1132 results
Influence of organic and cage housing system on egg quality in laying hens
- Alba Rodríguez-Mengod, María J. Domínguez-Gómez, Antonio Calvo, María D. Raigón, Carlos Mínguez
-
- Journal:
- Renewable Agriculture and Food Systems / Volume 39 / 2024
- Published online by Cambridge University Press:
- 20 September 2024, e19
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Most of the eggs for consumption are produced in a conventional housing system although the demand for organic eggs is increasing because consumers assume better nutritional characteristics. This study was conducted to compare the quality of organic eggs and enriched cage eggs. A total of 409 organic eggs and 385 eggs from hens housed in enriched cages were directly collected from 15 different farms, located in Spain and were analyzed within 4 days after laying. The differences in quality by removing the time bias that can be caused by marketing time were thus determined. All the hens were of three different lines, 47–50 weeks old and consumed commercial feed with the same nutritional composition. The quality traits evaluated were egg weight (EW g), egg shape index (SI), shell thickness (ST), shell percentage (SP), Haugh units (HU), dense albumen percentage (DAP), total albumen percentage (TAP), yolk color (YC), yolk percentage (YP), Roche scale (RS), moisture (M), ash content (AC), total protein (TP), total yolk carotenoids (TYC), total fat (TF), saturated fatty acids (SFA), monounsaturated fatty acids (MFA), and polyunsaturated fatty acids (PFA). Estimates of differences were obtained by generalized least squares using housing system, genetic line and their interaction as factors. Significant differences were observed for EW (65.3 vs 62.9), SI (77.60 vs 76.10), HU (83.60 vs 81.80), TAP (66.5 vs 64.17), YC (3.11 vs 1.89), RS (11.79 vs 9.48), TP (9.99 vs 8.55), TYC (4.188 vs 2.650), SFA (32.20 vs 30.00) and MFA (53.40 vs 44.20) in favor of the enriched cage system. In the organic system, the quality parameters that had higher and significant values were ST (0.34 vs 0.32), SP (10.52 vs 9.41), YP (25.20 vs 24.30), AC (1.12 vs 0.93) and PFA (26.00 vs 14.00). Significant interactions between the housing system and the hen line followed the same pattern observed for fixed effects. Organic eggs were lighter, less rounded with better shell quality and therefore showed lower Haugh unit values and a lower albumen percentage. Total protein, total fat, and lipid profile were within the usual average values for commercial eggs, although the proportion of polyunsaturated fatty acids, which are beneficial for consumers, was higher in organic eggs.
Guaranteed real-time cooperative collision avoidance for n-DOF manipulators
- Erick J. Rodríguez-Seda, Michael D. M. Kutzer
-
- Journal:
- Robotica , First View
- Published online by Cambridge University Press:
- 16 September 2024, pp. 1-25
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This paper presents a decentralized, cooperative, real-time avoidance control strategy for robotic manipulators. The proposed avoidance control law builds on the concepts of artificial potential field functions and provides tighter bounds on the minimum safe distance when compared to traditional potential-based controllers. Moreover, the proposed avoidance control law is given in analytical, continuous closed form, avoiding the use of optimization techniques and discrete algorithms, and is rigorously proven to guarantee collision avoidance at all times. Examples of planar and 3D manipulators with cylindrical links under the proposed avoidance control are given and compared with the traditional approach of modeling links and obstacles with multiple spheres. The results show that the proposed avoidance control law can achieve, in general, faster convergence, smaller tracking errors, and lower control torques than the traditional approach. Furthermore, we provide extensions of the avoidance control to robotic manipulators with bounded control torques.
Characterization of MoS2 films via simultaneous grazing incidence X-ray diffraction and grazing incidence X-ray fluorescence (GIXRD/GIXRF)
- Mark A. Rodriguez, Tomas F. Babuska, John Curry, James J. M. Griego, Mike T. Dugger, Steven R. Larson, Alex Mings
-
- Journal:
- Powder Diffraction / Volume 39 / Issue 2 / June 2024
- Published online by Cambridge University Press:
- 13 September 2024, pp. 60-68
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Physical vapor deposited (PVD) molybdenum disulfide (nominal composition MoS2) is employed as a thin film solid lubricant for extreme environments where liquid lubricants are not viable. The tribological properties of MoS2 are highly dependent on morphological attributes such as film thickness, orientation, crystallinity, film density, and stoichiometry. These structural characteristics are controlled by tuning the PVD process parameters, yet undesirable alterations in the structure often occur due to process variations between deposition runs. Nondestructive film diagnostics can enable improved yield and serve as a means of tuning a deposition process, thus enabling quality control and materials exploration. Grazing incidence X-ray diffraction (GIXRD) for MoS2 film characterization provides valuable information about film density and grain orientation (texture). However, the determination of film stoichiometry can only be indirectly inferred via GIXRD. The combination of density and microstructure via GIXRD with chemical composition via grazing incidence X-ray fluorescence (GIXRF) enables the isolation and decoupling of film density, composition, and microstructure and their ultimate impact on film layer thickness, thereby improving coating thickness predictions via X-ray fluorescence. We have augmented an existing GIXRD instrument with an additional X-ray detector for the simultaneous measurement of energy-dispersive X-ray fluorescence spectra during the GIXRD analysis. This combined GIXRD/GIXRF analysis has proven synergetic for correlating chemical composition to the structural aspects of MoS2 films provided by GIXRD. We present the usefulness of the combined diagnostic technique via exemplar MoS2 film samples and provide a discussion regarding data extraction techniques of grazing angle series measurements.
Liquor for breakfast, fighting against alcohol consumption
- N. Navarro Barriga, P. Marqués Cabezas, M. B. Arribas Simón, B. Rodríguez Rodríguez, C. Alario Ruiz, G. Guerra Valera, A. Aparicio Parras, M. J. Mateos Sexmero, M. Fernández Lozano, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, M. P. Pando Fernández, M. D. L. A. Guillén Soto, T. Jimenez Aparicio, M. D. C. Vallecillo Adame, C. De Andrés Lobo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S408-S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful consumption of alcohol is known for how tortuous its management can be in mental health, encouraging introspection of it as a serious problem is perhaps the main key to starting to battle against its damaging influence on the development of a functional and full life.
ObjectivesTo describe a clinical case showing an unpredictible complication in an alcohol detoxification process.
