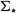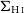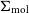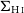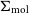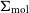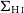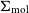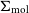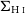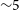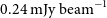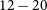115 results
Preventing unnecessary urine cultures at a Veteran’s affairs healthcare system
- Chad D. Nix, William B. Messer, Amy Boda, Kimberly T. MacKay, Jennifer Holmquist, La’Tonzia L. Adams, Eric Gladwin, Christopher D. Pfeiffer
-
- Journal:
- Infection Control & Hospital Epidemiology , First View
- Published online by Cambridge University Press:
- 25 March 2024, pp. 1-3
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
Virtual care during COVID-19: The perspectives of older adults and their healthcare providers in a cardiac rehabilitation setting
- Cecilia Flores-Sandoval, Shannon L. Sibbald, Bridget L. Ryan, Tracey L. Adams, Neville Suskin, Robert McKelvie, Jacobi Elliott, Joseph B. Orange
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement , First View
- Published online by Cambridge University Press:
- 23 February 2024, pp. 1-8
-
- Article
- Export citation
-
The present study aimed to explore the perspectives of older adults and health providers on cardiac rehabilitation care provided virtually during COVID-19. A qualitative exploratory methodology was used. Semi-structured interviews were conducted with 15 older adults and 6 healthcare providers. Five themes emerged from the data: (1) Lack of emotional intimacy when receiving virtual care, (2) Inadequacy of virtual platforms, (3) Saving time with virtual care, (4) Virtual care facilitated accessibility, and (5) Loss of connections with patients and colleagues. Given that virtual care continues to be implemented, and in some instances touted as an optimal option for the delivery of cardiac rehabilitation, it is critical to address the needs of older adults living with cardiovascular disease and their healthcare providers. This is particularly crucial related to issues accessing and using technology, as well as older adults’ need to build trust and emotional connection with their providers.
Increasing the equitability of data citation in paleontology: capacity building for the big data future
- Jansen A. Smith, Nussaïbah B. Raja, Thomas Clements, Danijela Dimitrijević, Elizabeth M. Dowding, Emma M. Dunne, Bryan M. Gee, Pedro L. Godoy, Elizabeth M. Lombardi, Laura P. A. Mulvey, Paulina S. Nätscher, Carl J. Reddin, Bryan Shirley, Rachel C. M. Warnock, Ádám T. Kocsis
-
- Journal:
- Paleobiology , First View
- Published online by Cambridge University Press:
- 28 December 2023, pp. 1-12
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Data compilations expand the scope of research; however, data citation practice lags behind advances in data use. It remains uncommon for data users to credit data producers in professionally meaningful ways. In paleontology, databases like the Paleobiology Database (PBDB) enable assessment of patterns and processes spanning millions of years, up to global scale. The status quo for data citation creates an imbalance wherein publications drawing data from the PBDB receive significantly more citations (median: 4.3 ± 3.5 citations/year) than the publications producing the data (1.4 ± 1.3 citations/year). By accounting for data reuse where citations were neglected, the projected citation rate for data-provisioning publications approached parity (4.2 ± 2.2 citations/year) and the impact factor of paleontological journals (n = 55) increased by an average of 13.4% (maximum increase = 57.8%) in 2019. Without rebalancing the distribution of scientific credit, emerging “big data” research in paleontology—and science in general—is at risk of undercutting itself through a systematic devaluation of the work that is foundational to the discipline.
6 Remote Smartphone Cognitive and Motor Testing in Frontotemporal Dementia Research: Feasibility, Reliability, and Validity
- Adam M Staffaroni, Jack Carson Taylor, Annie L Clark, Hilary W Heuer, Amy B Wise, Masood Manoochehri, Leah Forsberg, Carly T Mester, Meghana Roa, Danielle Brushaber, Julio C Rojas, Joel H Kramer, Bradley F Boeve, Howard J Rosen, Adam L Boxer
-
- Journal:
- Journal of the International Neuropsychological Society / Volume 29 / Issue s1 / November 2023
- Published online by Cambridge University Press:
- 21 December 2023, pp. 604-605
-
- Article
-
- You have access Access
- Export citation
-
Objective:
Therapeutics targeting frontotemporal dementia (FTD) are entering clinical trials. There are challenges to conducting these studies, including the relative rarity of the disease. Remote assessment tools could increase access to clinical research and pave the way for decentralized clinical trials. We developed the ALLFTD Mobile App, a smartphone application that includes assessments of cognition, speech/language, and motor functioning. The objectives were to determine the feasibility and acceptability of collecting remote smartphone data in a multicenter FTD research study and evaluate the reliability and validity of the smartphone cognitive and motor measures.
