107 results
Liquor for breakfast, fighting against alcohol consumption
- N. Navarro Barriga, P. Marqués Cabezas, M. B. Arribas Simón, B. Rodríguez Rodríguez, C. Alario Ruiz, G. Guerra Valera, A. Aparicio Parras, M. J. Mateos Sexmero, M. Fernández Lozano, P. Martínez Gimeno, M. A. Andreo Vidal, M. Calvo Valcárcel, M. P. Pando Fernández, M. D. L. A. Guillén Soto, T. Jimenez Aparicio, M. D. C. Vallecillo Adame, C. De Andrés Lobo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S408-S409
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The harmful consumption of alcohol is known for how tortuous its management can be in mental health, encouraging introspection of it as a serious problem is perhaps the main key to starting to battle against its damaging influence on the development of a functional and full life.
ObjectivesTo describe a clinical case showing an unpredictible complication in an alcohol detoxification process.
Methods54-year-old man, native of Cádiz, widowed for half a decade, without children. He resides with his parents in the family home. Currently unemployed for approximately a year. He has previously worked in the IT sector. As a notable somatic history, we found long-established arterial hypertension and a total hip replacement. He has been under irregular follow-up with a mental health team for anxiety-depressive symptoms in the context of grief. He goes to the emergency service brought by his family to begin the detoxification process in the hospital setting. He acknowledges ethanol consumption since he was widowed, which began when he awakes; quantities that ranged between one or up to three bottles of distilled liquor per day, generally consumption is in the home environment. A little less than a year ago, he began to isolate himself in his room and abandon his self-care, eating increasingly insufficient food intake, refusing to receive professional care to quit the habit, mainly because he did not recognize it as disruptive.
The patient was admitted to hospital with symptoms suggestive of withdrawal, making it extremely difficult to control blood pressure levels. On the third day of admission to the acute care unit, fever peaks, blood pressure levels well below normal parameters, and compromised level of consciousness began to be evident.
ResultsBlood tests were performed that, together with the clinical picture, suggested imminent septic shock, so critical care was contacted for transfer and stabilization. A germ of probable urinary etiology sensitive to a broad spectrum of antibiotics was isolated in blood cultures, and the medication of the detoxification process was progressively optimized. Once clinical stability was achieved at all levels, an inpatient cessation resource was managed, which the patient accepted and considered suitable for his complete recovery.
ConclusionsA holistic approach to the alcoholic patient is important, since serious problems of an organic nature often arise. This is why a multidisciplinary intervention is necessary, as well as a holistic approach to care, involving both classic pharmacology and assiduous long-term psychotherapeutic intervention.
Disclosure of InterestNone Declared
Ketamine enhanced ECT in refractory recurrent depression.
- B. Arribas-Simon, P. Martinez.Gimeno, M. Calvo-Valcarcel, C. Alario-Ruiz, O. Martin-Santiago
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S225
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Recurrent Depressive Disorder is a chronic condition that significantly impacts the quality of life. Despite various treatment options, some patients face severe and treatment-resistant relapses. This case is related to research on ketamine in Electroconvulsive Therapy (ECT) for RDD. One study highlighted the efficacy and safety of ketamine compared to other anaesthetic agents in ECT for major depression. Additionally, another study explored subanesthetic doses of ketamine before each ECT session to improve therapeutic outcomes and sleep quality in patients with major depressive disorder.
ObjectivesTo present a clinical case of a patient with Recurrent Depressive Disorder (RDD) who improved following a change in the Electroconvulsive Therapy (ECT) protocol using ketamine as an anaesthetic inducer.
MethodsWe examined the patient’s medical records, including her medical history, previous treatments, and therapeutic responses.
ResultsA 65-year-old childless woman with a history of stroke, bilateral carotid atheromatosis, and hypothyroidism suffered from RDD. Despite multiple prior treatments and ECT, she experienced a severe depressive relapse. Eight intensive ECT sessions were administered, with observed memory lapses. Due to the lack of response, the anaesthetic inducer etomidate was replaced with ketamine, resulting in a positive response. The patient continued pharmacological treatment with improved mood, but recent and evident memory alterations persisted, possibly related to anterograde amnesia.
ConclusionsThis case highlights the complexity of RDD in patients with comorbidities and treatment-resistant relapses. The change in the ECT protocol using ketamine was effective, emphasizing the importance of alternative therapeutic approaches in refractory cases. The successful treatment of RDD in this patient using ketamine in ECT underscores the need for personalized therapeutic options in treatment-resistant patients. These scientific resources reinforce the relevance of exploring therapeutic alternatives in contemporary clinical practice. We need more research to understand the underlying mechanisms and how this approach could be enhanced in similar cases.
Disclosure of InterestNone Declared
Investigation of peripheral inflammatory biomarkers in association with suicide risk in major depression
- B. Petho, T. Tenyi, R. Herold, P. Osvath, V. Voros, D. Simon, C. Molnar, M. A. Kovacs
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S792-S793
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicide is the most severe consequence of major depressive disorder (MDD). The most novel researches assume the role of immunological dysregulation in the background – several studies have reported alterations of inflammatory cells related to both MDD and suicidal behaviour (SB).
ObjectivesChanges in the number of certain immune cells and their ratios have been proposed as potential biomarkers of suicide risk (SR). The aim of our research was to investigate alterations of these values related not only to MDD as an assumed inflammatory state, but also to an increased risk of SB.
MethodsIn our restrospective cohort study carried out between January 2015 and January 2020, we investigated laboratory parameters of psychiatric patients diagnosed with MDD (n=101). Individuals with recent (≤48 hours prior) suicide attempt (SA) (n=22) and with past SA (>48 hours prior) (n=19) represented the high SR group. MDD patients with no history of SA (n=60) composed the intermediate SR group. We compared the number of neutrophil granulocytes, monocytes, lymphocytes, platelets, leukocytes, neutrophil-to-lymphocyte (NLR), monocyte-to-lymphocyte (MLR), platelet-to-lymphocyte ratio (PLR), red blood cell distribution width (RDW) and erythrocyte sedimentation rate (ESR). Furthermore, we evaluated alterations of these parameters related to antidepressant (AD) treatment, which has been proved to have anti-inflammatory effects. Statistical analyses were carried out using GraphPad 9.5.0 and MedCalc 16.8 programmes.