Methods54-year-old man, native of Cádiz, widowed for half a decade, without children. He resides with his parents in the family home. Currently unemployed for approximately a year. He has previously worked in the IT sector. As a notable somatic history, we found long-established arterial hypertension and a total hip replacement. He has been under irregular follow-up with a mental health team for anxiety-depressive symptoms in the context of grief. He goes to the emergency service brought by his family to begin the detoxification process in the hospital setting. He acknowledges ethanol consumption since he was widowed, which began when he awakes; quantities that ranged between one or up to three bottles of distilled liquor per day, generally consumption is in the home environment. A little less than a year ago, he began to isolate himself in his room and abandon his self-care, eating increasingly insufficient food intake, refusing to receive professional care to quit the habit, mainly because he did not recognize it as disruptive.
The patient was admitted to hospital with symptoms suggestive of withdrawal, making it extremely difficult to control blood pressure levels. On the third day of admission to the acute care unit, fever peaks, blood pressure levels well below normal parameters, and compromised level of consciousness began to be evident.
ResultsBlood tests were performed that, together with the clinical picture, suggested imminent septic shock, so critical care was contacted for transfer and stabilization. A germ of probable urinary etiology sensitive to a broad spectrum of antibiotics was isolated in blood cultures, and the medication of the detoxification process was progressively optimized. Once clinical stability was achieved at all levels, an inpatient cessation resource was managed, which the patient accepted and considered suitable for his complete recovery.
ConclusionsA holistic approach to the alcoholic patient is important, since serious problems of an organic nature often arise. This is why a multidisciplinary intervention is necessary, as well as a holistic approach to care, involving both classic pharmacology and assiduous long-term psychotherapeutic intervention.
Disclosure of InterestNone Declared
Bipolar disorder, Deafness and Culturality in Psychiatric Home Hospitalization: A Clinical Case
- J. Marti Bonany, G. De Iturbe Catania, R. Romar Navia, D. Tolosa Merlos, C. Montserrat Diez, E. Pechuan Martínez, R. Rodriguez Seoane, L. Gil Martinez, D. Garcia Hernandez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S435
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mental health in the deaf community is a complex issue. Challenges in diagnosis and treatment arise from a lack of experienced interpreters and difficulties in translating Sign Language to spoken language. Deaf individuals, due to auditory limitations, are more vulnerable to abuse, increasing their risk of mental health disorders, including bipolar affective disorder (BPAD). BPAD is a prevalent, debilitating condition with varied prevalence estimates. Managing it is tough due to its lifelong, unpredictable nature. A new approach called Psychiatric Home Hospitalization Unit aims to provide acute mental health care at home as an alternative to hospitalization.
ObjectivesTo show the management of severe bipolar disorder with comorbidity from a Psychiatric Home Hospitalization Unit
MethodsA clinical case of bipolar disorder with deafness attended at the Psychiatric Home Hospitalization Unit of our hospital is presented.
ResultsA 24-year-old deaf woman borned in Pakistan and later moving to Catalonia, she faced educational challenges but ultimately completed her studies with sign language support. Afterward, she struggled to find suitable employment, and her family had a history of bipolar disorder.
She exhibited a sudden change in behavior, characterized by irritability, paranoia, and distrust. Communication was challenging due to her speech difficulties, but assessments using sign language and observation were conducted. Her physical examination was normal, but her speech was disorganized and pressured, suggesting possible auditory hallucinations and thought disturbances. She was hospitalized and diagnosed with bipolar disorder with psychotic features.
During her initial hospitalization, she received lithium, olanzapine, clotiapine and benzodiacepines. After discharge, she continued treatment through a home hospitalization service during almost 4 month. During follow-up she presented a course with high affective instability, rapid cycling alternating brief periods of stability with other presenting manic and mixed features with high disorganization.
Due to the rapid cycling pattern Valproic acid was considered. Valproic acid was introduced up to 700 mg/d (97.1 mcg/mL). Treatment with lithium carbonate 800 mg/d (0.91 mEq/L) was maintained. Previous antipsychotic regimen was changed to quetiapine 400mg/d, olanzapine 5mg/d. Her condition improved significantly with the adjusted treatment regimen. She was discharged to an outpatient service.
ConclusionsDiagnosing and treating bipolar affective disorder (BPAD) in a deaf and mute patient posed unique challenges. The rapid mood cycling pattern and complexity of her case made treatment challenging. Family information and interpreter support were vital. Cultural factors were considered, and home hospitalization was crucial in managing symptoms that lasted over four months.
Disclosure of InterestNone Declared
Gestational age and sex interaction and risk for autism spectrum disorder in extremely preterm newborns: an 18‑month follow‑up study
- L. Pina-Camacho, J. Merchan-Naranjo, E. Rodriguez-Toscano, L. Martin, C. Romero, L. Boada, S. Zeballos, M. Arriaga, D. Blanco-Bravo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S281
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Extremely preterm newborns - EPTN (born ≤28 weeks gestational age) are at increased risk of developing autism spectrum disorders (ASD). Demographic and perinatal risk factors associated with ASD risk in EPTN are understudied.
Objectives(i) In EPTN and born at full-term healthy controls (HC), to characterize the emergence of ASD traits and autistic symptom load at age 18 months; (ii) in EPTN, to identify the influence of perinatal characteristics such as sex and gestational age on autistic symptom load at corrected-age 18 months.
MethodsObservational, longitudinal, prospective, 18-month follow-up study. We recruited a cohort of n=113 EPTN and n=47 HC (the PremTEA cohort); n=57 EPTN and n=42 HC successfully completed the 18-month follow-up visit. We assessed autistic symptom load & risk at 18 months using the M-CHAT-R/F questionnaire. For all EPTN and HC, we collected demographic and perinatal data. Using GLMs, we assessed, in EPTN, the association between demographic/perinatal variables and 18-month autistic symptom levels.
ResultsAt 18 months, EPTN children showed higher autistic symptom levels than HC (M-CHAT-R/F score, mean (SD) [range] = 2.21 (3.23) [0-12] in EPTN vs. 0.33 (0.57) [0-2] in HC; d=.873, p=.001. In EPTN, we identified differences by gestational age and sex in autistic symptom levels at 18 months (aR2=0.517, p=.006). In particular, female EPTNs born with lower gestational age showed higher autistic symptom load at age 18 months.
ConclusionsOur findings support the need for early screening of ASD symptomatology in EPTN infants, particularly in higher-risk subgroups, such as female patients born with lower gestational ages.
Disclosure of InterestNone Declared
Socio-demographic characteristics and pharmacological treatment options in patients with delirium
- F. J. Cruz Aviña, A. Salazar Rodriguez, D. N. M. Sanchez, E. A. C. Martinez, L. C. Rocha Reza, S. V. Nuñez Pichardo, H. A. Barranco Rogel, M. G. Ochoa Madrigal, O. Meneses Luna
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S368-S369
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Delirium is common in hospital settings, with approximately 3% to 45% of older patients in hospitals developing delirium during their stay. Among the elderly and those with severe or advanced medical conditions, the reported percentage of patients with delirium is over 56%. The three motor subtypes of delirium are hyperactive, hypoactive, and mixed. Another way to characterize delirium is based on whether it is reversible, irreversible, or terminal.
