236 results
Sex-dependent differences in vulnerability to early risk factors for posttraumatic stress disorder: results from the AURORA study
- Stephanie Haering, Antonia V. Seligowski, Sarah D. Linnstaedt, Vasiliki Michopoulos, Stacey L. House, Francesca L. Beaudoin, Xinming An, Thomas C. Neylan, Gari D. Clifford, Laura T. Germine, Scott L. Rauch, John P. Haran, Alan B. Storrow, Christopher Lewandowski, Paul I. Musey, Jr., Phyllis L. Hendry, Sophia Sheikh, Christopher W. Jones, Brittany E. Punches, Robert A. Swor, Nina T. Gentile, Lauren A. Hudak, Jose L. Pascual, Mark J. Seamon, Claire Pearson, David A. Peak, Roland C. Merchant, Robert M. Domeier, Niels K. Rathlev, Brian J. O'Neil, Leon D. Sanchez, Steven E. Bruce, Steven E. Harte, Samuel A. McLean, Ronald C. Kessler, Karestan C. Koenen, Jennifer S. Stevens, Abigail Powers
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 22 May 2024, pp. 1-11
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Knowledge of sex differences in risk factors for posttraumatic stress disorder (PTSD) can contribute to the development of refined preventive interventions. Therefore, the aim of this study was to examine if women and men differ in their vulnerability to risk factors for PTSD.
MethodsAs part of the longitudinal AURORA study, 2924 patients seeking emergency department (ED) treatment in the acute aftermath of trauma provided self-report assessments of pre- peri- and post-traumatic risk factors, as well as 3-month PTSD severity. We systematically examined sex-dependent effects of 16 risk factors that have previously been hypothesized to show different associations with PTSD severity in women and men.
ResultsWomen reported higher PTSD severity at 3-months post-trauma. Z-score comparisons indicated that for five of the 16 examined risk factors the association with 3-month PTSD severity was stronger in men than in women. In multivariable models, interaction effects with sex were observed for pre-traumatic anxiety symptoms, and acute dissociative symptoms; both showed stronger associations with PTSD in men than in women. Subgroup analyses suggested trauma type-conditional effects.
ConclusionsOur findings indicate mechanisms to which men might be particularly vulnerable, demonstrating that known PTSD risk factors might behave differently in women and men. Analyses did not identify any risk factors to which women were more vulnerable than men, pointing toward further mechanisms to explain women's higher PTSD risk. Our study illustrates the need for a more systematic examination of sex differences in contributors to PTSD severity after trauma, which may inform refined preventive interventions.
The occurrence of two opecoeliid digeneans in Mullus barbatus and M. surmuletus
- A. Martínez-Vicaria, J. Martín-Sánchez, P. Illescas, A.M. Lara, M. Jiménez-Albarrán, A. Valero
-
- Journal:
- Journal of Helminthology / Volume 74 / Issue 2 / June 2000
- Published online by Cambridge University Press:
- 12 April 2024, pp. 161-164
-
- Article
- Export citation
-
The infection by Opecoeloides furcatus and Poracanthium furcatum (Opecoeliidae) was studied in 121 Mullus barbatus and 113 M. surmuletus collected from the Spanish south-eastern Mediterranean. The prevalence of infection was most frequent in M. surmuletus with values of 81.42% for O. furcatus and 38.05% for P. furcatum. In M. barbatus the prevalences of O. furcatus and P. furcatum were 54.54% and 14.88% respectively. Statistically significant differences were found between the infection of the two hosts with P. furcatum. No significant differences in worm burdens could be attributable to host size or to seasonal changes, although a lower infection of M. barbatus by O. furcatus occurred in the autumn. Furthermore, the electrophoretic mobility of the enzyme malic dehydrogenase (MDH) was also studied and both digeneans presented different patterns, corresponding in both cases to homozygotic genotypes.
Relationships between functional alpha and beta diversities of flea parasites and their small mammalian hosts
- Boris R. Krasnov, Irina S. Khokhlova, M. Fernanda López Berrizbeitia, Sonja Matthee, Juliana P. Sanchez, Georgy I. Shenbrot, Luther van der Mescht
-
- Journal:
- Parasitology / Volume 151 / Issue 4 / April 2024
- Published online by Cambridge University Press:
- 04 March 2024, pp. 449-460
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
We studied the relationships between functional alpha and beta diversities of fleas and their small mammalian hosts in 4 biogeographic realms (the Afrotropics, the Nearctic, the Neotropics and the Palearctic), considering 3 components of alpha diversity (functional richness, divergence and regularity). We asked whether (a) flea alpha and beta diversities are driven by host alpha and beta diversities; (b) the variation in the off-host environment affects variation in flea alpha and beta diversities; and (c) the pattern of the relationship between flea and host alpha or beta diversities differs between geographic realms. We analysed alpha diversity using modified phylogenetic generalized least squares and beta diversity using modified phylogenetic generalized dissimilarity modelling. In all realms, flea functional richness and regularity increased with an increase in host functional richness and regularity, respectively, whereas flea functional divergence correlated positively with host functional divergence in the Nearctic only. Environmental effects on the components of flea alpha diversity were found only in the Holarctic realms. Host functional beta diversity was invariantly the best predictor of flea functional beta diversity in all realms, whereas the effects of environmental variables on flea functional beta diversity were much weaker and differed between realms. We conclude that flea functional diversity is mostly driven by host functional diversity, whereas the environmental effects on flea functional diversity vary (a) geographically and (b) between components of functional alpha diversity.
Unlocking archaeological data online via the PEPAdb (Prehistoric Europe's Personal Adornment Database) initiative for Open Science
- Galo Romero-García, Daniel Sánchez-Gómez, José Á. Garrido-Cordero, José M. Martínez-Blanes, Ana C. Sousa, Carlos P. Odriozola
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
PEPAdb (Prehistoric Europe's Personal Adornment Database) is a long-term, open-ended project that aims to improve access to archaeological data online. Its website (https://pepadb.us.es) publishes and analyses datasets about prehistoric personal adornment, drawing on the results of various research projects and bibliographic references.
Circular agriculture practices enhance phosphorus recovery for large-scale commercial farms under tropical conditions
- S. G. Moreira, G. Hoogenboom, M. R. Nunes, P. A. Sanchez
-
- Journal:
- The Journal of Agricultural Science / Volume 161 / Issue 6 / December 2023
- Published online by Cambridge University Press:
- 08 January 2024, pp. 763-777
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The objective of this research was to assess the adoption of circular agricultural practices as a tool to improve the recovery use efficiency of phosphorus (P) applied to tropical soils. Two Brazilian farms (1 and 2) that are under long-term no-till and cropped year-round with cover and/or cash crops were used in this study. Soybean, maize and common bean were grown during the summer season (October–February), followed by wheat, common bean and maize during the winter season (February–August). Brachiaria ruziziensis was intercropped with off-season maize. Farm 1 also grew sweet potatoes in rotation with grains. In the integrated crop–livestock system, the leftovers from the silos and crop residues were used to feed beef cattle, while the residues not used in the confinement were turned into compost and applied in the production fields. During the last 3 years, 80 (farm 1) and 71 (farm 2) kg/ha/year of P-fertilizer was applied to meet the demand of the different crops and 56% (farm 1) and 58% (farm 2) of P-fertilizer was exported through the crops and livestock. P-recovery represented more than 50% on both farms. Around 60% of the P consumed by animals was excreted in the form of faeces and urine and the animal manure was used to produce organic compost. Therefore, most of the P consumed by the livestock was returned back to the field to serve as organic fertilizer. This study showed that circular agricultural practices can enhance P-recovery.
41 Concussion History, Physical Activity, and Athletic Status Predict Subjective but not Objective Executive Functioning
- Madeline M. Doucette, Juan P. Sanchez, Ryan E. Rhodes, Mauricio A. Garcia-Barrera
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 914-915
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Factors such as physical activity and sports participation may have a positive effect on executive functioning. However, people involved in sports are at a higher risk of experiencing a concussion, which may have a detrimental effect. Previous research has yet to investigate those combined negative and positive effects while also utilizing a comprehensive assessment of executive function. This study aims precisely to examine the effects of physical activity, athletic status and concussion history on subjective (e.g., questionnaire) and objective measures (e.g., latent variables) of three well-established components of executive function (i.e., inhibiting, shifting, and updating) in young adults.
