The degree to which an individual follows medical advice is a major concern in every medical specialty (Reference Osterberg and BlaschkeOsterberg & Blaschke, 2005). Much attention has focused on methods to persuade patients to adhere to recommendations, without sufficient acknowledgement that avoidance of sometimes complex, costly and unpleasant regimens may be entirely rational (Reference MitchellMitchell, 2007a ). Equally overlooked is the influence of communication between patients and healthcare professionals. Put simply, if no clear agreement is formed with the patient at the onset of treatment then it should be of no surprise if concordance turns out to be less than ideal. In one study the chance of premature discontinuation was found to be less than half in patients who recalled being told to take the medication for at least 6 months compared with those not given this information (Reference Bull, Hunkeler and LeeBull et al, 2002b ). This task is made more difficult when patients lack insight into their condition (see below).
Given the necessity of therapeutic agreement, the term compliance has given way to adherence and concordance (Box 1) (Reference Haynes, McDonald and GargHaynes et al, 2002). In considering the nosology of concordance and adherence a useful distinction is between individuals who do not start a medication (similarly those who do not attend their first appointment) and those who start the course but either take medication incompletely (partial compliance or adherence) or discontinue prematurely against medical advice (Fig. 1). There has been little research on reluctance to start medication which equates to treatment refusal or overt non-adherence. Reference Kasper, Hoge and Feucht-HaviarKasper et al(1997) found in a group of 348 newly admitted psychiatric in-patients that 12.9% refused treatment but that 90% of these ended their refusal within 4 days. Synthesising data on adherence behaviour is difficult because of the wide range of assessment methods (for review see Reference Velligan, Lam and GlahnVelligan et al, 2006). Few studies have examined what advice patients actually receive and thus it is often impossible to test whether patient behaviour is truly at odds with what was agreed.

Fig. 1 Nosology of adherence behaviour.
Box 1 Working definitions about health behaviour
Adherence (compliance) is the extent to which an individual changes their health behaviour to coincide with medical advice
Concordance is the degree to which clinical advice and health behaviour agrees
Therapeutic alliance is an agreement between patients and health professionals to work together
Therapeutic disagreement is a divergence in the views of patients and doctors on the subject of treatment
It is useful to remember than many predictors are generic and applicable to all patients (Box 2). Three important predictors are complexity of the regimen, duration of the course and frequency of follow-up contact. Regular contact reduces rates of both missed medication and missed appointments (Reference Rittmannsberger, Pachinger and KeppelmullerRittmannsberger et al, 2004; this will be discussed further in Reference Mitchell and SelmesMitchell & Selmes, 2007). The complexity of a treatment regimen (number of tablets, number of medications and drug interval) adversely affects adherence. Equally, regimens that require disruption to lifestyle, or special techniques or arrangements are less welcome by patients. A systematic review found that the number of doses prescribed per day was inversely related to adherence (Reference Claxton, Cramer and PierceClaxton et al, 2001). In elderly patients acceptable adherence is common in those taking only one medicine but rapidly falls in those taking four or more. Regarding the length of the prescribed course of treatment, most imagine it is relatively simple to follow a 5-day antibiotic course but in reality only two-thirds manage to do so successfully. Ask patients to follow a 7-day course, with antibiotics four times a day, and ideal concordance is achieved by less than 40%. In psychiatry, we expect patients to agree to much longer courses of medication (occasionally for an indefinite period if risks are judged sufficiently high) (Reference MitchellMitchell, 2006a ).
Box 2 Predictors of treatment concordance problems
General
-
• Duration and complexity of regimen
-
• Lack of informal support
Patient (intentional)
-
• Concerns about the side-effects
-
• Few perceived benefits
-
• Stigma of taking medication
-
• Adjustment to suit daily routine
-
• Concerns about cost
-
• Concerns about availability
-
• Concerns about dependency
Patient (non-intentional)
-
• Slips and lapses
-
• External distractors
-
• Misunderstanding instructions
Clinician
-
• Poor doctor–patient relationship
-
• Poor empathy
-
• Poor explanation/communication
-
• Inadequate follow-up
Illness
-
• Severe illness
-
• Depression or distress
-
• Psychosis
-
• Cognitive impairment
In this review, we will examine the predictors of both partial adherence and discontinuation in those taking psychotropic medication, in an attempt to understand why some patients have difficulty following the advice of mental health professionals and why adherence rates appear to be lower than in other specialties (see also Reference Cramer and RosenheckCramer & Rosenheck, 1998).