ObjectivesIdentifying appropriate pharmacological treatment options among antipsychotics and their correlation with various precipitating and predisposing factors in the in-hospital context
MethodsThis was a retrospective, cross-sectional, observational study that utilized a database created by the psychiatry department at the National Medical Center 20 de Noviembre, with data collected from April 2021 to April 2022. The database contains anonymized administrative and clinical data of patients who were seen in the psychiatry department for the diagnosis of any type of delirium, using the CAM scale for classification. The database includes records and data of hospitalized patients, encompassing all specialties at this medical center
ResultsA total of 139 patients were included in the study, of which 39% were female and 61% were male, with a mean age of 67 and a median age of 68 years. It was observed that the average duration of delirium symptoms, from receiving the consultation to remission, was approximately 6 days (p <0.005) (OR 5.12-6.62), and the average length of hospital stay was approximately 20 days (OR 17.3-22.09). Among the patients, 50.39% were overweight, 63% had hypertension (HTA), 29% had chronic kidney injury, 24% had a history of delirium, and 73% had recent surgical interventions. Patients with diabetes mellitus had a 3.1 times higher risk, those with HTA had a 2.8 times higher risk, and those with kidney injury had a 3.8 times higher risk of having a positive CAM result. It was observed that haloperidol, used in 84% of the patients, showed the highest percentage reduction in CAM scores
Image:
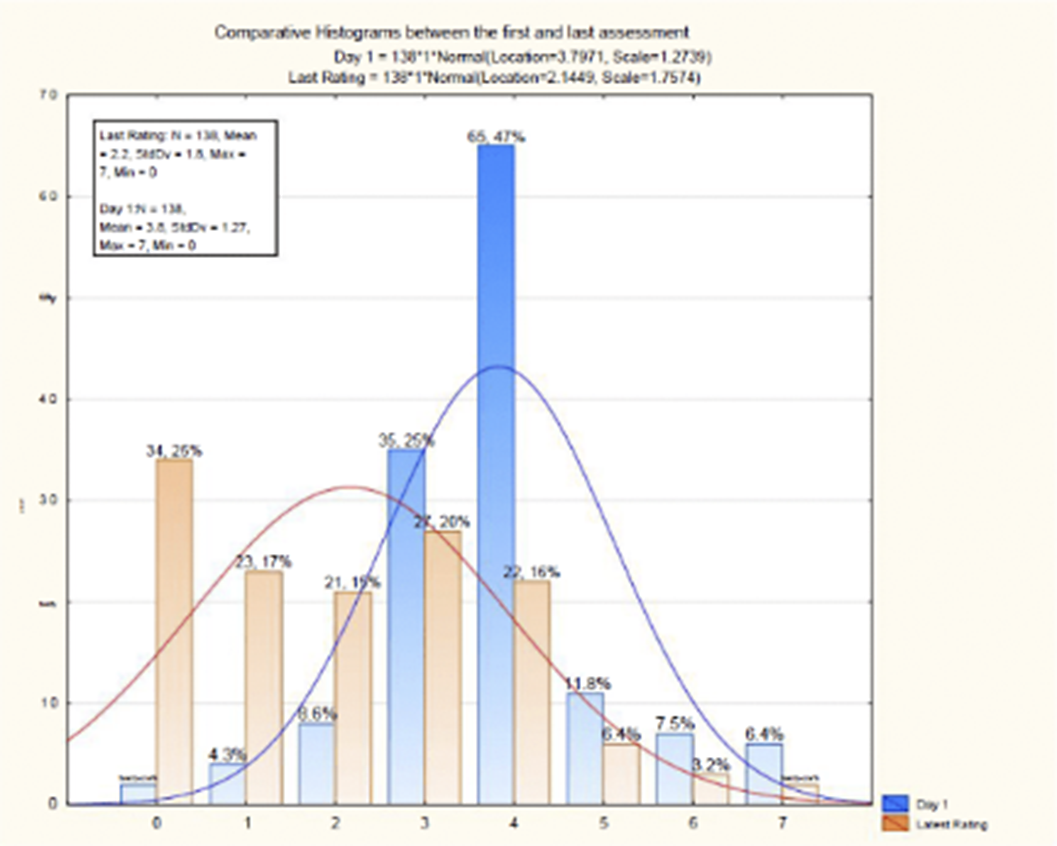
Image 2:
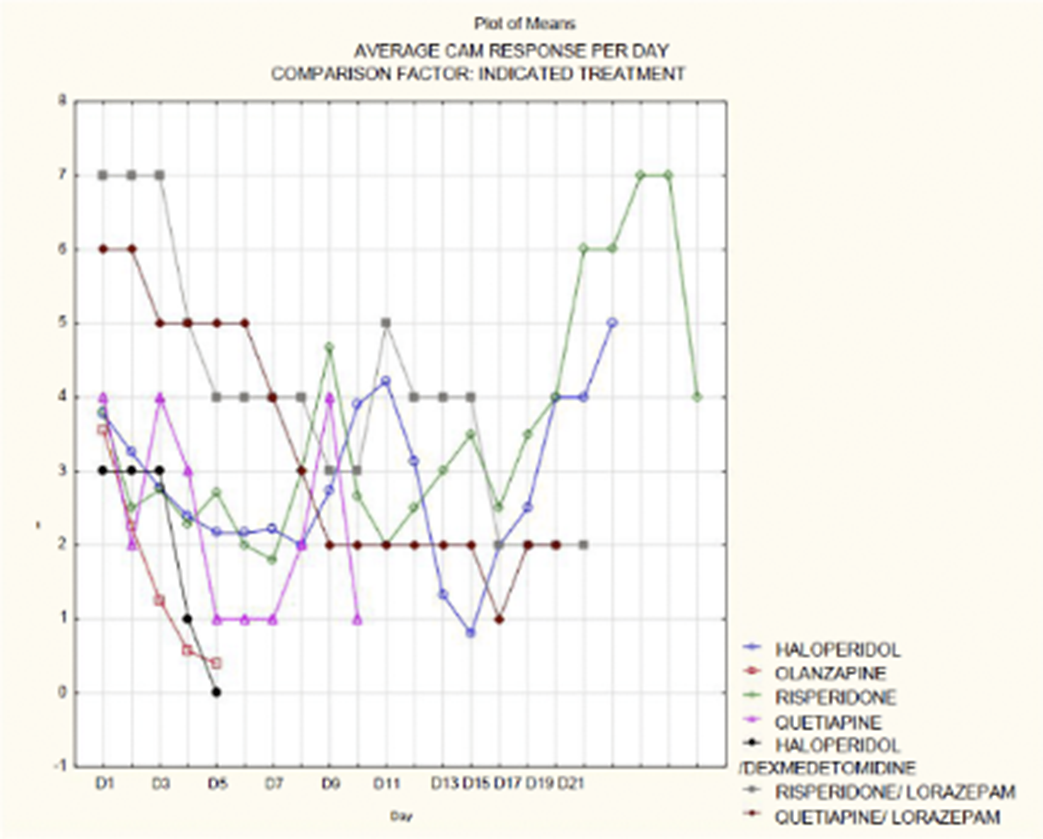 Conclusions
ConclusionsThe results of this study emphasize the importance of identifying risk factors associated with delirium and implementing effective treatment for this condition. It was observed that the average duration of delirium symptoms was approximately 6 days, which is relevant for understanding the course and management of this illness. Furthermore, it was found that the average hospital stay was 20 days, underscoring the burden that delirium can place on healthcare systems.