Participants and Methods:247 Canadian university students (ages 18 - 25; 83% female) completed a remote assessment of executive function involving nine computerized tasks and a behavioural self-report, in addition to demographic questionnaires and items assessing weekly physical activity, athletic status, and concussion history. A linear regression analysis was used to assess the effects of the predictor variables (age, sex, concussion history, physical activity and athletic status) on subjective reporting of executive functioning using the Executive Function Index. Furthermore, structural equation modelling (SEM) was used to predict objective executive function using a three-factor model (shifting, updating, inhibition).
Results:The three-factor measurement model of executive function fit the data adequately: x2 = 26.10, df = 17, p = 0.07, CFI = 0.97, TLI = 0.95, RMSEA = 0.05 [90% CI: 0.00-0.09], SRMR = 0.04. Then, the three-factor SEM of executive function also fit the data adequately: X2 = 66.38, df = 51, p = 0.07, CFI = 0.95, TLI = 0.93, RMSEA = 0.04 [90% CI: 0.00-0.06], SRMR = 0.05. Using SEM, no direct relationship was found between the factors of executive function and the predictor variables (i.e., age, physical activity, concussion history, and athletic status). Sex was significantly related to inhibition (b = 0.52, p = 0.02), such that males had greater inhibition. For the regression, physical activity (b = 0.09, p < .01), concussion history (b = 3.29, p < .05) and athletic status (b = -4.01, p < .05) were found to be significant predictors for the Executive Function Index.
Conclusions:Concussion history, physical activity, and athletic status were all predictive of subjective but not objective measures of executive function. Interestingly, these findings align with previous research that demonstrated performance-based executive function measures often do not align with self-report measures, which may suggest they are complementary but measure slightly different aspects of the underlying executive function construct. Mixed findings in the extant literature regarding sex differences and executive function require continued research to understand better the relationship and mechanisms behind the sex differences in inhibition. In summary, these findings offer support for the differentiation between subjective and objective measures of executive function when investigating their relationship with physical activity, sport participation, concussion history, age and sex.
How cultural factors along with mental health diagnoses influence the treatment of a stroke patient with no previous mental health history: a case report
- P. Setién Preciados, E. Arroyo Sánchez, A. Sanz Giancola, I. Romero Gerechter, M. Martín Velasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S822-S823
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health awareness campaigns in the past few years have vastly improved how medical professionals treat mental health patients. However, prejudices and ignorance still interfere in medical practice. In this context, with the case presented we can see that even in presumed mental health diagnoses along with cultural factors (race, language…), the best medical assistance is not ensured.
ObjectivesReview how different intersectional factors can determine the treatment patients receive at hospitals.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the influence of race, language barriers and mental health diagnoses when attending patients.
ResultsThe patient is presumed to suffer from a mental health condition after a battery of initial tests with inconclusive results do not demonstrate an organic origin. Instead of continuing with the medical study, the patient is disregarded as psychiatric even though his profile doesn´t fit beforehand of a fictitious or conversion disorder. The fact that there are also cultural factors in play (race and language) probably unconsciously influence how the medical team treats this patient’s case. Cultural social factors persistently present as barriers in clinical practice.
ConclusionsRace, language barriers and mental health diagnoses as well as other intersectional factors do have a great impact in the treatment patients receive. There is yet a lot to do when it comes to educating health professionals if we want to offer the best medical assistance.
Disclosure of InterestNone Declared
Suicide behaviour after hospitalisation and related factors: a case report.
- P. Setién Preciados, A. Sanz Giancola, E. Arroyo Sánchez, M. Martín Velasco, I. Romero Gerechter
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1115
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is a global epidemic, with the World Health Organization (WHO) estimating that there are roughly 800,000 suicides annually, accounting for 1.4% of all deaths, and making suicide the 18th leading cause of death in 2016 (World Health Organization. There is a pressing need to better understand factors that contribute to suicide risk. One important domain for suicide prevention is inpatient psychiatric treatment, as many patients are admitted precisely in order to reduce their risk of suicide. Although inpatient psychiatric treatment is often used for suicide risk prevention the risk of suicide after inpatient treatment remains high. Patients who have been recently discharged have a greater risk of suicide than non-hospitalised mentally ill people.
ObjectivesReview suicidal risk after hospitalisations and the factors that may have an influence on it.
MethodsPresentation of a patient’s case and review of existing literature, in regards to the rate of suicide after a patient is released from psychiatric hospitalisation and the factors that surround it.
ResultsThe patient in question is admitted into a psychiatric ward with a diagnosis of severe psychotic depression, after a suicide attempt trying to dissect his arms’ blood vessels. Health professionals at the hospital attend to his needs and the patient sees improvement. Not long after his release, there is a second hospital admission, which doesn’t have the same result and after his release he successfully ends his life. What comes to mind with these sorts of patients is: what kind of help would they have needed? Why hospital admission was not enough? And which factors and profile of patient is more prone to develop suicide behaviour?
ConclusionsAdmissions at psychiatric wards always have to be thought of as a beneficial resource for patients. There are some cases in which patients do not get the help they need by being hospitalised, increasing the risk of comitting suicide. A lot more studies will have to be carried out to understand what variables play a part in this. Meanwhile an improvement in outpatient care to support patients after hospital release is crucial.
Disclosure of InterestNone Declared
New-Onset Bipolar Disorder in Late Life: a case report and review of literature
- A. Sanz Giancola, E. Arroyo Sánchez, P. Setién Preciados, M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S691
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The elderly represents the fastest growing group of the population. It is fair to assume that the portion of old age patients suffering from bipolar disorder will grow in a similar manner. Elderly patients represent approximately 25% of the bipolar population. Summarizing, 5–10% of patients were 50 years of age when they experienced their first manic episode, constituting the subgroup of late onset bipolar disorder (LOBD).
ObjectivesThe purpose of this case report and literature review is to emphasise the importance of LOBD in old population and to highlight its still sparse-knowledge.
MethodsDescriptive case study and review of literature (Arnold,I. et al. Old Age Bipolar Disorder—Epidemiology, Aetiology and Treatment. Medicina 2021,57,587; Baldessarini et al. Onset-age of bipolar disorders at six international sites. J Affect Disord 2010;121(1-2):143-6).
ResultsA 60-year-old woman is brought to the emergency department for evaluation by her family. Over the past 7 days, the patient has become increasingly irritable and argumentative, is sleeping less, is talking faster than usual and has begun to express paranoid concerns about her students “stealing my exam”. The patient is a university professor.
In the assessment interview she is hyperverbal, expansive, and grandiose. The family has also just recently discovered that she has spent a large sum of money on the Internet.
She has no history of psychiatric contact or substance use disorders; however, she has a family history of severe depression.
In the absence of any plausible non-psychiatric condition that could mimic or induce mania, the working diagnosis is bipolar I disorder, most recent episode (MRE) manic with psychotic features.