Costs of less-than-ideal adherence
There is considerable evidence that premature medication discontinuation is costly (Reference Sullivan, Wells and MorgensternSullivan et al, 1995). Undisclosed (covert) non-adherence appears to be particularly hazardous (Task Force for Compliance, 1994). Reference Kang, Kim and KimKang et al(2005) examined antipsychotic adherence of individuals prior to admission to hospital with schizophrenia: 37.1% had been totally non-adherent during the 6 months prior to admission. Although the majority had missed medication on fewer than 20% of days, many relapsed anyway. Reduced adherence weakens treatment benefits, especially when no alternatives are explored (Reference Irvine, Baker and SmithIrvine et al, 1999).
Fewer studies in psychiatry have looked at the complications of partial concordance. Three of the most influential of these have been conducted in the USA. In a sample of 7864 Medicaid patients taking atypical antipsychotics, those who achieved less than 80% of ideal concordance were about 50% more likely than fully concordant patients to have been hospitalised (Reference Eaddy, Grogg and LocklearEaddy et al, 2005). Jeste's group (Reference Gilmer, Dolder and LacroGilmer et al, 2004) found a hierarchy of risk of admission, from those who were non-adherent, those who took medication to excess and finally those who were partially adherent. In the largest study, Reference Valenstein, Copeland and BlowValenstein et al(2002) showed that those with less than 80% concordance were 2.4 times more likely to be admitted than patients with good concordance.
General predictors of missed medication
A number of authors have reviewed factors predicting non-adherence, but only a handful have considered predictors in psychiatric populations (Reference Fenton, Blyler and HeinssenFenton et al, 1997). Predictors may be usefully divided into patient factors, clinician factors and illness factors (Box 2).
Patient factors
Intentional non-adherence
Distinguishing intentional non-adherence (missing or altering doses to suit one's needs) from unintentional non-adherence (e.g. forgetting to take medication) is a relatively recent development. In fact, in long-term studies understandable reasons for discontinuation are more common than irrational reasons. Intentional non-adherence is predicted by the balance of an individual's reasons for and against taking medication, as suggested by utility theory. Intentional non-adherence is a common reason not to start a course of medication, but it may be less common than accidental non-adherence in relation to missing individual doses (Reference Lowry, Dudley and OddoneLowry et al, 2005). Predictors of intentional non-adherence include less severe disease (and feeling well), the desire to manage independently of the medical profession (self-efficacy), disagreement with or low trust in clinicians, and receipt of low levels of medical information (Reference Piette, Heisler and KreinPiette et al, 2005).
Specific adverse effects
Weight gain due to medication has been linked with non-adherence and subjective distress (Reference Fakhoury, Wright and WallaceFakhoury et al, 2001). Obese individuals are more than twice as likely as those with a normal body mass index to miss their medication (Reference Weiden, Mackell and McDonnellWeiden et al, 2004a ). Reference FakhouryFakhoury (1999) found that more than 70% of patients described weight gain due to antipsychotics as extremely distressing, which was higher than that for any other side-effect.
Sexual dysfunction is a significant source of distress and may be linked to poor adherence. Reference Olfson, Uttaro and CarsonOlfson et al(2005) studied sexual dysfunction in 139 out-patients with DSM–IV schizophrenia who were receiving an antipsychotic but no other medications associated with sexual side-effects. Sexual dysfunction occurred in 45.3% of the group and was associated with significantly lower ratings on global quality of life. Reference Rosenberg, Bleiberg and KoscisRosenberg et al(2003) examined the effects of sexual side-effects on adherence. They found that 62.5% of men and 38.5% of women felt that their psychiatric medications were causing sexual side-effects; 41.7% of men and 15.4% of women admitted that they had stopped their medications at some point during treatment because of sexual side-effects. Importantly, 50% of the sample ‘never or infrequently’ spoke about sexual functioning with their primary mental healthcare providers, and 80% of the women with sexual side-effects had not discussed sexual dysfunction with their mental healthcare providers.