In conclusion, this study highlights the importance of identifying risk factors and providing appropriate treatment, such as the use of haloperidol, to improve outcomes in patients with delirium.
Disclosure of InterestNone Declared
“Ekbom syndrome: delirium engraved on the skin”
- C. Perez Aparicio, L. Rodriguez Rodriguez, M. J. Gordillo Montaño
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S759-S760
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Ekbom syndrome also known as Morgellons syndrome or delirium of parasitosis is a psychiatric condition where the patient has the absolute conviction of being infested in spite of medical evidence. Patients may even mutilate themselves or apply toxic substances in order to get rid of these hypothetical organisms. Sometimes they bring samples of these hypothetical parasites to the office to prove their existence, which is known as the “matchbox sign”, a pathognomonic finding.
ObjectivesThe aim of this clinical case is to make visible the impact that this psychiatric condition can have on the patient’s quality of life
MethodsWe present the case of a 40-year-old woman from Peru who was admitted to the otorhinolaryngology unit for injuries compatible with necrosis of the right pinna. When the patient was examined, scars were found on the lower limbs and back. The patient justifies the scratching lesions with the presence of pathogenic organisms, with no trace of them by the physician.
ResultsThe patient was evaluated by psychiatry service during her admission in otorhinolaryngology, being diagnosed with Ekbom’s delirium and starting treatment with 3 mL of Aripiprazole. Subsequently she was referred to the mental health unit where she left the follow-up until today.
ConclusionsDifferent effective treatments have been described, among them pimozide, atypical antipsychotics and some SSRIs. However, the complexity of treatment arises when dealing with the irreducible idea that the patient has of being infested, refusing in most cases to receive psychiatric treatment. This can degenerate into major organic and psychological problems that turn the patient’s life into a real hell, which often end up losing much of their daily functionality. The fact of empathizing with the patient and trying to elaborate a plan adjusted to the reality and needs of the moment, can help us to establish a good therapeutic bond that facilitates an early start of treatment and greater therapeutic adherence, enabling a significant improvement in their quality of life.
Disclosure of InterestNone Declared
Relationship between different PANSS cognitive factors and cognition assessed with MCCB in patients with first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, Á. Sánchez-Cabezudo, M. Scala, L. García-Fernández, L. Sánchez-Pastor, D. Rentero, I. Martínez-Gras, M. Caballero, J. M. Espejo-Saavedra, A. Nuñez-Doyle, O. Jiménez-Rodríguez, A. I. Aparicio-León, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S292-S293
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The Positive and Negative Syndrome Scale (PANSS) has been used as a universal instrument for clinical assessment of psychopathology in schizophrenia. Different studies have analyzed the factorial structure of this scale and have suggested a five-factor model: positive, negative, excited, depressive, and cognitive/disorganized factors. Two of the most used models are the Marder´s solution and the Wallwork´s one.
ObjectivesThe aim of this work was to study the correlations of the two cognitive factors (Marder and Wallwork) with a cognitive assessment performed with a standard cognitive battery, in a sample of patients with first psychotic episode of schizophrenia.
MethodsSeventy four patients with first psychotic episode of schizophrenia (26.9, SD:7.8 years old; 70.3% male) were included. The cognitive assessment was performed with the MATRICS Consensus Cognitive Battery (MCCB). The MCCB present seven cognitive domains: Speed of processing, Working memory, Attention/Vigilance, Verbal Learning, Visual Learning, Reasoning and Problem Solving, and Social cognition). Pearson correlations were performed between MCCB scores and Marder´s PANSS cognitive factor (P2, N5, G5, G10, G11, G13, G15) and Wallwork´s one (P2, N5, G11).
ResultsCorrelation between MCCB scores and cognitive factors of Marder and Wallwork can be seen in the table.
Marder´s cognitive factor Wallwork´s cognitive factor Speed of processing r = -0.461; p<0.001 r = -0.455; p<0.001 Attention/Vigilance r = -0.414; p<0.001 r = -0.415; p<0.001 Working memory r = -0.449; p<0.001 r = -0.468; p<0.001 Verbal Learning r = -0.511; p<0.001 r = -0.405; p<0.001 Visual Learning r = -0.252; p=0.024 r = -0.254; p=0.029 Reasoning and Problem Solving r = -0.244; p=0.036 r = -0.272; p=0.019 Social cognition r = -0.268; p=0.024 r = -0.202; p=0.091 ConclusionsBoth PANSS cognition factors show a moderate correlations with Speed of processing, Working memory, Attention/Vigilance and Verbal Learning assessed by MCCB. More discrete correlations were found with Visual Learning, Reasoning and Problem Solving, and with Social cognition (in fact, non-significant correlation with Wallwork´s cognitive factor was found).
Acknowledgements. This study has been funded by Instituto de Salud Carlos III (ISCIII) through the project PI19/00766 and co-funded by the European Union.
Disclosure of InterestNone Declared
A man stitches his mouth in the context of a personality disorder
- A. Monllor Lazarraga, P. Marques Cabezas, L. Rojas Vazquez, M. Rios Vaquero, G. Lorenzo Chapatte, T. Jimenez Aparicio, C. De Andres Lobo, C. Vallecillo Adame, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodriguez Rodriguez, M. Fernandez Lozano, M. A. Andreo Vidal, M. Calvo Valcarcel, M. P. Pando Fernandez, P. Martinez Gimeno, G. Guerra Valera
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S654-S655
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
A 28 year old patient will be presented. This paramilitary man was brought to the Emergency Room due to an autolytic attempt with Benzodiazepines, along with a mouth suture, in the context of a soon to be resolved problematic ankle osteosynthesis procedure. The patient claimed to be suffering pain, furthermore struggling due to the fact he could not be working due to his ankle issue. Language barrier was a problem during the interview.
