ortiz Ramos, Josep Vidal, Maria Mar Alcarria, Lidia Daimiel, Emilio Ros, Fernando Fernandez-Aranda, Stephanie K. Nishi, Oscar García Regata, Estefania Toledo, Jose V. Sorli, Olga Castañer, Antonio Garcia-Rios, Rafael Valls-Enguix, Napoleon Perez-Farinos, M. Angeles Zulet, Elena Rayó-Gago, Rosa Casas, Mario Rivera-Izquierdo, Lucas Tojal-Sierra, Miguel Damas-Fuentes, Pilar Buil-Cosiales, Rebeca Fernández-Carrion, Albert Goday, Patricia J. Peña-Orihuela, Laura Compañ-Gabucio, Javier Diez-Espino, Susanna Tello, Ana González-Pinto, Víctor de la O, Miguel Delgado-Rodríguez, Nancy Babio, Jordi Salas-Salvadó
-
- Journal:
- Psychological Medicine / Volume 54 / Issue 3 / February 2024
- Published online by Cambridge University Press:
- 05 September 2023, pp. 620-630
-
- Article
- Export citation
-
Background
The coronavirus disease 2019 (COVID-19) has serious physiological and psychological consequences. The long-term (>12 weeks post-infection) impact of COVID-19 on mental health, specifically in older adults, is unclear. We longitudinally assessed the association of COVID-19 with depression symptomatology in community-dwelling older adults with metabolic syndrome within the framework of the PREDIMED-Plus cohort.
MethodsParticipants (n = 5486) aged 55–75 years were included in this longitudinal cohort. COVID-19 status (positive/negative) determined by tests (e.g. polymerase chain reaction severe acute respiratory syndrome coronavirus 2, IgG) was confirmed via event adjudication (410 cases). Pre- and post-COVID-19 depressive symptomatology was ascertained from annual assessments conducted using a validated 21-item Spanish Beck Depression Inventory-II (BDI-II). Multivariable linear and logistic regression models assessed the association between COVID-19 and depression symptomatology.
ResultsCOVID-19 in older adults was associated with higher post-COVID-19 BDI-II scores measured at a median (interquartile range) of 29 (15–40) weeks post-infection [fully adjusted β = 0.65 points, 95% confidence interval (CI) 0.15–1.15; p = 0.011]. This association was particularly prominent in women (β = 1.38 points, 95% CI 0.44–2.33, p = 0.004). COVID-19 was associated with 62% increased odds of elevated depression risk (BDI-II ≥ 14) post-COVID-19 when adjusted for confounders (odds ratio; 95% CI 1.13–2.30, p = 0.008).
ConclusionsCOVID-19 was associated with long-term depression risk in older adults with overweight/obesity and metabolic syndrome, particularly in women. Thus, long-term evaluations of the impact of COVID-19 on mental health and preventive public health initiatives are warranted in older adults.
Psychiatric Comorbidity and Length of Stay in a general hospital
- R. Fernández Fernández, P. del Sol Calderón, Á. Izquierdo de la Puente, R. Blanco Fernández, M. Martín García
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S588-S589
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychiatric comorbidity has a significant impact on the patient’s overall health, with an increased risk of death for those patients with mental-physical comorbidity (Tan et al., 2021). This impacts, among other things, the average hospital stay of a patient with psychiatric comorbidity. For example, an American study shows that psychiatric comorbidity was associated with greater inpatient utilization, including the risk of additional hospitalizations, days of stay, and hospitalization charges (Sayers et al., 2007). Our study aims to confirm these results in patients admitted to a general hospital for any cause and presenting psychiatric comorbidity.
ObjectivesTo compare the mean length of stay of patients admitted to a general hospital for any cause according to whether they have psychiatric comorbidity or not.
MethodsWe made a descriptive retrospective study through the use of electronic medical records. The drug use history and average day of hospitalization were obtained for all patients admitted to the inpatient service of a general hospital during a 3-year period.
ResultsThe mean length of stay was longer in patients with psychiatric comorbidity (mean = 9.87 days, SD = 15.45) than in patients without psychiatric comorbidity (mean = 5.23 days, SD = 7.16), the difference being statistically significant for the analysis of variance with a small effect size (F = 18.2; p < 0.001, η²=0.038). The assumption of the equality of variances of the two groups is not fulfilled (Levene F = 29.0; p < 0.01) so Welch’s nonparametric test was applied, whose results do not modify those obtained.
N Mean SD SE No psychiatric comorbidity 296 5.23 7.16 0.416 Psychiatric comorbidity 238 9.87 15.45 1.002 ConclusionsOur results are in line with other studies, showing a longer mean length of stay in those patients admitted for any cause and with associated psychiatric comorbidity. This highlights the importance of having an integrated psychiatry service in a general hospital, as Bronson points out, where they find a shorter mean length of stay in units that have integrated, proactive psychiatric care (Bronson et al., 2019).
ReferencesBronson, B. D., Alam, A., & Schwartz, J. E. (2019). The Impact of Integrated Psychiatric Care on Hospital Medicine Length of Stay: A Pre-Post Intervention Design With a Simultaneous Usual Care Comparison. Psychosomatics.
Sayers, S. L., Hanrahan, N., Kutney, A., Clarke, S. P., Reis, B. F., & Riegel, B. (2007). Psychiatric comorbidity and greater hospitalization risk, longer length of stay, and higher hospitalization costs in older adults with heart failure. Journal of the American Geriatrics Society.
Tan, X. W., Lee, E. S., Toh, M., Lum, A., Seah, D., Leong, K. P., Chan, C., Fung, D., & Tor, P. C. (2021). Comparison of mental-physical comorbidity, risk of death and mortality among patients with mental disorders - A retrospective cohort study. Journal of psychiatric research.