Illness beliefs and knowledge of medication
Concepts of health and disease are important factors in adherence in mental health (Reference Kelly, Maimon and ScottKelly et al, 1987). Patients’ understanding of their condition and its need for treatment is positively related to adherence, and in turn adherence, satisfaction and understanding are all related to the amount and type of information given. Studies have shown that patients who understand the purpose of the prescription are twice as likely to collect it than those who do not understand (Reference Daltroy, Katz and MorlinoDaltroy et al, 1991). Awareness of treatment accounted for 20% and 34% of variation in subjective responses (satisfaction with medication and tolerability) to atypical and typical antipsychotic drugs in one recent report (Reference Ritsner, Perelroyzen and IlanRitsner et al, 2004).
It is often assumed that patients understand a reasonable amount about their illness, but how often is this assumption tested? In a classic report, Reference Joyce, Caple and MasonJoyce et al(1969) demonstrated that patients were unable to recall half of the information given to them by their physician. Two-thirds of individuals recently discharged from hospital did not know what time to take medication and less than 15% recalled the common side-effects (Reference Makaryus and FriedmanMakaryus & Friedman, 2005).
Preliminary work suggests that figures in psychiatry are comparable. Only 1 in 10 of those taking clozapine are aware of potential haematological risks (Reference Angermeyer, Loffler and MullerAngermeyer et al, 2001). Of those prescribed antipsychotics most do not feel involved in treatment decisions and state that they take medication only because they are told to (Reference Gray, Rofail and AllenGray et al, 2005). Patients typically leave the clinic with a poor understanding of the rationale for therapy (Reference Weiden, Mackell and McDonnellWeiden et al, 2004a ). In one study, two-thirds of psychiatric in-patients did not understand why they were taking medication, and the vast majority could not be said to have given informed consent to their treatment (Reference Brown, Billcliff and McCabeBrown et al, 2001). This finding was consistent in both detained and informal in-patients. Similarly, many patients misunderstand prescription instructions. Reference Col, Fanale and KronholmCol et al(1990) found that 50% of patients with depression believed they did not need their antidepressants when they began to feel better or that the medication could be taken as required. The UK public campaign Defeat Depression revealed that many people were wary of taking antidepressants because they believed that individuals with depression should ‘pull themselves together’ and more than three-quarters believed that the medications are addictive (Reference Paykel, Hart and PriestPaykel et al, 1998). In a small sample with mood disorder or schizophrenia, Reference Adams and ScottAdams & Scott (2000) found that two components of the health beliefs model (perceived severity and perceived benefits) and two modifying factors (dysfunctional attitudes and locus of control beliefs regarding health) differentiated significantly between highly adherent and poorly adherent individuals. Although little work has examined how illness beliefs (good and bad) are formed, previous bad experiences are an important predictor of future non-attendance and non-adherence (Reference Gonzalez, Williams and NoelGonzalez et al, 2005).
Clinician factors
The doctor–patient relationship
The importance of good communication between patient and health professional is increasingly acknowledged in relation to adherence (Reference Stevenson, Cox and BrittenStevenson et al, 2004). At its essence this means forging a joint therapeutic agreement with full patient involvement. This is a two-way process in which willingness to discuss mental health issues with a doctor is predicted largely by the perceived helpfulness of and trust in that doctor (Reference Wrigley, Jackson and JuddWrigley et al, 2005). This can be quantified using a tool that measures therapeutic alliance perceived by patient or clinician.