ObjectivesThe objetives of this case is to try to explain the issues that may arise in patients with personality disorders in the context of an autolytic attempt
MethodsThis patient will be presented, along with systematic bibliography review of the topic.
ResultsThe following results were extracted upon the attention given to this patient which was admitted to the Psychiatric Unit.
First of all, the mouth stitches were removed, along with a petition for toxicological analysis. The results gave positive for cannabis and benzodiazepines. The patient was also brought previously this year with another autolytic attempt, this time on cocaine consumption too. Furthermore, a thorough review was made of the other autolytic attempts, including those which happened in his country of origin. The patient has hundreds of small cuts among his arms, from previews cuts made in the past. Furthermore, subcutaneous wounds were auto inflicted in the ER, with a small blade.
Among the whole interview, it was clear he had a personality disorder, with high impulsivity levels and lack of control once the situation overflows.
We also tried to understand the outcome of suturing his mouth. The patient referred his acts of impulsiveness due to his overwhelming situation of both having no job at this moment and the pain he was suffering due to his ankle procedure.
The patient was admitted to our Unit due to the high risk he could repeat this act. Upon arrival, the same day he was admitted, the patient asked if he had to stay at the unit. When explaining the following already told event, furthermore insisting in the possibility of been evaluated by the Traumatology team, he proceeded to try and hang himself with his medical-hospital clothing.
The patient was treated with antipsychotics. Along with Lormetazepam at night. At the end of the hospitalization, and after been evaluated by the Psychiatrist of this Unit, the patient was also treated with Lithium due to its effectiveness in the treatment of autolytic attempts.
ConclusionsPersonality disorders are one of the psychiatric pathologies that prevail with greater frequency in autolytic attempts 1. Additionally, it should be taken into account the possible ongoing consumption of psychoactive drugs that could also derive in psychopathological decompensation. On top of the following, the use of antipsychotic treatment is indicated for the managing of conduction altercations 2, besides Lithium being a great option in managing suicidal temptations 3.
Disclosure of InterestNone Declared
From schizotypy to psychosis: is it a natural continuum?
- M. A. Andreo Vidal, M. B. Arribas Simón, M. Calvo Valcárcel, M. P. Pando Fernández, P. Martínez Gimeno, M. D. L. Á. Guillén Soto, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, C. De Andrés Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, Ó. Martín Santiago, A. Monllor Lazarraga, M. Ríos Vaquero, L. Rojas Vázquez, L. Sobrino Conde, A. Apario Parra, G. Lorenzo Chapatte
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S658-S659
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal personality is a condition suffered by 4% of the population. It is defined by presenting interpersonal, behavioral and perceptual features similar to the clinical features of psychotic disorders, such as schizophrenia, in less intensity and dysfunctionality, but at risk of reaching psychosis.
ObjectivesPresentation of a clinical case about a patient with premorbid schizotypal personality traits presenting with an acute psychotic episode.
MethodsLiterature review on association between schizotypal personality and psychosis.
ResultsA 57-year-old woman with a history of adaptive disorder due to work problems 13 years ago, currently without psychopharmacological treatment, goes to the emergency room brought by the emergency services due to behavioral alteration. She reports that “her husband and son wanted to sexually abuse her”, so she had to run away from home and has been running through the streets of the town without clothes and barefoot.
Her husband relates attitude alterations and extravagant behaviors of years of evolution, such as going on diets of eating only bread for 40 days or talking about exoteric and religious subjects, as believing that the devil got inside her husband through a dental implant. He reports that these behaviors have been accentuated during the last month. She has also created a tarot website, and has even had discussions with several users. She is increasingly suspicious of him, has stopped talking to him and stays in his room all day long, with unmotivated laughter and soliloquies.
It was decided to admit him to Psychiatry and risperidone 4 mg was started. At the beginning, she was suspicious and reticent in the interview. As the days went by, communication improved, she showed a relaxed gesture and distanced herself from the delirious ideation, criticizing the episode.
ConclusionsIn recent years, there has been increasing interest in understanding the association between schizotypy and serious mental disorder. Several theories understand schizotypy as a natural continuum of personality that reveals genetic vulnerability and that can lead to psychotic disorder when added to precipitating factors. Other theories define schizotypy as a “latent schizophrenia” where symptoms are contained and expressed in less intensity.
Around 20% evolves to paranoid schizophrenia or other serious mental disorders. It is complex to distinguish between those individuals in whom schizotypy is a prodrome and those in whom it is a stable personality trait. To date, studies applying early psychotherapeutic or pharmacological interventions have had insufficient and contradictory results, and the follow-up and treatment of these individuals could be a stress factor and a stigma. Some studies are looking for reliable markers of evolution to schizophrenia in order to establish adequate protocols for detention, follow-up and treatment.
Disclosure of InterestNone Declared
Conversive and Factitious disorders: Differential diagnosis based on a case report
- M. Fernandez Lozano, B. Rodriguez Rodriguez, N. Navarro Barriga, M. J. Mateos Sexmero, C. Alario Ruiz, L. Rodriguez Andrés, G. Medina Ojeda, T. Jimenez Aparicio, C. Vallecillo Adame, C. De Andres Lobo, M. A. Andreo Vidal, P. Martínez Gimeno, M. Calvo Valcarcel, M. P. Pando Fernández, L. Rojas Vazquez, M. Rios Vaquero, G. Lorenzo Chapatte, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S444
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Conversive disorder is characterised by the presence of one or more involuntary neurological symptoms that are not due to a clear medical pathology. On the other hand, consciously simulated illnesses fall into two diagnostic categories: factitious disorders and malingering, which are differentiated by both the motivation for the behaviour and the awareness of that motivation. Factitious disorder behaviours are motivated by an unconscious need to assume the sick role, whereas malingering behaviours are consciously driven to achieve external secondary gains.
ObjectivesStudy of the differences between conversion disorder and factitious disorder and their repercussions from a case of difficult diagnosis.
MethodsBibliographic review of scientific literature based on a relevant clinical case.
ResultsWe present the case of a 14-year-old male patient. Adoptive parents. Studying in high school. Social difficulties since childhood. He comes to the emergency department on several occasions referring stereotyped movements and motor tics in the four extremities with left cervical lateralization. Increase of these symptoms in the last month, so it was decided to admit him to the pediatric hospital. After observation and study of the patient’s movements with normal complementary tests he should return home. The following day he returned to the emergency department after an episode of dizziness, mutism and emotional block. It was decided to admit him to Psychiatry for behavioral observation and differential diagnosis.