Participants and Methods:A diagnostically mixed sample of 207 participants with FTD or from familial FTD kindreds (CDR®+NACC-FTLD=0 [n=91]; CDR®+NACC-FTLD=0.5 [n=39]; CDR®+NACC-FTLD>1 [n=39]; unknown [n=38]) were asked to remotely complete a battery of tests on their smartphones three times over two weeks. Measures included five executive functioning (EF) tests, an adaptive memory test, and participant experience surveys. A subset completed smartphone tests of balance at home (n=31) and a finger tapping test (FTT) in the clinic (n=11). We analyzed adherence (percentage of available measures that were completed) and user experience. We evaluated Spearman-Brown split-half reliability (100 iterations) using the first available assessment for each participant. We assessed test-retest reliability across all available assessments by estimating intraclass correlation coefficients (ICC). To investigate construct validity, we fit regression models testing the association of the smartphone measures with gold-standard neuropsychological outcomes (UDS3-EF composite [Staffaroni et al., 2021], CVLT3-Brief Form [CVLT3-BF] Immediate Recall, mechanical FTT), measures of disease severity (CDR®+NACC-FTLD Box Score & Progressive Supranuclear Palsy Rating Scale [PSPRS]), and regional gray matter volumes (cognitive tests only).
Results:Participants completed 70% of tasks. Most reported that the instructions were understandable (93%), considered the time commitment acceptable (97%), and were willing to complete additional assessments (98%). Split-half reliability was excellent for the executive functioning (r’s=0.93-0.99) and good for the memory test (r=0.78). Test-retest reliabilities ranged from acceptable to excellent for cognitive tasks (ICC: 0.70-0.96) and were excellent for the balance (ICC=0.97) and good for FTT (ICC=0.89). Smartphone EF measures were strongly associated with the UDS3-EF composite (ß's=0.6-0.8, all p<.001), and the memory test was strongly correlated with total immediate recall on the CVLT3-BF (ß=0.7, p<.001). Smartphone FTT was associated with mechanical FTT (ß=0.9, p=.02), and greater acceleration on the balance test was associated with more motor features (ß=0.6, p=0.02). Worse performance on all cognitive tests was associated with greater disease severity (ß's=0.5-0.7, all p<.001). Poorer performance on the smartphone EF tasks was associated with smaller frontoparietal/subcortical volume (ß's=0.4-0.6, all p<.015) and worse memory scores with smaller hippocampal volume (ß=0.5, p<.001).
Conclusions:These results suggest remote digital data collection of cognitive and motor functioning in FTD research is feasible and acceptable. These findings also support the reliability and validity of unsupervised ALLFTD Mobile App cognitive tests and provide preliminary support for the motor measures, although further study in larger samples is required.
Efficacy of maintenance electroconvulsive therapy in recurrent depression: a case series
- G. Guerra Valera, Ó. Martín Santiago, M. Esperesate Pajares, Q. D. L. de la Viuda, A. A. Gonzaga Ramírez, C. Vallecillo Adame, C. de Andrés Lobo, T. Jiménez Aparicio, N. Navarro Barriga, B. Rodríguez Rodríguez, M. Fernández Lozano, M. J. Mateos Sexmero, A. Aparicio Parras, M. Calvo Valcárcel, M. A. Andreo Vidal, P. Martínez Gimeno, M. P. Pando Fernández, M. D. L. Á. Guillén Soto
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S832
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Maintenance electroconvulsive therapy (mECT) is an option in the treatment of affective disorders which progress is not satisfactory. It is certainly neglected and underused during the clinical practice.
ObjectivesTo evaluate the efficacy of mECT in reducing recurrence and relapse in recurrent depression within a sample of three patients.
MethodsWe followed up these patients among two years since they received the first set of electroconvulsive sessions. We applied the Beck Depression Inventory (BDI) in the succesives consultations for evaluating the progress.