In practice, the process of making a joint therapeutic plan is often abbreviated. Doctors tend to overestimate the amount of information they have given to patients (Reference Makoul, Arntson and SchofieldMakoul et al, 1995). At the same time, patients often misunderstand medical words. According to one study (Reference Thompson and PledgerThompson & Pledger, 1993), 22% of patients have difficulty with the word ‘symptom’, 38% with the word ‘orally’ and 76% with the word ‘stroke’.
Patients who are very unwell or without insight are unlikely to tolerate an extensive dialogue about possibilities. Yet collaborative decision-making has been shown to be a consistent predictor of health outcomes. Reference Kaplan, Greenfield and GandekKaplan et al(1996) examined participatory decision-making style on a three-item scale. Higher scores for clinicians’ participatory styles were associated with greater patient satisfaction and less likelihood of changing doctor. Reference Bultman and SvarstadBultman & Svarstad (2000) conducted an impressive study on reasons for missed antidepressants. They found that 25% of clients were not satisfied with their medication and 82% reported missing doses or stopping treatment earlier than recommended. Path analysis showed that patients with more positive beliefs about the treatment are more likely to attend for follow-up and are more satisfied with treatment after attempting medication use. Physicians’ communication style during follow-up and client satisfaction were both predictive of better medication adherence. A collaborative communication style by the clinician enhanced client knowledge of the medication, improved satisfaction with medication and improved reliability of medication use.
Predictors of missed medication in specific psychiatric disorders
Depression and antidepressants
The adherence habits of those prescribed anti-depressants have recently been summarised elsewhere (Reference MitchellMitchell, 2006b ). Roughly 10% of patients prescribed antidepressants fail to pick up their first prescription and about a third collect only the initial (typically 4-week) prescription. Of those who start medication, non-adherence rates increase with time (Reference Bultman and SvarstadBultman & Svarstad, 2002). In a study of 200 patients attending 14 family doctors in five different practices, non-adherence rates were 16% at week one, 41% at week two, 59% at week three and 68% at week four (Reference JohnsonJohnson, 1981). In those on long-term maintenance treatment, discontinuation rates for selective serotonin reuptake inhibitors (SSRIs) are above 70% (Reference Mullins, Shaya and MengMullins et al, 2005). Of all those who discontinue medication, 60% have not informed their doctor by 3 months and a quarter have not done so by 6 months (Reference Maddox, Levi and ThompsonMaddox et al, 1994; Reference Demyttenaere, Enzlin and DeweDemyttenaere et al, 2001). This is sometimes referred to as covert non-adherence.
Predictors of missed antidepressant medication
Reference Sirey, Bruce and AlexopoulosSirey et al(2001) found that perceptions of stigma about depression at the start of treatment predicted subsequent medication adherence. Reference Aikens, Nease and NauAikens et al(2005) asked 81 primary care patients given maintenance antidepressant medications about their adherence. Variation in adherence could be primarily explained by the balance between patients’ perceptions of need v. perceptions of harm, with adherence being lowest when the perceived harm of the antidepressant exceeded the perceived need. Two consistent predictors of stopping medication are feeling better and adverse effects. About 35% of patients stop after feeling better at 3 months (Reference Maddox, Levi and ThompsonMaddox et al, 1994) and 55% stop after feeling better at 6 months (Reference Demyttenaere, Enzlin and DeweDemyttenaere et al, 2001). Reference Ayalon, Arean and AlvidrezAyalon et al(2005) examined both intentional and non-intentional discontinuation of antidepressants. After controlling for ethnicity and medication type, intentional non-adherence was associated with concerns about the side-effects of the medication and the stigma associated with taking antidepressants. Unintentional non-adherence was associated with greater cognitive impairment. In a study of adherence to SSRIs, Bull et al (2002a) found predictors of discontinuation to be length of treatment, low-dose prescription and the occurrence of one or more moderately or extremely bothersome adverse effect. If the adverse effect had been discussed in advance then the likelihood of discontinuation was halved. This is consistent with the finding that individuals with depression generally want more information about their condition than they are offered and want to be involved in decision-making (Reference Garfield, Francis and SmithGarfield et al, 2004). In depression, as in other areas, the more information that is given the better is adherence (Reference Maidment, Livingston and KatonaMaidment et al, 2002).