ConclusionsIn the assessment of patients it is essential to make an appropriate diagnosis taking into account the patient’s symptomatology and the patient’s background and life context. Conversion disorder is the unintentional production of neurological symptom, whereas malingering and factitious disorder represent the voluntary production of symptoms with internal or external incentives. They have a close history and this has been frequently confounded. Practitioners are often confronted to medically unexplained symptoms; they represent almost 30% of neurologist’s consultation. The first challenge is to detect them, and recent studies have confirmed the importance of “positive” clinical bedside signs based on incoherence and discordance. Multidisciplinary therapy is recommended with behavioral cognitive therapy, antidepressant to treat frequent comorbid anxiety or depression, and physiotherapy. Factitious disorder and malingering should be clearly delineated from conversion disorder. Factitious disorder should be considered as a mental illness and more research on its physiopathology and treatment is needed, when malingering is a non-medical condition encountered in medico-legal cases.
Disclosure of InterestNone Declared
“God speaks to me through a dove”. The evidence of clozapine in treatment-refractory psychosis
- B. Rodríguez Rodríguez, P. Marqués Cabezas, M. Queipo de Llano de La Viuda, N. Navarro Barriga, G. Guerra Valera, M. B. Arribas Simón, C. Alario Ruiz, M. J. Mateos Sexmero, M. Fernández Lozano, P. Marínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal, M. P. Pando Fernández, A. Monllor Lazarraga, M. Ríos Vaquero, G. Lorenzo Chapate, L. Rojas Vázquez, C. De Andrés Lobo, T. Jiménez Aparicio, M. D. C. Vallecillo Adame
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is an atypical antipsychotic synthesised in 1958. It was withdrawn from the market in the 1970s due to the appearance of agranulocytosis, but was reintroduced due to strong evidence of its efficacy and superiority over other antipsychotics in treatment-resistant schizophrenia.
ObjectivesTo describe the adequate response to clozapine in treatment-refractory psychosis.
MethodsReview of the scientific literature based on a relevant clinical case.
ResultsA 16-year-old woman was admitted to a psychiatric inpatient unit for psychotic symptoms and behavioural disorders. She lives with her father and older sister; she has not been in contact with her mother, who lives in another country, for several years. She attends secondary school, with poor academic performance. Maternal diagnosis of schizophrenia. She started using cannabis two years ago, with a progressive increase up to 20 grams per week. He reports the onset of a feeling of strangeness a year ago, with progressive isolation in his room, referring to delirious ideation of harm towards classmates and people from his town, self-referentiality and delirious interpretations of religious mystical content (“God speaks to me through a dove”). He comments on the phenomenon of theft and thought-reading. Soliloquies and unmotivated laughter are observed.
ConclusionsTreatment was started with risperidone, progressively increasing the dose up to optimisation, without achieving a decrease in positive symptoms, but with the appearance of excessive sedation and sialorrhoea. It was combined with aripiprazole up to 20mg, maintained for a couple of weeks, without significant clinical improvement. Given the failure of two lines of therapy, it was decided to change to clozapine up to a dose of 75mg, with adequate tolerance and response, achieving a distancing of the delirious ideation. Regular haematological controls were performed, with no alterations in haemogram or troponins.
Disclosure of InterestNone Declared
Brief Psychotherapeutic and Psychopharmacological Interventions as Facilitators of Bariatric Surgery Success in Patients on the Anxious-Impulsive Spectrum: A Pilot Study
- Í. Alberdi-Páramo, M. Navas Tejedor, M. Paz Otero, J. Sánchez- Rodríguez, D. Gimeno Álvarez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S491
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients undergoing bariatric surgery often present with impulsive behavior and symptoms of anxiety. In this context, brief psychotherapeutic interventions such as nutritional education, cognitive restructuring, and behavioral activation have been shown to enhance pre-surgery weight loss and improve the likelihood of successful surgical outcomes. Furthermore, anorexigenic pharmacological treatments involving fluoxetine, bupropion, naltrexone, eslicarbazepine, zonisamide, and topiramate have been associated with increased success rates of the bariatric intervention.
ObjectivesTo assess the impact of brief psychotherapeutic interventions and psychopharmacological treatments on the success of bariatric surgery in anxious-impulsive patients, investigating the effectiveness of combined strategies in enhancing preoperative weight loss and surgical outcomes.
MethodsWithin the framework of a third-level hospital’s Bariatric Surgery Protocol, a total of 63 obese patients were assessed using the MINI International Neuropsychiatric Interview (MINI), Hamilton Anxiety Rating Scale (HARS), and Barratt Impulsiveness Scale (BIS-11) during the pre-surgical evaluation. Patients with Axis I pathologies were excluded, leaving a sample of 56 participants (38 females; BMI: 43.58±8.72 kg/m2; age: 48.5±9.7 years). Individuals displaying mild anxiety (6-14 points on HARS) and moderate/severe anxiety (>14 points on HARS) and/or those with a BIS-11 score exceeding 32.5 were selected for combined psychotherapeutic and psychopharmacological interventions.
ResultsCategorized by anxiety and impulsiveness levels, the patient distribution was as follows:
Mild anxiety without impulsiveness: 19 patients
Mild anxiety with impulsiveness: 31 patients
Moderate/severe anxiety without impulsiveness: 2 patients
Moderate/severe anxiety with impulsiveness: 15 patients
This pilot study explores the potential synergy between brief psychotherapeutic interventions and psychopharmacological approaches in enhancing the outcomes of bariatric surgery for patients within the anxious-impulsive spectrum.
ConclusionsThe results shed light on the feasibility and potential benefits of a combined treatment strategy, contributing to the optimization of bariatric surgery success in this specific patient population. Further research is warranted to confirm and generalize these findings.
Disclosure of InterestNone Declared
Drug-induced psychosis and intravenous drug use in chemsex context
- J. Curto Ramos, A. Rodríguez Laguna, P. Barrio, L. Ibarguchi, A. García, I. Azqueta, H. Dolengevich Segal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S413
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Several studies have called atention to the mental health disorders associated with chemsex -the intentional use of drugs before or during sexual intercourse GBMSM (gay, bisexual and men who have sex with men) population-. Sexualized intravenous drug use is also known as slam or slamsex. There are few studies that analyze the mental health differences between intravenous drug users compared to non-intravenous drug users in chemsex context.
ObjectivesWe aim to analyze the relationship between the practice of slamsex and the development of drug-induced psychosis.