ResultsThe three patients were diagnosed with Recurrent Depressive Disorder (RDD). One of them is a 60 year old man that received initially a cycle of 12 sessions; since then he received 10 maintenance sessions. Other one is a 70 year old woman that received initially a cycle of 10 sessions; since then she received 6 maintenance sessions. The last one is a 55 year old woman that received initially a cycle of 14 sessions; since then she received 20 maintenance sessions.
All of them showed a significant reduction in depressive symptoms evaluated through BDI and clinical examination. In the first case, we found a reduction in the BDI from the first consultation to the last that goes from 60 to 12 points; in the second case, from 58 to 8 points; and in the last case, from 55 to 10 points. The main sections that improved were emotional, physical and delusional.
As side-effects of the treatment, we found anterograde amnesia, lack of concentration and loss of focus at all of them.
ConclusionsWe find mECT as a very useful treatment for resistant cases of affective disorders like RDD.
It should be considered as a real therapeutic option when the first option drugs have been proved without success.
Disclosure of InterestNone Declared
UNTIL IT BURSTS OR ALL OF US BURST. A SCHIZOTYPICAL CASE.
- B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, A. Aparicio Parras, M. D. L. Á. Guillén Soto, T. Jiménez Aparicio, M. D. C. Vallecillo Adame, C. de Andrés Lobo, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Queipo de Llano de la Viuda, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S967
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal disorder is conceptualized as a stable personality pathology (Cluster A) and as a latent manifestation of schizophrenia. It can be understood as an attenuated form of psychosis or high-risk mental state, which may precede the onset of schizophrenia or represent a more stable form of psychopathology that doesn’t necessarily progress to psychosis.
ObjectivesTo exemplify the continuum of psychosis
MethodsReview of scientific literature based on a relevant clinical case.
Results39-year-old male living with his parents. He started studying philosophy. He is a regular cannabis user and has an aunt with schizophrenia. He’s admitted to psychiatry for behavioral disturbance in public. He refers to having been hearing a beeping noise in his street for months, what he interprets as a possible way of being watched due to his past ideology. Without specifying who and why, he sometimes shouts “until it bursts” to stop the noise and he thinks that his neighbours alerted the police about his behavior. During the interview he alludes to Milgram’s experiment, saying that throughout history there have been crimes against humanity and those who pointed them out were labeled “crazy”. His father refers that he has always been “strange” and with certain extravagant revolutionary ideas and thoughts. He doesn’t maintain social relationships and dedicates himself to reading and writing.
ConclusionsIt’s important to understand psychosis as a continuum to advance the understanding of etiology, pathophysiology and resilience of psychotic disorders and to develop strategies for prevention and early intervention
Disclosure of InterestNone Declared
Delirious episode secondary to rotigotine: the psychotic patch
- M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, P. Pando Fernández, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, T. Jiménez Aparicio, M. D. C. Valdecillo Adame, C. de Andrés Lobo, G. Guerra Valera, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramirez, M. D. L. Á. Guillén Soto, A. Aparicio Parras, M. Esperesate Pajares
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S626
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a fine line separating psychiatry and neurology. Most movement disorders can have psychiatric symptoms, not only those caused by the disease itself, but also those induced by the drugs used to treat them.
ObjectivesPresentation of a clinical case about a patient diagnosed with Parkinson’s disease presenting a several-month-long delirious episode due to dopaminergic drugs.
MethodsLiterature review on drug-induced psychosis episodes in Parkinson’s disease.
ResultsA 57-year-old patient with diagnosis of Parkinson’s disease for six years, who went to the emergency room accompanied by his wife due to delirious ideation. He was being treated with levodopa, carbidopa and rasagiline for years, and rotigotine patches whose dosage was being increased over the last few months.
His wife reported celotypical clinical manifestations and multiple interpretations of different circumstances occurring around her. He chased her on the street, had downloaded an app to look for a second cell phone because he believed she was cheating on him, and was obsessed with sex. He had no psychiatric background. It was decided to prescribe quetiapine.
The following day, he returned because he refused to take the medication since he thought he was going to be put to sleep or poisoned. It was decided to admit him to Psychiatry.
During the stay, rasagiline and rotigotine were suspended. Olanzapine and clozapine were introduced, with behavioral improvement and distancing from the psychotic symptoms which motivated the admission. The patient was also motorically stable. Although levodopa is best known for causing psychotic episodes, the symptons were attributed to rotigotine patches for temporally overlapping the dose increase.