Image:
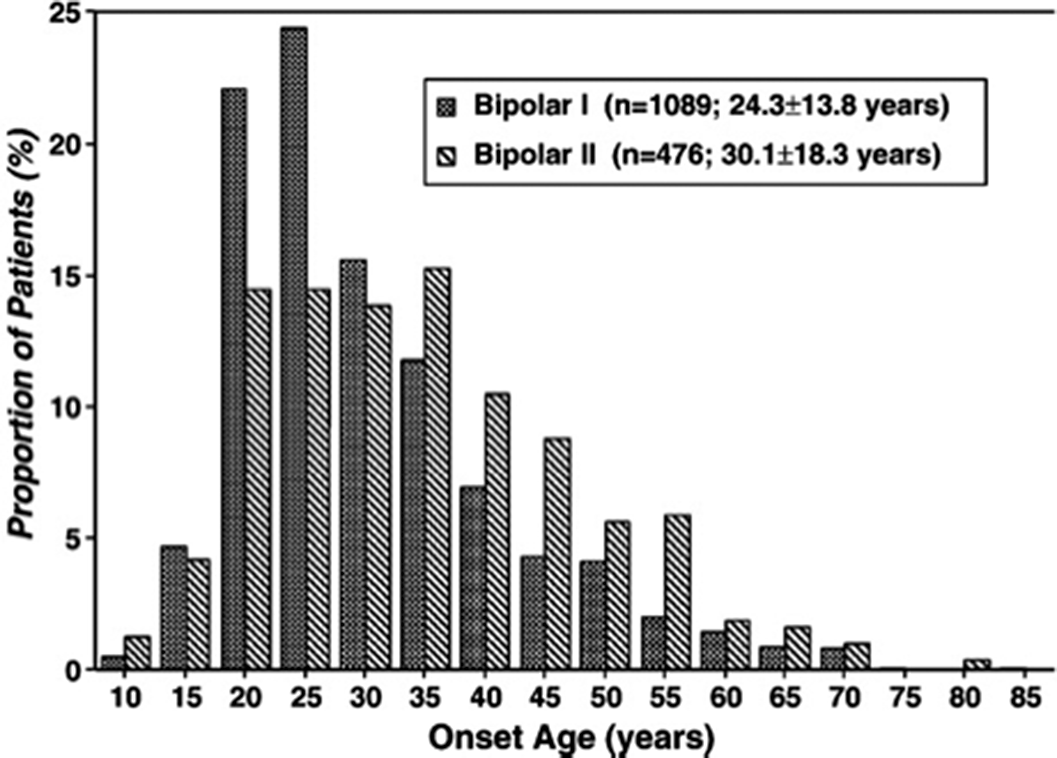
Image 2:
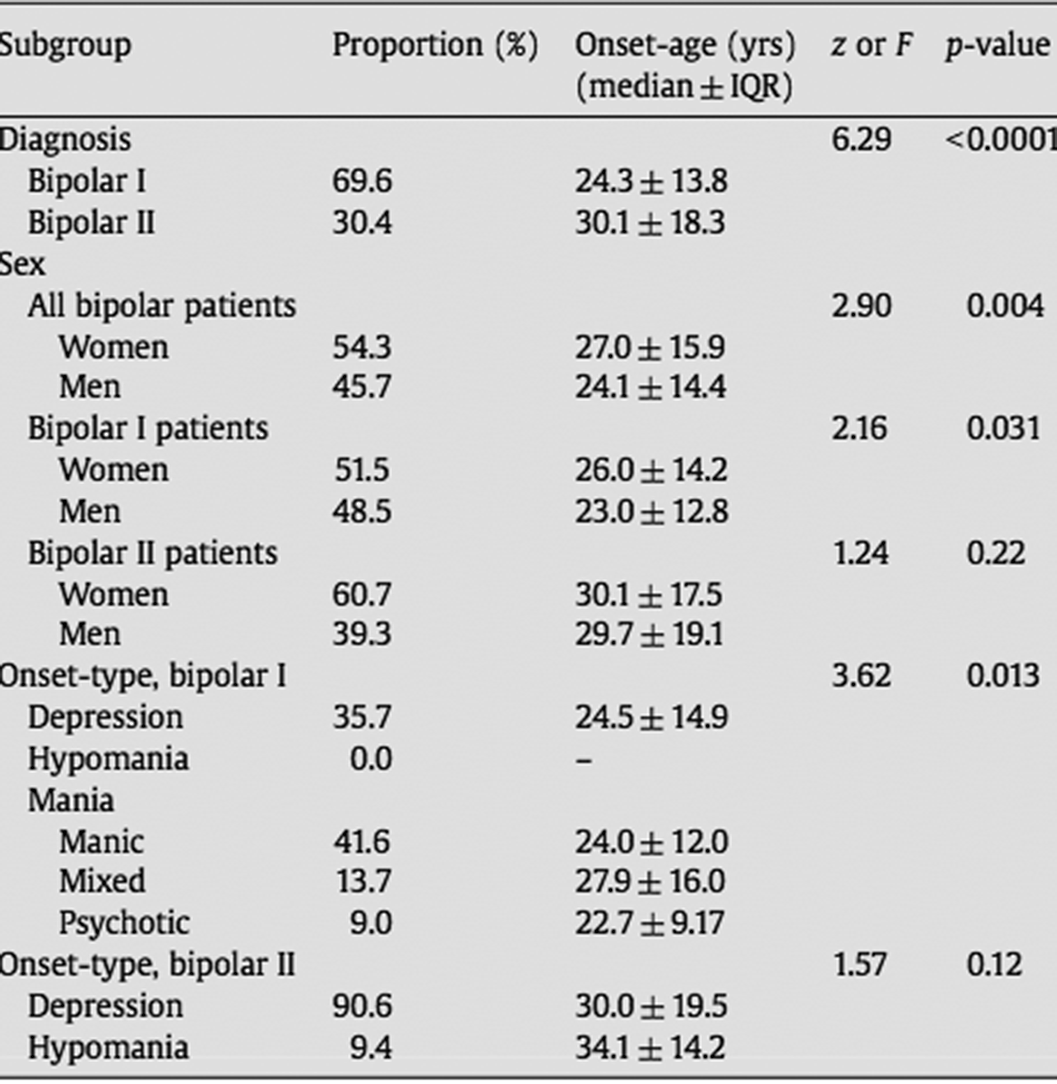 Conclusions
ConclusionsThe share of older age bipolar disorder will grow constantly in the next decades and further research on this neglected patient group is urgently required.
Disclosure of InterestNone Declared
Lithium management in pregnant patients with bipolar disorder
- I. Romero Gerechter, M. Martín Velasco, A. Sanz Giancola, E. Arroyo Sánchez, C. Díaz Mayoral, P. Setien Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S198
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Women with bipolar disorder often ask their treating clinician for information about family planning, as they are concerned about the impact of their illness on offspring. Pregnancy places additional stress on patients, and physiological changes are particularly acute during postpartum. On the other hand, the risk of abnormalities and teratogenicity from psychotropic drugs is significant. The decision wether resuming or discontinuating lithium is discussed.
ObjectivesWe present a theoretical review on the topic.
MethodsA bibliographic review is presented.
ResultsThe choice to continue medication during pregnancy balances the risks of an untreated illness with the risks of medication exposure. Abrupt discontinuation of psychotropic medications is associated with an increased risk for illness recurrence. Women with BD who discontinue their medications before or during pregnancy have a 71% risk of recurrence with new episodes occurring most frequently in the first trimester. Recurrent illness during pregnancy is associated with a 66% increase in the risk of postpartum episodes. Untreated or under-treated BD during pregnancy is associated with poor birth outcomes independent of pharmacotherapy exposure, including preterm birth, low birth-weight, intrauterine growth retardation, small for gestational age, fetal distress, and adverse neurodeve- lopmental outcomes. Women with untreated BD also have behavioral risk factors such as decreased compliance with prenatal care, poor nutrition, and high-risk behaviors. Impaired capacity to function may result in loss of employment, health care benefits, and social support. The biological and psychosocial risks of a BD episode are the justification for the risk of medication exposure.
Fetal exposure to lithium has been associated with an increased risk for cardiac abnormalities. The risk for Ebstein’s anomaly with first trimester exposure is 1 (0.1%) to 2 in 1000 (0.2%), but the absolute risk remains low. Folate supplementation with 5 mg reduces the risk and severity of congenital heart disease. Lithium toxicity causes lethargy, hypotonia, tachycardia, coma, cyanosis, and chronic twitching in the newborn.
Strategies to minimize fetal exposure and maintain efficacy include using the lowest effective dose, prescribing lithium twice daily to avoid high peak serum concentrations, and regular monitoring of lithium serum concentrations. The effective serum concentration must be established before pregnancy. If a therapeutic concentration has not been established, the lithium dose is titrated to a concentration within the therapeutic range. Breast feeding is discouraged in women taking lithium because of the high rate of transmission to the infant.
ConclusionsTreatment decisions for pregnant women with mood disorders must weigh the potential for increased risks of lithium during pregnancy, especially during the first trimester, against its effectiveness at reducing relapse.
Disclosure of InterestNone Declared
Clozapine use in drug induced psychosis in Parkinson´s disease: a case report and review of literature.
- A. Sanz Giancola, P. Setién Preciados, E. Arroyo Sánchez, I. Romero Gerecther, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1041
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The occurrence of psychotic symptoms induced by dopaminergic drugs marks a new phase in the course of Parkinson’s disease (PD). The term drug induced psychosis may be used when other significant psychiatric diseases are excluded in patients with no history of psychosis. The prevalence of dopaminomimetic psychosis varies from 5% to 20%. Therefore, knowledge of the psychopharmacological management of this condition is essential.