Mania and mood stabilisers
Studies appear to support the observation that one-quarter to one-third of patients maintained on lithium are poorly adherent (Reference CochranCochran, 1986). About a third of those prescribed lithium report that their adherence behaviour is poor and in a similar number sub-optimal serum levels indicate poor adherence (Reference Scott and PopeScott & Pope, 2002). Reference Johnson and McFarlandJohnson & McFarland (1996) performed a 6-year longitudinal cohort study to determine patterns of lithium use in a large US ‘health maintenance organisation’. Lithium users took the drug on an average of 34% of the days. As in other areas, more patients are partially adherent than entirely non-adherent (Reference Colom, Vieta and Martinez-AranColom et al, 2000).
In contrast to the above results, Reference MacLeod and SharpMacLeod & Sharp (2001) found much higher rates of adherence, but all of their sample were attending a lithium maintenance clinic, which may have influenced this finding.
Predictors of missed mood stabiliser medication
In the handful of studies that have examined adherence predictors in bipolar disorders, adverse effects and insight are common themes. In one study 61% of patients prescribed lithium reported slight or moderate side-effects compared with 21% on carbamazepine (Reference Greil and KleindienstGreil & Kleindienst, 1999). Recently Reference Bowden, Collins and McElroyBowden et al(2005) reported premature discontinuation rates of about 70% during a 1-year trial of lithium, placebo and divalproate: 23.2% of those initially dysphoric at entry who received lithium maintenance therapy and 17.1% of those treated with divalproate maintenance therapy discontinued prematurely because of side-effects compared with 4.8% of those treated with placebo. Regarding illness severity and insight, Reference Yen, Chen and KoYen et al(2005) found that insight at baseline predicted concordance up to 1 year later.
Schizophrenia and antipsychotics
Perhaps the most striking data come from studies of full discontinuation by people with schizophrenia. Even in highly monitored randomised controlled trials, discontinuation rates can be greater than 50%. At least five large-scale studies have shown that adherence with both old and new antipsychotics is poor in the long term. For example, Reference Rosenheck, Cramer and XuRosenheck et al(1997) found that 68% of patients treated with haloperidol and 43% of those treated with clozapine had discontinued medication before the end of a 1-year trial. In the 18-month Clinical Antipsychotic Trials for Intervention Effectiveness (CATIE) study (Reference Lieberman, Stroup and McEvoyLieberman et al, 2005) a remarkable 74% of patients discontinued medication prematurely. The most common reasons for discontinuation were patient choice, lack of effect or intolerability of side-effects.
Outside of randomised controlled trials many groups have looked at more subtle forms of poor concordance, including under- and excessive dosing by people with schizophrenia. Seven studies have recruited more than 1000 patients (these are reviewed by Reference Velligan, Lam and GlahnVelligan et al, 2006). Reference Rijcken, Tobi and VergouwenRijcken et al(2004) found that 33% of the patients in their sample had sub-optimal prescription renewals (less than 90%), 56% had good concordance and 11% had excess prescription renewals. Weiden et al (2004b) found that 90% of a sample of 675 individuals with schizophrenia had some degree of partial adherence and on 36% of the study days someone had run out of medication. Patient surveys suggest that almost half (44%) have at some point stopped taking their medication without agreement of their doctor (Reference Hogman and SandamasHogman & Sandamas, 2000).
Predictors of missed antipsychotic medication
There is a concern that people diagnosed with schizophrenia are infrequently involved in treatment decisions and sometimes not even told their diagnosis (Reference Bayle, Chauchot and MaurelBayle et al, 1999). One patient survey (Reference Gray, Rofail and AllenGray et al, 2005) reports that most of the participants prescribed antipsychotics did not feel involved in treatment decisions and had not been given written information about their treatment, warned about side-effects or offered non-pharmacological alternatives.