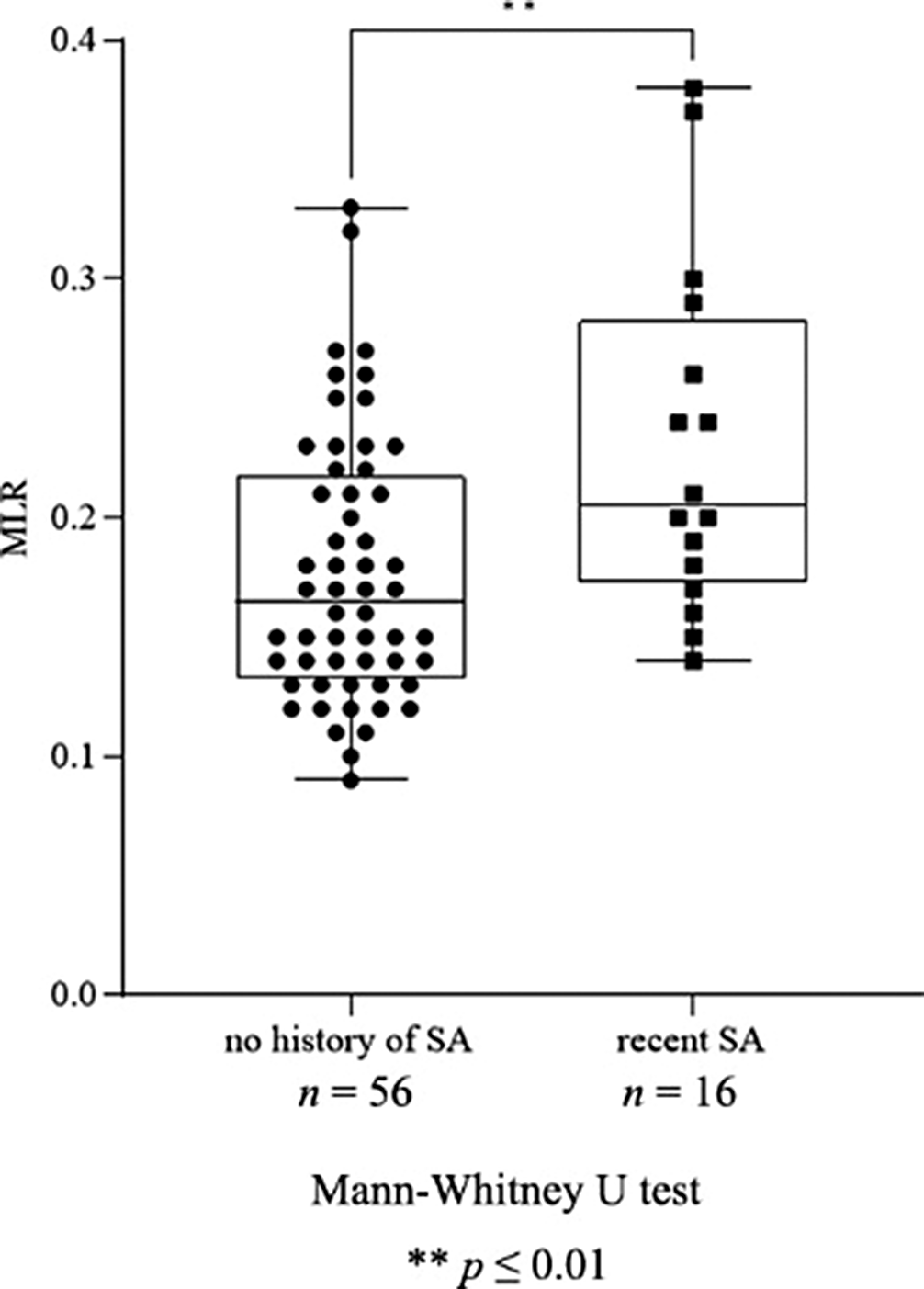
ResultsWe found a significant increase in neutrophil granulocyte count (p=0.016), NLR (p=0.031, Fig. 1), monocyte count (p≤0.0001), MLR (p=0.005, Fig. 2), leukocyte count (p=0.048) and ESR (p=0.037) in patients with recent SA compared to patients with no history of SA. Moreover, there was a significant elevation in monocyte count (p≤0.0001), MLR (p=0.020, Fig. 3), ESR (p=0.041) and RDW (p=0.037) in patients with high SR compared to patients with intermediate SR. AD treatment resulted in a significant decrease in neutrophil granulocyte count (p=0.0163) and NLR (p=0.016), however, it did not affect the rest of the parameters.
Image:
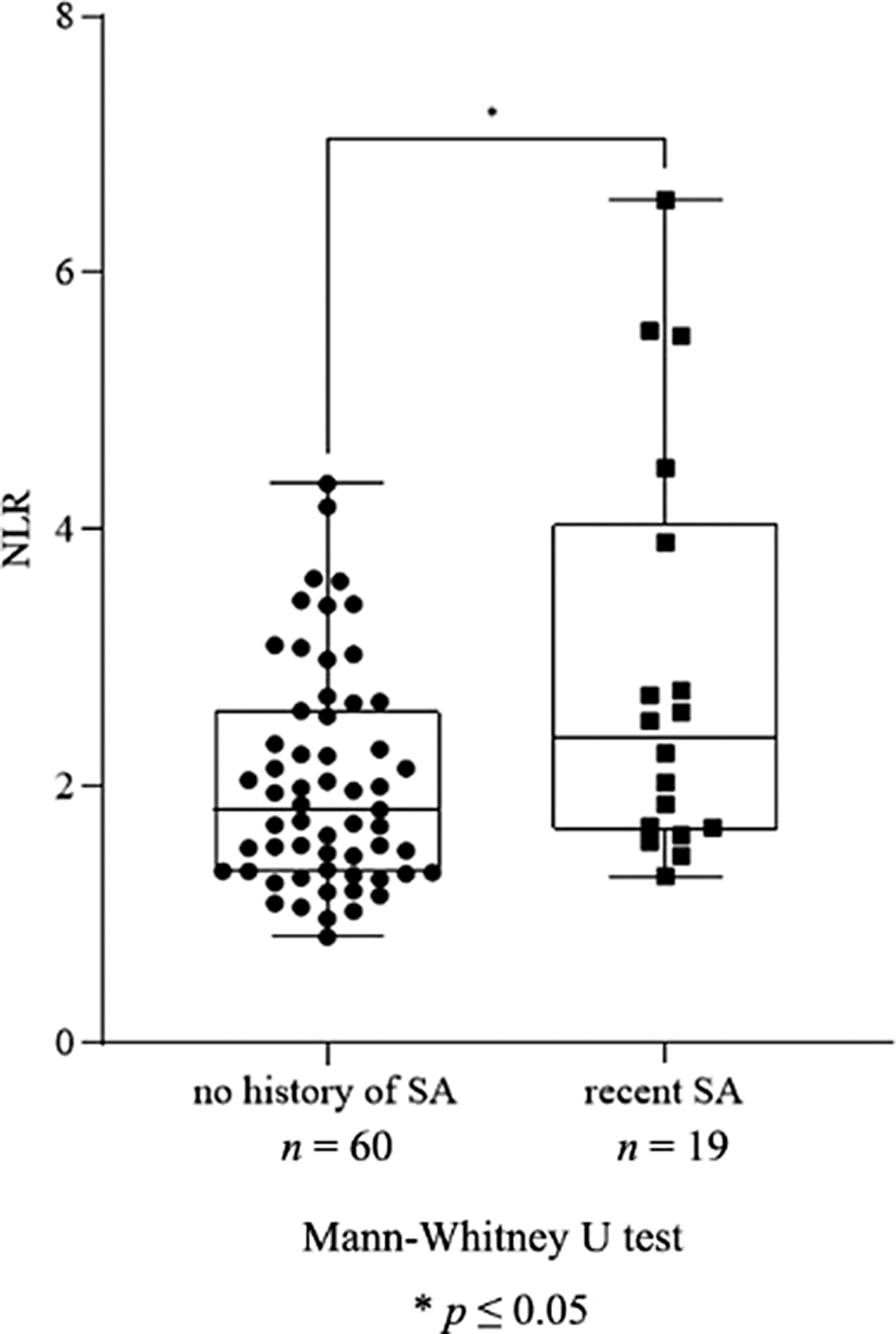
Image 2:
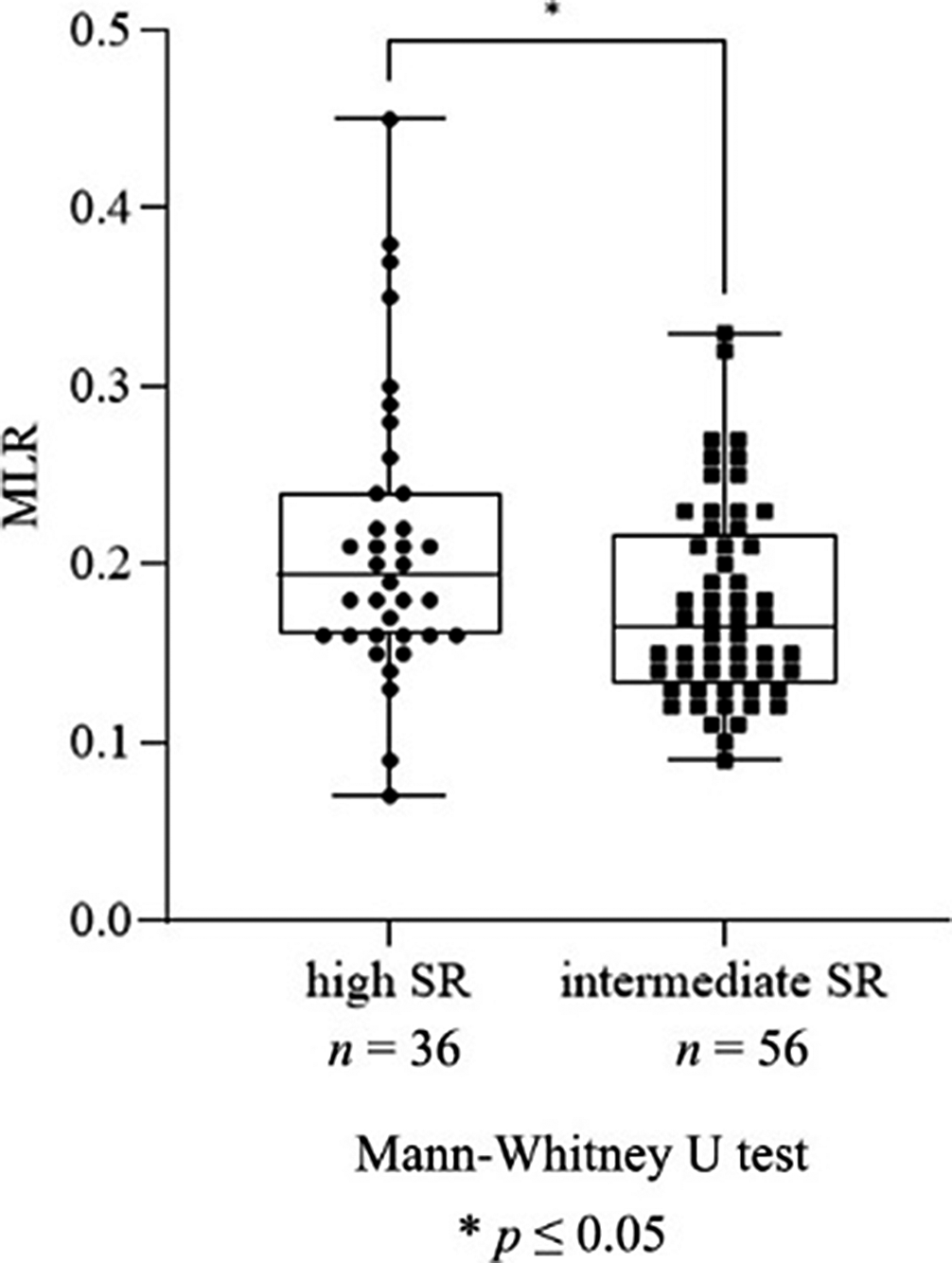
Image 3:
 Conclusions
ConclusionsAssuming immunological mechanisms in the background of MDD and SB, our findings support the role of NLR as a biomarker of acute SR, though its alterations may be masked by AD therapy in the long term. However, MLR – remaining unaffected by AD treatment – may be a possible indicator of both acute and long term suicidal vulnerability. In order to further specify the diagnostic value of these parameters, future prospective research is needed.
The study was supported by the FIKP-IV and the TNIL projects.
Disclosure of InterestNone Declared
From schizotypy to psychosis: is it a natural continuum?
- M. A. Andreo Vidal, M. B. Arribas Simón, M. Calvo Valcárcel, M. P. Pando Fernández, P. Martínez Gimeno, M. D. L. Á. Guillén Soto, B. Rodríguez Rodríguez, N. Navarro Barriga, M. Fernández Lozano, M. J. Mateos Sexmero, C. De Andrés Lobo, M. D. C. Vallecillo Adame, T. Jiménez Aparicio, Ó. Martín Santiago, A. Monllor Lazarraga, M. Ríos Vaquero, L. Rojas Vázquez, L. Sobrino Conde, A. Apario Parra, G. Lorenzo Chapatte
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S658-S659
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Schizotypal personality is a condition suffered by 4% of the population. It is defined by presenting interpersonal, behavioral and perceptual features similar to the clinical features of psychotic disorders, such as schizophrenia, in less intensity and dysfunctionality, but at risk of reaching psychosis.
ObjectivesPresentation of a clinical case about a patient with premorbid schizotypal personality traits presenting with an acute psychotic episode.
MethodsLiterature review on association between schizotypal personality and psychosis.
ResultsA 57-year-old woman with a history of adaptive disorder due to work problems 13 years ago, currently without psychopharmacological treatment, goes to the emergency room brought by the emergency services due to behavioral alteration. She reports that “her husband and son wanted to sexually abuse her”, so she had to run away from home and has been running through the streets of the town without clothes and barefoot.