Disclosure of InterestNone Declared
Does intensive home treatment change treatment trajectories of psychiatric disorders?
- A. Martín-Blanco, A. González-Fernández, A. Farré, S. Vieira, P. Alvaro, C. Isern, D. Giménez, C. Torres, V. de la Cruz, C. Martín, N. Moll, O. Castro, M. Sagué-Vilavella
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S167-S168
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Intensive home treatment (IHT) for people experiencing a mental health crisis has been progressively established in many western countries as an alternative to in-ward admission. But is this a real alternative? We previously reported that patients treated in our IHT unit only differ from those voluntarily admitted to hospital in suicidal risk and severe behaviour disorders (not in other factors such as clinical severity) (Martín-Blanco et al., Rev Psiquiatr Salud Ment 2022;15:213-5). Now we are interested in disentangle if those patients who used to require inward management can be successfully treated at home.
ObjectivesTo describe subsequent treatment trajectories of the first 1000 admissions to our IHT unit and to compare clinical characteristics among the different groups of trajectories.
MethodsRetrospective cohort study. Subsequent treatment trajectories were collected from December 2016 to October 2022 and classified: absence, hospital, IHT, and mixed (hospital and IHT). Statistical significance was tested by means of ANOVA or Kruskal-Wallis test for quantitative variables (corrected for multiple comparisons) and chi-square tests for qualitative variables.
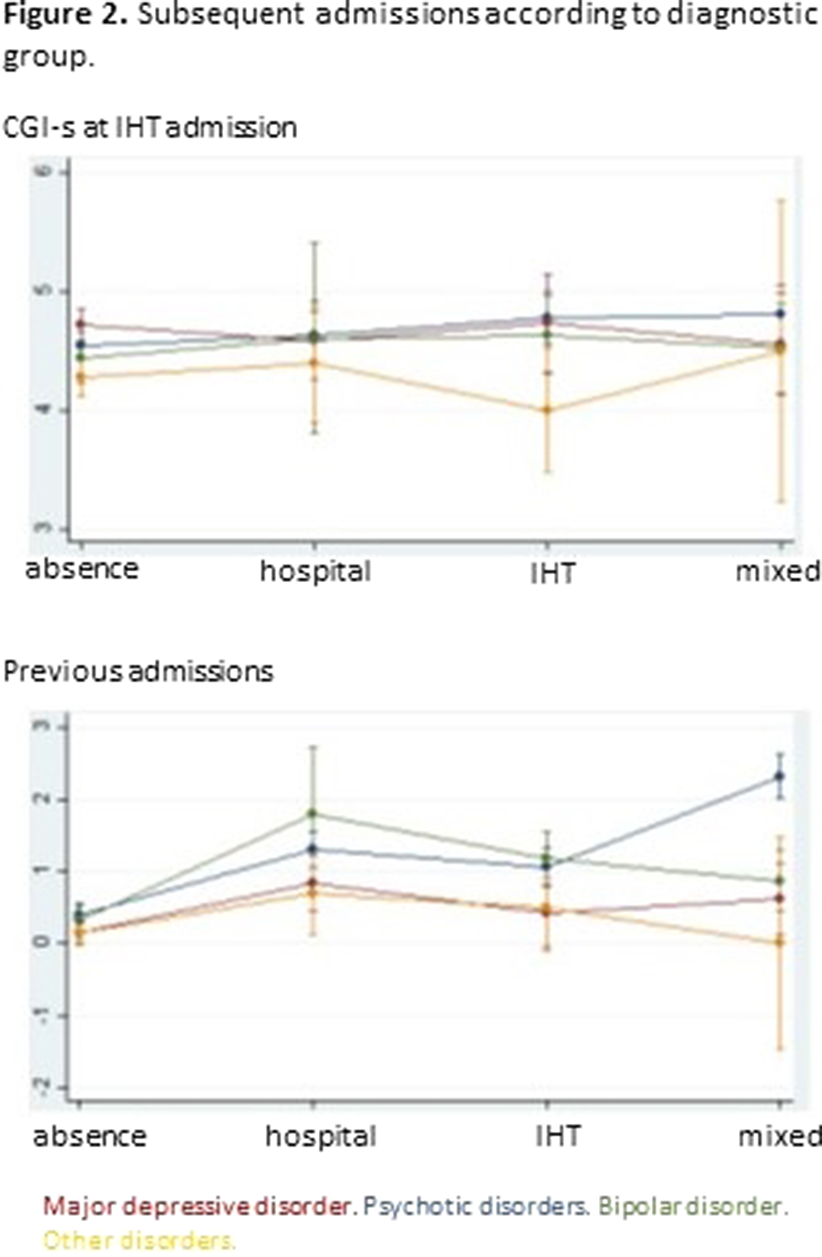
ResultsTables 1 shows the characteristics of the whole sample. Of the 1000 IHT admissions, 12.1% needed subsequent hospital admission(s), 12.7% IHT admission(s), and 9.3% mixed admission(s). There were no differences among these groups in median severity at IHT admission, but there were differences in the number of previous admissions (p=0.0001): the group with no subsequent admissions had less previous admissions than the other groups (pBonf<0.0001), and the group with subsequent IHT admissions had less than the group with mixed admissions (pBonf=0.0123). There were differences between groups regarding distribution of diagnoses (p<0.0001) (Fig. 1). When considering subsequent admissions by diagnosis, there were differences in severity at IHT admission (p=0.0068) and in number of previous hospitalizations (p<0.0001) (Fig. 2).