Several cross-sectional studies link severity of psychopathology to medication non-adherence (Reference Van Putten, Crumpton and YaleVan Putten et al, 1976; Reference Pan and TantamPan & Tantam, 1989). Grandiose thoughts and persecutory thoughts may carry particular risk (Reference Van Putten, Crumpton and YaleVan Putten et al, 1976). Low insight predicts non-adherence and, importantly, improvements in insight are often accompanied by improvements in concordance (Reference Rittmannsberger, Pachinger and KeppelmullerRittmannsberger et al, 2004). However, low insight may be linked to poorer cognitive function and one study suggests that during the first year of treatment, patients with poorer premorbid cognitive functioning are more likely to discontinue (Reference Robinson, Woerner and AlvirRobinson et al, 2002).
Lack of insight has been extensively examined but other factors have been relatively overlooked. Reference PerkinsPerkins (2002) reviewed articles published up to December 2002. Correlates of poor adherence included patients’ beliefs about their illness and the benefits of treatment (insight into illness, belief that medication can ameliorate symptoms), perceived costs of treatment (medication side-effects), and barriers to treatment (ease of access to treatment, degree of family or social support). More recent studies suggest that medication concerns are of prime importance. In a sample of 213 patients with schizophrenia, Reference Lambert, Conus and EideLambert et al(2004) found that those presenting with side-effects and those with past experience of side-effects had a significantly more negative general attitude toward antipsychotics. Reference Loffler, Kilian and ToumiLoffler et al(2003) conducted a study in which 307 people with schizophrenia were asked about their reasons for antipsychotic adherence or non-adherence, using the Rating of Medication Influences scale. A positive relationship with the therapist and a positive attitude of significant others towards antipsychotic treatment contributed to adherence. Reasons for non-adherence were lack of acceptance of the necessity for pharmacological treatment and lack of insight.
Drugs and alcohol
Reference Batel, Reynaud-Maurupt and LavignasseBatel et al(2004) examined risk factors of early dropout during induction of high-dose buprenorphine substitution therapy in 1085 individuals addicted to opiates. Younger age, lack of social support and partial access to care (lack of health insurance, previous contact with the prescriber) were significantly associated with early drop-out. Reference Herbeck, Fitek and SvikisHerbeck et al(2005) looked at predictors in those with dual diagnosis. Patients with treatment adherence problems were significantly more likely to have personality disorders, lower Global Assessment of Functioning scores, and medication side-effects than those who adhered to treatment. In a study of after-care attendance by severely substance-dependent residential treatment clients, Reference Sannibale, Hurkett and van den BosscheSannibale et al(2003) found that younger, male, heroin-dependent clients with poly-drug use who had refused opioid pharmacotherapy were more likely to drop out of treatment and to relapse early following treatment.
Discussion
Rates of non-adherence with psychotropic medication are difficult to summarise because they vary by setting, diagnosis and type of adherence difficulty. The overall weighted mean rate of non-adherence, calculated in a sample of 23 796 patients with psychosis from a systematic literature review was 25.78% (Reference Nose, Barbui and TansellaNose et al, 2003). Complete discontinuation of medication is thought to lead to about one in ten hospital admissions and one in five nursing home admissions (Reference Sullivan, Kreling and HazletSullivan et al, 1990). Reference Fenton, Blyler and HeinssenFenton et al(1997) found that non-adherent individuals with schizophrenia have a 3.7-fold greater risk of relapse than those who are adherent over 6–24 months. Where medication (or appointments) are missed for predominantly illness-related reasons such as lack of insight, there is a particularly high risk of readmission. Yet illness severity probably accounts for a minority of cases of poor adherence in the community (Reference Maddox, Levi and ThompsonMaddox et al, 1994). Further, the impact may be ameliorated if patients who have further symptoms seek help. Unfortunately, adverse experiences with medication may prejudice willingness to attend in the future (Reference Gonzalez, Williams and NoelGonzalez et al, 2005).
Potential solutions
A comprehensive summary of interventions that may reduce poor adherence is beyond the scope of this article. Advanced strategies such as adherence therapy and depot medication are reviewed by Reference O'Ceallaigh and FahyO'Ceallaigh & Fahy (2001) and Reference Nadeem, McIntosh and LawrieNadeem et al(2006). Many of the simpler interventions available to enhance adherence are listed in Box 3.