Her husband relates attitude alterations and extravagant behaviors of years of evolution, such as going on diets of eating only bread for 40 days or talking about exoteric and religious subjects, as believing that the devil got inside her husband through a dental implant. He reports that these behaviors have been accentuated during the last month. She has also created a tarot website, and has even had discussions with several users. She is increasingly suspicious of him, has stopped talking to him and stays in his room all day long, with unmotivated laughter and soliloquies.
It was decided to admit him to Psychiatry and risperidone 4 mg was started. At the beginning, she was suspicious and reticent in the interview. As the days went by, communication improved, she showed a relaxed gesture and distanced herself from the delirious ideation, criticizing the episode.
ConclusionsIn recent years, there has been increasing interest in understanding the association between schizotypy and serious mental disorder. Several theories understand schizotypy as a natural continuum of personality that reveals genetic vulnerability and that can lead to psychotic disorder when added to precipitating factors. Other theories define schizotypy as a “latent schizophrenia” where symptoms are contained and expressed in less intensity.
Around 20% evolves to paranoid schizophrenia or other serious mental disorders. It is complex to distinguish between those individuals in whom schizotypy is a prodrome and those in whom it is a stable personality trait. To date, studies applying early psychotherapeutic or pharmacological interventions have had insufficient and contradictory results, and the follow-up and treatment of these individuals could be a stress factor and a stigma. Some studies are looking for reliable markers of evolution to schizophrenia in order to establish adequate protocols for detention, follow-up and treatment.
Disclosure of InterestNone Declared
Hepatic encephalopathy in cirrhosis and alcohol dependence: complex clinical challenges and multidisciplinary management
- C. Alario-Ruiz, B. Arribas-Simon, P. Martinez.Gimeno, M. Calvo-Valcarcel, O. Martin-Santiago
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S489
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Liver cirrhosis, a chronic liver disease, can be closely linked to chronic alcohol abuse, posing a significant medical challenge. Hepatic encephalopathy (HE), a neuropsychiatric condition resulting from liver dysfunction, commonly occurs in cirrhotic patients due to the accumulation of neurotoxic substances like ammonia and manganese in the body. Managing cirrhosis and alcohol addiction is crucial to enhancing the quality of life for these patients, as HE can manifest in various ways and with varying degrees of severity.