Table 1. Clinical characteristics of the whole sample (N=1000) mean SD Age (years) 47.07 17.02 CGI-s at admission * 5 4-5 N % Sex (female) 548 54.8% Psychotic disorders 463 46.3% Affective disorder 257 25.7% Bipolar disorder 128 12.8% Other disorders 152 15.2% Hospital admission in the previous 5 years 313 31.3% CGI-s: clinical global impression - severity. * median and IQR
Image:
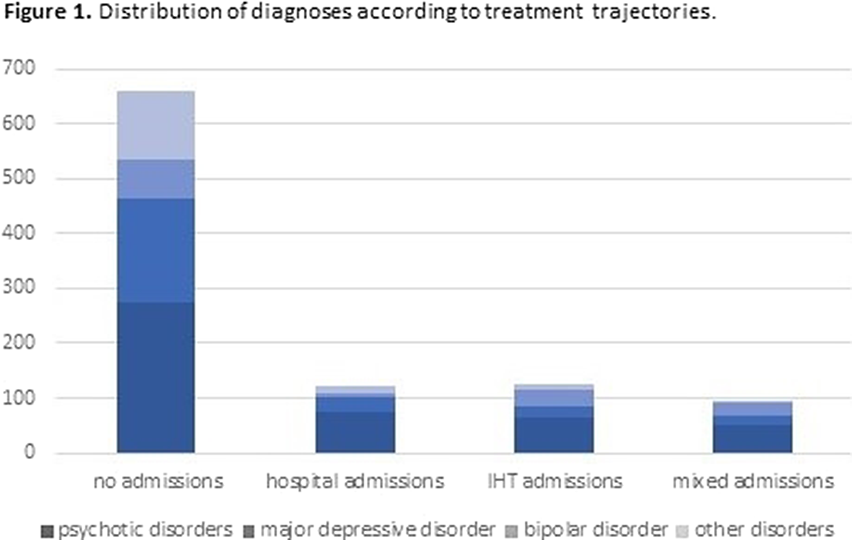
Image 2:
 Conclusions
ConclusionsPatients that used to require inward management can now be treated at home when suffering an acute episode. Therefore, IHT has changed treatment trajectories for some patients with psychiatric disorders.
Disclosure of InterestNone Declared
Relationship between dementia and depression: a case series
- A. Izquierdo De La Puente, P. del Sol Calderón, R. Fernández Fernádez, A. Rodríguez Rodriguez, M. Vizcaíno Da Silva, M. Martín García, O. Médez Gonzalez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S825
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Four cases are presented who debut with depressive episodes and after close follow-up, are diagnosed and treated for Alzheimer’s disease
ObjectivesThe aim of this case series is to give a brief review of the depressive prodrome of dementia.
MethodsFour women, aged 67-77 years, treated on an outpatient basis, consulted for depressive symptoms. In addition to affective symptoms such as apathy, lack of interest, sadness, increased emotional lability and anhedonia, all three reported cognitive impairment. In their follow-up after two years, they became progressively more dependent on their partners, with more memory lapses, forgetfulness and progressive loss of higher cognitive functions. With the progression of cognitive impairment, anxious symptoms have become increasingly present.
ResultsThe mean age of the patients is 70 years. Two of them had an insidious onset of depressive symptoms, while the other two had a psychotic onset of depression. None of the patients had no previous history of depression. All four were started on antidepressant treatment with little response. Following the diagnosis of cognitive impairment, treatment was started with rivastigmine, with an adequate response.
ConclusionsDementia and depression are very common in the elderly. It appears that up to 40% of patients with dementia have depressive symptoms. It appears that depression in old age may actually be a prodromal symptom of dementia.
Disclosure of InterestNone Declared
Acute mutism in a young female. A case report of a 20-year-old female who presents a 3-month mutism
- A. Gonzalez-Mota, A. Gonzalez-Gil, C. Martin-Gomez, J. A. Benito-Sanchez, I. M. Peso-Navarro, L. Fernandez-Alonso
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 20-year-old female presents with a progressive 3-month mutism, hyporexia (20kg weight loss), abulia, anhedonia, apathy, social isolation,seeking company of her parents even at night, bradypsychia, sialorrhea, psychomotor slowdown and hypomimia. She is hospitalized in the Psychiatric Brief Hospitalization Unit (PBHU).Her parents relate the beginning of this symptomatology to a breakup and gender violence,which the patient confirms during the interview by eye/cephalic movements and single words jotted down.
ObjectivesThe objective of this study is to describe the evolution of the patient during her hospitalization in the PBHU of Salamanca and to look into the available bibliography about mutism related to stress and sialorrhea.
MethodsWe carried out a follow-up of the hospitalization of the patient and a structured search in PubMed with the keywords “mutism”,“sialorrhea” and “stress” in the last 10 years in English,Spanish and French.
ResultsFew or no articles where found.Therefore, the articles about mutism and stress were analyzed, which focused mostly in selective mutism. Regarding fear,the response to cope with the threat(fight, flight, freeze) is mediated by the autonomic system. The “Polyvagal Theory” speaks about the vagus nerve participating in emotion regulation (social communication and mobilization). Dissociation, in this context,has adaptive and defensive purposes and its threshold can be reduced by repeated stress situations.Long-term alteration of the autonomic nervous system has been described in selective mutism.This malfunction can be related to an elevated production of saliva due to the activation of the parasympathetic in the salivary glands, causing sialorrhea in our patient.
The patient began treatment with sertraline 100mg and risperidone 2mg with the aim of its antidepressive and major tranquilizer effects, she also began individual and family psychotherapy, we assured her sleep and intakes and she began to progressively recover her speech and mobility,identifying a possible trigger for the symptomatology: a physical beating of gender violence after her breakup.
ConclusionsDissociation and “freeze” response can be a maladaptative mechanism to fear.The malfunction of the autonomic nervous system can explain the disconnection,poor gaze,low facial and body expression and inability to speak.