ObjectivesThe purpose of this case report and literature review is to to learn the psychopharmacological management of this not uncommon medical complication.
MethodsDescriptive case study and review of literature
ResultsWe present the case of a 71-year-old man with a medical history of Parkinson’s disease with partial response to treatment with high doses of levodopa and carbidopa.
He was brought to the emergency department by his family due to the presence of behavioural alterations at home.
The patient reported seeing men in foam trying to harm his family. In a disjointed way in his speech, he links this idea with the delusional belief that he is being watched by electronic devices placed throughout the house. In a variegated manner he links this with a coelotypical type of discourse, however the delusional ideation remains unstructured throughout.
With no previous personal or family history of mental health and ruling out underlying organic conditions, a diagnosis of psychosis secondary to pharmacological treatment for Parkinson’s disease is presumed.
Considering the risks and benefits, it was decided to maintain the anti-Parkinson’s dose in order to avoid worsening the patient’s motor function. Therefore, after reviewing the literature, the best option was to introduce clozapine at low doses, up to 50 mg at night, with the respective analytical control. After a week’s admission, the patient began to improve psychopathologically, achieving an ad integrum resolution of the psychotic symptoms.
ConclusionsDespite the availability of other antipsychotic treatments such as quetiapine or the more recent pimavanserin, clozapine remains the treatment of choice for drug-induced psychosis in Parkinson’s disease.
Disclosure of InterestNone Declared
Catatonia in a case of major depression resistant to pharmacotherapy. A case report
- C. M. Gil Sánchez, P. Casado de la Torre, M. V. Taillefer Aguanell
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S827
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Catatonia is a clinical syndrome characterized by behavioral alterations, which may include motor immobility or excitation. As a symptom, catatonia may be present in several mental disorders, primarily schizophrenia and mood disorders. Symptoms can be severe and can lead to dangerous and lethal conditions if not diagnosed and treated properly.
ObjectivesTo describe the complicated evolution of a case of major depression with psychotic symptoms, which developed catatonic status. We discuss the psychopharmacological approach and non-pharmacological therapies (ECT).
MethodsCase summary. We have conducted a systematic review of the descriptions published to date, regarding this case.
ResultsWe present a case of extreme severity, in a 55-year-old male, with a broad differential diagnosis with organic pathology, which required multidisciplinary management in conjunction with other specialties and multiple complementary tests.
Eventually diagnosed with major depression with psychotic symptoms evolving into a catatonic state. During more than one year of follow-up, multiple drugs have been tested sequentially: SSRI antidepressants, dual action, low-dose antipsychotics (caripracin, lurasidone, aripiprazole, olanzapine).
Finally, a good response was obtained in the treatment with lorazepam 1mg /6h and 12 sessions of ECT administered concomitantly.
In this case, the patient presented a refusal to eat and weight loss with a BMI of malnutrition. We had to be coordinated with the endocrinology service for a nutritional restitution strategy through dietary supplements. Once nutritional restitution was achieved, we started treatment with clomipramine, with good results on affective symptoms.
ConclusionsNowadays, the origin and treatment of catatonia are still unclear.
We present the case of a man with melancholic depression with psychotic symptoms, who evolved into a catatonic syndrome. A good response was achieved with the combination of ECT and benzodiazepines.
We want to highlight nutritional recovery as an important point to achieve good absorption of antidepressant drugs. Once achieved, we started treatment with clomipramine with good results.
During the treatment, he has presented multiple difficulties and finally, he was able to leave after five months of hospitalization in the acute mental health unit.
Disclosure of InterestNone Declared
Antiviral and Anti-Inflammatory Activities of Fluoxetine in a SARS-CoV-2 Infection Mouse Model