ObjectivesTo emphasize the importance of recognizing and treating hepatic encephalopathy as a potential complication of liver cirrhosis and sedatives during alcohol withdrawal.
MethodsWe compiled clinical data, medical history, neuroimaging tests, and therapeutic interventions applied.
ResultsA 55-year-old man with a complex medical history, including Child-Pugh B liver cirrhosis, portal hypertension, hypertension, diabetes mellitus, and chronic alcohol abuse with numerous prior hospitalizations for acute pancreatitis and severe head trauma related to alcohol consumption, presented to the emergency department with symptoms of alcohol withdrawal and suicidal thoughts, leading to lorazepam administration and a recommendation for admission to a specialized Therapeutic Community. After 72 hours, he developed hepatic encephalopathy with symptoms such as confusion, sleep disturbance, sweet-smelling breath, abnormal hand movements, conjunctival icterus, and urinary difficulties.
An EEG revealed a globally attenuated and disorganized bioelectrical activity with triphasic waves. The magnetic resonance imaging showed signs of hepato-cerebral degeneration, including T1-weighted hyperintensity in the lentiform and mesencephalic nuclei due to manganese deposition. Treatment was adjusted to reduce sedative use, and therapy with Rifaximin and Lactulose was initiated to control blood ammonia levels. After a week, the patient exhibited significant neurological improvement, underscoring the importance of appropriate management in patients with hepatic encephalopathy related to liver cirrhosis and chronic alcohol abuse.
ConclusionsThis case underscores the complexity of HE in patients with liver cirrhosis and alcohol dependence. HE can present in various ways, from subtle symptoms to severe episodes of confusion and coma. Findings on EEG, such as triphasic waves, are characteristic of HE and reflect brain dysfunction. Furthermore, manganese accumulation in the brain, as evidenced by magnetic resonance imaging, may contribute to neurological symptoms in cirrhotic patients. In this context, the early recognition and multidisciplinary treatment are emphasized to improve the quality of life and prevent the progression of this neuropsychiatric complication. EEG and magnetic resonance imaging findings play an essential role in the evaluation of these patients.
Disclosure of InterestNone Declared
“God speaks to me through a dove”. The evidence of clozapine in treatment-refractory psychosis
- B. Rodríguez Rodríguez, P. Marqués Cabezas, M. Queipo de Llano de La Viuda, N. Navarro Barriga, G. Guerra Valera, M. B. Arribas Simón, C. Alario Ruiz, M. J. Mateos Sexmero, M. Fernández Lozano, P. Marínez Gimeno, M. Calvo Valcárcel, M. A. Andreo Vidal, M. P. Pando Fernández, A. Monllor Lazarraga, M. Ríos Vaquero, G. Lorenzo Chapate, L. Rojas Vázquez, C. De Andrés Lobo, T. Jiménez Aparicio, M. D. C. Vallecillo Adame
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S740
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Clozapine is an atypical antipsychotic synthesised in 1958. It was withdrawn from the market in the 1970s due to the appearance of agranulocytosis, but was reintroduced due to strong evidence of its efficacy and superiority over other antipsychotics in treatment-resistant schizophrenia.
ObjectivesTo describe the adequate response to clozapine in treatment-refractory psychosis.
MethodsReview of the scientific literature based on a relevant clinical case.
ResultsA 16-year-old woman was admitted to a psychiatric inpatient unit for psychotic symptoms and behavioural disorders. She lives with her father and older sister; she has not been in contact with her mother, who lives in another country, for several years. She attends secondary school, with poor academic performance. Maternal diagnosis of schizophrenia. She started using cannabis two years ago, with a progressive increase up to 20 grams per week. He reports the onset of a feeling of strangeness a year ago, with progressive isolation in his room, referring to delirious ideation of harm towards classmates and people from his town, self-referentiality and delirious interpretations of religious mystical content (“God speaks to me through a dove”). He comments on the phenomenon of theft and thought-reading. Soliloquies and unmotivated laughter are observed.
ConclusionsTreatment was started with risperidone, progressively increasing the dose up to optimisation, without achieving a decrease in positive symptoms, but with the appearance of excessive sedation and sialorrhoea. It was combined with aripiprazole up to 20mg, maintained for a couple of weeks, without significant clinical improvement. Given the failure of two lines of therapy, it was decided to change to clozapine up to a dose of 75mg, with adequate tolerance and response, achieving a distancing of the delirious ideation. Regular haematological controls were performed, with no alterations in haemogram or troponins.
Disclosure of InterestNone Declared
Differences in the perception of stigma in schizophrenia between men and women: a brief qualitative approach
- P. Andres-Olivera, B. Arribas-Simon, E. D. Alvarez, B. Bote, C. Martin-Gomez, C. Payo, C. Munaiz, R. Brito, M. Ligero-Argudo
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S805-S806
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Men and women with psychosis have different courses and presentations of symptoms. Men with psychosis have an earlier onset of illness, more negative symptoms, and worse premorbid functioning. Women, on the other hand, have better social functioning and less substance abuse. Despite these evident differences, there are few studies that delve into these distinctions, especially from a subjective perspective.
ObjectivesThe aim of this study is to understand the differences in the perception of psychosis between men and women.
MethodsFive women and five men diagnosed with schizophrenia participated in the study. They were matched so that the age difference between them was no more than 5 years, with ages ranging from 40 to 56 years. Participants had not experienced acute decompensation of their underlying illness and had not required admission to an Acute Care Unit in the 6 months prior to inclusion in the study. Data collection was conducted through the Spanish translation of the Indiana Psychiatric Illness Interview, consisting of five parts: a narrative about their life, a narrative about the illness, questions related to how the illness has changed their life and what has not changed, the overall influence of the illness on their life, and lastly, expectations for the future.
ResultsMen expressed more concerns about work (4 men versus 2 women), while women expressed more concerns about not having become mothers (3 out of 5 women, compared to one man). All participants shared experiences of isolation in intimate relationships, including romantic relationships. Regarding stigma, three women believed that people treated them like children and dismissed their opinions. However, two of them viewed this behavior from their loved ones positively. Two women discussed the impact that psychosis and medications had on their bodies and how others had reacted to these changes
ConclusionsThe concerns and stigma associated with mental illness differ between genders. These differences should be taken into account when developing specific biopsychosocial treatment plans.
Disclosure of InterestNone Declared
Prevalence of diabetes and insulin resistance in patients with diagnosis of schizophrenia or other psicotic disorders
- P. Andres-Olivera, J. Seabra de Brito, B. Arribas-Simon, C. Martin-Gomez, B. Bote, C. Payo, C. Munaiz, R. Brito, M. Ligero-Argudo, D. Jimenez Martinez, C. Roncero
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S741
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Contrary to classical belief, people affected by this disease are at greater risk of developing organic pathologies.This risk has a very complex origin: a greater exposure to risk factors and specific socioeconomic conditions, a high prevalence of risk behaviors, the use of antipsychotics, and a potential common genetic background. (Reynolds et al.Int. J.Neuropsychopharmacol.2021; 24 854–855, Suvisaari J et al. Curr Diab Rep. 2016 16). Multiple studies demonstrate that Schizophrenia confers a high endogenous risk of Diabetes. Before patients diagnosed with Schizophrenia start taking antipsychotics (Andreassen OA et al. Am J Psychiatry. 2017;174 616-617), they have an approximately 3 times higher risk of developing Diabetes compared to the general population. The risk increases 3.6 times after the initiation of antipsychotic treatment compared to drug naive patients(Annamalai A et al World J Diabetes. 2017 390-396)
ObjectivesTo study the association between Schizophrenia or other Psychotic Disorders and Diabetes Mellitus in a sample of patients diagnosed with Schizophrenia or other Psychotic Disorders.