ConclusionsPsychiatric symptoms are the third most frequent group of complications in Parkinson’s disease after gastrointestinal complications and abnormal movements. All medication used to control motor disorders can lead to psychosis, not only dopaminergics, but also selegiline, amantadine and anticholinergics.
Excessive stimulation of mesocortical and mesolimbic dopaminergic pathways can lead to psychosis, which is the most common psychiatric problem related to dopaminergic treatment.
In the face of a psychotic episode, antiparkinsonian drugs which are not strictly necessary for motor control should be withdrawn. If this is not sufficient, levodopa dose should be reduced, considering the side effects that may occur. When the adjustment of antiparkinsonian treatment is not effective, neuroleptics, especially quetiapine or clozapine, should be administered. In a recent study, pimavanserin, a serotonin 5-HT2 antagonist, was associated with approximately 35% lower mortality than atypical antipsychotic use during the first 180 days of treatment in community-dwelling patients.
Medication should always be tailor-made to suit each patient and we usually have to resort to lowering or withdrawing the dopaminergic medication.
Disclosure of InterestNone Declared
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
“Keeping an eye on amylase”. Side effects of antidepressants
- T. Jiménez Aparicio, G. Medina Ojeda, A. Rodríguez Campos, L. Rodríguez Andrés, C. Vallecillo Adame, C. De Andrés Lobo, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. J. Mateos Sexmero, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M. P. Pando Fernández, P. Martínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S831
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Both in consultations with the general practitioner and with the psychiatrist, antidepressants are one of the most used drugs (1). These have multiple indications, and there are different groups according to their mechanism of action. In relation to this case, we are going to talk about Venlafaxine, a dual-type antidepressant, that is, it inhibits the reuptake of serotonin and norepinephrine. One of the most common side effects is digestive discomfort, which usually resolves after a few weeks (2). However, we should not ignore these symptoms, since they can hide something more serious.
ObjectivesPresentation of a clinical case on a patient who presented an increase in pancreatic amylase after starting treatment with Venlafaxine.
MethodsBibliographic review including the latest articles in Pubmed on side effects of antidepressant treatment, and more specifically at the gastrointestinal level (in this case we will talk about pancreatitis).
ResultsWe present the case of a 49-year-old woman, who was hospitalized 2 years ago, due to a first depressive episode. During this admission, psychopharmacological treatment was started for the first time, on that occasion with a selective serotonin reuptake inhibitor (SSRI), treatment of first choice (3). The patient had no side effects at that time, but the response was very modest, so it was decided to replace that antidepressant with Venlafaxine (with dual action), up to 150mg. The depressive symptoms improved markedly, however the patient began to feel digestive discomfort (which at first did not seem to be of great importance). A general analysis was performed, in which an increase in lipase (978 U/L) and amylase (528 U/L) was detected. An echoendoscopy, an abdominal scan, and a magnetic resonance cholangiography were performed; Pancreatitis secondary to drugs was suspected (a severe condition). Luckily, no significant lesions were found in the tests, and the levels of amylase and lipase decreased when Venlafaxine treatment was withdrawn (without reaching the normal range). The patient was discharged and continued to attend consultations. In the last control, amylase had dropped to 225 U/L. His abdominal pain disappeared. Treatment with Vortioxetine (a multimodal antidepressant) was started, however the amylase levels continue to be monitored, and the patient continues to see the gastroenterologist.
ConclusionsGastrointestinal side effects are very common when taking antidepressant treatment, and in most cases they do not usually represent a serious problem.
However, it is described in the scientific literature that in some cases, acute pancreatitis secondary to some drugs, including Venlafaxine, can occur (4). In order to detect it, it is necessary to perform a blood test and sometimes also other complementary tests.