- D. Péricat, S. A. Leon-Icaza, M. Sánchez-Rico, C. Mühle, I. Zoicas, F. Schumacher, R. Planès, R. Mazars, G. Gros, A. Carpinteiro, K. A. Becker, J. Izopet, N. Strub-Wourgaft, P. Sjö, O. Neyrolles, B. Kleuser, F. Limosin, E. Gulbins, J. Kornhuber, E. Meunier, N. Hoertel, C. Cougoule
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S119-S120
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The coronavirus disease 2019 (COVID-19) pandemic continues to cause significant morbidity and mortality worldwide. Since a large portion of the world’s population is currently unvaccinated or incompletely vaccinated and has limited access to approved treatments against COVID-19, there is an urgent need to continue research on treatment options, especially those at low cost and which are immediately available to patients, particularly in low- and middle-income countries. Prior in vitro and observational studies have shown that fluoxetine, possibly through its inhibitory effect on the acid sphingomyelinase/ceramide system, could be a promising antiviral and anti-inflammatory treatment against COVID-19.
ObjectivesThe aim of this sudy was to test the potential antiviral and anti-inflammatory activities of fluoxetine against SARS-CoV-2 in a K18-hACE2 mouse model of infection, and against several variants of concern in vitro, and test the hypothesis of the implication of ceramides and/or their derivatives hexosylceramides.
MethodsWe evaluated the potential antiviral and anti-inflammatory activities of fluoxetine in a K18-hACE2 mouse model of SARS-CoV-2 infection, and against variants of concern in vitro, i.e., SARS-CoV-2 ancestral strain, Alpha B.1.1.7, Gamma P1, Delta B1.617 and Omicron BA.5.
ResultsFluoxetine, administrated after SARS-CoV-2 infection, significantly reduced lung tissue viral titres (Figure 1) and expression of several inflammatory markers (i.e., IL-6, TNFα, CCL2 and CXCL10) (Figure 2). It also inhibited the replication of all variants of concern in vitro. A modulation of the ceramide system in the lung tissues, as reflected by the increase in the ratio HexCer 16:0/Cer 16:0 in fluoxetine-treated mice, may contribute to explain these effects (Figure 3).
Image:
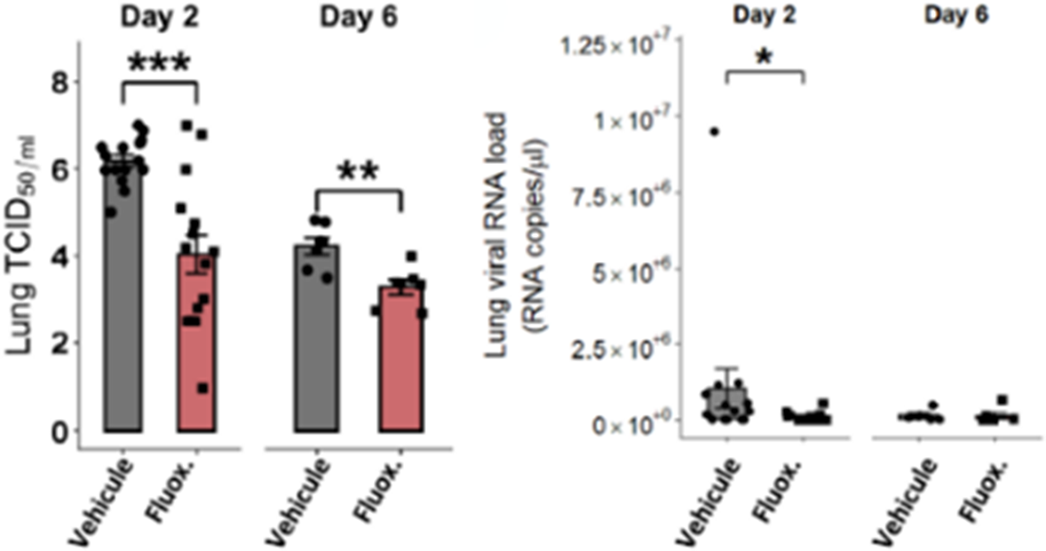
Image 2:
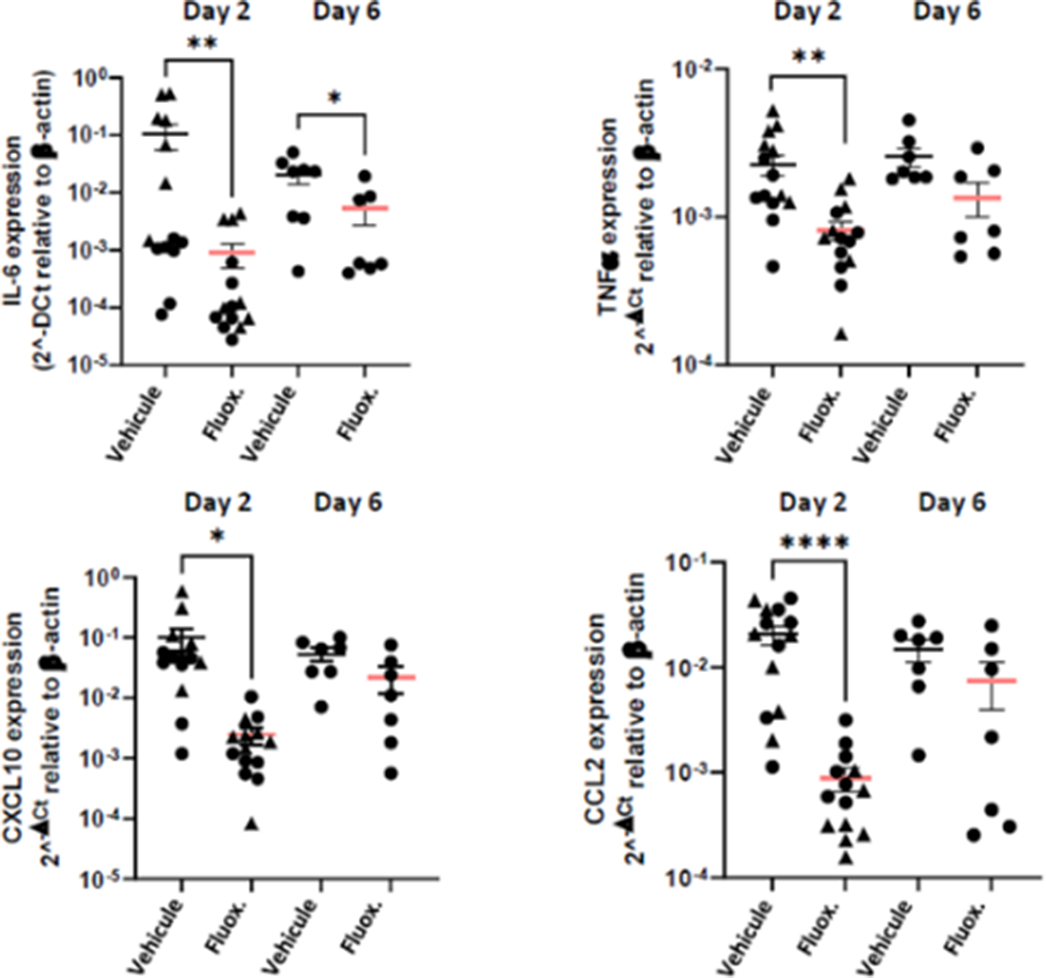
Image 3:
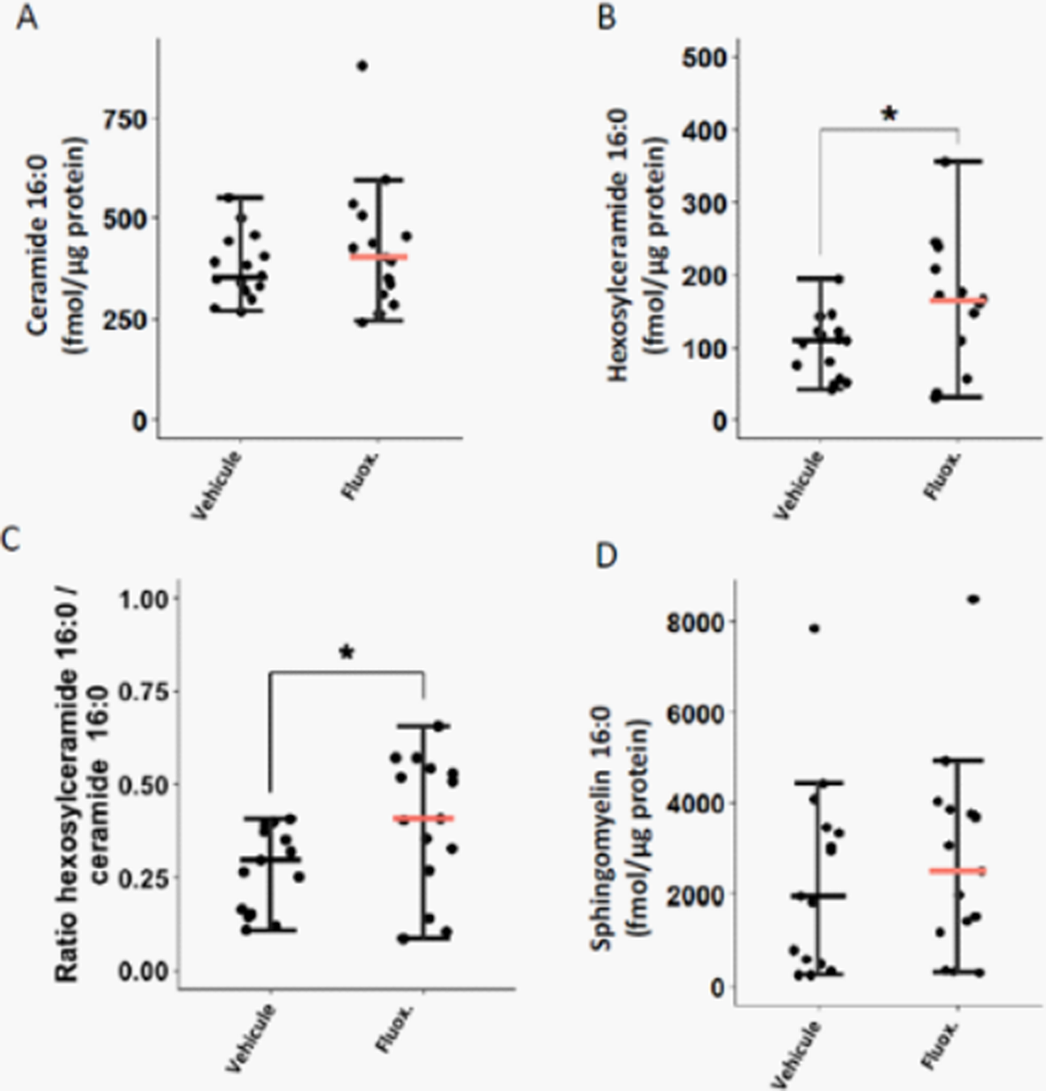 Conclusions
ConclusionsOur findings demonstrate the antiviral and anti-inflammatory properties of fluoxetine in a K18-hACE2 mouse model of SARS-CoV-2 infection, and its in vitro antiviral activity against variants of concern, establishing fluoxetine as a very promising candidate for the prevention and treatment of SARS-CoV-2 infection and disease pathogenesis.
Disclosure of InterestNone Declared
Psychotic denial of pregnancy: case report and narrative literature review.
- M. Martín Velasco, I. Romero Gerechter, C. Díaz Mayoral, E. Arroyo Sánchez, A. Sanz Giancola, P. Setién Preciados
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1129
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Denial of pregnancy is the phenomenon where a woman fails to recognize or accept her pregnancy at >20 weeks gestational age. It associates with increased morbidity and mortality of mother and child, and can be classified as non-psychotic or psychotic. There is fewer medical literature regarding the latter, making it difficult to recognize, let alone to treat, since we do not have robust data regarding incidence nor approved interventions or treatment.
ObjectivesTo describe this unfamiliar entity in order to be able to perform a proper diagnosis and thus prevent possible negative outcomes.
MethodsWe present a case report alongside a narrative literature review on the topic.
ResultsWe report the case of a 39-year-old caucasian woman, foreign, undomiciled, with an advanced pregnancy, who was admitted to a Psychiatry in-patient unit due to psychotic symptoms such as mistrust and delusions. She showed scarce collaboration during assessment and did not give any plausible information about her identity. Her birthplace and prior medical records were therefore unknown. Apparently, she had no family nor social support network. Despite the obvious signs, she did not recognize being pregnant and showed great irritability when asked; her responses ranged from claiming she was suffering from a gastric tumor and making delusional attributions of symptoms clearly related to the pregnancy to partially acknowledging her state but refusing to answer any questions on the matter. Blood work showed no significant abnormalities and obstetric ultrasound revealed a low risk 35 weeks pregnancy.