MethodsThis is a Descriptive and Cross-sectional Observational Study. Clinical Histories were reviewed and a personal or telephone interview was established to expand data related to the objectives of the study. The patients were recruited among the patients seen in the specific Severe Mental Disorder consultation who had a diagnosis of schizophrenia or other Psychotic Disorders, according to DSM 5-TR criteria.
ResultsFrom a sample of 93 patients, 24 had Diabetes. The Prevalence of Diabetes in patients with Schizophrenia or other Psychotic Disorders was 25.8%. Of the patients without a diagnosis of Diabetes, 15 of them had values of Glycosylated Hemoglobin (HbA1c) for Prediabetes. Using the Chi-Square Test, statistically significant differences were found between the variable Main Psychiatric Medication and Diabetes. Patients treated with Clozapine, Aripiprazole and Olanzapine had a Prevalence of Diabetes of 40.9%, 33.3% and 28.5%, respectively.
ConclusionsPrevalence of Diabetes in our sample was 3.4 times higher than the 7.51% of the general population in Spain. This presumes a significant importance and impact on the health of these patients. The diabetic patients in our sample were diagnosed with Diabetes years after the diagnosis of the mental illness, which seems to indicate that the causes have to do with lifestyle, dietary habits, weight, and exposure to chronic antipsychotics. Premature death in schizophrenia has several explanations, being of special importance the development of cardiovascular disorders and Diabetes This can be due to many reasons, but it is worth highlighting the metabolic side effects of some antipsychotics and lifestyle. In this sense, it is essential to carefully monitor this group of patients.
Disclosure of InterestNone Declared
Lithium nephropathy in Bipolar Disorder: a clinical challenge
- C. Alario-Ruiz, B. Arribas-Simon, P. Martinez.Gimeno, M. Calvo-Valcarcel, O. Martin-Santiago
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S429-S430
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lithium nephropathy can occur in long-term lithium-treated bipolar disorder patients. Key risk factors include duration of lithium exposure, cumulative dose, acute intoxication episodes, advanced age, and comorbidities such as hypertension, diabetes mellitus, hyperparathyroidism, and hyperuricemia, along with concurrent use of antipsychotics. The clinical presentation is gradual, with mild proteinuria, often accompanied by arginine vasopressin resistance. Histological studies show a correlation between interstitial fibrosis and cumulative lithium duration. Approximately 15 to 25 per cent of exposed patients may experience a gradual decline in glomerular filtration rate. The outcome after lithium discontinuation varies.
ObjectivesThis case study aims to analyze and document the clinical presentation, diagnosis, and management of lithium nephropathy in a patient with Bipolar Disorder.
MethodsWe gathered data on the medical history, lab results, and treatment approach for a patient with Bipolar Disorder.
ResultsThe patient, a 50-year-old woman, had been under the care of Psychiatry since 2008 due to a diagnosis of Bipolar Disorder Type I. During this time, she had experienced depressive and manic episodes but had not presented significant symptom decompensation for the past 14 years, successfully managed with lithium at a current dose of 600 mg per day. However, on this occasion, the patient sought hospitalization due to recent behavioural disturbances, including restlessness, disinhibition, abrupt changes in behaviour, pressured speech, sleep problems, agitation, and aggression. The patient also reported an increased sense of polyuria and polydipsia. Evaluation in the emergency department revealed elevated lithium levels of 1.47 mmol/L and hypokalemia, that justified lithium withdrawal. After lithium levels decreased, an estimated glomerular filtration rate remained low. She was diagnosed with lithium nephropathy, an adverse effect of long-term lithium therapy. Treatment with lithium changed to sodium valproate. Treatment with asenapine started and sustained for two months. Over the following two years, the patient experienced four additional hospital admissions in Psychiatry due to manic episodes.
ConclusionsLong-term lithium therapy can lead to lithium nephropathy with symptoms such as polyuria, polydipsia, and acute kidney failure. Consistent monitoring of patients receiving lithium is crucial to detect potential adverse effects.This case highlights the challenges in managing bipolar patients, as discontinuing lithium exacerbated symptoms despite switching to sodium valproate for nephropathy prevention. Long-term lithium treatment, while effective for bipolar disorder, poses significant renal risks. We emphasize continuous renal function monitoring and assessing the risk-benefit of lithium treatment while actively researching lithium nephropathy and its impact on glomerular function.
Disclosure of InterestNone Declared
Medication choice and psychosis Hospital readmissions: A two-year comparative study
- O. Martin-Santiago, M. Calvo-Valcarcel, P. Martinez.Gimeno, C. Alario-Ruiz, B. Arribas-Simon
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S288
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hospital readmissions in psychosis are a critical concern, with medication choice playing a vital role. Oral antipsychotics, though common, rely on patient adherence and can lead to relapses if not followed. Long-acting injectable atypical antipsychotics (LAIAs) provide an alternative, ensuring consistent medication release and reducing relapse risk due to missed doses. Studies indicate that LAIAs result in fewer readmissions due to improved adherence. Tailoring treatment to individual needs is essential. Medication choice significantly influences hospital readmission prevention in psychosis. LAIAs, which could offer greater adherence to treatment and symptom control, present a promising option. Individualized treatment decisions are a priority for long-term recovery.
ObjectivesThis study aimed to compare the hospital readmission rates within two years post-discharge among two groups of patients diagnosed with schizophrenia and other psychotic disorders who received either oral antipsychotic treatment or LAIAs.
MethodsWe collected sociodemographic and hospitalization data from 155 patients, 90 receiving oral antipsychotics and 65 receiving LAIAs, following their discharge from a psychiatric unit.
ResultsThere were 90 patients in the oral treatment group, and 65 in the LAIA group, with 67.6% receiving paliperidone and 26.1% receiving aripiprazole. There were no significant differences in age or gender between the two groups. However, patients in the LAIA group had longer stays in the hospital (M=14.7; SD=10.2 vs M=11.1; SD=6.4; t(153)=2.67; p<.01) and a higher number of prior admissions (M=3.2; SD=3.7 vs M=1.3; SD=3.5; t(153)=2.41; p<.01) compared to the oral antipsychotic group. Additionally, a higher percentage of patients in the LAIA group were diagnosed with schizophrenia (60%) compared to the oral antipsychotic group (24%) (X2 (1, N = 155)= 20.4, p<.01). After two years, readmission rates were 66.6% for the oral antipsychotic group and 61.5% for the LAIA group (X2 (1, N = 155)= 8.5, p > .05). However, the time to readmission was shorter for patients on oral antipsychotics (M=172.4; SD=162.0) compared to those on LAIAs (M=326.2; SD=211.4; t(153)=3.05; p<.01). Notably, 86.6% of patients on oral antipsychotics were readmitted within the first year, while only 52% of those on LAIAs experienced readmission during the same period (X2 (1, N = 155)= 8.5, p = .001).
ConclusionsLong-acting injectable antipsychotics (LAIAs) appear to reduce hospital readmissions, with a more pronounced effect in the first few months post-discharge. However, after two years, the readmission rates between LAIAs and oral antipsychotics become comparable. This data suggests that while LAIAs may reduce early readmissions, their long-term effectiveness is on par with oral antipsychotics.