For its treatment, the fundamental thing is to withdraw the causing drug, trying to find other alternatives, and carry out a control to monitor possible complications
Disclosure of InterestNone Declared
VERTICO V: The environmentally driven evolution of the inner cold gas discs of Virgo cluster galaxies
- Adam B. Watts, Luca Cortese, Barbara Catinella, Toby Brown, Christine D. Wilson, Nikki Zabel, Ian D. Roberts, Timothy A. Davis, Mallory Thorp, Aeree Chung, Adam R.H. Stevens, Sara L. Ellison, Kristine Spekkens, Laura C. Parker, Yannick M. Bahé, Vicente Villanueva, María Jiménez-Donaire, Dhruv Bisaria, Alessandro Boselli, Alberto D. Bolatto, Bumhyun Lee
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 40 / 2023
- Published online by Cambridge University Press:
- 27 April 2023, e017
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
The quenching of cluster satellite galaxies is inextricably linked to the suppression of their cold interstellar medium (ISM) by environmental mechanisms. While the removal of neutral atomic hydrogen (H i) at large radii is well studied, how the environment impacts the remaining gas in the centres of galaxies, which are dominated by molecular gas, is less clear. Using new observations from the Virgo Environment traced in CO survey (VERTICO) and archival H i data, we study the H i and molecular gas within the optical discs of Virgo cluster galaxies on 1.2-kpc scales with spatially resolved scaling relations between stellar (
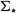 $\Sigma_{\star}$), H i (
$\Sigma_{\star}$), H i (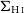 $\Sigma_{\text{H}\,{\small\text{I}}}$), and molecular gas (
$\Sigma_{\text{H}\,{\small\text{I}}}$), and molecular gas (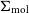 $\Sigma_{\text{mol}}$) surface densities. Adopting H i deficiency as a measure of environmental impact, we find evidence that, in addition to removing the H i at large radii, the cluster processes also lower the average
$\Sigma_{\text{mol}}$) surface densities. Adopting H i deficiency as a measure of environmental impact, we find evidence that, in addition to removing the H i at large radii, the cluster processes also lower the average 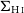 $\Sigma_{\text{H}\,{\small\text{I}}}$ of the remaining gas even in the central
$\Sigma_{\text{H}\,{\small\text{I}}}$ of the remaining gas even in the central 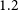 $1.2\,$kpc. The impact on molecular gas is comparatively weaker than on the H i, and we show that the lower
$1.2\,$kpc. The impact on molecular gas is comparatively weaker than on the H i, and we show that the lower 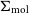 $\Sigma_{\text{mol}}$ gas is removed first. In the most H i-deficient galaxies, however, we find evidence that environmental processes reduce the typical
$\Sigma_{\text{mol}}$ gas is removed first. In the most H i-deficient galaxies, however, we find evidence that environmental processes reduce the typical 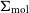 $\Sigma_{\text{mol}}$ of the remaining gas by nearly a factor of 3. We find no evidence for environment-driven elevation of
$\Sigma_{\text{mol}}$ of the remaining gas by nearly a factor of 3. We find no evidence for environment-driven elevation of 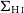 $\Sigma_{\text{H}\,{\small\text{I}}}$ or
$\Sigma_{\text{H}\,{\small\text{I}}}$ or 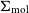 $\Sigma_{\text{mol}}$ in H i-deficient galaxies. Using the ratio of
$\Sigma_{\text{mol}}$ in H i-deficient galaxies. Using the ratio of 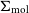 $\Sigma_{\text{mol}}$-to-
$\Sigma_{\text{mol}}$-to-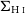 $\Sigma_{\text{H}\,{\small\text{I}}}$ in individual regions, we show that changes in the ISM physical conditions, estimated using the total gas surface density and midplane hydrostatic pressure, cannot explain the observed reduction in molecular gas content. Instead, we suggest that direct stripping of the molecular gas is required to explain our results.
$\Sigma_{\text{H}\,{\small\text{I}}}$ in individual regions, we show that changes in the ISM physical conditions, estimated using the total gas surface density and midplane hydrostatic pressure, cannot explain the observed reduction in molecular gas content. Instead, we suggest that direct stripping of the molecular gas is required to explain our results.
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Personality disorders and Juvenil Myoclonic Epilepsy
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S668
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a high comorbidity between psychiatric disorders and juvenile myoclonic epilepsy (JME), observed in up to 58% of these patients; specifically, mood disorders, anxiety and personality disorders (PD). In some patients with PD there are nonspecific alterations in the EEG, which nevertheless sometimes involve pathology. The presence of personality disorders along with JME has been repeatedly described. Previous studies have emphasized the difficulties in treating patients with JME, which have been attributed to some specific psychiatric, psychological and psychosocial characteristics.
ObjectivesDescribing distinctive personality traits in JME
MethodsReview of scientific literature based on a relevant clinical case.