Disclosure of InterestNone Declared
Moria or Mania? Manic symptoms as the clinical manifestation of glioblastoma recurrence: a case report
- F. Mayor Sanabria, M. E. Expósito Durán, M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. Paz Otero, I. Alberdi Páramo, B. Rodado León
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S520
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Up to 50% of patients with brain tumors experience psychiatric symptoms, and rates up to 80% have been reported in malignant neoplasms such as glioblastoma multiforme (GBM). Still, clinical presentation as mania-like syndromes is a rare phenomenon, mainly occurring when frontal structures are compromised.
We present the case of a 42-year-old woman who was admitted to our hospital due to manic symptoms coinciding with a recurrence of a bifrontal GBM, for which she underwent surgery 5 months prior.
Objectives1) To describe the clinical particularities of this case, focusing on the differential diagnosis.
2) To review the association between manic symptoms and frontal dysfunction caused by brain tumors, with special interest on GBM.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, we reviewed the available literature in relation to manic symptoms related to brain tumors.
ResultsThe patient’s GBM recurrence presented with late onset symptoms of mania, including euphoric mood, increased spending, ideas of grandiosity and hyper-religiosity. She had no previous psychiatric history but, interestingly, she had an extensive affective burden in her family, with 4 consummated suicides. However, she also presented other clinical signs, such as disorientation, perseveration, mild memory impairment and stereotyped motor behaviors, that pointed to relevant frontal lobe dysfunction, suggesting Moria as a possible contribution for the symptoms described.
Manic symptoms in the context of brain tumors appear in 7-15% of patients with psychiatric symptoms, usually associated with right frontal dysfunction (75% of cases). Bifrontal affectation, such as this patient, is only described in 6% of cases. Although fast growing, malignant tumors have been associated with higher rates of psychiatric symptoms, no correlation has been described between these and brain tumor histology.
Conclusions- The presence of atypical manic symptoms, such as those presented in this case, should raise clinical concern for secondary mania.
- Moria shares similarities with mania, including mood elevation, tendency to hilarity or hyper-sexuality, that may hinder diagnosis of patients with frontal dysfunction.
- This case outlines the difficulties in making a differential diagnosis in patient with both manic and neurological signs, and highlights the implication of frontal structures in the development of manic symptoms.
Disclosure of InterestNone Declared
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
Cultural factors in depressive experience and its severity: A case report
- C. Regueiro Martín-Albo, F. Mayor Sanabria, E. Expósito Durán, M. Fernández Fariña, M. Navas Tejedor
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S816
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
For a very long time, anthropologists and psychiatrists have studied how the symptomatology of mental diseases varies among cultures. Different social environments approach depression in different ways, and cultural practices and meanings influence how it develops. Culture also affects how symptoms are felt and described, how treatments are chosen, how patients and doctors interact, how likely it is that certain events, like suicide, will occur, and how professionals behave. As a result, all of these circumstances must be taken into consideration when approaching the diagnosis and management of depressive disorders. To illustrate the above, we present the case of a 31-year-old man, originally from Nigeria, who was admitted to the hospital after a suicide attempt by precipitation onto the subway tracks.
Objectives(1) To describe the clinical particularities of this case, focusing on the diagnostic difficulties we faced derived from intercultural contrasts (2) To review cross-cultural differences in the symptomatology and its implication on severity of depressive disorders.
MethodsA review of the patient’s clinical history and complementary tests performed was carried out. Likewise, a bibliographic review of the available scientific literature was also performed in relation to transcultural depressive experiences and its severity.
ResultsThere is little evidence in favor of a direct link between sociocultural factors and severe depression, but we reviewed the arguments that look significant for further research. Depressive illnesses are found in all societies and their symptomatic expression varies culturally, particularly in terms of somatization and delusional ideas. Similarly, the social and individual representations of the disease depend on the culture, and some conceptual models can increase the effects of stigmatization. These cross-cultural variations could influence the care-seeking process and therefore modulate the evolution of the disease in the sense of greater severity.
ConclusionsAll societies experience depressive disorders, which exhibit symptoms that vary culturally, especially in terms of somatization and delusional beliefs.
The care-seeking process is affected by cross-cultural differences, and as a result, the disease’s progression may also be modulated in terms of increased severity.
When we ignore cultural factors in understanding, assessing, and treating depression, we are contributing to misdiagnosis and errors in patient management.
Disclosure of InterestNone Declared
Visual hallucinosis and Linezolid use: A case report.
- M. Fernández Fariña, C. E. Regueiro Martín-Albo, M. E. Expósito Durán, F. Mayor Sanabria, Í. Alberdi Páramo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1012
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 78-year-old man with multiple somatic pathologies and associated depressive symptoms, under treatment with Citalopram 10mg, who was admitted due to cholangitis secondary to biliary prosthetic obstruction.
Empirical antibiotic treatment with Meropenem and Linezolid was started, along with an increase in the dose of Citalopram to 20mg due to mood worsening. The patient begins with symptoms consisting of complex and polymorphic visual hallucinosis, without any affective or behavioral repercussions. He does not present another semiology of the psychotic sphere.
ObjectivesTo highlight the importance of knowing the different interactions and adverse effects of drugs for good clinical management.
MethodsWe collected the complete medical history of our patient and we carried out a review of the interactions and adverse effects described with the antibiotic drug Linezolid.
ResultsAs the onset of hallucinations was temporarily correlated with the use of medications, drug-induced hallucinations were suspected, resolving completely after 2 days after withdrawal of Linezolid treatment.
Linezolid is a nonselective inhibitor of MAO A and B, preventing the destruction of monoamine neurotransmitters like serotonin, dopamine, or norepinephrine. It has dopaminergic properties that may enhance the central nervous system effects of anticholinergics and co-prescription with serotonergic drugs increases the risk of serotonin syndrome.
ConclusionsThis case highlights the importance of taking into account drug interactions and adverse effects to reduce the risk of drug induced symptoms and optimize their management.