MethodsA cross-sectional descriptive analysis of a sample of users attended by the non-governmental organization Apoyo Positivo in the program “Sex, Drugs and You” between 2016-2019 was performed.
ResultsWe included 217 participants. Drug-induced psychosis was found in 80 participants. Drug-induced psychosis was significantly higher in the intravenous drug use group compared to the non-intravenous drug use group (p<0.05).
ConclusionsPrevious studies have reported that MSM who practiced chemsex were more likely to experience from different mental health disorders, being psychosis one of the most frequent psychiatric diagnoses. In our study, drug-induced psychosis was higher in participants who engaged in intravenous drug use. Further studies analyzing the relationship between slamsex and drug-induced psychosis are needed.
Disclosure of InterestNone Declared
Persistent COVID an differential diagnosis with depression symptoms
- B. Arribas Simon, M. J. Mateos-Sexmero, O. Martin-Santiago, P. Andres-Olivera, B. Rodriguez-Rodriguez, P. Martinez-Gimeno, N. Navarro-Barriga, T. Jimenez-Aparicio, M. Andreo-Vidal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S502
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a 48-year-old woman, a nurse, referred from the Internal Medicine department for evaluation of depressive symptoms and accompanying somatic presentation following COVID-19. The aim is to highlight a recently emerging condition that we are increasingly encountering in our clinics, which can complicate the diagnosis of an underlying affective disorder
ObjectivesDiagnosed with COVID-19, confirmed by a positive PCR test, 6 months ago following an infection in the workplace. The clinical picture consisted of mild symptoms, with a ten-day course and apparent resolution at the time of hospitalization. She returned to her work activities and gradually began to report fluctuating symptoms, including headaches, mild shortness of breath, fatigue, as well as a tingling sensation in the upper extremities, especially in the hands. Additionally, she described feelings of restlessness, depressive mood, and intense fatigue. In additional tests: (CT-Scan) there are signs of mild bilateral lower lung fibrosis.
MethodsTreatment with Duloxetine was initiated for a case of depressive symptoms with accompanying physical symptoms. The differential diagnosis considered Major Depressive Disorder, Single Episode, and Adjustment Disorder with Depressed Mood.”
ResultsWe are facing a clear case of depressive clinic that may have endogenous features, if we adhere to criteria such as those in the DSM-5, as it would meet the criteria for Major Depressive Disorder, Single Episode. However, we have a clearly identified trigger, so we also need to perform a differential diagnosis, primarily with Adjustment Disorder with Depressed Mood: here, the symptoms appear within 3 months following the stressful agent (in this case, SARS-CoV-2 infection). Unlike Major Depressive Episode, once the agent has ceased, the symptoms do not persist beyond 6 months (which we do not know because the physical symptoms causing disability have not disappeared).In addition to purely psychiatric diagnoses that we are accustomed to, we must consider a new diagnostic entity that is becoming more prevalent as the pandemic progresses, namely “long-covid” or persistent COVID.These are generally middle-aged women who, several months after infection, continue to manifest a multifactorial complex of symptoms. These symptoms persist over time, not only the classical ones but also many others that can appear during the ongoing course of the disease.
ConclusionsBeyond the purely psychiatric diagnoses we are accustomed to, we must also consider a new diagnostic entity that is becoming more prevalent as the pandemic continues to advance: Persistent COVID or ‘long-COVID.’ Generally, this condition affects middle-aged women who, several months after contracting the virus, continue to exhibit a multifactorial complex of symptoms. The most common symptoms include fatigue/asthenia (95.91%); general discomfort (95.47%); headaches (86.53%); and low mood (86.21%)
Disclosure of InterestNone Declared
Artificial intelligence and virtual reality applied to the clinical care of women with schizophrenia: A systematic review.
- J. P. Paolini San Miguel, M. Natividad, M. V. Seeman, B. Palacios, A. Balagué, E. Román, N. Bagué, E. Izquierdo, H. Cachinero, J. A. Monreal, A. González Rodríguez
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S734-S735
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Artificial intelligence (AI) and virtual reality (VR) are useful tools that can improve precision medicine and can prove useful in the clinical care of patients with psychosis.
ObjectivesOur aim was to determine whether AI and VR have been applied to the prediction of clinical response in women with schizophrenia.
MethodsA systematic review was carried out in PubMed and Scopus from inception to September 2023 by using the PRISMA guidelines. Search terms: (“artificial intelligence” OR “intelligent support” OR “machine intelligence” OR “machine learning” OR “virtual reality” OR “intelligent agent” OR “neural networks” OR “virtual reality” OR “digital twins”) AND (“schizophrenia” OR “psychosis”) AND (“women” OR gender”). Inclusion criteria: 1)English, French, German or Spanish language, 2) reporting treatment response in schizophrenia (as long as information in women was included), and 3) including AI and VR techniques.
ResultsFrom a total of 320 abstracts initially screened (PubMed:182, Scopus:138), we selected 6 studies that met criteria.
- Prediction of treatment response. (1) Clinical information, genetic risk score and proxy methylation score have been shown to improve prediction models. (2) Graph-theory-based measures have been combined with machine learning.
- Therapeutic drug monitoring. (1) A machine learning model has been useful in predicting quetiapine blood concentrations.
- Pharmacovigilance. (1) Machine learning has connected prolactin levels and response in olanzapine-treated patients. (Zhu et al., 2022).
- Treatment-resistant schizophrenia (TRS). (1) Women with TRS have been found to receive clozapine less frequently than men (adjusted for sociodemographic, biological and clinical factors). (2) Statistical learning approach: Women have been found to respond better to clozapine than men.
ConclusionsAI, including machine learning, show promising results in the prediction of treatment response in women with schizophrenia. As of yet, digital twins have not been investigated to test specific interventions or to personalize treatment in women with schizophrenia.
Disclosure of InterestNone Declared
Bipolar Disorder in Pregnancy: A Challenging Case Managed with Maintenance Electroconvulsive Therapy
- B. Arribas-Simon, M. J. Mateos-Sexmero, O. Martin-Santiago, P. Andres-Olivera, B. Rodriguez-Rodriguez, P. Martinez-Gimeno, N. Navarro-Barriga, T. Jimenez-Aparicio, P. Fernandez-Pando, M. Andreo-Vidal
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S115-S116
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Pregnancy is a high-risk period for major affective disorders and can lead to a destabilizing period for our patients. Standard pharmacological strategies must be carefully evaluated due to potential teratogenic or side effects. We present a case of bipolar disorder type I with challenging-to-control maniac episodes during pregnancy, which has required Electroconvulsive Therapy for its management.