Results19-year-old woman, single. Psychiatric history since she was 12 due to anxiety-depressive symptoms, after being diagnosed with JME. 4 admissions in Psychiatry, with a variety of diagnoses: eating disorder, attention deficit hyperactivity disorder and borderline personality disorder. The evolution of both disorders has been parallel, presenting epileptic seizures due to irregular therapeutic adherence together with pseudo-seizures, which made difficult their differential diagnosis. In addition, he has had frequent visits to the emergency room for suicide attempts and impulsive behaviors.
ConclusionsIn 1957, for the first time, distinctive personality traits were described in patients with JME: lack of control and perseverance, emotional instability, variable self-concept and reactive mood, which have been confirmed in subsequent studies. It is believed as epilepsy progresses, patients tend to develop symptoms of depression, anxiety, social problems, and attention deficit. Therefore, these patients have difficulty in following medical recommendations, especially precautions regarding precipitating factors for seizures.
DisclosureNo significant relationships.
Voices change my name
- C. Vallecillo Adame, T. Jiménez Aparicio, C. De Andrés Lobo, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, B. Rodríguez Rodríguez, M. Fernández Lozano, M.J. Mateos Sexmero, N. Navarro Barriga, N. De Uribe Viloria, G. Medina Ojeda, L. Rodriguez Andrés
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S801
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the clinical case of a patient where the psychotic clinic coexists with gender dysphoria. This scenario can be the result of a change in gender identity derived from the psychotic process or appear independently of it.
ObjectivesWe want to explain the importance of knowing how to act with a patient in whom these two processes coexist.
Methods20-year-old woman, with no history of mental health. She comes to the emergency department for behavioral alteration. The family observes strange behaviors, unmotivated laughter, soliloquies and aggressive episodes. Abandonment of studies, hobbies and radical physical change. Delusions of prejudice and self-referential delusions. Possible phenomena of echo and diffusion of the thought. Auditory hallucinations talking to her in male gender, since then she presents doubts about her sexual identity and manifests her desire to change sex. Altered judgment of reality.
ResultsDuring admission, we started treatment with an antipsychotic with good tolerance and she was referred to mental health team, where psychopharmacological treatment was adjusted with good response. In the following medical appointments the psychotic clinic disappeared at the same time that sexual identification was completely restored and made a critique of the behavior and experiences.
ConclusionsThis case highlights the importance of assessing the chronology of symptoms, the patient’s criticality, the response to antipsychotic treatment and the need to exclude the psychotic background of the desire for gender reassignment before making a therapeutic decision.
DisclosureNo significant relationships.
9 - Considerations for First-Generation Students in Graduate School
- from Part II - Beginning your Career
- Edited by Mitchell J. Prinstein, University of North Carolina, Chapel Hill
-
- Book:
- The Portable Mentor
- Published online:
- 21 July 2022
- Print publication:
- 04 August 2022, pp 166-178
-
- Chapter
- Export citation
-
Summary
Many graduate programs are sincerely invested in fostering diversity and increasing the number of students from underrepresented backgrounds who will contribute to our discipline.But increasing representation is only one step needed to address inequities, disparities, and injustices.Helping all students thrive, and have an equal opportunity to achieve their educational goals requires the creation of “safe spaces” in which demographic differences are understood, appreciated, and considered in larger educational systems.This chapter discusses a frequently overlooked identity characteristic that can significantly impact the graduate school experience:being a first-generation college student.
Psychopathology in adults with copy number variants
- Rachael L. Adams, Alister Baird, Jacqueline Smith, Nigel Williams, Marianne B. M. van den Bree, David E. J. Linden, Michael J. Owen, Jeremy Hall, Stefanie C. Linden
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 7 / May 2023
- Published online by Cambridge University Press:
- 11 February 2022, pp. 3142-3149
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Copy number variants (CNVs) have been associated with the risk of schizophrenia, autism and intellectual disability. However, little is known about their spectrum of psychopathology in adulthood.
MethodsWe investigated the psychiatric phenotypes of adult CNV carriers and compared probands, who were ascertained through clinical genetics services, with carriers who were not. One hundred twenty-four adult participants (age 18–76), each bearing one of 15 rare CNVs, were recruited through a variety of sources including clinical genetics services, charities for carriers of genetic variants, and online advertising. A battery of psychiatric assessments was used to determine psychopathology.