The increase in resistance to antibiotic treatment allows us to anticipate that the use of Linezolid will increase in the coming years, and it is important to know its mechanism of action given the interactions with psychotropic drugs that we use in our usual clinical practice
Disclosure of InterestNone Declared
Correlation between BDNF levels and folic acid levels at baseline in drug-naïve First Episode Psychosis
- A. Toll, D. Bergé, I. Canosa, M. Martín - Subero, T. Legido, C. Fernandez - Hinchado, V. Perez - Sola, A. Mané
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S184-S185
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizophrenia is a severe and common psychiatric disorder characterized by disturbed brain development. Brain-derived neurotrophic factor (BDNF) mediates differentiation and survival of neurons as well as synaptic plasticity during the brain development. Several studies have shown decreased serum levels of BDNF in chronic, first episode, and drug naïve schizophrenia patients. Folate provides the substrate for intracellular methylation reactions that are essential to normal brain development and function. Abnormal folate metabolism has been implicated in schizophrenia. For example, reduced maternal folate intake associated with an increased risk for schizophrenia. Also, low blood levels of folate have been reported in patients with schizophrenia, and are associated with clinical manifestation especially in the negative symptom domain.
ObjectivesWith this study, we want to know how BDNF levels at baseline in drug-naïve FEP are associated with folic acid.
MethodsFifty drug-naïve FEP treated between April 2013 and July 2017 at the ETEP Program at Hospital del Mar were included. Inclusion criteria were: 1) age 18-35 years; 2) DSM-IV-TR criteria for brief psychotic disorder, schizophreniform disorder, schizophrenia or unspecified psychosis; 3) no previous history of severe neurological medical conditions or severe traumatic brain injury; 4) presumed IQ level > 80, and 5) no substance abuse or dependence disorders except for cannabis and/or nicotine use. All patients underwent an assessment at baseline including sociodemographic and clinical variables. Fasting blood samples were obtained before administering any medication at baseline and used to determine folic acid and BDNF levels.
ResultsIn our drug-naïve FEP sample, folic acid levels showed a significative positive correlation with BDNF levels at baseline (r = 0.584; p = 0.003). Moreover, we did a lineal regression model that showed that the baseline variables that better predict BDNF levels were folic acid levels, and cannabis use.
ConclusionsOur results are consistent with the findings from some of previous studies that also shows that lower folic acid levels are associated with lower BNDF levels at baseline in drug-naïve FEP. Folate deficiency is associated with cerebrovascular and neurological diseases, and mood disorders. The importance of folate in the nervous system was initially demonstrated in studies that established a greatly increased risk of neurodevelopmental disorders in the offspring of folate-deficient pregnant women. In the adult, epidemiological studies have linked lack of folate to neurodegenerative and neuropsychiatric diseases. However, the mechanisms by which chronic folate deficiency adversely affects CNS function are incompletely understood. Some studies in animals models have hypothesized that folate deficiency in animals could be associated with pyramidal cell loss and reduced hippocampal BDNF.
Disclosure of InterestNone Declared
Memory complaints and quality of life in a patient with mild cognitive impairment
- M. P. Pando Fernández, M. A. Andro Vidal, M. Calvo Valcarcel, P. Martinez Gimeno, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, C. De Andrés Lobo, T. Jimenez Aparicio, C. Vilella Martin, M. Fernández Lozano, B. Rodríguez Rodríguez, M. J. Mateos Sexmero, N. Navarro Barriga
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S937-S938
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Subjective memory complaints remain a relevant aspect to be considered in patients with mild cognitive impairment. Likewise, their association with depressive symptoms, quality of life and cognitive performance is also an objective to be studied in such patients.
ObjectivesOur clinical case represents just one opportunity to study how memory complaints are related to depressive states and how they affect the quality of life of patients with mild cognitive impairment.
MethodsWe conducted a bibliographical review by searching for articles in Pubmed.
ResultsPERSONAL HISTORY: Male, 73 years old, separated, residing alone in Valladolid. He has home help, a person comes to help him with the household chores. Little social and family circle.
History in Mental HealthHe has a history of an admission in 2013 to this Short Hospitalization Unit for ethanol detoxification. Since then, he has been followed up in the Mental Health Unit. According to the reports, he has been diagnosed with depressive disorder and cluster B personality disorder.
Current psychopharmacological treatment: diazepam, olanzapine, duloxetine 60 mg, quetiapine.
Toxic habits: history of chronic ethanol consumption. Smoker. He denies other toxic habits.
Current EpisodeThe patient presents a worsening of his mood of 15 days of evolution, coinciding with a voluntary decrease of his psychopharmacological treatment that the patient has carried out on his own. He walks with the aid of a crutch. Hypomimic facies. Slowed language, circumstantial, with speech focused on current discomfort.
On assessment, he reports initial improvement after reducing his medication, but in recent days he has experienced a decrease in initiative accompanied by feelings of emptiness, sadness and loneliness. He refers to memory complaints for which he is awaiting evaluation by Neurology. The patient explains that at other times in his life he has presented self-harming ideas that he has been controlling. At this time he expresses desire for improvement and adequate future plans, and accepts plans to attend a memory workshop. He also reports visual hallucinations with no affective repercussions and preserved judgment of reality.
Therapeutic PlanTreatment adjustment: Duloxetine 60 mg, 2cp/day. The patient is recommended to lead an active lifestyle and attend a day center or memory workshop.
ConclusionsIn numerous patients with mild cognitive impairment, we have observed that memory complaints are closely related to depressive symptoms and to the patient’s functioning in daily life.
In one study memory complaints were a negative predictor of quality of life in these patients.
Therefore, in addition to considering the importance of treating depressive symptoms, it is also important to address quality of life in patients with mild cognitive impairment.