Box 3 Simple strategies to improve concordance
Basic communication
-
• Establish a therapeutic relationship and trust
-
• Identify the patient's concerns
-
• Take into account the patient's preferences
-
• Explain the benefits and hazards of treatment options
Strategy-specific interventions
-
• Adjusting medication timing and dosage for least intrusion
-
• Minimise adverse effects
-
• Maximise effectiveness
-
• Provide support, encouragement and follow-up
Reminders
-
• Consider adherence aids such as medication boxes and alarms
-
• Consider reminders via mail, email or telephone
-
• Home visits, family support, counselling
Evaluating adherence
-
• Ask about problems with medication
-
• Ask specifically about missed doses
-
• Ask about thoughts of discontinuation
-
• With the patient's consent, consider direct methods: pill counting, measuring serum or urine drug levels
-
• Liaise with general practitioners and pharmacists regarding prescriptions
Barriers to healthcare are a reversible cause of poor medication and appointment adherence. Common factors that reliably influence adherence include patient expectation and knowledge (perception of benefits and hazards of therapy), involvement in medical decisions, availability of social support, and complexity and duration of the prescribed regime.
In the past it has been common to blame the individual for discontinuing medication or dropping out of treatment against medical advice (Reference DemyttenaereDemyttenaere, 1998). In addition, patients who do not follow medical advice are likely to be discharged early, compounding the problem. In the future this may be seen as inadequate care. Not too long ago it was considered unusual to give the patient information about their condition or, in some cases, even to reveal the truth about a diagnosis, despite the patient's requests (Reference MitchellMitchell, 2007b ).
Doctors do not diagnose perfectly or prescribe carefully all of the time (Reference Nirodi and MitchellNirodi & Mitchell, 2002; Reference Grasso, Genest and JordanGrasso et al, 2003; Reference Laurila, Pitkala and StrandbergLaurila et al, 2004). Thus the patient is not always acting irrationally if they attempt to allow for adverse effects or minimise stigma by adjusting doses or times of administration. Adverse effects are problematic in at least half of those taking psychotropic medication and may be a rational reason for their choosing to discontinue medication (Reference Greil and KleindienstGreil & Kleindienst, 1999; Reference Bull, Hu and HunkelerBull et al, 2002a ; Reference Lambert, Conus and EideLambert et al, 2004). It may be surprising therefore that only about a quarter of those discontinuing antidepressants or antipsychotics cite adverse effects as the reason (Reference Maddox, Levi and ThompsonMaddox et al, 1994). In other words, only a minority of those experiencing significant adverse effects will discontinue medication without advice.
A substantial minority (about a quarter to a half) do not tell their doctor after stopping or interrupting medication (Reference Hogman and SandamasHogman & Sandamas, 2000; Reference Demyttenaere, Enzlin and DeweDemyttenaere et al, 2001). In part this may be fear of rejection or being disbelieved, or embarrassment about discussing adverse effects such as weight gain or sexual problems (Reference Zimmermann, Kraus and HimmerichZimmermann et al, 2003; Reference Weiden, Mackell and McDonnellWeiden et al, 2004a ). A contributing factor may be that the frequency of side-effects such as these is greatly underestimated by doctors (Reference Smith, O'Keane and MurraySmith et al, 2002; Reference RooseRoose, 2003). About half of people who stop their medication after taking it for more than a month do so intentionally (Reference Barber, Parsons and CliffordBarber et al, 2004). Even when patients have discontinued medication unexpectedly, studies in general medicine suggest that more than half will offer some kind of rational explanation.
Clearly the emerging concept of partial adherence requires further study. The available evidence suggests that the outcome for patients who vary medication doses without consulting a professional is poorer (Reference Svarstad, Shireman and SweeneySvarstad et al, 2001). However, many patients vary regular medication in a flexible as-required manner apparently without harmful effect (Reference MitchellMitchell, 2007a ).