ResultsThe frequencies of psychopathology were consistently higher for the CNV group compared to general population rates. We found particularly high rates of neurodevelopmental disorders (NDDs) (48%), mood disorders (42%), anxiety disorders (47%) and personality disorders (73%) as well as high rates of psychiatric multimorbidity (median number of diagnoses: 2 in non-probands, 3 in probands). NDDs [odds ratio (OR) = 4.67, 95% confidence interval (CI) 1.32–16.51; p = 0.017) and psychotic disorders (OR = 6.8, 95% CI 1.3–36.3; p = 0.025) occurred significantly more frequently in probands (N = 45; NDD: 39[87%]; psychosis: 8[18%]) than non-probands (N = 79; NDD: 20 [25%]; psychosis: 3[4%]). Participants also had somatic diagnoses pertaining to all organ systems, particularly conotruncal cardiac malformations (in individuals with 22q11.2 deletion syndrome specifically), musculoskeletal, immunological, and endocrine diseases.
ConclusionsAdult CNV carriers had a markedly increased rate of anxiety and personality disorders not previously reported and high rates of psychiatric multimorbidity. Our findings support in-depth psychiatric and medical assessments of carriers of CNVs and the establishment of multidisciplinary clinical services.
Meltwater drainage and iceberg calving observed in high-spatiotemporal resolution at Helheim Glacier, Greenland
- Sierra M. Melton, Richard B. Alley, Sridhar Anandakrishnan, Byron R. Parizek, Michael G. Shahin, Leigh A. Stearns, Adam L. LeWinter, David C. Finnegan
-
- Journal:
- Journal of Glaciology / Volume 68 / Issue 270 / August 2022
- Published online by Cambridge University Press:
- 25 January 2022, pp. 812-828
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Marine-terminating glaciers lose mass through melting and iceberg calving, and we find that meltwater drainage systems influence calving timing at Helheim Glacier, a tidewater glacier in East Greenland. Meltwater feeds a buoyant subglacial discharge plume at the terminus of Helheim Glacier, which rises along the glacial front and surfaces through the mélange. Here, we use high-resolution satellite and time-lapse imagery to observe the surface expression of this meltwater plume and how plume timing and location compare with that of calving and supraglacial meltwater pooling from 2011 to 2019. The plume consistently appeared at the central terminus even as the glacier advanced and retreated, fed by a well-established channelized drainage system with connections to supraglacial water. All full-thickness calving episodes, both tabular and non-tabular, were separated from the surfacing plume by either time or by space. We hypothesize that variability in subglacial hydrology and basal coupling drive this inverse relationship between subglacial discharge plumes and full-thickness calving. Surfacing plumes likely indicate a low-pressure subglacial drainage system and grounded terminus, while full-thickness calving occurrence reflects a terminus at or close to flotation. Our records of plume appearance and full-thickness calving therefore represent proxies for the grounding state of Helheim Glacier through time.
Seed-shattering phenology at soybean harvest of economically important weeds in multiple regions of the United States. Part 3: Drivers of seed shatter
- Lauren M. Schwartz-Lazaro, Lovreet S. Shergill, Jeffrey A. Evans, Muthukumar V. Bagavathiannan, Shawn C. Beam, Mandy D. Bish, Jason A. Bond, Kevin W. Bradley, William S. Curran, Adam S. Davis, Wesley J. Everman, Michael L. Flessner, Steven C. Haring, Nicholas R. Jordan, Nicholas E. Korres, John L. Lindquist, Jason K. Norsworthy, Tameka L. Sanders, Larry E. Steckel, Mark J. VanGessel, Blake Young, Steven B. Mirsky
-
- Journal:
- Weed Science / Volume 70 / Issue 1 / January 2022
- Published online by Cambridge University Press:
- 15 November 2021, pp. 79-86
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Seed retention, and ultimately seed shatter, are extremely important for the efficacy of harvest weed seed control (HWSC) and are likely influenced by various agroecological and environmental factors. Field studies investigated seed-shattering phenology of 22 weed species across three soybean [Glycine max (L.) Merr.]-producing regions in the United States. We further evaluated the potential drivers of seed shatter in terms of weather conditions, growing degree days, and plant biomass. Based on the results, weather conditions had no consistent impact on weed seed shatter. However, there was a positive correlation between individual weed plant biomass and delayed weed seed–shattering rates during harvest. This work demonstrates that HWSC can potentially reduce weed seedbank inputs of plants that have escaped early-season management practices and retained seed through harvest. However, smaller individuals of plants within the same population that shatter seed before harvest pose a risk of escaping early-season management and HWSC.