Disclosure of InterestNone Declared
250 A Living Library for Uveal Melanoma
- Part of
- Lauren A. Dalvin, Samantha R. Erickson, Cynthia M. Pfannkoch, David R. Miley, Diva R. Salomao, Michael P. Fautsch, Svetomir N. Markovic, Martin E. Fernandez-Zapico
-
- Journal:
- Journal of Clinical and Translational Science / Volume 7 / Issue s1 / April 2023
- Published online by Cambridge University Press:
- 24 April 2023, p. 77
-
- Article
-
- You have access Access
- Open access
- Export citation
-
OBJECTIVES/GOALS: Overall response rates for metastatic uveal melanoma (UM), regardless of treatment modality, are less than 20%, highlighting an urgent need for novel therapies. Herein, we present a UM patient-derived organoid (PDO) biobank as a novel platform for translational research. METHODS/STUDY POPULATION: Patients with primary choroidal or ciliochoroidal UM undergoing enucleation from 7/1/2019-9/30/2022 were invited to enroll. Tumor tissue was harvested within 30 minutes of globe removal. Cells were isolated using the human tumor isolation kit and gentleMACS dissociation protocol (Miltenyi Biotech). PDOs were placed on Cultrex-coated multiwell plates and cultured in supplemented RPMI media. DNA and RNA were isolated using kits from Zymo Research. Exon-enriched libraries and RNA were sequenced using an Illumina HiSeq 4000. Immunohistochemistry (IHC) assessed the following histone post-translational modifications: H3K4me1/3, H3K27Ac, and H3K27me. RESULTS/ANTICIPATED RESULTS: PDOs were established in 19 of 20 (95%) attempted cases. BAP1 protein expression was retained (n=7) or lost (n=12) in the primary tumors, with matching phenotype confirmed in PDOs. In 9 sequenced cases, a driving mutation was present in GNAQ (n=4), GNA11 (n=4), or CYSLTR2 (n=1). Morphology ranged from spindle-like to epithelioid clusters, mimicking primary tumor histopathology. Pigmentation increased with time in culture. Growth in culture was slow, and 1-2 months were allotted prior to passaging in most cases. Whole exome and RNA-sequencing confirmed distinct molecular profiles, with differential staining of active chromatin marks by IHC. DISCUSSION/SIGNIFICANCE: A biobank of primary UM PDOs with unique morphological and molecular characteristics has been established. These will serve as a model of human disease to facilitate translational research and investigate personalized treatments for patients with UM.
Psychiatric comorbidity in epilepsy and difficulties in treatment: A case report
- M. Fernández Fariña, F. Mayor Sanabria, C. Regueiro Martín-Albo, M.E. Expósito Durán, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S462
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 36-year-old male with depressive states, impulsive traits and fits of anger (including episodes of self and heteroagressiveness) since early childhood, in the context of traumatic family history and the beginning of an epileptic disease. These symptoms have been maintained over the years, in addition to other variable and recurrent symptoms, such as severe anxiety, somatizations or serious depressive symptoms.
ObjectivesTo highlight the possible influence of epilepsy in the course of mental illnesses, especially depression, as well as the increased difficulty in management.
MethodsWe collected the complete medical history of a patient with an important history of mental health in addition to epileptic disease since childhood and we carried out a review of the comorbidity between these diseases and their treatment.
ResultsThe epileptic disease of our patient may have influenced the behavioural alterations and the depressive symptoms since childhood, as well as the personality traits with aggressiveness and impulsiveness. There is an added difficulty in treating this case given the possible interactions between antiepileptic and antidepressant medications.
ConclusionsThis case highlights the importance of taking into account the influence of this comorbidity on the prognosis of patients. Knowing the interactions and side effects of drugs is essential for good clinical management.
DisclosureNo significant relationships.
Psychosis: Risk Factors and Prognosis
- M. Fernández Lozano, I. Santos Carrasco, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Queipo De Llano De La Viuda, G. Guerra Valera, A. Gonzaga Ramírez, J. Gonçalves Cerejeira, O. Segurado Martín
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S313
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There are life events that may increase the possibilities of suffering some kind of Psychopathology. The most validated model for understanding the aetiology of psychosis is based on genetic and environmental risk factors and their interaction, likely involving epigenetic mechanisms. It is necessary to consider those events as risk factors for Mental Health.
ObjectivesStudy of risk and prognostic factors in psychosis.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 28-year-old male patient from Peru, currently living in Germany. History of sexual abuse in childhood. He started taking drugs at the age of 8. In the emergency department, he reports that since the beginning of the pandemic, after listening to a speech by the Pope, he begins to interpret signals about situations occurring around him. He begins to read about mystical-religious subjects, changes the style of music he listens to and recognises changes in his personality. He says for months he has been feeling watched, persecuted and expresed someone wants to kill him. He says hears voices and that they communicate with him through bodily sensations.
ConclusionsChildhood trauma, immigration and cannabis use are significantly associated with an increased risk of functional psychosis. A neurotic personality also independently contributes to this risk. The accumulation of these factors increases vulnerability to mental disorders and leads to a worse prognosis and evolution of these pathologies. These findings could help to improve the prevention of psychosis and the development of specific treatment strategies in this particular population.
DisclosureNo significant relationships.
Malignant catatonia due to clozapine withdrawal: A case report and a brief review of the literature
- C. Regueiro Martín-Albo, F. Mayor Sanabria, M. Fernández Fariña, M.E. Expósito Durán, A. García Recio
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S710-S711
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Withdrawal symptoms are common upon discontinuation of many psychotropic drugs. Catatonia, a neuropsychiatric condition characterized by a number of motor, behavioral, emotional, and autonomic abnormalities, has been described as a withdrawal syndrome in a growing number of case reports, but it is not well recognized. Treatment of catatonia usually includes benzodiazepines and electroconvulsive therapy. Standard consensus states that the use of neuroleptics should be avoided, as they are thought to worsen catatonia.