The therapeutic alliance
The early period of contact between clinician and patient is important in terms of forming a therapeutic alliance and making a joint therapeutic plan. Most patients with mental health problems themselves recognise the difficulty in adhering to complex medication regimens (Reference Irani, Dankert and BrensingerIrani et al, 2004). Before starting a new psychotropic drug we suggest that clinicians should explicitly acknowledge to the patient the difficulties of taking medication, outline realistic benefits and discuss possible adverse effects and consideration of treatment alternatives. Patients who receive this kind of communication are more knowledgeable and have more positive initial beliefs about their medication (Reference Bultman and SvarstadBultman & Svarstad, 2000). Yet analysis of doctor–patient discourses illustrates that clinicians prescribing antidepressants ask roughly one in five patients how well the drugs are working and only one in ten whether they are experiencing any side-effects (Reference Sleath, Rubin and HustonSleath et al, 2003; Reference Young, Bell and EpsteinYoung et al, 2006). These questions may be even more rarely asked of patients in minority ethnic groups and in vulnerable groups such as those with intellectual disability (Reference Lewis-Fernandez, Das and AlfonsoLewis-Fernandez et al, 2005).
Once a person has started a course of psychotropic medication we recommend that regular follow-up contact with a clinician be arranged. In clozapine treatment, weekly rather than fortnightly monitoring reduced discontinuation rates by 10% over the course of a year and up to 50% overall (Reference Patel, Crismon and MillerPatel et al, 2005).
Given the relatively high rates of missed medication and missed appointments in psychiatry we suggest that methods are developed that help patients who have adherence/attendance difficulties. These should be applicable to routine clinical care. Research will then be required to discover which methods are most effective in each setting. Further, we suggest caution before automatically discharging patients who have had initial difficulty following medical advice: at the very least clinicians should ascertain whether there are any removable barriers to continuing care.
Declaration of interest
None.
MCQs
-
1 Low concordance with prescribing advice is predicted by:
-
a a short course of medication
-
b low number of doses per day
-
c regular contact with a healthcare professional
-
d concomitant psychological treatment
-
e young age.
-
-
2 The following are linked with intentional non-adherence:
-
a severity of illness
-
b high trust in physicians
-
c a desire for self-efficacy
-
d receipt of adequate levels of drug information
-
e missed doses after long period on treatment.
-
-
3 Regarding patients’ understanding of drug therapy:
-
a the majority of patients leaving hospital on medication understand why they are taking it
-
b most of those taking clozapine are aware of its potentially serious haematological side-effects
-
c it is usual for people with depression to understand their need for regular antidepressant therapy
-
d antidepressants are commonly perceived as addictive
-
e in general patients can recall significant information given by clinicians.
-
-
4 Regarding the treatment of schizophrenia:
-
a patient-initiated discontinuation of medication is a rare event
-
b taking too much medication is a recognised form of less-than-ideal adherence
-
c a clinician may reasonably assume that patients use all medication at the prescribed dose and time
-
d repeat prescription data show that almost all patients underuse medication
-
e periods of missed medication typically last a few days.
-
-
5 Patients with schizophrenia commonly report that:
-
a they understand the purpose of the medication they are taking
-
b their diagnosis is not explained to them
-
c they are given written information about their treatment
-
d they are involved in treatment decisions
-
e they are routinely offered non-pharmacological treatment.
-
MCQ answers
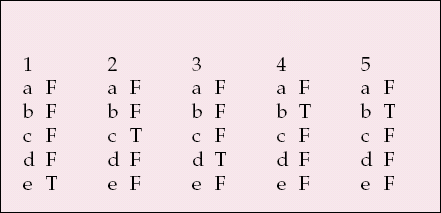
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | F |
| b | F | b | F | b | F | b | T | b | T |
| c | F | c | T | c | F | c | F | c | F |
| d | F | d | F | d | T | d | F | d | F |
| e | T | e | F | e | F | e | F | e | F |




eLetters
No eLetters have been published for this article.