The ASKAP Variables and Slow Transients (VAST) Pilot Survey
- Part of
- Tara Murphy, David L. Kaplan, Adam J. Stewart, Andrew O’Brien, Emil Lenc, Sergio Pintaldi, Joshua Pritchard, Dougal Dobie, Archibald Fox, James K. Leung, Tao An, Martin E. Bell, Jess W. Broderick, Shami Chatterjee, Shi Dai, Daniele d’Antonio, Gerry Doyle, B. M. Gaensler, George Heald, Assaf Horesh, Megan L. Jones, David McConnell, Vanessa A. Moss, Wasim Raja, Gavin Ramsay, Stuart Ryder, Elaine M. Sadler, Gregory R. Sivakoff, Yuanming Wang, Ziteng Wang, Michael S. Wheatland, Matthew Whiting, James R. Allison, C. S. Anderson, Lewis Ball, K. Bannister, D. C.-J. Bock, R. Bolton, J. D. Bunton, R. Chekkala, A. P Chippendale, F. R. Cooray, N. Gupta, D. B. Hayman, K. Jeganathan, B. Koribalski, K. Lee-Waddell, Elizabeth K. Mahony, J. Marvil, N. M. McClure-Griffiths, P. Mirtschin, A. Ng, S. Pearce, C. Phillips, M. A. Voronkov
-
- Journal:
- Publications of the Astronomical Society of Australia / Volume 38 / 2021
- Published online by Cambridge University Press:
- 12 October 2021, e054
-
- Article
-
- You have access Access
- HTML
- Export citation
-
The Variables and Slow Transients Survey (VAST) on the Australian Square Kilometre Array Pathfinder (ASKAP) is designed to detect highly variable and transient radio sources on timescales from 5 s to
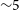 $\sim\!5$
yr. In this paper, we present the survey description, observation strategy and initial results from the VAST Phase I Pilot Survey. This pilot survey consists of
$\sim\!5$
yr. In this paper, we present the survey description, observation strategy and initial results from the VAST Phase I Pilot Survey. This pilot survey consists of 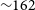 $\sim\!162$
h of observations conducted at a central frequency of 888 MHz between 2019 August and 2020 August, with a typical rms sensitivity of
$\sim\!162$
h of observations conducted at a central frequency of 888 MHz between 2019 August and 2020 August, with a typical rms sensitivity of 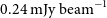 $0.24\ \mathrm{mJy\ beam}^{-1}$
and angular resolution of
$0.24\ \mathrm{mJy\ beam}^{-1}$
and angular resolution of 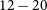 $12-20$
arcseconds. There are 113 fields, each of which was observed for 12 min integration time, with between 5 and 13 repeats, with cadences between 1 day and 8 months. The total area of the pilot survey footprint is 5 131 square degrees, covering six distinct regions of the sky. An initial search of two of these regions, totalling 1 646 square degrees, revealed 28 highly variable and/or transient sources. Seven of these are known pulsars, including the millisecond pulsar J2039–5617. Another seven are stars, four of which have no previously reported radio detection (SCR J0533–4257, LEHPM 2-783, UCAC3 89–412162 and 2MASS J22414436–6119311). Of the remaining 14 sources, two are active galactic nuclei, six are associated with galaxies and the other six have no multi-wavelength counterparts and are yet to be identified.
$12-20$
arcseconds. There are 113 fields, each of which was observed for 12 min integration time, with between 5 and 13 repeats, with cadences between 1 day and 8 months. The total area of the pilot survey footprint is 5 131 square degrees, covering six distinct regions of the sky. An initial search of two of these regions, totalling 1 646 square degrees, revealed 28 highly variable and/or transient sources. Seven of these are known pulsars, including the millisecond pulsar J2039–5617. Another seven are stars, four of which have no previously reported radio detection (SCR J0533–4257, LEHPM 2-783, UCAC3 89–412162 and 2MASS J22414436–6119311). Of the remaining 14 sources, two are active galactic nuclei, six are associated with galaxies and the other six have no multi-wavelength counterparts and are yet to be identified.