ObjectivesWith this case report, we attempt to contribute to the finding in literature that the withdrawal of clozapine may be associated with catatonia, and how reintroduction of clozapine could be indicated for its treatment.
MethodsA clinical case is presented of a 37-year-old female with a history of schizophrenia, presenting with altered mental status and new onset of catatonic signs and symptoms in the setting of a 7-day emetic syndrome. The possibility that vomiting prevented proper absorption of clozapine is postulated, causing the patient to present clinical features compatible with malignant catatonia.
ResultsThe patient required treatment with benzodiazepines, electroconvulsive therapy and clozapine re-initiation, leading to improvement of catatonic symptoms within a few days.
ConclusionsThis case serves as a reminder to consider alternative diagnostic hypotheses in cases of catatonic syndrome unresponsive to standard treatments. When the clinical suspicion of drug withdrawal is high, restarting the discontinued medication, even an antipsychotic agent, may be indicated.
DisclosureNo significant relationships.
Behavioural disturbances as the clinical presentation of Wernicke Encephalopathy: a case report
- F. Mayor Sanabria, A. Bermejo Pastor, M. Fernández Fariña, M.E. Expósito Durán, C. Regueiro Martín-Albo, M. Jiménez Cabañas, C. Ortiz Sánchez-Expósito
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S473
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Wernicke Encephalopathy (WE) is the best characterized neurological complication of thiamine deficiency. Its clinical presentation can be diverse, including hallucinatory or delusional symptoms, and not necessarily associated with the classical triad of WE. This correlates with higher rates of under diagnosis. We present the case of a 72-year-old man with a history of alcoholism who was admitted to the hospital due to behavioural disturbances and subacute delusional ideas of harm.
ObjectivesTo review the epidemiology and clinical features of WE, as well as its clinical management.
MethodsReview of the literature on WE clinical presentation and management, focusing on psychopathological symptoms, applying the information to this specific case.
ResultsClassical triad of WE is only to be found in 10-17% of patients. The most common clinical presentation is changes in mental state (82%), varying from subtle changes in memory, apathy, subtle disorientation or indifference to more severe presentations such as delirium, stupor or coma. Other frequent symptoms include oculomotor dysfunction and gait ataxia. High dose thiamine supplementation therapy has proven effective in preventing clinical progression and permanent neurological damage.
Conclusions- WE is the most prevalent complication of thiamine deficiency, being associated to alcoholism in 50% of cases. - Changes in mental state is the most frequent form of clinical presentation, not necessarily associated with the classical triad of WE. - WE is a medical emergency that requires high dose thiamine supplementation therapy to prevent permanent neurological damage.
DisclosureNo significant relationships.
Assessing parasite epidemiology in the epidemiological importance of Patagonian Late Holocene rockshelters using carnivore coprolites in the past: new data from Piedra Parada, Argentina
- Martín H. Fugassa, Pablo M. Fernández, Cristina Bellelli, Mariana Carballido Calatayud
-
- Journal:
- Parasitology / Volume 149 / Issue 12 / October 2022
- Published online by Cambridge University Press:
- 04 August 2022, pp. 1556-1564
-
- Article
- Export citation
-
The aim of this research was to analyse the variability of parasite assemblages on a small spatial scale, by examining carnivore coprolites from the archaeological site Campo Moncada 2 (CM2), Piedra Parada area, Chubut province, Argentina, and comparing the results with those previously obtained from the archaeological site Campo Cerda 1 (CCe1), located in the same area. Six carnivore coprolites from CM2 were analysed: 4 obtained in sub-level 2a and 2 obtained in sub-level 2a/b. Two radiocarbon dates associated with the coprolites placed the samples chronologically between 780 ± 80 and 860 ± 80 years before present. The rehydrated sediments were sieved and then allowed to sediment spontaneously. The sediment was used for parasitological examination under light microscopy. Conservative estimation of total parasite richness resulted in 21 parasitic taxa. The taxa with the highest fecal prevalence (>50%) corresponded to parasites prevalent in modern carnivores (Alaria sp., Toxocara cf. canis, Toxascaris sp., Eucoleus cf. aerophila, Trichuris sp. and Ancylostomatidae gen. sp.). Assuming that the fox coprolites are contemporaneous, the total fecal parasite richness estimated for CM2 and previously for CCe1 was similar. The high total parasite richness found suggests a network of host–parasite relationships that could include regional hunter-gatherers. The results obtained in carnivore coprolites allow us to infer a very diverse biological community in Piedra Parada area, so the regional caves and rockshelters could have a proportional epidemiological importance as parasite exchange nodes.
Dietary diversity and depression: cross-sectional and longitudinal analyses in Spanish adult population with metabolic syndrome. Findings from PREDIMED-Plus trial
- Naomi Cano-Ibáñez, Lluis Serra-Majem, Sandra Martín-Peláez, Miguel Ángel Martínez-González, Jordi Salas-Salvadó, Dolores Corella, Camille Lassale, Jose Alfredo Martínez, Ángel M Alonso-Gómez, Julia Wärnberg, Jesús Vioque, Dora Romaguera, José López-Miranda, Ramon Estruch, Ana María Gómez-Pérez, José Lapetra, Fernando Fernández-Aranda, Aurora Bueno-Cavanillas, Josep A Tur, Naiara Cubelos, Xavier Pintó, José Juan Gaforio, Pilar Matía-Martín, Josep Vidal, Cristina Calderón, Lidia Daimiel, Emilio Ros, Alfredo Gea, Nancy Babio, Ignacio Manuel Gimenez-Alba, María Dolores Zomeño-Fajardo, Itziar Abete, Lucas Tojal Sierra, Rita P Romero-Galisteo, Manoli García de la Hera, Marian Martín-Padillo, Antonio García-Ríos, Rosa M Casas, JC Fernández-García, José Manuel Santos-Lozano, Estefanía Toledo, Nerea Becerra-Tomas, Jose V Sorli, Helmut Schröder, María A Zulet, Carolina Sorto-Sánchez, Javier Diez-Espino, Carlos Gómez-Martínez, Montse Fitó, Almudena Sánchez-Villegas
-
- Journal:
- Public Health Nutrition / Volume 26 / Issue 3 / March 2023
- Published online by Cambridge University Press:
- 19 July 2022, pp. 598-610
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Objective:
To examine the cross-sectional and longitudinal (2-year follow-up) associations between dietary diversity (DD) and depressive symptoms.