With an estimated prevalence of 1:475 in general population, denial of pregnancy is not as rare as it may seem. The psychotic variant, however, is rather uncommon. Typically, women with psychotic pregnancy denial have prior history of major mental illness, most frequently schizophrenia, and suffer from extreme psychosocial vulnerability. They usually present previous or anticipated child custody loss, which hampers the process of developing antenatal attachment behaviours. Psychotic denial does not associate with concealing, since these women are mentally detached from the gestation and tend to create delusional explanations to their pregnancy symptoms. Not all of them show complete denial, some being able to acknowledge it, though mostly in an inconsistent way. These patients often fail to seek prenatal care or are noncompliant, they are at greater risk of drug exposure, and some are unable to recognize symptoms of labour, all of which increases the rate of negative outcomes for mother and baby, including neonaticide.
ConclusionsPsychotic denial is a rare diagnosis which should be properly assessed due to its clinical implications and the need to prevent potential negative outcomes for mother and baby.
Disclosure of InterestNone Declared
Psychiatric comorbidity profiles among suicidal attempters: A cohort study
- Y. Sanchez-Carro, M. Diaz-Marsa, V. Fernandez-Rodrigues, W. Ayad-Ahmed, A. Pemau, I. Perez-Diaz, A. Galvez-Merlin, P. de la Higuera-Gonzalez, V. Perez-Sola, P. Saiz, I. Grande, A. Cebria, J. Andreo-Jover, P. Lopez-Peña, M. Ruiz-Veguilla, A. de la Torre-Luque
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S318-S319
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
More than 700,000 people die by suicide in 2019 globally (World Health Organitation 2021). Mental health problems constitute a risk factor for suicidal behavior and death by suicide (Hoertel et al. Mol Psychiatry 2015; 20 718–726). Different mental disorders have been related to different forms of suicidal ideation and behavior (Conejero et al. Curr Psychiatry Rep 2018; 20, 33) (Quevedo et al. Compr Psychiatry 2020; 102 152194). However, little is known on comorbidity profiles among suicide attempters.
ObjectivesThe aim of our work was to identify the psychiatric comorbidity profiles of individuals who were admitted a hospital emergency department due to a suicide attempt. Moreover, it intended to know their clinical characteristics according to comorbidity profile.
MethodsA sample of 683 attempters (71.30% female; M age= 40.85, SD= 15.48) from the SURVIVE study was used. Patients were assessed within the 15 days after emergency department admission. Sociodemographic (i.e., sex, age, marital status and employment status) and clinical data were collected. The International Neuropsychiatric Interview (MINI) was used to assess DSM-V Axis 1 mental health diagnoses and the Columbia Suicide Rating Scale (C-SSRS) to assess suicidal ideation and behavior. The Acquired Capacity for Suicide-Fear of Death Scale (ACSS-FAD), the Patient Health Questionnaire (PHQ-9) to assess the frequency of depressive symptoms during the past 2 weeks, and the General Anxiety Disorder-7 (GAD-7) scale to assess symptoms of worry and anxiety were also conducted. For the identification of comorbidity profiles, latent class analysis framework was followed considering diagnosis to each individual disorder as clustering variables. On the other hand, binary logistic regression was used to study the relationship between comorbidity profile membership and clinical factors.
ResultsTwo classes were found (Class I= mild symptomatology class, mainly featured by emotional disorder endorsement; and Class II= high comorbidity class, featured by a wide amount of endorsed diagnoses) (see figure 1). Individuals from the High comorbidity class were more likely to be female (OR= 0.98, p<.05), younger in age (OR= 0.52, p< .01), with more depressive symptoms (OR=1.09, p<.001) and have greater impulsivity (OR= 1.01, p<.05).
Image:
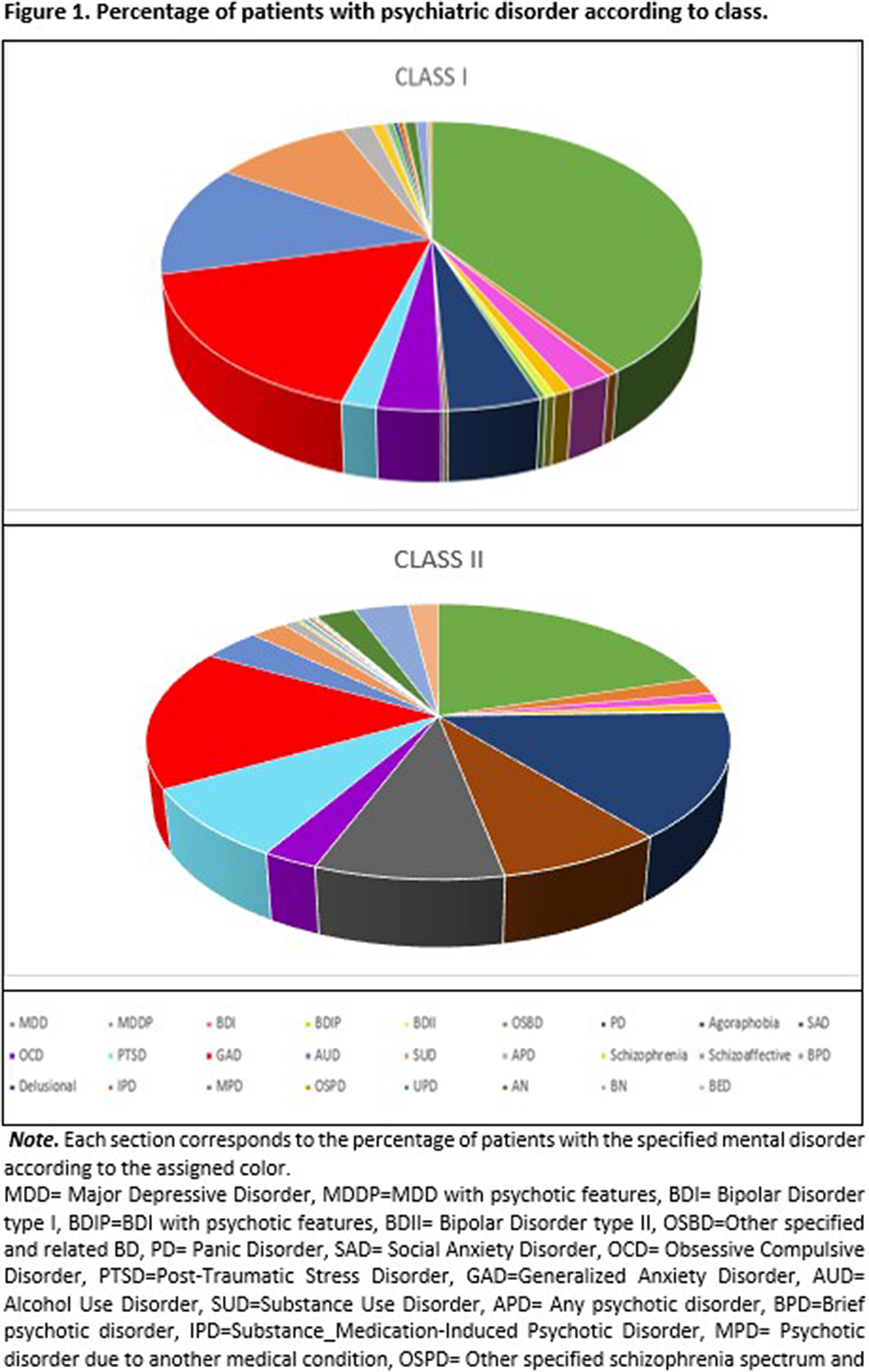 Conclusions
ConclusionsWe found two profiles of people with suicidal behavior based on the presence of mental disorders. Each of the suicidal subtypes had different associated risk factors. They also had a different profile of suicidal behavior.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
Sociodemographic and clinical characteristics of the population with a first psychotic episode attended in the mental health services of area 5 of Madrid (Spain)
- J. Garde González, P. Herrero Ortega, A. Oliva Lozano, I. I. Louzao Rojas, M. P. Vidal-Villegas, A. Muñoz-Sanjosé, M. P. Sánchez-Castro, G. Lahera, S. Sánchez Quílez, M. F. Bravo-Ortiz, O. B. O. A.-M. Group
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S443
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Risk of functional impairment and progression to chronic illness in people with a first episode of psychosis (FEP) has motivated early intervention programs, showing promising results. Defining the characteristics of people with FEP at local level enables the clinicians to adjust interventional models to the reality of the population. The area 5 of Madrid (Spain) is referred to La Paz University Hospital and it serves a catchment area of roughly 527,000 people.