Disclosure of InterestNone Declared
Male gynecomastia linked to antipsychotics: a case report
- O. Martin-Santiago, P. Martinez.Gimeno, M. Calvo-Valcarcel, C. Alario-Ruiz, B. Arribas-Simon
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S739
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Gynecomastia refers to the abnormal development of breast tissue in males, often posing a concerning symptom. Often, gynecomastia is associated with multiple factors, including the use of various drugs, notably certain atypical antipsychotics. Gynecomastia is a significant side effect that affects the quality of life of male patients taking antipsychotic medications. Among these, risperidone and paliperidone have been identified as the most prone to causing gynecomastia, although aripiprazole has garnered attention for its superior profile in controlling prolactin and gynecomastia. The relationship between these drugs and the development of gynecomastia lies in their ability to elevate prolactin levels, a hormone that regulates reproductive function and is involved in milk production. Several studies have shown that prolactin levels are more commonly elevated with risperidone and paliperidone prescription, thus triggering gynecomastia.
ObjectivesThe study aims to investigate the management of gynecomastia in male patients receiving antipsychotic medications.
MethodsThis research employs a retrospective analysis of patient records to examine the association between specific antipsychotic drugs, prolactin levels, and the development of gynecomastia, while also evaluating the effectiveness of aripiprazole as an alternative treatment.
ResultsWe present the case of a 21-year-old male with no prior medical history who initiated treatment with oral paliperidone and later switched to 100 mg of long-acting injectable paliperidone once monthly during his initial admission for psychotic symptoms. After six months, he developed gynecomastia, which was ruled out as breast tissue and was determined to be an increase in adipose tissue. Since his hospital discharge, he has gained 25 kg (30%) in body weight, and his baseline prolactin level has decreased. This weight gain, a common side effect of several antipsychotics, was linked to gynecomastia. However, a promising approach for gynecomastia antipsychotic-associated treatment is aripiprazole, which has a milder impact on prolactin levels. In this case, during the next appointment, a switch to 400 mg of long-acting injectable aripiprazole once-monthly was made, which led to weight loss, a reduction in breast size and blood prolactin levels in the following weeks.
ConclusionsThe detection and management of gynecomastia in these patients are crucial to improving their quality of life and treatment adherence. This management encompasses changes in medication, hormonal therapy, or surgery in severe cases. Physicians must be aware of this potential complication when prescribing antipsychotics and closely monitor at-risk patients. In summary, antipsychotic-associated gynecomastia in men represents a medical challenge that requires careful attention and an individualized treatment strategy for each affected patient.
Disclosure of InterestNone Declared
Trends in cannabis consumption: psychotic and anxiety symptoms among users
- O. Martin-Santiago, P. Martinez.Gimeno, M. Calvo-Valcarcel, C. Alario-Ruiz, B. Arribas-Simon
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S101
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
During cannabis use, some individuals may experience psychotic symptoms, such as unusual perceptions or irrational thoughts, including mild hallucinations or temporary paranoia. Anxiety is also common, characterized by excessive worry or intense fear. The occurrence of these symptoms varies based on cannabis quantity, individual sensitivity, and surroundings. Although not all users experience these effects, the link between cannabis and psychotic or anxiety symptoms highlights the need for a thorough risk assessment.
ObjectivesOur goal is to analyze trends in cannabis use, as well as the psychotic and anxiety symptoms experienced by users, and to examine whether cannabis use is associated with other substances consumption.
MethodsWe collected demographic and substance consumption data from two groups: 29 individuals aged 18 to 28 who had tried cannabis at least once and 19 regular consumers through a structured questionnaire.
ResultsRegular cannabis consumers had a higher proportion of males than those who had tried it once (X²(1)=4.81; p=0.028). There were no significant differences in age, alcohol or tobacco consumption between the groups. Notably, regular cannabis consumers had a history of using other illegal drugs, both in the past and within the last month (X²(1)=8.53; p=0.003). Regarding cannabis effects, regular users more frequently reported sensations like euphoria, relaxation, altered time perception, tachycardia, motor coordination difficulties, and impaired clear thinking compared to one-time users (X²(1)=10.12; p=0.001). Regarding anxiety symptoms during cannabis consumption, both groups experienced a similar frequency. Finally, regular cannabis consumers reported strange ideas or perceptions more often than one-time users (X²(1)=0.743; p=0.019). However, the associated discomfort level was similar in both groups.
ConclusionsThis study highlights that regular cannabis use is associated with a greater likelihood of using other substances and experiencing more pronounced effects, including psychotic symptoms. However, it doesn’t necessarily lead to increased anxiety symptoms compared to one-time users. It’s important to acknowledge that the relationship between cannabis and psychosis is intricate and influenced by factors like consumption quantity and individual sensitivity. These findings stress the importance of understanding cannabis’s impact on mental health and its connection to the use of other substances.
Disclosure of InterestNone Declared
Increased emergency room visits without corresponding rehospitalizations in cannabis users with psychosis
- O. Martin-Santiago, M. Calvo-Valcarcel, P. Martinez.Gimeno, C. Alario-Ruiz, B. Arribas-Simon
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S388-S389
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Epidemiological studies have established a complex relationship between cannabis consumption and a heightened risk of psychotic disorders, including schizophrenia. However, this connection is multifaceted, influenced by genetics, environment, and individual psychology. Surprisingly, despite a surge in emergency room (ER) visits associated with cannabis consumption and psychosis, there haven’t been significant increases in hospital readmissions. This rise in ER visits can be attributed to the increasing social acceptance of cannabis and its legalization in some regions, increasing the likelihood of adverse effects. Furthermore, the higher potency of contemporary cannabis can trigger psychotic reactions, particularly in those consuming elevated levels of THC, its primary psychoactive component.
ObjectivesThis study aimed to compare the rates of readmissions and ER visits one year after hospital discharge among patients diagnosed with schizophrenia and other psychotic disorders, stratified by cannabis consumption.
MethodsWe collected sociodemographic and clinical data from 109 patients after discharge from a psychiatric hospitalization unit.
ResultsPatients who consumed cannabis (N=35) were younger than non-consumers (M=31.4; SD=10.0 vs M=44.3; SD=11.4; t(107)=5.71; p<.01), with no significant gender differences, hospital stay durations, or proportions of schizophrenia diagnoses (33.3%). The readmission rates and time to readmission were similar between both groups. Interestingly, 54.2% of cannabis consumers required emergency care (X2 (1, N = 109)= 4.1, p = .04), with 73.6% not needing admission (X2 (1, N = 109)= 5.5, p = .01), in contrast to 33.7% and 56% in the non-consumer group. The time to the first urgent care visit was shorter in the consumer group (M=59.5; SD=56.3) compared to the non-consumer group (M=105.8; SD=93.1; t(107)=1.92; p=.03).
ConclusionsThis study reveals that patients with psychosis and cannabis consumption tend to visit ER services more frequently despite utilizing fewer hospital resources like hospitalizations. Notably, despite the increased ER visits, there hasn’t been a corresponding rise in hospital readmissions. These would be due to individuals experiencing cannabis-related psychotic episodes receiving suitable assessment and treatment in the ER, obviating the need for prolonged hospitalization. Furthermore, some psychotic episodes may naturally resolve over time, particularly with reduced or discontinued cannabis consumption. Our result highlights the need for personalized care approaches targeting this group, effectively addressing acute episodes related to cannabis use and psychosis. Addressing this trend requires a multidisciplinary approach involving mental health professionals, addiction specialists, and emergency response teams.