Design:An energy-adjusted dietary diversity score (DDS) was assessed using a validated FFQ and was categorised into quartiles (Q). The variety in each food group was classified into four categories of diversity (C). Depressive symptoms were assessed with Beck Depression Inventory-II (Beck II) questionnaire and depression cases defined as physician-diagnosed or Beck II >= 18. Linear and logistic regression models were used.
Setting:Spanish older adults with metabolic syndrome (MetS).
Participants:A total of 6625 adults aged 55–75 years from the PREDIMED-Plus study with overweight or obesity and MetS.
Results:Total DDS was inversely and statistically significantly associated with depression in the cross-sectional analysis conducted; OR Q4 v. Q1 = 0·76 (95 % CI (0·64, 0·90)). This was driven by high diversity compared to low diversity (C3 v. C1) of vegetables (OR = 0·75, 95 % CI (0·57, 0·93)), cereals (OR = 0·72 (95 % CI (0·56, 0·94)) and proteins (OR = 0·27, 95 % CI (0·11, 0·62)). In the longitudinal analysis, there was no significant association between the baseline DDS and changes in depressive symptoms after 2 years of follow-up, except for DD in vegetables C4 v. C1 = (β = 0·70, 95 % CI (0·05, 1·35)).
Conclusions:According to our results, DD is inversely associated with depressive symptoms, but eating more diverse does not seem to reduce the risk of future depression. Additional longitudinal studies (with longer follow-up) are needed to confirm these findings.
Association between the Prime Diet Quality Score and depressive symptoms in a Mediterranean population with metabolic syndrome. Cross-sectional and 2-year follow-up assessment from PREDIMED-PLUS study
- Naomi Cano-Ibáñez, Lluis Serra-Majem, Sandra Martín-Peláez, Miguel Ángel Martínez-González, Jordi Salas-Salvadó, Maria Dolores Corella Piquer, Camille Lassale, José Alfredo Martínez Hernandez, Ángel M. Alonso-Gómez, Julia Wärnberg, Jesús Vioque Lopez, Dora Romaguera, José López-Miranda, Ramon Estruch, Ana María Gómez-Pérez, José Manuel Santos-Lozano, Fernando Fernández-Aranda, Aurora Bueno-Cavanillas, Josep A. Tur, Vicente Martín, Xavier Pintó Sala, Miguel Delgado-Rodríguez, Pilar Matía Martín, Josep Vidal, Jersy J. Cárdenas, Lidia Daimiel Ruiz, Emilio Ros, Pilar Buil-Cosiales, Nerea Becerra-Tomás, Carmen Saiz, Miguel-Ángel Muñoz-Perez, Itziar Abete, Lucas Tojal-Sierra, Olga Fernández-Barceló, Andrea Bernabé-Casanova, Jadwiga Konieczna, Antonio García-Ríos, Rosa Casas, Maria Rosa Bernal-López, José Lapetra, Estefanía Toledo, Carlos Gómez-Martínez, Oscar Coltell, Mireia Malcampo-Manrúbia, María Angeles Zulet, Carolina Sorto-Sánchez, Alfredo Gea, José Luis Hernández-Fleta, Olga Castañer Niño, Almudena Sánchez-Villegas
-
- Journal:
- British Journal of Nutrition / Volume 128 / Issue 6 / 28 September 2022
- Published online by Cambridge University Press:
- 29 October 2021, pp. 1170-1179
- Print publication:
- 28 September 2022
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The burden of depression is increasing worldwide, specifically in older adults. Unhealthy dietary patterns may partly explain this phenomenon. In the Spanish PREDIMED-Plus study, we explored (1) the cross-sectional association between the adherence to the Prime Diet Quality Score (PDQS), an a priori-defined high-quality food pattern, and the prevalence of depressive symptoms at baseline (cross-sectional analysis) and (2) the prospective association of baseline PDQS with changes in depressive symptomatology after 2 years of follow-up. After exclusions, we assessed 6612 participants in the cross-sectional analysis and 5523 participants in the prospective analysis. An energy-adjusted high-quality dietary score (PDQS) was assessed using a validated FFQ. The cross-sectional association between PDQS and the prevalence of depression or presence of depressive symptoms and the prospective changes in depressive symptoms were evaluated through multivariable regression models (logistic and linear models and mixed linear-effects models). PDQS was inversely associated with depressive status in the cross-sectional analysis. Participants in the highest quintile of PDQS (Q5) showed a significantly reduced odds of depression prevalence as compared to participants in the lowest quartile of PDQS (Q1) (OR (95 %) CI = 0·82 (0·68, 0·98))). The baseline prevalence of depression decreased across PDQS quintiles (Pfor trend = 0·015). A statistically significant association between PDQS and changes in depressive symptoms after 2-years follow-up was found (β (95 %) CI = −0·67 z-score (–1·17, −0·18). A higher PDQS was cross-sectionally related to a lower depressive status. Nevertheless, the null finding in our prospective analysis raises the possibility of reverse causality. Further prospective investigation is required to ascertain the association between PDQS and changes in depressive symptoms along time.