ObjectivesWe aim to identify sociodemographic and clinical characteristics of patients in the area 5 of Madrid (Spain) who meet the criteria of FEP.
MethodsA descriptive retrospective study including 179 people (age range 18-40 years) who were attended in mental health services of La Paz University Hospital (area 5 of Madrid, Spain), between January 2019 and May 2020, having suffered a psychotic episode in the last five years.
ResultsThe average age of people with FEP was 29.32 years, with a higher proportion of men (62%). The mean duration of untreated psychosis (DUP) was 3.64 months and 47% of patients consume cannabis. We found disparities in DUP among the different districts in the area and we also observed differences depending on the district for inclusion in rehabilitation programs or psychotherapy. The following averages were obtained for the aggregate sample: 1.01 hospitalization/year, 1.42 emergency room visits/year, 1.81 years of illness and a mean dosage equivalent to olanzapine 6.75 mg/day. The incidence of psychosis in our area has been 7.01 cases per 100000 inhabitants/year.
ConclusionsThe incidence of psychosis has been as expected according to data recorded at previous studies in Spain. The results obtained in our sample have included a lower DUP and a higher use of cannabis than those described in the literature. We have also found differences when observing the inclusion of patients in different treatments (psychotherapy, rehabilitation), which may be related to the differences in the DUP by districts. Further exploration in this field is needed to draw causal conclusions.
Disclosure of InterestNone Declared
Mania induced after corticosteroid treatment: a case report
- E. Arroyo Sánchez, A. Sanz- Giancola, P. Setién Preciados, I. Romero Gerechter, M. Martín Velasco, C. Díaz Mayoral
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S697
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Corticosteroids are drugs widely used in clinical practice for their anti-inflammatory and immunosuppressive properties. Despite their beneficial effects, a high association of these drugs with neuropsychiatric adverse effects such as psychosis, mania, depression, delirium or increased risk of suicide, among others, has been observed. We present the case of 54-year-old man who started treatment with hydroaltesone 20 mg/8h after undergoing surgery for a pituitary macroadenoma who began with maniform clinic.
ObjectivesTo know the prevalence, risk factors and treatment of mania as a side effect of corticosteroid drugs.
MethodsPresentation of the case and review of the available literature on the risk of developing mania after corticosteroid treatment.
ResultsSeveral studies confirm that the incidence of psychiatric adverse effects after the use of corticosteroids is around 6% if we refer to severe reactions; 28% moderate reactions; and 72% if we consider milder reactions. The direct relationship between these drugs and affective symptoms ranges in rates between 1-50% of cases, the most frequent being depression and mania. The risk of mania after treatment with corticosteroids is 4-5 times higher than if we compare it with a group of population not exposed to these drugs. There is a dose-response relationship, increasing the risk from a daily dose of 40 mg/day, with an average duration of symptoms of around 21 days. Female sex seems to be a risk factor in relation to the fact that diseases requiring this type of treatment are more common in this gender. As first-line treatment for mania secondary to corticosteroids, a decrease in treatment dose or its interruption, whenever possible, is proposed. Adjuvant treatment may be required, with atypical antipsychotics being the first choice.
ConclusionsCorticosteroid therapy has a direct dose-response relationship with the presence of psychiatric adverse effects such as mania. Dose and sex have been studied as possible adverse effects. Therefore, the pharmacological treatment of choice consists of a reduction in the dose of corticosteroids administered or withdrawal, if possible, and may be combined with an atypical antipsychotic such as olanzapine, quetiapine or risperidone. Re-evaluation is recommended until complete resolution of the clinical picture and then antipsychotic treatment can be progressively withdrawn.
Disclosure of InterestNone Declared
Cyclothymia, bipolar disorder and multiple sclerosis: A case report
- M. D. P. Paz Otero, E. Lozano Bori, J. Sánchez Rodríguez, S. Puyal González, M. Fernández Fariña, F. Mayor Sanabria, A. Francos Ajona
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S703-S704
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 49-year-old woman who was diagnosed with multiple sclerosis at the age of 19 and suffers from an affective disorder that has been evolving for years. This condition, for which she has been followed by psychiatry and psychology for more than ten years, consists of alternating periods of hypomania lasting weeks and phases in which frank depressive symptomatology predominates, with no phases of euthymia in between and with a predominance of severe deterioration of her functionality at both poles.