Disclosure of InterestNone Declared
Retinal microvascular function and incidence and trajectories of clinically relevant depressive symptoms: the Maastricht Study
- April C. E. van Gennip, Monideepa D. Gupta, Alfons J. H. M. Houben, Tos T. J. M. Berendschot, Carroll A. B. Webers, Marleen M. J. van Greevenbroek, Carla J. H. van der Kallen, Annemarie Koster, Anke Wesselius, Simone J. P. M. Eussen, Casper G. Schalkwijk, Bastiaan E. de Galan, Sebastian Köhler, Miranda T. Schram, Coen D. A. Stehouwer, Thomas T. van Sloten
-
- Journal:
- Psychological Medicine , First View
- Published online by Cambridge University Press:
- 12 March 2024, pp. 1-10
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Cerebral microvascular dysfunction may contribute to depression via disruption of brain structures involved in mood regulation, but evidence is limited. We investigated the association of retinal microvascular function, a proxy for microvascular function in the brain, with incidence and trajectories of clinically relevant depressive symptoms.
MethodsLongitudinal data are from The Maastricht Study of 5952 participants (59.9 ± 8.5 years/49.7% women) without clinically relevant depressive symptoms at baseline (2010–2017). Central retinal arteriolar equivalent and central retinal venular equivalent (CRAE and CRVE) and a composite score of flicker light-induced retinal arteriolar and venular dilation were assessed at baseline. We assessed incidence and trajectories of clinically relevant depressive symptoms (9-item Patient Health Questionnaire score ⩾10). Trajectories included continuously low prevalence (low, n = 5225 [87.8%]); early increasing, then chronic high prevalence (early-chronic, n = 157 [2.6%]); low, then increasing prevalence (late-increasing, n = 247 [4.2%]); and remitting prevalence (remitting, n = 323 [5.4%]).
ResultsAfter a median follow-up of 7.0 years (range 1.0–11.0), 806 (13.5%) individuals had incident clinically relevant depressive symptoms. After full adjustment, a larger CRAE and CRVE were each associated with a lower risk of clinically relevant depressive symptoms (hazard ratios [HRs] per standard deviation [s.d.]: 0.89 [95% confidence interval (CI) 0.83–0.96] and 0.93 [0.86–0.99], respectively), while a lower flicker light-induced retinal dilation was associated with a higher risk of clinically relevant depressive symptoms (HR per s.d.: 1.10 [1.01–1.20]). Compared to the low trajectory, a larger CRAE was associated with lower odds of belonging to the early-chronic trajectory (OR: 0.83 [0.69–0.99]) and a lower flicker light-induced retinal dilation was associated with higher odds of belonging to the remitting trajectory (OR: 1.23 [1.07–1.43]).
ConclusionsThese findings support the hypothesis that cerebral microvascular dysfunction contributes to the development of depressive symptoms.
Associations of an individual's need for cognition with structural brain damage and cognitive functioning/impairment: cross-sectional population-based study
- Lotte S. Truin, Sebastian Köhler, Irene S. Heger, Martin P. J. van Boxtel, Miranda T. Schram, Walter H. Backes, Jacobus F. A. Jansen, Martien M. C. J. M. van Dongen, Nanne K. de Vries, Hein de Vries, Simone J. P. M. Eussen, Coen D. A. Stehouwer, Marjolein E. de Vugt, Kay Deckers
-
- Journal:
- The British Journal of Psychiatry / Volume 224 / Issue 6 / June 2024
- Published online by Cambridge University Press:
- 18 December 2023, pp. 189-197
- Print publication:
- June 2024
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
High cognitive activity possibly reduces the risk of cognitive decline and dementia.
AimsTo investigate associations between an individual's need to engage in cognitively stimulating activities (need for cognition, NFC) and structural brain damage and cognitive functioning in the Dutch general population with and without existing cognitive impairment.
MethodCross-sectional data were used from the population-based cohort of the Maastricht Study. NFC was measured using the Need For Cognition Scale. Cognitive functioning was tested in three domains: verbal memory, information processing speed, and executive functioning and attention. Values 1.5 s.d. below the mean were defined as cognitive impairment. Standardised volumes of white matter hyperintensities (WMH), cerebrospinal fluid (CSF) and presence of cerebral small vessel disease (CSVD) were derived from 3T magnetic resonance imaging. Multiple linear and binary logistic regression analyses were used adjusted for demographic, somatic and lifestyle factors.
ResultsParticipants (n = 4209; mean age 59.06 years, s.d. = 8.58; 50.1% women) with higher NFC scores had higher overall cognition scores (B = 0.21, 95% CI 0.17–0.26, P < 0.001) and lower odds for CSVD (OR = 0.74, 95% CI 0.60–0.91, P = 0.005) and cognitive impairment (OR = 0.60, 95% CI 0.48–0.76, P < 0.001) after adjustment for demographic, somatic and lifestyle factors. The association between NFC score and cognitive functioning was similar for individuals with and without prevalent cognitive impairment. We found no significant association between NFC and WMH or CSF volumes.
ConclusionsA high need to engage in cognitively stimulating activities is associated with better cognitive functioning and less presence of CSVD and cognitive impairment. This suggests that, in middle-aged individuals, motivation to engage in cognitively stimulating activities may be an opportunity to improve brain health.
A Good Investment: Expanding Capacity to Care for Older Adults in the Home and Community Care Sector Through Increased Personal Support Worker Wages
- Katherine A. P. Zagrodney, Emily C. King, Deborah Simon, Kathryn A. Nichol, Sandra M. McKay
-
- Journal:
- Canadian Journal on Aging / La Revue canadienne du vieillissement / Volume 43 / Issue 2 / June 2024
- Published online by Cambridge University Press:
- 18 September 2023, pp. 197-202
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Most older adults prefer to age in place, which for many will require home and community care (HCC) support. Unfortunately, HCC capacity is insufficient to meet demand due in part to low wages, particularly for personal support workers (PSWs) who provide the majority of paid care. Using Ontario as a case study, this paper estimates the cost and capacity impacts of implementing wage parity between PSWs employed in HCC and institutional long-term care (ILTC). Specifically, we consider the cost of increased HCC PSW wages versus expected savings from avoiding unnecessary ILTC placement for those accommodated by HCC capacity growth. The expected increase in HCC PSW retention would create HCC capacity for approximately 160,000 people, reduce annual health system costs by approximately $7 billion, and provide an 88 per cent return on investment. Updating wage structures to reduce turnover and enable HCC capacity growth is a cost-efficient option for expanding health system capacity.
A scoping review of factors associated with antimicrobial-resistant Campylobacter species infections in humans
- Christine M. Neustaedter, Kelsey Robertson, Dana Tschritter, Richard J. Reid-Smith, Melissa C. MacKinnon, Colleen P. Murphy, Brennan Chapman, Norman F. Neumann, Simon J. G. Otto
-
- Journal:
- Epidemiology & Infection / Volume 151 / 2023
- Published online by Cambridge University Press:
- 07 June 2023, e100
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Human infection with antimicrobial-resistant Campylobacter species is an important public health concern due to the potentially increased severity of illness and risk of death. Our objective was to synthesise the knowledge of factors associated with human infections with antimicrobial-resistant strains of Campylobacter. This scoping review followed systematic methods, including a protocol developed a priori. Comprehensive literature searches were developed in consultation with a research librarian and performed in five primary and three grey literature databases. Criteria for inclusion were analytical and English-language publications investigating human infections with an antimicrobial-resistant (macrolides, tetracyclines, fluoroquinolones, and/or quinolones) Campylobacter that reported factors potentially linked with the infection. The primary and secondary screening were completed by two independent reviewers using Distiller SR®. The search identified 8,527 unique articles and included 27 articles in the review. Factors were broadly categorised into animal contact, prior antimicrobial use, participant characteristics, food consumption and handling, travel, underlying health conditions, and water consumption/exposure. Important factors linked to an increased risk of infection with a fluoroquinolone-resistant strain included foreign travel and prior antimicrobial use. Identifying consistent risk factors was challenging due to the heterogeneity of results, inconsistent analysis, and the lack of data in low- and middle-income countries, highlighting the need for future research.