ObjectivesPresenting maintenance electroconvulsive therapy (ECT) as a safe and effective therapeutic strategy during pregnancy, with the presentation of a case in which it has been administered every 3 weeks from the second trimester until the baby’s birth at 37 weeks
MethodsThis concerns a 28-year-old immigrant woman, married, with a 10-year-old child. She was diagnosed with bipolar disorder type I at the age of 16 when she experienced her first manic episode in her country of origin. Subsequently, during her first pregnancy, she required hospitalization for electroconvulsive therapy (ECT) treatment, with a positive response after a single session. She remained stable for several years without maintenance pharmacological treatment or follow-up until the ninth week of her second pregnancy when she experienced a manic episode requiring hospitalization.
ResultsShe was initially treated with Olanzapine and Lorazepam with a positive response, but three weeks later, she was readmitted with a similar episode. These decompensations occurred almost monthly, leading to the consideration of introducing mood stabilizers after the first trimester. However, due to the patient’s severe hyperemesis gravidarum, this stabilizing treatment was ruled out due to the difficulty in controlling its blood levels and the associated risk of intoxication. During the fifth admission at the 20th week of gestation, the decision was made to initiate ECT treatment, which yielded an excellent response and subsequent maintenance.
ConclusionsThe indications for electroconvulsive therapy (ECT) during pregnancy are the same as in the rest of adult patients. In individuals with a psychiatric history, it is possible for a relapse of mental illness to occur during pregnancy, although the risk is considerably higher during the postpartum period. ECT is considered an effective and safe treatment option in all three trimesters of pregnancy and the postpartum period. During the informed consent process, patients should be informed about the potential impact of ECT as well as alternative treatment options.
Disclosure of InterestNone Declared
Lithium withdrawal and relapse in bipolar disorder when kidney function deteriorates
- C. De Andrés-Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, A. Rodríguez Campos, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Fernández Lozano, M. Calvo Valcárcel, M. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, L. Rojas Vázquez, G. Lorenzo Chapatte, M. Ríos Vaquero, A. Monllor Lazarraga
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S427-S428
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium was the first mood stabilizer and today continues to be a first-line treatment in the treatment of bipolar disorder despite its adverse effects, which make it important to monitor blood levels and control kidney function.
ObjectivesPresentation of a case of litium withdrawal and relapse in bipolar disorder. Literature review relating to the risk of relapse when lithium treatment is interrupted.
MethodsWe present a clinical case of a patient who suffers a deterioration in renal function that requires the withdrawal of lithium and who consequently suffers a relapse. We conducted a bibliographic research of articles in Pubmed on this topic.
ResultsA 49-year-old male, with a history of multiple admissions to UHB since the age of 18 with a diagnosis of bipolar disorder and treatment with lithium. Decompensations towards the manic pole have always been related to interruptions in lithium treatment. On several occasions when the patient was feeling well emotionally, he believed himself to be “cured” and abandoned the treatment, triggering a manic episode, showing verbal aggression, increased self-esteem and delusional ideation of harm. Remission was usually achieved with the reintroduction of lithium and the addition of high-dose quetiapine. Between episodes, constant overvalued ideas of economic scarcity seemed to persist, which were accentuated in the form of delusional ideas of ruin in depressive decompensations. After 7 years of stability, control analysis showed blood litemia of 2.2 mEq/L with deterioration of kidney function and generalized tremor was observed, without improvement after serum therapy. He was admitted for dialysis and lithium was suspended. Treatment with valproate was started and a consultation scheduled in a week to adjust the dose. The patient did not attend that consultation and was admitted three days later to Psychiatry Hospitalization showing a challenging attitude, evident dysphoric mood, accelerated speech, with derailments and echolalia. Delusional ideation of harm with auditory hallucinations. Insomnia and hyporexia. Chronic renal failure persisted.
ConclusionsLithium is a very effective drug but with a narrow therapeutic range that requires adequate monitoring due to the possible consequences of its use at different organs and systems of the body. when lithium is found in the blood at toxic levels with deterioration of kidney function and glomerular filtration fails to recover, lithium treatment should be suspended. Sudden withdrawal of lithium significantly increases the risk of relapse due to rebound effect. More than 50% of patients experience a recurrence within 10 weeks of withdrawal.
Disclosure of InterestNone Declared
Sodium Oxybate-Induced secondary mania with psychotic symptoms: a case report and literature review
- C. Cárdenes Moreno, S. Yelmo-Cruz, I. Pérez Sagaseta de Ilurdoz, J. J. Tascón-Cervera, G. P. González-Rodríguez, M. Gallego-Restrepo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S693
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Sodium oxybate, an effective treatment for narcolepsy-associated daytime sleepiness and cataplexy, has been extensively. Despite its therapeutic benefits, sodium oxybate is not without its risks, and adverse psychiatric effects have been documented. This case report highlights a rare manifestation of sodium oxybate-related secondary mania with psychotic symptoms in a patient with narcolepsy, emphasizing the importance of recognizing and managing such adverse events. Additionally, we provide a brief review of similar cases reported in the literature.
ObjectivesThis report aims to describe the presentation, evaluation, and management of sodium oxybate-induced secondary mania with psychotic symptoms in a patient with narcolepsy. We also discuss the potential mechanisms underlying this adverse reaction and its clinical implications. Furthermore, we summarize findings from previous studies that have reported cases of secondary mania associated with sodium oxybate use.
MethodsWe present the case of Mr. X, a 48-year-old male diagnosed with “Narcolepsy with cataplexy,” who had been receiving sodium oxybate treatment for 11 years. He was admitted to the hospital following a mild head injury and the emergence of a manic episode with psychotic features. Comprehensive clinical evaluation, including medical history, toxicology screening, and neuroimaging, was conducted.
ResultsUpon evaluation, Mr. X exhibited hyperactivity, restlessnes, grandiose delusions, paranoid delusions related to hospital staff, and decreased need for sleep. Notably, he had been consuming sodium oxybate excessively. Sodium oxybate was discontinued, and low-dose olanzapine was initiated. Within 24 hours, his manic and psychotic symptoms resolved. He admitted to overusing his medication, and his family reported a recent increase in his activity level. A review of the literature revealed similar cases of sodium oxybate-induced secondary mania with psychotic symptoms.
ConclusionsThis case underscores the importance of vigilance for psychiatric side effects of sodium oxybate, particularly in patients with a history of substance abuse or potential overuse. Secondary mania associated with medications is a rare but significant clinical entity. Prompt recognition and intervention are crucial for patient safety and well-being. Further research is needed to elucidate the mechanisms underlying such reactions and to establish guidelines for their prevention and management.
Disclosure of InterestNone Declared