Objectives(1) We will review the term cyclothymia and explore the concept of “cyclothymic temperament” advocated by some authors, in order to be able to understand the dimension of the present case and reformulate its approach.
(2) The relationship between multiple sclerosis and bipolar spectrum disorders will be covered, reviewing the current knowledge in this regard and relating it to the patient’s symptomatology.
MethodsA review of the patient’s clinical history will be carried out, taking into account her life history, the complementary tests performed as well as the multiple therapeutic approaches tried over the last few years.
Likewise, a bibliographic review of the available scientific literature will be carried out in relation to the diagnosis of cyclothymia or bipolar disorder type II, the controversial term “cyclothymic temperament”, and the relationship that these diagnoses have with the diagnosis of Multiple Sclerosis.
Results(1) Our patient could fit into what many authors define as a cyclothymic temperament, fulfilling, in certain episodes, the criteria that the manuals propose for bipolar disorder type II.
(2) 2.1 The prevalence of bipolar affective disorder in MS is approximately twice as high as in the general population (rates of 0.3-2.4%). 2.2 Patients with MS have higher scores in cyclothymic and hyperthymic temperament than the control group. 2.3 Certain drugs generally used in BD also seem to have a beneficial effect on MS.
Image:
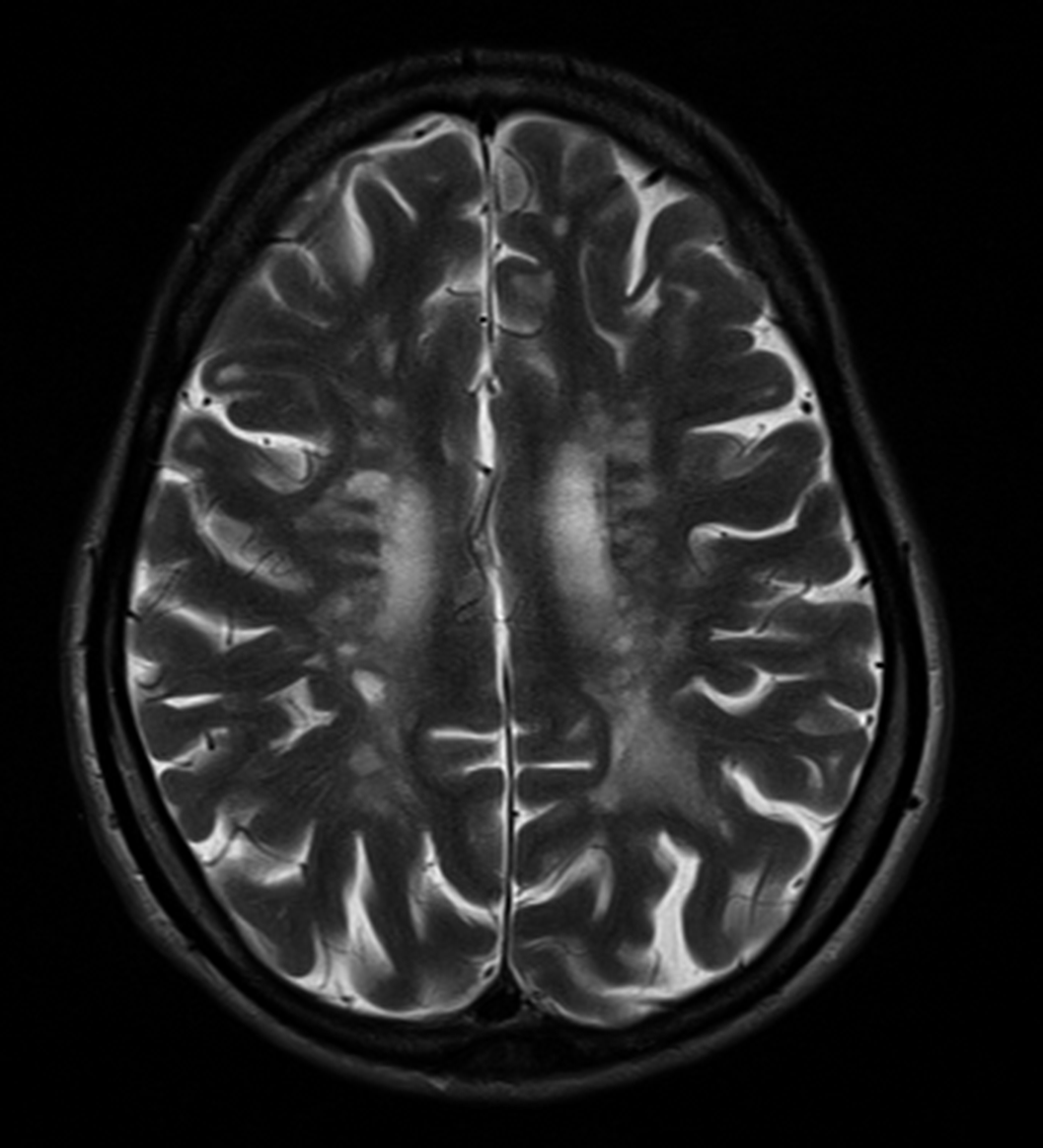
Image 2:
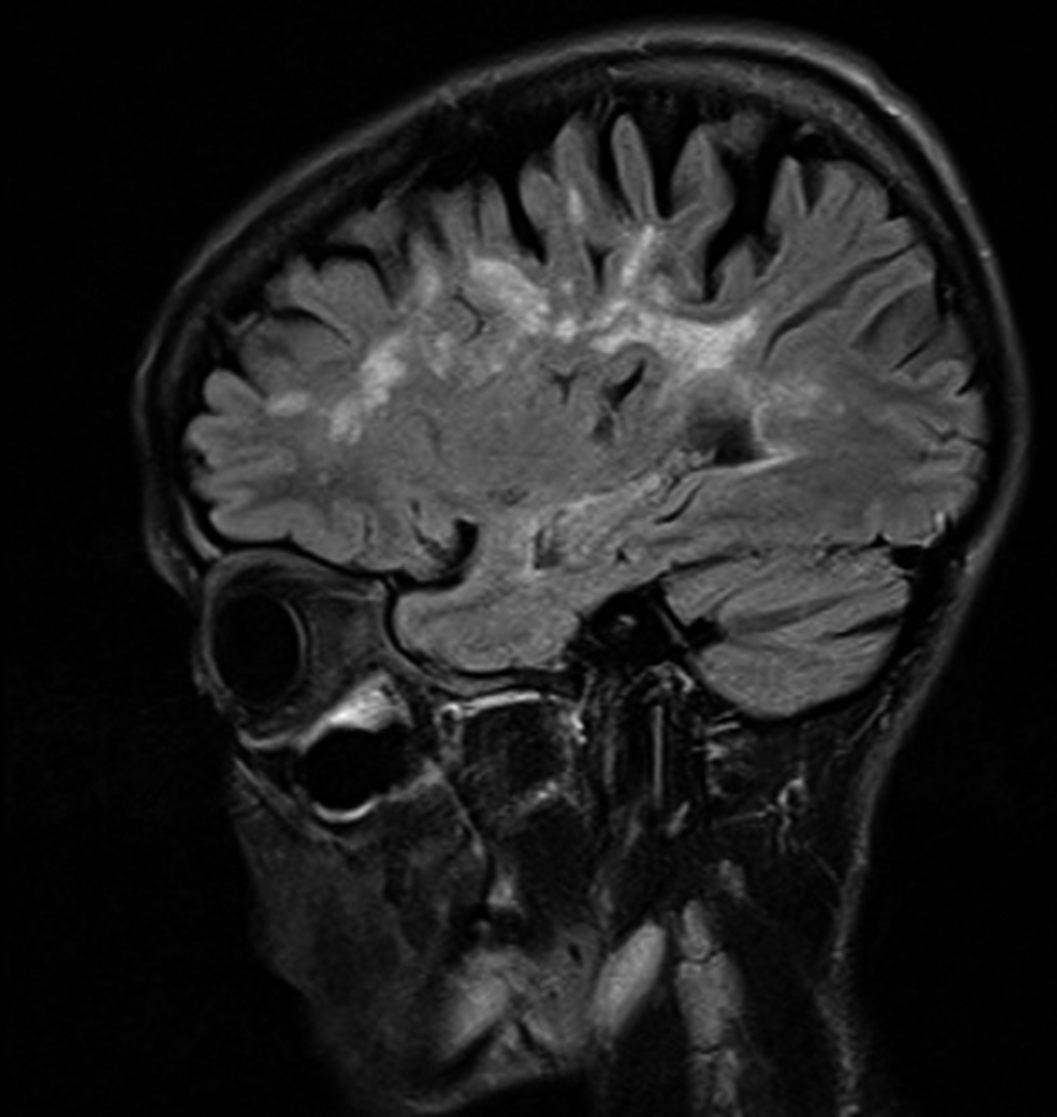 Conclusions
ConclusionsThe reformulation of the concept of cyclothymia would allow us to recognize in our patient a basic temperament of long evolution that would be the substrate on which different factors have subsequently influenced, such as antidepressant drugs or multiple sclerosis. In addition, it is necessary to know the association between BD and MS, in order to be able to offer an adequate treatment, contemplating some pharmacological options such as Lithium or some Atypical Antipsychotics, given the beneficial effect both for the affective disorder and for the neurological process.
Disclosure of InterestNone Declared
An empirical staging model for schizophrenia using machine learning
- M.-C. Clara, F. Sánchez-Lasheras, A. García-Fernández, L. González-Blanco, P. A. Sáiz, J. Bobes, M. P. García-Portilla
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S626-S627
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the great challenges still to be achieved in schizophrenia is the development of a staging model that reflects the progression of the disorder. The previous models suggested have been developed from a theoretical point of view and do not include objective variables such as biomarkers, physical comorbidities, or self-reported subjective variables (Martinez-Cao et al. Transl Psychiatry 2022; 12(1) 1-11).
ObjectivesDevelop a multidimensional staging model for schizophrenia based on empirical data.
MethodsNaturalistic, cross-sectional study. Sample: 212 stable patients with Schizophrenia (F20). Assessments: ad hoc questionnaire (demographic and clinical information); psychopathology: PANSS, CDS, OSQ, CGI-S; functioning: PSP; cognition: MATRICS; laboratory tests: C-Reactive Protein (CRP), IL-1RA, IL-6, Platelets/Lymphocytes (PLR), Neutrophils/Lymphocytes (NLR), and Monocytes/Lymphocytes (MLR) ratios. Statistical analysis: Variables selection was performed with an ad hoc algorithm developed for this research. The referred algorithm makes use of genetic algorithms (GA) to select those variables that show the best performance for the patients classification according to their global CGI-S. The objective function of the GA maximizes the individuals correct classification of a support vector machines (SVM) model that employs as input variables those given by the GA (Díez-Díaz et al. Mathematics 2021; 9(6) 654). Models performance was assessed with the help of 3-fold cross-validation and these process was repeated 10,000 times for each one of the models assessed.
ResultsMean age(SD): 39.5(13.54); men: 63.5%; secondary education: 59.50%. Most patients in our sample had never been married (74.10%), and more than a third received disability benefits due to schizophrenia (37.70%). The mean length of the disease was 11.98(12.02) years. The best SVM model included the following variables: 1)Clinical: number of hospitalizations, positive, negative, depressive symptoms and general psychopathology; 2)Cognition: speed of processing, visual learning and social cognition; 3)Functioning: PSP total score; 4)Biomarkers: PLR, NLR and MLR. This model was executed again 100,000 times applying again 3-fold cross-validation. In 95% of the algorithm executions more than a 53.52% of the patients were classfied in the right CGI-S category. On average the right classification was of 61.93%. About specificity and sensitivity the average values obtained were of 0.85 and 0.64 respectively.
ConclusionsOur staging model is a robust method that appropriately distributes patients according to the severity of the disorder. Highlights the importance of clinical, functional and cognitive factors to classify patients. Finally, the inflammatory parameters PLR, NLR and MLR have also emerged as potential biomarkers for staging schizophrenia.
Disclosure of InterestNone Declared