The combination of olfactory dysfunction and depression increases the risk of incident dementia in older adults
- Shafi Kalam, Katya Numbers, Darren M. Lipnicki, Ben C. P. Lam, Henry Brodaty, Simone Reppermund
-
- Journal:
- International Psychogeriatrics / Volume 36 / Issue 2 / February 2024
- Published online by Cambridge University Press:
- 02 June 2023, pp. 130-141
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Objectives:
Olfactory dysfunction and depression are common in later life, and both have been presented as risk factors for dementia. Our purpose was to investigate the associations between these two risk factors and determine if they had an additive effect on dementia risk.
Design:Olfactory function was assessed using the Brief Smell Identification Test (BSIT), and depression was classified using a combination of the 15-item Geriatric Depression Scale (GDS) score and current antidepressant use. Cross-sectional associations between depression and olfactory function were examined using correlations. Cox regression analyses were conducted to examine the longitudinal relationship between olfaction and depression and incident dementia across 12-years of follow-up.
Participants:Participants were 780 older adults (aged 70–90 years; 56.5% female) from the Sydney Memory and Ageing Study (MAS) without a diagnosis of dementia at baseline.
Results:Partial correlation revealed a nonsignificant association between baseline depression and olfactory function after accounting for covariates (r = −.051, p = .173). Cox regression showed that depression at baseline (hazard ratio = 1.706, 95% CI 1.185–2.456, p = .004) and lower BSIT scores (HR = .845, 95%CI .789–.905, p < .001) were independently associated with a higher risk of incident dementia across 12 years. Entering both predictors together improved the overall predictive power of the model.
Conclusions:Lower olfactory identification scores and depressive symptoms predict incident dementia over 12 years. The use of BSIT scores and depression in conjunction provides a greater ability to predict dementia than either used alone. Assessment of olfactory function and depression screening may provide clinical utility in the early detection of dementia.
Magnitude of terminological bias in international health services research: a disambiguation analysis in mental health
- M. R. Gutierrez-Colosia, P. Hinck, J. Simon, A. Konnopka, C. Fischer, S. Mayer, V. Brodszky, L. Hakkart-van Roijen, S. Evers, A. Park, H. H König, W. Hollingworth, J. A Salinas-Perez, the PECUNIA Group, L. Salvador-Carulla
-
- Journal:
- Epidemiology and Psychiatric Sciences / Volume 31 / 2022
- Published online by Cambridge University Press:
- 22 August 2022, e59
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Aims
Health services research (HSR) is affected by a widespread problem related to service terminology including non-commensurability (using different units of analysis for comparisons) and terminological unclarity due to ambiguity and vagueness of terms. The aim of this study was to identify the magnitude of the terminological bias in health and social services research and health economics by applying an international classification system.
MethodsThis study, that was part of the PECUNIA project, followed an ontoterminology approach (disambiguation of technical and scientific terms using a taxonomy and a glossary of terms). A listing of 56 types of health and social services relevant for mental health was compiled from a systematic review of the literature and feedback provided by 29 experts in six European countries. The disambiguation of terms was performed using an ontology-based classification of services (Description and Evaluation of Services and DirectoriEs – DESDE), and its glossary of terms. The analysis focused on the commensurability and the clarity of definitions according to the reference classification system. Interrater reliability was analysed using κ.
ResultsThe disambiguation revealed that only 13 terms (23%) of the 56 services selected were accurate. Six terms (11%) were confusing as they did not correspond to services as defined in the reference classification system (non-commensurability bias), 27 (48%) did not include a clear definition of the target population for which the service was intended, and the definition of types of services was unclear in 59% of the terms: 15 were ambiguous and 11 vague. The κ analyses were significant for agreements in unit of analysis and assignment of DESDE codes and very high in definition of target population.
ConclusionsService terminology is a source of systematic bias in health service research, and certainly in mental healthcare. The magnitude of the problem is substantial. This finding has major implications for the international comparability of resource use in health economics, quality and equality research. The approach presented in this paper contributes to minimise differentiation between services by taking into account key features such as target population, care setting, main activities and type and number of professionals among others. This approach also contributes to support financial incentives for effective health promotion and disease prevention. A detailed analysis of services in terms of cost measurement for economic evaluations reveals the necessity and usefulness of defining services using a coding system and taxonomical criteria rather than by ‘text-based descriptions’.
Hyperemesis gravidarum severity, enteral tube feeding and cardiometabolic markers in offspring cord blood
- Kelly Nijsten, Marjette H. Koot, Joke M. J. Bais, Carrie Ris-Stalpers, Rik van Eekelen, Henk A. Bremer, David P. van der Ham, Wieteke M. Heidema, Anjoke Huisjes, Gunilla Kleiverda, Hinke Kruizenga, Simone M. Kuppens, Judith O. E. H. van Laar, Josje Langenveld, Flip van der Made, Dimitri Papatsonis, Marie-José Pelinck, Paula J. Pernet, Leonie van Rheenen-Flach, Robbert J. Rijnders, Hubertina C. J. Scheepers, Tatjana Vogelvang, Ben W. Mol, Iris J. Grooten, Tessa J. Roseboom, Rebecca C. Painter
-
- Journal:
- British Journal of Nutrition / Volume 128 / Issue 12 / 28 December 2022
- Published online by Cambridge University Press:
- 24 February 2022, pp. 2421-2431
- Print publication:
- 28 December 2022
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
This study aimed to investigate the association between hyperemesis gravidarum (HG) severity and early enteral tube feeding on cardiometabolic markers in offspring cord blood. We included women admitted for HG, who participated in the MOTHER randomised controlled trial (RCT) and observational cohort. The MOTHER RCT showed that early enteral tube feeding in addition to standard care did not affect symptoms/birth outcomes. Among RCT and cohort participants, we assessed how HG severity affected lipid, c-peptide, glucose and free thyroxine cord blood levels. HG severity measures were severity of vomiting at inclusion and 3 weeks after inclusion, pregnancy weight gain and 24-h energy intake at inclusion, readmissions and duration of hospital admissions. Cord blood measures were also compared between RCT participants allocated to enteral tube feeding and those receiving standard care. Between 2013-2016, 215 women were included: 115 RCT and 100 cohort participants. Eighty-one cord blood samples were available. Univariable not multivariable regression analysis showed that lower maternal weight gain was associated with higher cord blood glucose levels (β: –0·08, 95% CI –0·16, –0·00). Lower maternal weight gain was associated with higher Apo-B cord blood levels in multivariable regression analysis (β: –0·01, 95% CI –0·02, –0·01). No associations were found between other HG severity measures or allocation to enteral tube feeding and cord blood cardiometabolic markers. In conclusion, while lower maternal weight gain was associated with higher Apo-B cord blood levels, no other HG severity measures were linked with cord blood cardiometabolic markers, nor were these markers affected by enteral tube feeding.




